History and clinical signs
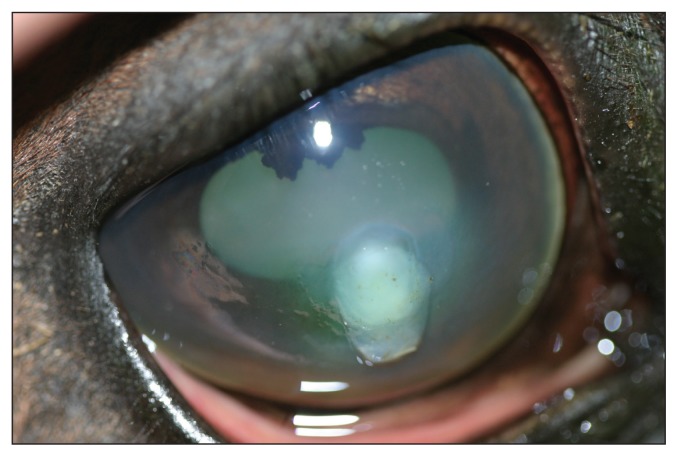
A 10-year-old, castrated male Quarter horse was examined at the ophthalmology service at the Western College of Veterinary Medicine related to a 3-day history of squinting, ocular discharge, and a white spot on the cornea of the right eye. The horse was currently being treated with topical BNP ophthalmic ointment, and a systemic non-steroidal anti-inflammatory drug (NSAID), Flunixin meglumine (Flunazin; Vétoquinol Canada, Lavaltrie, Quebec). The menace responses, and palpebral and occulocephalic reflexes were present bilaterally. The direct and consensual pupillary light reflexes were present bilaterally. Schirmer tear test (Schirmer Tear Test Strips; Alcon Canada, Mississauga, Ontario) values were 35 and 20 mm/min in the right and left eye, respectively. The intraocular pressures were estimated with a rebound tonometer (Tonvet; Tiolat, Helsinki, Finland) and were 7 and 17 mmHg in the right and left eye, respectively. Fluorescein staining (Fluorets; Bausch & Lomb Canada, Markham, Ontario) was positive over a 6-mm oval area in the central right cornea. On direct examination there was moderate blepharospasm, conjunctival hyperemia, and mucopurulent ocular discharge in the right eye. Biomicroscopic examination (Osram 64222; Carl Zeiss Canada, Don Mills, Ontario) of the cornea revealed a diffusely edematous, central, 6 mm, oval, gray-white, soft, slighty raised, and ulcerated lesion. The right pupil was miotic and moderate aqueous flare was present. The right pupil did not completely dilate following application of 0.5% tropicamide (Mydriacyl; Alcon Canada). Indirect ophthalmoscopic (Heine Omega 200; Heine Instruments Canada, Kitchener, Ontario) examination was normal bilaterally. A photograph of the right eye following mydriasis is provided for your assessment (Figure 1).
Figure 1.
Photograph of the right eye of a 10-year-old Quarter horse.
What are your clinical diagnosis, differential diagnoses, therapeutic plan, and prognosis?
Discussion
Our clinical diagnosis was a melting corneal ulcer and anterior uveitis in the right eye. A melting ulcer is a form of complex corneal ulceration. This is a clinical category of corneal ulcers which includes those that are infected, melting, and/or deep/perforated. Melting is more appropriately referred to as keratomalacia. Keratomalacia occurs due to enzymatic breakdown of the cornea (1,2). Microbial enzymes, such as collagenases and proteinases incite dissolution of the corneal intercellular ground substance and collagen lamellae. Neutrophils, attracted by chemotactic factors invade the corneal stroma, then degranulate and release additional degradative proteinases (1,2). Progressive stromal necrosis can result in rapid, increasing depth of the stromal lesion.
The clinical manifestations of a melting corneal ulcer include photophobia, blepharospasm, corneal edema, lacrimation, and often a purulent ocular discharge. There is frequently a yellow/white infiltrate of inflammatory cells in the ulcer bed. In addition, the corneal stroma becomes opaque, soft, and liquid-like. Melting corneal ulcers, like all complex corneal ulcers, are accompanied by anterior uveitis. Manifestations of anterior uveitis include miosis, ciliary spasm causing pain and photophobia, lacrimation, aqueous flare, and a lowered intraocular pressure.
The diagnosis of a melting corneal ulcer is based on clinical manifestations and positive fluorescein staining. Further diagnostic testing in all cases of complex corneal ulcers should include aerobic and anaerobic bacterial and fungal culture and sensitivities and corneal ulcer cytology. Cultures and scrapings for cytology must be taken directly from the corneal ulcer to obtain meaningful results. If surgery is part of the therapeutic plan, keratectomy specimens removed at the time of surgery are submitted for histopathology and laboratory analysis for potential microbial colonization of these lesions.
Melting ulcers are ocular emergencies as progression may result in loss of the cornea and eye within 24 to 48 h. Progression of melting ulcers may result in corneal perforation and development of septic endophthalmitis. Treatment of all complex corneal ulcers requires aggressive medical therapy, often in combination with surgical therapy (3,4). The choice of antimicrobial is most appropriately made based upon the results of culture and sensitivity. However, results of cultures are often not available for 48 to 72 h following submission. Cytologic examination may aid in identification of bacterial or fungal organisms and may be useful in directing initial therapy while awaiting culture results. Pseudomonas spp. are the most notorious organisms associated with melting ulcers. Tobramycin or amikacin are good antibiotic choices to initially treat a melting ulcer due to the susceptibility of most Pseudomonas spp. (5). Frequency of administration of antimicrobials in complex ulcers should be every 1 to 4 h with the higher frequencies used in severely infected or melting ulcers.
Anticollagenases are required for treatment of keratomalacia. There are several different anticollagenases reported for use in melting ulcers including autologous serum, 10% N-acetylcysteine, 0.05% potassium EDTA, and tetracycline antibiotics (2). However, the most commonly used, readily available, and broad-spectrum anticollagenase is autologous serum. Serum is obtained from the patient and must be stored and handled in a sterile manner to prevent bacterial growth. It may be kept in the refrigerator and should be replaced with fresh serum at least every 8 d (1,2). Anticollagenases are most often applied every hour for the first 24 h or until stromal liquefaction is halted, and then frequency of administration is tapered.
In addition to antimicrobial and anticollagenase therapy, control of uveitis is essential. The mainstay of treatment for uveitis is a combination of anti-inflammatory and anticholinergic therapy. Systemic non-steroidal anti-inflammatory drugs (NSAIDs) should be used to reduce pain and inflammation. Topical NSAIDs applied up to 4 times daily are also recommended to reduce anterior uveitis in cases of complex corneal ulceration. Topically applied anticholinergics (1% to 2% atropine) are useful for 3 reasons: they reduce protein and cellular leakage from inflamed uveal blood vessels, they dilate the pupil which protects the eye from development of posterior synechia, and they relax ciliary muscle spasm, which is a major factor in discomfort associated with uveitis (3).
Following initiation of appropriate medical treatment, prompt referral to an ophthalmologist for potential surgery is recommended in all cases of complex corneal ulceration. Infected and melting ulcers benefit from a keratectomy to remove infected and necrotic cornea and this is usually followed by placement of a conjunctival or corneal graft (3,4). The most commonly performed grafting procedure in these cases is the conjunctival pedicle graft in which the base of the graft retains a connection to the bulbar conjunctiva. The benefits of the conjunctival pedicle graft include replacement of tissue to strengthen the corneal defect and the continued presence of a blood supply. This is useful to provide the affected cornea with the antibacterial, antifungal, antiprotease, and anticollagenase properties of serum. The deeper layers of the graft provide immediate fibroblasts and collagen with which to rebuild the corneal stroma (3,4). Medical therapy is initiated to stabilize the corneal disease prior to surgery to reduce protease digestion of the absorbable sutures that will hold the graft in place (usually 12 to 24 h before surgery) and continued after surgery for 3 to 4 wk (3,4).
Treatment of this horse was initiated with topical Tobramycin 0.3% (Tobrex; Alcon Canada), q4h. Autologous serum was also applied q4h. A topical NSAID, diclofenac sodium 0.1% (Voltaren; Novartis, Mississauga, Ontario), q6h and a systemic NSAID, Flunixin meglumine (Flunazin; Vétoquinol Canada), 1.1 mg/kg body weight (BW), q12h, IV were initiated to reduce intraocular inflammation. Topical atropine sulphate 1% (Isopto-atropine; Alcon Canada) was administered q6h. The eye was treated medically until surgery the following day at which time the abnormal corneal tissue was removed by lamellar keratectomy. This tissue was submitted for histopathologic examination for bacterial and fungal organisms. A vascularized conjunctival pedicle graft was sutured into the corneal defect. A subpalpebral lavage system (Mila International, Florence, Kentucky, USA) was placed to facilitate post-operative medical therapy.
Results of corneal cultures were negative for bacterial and fungal organisms in this case. Cytologic and histopathologic examinations revealed suppurative keratitis but organisms were not identified. Corneal cultures may be negative either due to superficial culture collections that miss deeper organisms or previous use of antimicrobials before cultures are attempted. Topical and systemic medical therapies were continued for 3 wk following surgery, after which re-evaluation revealed a comfortable and sighted eye. The conjunctival graft was healing and incorporated into the cornea. The remainder of the ocular examination was normal. The subpalpebral lavage system was removed and all ocular medications were discontinued.
The prognosis for any complex corneal ulcer is guarded as there is the potential for rapid progression. Early and accurate diagnosis and instituting aggressive medical therapy contribute greatly to a successful outcome. A combination of medical and surgical therapy is often required in the management of complex corneal ulcers.
Footnotes
Use of this article is limited to a single copy for personal study. Anyone interested in obtaining reprints should contact the CVMA office (hbroughton@cvma-acmv.org) for additional copies or permission to use this material elsewhere.
References
- 1.Brooks DE. Inflammatory stromal keratopathies: Medical management of stromal keratomalacia, stromal abscesses, eosinophilic keratitis and band keratopathy in the horse. Vet Clin North Am Equine Pract. 2004;20:345–360. doi: 10.1016/j.cveq.2004.04.007. [DOI] [PubMed] [Google Scholar]
- 2.Brooks DE, Ollivier FJ. Matrix metalloproteinase inhibition in corneal ulceration. Vet Clin North Am Small Anim Pract. 2004;34:611–622. doi: 10.1016/j.cvsm.2003.12.005. [DOI] [PubMed] [Google Scholar]
- 3.Brooks DE, Matthews AG. Equine Ophthalmology. In: Gelatt KN, editor. Veterinary Ophthalmology. 4th ed. Ames, Iowa: Blackwell Publishing; 2007. pp. 1165–1274. [Google Scholar]
- 4.McLauglin SA, Gilger BC, Whitley RD. Infectious keratitis in horses: Evaluation and management. Compend Contin Edu Pract Vet. 1992;14:372–379. [Google Scholar]
- 5.Sweeny CR, Irby NL. Topical treatment of Pseudomonas sp-infected corneal ulcers in horses: 70 cases (1977–1994) J Am Vet Med Assoc. 1996;209:954–957. [PubMed] [Google Scholar]