Abstract
OBJECTIVE
To examine the impact of individual and community characteristics on access to specialized epilepsy care.
METHODS
This retrospective cross-sectional study analyzed data from the California State Inpatient Sample, the State Ambulatory Surgery Database, and the State Emergency Department Database, that were linked with the 2009 Area Resource File and the location of the National Association of Epilepsy Center’s epilepsy centers. The receipt of video-EEG monitoring was measured and used to indicate access to specialized epilepsy care in subjects with persistent seizures, identified as those who had frequent seizure-related hospital admissions and/or ER visits. A hierarchical logistic regression model was employed to assess barriers to high quality care at both individual and contextual levels.
RESULTS
Among 115,632 persons with persistent seizures, individuals who routinely received care in an area where epilepsy centers were located were more likely to have access to specialized epilepsy care (OR: 1.81, 95% CI: 1.20, 2.72). Interestingly, the availability of epilepsy centers did not influence access to specialized epilepsy care in people who had private insurance. In contrast, uninsured individuals and those with public insurance programs including Medicaid and Medicare had significant gaps in access to specialized epilepsy care. Other individual characteristics such as age, race/ethnicity, and the presence of comorbid conditions were also associated with disparities in access to specialized care in PWE.
CONCLUSION
Both individual and community characteristics play substantial roles in access to high quality epilepsy care. Policy interventions that incorporate strategies to address disparities at both levels are necessary to improve access to specialized care for PWE.
Keywords: Epilepsy, Healthcare access, Healthcare disparities
1. INTRODUCTION
Disparities in access to specialized care pose significant challenges to the treatment and quality of care improvement in persons with epilepsy (PWE) (Institute of Medicine; 2012a). Previous studies provide evidence that gaps in access to comprehensive high-quality epilepsy care exist in people with low socioeconomic status, and in racial minority populations (Kelvin et al.; 2007, Begley et al.; 2009, Burneo et al.; 2009). In addition, insurance status have also been found to be important factor that can influence access to specialized care in PWE (McClelland et al.; 2007, Begley et al.; 2009, McClelland et al.; 2010, Halpern et al.; 2011, Baca et al.; 2013). So far, very little attention has been paid to the role of contextual factors in the variation of access to epilepsy care. Several studies in other disease entities have shown that characteristics of the area of residence such as socioeconomic status of the neighborhood, degree of urbanization, availability of resources and services including provider availability and managed care penetration also play an important role in access to specialty care (Gresenz et al.; 2000, Diez Roux et al.; 2001, Litaker et al.; 2005). A recent study found that geographic location of residence influenced the timing of referral for epilepsy surgery evaluation (Hauptman et al.; 2013). As the availability of specialized epilepsy care is mostly limited to urban large medical centers (Schiltz et al.; 2013), comprehensive analysis of the influence of contextual and individual attributes is a vital step for planning effective policies to reduce disparities in access to care for PWE.
The objective of this study was to examine the nature of multilevel relationships in accessing specialized epilepsy care in PWE. We used the receipt of video-EEG (VEEG) monitoring as an indicator for access to specialized epilepsy care and examined barriers to VEEG monitoring at both individual and contextual levels. VEEG monitoring is an important diagnostic test that is commonly used to confirm a diagnosis of a seizure disorder and to classify seizure type, especially in persons with persistent seizures (Cascino; 2002). Moreover, determination of candidacy for epilepsy surgery requires VEEG monitoring. It, therefore, is likely that most, if not all, of individuals with persistent seizures would have undergone VEEG monitoring, had they had access to specialized epilepsy care.
2. MATERIAL AND METHODS
The study protocol was approved by Institutional Review Board at Case Western Reserve University.
2.1 Data sources
We performed a retrospective cross-sectional study using 2005-2009 data from the California State Inpatient Sample (SID), the California State Ambulatory Surgery Database (SASD), and the California State Emergency Department Database (SEDD). These datasets are part of the Healthcare Cost and Utilization Project (HCUP) sponsored by the Agency for Healthcare Research and Quality (AHRQ) (Agency for Healthcare Research and Quality; 2011). The HCUP SID, SASD, and SEDD provide complete information on all hospital discharges, ambulatory surgeries, and emergency room (ER) visits. Each record contains patient demographic information, hospital and county identifier, diagnoses, procedures, discharge status, length of stay, as well as total charges and payment source.
Since an individual record in the HCUP State databases represents one discharge abstract rather than an individual patient, we used the HCUP revisit variables to link multiple records belonging to the same individual across facilities and hospital settings (Agency for Healthcare Research and Quality; 2012), thus making it possible to analyze the data at the individual level, rather than at the encounter level. The revisit variables are states and year specific, and can only be created for states that provide unique encrypted patient identifier (Agency for Healthcare Research and Quality; 2012). In 2005, the revisit variables for all HCUP state data including SID, SASD, and SEDD were available in 4 states including California, Florida, Nebraska, and Utah (Agency for Healthcare Research and Quality; 2013). California data were readily available to us, and therefore were used for the analysis of this study.
In addition, we used the Area Resource File (ARF), which provided a comprehensive collection of contextual data, including socioeconomic and environmental characteristics for each county within the US (US Department of Health and Human Services; 2011). ARF 2009 data elements were linked to the California SID, SASD, and SEDD based on the location of hospital and/or ambulatory centers by a common 5-digit Federal Information Processing Standards (FIPS) code that was unique to each US county.
We also obtained the address of all Level 3 and Level 4 epilepsy centers (ECs) in the State of California from the National Association of Epilepsy Center (NAEC) website (http://www.naec-epilepsy.org/find.htm) and linked the location of ECs to other socioeconomic and environmental variables in the ARF by matching the county of each individual center to a corresponding FIPS code.
2.2 Study population
Individuals with at least 1 occurrence of the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) code for epilepsy (ICD-9-CM: 345.xx), or 2 or more occurrences, at least 30 days apart, of ICD-9-CM codes for convulsion (ICD-9-CM: 780.39) were included. These criteria have been shown to have high degree of accuracy for identifying epilepsy cases from facility-based administrative records (Jette et al.; 2010, Faught et al.; 2012). We further limited our study population to individuals with persistent seizures, identified as those who had frequent (≥5) seizure-related hospital admissions and/or ER visits during the study period. This operational definition was designed based on the Institute of Medicine report that patients with persistent seizures require a referral to more advance level of care for further diagnosis and treatment (Institute of Medicine; 2012a). The sensitivity analysis in subjects with higher number of seizure-related hospital admissions and/or ER visits (≥10 and ≥15) was also performed to test the robustness of our findings. Individuals over age 65 were excluded.
2.3 Outcomes
The outcome was the receipt of VEEG monitoring, identified by the presence of primary ICD-9-CM procedure codes 89.19.
2.4 Individual level characteristics
Data on all individual level variables were obtained from the California SID, SASD, and SEDD. Age was categorized as children (0-17 years), young adults (18-34 years), and adults (35-64 years). Race/ethnicity was classified as white, black, Hispanic, and other races. Based on the source of payment documented in hospital discharge records, insurance status was categorized as private (or commercial), Medicaid, Medicare, uninsured, and others. In the US, Medicaid and Medicare programs are public health insurance programs funded by state and federal governments. Medicaid, the largest health insurance program in the US, is a program for low-income and medically vulnerable groups of people including children, pregnant women, adults with dependent children, people with severe disabilities, and the elderly (Schneider & Elias; 2002). In order to qualify for Medicaid, a person must belong to one of the Medicaid’s categorically eligible groups and meet financial criteria. Each state determines its eligibility criteria for Medicaid program, particularly the minimum income threshold and the definition of disability (Schneider et al.; 2000). Medicare is a health insurance program for individuals older than 65, people suffering from end-stage renal disease, or amyotrophic lateral sclerosis, regardless of their income (The Henry J. Kaiser Family Foundation; 2010). Persons younger than 65 can also be qualified for Medicare benefits if they have permanent disabilities and receive Social Security Disability Income for at least 2 years (The Henry J. Kaiser Family Foundation; 2010). Some low-income seniors and persons with disabilities receive both Medicaid and Medicare benefits. Medicare is the primary source of coverage for these dual eligible beneficiaries (Jacobson et al.; 2012). We used Elixhauser comorbid measurement (Elixhauser et al.; 1998) to identify the patient’s comorbid conditions.
2.5 Contextual level characteristics
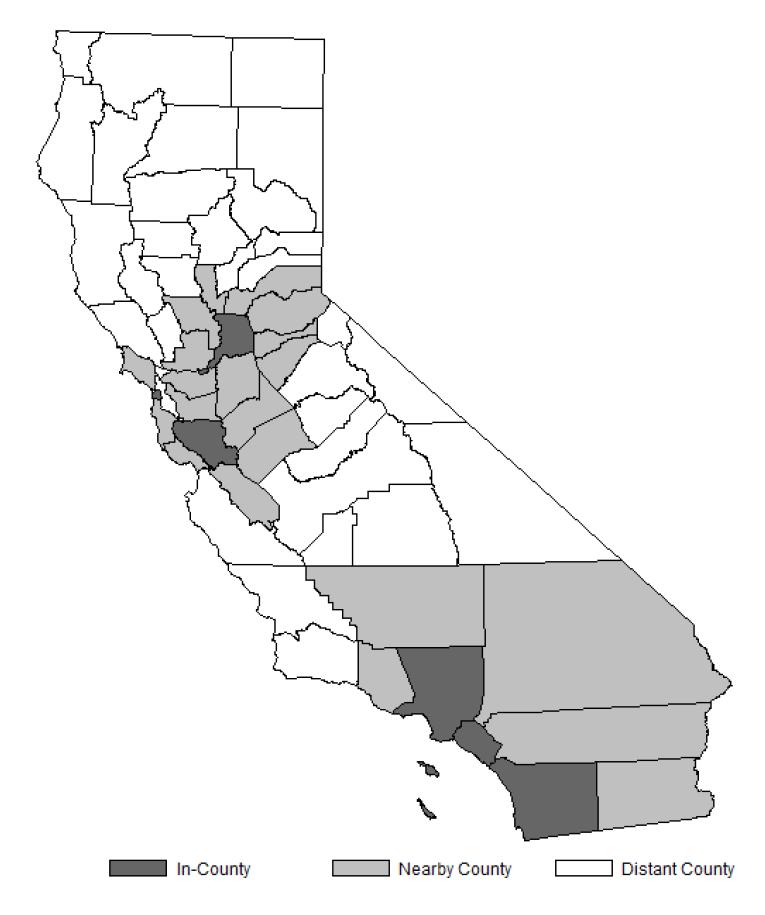
The contextual characteristics were obtained at the county level from the ARF including the proportion of residents living in poverty, percentage with a 4-year college degree, urban/rural designation, and whether the county was designated as a high unemployment area as defined by the National Bureau of Economic Research. We matched each individual patient to a county based on the location of the hospital and/or ambulatory centers (s)he attended most often. For patients with no regular source of care (1.7%), the location of the first hospital or ambulatory centers visited was used. We classified counties where the patients received their medical care into 3 mutually exclusive groups based on the availability of Level 3 or Level 4 ECs (Figure 1). EC counties were home to at least 1 Level 3 or Level 4 ECs. Nearby counties shared a geographic border with an EC county, while the remaining counties were categorized as distant.
Figure 1.
Location of Level 3 and Level 4 epilepsy centers in the State of California and classification of the availability of epilepsy centers by counties.
2.6 Statistical analysis
We used hierarchical logistic regression to examine the impact of individual and contextual characteristics on access to specialized epilepsy care. This multilevel analytic approach accounts for shared characteristics of individuals within the same clusters or units, and provides robust standard errors and reduces the potential for type I error (Barcikowski; 1981). Hierarchical models, therefore, are useful when the associations of interest arise from multiple sources or within organizational units (Raudenbush & Bryk; 2002). We first analyzed the association between individual level factors and the receipt of VEEG monitoring (Table 3; Individual model). All individual characteristics were retained for the second analysis, which assessed the association between the presence of epilepsy centers and the receipt of VEEG monitoring (Table 3; Hierarchical model I). Our third model kept the covariates from the first 2 models and then added social and economic community factors (Table 3; Hierarchical Model II). In addition, we tested several a priori cross-level interactions to explore differential relationships between individual and contextual characteristics. Specifically, interactions between insurance status and all contextual level variables, and between proximity to ECs and all individual level variables were examined. We used version 9.2 of the SAS system for UNIX (SAS Institute Inc., Cary, NC) for all descriptive statistics and HLM version 7 for Windows (Scientific Software International, Lincolnwood, IL) for hierarchical analyses.
Table 3.
Adjusted odds ratio of individual and contextual characteristics on the access to specialized epilepsy care based on the Andersen behavioral model of health service utilization (Andersen; 2008).
| Individual model OR (95% CI) |
Hierarchical Model I OR (95% CI) |
Hierarchical Model II OR(95% CI) |
|
|---|---|---|---|
| PREDISPOSING FACTORS | |||
| Gender | |||
| Female | 1.34 (1.25-1.43)† | 1.34 (1.25-1.43)† | 1.34 (1.25-1.43)† |
| Age | |||
| 0 to 17 | 2.42 (2.20-2.66)† | 2.42 (2.20-2.66)† | 2.42 (2.20-2.66)† |
| 18 to 34 | 2.04 (1.88-2.22)† | 2.04 (1.88-2.22)† | 2.04 (1.88-2.22)† |
| 35-64 | Reference | Reference | Reference |
| Race | |||
| Black | 0.54 (0.48-0.61)† | 0.54 (0.47-0.60)† | 0.54 (0.47-0.60)† |
| Hispanic | 0.87 (0.80-0.95)§ | 0.87 (0.80-0.95)§ | 0.87 (0.80-0.95)§ |
| Other race | 1.03 (0.89-1.19) | 1.02 (0.89-1.18) | 1.02 (0.89-1.18) |
| White | Reference | Reference | Reference |
| ENABLING FACTORS | |||
| Insurance status | |||
| Medicaid | 0.49 (0.45-0.53)† | 0.49 (0.45-0.53)† | 0.49 (0.45-0.53)† |
| Medicare | 0.69 (0.63-0.76)† | 0.69 (0.63-0.76)† | 0.69 (0.63-0.76)† |
| Uninsured | 0.14 (0.11-0.18)† | 0.14 (0.11-0.18)† | 0.14 (0.11-0.18)† |
| Private | Reference | Reference | Reference |
| NEED FACTORS | |||
| Comorbid conditions | |||
| One | 0.90 (0.83-0.98)§ | 0.90 (0.83-0.98)§ | 0.90 (0.83-0.98)§ |
| Two or more | 0.50 (0.45-0.55)† | 0.50 (0.45-0.55)† | 0.50 (0.45-0.55)† |
| None | Reference | Reference | Reference |
| HEALTH SYSTEM FACTORS | |||
| Location of epilepsy centers | |||
| In the county | 1.81 (1.20-2.72)§ | 1.49 (0.97-2.29) | |
| In nearby county | 1.05 (0.77-1.43) | 0.95 (0.70-1.29) | |
| Far from the county | Reference | Reference | |
| SOCIAL AND ECONOMIC FACTORS | |||
| Poverty level of the community | |||
| Higher than median a | 0.78 (0.54-1.14) | ||
| Proportion of individuals with 4 year college education | |||
| Highest quartile | 1.36 (0.69-2.68) | ||
| Middle quartiles | 1.14 (0.65-2.00) | ||
| Lowest quartile | Reference | ||
| Employment | |||
| High unemployment | 1.16 (0.68-1.97) | ||
Abbreviations: CI, Confidence interval; OR, Odds ratio.
Level of statistical significance: P≤;0.001;
0.001< P≤ 0.05.
Reference categories: Poverty level of the community below the state median.
3. RESULTS
Our study included 115,632 individuals with persistent seizures, among whom 3,692 subjects underwent VEEG monitoring during the study period. Table 1 described our study population by various individual characteristics. In particular, the rates of VEEG monitoring in patients who were uninsured or who had public insurance were significantly lower than the rates for patients who had private insurance. VEEG monitoring was least common among blacks, males, and those with multiple comorbid conditions. In addition, adults (age 35-64) had the lowest rates of VEEG monitoring.
Table 1.
Individual level characteristics of all adults with persistent seizures, and those who had access to specialized epilepsy care in California between 2005 and 2009.
| Study population | Subjects with access to specialized epilepsy care | ||
|---|---|---|---|
| n (%) | n (%) | Row percent | |
| Overall | 115,632 (100%) | 3,692 (100%) | 3.2% |
| Gender | |||
| Male | 58,728 (51%) | 1,535 (42%) | 2.6% |
| Female | 56,686 (49%) | 2,064 (56%) | 3.6% |
| Age | |||
| 0 - 17 | 15,934 (14%) | 846 (23%) | 5.3% |
| 18 - 34 | 25,758 (22%) | 1,155 (31%) | 4.5% |
| 35 - 64 | 73,940 (64%) | 1,691 (46%) | 2.3% |
| Race | |||
| White | 63,841 (55%) | 2,091 (57%) | 3.3% |
| Black | 18,852 (16%) | 338 (9%) | 1.8% |
| Hispanic | 27,183 (24%) | 903 (24%) | 3.3% |
| Other | 5,347 (5%) | 233 (6%) | 4.4% |
| Missing | 409 (0%) | 127 (3%) | 31.1% |
| Insurance status | |||
| Private | 28,126 (24%) | 1,637 (44%) | 5.8% |
| Medicare | 27,439 (24%) | 717 (19%) | 2.6% |
| Medicaid | 42,276 (37%) | 1,121 (30%) | 2.7% |
| Uninsured | 11,828 (10%) | 87 (2%) | 0.7% |
| Others | 5,963 (5%) | 130 (4%) | 2.2% |
| Comorbid conditions | |||
| None | 60,584 (52%) | 2,376 (64%) | 3.9% |
| One | 25,082 (22%) | 826 (22%) | 3.3% |
| Two or more | 29,966 (26%) | 490 (13%) | 1.6% |
Table 2 summarized the contextual characteristics of the study population. There were 6 counties that had Level 3 or Level 4 ECs in the State of California (Figure 1). The majority of persons with persistent seizures (87%) in our study lived in or adjacent to the counties where these ECs were located. They also lived in the metropolitan area and in counties with a high proportion of people with college education and low unemployment.
Table 2.
Contextual characteristics of all adults with persistent seizures and those who had access to specialized epilepsy care in California between 2005 and 2009.
| County characteristics | Number of counties |
Study population (%) | Subjects with access to specialized care (%) |
|---|---|---|---|
| Total | 58 | 115,632 (100%) | 3,692 (100%) |
| Location of epilepsy centers | |||
| Within the county | 6 | 59,993 (52%) | 2,418 (65%) |
| Adjacent to the county | 21 | 38,512 (33%) | 831 (23%) |
| Far from the county | 31 | 17,127 (15%) | 443 (12%) |
| Poverty level of the community | |||
| Under state median | 29 | 55,520 (48%) | 1,778 (48%) |
| Over state median | 29 | 60,112 (52%) | 1,914 (52%) |
| Proportion of individuals with 4 year college education | |||
| Lowest quartile | 15 | 11,076 (10%) | 246 (7%) |
| Middle quartile | 28 | 67,172 (58%) | 2,101 (57%) |
| Highest quartile | 15 | 37,384 (32%) | 1,345 (36%) |
| Employment | |||
| High unemployment | 18 | 14,523 (13%) | 328 (9%) |
| Low unemployment | 40 | 101,109 (87%) | 3,364 (91%) |
| Urban/ Rural Class | |||
| Metro | 37 | 111,959 (97%) | 3,606 (98%) |
| Non-metro or Rural | 21 | 3,673 (3%) | 86 (2%) |
Multiple logistic regression on the individual level predictors revealed that several factors were associated with access to specialized epilepsy care (Table 3, Individual model). Patients who were uninsured or publicly insured including Medicaid and Medicare were less likely than patients who were privately insured to have access to VEEG monitoring. Gaps in access to specialized epilepsy care were also noted among blacks, Hispanics, and those with comorbid conditions. Age also played a role. Younger patients (children and young adults) were more likely to have access to specialized epilepsy care compared to adults. We found no change in significance or direction of individual level coefficients after the addition of contextual level characteristics.
Moving to our contextual covariates, receiving care in an EC county was associated with an increased likelihood of the receipt of sophisticated epilepsy care (OR: 1.81, 95% CI: 1.20, 2.72) (Table 3, Hierarchical Model I). We also found that none of the other county level covariates such as level of poverty, education, and unemployment had significant impact on the access to specialized care among PWE (Table 3; Hierarchical Model II). Tests of pairwise combinations of individual and contextual levels did not show any significant cross-level interactions.
The sensitivity analysis in individuals with higher number of seizure-related hospital admissions and/or ER visits provided essentially similar results as the primary analysis (data not shown).
4. DISCUSSION
This is the first population-based study that explores the impact of individual and community characteristics on disparities in access to specialized care in PWE. We showed that individuals with persistent seizures who routinely received medical services in the area where the epilepsy centers were located tended to have access to high quality epilepsy care than those who received care elsewhere. The availability of ECs, therefore, plays an important role in access to specialized care in PWE. Simply providing health insurance to the uninsured without expansion of ECs is unlikely to eliminate or reduce disparities. Actions in the form of policy changes, such as an expansion of the Medicaid program (Baicker et al.; 2013), an implementation of health insurance exchange program that subsidizes the purchase of private insurance for low-income people (Rosenbaum & Sommers; 2013), an improvement of reimbursement policies (Cunningham & Nichols; 2005), and an enactment of effective care coordination particularly specialty referral (Bodenheimer; 2008) are needed to ensure that PWE particularly those who are uninsured and those on Medicaid and/or Medicare have access to the highly effective epilepsy management.
Impact of insurance status on access to care in PWE has been studied very rarely. A survey of health care utilization at 4 epilepsy clinics that serve sociodemographically diverse populations shows that individuals with public insurance and those who are uninsured had lower rates of specialty care and higher rates of hospitalizations than privately insured individuals (Begley et al.; 2009). An analysis of the Medical Expenditure Panel Survey (MEPS), which provides a nationally representative sample of the US civilian non-institutionalized population, also suggests that uninsured individuals with epilepsy have significantly fewer physician and ER visits but greater costs for medications than those who are privately insured (Halpern et al.; 2011). Moreover, few studies that examine the receipt of epilepsy surgery find that privately insured individuals are more likely than those who are uninsured or publicly insured to undergo surgery (McClelland et al.; 2007, 2010). Public insurance programs, particularly Medicaid, are designed to provide access to medical care for those who otherwise would be uninsured. Yet, people who carry this most basic form of health insurance continue to face barriers to specialized care (Gold et al.; 2006, Bisgaier & Rhodes; 2011). The reason for inaccessibility to high quality care in Medicaid enrollees appears to be multifactorial. Low reimbursement (Cunningham & Nichols; 2005), delay in payment, difficulty of payment procedures (Berman et al.; 2002), size of community where practices are located, underlying providers’ attitudes, and knowledge about Medicaid programs (Margolis et al.; 1992) are important determinants of physicians’ decisions to participate in Medicaid. As a result, Medicaid programs often rely on a network of a small number of specialists (Landon et al.; 2007, Bisgaier & Rhodes; 2011). There is little doubt that Medicaid coverage improves access to general medical care for PWE (Halpern et al.; 2011). However, access to specialized high quality care in this indigent population remains extremely limited.
Studies in other disease entities usually show that Medicare as well as privately insured patients are more likely to receive better care than Medicaid patients or those who are uninsured (Liu et al.; 2006, LaPar et al.; 2012). In contrast, Medicare beneficiaries with epilepsy are found to have significantly lower likelihood of specialist visits and higher likelihood of visits with general physicians, compared to privately insured individuals (Begley et al.; 2009). We confirm that having Medicare does not guarantee access to high quality epilepsy management. However, since we limited our study population to individuals younger than 65, the results of this study can be applied only to the non-elderly Medicare beneficiaries.
Our findings highlight the significance of racial disparities in accessing specialized epilepsy care. We showed that not only blacks but also Hispanics with epilepsy were less likely than their white counterparts to have access to specialized care. The reasons for racial disparities in access to care are complex and likely influenced by several factors related to the patients themselves (e.g., attitudes toward risk, the health care system, and care-seeking behavior) (Zuvekas & Taliaferro; 2003), as well as those related to physicians (e.g., communication skills, quantity and quality of information provided) (Griggs & Engel; 2005). An inverse relationship between age and comorbid conditions in access to epilepsy care has been shown previously (Navaneethan et al.; 2007, Mukherjee et al.; 2010). As a large number of aging population increases, the impact of age and comorbidities on access to high quality care in PWE deserves further study.
Measuring access to care is complex. In this study, we focused mainly on the receipt of VEEG monitoring, which represented merely one aspect of specialized epilepsy care. In addition, very few individuals may undergo surgery without VEEG monitoring. We, therefore, could have missed a small group of people who in fact had access to specialized epilepsy care. Exclusion of these subjects was unlikely to affect our findings.
Whether our findings can be generalized to other states or the entire US is arguable. California is a large state that has several unique characteristics, including a substantial proportion of ethnic minorities, especially Asian and Hispanic, and a high number of uninsured individuals (Fronstin; 2012). Moreover, a large presence of integrated delivery systems, particularly Kaiser Permanente, and a high penetration of Health Maintenance Organization (HMO) in California might have augmented access to specialized epilepsy care among privately insured individuals through better care coordination and referral. Since each state operates its own Medicaid program, the variation of Medicaid policies at a state level, leading to significant differences in access and quality of care among Medicaid enrollees in different geographic regions (Subramanian & Chen; 2013), must be carefully considered.
Our contextual-level findings should be interpreted with some caution. Defining proximity to an EC at the county level is somewhat crude, especially for areas where counties are large such as the southern part of California. More detailed geographic data at the patient level such as address or zip code would allow for a better measure of proximity. In addition, smaller geographic units would also yield more power to detect effects at the contextual level, as our power was limited by the number of counties. Nonetheless, our findings were in line with a recent study that assessed a referral pattern among children with refractory epilepsy who underwent surgery at the University of California, Los Angeles (Hauptman et al.; 2013). Hauptman et al. found that patients from Los Angeles County had shorter interval from seizure onset to referral, compared to those from the Western US. (Hauptman et al.; 2013).
Limitations, especially those that are inherent to studies using claims data, should also be considered. The SID, SASD, and SEDD datasets do not contain detailed clinical information or prescribed medications. The accuracy of epilepsy case ascertainment, therefore, is mainly based on diagnosis codes without other information. Recent studies showed that the use of diagnosis codes to identify PWE in administrative data generally had high sensitivity and good positive predictive values (Kee et al.; 2012, Reid et al.; 2012). Moreover, our operational definition of epilepsy was designed to capture subgroup of people with persistent seizures, rather than people with refractory epilepsy. This particular group of people with frequent seizures should be referred to specialized epilepsy centers for further investigation, particularly VEEG monitoring.
Some of them might turn out to have non-epileptic or psychogenic spells after a thorough work-up. The robustness of our findings was confirmed by sensitivity analysis in subjects with a higher number of admissions and/or ER visits.
Besides the accuracy of case definition, coding errors are also important and could potentially affect the results of this study. Nonetheless, such errors are likely diluted (owing to the large sample) and not likely to strongly bias the overall results. It is also important to note that we identified the location of specialized epilepsy centers based on the membership of the NAEC. The NAEC membership is voluntary and the classification of Level 3 and Level 4 ECs are self-designated without external evaluation to assess whether the NAEC’s ECs actually provide the level of care that they report (Institute of Medicine; 2012b). However, the NAEC is the only organization that defines the criteria for and collects the data on comprehensive epilepsy management in the US. Many hospitals that provide specialized epilepsy care, such as the Department of Veteran Affairs (VA) Epilepsy Centers of Excellence and the Kaiser Foundation Hospitals may not join the NAEC and, therefore, are not included in the contextual level analysis of this study. Our recent report on trends in pre-surgical evaluations and epilepsy surgery in the US showed that >90% of VEEG monitoring are still performed in large academic medical centers (Schiltz et al.; 2013), most of which are likely to be Level 4 ECs of the NAEC. Nevertheless, an inclusion of hospitals that provide comprehensive epilepsy care, like the VA Epilepsy Center of Excellence and the Kaiser Foundation Hospitals, in our contextual level analysis would likely strengthen the association between the availability of ECs and the access to specialized epilepsy management.
HIGHLIGHT.
-
■
Uninsured PWE and those with Medicaid/Medicare had gaps in access to epilepsy care.
-
■
The availability of epilepsy centers can influence access to care in PWE.
-
■
Privately insured PWE did not have difficulty in access to epilepsy centers.
ACKNOWLEDGEMENTS
Mr. Schiltz is supported by the Agency for Healthcare Research and Quality (AHRQ) T32 Institutional Training Grant, #5T32HS000059-18. Dr. Kaiboriboon is supported by the Epilepsy Foundation. This study was also supported in part by the Case Western Reserve University/Cleveland Clinic CTSA Grant Number UL1 RR024989 from the National Center for Research Resources (NCRR), a component of the National Institutes of Health and NIH roadmap for Medical Research. Its contents are solely the responsibility of the authors and do not necessarily represent the official view of NCRR or NIH.
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
REFERENCES
- Agency for Healthcare Research and Quality HCUP Supplemental Variables for Revisit Analyses. 2013 Retrieved July 4, 2013, from http://www.hcup-us.ahrq.gov/toolssoftware/revisit/revisit.jsp#user.
- Agency for Healthcare Research and Quality HCUP Supplemental Files for Revisit Analyses. 2012 Retrieved July 4, 2013, from www.hcup-us.ahrq.gov/toolssoftware/revisit/revisit.jsp.
- Agency for Healthcare Research and Quality HCUP Databases. 2011 doi: 10.1080/15360280802537332. Retrieved July 4, 2013, from http://www.hcup-us.ahrq.gov/databases.jsp. [DOI] [PubMed]
- Andersen RM. National health surveys and the behavioral model of health services use. Med Care. 2008;46:647–653. doi: 10.1097/MLR.0b013e31817a835d. [DOI] [PubMed] [Google Scholar]
- Baca CB, Vickrey BG, Vassar S, Hauptman JS, Dadour A, Oh T, Salamon N, Vinters HV, Sankar R, Mathern GW. Time to pediatric epilepsy surgery is related to disease severity and nonclinical factors. Neurology. 2013;80:1231–1239. doi: 10.1212/WNL.0b013e3182897082. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Baicker K, Taubman SL, Allen HL, Bernstein M, Gruber JH, Newhouse JP, Schneider EC, Wright BJ, Zaslavsky AM, Finkelstein AN, Carlson M, Edlund T, Gallia C, Smith J. The Oregon experiment--effects of Medicaid on clinical outcomes. N Engl J Med. 2013;368:1713–1722. doi: 10.1056/NEJMsa1212321. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barcikowski RS. Statistical power with group mean as the unit of analysis. Journal of Educational and Behavioral Statistics. 1981;6:267–285. [Google Scholar]
- Begley CE, Basu R, Reynolds T, Lairson DR, Dubinsky S, Newmark M, Barnwell F, Hauser A, Hesdorffer D, Hernandez N, Karceski SC, Shih T. Sociodemographic disparities in epilepsy care: Results from the Houston/New York City health care use and outcomes study. Epilepsia. 2009;50:1040–1050. doi: 10.1111/j.1528-1167.2008.01898.x. [DOI] [PubMed] [Google Scholar]
- Berman S, Dolins J, Tang SF, Yudkowsky B. Factors that influence the willingness of private primary care pediatricians to accept more Medicaid patients. Pediatrics. 2002;110:239–248. doi: 10.1542/peds.110.2.239. [DOI] [PubMed] [Google Scholar]
- Bisgaier J, Rhodes KV. Auditing access to specialty care for children with public insurance. N Engl J Med. 2011;364:2324–2333. doi: 10.1056/NEJMsa1013285. [DOI] [PubMed] [Google Scholar]
- Bodenheimer T. Coordinating care--a perilous journey through the health care system. N Engl J Med. 2008;358:1064–1071. doi: 10.1056/NEJMhpr0706165. [DOI] [PubMed] [Google Scholar]
- Burneo JG, Jette N, Theodore W, Begley C, Parko K, Thurman DJ, Wiebe S. Disparities in epilepsy: report of a systematic review by the North American Commission of the International League Against Epilepsy. Epilepsia. 2009;50:2285–2295. doi: 10.1111/j.1528-1167.2009.02282.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cascino GD. Clinical indications and diagnostic yield of video-electroencephalographic monitoring in patients with seizures and spells. Mayo Clin Proc. 2002;77:1111–1120. doi: 10.4065/77.10.1111. [DOI] [PubMed] [Google Scholar]
- Cunningham PJ, Nichols LM. The effects of medicaid reimbursement on the access to care of medicaid enrollees: a community perspective. Med Care Res Rev. 2005;62:676–696. doi: 10.1177/1077558705281061. [DOI] [PubMed] [Google Scholar]
- Diez Roux AV, Merkin SS, Arnett D, Chambless L, Massing M, Nieto FJ, Sorlie P, Szklo M, Tyroler HA, Watson RL. Neighborhood of residence and incidence of coronary heart disease. N Engl J Med. 2001;345:99–106. doi: 10.1056/NEJM200107123450205. [DOI] [PubMed] [Google Scholar]
- Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998;36:8–27. doi: 10.1097/00005650-199801000-00004. [DOI] [PubMed] [Google Scholar]
- Faught E, Richman J, Martin R, Funkhouser E, Foushee R, Kratt P, Kim Y, Clements K, Cohen N, Adoboe D, Knowlton R, Pisu M. Incidence and prevalence of epilepsy among older US Medicare beneficiaries. Neurology. 2012;78:448–453. doi: 10.1212/WNL.0b013e3182477edc. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fronstin P. California’s uninsured: treading water. 2012 Retrieved July 12, 2013, from http://www.chcf.org/~/media/MEDIA%20LIBRARY%20Files/PDF/C/PDF%20CaliforniaUninsured2012.pdf.
- Gold M, Kuo S, Taylor EF. Translating research to action: improving physician access in public insurance. J Ambul Care Manage. 2006;29:36–50. doi: 10.1097/00004479-200601000-00005. [DOI] [PubMed] [Google Scholar]
- Gresenz CR, Stockdale SE, Wells KB. Community effects on access to behavioral health care. Health Serv Res. 2000;35:293–306. [PMC free article] [PubMed] [Google Scholar]
- Griggs JJ, Engel JJ. Epilepsy surgery and the racial divide. Neurology. 2005;64:8–9. doi: 10.1212/01.WNL.0000148962.13913.BD. [DOI] [PubMed] [Google Scholar]
- Halpern MT, Renaud JM, Vickrey BG. Impact of insurance status on access to care and out-of-pocket costs for U.S. individuals with epilepsy. Epilepsy Behav. 2011;22:483–489. doi: 10.1016/j.yebeh.2011.07.007. [DOI] [PubMed] [Google Scholar]
- Hauptman JS, Dadour A, Oh T, Baca CB, Vickrey BG, Vassar SD, Sankar R, Salamon N, Vinters HV, Mathern GW. Sociodemographic changes over 25 years of pediatric epilepsy surgery at UCLA. J Neurosurg Pediatr. 2013;11:250–255. doi: 10.3171/2012.11.PEDS12359. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Institute of Medicine (IOM) Epilepsy across the spectrum: promoting health and understanding. The National Academic Press; Washington, DC: 2012a. [Google Scholar]
- Institute of Medicine (IOM) Health care: quality, access, and value. In: England MJ, Liverman CT, Schultz AM, Strawbridge LM, editors. Epilepsy across the spectrum: Promoting health and understanding. The National Academy Press; Washington DC: 2012b. pp. 113–161. [PubMed] [Google Scholar]
- Jacobson G, Neuman T, Damico A. Medicare’s role for dual eligible beneficiaries. 2012 Retrieved July 4, 2013, from http://kaiserfamilyfoundation.files.wordpress.com/2013/01/8138-02.pdf.
- Jette N, Reid AY, Quan H, Hill MD, Wiebe S. How accurate is ICD coding for epilepsy? Epilepsia. 2010;51:62–69. doi: 10.1111/j.1528-1167.2009.02201.x. [DOI] [PubMed] [Google Scholar]
- Kee VR, Gilchrist B, Granner MA, Sarrazin NR, Carnahan RM. A systematic review of validated methods for identifying seizures, convulsions, or epilepsy using administrative and claims data. Pharmacoepidemiol Drug Saf. 2012;21(Suppl 1):183–193. doi: 10.1002/pds.2329. [DOI] [PubMed] [Google Scholar]
- Kelvin EA, Hesdorffer DC, Bagiella E, Andrews H, Pedley TA, Shih TT, Leary L, Thurman DJ, Hauser WA. Prevalence of self-reported epilepsy in a multiracial and multiethnic community in New York City. Epilepsy Res. 2007;77:141–150. doi: 10.1016/j.eplepsyres.2007.09.012. [DOI] [PubMed] [Google Scholar]
- Landon BE, Schneider EC, Normand SL, Scholle SH, Pawlson LG, Epstein AM. Quality of care in Medicaid managed care and commercial health plans. JAMA. 2007;298:1674–1681. doi: 10.1001/jama.298.14.1674. [DOI] [PubMed] [Google Scholar]
- LaPar DJ, Stukenborg GJ, Guyer RA, Stone ML, Bhamidipati CM, Lau CL, Kron IL, Ailawadi G. Primary payer status is associated with mortality and resource utilization for coronary artery bypass grafting. Circulation. 2012;126:S132–9. doi: 10.1161/CIRCULATIONAHA.111.083782. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Litaker D, Koroukian SM, Love TE. Context and healthcare access: looking beyond the individual. Med Care. 2005;43:531–540. doi: 10.1097/01.mlr.0000163642.88413.58. [DOI] [PubMed] [Google Scholar]
- Liu JH, Zingmond DS, McGory ML, SooHoo NF, Ettner SL, Brook RH, Ko CY. Disparities in the utilization of high-volume hospitals for complex surgery. JAMA. 2006;296:1973–1980. doi: 10.1001/jama.296.16.1973. [DOI] [PubMed] [Google Scholar]
- Margolis PA, Cook RL, Earp JA, Lannon CM, Keyes LL, Klein JD. Factors associated with pediatricians’ participation in Medicaid in North Carolina. JAMA. 1992;267:1942–1946. [PubMed] [Google Scholar]
- McClelland S, Curran CC, Davey CS, Okuyemi KS. Intractable pediatric temporal lobe epilepsy in the United States: examination of race, age, sex, and insurance status as factors predicting receipt of resective treatment. J Neurosurg. 2007;107:469–473. doi: 10.3171/PED-07/12/469. [DOI] [PubMed] [Google Scholar]
- McClelland S, Guo H, Okuyemi KS. Racial disparities in the surgical management of intractable temporal lobe epilepsy in the United States: a population-based analysis. Arch Neurol. 2010;67:577–583. doi: 10.1001/archneurol.2010.86. [DOI] [PubMed] [Google Scholar]
- Mukherjee D, Zaidi HA, Kosztowski T, Chaichana KL, Brem H, Chang DC, Quinones-Hinojosa A. Disparities in access to neuro-oncologic care in the United States. Arch Surg. 2010;145:247–253. doi: 10.1001/archsurg.2009.288. [DOI] [PubMed] [Google Scholar]
- Navaneethan SD, Nigwekar S, Sengodan M, Anand E, Kadam S, Jeevanantham V, Grieff M, Choudhry W. Referral to nephrologists for chronic kidney disease care: is non-diabetic kidney disease ignored? Nephron Clin Pract. 2007;106:c113–8. doi: 10.1159/000102998. [DOI] [PubMed] [Google Scholar]
- Raudenbush SW, Bryk AS. Hierarchical linear models: Applications and data analysis methods. Sage Publications, Inc; 2002. [Google Scholar]
- Reid AY, St Germaine-Smith C, Liu M, Sadiq S, Quan H, Wiebe S, Faris P, Dean S, Jette N. Development and validation of a case definition for epilepsy for use with administrative health data. Epilepsy Res. 2012;102(3):173–179. doi: 10.1016/j.eplepsyres.2012.05.009. [DOI] [PubMed] [Google Scholar]
- Rosenbaum S, Sommers BD. Using medicaid to buy private health insurance - the great new experiment? N Engl J Med. 2013;369:7–9. doi: 10.1056/NEJMp1304170. [DOI] [PubMed] [Google Scholar]
- Schiltz NK, Koroukian SM, Lhatoo SD, Kaiboriboon K. Temporal trends in pre-surgical evaluations and epilepsy surgery in the U.S. from 1998 to 2009. Epilepsy Res. 2013;103:270–278. doi: 10.1016/j.eplepsyres.2012.07.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schneider A, Elias R. The Medicaid resource book. Kaiser Commission on Medicaid and the Uninsured; 2002. [Google Scholar]
- Schneider A, Strohmeyer V, Ellberger R. Medicaids eligibility for individuals with disabilities. 2000 Retrieved July 4, 2013, from http://www.kff.org/medicaid/loader.cfm?url=/commonspot/security/getfile.cfm&PageID=13323.
- Subramanian S, Chen A. Treatment patterns and survival among low-income medicaid patients with head and neck cancer. JAMA Otolaryngol Head Neck Surg. 2013;139:489–495. doi: 10.1001/jamaoto.2013.2549. [DOI] [PubMed] [Google Scholar]
- The Henry J. Kaiser Family Foundation Medicare: a primer. 2010 Retrieved July 4, 2013, from http://kaiserfamilyfoundation.files.wordpress.com/2013/01/7615-03.pdf.
- US Department of Health and Human Services Area Resource File (ARF) 2011 Retrieved July 4, 2013, from http://arf.hrsa.gov/index.htm.
- Zuvekas SH, Taliaferro GS. Pathways to access: health insurance, the health care delivery system, and racial/ethnic disparities, 1996-1999. Health Aff (Millwood) 2003;22:139–153. doi: 10.1377/hlthaff.22.2.139. [DOI] [PubMed] [Google Scholar]