Abstract
Objectives
To determine the acceptability of a pre-consultation checklist for older patients who attend medical visits with an unpaid companion and to evaluate its effects on visit communication.
Design
Randomized controlled pilot study.
Setting
Academic geriatrics ambulatory clinic.
Participants
Thirty-two patients age 65+ and their unpaid companion.
Intervention
A self-administered checklist was compared to usual care. The checklist was designed to: (1) elicit and align patient and companion perspectives regarding health concerns to discuss with the doctor, and (2) stimulate discussion about the companion’s role in the visit.
Measurement
Primary outcome: ratio of patient-centered communication, coded from visit audiotapes. Secondary outcomes: checklist acceptability; visit duration; patient-companion verbal activity; patient- and physician- reported perspectives of the visit.
Results
All intervention patients and companions (n=17) completed the checklist, and all participants (n=32 dyads) completed the study. Patients and companions stated the checklist was easy to complete (88%), useful (91%), and they uniformly (100%) recommended it to other patients. Communication was significantly more patient-centered in intervention (versus control) group visits (ratio of 1.22 versus 0.71; p=0.03). Visit duration (35.0 and 30.6 minutes; p=0.34) and percent of total verbal activity contributed by patients and companions (58.2% and 56.3% of visit statements; p=0.50) were comparable in intervention and control groups, respectively. Physicians were more likely to indicate intervention (versus control) companions “helped them provide good care to the patient” (94% vs. 60%; p=0.02). Intervention (versus control) patients were more likely to indicate they “better understood their doctor’s advice and explanations” because their companion was present (82% vs. 47%; p=0.03).
Conclusion
A checklist to elicit and align perspectives of older patients and their companions resulted in enhanced patient-centered medical visit communication.
Keywords: Family caregiver, primary health care, physician office, patient-provider communication
INTRODUCTION
With low levels of educational attainment1 and a high prevalence of sensory and cognitive deficits,2,3 many older adults are ill equipped to successfully function in today’s complex health care environment. Patient-directed pre-consultation interventions have been developed to prompt patient engagement in their care.4,5 Health literacy universal precautions have been developed to reduce health system demands.6,7 No interventions to date specifically address the fact that 4 in 10 primary care patients – those who are older, less educated, and in worse physical health – regularly attend routine medical visits with an unpaid companion, usually a family member.8,9 The companions who accompany older adults to medical visits participate in visit communication8,9 and their attendance in medical visits persists over time.10
We developed a pre-consultation checklist to strengthen the existing but under-recognized older patient-companion partnership. The checklist was designed to:(1). elicit and align patient and companion perspectives regarding patient health concerns to discuss with the doctor, and (2). stimulate discussion about the patient’s desires for assistance from the companion in the visit. In this paper we describe the checklist and present preliminary evidence of its acceptability and effect on medical visit communication in a pilot randomized study conducted in an academic geriatrics ambulatory clinic.
METHODS
Our intervention is guided by theory and informed by evidence from the patient-provider communication literature. We posit that previously described aspects of the patient-provider relationship11 and medical communication processes12 may be extended to the older patient and their companion, when present. Prior studies find older patients are often unable or unwilling to articulate their desired preferences for communicating with medical providers13,14 and that patient, family, and provider assessments of patient symptoms 15,16 and treatment priorities 17,18 commonly diverge. Medical communication that is aligned with patient information sharing and decision-making preferences is associated with varied end-points such as patient satisfaction, emotional well-being, treatment adherence, and physiologic measures such as lower symptom burden.19 These favorable endpoints are thought to result at least in part from greater patient responsiveness when medical communication is tailored to their expectations, interpersonal behaviors, and autonomy beliefs.19,20 We hypothesized that a pre-consultation checklist to: (1). elicit and align patient and companion perspectives regarding patient health concerns to discuss with the doctor, and (2). stimulate discussion about the role to be assumed by the companion in the visit would facilitate patient-centered communication by clarifying the visit agenda and specifying patient preferences for the companions’ role in the encounter.
We sought to develop a checklist that was brief and appropriate for self-administration in a clinic waiting room. Careful attention was paid to considerations of the busy physician practice and the diverse older adult population. We reviewed a wide range of existing health-related quality of life, functional status, and needs assessment instruments to construct an item pool of common older patient concerns that were appropriate for discussion in primary care visits. To establish face and content validity, a panel of 3 geriatricians and 1 geriatric psychiatrist then reviewed and nominated candidate items for inclusion. We generated a final list of 23 common patient concerns that was balanced across physical, mental, and social role function domains.
The checklist (see Appendix) involves two activities that are completed by a patient and their companion before a scheduled appointment. The first activity involves completing the checklist of common geriatric health concerns using three steps. Instructions separately elicit patient and companion notation of concern (“not at all”, “a little”, and “a lot”) for each health concern, and then together, to identify or negotiate which concerns to discuss with the doctor in the upcoming visit. Instructions to the patient state: “the patient may work independently or the companion may read the list and record the (patient’s) answer.” Instructions to the companion state: “it is fine if the companion has different concerns than the patient.” In a second activity, patients are asked to identify ways they would like their companion to help them during their visit from a list of previously observed behaviors.9 All text is in large (16-point) font.
Recruitment and Eligibility Criteria
We conducted a pilot study of the checklist at the Beacham Ambulatory Care Center, operated by the Johns Hopkins University Division of Geriatric Medicine and Gerontology between April and August 2012. Clinic staff mailed recruitment letters to established patients of 4 participating geriatricians with upcoming scheduled visits. Patients who did not “opt out” by mail were contacted by a member of the research team to discuss the study and administer a brief telephone screening interview. Inclusion criteria included: 65 years of age or older, English speaking, hears well enough to communicate by phone, sees well enough to read large print, typically accompanied to doctor visits by an unpaid companion, and provided contact information for their companion. As this study was designed as a proof of concept pilot study, we sought to recruit a more homogeneous clinical study sample that would be able to complete the checklist. Therefore, older adults with significant cognitive deficits on the basis of more than two incorrect answers on a 6-item cognitive screen21 were excluded. Comparable sensory and cognition exclusion criteria applied to companions who also completed screening calls.
Study Procedures
Eligible patient-companion dyads who expressed an interest in the study met a member of the research team 30 minutes before the patient’s scheduled appointment in the physician office waiting room. After providing informed consent using an institutional review board approved form, each dyad was randomized to the checklist or to usual care using stratified, blocked randomization with alternating block sizes of 4 and 6 for each physician. Dyads assigned to the intervention received a clipboard, pen, and a copy of the checklist that they completed together in the clinic waiting room without research or office staff assistance. Dyads assigned to usual care waited for their visit as usual. All medical encounters were audio-recorded but otherwise proceeded as usual, without research or office staff involvement. Physicians, patients, and companions completed surveys immediately after the visit in the office suite. Patients and companions were contacted by telephone two weeks following the visit and were asked additional questions about the medical visit, as well as socio-demographic factors and health status. Patients and companions received a $20 gift card after the medical visit and again after the two-week telephone interview.
Study Measures
Patient attributes
Patient attributes included age, gender, living arrangement, educational attainment, self-rated health, and whether they received assistance with self-care and household activities. Patients were asked to respond to a single-item health literacy screen “how confident are you filling out medical forms by yourself,”22 years under the care of the physician, and numbers of daily prescribed and over-the-counter medications.
Companion attributes
Companion attributes included age, gender, relationship to the patient, educational attainment, and employment. In post-visit surveys, patients, companions, and physicians were asked about visit communication. Intervention patients and companions were asked questions regarding checklist acceptability, including its utility, burden, and helpfulness.
Recordings of medical visit dialogue were coded using the Roter Interaction Analysis System (RIAS), a validated system for empirically describing medical visit communication.23 A trained RIAS-coder who was blinded to group assignment coded visit recordings by assigning each complete statement to one of thirty-eight mutually exclusive and exhaustive communication categories. The large numbers of codes were collapsed to ten summary RIAS categories. For each RIAS summary category, we examined the proportion of visit statements contributed by the patient and companion, together, in relation to aggregate visit statements. Physician contribution to visit communication is not presented as the focus of this investigation is the patient-companion dyad. Three measures of visit processes were also examined:
Patient-centered communication is operationalized as a ratio of statements that encompass psychosocial and socio-emotional elements of exchange reflecting the lived experience of patients relative to statements that reflect a more biomedical and disease-focused perspective.23,24 A value greater than 1 indicates a more patient-centered encounter, whereas a value less than 1 indicates a more physician-centered encounter.
Medical visit duration, expressed in minutes.
Patient and companion verbal activity, reflecting the proportion of total visit statements contributed by patient and companion.
Data Analysis
Analyses were performed in SAS statistical software, version 9.3 (SAS, Cary, NC), with each patient-companion dyad and their recorded medical encounter as the unit of analysis. Simple descriptive statistics (frequency distributions, group means)were used to evaluate between-group differences in patient and companion attributes and patient, companion and physician post-visit responses to questions about visit communication and the role of the companion.
RESULTS
Study Sample Characteristics
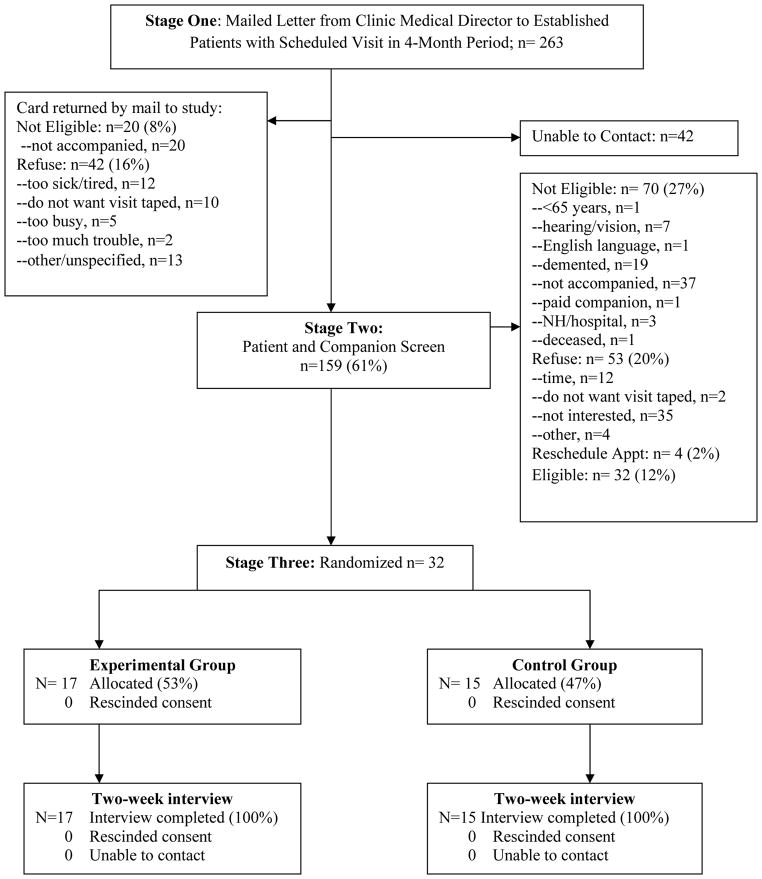
Recruitment letters were mailed to 263 established patients of four participating geriatricians with upcoming scheduled visits. Of these patients, 20 (7.6%) returned cards indicating they were not accompanied, 42 (16.0%) refused participation by mail, and 42 (16.0%) patients could not be reached. Screening calls were made to 159 (60.5%) patients: 70 (26.6%) were not eligible, 53 (20.2%) refused participation, 4 (1.5%) were not available due to rescheduled appointments. A total of 32 patients and companions were eligible and consented to participate. These 32 dyads were randomized to usual care (n=15) or to the checklist (n=17); all 32 patients and companions (100%) completed follow-up interviews (Figure 1).
Figure 1.
Study Participant Recruitment and Randomization.
Enrolled patients (n=32) were on average 81.8 years, female (59.4%), lived alone (61.3%), and completed high school (41.9%) or some college(41.9%; Table 1). Approximately one-third (34.4%) of patients were suspected of low or marginal health literacy.22 Patients rated their health as excellent/very good (28.1%), good (31.3%), or fair/poor(40.6%). They were taking an average of 8.9 prescribed and over-the-counter medications daily. Patients received assistance with dressing or bathing (15.6%), coordination of services (34.4%), managing medications (43.8%), scheduling physician appointments (46.9%), medical bills and paperwork (50.0%), coordination of health information (53.1%), and transportation (75.0%). Patients overwhelmingly indicated their companion was the person who helped the most with these activities (87.5%). Companions were mostly spouses (31.3%) and adult children (53.1%). Nearly half (45.2%) of companions were employed for pay and they worked an average of 30 hours per week. No group differences in patient characteristics were statistically significant. Companions in the control (versus intervention) group were more likely to be female(86.7% versus 52.9%; p=0.04).
Table 1.
Enrolled Study Sample by Group Assignment
| Patient Characteristics | Total Sample (n=32) | Group Assignment
|
P-value | |
|---|---|---|---|---|
| Checklist n=17 (53.1%) | Usual Care n=15 (46.9%) | |||
| Age; mean (range) | 81.8 (65–99) | 80.7 (65–99) | 82.9 (69–96) | 0.471 |
| Female; n (%) | 19 (59.4%) | 9 (52.9%) | 10 (66.7%) | 0.446 |
| Lives alone; n (%) | 19 (59.4%) | 10 (58.8%) | 9 (60.0%) | 0.660 |
| Educational attainment; n (%) | ||||
| Elementary | 5 (16.1%) | 2 (11.8%) | 3 (20.0%) | 0.706 |
| High school | 13 (41.9%) | 7 (41.2%) | 6 (40.0%) | |
| College or beyond | 13 (41.9%) | 7 (41.2%) | 6 (40.0%) | |
| Self-rated health; n (%) | ||||
| Excellent/Very Good | 9 (28.1%) | 6 (35.3%) | 3 (20.0%) | 0.626 |
| Good | 10 (31.3%) | 6 (35.3%) | 4 (26.7%) | |
| Fair/Poor | 12 (38.7%) | 5 (29.4%) | 8 (53.3%) | |
| Lower literacy; n (%) | 11 (34.4%) | 4 (23.5%) | 7 (46.7%) | 0.169 |
| Years under physician care; mean (range) | 3.9 (1–15) | 3.9 (1–15) | 3.9 (1–10) | 0.954 |
| Daily medications; mean (range) | 8.9 (4–22) | 9.9 (4–22) | 7.8 (4–17) | 0.232 |
| Companion Characteristics | ||||
| Age; mean (range) | 62.4 (35–81) | 60.6 (35–79) | 64.6 (48–81) | 0.329 |
| Female; n (%) | 22 (68.8%) | 9 (52.9%) | 13 (86.7%) | 0.040 |
| Relationship to Patient; n (%) | ||||
| Spouse | 10 (31.3%) | 4 (23.5%) | 6 (40.0%) | 0.604 |
| Adult Child | 17 (53.1%) | 10 (58.8%) | 7 (46.7%) | |
| Other (friend, partner, other relative) | 5 (16.1%) | 3 (17.6%) | 2 (13.3%) | |
| Educational attainment; n (%) | ||||
| High school | 6 (18.8%) | 4 (23.5%) | 2 (13.3%) | 0.762 |
| College or beyond | 26 (81.3%) | 13 (76.5%) | 13 (86.7%) | |
| Employed for Pay; n (%) | 14 (43.8%) | 9 (52.9%) | 5 (33.3%) | 0.265 |
Acceptability of Checklist
Intervention participants responded to questions regarding checklist burden, utility, and helpfulness. All patients (100%) and most companions (81.3%) indicated that the amount of time it took to complete the checklist was “just right.” The vast majority of patients (94.1%) and companions (87.5%) agreed or strongly agreed that completing the checklist was useful, and easy to complete (88.2% for patients and companions). Most patients agreed or strongly agreed that completing the checklist improved their companion’s understanding of their most important concerns (82.4%) and discussions with the doctor (88.2%). Patients and companions unanimously (100%) stated that they would recommend completing the checklist to other patients and nearly all (94.1% of patients and 100% of companions) indicated they would like to continue responding to the checklist in the future.
Group Differences in Communication
Communication was significantly more patient-centered in intervention (versus control) group visits (patient-centered communication ratio of 1.22 versus 0.71; p=0.03). Intervention patients and companions engaged in significantly less biomedical information exchange than patients and companions in the control group (34.0% versus 47.8% of visit statements, respectively; p<0.01)but asked more lifestyle and psychosocial questions (0.9% versus 0.3% of visit statements, respectively; p=0.03) and provided more lifestyle and psychosocial information (22.8% versus 15.9% of visit statements, respectively; p=0.05). Visits for patients in the intervention group were 4.4 minutes longer than control group visits (35.0 versus 30.6 minutes; p=0.34; see Table 2). Percent of total verbal activity contributed by patients and companions was comparable for intervention and control group dyads (58.2% versus 56.3% of visit statements, respectively; p=0.49).
Table 2.
Group Differences in Communication
| Group Assignment
|
P-value | ||
|---|---|---|---|
| Checklist | Usual Care | ||
|
| |||
| Patient-Centered Communication * | 1.22 | 0.71 | 0.034 |
| Visit Duration (in minutes) | 35.0 | 30.6 | 0.338 |
| Verbal Activity † | |||
| Patient Verbal Activity | 37.7% | 38.4% | 0.876 |
| Companion Verbal Activity | 20.5% | 17.9% | 0.630 |
| Patient & Companion Verbal Activity | 58.2% | 56.3% | 0.498 |
| Categories of Patient and Companion Talk‡ | |||
| Biomedical Data Gathering | 3.2% | 3.4% | 0.747 |
| Biomedical Information Giving | 34.0% | 47.8% | 0.001 |
| Lifestyle and Psychosocial Data Gathering | 0.9% | 0.3% | 0.033 |
| Lifestyle and Psychosocial Information Giving | 22.8% | 15.9% | 0.048 |
| Facilitation and Patient Activation | 10.9% | 8.3% | 0.199 |
| Positive Talk | 12.8% | 10.7% | 0.178 |
| Emotional Talk | 9.7% | 8.3% | 0.720 |
| Negative Talk | 0.7% | 0.6% | 0.751 |
| Social Talk | 1.8% | 1.6% | 0.857 |
| Procedural Talk | 3.0% | 2.6% | 0.317 |
Patient-Centered Communication refers broadly to the ratio of psychosocial and socio-emotional statements contributed by the patient, companion, and physician ((physician psychosocial questions, lifestyle and psychosocial information and counseling; facilitation and patient activation; positive, emotional talk) and patient and companion biomedical and psychosocial questions, psychosocial and lifestyle disclosure, and emotional talk)) relative to biomedical talk and orientations (physician biomedical questions, biomedical information and counseling; procedural talk and patient and companion biomedical disclosure).
Verbal Activity reflects the proportion of statements contributed by the patient alone, the companion alone, and the patient and companion together, in relation to overall visit statements (including statements by the physician).
Categories of Patient and Companion Talk refer to the proportion of statements contributed by the patient and companion with in each RIAS summary category relative to total patient and companion visit statements (see Roter and Larson, 2002 or www.riasworks.com for more information).
Group Differences in Patient, Companion, and Physician Perspectives on Communication
Physician, patient, and companion responses to questions about medical visit communication suggest that intervention (versus control) group companions were more active in facilitating information exchange. Physicians were 34% more likely to agree or strongly agree that intervention (versus control) group companions “helped them provide good care to the patient” (94.1% vs. 60.0%; p=0.02). Intervention patients were more likely to agree or strongly agree that because their companion was present they “better understood their doctor’s advice and explanations” (82.4% vs. 46.7%; p=0.03) and that “their doctor understood their concerns more fully” (64.7% vs. 40.0%; p=0.31) than their control group counterparts.
CONCLUSION
Our study indicates that a pre-consultation checklist to strengthen the partnership between the older patient and their unpaid visit companion is acceptable and may confer benefit to medical visit communication. Patient-companion dyads successfully self-administered the checklist in a clinic waiting room immediately prior to a scheduled visit. Nearly all intervention participants reported the checklist was helpful to visit discussions and expressed a willingness to continue responding to it in the future. Our most notable findings relate to the consistency across both post-visit survey responses and audio taped dialogue suggesting that intervention group companions were more actively engaged in the medical visit in a manner that was beneficial to patient-centered communication. Intervention patients and companions engaged in significantly more lifestyle and psychosocial dialogue and less biomedical discussion, differences that are indicative of more patient-centered care.24
Study participants are drawn from a complex older patient population for whom evidence-based guidelines are less applicable and quality of care is poor.25,26 Enrolled patients were on average 82 years of age, taking nearly ten daily prescribed and over-the-counter medications and they were overwhelmingly accompanied by the spouse or the adult child they reported helped them “the most” with health-related activities. That patients’ companions were generally more highly educated and in better health, and that their role was endorsed as influential to information exchange and understanding is consistent with foundational frameworks27 and qualitative studies28 suggesting that social support may bridge communication barriers and health literacy deficits for vulnerable patients. Companions were generally younger than patients; cohort differences may exist in regard to patient and companion preferences and expectations for interactions with medical providers.
Our intervention acknowledges the independent perspective and role of companions in older patients’ health care encounters. By striving to engage the companion as desired by the patient, our intervention is consistent with ethical guidance recently set forth by physician organizations in emphasizing respect for patient dignity, rights, and values, the use of physician communication to support accurate and shared understanding of the patient’s condition and treatment goals, and the value of family involvement in continuity of care.29 Although patient privacy has been raised as an impediment to health care strategies that formally recognize and partner with patients’ broader social support networks, concerns regarding patient privacy did not emerge as a problem in this study. Potential unintended consequences of the intervention that pertain to privacy, interpersonal conflict, as well as provider practice-based implications (e.g. patient flow, visit duration)will be carefully monitored in future work.
Several limitations of this study merit comment. Most notably, this was a pilot study to evaluate acceptability of a patient-companion pre-consultation checklist and establish proof of concept. Our findings suggest that a Phase III efficacy trial with a larger sample and diverse clinical settings is warranted. As a pilot, the study was not powered to detect between-group differences, or to perform multivariate analyses to account for differences in patient or companion characteristics. Given that the study was conducted in a single academic ambulatory geriatrics clinic, results cannot be extrapolated to mainstream primary care practice. Patients with severe cognitive and sensory impairments were excluded from the study, as were patients who were accompanied to their medical visit by a paid companion.
Health care delivery interventions for complex older adults have targeted patient, provider, and health system-level factors. In contrast, this intervention targeted the existing but under-recognized patient-companion partnership. The approach has several attractive and practical features. The approach is directed to a population that has been shown to be both high-risk and costly8 and to a partnership that is enduring.10 The strategy is practical in that it seeks to optimize a naturally occurring partnership between patients and their existing social supports. The approach that we have developed involves minimal cost and does not require restructuring of provider practice. Further research is needed to evaluate this intervention in a larger sample with longer duration of follow-up.
Acknowledgments
FUNDING: This study was supported by National Institute of Mental Health grant K01MH082885 “Optimizing Family Involvement in Late-Life Depression Care” (JLW). The sponsor of this research was not involved in its study concept or design, recruitment of subjects or acquisition of data, data analysis or interpretation, or in the preparation of this manuscript.
We gratefully acknowledge Laura Vernon Russell for her invaluable assistance with recruitment of study participants. We recognize the contributions of Beacham Ambulatory Clinic staff in facilitating study operations. We would like to acknowledge study participants, whose tremendous generosity, time, and valuable insight made this study possible. The author would like to thank Paul Duberstein and Karen Davis for their thoughtful comments on early drafts of the manuscript.
Sponsor’s Role: The sponsor of this research was not involved in its study concept or design, recruitment of subjects or acquisition of data, data analysis or interpretation, or in the preparation of this manuscript. Dr. Boyd’s time was supported by a Paul Beeson Career Development Award Program (NIA K23 AG032910, AFAR, The John A. Hartford Foundation, The Atlantic Philanthropies, The Starr Foundation and an anonymous donor).
Appendix. Patient-Companion Preconsultation Checklist
Instructions
The next page lists some common patient concerns. Use the following three steps to work together to review and discuss this list.
First, the patient should identify their level of concern (“not at all”, “a little”, or “a lot) for each topic. The patient may work independently, or the companion may read the list and record the patient’s answer. Circle the number that reflects the patient’s stated level of concern.
Next, the companion should identify their level of concern (“not at all”, “a little”, or “a lot) for each topic in regard to the patient’s health. Draw an “X” through the number that reflects the companion’s level of concern. It is fine if the companion’s concerns are different than those of the patient.
Together decide which identified concern or concerns are most important to discuss with the doctor. Use the right column to check at least three topics to discuss with your doctor today.
It is important to remember that doctors are used to talking about all kinds of health and personal matters, including topics that may be sensitive, like memory problems, depression, or sexual function. Talking honestly with your doctor about your concerns is the first step in an effective partnership.
Concerns to Discuss with Your Doctor Today
| Common Concerns | Level of Concern | Discuss with Doctor | ||
|---|---|---|---|---|
| Not at All | A Little | A Lot | ||
| Shortness of breath | 1 | 2 | 3 | |
| Pain | 1 | 2 | 3 | |
| Falling or fear of falling | 1 | 2 | 3 | |
| Dizziness or balance | 1 | 2 | 3 | |
| Hearing or vision | 1 | 2 | 3 | |
| Trouble with sleep | 1 | 2 | 3 | |
| Lack of energy | 1 | 2 | 3 | |
| Incontinence/bladder problems | 1 | 2 | 3 | |
| Constipation or bowel problems | 1 | 2 | 3 | |
| Poor appetite or weight loss | 1 | 2 | 3 | |
| Concerns about driving | 1 | 2 | 3 | |
| Difficulty bathing, dressing, or walking | 1 | 2 | 3 | |
| Receiving the help I need | 1 | 2 | 3 | |
| Getting out to do the things I enjoy | 1 | 2 | 3 | |
| Regular exercise | 1 | 2 | 3 | |
| Stress or worry | 1 | 2 | 3 | |
| Feeling sad or blue | 1 | 2 | 3 | |
| Trouble concentrating or remembering | 1 | 2 | 3 | |
| Sexual function or sexuality | 1 | 2 | 3 | |
| Smoking or alcohol use | 1 | 2 | 3 | |
| Medication issues side effects | 1 | 2 | 3 | |
| Results from a lab test or consultation | 1 | 2 | 3 | |
| Keeping up with appointments | 1 | 2 | 3 | |
| Other issues/concerns | 1 | 2 | 3 | |
| 1 | 2 | 3 | ||
Help from Your Companion
Having a companion attend a doctor visit can be useful, particularly when they know how to help. Listed below are several ways a companion might support a patient during their doctor visit. Read through this list together. Then, the patient should identify what help they would like from their companion during today’s visit.
There may be some visits where a patient would like the help of their companion and other visits they prefer to attend alone. This is fine too. Often, it is just a matter of talking about your wishes. Take a few minutes to talk about the visit today.
| I would like my companion to (check all that apply) |
|---|
| Listen to what the doctor says. |
| Take notes (for example, about your diagnosis, medications, diet, or referrals). |
| Remind me to ask my questions. |
| Ask the doctor questions directly, on my behalf. |
| Remind me to tell the doctor about my symptoms. |
| Provide information about my health to the doctor. |
| Make sure I understand what the doctor says. |
| Stay in the waiting room for part of the visit. |
| Stay in the waiting room for the entire visit so that I may talk to the doctor alone. |
| List other help you would like from your companion below: |
There may be some visits where a patient would like the help of their companion and other visits they prefer to attend alone. This is fine too. Often, it is just a matter of talking about your wishes. Take a few minutes to talk about the visit today.
Footnotes
Author Contributions: Wolff: Study concept and design, acquisition of subjects, analysis and interpretation of data, and preparation of manuscript. Roter: Study concept, interpretation of data, and critical revision of manuscript. Barron: acquisition of subjects, interpretation of data, and critical revision of final manuscript. Boyd: Study concept, interpretation of data, and critical revision of manuscript. Leff: Study concept, interpretation of data, and critical revision of manuscript. Finucane: acquisition of subjects, interpretation of data, and critical revision of final manuscript. Gallo: Study concept, interpretation of data, and critical revision of manuscript. Rabins: Study concept, interpretation of data, and critical revision of manuscript. Roth: Study design, interpretation of data, and approval of manuscript. Gitlin: Study concept and design, interpretation of data, and critical revision of manuscript.
Conflict of Interest:
FUNDING: This study was supported by National Institute of Mental Health grant K01MH082885 “Optimizing Family Involvement in Late-Life Depression Care” to Jennifer Wolff.
Jennifer Wolff: (In respect to Grants) reports funding from National Institute of Mental Health grant K01MH082885
Debra Roter: (In respect to Royalties). I am the author of the Roter Interaction Analysis System (RIAS) and hold the copyright for the system. Johns Hopkins University also has rights to the RIAS coding software. Neither Debra Roter nor Johns Hopkins collects royalties for use of the system in research as is the case for the current study.
(In respect to Affiliation) I am a co-owner of RIASWorks LLC, a company that provides RIAS coding services for non-university projects and it is possible that RIASWorks would benefit indirectly from dissemination of the current research.
Jeremy Barron: no conflicts
Cynthia Boyd: (In respect to Grants) reports receipt of a Paul Beeson Career Development Award (NIA K23 AG032910 from AFAR, The John A. Hartford Foundation, The Atlantic Philanthropies, The Starr Foundation and an anonymous donor).
Bruce Leff: (In respect to Affiliation) reports member of Measure Application Partnership, National Quality Forum Post-Acute and Long-Term Care Committee, (In respect to Grants) reports funding from NIA, John A. Hartford Foundation, Commonwealth Fund, and Retirement Research Fund, (In respect to Honoraria) reports CMS Technical Expert Panels, (In respect to Consultant) reports L&M Policy Research Group, (In respect to Royalties) reports Hospital at Home, (in respect to Board Member) reports American Academy of Home Care Physicians, American College of Physicians, Alliance for Home Health Quality and Innovation.
Thomas Finucane: no conflicts
Peter Rabins: (In respect to Royalties). I receive book royalties for “The 36-Hour Day.”
Joseph Gallo: no conflicts
David Roth: no conflicts
Laura Gitlin: no conflicts
References
- 1.Ryan C, Siebens J. Educational attainment in the United States: 2009. Washington, DC: US Census Bureau; 2012. pp. P20–566. [Google Scholar]
- 2.Plassman BL, Langa KM, Fisher GG, et al. Prevalence of dementia in the United States: the aging, demographics, and memory study. Neuroepidemiology. 2007;29:125–132. doi: 10.1159/000109998. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Lin FR, Niparko JK, Ferrucci L. Hearing loss prevalence in the United States. Arch Intern Med. 2011;171:1851–1852. doi: 10.1001/archinternmed.2011.506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Kinnersley P, Edwards A, Hood K, et al. Interventions before consultations to help patients address their information needs by encouraging question asking: Systematic review. BMJ. 2008;337:a485. doi: 10.1136/bmj.a485. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Haywood K, Marshall S, Fitzpatrick R. Patient participation in the consultation process: a structured review of intervention strategies. Patient Educ Couns. 2006;63:12–23. doi: 10.1016/j.pec.2005.10.005. [DOI] [PubMed] [Google Scholar]
- 6.Berkman ND, Sheridan SL, Donahue KE, et al. Health literacy interventions and outcomes: An updated systematic review. Evid Rep Technol Assess. 2011;199:1–941. [PMC free article] [PubMed] [Google Scholar]
- 7.Manafo E, Wong S. Health literacy programs for older adults: A systematic literature review. Health Educ Res. 2012;27:947–960. doi: 10.1093/her/cys067. [DOI] [PubMed] [Google Scholar]
- 8.Wolff J, Roter D. Hidden in plain sight: Medical visit companions as a quality of care resource for vulnerable older adults. Arch Intern Med. 2008;168:1409–1415. doi: 10.1001/archinte.168.13.1409. [DOI] [PubMed] [Google Scholar]
- 9.Wolff J, Roter D. Family presence in routine medical visits: A meta-analytical review. Soc Sci Med. 2011;72:823–831. doi: 10.1016/j.socscimed.2011.01.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Wolff J, Boyd C, Gitlin L, et al. Going it Together: Persistence of older adults’ accompaniment to physician visits by a family companion. J Am Geriatr Soc. 2012;60:106–112. doi: 10.1111/j.1532-5415.2011.03770.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Ong L, de Haes J, Hoos A, et al. Doctor-patient communication: A review of the literature. Soc Sci Med. 1995;40:903–918. doi: 10.1016/0277-9536(94)00155-m. [DOI] [PubMed] [Google Scholar]
- 12.Brundage MD, Feldman-Stewart D, Tishelman C, et al. How do interventions designed to improve provider-patient communication work? Illustrative applications of a framework for communication. Acta Oncol. 2010;49:136–143. doi: 10.3109/02841860903483684. [DOI] [PubMed] [Google Scholar]
- 13.Protheroe J, Brooks H, Chew-Graham C, et al. ‘Permission to participate?’: A qualitative study of participation in patients from differing socio-economic backgrounds. J Health Psychol. 2013;18:1046–1055. doi: 10.1177/1359105312459876. [DOI] [PubMed] [Google Scholar]
- 14.Adelman R, Greene M, Ory M. Communication between older patients and their physicians. Clin Geriatr Med. 2000;16:1–24. doi: 10.1016/s0749-0690(05)70004-5. [DOI] [PubMed] [Google Scholar]
- 15.Sneeuw KC, Sprangers MA, Aaronson NK. The role of health care providers and significant others in evaluating the quality of life of patients with chronic disease. J Clin Epidemiol. 2002;55:1130–1143. doi: 10.1016/s0895-4356(02)00479-1. [DOI] [PubMed] [Google Scholar]
- 16.Silveira MJ, Given CW, Given B, et al. Patient-caregiver concordance in symptom assessment and improvement in outcomes for patients undergoing cancer chemotherapy. Chronic illn. 2010;6:46–56. doi: 10.1177/1742395309359208. [DOI] [PubMed] [Google Scholar]
- 17.Bogardus S, Bradley E, Williams C, et al. Goals for the care of frail older adults: Do caregivers and clinicians agree? Am J Med. 2001;110:97–102. doi: 10.1016/s0002-9343(00)00668-9. [DOI] [PubMed] [Google Scholar]
- 18.Glazier S, Schuman J, Keltz E, et al. Taking the next steps in goal ascertainment: A prospective study of patient, team, and family perspectives using a comprehensive standardized menu in a geriatric assessment and treatment unit. J Am Geriatr Soc. 2004;52:284–289. doi: 10.1111/j.1532-5415.2004.52072.x. [DOI] [PubMed] [Google Scholar]
- 19.Kiesler D, Auerbach S. Optimal matches of patient preferences for information, decision-making and interpersonal behavior: Evidence, models and interventions. Patient Educ Couns. 2006;61:319–341. doi: 10.1016/j.pec.2005.08.002. [DOI] [PubMed] [Google Scholar]
- 20.Strickland BR. Internal-external expectancies and health-related behaviors. J Consult Clin Psychol. 1978;46:1192–1211. doi: 10.1037//0022-006x.46.6.1192. [DOI] [PubMed] [Google Scholar]
- 21.Callahan CM, Unverzagt FW, Hui SL, et al. Six-item screener to identify cognitive impairment among potential subjects for clinical research. Med Care. 2002;40:771–781. doi: 10.1097/00005650-200209000-00007. [DOI] [PubMed] [Google Scholar]
- 22.Wallace LS, Rogers ES, Roskos SE, et al. Brief report: Screening items to identify patients with limited health literacy skills. J Gen Intern Med. 2006;21:874–877. doi: 10.1111/j.1525-1497.2006.00532.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Roter D, Larson S. The Roter interaction analysis system (RIAS): Utility and flexibility for analysis of medical interactions. Patient Educ Couns. 2002;46:243–251. doi: 10.1016/s0738-3991(02)00012-5. [DOI] [PubMed] [Google Scholar]
- 24.Mead N, Bower P. Measuring patient-centredness: A comparison of three observation-based instruments. Patient Educ Couns. 2000;39:71–80. doi: 10.1016/s0738-3991(99)00092-0. [DOI] [PubMed] [Google Scholar]
- 25.Patient-centered care for older adults with multiple chronic conditions: a stepwise approach from the american geriatrics society: American Geriatrics Society expert panel on the care of older adults with multimorbidity. J Am Geriatr Soc. 2012;60:1957–1968. doi: 10.1111/j.1532-5415.2012.04187.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Boyd C, Darer J, Boult C, et al. Clinical practice guidelines and quality of care for older patients with multiple comorbid diseases: implications for pay for performance. JAMA. 2005;294:716–724. doi: 10.1001/jama.294.6.716. [DOI] [PubMed] [Google Scholar]
- 27.Paasche-Orlow MK, Wolf MS. The causal pathways linking health literacy to health outcomes. Am J Health Behav. 2007;31 (Suppl 1):S19–26. doi: 10.5555/ajhb.2007.31.supp.S19. [DOI] [PubMed] [Google Scholar]
- 28.Smith SK, Dixon A, Trevena L, et al. Exploring patient involvement in healthcare decision making across different education and functional health literacy groups. Soc Sci Med. 2009;69:1805–1812. doi: 10.1016/j.socscimed.2009.09.056. [DOI] [PubMed] [Google Scholar]
- 29.Mitnick S, Leffler C, Hood V. Family caregivers, patients and physicians: Ethical guidance to optimize relationships. J Gen intern Med. 2010;25:255–260. doi: 10.1007/s11606-009-1206-3. [DOI] [PMC free article] [PubMed] [Google Scholar]