Abstract
Objectives
Depression is prevalent in mothers receiving home visiting. Little is known about the impact of treatment on associated features of maternal depression in this population. The purpose of this study was to examine the impact of a novel, adapted treatment for depressed mothers in home visiting on psychological distress and social functioning.
Methods
In-Home Cognitive Behavioral Therapy (IH-CBT) was developed to treat depressed mothers in home visiting. A randomized clinical trial design was used in which subjects were 93 new mothers in a home visiting program. Mothers with major depressive disorder identified at 3 months postpartum were randomized into IH-CBT and ongoing home visiting (n = 47) or standard home visiting (SHV; n = 46) in which they received home visitation alone and could obtain treatment in the community. Measures of psychological distress, social support, and social network were measured at pre-treatment, post-treatment, and three-month follow-up. Clinical features of depression and home visiting parameters were examined as potential moderators.
Results
Subjects receiving IH-CBT reported decreased psychological distress at post-treatment (ES = 0.77) and follow-up (ES = 0.73). Examination of types of psychological distress indicated broad improvements at both time points. Those receiving IH-CBT reported increased social support over time relative to those in the SHV condition. Effect sizes were modest at post-treatment (ES = 0.38) but increased at follow-up (ES = 0.65). Improvements were seen in affiliative and belonginess aspects of social support, in contrast to tangible support which was statistically non-significant. Findings were not moderated by clinical features of depression or home visiting parameters. No group differences were found in size of and involvement with social networks.
Conclusions
IH-CBT is effective in reducing psychological distress and improving perceived social support in depressed mothers receiving home visiting. To the extent that mothers are better adjusted and feel socially supported, they are more available to their children and more amenable to home visiting services. IH-CBT is a feasible, readily adopted treatment that is compatible with multiple home visiting models. As a result it is a promising approach to help depressed mothers in home visiting. Additional interventions may be needed to support depressed mothers in building sizable and stable social networks.
Keywords: Home visiting, Maternal depression, Cognitive behavioral therapy, Psychological distress, Social functioning
Home visiting is a widely-used prevention strategy for young children and their mothers (Boller & Strong, 2010). Although home visiting models use different formats and strategies, they typically share common elements: (1) enrollment prenatally or early in the child’s life, (2) engagement of mothers early in their roles as parents, (3) strengthening of individual and family protective factors and mitigating risk factors to promote normative development, (4) frequent contact between home visitors and families, and (5) extended program duration to ensure presence during emerging developmental periods.
There are at least 500,000 children and their mothers served by home visiting programs in the USA (Astuto & Allen, 2009). Mothers served by home visiting are typically socially isolated, impoverished, and undereducated. As a result, home visiting programs spend considerable time working directly with mothers to address issues such as stress and coping, health, and educational advancement. By strengthening these domains, mothers are more available to their children, better able to meet child needs, and are responsive to the psychoeducational approaches used by home visitors. Maternal depression has a profound and negative impact on these areas. Research shows that up to 61% of mothers in home visiting report clinically elevated levels of depression during the course of service (Ammerman, Putnam, Bosse, Teeters, & Van Ginkel, 2010). Home visitors report being unprepared to help depressed mothers (Tandon, Parillo, Jenkins, & Duggan, 2005), that depressed mothers are more difficult to engage and are less able to benefit from services (Stevens, Ammerman, Putnam, Gannon, & Van Ginkel, 2005), and that depression interferes with implementation of program curricula (Administration on Children Youth and Families, 2002). Research on depression in home visiting has relied exclusively on self-report measures of depressive symptoms. As a result, little is known about the prevalence or impact on home visiting of mothers who meet diagnostic criteria for major depressive disorder (MDD), the more severe and clinical manifestation of depression.
Maternal depression affects other areas of adjustment that are relevant to home visiting. Psychological distress and social functioning are particularly salient. Psychological distress and comorbid symptoms are common associated features of depression (Scott et al., 2000). These include anxiety, preoccupation with physical concerns, and disturbing thoughts. As with depression, psychological distress interferes with maternal functioning, and negatively impacts motivation, learning, and nurturing parenting. Although co-occurring with depression, psychological distress may emerge and be maintained by separate and independent processes. Remission from depression can lead to corresponding improvements in psychological distress, but this is not always the case and significant symptoms may remain after depressed mood has resolved (Rhebergen et al., 2010). Successful strategies for helping depressed mothers in home visiting must demonstrate effectiveness in reducing general psychological distress in addition to depressive symptoms.
Social functioning, including perceived social support and the size and quality of social networks, is critically important for new mothers and is another secondary focus of home visiting (Howard & Brooks-Gunn, 2009). High levels of social support provide mothers with outlets to discuss challenging situations, and receive affirmation from others that contributes to feelings of belongingness and self-efficacy (Lakey & Orehek, 2011). Lack of social support is linked to increased parenting stress, poorer coping, and risk for depression (Balaji et al., 2007; Lakey & Cronin, 2008). Research has demonstrated that perceived support contributes to psychological well-being even in the context of an unstable social network. Yet, strong and large social networks provide resources and tangible support to new mothers and contribute independently to maternal effectiveness and adjustment. Together, perceived social support and stable networks provide a context for healthy maternal and child functioning. Low levels of social support and social isolation are frequently observed in depressed adults (Rhebergen et al., 2010). Although these may improve as depressive symptoms remit, there is considerable evidence that social support and social network are independent constructs that may only partially recover or be unchanged following successful treatment for depression (Denninger et al., 2011). As with psychological distress, successful treatments for depressed mothers in home visiting will also impact social functioning.
Clinical trials suggest that home visiting alone provides little to no benefit in reducing maternal depressive symptoms (Duggan, Fuddy, Burrell et al., 2004), or that symptom reduction is temporary (Landsverk et al., 2002) or occurs only after the end of services (Chazan-Cohen et al., 2007). Home visitors often do not identify depression (Duggan, Fuddy, McFarlane et al., 2004), and depressed mothers rarely obtain mental health treatment even when the need is recognized (Tandon, Parillo, Mercer, Keefer, & Duggan, 2008). In response, Ammerman et al. (2011) systematically adapted cognitive behavioral therapy to address the needs of depressed mothers receiving home visiting. In-Home Cognitive Behavioral Therapy (IH-CBT) is implemented by therapists who provide treatment concurrently with ongoing home visiting. IH-CBT combines the core principles and techniques of CBT (Beck, 2011) with procedures and strategies that promote engagement, make content relevant to the needs of mothers in home visiting, facilitate delivery in the home, and explicitly foster a collaborative relationship between the therapist and home visitor in order to smoothly coordinate services. IH-CBT is an enhancement to standard home visiting that emphasizes the reduction of maternal depressive symptoms and recovery from MDD, thereby allowing home visitors to attend to issues related to parenting, maternal functioning, and child development.
Empirical support for IH-CBT in treating maternal depression was obtained in a clinical trial (Ammerman et al., 2013) comparing mothers who received IH-CBT and concurrent home visiting with those who received home visiting alone. In this study, 93 mothers participating in home visiting were first identified using a screen (Edinburgh Postnatal Depression Scale;Cox, Holden, & Sagovsky, 1987) administered at three months postpartum. This was followed by determination of major depressive disorder (MDD) using the Structured Clinical Interview for DSM-IV Axis I Disorders (SCID; Spitzer, Williams, Gibbon, & First, 1992). Following random assignment to treatment and control groups, mothers were re-assessed at post-treatment and at a three-month follow-up. Results indicated that mothers receiving IH-CBT experienced significant benefits in terms of depression relative to controls. Compared to those receiving home visiting alone, mothers in the IH-CBT condition were less likely to meet diagnostic criteria for MDD at post-treatment (70.7% vs. 30.2%), reported fewer depressive symptoms, and obtained lower scores on clinician ratings of depression severity. Gains were maintained through three-month follow-up. Importantly, findings remained when controlling for psychiatric comorbidity, severity of MDD at baseline, therapist, home visiting model, and number of home visits. While these findings are encouraging, the focus of the study was on depression and other areas of functioning that are relevant to maternal adjustment and home visiting were unaddressed.
The purpose of this study was to examine the efficacy of IH-CBT in addressing maternal psychological distress and social functioning in the clinical trial. Specifically, new mothers enrolled in a community-based home visiting program were identified using a two-step process comprised of a screen and subsequent confirmation of MDD diagnosis. Mothers were 16 years of age or older and were identified at three months postpartum. They were randomly assigned to IH-CBT + home visiting or standard home visiting (in which mothers were permitted to obtain treatment in the community). Measures of psychological distress and social functioning were administered at pre-treatment, post-treatment, and three-month follow-up. We posited that the synergistic relationship between IH-CBT and concurrent home visiting would impart significant benefits to depressed mothers in terms of reduced psychological distress and improved social functioning. It was hypothesized that, at post-treatment, mothers receiving IH-CBT would report lower levels of psychological distress, higher levels of social support, and increased social network size and involvement in contrast with controls. It was further expected that improvements in the IH-CBT group would be sustained over the three-month follow-up.
Method
Participants
Subjects consisted of 93 new mothers aged 16 or older who participated in a home visiting program and were diagnosed with major depressive disorder (MDD). Mothers were enrolled in Every Child Succeeds, a community-based home visiting program serving Southwestern Ohio and Northern Kentucky (USA). The geographic area covered by the program included urban, suburban and rural areas. Two models of home visiting were utilized in this program: Healthy Families America (HFA; Holton & Harding, 2007) and Nurse-Family Partnership (NFP; Olds, 2010). Participating mothers had at least one of the following demographic risk characteristics needed for eligibility: unmarried, low income, ≤18 years, and inadequate prenatal care. Mothers were enrolled in home visiting prior to 28 weeks gestation in NFP as per model parameters and from 20 weeks gestation through the child reaching three months of age for HFA. Mothers were referred from prenatal clinics, hospitals, social service agencies, and community physicians. NFP home visits were provided by nurses, while in HFA home visits were provided by social workers, related professionals and paraprofessionals. The goals of the home visiting program were to (1) improve pregnancy outcomes through nutrition education and substance use reduction; (2) support parents in providing children with a safe, nurturing, and stimulating home environment; (3) optimize child health and development; (4) link families to healthcare and other needed services; and (5) promote economic self-sufficiency.
Mothers were young (range was 16–37 years, M = 21.9, SD = 4.8), predominantly Caucasian (62.4%) and African-American (32.2%), unmarried (87.1%), and low income (76.3% <$20,000 annual household income). The SCID (Spitzer et al., 1992) was used to diagnose MDD and other psychiatric disorders at pre-treatment. The breakdown of MDD severity was Mild = 28.0%, Moderate = 48.4%, and Severe = 23.6%. Recurrent depression was reported by 74.2% of mothers (mean number of episodes = 2.6 (SD = 1.6), mean age of first episode = 15.2 years (SD = 5.1)). Comorbidity was high, with 76.1% of participants meeting criteria for other psychiatric disorders. The five most represented diagnoses were: PTSD = 40.9%, generalized anxiety disorder = 36.6%, social phobia = 30.1%, obsessive-compulsive disorder = 26.9%, panic disorder = 25.8%.
Design
A randomized clinical trial design was used with assessments at pre-treatment, post-treatment, and three-month follow-up. Participants were randomized to IH-CBT (IH-CBT + home visiting) or standard home visiting (SHV; home visiting alone) groups following the pre-treatment assessment. Randomization was stratified by race and home visiting model (HFA, NFP). Within the IH-CBT group a further randomization was done to assign individuals to therapists (n = 2). The randomization schedule was prepared prior to the start of the study and assignments were placed in separate envelopes that were opened when each subject was eligible to be randomized.
During recruitment, 1,768 mothers were enrolled in the home visiting program and eligible to be screened for depression. Of these, 1,240 (70.1%) were screened using the Edinburgh Postnatal Depression Screen (Cox et al., 1987). Of those screened, 306 (24.7%) had scores of ≥11 which suggested potential MDD (Gibson, McKenzie-McHarg, Shakespeare, Price, & Gray, 2009). Among mothers with scores at or above the screening cutoff, 151 (49.3%) were referred to the study. Reasons for not being referred included already receiving treatment in the community, disinterest, and not having time to participate. No differences were found between screened and unscreened mothers, those with scores above or below the cutoff, and those referred or not referred on mother age and race, household income, baby age, or home visiting model (all p > 0.05). Mothers with scores at or above the cutoff who were referred to the study had higher EPDS scores at screening relative to those not referred (M = 15.9 (SD = 5.2) vs. M = 14.5 (SD = 3.4), t = 2.8, p < 0.01).
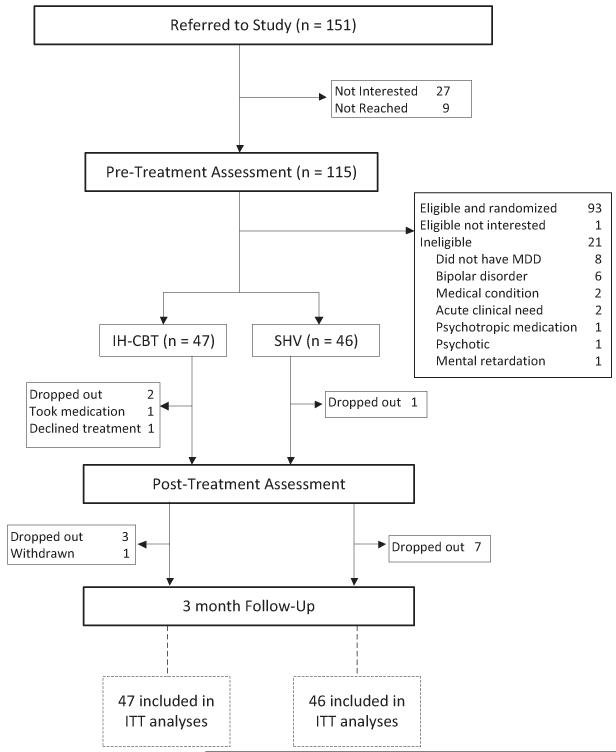
Fig. 1 shows the CONSORT diagram starting at referral. Of the 151 referred mothers, 115 received a pre-treatment assessment. Twenty-seven referred mothers were not interested in participating, and 9 were unable to be reached. There were no differences between assessed and non-assessed participants on mother age, mother race, household income, baby age, or home visiting model (all p > 0.05). Ninety-four of 115 participants were found to be eligible. Reasons for ineligibility were not having MDD (8), having bipolar disorder (6), medical condition contributing to psychiatric presentation (2), acute clinical need (2), taking psychotropic medication (1), psychotic (1), and mental retardation (1). One mother was disinterested in participating following the assessment but prior to randomization. The remaining 93 mothers were randomized to IH-CBT (n = 47) or SVH (n = 46) and comprised the intent to treat sample. Between pre-treatment and post-treatment assessments, 1 mother in IH-CBT started medication following the 1st treatment session and another declined treatment after randomization. Three mothers dropped out of the study between pre-treatment and post-treatment, and an additional 10 dropped out between post-treatment and follow-up. There were no differences in dropout rate between conditions, and dropout was unrelated to initial MDD severity, recurrent vs. single episode MDD, or psychiatric comorbidity (p > 0.05). One mother in IH-CBT did not receive the follow-up assessment as it coincided with the death of her child. Overall, 93.5% of participants received at least one of the post-treatment and follow-up assessments.
Fig. 1.
Flow of participants through study. Randomization was stratified by race, home visiting model, and therapist.
Procedures
Mothers were recruited in a two-step process. First, home visitors administered the EPDS to mothers at three months postpartum. Mothers who screened positive were approached to participate in the study. Following presentation of the consent form, interested mothers received a pre-treatment and eligibility assessment. Inclusion criteria were ≥ 16 years of age and current diagnosis of MDD. Exclusion criteria were bipolar disorder, current substance dependence, psychosis, mental retardation, suicidality or homicidality requiring acute intervention, or current use of psychotropic medications or psychotherapy. Mothers with a history of receiving medication and/or psychotherapy but who had not received treatment in the six months prior to enrollment in the study were included. Assessments were conducted at pre-treatment, post-treatment (about 5 months later), and three month follow-up. Each assessment was conducted in the home over one or two sessions. Participants received $35 for completion of the post-treatment assessment and $45 for the follow-up assessment.
Mothers assigned to IH-CBT were asked not to receive additional treatment during treatment phase of the trial. Receipt of mental health treatment was documented in the SHV group at post-treatment and in both the IH-CBT and SHV groups at follow-up assessments. Mothers in the SHV group were permitted to obtain treatment in the community. Those who still met diagnostic criteria using the SCID at post-treatment had the option of receiving IH-CBT. Both receipt and adequacy of treatment was documented and explored in secondary analyses. The study was approved by our hospital’s Institutional Review Board.
Experimental conditions
In-Home Cognitive Behavioral Therapy
Mothers in the IH-CBT condition received IH-CBT + home visiting. IH-CBT was delivered in the home by two licensed master’s level social workers. Treatment consisted of 15 sessions that were scheduled weekly and lasted 60 min plus a booster session one month post-treatment. The focus and content of treatment followed the directives of CBT (Beck, 2011). The primary target of treatment was depression reduction. Treatment components included behavioral activation, identification of automatic thoughts and schemas, thought restructuring, and relapse prevention (Hollon & Dimidjian, 2009). Significant adaptations to CBT were made to address setting, population, and context in order to maximize engagement and outcomes (Goodheart, Kazdin, & Sternberg, 2006). These adaptations were made based upon a review of the literature, consultation with home visitors, and input from mothers in home visiting.
First, IH-CBT was delivered in the home. Although CBT has been provided in the home before, there are unique challenges in administering treatment in the homes of young, low income mothers. These require creative solutions and accommodations to ensure effective treatment delivery in environments where privacy was often difficult to guarantee, the child was present, and unexpected interruptions occurred. However, providing treatment in the home offered advantages in that many of the clinical issues that were addressed in treatment occurred in the home setting, and the therapist was able to observe elements of the home that may have been contributory to the clinical presentation.
The second adaptation involved addressing the primary concerns of young, low income, new mothers who were socially isolated (Levy & O’Hara, 2010). Treatment content focused on issues relevant to this population, such as transition to adult roles, stress management, parenting challenges, and family relationships. For the youngest mothers, additional contextual and developmental issues were incorporated into treatment (e.g., school attendance, living with parents). As many of these mothers have experienced significant trauma in their lives (Ammerman Putnam, Chard, Stevens, & Van Ginkel, 2012) this, too, is addressed in treatment.
The third adaptation sought to facilitate close collaboration with home visitors. Collaboration occurred through frequent written communication between therapist and home visitor utilizing a shared web-based documentation system, and telephone contact as needed. In addition, the home visitor attended the 15th session with the mother and therapist. Weekly supervision was provided by doctoral level clinicians and included review of audiotaped sessions. Therapists completed a self-reported fidelity checklist indicating adherence to elements of CBT (e.g., use of CBT tools) and IH-CBT particularly (e.g., contacted home visitor to collaborate).
In the trial, mothers receiving IH-CBT had a mean of 11.2 (SD = 5.5) sessions. Those who completed all 15 sessions + 1 month booster comprised 48.9% of this group. Among those who partially completed treatment, the range was 1–14 sessions and the median number of sessions was 7. All randomized subjects were included in analyses regardless of the number of sessions received in the IH-CBT condition consistent with the intent to treat approach.
Standard home visiting
In standard home visiting (SHV), mothers received services from home visitors as per the HFA and NFP model directives. Both models call for regular home visits during the intervals covered during the trial, and home visitors are given discretion to increase frequency of visits if needed. Curricula for both models are distinct but emphasize child health and development, nurturing mother-child relationship, maternal health and self-sufficiency, and linkage to other community services. Consistent with standard of care, mothers in the SHV condition were permitted to receive treatment for depression in the community. Tracking of treatment utilization indicated that 34.9% of SHV mothers received mental health treatment in the community between pre-treatment and post-treatment (20.9% received medication, 16.3% received psychotherapy). Between post-treatment and follow-up, 44.7% received community treatment (18.4% received medication, 36.8% received psychotherapy). Guided by Kessler et al. (2003), we generated definitions of adequacy of treatment received. For medication, adequate treatment was defined as receiving an approved antidepressant and maintenance for at least two months. For psychological treatment, adequate treatment was defined as receiving psychotherapy for at least 4 sessions over two months. During the pre-treatment to post-treatment interval for the SHV group as a whole, 7.0% were found to have received adequate treatment. During the post-treatment to follow-up interval, 15.8% were found to have received adequate treatment.
Measures
Edinburgh Postnatal Depression Scale (EPDS; Cox et al., 1987)
The EPDS is a 10 item self-report measure of depressive symptoms. Items consist of depressive symptoms that are endorsed on a four point scale indicating occurrence and severity over the past week, yielding a total score. The EPDS was used to screen mothers for eligibility for the pre-treatment assessment using a cutoff of ≥ 11. The Cronbach’s alpha for the measure was 0.91.
Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I, January 2007 version; Spitzer et al., 1992)
The SCID is a semi-structured psychiatric interview that is widely used in research and clinical practice. It is used to diagnose 14 common psychiatric disorders, including MDD. Interviews were audio-recorded and 25% were rated by a second rater yielding a kappa coefficient = 0.89. The full SCID was administered at the pre-treatment assessment and used to diagnose MDD, determine parameters of MDD (e.g., recurrence), and diagnose comorbid conditions.
Brief Symptom Inventory (BSI; Derogatis, 1993)
The BSI is a brief version of the widely used Symptom Checklist-90 (SCL-90), a measure of global psychological distress. The BSI consists of 53 items endorsed using a 5 point scale reflecting level of distress of each symptom. Standardized scores are yielded for three global (Global Severity Index, Positive Symptom Distress Index, Positive Symptom Total) and nine clinical (Somatization, Obsessive-Compulsive, Interpersonal Sensitivity, Depression, Anxiety, Hostility, Phobic Anxiety, Paranoid Ideation, Psychoticism) scales. The Global Severity Index (GSI) was used as the primary indicator of psychological distress followed by post hoc comparisons on the remaining global and clinical scales. The Cronbach’s alpha for the measure in this sample ranged from 0.94 to 0.95 across the three assessment points.
Interpersonal Support Evaluation List (ISEL; Cohen & Hoberman, 1983)
The ISEL is a widely used self-report of social support that has been utilized with multiple clinical and non-clinical populations. This 40-item measure consists of statements regarding the availability and use of tangible and emotional support from others that are endorsed using a 4-point scale reflecting the degree to which they are true. Sample items include: “If I were sick, I could easily find someone to help me with my daily chores,” and “There is at least one person I know whose advice I really trust.” The total score was used as the primary indicator in the current study. Post hoc comparisons were conducted on the four subscale scores: Appraisal (availability of someone to talk to), Tangible (availability of material aid), Self-Esteem (availability of a positive comparison when comparing oneself to others), and Belonging (availability of people with whom one can do things). The ISEL has excellent reliability and validity (Cohen and Hoberman). The Cronbach’s alpha for the measure in this sample ranged from 0.93 to 0.95 across the three assessment points.
Social Network Index (SNI; Cohen, Doyle, Skoner, Rabin, & Gwaltney, 1997)
The SNI consists of 12 items that document the size and features of the mother’s social network. The SNI yields three summary scores. Network size reflects the number of people with whom the mother has had contact in the prior two weeks. Network diversity is the number of social roles (e.g., parent, close friend, employee) in which the mother has regular contact. Embedded networks reflects the number of different network domains (e.g., family, school) in which the mother is active.
Results
Overview of analyses
An intent to treat approach was used such that all randomized subjects were included in analyses. As groups did not differ on demographics and baseline clinical characteristics, these were not included as covariates. Therapist, single episode vs. recurrent MDD, and initial MDD severity were examined as moderators of outcomes. Primary analyses involved summary scores for the BSI (Global Severity Index), ISEL (total score), and the three scales of the SNI. Secondary post hoc comparisons were conducted on subscale scores of the BSI and ISEL. Analyses used linear mixed effect regression with restricted maximum likelihood estimation (PROC MIXED, SAS version 9.3). This approach accounts for missing data and uses all data in estimating effects (Verbeke & Molenberghs, 2000). The basic model included terms for group assignment (IH-CBT or SHV), time (pre-treatment, post-treatment and follow-up) and the interaction between group and time. Different correlation structures for the repeated measurements were explored and compared using a goodness of fit test. When a significant time by group interaction term was observed, we conducted follow-up analyses by dividing the data on the level of the interaction variables and reporting the corresponding least square means which are the predicted means derived from the fitted model. We also report group comparisons at post-treatment and follow-up time points. Effect size measures were generated using the least square means and corresponding standard errors along the respective sample size for each group that resulted from fitting the mixed model based on the intent to treat sample. To control for multiple comparisons the reported p-values for the primary analyses were adjusted using a false discovery rate methodology (Benjamini & Hochberg, 2000).
Sample characteristics
Table 1 shows the demographics of the two groups. No differences were found between treatment and control groups on these variables. In addition, there were no differences between groups on the risk variables (unmarried, low income, ≤18 years, inadequate prenatal care) used to determine eligibility for the home visiting program. In terms of home visiting model, 81 mothers were in the HFA model and 12 in the NFP model. Eighty-five mothers were primiparous and 8 had more than one child (all of these were in the HFA model). Mothers received a mean of 13.9 (SD = 9.2) home visits prior to assessment. No differences were found on one vs. multiple children (χ2(1) = 0.0, p > 0.05) or number of home visits received (t(91) = 1.2, p > 0.05).
Table 1.
Demographic characteristics of IH-CBT (n = 47) and SHV (n = 46) participants
| Variable | IH-CBT condition M (SD) or N (%) |
SHV condition M (SD) or N (%) |
t or x2 | p-value |
|---|---|---|---|---|
| Mother age (years) | 22.4 (5.2) | 21.5 (3.9) | 0.9 | ns |
| Mother race | ||||
| White | 30 (63.8%) | 28 (60.8%) | 1.2 | ns |
| African American | 14 (29.9%) | 16 (34.8%) | ||
| Native American | l (2.1%) | 0 (0.0%) | ||
| Native Hawaiian or other Pacific Islander | l (2.1%) | 1 (2.2%) | ||
| Bi-racial | 1 (2.1%) | 1 (2.2%) | ||
| Mother ethnicity | ||||
| Latina | 3 (6.4%) | 4 (8.7%) | 0.5 | ns |
| None | 44 (93.6%) | 42 (91.3%) | ||
| Marital status | ||||
| Single, never married | 41 (87.2%) | 39 (84.8%) | 1.0 | ns |
| Married | 6 (12.8%) | 6 (13.0%) | ||
| Separated | 0 (0.0%) | 1 (2.2%) | ||
| Education (years) | 11.6 (2.0) | 11.3 (1.7) | 1.0 | ns |
| Income | ||||
| $0–9,999 | 27 (58.7%) | 25 (54.3%) | 7.5 | ns |
| $10,000–19,999 | 6 (13.0%) | 13 (28.3%) | ||
| $20,000–29,999 | 10 (21.7%) | 4 (8.7%) | ||
| $30,000–39,999 | 2 (4.3%) | 1 (2.2%) | ||
| $40,000–49,999 | 0 (0.0%) | 2 (4.3%) | ||
| >$50,000 | 1 (2.2%) | 1 (2.2%) | ||
| Child’s age (days) | 159.8 (73.7) | 146.1 (74.4) | 0.9 | ns |
Moderating variables
Recurrent depression (single episode vs. recurrent MDD), initial MDD severity, home visiting model, and home visitor were examined as moderating variables by including them in the mixed model that contains the terms group, time, and group by time interaction, as a main effect and interaction terms (two-and three-way). These variables were found to be non-significant on all outcome variables (p > 0.05). In the IH-CBT condition, no significant differences were found between therapists on baseline subject demographic and clinical characteristics and on all outcome variables.
Group comparisons
Table 2 presents the means, SDs, and F-values (group × time) for the primary and secondary comparisons of the IH-CBT and SHV groups across the three time points (pre-treatment, post-treatment, follow-up). In terms of primary comparisons, results indicated statistically significant reductions in psychological distress (Global Severity Index of the BSI) in the IH-CBT group relative to those in the SHV group over time (p < 0.001). Effect sizes were 0.77 at post-treatment and 0.73 at follow-up, reflecting the upper range of moderate effect sizes. T-tests at post-treatment and follow-up showed significantly lower scores on this variable for the IH-CBT group in contrast to the SHV condition at each time point (t = 3.47, p < 001, and t = 3.22, p < .001, respectively). Post hoc group contrasts on BSI subscales showed large and broad reductions in different aspects of psychological distress as measured by the instrument. Statistically significant group × time interactions were found in all scales. T-tests comparing groups at post-treatment and follow-up revealed large and statistically significant (p < 0.05) drops in the IH-CBT vs. the SHV conditions on all subscales at each time point with the exception of Anxiety. Although the IH-CBT group had lower Anxiety scores at post-treatment (t = 3.0, p < 001) than their SHV counterparts, this comparison was non-significant at follow-up (t = 1.73, p = 0.088).
Table 2.
Comparisons between IH-CBT (N= 47) and SHV (N=46) groups on psychological distress and social functioning at each time point.
| Measure | Group |
F-value (group × time) |
|||||
|---|---|---|---|---|---|---|---|
| IH-CBT |
SHV |
||||||
| Pre | Post | Follow-up | Pre | Post | Follow-up | ||
| Brief Symptom Inventory | |||||||
| Global severity | 74.3 (5.2) | 60.8 (12.2) | 57.6 (16.5) | 74.4 (5.7) | 69.4 (10.0) | 67.8 (10.7) | 7.95*** |
| Positive symptom distress | 70.6 (5.7) | 59.4 (11.1) | 56.4 (13.0) | 70.7 (6.3) | 65.4 (9.8) | 64.4 (9.1) | 4.87*** |
| Positive symptom total | 81.1 (l1.9) | 62.3 (16.4) | 56.7 (20.8) | 79.5 (12.5) | 71.2 (12.8) | 66.5 (18.1) | 5.64*** |
| Somatization | 66.5 (l0.l) | 56.2 (12.5) | 53.8 (13.2) | 66.6 (10.8) | 62.4 (11.0) | 60.5 (10.7) | 4.52* |
| Obsessive-compulsive | 73.4 (6.0) | 62.1 (12.6) | 58.1 (15.8) | 74.0 (7.2) | 69.6 (9.9) | 67.8 (10.0) | 5.37** |
| Interpersonal sensitivity | 71.2 (6.4) | 58.9 (11.6) | 54.7 (12.6) | 70.4 (6.2) | 65.4 (10.3) | 64.0 (11.9) | 9.08*** |
| Depression | 70.2 (5.2) | 57.4 (11.7) | 55.1 (11.7) | 71.1 (4.4) | 65.8 (9.9) | 63.4 (10.9) | 6.31** |
| Anxiety | 67.7 (6.5) | 54.5 (12.9) | 53.4 (13.6) | 67.3 (8.2) | 62.3 (9.9) | 58.46 (12.0) | 5.72** |
| Hostility | 73.7 (6.2) | 62.4 (11.6) | 58.5 (14.9) | 74.6 (5.5) | 70.2 (8.5) | 68.4 (12.0) | 7.10** |
| Phobic anxiety | 66.7 (10.0) | 55.0 (11.5) | 53.4 (11.0) | 65.5 (10.1) | 63.4 (10.7) | 60.5 (10.3) | 7.81*** |
| Paranoid ideation | 73.7 (7.0) | 62.1 (13.2) | 59.2 (13.3) | 72.7 (6.9) | 68.7 (8.9) | 65.3 (11.2) | 5.23** |
| Psychoticism | 74.5 (5.6) | 61.3 (12.0) | 58.5 (12.2) | 74.9 (5.4) | 70.6 (10.1) | 67.1 (12.5) | 8.66*** |
| Interpersonal Support Evaluation List | |||||||
| Total score | 55.8 (21.4) | 75.8 (22.9) | 83.6 (21.4) | 60.4 (21.8) | 66.5 (25.5) | 68.1 (26.4) | 5.08*** |
| Appraisal | 14.6 (6.8) | 20.6 (7.0) | 22.9 (5.7) | 15.6 (7.6) | 18.0 (7.8) | 18.1 (8.2) | 4.12* |
| Tangible | 15.0 (6.3) | 19.4 (6.5) | 20.4 (6.1) | 16.7 (6.9) | 17.7 (7.5) | 18.6 (6.9) | 3.18* |
| Self-Esteem | 12.8 (5.5) | 17.5 (5.7) | 19.8 (5.9) | 12.9 (4.9) | 14.7 (6.0) | 14.9 (6.6) | 4.46* |
| Belonging | 13.5 (6.5) | 18.3 (6.3) | 20.6 (6.1) | 15.2 (6.9) | 16.1 (7.9) | 16.5 (7.6) | 4.88** |
| Social Network Index | |||||||
| Network size | 7.9 (4.1) | 11.6 (7.9) | 12.8 (8.8) | 10.8 (6.1) | 12.4 (7.5) | 12.5 (6.8) | 1.88 |
| Network diversity | 5.1 (1.3) | 5.4 (1.9) | 5.5 (1.6) | 5.6 (1.7) | 5.6 (1.6) | 5.6 (1.4) | 0.63 |
| Embedded networks | 0.9 (0.7) | 1.4 (1.1) | 1.7 (1.5) | 1.4 (1.0) | 1.6 (1.1) | 1.5 (1.2) | 2.23 |
p < 0.05.
p < 0.01.
p < 0.001.
A significant group × time effect was also found for the ISEL total score, indicating that subjects in the IH-CBT condition reported increased social support (p < 0.001) over time relative to those in the SHV group. Effect sizes were 0.38 at post-treatment and 0.65 at follow-up, reflecting a small effect at post-treatment and a moderate effect at follow-up. T-tests at post-treatment and follow-up showed no group difference on the ISEL total score at post-treatment (t = 1.75, p = 0.084) although there was a significantly higher score for the IH-CBT group in contrast to the SHV condition at follow-up (t = 2.84, p < 0.01). Post hoc group contrasts on the subscales of the ISEL showed broad improvements in social support in the IH-CBT vs. SHV conditions over time. Examination of groups at each time point revealed differential patterns of social support types. Non-significant comparisons were found on the Appraisal (t = 1.63, p > 0.05), Tangible (t = 1.08, p > 0.05), and Belonging (t = 1.42, p > 0.05) subscales at post-treatment. The Tangible subscale remained non-significant at follow-up (t = 1.20, p > 0.05), although significant group contrasts emerged at follow-up on the Appraisal (t = 2.98, p < 0.01) and Belonging (t = 2.59, p < 0.05) subscales indicating increased social support in IH-CBT subjects relative to SHV subjects. The Self-Esteem subscale was significantly different at post-treatment (t = 2.23, p < 0.05) and follow-up (t = 3.39, p < 0.01) indicating increased social support in IH-CBT than SHV subjects at both time points.
In contrast to psychological distress and social support, group × time interactions were statistically non-significant for all three social network domains of the SNI. For each scale, both groups either remained stable over time or showed increases over time.
Discussion
This study reported results of a clinical trial of an adapted treatment for depressed mothers in home visiting with an emphasis on changes in psychological distress and social functioning. IH-CBT is among the first treatments specifically designed for depressed new mothers in home visiting. Although IH-CBT is focused on and has demonstrated efficacy in ameliorating depressive symptoms, this study examined its potentially broader impact on psychological distress and social adjustment. Findings revealed that relative to controls, mothers receiving IH-CBT had decreased levels of psychological distress and increased social support. These areas are important for maternal health and effective parenting and are typically targeted in home visiting programs. To the extent that IH-CBT has a positive impact on maternal psychological distress and social functioning, home visiting programs are in a better position to yield optimal outcomes for mothers and children.
Improvements in psychological distress were documented across multiple areas. Almost all of the scales of the Brief Symptom Inventory (BSI), including global indices and specific clinical domains, showed reductions over time in the IH-CBT compared to the SHV conditions. Effect sizes were robust at both post-treatment (0.77) and at three month follow-up (0.73), indicating that improvements emerged at the end of treatment were maintained through follow-up. The decrease in psychological distress may reflect a shared pathway with depression, which in a prior report was shown to drop significantly in mothers receiving IH-CBT (Ammerman et al., 2013). Comorbid symptoms may also be driven by independent processes that also responded to the CBT approach and the components of IH-CBT designed to maximize engagement and impact (e.g., delivery in the home setting; focus on issues relevant to young, low income new mothers; strong collaboration between home visitor and therapist). When mothers are less preoccupied with psychological distress, they are more available to their children and more amenable to home visiting.
Mothers receiving IH-CBT also reported higher levels of social support in contrast to those in the SHV condition. Both the total score of the Interpersonal Support Evaluation List (ISEL) and the subscale scores reflected increased support in treated mothers over time. The robustness of the effect was lagged over time in that effect sizes were only 0.38 at post-treatment but increased to 0.65 at follow-up. T-tests of subscale sores at each time point confirmed that the benefits of IH-CBT for social support emerged slowly and were most evident at follow-up. It is possible that decreases in psychological distress (and depression) precede and contribute to improvements in perceived social support. As mothers experience a reduction in debilitating psychological symptoms, they may be more likely to reach out to existing social resources. This process is likely facilitated by home visitors, who are encouraged to help mothers strengthen natural social ties and relationships. Indeed, number of home visits is associated with improved depression outcomes in mothers receiving IH-CBT (Ammerman, Peugh, Putnam, & Van Ginkel, 2012). It is notable that the affiliation and affirming subscales of the ISEL improved over time in IH-CBT compared to SHV mothers, but group differences were not found in the Tangible subscale at post-treatment or follow-up. Mothers reported increased emotional support from and connection with others, but there was no change in the availability of practical assistance. As perceived social support is important to physical and mental health and nurturing parenting (Balaji et al., 2007), an intervention such as IH-CBT helps mothers access and utilize their supports in a way that benefits both mothers and children.
No differences between IH-CBT and SHV were found for social network. Thus, although mothers in IH-CBT felt more supported by others, this was not attributable to growth in the number of individuals in the network or increased involvement with existing networks. The lack of change in network is also consistent with the non-significant finding for the Tangible subscale of the ISEL, which would benefit from a more robust and reliable social network. IH-CBT has a relatively focused emphasis on mood management and reduction of depressive symptoms, not increasing social networks, which may partially account for this result. In addition, findings also underscore the isolation of mothers in home visiting (Harden, 2010) and the challenges encountered by mothers in expanding social networks during the perinatal period. Of course, the quality of the social network is important—large but unsupportive networks may have detrimental effects on maternal functioning. Small social networks, however, leave mothers vulnerable to further isolation. Increasing social supports, including expanding social networks, is a secondary objective of home visiting. Results from this study suggest that, for depressed mothers, such efforts are particularly impeded. Depressed mothers may need additional help and support in building strong and durable social networks, even when depression, psychological distress, and social support have improved.
Future research needs to extend and expand study of the potential benefits and limitations of IH-CBT as a treatment for depression and associated clinical features in mothers in home visiting. It is important to know if mothers receiving IH-CBT improve in parenting skills, nurturing, and attachment with their children. Although decreased psychological distress and increased social support provide a more favorable context for learning these skills, this remains an empirical question in need of further research. The longer term impact of treatment is unknown, as this study followed mothers for three months post-treatment. Risk for relapse is high in depression, and it is possible that gains made during and in the three month interval after treatment may dissipate should a new depressive episode emerge. In contrast, risk for relapse is lower in those treated with CBT relative to most other treatments for depression (Dobson et al., 2008), and mothers in home visiting who have recovered from depression as a result of treatment may experience longer intervals between depressive episodes as a result of the support provided by continued home visiting services.
The study had several strengths. First, the design provided a rigorous framework within which to examine IH-CBT and its impact on psychological distress and social functioning. Given that some home visiting programs have made investments in approaches that are untested and may be ineffective, this study offers evidence for a treatment that benefits depressed women. Findings are generalizable to low income, socially isolated mothers, who in turn reflect the largest population enrolled in home visiting programs. Second, the use of a semi-structured diagnostic interview to identify mothers with MDD is an improvement on research that relies solely on a self-report screen of depression. Third, an intent to treat strategy was used and retention of the sample was good, particularly for this high-risk population. Fourth, two widely disseminated models of home visiting were represented in the sample. IH-CBT was designed to fit seamlessly with different home visiting models. The fact that model did not moderate response to treatment provides support that IH-CBT is efficacious across multiple approaches and is generalizable to other home visiting programs.
The study also has several limitations that warrant caution in interpreting findings. First, the sample size was relatively small, limiting power particularly for moderating analyses. Regardless, effect sizes for moderating variables were small and statistically non-significant. Second, outcome measures were self-report. However, the clear referents on the Social Network Index make it less vulnerable to the biases inherent in more subjective self-report measures. Third, there was no long term follow-up. It is not known if gains were sustained beyond the three month follow-up time point. Fourth, some mothers in the SHV condition received treatment in the intervals between pre-treatment, post-treatment and follow-up. This was by design in that the SHV condition reflected “home visiting as usual” in which mothers were permitted to obtain community treatment. As noted, only a small minority received adequate treatment. To the extent that community treatment may have benefited some mothers in the SHV condition, this provides a more conservative test of the efficacy of IH-CBT in addressing psychological distress and social functioning. Fifth, because some home visitors had mothers in both IH-CBT and SHV conditions, there is a risk of contamination. Such a confound would mitigate effect sizes and it is unlikely that this was a significant concern given the robustness of the superiority of IH-CBT to home visiting alone. Moreover, none of the home visitors were taught CBT strategies, and it is improbable that they would acquire such skills simply by having mothers in the treatment condition. And sixth, findings may not be generalizable to more affluent mothers with higher levels of social and emotional resources.
Conclusions
Results from this study add to the growing body of literature demonstrating that systematic adaptations to evidence-based treatments have the potential to yield clinically meaningful and efficacious interventions for high risk populations (Barrera, Castro, Strycker, & Toobert, 2012). IH-CBT provides an effective option for new mothers enrolled in home visiting who otherwise may go unidentified and untreated. Modifications to treatment implementation break down barriers to access, take advantage of other care providers already in the home to foster strong working relationships, and address salient needs in this population. Benefits of treatment appear to be broad, encompassing depression, psychological distress, and social support. IH-CBT is feasible and lends itself to adoption by other home visiting programs. It has the potential to significantly expand access to effective treatment to new mothers with depression and its associated features who otherwise face overwhelming barriers to care. Future research needs to further examine the impact of IH-CBT on other aspects of maternal and child functioning (e.g., parenting, child development) and the potential longer term benefits of treatment.
Acknowledgements
The authors thank Drs. Neil M. Richtand, Lawson R. Wulsin, and Floyd R. Sallee for their assistance to the study.
Footnotes
Supported by Grant R34MH073867 from the National Institute of Mental Health. The authors acknowledge the participation and support of The Health Foundation of Greater Cincinnati, United Way of Greater Cincinnati, Kentucky H.A.N.D.S., Ohio Help Me Grow, and www.OhioCanDo4Kids.org.
References
- Administration on Children Youth and Families . Making a difference in the lives of children and families: The impacts of Early Head Start Programs on infants and toddlers and their families. U.S. Department of Health and Human Services; Washington, DC: 2002. [Google Scholar]
- Ammerman RT, Peugh JL, Putnam FW, Van Ginkel JB. Predictors of treatment response in depressed mothers receiving In-Home Cognitive Behavioral Therapy and concurrent home visiting. Behavior Modification. 2012;36:462–481. doi: 10.1177/0145445512447120. http://dx.doi.org/10.1177/0145445512447120. [DOI] [PubMed] [Google Scholar]
- Ammerman RT, Putnam FW, Altaye M, Stevens J, Teeters AR, Van Ginkel JB. A clinical trial of In-Home CBT for depressed mothers in home visitation. Behavior Therapy. 2013 doi: 10.1016/j.beth.2013.01.002. http://dx.doi.org/10.1016/j.beth.2013.01.002. Advanced online publication. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ammerman RT, Putnam FW, Bosse NR, Teeters AR, Van Ginkel JB. Maternal depression in home visiting: A systematic review. Aggression and Violent Behavior. 2010;15:191–200. doi: 10.1016/j.avb.2009.12.002. http://dx.doi.org/10.1016/j.avb.2009.12.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ammerman RT, Putnam FW, Chard KM, Stevens J, Van Ginkel JB. PTSD in depressed mothers in home visitation. Psychological Trauma: Theory, Research, Practice and Policy. 2012;4:186–195. doi: 10.1037/a0023062. http://dx.doi.org/10.1037/a0023062. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ammerman RT, Putnam FW, Stevens J, Bosse NR, Short JA, Bodley AL, Van Ginkel JB. An open trial of In-Home CBT for depressed mothers in home visiting. Maternal and Child Health Journal. 2011;15:1333–1341. doi: 10.1007/s10995-010-0691-7. http://dx.doi.org/10.1007/s10995-010-0691-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Astuto J, Allen L. Home and young children: An approach worth investing in? Society for Research in Child Development, Social Policy Report. 2009;23:3–22. [Google Scholar]
- Balaji AB, Claussen AH, Smith DC, Visser SN, Morales MJ, Perou R. Social support networks and maternal mental health and well-being. Journal of Women’s Health. 2007;16:1386–1396. doi: 10.1089/jwh.2007.CDC10. http://dx.doi.org/10.1089/jwh.2007.CDC10. [DOI] [PubMed] [Google Scholar]
- Barrera M, Jr., Castro FG, Strycker LA, Toobert DJ. Cultural adaptations of behavioral health interventions: A progress report. Journal of Consulting and Clinical Psychology, advance online publication. 2012 doi: 10.1037/a0027085. http://dx.doi.org/10.1037/a0027085. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Beck JS. Cognitive behavior therapy: Basics and beyond. 2nd edn Guilford; New York: 2011. [Google Scholar]
- Benjamini Y, Hochberg Y. On the adaptive control of the false discovery rate in multiple testing with independent statistics. Journal of Educational and Behavioral Statistics. 2000;25:60–83. [Google Scholar]
- Boller K, Strong DA. Home visiting: Looking back and moving forward. Zero to Three. 2010;30:4–9. [Google Scholar]
- Chazan-Cohen R, Ayoub C, Pan BA, Roggman L, Raikes H, McKelvey L, Whiteside-Mansell L, Hart A. It takes time: Impacts of Early Head Start that lead to reductions in maternal depression two years later. Infant Mental Health Journal. 2007;28:151–170. doi: 10.1002/imhj.20127. http://dx.doi.org/10.1002/imhj.20127. [DOI] [PubMed] [Google Scholar]
- Cohen S, Doyle WJ, Skoner DP, Rabin BS, Gwaltney JM., Jr. Social ties and susceptibility to the common cold. Journal of the American Medical Association. 1997;277:1940–1944. [PubMed] [Google Scholar]
- Cohen S, Hoberman HM. Positive events and social supports as buffers of life change stress. Journal of Applied Social Psychology. 1983;13:99–125. http://dx.doi.org/10.1111/j.1559-1816.1983.tb02325.x. [Google Scholar]
- Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. British Journal of Psychiatry. 1987;150:782–786. doi: 10.1192/bjp.150.6.782. [DOI] [PubMed] [Google Scholar]
- Denninger JW, van Nieuwenhuizen AO, Wisniewski SR, Luther JF, Trivedi MH, Rush AJ, Gollan JK, Pizzagalli DA, Fava M. Changes in depressive symptoms and social functioning in the Sequenced Treatment Alternatives to Relieve Depression Study. Journal of Nervous and Mental Disease. 2011;199:807–810. doi: 10.1097/NMD.0b013e31822fcbe2. http://dx.doi.org/10.1097/NMD.0b013e31822fcbe2. [DOI] [PubMed] [Google Scholar]
- Derogatis LR. Brief Symptom Inventory (BSI): Administration, scoring, and procedures manual. 3rd ed. National Computer Systems; Minneapolis, MN: 1993. [Google Scholar]
- Dobson KS, Hollon SD, Dimidjian S, Schmaling KB, Kohlenberg RJ, Gallop RJ, Rizvi SL, Gollan JK, Dunner DL, Jacobson NS. Randomized trial of behavioral activation, cognitive therapy, and antidepressant medication in the prevention of relapse and recurrence in major depression. Journal of Consulting and Clinical Psychology. 2008;76:468–477. doi: 10.1037/0022-006X.76.3.468. http://dx.doi.org/10.1037/0022-006X.76.3.468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Duggan A, Fuddy L, Burrell L, Higman SM, McFarlane E, Windham A, Sia C. Randomized trial of a statewide home visiting program to prevent child abuse: Impact in reducing parental risk factors. Child Abuse & Neglect. 2004;28:623–643. doi: 10.1016/j.chiabu.2003.08.008. http://dx.doi.org/10.1016/j.chiabu.2003.08.008. [DOI] [PubMed] [Google Scholar]
- Duggan A, Fuddy L, McFarlane E, Burrell L, Windham A, Higman S, Sia C. Evaluating a statewide home visiting program to prevent child abuse in at-risk families of newborns: Fathers’ participation and outcomes. Child Maltreatment. 2004;9:3–17. doi: 10.1177/1077559503261336. http://dx.doi.org/10.1177/1077559503261336. [DOI] [PubMed] [Google Scholar]
- Gibson J, McKenzie-McHarg K, Shakespeare J, Price J, Gray R. A systematic review of studies validating the Edinburgh Postnatal Depression Scale in antepartum and postpartum women. Acta Psychiatrica Scandinavica. 2009;119:350–364. doi: 10.1111/j.1600-0447.2009.01363.x. http://dx.doi.org/10.1111/j.1600-0447.2009.01363.x. [DOI] [PubMed] [Google Scholar]
- Goodheart CD, Kazdin AE, Sternberg RJ, editors. Evidence-based psychotherapy: Where practice and research meet. American Psychological Association; Washington, DC: 2006. [Google Scholar]
- Harden BJ. Home visitation with psychologically vulnerable families: Development in the profession and in the professional. Zero to Three. 2010;30:44–51. [Google Scholar]
- Hollon SD, Dimidjian S. Cognitive and behavioral treatment of depression. In: Gotlib IH, Hammen CL, editors. Handbook of depression. 2nd edn Guilford; New York: 2009. pp. 586–603. [Google Scholar]
- Holton JK, Harding K. Healthy Families America: Ruminations on implementing a home visiting program to prevent child maltreatment. Journal of Prevention and Intervention in the Community. 2007;34:13, 38. doi: 10.1300/J005v34n01_02. http://dx.doi.org/10.1300/J005v34n0102. [DOI] [PubMed] [Google Scholar]
- Howard KS, Brooks-Gunn J. The role of home-visiting programs in preventing child abuse and neglect. The Future of Children. 2009;19:119–146. doi: 10.1353/foc.0.0032. [DOI] [PubMed] [Google Scholar]
- Kessler RC, Berglund P, Demler O, Jin R, Koretz D, Merikangas KR, Rush AJ, Walters EE, Wang PS. The epidemiology of major depressive disorder: Results from the National Comorbidity Survey Replication (NCS-R) Journal of the American Medical Association. 2003;289:3095–3105. doi: 10.1001/jama.289.23.3095. http://dx.doi.org/10.1001/jama.289.23.3095. [DOI] [PubMed] [Google Scholar]
- Lakey B, Cronin A. Low social support and major depression: Research, theory and methodological issues. In: Dobson KS, Dozois DJA, editors. Risk factors in depression. Elsevier/Academic Press; Oxford: 2008. pp. 385–408. [Google Scholar]
- Lakey B, Orehek E. Relational regulation theory: A new approach to explain the link between perceived social support and mental health. Psychological Review. 2011;118:482–495. doi: 10.1037/a0023477. doi: 2011-09097-001 [pii] 10.1037/a0023477. [DOI] [PubMed] [Google Scholar]
- Landsverk J, Carrilio T, Connelly CD, Granger WC, Slymen DJ, Newton RR, Leslie L, Jones C. Healthy Families San Diego clinical trial: Technical Report. San Diego Children’s Hospital and Health Center; San Diego: 2002. [Google Scholar]
- Levy LB, O’Hara MW. Psychotherapeutic interventions for depressed, low-income women: A review of the literature. Clinical Psychology Review. 2010;30:934–950. doi: 10.1016/j.cpr.2010.06.006. http://dx.doi.org/10.1016/j.cpr.2010.06.006. [DOI] [PubMed] [Google Scholar]
- Olds DL. The Nurse-Family Partnership: From trials to practice. In: Reynolds AJ, Rolnick AJ, Englund MM, Temple JA, editors. Childhood programs and practices in the first decade of life: A human capital integration. Cambridge University Press; New York: 2010. pp. 49–75. [Google Scholar]
- Rhebergen D, Beekman ATF, de Graaf R, Nolen WA, Spijker J, Hoogendijk WJ, Penninx BWJH. Trajectories of recovery of social and physical functioning in major depression, dysthymic disorder and double depression: A 3-year follow-up. Journal of Affective Disorders. 2010;124:148–156. doi: 10.1016/j.jad.2009.10.029. http://dx.doi.org/10.1016/j.jad.2009.10.029. [DOI] [PubMed] [Google Scholar]
- Scott J, Teasdale JD, Paykel ES, Johnson AL, Abbott R, Hayhurst H, Moore R, Garland A. Effects of cognitive therapy on psychological symptoms and social functioning in residual depression. British Journal of Psychiatry. 2000;177:440–446. doi: 10.1192/bjp.177.5.440. http://dx.doi.org/10.1192/bjp.177.5.440. [DOI] [PubMed] [Google Scholar]
- Spitzer RL, Williams JB, Gibbon M, First MB. The Structured Clinical Interview for DSM-III-R (SCID). I: History, rationale, and description. Archives of General Psychiatry. 1992;49:624–629. doi: 10.1001/archpsyc.1992.01820080032005. [DOI] [PubMed] [Google Scholar]
- Stevens J, Ammerman RT, Putnam FW, Gannon TA, Van Ginkel JB. Facilitators and barriers to engagement in home visiting: A qualitative analysis of maternal, provider, and supervisor data. Journal of Aggression, Maltreatment, and Trauma. 2005;11:75–93. [Google Scholar]
- Tandon SD, Parillo K, Mercer C, Keefer M, Duggan AK. Engagement in paraprofessional home visiting: Families’ reasons for enrollment and program response to identified reasons. Womens Health Issues. 2008;18:118–129. doi: 10.1016/j.whi.2007.10.005. http://dx.doi.org/10.1016/j.whi.2007.10.005. [DOI] [PubMed] [Google Scholar]
- Tandon SD, Parillo KM, Jenkins C, Duggan AK. Formative evaluation of home visitors’ role in addressing poor mental health, domestic violence, and substance abuse among low-income pregnant and parenting women. Maternal and Child Health. 2005;9:273–283. doi: 10.1007/s10995-005-0012-8. http://dx.doi.org/10.1007/s10995-005-0012-8. [DOI] [PubMed] [Google Scholar]
- Verbeke G, Molenberghs G. Linear mixed models for longitudinal data. Springer; New York: 2000. [Google Scholar]