Abstract
Population pharmacokinetic and dynamic (PK/PD) modeling is often employed to analyze data of steady state trough serum digoxin concentrations in the course of what is frequently regarded as routine therapeutic drug monitoring (TDM). Such a monitoring protocol is extremely uninformative. It permits only estimation of a single parameter of a one- compartment model, such as clearance. Use of D-optimal design strategies permit much more information to be obtained, employing models having really meaningful structure. Strategies and protocols for routine TDM policies greatly need to be improved, incorporating these principles of optimal design.
Keywords: Population pharmacokinetic/dynamic modeling, Therapeutic drug monitoring, Optimal Individualized Drug Dosage, Digoxin, Atrial Fibrillation
Software for population PK modeling has been dominated by NONMEM. However, since NONMEM is a parametric method, it must assume a shape for the model parameter distributions. If the assumption is not correct, the model will be in error, and the most likely results given the raw data will not be obtained. In addition, the likelihood as computed by NONMEM is only approximate, not exact. This impairs statistical consistency, and reduces statistical efficiency and the resulting precision of model parameter estimates. Other parametric methods are superior, as they provide exact likelihoods. However, they still suffer from the constraints of assuming the shape of the model parameter distributions.
Nonparametric (NP) methods are more flexible. One need not make any assumptions about the shape of the parameter distributions. NP methods also provide exact likelihoods, and are statistically consistent, efficient, and precise. They also permit maximally precise dosage regimens to be developed for patients using multiple model (MM) dosage design, something parametric modeling methods cannot do.
Laboratory assay errors are better described by the reciprocal of the assay variance of each measurement rather than by coefficient of variation. This is easy to do and permits more precise models to be made. This also permits estimation of assay error separately from the other sources of uncertainty in the clinical environment. This is most useful scientifically.
Digoxin has at least 2 compartment behavior. Its pharmacologic and clinical effects correlate not with serum digoxin concentrations, but with those in the peripheral nonserum compartment. Some illustrative clinical examples are discussed. It appears that digitalis therapy, guided by TDM and our 2 compartment models based on that of Reuning et al, can convert at least some patients with atrial fibrillation and flutter to regular sinus rhythm.
Investigators have often used steady state trough concentrations only to make a 1 compartment model, and have sought only to predict future steady state trough concentrations. Much more than this can be done, and clinical care can be much improved. Further work along these lines is greatly to be desired.
Population Modeling Based on Routine Data from Therapeutic Drug Monitoring (TDM)
Investigators frequently perform population studies of drug behavior in patients by using data of what they regard as routine therapeutic drug monitoring (TDM). This often involves analyzing data of trough serum drug concentrations drawn in the steady state. In addition, the goal of such studies often is oriented only to predicting similar steady state trough concentrations in the future.
Provided are some comments and suggestions about this strategy, especially as it pertains to population modeling of digoxin, the use of serum digoxin concentrations in evaluating both the clinical as well as the pharmacokinetic and dynamic (PK/PD) behavior of the drug, and the utility of TDM combined with software employing nonparametric (NP) population models and multiple model (MM) dosage design for the optimization of digoxin therapy.
Investigators often use data of steady state trough serum digoxin concentrations to make the only model possible from that data, namely a 1-compartment model. The absorption rate constant and apparent volume of distribution are often fixed at literature values from other studies. The only parameter estimated may be clearance. The goal of the study is often restricted only to the prediction of similar steady state trough serum concentrations in the future, which they may do well enough.
The impression, held by many, is that one can make meaningful population PK models from such steady state, trough only, data. This is an illusion. Even though population models can obtain results from as little as a single sample per patient, no model having any real structure can be made from such minimally informative steady state trough only data. The rationale usually offered for such lack of concern for experimental design is that as long as the total number of data points is greater than the number of model parameters, then population modeling will work.
The Crucial Role of Informative Data
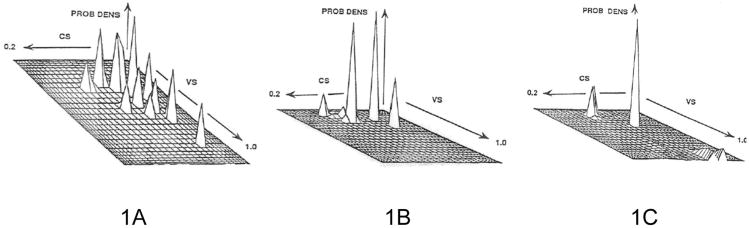
An example of the crucial role of experimental design and the results obtained is shown in Figure 1, which was reproduced with permission from Jelliffe et al1. Figure 1A shows the results obtained using a nonparametric method of population analysis2 of a full dataset of 177 patient serum concentrations obtained at various times after a dose in 20 patients receiving repeated doses of gentamicin, using a 1-compartment PK model. Figure 1B shows the degraded results obtained from restricting the dataset to only 20 measurements, one sample per patient, the highest peak obtained from ten of the patients, and the lowest trough from the other ten. Figure 1C shows the still more degraded results obtained by sampling only the single lowest trough from each patient. The figure reveals that the protocol used in obtaining data from which a population PK model is made has a truly profound effect upon the results obtained, even though the population modeling software actually works correctly, obtaining the most likely results given the data, in all cases.
Figure 1.
Figure 1A, left, shows the NP estimated density of clearance slope (CS) per unit of creatinine clearance (ml/min/1.73 M2, horizontal axis), volume slope (l/kg, downward and rightward axis), and probability (vertical axis). The vertical spikes are the discrete nonparametric support points which constitute the estimated entire model (1 compartment) joint parameter distribution. Results obtained from the full dataset of 177 measured gentamicin concentrations in 20 patients.
Figure 1B, center, shows the much different parameter estimates, based only on data of a single serum sample per patient, the highest peak in 10 randomly selected patients, and the lowest trough from the other 10 patients. Note the degraded results. Axes as in 1A.
Figure 1C, right, shows the even more different results when the dataset is restricted to only the single lowest trough sample from each of the 20 patients. Axes as in 1A.
A good discussion of the issues of optimal experimental design for guiding pharmacokinetic experiments, and of managing TDM in general is given by D'Argenio3. Use of optimal design strategies can greatly increase the capability of any PK study and also of policies for routine TDM. They permit making either a population or an individual model of a drug in a patient that has real structure to it. For TDM of digoxin, which has a highly significant peripheral nonserum compartment4, it is suggested to draw serum samples at times close to the D-optimal times - a peak serum sample drawn either about 5 min after a 15 min intravenous infusion, for example, or about 1.5 to 1.75 hours after an oral dose, and a trough. In addition, it is often useful, to supplement them with measurements taken 0.5 hour and 7 hours after a dose is given or started (by either route) to best estimate the rate constants from the central out to the peripheral compartment and back again5. In managing patients using TDM, one can obtain not only a peak and trough pair in one dose interval, but also the other pair in a different dose interval, for example, going back and forth if needed.
One reason that monitoring trough serum drug concentrations has been so popular is that the effects caused by the errors made in recording the times of dose administration and of drawing the blood upon the measurement obtained are minimized when the trough sample is obtained. The result of that strategy, however, is that information of drug kinetics over time is also minimized. Without kinetic information obtained by meaningful experimental design, as outlined by D'Argenio3, no meaningful PK or PK/PD model can be made without better chosen data. A corollary of this is that it is always crucial to record accurately the times at which doses are given and serum samples are drawn. Also, in general, one probably needs to get, at a minimum, and over several dose intervals if needed, at least 1 sample for each model parameter to be estimated, either for a PK study or for a good routine TDM protocol.
Pharmaceutical companies often use D-optimal design to make population models, as they get better information from fewer patients at minimal cost. For example, they may begin by studying about 5 patients using an initial protocol, and then make a population model based on those 5 patients. Then they may use design strategies to optimize the sampling protocol, and study several more patients. They may iterate this process until the optimal sampling strategy becomes stable, and they have developed the best model (out of several candidate models) from sampling the fewest patients. By using such an adaptively optimized sampling strategy they have obtained the most information from the fewest patients for the dollars spent doing the study.
Software for Population Modeling
NONMEM6 has probably been the most widely used population modeling method. It uses a parametric model. As such, it must assume the shape of the distribution of the model parameters, such as normal, lognormal, or perhaps bi- or multi-modal. Some distributions, such as lognormal, may well be chosen for statistical convenience, avoiding negative parameter values in the distribution. The NONMEM parameter estimates obtained are single point estimates of the model parameter means, variances, and covariances. These are estimates of mean and standard deviation, for example, of the single point parameter values in the equation which describes the assumed shape, such as that for a normal Gaussian distribution. That is why they are called parametric methods.
The word nonparametric, as used herein, specifically does not refer to the development of noncompartmental models based on statistical moments, which also have been called nonparametric by some.
In contrast to parametric compartmental models and the above noncompartmental models, rigorous nonparametric (NP) population modeling methods estimate the entire model parameter distributions2,7-9. There is no equation required any more to describe any assumed shape of the model distributions. Further, if one uses a parametric model to develop a dosage regimen to achieve a desired therapeutic target goal, the separation principle10 states that the task is done suboptimally, as there is no performance index employed to evaluate and optimize the expected precision with which the selected therapeutic target goal will be achieved. Information from the full model parameter distributions is not available. One simply develops a regimen designed to achieve a desired target goal exactly, and knows that it will not do so.
In addition, the likelihoods computed by NONMEM are only approximate (the FO, FOCE, and similar algorithms). Because of this, results are approximate, with an error often approximately 2% for means, but approximately 30% for variances, and really gross, frequently in the opposite direction, for correlations8. Because of those approximations, there is also no mathematical guarantee that if one studies more patients, the estimated parameter values will approach the true ones more closely2,7-8. In short, there is no guarantee of statistical consistency. Other parametric methods, though, do have exact likelihoods, and thus do have the guarantee of statistical consistency11-12. However, they still lack flexibility from assuming the shape of the assumed model parameter distributions, and from obtaining only single point estimates of those distributions. Even though the likelihoods obtained may be exact, if the assumed shape is not the correct (true) one given the data, the results will still be in error, as the likelihood obtained by such a constrained parametric method is often not the most likely one8.
The parameter distributions provided by NP modeling methods2,7-9 obtain a discrete distribution, based on the theorems of Caratheodory, Lindsay, and Mallet2,7,13. The NP model parameter distributions thus consist of multiple discrete points (support points), up to 1 per patient studied in the population. In addition, the likelihoods calculated are exact, and statistical consistency is assured. Each discrete support point (see Figure 1) consists of an estimated value for each model parameter, and an estimate of the probability of that point in the population. In such discrete population distributions, subpopulations such as fast and slow metabolizers are easily recognized without further effort.
There has recently been a nonparametric option implemented in NONMEM14,15. It appears to be superior to the parametric methods in NONMEM. However, for determining the location of the support points, that option uses only the maximum aposteriori probability (MAP) Bayesian posterior values of the individual subjects studied, and then computes their probability. This leads to significant errors in locating the support points, as shown by Leary et al16. Because of this, the simplified nonparametric method in NONMEM is demonstrably inferior to the rigorous methods discussed above2,7-9.
Multple Model Dosage Design
The multiple support points in the rigorous NP population models obtained by estimating the entire parameter distributions2,7-9 permit multiple predictions of future serum concentrations and other responses. As a candidate regimen is presented to each population model support point, each future prediction obtained from each support point is weighted by its estimated probability. It is easy to calculate the weighted squared error with which any dosage regimen fails to hit a specific desired therapeutic target goal at the desired time. This optimization process continues iteratively until the regimen is found which specifically minimizes that expected weighted squared error. In this way one develops the regimen that now hits the target with maximum precision. This is known as multiple model (MM) dosage design17-19. MM design and MM Bayesian adaptive control are well known and widely used in the aerospace community for flight control and spacecraft guidance systems. One cannot control a system merely by the process of Bayesian forecasting. It requires real control, not simply forecasting. The MM-USCPACK software19 uses NP population modeling (now the Pmetrics software) and MM dosage design (now the RightDose software) to obtain maximally precise dosage regimens. It also uses MM Bayesian adaptive control. It is the combination of NP modeling and MM RightDose software that permits maximally precise MM Bayesian adaptive control, rather than the less capable parametric population modeling and maximum aposteriori probability (MAP) Bayesian adaptive control. MM Bayesian adaptive control develops dosage regimens, individualized for each patient, which achieve with maximum precision a specific target goal selected for each patient according to his/her perceived clinical need for the drug, including, for digoxin, a clinically selected target in either the central (serum) or, especially, in the peripheral (nonserum) compartment.
Instead of merely using a population modeling method with which to do a study, simply because it is available, investigators should examine the real capabilities of the many methods now available, both parametric and nonparametric, which have exact (rather than only approximate) calculations of the likelihood function, and that investigators justify in their work the specific scientific reasons why they have selected a particular population modeling method for use in their studies.
Analysis of Assay Errors and Weighting of Data
Weighting schemes used in fitting models to data have a most significant effect on the results obtained. It is often assumed that the drug assay error is only a small part of the total error involved in doing a study. If one does as many investigators do, examining various overall error models and then estimating parameter values of the model giving the best fit, one will never know how much of that overall error is due to the assay error and how much is due to all other factors in the clinical environment, such as the errors in preparing and giving the doses, errors in recording the times of doses and of drawing the blood samples, model mis-specification, and possibly changing parameter values during the period of data analysis. The real quantitative information of the assay error itself is all too often discarded once it is regarded as being acceptably precise.
Instead of using the assay percent coefficient of variation (CV%), as has usually been done to determine assay precision, one can first determine the standard deviation (SD) of the assay itself, expressed not as the percent coefficient of variation (CV%) but as the actual SD itself of each particular assay measurement. One must first get the SD of the assay anyway in order to calculate the CV%. If one obtains the assay SD, one can square that to get the variance of the measurement at that concentration. Then one can give weight to the assay concentration using the reciprocal of the assay variance at that point, to obtain the Fisher information of that data point20,21.
The method of determining the assay error as a polynomial function of replicate concentrations measured over the working range of the assay has been described by Jelliffe et al21. Further, if one does this, then one does not need to censor low measured concentrations perceived as having an unacceptably high CV%21, which are commonly regarded as being below the limit of quantification. There are many assays such as those for HIV, HCV, and HBV, for which, in addition to drug concentrations, there is no scientific reason whatever to censor and ignore any low values at all. Instead, with appropriate treatment, one really wishes to drive those measurements to zero, fully down into the machine noise (where the assay CV% is infinite), and to document this fact. Giving correct weight to the measured concentrations insures a model with maximally precise parameter values and distributions. This can be done easily and cost-effectively by determining the assay SD as a polynomial function of replicate measurements of several samples ranging from the blank to extremely high values21. The remaining error due to the environmental factors can then easily be estimated separately and distinctly from the previously determined assay error polynomial21.
For example, one can estimate gamma, in the MM-USCPACK and its new Pmetrics population modeling software22. Gamma is a multiplicative environmental error term. If gamma is 2.0, it means that the total noise, assay plus environmental noise, is twice the assay error. If so, one can be comforted, as the environmental error is relatively small. On the other hand, if gamma is 10.0, for example, it reveals considerable noise in the clinical part of the study, and one may wish to take steps to make that part of the study more precise. A defect of gamma is that it multiplies the assay error polynomial, further accentuating its polynomial curvature.
If desired, one can now choose instead to estimate an additive term which we call lambda, instead of the multiplicative term gamma. Estimating lambda is probably a better strategy than estimating gamma, as it does not multiply up the usual curvatures present in the assay error polynomial21. It examines lambda as an SD, as well as the SD of each measured concentration. It squares each SD to get their variances, adds them to get the total variance, and then takes the square root of that to reflect the overall SD present at that measurement time. In this way, the two error variances are more equitably added to reflect the total uncertainty present at the time each measurement was made, giving a better reflection of the relative combination of how the two errors, assay and environmental noises, act together to make the overall population model.
Modeling Digoxin
The most common clinical study of digoxin PK has been to use a 1-compartment model. However, Reuning et al4 and others23-27, 37 have clearly shown that digoxin has at least 2-compartment behavior, and, most significantly, that the pharmacological effect of the drug correlates, not with serum concentrations, but rather with drug amounts in the nonobservable but easily calculable peripheral nonserum compartment4. These important works generally appear not to have been appreciated.
The USC Laboratory of Applied Pharmacokinetics created an adult population model based upon the work of Reuning et al. In this model, there is an absorptive compartment into which oral doses are given, a central compartment into which intravenous infusions are given and from which serum concentrations are measured, and a peripheral nonserum compartment which reflects overall tissue concentrations. Since only serum concentrations can be measured, only the central (serum) compartment has a definite apparent volume of distribution. In contrast, concentrations in the peripheral compartment can never be observed. Only amounts of drug in that compartment can be calculated. In our model, these amounts are normalized by dividing them by the patient's total body weight, yielding estimated concentrations in the peripheral compartment as ug of drug per kg body weight.
We estimated the peripheral compartment concentrations resulting from standard dosage regimens given to patients regarded as being average, as well as the resulting D-optimal times to obtain blood samples. We developed software to calculate dosage regimens of digoxin to achieve selected target concentration goals at selected target times, in either the serum or in the peripheral compartment. For target trough serum concentrations of about 0.9-1.0 ng/ml, conventional dosage regimens of about 250 ug/day largely achieve these goals in average patients when renal function is normal, and one can see that the peak peripheral compartment concentrations are about 7 ug/kg5. This model has worked extremely well clinically in our hands for individualizing digoxin dosage regimens in patients of differing body weight and renal function who have regular sinus rhythm.
Digoxin Serum Concentrations
The range of serum digoxin concentrations generally regarded as being therapeutic is often said to be from about 0.5 to 2.0 ng/ml, and most patients in regular sinus rhythm (RSR) do well with trough serum concentrations of about 0.9 ng/ml. Most patients with toxicity have serum concentrations over 2.0 ng/ml. However, it is clear that quite a few patients tolerate serum digoxin concentrations well over 3 ng/ml, and actually as high as 6.5 ng/ml, without any toxicity28. In addition, patients with atrial fibrillation (AF) who have good atrioventricular nodal conduction often require serum concentrations of about 2.0 ng/ml for adequate control of ventricular rate29,30. Others have commented on the inadequacy of therapeutic serum concentrations to get good rate control in AF31. However, it seems not to have been considered by most cardiologists that patients with AF might require their own separate therapeutic ranges or target concentrations.
Rigid use of therapeutic ranges neglects the great variation in sensitivity of individual patients to digoxin, or to any drug. Doherty28 has also shown that patients may tolerate quite high serum digoxin concentrations, up to 6.5 ng/ml without toxicity. For example, I have seen a patient with AF who required a serum concentration of 8.0 ng/ml for adequate ventricular rate control, (without toxicity)5, and a colleague has had a patient who required 6.0 ng/ml to obtain the same effect32. This great variation in sensitivity, possibly due to genetic polymorphism in determining the binding constants of digoxin to membrane Na – K ATPase, seems to have been overlooked by many clinicians, who are taught to work within established guidelines, such as therapeutic ranges. Such ranges are usually never explicitly defined, except by eye, and are usually developed by committees who have never seen the particular patient under one's clinical care. Physicians should accept their individual clinical responsibility rather than evade it by blindly following such guidelines. They should look at each individual patient's clinical response, and should decide what serum compartment, or especially, what peripheral compartment target digoxin concentration appears best for each particular patient, according to his/her perceived need for the drug. As shown by Reuning et al4, it is what is in the tissue, on the receptor sites, or on the cell membrane that has both the therapeutic, and probably also, the toxic effects, and not the serum concentration itself.
Digoxin acts by competing with potassium for binding sites on the cell membrane Na–K ATPase. Inward flow of K is slowed. The cell loses K, gains Na, and through exchange with Na–Ca ATPase, the cell gains Ca. It is the greater availability of Ca that appears to result in the increased inotropic effect of digoxin. In addition, almost all the manifestations of digitalis toxicity are also seen in patients with hypercalcemia from any cause – the anorexia, nausea, vomiting, arrhythmias, delirium, and psychoses. The visual symptoms seen with digoxin toxicity may well be due to retinal cell ectopic activity, where they may fire several times when stimulated rather than only once. The released visual pigment apparently diffuses to surrounding areas and alters the color perception of adjacent retinal cells. In this way, it is my speculation that digitalis compounds may well facilitate the formation of afterimages in the retina, thus causing the many and varied visual symptoms.
Digoxin in Atrial Fibrillation
In addition to treating patients with regular sinus rhythm (RSR) in a stable steady state, there are also rapidly evolving clinical situations when one does not wish simply to achieve a final steady state target serum concentration goal. It is often clinically imperative to achieve and maintain a selected target concentration quite rapidly, especially in the peripheral compartment, as when one wishes to obtain good control of ventricular rate in patients with atrial fibrillation or flutter, or perhaps even to convert such a patient to sinus rhythm. After obtaining successful conversion, it is then imperative to decide upon the proper dosage regimen to maintain the peripheral concentration present when conversion was obtained. This clinical decision is what is all too often impossible to reach without guidance by PK/PD models and software.
One might perhaps consider carefully titrating a patient up to a target serum trough digoxin concentration of about 1.5 – 2.3 ng/ml for control of ventricular rate, and to perhaps a peak peripheral concentration of 9-13 ug/kg, and sometimes up to 18 ug/kg of body weight, at 7 hours after an oral dose, or 4 hours after an IV dose, for conversion to RSR. Watch the rate, watch for toxicity, and watch for conversion to RSR.
In 3 out of 4 cases that I have been involved with, conversion to sinus rhythm was achieved by careful clinical titration. In the fourth, who was also hyperthyroid and weighed 136 kg, the rate was controlled, but it required doses up to 1.0 mg/day, beyond which others were not willing to go. His serum concentrations were mostly 1.5 to 2.0 ng/ml, though one was 2.7 ng/ml. His computed peripheral concentrations never rose over 7.0 ug/kg.
One of the above patients who converted was on digitoxin, and had had chronic stable atrial flutter with 2/1 atrioventricular block for the past three years. Calculated peripheral compartment digitoxin concentration in this patient at the time of conversion was and thereafter was maintained at 18 ug/kg. Serum digitoxin concentrations were peaks of about 55 and troughs of about 45 ng/ml on an average maintenance dose of 0.7 mg/day. He had a significant problem of reduced bioavailability.
In these three patients who converted to RSR, peripheral compartment glycoside concentrations ranged from 9.5 to 18 ug/kg
In another illustrative clinical example21, a patient with new onset atrial fibrillation was converted three times with titrated doses of digoxin, only to revert back to AF twice because an adequate maintenance dose was not given until after the situation was analyzed with our software and a successful maintenance dosage regimen was then developed for him. Finding the correct maintenance dose without such models is a real problem clinically because the relationships between doses, serum concentrations, and peripheral compartment concentrations cannot be seen or evaluated quantitatively. Models and software are required.
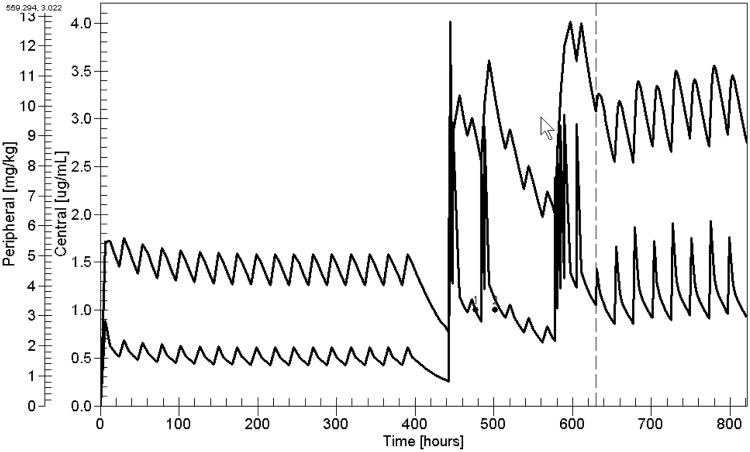
Figure 3 below analyzes the data of that patient, previously described by Jelliffe et al.21. The patient was a 58 year old man, 68 in tall, weighing 75 kg, with a stable serum creatinine of 0.8 mg/dL. He had been in a steady state in regular sinus rhythm (RSR) on chronic oral digoxin maintenance therapy of 0.25 mg/day. However, the patient missed a dose one day, and developed new onset rapid AF. He was titrated with several IV doses of digoxin, while being observed for control of his ventricular rate, development of toxicity, or possible conversion to regular sinus rhythm (RSR). After 4 IV doses of 0.25 mg each, given over 1 day, he converted to RSR.
Figure 3.
The three measured serum concentrations (dots) and their weighted average estimated values at the other times (the thick line), using the fitted 2 compartment digoxin model. At left, estimated concentrations (trough = 0.5 ug/L) before onset of atrial fibrillation, Right of center, the dip in estimated concentrations from missing his dose that day, associated with the appearance of new onset atrial fibrillation. The three regions of higher serum concentrations reflect the three courses of extra intravenous digoxin that resulted in conversion to sinus rhythm three times, followed by recurrence of atrial fibrillation twice. The patient was in sinus rhythm for the third time at the right end of the plot, when a new dosage regimen, based on this analysis, was then developed for him. The dashed line shows the weighted average estimated peripheral compartment values, using the 2 compartment digoxin model fitted to the serum concentration data. At left of center, estimated concentrations before onset of atrial fibrillation. Right of center, the dip in estimated concentrations from missing his dose that day, resulting in the appearance of new onset atrial fibrillation. The three regions of higher peripheral concentrations reflect the three courses of extra intravenous digoxin that resulted in conversion to sinus rhythm, followed by recurrence of atrial fibrillation twice. The patient was in RSR when his peak peripheral concentrations ranged from 10 to 13 ug/kg. Labels and axes as in Figure 2.
The next clinical question was what dosage regimen to give next to keep him in the RSR that had once again been achieved. His previous maintenance dose of 0.25 mg/day was again given, as it was not clear whether his requirements for digoxin had really changed or not. However, he excreted his extra digoxin, and went back into AF within two days on that maintenance regimen, as it did not in fact maintain the peripheral compartment concentration at the value associated with successful conversion for him. At this point a serum digoxin sample was taken 11 hours and 15 minutes after the last dose. It was 1.0 ng/ml, and the patient was in AF at that time. The patient was again titrated with extra IV digoxin. He again converted to RSR, this time after only two IV doses of 0.25 mg given three hours apart. A serum sample was obtained 14 hours 20 minutes after the second of the above two doses, when he was in RSR. The concentration, surprisingly, was exactly the same – 1.0 ng/ml.
The important clinical question is - how can someone be in AF at one time and in RSR at another time and have exactly the same serum concentration? It is strongly felt by many cardiologists that serum digoxin concentrations do not correlate at all well with clinical behavior. The patient described here is a striking example of this.
Clinical Interpretation and Management
Two related questions are worth asking. First, was the patient in a true steady state each time before each serum sample was taken? The answer is clearly no. At the time of the first sample (1.0 ng/ml), he had just slipped back into AF. At the second, (also 1.0 ng/ml) he had just received the extra digoxin doses and had just converted back to RSR. The same for the third sample, which was 1.2 ng/ml. So he was not at all in the usual steady state to permit the conventional interpretation of the relationship between trough serum digoxin concentrations and clinical behavior. Second, were the serum samples taken at the same time after the dose? Again, no.
The clinical problem once again was what dosage regimen to decide upon in order to maintain the patient in RSR. After his second conversion to RSR, he was again put back on the same regimen of 0.25 mg/day. After three days, the patient again reverted back to AF. At that time he had only 7.0 ug/kg in his peripheral compartment. He was again titrated with five doses of 0.25 mg of IV digoxin over the next 36 hours. He again converted, for a third time, to RSR. At that time he had 12.7 ug/kg in his peripheral compartment after the pharmacokinetic analysis. There was no clinical evidence of toxicity. A serum sample drawn 14 hours 45 minutes after the fourth of those doses was 1.2 ng/ml, and he was in RSR. There was clearly no correlation between the raw data of the measured serum concentrations and the patient's clinical behavior. He was in AF with a concentration of 1.0, and in RSR with concentrations of 1.0 and 1.2 ng/ml. It was at this time that the telephone consultation with us was done.
Such puzzling clinical behavior is typical of that seen in many patients who are being monitored by measuring occasional serum digoxin concentrations and looking for empirical clinical correlations with them. They simply are not there, and many internists and cardiologists strongly feel that monitoring digoxin serum concentrations is simply not useful. They are quite correct, if one only looks at the raw data as presented above, and/or if one uses only a 1-compartment pharmacokinetic model of digoxin which can only consider serum concentration data.
However, if one uses that raw TDM data, analyzes it with the above 2-compartment model based on the work of Reuning et el4, and uses software to permit making an individualized patient pharmacokinetic model by using Bayes' theorem and fitting the model to the patient's serum concentration data19, one can see the plot of that patient's events in the peripheral compartment, as shown in Figure 3.
The relationship between the patient's clinical behavior and the profile of his measured and estimated serum concentrations was not at all clear (raw data = AF at 1.0, and RSR also at 1.0 and at 1.2 ng/ml), as in Figure 3). However, the relationship between his clinical behavior and the profile of his computed peripheral compartment concentrations was immediately easy to see and understand. For some reason, not clinically clear, the patient's requirements for digoxin really had changed, and he now remained in RSR only when his computed peripheral compartment concentrations ranged between 10 and 13 ug/kg, not down to about 5 ug/kg, as they had been before the patient missed his dose and developed AF, as shown in Figures 3 and 4.
Figure 4.
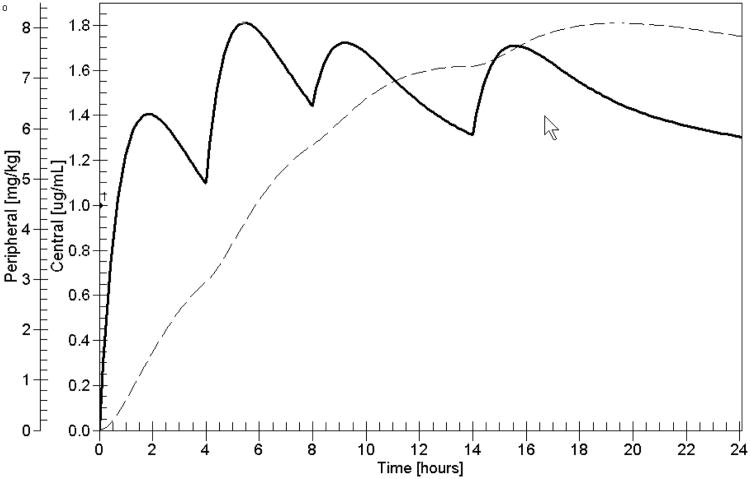
Plot of estimated serum and peripheral compartment digoxin concentrations (ug/kg) on the planned future regimen (to the right of the vertical dashed line between past and future). Labels and axes as in Figure 2. Peak concentrations are close to the target of 11.5 ug/kg. Estimated trough serum concentrations are close to 1.1 ug/L.
Based on this analysis, coupled with appraisal of the patient's clinical behavior, a target peak goal in the peripheral compartment of 11.5 ug/kg 7 hours (the usual peak time after an oral dose) was selected. An ideal dosage regimen of 468 ug, followed by 578 ug, and then by 572 ug/day was computed by the RightDose software. This was judgmentally revised to a first dose of 250 ug, and then (since 572 ug was about halfway between 500 and 625 ug), to 625 and 500 ug on alternate days, which averages 562.5 ug/day. Clinical observation (along with Figure 3) had shown that his previous maintenance dose of 250 ug/day was no longer able to maintain him in RSR, that his estimated trough serum concentrations when he was previously in RSR were only about 0.5 ng/ml back then, and that his estimated peak peripheral concentrations back then were only about 5.0 ug/kg. On his new dosage regimen, his estimated trough serum concentrations ranged from 0.88 ng/ml the first day to 0.92 after one week, and the target peripheral compartment goal of 11.5 ug/kg was predicted to be closely approximated. He was given the revised regimen described above. The target goal was closely approximated, as shown in Figure 4. See Jelliffe et al21 for a full discussion
On the above revised regimen, with events predicted as in Figure 4, the patient remained in RSR, and was able to leave the hospital in RSR, whereas a full week of therapy without such software assistance had been unsuccessful in maintaining the RSR which had already been achieved before on two separate occasions before, but not successfully maintained. Two weeks later, still on the above regimen, he was still in RSR when seen in the follow-up clinic. Unfortunately, no serum sample was obtained.
Literature Review
It is described in the literature that digoxin is no better than placebo for converting patients with atrial fibrillation to sinus rhythm. The study by Falk et al33 is widely cited as having shown this. The problem is that the study was extremely underpowered. There were only 18 patients each in both the study arm and control arm, making it almost impossible to detect any significant difference between them. Further, they gave digoxin only in the form of a fixed protocol, rather than by using thoughtful clinical titration, and did not report the age, weight, or renal function of their patients. Eight of 18 placebo patients spontaneously converted within 24 hours, compared with 9 of 18 in the digoxin arm. It is quite possible that Falk et al did not give enough digoxin to obtain the desired effect, as discussed below.
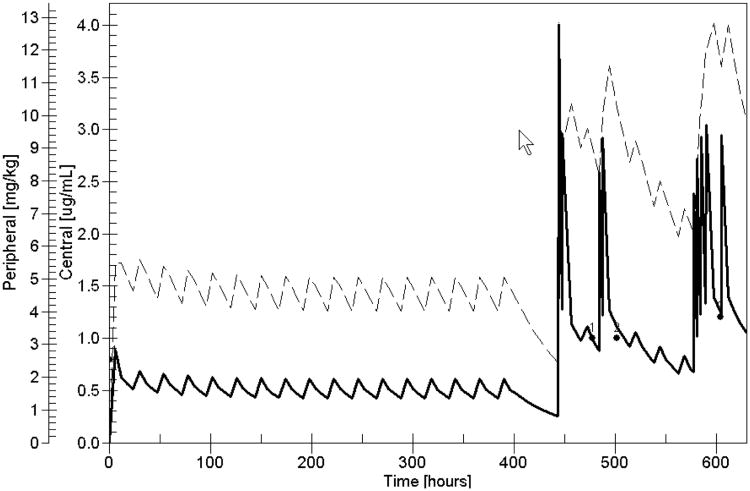
If one assumes a 65 year old man, 70 inches tall, weighing 70 kg, with a serum creatinine of 1.0 mg/dL, his estimated creatinine clearance34 is 69mL/min/1.73 m2. If one uses the RightDose software and the oral digoxin protocol described by Falk et al which was to give 0.6 mg orally at first, then 0.4 mg at 4 hours, followed by 0.2 mg at 8 hours, and finally 0.2 mg at 14 hours, Figure 2 (thick black line) shows the resulting predicted trajectory of the weighted average estimated serum concentrations over the first 24 hours. The highest predicted serum concentration is 1.8 ng/ml, and the final concentration is 1.4 ng/ml, 10 hours after the last dose above.
Figure 2.
Plot of estimated serum concentration profile (thick black line) and peripheral compartment profile (dashed line) over 24 hours when the regimen given by Falk et al33 was given to the patient described above. All values are in the range useful mainly for patients with RSR. No clear relationship between doses, serum concentrations, and clinical response is seen from the serum concentration profile. Note that peripheral concentrations correlate well with the additive effect of each dose, but rise only to 8 ug/kg, only a little above the 7 ug/kg at which most patients in RSR do well. Vertical axis: central serum concentrations in ug/L, NOT ug/ml as shown by the not so flexible software. Peripheral compartment concentrations in ug/kg, NOT mg/kg as shown by the not so flexible software. Horizontal axis: hours into the regimen.
Figure 2 also shows the time course of the estimated digoxin concentrations in the peripheral nonserum compartment, based on the model of Reuning et al4. The highest peripheral concentration reached was 8.0 ug/kg, only a little higher than the 7.0 ug/kg associated with reasonable therapy for patients in congestive failure with RSR, and with a predicted steady state trough serum concentration of 0.9 – 1.0 ng/ml 24 hours after the last dose.
Another interesting study was that of the DAAF Trial Group35 in which 239 patients with new onset AF were given intravenous digoxin. Their average age was 66.2 years, and weight was 78.2 kg. Half were male and half female. They received intravenous digoxin (duration of infusion not stated) at average doses of 0.455 mg, 0.308 mg, and 0.318 mg at 0, 2 and 6 hours into the regimen respectively. If one assumes that their average serum creatinine was 1.0 mg/dL, and gives the above regimen intravenously, the results using the RightDose software showed a predicted peak serum concentration of 3.91 ng/ml at the end of the infusion of the 2nd dose and 3.90 at the end of the 3rd dose. The predicted weighted average peak concentration in the peripheral compartment reached 9.23 ug/kg at 9.25 hours into the regimen. The estimated 95% distance ranged from 7.9 to 11.0 ug/kg. This is only slightly higher than that predicted from the study of Falk above. The DAAF group found a significant relationship between the concentration of digoxin in their peripheral compartment with regard to slowing of ventricular rate in patients with AF, but was not able to find such a relationship with regard to conversion to RSR. Again it is likely in retrospect that they did not give enough drug, only reaching a peripheral concentration of 9.23 ug/kg.
Another study by Jordaens et al36 examined still higher doses in 19 patients randomized to IV digoxin and 20 to placebo. Average body weight was 73 kg. They gave 0.75 mg at the start, over 10 min, then 0.25 mg over 5 min at 4 hours, and another 0.25 mg over 5 min at 8 hours into the regimen. Nine digoxin and 8 placebo patients converted to RSR. Digoxin also slowed the ventricular rate significantly. If one gives the regimen they received to a simulated patient of their stated average age, and weight, and assumes a height of 70 in, male gender, and serum creatinine of 1.0 mg.dL, the peak predicted serum concentrations using the population model in the RightDose software were 6.9 ng/ml at the end of the first infusion. The next highest peak was 3.89 ng/ml at 8.0 hours into the regimen. Peak concentrations in the peripheral compartment were 11.23 ug/kg at 11.55 hours into the regimen. In this study, they clearly gave more drug, and had higher estimated concentrations in the peripheral compartment, using the RightDose software.
Calculated peripheral compartment digoxin concentrations in these patients at the time of conversion ranged from a low of 9.5 to a high of 11.23 ug/kg. In none of these three studies, was individualized clinical titration for each patient done, nor was renal function evaluated.
Weiner et al37 examined the clinical course of patients with acute AF treated with rapid IV digitalization. Renal function was evaluated but not stated. Body weight and the duration of IV infusion of digoxin were not stated. An initial dose of 0.5 mg was given, another 0.5 mg IV at 4 hours, then 0.25 mg at 8 hours, and finally 0.25 mg at 12 hours. In that nonrandomized, non placebo-controlled observational study, 40 of 47 episodes of AF in 45 patients were converted to RSR. Assuming our 65 year old man, 70 kg, 70 in tall, with a serum creatinine of 1.0 mg/dL (creatinine clearance of 69 ml/min/1.73 M2), predicted weighted average peak serum concentrations of 5.49 ng/ml were reached at 4.2 hours into the regimen at the end of the second IV infusion. The next peak was 4.33 ng/ml at 12.2 hours (the end of the last infusion). Weighted average predicted concentrations in the peripheral compartment peaked at 13.9 ug/ml at 15.32 hours into the regimen.
Hornestam et al have also modeled digoxin as a 2 compartment model with an effect compartment38. In their placebo-controlled study of patients with AF, they were not able to find a relationship to conversion to RSR, but did find an effect with respect to the reduction of ventricular rate. Using our model, peripheral concentrations peaked at 11 ug/kg. Slowing of ventricular rate was proportional to the baseline ventricular rate at start of therapy, and was linearly related to the computed digoxin concentration at the effect site, similar to the relationship between computed concentration in the peripheral compartment and inotropic effect found by Reuning et al4. It thus appears that both contractility and slowing of ventricular rate in patients with AF appear linearly related to computed digoxin concentrations in a peripheral nonserum location, as does conversion to RSR.
Conclusion
It is difficult to see so many thoughtful investigators strive for so little when they use only steady state trough serum data to make a population model, analyze it with a parametric method which does not have exact likelihoods, and then seek only to predict steady state serum concentrations of a drug, especially this important drug. So much more has been4 and can be done. It is not difficult, using optimal experimental design for TDM and better methods for modeling and control, to do it.
Most encouraging clinical results have been obtained using a 2-compartment model and controlling target peak peripheral compartment digoxin concentrations with regard to converting patients with atrial fibrillation to regular sinus rhythm. Patient behavior in the cases described here correlated well and immediately with the behavior of their individualized 2-compartment digoxin models. This is a new and provocative finding. It strongly suggests that digoxin does convert some patients with atrial fibrillation, and even with chronic established atrial flutter5, to regular sinus rhythm, and maintain it. A 1-compartment model simply cannot show these important clinical PK/PD relationships, and cannot lead to the same informed clinical dosage decisions.
Modeling approaches and strategies for development of optimally individualized dosage regimens can result in significantly more capable clinical models and in improved patient care. Much further work along these most interesting lines needs to be done.
Acknowledgments
Supported by NIH grants EB005803 and GM068968
Footnotes
Financial disclosure: The author has no financial relationship with any pharmaceutical company.
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
- 1.Jelliffe R, Gomis P, Schumitzky A. Technical Report. Laboratory of Applied Pharmacokinetics, USC Keck School of Medicine; Los Angeles CA: 1990. A Population Model of Gentamicin made with a new Nonparametric Algorithm; pp. 90–4. [Google Scholar]
- 2.Schumitzky A. Nonparametric EM Algorithms for Estimating Prior Distributions. App Math and Computation. 1991;45:143–157. [Google Scholar]
- 3.D'Argenio D. Optimal Sampling Times for Pharmacokinetic Experiments. J Pharmacokin Biopharmaceut. 1981;9:739–756. doi: 10.1007/BF01070904. [DOI] [PubMed] [Google Scholar]
- 4.Reuning R, Sams R, Notari R. Role of Pharmacokinetics in Drug Dosage Adjustment 1 Pharmacologic Effects, Kinetics, and Apparent Volume of Distribution of Digoxin. J Clin Pharmacol. 1973;13:127–141. doi: 10.1002/j.1552-4604.1973.tb00074.x. [DOI] [PubMed] [Google Scholar]
- 5.Jelliffe R. Unpublished data [Google Scholar]
- 6.Beal S, Sheiner L. NONMEM Project Group. NONMEM User's Guide. University of California; San Francisco: 1995. [Google Scholar]
- 7.Mallet A. A Maximum Likelihood Estimation Method for Random Coefficient Regression Models. Biometrika. 1986;73:645–656. [Google Scholar]
- 8.Bustad A, Terziivanov D, Leary R, Port R, Schumitzky A, Jelliffe R. Parametric and Nonparametric Population Methods: Their Comparative Performance in Analyzing Clinical Data Set and Two Monte Carlo Simulation Studies. Clin Pharmacokin. 2006;45:365–383. doi: 10.2165/00003088-200645040-00003. [DOI] [PubMed] [Google Scholar]
- 9.Premaud A, Weber L, Tonshoff B, Armstrong V, Oellerich M, Urien S, Marquet P, Rousseau A. Population Pharmacokinetics of mycophenolic acid in pediatric renal transplant patients using parametric and nonparametric approaches. Pharmacological Research. 2011;63:216–224. doi: 10.1016/j.phrs.2010.10.017. [DOI] [PubMed] [Google Scholar]
- 10.Bertsekas D. Dynamic Programming: deterministic and stochastic models. Englewood Cliffs (NJ): Prentice-Hall; 1987. pp. 144–146. [Google Scholar]
- 11.Bulitta J, Bingolbali A, Shin B, Landersdorfer C. Development of a new prre- and post- processing tool (SADAPT – TRAN) for Nonlinar Mixed Effect Modeling is S-ADAPT. AAPS J. 2011;2:201–2121. doi: 10.1208/s12248-011-9257-x. Epub 2011, Mar 3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Chan P, Jacqmin P, Lavielle M, McFayden L, Weatherly B. The use of the SAEM algorithm in MONOLIX software for estimation of population pharmacokinetic – pharmacodynamic – viral dynamics parameters of maraviroc in asymptmatic HIV subjects. J Pharmacokin Pharmacodyn. 2011;38:41–61. doi: 10.1007/s10928-010-9175-z. Epub 2010 Nov 19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Lindsay B. The Geometry of Mixture Likelihoods: A General Theory. Annals of Statistics. 1983;11:86–94. [Google Scholar]
- 14.Savic R, Kjellson, Karlsson M. Evaluation of the Nonparametric Estimation Method in NONMEM VI. Europ J Pharmaceut Sci. 2009;37:27–35. doi: 10.1016/j.ejps.2008.12.014. [DOI] [PubMed] [Google Scholar]
- 15.Baverel P. Ph D Dissertation. University of Uppsala; Sweden: Mar 11, 2011. Development and Evaluation of Nonparametric Mixed Effects Models. [Google Scholar]
- 16.Leary R, Chittenden J. A Nonparametric Analogue to POSTHOC Estimates for Exploratory Data Analysis; A poster presentation at the Population Approach Group Europe Meeting; Marseille, France. June 2008. [Google Scholar]
- 17.Jelliffe R, Bayard D, Milman M, Van Guilder M, Schumitzky A. Achieving Target Goals most Precisely using Nonparametric Compartmental Models and “Multiple Model” Design of Dosage Regimens. Ther Drug Monit. 2000;22:346–353. doi: 10.1097/00007691-200006000-00018. [DOI] [PubMed] [Google Scholar]
- 18.Bayard D, Jelliffe R, Schumitzky A, Millman M, Van Guilder M. Selected Topics in Mathematical Physics, Professor R Vasudevan Memorial Volume. Allied Publishers Ltd.; Madras, India: 1995. Precision Drug Dosage Regimens Using Multiple Model Adaptive Control: Theory, and Application to Simulated Vancomycin Therapy; pp. 407–426. [Google Scholar]
- 19.Jelliffe R, Bayard D, Schumitzky A, Milman M, Jiang F, Leonov S, Gandhi A, Botnen A. A New Clinical Software Package for Multiple Model (MM) Design of Drug Dosage Regimens for Planning, Monitoring, and Adjusting Optimally Individualized Drug Therapy for Patients; Presented at the 4th International Meeting on Mathematical Modeling, Technical University of Vienna; Vienna, Austria. February 6, 2003. [Google Scholar]
- 20.DeGroot M. Probability and Statistics. 2nd. Addison-Wesley Publishing Co; 1989. pp. 420–423. [Google Scholar]
- 21.Jelliffe RW, Schumitzky A, Van Guilder M, Liu M, Hu L, Maire P, Gomis P, Barbaut X, Tahani B. Individualizing Drug Dosage Regimens: Roles of Population Pharmacokinetic and Dynamic Models, Bayesian Fitting, and Adaptive Control. Ther Drug Monit. 1993;15:380–393. [PubMed] [Google Scholar]
- 22.Neely M. Pmetrics A software package in R for parametric and nonparametric population modeling and Monte Carlo simulation. Available from www.lapk.org.
- 23.Kramer W, Lewis R, Cobb T, Forester W, Visconti J, Wanke L, Boxenbaum H, Reuning R. Pharmacokinetics of Digoxin: Comparison of a two and a three compartment model in man. J Pharmacokin Biopharmaceut. 1974;2:299–312. doi: 10.1007/BF01061404. [DOI] [PubMed] [Google Scholar]
- 24.Sumner D, Russell A. Digoxin Pharmacokinetics: Multicompartmental Analysis and its Clinical Implications. J Clin Pharmacol. 1976;3:2221–229. doi: 10.1111/j.1365-2125.1976.tb00596.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lisalo E. Clinical Pharmacokinetics of Digoxin. Clin Pharmacokin. 1977;2:1–16. doi: 10.2165/00003088-197702010-00001. [DOI] [PubMed] [Google Scholar]
- 26.Wettrell G. Distribution and Elimination of Digoxin in Infants. European J Clin Pharmacol. 1977;11:329–335. doi: 10.1007/BF00566529. [DOI] [PubMed] [Google Scholar]
- 27.Morselli P, Assael B, Gomeni R, Mandelli M, Marini A, Reali E, Visconti U, Sereni F. Digoxin Pharmacokinetics During Human Development. In: Morselli P, Garattini S, Sereni F, editors. Basic and Therapeutic Aspects of Perinatal Pharmacology. Raven Press; New York: 1975. [Google Scholar]
- 28.Doherty J. Digitalis Glycosides – Pharmacokinetics and their Clinical Implications. Ann Int Med. 1973;79:229–238. doi: 10.7326/0003-4819-79-2-229. [DOI] [PubMed] [Google Scholar]
- 29.Chamberlain D, White R, Howard M, Smith T. Plasma Digoxin Concentrations in Patients with Atrial Fibrillation. Brit Med J. 1970;3:429–432. doi: 10.1136/bmj.3.5720.429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Chamberlain D. Plasma Digoxin Concentrations as a Guide to Therapeutic Requirements. In: Davies D, Prichard B, editors. Biological Effects of Drugs in Relation to their Plasma Concentrations. University Park Press; 1973. pp. 135–143. [Google Scholar]
- 31.Goldman S, Probst P, Selzer A, Cohn K. Inefficacy of “Therapeutic” Serum Levels of Digoxin in Controlling the Ventricular Rate in Atrial Fibrillation. Am J Cardiol. 1975;35:651–655. doi: 10.1016/0002-9149(75)90051-x. [DOI] [PubMed] [Google Scholar]
- 32.Richard Lueker MD. personal communication. Albuquerque NM: [Google Scholar]
- 33.Falk R, Knowlton A, Bernard S, Gotlieb N, Battinelli N. Digoxin for converting atrial fibrillation to sinus rhythm A random double-blinded trial. Ann Int Med. 1987;4:503–506. doi: 10.7326/0003-4819-106-4-503. [DOI] [PubMed] [Google Scholar]
- 34.Jelliffe R. Estimation of Creatinine Clearance in Patients with Unstable Renal Function, without a Urine Specimen. Am J Nephrology. 2002;22:320–324. doi: 10.1159/000065221. [DOI] [PubMed] [Google Scholar]
- 35.The Digitalis in Acute Atrial Fibrillation (DAAF) Trial Group - Intravenous digoxin in acute atrial fibrillation. Results of a randomized, placebo-controlled multicentre trial in 239 patients. Eur Heart J. 1997;18:649–654. doi: 10.1093/oxfordjournals.eurheartj.a015311. [DOI] [PubMed] [Google Scholar]
- 36.Jordaens L, Trouerbach J, Calle P, Taviernier E, Derycke E, Vertongen P, Bergez B, Vanderkerckhove Y. Conversion of atrial fibrillation to sinus rhythm and rate control by digoxin in comparison to placebo. Eur Heart J. 1997;18:643–648. doi: 10.1093/oxfordjournals.eurheartj.a015310. [DOI] [PubMed] [Google Scholar]
- 37.Weiner P, Bassan M, Jarchovsky J, Iusim S, Plavnick L. Clinical course of acute atrial fibrillation treated with rapid digitalization. Am Heart J. 1983;105:223–227. doi: 10.1016/0002-8703(83)90517-3. [DOI] [PubMed] [Google Scholar]
- 38.Hornestam B, Jerling M, Karlsson M, Help P. Intravenously administered digoxin in patients with acute atrial fibrillation: a population pharmacokinetic/pharmacodynamic analysis based on the Digitalis on Acute Atrial Fibrillation trial. Eur J Clin Pharmacol. 2003;58:747–755. doi: 10.1007/s00228-002-0553-3. [DOI] [PubMed] [Google Scholar]