Abstract
High density lipoproteins (HDLs) have a number of properties that have the potential to inhibit the development of atherosclerosis and thus reduce the risk of having a cardiovascular event. These protective effects of HDLs may be reduced in patients with type 2 diabetes, a condition in which the concentration of HDL cholesterol is frequently low. In addition to their potential cardioprotective properties, HDLs also increase the uptake of glucose by skeletal muscle and stimulate the synthesis and secretion of insulin from pancreatic β cells and may thus have a beneficial effect on glycemic control. This raises the possibility that a low HDL concentration in type 2 diabetes may contribute to a worsening of diabetic control. Thus, there is a double case for targeting HDLs in patients with type 2 diabetes: to reduce cardiovascular risk and also to improve glycemic control. Approaches to raising HDL levels include lifestyle factors such as weight reduction, increased physical activity and stopping smoking. There is an ongoing search for HDL-raising drugs as agents to use in patients with type 2 diabetes in whom the HDL level remains low despite lifestyle interventions.
Keywords: Lipoproteins, HDL; Diabetes; Atherosclerosis
INTRODUCTION
Patients with type 2 diabetes frequently have a dyslipidemia that includes a low concentration of high density lipoprotein cholesterol (HDL-C) [1]. There is also evidence that the functionality of HDL particles is impaired in people with diabetes [2]. Given that that there are several known functions of HDLs with the potential to inhibit the development of atherosclerotic cardiovascular disease, it is highly likely that a reduced HDL concentration in patients with type 2 diabetes, combined with a reduction in HDL functionality, will result in a reduced level of HDL-mediated protection and thus an increased cardiovascular risk in such patients.
In addition to their antiatherogenic properties, HDLs have also been shown to have antidiabetic effects. HDLs enhance the uptake of glucose by skeletal muscle [3] and stimulate the synthesis and secretion of insulin from pancreatic β cells [4]. Furthermore, glycemic control has been shown to be improved in patients with type 2 diabetes when their HDL concentration is increased by treatment with a cholesteryl ester transfer protein (CETP) inhibitor [5]. These observations raise the possibility that a low concentration of HDLs may not only be a consequence of the diabetic state and a contributor to the increased cardiovascular risk in patients with diabetes but may also lead to a worsening of glycemic control. Collectively, these findings provide a compelling case for considering HDLs as a therapeutic target designed both to improve glycemic control and to reduce cardiovascular risk in people with type 2 diabetes.
MECHANISMS RESPONSIBLE FOR A LOW HDL-C IN DIABETES
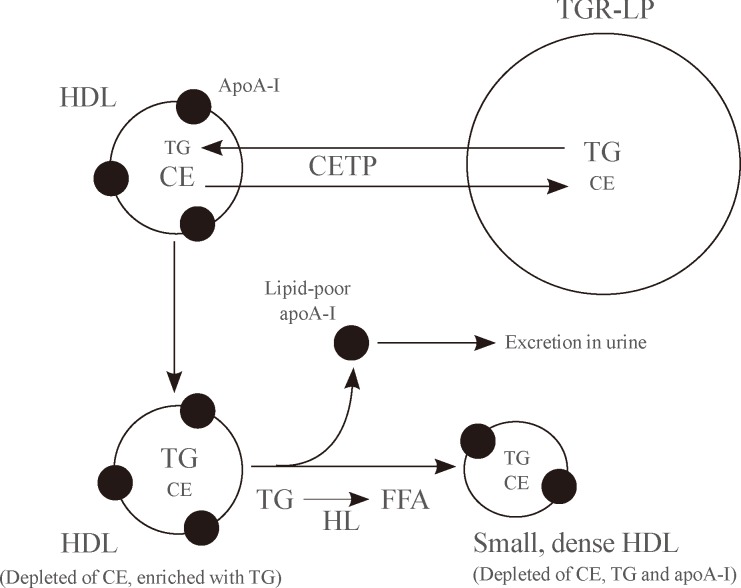
The typical dyslipidemia in type 2 diabetes includes an elevated level of plasma triglyceride, a low level of HDL-C and a low density lipoprotein (LDL) fraction that is characterized by small dense particles [1]. The low level of HDL-C in these patients is associated with the presence of HDL particles are also smaller and denser than normal. The precise mechanism responsible for a low HDL concentration in diabetes is no known, although there is evidence that the interaction of an increased concentration of triglyceride-rich lipoproteins (TRLs) with activities of CETP and hepatic lipase plays a part [6]. As outlined in Fig. 1, CETP promotes the transfer of cholesteryl esters from HDLs to TRLs in exchange for triglyceride. This generates HDL particles that are depleted of cholesteryl esters and enriched in triglyceride. This triglyceride enrichment provides HDLs with the preferred substrate for hepatic lipase that hydrolyses the newly acquired HDL TG. The resulting reduction in volume of the HDL particle core and consequent decrease in HDL particle size leads to the dissociation apolipoprotein (apo) A-I (the main HDL protein) from the HDL particle surface. The dissociated apoA-I may then be excreted in the urine and thus lost from the body. This dissociation of apoA-I from HDLs and subsequent excretion in urine provides an explanation for why, in addition to the reduced level of HDL-C, the concentration of apoA-I also tends to be low in conditions of hypertriglyceridemia such as occur in type 2 diabetes.
Fig. 1.
Low concentration of high density lipoprotein cholesterol (HDL-C) and apoA-I in patients with hypertriglyceridemia. Cholesteryl ester transfer protein (CETP) promotes the transfer of cholesteryl esters (CE) from high density lipoproteins (HDLs) to triglyceride-rich lipoproteins in exchange for triglyceride (TG). This generates HDL particles that are depleted of cholesteryl esters and enriched in triglyceride. This triglyceride enrichment provides HDLs with the preferred substrate for hepatic lipase that hydrolyses the newly acquired HDL TG. The resulting reduction in volume of the HDL particle core and consequent decrease in HDL particle size leads to the dissociation apolipoprotein (apo) A-I (the main HDL protein) from the HDL particle surface. The dissociated apoA-I may then be excreted in the urine and thus lost from the body. TGR-LP, triglyceride-rich lipoproteins; HL, hepatic lipase; FFA, free fatty acid.
CARDIOPROTECTIVE PROPERTIES OF HDLs
HDLs have a number of properties with the potential to protect against cardiovascular disease (Table 1) [7]. The best known of these relates to the ability of HDLs to promote the efflux of cholesterol from macrophages in the artery wall. However, HDLs have several additional properties with the potential to protect against atherosclerotic cardiovascular disease. These include antioxidant, antithrombotic, and anti-inflammatory properties. HDLs have also been shown to enhance endothelial function and promote both the repair of damaged endothelium and the formation of new blood vessels. And finally, there is now compelling evidence that HDLs have the ability to improve diabetic control [3-5].
Table 1.
Known Potentially Protective Properties of High Density Lipoproteins

HDL FUNCTION MAY BE ABNORMAL IN PATIENTS WITH DIABETES
Some of the potentially protective functions of HDLs are reduced in patients with diabetes. For example, apoA-I may become glycated in people with diabetes. Such glycation impairs both the ability of HDLs to promote cholesterol efflux from macrophages [8] and their ability to inhibit vascular inflammation [9] and highlights the importance of maintaining good glycemic control in people with diabetes. There is also evidence that the ability of HDLs to stimulate endothelial production of nitric oxide and thus to enhance endothelial function is impaired in patients with diabetes [2].
EFFECTS OF HDLs ON GLUCOSE HOMEOSTASIS
There is robust experimental evidence showing that HDLs impact beneficially on glucose homeostasis both by increasing pancreatic β cell function and by enhancing plasma glucose disposal.
HDLs and pancreatic β cell function
The ATP binding cassette transporter A1 (ABCA1) promotes efflux of cholesterol from cells to lipid-free/lipid-poor apoA-I in the extracellular space. It has been reported that ABCA1 deletion results in cholesterol accumulation in the cell membrane of pancreatic β cells, with a subsequent inhibition of the exocytosis of insulin from secretory granules and thus an inhibition of insulin secretion [10]. In addition to their role as acceptors of the cholesterol released from cells by ABCA1, HDLs have beneficial effects on β cells by inhibiting apoptosis [11]. It has also been shown in studies conducted in vitro using both Min6 cells and primary pancreatic islets that HDLs isolated from human plasma (and also the two major HDL apos, apo A-I, and apoA-II) increase insulin synthesis and secretion up to 5-fold [4].
HDL and muscle glucose uptake
The observation that HDLs increase cellular glucose uptake in cultures of primary human skeletal muscle cells isolated from patients with type 2 diabetes mellitus [3] provides another mechanism by which HDLs may improve diabetic control (and possibly delay the development of new onset diabetes).
STRATEGIES FOR RAISING HDL-C IN PATIENTS WITH TYPE 2 DIABETES
Lifestyle
Weight reduction
Most overweight people, especially those with type 2 diabetes, have a low concentration of HDL-C [1]. Weight reduction in such people is usually accompanied by an increase in the HDL-C level, although to be effective, the weight loss needs to be sustained long term (Table 2). The precise mechanism underlying the relationship between body weight and HDL-C concentration is uncertain.
Table 2.
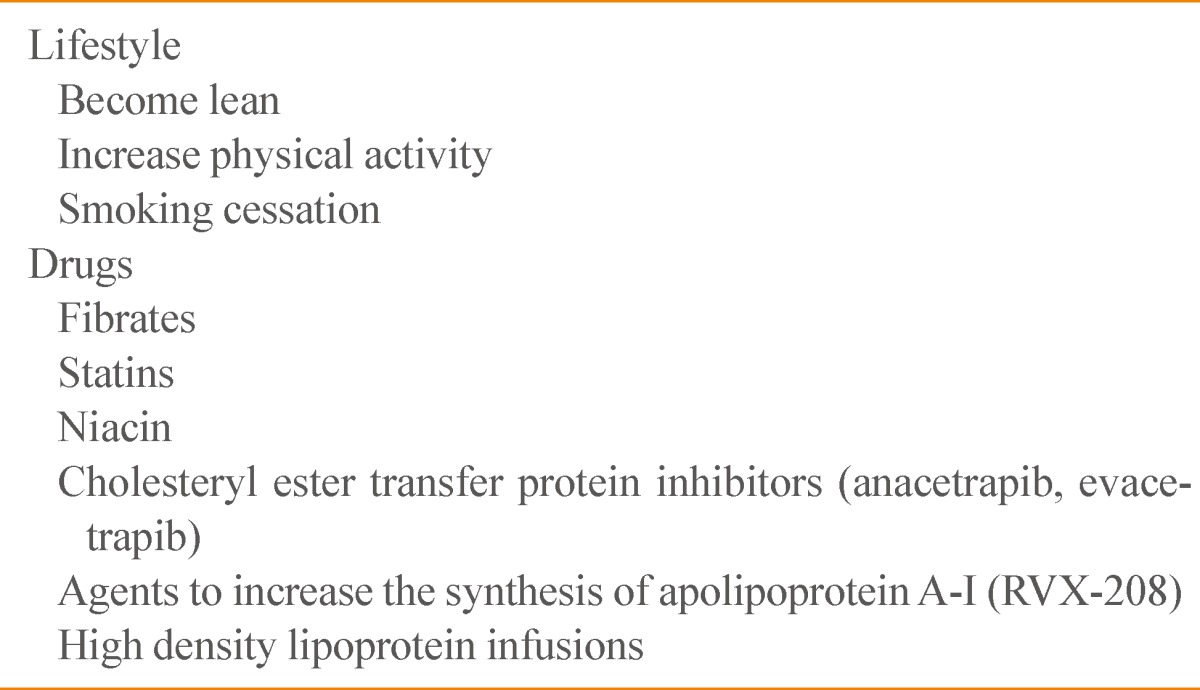
Therapeutic Strategies to Increase High Density Lipoprotein Levels
Physical activity
High levels of aerobic activity are associated with high levels of HDL-C [12] (Table 2). There is evidence that increasing the level of physical activity in people with low levels of HDL-C, especially in those who are overweight, increases the HDL-C concentration, possibly secondary to an increased activity of lipoprotein lipase and the consequent decrease in the concentration of plasma triglyceride [13]. It may be argued that the single most important preventable cause of low HDL-C in the modern world is a low level of physical activity.
A recent meta-analysis has confirmed the benefit of regular aerobic exercise on raising HDL-C levels and provided some insights into how much exercise is required [14]. The analysis included 25 randomized controlled studies that were designed to evaluate the effect of exercise training on HDL-C levels. Overall, the mean exercise-induced increase in HDL-C was 2.53 mg/dL (P<0.001). Importantly, an increase in HDL-C concentration was apparent only in people who expended at least 900 kcal or exercised for at least 120 minutes each week. In these people, every 10 minutes prolongation of exercise per session was associated with a 1.4 mg/dL increase in HDL-C. In further analyses it was found that the increase in HDL-C was greatest in people whose body mass index was <28 kg/m2. Another meta-analysis of the effects of physical activity on plasma lipids concluded that supervised exercise is also effective in elevating HDL-C levels in people with diabetes [15].
These findings emphasise the importance of recommending an increase in physical activity as a strategy to increase HDL-C levels and to reduce cardiovascular risk in people with type 2 diabetes.
Alcohol consumption
Alcohol consumption increases the level of HDL-C, possibly secondary to an inhibition of CETP [15]. However, it should be emphasized that it is not known whether the HDL-C elevation associated with alcohol consumption is cardioprotective. It should also be emphasised that a possible alcohol-induced reduction in cardiovascular risk may be counter-balanced by a wide range of adverse effects known to be associated with alcohol consumption. Thus, alcohol should not be recommended as a strategy to raise the concentration of HDL-C.
Smoking cessation
Smoking reduces the concentration of HDL-C and smoking cessation is associated with an increase in HDL-C level [16] (Table 2). While the mechanism by which smoking reduces the level of HDL-C is not known, the fact that it occurs and can be reversed by stopping smoking highlights the importance of smoking cessation in people with diabetes.
Pharmacological management
While lifestyle modification has the ability to return HDL-C levels to normal in most people, a disturbingly large number of people (especially those with diabetes) do not sustain the lifestyle required to keep HDL-C at acceptable levels. Under these circumstances, consideration should be given to raising the level of HDL-C by the use of pharmacological agents. In contrast to the availability of agents such as statins that are highly effective in reducing levels of LDL cholesterol (LDL-C), currently available HDL-raising agents are relatively ineffective. Furthermore, there is still no evidence from cardiovascular clinica outcome trials that the risk of having a major cardiovascular event is reduced by treatment with HDL-raising agents in people whose LDL-C levels have been reduced to low levels by treatment with a statin.
Currently available HDL-raising agents include fibrates, statins, and niacin (Table 2). Additional HDL-raising agents in development include inhibitors of CETP and agents that induce the synthesis of the main protein of HDL, apoA-I. Infusible forms of HDL are also under investigation.
Fibrates
The ability of fibrates to increase the concentration of HDL-C in patients with type 2 diabetes is rather modest, with increases of only 2% to 3% reported in two large clinical trials [17,18]. It should be noted, however, that treatment with fibrates (including gemfibrozil, bezafibrate, and fenofibrate) is highly effective in reducing cardiovascular risk in patients who have the combination of low HDL-C and elevated triglyceride [19]. Such results have been observed in both diabetic [17,18] and nondiabetic [20,21] subjects. However, the cardiovascular benefits of fibrates in people with low HDL-C and high triglyceride appear to be largely unrelated to fibrate-induced changes in levels of either HDL-C or triglyceride [19]. This suggests that a dyslipidemia characterized by a low HDL-C and high triglyceride identifies a group of people who derive substantial cardiovascular benefit from treatment with a fibrate but that the benefit is by mechanisms other than increases in HDL concentration.
Statins
Statins are very effective LDL-lowering agents. However, they also have a modest effect on the level of HDL-C, with reported increases in the range of 3% to 15% [22]. The increase is greatest in those in whom the baseline level of HDL-C is low [22]. Given that the level of HDL-C tends to be low in patients with type 2 diabetes, it might be expected that the HDL-C increase induced by a statin would be greater in diabetics than in nondiabetics. However, the reality is the opposite, with evidence that the increase in level of HDL-C following treatment with a statin is much smaller in diabetic than in nondiabetic patients [22]. The explanation and the clinical implications of a reduced HDL-C response to statins in people with diabetes are not known.
Statins have an adverse effect on glucose homeostasis, with documented evidence that they increase the risk of developing new onset diabetes [23]. The mechanism is not known. The cholesterol content of pancreatic β islet cells does impact of insulin synthesis and secretion, with evidence that an increase in cell cholesterol content decreases insulin secretion [24]. However, given that statin treatment will, if anything, decrease cell cholesterol levels, this is an unlikely explanation for the observed increase in new onset diabetes in people treated with statins. It is more likely that statins decrease insulin sensitivity in the liver or muscle, although there is no direct experimental evidence to support this. Thus, it is currently not known why statins impact adversely on glucose homeostasis. However, given the strong evidence that statins markedly reduce cardiovascular risk patients with type 2 diabetes [25], the clinical impact of a small increase in new onset diabetes is probably very small.
Niacin
Niacin increases HDL-C by up to 35% [26]. In addition, treatment with niacin is associated with a change in the subpopulation distribution of HDLs towards larger particles [27], a change predictive of both a slowing of coronary disease progression and a reduction in CV events.
The precise mechanism by which niacin increases the concentration of HDL-C is not known, although there is evidence that It delays the catabolism of HDL particles, possibly by decreasing activity of CETP. There is also evidence that niacin increases the synthesis of apoA-I.
In addition to increasing the plasma concentration of HDL-C and apoA-I, niacin has the capacity to modify HDLs in such a way that their function is enhanced. In one study HDLs were isolated from patients with type 2 diabetes and compared with HDLs isolated from healthy subjects [2]. Effects of the isolated HDLs on endothelium-dependent vasodilation and early endothelial progenitor cell-mediated endothelial repair were measured. Whereas the HDLs from healthy subjects stimulated endothelial nitric oxide production, reduced endothelial oxidant stress and improved both endothelium-dependent vasodilation and early endothelial progenitor cell-mediated endothelial repair, these beneficial endothelial effects of HDL were not observed in the HDLs isolated from diabetic patients. However, after the diabetic patients had been treated for 3 months with niacin, the ability of the isolated HDLs to stimulate endothelial nitric oxide, to reduce superoxide production and to promote endothelial progenitor cell-mediated endothelial repair were greatly improved [2]. Niacin has also been reported both to enhance the anti-inflammatory effects of HDLs [28] and to inhibit vascular inflammation by a mechanism that appears to be unrelated to changes in plasma lipids [29].
There is evidence that treatment with niacin reduces cardiovascular events [30] and promotes regression of atherosclerosis [31] as revealed by imaging studies in human. However, in recent clinical outcome trials [32], the addition of niacin to effective statin therapy did not reduce cardiovascular events and, in one study [33], was associated with a significant increase in serious adverse events. These findings, combined with the fact that niacin adversely impacts on glucose homeostasis by decreasing insulin sensitivity and worsening diabetic control, suggest that niacin does not have a place as an HDL-raising agent in people with type2 diabetes.
CETP inhibitors
CETP promotes net mass transfers of cholesteryl esters from HDLs to other plasma lipoprotein fractions [34]. As predicted, inhibition of CETP increases the concentration of cholesterol in the potentially protective HDL fraction, while decreasing it in potentially proatherogenic non-HDL fractions. Inhibition of CETP in rabbits has been shown to inhibit the development of diet-induced atherosclerosis [34].
However, use of the CETP inhibitor, torcetrapib, in humans did not reduce atheroma in three imaging trials [35-37] and caused an excess of deaths and cardiovascular events in a large clinical outcome trial [38]. The precise explanation for the harm caused by torcetrapib is unknown, but may relate to documented, harmful effects unrelated to inhibition of CETP [34].
There was one unexpected beneficial effect of torcetrapib that was observed in the 6,000 patients with type 2 diabetes who participated in the clinical outcome trial; the patients with diabetes who received the drug had a highly significant improvement in diabetic control [5]. It will be of great interest to see whether this result is confirmed in large, ongoing trials with other CETP inhibitors.
Another CETP inhibitor trial [39] was conducted using dalcetrapib, a weak CETP inhibitor that raises HDL levels less than torcetrapib, and which does not lower non-HDL lipoprotein levels. This trial was terminated early for reasons of futility. There was no evidence that dalcetrapib caused harm in that trial. The explanation for the failure of this trial is not known, although it was observed that the level of HDL-C in the placebo group was not predictive of cardiovascular events [39]. This may reflect the acute coronary syndrome population studied in this trial as it has been shown that HDL function is abnormal for some time after an acute coronary event [40].
Despite these setbacks, the hypothesis that CETP inhibitors will be antiatherogenic in humans is currently being tested in very large clinical outcome trials with anacetrapib and evacetrapib, two CETP inhibitors that are much more potent than dalcetrapib and which do not share the off target adverse effects of torcetrapib.
ApoA-1 synthesis inducing agents
RVX-208 is a small molecule that increases production of apoA-1 by stimulating its gene transcription [41]. It increases the concentrations of bot HDL-C and apoA-1 in humans [42], with evidence of an increase in the pre-β HDL particles that are known to be the preferred acceptors of cholesterol released from cells by the ABCA1 transporter. The effects of RVX-208 on human coronary atherosclerosis is currently being investigated.
HDL infusions
Reconstituted HDLs (rHDLs) consist of complexes of phospholipids with the main HDL apo, apoA-I. Intravenous infusions of rHDLs have been shown consistently in a variety of animal models to inhibit experimental atherosclerosis [43,44]. There are also two proof of concept studies suggesting a similar antiatherogenic effect of infusing rHDLs into humans [45,46]. Infusions of rHDLs have been shown to improve diabetic control [3].
Another novel technique related to the concept of rHDL infusion involves the collection of plasma that is subsequently subjected to a process that selectively remove lipid from HDLs. The resulting lipid poor HDLs resemble the apoA-I/phospholipid rHDLs described above. They are then reinfused back into the patient. In one small human trial involving 28 patients with acute coronary syndrome, seven once weekly treatments resulted in a numerical trend towards a decrease in atheroma volume compared to baseline [47].
The place of HDL infusions as an approach to increasing HDL levels and reducing cardiovascular risk in patients with diabetes has not yet been addressed.
CONCLUSIONS
Many patients with type 2 diabetes have a low plasma concentration of HDL-C that may contribute to an increased risk of developing cardiovascular disease. The observation that HDLs have beneficial effects on pancreatic β cell function and glucose uptake by skeletal muscle, adds support to the proposition that HDL-raising in people with type 2 diabetes may be antiatherogenic as a consequence of both direct effects on the artery wall and also by improving diabetic control. It will be of great interest to see whether ongoing studies with new HDL raising agents have beneficial effects on diabetic control.
ACKNOWLEDGMENT
This work was supported in part by a program grant from the National Health and Medical Research Council of Australia.
Footnotes
No potential conflict of interest relevant to this article was reported.
References
- 1.Mooradian AD. Dyslipidemia in type 2 diabetes mellitus. Nat Clin Pract Endocrinol Metab. 2009;5:150–159. doi: 10.1038/ncpendmet1066. [DOI] [PubMed] [Google Scholar]
- 2.Sorrentino SA, Besler C, Rohrer L, Meyer M, Heinrich K, Bahlmann FH, Mueller M, Horvath T, Doerries C, Heinemann M, Flemmer S, Markowski A, Manes C, Bahr MJ, Haller H, von Eckardstein A, Drexler H, Landmesser U. Endothelial-vasoprotective effects of high-density lipoprotein are impaired in patients with type 2 diabetes mellitus but are improved after extended-release niacin therapy. Circulation. 2010;121:110–122. doi: 10.1161/CIRCULATIONAHA.108.836346. [DOI] [PubMed] [Google Scholar]
- 3.Drew BG, Duffy SJ, Formosa MF, Natoli AK, Henstridge DC, Penfold SA, Thomas WG, Mukhamedova N, de Courten B, Forbes JM, Yap FY, Kaye DM, van Hall G, Febbraio MA, Kemp BE, Sviridov D, Steinberg GR, Kingwell BA. High-density lipoprotein modulates glucose metabolism in patients with type 2 diabetes mellitus. Circulation. 2009;119:2103–2111. doi: 10.1161/CIRCULATIONAHA.108.843219. [DOI] [PubMed] [Google Scholar]
- 4.Fryirs MA, Barter PJ, Appavoo M, Tuch BE, Tabet F, Heather AK, Rye KA. Effects of high-density lipoproteins on pancreatic beta-cell insulin secretion. Arterioscler Thromb Vasc Biol. 2010;30:1642–1648. doi: 10.1161/ATVBAHA.110.207373. [DOI] [PubMed] [Google Scholar]
- 5.Barter PJ, Rye KA, Tardif JC, Waters DD, Boekholdt SM, Breazna A, Kastelein JJ. Effect of torcetrapib on glucose, insulin, and hemoglobin A1c in subjects in the Investigation of Lipid Level Management to Understand its Impact in Atherosclerotic Events (ILLUMINATE) trial. Circulation. 2011;124:555–562. doi: 10.1161/CIRCULATIONAHA.111.018259. [DOI] [PubMed] [Google Scholar]
- 6.Barter P. Metabolic abnormalities: high-density lipoproteins. Endocrinol Metab Clin North Am. 2004;33:393–403. doi: 10.1016/j.ecl.2004.03.006. [DOI] [PubMed] [Google Scholar]
- 7.Barter PJ, Nicholls S, Rye KA, Anantharamaiah GM, Navab M, Fogelman AM. Antiinflammatory properties of HDL. Circ Res. 2004;95:764–772. doi: 10.1161/01.RES.0000146094.59640.13. [DOI] [PubMed] [Google Scholar]
- 8.Hoang A, Murphy AJ, Coughlan MT, Thomas MC, Forbes JM, O'Brien R, Cooper ME, Chin-Dusting JP, Sviridov D. Advanced glycation of apolipoprotein A-I impairs its antiatherogenic properties. Diabetologia. 2007;50:1770–1779. doi: 10.1007/s00125-007-0718-9. [DOI] [PubMed] [Google Scholar]
- 9.Nobécourt E, Tabet F, Lambert G, Puranik R, Bao S, Yan L, Davies MJ, Brown BE, Jenkins AJ, Dusting GJ, Bonnet DJ, Curtiss LK, Barter PJ, Rye KA. Nonenzymatic glycation impairs the antiinflammatory properties of apolipoprotein A-I. Arterioscler Thromb Vasc Biol. 2010;30:766–772. doi: 10.1161/ATVBAHA.109.201715. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Kruit JK, Kremer PH, Dai L, Tang R, Ruddle P, de Haan W, Brunham LR, Verchere CB, Hayden MR. Cholesterol efflux via ATP-binding cassette transporter A1 (ABCA1) and cholesterol uptake via the LDL receptor influences cholesterol-induced impairment of beta cell function in mice. Diabetologia. 2010;53:1110–1119. doi: 10.1007/s00125-010-1691-2. [DOI] [PubMed] [Google Scholar]
- 11.Kruit JK, Brunham LR, Verchere CB, Hayden MR. HDL and LDL cholesterol significantly influence beta-cell function in type 2 diabetes mellitus. Curr Opin Lipidol. 2010;21:178–185. doi: 10.1097/MOL.0b013e328339387b. [DOI] [PubMed] [Google Scholar]
- 12.Adner MM, Castelli WP. Elevated high-density lipoprotein levels in marathon runners. JAMA. 1980;243:534–536. [PubMed] [Google Scholar]
- 13.Kantor MA, Cullinane EM, Sady SP, Herbert PN, Thompson PD. Exercise acutely increases high density lipoprotein-cholesterol and lipoprotein lipase activity in trained and untrained men. Metabolism. 1987;36:188–192. doi: 10.1016/0026-0495(87)90016-3. [DOI] [PubMed] [Google Scholar]
- 14.Kodama S, Tanaka S, Saito K, Shu M, Sone Y, Onitake F, Suzuki E, Shimano H, Yamamoto S, Kondo K, Ohashi Y, Yamada N, Sone H. Effect of aerobic exercise training on serum levels of high-density lipoprotein cholesterol: a meta-analysis. Arch Intern Med. 2007;167:999–1008. doi: 10.1001/archinte.167.10.999. [DOI] [PubMed] [Google Scholar]
- 15.Hayashino Y, Jackson JL, Fukumori N, Nakamura F, Fukuhara S. Effects of supervised exercise on lipid profiles and blood pressure control in people with type 2 diabetes mellitus: a meta-analysis of randomized controlled trials. Diabetes Res Clin Pract. 2012;98:349–360. doi: 10.1016/j.diabres.2012.10.004. [DOI] [PubMed] [Google Scholar]
- 16.Maeda K, Noguchi Y, Fukui T. The effects of cessation from cigarette smoking on the lipid and lipoprotein profiles: a meta-analysis. Prev Med. 2003;37:283–290. doi: 10.1016/s0091-7435(03)00110-5. [DOI] [PubMed] [Google Scholar]
- 17.Keech A, Simes RJ, Barter P, Best J, Scott R, Taskinen MR, Forder P, Pillai A, Davis T, Glasziou P, Drury P, Kesäniemi YA, Sullivan D, Hunt D, Colman P, d'Emden M, Whiting M, Ehnholm C, Laakso M FIELD study investigators. Effects of long-term fenofibrate therapy on cardiovascular events in 9795 people with type 2 diabetes mellitus (the FIELD study): randomised controlled trial. Lancet. 2005;366:1849–1861. doi: 10.1016/S0140-6736(05)67667-2. [DOI] [PubMed] [Google Scholar]
- 18.ACCORD Study Group. Ginsberg HN, Elam MB, Lovato LC, Crouse JR, 3rd, Leiter LA, Linz P, Friedewald WT, Buse JB, Gerstein HC, Probstfield J, Grimm RH, Ismail-Beigi F, Bigger JT, Goff DC, Jr, Cushman WC, Simons-Morton DG, Byington RP. Effects of combination lipid therapy in type 2 diabetes mellitus. N Engl J Med. 2010;362:1563–1574. doi: 10.1056/NEJMoa1001282. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Barter PJ, Rye KA. Is there a role for fibrates in the management of dyslipidemia in the metabolic syndrome? Arterioscler Thromb Vasc Biol. 2008;28:39–46. doi: 10.1161/ATVBAHA.107.148817. [DOI] [PubMed] [Google Scholar]
- 20.Frick MH, Elo O, Haapa K, Heinonen OP, Heinsalmi P, Helo P, Huttunen JK, Kaitaniemi P, Koskinen P, Manninen V, Maenpaa H, Malkonen M, Manttari M, Norola S, Pasternack A, Pikkarainen J, Romo M, Sjoblom T, Nikkila EA. Helsinki Heart Study: primary-prevention trial with gemfibrozil in middle-aged men with dyslipidemia. Safety of treatment, changes in risk factors, and incidence of coronary heart disease. N Engl J Med. 1987;317:1237–1245. doi: 10.1056/NEJM198711123172001. [DOI] [PubMed] [Google Scholar]
- 21.The BIP Study Group. Secondary prevention by raising HDL cholesterol and reducing triglycerides in patients with coronary artery disease: the Bezafibrate Infarction Prevention (BIP) study. Circulation. 2000;102:21–27. doi: 10.1161/01.cir.102.1.21. [DOI] [PubMed] [Google Scholar]
- 22.Barter PJ, Brandrup-Wognsen G, Palmer MK, Nicholls SJ. Effect of statins on HDL-C: a complex process unrelated to changes in LDL-C: analysis of the VOYAGER Database. J Lipid Res. 2010;51:1546–1553. doi: 10.1194/jlr.P002816. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Sattar N, Preiss D, Murray HM, Welsh P, Buckley BM, de Craen AJ, Seshasai SR, McMurray JJ, Freeman DJ, Jukema JW, Macfarlane PW, Packard CJ, Stott DJ, Westendorp RG, Shepherd J, Davis BR, Pressel SL, Marchioli R, Marfisi RM, Maggioni AP, Tavazzi L, Tognoni G, Kjekshus J, Pedersen TR, Cook TJ, Gotto AM, Clearfield MB, Downs JR, Nakamura H, Ohashi Y, Mizuno K, Ray KK, Ford I. Statins and risk of incident diabetes: a collaborative metaanalysis of randomised statin trials. Lancet. 2010;375:735–742. doi: 10.1016/S0140-6736(09)61965-6. [DOI] [PubMed] [Google Scholar]
- 24.Hao M, Bogan JS. Cholesterol regulates glucose-stimulated insulin secretion through phosphatidylinositol 4,5-bisphosphate. J Biol Chem. 2009;284:29489–29498. doi: 10.1074/jbc.M109.038034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Cholesterol Treatment Trialists' (CTT) Collaborators. Kearney PM, Blackwell L, Collins R, Keech A, Simes J, Peto R, Armitage J, Baigent C. Efficacy of cholesterol-lowering therapy in 18,686 people with diabetes in 14 randomised trials of statins: a meta-analysis. Lancet. 2008;371:117–125. doi: 10.1016/S0140-6736(08)60104-X. [DOI] [PubMed] [Google Scholar]
- 26.Duggal JK, Singh M, Attri N, Singh PP, Ahmed N, Pahwa S, Molnar J, Singh S, Khosla S, Arora R. Effect of niacin therapy on cardiovascular outcomes in patients with coronary artery disease. J Cardiovasc Pharmacol Ther. 2010;15:158–166. doi: 10.1177/1074248410361337. [DOI] [PubMed] [Google Scholar]
- 27.Kuvin JT, Dave DM, Sliney KA, Mooney P, Patel AR, Kimmelstiel CD, Karas RH. Effects of extended-release niacin on lipoprotein particle size, distribution, and inflammatory markers in patients with coronary artery disease. Am J Cardiol. 2006;98:743–745. doi: 10.1016/j.amjcard.2006.04.011. [DOI] [PubMed] [Google Scholar]
- 28.Yvan-Charvet L, Kling J, Pagler T, Li H, Hubbard B, Fisher T, Sparrow CP, Taggart AK, Tall AR. Cholesterol efflux potential and antiinflammatory properties of high-density lipoprotein after treatment with niacin or anacetrapib. Arterioscler Thromb Vasc Biol. 2010;30:1430–1438. doi: 10.1161/ATVBAHA.110.207142. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Wu BJ, Yan L, Charlton F, Witting P, Barter PJ, Rye KA. Evidence that niacin inhibits acute vascular inflammation and improves endothelial dysfunction independent of changes in plasma lipids. Arterioscler Thromb Vasc Biol. 2010;30:968–975. doi: 10.1161/ATVBAHA.109.201129. [DOI] [PubMed] [Google Scholar]
- 30.Canner PL, Berge KG, Wenger NK, Stamler J, Friedman L, Prineas RJ, Friedewald W. Fifteen year mortality in Coronary Drug Project patients: long-term benefit with niacin. J Am Coll Cardiol. 1986;8:1245–1255. doi: 10.1016/s0735-1097(86)80293-5. [DOI] [PubMed] [Google Scholar]
- 31.Villines TC, Stanek EJ, Devine PJ, Turco M, Miller M, Weissman NJ, Griffen L, Taylor AJ. The ARBITER 6-HALTS Trial (Arterial Biology for the Investigation of the Treatment Effects of Reducing Cholesterol 6-HDL and LDL Treatment Strategies in Atherosclerosis): final results and the impact of medication adherence, dose, and treatment duration. J Am Coll Cardiol. 2010;55:2721–2726. doi: 10.1016/j.jacc.2010.03.017. [DOI] [PubMed] [Google Scholar]
- 32.AIM-HIGH Investigators. Boden WE, Probstfield JL, Anderson T, Chaitman BR, Desvignes-Nickens P, Koprowicz K, McBride R, Teo K, Weintraub W. Niacin in patients with low HDL cholesterol levels receiving intensive statin therapy. N Engl J Med. 2011;365:2255–2267. doi: 10.1056/NEJMoa1107579. [DOI] [PubMed] [Google Scholar]
- 33.HPS2-THRIVE Collaborative Group. HPS2-THRIVE randomized placebo-controlled trial in 25 673 high-risk patients of ER niacin/laropiprant: trial design, pre-specified muscle and liver outcomes, and reasons for stopping study treatment. Eur Heart J. 2013;34:1279–1291. doi: 10.1093/eurheartj/eht055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Barter PJ, Rye KA. Cholesteryl ester transfer protein inhibition as a strategy to reduce cardiovascular risk. J Lipid Res. 2012;53:1755–1766. doi: 10.1194/jlr.R024075. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Nissen SE, Tardif JC, Nicholls SJ, Revkin JH, Shear CL, Duggan WT, Ruzyllo W, Bachinsky WB, Lasala GP, Tuzcu EM ILLUSTRATE Investigators. Effect of torcetrapib on the progression of coronary atherosclerosis. N Engl J Med. 2007;356:1304–1316. doi: 10.1056/NEJMoa070635. [DOI] [PubMed] [Google Scholar]
- 36.Kastelein JJ, van Leuven SI, Burgess L, Evans GW, Kuivenhoven JA, Barter PJ, Revkin JH, Grobbee DE, Riley WA, Shear CL, Duggan WT, Bots ML RADIANCE 1 Investigators. Effect of torcetrapib on carotid atherosclerosis in familial hypercholesterolemia. N Engl J Med. 2007;356:1620–1630. doi: 10.1056/NEJMoa071359. [DOI] [PubMed] [Google Scholar]
- 37.Bots ML, Visseren FL, Evans GW, Riley WA, Revkin JH, Tegeler CH, Shear CL, Duggan WT, Vicari RM, Grobbee DE, Kastelein JJ RADIANCE 2 Investigators. Torcetrapib and carotid intima-media thickness in mixed dyslipidaemia (RADIANCE 2 study): a randomised, double-blind trial. Lancet. 2007;370:153–160. doi: 10.1016/S0140-6736(07)61088-5. [DOI] [PubMed] [Google Scholar]
- 38.Barter PJ, Caulfield M, Eriksson M, Grundy SM, Kastelein JJ, Komajda M, Lopez-Sendon J, Mosca L, Tardif JC, Waters DD, Shear CL, Revkin JH, Buhr KA, Fisher MR, Tall AR, Brewer B ILLUMINATE Investigators. Effects of torcetrapib in patients at high risk for coronary events. N Engl J Med. 2007;357:2109–2122. doi: 10.1056/NEJMoa0706628. [DOI] [PubMed] [Google Scholar]
- 39.Schwartz GG, Olsson AG, Abt M, Ballantyne CM, Barter PJ, Brumm J, Chaitman BR, Holme IM, Kallend D, Leiter LA, Leitersdorf E, McMurray JJ, Mundl H, Nicholls SJ, Shah PK, Tardif JC, Wright RS dal-OUTCOMES Investigators. Effects of dalcetrapib in patients with a recent acute coronary syndrome. N Engl J Med. 2012;367:2089–2099. doi: 10.1056/NEJMoa1206797. [DOI] [PubMed] [Google Scholar]
- 40.Besler C, Heinrich K, Rohrer L, Doerries C, Riwanto M, Shih DM, Chroni A, Yonekawa K, Stein S, Schaefer N, Mueller M, Akhmedov A, Daniil G, Manes C, Templin C, Wyss C, Maier W, Tanner FC, Matter CM, Corti R, Furlong C, Lusis AJ, von Eckardstein A, Fogelman AM, Luscher TF, Landmesser U. Mechanisms underlying adverse effects of HDL on eNOS-activating pathways in patients with coronary artery disease. J Clin Invest. 2011;121:2693–2708. doi: 10.1172/JCI42946. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Bailey D, Jahagirdar R, Gordon A, Hafiane A, Campbell S, Chatur S, Wagner GS, Hansen HC, Chiacchia FS, Johansson J, Krimbou L, Wong NC, Genest J. RVX-208: a small molecule that increases apolipoprotein A-I and high-density lipoprotein cholesterol in vitro and in vivo. J Am Coll Cardiol. 2010;55:2580–2589. doi: 10.1016/j.jacc.2010.02.035. [DOI] [PubMed] [Google Scholar]
- 42.Nicholls SJ, Gordon A, Johansson J, Wolski K, Ballantyne CM, Kastelein JJ, Taylor A, Borgman M, Nissen SE. Efficacy and safety of a novel oral inducer of apolipoprotein a-I synthesis in statin-treated patients with stable coronary artery disease a randomized controlled trial. J Am Coll Cardiol. 2011;57:1111–1119. doi: 10.1016/j.jacc.2010.11.015. [DOI] [PubMed] [Google Scholar]
- 43.Badimon JJ, Badimon L, Fuster V. Regression of atherosclerotic lesions by high density lipoprotein plasma fraction in the cholesterol-fed rabbit. J Clin Invest. 1990;85:1234–1241. doi: 10.1172/JCI114558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Nicholls SJ, Cutri B, Worthley SG, Kee P, Rye KA, Bao S, Barter PJ. Impact of short-term administration of high-density lipoproteins and atorvastatin on atherosclerosis in rabbits. Arterioscler Thromb Vasc Biol. 2005;25:2416–2421. doi: 10.1161/01.ATV.0000184760.95957.d6. [DOI] [PubMed] [Google Scholar]
- 45.Nissen SE, Tsunoda T, Tuzcu EM, Schoenhagen P, Cooper CJ, Yasin M, Eaton GM, Lauer MA, Sheldon WS, Grines CL, Halpern S, Crowe T, Blankenship JC, Kerensky R. Effect of recombinant ApoA-I Milano on coronary atherosclerosis in patients with acute coronary syndromes: a randomized controlled trial. JAMA. 2003;290:2292–2300. doi: 10.1001/jama.290.17.2292. [DOI] [PubMed] [Google Scholar]
- 46.Tardif JC, Gregoire J, L'Allier PL, Ibrahim R, Lesperance J, Heinonen TM, Kouz S, Berry C, Basser R, Lavoie MA, Guertin MC, Rodes-Cabau J Effect of rHDL on Atherosclerosis-Safety and Efficacy (ERASE) Investigators. ERASE) Investigators. Effects of reconstituted high-density lipoprotein infusions on coronary atherosclerosis: a randomized controlled trial. JAMA. 2007;297:1675–1682. doi: 10.1001/jama.297.15.jpc70004. [DOI] [PubMed] [Google Scholar]
- 47.Waksman R, Torguson R, Kent KM, Pichard AD, Suddath WO, Satler LF, Martin BD, Perlman TJ, Maltais JA, Weissman NJ, Fitzgerald PJ, Brewer HB., Jr A first-in-man, randomized, placebo-controlled study to evaluate the safety and feasibility of autologous delipidated high-density lipoprotein plasma infusions in patients with acute coronary syndrome. J Am Coll Cardiol. 2010;55:2727–2735. doi: 10.1016/j.jacc.2009.12.067. [DOI] [PubMed] [Google Scholar]