ABSTRACT
Purpose: To explore the frequency and patterns of ultrasound (US) usage among physical therapists, to describe the most common purposes for using therapeutic US, and to investigate beliefs about therapeutic US. Methods: A survey was sent to 95% of physical therapists licensed to practise in the province of Alberta, Canada. Results: Of 2,269 physical therapists to whom email invitations were sent, 438 (19.3%) provided full responses. Results indicate that US is still frequently incorporated into treatment regimens and is widely believed to be effective; however, the study also found a decrease in US usage over the past 15 years. While physical therapists recognize the lack of evidence for the effectiveness of US, many consider it clinically useful. Physical therapists using US rely largely on their clinical experience when making decisions about its use, but this depends on level of education: clinicians with an MScPT degree tended to base more of their US decisions on research evidence, likely because of the increasing emphasis on research evidence in graduate education. Conclusions: Despite the questionable effectiveness of therapeutic US, physical therapists still commonly use this treatment modality, largely because of a belief that US is clinically useful. However, US usage has decreased over the past 15 years.
Key Words: ultrasonic therapy, surveys, beliefs
RÉSUMÉ
Objectif : Explorer la fréquence et les tendances de l'utilisation de l'échographie chez les physiothérapeutes, décrire les raisons thérapeutiques les plus courantes d'utiliser l'échographie thérapeutique et analyser les croyances relatives à l'échographie thérapeutique. Méthodes : On a envoyé un questionnaire à 95% des PT autorisés à pratiquer en Alberta, au Canada. Résultats : Sur 2 269 physiothérapeutes qui ont été invités par courriel, 438 (19,3%) ont répondu au questionnaire au complet. Les résultats indiquent que l'échographie fait toujours partie fréquemment des protocoles de traitement et que l'on croit généralement qu'elle est efficace. L'étude a toutefois révélé aussi une baisse de l'utilisation de l'échographie au cours des 15 dernières années. Les physiothérapeutes reconnaissent peut-être le manque de données probantes sur l'efficacité de l'échographie, mais beaucoup d'entre eux la jugent utile sur le plan clinique. Les physiothérapeutes qui utilisent l'échographie s'en remettent en grande partie à leur expérience clinique lorsqu'ils prennent une décision sur son utilisation, mais tout dépend du niveau d'éducation: les cliniciens qui ont une maîtrise en physiothérapie ont tendance à fonder davantage leur décision d'y recourir sur des données de recherche, probablement parce qu'on accorde de plus en plus d'importance aux données de recherche au cours des études supérieures. Conclusions : En dépit de l'efficacité douteuse de l'échographie thérapeutique, les physiothérapeutes utilisent encore couramment ce mode de traitement, surtout parce que l'on croit qu'elle utile sur le plan clinique. L'utilisation de l'échographie a toutefois diminué au cours des 15 dernières années.
Mots clés : échographie, sondage, croyance
Ultrasound (US) refers to mechanical vibrations (i.e., sound waves) below the range of human hearing, commonly at either 1 or 3 MHz (millions of cycles per second).1 These waves travel through tissue and are preferentially absorbed in dense collagen structures with lower water content and high protein content (i.e., tendons, ligaments, joint capsules).2 Therapeutic US has a long history of use in physical therapy practice; its clinical application has evolved over the past several decades, from being used as a thermal modality to being employed for its non-thermal effects, particularly in tissue repair and wound healing.2
Therapeutic US has become one of the most commonly used electrophysical modalities; surveys carried out in different countries have consistently identified it as a central component of physical therapy practice.3–7 Therapeutic US has been applied to a wide range of health conditions, including acute, sub-acute, and chronic musculoskeletal conditions. Benefits of therapeutic US have been claimed for a variety of phenomena, including wound healing,8 soft-tissue lesion management,9,10 increasing soft-tissue extensibility,11,12 remodelling scar tissue,9,13 diagnosing stress fractures,14,15 and pain relief.16–18
Yet the clinical effectiveness of therapeutic US remains questionable.1,19–23 Overall, results of clinical studies have been mixed; only a few well-designed clinical studies have demonstrated positive effects on clinical outcomes.16,24,25 Several of the studies showing significant support for US application, particularly in the area of enhancing repair of soft tissue following injury, have been laboratory (i.e., cellular or animal) studies with questionable relevance to humans.26–32 The discrepancy in results between experimental and clinical studies warrants further research to clarify the therapeutic effectiveness of US in clinical practice. The limited clinical evidence also raises questions about why US is commonly used in clinical practice.
Previous surveys of therapists' US usage patterns have not explored in depth physical therapists' reasons for continuing to use US. Finding out why physical therapists value US so highly is an important step toward understanding the discrepancy between the clinical evidence and current practice. Lindsay and colleagues' (1995) report of US usage among private-practice physical therapists in Alberta, Canada, indicated very high levels of usage (94% reported using US at least once per day).3 This information is somewhat dated, however, and no information is available from therapists working in other practice settings. Moreover, the information was drawn from a survey of overall use of electrotherapy modalities that did not focus only on US and did not explore respondents' beliefs about therapeutic US. To overcome these limitations, we conducted a survey to investigate current usage patterns and beliefs about US use.
Our specific objectives in this study were (1) to measure the frequency and patterns of US usage among physical therapists licensed to practise in the province of Alberta, Canada, who had valid email addresses registered with the regulatory body; (2) to describe the most common therapeutic purposes for using US; (3) to investigate beliefs about therapeutic US and whether practice setting (private practice vs. other practice types) or the educational level of the therapist influenced US usage; and (4) to examine differences between therapists who report using US and those who report never using it.
Methods
This exploratory population-based cross-sectional survey study was approved by the University of Alberta Health Research Ethics Board.
Target population
The survey was sent to all physical therapists licensed to practice physical therapy in Alberta who had valid email addresses listed with the regulatory body at the time of the study (October–December 2010).
Data collection
We developed a survey based on information from a literature review and discussions with experts in the field, including researchers who had previously conducted surveys of US usage among physical therapists. The authors of earlier surveys7,33 provided copies of their survey questions, along with permission to use or modify the questions for our study. We pilot-tested our survey with a convenience sample of 25 practising physical therapists, who gave feedback on content and form in four group discussion sessions. After the first pilot group, we made minor modifications to questions to improve flow and clarity, as well as minor grammatical changes to three questions; this revised version was then tested in the next three pilot groups. After the fourth pilot session, which generated no new suggestions for modifications, further pilot testing was deemed unnecessary and the survey questions were considered relevant for the objectives of the study. A copy of the survey is provided in Appendix 1 (online only).
The survey had four main sections. The first section gathered information on the use of US. The second asked about use of US for each of the following impairments or therapeutic purposes: to control acute inflammation, to improve chronic inflammation, to enhance fibroblast proliferation and improve collagen synthesis, to modulate acute pain, to modulate chronic pain, to remodel soft tissue or scar tissue, to increase extensibility of soft tissue or scar tissue, to meet patients' expectations, for placebo effect, or for other reasons. The third section assessed beliefs about the clinical importance of therapeutic US for managing these impairments; the fourth collected general demographic data.
Since most licensed physical therapists in Alberta (95%) have email addresses registered with the regulatory board, we distributed the survey electronically using SurveyMonkey. On October 21, 2010, one investigator (DG) sent an email to all registered physical therapists describing the study and providing a link to access the survey. We gave respondents 3 months to complete the survey, and sent two reminders (on October 28 and November 19, 2010).
Data analysis
Our analysis was primarily descriptive in nature, using percentages, means, and standard deviations to quantify responses to various survey items. Data were analyzed only for those who responded; we did not impute or replace missing data. To determine whether there were differences by level of education (diploma vs. BSc vs. MSc) in US usage, beliefs about US and perceptions of effectiveness, we constructed contingency tables and conducted chi-square or Fisher exact tests to test for significance between factors. In addition, we conducted chi-square or Fisher exact tests to determine whether sample characteristics such as gender, age, practice area, conditions treated, training location, and beliefs about US and perceptions of the effectiveness of US were different between respondents who reported using US and those who reported never using it, or between those who work in private practice and those who work in other settings. The alpha level was set at α=0.05. We performed our analyses using the Statistical Package for the Social Sciences, version 17 (SPSS Inc., Chicago, IL) and STATA 10 (StataCorp LP, College Station, TX) statistical software.
Results
General population demographics
Of the 2,269 physical therapists to whom we sent email invitations, 558 (25%) responded to the survey; of these, 438 (19%) had no missing data. There was no statistically significant difference between those with and without missing data in terms of US usage (18% and 17% respectively reported not using US, p=0.83).
Respondents were predominantly women (338, 77%), and most (271, 61%) fell into the 31–50 age range. The primary areas of practice were private practice (237, 53%) and hospital practice (114, 25%); the primary caseload was musculoskeletal conditions (297, 66%). Approximately 67% (300) held a BSc in physical therapy, 23% (104) held either an MSc or an MHSc in physical therapy, and 9% (39) had a diploma in physical therapy; only 1% of all respondents (4) held a PhD. For full demographic details, see Tables 1 and 2.
Table 1.
Respondent Characteristics Stratified by Ultrasound Use
| % of respondents* |
|||
|---|---|---|---|
| Characteristics | Entire sample (n=438) |
Use US (n=365) |
Never use US (n=73) |
| Sex | |||
| Female | 77.2 | 77.3 | 76.7 |
| Age category, y | |||
| 20–30 | 16.5 | 17.0 | 13.7 |
| 31–40 | 35.4 | 36.4 | 30.1 |
| 41–50 | 25.1 | 24.1 | 30.1 |
| 51–60 | 17.8 | 18.1 | 16.4 |
| >60 | 5.3 | 4.4 | 9.6 |
| Years in practice | |||
| <1 | 4.1 | 4.1 | 4.1 |
| 1–3 | 8.0 | 8.5 | 5.5 |
| 4–9 | 21.7 | 21.9 | 20.5 |
| 10–15 | 19.6 | 20.8 | 13.7 |
| >15 | 46.6 | 44.7 | 56.2 |
| Practice setting† | |||
| Private physical therapy clinic | 53.1 | 58.4 | 9.6 |
| Hospital | 25.4 | 21.4 | 37.0 |
| Community health centre | 5.8 | 4.9 | 8.2 |
| Rehabilitation facility | 5.8 | 4.9 | 8.2 |
| Home care | 4.8 | 4.1 | 6.8 |
| Long-term care facility | 2.7 | 1.9 | 5.5 |
| Pediatrics | 2.4 | 0.5 | 11.0 |
| Other (academic, rheumatology, etc.) | 5.5 | 3.8 | 13.7 |
| Area of practice† | |||
| Musculoskeletal | 66.4 | 74.8 | 35.6 |
| Geriatrics / long-term care | 5.9 | 5.5 | 8.2 |
| Neurological | 4.8 | 3.3 | 12.3 |
| Rheumatologic | 4.8 | 5.2 | 2.7 |
| Mixed caseload | 3.4 | 2.5 | 8.2 |
| Chronic pain | 3.2 | 3.3 | 2.7 |
| Hands/burns | 3.0 | 3.3 | 1.4 |
| Paediatrics | 2.7 | 0 | 16.4 |
| Cardiorespiratory | 1.4 | 0.5 | 5.5 |
| Women's health | 0.9 | 0.8 | 1.4 |
| Administration | 0.9 | 0 | 5.5 |
| Other (oncology, teaching, etc.) | 0.7 | 0.8 | 0 |
| Level of education | |||
| Diploma | 8.7 | 9.3 | 5.5 |
| Bachelor's degree | 67.1 | 66.3 | 71.2 |
| Master's degree | 23.3 | 23.8 | 20.5 |
| Other (PhD, DSc, etc.) | 0.9 | 0.5 | 2.7 |
| Training location | |||
| Canada | 84.9 | 84.4 | 87.7 |
| United Kingdom | 5.5 | 4.9 | 8.2 |
| Australia or New Zealand | 2.1 | 2.2 | 1.4 |
| Africa | 1.8 | 2.2 | 0 |
| India or Pakistan | 1.6 | 1.6 | 1.4 |
| United States | 1.1 | 1.4 | 0 |
| Mainland Europe | 0.9 | 1.1 | 0 |
| South America | 0.7 | 0.8 | 0 |
| Other (Jamaica, China, etc.) | 1.4 | 1.4 | 1.4 |
| Has taken post-graduate course on US | 39.3 | 40.5 | 32.9 |
n=558; data are for 438 respondents (79%) with no missing data.
Indicates statistically significant difference between those who reported using therapeutic US and those who reported not using therapeutic US.
US=ultrasound.
Table 2.
Respondent Characteristics Stratified by Practice Setting (n=438)
| % of respondents |
||
|---|---|---|
| Characteristics | Private practice (n=220) |
Other setting (n=218) |
| Frequency of US use* | ||
| Never | 3.2 | 30.3 |
| Daily | 60.9 | 16.1 |
| Weekly | 23.2 | 21.1 |
| Monthly | 9.1 | 12.4 |
| Yearly | 3.6 | 20.2 |
| Sex | ||
| Female* | 70.9 | 83.5 |
| Age category,* y | ||
| 20–30 | 22.3 | 10.6 |
| 31–40 | 40.0 | 30.7 |
| 41–50 | 23.2 | 27.1 |
| 51–60 | 11.8 | 23.9 |
| >60 | 2.7 | 7.8 |
| Years in practice* | ||
| <1 | 6.4 | 1.8 |
| 1–3 | 9.1 | 6.9 |
| 4–9 | 24.1 | 19.3 |
| 10–15 | 22.3 | 17.0 |
| >15 | 38.2 | 55.0 |
| Area of practice* | ||
| Musculoskeletal | 93.6 | 42.7 |
| Geriatrics / long-term care | 0 | 11.9 |
| Neurological | 0.9 | 8.7 |
| Rheumatologic | 0 | 9.6 |
| Mixed caseload | 0.5 | 6.4 |
| Chronic pain | 3.2 | 3.2 |
| Hands/burns | 0.5 | 5.5 |
| Paediatrics | 0 | 5.5 |
| Cardiorespiratory | 0 | 2.8 |
| Women's health | 1.4 | 0.5 |
| Administration | 0 | 1.8 |
| Other (oncology, teaching, etc.) | 0 | 1.4 |
| Level of education* | ||
| Diploma | 5.9 | 11.5 |
| Bachelor's degree | 63.2 | 71.1 |
| Master's degree | 29.5 | 17.5 |
| Other (PhD, DSc, etc.) | 1.4 | 0.5 |
| Training location | ||
| Canada | 83.2 | 86.7 |
| Elsewhere | 16.8 | 13.3 |
| Has taken post-graduate course on US* | 33.6 | 45.0 |
Indicates statistically significant difference (p<0.05) between private practice and other setting.
US=Ultrasound.
Demographics by ultrasound usage and practice setting
Table 1 shows respondent demographics stratified by reported US use, while Table 2 shows the same data stratified by practice setting (private practice vs. other). Most respondents who reported using US work in private practice (58%) and treat mainly musculoskeletal conditions (75%), whereas most of those who do not use US work in hospital settings (37%). In addition, a slightly higher percentage of therapists who reported using US than of those who did not had taken a post-graduate course on US (41% vs. 33%). Therapists working in private practice reported significantly higher use of US than those working in other settings: approximately 61% reported using US daily.
Ultrasound usage: General sample
A high proportion of respondents (499, 89%) had access to an US machine in their area of practice. In addition, 196 (36%) reported using US at least daily, and 124 (23%) at least weekly. On the other hand, 94 respondents (18%) reported that they never used US (see Table 3). Among the reasons respondents gave for not using US were that US is not applicable to their practice (73, 78%), that US is not effective in their clinical experience (20, 21%), that they achieve better results with other modalities (12, 14%), that US is too time consuming (7, 7%), and that US equipment is not available in their clinic (3, 3%).
Table 3.
Ultrasound Access and Usage for All Respondents
| Variable | Mean (range) | No. (%) |
|---|---|---|
| US access in area of practice | ||
| Yes | 499 (89.4) | |
| No | 59 (10.6) | |
| Therapists who use US in practice | ||
| At least daily | 196 (36.4) | |
| At least weekly | 124 (23) | |
| At least monthly | 57 (10.6) | |
| At least yearly | 67 (12.4) | |
| Never | 94 (17.6) | |
| Who applies the US treatment? | ||
| I apply it myself | 247 (55.4) | |
| The PTA or other support staff | 13 (2.9) | |
| Combination | 186 (41.7) | |
| Patients treated with US per day | 11 (0–40) | |
| % of patients treated with US | 40 (5–95) |
US=ultrasound; PTA=physiotherapy assistant.
General use of ultrasound for therapeutic purposes
Of those who reported using US, the largest proportion (74%) said they use it to resolve acute inflammation (see Figure 1). Most therapists answering this question (90%) believed that US is moderately to highly effective in accomplishing this therapeutic purpose. Remodelling soft tissue and scar tissue was also reported to be a very important reason for using US (74%); 95% believed that US is moderately (41%) to highly (55%) effective for this purpose. (For details of therapists' perception of US effectiveness, see Table 4).
Figure 1.
Percentage of therapists using ultrasound for different therapeutic objectives
Table 4.
Therapists' Perceptions of the Effectiveness of Ultrasound for Specific Impairments or Specific Therapeutic Goals
| % (no.) of responses |
||||
|---|---|---|---|---|
| Impairment or purpose | Total responses (no.) | US not effective | US moderately effective | US highly effective |
| Acute inflammation | 307 | 9 (29) | 46 (142) | 44 (136) |
| Chronic inflammation | 251 | 12 (29) | 46 (115) | 43 (107) |
| Promote fibroblast and collagen synthesis | 233 | 12 (27) | 50 (117) | 38 (89) |
| Modulate acute pain | 146 | 7 (10) | 51 (74) | 42 (62) |
| Modulate chronic pain | 95 | 9.5 (9) | 41 (39) | 49.5 (47) |
| Remodel soft tissue or scar tissue | 291 | 4.5 (14) | 41 (119) | 54.5 (158) |
| Increase extensibility | 249 | 4.4 (11) | 40 (99) | 55.6 (138) |
| Meet patient's expectations | 145 | 6 (9) | 27 (39) | 67 (97) |
| Placebo effect | 71 | 8.5 (6) | 34 (24) | 57.5 (41) |
| Other (e.g., muscle spasm) | 63 | 8 (5) | 29 (18) | 63 (40) |
US=ultrasound.
A total of 65% of respondents reported using therapeutic US to increasing the extensibility of soft tissue and scar tissue. Control of chronic inflammation (61%) was also considered an important therapeutic goal; 89% considered US moderately to highly effective for this purpose. In addition, 59% of therapists reported using US to promote fibroblast proliferation, 37% for modulating acute pain, and 37% to meet patient expectations. A smaller number used US to obtain a placebo effect (18%) or to modulate chronic pain (24%; see Figure 1).
Why US is used: Opinion and confidence when using US
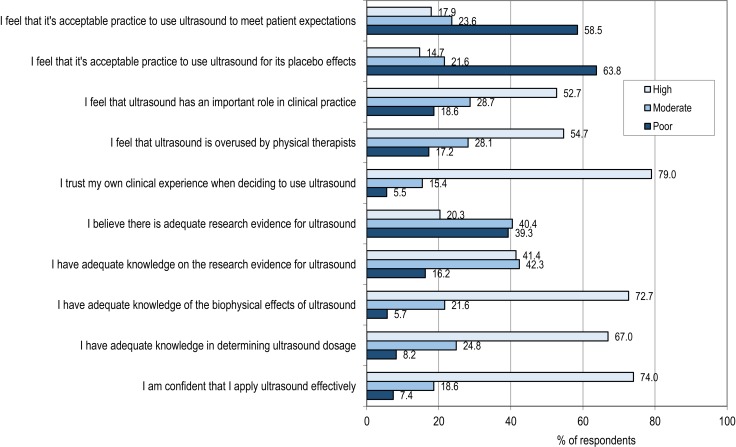
When asked about their opinions of US treatment and how confident they were that they apply US effectively, most respondents (74%, 322/435) reported feeling highly confident that they apply US effectively (see Figure 2); 67% felt they had adequate knowledge to determine US dosage. Similarly, 73% of respondents reported having “adequate knowledge about biophysical effects.” Responses to the survey item asking about “adequacy of knowledge about the research evidence” for use of US varied: 16% of respondents felt their knowledge was not adequate, 42% reported “moderately adequate” knowledge, and 41% felt they had adequate knowledge about the research evidence for US use.
Figure 2.
Therapists' opinions about ultrasound.
Respondents also had mixed beliefs about whether or not there is adequate research evidence to support the use of US: 39.3% reported believing there is not adequate research evidence, while 20.3% believe there is. While 64% of respondents (278) consider it unacceptable to use US for placebo and 59% (255) believe it is unacceptable to use it to meet patient expectations, 21% (94) feel that is acceptable practice to use US for its placebo effect, and 51% (223) reported using US at patients' request.
Sources of knowledge about US
When making clinical decisions about US use, respondents most commonly (∼40%) used clinical experience as a source of knowledge (see Figure 3), followed by undergraduate training (19%), the research evidence base (13%), continuing-education courses (10%), opinion of experts or colleagues (6%), and electrotherapy books (6%).
Figure 3.
Sources of knowledge used when applying US.
The influence of level of education
When we analyzed the influence of level of education (diploma vs. BSc vs. MSc) on respondents' attitudes toward, beliefs about, and use of US, we found no statistically significant difference in the frequency of US usage (Fisher exact=0.75) or in level of confidence when applying US (Fisher exact=0.53). However, there was a statistically significant difference in adequacy of knowledge for determining US dosage (p=0.020) and adequacy of knowledge on the research evidence for US (p=0.05): approximately 65% of respondents with a BSc believed they had adequate knowledge, versus 52% of those with an MSc, and approximately 37% of respondents with a BSc rated their knowledge of the research evidence as adequate, versus 59% of those with an MSc. However, there were no significant differences in respondents' views on whether US has an important role in clinical practice (Fisher exact=0.36). Nor did we find any difference in their views on whether it is acceptable to use US for its placebo effect (Fisher exact=0.05); nevertheless, when respondents were asked if they themselves had used US for this purpose, there was a statistically significant difference by level of education (Fisher exact=0.009): those holding a diploma or BSc were less likely than those with an MSc to report using US for its placebo effect (7%, 20%, and 29% respectively, p=0.003).
There were significant differences by level of education in respondents' feelings about using US to meet patient expectations (Fisher exact=0.007): the majority (70%) of those holding a diploma considered this unacceptable, while the remaining 30% considered it moderately (27.03%) or highly acceptable (2.70%). Smaller majorities of those holding a BSc (58.60%) or MSc (47.87%) also considered this practice unacceptable.
We also found significant differences by level of education in respondents' preferred sources of knowledge for deciding whether or not to use US (Fisher exact = 0.001). Comparing the highest preferences (graduate training, clinical experience, and research evidence base) across levels of education revealed significant differences in the use of these sources of knowledge between diploma and BSc holders (Fisher exact=0.001) and between diploma and MSc holders (p<0.001). While 72% of respondents holding a diploma use their clinical experience when deciding whether to use US, those with a BSc or MSc—although still relying mostly on clinical experience (55% and 54% respectively)—also rely on entry-level training (30% and 39% respectively) and the research evidence base (15% and 7% respectively).
Ultrasound usage: Beliefs and opinions about US
When we analyzed the data dividing the population between those who use US on a regular basis and those who do not use it at all, we found statistically significant differences in confidence in applying US, knowledge for determining US dosage, knowledge of the biophysical effect of US, knowledge of the research evidence for US, beliefs about adequacy of evidence for US, trusting clinical experience to decide on use of US, belief that US plays an important role in clinical practice, and belief that using US to meet patient expectations is acceptable. Practitioners who normally use US had higher levels of confidence in, knowledge of, and positive beliefs about US than those who never use it; furthermore, respondents who use US place more trust in clinical experience when deciding whether to use US (43% vs. 23%, p=0.013), while those who never use US reported using their entry-level training significantly more than respondents who do use US (36% vs. 16%, p=0.030).
Practice setting: Beliefs and opinions about US
When we analyzed the data stratified by practice setting (private practice vs. other settings), we found statistically significant differences in confidence in applying US, knowledge for determining US dosage, knowledge of the research evidence for US, opinions on whether US is overused in clinical practice, and beliefs about whether US use is acceptable for placebo effect and to meet patient expectations. Respondents working in private practice generally had higher levels of confidence in, knowledge of, and positive beliefs about US than those working in other settings (see Appendix 2 online).
Discussion
Therapeutic US continues to be commonly used by practising physical therapists. Although a high proportion of respondents to our survey had access to US (85%) and considered US use relevant to their practice (81%), the proportion who use US daily (36%) was lower than proportions reported in previous surveys (84–95%).3,33 This is probably because our survey targeted all physical therapists in Alberta, regardless of specialization area, and therefore involved physical therapists working in areas where US may not be relevant. In fact, 78% of respondents who reported not using US also said that US was not applicable to their practice setting. Even among respondents working in private practice, however, only ∼61% reported daily use of US, which indicates that daily use is diminishing. Factors that may be contributing to this decreased use of US are unconvincing evidence for its effectiveness (35% of our respondents reported that US was not effective in their clinical experience and that they prefer other modalities to accomplish therapeutic objectives) and a lower rate of access to US equipment (81%) relative to that reported in other surveys (99%).3,33
General use of US for therapeutic purposes
The majority of therapists surveyed use US for resolving acute inflammation, remodelling or modifying soft tissue or scar tissue, and increasing the extensibility of soft tissue or scar tissue. These findings concur with those of previous surveys in which physical therapists considered US clinically important for managing acute inflammation and chronic scar tissue.7,34 The use of US in the inflammatory process is not surprising, since clinicians believe that US has some anti-inflammatory properties. Experimental evidence, however, points in the opposite direction: for example, the application of US has been associated with a stimulating effect on mast cells, platelets, and inflammatory mediators.13,35 In fact, it is believed that US may optimize the inflammatory process, allowing tissues to move into their new phase (proliferation) more efficiently.2,13 It is not known whether the widespread use of US by physical therapists in the inflammatory phase is intended as an “inflammatory catalyzer” or whether it is used for its erroneously perceived “anti-inflammatory” effects.
Although rates of US usage to treat the above conditions are very high, existing research evidence on the clinical effectiveness, parameters, and clear biophysical effects of US does not provide strong support for using US for these objectives; it is not known whether the application of US for these therapeutic objectives makes a difference to patients' health outcomes. It is surprising, therefore, that a high proportion of therapists (74%) felt confident that they apply US effectively, have adequate knowledge to determine US dosage (67%), and have adequate knowledge of the biophysical effects of US (73%), yet also reported that US does not have adequate evidence. In addition, when we asked participants about their opinions on US use, a high proportion (79%) reported that they trust their own experience when deciding whether to use US (see Figure 2). This indicates that therapists who use US do so confidently while recognizing that there is limited research evidence supporting its use. Despite reduced US usage, there is still opportunity for knowledge-transfer activities aimed at disseminating research results for uptake in daily practice by clinicians.36,37
Beliefs about the effectiveness of US as a treatment modality
Most respondents reported that they consider US moderately to highly effective for achieving specific treatment goals, echoing the findings of Warden and McMeeken's survey33 on the use of US for acute inflammation and for improving fibroblast proliferation: similar proportions of respondents in both surveys (81% and 74% for inflammation; 59% and 44% for fibroblast proliferation) reported using US to treat these conditions. However, there is an important difference between surveys in the use of US for treating pain: a majority of Warden and McMeeken's respondents reported using US to treat acute and chronic pain (74% and 66% respectively),33 while a much lower proportion of our respondents did so (37% and 24% respectively). In addition, a lower proportion of our respondents (65%, vs. 82% in Warden and McMeeken's study33) used US for tissue extensibility in chronic stages. These discrepancies may be explained by the specialty areas of respondents, as Warden and McMeeken's survey focused on sport physical therapy, an area where pain and connective-tissue disorders are likely common.33 In addition, sport physical therapists generally take a more aggressive treatment approach, and their patients (athletes) must often be treated very quickly for various musculoskeletal problems. Our survey respondents, in contrast, work in many practice areas, and some may not treat pain or connective-tissue disorders frequently.
Interestingly, a relatively large proportion of respondents in our survey considered US highly effective for meeting patients' expectations (67%) and as a placebo (58%); these values are higher than those for other therapeutic objectives, which may be one reason that clinicians continue to use US in practice. This is important because providers' personal beliefs and expectations can influence the outcome of therapy and placebo analgesia;38–40 thus, therapists' positive expectations of US may translate to patients, possibly producing an enhanced placebo effect and resulting in therapeutic benefits. It is also plausible that the use of new, expensive, and technologically impressive US machines in physical therapy treatments may build an adequate psychosocial context to help motivate patients to achieve better outcomes. Thus, US may have an important placebo effect, and this could contribute to the perception of its effectiveness among physical therapists.
Sources of knowledge used in making decisions about US
The majority of respondents reported basing their decisions about use of US on clinical practice experience (∼40%); the next most common sources of knowledge reported were undergraduate training (19%) and research evidence (13%). Our results confirm that therapists who commonly use US are more likely than those who do not use it to base decisions on their clinical experience (43% vs. 23%, p=0.013), which highlights the need to improve transfer of research knowledge into clinical practice and educate the clinical community on the importance of evidence and of implementing research findings in real-world situations.36 Although the trend toward evidence-based practice seen among BSc and MSc degree holders is encouraging, additional knowledge-translation efforts, such as workshops or continuing-education modules, may be needed to change clinical practice,36,41 since physical therapists have rated “courses” as the most important method of keeping up to date in clinical practice.36
Levels of education and differences in US use
Respondents holding a BSc reported greater “adequacy of knowledge in determining US dosage” than those holding an MSc. There could be many possible reasons for MSc degree holders to feel less confident in determining US dosage, one of which is that the lack of evidence on optimal dosimetry for US is widely discussed during the physical therapy entry-level programme at the University of Alberta;42 this suggestion is speculative, and additional research is needed to confirm it. In addition, BSc holders may have more years of clinical experience than MSc graduates, and thus feel more confident in applying US.
As expected, we found significant differences by level of education in respondents' preferred sources of knowledge: physical therapists with higher levels of education use other sources of knowledge, including research evidence, rather than relying solely on their own clinical experience. This is an important finding because the development of stronger evidence-based practice curricula in physical therapy programmes may be one reason why therapists with higher levels of education prefer to use more formal knowledge sources when deciding whether to apply US in clinical practice. This should encourage educators and curriculum developers to reinforce the important concept of evidence-based practice in educating future physical therapists. However, clinical experience continues to be an important factor that influences physical therapists' treatment choices, and its value should not be undermined, especially when research evidence is inconclusive or lacking.43
Strengths and limitations
Our study used a large, comprehensive population-based survey and achieved a response rate typical for population surveys (∼20%). Although our sample was similar in gender to the population of all registered physical therapists practising in Alberta, a higher proportion of the sample worked in private practice; private practice therapists were both more likely to use US and more likely to respond to our survey. This is the largest survey of US use conducted to date and, as such, provides some insight into current use of, beliefs about, and perceptions of US in the clinical community. However, it was limited to physical therapists licensed to practise in Alberta, and therefore may not be generalizable to other jurisdictions. In addition, our results document only what respondents report that they do, not what they actually do. Finally, the descriptive analyses we conducted do not allow us to draw firm conclusions about the different factors influencing the use of US (education, years of experience, practice setting, etc.).
Conclusions
US is frequently incorporated into physical therapy treatment regimens, based largely on the belief that it is clinically useful. However, US usage has decreased over the past 15 years in the province of Alberta.3 Physical therapists using US rely primarily on their clinical experience to make decisions about its use, but their reliance on clinical experience depends on their level of education: clinicians with an MSc degree tend to base US decisions on research evidence, likely because of the increasing emphasis on research evidence in graduate education. The results of this survey should encourage educators to continue their focus on evidence-based educational content, but also to re-evaluate strategies for transferring research knowledge to daily practice.
Key Messages
What is already known on this topic
Surveys conducted in various countries have consistently identified therapeutic ultrasound (US) as a central component of physical therapy practice. However, the reasons why physical therapists continue to use US have not been explored.
What this study adds
Although US is still commonly used by physical therapists, its use has decreased over the past 15 years. Physical therapists using US rely largely on their clinical experience when making decisions about its use, although this varies by level of education.
Supplementary Material
Physiotherapy Canada 2013; 65(3);289–299; doi:10.3138/ptc.2012-30BC
References
- 1.Robertson VJ, Baker KG. A review of therapeutic ultrasound: effectiveness studies. Phys Ther. 2001;81(7):1339–50. Medline:11444997. [PubMed] [Google Scholar]
- 2.Watson T. Ultrasound in contemporary physiotherapy practice. Ultrasonics. 2008;48(4):321–9. doi: 10.1016/j.ultras.2008.02.004. http://dx.doi.org/10.1016/j.ultras.2008.02.004. Medline:18466945. [DOI] [PubMed] [Google Scholar]
- 3.Lindsay DM, Dearness J, McGinley CC. Electrotherapy usage trends in private physiotherapy practice in Alberta. Physiother Can. 1995;47(1):30–4. Medline:10140421. [PubMed] [Google Scholar]
- 4.Pope GD, Mockett SP, Wright JP. A survey of electrotherapeutic modalities: Ownership and use in the NHS in England. Physiotherapy. 1995;81(2):82–91. http://dx.doi.org/10.1016/S0031-9406(05)67050-2. [Google Scholar]
- 5.Roebroeck ME, Dekker J, Oostendorp RAB. The use of therapeutic ultrasound by physical therapists in Dutch primary health care. Phys Ther. 1998;78(5):470–8. doi: 10.1093/ptj/78.5.470. Medline:9597061. [DOI] [PubMed] [Google Scholar]
- 6.Chipchase LS, Williams MT, Robertson VJ. A national study of the availability and use of electrophysical agents by Australian physiotherapists. Physiother Theory Pract. 2009;25(4):279–96. doi: 10.1080/09593980902782611. http://dx.doi.org/10.1080/09593980902782611. Medline:19418365. [DOI] [PubMed] [Google Scholar]
- 7.Wong RA, Schumann B, Townsend R, et al. A survey of therapeutic ultrasound use by physical therapists who are orthopaedic certified specialists. Phys Ther. 2007;87(8):986–94. doi: 10.2522/ptj.20050392. http://dx.doi.org/10.2522/ptj.20050392. Medline:17553923. [DOI] [PubMed] [Google Scholar]
- 8.Al-Kurdi D, Bell-Syer SEM, Flemming K. Therapeutic ultrasound for venous leg ulcers. Cochrane Database Syst Rev. 2008;(1):CD001180. doi: 10.1002/14651858.CD001180.pub2. Medline:18253986. [DOI] [PubMed] [Google Scholar]
- 9.Nussbaum E. The influence of ultrasound on healing tissues. J Hand Ther. 1998;11(2):140–7. doi: 10.1016/s0894-1130(98)80012-4. http://dx.doi.org/10.1016/S0894-1130(98)80012-4. Medline:9602971. [DOI] [PubMed] [Google Scholar]
- 10.Nussbaum EL. Ultrasound: to heat or not to heat—that is the question. Phys Ther Rev. 1997;2(2):59–72. http://dx.doi.org/10.1179/108331997787247608. [Google Scholar]
- 11.Chan AK, Myrer JW, Measom GJ, et al. Temperature changes in human patellar tendon in response to therapeutic ultrasound. J Athl Train. 1998;33(2):130–5. Medline:16558499. [PMC free article] [PubMed] [Google Scholar]
- 12.Draper DO, Castel JC, Castel D. Rate of temperature increase in human muscle during 1 MHz and 3 MHz continuous ultrasound. J Orthop Sports Phys Ther. 1995;22(4):142–50. doi: 10.2519/jospt.1995.22.4.142. Medline:8535471. [DOI] [PubMed] [Google Scholar]
- 13.Maxwell L. Therapeutic ultrasound: its effects on the cellular and molecular mechanisms of inflammation and repair. Physiotherapy. 1992;78(6):421–6. http://dx.doi.org/10.1016/S0031-9406(10)61528-3. [Google Scholar]
- 14.Moss A, Mowat AG. Ultrasonic assessment of stress fractures. Br Med J (Clin Res Ed) 1983;286(6376):1479–80. doi: 10.1136/bmj.286.6376.1479. http://dx.doi.org/10.1136/bmj.286.6376.1479. Medline:6405851. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Romani WA, Perrin DH, Dussault RG, et al. Identification of tibial stress fractures using therapeutic continuous ultrasound. J Orthop Sports Phys Ther. 2000;30(8):444–52. doi: 10.2519/jospt.2000.30.8.444. Medline:10949501. [DOI] [PubMed] [Google Scholar]
- 16.Ebenbichler GR, Resch KL, Graninger WB. Resolution of calcium deposits after therapeutic ultrasound of the shoulder. J Rheumatol. 1997;24(1):235–6. Medline:9002055. [PubMed] [Google Scholar]
- 17.Durmus D, Akyol Y, Cengiz K, et al. Effects of therapeutic ultrasound on pain, disability, walking performance, quality of life, and depression in patients with chronic low back pain: a randomized, placebo controlled trial. Turkish Journal of Rheumatology. 2010;25(2):82–7. doi: 10.1007/s00296-009-1072-7. http://dx.doi.org/10.5152/tjr.2010.07. [DOI] [PubMed] [Google Scholar]
- 18.Goren A, Yildiz N, Topuz O, et al. Efficacy of exercise and ultrasound in patients with lumbar spinal stenosis: a prospective randomized controlled trial. Clin Rehabil. 2010;24(7):623–31. doi: 10.1177/0269215510367539. http://dx.doi.org/10.1177/0269215510367539. Medline:20530650. [DOI] [PubMed] [Google Scholar]
- 19.Baker KG, Robertson VJ, Duck FA. A review of therapeutic ultrasound: biophysical effects. Phys Ther. 2001;81(7):1351–8. Medline:11444998. [PubMed] [Google Scholar]
- 20.Dogru H, Basaran S, Sarpel T. Effectiveness of therapeutic ultrasound in adhesive capsulitis. Joint Bone Spine. 2008;75(4):445–50. doi: 10.1016/j.jbspin.2007.07.016. http://dx.doi.org/10.1016/j.jbspin.2007.07.016. Medline:18455944. [DOI] [PubMed] [Google Scholar]
- 21.Zammit E, Herrington L. Ultrasound therapy in the management of acute lateral ligament sprains of the ankle joint. Phys Ther Sport. 2005;6(3):116–21. http://dx.doi.org/10.1016/j.ptsp.2005.05.002. [Google Scholar]
- 22.van der Windt DAWM, van der Heijden GJMG, van den Berg SGM, et al. Ultrasound therapy for musculoskeletal disorders: a systematic review. Pain. 1999;81(3):257–71. doi: 10.1016/S0304-3959(99)00016-0. http://dx.doi.org/10.1016/S0304-3959(99)00016-0. Medline:10431713. [DOI] [PubMed] [Google Scholar]
- 23.Gam AN, Johannsen F. Ultrasound therapy in musculoskeletal disorders: a meta-analysis. Pain. 1995;63(1):85–91. doi: 10.1016/0304-3959(95)00018-N. http://dx.doi.org/10.1016/0304-3959(95)00018-N. Medline:8577494. [DOI] [PubMed] [Google Scholar]
- 24.Köybaşi M, Borman P, Kocaoğlu S, et al. The effect of additional therapeutic ultrasound in patients with primary hip osteoarthritis: a randomized placebo-controlled study. Clin Rheumatol. 2010;29(12):1387–94. doi: 10.1007/s10067-010-1468-5. http://dx.doi.org/10.1007/s10067-010-1468-5. Medline:20499122. [DOI] [PubMed] [Google Scholar]
- 25.Ebenbichler GR, Resch KL, Nicolakis P, et al. Ultrasound treatment for treating the carpal tunnel syndrome: randomised “sham” controlled trial. BMJ. 1998;316(7133):731–5. doi: 10.1136/bmj.316.7133.731. http://dx.doi.org/10.1136/bmj.316.7133.731. Medline:9529407. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Mortimer AJ, Dyson M. The effect of therapeutic ultrasound on calcium uptake in fibroblasts. Ultrasound Med Biol. 1988;14(6):499–506. doi: 10.1016/0301-5629(88)90111-1. http://dx.doi.org/10.1016/0301-5629(88)90111-1. Medline:3227573. [DOI] [PubMed] [Google Scholar]
- 27.Ng GYF, Fung DTC. The effect of therapeutic ultrasound intensity on the ultrastructural morphology of tendon repair. Ultrasound Med Biol. 2007;33(11):1750–4. doi: 10.1016/j.ultrasmedbio.2007.05.019. http://dx.doi.org/10.1016/j.ultrasmedbio.2007.05.019. Medline:17630094. [DOI] [PubMed] [Google Scholar]
- 28.Ng GYF, Ng COY, See EKN. Comparison of therapeutic ultrasound and exercises for augmenting tendon healing in rats. Ultrasound Med Biol. 2004;30(11):1539–43. doi: 10.1016/j.ultrasmedbio.2004.08.030. http://dx.doi.org/10.1016/j.ultrasmedbio.2004.08.030. Medline:15588965. [DOI] [PubMed] [Google Scholar]
- 29.Piedade MCB, Galhardo MS, Battlehner CN, et al. Effect of ultrasound therapy on the repair of gastrocnemius muscle injury in rats. Ultrasonics. 2008;48(5):403–11. doi: 10.1016/j.ultras.2008.01.009. http://dx.doi.org/10.1016/j.ultras.2008.01.009. Medline:18384832. [DOI] [PubMed] [Google Scholar]
- 30.Ramirez A, Schwane JA, McFarland C, et al. The effect of ultrasound on collagen synthesis and fibroblast proliferation in vitro. Med Sci Sports Exerc. 1997;29(3):326–32. doi: 10.1097/00005768-199703000-00007. http://dx.doi.org/10.1097/00005768-199703000-00007. Medline:9139171. [DOI] [PubMed] [Google Scholar]
- 31.Young SR, Dyson M. The effect of therapeutic ultrasound on angiogenesis. Ultrasound Med Biol. 1990;16(3):261–9. doi: 10.1016/0301-5629(90)90005-w. http://dx.doi.org/10.1016/0301-5629(90)90005-W. Medline:1694604. [DOI] [PubMed] [Google Scholar]
- 32.Freitas TP, Gomes M, Fraga DB, et al. Effect of therapeutic pulsed ultrasound on lipoperoxidation and fibrogenesis in an animal model of wound healing. J Surg Res. 2010;161(1):168–71. doi: 10.1016/j.jss.2009.04.002. http://dx.doi.org/10.1016/j.jss.2009.04.002. Medline:19577772. [DOI] [PubMed] [Google Scholar]
- 33.Warden SJ, McMeeken JM. Ultrasound usage and dosage in sports physiotherapy. Ultrasound Med Biol. 2002;28(8):1075–80. doi: 10.1016/s0301-5629(02)00552-5. http://dx.doi.org/10.1016/S0301-5629(02)00552-5. Medline:12217443. [DOI] [PubMed] [Google Scholar]
- 34.Chipchase LS, Trinkle D. Therapeutic ultrasound: clinician usage and perception of efficacy. Hong Kong Physiotherapy Journal. 2003;21(1):5–14. http://dx.doi.org/10.1016/S1013-7025(09)70034-X. [Google Scholar]
- 35.Leung MC, Ng GY, Yip KK. Effect of ultrasound on acute inflammation of transected medial collateral ligaments. Arch Phys Med Rehabil. 2004;85(6):963–6. doi: 10.1016/j.apmr.2003.07.018. http://dx.doi.org/10.1016/j.apmr.2003.07.018. Medline:15179651. [DOI] [PubMed] [Google Scholar]
- 36.Menon A, Korner-Bitensky N, Kastner M, et al. Strategies for rehabilitation professionals to move evidence-based knowledge into practice: a systematic review. J Rehabil Med. 2009;41(13):1024–32. doi: 10.2340/16501977-0451. http://dx.doi.org/10.2340/16501977-0451. Medline:19893996. [DOI] [PubMed] [Google Scholar]
- 37.Grimshaw JM, Shirran L, Thomas R, et al. Changing provider behavior: an overview of systematic reviews of interventions. Med Care. 2001;39(8) Suppl 2:II2–45. Medline:11583120. [PubMed] [Google Scholar]
- 38.Finniss DG, Kaptchuk TJ, Miller F, et al. Biological, clinical, and ethical advances of placebo effects. Lancet. 2010;375(9715):686–95. doi: 10.1016/S0140-6736(09)61706-2. http://dx.doi.org/10.1016/S0140-6736(09)61706-2. Medline:20171404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Gracely RH, Dubner R, Deeter WR, et al. Clinicians' expectations influence placebo analgesia. Lancet. 1985;1(8419):43. doi: 10.1016/s0140-6736(85)90984-5. http://dx.doi.org/10.1016/S0140-6736(85)90984-5. Medline:2856960. [DOI] [PubMed] [Google Scholar]
- 40.Houben RMA, Ostelo RWJG, Vlaeyen JWS, et al. Health care providers' orientations towards common low back pain predict perceived harmfulness of physical activities and recommendations regarding return to normal activity. Eur J Pain. 2005;9(2):173–83. doi: 10.1016/j.ejpain.2004.05.002. http://dx.doi.org/10.1016/j.ejpain.2004.05.002. Medline:15737810. [DOI] [PubMed] [Google Scholar]
- 41.Cook C, McCluskey A, Bowman J. Occupational therapists report increased use of outcome measures after participation in an education programme. Br J Occup Ther. 2007;70(11):487–92. [Google Scholar]
- 42.Robertson VJ. Dosage and treatment response in randomized clinical trials of therapeutic ultrasound. Phys Ther Sport. 2002;3(3):124–33. [Google Scholar]
- 43.Stevenson K, Lewis M, Hay E. Do physiotherapists' attitudes towards evidence-based practice change as a result of an evidence-based educational programme? J Eval Clin Pract. 2004;10(2):207–17. doi: 10.1111/j.1365-2753.2003.00479.x. http://dx.doi.org/10.1111/j.1365-2753.2003.00479.x. Medline:15189387. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.