Abstract
Objectives. We assessed the effectiveness of P4 for Women, a faith-based HIV intervention.
Methods. We used a 2-arm comparative effectiveness trial involving 134 African American women aged 18 to 34 years to compare the effectiveness of the Centers for Disease Control and Prevention–defined evidence-based Sisters Informing Sisters about Topics on AIDS (SISTA) HIV intervention with P4 for Women, an adapted faith-based version of SISTA. Participants were recruited from a large black church in Atlanta, Georgia, and completed assessments at baseline and follow-up.
Results. Both SISTA and P4 for Women had statistically significant effects on this study’s primary outcome—consistent condom use in the past 90 days—as well as other sexual behaviors. However, P4 for Women also had statistically significant effects on the number of weeks women were abstinent, on all psychosocial mediators, and most noteworthy, on all measures of religious social capital. Results were achieved by enhancing structural social capital through ministry participation, religious values and norms, linking trust and by reducing negative religious coping. High intervention attendance may indicate the feasibility of conducting faith-based HIV prevention research for African American women.
Conclusions. P4 for Women enhanced abstinence and safer sex practices as well as religious social capital, and was more acceptable than SISTA. Such efforts may assist faith leaders in responding to the HIV epidemic in African American women.
One little-understood social determinant of health is religion.1 Although 56% of all Americans consider religion very important in their lives, this percentage approaches 80% among African Americans.2 Of all major racial and ethnic groups in the United States, African Americans are most likely to report a formal religious affiliation. Nearly 60% of Black adults are affiliated with historically Black Protestant churches. African Americans in the South are more likely than African Americans from other regions of the United States to belong to historically Black churches. The Black church is often among the most visible, respected and credible agencies in the African American community3,4 and is acknowledged as a critical partner in improving ethical engagement of African Americans in health research.
Research has demonstrated that religious participation reduces mortality risks5–14 and improves health status6,7 and quality of life for African Americans.6,7,15–17 As early as the 1920s, Black churches were involved in outreach programs to address the health needs of community members through the provision of free clinics.18 Today, churches remain increasingly popular settings in which to conduct health research among African Americans. Scarce resources as well as conflicts between the historically Black church’s role of worship and its role in providing HIV-related services initially hindered efforts to address HIV.19 However, recently, faith-based HIV prevention research emphasizing abstinence among adolescents has emerged.20
African American women are disproportionately affected by HIV.21 Because African American women constitute more than 60% of the congregation in historically Black churches,2 serve in key positions in sustaining the churches’ social programs (ministries), and tend to seek solace from faith-based institutions, a closer examination of the church’s role in HIV prevention efforts with this population should be explored. The current effectiveness study hypothesized that P4 for Women would be more appropriate in faith-based settings compared with the widely disseminated, Centers for Disease Control and Prevention (CDC)-defined, evidence-based HIV intervention for African American women called Sisters Informing Sisters about Topics on AIDS (SISTA),22 which is often delivered in public health venues. P4 for Women was created as a faith-based adaptation of SISTA23,24 delivered at a historically Black church in the Atlanta, Georgia, metropolitan area.
METHODS
A large African American church, with whom the study investigators have maintained an ongoing relationship for more than 7 years, served as the study site. This church has a congregation of 25 000 members, 98% of whom are African American. A 10-member Church Advisory Board (CAB) was established, which included the Director of Pastoral Care Services, the Co-Directors of the Health Services Ministry, and the Director of the College and Singles Ministry as well as members of the Women’s Ministry. The CAB members were given the authority to modify the study to avoid risks to participants, risks to nonparticipating members of the church, as well as risks that could be perceived as undermining the church’s moral beliefs. CAB members were involved in selecting recruitment sources and disseminating recruitment materials. Recruitment sources included pulpit and video announcements, advertisements on the church Web site, on-site study recruiters, posters distributed at church conferences (i.e., women’s conferences), and word of mouth. Aside from the CAB members and Emory University study staff, nobody at the church was aware of the study eligibility criteria.
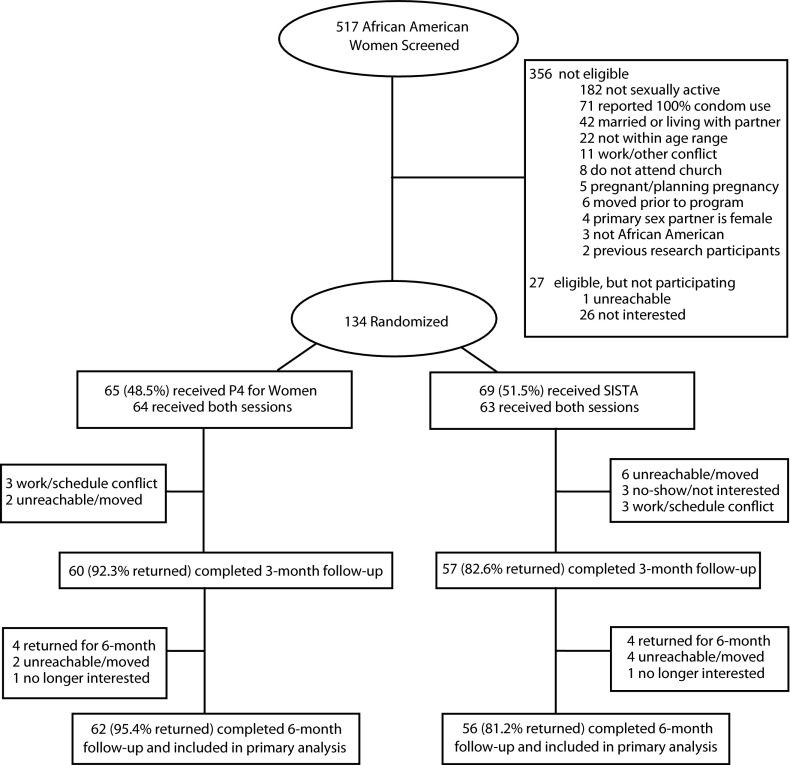
From January 2010 through August 2011, recruiters screened a convenience sample of 517 women from the faith-based institution. Of these, 161 (31.1%) met the study eligibility criteria of being an African American woman aged 18 to 34 years, reporting unprotected vaginal intercourse with a male partner during the past 180 days, being unmarried and not living with a male sexual partner, not being pregnant or planning pregnancy, attending church services at a Black church, and providing written informed consent (Figure 1). Of the 161 eligible women, 134 (83.2%) consented to participate and were randomized to study conditions. At each visit, participants received a $50 monetary incentive for completing assessments and to compensate them for time.
FIGURE 1—
P4 for Women participant allocation.
Note. Sisters Informing Sisters about Topics on AIDS (SISTA) is a Centers for Disease control and Prevention, evidence-based HIV intervention for African American women. P4 is a faith-based adaptation of SISTA. Totals may not add up exactly because of rounding.
Design
A 2-arm comparative effectiveness trial25 compared the relative effectiveness of the adapted faith-based HIV intervention, P4 for Women, with the original SISTA HIV intervention. Participants were randomly assigned, using a random-numbers table, to receive either the two 3-hour SISTA HIV intervention sessions or the two 3-hour P4 for Women sessions. The CAB also believed that providing HIV testing to all women was critical; thus, HIV testing was provided to all participants.
Theory
P4 for Women sought to enhance religious social capital to improve HIV prevention outcomes for women. Stark and Finke conceptualized religious capital as the degree of mastery of, and attachment to, a particular religious culture.26 Other scholars have approached religious engagement as a factor that contributes to social capital. We apply religious social capital as defined by Maselko et al.: those social resources available to individuals and groups through social connections within a religious community.1 The social resources within a religious community include shared values, levels of trust among members, as well as levels of socializing that are specific to that particular religious group. Religious social capital might be an especially significant social determinant of health precisely because the ties within an average religious community are quite strong. Additionally, religious communities tend to be rather homogeneous in terms of health-related beliefs and acceptable behavior, and individuals are more receptive to those unified ideals. This cohesiveness could have important salubrious effects. Moreover, in lower socioeconomic neighborhoods where other sources of social capital are less available, religious social capital may be a more accessible form of social capital.1
The act of communing to worship is an important form of social capital in Black churches. Moreover, compared with White and African American adults, African American women are among the most religious group, and they rely on God the most during crises.27 Faith-based public health initiatives designed to enhance religious social capital may have their greatest impact on African American women residing in lower resource communities. Thus, the current study sought to develop a faith-based HIV-prevention intervention utilizing religious social capital to foster acceptable behaviors such as abstinence28 and other safer sex practices.29
Intervention Methods
Initial intervention efforts occurred at the institutional level and included forming the CAB, and collaborating with the church leadership to obtain their support for integrating P4 for Women into existing church venues.30 Facilitating the CAB’s decision for this integration was SISTA’s established efficacy with sexually active African American women (SISTA is a tier 1, CDC-defined, evidence-based HIV intervention), its successful dissemination across the United States, and the CAB’s commitment to prioritize HIV among women as an issue within their faith institution. Subsequently, based on the CAB’s recommendations, adaptations were made to the SISTA intervention to enhance its relevance for faith institutions and create P4 for Women.23,24 Key adaptations included having a greater focus on sexual abstinence and religious social capital (Table 1). In both study conditions, the CAB eliminated condom demonstrations and proactive condom distribution efforts; so, although condom-related activities were present in the original SISTA intervention, condoms were not accepted in the church.
TABLE 1—
Sisters Informing Sisters About Topics on AIDS (SISTA) and P4 for Women Intervention Content
| Discussion/Acitivities |
||
| Session Content | SISTA | P4 for Women |
| Session 1: ethnic and gender pride | The joys and challenges of being an African American woman | The values of being an African American Christian woman |
| Role models and how they positively influence our lives | The role Christianity has played in the African American community | |
| Reviewing HIV risk reduction strategies | Promoting sexual abstinence and safer sex | |
| Personal values clarification | Enhancing norms supportive of sexual abstinence | |
| Resisting sexualized images of African American women in popular music | ||
| Session 2: enhancing coping and skills | Enhancing norms supportive of HIV risk reduction | Exploring the use of religious coping (i.e., participation in church ministries and religious activities, talking to peers and leaders within church) to overcome sexual temptations |
| Building sexual negotiation, condom use, and partner selection | Building sexual negotiation, condom use, and partner selection | |
| Exploring risk levels involved in behaviors | Encouraging HIV and STI testing | |
Note. STI = sexually transmitted infection. SISTA is a Centers for Disease Control and Prevention, evidence-based HIV intervention for African American women. P4 for Women is a faith-based adaptation of SISTA.
Furthermore, while 2 African American females cofacilitated the interventions, at least 1 of the facilitators in P4 for Women was a member of the church where the intervention was implemented. Facilitators from the church received extensive training by study staff to enhance the church’s role as a research partner.
Dissemination and Data Collection
After the research funding expired, Emory staff held a 3-day training to facilitate dissemination of P4 for Women results with 28 key leaders from faith communities across Atlanta who had been identified by the CAB. The dissemination focused on presenting results in a way that would not implicate the church as a whole but rather to the subgroup of women who were eligible, so as to eliminate any social harm to nonparticipants as well as protect the identity of study participants.
Baseline surveys were administered immediately prior to random assignment; each assessment lasted approximately 45 minutes. Data to assess study efficacy were collected at baseline and at 3- and 6-month postintervention follow-up visits, using audio computer-assisted self-interviewing (ACASI). Data collectors were blinded to the women’s study condition.
Outcomes
Consistent condom use was selected as the primary outcome for the study because of its demonstrated effectiveness for reducing sexually transmitted HIV infections.29 Consistent condom use was defined as self-reported condom use during every episode of vaginal intercourse in the 90 days prior to the 3- and 6-month follow-up visits.
Other behavioral outcomes included proportion of participants who reported never using condoms, condom use at last vaginal intercourse, and proportion of condom-protected vaginal sex acts. The ACASI also assessed whether participants remained abstinent since the last assessment (3 months ago), and if so, the length of time participants had been abstinent from vaginal intercourse.
Psychosocial constructs were assessed, including HIV knowledge, which was measured using a 9-item scale, with higher scores indicating greater knowledge about HIV.31 Perceived barriers to condom use were measured with an 8-item scale that assessed attitudes which can impede participants’ ability to effectively use condoms,32 with higher scores indicating more perceived barriers (α = 0.85). Participants’ self-efficacy for negotiating safe sex with their male partners was measured using a 7-item scale (α = 0.84), with higher scores indicating greater comfort level with negotiating safer sex options.33 Condom use self-efficacy was measured by applying a 9-item scale that assessed participants’ confidence in their ability to properly use condoms, with higher scores indicating greater self-efficacy (α = 0.90).34
Religious Social Capital
Four domains captured the assessment of religious social capital.1 Structural social capital (α = 0.85) was assessed by 6 items and tapped into participants’ level of religious engagement with their faith institution. Religious engagement was represented by the number of ministries (out of a total of 6) women were engaged with at the church. Participants were asked how often they participated in services offered by the Women’s ministry (i.e., women’s conferences, women-only services); the Health ministry (i.e., health fairs); the Counseling ministry (i.e., for consoling needs); the Christians singles’ ministry (i.e., monthly events for single women); College ministry (i.e., campus outreach activities); or the Women of Wisdom Ministry (i.e., a ministry where women take classes to learn how to mentor other women). We also assessed structural social capital by asking participants how active they consider themselves in their church.
We assessed religious values and norms regarding secondary abstinence by asking participants if the doctrines or belief systems of their church influence the likelihood of their avoiding situations that might lead to having sexual intercourse. Additionally, religious values and norms regarding safer sex were assessed by asking participants if their decision to use condoms was based on their religious beliefs.
Linking trust refers to the level of trust participants have with their religious leaders. Linking trust was assessed by asking participants, “In times of need, how often do you talk with a religious or spiritual leader at church?”
Religious coping was assessed using the 14-item Religious Coping (RCOPE) scale.35 RCOPE includes a positive religious coping (PRC) subscale and a negative religious coping (NRC) subscale. PRC (α = 0.87) taps into having a secure relationship with a caring God, and the NRC (α = 0.88) is characterized by signs of spiritual tension, conflict and struggle with God and others.
Analysis
We performed analyses only on prespecified hypotheses using an intention-to-treat protocol in which participants were analyzed in their original assigned treatment conditions irrespective of the number of treatment sessions attended.36 To determine the differences between study conditions, we used the t-test for continuous variables and χ2 analysis for categorical variables.37 The study had 78% power to detect a medium-effect size and a 2-sided type I error rate of 5%.38 Sociodemographic or partner characteristics that approached significance (P ≤ .1) were included as covariates.
The effects of SISTA and P4 for Women were assessed for the entire 6-month period. We used the t-test and χ2 analysis to assess unadjusted differences in means and proportions, respectively, between the baseline and 6-month follow-up for each condition. To obtain adjusted mean differences or odds ratios over the 6-month period, we constructed linear and logistic generalized estimating equation (GEE) regression models to control for repeated within-subject measurements. Each model included sociodemographic variables as covariates39 as well as 2 dummy variables representing an interaction between treatment and time period. Fitted GEE parameters can be interpreted as adjusted odds ratios in logistic models and adjusted mean differences in linear models.
We used noninferiority testing as our intention was not to prove that we had developed a treatment superior to the well-established SISTA program, but that P4 for Women was not inferior to SISTA. To assess whether the effects of P4 for Women were noninferior to the effects of SISTA, following each GEE, we performed a one-sample t-test to test a null-hypothesis that the lower bound of 95% confidence interval (CI) around the difference between the effects of P4 for Women and SISTA lies below the preselected margin.40 Rejecting the null hypothesis means that the effects of P4 for Women are noninferior to SISTA. We set the margin at 20% of standard errors for adjusted mean differences or adjusted odds ratios for a SISTA small standardized effect.
RESULTS
Of the 134 randomized participants, 65 (49%) were assigned to P4 for Women and 69 (51%) were assigned to SISTA. Differences between participants in the study conditions on sociodemographic, behavioral, psychosocial, and religious variables were assessed at baseline. With the exception of condom-use self-efficacy, these analyses suggest that both interventions were comparable in terms of participants’ characteristics. On average, women in our sample were 24.57 years old (SD = 4.09), and 49.3% (n = 66) received public assistance. In the 6 months prior to the study, women had a mean of 2.9 sexual partners (SD = 5.33), and at baseline, 61.2% (n = 82) of women had a main sexual partner, 78.4% (n = 105) of women reported not using a condom during their last sex act, and 29.1% (n = 39) reported no condom use in the 6 months prior to the study. Finally, 73% (n = 98) of participants were Baptist, 77.6% (n = 104) paid tithes and 41% (n = 55) were involved in church ministries.
Of the 134 participants enrolled at baseline, P4 for Women and SISTA retained, respectively, 60 (92%) and 57 (83%) of participants at 3-month follow-up. At 6-month follow-up, 62 (95%) were retained in P4 for Women and 56 (81%) in SISTA. Those women who were lost to follow-up did not show any statistically significant differences in their demographic characteristics. Also, there were no statistically significant differences in loss to follow-up among the 2 study conditions (P = .067).
The adjusted results in Table 2 show that, over the 6-month follow-up period, as compared with baseline, participants in P4 for Women were 3.6 times as likely to report using condoms consistently during the past 90 days (P = .004), 2.3 times as likely to report using a condom at last sex act (P = .003), and 2.4 times as likely to report being abstinent for more than 30 days (P < .001). Moreover, the tests of noninferiority suggest that the effects of P4 for Women on the above outcomes were not inferior to the effects of SISTA. Thus, the noninferiority test for condom use at last sex showed that we can reject the null-hypothesis that lower bound of 95% CI (–0.75, 0.41) for treatment difference between P4 for Women and SISTA lies below the noninferiority margin of −1.20 (P < .001), which leads to the conclusion of noninferiority.
TABLE 2—
Effects of Sisters Informing Sisters About Topics on AIDS (SISTA) and P4 for Women Interventions on Dichotomous Measures of Sexual Behavior: Atlanta, GA, January 2010–August 2011
| SISTAa |
P4 for Womena |
Noninferiority Testing, Baseline to 6 Months (SISTA vs P4 for Women) |
|||||
| Variable | OR (95% CI) | P | OR (95% CI) | P | Treatment Difference (95% CI) | Noninferiority Margin | P |
| Consistent condom use, past 90 d | 5.80 (2.67, 12.62) | < .001 | 3.57 (1.52, 8.39) | .004 | −0.49 (−1.31, 0.33) | −1.40 | .015 |
| Condom use at last sex | 2.68 (1.45, 4.95) | .002 | 2.26 (1.32, 3.88) | .003 | −0.17 (−0.75, 0.41) | −1.20 | < .001 |
| Never condom use in past 30 d | 0.61 (0.33, 1.15) | .126 | 0.55 (0.31, 0.97) | .039 | −0.11 (−0.71, 0.49) | −1.03 | .001 |
| % abstinent for > 30 d | 2.73 (1.67 4.49) | < .001 | 2.40 (1.50, 3.85) | < .001 | −0.13 (−0.61, 0.36) | −0.97 | < .001 |
Note. CI = confidence interval; OR = odds ratio. SISTA is a Centers for Disease Control and Prevention, evidence-based HIV intervention for African American women. P4 for Women is a faith-based adaptation of SISTA.
Generalized estimating equation models from baseline to 6 month follow-up, adjusted by the following covariates: participant’s age, living alone, having risky sexual partner.
Over 6-month follow-up assessment, as compared with baseline, participants in SISTA reported increased mean percent condom use during the past 90 days (mean difference = 16.34; P = .001) and decreased mean number of current male partners (mean difference = −0.62; P = .044; Tables 2 and 3). However, participants in P4 for Women were 45% less likely to report never using condoms in the past 30 days during the 6-month follow-up than at baseline (adjusted odds ratio = 0.55; P = .039); they also showed an increase in the mean number of weeks abstinent (mean difference = 7.37; P = .002).
TABLE 3—
Effects of Sisters Informing Sisters About Topics on AIDS (SISTA) and P4 for Women Interventions on Continuous Measures of Sexual Behavior, Psychosocial Mediators, and Religious Practices: Atlanta, GA, January 2010–August 2011
| Adjusted GEE Models,a Baseline to 6 Months |
Noninferiority Testing, Baseline to 6 Months |
|||||||
| Variables | Mean Difference (95% CI) | P | Mean Difference (95% CI) | P | Treatment Difference (95% CI) | Noninferiority Margin |
P |
|
| Measures of sexual behavior | ||||||||
| Condom use, past 90 d, % | 16.34 (6.36, 26.31) | .001 | 8.72 (−0.58, 18.02) | .066 | −7.62 (−17.29, 2.06) | −17.92 | .019 | |
| Current male partners, no. | −0.62 (−1.23, −0.02) | .044 | −0.32 (−0.89, 0.24) | .259 | 0.30 (−0.29, 0.88) | −1.18 | < .001 | |
| Length of time abstinent, wk | 5.68 (1.41, 9.95) | .009 | 7.37 (2.67, 12.06) | .002 | 1.68 (−2.84, 6.21) | −4.95 | .002 | |
| Psychosocial mediators | ||||||||
| Condom use barriers | −1.70 (−2.70, −0.69) | .001 | −1.67 (−2.55, −0.79) | < .001 | 0.02 (−0.92, 0.97) | −1.96 | < .001 | |
| Condom negotiation self-efficacy | 2.84 (1.75, 3.92) | < .001 | 2.36 (1.19, 3.53) | < .001 | −0.48 (−1.61, 0.65) | −2.12 | .002 | |
| Condom responsibility | 0.69 (0.26, 1.13) | .002 | 0.43 (0.13, 0.74) | .006 | −0.26 (−0.63, 0.11) | −0.85 | .001 | |
| Condom use self-efficacy | 3.59 (2.28 4.90) | < .001 | 3.87 (2.27, 5.46) | < .001 | 0.28 (−1.18, 1.74) | −2.57 | < .001 | |
| STI testing barriers | 0.86 (0.27, 1.45) | .004 | 0.72 (0.10, 1.35) | .022 | −0.13 (−0.74, 0.47) | −1.15 | .001 | |
| STI knowledge | 0.17 (−0.15, 0.49) | .301 | 0.48 (0.23, 0.72) | < .001 | 0.31 (0.02, 0.59) | −0.63 | < .001 | |
| Perception of neighborhood violence | −0.18 (−0.55, 0.19) | .347 | −0.50 (−0.0.81, −0.18) | .002 | −0.32 (−0.66, 0.03) | −0.73 | .009 | |
| Structural social capital | ||||||||
| Frequency of participation in | ||||||||
| Women’s ministry | 0.19 (−0.01, 0.38) | .059 | 0.18 (0.03, 034) | .018 | −0.002 (−0.18, 0.17) | −0.38 | < .001 | |
| Health ministry | 0.19 (0.01, 0.36) | .034 | 0.23 (0.08, 0.38) | .004 | 0.04 (−0.12, 0.21) | −0.34 | < .001 | |
| Counseling ministry | 0.08 (−0.07, 0.23) | .287 | 0.16 (0.04, 0.28) | .007 | 0.08 (−0.05, 0.21) | −0.29 | < .001 | |
| Singles’ ministry | 0.17 (−0.01, 0.34) | .056 | 0.19 (0.06, 0.33) | .006 | 0.02 (−0.13, 0.18) | −0.34 | < .001 | |
| WOW group | 0.20 (0.06, 0.34) | .004 | 0.16 (0.04, 0.28) | .01 | −0.05 (−0.18, 0.09) | −0.27 | < .001 | |
| Overall ministries participation | 0.89 (0.14, 1.65) | .02 | 1.06 (0.45, 1.66) | .001 | 0.16 (−0.52, 0.84) | −1.47 | < .001 | |
| Level of activity in church | 0.16 (0.003, 0.31) | .046 | 0.31 (0.11, 0.52) | .002 | 0.16 (−0.02, 0.34) | −0.3 | < .001 | |
| Religious values and norms | ||||||||
| Church influence on sex avoidance | 0.10 (−0.04, 0.24) | .143 | 0.10 (−0.02, 0.23) | .095 | 0.001 (−0.13, 0.13) | −0.27 | < .001 | |
| Influence of faith on condom use | 0.22 (0.04, 0.40) | .017 | 0.20 (0.01, 0.38) | .04 | −0.02 (−0.21, 0.16) | −0.35 | < .001 | |
| Frequency of fasting | 0.13 (−0.02, 0.27) | .08 | 0.19 (0.04, 0.33) | .012 | 0.06 (−0.09, 0.20) | −0.28 | < .001 | |
| Religious coping | ||||||||
| Frequency–wondered whether: | ||||||||
| Abandoned by God | −0.28 (−0.50, −0.07) | .009 | −0.29 (−0.53, −0.06) | .013 | −0.01 (−0.23, 0.21) | −0.42 | < .001 | |
| Punished by God | −0.26 (−0.47, −0.05) | .015 | −0.23 (−0.44, −0.02) | .029 | 0.03 (−0.18, 0.24) | −0.41 | < .001 | |
| Did something to be punished by God | −0.28 (−0.48, −0.08) | .006 | −0.30 (−0.51, −0.08) | .007 | −0.02 (−0.23, 0.19) | −0.39 | < .001 | |
| Loved by God | −0.22 (−0.42, −0.02) | .027 | −0.15 (−0.33, 0.03) | .106 | 0.07 (−0.12, 0.26) | −0.38 | < .001 | |
| Devil made this happen | −0.20 (−0.39, −0.02) | .026 | −0.06 (−0.25, 0.13) | .506 | 0.14 (−0.05, 0.33) | −0.36 | < .001 | |
| Positive religious coping | −0.15 (−0.31, 0.002) | .054 | −0.06 (−0.24, 0.12) | .509 | 0.09 (−0.08, 0.26) | −0.3 | < .001 | |
| Negative religious coping | −1.35 (−2.22, −0.48) | .002 | −1.13 (−2.08, −0.17) | .021 | 0.22 (−0.70, 1.14) | −1.7 | < .001 | |
| Linking trust | ||||||||
| Frequency of communication with religious leader | 0.11 (−0.07, 0.28) | .243 | 0.22 (0.06, 0.37) | .006 | 0.11 (−0.06, 0.28) | 0.09 | < .001 | |
Note. CI = confidence interval; GEE = generalized estimating equations; STI = sexually transmitted infection; WOW = Women of Wisdom. Psychosocial mediators and religious variables are based on scale scores. SISTA is a Centers for Disease Control and Prevention, evidence-based HIV intervention for African American women. P4 for Women is a faith-based adaptation of SISTA.
Models adjusted by the following covariates: participant’s age, living alone, having risky sexual partner.
Over the 6-month period, participants in P4 for Women showed a significant increase in their condom-negotiation self-efficacy score (mean difference = 2.36; P < .001) and condom-use self-efficacy (mean difference = 3.87; P < .001), and a significant decrease in perceived condom use barriers score (mean difference = −1.67; P < .001; Table 3). Furthermore, the test for noninferiority indicates that the benefits enjoyed by persons in the P4 for Women were not inferior to the benefits enjoyed by persons in SISTA.
The adjusted results show that P4 for Women participants had significant increases from baseline over the 6-month study period on overall level of activity in the church (mean difference = 0.31; P = .002; Table 3). Out of measures of religious values and norms, both interventions had statistically significant effects on influence of faith on condom use, but only P4 for Women showed an increase over the follow-up period in faith influence on frequency of fasting (mean difference = 0.19; P = .012). Neither intervention had statistically significant effects on positive religious coping; however, both SISTA and P4 for Women significantly reduced negative religious coping over the 6-month period as compared with baseline, with adjusted mean differences in scores of, respectively, –1.35 (P = .002) and –1.13 (P = .021). Lastly, only P4 for Women had a statistically significant positive effect on the linking trust construct, namely increased frequency of communication with a religious leader. Importantly, the tests for noninferiority indicated that for all religious variables considered, the effects of P4 for Women were not inferior to the effects of SISTA.
DISCUSSION
Our study highlights how a faith-based intervention designed to enhance a prosocial determinant of health, religious social capital, can reduce African American women’s risk of HIV. This successful adaptation represents the first faith-based adaptation of SISTA. Numerous scientists have called upon the need for a faith-based HIV intervention for African American women.41–44 Both SISTA and P4 for Women had statistically significant effects on this study’s primary outcome—consistent condom use in the past 90 days—as well as other sexual behaviors. However, P4 for Women also had statistically significant effects on the number of weeks women were abstinent, on all psychosocial mediators, and most noteworthy, on all measures of religious social capital. Observed results were achieved by enhancing structural social capital through ministry participation, religious values and norms, linking trust and by reducing negative religious coping. Moreover, the greater compatibility of P4 for Women with participants’ religious values may have resulted in there being more P4 for Women participants available at both the 3- and 6- month follow-ups than SISTA participants. Additionally, high intervention attendance may be indicative of the feasibility of conducting faith-based HIV prevention research for African American women. Compared with traditional HIV prevention efforts for African American women, which are often delivered in clinical venues, faith-based HIV-prevention interventions may be more appropriate because African American women at risk for HIV often attend and engage in faith-based services. Furthermore, unlike SISTA participants, investment in religious social capital among P4 for Women participants may have reduced their perception of their neighborhood as violent.
The creation of a CAB that assisted in the fair selection of participants, reviewed informed consent protocols, assisted in creating P4 for Women and dissemination efforts, and facilitated minimizing risks associated with the implementation of an HIV-prevention study within a faith-based setting.30
Limitations
Limitations include small sample size and a relatively short follow-up period. While ACASI was used to enhance reliability of self-reports, another limitation is that participants’ responses regarding abstinence may have been influenced by social desirability, given the strong cultural value that faith institutions place on abstinence. Moreover, the study results may not be generalizable to unmarried women living with a male partner. Owing to the substantial variation among churches in their role, their structure in implementing religious doctrines, and in individual agency, the results are not applicable to all Black churches. Future trials should be conducted with African American women seeking worship at Baptist Churches of different sizes and in different geographical regions, and with Black churches representing other denominations. The study has numerous strengths which include collaboration of a university with a faith-based institution to develop a comparative effectiveness trial evaluating the impact of a structural level HIV intervention on a social determinant of health, religious social class, as well as abstinence and other safer sex practices.
Conclusions
Given the Black church’s historical involvement in advocacy for African Americans, the social justice issues posed by HIV among African Americans, and the presence of 21 000 Black Churches across the United States, the National Association for the Advancement of Colored People (NAACP) has encouraged faith leaders to engage in HIV advocacy.45 The NAACP’s social justice imperative for Black churches states that 39 million African Americans live in the United States and 53% of African Americans attend church weekly. This equates to the power of 20 million to end the HIV epidemic in this population. Addressing issues of acceptability, feasibility and, dissemination of evidence-based HIV-prevention efforts for faith institutions may play a key role in helping faith leaders respond to the HIV epidemic in African American women.
Acknowledgments
Funding for this study was provided by the Centers for Disease Control and Prevention (CDC; grant 5R18PS001157), the Center for Contextual Genetics and Prevention (P30 DA027827), the Emory CFAR (P30 AI050409), and the Women’s Interagency HIV Study (WIHS) U01AI103408.
We would like to acknowledge all of those who assisted us, including our health educators, Tiffiany M. Cummings Aholou, PhD, MPH, Tanisha S. Grimes, PhD, MPH, Tiffany A. Pennick, MPH, and Ayesha McAdams-Mahmoud, MPH; our project recruiters, Estee N. Dillard, Alicia N. Wigfall, and Cynthia R. Reid; our data collection assistants, Christina M. White, MPH, Sarah M. Dickey, MPH, and Christina L. Lee; our Church Advisory Board, Elder Wallace Prude, Elder Alice Evans, Elder Judy Taylor, Jean Henry, Mary A. Smith, Elder Lori Allen, Elder Jaquatte Williams, Elder Roberto Woods, Ashlei Porter, Christine Chavis, Lisa Edwards, Rosemary Nix, Christine Chavis, and Zenobia Storey. Additionally, we appreciate all of the support with HIV testing from the staff at AID Atlanta.
Note. The findings and conclusions in this report are those of the authors and do not necessarily represent the views of the CDC.
Human Participant Protection
The Emory University institutional review board (IRB; 00014227) approved the study protocol. Prior to receipt of IRB approval from Emory University, the Church Advisory Board members reviewed the IRB protocols and procedures and completed an IRB Authorization Agreement, consenting to be governed by Emory’s IRB. The informed consent explicitly stated that involvement in the study would not compromise any of the services that participants receive at the faith institution. Moreover, the consent stated that research participants’ involvement in or data from any aspect of the study would remain confidential.
References
- 1.Maselko J, Hughes C, Cheney R. Religious social capital: its measurement and utility in the study of the social determinants of health. Soc Sci Med. 2011;73(5):759–767. doi: 10.1016/j.socscimed.2011.06.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Pew Forum on Religion & Public Life. US religious landscape survey. 2008. Available at: http://religions.pewforum.org/pdf/report-religious-landscape-study-full.pdf. Accessed October 10, 2012.
- 3.Taylor RJ, Chatters L, Levin J. Religion in the Lives of African Americans: Social, Psychological, and Health Perspectives. Thousand Oaks, CA: Sage; 2004. [Google Scholar]
- 4.Corbie-Smith G, Ammerman AS, Katz ML et al. Trust, benefit, satisfaction, and burden: a randomized controlled trial to reduce cancer risk through African-American churches. J Gen Intern Med. 2003;18(7):531–541. doi: 10.1046/j.1525-1497.2003.21061.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Hummer RA, Rogers RG, Nam CB, Ellison CG. Religious involvement and US adult mortality. Demography. 1999;36:273–285. [PubMed] [Google Scholar]
- 6.Livingston IL, Levine DM, Moore RD. Social integration and black intraracial variation in blood pressure. Ethn Dis. 1991;1:135–149. [PubMed] [Google Scholar]
- 7.Steffen PR, Hinderliter AL, Blumenthal JA, Sherwood A. Religious coping, ethnicity, and ambulatory blood pressure. Psychosom Med. 2001;63:523–530. doi: 10.1097/00006842-200107000-00002. [DOI] [PubMed] [Google Scholar]
- 8.Strawbridge WJ, Cohen RD, Shema SJ, Kaplan GA. Frequent attendance at religious services and mortality over 28 years. Am J Public Health. 1997;87:957–961. doi: 10.2105/ajph.87.6.957. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Strawbridge WJ, Shema SJ, Cohen RD, Roberts RE, Kaplan GA. Religiosity buffers effects of some stressors on depression but exacerbates others. J Gerontol B Psychol Sci Soc Sci. 1998;53(3):S118–S126. doi: 10.1093/geronb/53b.3.s118. [DOI] [PubMed] [Google Scholar]
- 10.Strawbridge WJ, Cohen RD, Shema SJ. Comparative strength of association between religious attendance and survival. Int J Psychiatry Med. 2000;30:299–308. doi: 10.2190/ECB2-0Q3M-333C-GK62. [DOI] [PubMed] [Google Scholar]
- 11.Strawbridge WJ, Shema SJ, Cohen RD, Kaplan GA. Religious attendance increases survival by improving and maintaining good health behaviors, mental health, and social relationships. Ann Behav Med. 2001;23:68–74. doi: 10.1207/s15324796abm2301_10. [DOI] [PubMed] [Google Scholar]
- 12.Koenig HG. Religion and medicine I: historical background and reasons for separation. Int J Psychiatry Med. 2000;30(4):385–398. doi: 10.2190/2RWB-3AE1-M1E5-TVHK. [DOI] [PubMed] [Google Scholar]
- 13.Musgrave CF, Allen CE, Allen GJ. Spirituality and health for women of color. Am J Public Health. 2002;92:557–560. doi: 10.2105/ajph.92.4.557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Helm HM, Hays JC, Flint EP, Koenig HG, Blazer DG. Does private religious activity prolong survival? A six-year follow-up study of 3,851 older adults. J Gerontol A Biol Sci Med Sci. 2000;55:M400–M405. doi: 10.1093/gerona/55.7.m400. [DOI] [PubMed] [Google Scholar]
- 15.Pardini DA, Plante TG, Sherman A, Stump JE. Religious faith and spirituality in substance abuse recovery: determining the mental health benefits. J Subst Abuse Treat. 2000;19:347–354. doi: 10.1016/s0740-5472(00)00125-2. [DOI] [PubMed] [Google Scholar]
- 16.Levin JS, Chatters LM, Taylor RJ. Religious effects on health status and life satisfaction among Black Americans. J Gerontol B Psychol Sci Soc Sci. 1995;50(3):S154–S163. doi: 10.1093/geronb/50b.3.s154. [DOI] [PubMed] [Google Scholar]
- 17.Bourjolly JN. Differences in religiousness among Black and White women with breast cancer. Soc Work Health Care. 1998;28:21–39. doi: 10.1300/J010v28n01_02. [DOI] [PubMed] [Google Scholar]
- 18.Campbell MK, Hudson MA, Resnicow K, Blakeney N, Paxton A, Baskin M. Church-based health promotion interventions: evidence and lessons learned. Annu Rev Public Health. 2007;28:213–234. doi: 10.1146/annurev.publhealth.28.021406.144016. [DOI] [PubMed] [Google Scholar]
- 19.Cunningham SD, Kerrigan DL, McNeely CA, Ellen JM. The role of structure versus individual agency in churches’ responses to HIV/AIDS: a case study of Baltimore City churches. J Relig Health. 2011;50(2):407–421. doi: 10.1007/s10943-009-9281-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Coleman JD, Lindley LL, Annang L, Saunders RP, Gaddist B. Development of a framework for HIV/AIDS prevention programs in African American churches. AIDS Patient Care STDS. 2012;26(2):116–124. doi: 10.1089/apc.2011.0163. [DOI] [PubMed] [Google Scholar]
- 21.CDC. HIV surveillance—United States, 1981-2008. MMWR Morb Mortal Wkly Rep. 2011;60:689–693. [PubMed] [Google Scholar]
- 22.DiClemente RJ, Wingood GM. A randomized controlled trial of an HIV sexual risk-reduction intervention for young African American women. JAMA. 1995;274(16):1271–1276. [PubMed] [Google Scholar]
- 23.Wingood GM, Simpson-Robinson L, Braxton ND, Raiford JL. Design of a faith-based HIV intervention: successful collaboration between a university and a church. Health Promot Pract. 2011;12(6):823–831. doi: 10.1177/1524839910372039. [DOI] [PubMed] [Google Scholar]
- 24.Wingood GM, DiClemente RJ. The ADAPT-ITT model: a novel method of adapting evidence-based HIV Interventions. J Acquir Immune Defic Syndr. 2008;47(Suppl 1):S40–S46. doi: 10.1097/QAI.0b013e3181605df1. [DOI] [PubMed] [Google Scholar]
- 25.Methodology Committee of the Patient-Centered Outcomes Research Institute (PCORI) Methodological standards and patient-centeredness in comparative effectiveness research. The PCORI perspective. JAMA. 2012;307(15):1636–1640. doi: 10.1001/jama.2012.466. [DOI] [PubMed] [Google Scholar]
- 26.Stark R, Finke R. Acts of Faith: Explaining the Human Side of Religion. Berkely, CA: University of California Press; 2000. [Google Scholar]
- 27. Washington Post-Kaiser Family Foundation poll of black women in America. Washington Post. January 23, 2012. Available at: http://www.washingtonpost.com/wp-srv/special/nation/black-women-in-america. Accessed October 12, 2013.
- 28.Santelli J, Ott MA, Lyon M, Rogers J, Summers D, Schleifer R. Abstinence and abstinence-only education: a review of US policies and programs. J Adolesc Health. 2006;38(1):72–81. doi: 10.1016/j.jadohealth.2005.10.006. [DOI] [PubMed] [Google Scholar]
- 29.de Vincenzi I. A longitudinal study of human immunodeficiency virus transmission by heterosexual partners. N Engl J Med. 1994;331:341–346. doi: 10.1056/NEJM199408113310601. [DOI] [PubMed] [Google Scholar]
- 30.Ross LF, Loup A, Nelson RM et al. Nine key functions for a human subjects protection program for community-engaged research: points to consider. J Empir Res Hum Res Ethics. 2010;5(1):33–47. doi: 10.1525/jer.2010.5.1.33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Sikkema K, Kelly J, Winett R et al. Outcomes of a randomized community-level HIV prevention intervention for women living in 18 low-income housing developments. Am J Public Health. 2000;90(1):57–63. doi: 10.2105/ajph.90.1.57. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.St Lawrence JS, Chapdelaine AP, Devieux JG, O’Bannon RE, 3rd, Brasfield TL, Eldridge GD. Measuring perceived barriers to condom use: psychometric evaluation of the condom barriers scale. Assessment. 1999;6(4):391–404. doi: 10.1177/107319119900600409. [DOI] [PubMed] [Google Scholar]
- 33.Marín BV, Gomez CA, Tschann JM, Gregorich SE. Self-efficacy to use condoms in unmarried Latino adults. Am J Community Psychol. 1998;26(1):53–71. doi: 10.1023/a:1021882107615. [DOI] [PubMed] [Google Scholar]
- 34.Marín BV, Gomez CA, Tschann JM, Gregorich SE. Condom use in unmarried Latino men: a test of cultural constructs. Health Psychol. 1997;16:458–467. doi: 10.1037//0278-6133.16.5.458. [DOI] [PubMed] [Google Scholar]
- 35.Pargament K, Feuille M, Burdzy D. The Brief RCOPE: current psychometic status of a short measure of religious coping. Religions. 2011;2:51–76. [Google Scholar]
- 36.Pocock SJ. Clinical Trials: A Practical Approach. New York, NY: John Wiley & Sons; 1993. [Google Scholar]
- 37.Fleiss JL, Levin B, Paik MC. Statistical Methods for Rates and Proportions. 3rd ed. New York, NY: Wiley & Sons; 1989. [Google Scholar]
- 38.Cohen J. A power primer. Psychol Bull. 1992;112(1):155–159. doi: 10.1037//0033-2909.112.1.155. [DOI] [PubMed] [Google Scholar]
- 39.Hardin JW, Hilbe JM. Generalized Estimating Equations. New York, NY: Chapman & Hall/CRC; 2003. [Google Scholar]
- 40.Schumi J, Wittes JT. Through the looking glass: understanding non-inferiority. Trials. 2011;12:106. doi: 10.1186/1745-6215-12-106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Jarama SL, Belgrave FZ, Bradford J, Young M, Honnold JA. Family, cultural and gender role aspects in the context of HIV risk among African American women of unidentified HIV status: an exploratory qualitative study. AIDS Care. 2007;19(3):307–317. doi: 10.1080/09540120600790285. [DOI] [PubMed] [Google Scholar]
- 42.McKoy JN, Petersen R. Reducing African-American women’s sexual risk: can churches play a role? J Natl Med Assoc. 2006;98(7):1151–1159. [PMC free article] [PubMed] [Google Scholar]
- 43.Smith J, Simmons E, Mayer KH. HIV/AIDS and the Black Church: what are the barriers to prevention services? J Natl Med Assoc. 2005;97(12):1682–1685. [PMC free article] [PubMed] [Google Scholar]
- 44.Williams MV, Palar K, Derose KP. Congregation-based programs to address HIV/AIDS: elements of successful implementation. J Urban Health. 2011;88(3):517–532. doi: 10.1007/s11524-010-9526-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45. National Association for the Advancement of Colored People (NAACP). The Black Church and HIV: the social justice imperative. Available at: http://www.theblackchurchandHIV.org. Accessed October 1, 2012.