The cost of providing care to critically ill patients in the United States consumes roughly 15% of all health care dollars, or 1% of the gross national product.1 Contributing to this economic burden are patients admitted to the intensive care unit (ICU) who require mechanical ventilation and patients with complications from their dependence on this technology.2,3 In fact, 50% of ICU patients receive mechanical ventilation.4
Often, sedation is required to increase patients’ tolerance of the endotracheal tube, reduce anxiety, and facilitate sleep. In particular, sedation is used frequently to reduce patient-ventilator dyssynchrony (PVD).5–9 Sassoon and Foster10 define PVD as a mismatching between the patient’s breaths (neural) and ventilator-assisted breaths (phase asynchrony), as well as the inability of the ventilator’s flow delivery to match the patient’s flow demand (flow asynchrony). This definition suggests a faulty interaction between the patient and ventilator that is commonly managed by sedation and advanced ventilator modes and adjustments. The correction of PVD is complex and multifaceted given the current capabilities of traditional ventilators. An imperfect solution exists because the sensitivity and responsiveness of both the patient and the ventilator during the interaction is confounded by factors related to the patient and the ventilator. However, in light of the most serious complications (hypoxemia, barotrauma, prolonged mechanical ventilation, and discomfort) of PVD, and an imperfect solution for the resolution of PVD at the current time, nurses continue to face the challenge of preventing the consequences of PVD as well as complications due to oversedation or undersedation.
In this article, we discuss the factors contributing to PVD; the manifestations, measurement, types, and causes of PVD; nursing implications; and future directions for improvement, with nursing research questions proposed for consideration.
Factors Affecting Patient-Ventilator Interaction
Patient-ventilator interaction is influenced by factors related to the patient (respiratory center output, respiratory system mechanisms, disease states and conditions, artificial airway) and factors related to the ventilator (ventilator triggering, ventilator cycling off).
Patient-Related Factors
Achieving patient-ventilator synchrony during interactive modes of ventilation (assist control [AC] and synchronized intermittent mandatory ventilation [SIMV]) is a daunting task because patients’ ventilation is controlled by mechanical, chemical, behavioral, and reflex mechanisms that are highly dynamic. These factors can disrupt the patient-ventilator interface because the ventilator responds to the patient’s inspiratory and expiratory signals, which affect pressure and flow in the ventilator circuit.11 Given patients’ dynamic conditions during critical illness, patient-related factors such as respiratory center output, respiratory mechanics, disease states or conditions, and endotracheal tube type or size influence the patient-ventilator interaction (Table 1).
Table 1.
Patient- and ventilator-related factors that affect patient-ventilator interaction
| Patient-related factors | Ventilator-related factors |
|---|---|
| Respiratory center output | Triggering |
|
|
| Respiratory system mechanics | Cycling off |
| Disease states and conditions | Ventilator causes of patient agitation |
| Artificial airway in place | Dead space |
|
Respiratory Center Output
The patient’s respiratory center output can produce a decreased or increased drive that may contribute to the development of PVD. Respiratory drive is dependent on both voluntary and autonomic control. Voluntary control is operationalized through the cerebral cortex (forceful inspiration/expiration, breath holding) and thalamus (emotional behaviors associated with intense feelings, fear, pain, anger, sorrow).21 Autonomic control is operationalized by the brainstem, with the pneumotaxic and apneustic respiratory centers in the pons and 2 neuronal groups, called the dorsal (inspiratory) and ventral (inspiratory/expiratory) respiratory groups, located in the medulla.21 Afferent neurotransmissions from the body are communicated to the medullary neuronal groups from multiple receptors throughout the body. Table 2 describes these receptors specifically and their influence on the autonomic control of respiratory drive. Once the medulla receives impulses, the inspiratory and expiratory centers respond by determining whether inspiration or expiration should be stimulated or inhibited. The pneumotaxic center of the pons fine-tunes the rhythmicity of the ventilatory drive, and the efferent message is sent to the phrenic and intercostal nerves to stimulate or inhibit ventilation.21
Table 2.
Receptors and their effect on autonomic respiratory drivea
| Peripheral chemoreceptors | Pulmonary stretch receptors | Irritant receptors | Pulmonary juxtapulmonary capillary receptors | Baroreceptors | Proprioceptors | Other receptors | Central chemoreceptors | |
|---|---|---|---|---|---|---|---|---|
| Location | Aortic arch Carotid bodies |
Airway smooth muscle | Epithelium of nose, pharynx, larynx, trachea, bronchi | Pulmonary capillary walls | Aortic arch | Muscles and joints (tendon organs) | Nociceptors in skin, organs Mechanoreceptors in skin |
Ventrolateral surface of each side of medulla |
| Sense | Hypoxemia Acidosis Hypercapnia |
Lung inflation Increased pulmonary pressures |
Inhaled irritants Mechanical factors: Anaphylaxis Pulmonary congestion |
Pulmonary congestion Increased interstitial fluid Chemical irritants Microemboli |
Change in blood pressure | Body movement | Pain Touch |
Hydrogen ion concentration in cerebrospinal fluid Carbon dioxide crosses blood-brain barrier and yields carbonic acid |
| Sent to medulla by | Vagus and glossopharyngeal nerves | Vagus nerve | Vagus nerve | Vagus nerve | Vagus nerve | Ascending spinal nerves | Ascending spinal nerves | Bathing cerebrospinal fluid |
| Effect on respiratory drive |
If acidotic or hypoxemic: Increased rate and tidal volume If alkalotic: Decreased rate and tidal volume |
Increased inspiratory time Increased rate |
Hyperpnea Cough Laryngospasm |
Rapid, shallow breathing Hypoventilation |
If low blood pressure: Hyperventilation If high blood pressure: Hypoventilation |
Increased rate and tidal volume |
Visceral pain: Decreased drive Somatic pain: Increased drive |
Acidosis: Increased drive Alkalosis: Decreased drive |
Based on data from Kacmarek et al.21
If respiratory drive is decreased, the ventilator may not be able to respond to the reduced effort, especially if the clinician does not preset the ventilator’s sensitivity at a level that will detect the patient’s effort.10 A reduced drive can be caused by sedatives, opioids, and hypnotics. Sedatives, opioids, and sleep all increase the time delay between the start of the patient’s inspiratory effort and ventilator triggering.20 Metabolic states of alkalosis, sleep deprivation, severe hypothyroidism, and bilateral injury of the mid to lower medulla can decrease respiratory drive, thereby influencing the patient-ventilator interaction.12
If a patient’s respiratory drive increases vigorously, however, the duration of inspiratory drive may become longer than ventilator inflation time, causing the ventilator to trigger more than once (double trigger).20 An increased respiratory drive can cause the patient to need more flow from the ventilator.12 If the preset flow does not meet patient demand, flow dyssynchrony can occur. An increased respiratory output can be caused by increased chemoreceptor stimulation, pain, psychogenic alteration, medications, and increased ventilatory demand, metabolic rate, and workload.
Respiratory System Mechanics
A patient’s respiratory mechanics can contribute to dyssynchrony. The patient may have a prolonged inspiratory time. If inspiratory time is longer than the ventilator’s preset inspiratory time, the patient may take an additional breath because the need for ventilation has not been met, thereby causing double triggering.10
On the other hand, the patient may have a shortened exhalation time that increases the amount of intrinsic positive pressure at the end of expiration (PEEPi, auto-PEEP) because all volume has not been exhaled. This leads to dynamic hyperinflation causing the patient to breathe with high lung volumes and high elastic recoil pressures.12 The excess pressure on the alveoli at the end of expiration (auto-PEEP) causes increased workload for the patient’s diaphragm. Auto-PEEP is a common cause of failure-to-trigger PVD because the patient must overcome excess auto-PEEP by dropping intrathoracic pressure through muscular effort of sufficient magnitude to be sensed by the ventilator.
It is also important to consider the strength of the diaphragm and accessory muscles. Muscular strength may be decreased because of diaphragm deconditioning (prolonged ventilator assistance, physical immobility), malnutrition, and neuromuscular disease. Weakened respiratory muscles reduce the ability to meet the threshold necessary to initiate a ventilated breath during interactive modes.12
Patients’ Disease States and Conditions
Patients’ underlying diseases and conditions can lead to PVD. For example, patients with obstructive lung disease or high ventilatory demand and patients receiving inverse-ratio ventilation or airway pressure release ventilation can have dynamic hyperinflation.12 Dynamic hyperinflation moves the diaphragm to a flattened, less domelike configuration, which limits the patient’s ability to generate a forceful inspiration and creates a greater trigger threshold to overcome, leading to failed efforts.12 Pain and splinting from surgical or other sources may reduce a patient’s inspiratory effort and contribute to PVD.14
In addition, psychogenic mechanisms from agitation,12 fear, and stress may contribute to PVD because of resulting tachypnea and reduced mental capacity from overriding anxiety. Disease and ventilator-related factors can also agitate patients (Table 1). Agitation in patients who are receiving mechanical ventilation can be exacerbated by many factors, such as disease states (pulmonary edema, pulmonary embolism, pneumothorax), body posture, abdominal distension, retained airway secretions, pain, and bronchospasm.13 Last, the environment can be the source of noxious stimuli such as excessive noise, light, or physical stimulation that may contribute to the patient’s stress response, thereby increasing anxiety and possible agitation.15
Artificial Airway in Place
Finally, the size and type of airway may contribute to PVD.14 An endotracheal tube of inadequate diameter may increase resistance and limit flow for a patient with high ventilatory demand. The internal diameter of the endotracheal tube can be reduced by accumulation of secretions and debris that can markedly increase airway resistance.16 The patient-ventilator interaction is dependent on the patient’s ability to overcome this resistance and the amount of ventilator assistance.12
Ventilator-Related Factors
Synchronous patient-ventilator interaction requires a ventilator to be sensitive to respiratory efforts and responsive to airflow demand.11 Two major factors contributing to PVD are ventilator triggering (signal opens inspiratory valve) and cycling (signal opens expiratory valve at end inspiration).11,22
Ventilator Triggering
The ventilator should ideally respond to a patient’s inspiratory effort immediately. The sensitivity trigger is typically set to be stimulated on the basis of pressure, flow, or time. Unfortunately, in some situations, the sensitivity level may be set too low to sense the patient’s effort. In this situation, the patient’s effort may be wasted and not trigger a breath, which may lead to increased respiratory muscle loading.22,23 A prolongation of the trigger phase may also occur because of errors in the ventilator’s pressure transducer, the ventilator’s delay in sampling pressure signals, the duration of time from onset of diaphragm contraction to actual decrease in airway pressure, the duration of time from decrease of airway pressure to be sensed by the ventilator, and the duration of time from when the valve is signaled to when flow reaches the airway circuit.11 These factors generate phase dyssynchrony.
In phase dyssynchrony, a lag (termed delay time) occurs between the time when the ventilator first senses the trigger and the time when the ventilator responds by delivering gas flow.14 When the inspiration trigger is driven by a change in pressure (pressure trigger), the delay time by most commercial ventilators may reach 110 to 120 milliseconds before gas flows into the patient’s circuit.11 If the inspiratory trigger delay becomes too prolonged, the patient may try to increase his inspiratory efforts.11 Therefore to avoid trigger dyssynchrony, it is best for clinicians to set the shortest trigger delay time, which will minimize patients’ efforts to trigger an inspiration in interactive modes.11
Newer Ventilator Modes to Improve Ventilator Triggering
Traditional ventilators can only measure and respond to patient airway pressures at the airway opening and flow downstream on the expiratory limb of the ventilator circuit.24,25 The greater the distance from the central nervous system’s respiratory center that the ventilator senses the trigger drive, the greater the potential for PVD.11 New, experimental techniques offer different ways and sites to sense and respond to patients’ inspiratory signals. Proportional assist ventilation enhances synchrony by using a feedback mechanism to “amplify airway pressure proportionally to inspiratory flow and volume.”24(p26) This mechanism enables the ventilator to track changes in the patient’s ventilatory effort, thereby resulting in a more physiological breathing pattern.24 Other factors such as air leaks and water in the ventilator tubing can dampen the signal being sent from the patient to the ventilator during this interaction.11
Neurally adjusted ventilatory assist senses the diaphragm’s electric stimulation signal through an esophageal probe on the end of a nasogastric tube that sits close to the diaphragm.26 The signal is amplified, filtered, and processed by the ventilator’s software to then generate adjusted ventilation pressures specific to the patient’s initiated diaphragmatic output.27
Methods that are used less frequently may also be effective. Pdi-driven servoventilation adjusts ventilated pressure breaths in response to the patient’s transdiaphragmatic pressures (Pdi).27 This ventilator is triggered through the Pdi or a preset flow threshold, whichever is generated first. Inspiration ends when the inspiratory flow reaches a preset threshold.27 Shape-signal or flow-shape triggering28 depends on a distorted expiratory waveform that is generated when the patient initiates a breath in order to sense a patient’s inspiratory trigger. The ventilator algorithm generates a new flow signal that is offset from the patient’s actual flow by 0.25 L/s and delays it for 300 milliseconds, thereby allowing the signal to lag behind the patient’s actual flow rate so that, once the patient initiates a breath, the sudden decrease in expiratory flow will cross the generated shape signal to initiate a ventilated breath.20
Ventilator Cycling Off
Cycling off terminates the mechanical breath harmoniously when the patient desires to end inspiration and begin exhalation.20 Moving from inspiration to expiration on the ventilator is operationalized through volume, pressure, flow, or time cycling. To achieve this, clinicians preset ventilator settings of (a) target volumes, (b) peak inspiratory pressures, (c) peak flow rates/flow shape signal, or (d) inspiratory time limit or changes in inspiratory:expiratory ratio.22 The settings to obtain perfect synchrony between the end of inspiration and beginning of expiration, however, are not ideal. Usually termination of ventilator flow occurs either before or after the patient stops inspiratory effort.15
Premature Termination
If a mechanical breath is terminated before the patient desires (premature termination), the patient continues to contract inspiratory muscles, allowing pressure to overcome elastic recoil and resulting in the ability to meet the trigger threshold and initiate a new breath, called double triggering.20 Premature termination of ventilator flow causes excessive inspiratory muscle work into and during the expiratory phase and an overestimation of respiratory rate.12,20 Nurses should be able to identify double triggering on the ventilator’s pressure-time waveform (Figure 1) and recognize that double triggering may be a cause of increased respiratory frequency.
Figure 1.
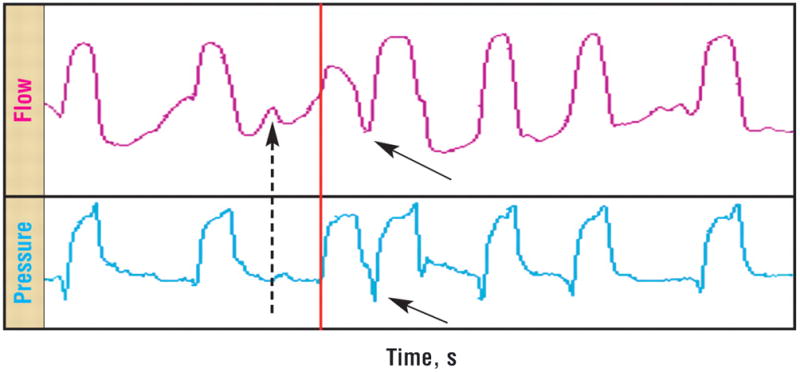
Trigger dyssynchrony, double trigger. Display of flow (top) and pressure (bottom) vs time. Note the start of the third successfully triggered breath (red line). In this breath cycle, patient effort initiates a second breath (solid arrows), represented by a quick decrease in pressure at the trigger threshold, such that flow increases. In addition, an ineffective missed effort (dashed arrow) just before the double trigger is demonstrated by an increase in flow and a decrease in pressure.
Delayed Termination
On the other hand, if the mechanical breath does not terminate when the patient’s muscular inspiration is complete (delayed termination), the time for exhalation is limited and expiratory workload and sometimes auto-PEEP increase, resulting in possible ineffective and/or failed trigger on the following breath.17,18,29 Delayed termination causes patients to resist or “fight” incoming ventilator flow by using their expiratory muscles. This resistance results in increased expiratory load and excessive PEEPi, thereby leading to possible pneumothoraces, barotrauma, and altered cerebral blood flow.29 Indeed, the perfect maneuver would be to program a ventilator breath-by-breath on the basis of a patient’s inspiratory time. Such a feature is currently not available on any ventilator, except for the Servo-i ventilator with the option of neurally adjusted ventilatory assist by Maquet, Inc, that was recently released commercially.30
A second effect of delayed termination results in ineffective triggering after the breath. If ineffective triggering occurs during exhalation, inspiratory muscles will be contracting when they would normally be lengthening (pliometric contraction), which has caused ultrastructural damage to muscle fibers and reduced strength in animal models.31,32 Although not studied in human models, muscle injury from ineffective triggering may prolong weaning.17
Patient-ventilator interaction is complex and dynamic, making the ideal interface elusive. Despite the advantage of interactive ventilator modes in promoting greater involvement of patients and limiting atrophy of respiratory muscles, a consequence is PVD. MacIntyre and Branson25 state that ventilators should be sensitive to the patient’s ventilatory effort and responsive to the patient’s demands.
Prevalence of PVD
PVD, a mismatch of respiratory cycling and flow of ventilation between the ventilator and the patient, occurs frequently and is underappreciated.12,33–35 Thille et al36 found a high prevalence of dyssynchrony in 62 patients intubated longer than 24 hours, and those patients with the most dyssynchrony had a longer duration of mechanical ventilation. Indeed, 24% of this sample experienced a significant amount of PVD, which was observed within 30 minutes of data collection.36 The most frequent types were ineffective triggering and double trigger with males and patients with chronic obstructive pulmonary disease experiencing more ineffective triggering.36
Use of continuous sedation during mechanical ventilation may prolong hospital stay and influence the prevalence of PVD. Because the assessment of sedation level is not precise, oversedation and undersedation are possible. A variety of approaches, such as daily interruption of sedation (“daily awakening trials”) or intermittent dosing of sedative and opioid medications can reduce the likelihood of excessive sedation.37 However, the use of daily awakening trials may aggravate PVD as patients become more alert, potentially placing high-risk patients in jeopardy for complications.
On the other extreme of the sedation scale, de Wit et al38 conducted a small study of 20 patients receiving mechanical ventilation and reported that the incidence of ineffective triggering was significantly correlated with lower scores (ie, patients more deeply sedated) on the Richmond Agitation Sedation Scale (RASS). This finding suggests that highly sedated patients may reduce their respiratory drive so much that they become ineffective in generating an inspiratory trigger sufficient to initiate a ventilated breath.
Consequences of PVD
Patient-ventilator synchrony is important for achieving optimal oxygenation and ventilation. Tobin et al4 state that patient-ventilator interaction is a major factor in determining how much respiratory muscle unloading can be completed by the machine, and the most effective unloading occurs when the patient and ventilator are synchronous.35 Achieving synchrony during interactive ventilator modes requires ventilator sensitivity and responsiveness to the patient’s demands, which is not always possible with current ventilators. Potential outcomes of patient-ventilator synchrony include prevention of hypocapnia, decreased sensation of dyspnea, reduced ineffective or wasted respiratory efforts, and reduced likelihood of periodic breaths during sleep.23 In addition, prolonged mechanical ventilation and longer hospital stay due to continuous sedation may be avoided.
The resulting unbalanced breathing pattern from PVD can lead to hypoxemia, increased workload on respiratory muscles, cardiovascular compromise, and discomfort.11,12,39 In addition, evidence indicates that PVD may result in respiratory muscle injury.10,15 In 1 study,36 patients with PVD had a longer duration of mechanical ventilation, whereas other reports10 have been unclear. Other specific effects and outcomes of PVD over time are not well known or documented. Because these consequences may aggravate an already existing critical illness and possibly increase ventilator-related morbidity,40 nurses should establish the goal of achieving patient-ventilator synchrony. To achieve these goals, nurses must learn how to analyze graphic waveforms for PVD, observe for manifestations of PVD such as those listed in Table 3, investigate and prevent possible causes of PVD, and work with the collaborative team to optimize ventilator settings, sedative titration, and psychosocial support to patients.
Table 3.
Markers of patient-ventilator dyssynchrony
| Biological markers | Behavioral markers | Patients’ reports of breathing with the ventilator |
|---|---|---|
| Pressure/flow-time waveforms12,14 Tachycardia12,41 Tachypnea12,42 Decreased oxygen saturation12 |
Paradoxical thoracoabdominal breaths12 Nasal flaring12 Expiratory muscle activity, forceful exhalation12,41 Inspiratory intercostal retractions12 Increased movement of extremities43 Coughing44 Agitation12 Abdominal excursions12 Increased use of accessory muscles12 Inspiratory effort without triggering the ventilator12 |
Difficulty with sensations of altered ventilation: “Even on the ventilator, the rate didn’t bother me, it was the force of air”39 Difficulty breathing independently (forced to adapt to the machine): “Sometimes, it’s too fast for you. So instead of the machine synchronizing with you, you have to synchronize with the machine”39 Realized if they relaxed, their experience was easier: “I never had a feeling of suffocation like I thought I would if I became out of synch with the ventilator”39 Blamed clinicians for not providing information about being “out of synch”: “I was able to, in my own sort of way, put two and two together and figure, as soon as I get in sync here, that will stop”39 Subjects desired to know more about dyssynchrony: “To know that there may be a time where my breathing and the ventilator’s breathing are not going to match”39 Subjects desired that nurses provide coping strategies: Patients would prefer to know that “you can relax, and try to get back in sync with it, or let the nurses know that you’re waking up”39 Discomfort, breathlessness, air hunger12,15,41,45 |
Measurement/Identification of PVD
Types of Dyssynchrony and Contributing Factors
Categorization of types of dyssynchrony may enable clinicians to identify PVD more readily and accurately. Nilsestuen and Hargett14 describe 4 major types of PVD that can be conceptualized within the different phases of a patient’s assisted ventilated breath (Table 4).
Table 4.
Phases of an assisted ventilated breath associated with patient-ventilator dyssynchronya
| Phase of an assisted ventilated breath | Type of patient-ventilator dyssynchrony |
|---|---|
| Patient initiates a breath | Trigger asynchrony
|
| Patient demands air flow from ventilator | Flow asynchrony |
| End of inspiration and breath triggering | Termination asynchrony
|
| End of expiration | Expiratory asynchrony |
Based on data from Nilsestuen and Hargett.14
Trigger Dyssynchrony
The first phase of a ventilator-assisted breath is its initiation. The factors that influence this stage include patient factors (having an adequate respiratory drive and inspiratory effort) and ventilator factors (having adequate responsiveness to detect the signal-pressure or flow, ability to reach a pressure maximum, appropriately set trigger levels/adequate delay time, and ability to pressurize the circuit).14 To avoid trigger dyssynchrony, these factors must be functional. Trigger dyssynchrony is a common category of PVD, and its types can range from failure to trigger to auto-triggering.
Failure to trigger occurs when the ventilator does not sense the pressure or flow trigger. This situation is the result of a poor respiratory drive or excessive PEEPi that prevents the patient’s effort from being sent to the ventilator’s sensor.14 Excess hyperinflation causes a larger pressure gradient, and the patient cannot usually overcome the trigger threshold. Therefore, the ventilator does not generate flow for the patient’s initiated breath. This same situation occurs in patients with chronic obstructive pulmonary disease or when trigger levels are not adjusted appropriately by clinicians. Ineffective triggering is shown in Figure 2.
Figure 2.
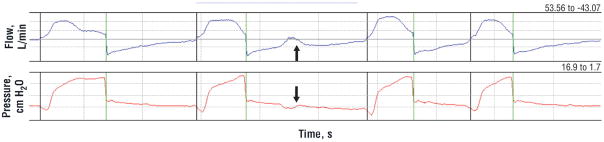
Trigger dyssynchrony, ineffective effort. Display of flow (top) and pressure (bottom) vs time. An ineffective effort, or failure to trigger dyssynchrony event, is noted at the arrow. Note the negative deflection of the pressure waveform and the transient positive flow deflection after the second breath.
Double triggering occurs when the patient is triggering the ventilator excessively through an excess demand for flow or volume that the ventilator is not preset to deliver.14 Clinical situations that could lead to this phenomenon include sighs, coughing with breathing, change in clinical status, or inappropriate ventilator settings. Determining the cause of the double triggering is important in order to resolve PVD. If the cause is a temporary situation, such as excessive coughing, the ventilator may be disconnected for a short duration until the episode is over.14 If double triggering is noted, nurses should consult with the collaborative team to adjust ventilator flow or volume settings to meet the patient’s demand (Figure 1).
Auto-triggering is caused by a maladjusted ventilator sensitivity level that recognizes signals other than the patient’s initiation of a breath. Examples of triggers that could cause auto-triggering include random noise in the circuit such as water (increased resistance); leaks (ie, circuit leaks, cuff leaks); and cardiogenic oscillations from patients with larger heart size, higher cardiac output, and higher ventricular filling pressures.14,19 Factors that promote auto-triggering include a low respiratory drive and decreased respiratory rate when hyperinflation is absent.15 Nurses should observe for causes of auto-triggering to prevent its occurrence and collaborate with the team to adjust the sensitivity level appropriately.
Flow Dyssynchrony
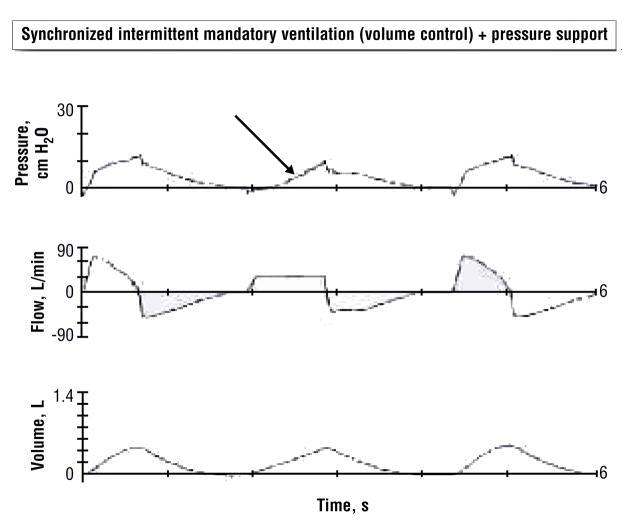
The second step of inspiration is the demand for air flow. Flow dyssynchrony can occur when the ventilator is not set correctly for the patient’s demand. Typically, the flow rate is set too low (eg, 40 L/min) compared with the patient’s inspiratory demand. One consequence of flow dyssynchrony is the creation of auto-PEEP; auto-PEEP is easily identified when the expiratory flow waveform does not return to zero before the next breath and a subsequent increase in peak inspiratory pressure is apparent.14 Flow dyssynchrony can occur in ventilated settings of volume- or pressure-cycled ventilation. During volume ventilation, the flow pattern is fixed and flow dyssynchrony can be identified by comparing the shapes of the pressure-time waveforms during complete passive breathing and patient-triggered breathing. A “dished out” appearance of the pressure wave during inhalation indicates flow dyssynchrony14 (Figure 3).
Figure 3.
Flow dyssynchrony. Display of pressure (top), flow (middle), and volume (bottom) vs time. During second breath, the ventilator square-wave flow is not adequate (pressure trace is dished out).
Figure courtesy of Jon Nilsestuen, PhD, RRT, University of Texas Medical Branch, School of Allied Health, Galveston.
Termination Dyssynchrony
Next in the cycle of a breath is the end of inspiration and breath triggering; it is at this point that termination dyssynchrony can occur.14 Basically, this type of PVD occurs in all ventilator modes because clinicians cannot set the perfect expiratory time based on the dynamic and changing patient’s initiated inspiratory time. Du and Yamada29 state that the most important factor to consider with this type of PVD is the length of time between the patient’s inhalation effort and the end of ventilator flow. Termination PVD can be premature or delayed (Figure 4). In premature termination, the flow of air stops before the patient stops inhaling. In delayed termination, the patient is exhaling as the machine continues to deliver a breath.
Figure 4.
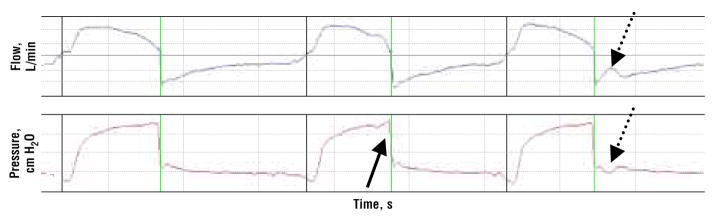
Termination dyssynchrony. Display of flow (top) and pressure (bottom) versus time reveals an example of “delayed termination dyssynchrony” (solid arrow) as the patient attempts exhalation before completion of the inspiratory breath, and “premature termination dyssynchrony” (dotted arrows) as the patient makes an inspiratory effort early in the expiratory phase.
Expiratory Dyssynchrony
When the end of expiration is unmatched with the patient’s efforts, expiratory dyssynchrony can occur.14 During this time, expiration may be shortened or prolonged. In the event of shortened expiration, the consequence can be air trapping, auto-PEEP, and a possible inability to reach the trigger threshold that leads to failure to trigger.14 On the other hand, prolonged expiration does not usually cause difficulties for the patient, unless the patient initiates a breath before the expiratory cycle is complete. Prolonged expiration may cause hypoventilation.14
Manifestations and Measures of PVD
Maintaining patient-ventilator synchrony in critically ill patients is required to prevent hypoxemia, hypercapnia, cardiovascular compromise, and excessive or inadequate sedation. Thanks to their frequent contact with patients, nurses and respiratory therapists are usually the first to observe that a patient is experiencing PVD. Although they may both detect changes in status, nurses and respiratory therapists may use different data to identify the change. Nurses describe patients who are “fighting the ventilator,”46 whereas respiratory therapists may be more likely to recognize PVD by noticing changes in the pressure/flow waveform.47,48
PVD can be detected by noting changes in the volume, pressure, and flow graphic waveforms displayed on the ventilator. Although PVD can be detected through waveform analysis,49 it is not clear whether nurses evaluate these waveforms accurately or whether nurses use data obtained from waveform analysis in their clinical practice. Indeed, Burns50 reported that few clinicians are proficient in understanding and applying the waveform graphic findings at the bedside. On the other hand, nurses may more often use markers of physiological instability and agitation as well as patients’ behaviors in general rather than pressure/flow waveforms to identify PVD. Table 3 summarizes the biobehavioral markers and experiences of patients with dyssynchrony. This table links the biological and behavioral manifestations with documented reports of PVD events by patients in an attempt to more fully explain and understand this complex phenomenon.
Nasal flaring, forceful exhalation, use of accessory muscles, inspiratory intercostal retractions, paradoxical thoracoabdominal movements, and recruitment of accessory muscles in the neck may all indicate PVD.12 Biologic measures such as tachycardia, tachypnea, hypoxemia, and real-time graphic displays of airway pressures have also been used.12,14 In addition, patients’ behaviors such as agitation, coughing, or grimacing, as well as frequent ventilator pressure alarms alert nurses to PVD. However, these behaviors and physiological responses of patients have not been validated as reliable measures of PVD.
The most widely used and objective measure of PVD is the pressure-flow graphic waveform; however, clinical application by nurses is not widespread.51 Therefore, in the absence of accessible, empirically based measures of PVD, the use of inadequate or excessive sedation may occur, leading to physiological instability and agitation, which may result in inappropriate use of sedation.
Nursing Implications for Improving the Phenomena of PVD
Monitoring of PVD
Correction of PVD remains a clinical priority. Achieving optimal patient-ventilator synchrony is enhanced by recognizing the problem, accurately assessing the patient’s behavior, adjusting various ventilatory parameters, and optimizing sedative therapy. It is noteworthy, however, that simply increasing the level of sedation, without identifying the cause of PVD or simply making ventilator adjustments, may unnecessarily prolong time receiving mechanical ventilation.52 Although waveform analysis has been available for the past decade, the technology is underused.14 This underuse may be due to interpretation complexity, limited resources in ICU, and limited educational preparation of nurses.
Burns50 offers a technique to monitor continuous airway pressures by using a transducer system connected to the side port of the ventilator circuit. This monitoring technique provides pressure/volume data similar to the data available on the ventilator display panel and offers a continuous view of the patient’s pulmonary dynamics, including evidence of dyssynchrony, auto-PEEP, and “breakthrough” respiratory efforts when sedatives and paralytic agents are used.50 The primary benefit of its use is the ability to record and print these graphics, allowing novice nurses time to identify and evaluate dyssynchronous patterns. Therefore use of Burns’s technique would augment real-time appreciation and management of PVD, much like the use of cardiac monitoring to detect and manage dysrhythmias.
PVD as Part of Sedation Assessment
Because sedation is used to optimize the patient-ventilator interaction and reduce dyssynchrony, identification of PVD is paramount for optimal management of sedation. However, no definitions of PVD have been uniformly accepted, and evaluation of ventilator synchrony has not been included in commonly used tools for evaluating sedation, such as the Ramsay Scale,53 the Riker Sedation-Agitation Scale,54 or the RASS,55 which is primarily used to evaluate level of consciousness and agitation.
National organizations have stressed the need to evaluate and validate measures that ensure all goals of sedation are being met. The American Association of Critical-Care Nurses has called for prospective studies to establish and study population-specific, goal-oriented sedation-agitation scales to enhance the consistency of caregiver observations and allow comparison of drug effects in adults.56 In addition, the Society of Critical Care Medicine’s published clinical practice guidelines recommend that a sedation end point, using a validated sedation assessment scale, be regularly redefined with caregivers.6 In a systematic review of instruments for measuring the level and effectiveness of sedation in adult and pediatric ICU patients, De Jonghe et al57 reported that although many instruments have been used to measure effectiveness of sedation in ICU patients, none have been tested for their utility in detecting change in sedation status over time (responsiveness), and few of them help clinicians assess sedation.
More recently, sedation assessment tools have attempted to include an evaluation of PVD, using measurements of the patient-ventilator interaction. DeJonghe et al44,57 used international focus groups of bedside nurses, residents, and intensivists to identify PVD parameters to be included in their Adaptation to the Intensive Care Environment sedation tool44; however, the characteristics chosen have not been tested for validity against graphic analysis of dyssynchrony, and reliability has not been determined. Although the Adaptation to the Intensive Care Environment tool uses a 4-item scale for assessing “blockade of inspiratory phase of ventilation,” respiratory rate more than 30/min, cough, and use of accessory muscles to assess ventilator synchrony, it is not clear if the inclusion of those factors is empirically based. A second tool, the RASS, uses a 10-item scale that is focused on level of consciousness and agitation, but it does include a behavior of “fights ventilator” as a criterion for agitation.55
A consensus panel for the American Association of Critical-Care Nurses has developed a sedation assessment tool that includes the evaluation of PVD.58 This scale ranges from best (“appropriate physiological response achieved from patient-ventilator interface”) to worst (“patient-ventilator dyssynchrony with detrimental physiological response”), although specific descriptions of physiological response are not included. Even though newer tools for evaluating sedation are being developed that include measures of PVD, they remain insufficient to measure this phenomenon reliably. Measurement of PVD is a priority for optimal use of sedation; however, sedation scales either do not include it in the evaluation of sedation level or the proposed measure has not been derived from an empirical foundation. Therefore, future nursing research is needed to identify the biobehavioral markers of PVD.
Collaboration With the Health Care Team
Collaboration between nurses, physicians, and respiratory therapists to manage PVD is imperative. Each professional assumes a different responsibility in patient care and contributes valuable information to the team. Uniquely, each team member brings a special school of thought to the phenomenon of PVD. Respiratory therapists are skilled in knowing the details of ventilator operation and modes, assessment of patients’ responses, and detection of airway pressure monitoring. Physicians are skilled in these similar attributes, as well as therapeutic disease management of patients receiving mechanical ventilation. Nurses are specifically skilled in observing and managing human responses to disease and the technology interface, but hold a prominent role in the coordination of patient care. Their role in understanding the larger picture greatly influences patients’ outcomes.
It is imperative that nurses commence interventions for improvement of care, which start by recognizing PVD. Establishing routine monitoring of airway pressure and flow real-time waveforms for PVD in patients receiving mechanical ventilation by using continuous airway pressure monitoring would be a significant contribution. Commercial ventilator vendors may consider adding graph paper for printouts of real-time waveforms for analysis and documentation of PVD, similar to the printouts from cardiac monitors used for rhythm strip interpretation. Automated techniques have been used in research to continuously detect ineffective and double triggering; when these methods are clinically realized, clinicians and their patients will benefit from the identification of PVD.59,60 Table 5 describes how to identify different types of PVD, their causes, and nursing contributions for collaboration with the health care team.
Table 5.
Identification, causes, and collaborative interventions for patient-ventilator dyssynchrony
| Types/waves | Cause | Collaborative interventions |
|---|---|---|
|
Trigger (before inspiration) LOOK FOR:
|
|
|
|
Flow (during inspiration) LOOK FOR:
|
|
|
|
Termination (inspiration terminated when cycling variable reached) LOOK FOR: |
|
|
|
Expiratory (on expiration) LOOK FOR:
|
|
|
Abbreviations: Auto-PEEP, automatic positive end-expiratory pressure; COPD, chronic obstructive pulmonary disease; Paw, airway pressure in ventilator circuit; PEEP, positive end-expiratory pressure.
Last, teaching patients receiving mechanical ventilation how to become acclimated to the ventilator is important. Explaining and realizing sensations that patients may experience is essential. Nurses do not know how the circumstances of the “normal” ventilator experience affect the condition of PVD; however, nurses should provide psychosocial support and maintain excellent communication with patients, especially when other caregivers are in the room.
Nurses may need to use coaching strategies to help patients develop a breath pattern to assist with PVD until the cause is found. Patient stressors and the critical care environment should be assessed to determine the degree of conditions that could be changed for the patient’s benefit during PVD. Excessive environmental or psychological stressors may affect the interaction between patient and ventilator. Accordingly, early and accurate identification of PVD will enhance optimal use of sedative therapy and reduce duration of mechanical ventilation.
Future Directions for Research
The collaborative health care team is contributing to the advancement of knowledge in the realm of PVD. Physicians are experimenting with different triggers and modes, and respiratory therapists are identifying strategies to detect PVD and manage it. Nursing publications on this topic are scarce, yet nurses have much to contribute. We plan to describe the biobehavioral markers of PVD, through direct observations and continuous data recordings of heart rate, respiratory rate, end-tidal carbon dioxide, and oxygen saturation by using continuous airway pressure monitoring to detect dyssynchrony. The hope is to recognize those manifestations that can be assessed to detect PVD. New questions about PVD can be raised (Table 6).
Table 6.
List of potential research questions for the future direction of nursing research on patient-ventilator dyssynchrony
|
In conclusion, clinicians are challenged to recognize PVD and treat it appropriately. Collaborative teamwork will resolve the identification and treatment of PVD.
PRIME POINTS.
Dyssynchrony may result because mechanical ventilators lack the simultaneous responsiveness needed for interaction with the dynamic conditions of patients.
Patient-ventilator dyssynchrony can prolong mechanical ventilation and hospital stay, and is common yet underappreciated in critically ill patients.
Sedation is a common solution for managing dyssynchrony, but it may not always be the best answer for all types of dyssynchrony.
Footnotes
To purchase electronic or print reprints, contact The InnoVision Group, 101 Columbia, Aliso Viejo, CA 92656. Phone, (800) 899-1712 or (949) 362-2050 (ext 532); fax, (949) 362-2049; reprints@aacn.org.
eLetters
Now that you’ve read the article, create or contribute to an online discussion about this topic using eLetters. Just visit www.ccnonline.org and click “Respond to This Article” in either the full-text or PDF view of the article.
Financial Disclosures
Karen G. Mellott and this project were supported by grant number F31NR009623 from the National Institute of Nursing Research. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute of Nursing Research or the National Institutes of Health.
Contributor Information
Karen G. Mellott, Doctoral candidate and a National Institute for Nursing Research pre-doctoral fellow in the School of Nursing at Virginia Commonwealth University in Richmond. Her research focuses on patient-ventilator dyssynchrony and the patient/technology interface.
Mary Jo Grap, Professor in the School of Nursing at Virginia Commonwealth University. She is an expert nurse researcher in mechanical ventilation and critical care nursing.
Cindy L. Munro, Professor in the School of Nursing at Virginia Commonwealth University and volunteers as an adult nurse practitioner at Petersburg Health Care Alliance in Virginia. Her research examines the impact of oral health on the general health of patients and the care of patients receiving mechanical ventilation. She is also the coeditor of the American Journal of Critical Care.
Curtis N. Sessler, Orhan Muren Professor of Medicine at Virginia Commonwealth University. His current research interests are sepsis and multiorgan failure, prevention of nosocomial infection, and agitation and sedation in intensive care patients.
Paul A. Wetzel, Associate professor in the department of biomedical engineering at Virginia Commonwealth University. His primary research emphasis is on development of human-machine interfaces on the basis of eye movement and visual analysis.
References
- 1.Cheng EY. The cost of sedating and paralyzing the critically ill patient. Crit Care Clin. 1995;11(4):1005–1019. [PubMed] [Google Scholar]
- 2.Burns SM, Earven S, Fisher C, et al. Implementation of an institutional program to improve clinical and financial outcomes of mechanically ventilated patients: one-year outcomes and lessons learned. Crit Care Med. 2003;31(12):2752–2763. doi: 10.1097/01.CCM.0000094217.07170.75. [DOI] [PubMed] [Google Scholar]
- 3.Tobin MJ. Advances in mechanical ventilation. N Engl J Med. 2001;344(26):1986–1996. doi: 10.1056/NEJM200106283442606. [DOI] [PubMed] [Google Scholar]
- 4.Tobin MJ, Laghi F, Jubran A. Respiratory muscle dysfunction in mechanically ventilated patients. Mol Cell Biochem. 1998;179(1–2):87–98. doi: 10.1023/a:1006807904036. [DOI] [PubMed] [Google Scholar]
- 5.Sessler CN. Comfort and distress in the ICU: scope of the problem. Sem Respir Crit Care Med. 2001;22(2):111–114. doi: 10.1055/s-2001-13825. [DOI] [PubMed] [Google Scholar]
- 6.Jacobi J, Fraser GL, Coursin DB, et al. Clinical practice guidelines for the sustained use of sedatives and analgesics in the critically ill adult. Crit Care Med. 2002;30(1):119–141. doi: 10.1097/00003246-200201000-00020. [DOI] [PubMed] [Google Scholar]
- 7.Rhoney DH, Murry KR. National survey of the use of sedating drugs, neuromuscular blocking agents, and reversal agents in the intensive care unit. J Intensive Care Med. 2003;18(3):139–145. doi: 10.1177/0885066603251200. [DOI] [PubMed] [Google Scholar]
- 8.Blanchard AR. Sedation and analgesia in intensive care: medications attenuate stress response in critical illness. Postgrad Med. 2002;111(2):59–60. 63–64, 67–70. doi: 10.3810/pgm.2002.02.1107. [DOI] [PubMed] [Google Scholar]
- 9.Tufano R. Analgesia and sedation in intensive care: a progress report. Minerva Aneste-siol. 2003;69(10):735–737. [PubMed] [Google Scholar]
- 10.Sassoon CS, Foster GT. Patient-ventilator asynchrony. Curr Opin Crit Care. 2001;7(1):28–33. doi: 10.1097/00075198-200102000-00005. [DOI] [PubMed] [Google Scholar]
- 11.Racca F, Squadrone V, Ranieri VM. Patient-ventilator interaction during the triggering phase. Respir Care Clin. 2005;11(2):225–245. doi: 10.1016/j.rcc.2005.01.001. [DOI] [PubMed] [Google Scholar]
- 12.Dick CR, Sassoon CS. Patient-ventilator interactions. Clin Chest Med. 1996;17(3):423–438. doi: 10.1016/s0272-5231(05)70325-7. [DOI] [PubMed] [Google Scholar]
- 13.Tobin MJ, Fahey PJ. Management of the patient who is “fighting the ventilator. In: Tobin MJ, Fahey PJ, editors. Principles and Practice of Mechanical Ventilation. New York: NY: McGraw Hill; 1994. [Google Scholar]
- 14.Nilsestuen JO, Hargett KD. Using ventilator graphics to identify patient-ventilator asynchrony. Respir Care. 2005;50(2):202–234. [PubMed] [Google Scholar]
- 15.Kondili E, Prinianakis G, Georgopoulos D. Patient-ventilator interaction. Br J Anaesth. 2003;91(1):106–119. doi: 10.1093/bja/aeg129. [DOI] [PubMed] [Google Scholar]
- 16.Glass C, Grap MJ, Sessler CN. Endotracheal tube narrowing after closed-system suctioning: prevalence and risk factors. Am J Crit Care. 1999;8(2):93–100. [PubMed] [Google Scholar]
- 17.Younes M, Kun J, Webster K, Roberts D. Response of ventilator-dependent patients to delayed opening of exhalation valve. Am J Respir Crit Care Med. 2002;166(1):21–30. doi: 10.1164/rccm.2107143. [DOI] [PubMed] [Google Scholar]
- 18.Parthasarathy S, Jubran A, Tobin MJ. Cycling of inspiratory and expiratory muscle groups with the ventilator in airflow limitation. Am J Respir Crit Care Med. 1998;158(5 Pt 1):1471–1478. doi: 10.1164/ajrccm.158.5.9802014. [DOI] [PubMed] [Google Scholar]
- 19.Imanaka H, Nishimura M, Takeuchi M, Kimball WR, Yahagi N, Kumon K. Autotrig-gering caused by cardiogenic oscillation during flow-triggered mechanical ventilation. Crit Care Med. 2000;28(2):402–407. doi: 10.1097/00003246-200002000-00019. [DOI] [PubMed] [Google Scholar]
- 20.Prinianakis G, Kondili E, Georgopoulos D. Patient-ventilator interaction: an overview. Respir Care Clin. 2005;11(2):201–224. doi: 10.1016/j.rcc.2005.02.007. [DOI] [PubMed] [Google Scholar]
- 21.Kacmarek RM. Neurologic control of ventilation. In: Kacmarek RM, Dimas S, Mack CW, editors. The Essentials of Respiratory Care. 4. St Louis, MO: Elsevier Mosby; 2005. pp. 113–124. [Google Scholar]
- 22.Fenstermacher D, Hong D. Mechanical ventilation: what have we learned? Crit Care Nurs Q. 2004;27(3):258–294. doi: 10.1097/00002727-200407000-00006. [DOI] [PubMed] [Google Scholar]
- 23.Ramar K, Sassoon CS. Potential advantages of patient-ventilator synchrony. Respir Care Clin. 2005;11(2):307–317. doi: 10.1016/j.rcc.2005.02.005. [DOI] [PubMed] [Google Scholar]
- 24.Branson R. Understanding and implementing advances in ventilator capabilities. Curr Opin Crit Care. 2004;10(1):23–32. doi: 10.1097/00075198-200402000-00005. [DOI] [PubMed] [Google Scholar]
- 25.MacIntyre NR, Branson RD. Mechanical Ventilation. Philadelphia, PA: WB Saunders; 2001. [Google Scholar]
- 26.Navalesi P, Costa R. New modes of mechanical ventilation: proportional assist ventilation, neurally adjusted ventilatory assist, and fractal ventilation. Curr Opin Crit Care. 2003;9(1):51–58. doi: 10.1097/00075198-200302000-00010. [DOI] [PubMed] [Google Scholar]
- 27.Kondili E, Georgopoulos D. New and future developments to improve patient-ventilator interaction. Respir Care Clin. 2005;11(2):319–339. doi: 10.1016/j.rcc.2005.02.006. [DOI] [PubMed] [Google Scholar]
- 28.Prinianakis G, Kondili E, Georgopoulos D. Effects of the flow waveform method of triggering and cycling on patient-ventilator interaction during pressure support. Intensive Care Med. 2003;29(11):1950–1959. doi: 10.1007/s00134-003-1703-5. [DOI] [PubMed] [Google Scholar]
- 29.Du HL, Yamada Y. Expiratory asynchrony. Respir Care Clin. 2005;11(2):265–280. doi: 10.1016/j.rcc.2005.02.001. [DOI] [PubMed] [Google Scholar]
- 30.Maquet Inc. [Accessed August 10, 2009.];Maquet Critical Care receives FDA 510(K) clearance for major advance in mechanical ventilation [press release] 2007 Apr 3; http://www.maquet.com/content/Documents/PressReleases/SERVOI_Pressrel_NAVAreleaseFINALAPPROVED-US-SOLNA_v1-1_EN_US.pdf.
- 31.Devor ST, Faulkner JA. Regeneration of new fibers in muscles of old rats reduces contraction-induced injury. J Appl Physiol. 1999;87(2):750–756. doi: 10.1152/jappl.1999.87.2.750. [DOI] [PubMed] [Google Scholar]
- 32.Hunter KD, Faulkner JA. Pliometric contraction-induced injury of mouse skeletal muscle: effect of initial length. J Appl Physiol. 1997;82(1):278–283. doi: 10.1152/jappl.1997.82.1.278. [DOI] [PubMed] [Google Scholar]
- 33.Branson RD. Functional principles of positive pressure ventilators: implications for patient-ventilator interaction. Respir Care Clin. 2005;11(2):119–145. doi: 10.1016/j.rcc.2005.02.002. [DOI] [PubMed] [Google Scholar]
- 34.Nava S, Bruschi C, Fracchia C, Braschi A, Rubini F. Patient-ventilator interaction and inspiratory effort during pressure support ventilation in patients with different pathologies. Eur Respir J. 1997;10(1):177–183. doi: 10.1183/09031936.97.10010177. [DOI] [PubMed] [Google Scholar]
- 35.Tobin MJ, Jubran A, Laghi F. Patient-ventilator interaction. Am J Respir Crit Care Med. 2001;163(5):1059–1063. doi: 10.1164/ajrccm.163.5.2005125. [DOI] [PubMed] [Google Scholar]
- 36.Thille AW, Rodriguez P, Cabello B, Lellouche F, Brochard L. Patient-ventilator asynchrony during assisted mechanical ventilation. Intensive Care Med. 2006;32(10):1515–1522. doi: 10.1007/s00134-006-0301-8. [DOI] [PubMed] [Google Scholar]
- 37.Kress JP, Pohlman AS, O’Connor MF, Hall JB. Daily interruption of sedative infusions in critically ill patients undergoing mechanical ventilation. N Engl J Med. 2000;342(20):1471–1477. doi: 10.1056/NEJM200005183422002. [DOI] [PubMed] [Google Scholar]
- 38.de Wit M, Pedram S, Best AM, Epstein SK. Relationship between patient ventilator dysynchrony and sedation level. Intensive Care Med. 2005;170:S195. [Google Scholar]
- 39.Jablonski R. The experience of being mechanically ventilated. Qual Health Res. 1994;4:186–207. [Google Scholar]
- 40.Kirby RR. Improving ventilator-patient interaction: reduction of flow dyssynchrony [editorial] Crit Care Med. 1997;25(10):1630. doi: 10.1097/00003246-199710000-00007. [DOI] [PubMed] [Google Scholar]
- 41.Jubran A, Van de Graaff WB, Tobin MJ. Variability of patient-ventilator interaction with pressure support ventilation in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 1995;152(1):129–136. doi: 10.1164/ajrccm.152.1.7599811. [DOI] [PubMed] [Google Scholar]
- 42.MacIntyre NR, Ho LI. Effects of initial flow rate and breath termination criteria on pressure support ventilation. Chest. 1991;99(1):134–138. doi: 10.1378/chest.99.1.134. [DOI] [PubMed] [Google Scholar]
- 43.Mellott KG, Grap MJ, Sessler CN, Wetzel P. Manifestations of patient ventilator dyssynchrony in critically ill patients. Paper presented at: 19th annual conference of the Southern Nursing Research Society; February 3, 2005; Atlanta, Georgia. [Google Scholar]
- 44.De Jonghe B, Cook D, Griffith L, et al. Adaptation to the Intensive Care Environment (ATICE): development and validation of a new sedation assessment instrument. Crit Care Med. 2003;31(9):2344–2354. doi: 10.1097/01.CCM.0000084850.16444.94. [DOI] [PubMed] [Google Scholar]
- 45.Manning HL, Molinary EJ, Leiter JC. Effect of inspiratory flow rate on respiratory sensation and pattern of breathing. Am J Respir Crit Care Med. 1995;151(3 Pt 1):751–757. doi: 10.1164/ajrccm/151.3_Pt_1.751. [DOI] [PubMed] [Google Scholar]
- 46.Egerod I. Uncertain terms of sedation in ICU: how nurses and physicians manage and describe sedation for mechanically ventilated patients. J Clin Nurs. 2002;11(6):831–840. doi: 10.1046/j.1365-2702.2002.00725.x. [DOI] [PubMed] [Google Scholar]
- 47.Kallet RH, Luce JM. Detection of patient-ventilator asynchrony during low tidal volume ventilation, using ventilator waveform graphics. Respir Care. 2002;47(2):183–185. [PubMed] [Google Scholar]
- 48.Marini JJ. What derived variables should be monitored during mechanical ventilation? Respir Care. 1992;37(9):1097–1107. [PubMed] [Google Scholar]
- 49.Burton S, Hubmayer RD. Determination of patient-ventilator interactions. In: Tobin MJ, editor. Principles and Practices of Mechanical Ventilation. New York, NY: McGraw-Hill; 1994. pp. 655–666. [Google Scholar]
- 50.Burns SM. Continuous airway pressure monitoring. Crit Care Nurse. 2004;24(6):70–74. [PubMed] [Google Scholar]
- 51.Burns SM. Working with respiratory waveforms: how to use bedside graphics. AACN Clin Issues. 2003;14(2):133–144. doi: 10.1097/00044067-200305000-00003. [DOI] [PubMed] [Google Scholar]
- 52.Kollef MH, Levy NT, Ahrens TS, Schaiff R, Prentice D, Sherman G. The use of continuous i.v. sedation is associated with prolongation of mechanical ventilation. Chest. 1998;114(2):541–548. doi: 10.1378/chest.114.2.541. [DOI] [PubMed] [Google Scholar]
- 53.Ramsay MA, Savege TM, Simpson BR, Goodwin R. Controlled sedation with alphaxalone-alphadolone. Br J Med. 1974;2(5920):656–659. doi: 10.1136/bmj.2.5920.656. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Riker RR, Picard JT, Fraser GL. Prospective evaluation of the Sedation-Agitation Scale for adult critically ill patients. Crit Care Med. 1999;27(7):1325–1329. doi: 10.1097/00003246-199907000-00022. [DOI] [PubMed] [Google Scholar]
- 55.Sessler CN, Gosnell MS, Grap MJ, et al. The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002;166(10):1338–1344. doi: 10.1164/rccm.2107138. [DOI] [PubMed] [Google Scholar]
- 56.Luer J. Sedation and neuromuscular blockade in patients with acute respiratory failure. In: Chulay M, Burns SM, editors. Care of the Mechanically Ventilated Patient. Aliso Viejo, CA: American Association of Critical Care Nurses; 1998. pp. 1–25. [Google Scholar]
- 57.De Jonghe B, Cook D, Appere-de-Vecchi C, Guyatt G, Meade M, Outin H. Using and understanding sedation scoring systems: a systematic review. Intensive Care Med. 2000;26(3):275–285. doi: 10.1007/s001340051150. [DOI] [PubMed] [Google Scholar]
- 58.Consensus Conference on Sedation Assessment: a collaborative venture by Abbott Laboratories, American Association of Critical-Care Nurses, and Saint Thomas Health System. Crit Care Nurse. 2004;24(2):33–41. [PubMed] [Google Scholar]
- 59.Chen CW, Lin WC, Hsu CH, Cheng KS, Lo CS. Detecting ineffective triggering in the expiratory phase in mechanically ventilated patients based on airway flow and pressure deflection: feasibility of using a computer algorithm. Crit Care Med. 2008;36(2):455–461. doi: 10.1097/01.CCM.0000299734.34469.D9. [DOI] [PubMed] [Google Scholar]
- 60.Mulqueeny Q, Ceriana P, Carlucci A, Fan-fulla F, Delmastro M, Nava S. Automatic detection of ineffective triggering and double triggering during mechanical ventilation. Intensive Care Med. 2007;33(11):2014–2018. doi: 10.1007/s00134-007-0767-z. [DOI] [PubMed] [Google Scholar]
- 61.Georgopoulos D, Prinianakis G, Kondili E. Bedside waveforms interpretation as a tool to identify patient-ventilator asynchronies. Intensive Care Med. 2006;32(1):34–47. doi: 10.1007/s00134-005-2828-5. [DOI] [PubMed] [Google Scholar]
- 62.Kondili E, Xirouchaki N, Georgopoulos D. Modulation and treatment of patient-ventilator dyssynchrony. Curr Opin Crit Care. 2007;13(1):84–89. doi: 10.1097/MCC.0b013e328011278d. [DOI] [PubMed] [Google Scholar]