Abstract
Background
Early childhood adiposity may have significant later health effects. This study examines the prevalence and recognition of obesity and severe obesity among preschool-aged children.
Methods
The electronic medical record was used to examine body mass index (BMI), height, sex and race/ethnicity in 42,559 children aged 3-5 years between 2007-2010. Normal or underweight (BMI<85th percentile); overweight (BMI 85th-94th percentile); obesity (BMI≥95th percentile); and severe obesity (BMI≥1.2×95th percentile) were classified using the 2000 Centers for Disease Control and Prevention growth charts. Provider recognition of elevated BMI was examined for obese children aged 5 years.
Results
Among 42,559 children, 12.4% of boys and 10.0% of girls had BMI ≥95th percentile. The prevalence was highest among Hispanics (18.2% boys, 15.2% girls), followed by blacks (12.4% boys, 12.7% girls). A positive trend existed between increasing BMI category and median height percentile, with obesity rates highest in the highest height quintile. The prevalence of severe obesity was 1.6% overall and somewhat higher for boys compared to girls (1.9% versus 1.4%, p<0.01). By race/ethnicity, the highest prevalence of severe obesity was seen in Hispanic boys (3.3%). Among those aged 5 years, 77.9% of obese children had provider diagnosis of obesity or elevated BMI, increasing to 89.0% for the subset with severe obesity.
Conclusions
Obesity and severe obesity are evident as early as age 3-5 years, with race/ethnic trends similar to older children. This study underscores the need for continued recognition and contextualization of early childhood obesity in order to develop effective strategies for early weight management.
Keywords: obesity, children, preschool, severe obesity, children
Introduction
The current pediatric obesity epidemic in the United States1 includes approximately 12 million (17%) children aged 2-19 years,2 with obesity defined as body mass index (BMI) at or above the 95th percentile using the year 2000 Centers for Disease Control and Prevention (CDC) BMI-for-age growth charts.3, 4 While the prevalence of obesity in children appears to have plateaued in recent years,3-5 it is now roughly triple what it was three decades ago.6, 7 Moreover, there is a growing spectrum of severe obesity, previously classified using a threshold of BMI ≥99th percentile1, 8, 9 but now using the more recently accepted threshold of BMI ≥120% of the 95th BMI percentile10-12 adjusted for age and sex. Using these definitions, studies in selected pediatric populations have found that the prevalence of severe obesity in children ranges from 3.8% to 7.7%,8, 11-13 with severe obesity beginning as early as the preschool years.8, 11, 12
The age at which excess weight gain occurs has important implications for child health and development.14 The range of normal BMI changes during childhood growth, with values generally lowest during age 4-6 years (adiposity nadir) followed by an increase (adiposity rebound) and subsequent steady rise into the adolescent years.15-17 Early adiposity rebound is associated with greater adiposity in mid-childhood,15, 16 which, in turn, has been associated with accelerated growth, advanced bone age, earlier pubertal transition and adult obesity.16, 18-25 In older children, both overweight and obesity contribute to an increased risk of metabolic syndrome, type 2 diabetes, hypertension, dyslipidemia, non-alcoholic steatohepatitis and obstructive sleep apnea.1, 26 Thus, early recognition of severe obesity is an important step towards preventing long term adverse health consequences.
There are few epidemiologic studies from large healthcare delivery systems examining obesity rates in pre-school aged children. Recent implementation of sophisticated electronic health information technology provides the unique opportunity to monitor onset and progression of overweight and obesity in large community populations, as well as the future ability to link early anthropometric findings to clinical outcomes. The primary objective of this study was to examine anthropometric findings obtained in clinical practice from a large contemporary cohort of children aged 3-5 years to 1) determine the prevalence of obesity and severe obesity and differences by race/ethnicity, sex and stature; 2) compare estimates using BMI percentile, Z score or percentage above the 95th BMI percentile as thresholds for extremely high BMI-for age; 3) determine whether children with BMI ≥95th percentile were recognized by their provider; and 4) to review the anthropometric records of individuals whose measured weight and/or BMI values were flagged by the CDC growth chart program27 as being biologically implausible values28 to determine whether these were actually children with extreme obesity.
Methods
Kaiser Permanente Northern California (KPNC) is a large integrated healthcare delivery system providing care to over three million members in Northern California, of whom approximately 6% are children under the age of 6 years. This study examines data derived from 42,620 3-5 year old children from a retrospective cohort of 160,300 KPNC children aged 3-17 years who had BMI and blood pressure obtained during a well-child visit between 1/1/2007-12/31/2010. All children had at least six months health plan membership prior to the index visit and received care within three large KPNC sub-regions. The Institutional Review Board at HealthPartners Institute for Education and Research approved the study with ceding of oversight authority by the KPNC Institutional Review Board. A waiver of informed consent was obtained due to the nature of the study.
The electronic medical record was used to obtain information on age, sex, race/ethnicity and measured height and weight, with BMI calculated as weight (kilograms) divided by height (meters) squared. The year 2000 CDC growth charts were used to calculate age and sex-specific BMI, height and weight percentiles and BMI standard deviation (Z) scores using publically available programs provided by the CDC.27 Both BMI percentile and the BMI percentage above the 95th BMI percentile were used to categorize higher degrees of obesity, including a threshold of 1.2 times the 95th BMI percentile to define severe obesity. Subsequent outpatient visits and recognition of obesity and/or elevated BMI within the ensuing year were examined using electronic medical record diagnoses (International Classification of Diseases, 9th revision codes 278.00 for obesity, 278.02 for overweight, V85.54 for BMI ≥95th percentile and V85.53 for BMI 85th-94th percentile).
We used three primary methods for data validation because of potential errors in height and weight measurements extracted from the electronic medical record. First, we excluded children in whom the height was flagged as a “biologically implausible value” by the CDC program 28 (N=30) and children whose index visit measurement included a height <61 centimeters (24 inches), weight <4.5 kilograms (10 pounds) or BMI <10 kg/m2 (N=3).
Among the remaining 42,587 children with well-child visit data, we examined growth charts for children flagged with high biologically implausible values for weight and/or BMI (N=237) and only 14 were found to be erroneous and excluded. Three children with missing BMI percentile due to erroneously high BMI >150 kg/m2 were also excluded. Finally, we reviewed growth charts for obese children with BMI or height differing by more than 15% or weight by more than 20% per year at a prior or subsequent visit within 2 years (requiring age ≥2 years) who also had an (A) index BMI ≥99th percentile, (B) index BMI ≥1.2 times the 95th percentile, (C) index BMI Z score ≥2.5 or (D) index BMI 95th-98th percentile with another BMI <95th percentile (N=193) of whom only 11 were erroneous and excluded. Height, weight or BMI values that were part of a pattern of rapid growth or weight gain persisting over two or more measurements were considered valid. If the anthropometric data provided insufficient information or if no prior/subsequent measurements were available (N=35), progress note documentation of obesity and/or elevated BMI was also examined.
In total, 430 growth charts were reviewed by a pediatric endocrinologist (LCG) with exclusion of 28 children (0.06% of the entire cohort) due to erroneous or inconsistent values. The final study cohort included 42,559 3-5 year old children.
Statistical Methods
All analyses were conducted using SAS version 9.1 (SAS Institute, Cary NC). Differences between subgroups were compared using the chi-squared test for categorical data. The Cochrane-Armitage test was used to examine the trend in proportions across categories. Linear regression techniques were used to examine the relationship between median height percentile and BMI percentile category. A p-value of <0.05 was considered statistically significant.
Results
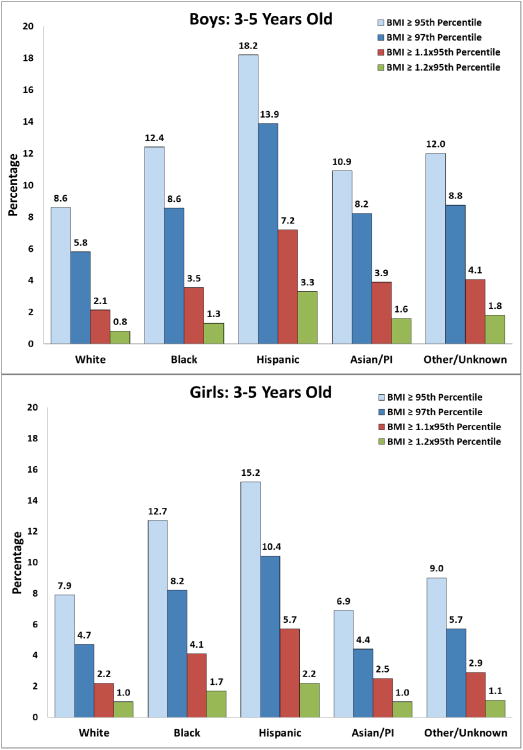
Among the final cohort of 42,559 children, 7,934 (18.6%) were 3 years, 23,351 (54.9%) were 4 years, and 11,274 (26.5%) were 5 years old (Table 1). Half of the cohort (49.0%) was female. The cohort was racially and ethnically diverse, consisting of 26.1% white, 5.9% black, 24.4% Hispanic, 21.8% Asian (including Pacific Islanders), and 21.8% of other or unknown race/ethnicity. There were 4775 (11.2%) children who met criteria for obesity, defined by BMI ≥95th percentile. Overall and within each of the age stratum, the proportion with BMI ≥95th percentile was slightly but significantly greater for boys than girls (12.4% versus 10.0% overall, p<0.05 for all comparisons). The prevalence of obesity was significantly lower in 4 year old children (boys, 11.7%; girls, 9.0%) compared to 3 year old children (boys, 12.9%; girls, 11.2%) and 5 year old children (boys, 13.6%; girls, 11.0%) (all p<0.05), possibly reflecting the adiposity nadir. Across racial/ethnic subgroups (Figure 1), the prevalence of obesity was highest among Hispanics (boys, 18.2%; girls, 15.2%) followed by blacks (boys, 12.4%; girls, 12.7%), p<0.05 for within gender comparisons). Asian girls tended to have a lower prevalence (6.9%) compared with white girls (7.9%) (p=0.05), and Asian boys had a higher prevalence (10.9%) compared with white boys (8.6%) (p<0.001). A total of 7.8% of children had BMI ≥97th percentile, with a greater proportion among boys compared with girls (9.1% versus 6.4%, p<0.001) and the highest proportions in Hispanic children (13.9% for boys; 10.4% for girls, Figure 1). Approximately half (49.2%) of the children with BMI ≥97th percentile also had a BMI ≥1.1 × 95th percentile. When categorized by BMI Z score ≥3.00, only 0.3% of girls were identified compared to 2.0% of boys (p<0.001), with almost no girls identified by age 5 years (0.1%).
Table 1. Body mass index (BMI) classification among children age 3-5 years with a well child visit during 2007-2010.
Numbers represent row percentages.
| BMI PERCENTILE | BMI % ≥ 1.1 × 95th percentile | BMI % ≥ 1.2 × 95th percentile | BMI Z Score | |||||
|---|---|---|---|---|---|---|---|---|
|
|
|
|||||||
| < 85th | 85th – 94th | ≥ 95th | ≥ 97th | 2.00 – 2.99 | ≥ 3.00 | |||
|
| ||||||||
| BOYS (21,720) | 15,946 (73.4%) | 3,076 (14.2%) | 2,698 (12.4%) | 1,980 (9.1%) | 926 (4.3%) | 403 (1.9%) | 1,276 (5.9%) | 428 (2.0%) |
|
| ||||||||
| Age in years (N) | ||||||||
| 3 years (4,042) | 2,945 (72.9%) | 576 (14.3%) | 521 (12.9%) | 384 (9.5%) | 141 (3.5%) | 43 (1.1%) | 247 (6.1%) | 86 (2.1%) |
| 4 years (11,947) | 8,898 (74.5%) | 1,650 (13.8%) | 1,399 (11.7%) | 1,023 (8.6%) | 434 (3.6%) | 187 (1.6%) | 641 (5.4%) | 234 (2.0%) |
| 5 years (5,731) | 4,103 (71.6%) | 850 (14.8%) | 778 (13.6%) | 573 (10.0%) | 351 (6.1%) | 173 (3.0%) | 388 (6.8%) | 108 (1.9%) |
|
| ||||||||
| GIRLS (20,839) | 15,573 (74.7%) | 3,189 (15.3%) | 2,077 (10.0%) | 1,338 (6.4%) | 705 (3.4%) | 285 (1.4%) | 1,021 (4.9%) | 61 (0.3%) |
|
| ||||||||
| Age in years (N) | ||||||||
| 3 years (3,892) | 2,826 (72.6%) | 630 (16.2%) | 436 (11.2%) | 312 (8.0%) | 147 (3.8%) | 39 (1.0%) | 228 (5.9%) | 26 (0.7%) |
| 4 years (11,404) | 8,640 (75.8%) | 1,734 (15.2%) | 1,030 (9.0%) | 633 (5.6%) | 314 (2.8%) | 128 (1.1%) | 473 (4.2%) | 29 (0.3%) |
| 5 years (5,543) | 4,107 (74.1%) | 825 (14.9%) | 611 (11.0%) | 393 (7.1%) | 244 (4.4%) | 118 (2.1%) | 320 (5.8%) | 6 (0.1%) |
BMI < 85th percentile – normal or underweight
BMI 85th – 94th percentile – overweight
BMI ≥ 95th percentile – obesity
BMI ≥ 1.2 × 95th percentile – severe obesity
Figure 1. The proportion of children by sex and race/ethnicity according to BMI classification.
BMI ≥ 95th percentile – obesity, BMI ≥ 1.2 × 95th percentile – severe obesity.
Using BMI-for-age criteria for severe obesity, 1.6% of children had BMI ≥1.2 times the 95th BMI percentile (1.9% for boys and 1.4% for girls, p<0.001). This prevalence was significantly lower than that ascertained when using a threshold of BMI ≥99th percentile (3.9% overall, 5.1% for boys and 2.7% for girls, p<0.001). For both thresholds, a male predominance was seen. Across racial/ethnic subgroups, Hispanic boys had the highest prevalence of severe obesity (3.3%, p<0.01 compared to boys of white, black or Asian race/ethnicity and compared to Hispanic and black girls). Among girls, Hispanic and black girls had the highest prevalence of severe obesity (2.2% and 1.7%, respectively, p<0.05 when compared to white and Asian girls; p=0.30 when comparing Hispanic and black girls).
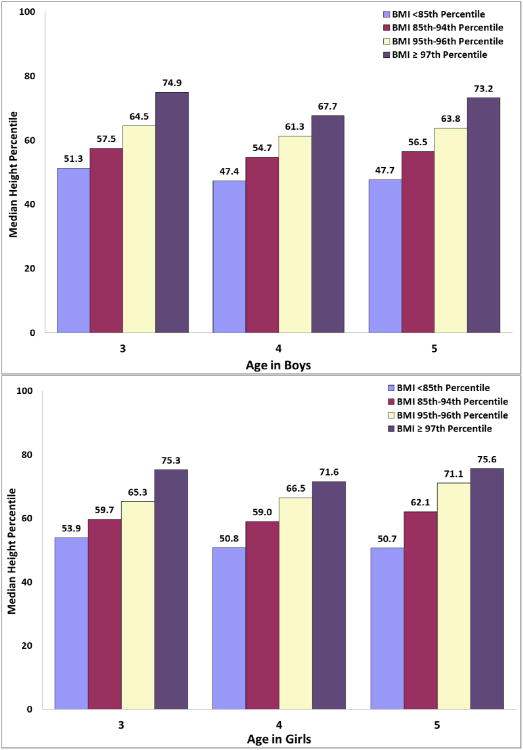
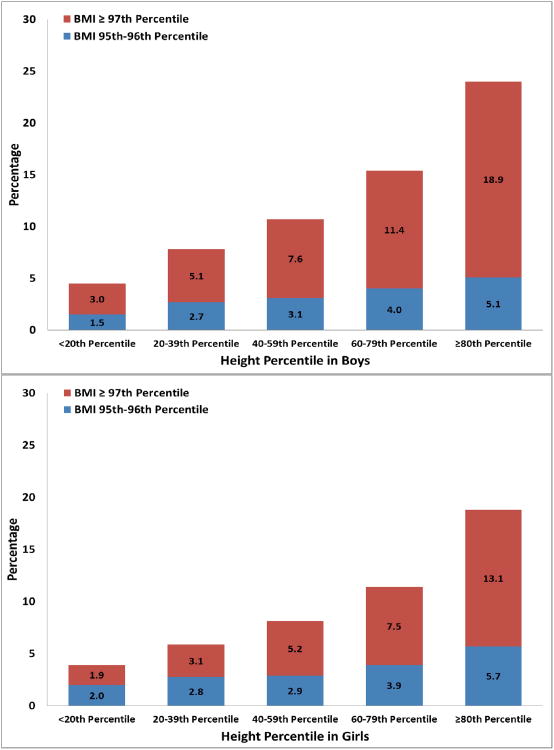
Figure 2 shows the median height percentile by BMI percentile subgroup for each age by gender. Among children with BMI <85th percentile, the median height percentile was around the 50th percentile. However, increasing BMI percentile category was associated with an increase in the median height percentile (significant linear trend, p<0.001) within each age-sex stratum. Figure 3 shows the increasing proportions of children with BMI at or above the 95th and 97th percentiles across increasing height percentile in quintiles, (p<0.001, test for trend).
Figure 2. Median height percentile by body mass index (BMI) percentile in boys and girls.
Significant differences in median height percentile were seen across BMI categories for each age-sex stratum, with a significant linear trend (p<0.001 within each age-sex category).
Figure 3. Proportion of children with BMI ≥ 95th percentile (BMI 95th-96th percentile or BMI ≥ 97th percentile) by increasing height quintile in boys and girls age three to five years old.
P <0.001 for trend across increasing height category.
Included in this study were 223 children with extreme BMI (N=156) or both extreme BMI and weight (N=67) values that were correct despite identification by the CDC-based program as high “biologically implausible values”. As shown in Table 2, these included 3.5-fold more boys than girls and the majority were of Hispanic or Asian race/ethnicity. All 223 children had BMI and weight percentile values in the 99th-100th percentile range, BMI Z score above 2.5, and BMI exceeding 1.2 times the 95th BMI percentile for age and sex (Table 2). Each age-sex group also demonstrated extremely high median height percentiles (>80th percentile). Although 0.9% had Prader-Willi syndrome, most did not demonstrate obesity-related conditions. The most prominent comorbidity was asthma, identified in 17.5% of this subgroup based on coded visit diagnoses in the prior six months.
Table 2.
Demographic and anthropometric findings in the 223 children with valid measurements of weight and body mass index despite designation as high “biologically implausible values” using the Year 2000 Centers for Disease Control and Prevention growth chart reference data.
| Median (IQR) Weight (kg) | Median (IQR) Height (centimeters) | Median (IQR) Height Percentile | Median (IQR) Body Mass Index (kg/m2) | ≥ 1.5 × 95th BMI Percentile N (%) | Race / Ethnicity | |
|---|---|---|---|---|---|---|
| BOYS (N =173) | 31.5 (28.0 – 34.5) | 111.1 (106.7 – 114.3) | 82.1 (65.4 – 92.1) | 25.1 (24.1 – 26.9) | 42 (24.3%) | 12.1 %White 4.1 % Black 43.9 % Hispanic 24.9 % Asian |
| Age 3 (N = 20) | 27.9 (25.4 – 30.3) | 105.7 (101.6 – 106.7) | 90.7 (78.1 – 93.1) | 25.3 (23.5 – 27.0) | 5 (25.0%) | |
| Age 4 (N = 93) | 29.7 (27.0 – 33.6) | 108.5 (105.4 – 113.0) | 81.5 (64.9 – 93.1) | 24.6 (23.8 – 26.9) | 24 (25.8%) | |
| Age 5 (N = 60) | 34.0 (32.3 – 37.7) | 114.9 (113.0 –117.8) | 80.3 (68.9 – 88.5) | 25.5 (24.8 – 26.7) | 13 (21.7%) | |
| GIRLS (N = 50) | 32.1 (28.6 – 35.5) | 108.6 (104.8 – 114.3) | 84.9 (71.0 – 91.8) | 26.5 (25.7 – 27.7) | 14 (28.0%) | 6.0 % White 6.0 % Black 60.0 % Hispanic 14.0 % Asian |
| Age 3 (N = 13) | 27.7 (26.2 – 28.8) | 103.5 (100.3 – 105.4) | 91.4 (60.3 - 91.8) | 25.7 (25.2 - 26.4) | 3 (23.1%) | |
| Age 4 (N = 20) | 31.1 (28.7 – 33.0) | 106.6 (105.4 – 112.4) | 82.6 (73.4 - 95.1) | 26.4 (25.4 – 27.2) | 5 (25.0%) | |
| Age 5 (N = 17) | 35.6 (34.8 – 38.7) | 114.3 (113.0 – 118.1) | 85.1 (74.5 – 90.1) | 27.5 (26.6 – 28.6) | 6 (35.3%) |
All children had BMI and weight values approaching the 100th percentile and a BMI value ≥1.2 × 95th BMI percentile
IQR: Interquartile range. Percentage numbers represent row percentages
We examined the frequency of overweight and obesity recognition over the ensuing year after the index well child visit in the 1,389 (12.3%) of 11,274 children aged 5 years with BMI ≥95th percentile because this age represents the beginning of the BMI trajectory beyond the adiposity nadir. The majority (86.9%) had continuous membership for at least one year after the well-child visit, with one or more subsequent ambulatory visits among 76.5% overall and 80.2% for obese children. Among these 1,389 children, 71.0% had a visit diagnosis of either obesity or elevated BMI ≥95th percentile and an additional 6.9% had a diagnosis relating to overweight (or BMI 85th-94th percentile), all of whom received routine nutrition and/or exercise counseling. There were 573 boys and 393 girls aged five years with BMI ≥97th percentile in whom recognition of elevated BMI ≥95th percentile and/or obesity was documented in 77.6%. Among the subset of 173 boys and 118 girls with severe obesity (BMI ≥1.2 × 95th BMI for age percentile), recognition of elevated BMI ≥95th percentile and/or obesity was higher at 89.0%.
Discussion
In this cohort of more than 40,000 preschool-aged children (3-5 years old), 12.4% of boys and 10.0% of girls met criteria for obesity (BMI ≥95th percentile). While fewer children met criteria for severe obesity defined by BMI ≥1.2 times the 95th percentile (1.6%), the majority of obese children (69.5%) exceeded the 97th BMI percentile. Across increasing BMI strata, the prevalence was highest among Hispanic boys. These findings complement data from other studies demonstrating that the prevalence of high BMI-for-age in older children is greatest among Hispanic boys and African American girls.5, 8 A study of 2,452 younger urban children similarly found that a disparity between Hispanic and non-Hispanic children can be identified as early as 3 years of age.29
This study found that in the context of routine pediatric care, a relatively high percentage of obese 5 year old children had their obesity recognized by their clinical caregivers, as ascertained from the electronic medical record; it is possible that recognition rates would have been even higher had all clinical encounter notes been systematically reviewed for this study. The proportion of children with subsequent outpatient visits during the ensuing year was also extremely high, suggesting there are opportunities to initiate preventive measures at this early age.
Both the 99th BMI-for-age percentile threshold and a BMI threshold of 1.2 times the 95th percentile have been used as measures of severe obesity.1, 8-12 While the 99th percentile identified a larger proportion of children, concerns have been raised about the accuracy of this threshold when using the CDC growth charts, given the lack of fit to empiric data.10 Furthermore, use of BMI percentile for stratification of extremely high BMI values is limited by contraction of percentile values at the upper bound where large changes in BMI result in minimal change in BMI percentile.30, 31 The use of BMI Z score is also limited by an upper bound, depending on age and sex.31 Almost no girls aged 5 years had a Z score ≥3.00, due to the fact that Z scores beyond 4.00 are undefined for girls and boys over the age of 4 and 6 years, respectively.31 These findings highlight challenges in classification of extremely high BMI-for-age in children, particularly for contemporary populations who represent a rightward shift from historic populations used for development of the year 2000 CDC growth charts.17 Classifying high BMI values as a percentage of the 95th percentile has been proposed as a more flexible approach to characterizing obesity severity based on evidence that this approach provides a better fit to empiric data than BMI percentile estimates above the 97th percentile.10 The currently preferred definition of severe obesity is a BMI ≥1.2 times the 95th percentile when using the CDC growth charts,10-12 a threshold that demonstrates better approximation of the empiric 99th BMI percentile.10 Consistent with these recommendations, a new growth chart based on BMI percentage above the 95th percentile has recently been proposed for clinical tracking of severely obese children.32 Our study found that using a BMI threshold of ≥1.2 × 95th percentile identified 1.9% of boys and 1.4% of girls who met criteria for severe obesity. Because the range of BMI values within this young age group is relatively narrow compared to older children where the growth curves widen considerably, use of lower thresholds such as the 97th percentile or 1.1 × 95th percentile may also be helpful in targeting young obese children at risk for progression to more severe degrees of obesity.
Most children initially flagged as having biologically implausible high values for BMI and/or weight had, in fact, valid measurements of these indices. More than three quarters were boys, of whom a large proportion were Hispanic (44%) or Asian (25%). The CDC program uses fixed exclusion ranges provided by the World Health Organization to define “biologically implausible values” with the goal of removing these excessively high values that may be due to entry errors or mis-measurement.27, 28 However, our findings demonstrate that values labeled as implausible should not be automatically excluded in young children without more careful evaluation of growth trajectory. Other investigators have used algorithms based on incremental weight or height values below the 1st or above the 99th percentiles to identify potential errors in the electronic medical record;33 using those methods in our study identified no additional children for exclusion. In this study, we used data from prior and/or subsequent clinical visits, where inconsistencies in measured height, weight and BMI within specific subgroups were used to determine the need for individual growth chart review.
Level of BMI was directly associated with height percentile, consistent with the known interrelationship of BMI and linear growth; heavier children were taller and those in the highest BMI category had the tallest stature. The increasing proportion of children with BMI ≥95th percentile or ≥97th percentile across increasing height quintiles is consistent with data from others who observed a more than 10-fold increase in obesity prevalence across lowest to highest height quintile for children 3-10 years of age.34 This early association between BMI and growth may have important implications for subsequent pubertal development, final adult height and adult adiposity. One of the challenges associated with assessment of adiposity status during the early years of growth is that changes in BMI represent both changes in adiposity and changes in lean mass. However, calculated BMI is strongly correlated with percent body fat measured by dual energy x-ray absorptiometry,35 and differences in BMI at a given height are associated with differences in body fatness. Additional demographic variation in the relationship of BMI to body fat may also be relevant when comparing BMI-for-age across different population subgroups.36
It is not clear whether obesity at this early age is related to differences in behaviors and feeding patterns, e.g., breast milk versus formula and the timing of introduction of solid foods, particularly in a racially and ethnically diverse cohort. Parental obesity, maternal conditions, environment and behavior are also known to modulate the risk of childhood obesity,37, 38 but these contextual factors could not be ascertained in this study due to the limitations of the electronic medical record. Although this study did not include children under age 3 years, obesity trends may begin as early as infancy where examination of weight-for-length has been used to estimate the prevalence of infant obesity.39
In summary, the high prevalence of early onset obesity is of great concern from a public health perspective, because of the strong tracking effect of childhood obesity and relation of childhood obesity to adult metabolic complications and other clinical comorbidities. This concern is underscored by the finding that extreme obesity is significantly higher in specific ethnic groups and, in particular, Hispanics. While future research is needed to track the long-term outcomes among these children, the early recognition of obesity by healthcare providers and the high proportion with follow-up care within this young age group may provide an important framework to support delivery of effective and timely interventions for obesity management and prevention at an early age.
What is already known about this subject
The prevalence of obesity in the U.S. has increased dramatically over the past 3 decades.
There is a growing spectrum of severe obesity among children and adolescents.
Obesity trends and race/ethnic differences may be evident at a young age.
What this study adds
Among children age 3-5 years old, the prevalence of obesity and severe obesity was higher in boys than girls and highest among children of Hispanic ethnicity.
Within this young age group, higher BMI was associated with greater height percentile.
Among obese children age 5 years old, provider recognition of obesity or elevated body mass index was high, approaching 80% of children.
Acknowledgments
JL, BM, MC, SD, AS and LG conceived the project. MC conducted the data analyses. JL, BM and LG drafted the initial manuscript. All authors provided critical input on data analysis and interpretation, revised the manuscript for important intellectual content, and approved the final version. The authors would like to acknowledge Joel Gonzalez for his support with manuscript preparation. This study was funded by the National Heart, Lung and Blood Institute at the National Institutes of Health 1RO1HL093345 to HealthPartners Research Foundation (Patrick O'Connor, Principal Investigator) and conducted within the Cardiovascular Research Network, a consortium of research organizations affiliated with the HMO Research Network and sponsored by the National Heart Lung and Blood Institute (U19 HL91179-01).
Footnotes
Conflicts of Interest: None
References
- 1.Barlow SE. Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: summary report. Pediatrics. 2007;120(4):S164–92. doi: 10.1542/peds.2007-2329C. [DOI] [PubMed] [Google Scholar]
- 2.Ogden CL, Lamb MM, Carroll MD, Flegal KM. NCHS Data Brief. 2010. Obesity and socioeconomic status in children and adolescents: United States, 2005-2008; pp. 1–8. [PubMed] [Google Scholar]
- 3.Ogden CL, Carroll MD, Curtin LR, Lamb MM, Flegal KM. Prevalence of high body mass index in US children and adolescents, 2007-2008. JAMA. 2010;303:242–9. doi: 10.1001/jama.2009.2012. [DOI] [PubMed] [Google Scholar]
- 4.Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of Obesity and Trends in Body Mass Index Among US Children and Adolescents, 1999-2010. JAMA: The Journal of the American Medical Association. 2012 doi: 10.1001/jama.2012.40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Ogden CL, Carroll MD, Flegal KM. High body mass index for age among US children and adolescents, 2003-2006. JAMA. 2008;299:2401–5. doi: 10.1001/jama.299.20.2401. [DOI] [PubMed] [Google Scholar]
- 6.Hedley AA, Ogden CL, Johnson CL, Carroll MD, Curtin LR, Flegal KM. Prevalence of overweight and obesity among US children, adolescents, and adults, 1999-2002. JAMA. 2004;291:2847–50. doi: 10.1001/jama.291.23.2847. [DOI] [PubMed] [Google Scholar]
- 7.Ogden CL, Carroll MD. Prevalence of obesity among children and adolescents: United States, Trends 1963-1965 through 2007-2008. NCHS Health E-Stat. 2010:1–5. [Google Scholar]
- 8.Skelton JA, Cook SR, Auinger P, Klein JD, Barlow SE. Prevalence and trends of severe obesity among US children and adolescents. Acad Pediatr. 2009;9:322–9. doi: 10.1016/j.acap.2009.04.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Freedman DS, Mei Z, Srinivasan SR, Berenson GS, Dietz WH. Cardiovascular risk factors and excess adiposity among overweight children and adolescents: the Bogalusa Heart Study. J Pediatr. 2007;150:12–7. e2. doi: 10.1016/j.jpeds.2006.08.042. [DOI] [PubMed] [Google Scholar]
- 10.Flegal KM, Wei R, Ogden CL, Freedman DS, Johnson CL, Curtin LR. Characterizing extreme values of body mass index-for-age by using the 2000 Centers for Disease Control and Prevention growth charts. Am J Clin Nutr. 2009;90:1314–20. doi: 10.3945/ajcn.2009.28335. [DOI] [PubMed] [Google Scholar]
- 11.Koebnick C, Smith N, Coleman KJ, et al. Prevalence of extreme obesity in a multiethnic cohort of children and adolescents. J Pediatr. 2010;157:26–31. e2. doi: 10.1016/j.jpeds.2010.01.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Wang YC, Gortmaker SL, Taveras EM. Trends and racial/ethnic disparities in severe obesity among US children and adolescents, 1976-2006. Int J Pediatr Obes. 2011;6:12–20. doi: 10.3109/17477161003587774. [DOI] [PubMed] [Google Scholar]
- 13.Benson L, Baer HJ, Kaelber DC. Trends in the diagnosis of overweight and obesity in children and adolescents: 1999-2007. Pediatrics. 2009;123:e153–8. doi: 10.1542/peds.2008-1408. [DOI] [PubMed] [Google Scholar]
- 14.Dietz WH. Critical periods in childhood for the development of obesity. Am J Clin Nutr. 1994;59:955–9. doi: 10.1093/ajcn/59.5.955. [DOI] [PubMed] [Google Scholar]
- 15.Rolland-Cachera MF, Deheeger M, Bellisle F, Sempe M, Guilloud-Bataille M, Patois E. Adiposity rebound in children: a simple indicator for predicting obesity. Am J Clin Nutr. 1984;39:129–35. doi: 10.1093/ajcn/39.1.129. [DOI] [PubMed] [Google Scholar]
- 16.Rolland-Cachera MF, Deheeger M, Maillot M, Bellisle F. Early adiposity rebound: causes and consequences for obesity in children and adults. Int J Obes (Lond) 2006;30(4):S11–7. doi: 10.1038/sj.ijo.0803514. [DOI] [PubMed] [Google Scholar]
- 17.Kuczmarski RJ, Ogden CL, Guo SS, et al. Vital Health Stat 11. 2002. 2000 CDC Growth Charts for the United States: methods and development; pp. 1–190. [PubMed] [Google Scholar]
- 18.Demerath EW, Jones LL, Hawley NL, et al. Rapid infant weight gain and advanced skeletal maturation in childhood. The Journal of pediatrics. 2009;155:355–61. doi: 10.1016/j.jpeds.2009.03.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Forbes GB. Nutrition and growth. The Journal of pediatrics. 1977;91:40–2. doi: 10.1016/s0022-3476(77)80440-x. [DOI] [PubMed] [Google Scholar]
- 20.Mamun AA, Hayatbakhsh MR, O'Callaghan M, Williams G, Najman J. Early overweight and pubertal maturation--pathways of association with young adults' overweight: a longitudinal study. International journal of obesity. 2009;33:14–20. doi: 10.1038/ijo.2008.220. [DOI] [PubMed] [Google Scholar]
- 21.Must A, Naumova EN, Phillips SM, Blum M, Dawson-Hughes B, Rand WM. Childhood overweight and maturational timing in the development of adult overweight and fatness: the Newton Girls Study and its follow-up. Pediatrics. 2005;116:620–7. doi: 10.1542/peds.2004-1604. [DOI] [PubMed] [Google Scholar]
- 22.Sandhu J, Ben-Shlomo Y, Cole TJ, Holly J, Davey Smith G. The impact of childhood body mass index on timing of puberty, adult stature and obesity: a follow-up study based on adolescent anthropometry recorded at Christ's Hospital (1936-1964) International journal of obesity. 2006;30:14–22. doi: 10.1038/sj.ijo.0803156. [DOI] [PubMed] [Google Scholar]
- 23.Freedman DS, Khan LK, Serdula MK, Dietz WH, Srinivasan SR, Berenson GS. The relation of menarcheal age to obesity in childhood and adulthood: the Bogalusa heart study. BMC pediatrics. 2003;3:3. doi: 10.1186/1471-2431-3-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Whitaker RC, Pepe MS, Wright JA, Seidel KD, Dietz WH. Early adiposity rebound and the risk of adult obesity. Pediatrics. 1998;101:E5. doi: 10.1542/peds.101.3.e5. [DOI] [PubMed] [Google Scholar]
- 25.Williams SM, Goulding A. Early adiposity rebound is an important predictor of later obesity. Obesity (Silver Spring) 2009;17:1310. doi: 10.1038/oby.2009.104. [DOI] [PubMed] [Google Scholar]
- 26.Daniels SR, Jacobson MS, McCrindle BW, Eckel RH, Sanner BM. American Heart Association Childhood Obesity Research Summit: executive summary. Circulation. 2009;119:2114–23. doi: 10.1161/CIRCULATIONAHA.109.192215. [DOI] [PubMed] [Google Scholar]
- 27.A SAS Program for the CDC Growth Charts. [Accessed October 20, 2011]; http://www.cdc.gov/nccdphp/dnpao/growthcharts/resources/sas.htm.
- 28.Cut-offs to define outliers in the 2000 CDC Growth Charts. [Accessed April 26, 2012]; http://www.cdc.gov/nccdphp/dnpa/growthcharts/resources/BIV-cutoffs.pdf.
- 29.Whitaker RC, Orzol SM. Obesity among US urban preschool children: relationships to race, ethnicity, and socioeconomic status. Archives of pediatrics & adolescent medicine. 2006;160:578–84. doi: 10.1001/archpedi.160.6.578. [DOI] [PubMed] [Google Scholar]
- 30.Cole TJ, Faith MS, Pietrobelli A, Heo M. What is the best measure of adiposity change in growing children: BMI, BMI %, BMI z-score or BMI centile? Eur J Clin Nutr. 2005;59:419–25. doi: 10.1038/sj.ejcn.1602090. [DOI] [PubMed] [Google Scholar]
- 31.Woo JG. Using body mass index Z-score among severely obese adolescents: a cautionary note. Int J Pediatr Obes. 2009;4:405–10. doi: 10.3109/17477160902957133. [DOI] [PubMed] [Google Scholar]
- 32.Gulati AK, Kaplan DW, Daniels SR. Clinical tracking of severely obese children: a new growth chart. Pediatrics. 2012;130:1136–40. doi: 10.1542/peds.2012-0596. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Smith N, Coleman KJ, Lawrence JM, et al. Body weight and height data in electronic medical records of children. Int J Pediatr Obes. 2010;5:237–42. doi: 10.3109/17477160903268308. [DOI] [PubMed] [Google Scholar]
- 34.Freedman DS, Khan LK, Serdula MK, Dietz WH, Srinivasan SR, Berenson GS. Inter-relationships among childhood BMI, childhood height, and adult obesity: the Bogalusa Heart Study. Int J Obes Relat Metab Disord. 2004;28:10–16. doi: 10.1038/sj.ijo.0802544. [DOI] [PubMed] [Google Scholar]
- 35.Lindsay RS, Hanson RL, Roumain J, Ravussin E, Knowler WC, Tataranni PA. Body mass index as a measure of adiposity in children and adolescents: relationship to adiposity by dual energy x-ray absorptiometry and to cardiovascular risk factors. The Journal of clinical endocrinology and metabolism. 2001;86:4061–7. doi: 10.1210/jcem.86.9.7760. [DOI] [PubMed] [Google Scholar]
- 36.Daniels SR, Khoury PR, Morrison JA. The utility of body mass index as a measure of body fatness in children and adolescents: differences by race and gender. Pediatrics. 1997;99:804–7. doi: 10.1542/peds.99.6.804. [DOI] [PubMed] [Google Scholar]
- 37.Reilly JJ, Armstrong J, Dorosty AR, et al. Early life risk factors for obesity in childhood: cohort study. BMJ. 2005;330:1357. doi: 10.1136/bmj.38470.670903.E0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Salsberry PJ, Reagan PB. Dynamics of early childhood overweight. Pediatrics. 2005;116:1329–38. doi: 10.1542/peds.2004-2583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.McCormick DP, Sarpong K, Jordan L, Ray LA, Jain S. Infant obesity: are we ready to make this diagnosis? J Pediatr. 2010;157:15–9. doi: 10.1016/j.jpeds.2010.01.028. [DOI] [PubMed] [Google Scholar]