Abstract
Because public health challenges are changing rapidly, over the past 3 years, we have turned a critical eye to the master of public health program at the Columbia University Mailman School of Public Health.
Under a process dubbed “curriculum renewal,” we engaged more than 170 faculty, staff, and students (and hundreds of alumni and employers of our graduates) in an initiative to develop a completely new design for master of public health education that launched in fall 2012.
We have described its design and structure and presented some preliminary evaluation data.
Current and emerging challenges to the public’s health in the 21st century are vastly different from those in previous centuries. As we articulated in a companion article,1 the changes in the challenges demand corresponding changes in public health education. Key elements of a reenvisioned educational program include knowledge of the role of public health in a successful society, familiarity with evolving global and local health challenges and methods for research and practice, facility with a life course approach to prevention, disciplinary strength, interdisciplinary strategies for solving complex problems, the ability to think critically, and the capacity for leadership, innovation, and teamwork.1–12
The Association of Schools of Public Health recognized these challenges several years ago. Under its auspices, faculty working groups were assembled to take a fresh look at master of public health (MPH) competencies; they deliberately distanced themselves from tradition and from current practices to develop curricula that promote interdisciplinary thinking, recognize the value of community partnerships to promote health, and incorporate broad definitions of health that span its physical, mental, and social dimensions.13 The working groups developed a new set of core public health competencies; these are presented on the Association of Schools of Public Health Web site.14 The Association of Schools of Public Health concluded its initiative by determining to continue its support of the development of competencies in the 5 traditional areas of public health specialization (biostatistics, environmental health sciences, epidemiology, health policy and management, and social and behavioral health), but it extended these domains with interdisciplinary or crosscutting competencies, for example those in the areas of communication, leadership, and systems thinking.
With the 2006 Association of Schools of Public Health recommendations, an extensive and growing literature, and our own responsibility for ensuring cutting-edge public health education for 21st-century leaders as motivating factors, the Mailman School of Public Health of Columbia University undertook a major school-wide initiative to revise and renew its MPH curriculum. We have described the content and structure for the new Columbia MPH curriculum (which launched in the fall 2012 term) and presented some early evaluation data on its initial implementation. We described the overall curricular goals in the companion article.1
BACKGROUND AND HISTORY OF THE COLUMBIA MPH PROGRAM
For the past 20 years or more, the MPH program at Mailman has typically comprised 45 academic points, with 15 credits of required core coursework in biostatistics, environmental health sciences, epidemiology, health policy and management, and sociomedical sciences. As at many schools of public health, the 5 core courses were traditionally taught independently with little focus on integrating content or highlighting areas of intersection.
The order or timeframe among core course completion varied substantially by department. In addition, students would take the majority of courses in their home departments, with subspecialization achieved through pursuit of distinct tracks of study, which were mainly nested within a department (with the exception of the global health track, established as a cross-disciplinary, cross-departmental effort in 2005). Students who desired to take courses outside their home departments were free to do so, but this was not required. There were no school-wide requirements with respect to developing knowledge and skills in communications, diversity and culture, leadership and professionalism, program planning, human biology, or systems thinking—although some departments and tracks developed their own specialized programming in 1 or 2 of these areas.
RATIONALE AND STRUCTURE TO ENACT CHANGE
In April 2009, the dean at Columbia’s Mailman School, Linda P. Fried, MD, MPH, articulated a case for change in public health education and challenged the faculty at a school-wide assembly to envision the education that would most effectively prepare the field’s leaders for the challenges of population health in the 21st century and leadership in 2050 as well as 2020. Extensive discussions had revealed that there had not been a comprehensive reevaluation of the curriculum in decades. The Mailman School leadership and faculty decided the time was right to develop a new curriculum that would best prepare our MPH students to lead in the science and solutions needed for current and future public health challenges and that would support the school’s overall mission and build on its strengths. This was the beginning of the Columbia MPH curriculum renewal initiative.
The curriculum renewal initiative began in earnest in March 2010, when the dean appointed Sandro Galea, MD, DrPH, the Mailman School’s Department of Epidemiology chair, to lead the curriculum renewal task force, an interdisciplinary team of faculty and staff representing all major departments and academic units of the school. She charged the task force to create the vision and goals for a transformed MPH curriculum. The task force began its work by enumerating the principles behind an MPH curriculum. The group concluded that their activities and recommendations should do the following:
Offer a vision for the next generation of public health education;
Align with the school’s strategic vision regarding societal needs;
Educate students to be leaders in domestic and global public health research and practice;
Educate students in advanced technical skills and critical thinking ability to apply them to improve population health;
Create and implement an integrated interdisciplinary school-wide curriculum that ensures all graduates are aware of the breadth of expertise that constitutes public health;
Ensure continued excellence of departmental and disciplinary training; and
Seek an optimal balance between departmental strengths and an integrated core public health curriculum.
The curriculum renewal task force concluded that a significant reformulation of public health education was required to meet its goals. The task force subsequently spawned 10 primary subcommittees, each chaired by a task force member. The 10 subcommittees, comprising more than 170 faculty members, students, and staff members, worked over the next 2 years to develop a dramatically new MPH curriculum.
DESIGN FOR THE NEW COLUMBIA MPH CURRICULUM
The new MPH curriculum, launched in fall 2012, aims to teach public health the same way that we work in public health: in interdisciplinary teams, bringing to bear strong disciplinary skills and integrating knowledge and practice across disciplinary boundaries to address complex health challenges, with effective leadership, management, innovation, and partnership capabilities. The curriculum is composed of 6 major elements, some of which are concentrated in a single semester, whereas others extend over the entire duration of MPH study (12–24 months):
an integrated core semester experience that develops from a background in 21st-century necessities and challenges for public health;
disciplinary coursework;
a new, case-based course called “Integration of Science and Practice” designed to foster decision-making and critical thinking skills;
a new course, titled “Leadership and Innovation,” intended to develop skills in communication, leadership and professionalism, and creative thinking;
enhanced structures, preparation (including cultural awareness), and evaluation methods for the practicum; and
certificate programs that allow students to specialize in an area beyond their disciplinary concentration or department, leading to an additional credential pursued simultaneously with the MPH and permitting greater latitude in interdisciplinary training.
The Core Semester
Rather than continuing to teach the core disciplines of public health in isolation, we replaced the 5 distinct core courses with the new and comprehensive Columbia MPH core curriculum; this is taught to incoming MPH students in the first semester. The new core gives students a broad introduction to public health, spanning the historical, ethical, biological, social, environmental, and quantitative foundations of population health. The 400 incoming MPH students complete their core coursework in cohorts of 100, heterogeneously composed of students from all different departments and programs so that interdisciplinary interactions are ubiquitous. The Columbia core is composed of a series of minicourses (called “modules”) of varying duration: anywhere from 2 to 13 weeks. Faculty receive compensation for teaching in proportion to module duration. In fall 2012, there were 18 modules in total, grouped within 5 studios of knowledge:
foundations of public health;
biological and environmental determinants of population health;
social, behavioral, and structural determinants of health;
health systems; and
methods for research design and evaluation.
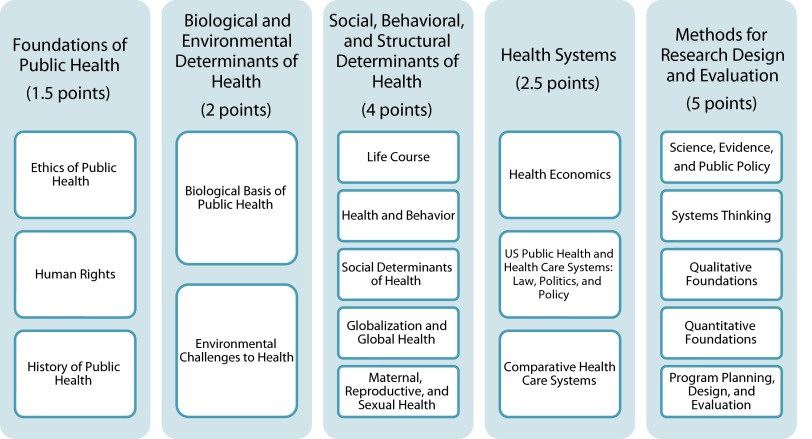
Although the 5 studios may at first appear to be simply a reconfiguration of the prior 5 core courses, there is a critically important difference: faculty from multiple departments and disciplines developed and are collaboratively teaching the content of almost every studio, bringing interdisciplinary perspectives, tools, and experiences to each content area (while also demonstrating for students a model for public health action). Each studio contains 2 to 5 distinct but interrelated modules. The modules within each studio are described in Figure 1.
FIGURE 1—
Components of the Columbia Master of Public Health (MPH) core curriculum.
We have designed several programmatic options that allow the curriculum to be tailored to the needs of a student body with diverse backgrounds, areas of focus, and experience levels. Students in each of the following programs are strongly encouraged to devote themselves full time to their studies during the first semester. Most students enter the 2-year program, which we call the Columbia MPH (Figure 2a). Students in the Columbia MPH focus primarily on the shared and disciplinary coursework in year 1 as well as practicum preparation. Most undertake the practicum experience in the summer between years 1 and 2. They then complete their coursework in year 2.
FIGURE 2—
Schematic diagrams of 4 versions of the Columbia Public Health Program: (a) the Columbia MPH (2-year program; 45–60 credits), (b) the accelerated MPH (1-year program for professionals; 42 credits), (c) the global MPH (2-year program with 6-month practicum; minimum 45 credits), and (d) the health policy and management model (16-month program; minimum 45 credits).
Note. MPH = master of public health.
In recognition of the experience already garnered by students who enter the program with professional degrees, we have added an intensive, 1-year program: the accelerated MPH (Figure 2b). In addition, we have tailored a 2-year MPH for students focusing on global health, which allows an all-important, 6-month overseas practicum placement (Figure 2c). Finally, we have also maintained a 16-month model for MPH students focusing on health policy and management (Figure 2d). Through this suite of options, which all incorporate the new curricular enhancements recently launched (i.e., 21 credits comprising the new core and the integration of the science and practice course with the leadership and innovation course), we maintain a cohesive set of offerings while allowing the flexibility necessary for the diverse student population pursuing public health education.
Disciplinary Coursework and Specialization in Public Health
Because of the importance of disciplinary strength combined with interdisciplinary preparedness1 for public health leadership of the future, the new MPH curriculum continues to emphasize disciplinary knowledge and the expertise of our faculty.
Although interdisciplinary skills are key, we recognize the wisdom of the following observation from the Interdisciplinary Graduate Education for Research and Training program, which the National Science Foundation sponsors: to be a successful interdisciplinarian, “one must have both disciplinary capability and interdisciplinary conversance.”15(p2) Therefore, in the second semester, students begin to focus intently on the development of disciplinary skills in one of the 6 departments of the school (biostatistics, environmental health sciences, epidemiology, health policy and management, population and family health, and sociomedical sciences).
Integration of Science and Practice
A novel aspect of the new curriculum is the inclusion of a new course titled “Integration of Science and Practice.” Integration of Science and Practice is a year-long course intended to bridge the gap between the academy and the workplace by simulating real-world experiences in a safe environment via case studies. Through the case method, students learn by doing and develop the ability to
synthesize information from multiple sources to advance population health practices and research,
identify knowledge gaps that hinder the development of health policy and health systems of the future,
evaluate potential responses to population health problems,
communicate complex concepts to academic and lay audiences, and
weigh the risks and benefits inherent in public health decision-making.
The Integration of Science and Practice course combines case-based study with small-group work and opportunities for open discussion that can enhance students’ comfort with decision-making in the face of uncertainty.
Leadership and Innovation
Leaders create a vision, motivate, and facilitate the work of others to reach mission-driven goals.16,17 Innovation, which Ness defines as “creativity with a purpose,”18(p2) is the intentional bringing into existence of something new that can be sustained and repeated and that has some value or utility.19 Effectiveness in public health requires expertise in both leadership and innovation; this requirement was the motivation for developing a new Leadership and Innovation course for all MPH students. The Leadership and Innovation course is designed to enhance self-reflection abilities. It fosters the facilitation of individual work and teamwork to create optimal performance, paying special attention to developing the skills needed to generate and implement new policies, programs, and practices—on the basis of science and need—to improve the public’s health.
The course, offered for the first time in the spring 2013 term, introduces students to the distinctions between and benefits of both critical thinking (emphasizing evaluation and analysis) and creative thinking (emphasizing openness to alternative possibilities and reworking old ideas to achieve new solutions). Students should emerge from the course better able to lead and manage individuals and teams in a variety of contexts; perform effectively as team members and individual contributors; and promote and implement innovative ideas and solutions at the individual, team, and organizational levels. Much of the inspiration for the Leadership and Innovation course has emerged from the world of business and management schools, which have successfully promoted leadership development through conceptual and experiential learning for many years.
The Integrative Practicum Experience
Practical field experience has always been required of Columbia MPH students, per recommendations from the field and the requirements imposed by the Council on Education for Public Health.20 In the past, practicum experiences were largely department based, with policies for preparation, guidance in the field, and evaluation postpracticum the sole responsibility of the individual departments. However, the curriculum renewal initiative gave us an opportunity to reevaluate the practicum experience and reenvision it as an integrated, interdisciplinary, and substantive experience across as well as within departments. The result is the school-wide “integrative practicum experience,” which is built on school-wide vision, policies, and standards.
Students prepare for their field experiences through a series of prepracticum workshops as well as through the skill-building activities of the Leadership and Innovation course. The earliest workshop begins during orientation for new students with an introduction to cultural awareness. Faculty members (who have been specially trained) lead groups of approximately 20 students during orientation through a day-long series of activities and discussions aimed at increasing self, social, and global awareness. Other prepracticum workshops include sessions on choosing a practicum, developing learning goals and methods of assessment, and developing professionalism in the workplace (integrating well with the leadership and management skills emphasized in the Leadership and Innovation course).
After selecting a practicum site, students work with their faculty advisors and site supervisors to develop a learning contract with specific objectives and outcome measures to guide their field activities. Once in the field, onsite supervisors and school-based faculty advisors continue to be the mainstay for students, who remain connected electronically. We have expanded support systems for the onsite supervisors, which will ultimately include a resource Web site and on-campus training sessions. After returning from the field experience, students and their site supervisors complete standardized evaluation forms. We are also completing development of a suite of school-wide events in which students can present summaries of and reflections on their field experiences to other students and faculty.
The Certificate Programs
We have created formal university-approved and state-sanctioned certificate programs that make it possible for students to specialize in an area of public health theory or practice beyond their disciplinary concentration or department. As part of the 2-year MPH program, a student selects a certificate program to augment disciplinary training with a focus on a complementary or more advanced subject that may draw from resources across the Mailman School and Columbia University more broadly. Most certificates represent interdisciplinary professional education focused on key public health problems, such as health in an aging society, environmental health policy, climate and health, applied biostatistical methods, public health research methods, health promotion research and practice, and global health. Other certificates afford students the opportunity for deeper study of their chosen discipline (e.g., advanced epidemiology, health policy analysis, and toxicology).
A listing of current certificate offerings is available on our Web site at http://publichealth.columbia.edu/degree-programs/columbia-mph/certificate-program. Mailman School alumni and employers of our graduates endorsed certificates as a valuable credential for new hires, with the potential to increase the attractiveness of our graduates in the job market because of their rigorous interdisciplinary training and fluency in the most advanced and topical issues in public health.
INTEGRATION
Throughout the development of the Columbia MPH program, one of our most crucial objectives has been to establish effective and sustained linkages across the curriculum. In achieving this goal, we would be assured that our curriculum truly reflects the integrative nature of public health theory and practice and indeed mirrors the typical work style and approaches of successful, interdisciplinary public health teams. With this goal in mind, we have devoted significant effort toward integration across all curricular elements. Specifically, we implemented a strategic decision to meet in interdisciplinary, interdepartmental groups for more than 1 year before launch to share the content of all the individual courses and modules under development.
For our launch year, faculty familiarized themselves with content across the curriculum by studying the syllabi and even the presentation notes and slides for their colleagues’ core modules; some even attended some of their colleagues’ lectures (or viewed them online). To further assist students to see the connections between various curricular elements and the cohesiveness of the overall program, we also chose to offer an introductory, framing lecture about the core at the start of the fall term and a closing, consolidating lecture at the end of the term. We feel strongly that integration is essential to the success of the program.
PRELIMINARY EVALUATION
A major challenge is assessing the effectiveness of the new curriculum on student learning and professional success. We established a committee to take advantage of expertise in assessment and evaluation from faculty across the school. The committee developed a comprehensive series of evaluation protocols and drafted a number of new instruments that assess not only student satisfaction with courses but also the overall impact of the program through the eyes of students and faculty. Measuring interdisciplinary conversance or facility with interdisciplinary efforts is a formidable challenge, but the committee is actively pursuing options for gauging how well the new curriculum enables students to integrate knowledge across domains.
We have data from only 1 semester (fall 2012) of the new program. Figure 3 presents some key responses from students and faculty regarding the fall semester experience. We collected these student data in January 2013, about 1 month after the end of the fall term. About 78% of students (n = 292) responded to the survey. The students indicated high levels of enthusiasm for the overall fall term experience (78% positive), course quality (83% positive), and quality of instruction (90%). They also indicated that they were able to integrate concepts across core modules (98%) and across the core and Integration of Science and Practice courses (91%).
FIGURE 3—
Preliminary evaluation data from students and faculty of the Columbia MPH program: (a) student responses on the quality of the experience, the courses, and the teaching; (b) students’ self-evaluation of their ability to integrate concepts across classes (core modules and the Integration of Science and Practice course); and (c) faculty assessment of student levels of academic preparation, professionalism and maturity, and intellectual engagement.
Note. MPH = master of public health. Data from students were measured 1 month after the end of the fall term, and data from faculty were measured at the end of their teaching assignments. For Figure 3c, the faculty sample size was n = 29.
In their feedback, students expressed anxieties about the logistics and demands of the fall term. These anxieties peaked around the beginning of November (which coincided with midterm exams and the arrival of Hurricane Sandy, which left many students and faculty without power or convenient means of transportation for a week or more) and then began to recover in December. Students expressed dissatisfaction with the frequency of exams and with the presentation of materials on the course Web sites. However, despite their anxieties, students performed well in the new curriculum, and fewer than usual struggled to complete the fall term (as indicated by a decrease in the number of grades of incomplete for fall 2012 compared with fall 2011).
We collected faculty data at the point at which each faculty member’s course module ended. Faculty were also positive about the program, with 69% reporting that their students were academically prepared for the rigors of the new curriculum, 90% reporting that their students demonstrated professionalism and maturity in the endeavor, and 93% reporting that their students were intellectually engaged. Clearly these are short-term measures and further follow-up is needed. We plan to continue our evaluation efforts and follow our alumni over time to monitor their changing views on the Columbia MPH curriculum and its impact on their career trajectories.
These initial data represent only a small part of our overall evaluation plan. We are continuing to collect extensive data, not only on program satisfaction and initial impressions but also on perceived utility and knowledge over time, with follow-ups planned throughout training and even after graduation.
CONCLUSIONS
The new Columbia MPH curriculum is a fully reenvisioned approach for public health education that is more rigorous, more interdisciplinary, and more comprehensive than any we have previously offered. It is anchored in an integrated first-semester core curriculum that offers all students the interdisciplinary foundation of public health theory, values, science, and practice. Redesigned departmental coursework ensures excellence in the primary disciplines of public health. Three novel, integrated educational engagements (integration of science and practice, leadership and innovation, and the integrative practicum experience) solidify and expand on fundamental professional skills and give students the opportunity to apply their newly acquired knowledge and abilities for a variety of purposes. Certificate credentialing affords our students the opportunity to graduate from the program with tangible documentation of their expertise in an area beyond (or more deeply embedded in) their main MPH concentration.
In 2010, as we completed the goals and initiated designing the new Columbia MPH curriculum, the Rockefeller Commission3 published recommendations for the education of health professionals to meet the goals of preparing a global workforce with consistently high standards to meet 21st-century health needs and to be able to function in current health systems and lead in improved ones. The report also called for rigorous evaluation and the communication of results. We think that our goals and the methods of the new Columbia MPH may offer the first comprehensive response to the call by the Rockefeller Commission report.
The Columbia MPH curriculum offers multiple opportunities and diverse strategies for students to practice applying, integrating, and sharpening the skills they have learned in the classroom to address real-world problems in population health and health systems. At numerous points, students are required to translate their knowledge and develop a series of action steps to address a specific public health challenge, obtaining feedback from their professors and fellow students along the way. These opportunities distinguish our new curriculum from its predecessor and should produce graduates with enhanced ability to leap into public health practice and their first jobs with greater facility, effectiveness, and confidence. Our future evaluation efforts will focus on career experiences and trajectories, incorporating data from both our graduates and their employers.
Acknowledgments
The work discussed in this article builds directly on the involvement of many colleagues engaged in the Columbia curriculum renewal process. Particular thanks go to Sasha Rudenstine and the Curriculum Renewal Task Force and to deans Jim Glover and Marlyn Delva for their roles in implementing the renewed curriculum. Thanks also go to Laura Sampson for editorial help with this article.
Human Participant Protection
The Columbia University Medical Center institutional review board determined this study to be exempt because it falls into the categories of educational testing, survey, or observational research and educational practices research.
References
- 1.Fried LP, Begg MD, Bayer R, Galea S. MPH education for the 21st century: motivation, rationale, and key principles for the new Columbia public health curriculum. Am J Public Health. 2014;104(1):23–30. doi: 10.2105/AJPH.2013.301399. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Zerhouni E. The NIH roadmap. Science. 2003;302(5642):63–72. doi: 10.1126/science.1091867. [DOI] [PubMed] [Google Scholar]
- 3.Frenk J, Chen L, Bhutta ZA et al. Health professionals for a new century: transforming education to strengthen health systems in an interdependent world. Lancet. 2010;376(9756):1923–1958. doi: 10.1016/S0140-6736(10)61854-5. [DOI] [PubMed] [Google Scholar]
- 4.Roy R. Interdisciplinary science on campus—the elusive dream. Chem Eng News. 1977;55(35):28–30. [Google Scholar]
- 5.Committee for the Study of the Future of Public Health Division of Health Care Services. The Future of Public Health. Washington, DC: Institute of Medicine; 1988. [Google Scholar]
- 6.Fineberg HV, Green GM, Ware JH, Anderson BL. Changing public health training needs: professional education and the paradigm of public health. Annu Rev Public Health. 1994;15:237–257. doi: 10.1146/annurev.pu.15.050194.001321. [DOI] [PubMed] [Google Scholar]
- 7.Shortell SM, Weist EM, Sow MS, Foster A, Tahir R. Implementing the Institute of Medicine’s recommended curriculum content in schools of public health: a baseline assessment. Am J Public Health. 2004;94(10):1671–1674. doi: 10.2105/ajph.94.10.1671. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Sommer A. Toward a better educated public health workforce. Am J Public Health. 2000;90(8):1194–1195. doi: 10.2105/ajph.90.8.1194. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Allegrante JP, Moon RW, Auld ME, Gebbie KM. Continuing-education needs of the currently employed public health education workforce. Am J Public Health. 2001;91(8):1230–1234. doi: 10.2105/ajph.91.8.1230. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Moser JM. Core academic competencies for master of public health students: one health department practitioner’s perspective. Am J Public Health. 2008;98(9):1559–1561. doi: 10.2105/AJPH.2007.117234. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Petersen DJ, Hovinga ME, Pass MA, Kohler C, Oestenstad RK, Katholi C. Assuring public health professionals are prepared for the future: the UAB public health integrated core curriculum. Public Health Rep. 2005;120(5):496–503. doi: 10.1177/003335490512000504. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Wright K, Rowitz L, Merkle A et al. Competency development in public health leadership. Am J Public Health. 2000;90(8):1202–1207. doi: 10.2105/ajph.90.8.1202. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Clark N, Weist E. Mastering the new public health. Am J Public Health. 2000;90(8):1208–1211. doi: 10.2105/ajph.90.8.1208. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Association of Schools of Public Health Education Committee. Master’s degree in public health core competency model, version 2.3. 2006. Available at: http://www.asph.org/userfiles/Version2.3.pdf. Accessed July 8, 2011.
- 15.Von Hartesveldt C, Giordan J National Science Foundation. Impact of transformative interdisciplinary research and graduate education on academic institutions: workshop report. 2008. Available at: www.nsf.gov/pubs/2009/nsf0933/igert_workshop08.pdf. Accessed November 24, 2010.
- 16.Senge PM. The leader’s new work: building learning organizations. Sloan Manage Rev. 1990;32(1):7–23. [Google Scholar]
- 17.Steffen D. Leadership, communication, and public health: moving beyond statistics to stories. 2012. Available at: http://www.heartlandcenters.slu.edu/nln/events/072012Webex-slides.pdf. Accessed November 1, 2012.
- 18.Ness RB. Innovation Generation: How to Produce Creative and Useful Scientific Ideas. New York, NY: Oxford University Press; 2012. [Google Scholar]
- 19.Selman J. Leadership and innovation. Available at: http://www.paracomm.com/leadership-and-innovation. Accessed September 4, 2012.
- 20.Council on Education for Public Health. Accreditation criteria schools of public health. 2011. Available at: http://www.ceph.org/assets/SPH-Criteria-2011.pdf. Accessed March 30, 2012.