Abstract
U.S. birth and longer length of U.S. residence among the foreign-born have been linked to higher anthropometric measures. However previous studies have been cross-sectional and few have examined heterogeneity by ethnic group. Cross-sectional findings that show immigrant weight converging to U.S.-born levels with longer time in the U.S. imply that immigrants’ weight is increasing at a faster rate relative to U.S.-born individuals. Prospective studies are necessary to confirm this pattern. Using longitudinal data from 1486 Hispanic and 802 Chinese adults aged 45–84 years in the Multi-ethnic Study of Atherosclerosis, we examined whether foreign-born participants experienced greater increases in body mass index (BMI) and waist circumference (WC) than the U.S.-born over a median follow-up of 5 years. We also investigated heterogeneity in these associations by Hispanic subgroup. Among Hispanics and Chinese, the foreign-born had a lower adjusted mean BMI and WC at baseline than the U.S.-born, but there were no significant differences in BMI or WC change over time. There was heterogeneity by Hispanic subgroup: despite small baseline nativity differences in WC, foreign-born Mexican Hispanics had a greater annual mean increase in WC over time compared to U.S.-born Mexican Hispanics (mean difference in annual change=0.28 cm, P=0.03). There were no nativity differences in the rate of WC increase over time among non-Mexican Hispanics. Foreign-born Mexican Hispanics also experienced a faster rate of WC increase compared to foreign-born non-Mexican Hispanics (mean difference in annual change=0.24 cm, P=0.01). Longer time in the U.S., examined prospectively, may only be linked to adverse anthropometric changes in some immigrant groups.
INTRODUCTION
Over the past two decades, immigrants have represented a growing share of the U.S. population (1). Their increasing presence will have implications for overall population health and healthcare costs. A better understanding of immigrant health patterns is important for the design of public health interventions.
A common finding in studies of immigrants is a lower prevalence of obesity relative to the U.S.-born despite the comparatively low socioeconomic position of immigrants (2–6). However, longer length of U.S. residence has been associated with higher weight in immigrants suggesting that over time, the weights of immigrants converge to the levels observed among the U.S.-born (7–10). Acculturation to U.S. behavioral norms, such as poor diet and sedentary lifestyle, has been hypothesized to explain this relationship (11).
Existing research is primarily cross-sectional, precluding examination of change over time. In cross-sectional studies, the effects of time in the U.S. may be conflated with cohort or age effects. Conclusions drawn from cross-sectional studies assume that the weights of newly-arrived immigrant cohorts have remained relatively stable over time. However variability in immigrant selection processes and greater exposure to Western lifestyle behaviors within sending countries may invalidate this assumption (12, 13). Another challenge is separating the effects of longer U.S residence from those of age-related and secular increases in obesity (14, 15). The cross-sectional observation that longer-term immigrants have higher body mass index (BMI) or waist circumference (WC) may merely be a function of secular trends in weight impacting all segments of society rather than an effect of longer time in the U.S. Prospective data are thus critical to determine if immigrants’ weight is increasing at a rate faster than would be expected net of aging and period effects (16).
Although several studies have examined heterogeneity in these associations by race or ethnicity, data on various race or ethnic subgroups remains limited (6, 17). Ethnic variation may be a function of exposures occurring within the countries of origin, and/or of features of the receiving environment. Most contemporary U.S. immigrants come from Latin America and Asia (18); Mexican and Chinese-origin individuals constitute the largest segments of the Hispanic and Asian populations in the U.S., respectively (18, 19). Pan-ethnic categorizations of Hispanics and Asians mask considerable heterogeneity in culture, immigration history, and health profiles. Relative to other Hispanic subgroups, for example, individuals of Mexican-origin have been disproportionately impacted by obesity (20, 21). Whether the weight of Mexican-origin Hispanics is differentially influenced by greater exposure to the U.S. context relative to other Hispanics is unknown. Examination of these differences is important to better understand U.S. immigrant health patterns.
Using longitudinal data from the Multi-ethnic Study of Atherosclerosis (MESA), we examined whether Hispanic and Chinese foreign-born participants experienced greater increases in body mass index (BMI) and waist circumference (WC) over a median follow-up of 5 years relative to their U.S.-born counterparts. We also explored heterogeneity in this association by Hispanic subgroup.
METHODS AND PROCEDURES
MESA is a prospective cohort study designed to investigate risk factors for subclinical cardiovascular diseases (CVD). MESA design details are provided elsewhere (22). Briefly, participants aged 45–84 years, free of clinical CVD at baseline were recruited from six sites (Baltimore, MD; Chicago, IL; Forsyth County, NC; Los Angeles County, CA; Manhattan, NY; St. Paul, MN). The cohort includes 6814 self-identified white, African-American, Hispanic, and Chinese-American individuals. The baseline examination took place between 2000 and 2002. Participants attended three follow-up examinations 18–24 months apart. Analyses were restricted to Hispanic and Chinese participants due to small numbers of foreign-born individuals in other race/ethnic groups.
Height (m) and weight (kg) (to calculate body mass index (BMI) (kg/m2)) and waist circumference (WC) (cm) were measured at all study visits using standardized procedures. For descriptive purposes, BMI was also dichotomized based on obesity status (BMI ≥ 30 kg/m2); WC was dichotomized based on the World Health Organization’s criteria for abdominal obesity (23). Although there is no clear consensus on the best anthropometric measure to use among older individuals, several studies show WC to be a better predictor of cardiovascular risk and mortality than BMI (24, 25). Because of age-related changes in body composition, BMI comparisons across groups in older populations may be more likely to reflect variation in lean body mass than in fat mass, reducing the validity of BMI as a marker of adiposity (25). For these reasons, although we present results for both BMI and WC, we focus primarily on WC.
Nativity (U.S.-born, foreign-born), length of U.S. residence (<15 years, 15–30 years, >30 years, missing), age (continuous, mean-centered at 63 years), sex, race/ethnicity (Hispanic, Chinese), Mexican-origin ethnicity among Hispanics (yes/no), education (< high school, high school graduate, some college, college graduate), and family income within the past 12 months (13 categories: <$5,000 to $100,000+) were obtained during the baseline interview. Baseline income was available for 97.6% of Hispanics and 99.3% of Chinese. When missing, income data from follow-up exams were used. A continuous measure of household-equivalized income was created by taking the midpoint for each income category and dividing it by the number of household members. The variable was expressed as quartiles of the sample distribution. Time since baseline (years) was used to examine change in BMI and WC over time.
We also tested whether lifestyle behaviors mediated associations between BMI and WC with nativity and length of U.S. residence. Current cigarette smoking status (yes/no/former) and current alcohol consumption (yes/no) were ascertained at all visits. Physical activity, available at the first 3 exams, was measured as metabolic equivalent task-minutes per week for walking and moderate- and vigorous-intensity sports and conditioning activities, estimated from a physical activity questionnaire adapted from the Cross-Cultural Activity Participation Study (26). Diet was measured at baseline using an adapted 120-item food frequency questionnaire, validated for multi-ethnic populations (27). We operationalized diet in two ways: total caloric intake (kilocalories) and a dietary pattern score that characterizes intake of fats and processed foods. The latter was identified through a factor analysis of diet patterns among 47 food groups (28). Higher scores indicate higher intake of fats and processed foods.
Of the 2299 Hispanic and Chinese participants, 11 did not have information on key covariates, yielding a sample of 1486 Hispanics (794 Mexican, 692 non-Mexican) and 802 Chinese. Of the non-Mexican Hispanics, 29% were Puerto Rican, 25% were Dominican, 8% were Cuban, and the remaining were from several Central and South American countries. Mediation analyses using diet were restricted to 1350 Hispanics and 790 Chinese because of missing diet data. Of the 2288 baseline sample, 77% had information for all four visits, 13% had information for two or three visits, and 7% had only baseline information. Analyses included all 2288 baseline participants regardless of missing follow-up information. All MESA participants provided written informed consent.
Statistical Analysis
Results were race/ethnicity-stratified (Hispanics and Chinese). We used graphical methods to explore relationships of BMI and WC with age and time since baseline in order to evaluate departures from linearity. BMI had a curvi-linear relationship with age; thus, we included a quadratic age term in all BMI models. We estimated cross-sectional and longitudinal associations between nativity and BMI and WC, separately, using a repeated measures analysis with the unstructured covariance specification to account for within-person correlations (29) (PROC MIXED SAS 9.2; SAS Institute Inc., Cary, NC). Models were adjusted for baseline age, sex, site, education, income, and time since baseline. Baseline age-by-time interactions were retained to account for the significantly greater BMI and WC increases among participants younger at baseline. We also included time interactions with education and income to adjust for differential trends by socioeconomic status (SES). To evaluate if BMI and WC change varied by nativity, we tested nativity-by-time interactions.
We also examined whether differences in physical activity, smoking, alcohol, and diet potentially mediated the relationship between nativity and BMI or WC by including these measures as time-varying covariates when available. Since diet was only ascertained at baseline, we modeled its interaction with time in lieu of a time-varying covariate. To examine heterogeneity in the associations of nativity with BMI and WC by Hispanic subgroup, we included a covariate for Mexican-origin status in Hispanic models. Mexican-origin status was interacted with nativity and with time. We also included a three-way interaction between Mexican-origin, nativity, and time to determine whether Mexican origin modified the impact of nativity on time trends. We computed estimates of adjusted mean annual change in BMI and WC by nativity and by Mexican-origin using model coefficients.
To examine whether change in BMI or WC differed by time lived in the U.S. at baseline, we also fit models that replaced the nativity indicator with a 5-level variable that combined birthplace and baseline length of U.S. residence among the foreign-born (FB) (FB: <15 years; FB: 15–30 years; FB: >30 years; FB: missing years in U.S.; and U.S.-born (referent)). We tested an interaction between this 5-level variable and time in ethnicity-stratified models.
Because 23% of our sample did not have complete information on all study visits, we re-ran all models on individuals with complete data for all four visits. Change-over-time estimates from our complete-case analysis were robust regardless of follow-up length, suggesting that BMI and WC trajectories among individuals lost to follow-up did not differ from those remaining in the study.
RESULTS
Foreign-born (FB) Hispanic and Chinese participants had lower baseline BMI and WC than their U.S.-born (USB) counterparts (mean WC for FB and USB: 99 vs. 103 cm, P <0.0001 for Hispanics; and 87 vs. 92 cm, P=0.09 for Chinese). The proportion of individuals who were obese or abdominally obese was also lower in the foreign-born (Table 1). The foreign-born also had greater 5-year mean increase in BMI and WC though differences were not statistically significant (5-year increase in WC in FB vs. USB: 1.75 vs. 1.08 cm, P=0.09 in Hispanics; 1.21 vs. 0.26 cm, P=0.40 in Chinese). Foreign-born participants were disproportionately represented in the lowest socioeconomic categories, and had lower physical activity levels, but more favorable profiles for diet, smoking, and alcohol consumption compared to the U.S.-born. Nativity differences among Hispanics were similar regardless of ethnicity with some exceptions. First, the nativity difference in baseline BMI and WC was smaller among Mexican Hispanics. Second, the proportion of women with abdominal obesity was higher among foreign-born Mexicans compared with the U.S.-born; this pattern was reversed among non-Mexican Hispanics. Finally, SES disparities by nativity were considerably wider for Mexican than for non-Mexican Hispanics.
Table 1.
Sample Characteristics by Nativity and Ethnicity, the Multi-Ethnic Study of Atherosclerosis
| All Hispanics | Mexican Hispanics | Non-Mexican Hispanics | Chinese | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Birth Country | Birth Country | Birth Country | Birth Country | ||||||
| U.S. | Other | U.S. | Other | U.S. | Other | U.S. | Other | ||
| (n=465) | (n=1021) | (n=403) | (n=391) | (n=62) | (n=630) | (n=30) | (n=772) | ||
| Mean body mass index (kg/m2) (SD) [n] | |||||||||
| Baseline | 30.5 (5.7) [465] | 28.9 (4.7)a [1021] | 30.4 (5.6) [403] | 29.4 (4.8)a [391] | 31.0 (6.3) [62] | 28.6 (4.7)a [630] | 25.7 (5.0) [30] | 23.9 (3.2) [772] | |
| First follow-up | 30.6 (5.9) [434] | 29.1 (4.9)a [914] | 30.4 (5.8) [376] | 29.7 (4.9) [337] | 31.3 (6.7) [58] | 28.7 (4.9)a [577] | 25.8 (5.0) [30] | 24.0 (3.2)a [697] | |
| Second follow-up | 30.6 (5.9) [415] | 29.1 (4.9)a [839] | 30.5 (5.8) [359] | 29.9 (4.9) [298] | 31.3 (6.3) [56] | 28.7 (4.9)a [541] | 25.8 (4.9) [29] | 23.9 (3.3)a [667] | |
| Third follow-up | 30.6 (6.0) [408] | 29.2 (5.1)a [812] | 30.5 (5.9) [353] | 30.2 (5.2) [288] | 31.5 (6.7) [55] | 28.7 (4.9)a [524] | 25.6 (4.6) [28] | 24.0 (3.4) [630] | |
| Mean 5-year change in body mass index (SD) | −0.012 (2.3) | 0.16 (2.1) | 0.002 (2.1) | 0.38 (2.1)a | −0.11 (2.9) | 0.03 (2.0) | 0.006 (1.5) | 0.02 (1.4) | |
| Obeseb, baseline (%) | 46.9 | 34.9a | 46.7 | 39.9 | 48.4 | 31.8a | 16.7 | 4.0a | |
| Mean waist circumference (cm) (SD) [n] | |||||||||
| Baseline | 103.2 (14.5) [465] | 99.4 (12.2)a [1021] | 102.8 (14.4) [403] | 100.9 (11.5)a [391] | 105.6 (15.1) [62] | 98.5 (12.6)a [630] | 91.8 (15.4) [30] | 86.9 (9.6) [772] | |
| First follow-up | 103.1 (15.2) [434] | 99.7 (12.4)a [914] | 102.7 (15.1) [376] | 101.3 (11.6) [337] | 105.4 (15.7) [58] | 98.7 (12.8)a [577] | 91.5 (15.6) [30] | 86.7 (9.5) [697] | |
| Second follow-up | 104.1 (14.9) [415] | 100.2 (12.5)a [839] | 103.6 (14.8) [359] | 102.9 (11.8) [298] | 107.7 (15.1) [56] | 98.7 (12.6)a [541] | 91.2 (16.0) [29] | 87.1 (9.6) [667] | |
| Third follow-up | 104.4 (15.1) [408] | 101.1 (12.9)a [812] | 104.0 (14.9) [353] | 103.8 (12.2) [288] | 107.5 (16.1) [55] | 99.7 (13.1)a [524] | 91.5 (13.9) [28] | 88.1 (9.6) [630] | |
| Mean 5-year change in waist circumference (SD) | 1.08 (6.7) | 1.75 (6.4) | 1.23 (6.5) | 2.23 (6.4)a | 0.1 (7.5) | 1.48 (6.5) | 0.26 (0.57) | 1.21 (5.2) | |
| Abdominal obesity, baseline (%) | |||||||||
| Men: ≥ 102 cmc | 48.4 | 37a | 48.8 | 37.4a | 45.2 | 36.7 | 17.6 | 7 | |
| Women: ≥ 88 cmc | 82.2 | 80.3 | 80.8 | 88.7a | 90.3 | 75.3a | 53.8 | 40.8 | |
| Study site (%) | |||||||||
| Forsyth County, NC | 0.4 | 0.1a | 0 | 0 | 3.2 | 0.16a | 0 | 0 | |
| New York, NY | 8.4 | 44.8 | 0.5 | 0.51a | 59.7 | 72.2 | 0 | 0.26a | |
| Minneapolis, MN | 52.7 | 20.7 | 58.6 | 36.1 | 14.5 | 11.1 | 0 | 0 | |
| Chicago, IL | 0 | 0 | 0 | 0 | 0 | 0 | 66.7 | 36.7 | |
| Los Angeles, CA | 38.5 | 34.5 | 40.9 | 63.4 | 22.6 | 16.5 | 33.3 | 63.1 | |
| Mean age, baseline (SD) | 61.6 (10.5) | 61.1 (10.2) | 62.0 (10.3) | 60.8 (10.2) | 58.8 (11.3) | 61.2 (10.3) | 61.1 (10.0) | 62.4 (10.3) | |
| Female (%) | 47.1 | 53.7a | 46.6 | 52.2 | 50 | 54.6 | 43.3 | 51.8 | |
| Mexican origin (%) | 86.7 | 38.3a | |||||||
| Years lived in U.S., baseline (among foreign-born) (%) | |||||||||
| < 15 years | 15.6 | 21 | 12.2 | 36.3 | |||||
| 15–30 years | 24.6 | 25.3 | 24.1 | 38.3 | |||||
| > 30 years | 48.4 | 41.9 | 52.4 | 18.6 | |||||
| Missing | 11.5 | 11.8 | 11.3 | 6.7 | |||||
| Education (%) | |||||||||
| Less than high school | 20 | 55.7a | 21.3 | 73.7a | 11.3 | 44.6 | 3.3 | 25.6a | |
| Completed high school/GED | 28.2 | 16.8 | 28.3 | 10.5 | 27.4 | 20.8a | 20 | 16.1 | |
| Some college/technical school | 39.3 | 18.6 | 38.2 | 13.5 | 46.8 | 21.7 | 13.3 | 20.3 | |
| Bachelor’s/graduate degree | 12.5 | 8.8 | 12.2 | 2.3 | 14.5 | 12.9 | 63.3 | 38 | |
| Income quartiles, U.S.$ d (%) | |||||||||
| 0 | 12 | 35.3a | 12.2 | 47.8a | 11.3 | 27.5a | 3.3 | 29.8a | |
| 1 | 13.3 | 23.5 | 13.1 | 25.3 | 14.5 | 22.4 | 3.3 | 23.5 | |
| 2 | 34 | 24.4 | 34.7 | 18.2 | 29 | 28.2 | 26.7 | 20.3 | |
| 3 | 40.6 | 16.8 | 40 | 8.7 | 45.2 | 21.9 | 66.7 | 26.4 | |
| Diet of high fats, processed foods, mean score (SD)e | 0.05 (0.94) | −0.48 (0.80)a | 0.0144 (0.93) | −0.57 (0.72)a | 0.31 (1.02) | −0.42 (0.84)a | −0.06 (0.79) | −0.69 (0.46)a | |
| Mean caloric intake, kilocalories (SD)e | 1812 (1014) | 1779 (890) | 1790 (1023) | 2027 (883)a | 1973 (947) | 1608 (855)a | 1710 (762) | 1320 (572)a | |
| Total intentional exercise, baseline (MET-min/week) (%) | |||||||||
| 0 | 23.4 | 34.5a | 23.8 | 41.9a | 21 | 29.9 | 10 | 25.9a | |
| < 2400 | 49 | 51.9 | 48.4 | 51.4 | 53.2 | 52.1 | 60 | 60.9 | |
| ≥ 2400 | 27.5 | 13.6 | 27.8 | 6.7 | 25.8 | 18 | 30 | 13.2 | |
| Smoking status, baseline (%) | |||||||||
| Never | 46.4 | 57.4a | 47.2 | 57a | 41.9 | 57.6a | 43.3 | 76.5a | |
| Former | 38.9 | 29.6 | 38.7 | 32.2 | 40.3 | 27.9 | 50 | 17.9 | |
| Current | 14.6 | 13 | 14.1 | 10.8 | 17.7 | 14.4 | 6.7 | 5.6 | |
| Current alcohol drinker, baseline (%) | |||||||||
| Yes | 55.3 | 43.6a | 54.8 | 39.6a | 58.1 | 46.1 | 56.7 | 30.3a | |
| No | 44.7 | 56.4 | 45.2 | 60.4 | 41.9 | 53.9 | 43.3 | 69.7 | |
Abbreviations: SD, standard deviation; MET, metabolic equivalent task
p < 0.05, comparing foreign-born to U.S.-born within ethnic groups
Body mass index ≥ 30 kg/m2
Based on the World Health Organization’s sex-specific cutoffs for waist circumference measurements at high risk for metabolic syndrome
Continuous measure of income adjusted for household size, expressed as quartiles
Based on restricted sample of 1350 Hispanics (424 U.S.-born (USB), 926 foreign-born (FB)); 749 Mexican (372 USB, 377 FB); 601 non-Mexican Hispanics (52 USB, 549 FB); and 790 Chinese (28 USB, 762 FB)
Multivariable analyses
Table 2 shows adjusted mean differences in baseline BMI and WC and in annual changes in BMI and WC by nativity for Hispanics and Chinese. Adjusting for age, sex, site, education, income, and time (Model 1), the foreign-born had a significantly lower mean baseline BMI and WC than the U.S.-born (Hispanics (BMI): mean difference= −1.55 kg/m2P<0.0001; (WC): −3.66 cm, P<0.0001; Chinese (BMI): −1.68 kg/m2P<0.01; (WC): −5.13 (cm), P<0.01). Mean annual changes in BMI were not statistically significant and there were no differences by nativity status in change over time. All groups except U.S.-born Chinese experienced statistically significant annual increases in WC, but there were no significant differences by nativity status for either ethnic group. Inclusion of time-varying measures of physical activity, smoking, and alcohol (Model 2) slightly increased nativity differences at baseline. Further, addition of baseline dietary measures (Model 3) partially reduced nativity differences in baseline BMI and WC for Hispanics and in baseline WC for Chinese.
Table 2.
Adjusted Mean Difference at Baseline and Mean Annual Change in Body Mass Index (BMI) (kg/m2) and Waist Circumference (WC) (cm) by Nativity, Hispanics and Chinese
| Model 1 | Model 2 | Model 3 | |||||
|---|---|---|---|---|---|---|---|
| HISPANICS (n=1486) | |||||||
| BMI | WC | BMI | WC | BMI | WC | ||
| Mean difference in baseline BMI and WC | |||||||
| U.S. born | ref | ref | ref | ref | ref | ref | |
| Foreign-born | −1.55 (0.34)a | −3.66 (0.87)a | −1.58 (0.34)a | −3.76 (0.87)a | −1.44 (0.36)a | −3.42 (0.93)b | |
| Mean annual change in BMI and WC by nativitye | |||||||
| U.S. born | 0.03 (0.03) | 0.28 (0.11)c | 0.03 (0.04) | 0.25 (0.11)d | 0.04 (0.04) | 0.28 (0.11)d | |
| Foreign-born | 0.04 (0.02) | 0.39 (0.07)a | 0.04 (0.02) | 0.39 (0.08)a | 0.05 (0.03) | 0.38 (0.08)a | |
| Mean difference in annual change in BMI and WC | |||||||
| U.S. born | ref | ref | ref | ref | ref | ref | |
| Foreign-born | 0.01 (0.03) | 0.11 (0.08) | 0.01 (0.03) | 0.14 (0.08) | 0.01 (0.03) | 0.11 (0.09) | |
| CHINESE (n=802) | |||||||
| Mean difference in baseline BMI and WC | |||||||
| U.S. born | ref | ref | ref | ref | ref | ref | |
| Foreign-born | −1.68 (0.62)c | −5.13 (1.83)c | −1.70 (0.62)c | −5.23 (1.84)c | −1.72 (0.66)c | −4.78 (1.95)d | |
| Mean annual change in BMI and WC by nativitye | |||||||
| U.S. born | 0.07 (0.06) | 0.24 (0.23) | 0.07 (0.06) | 0.24 (0.23) | 0.05 (0.06) | 0.16 (0.24) | |
| Foreign-born | 0.04 (0.03) | 0.37 (0.10)b | 0.04 (0.03) | 0.36 (0.10)b | 0.03 (0.03) | 0.33 (0.11)c | |
| Mean difference in annual change in BMI and WC | |||||||
| U.S. born | ref | ref | ref | ref | ref | ref | |
| Foreign-born | −0.03 (0.06) | 0.13 (0.21) | −0.03 (0.06) | 0.12 (0.21) | −0.02 (0.06) | 0.17 (0.22) | |
p < 0.0001,
p < 0.001,
p < 0.01,
p < 0.05
Model 1 adjusted for age, sex, site, baseline education and income, time since baseline, and interactions for age*time, education*time, and income*time. BMI model includes age2 term.
Model 2 adds controls for time-varying health behaviors: physical activity, current smoking status, current alcohol use
Model 3 adds baseline dietary measures (diet of high fats, processed foods; total caloric intake); restricted to 1350 Hispanics and 790 Chinese on whom dietary data was available. Sensitivity analyses confirmed that results from previous models excluding missing dietary data did not appreciably affect results.
Estimates shown were calculated to correspond to the mean age of the entire sample (age=63) and to those with less than high school education and in the lowest income quartile.
Tests for interactions revealed significant heterogeneity by Mexican-origin among Hispanics (Likelihood ratio test: BMI model: P=0.0087; WC model: P=0.0020). The patterns were generally similar in both BMI and WC models, but associations were more pronounced in WC models, so only those results are shown (Table 3) (see Supplementary Table S1 for results for BMI models). Mexican Hispanics had significantly smaller nativity differences in baseline WC (mean difference =-2.19, P<0.05) compared with non-Mexican Hispanics (mean difference=-7.88, P<0.0001) (Model 1). Although all 4 Mexican-origin/nativity combinations experienced increases in WC over time, the Mexican foreign-born had greater increases over time compared to both the Mexican U.S.-born (difference in mean annual change=0.28, P<0.05), and the non-Mexican foreign-born (difference in mean annual change=0.24, P<0.01) (Model 1). In contrast, we found no significant difference by nativity in mean change over time among non-Mexican Hispanics. There were also no differences in mean change over time between Mexican and non-Mexican U.S.-born individuals. Inclusion of health behaviors did not meaningfully alter estimates (Model 2). Results were robust to adjustment for length of U.S. residence among the foreign-born.
Table 3.
Adjusted Mean Waist Circumference (WC) (cm) at Baseline and Mean Annual Change in WC by Nativity and Mexican Ethnicity
| Model 1 | Model 2e | |||||
|---|---|---|---|---|---|---|
| Adjusted mean baseline WC (SE)f |
Mean difference in baseline WC by nativity (SE)g |
Adjusted mean baseline WC (SE)f |
Mean difference in baseline WC by nativity (SE)g |
|||
| U.S.-born | Foreign-born | U.S.-born | Foreign-born | |||
| MEXICAN HISPANICS (n=794) | 103.40 (1.18) | 101.21 (0.89) | −2.19 (1.04)d | 103.66 (1.21) | 101.32 (0.95) | −2.34 (1.10)d |
| NON-MEXICAN HISPANICS (n=692) | 107.34 (1.98) | 99.47 (1.15) | −7.88 (1.75)a | 107.67 (2.10) | 100.22 (1.17) | −7.45 (1.89)a |
| Mean difference in baseline WC by Mexican ethnicity for each nativity group (SE)h | −3.94 (1.89)d | 1.74 (1.14) | −4.01 (1.99)d | 1.10 (1.15) | ||
|
Adjusted mean annual change (SE)f |
Mean difference in annual change in WC by nativity (SE)g |
Adjusted mean annual change (SE)f |
Mean difference in annual change in WC by nativity (SE)g |
|||
| U.S.-born | Foreign-born | U.S.-born | Foreign-born | |||
| MEXICAN HISPANICS | 0.23 (0.11)d | 0.51 (0.09)a | 0.28 (0.11)d | 0.23 (0.12)d | 0.52 (0.10)a | 0.28 (0.12)d |
| NON-MEXICAN HISPANICS | 0.13 (0.19) | 0.26 (0.09)b | 0.13 (0.18) | 0.08 (0.21) | 0.26 (0.09)c | 0.17 (0.20) |
| Mean difference in annual change in WC by Mexican ethnicity for each nativity group (SE)h | 0.10 (0.18) | 0.24 (0.09)c | 0.15 (0.20) | 0.26 (0.10)c | ||
p < 0.0001,
p < 0.001,
p < 0.01,
p < 0.05
Model 1 adjusted for age, sex, site, baseline education and income, Mexican-origin status, time since baseline, and interactions for age*time, education*time, income*time, Mexican-origin*time, Mexican-origin*nativity, and Mexican-origin*nativity*time
Model 2 adds controls for time-varying health behaviors: physical activity, current smoking status, current alcohol use; and baseline dietary measures (diet of high fats, processed foods; total caloric intake)
Model 2 restricted to 749 Mexicans and 601 non-Mexican Hispanics on whom dietary data was available. Sensitivity analyses confirmed that results from previous model excluding missing dietary data did not appreciably affect results
Adjusted mean estimates shown are calculated to correspond to the mean age of the entire sample (age=63) and to those with less than high school education and in the lowest income quartile.
Compares foreign-born to U.S.-born referent for each Mexican-origin group
Compares Mexican to Non-Mexican referent for each nativity group
Likelihood ratio test comparing nested models with and without interaction terms for Mexican ethnicity: p = 0.0082
Figures 1A–C present 5-year trends in adjusted mean WC by baseline length of U.S. residence. Since BMI changed little over time, we only graphed the findings from WC models. Among Mexican Hispanics, only the most recent immigrants (<15 years) had a significantly lower baseline mean WC than the U.S.-born (Fig. 1A) (mean difference= −3.77 cm, P=0.0470). However rates of increase over time for this group were significantly greater than for the U.S.-born (mean difference in annual change=0.48 cm, P<0.0236); after 5 years, WC estimates for recent immigrants no longer statistically differed from the U.S.-born. Although the other Mexican immigrant groups did not differ from the U.S.-born in baseline WC, , they also had a significantly greater rate of increase than the U.S.-born. Results were robust to stratification by baseline age.
Figure 1.

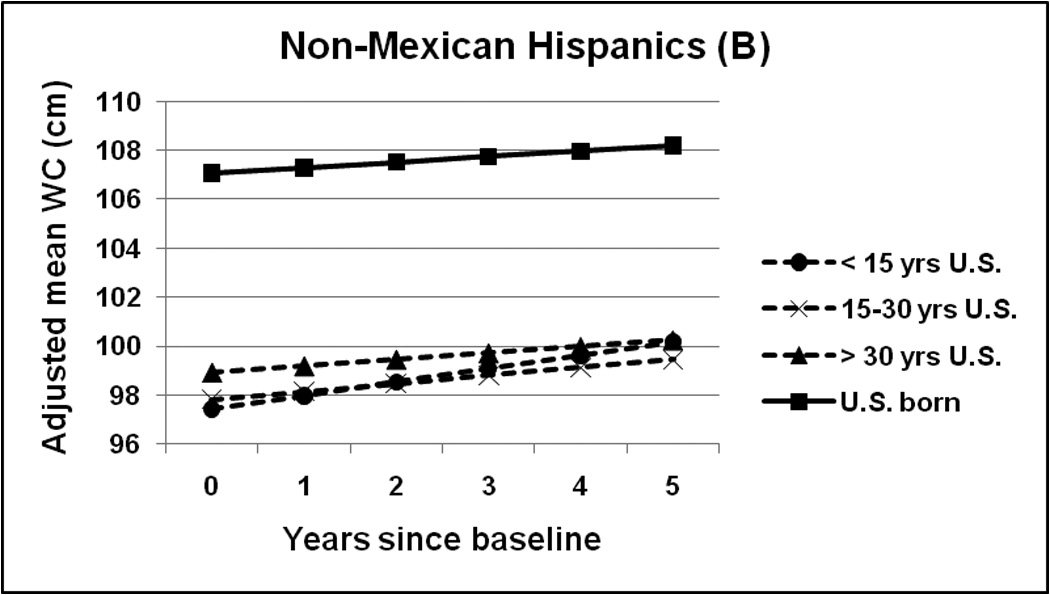

Adjusted mean waist circumference trajectories over time by baseline length of U.S. residence among the foreign-born and the U.S.-born. A) Mexican Hispanics, B) Non-Mexican Hispanics, C) Chinese. WC=waist circumference; Yrs=years. All models adjusted for age, sex, site, education, income, baseline length of U.S. residence, age*time, education*time, income*time, baseline length of U.S. residence*time, and health behaviors (physical activity, smoking, alcohol, and diet). Estimates shown were calculated to correspond to the mean age of the entire sample (age=63) and to those with less than high school education and in the lowest income quartile. Foreign-born with missing data on baseline length of U.S. residence included in all models but not plotted in figures.
Among non-Mexican Hispanics (Fig. 1B) and Chinese (Fig. 1C), the baseline WC of the foreign-born was significantly lower relative to the U.S.-born, regardless of length of residence, but there were no differences in WC change over time.
DISCUSSION
We examined differences in BMI and WC and in their change over time by nativity and ethnicity in a prospective multi-ethnic cohort. Foreign birth was associated with a lower adjusted mean baseline BMI and WC among both Hispanics and Chinese, but there were no significant time trend differences by nativity. However among Hispanics, there was significant heterogeneity by subgroup. Baseline nativity differences in WC for Mexican Hispanics were narrower than they were for non-Mexican Hispanics. Foreign-born Mexicans also experienced greater annual mean increases in WC than both U.S.-born Mexican and foreign-born non-Mexican Hispanics, regardless of how long they had lived in the U.S.
Consistent with our baseline results, prior cross-sectional work has documented lower weight in the foreign-born than the U.S.-born among Hispanics (3, 5, 6, 8, 16, 30, 31), Mexican-Americans (32–36), Asians (2, 4, 6, 30, 31, 36), and Chinese-Americans (36), though null findings among Asians have also been reported (5). Studies examining cross-sectional associations between length of residence and weight show evidence of higher BMI, WC, or obesity with longer U.S. residence in nationally-representative studies of Hispanics (2, 3, 8–10), as well as in region-specific studies (5, 6), and studies specific to Mexican and Puerto Rican subgroups (7, 32). Results among Asians (2, 4–6) and Chinese (36, 37) are mixed. To our knowledge, no longitudinal studies have directly examined the relation between time in the U.S. and changes in weight over time among adults.
A major limitation in drawing inferences regarding the causal effect of length of residence on weight from cross-sectional analyses is the inability to differentiate the influence of time in the U.S. from cohort and aging effects. Controlling for age and its interaction with time in a longitudinal design, we were able to directly examine whether the foreign-born experienced greater increases in BMI or WC with longer length of residence relative to the U.S.-born, net of age and birth cohort. Contrary to much of the cross-sectional literature that did not account for these influences, we did not find evidence of greater BMI and WC increases over time among foreign-born Hispanics and Chinese. However, our results were consistent with one cross-sectional study of Hispanics that did account for age and cohort influences. Park et al. utilized a series of repeated cross-sections to evaluate changes in the obesity prevalence of foreign and U.S.-born age-matched cohorts over a period of 10 years. They found no evidence that immigrant obesity converged to U.S.-born levels. (16). In another longitudinal analysis conducted in a sample of multi-ethnic adolescents (whites, blacks, Hispanics, and Asians), first generation immigrants experienced slower increases in BMI than second and third generation adolescents (38). Of relevance, these patterns remained consistent for Hispanics and Asians. Taken together, these two studies support our findings in older Hispanic and Chinese adults in which we find no evidence of faster increases in BMI or WC in the foreign-born compared to the U.S.-born after accounting for aging and cohort influences.
A strength of our analysis was the ability to examine whether patterns differed in Hispanic subgroups. Failure to distinguish by subgroup can mask heterogeneity among Hispanics. Although analyses pooling Hispanics showed no evidence that the foreign-born experienced a more rapid increase in BMI or WC than the U.S.-born, foreign-born Hispanics of Mexican origin experienced more rapid increases than U.S.-born Mexican-Americans. They also experienced more rapid increases than other foreign-born Hispanics. Reasons underlying the findings among foreign-born Mexicans remain unclear. Adoption of negative health behaviors has been hypothesized to account for the increased weight associated with longer length of U.S. residence (11), however inclusion of behavioral covariates in models did not fully account for our findings. Measurement error may have resulted in underestimates of their importance as mediators; missing dietary data and the availability of baseline-only measurements likely limited our ability to quantify the relevance of diet. Similarly, we used leisure-time activity to measure energy expenditure, which does not capture activity associated with occupation, or with activity not considered ‘leisure-time’ by respondents.
There are other factors that could explain why trajectories over time in anthropometric characteristics among the foreign born differed depending on their ethnic origin. These factors may include exposure to different cultural environments, variation in opportunity for socioeconomic advancement, and the influence of characteristics associated with a migrant’s country of origin (11). Health behaviors established in the sending country likely remain important influences after migration. Among immigrants from Mexico, a country where the obesity epidemic rivals that of the U.S. (39), poorer health behaviors established prior to migration may contribute to more adverse weight patterning among Mexican origin individuals compared to immigrants from other parts of Latin America where obesity has not yet reached epidemic levels.
The receiving environments may also differ across various groups of immigrants. Migration to and residence in environments marked by poverty, crime, and deficiency in physical and social resources may reinforce poorer health behaviors, and contribute to adverse changes in anthropometric indicators. (40). There is also some work to suggest that residence in immigrant enclaves may facilitate retention of traditional, healthier diets through greater availability of fruits and vegetables and other ethnic-specific food options (41, 42). Better access to health –promoting resources in the receiving environment may be one mechanism through which some immigrants may be buffered against the health declines commonly associated with longer time in the U.S. Although it is unclear if access to such resources was differentially distributed between foreign-born Mexicans and non-Mexican Hispanics, for example future exploration of the impact of contextual features could provide additional insight into the factors that facilitate, or buffer against, weight gain across immigrant groups.
Methodological explanations may also underlie findings among foreign-born Mexicans. Despite the robustness of our complete-case analysis, if loss to follow-up among the foreign-born was correlated with a lower propensity to gain weight, this would bias findings in the direction we observed. We also elected against adjustment for baseline BMI and WC in multivariable models. The extent to which baseline values should be controlled for in models estimating change over time is debatable, especially when the variables of interest are associated with the baseline measurements, and when there is error in the baseline measurement (43). However, since the most notable change-estimate differences were between groups with smaller differences in baseline measurements, we believe baseline differences are an unlikely explanation for our main findings.
Our study had some limitations. Sample size precluded investigation of heterogeneity among non-Mexican Hispanics. The small number of U.S.-born Chinese may have also hampered our ability to detect nativity differences. Future studies with larger samples of U.S.-born Chinese and Hispanic subgroups are warranted to confirm our findings. Sample size limitations also made it difficult for us to investigate whether the complex patterns we report differed across socioeconomic groups. Additional work is needed to further clarify the interplay of migration, ethnicity, and socioeconomic position in shaping health trajectories after migration. The older age of the cohort and relatively short follow-up may have also limited our ability to examine factors associated with changes over time. Trajectories of weight gain may be established much earlier in life, and factors proxied by the nativity variables we utilized may have limited impact at older ages. Finally, because MESA is a relatively older, healthy cohort sampled from selected sites, the generalizability of these findings to other U.S. immigrant groups may be limited.
To our knowledge, this is among the first studies to examine trajectories of BMI and WC among immigrants in a longitudinal multi-ethnic cohort of adults. We found ethnic heterogeneity in BMI and WC change over time with Mexican immigrants exhibiting greater increases relative to both U.S.-born Mexican Hispanics and foreign-born non-Mexican Hispanics. High WC has consequences for progression to CVD and metabolic abnormalities (25). Since Mexican Hispanics constitute the largest immigrant group and Hispanic subgroup in the U.S., if confirmed in larger national samples, the findings we report will have implications for the future disease burden and mortality in the U.S. The ethnic heterogeneity we observed suggests that the acculturation process and its associated health consequences may not be homogeneous for all immigrants. It is important to develop a better understanding of the multiplicity of factors that may buffer some groups against more adverse health outcomes while placing others at higher risk of health decline with more time in the U.S. Further insight into what may underlie these patterns would facilitate development of interventions to prevent the health deterioration that appears with longer U.S. residence in some immigrant groups. Moreover, understanding what factors may buffer some immigrant groups against deleterious health consequences of more time in the U.S. may help uncover targets for intervention that may benefit other immigrant groups in the future.
Supplementary Material
ACKNOWLEDGEMENTS
This work was supported by the National Heart, Lung, and Blood Institute grant R01 HL071759 (Diez Roux); the Research Supplement to Promote Diversity in Health-Related Research (PA-08-190) -supplement to grant R01 HL071759 05A1 (Diez Roux); and by the Michigan Center for Integrative Approaches to Health Disparities (P60 MD002249) funded by the National Institute on Minority Health and Health Disparities. The Multi-Ethnic Study of Atherosclerosis is supported by contracts N01-HC-95159 through N01-HC-95169 from the National Heart, Lung, and Blood Institute.
The authors thank the other investigators, staff, and participants of the MESA study for their valuable contributions. A full list of participating MESA investigators and institutions can be found at: http://www.mesa-nhlbi.org.
Footnotes
DISCLOSURE
The authors declared no conflict of interest.
REFERENCES
- 1.Martin P, Midgley E. Immigration: Shaping and Reshaping America. Washington, DC: Population Reference Bureau; 2003. [Google Scholar]
- 2.Goel MS, McCarthy EP, Phillips RS, Wee CC. Obesity among US immigrant subgroups by duration of residence. JAMA. 2004 Dec 15;292(23):2860–2867. doi: 10.1001/jama.292.23.2860. [DOI] [PubMed] [Google Scholar]
- 3.Akresh IR. Overweight and obesity among foreign-born and US-born Hispanics. Biodemography Soc Biol. 2008 Fall;54(2):183–199. doi: 10.1080/19485565.2008.9989141. [DOI] [PubMed] [Google Scholar]
- 4.Lauderdale DS, Rathouz PJ. Body mass index in a US national sample of Asian Americans: effects of nativity, years since immigration and socioeconomic status. Int J Obes Relat Metab Disord. 2000 Sep;24(9):1188–1194. doi: 10.1038/sj.ijo.0801365. [DOI] [PubMed] [Google Scholar]
- 5.Park Y, Neckerman KM, Quinn J, Weiss C, Rundle A. Place of birth, duration of residence, neighborhood immigrant composition and body mass index in New York City. Int J Behav Nutr Phys Act. 2008;5:19. doi: 10.1186/1479-5868-5-19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Sanchez-Vaznaugh EV, Kawachi I, Subramanian SV, Sanchez BN, Acevedo-Garcia D. Differential effect of birthplace and length of residence on body mass index (BMI) by education, gender and race/ethnicity. Soc Sci Med. 2008 Oct;67(8):1300–1310. doi: 10.1016/j.socscimed.2008.06.015. [DOI] [PubMed] [Google Scholar]
- 7.Himmelgreen DA, Perez-Escamilla R, Martinez D, Bretnall A, Eells B, Peng Y, Bermudez A. The longer you stay, the bigger you get: length of time and language use in the US are associated with obesity in Puerto Rican women. Am J Phys Anthropol. 2004 Sep;125(1):90–96. doi: 10.1002/ajpa.10367. [DOI] [PubMed] [Google Scholar]
- 8.Antecol H, Bedard K. Unhealthy assimilation: why do immigrants converge to American health status levels? Demography. 2006 May;43(2):337–360. doi: 10.1353/dem.2006.0011. [DOI] [PubMed] [Google Scholar]
- 9.Kaplan MS, Huguet N, Newsom JT, McFarland BH. The association between length of residence and obesity among Hispanic immigrants. Am J Prev Med. 2004 Nov;27(4):323–326. doi: 10.1016/j.amepre.2004.07.005. [DOI] [PubMed] [Google Scholar]
- 10.Oza-Frank R, Cunningham SA. The weight of US residence among immigrants: a systematic review. Obes Rev. 2009 Jun 15; doi: 10.1111/j.1467-789X.2009.00610.x. [DOI] [PubMed] [Google Scholar]
- 11.Lara M, Gamboa C, Kahramanian MI, Morales LS, Bautista DE. Acculturation and Latino health in the United States: a review of the literature and its sociopolitical context. Annu Rev Public Health. 2005;26:367–397. doi: 10.1146/annurev.publhealth.26.021304.144615. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Popkin BM. Global nutrition dynamics: the world is shifting rapidly toward a diet linked with noncommunicable diseases. Am J Clin Nutr. 2006 Aug;84(2):289–298. doi: 10.1093/ajcn/84.1.289. [DOI] [PubMed] [Google Scholar]
- 13.Portes A. Immigration theory for a new century: some problems and opportunities. Int Migr Rev. 1997 Winter;31(4):799–825. [PubMed] [Google Scholar]
- 14.Reynolds SL, Himes CL. Cohort differences in adult obesity in the United States, 1982–2002. J Aging Health. 2007 Oct;19(5):831–850. doi: 10.1177/0898264307305182. [DOI] [PubMed] [Google Scholar]
- 15.Wang YC, Colditz GA, Kuntz KM. Forecasting the obesity epidemic in the aging US population. Obesity (Silver Spring) 2007 Nov;15(11):2855–2865. doi: 10.1038/oby.2007.339. [DOI] [PubMed] [Google Scholar]
- 16.Park J, Myers D, Kao D, Min S. Immigrant obesity and unhealthy assimilation: alternative estimates of convergence or divergence, 1995–2005. Soc Sci Med. 2009 Dec;69(11):1625–1633. doi: 10.1016/j.socscimed.2009.09.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Bates LM, Acevedo-Garcia D, Alegria M, Krieger N. Immigration and generational trends in body mass index and obesity in the United States: results of the National Latino and Asian American Survey, 2002–2003. Am J Public Health. 2008 Jan;98(1):70–77. doi: 10.2105/AJPH.2006.102814. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Martin P, Midgley E. Immigration: Shaping and Reshaping America. Washington, DC: Population Reference Bureau; 2006. [Google Scholar]
- 19.Dockterman D, Velasco G. Statistical Portrait of Hispanics in the United States, 2008. Washington, DC: Pew Hispanic Center; 2010. [Google Scholar]
- 20.Nichaman MZ, Garcia G. Obesity in Hispanic Americans. Diabetes Care. 1991 Jul;14(7):691–694. doi: 10.2337/diacare.14.7.691. [DOI] [PubMed] [Google Scholar]
- 21.Rivera JA, Barquera S, Gonzalez-Cossio T, Olaiz G, Sepulveda J. Nutrition transition in Mexico and in other Latin American countries. Nutr Rev. 2004 Jul;62(7 Pt 2):S149–S157. doi: 10.1111/j.1753-4887.2004.tb00086.x. [DOI] [PubMed] [Google Scholar]
- 22.Bild DE, Bluemke DA, Burke GL, Detrano R, Diez Roux AV, Folsom AR, Greenland P, Jacob DR, Jr, Kronmal R, Liu K, Nelson JC, O'Leary D, Saad MF, Shea S, Szklo M, Tracy RP. Multi-ethnic study of atherosclerosis: objectives and design. Am J Epidemiol. 2002 Nov 1;156(9):871–881. doi: 10.1093/aje/kwf113. [DOI] [PubMed] [Google Scholar]
- 23.Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med. 1998 Jul;15(7):539–553. doi: 10.1002/(SICI)1096-9136(199807)15:7<539::AID-DIA668>3.0.CO;2-S. [DOI] [PubMed] [Google Scholar]
- 24.Seidell JC, Visscher TL. Body weight and weight change and their health implications for the elderly. Eur J Clin Nutr. 2000 Jun;54(Suppl 3):S33–S39. doi: 10.1038/sj.ejcn.1601023. [DOI] [PubMed] [Google Scholar]
- 25.Hu FB. Obesity Epidemiology. New York: Oxford University Press; 2008. [Google Scholar]
- 26.LaMonte MJ, Durstine JL, Addy CL, Irwin ML, Ainsworth BE. Physical activity, physical fitness, and Framingham 10-year risk score: the cross-cultural activity participation study. J Cardiopulm Rehabil. 2001 Mar-Apr;21(2):63–70. doi: 10.1097/00008483-200103000-00001. [DOI] [PubMed] [Google Scholar]
- 27.Mayer-Davis EJ, Vitolins MZ, Carmichael SL, Hemphill S, Tsaroucha G, Rushing J, Levin S. Validity and reproducibility of a food frequency interview in a Multi-Cultural Epidemiology Study. Ann Epidemiol. 1999 Jul;9(5):314–324. doi: 10.1016/s1047-2797(98)00070-2. [DOI] [PubMed] [Google Scholar]
- 28.Nettleton JA, Steffen LM, Mayer-Davis EJ, Jenny NS, Jiang R, Herrington DM, Jacobs DR., Jr Dietary patterns are associated with biochemical markers of inflammation and endothelial activation in the Multi-Ethnic Study of Atherosclerosis (MESA) Am J Clin Nutr. 2006 Jun;83(6):1369–1379. doi: 10.1093/ajcn/83.6.1369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Littell RC, Milliken GA, Stroup GA, Wolfinger RD. SAS System for Mixed Models. Cary, NC: SAS Institute Inc; 1996. [Google Scholar]
- 30.Kaushal N. Adversities of acculturation? Prevalence of obesity among immigrants. Health Econ. 2009 Mar;18(3):291–303. doi: 10.1002/hec.1368. [DOI] [PubMed] [Google Scholar]
- 31.Dey AN, Lucas JW. Physical and mental health characteristics of US-and foreign-born adults: United States, 1998–2003. Adv Data. 2006 Mar 1;(369):1–19. [PubMed] [Google Scholar]
- 32.Barcenas CH, Wilkinson AV, Strom SS, Cao Y, Saunders KC, Mahabir S, Hernandez-Valero MA, Forman MR, Spitz MR, Bondy ML. Birthplace, years of residence in the United States, and obesity among Mexican-American adults. Obesity (Silver Spring) 2007 Apr;15(4):1043–1052. doi: 10.1038/oby.2007.537. [DOI] [PubMed] [Google Scholar]
- 33.Sundquist J, Winkleby M. Country of birth, acculturation status and abdominal obesity in a national sample of Mexican-American women and men. Int J Epidemiol. 2000 Jun;29(3):470–477. [PubMed] [Google Scholar]
- 34.Karlamangla AS, Merkin SS, Crimmins EM, Seeman TE. Socioeconomic and ethnic disparities in cardiovascular risk in the United States, 2001–2006. Ann Epidemiol. Aug;20(8):617–628. doi: 10.1016/j.annepidem.2010.05.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Khan LK, Sobal J, Martorell R. Acculturation, socioeconomic status, and obesity in Mexican Americans, Cuban Americans, and Puerto Ricans. Int J Obes Relat Metab Disord. 1997 Feb;21(2):91–96. doi: 10.1038/sj.ijo.0800367. [DOI] [PubMed] [Google Scholar]
- 36.Singh GK, Siahpush M, Hiatt RA, Timsina LR. Dramatic Increases in Obesity and Overweight Prevalence and Body Mass Index Among Ethnic-Immigrant and Social Class Groups in the United States, 1976–2008. J Community Health. Jun;12 doi: 10.1007/s10900-010-9287-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Yeh MC, Fahs M, Shelley D, Yerneni R, Parikh NS, Burton D. Body Weight and Length of Residence in the US Among Chinese Americans. J Immigr Minor Health. 2007 Dec 18; doi: 10.1007/s10903-007-9113-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Harris KM, Perreira KM, Lee D. Obesity in the transition to adulthood: predictions across race/ethnicity, immigrant generation, and sex. Arch Pediatr Adolesc Med. 2009 Nov;163(11):1022–1028. doi: 10.1001/archpediatrics.2009.182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Sassi F. Obesity and the Economics of Prevention: Fit Not Fat. Paris: Organization for Economic Co-operation and Development (OECD) 2010 [Google Scholar]
- 40.Papas MA, Alberg AJ, Ewing R, Helzlsouer KJ, Gary TL, Klassen AC. The built environment and obesity. Epidemiol Rev. 2007;29:129–143. doi: 10.1093/epirev/mxm009. [DOI] [PubMed] [Google Scholar]
- 41.Osypuk TL, Roux AV, Hadley C, Kandula NR. Are immigrant enclaves healthy places to live? The Multi-ethnic Study of Atherosclerosis. Soc Sci Med. 2009;69:110–120. doi: 10.1016/j.socscimed.2009.04.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Park Y, Neckerman K, Quinn J, Weiss C, Jacobson J, Rundle A. Neighbourhood immigrant acculturation and diet among Hispanic female residents of New York City. Public Health Nutr. :1–8. doi: 10.1017/S136898001100019X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Glymour MM, Weuve J, Berkman LF, Kawachi I, Robins JM. When is baseline adjustment useful in analyses of change? An example with education and cognitive change. Am J Epidemiol. 2005 Aug 1;162(3):267–278. doi: 10.1093/aje/kwi187. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.


