Abstract
Objective:
Positive family history is associated with increased type 2 diabetes (T2D) risk, and reflects both genetic and environmental risks. Several studies have suggested an excess maternal transmission of T2D, although the underlying mechanism is unknown. We aimed to examine the association between maternal diabetes and cardiometabolic risk in the offspring.
Methods:
Parental history of diabetes and clinical data including anthropometric traits, fasting plasma glucose and insulin (FPG, FPI), blood pressure and lipid profile were collected from 2581 unrelated Chinese offspring (2026 adolescents from a population-based school survey and 555 adults from a community-based health screening programme). A subset of subjects (n=834) underwent oral glucose tolerance test to measure the glucose and insulin concentrations at 0, 15, 30, 60 and 120 min for evaluation of the areas under the curve (AUC) of glucose and insulin at 0–120 min, homoeostasis model assessment of insulin resistance (HOMA-IR) and bell-cell function, insulinogenic index, insulin sensitivity index (ISI) and oral disposition index (DI).
Results:
A positive parental history of diabetes was associated with increased risk of obesity (odd ratios (OR) (95% confidence interval (CI))=1.48 (1.10–2.00)), central obesity (OR (95% CI)=1.67 (1.21–2.32)), higher FPI, HOMA-IR, 2-h insulin, AUC of glucose at 0–120 min, triglycerides, reduced ISI and DI. Compared with individuals without parental diabetes, offspring with diabetic mother had significantly increased risk of obesity (OR (95% CI)=1.59 (1.07–2.35)), central obesity (OR (95% CI)=1.88 (1.23–2.88)), higher glucose levels and BP, were more insulin resistant but also had impaired first-phase insulin response and worse lipid profile. However, paternal history of diabetes had no effect on any of the studied traits, except higher body mass index, waist circumference in females and FPG.
Conclusions:
Our findings suggested that maternal history of diabetes conferred increased risk of cardiometabolic abnormalities, and was associated with both insulin resistance and impaired first-phase insulin secretion. Further investigation into the mechanism of transgenerational diabetes is warranted.
Introduction
With the adoption of a modern lifestyle and the lack of physical activity, there has been a twofold increase in the prevalence of type 2 diabetes (T2D) in China during the last two decades.1 T2D is a multifactorial disease resulting from the interaction between genetic and environmental factors, leading to insulin resistance and β-cell dysfunction.2 The genetic component has been strongly supported by the familial clustering of the disease in multiple populations.3, 4, 5, 6, 7, 8, 9 These studies have shown that a positive family history (FH) of diabetes is associated with an increased risk of T2D3, 4, 5, 6, 7, 8, 9 and an earlier age of onset in the offspring.10, 11 Moreover, a study conducted in Singapore demonstrated the association between FH of T2D and the presence of cardiometabolic risk factors, including obesity, increased homoeostasis model assessment of insulin resistance (HOMA-IR), fasting triglyceride (TG), and reduced high-density lipoprotein (HDL) cholesterol and homoeostasis model assessment of β-cell function (HOMA-β).8
Recently, evidence of excess maternal inheritance of T2D has accumulated from epidemiological studies and animal models. For example, our previous study observed a higher frequency of diabetes in mother than in father among T2D patients.6 Moreover, women with gestational diabetes have been more frequently reported to have a diabetic mother than a diabetic father.12 Animal models also demonstrated the effect of maternal diabetes on impaired glucose tolerance in their offspring.13 Some6, 8, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27 but not all5, 7, 28, 29, 30 studies reported that offspring with maternal history of diabetes are more likely to develop diabetes and cardiometabolic disorders such as obesity, impaired glucose tolerance, insulin resistance, hyperinsulinaemia and dyslipidaemia compared with those with paternal history of diabetes. However, only limited data are available on the association between the parental history (PH) of diabetes and cardiometabolic risk. Therefore, we aimed to examine the associations of cardiometabolic risk factors with (1) PH of diabetes (at least one parent diagnosed with diabetes); (2) paternal history of diabetes; (3) maternal history of diabetes; and (4) biparental history of diabetes in two independent cohorts of Chinese adolescents and adults. Finally, we estimate the odd ratios (ORs) (95% confidence intervals (CIs)) for obesity and central obesity by comparing subjects with PH of diabetes to those without PH of diabetes.
Materials and methods
Subjects
The study design, ascertainment, inclusion criteria and phenotyping of the study subjects have been described previously.31, 32, 33 All subjects were of southern Han Chinese ancestry residing in Hong Kong. Our study cohorts consist of 2309 adolescents and 559 adults selected from a population-based school survey for risk factor assessment and a community-based health screening programme, respectively. All participants or parents of adolescents were asked to complete a questionnaire including questions on FH of diabetes. We did not document the age at which the parents were diagnosed with diabetes. Positive PH was defined as having at least one diabetic parent. To estimate the parental transmission of cardiometabolic traits, participants with a positive PH of diabetes were further divided into three groups: (1) paternal history was defined as having only father with diabetes; (2) maternal history was defined as having only mother with diabetes; and (3) biparental history was defined as having both parents with diabetes. These groups were mutually exclusive. We excluded 283 (12.3%) adolescents and 4 (0.7%) adults with unknown diabetes status of their parents. Finally, 2026 adolescents (mean age 15.6±2.0 years, 45.5% male) and 555 adults (mean age 43.5±8.2 years, 48.3% male) were included in the subsequent analyses. This study was approved by the Clinical Research Ethics Committee of the Chinese University of Hong Kong. All participants or parents of adolescents gave written informed consent as appropriate.
Clinical studies
All study subjects were examined in the morning after an overnight fast. Anthropometric indices including body weight and height (BW), waist and hip circumference (WC and HC), and systolic and diastolic blood pressure (SBP and DBP) were measured. The body fat percentage (FAT) was measured by bioimpedence analysis (Tanita Corp., Tokyo, Japan). Body mass index (BMI) was calculated as weight (kg) divided by squared height (m2). Waist–hip ratio (WHR) was calculated as WC (cm) divided by HC (cm). A random spot specimen of urine was collected for the measurements of albumin-creatinine ratio (ACR). Fasting blood samples were collected for the measurements of fasting plasma glucose and insulin (FPG and FPI), as well as lipid profile (total cholesterol, TG, HDL cholesterol and low-density lipoprotein cholesterol ). HOMA-IR was calculated as (FPI × FPG)÷22.5, and HOMA-β was calculated as FPI × 20÷(FPG−3.5).34
A subset of the subjects (279 adolescents and 555 adults) also underwent a 75 g oral glucose tolerance test (OGTT) to measure the glucose and insulin concentrations at 0, 15, 30, 60 and 120 min. Areas under the curve (AUC) for glucose and insulin during OGTT at 0–120 min were calculated using the trapezoid rule. Insulinogenic index was assessed as (insulin during OGTT at 30 min−0 min)÷(glucose during OGTT at 30 min−0 min).35 Insulin sensitivity index (ISI) was estimated using the formula proposed by Matsuda and DeFronzo:36 10 000÷square root of [FPG × FPI × (mean glucose during OGTT) × (mean insulin during OGTT)]. Oral disposition index (DI) was calculated as (insulin during OGTT at 30 min−0 min)÷(glucose during OGTT at 30 min−0 min)÷HOMA-IR.37
In adolescents, overweight or obesity was defined on the basis of the age- and sex-specific cutoff for BMI from an international survey.38 Central obesity was defined using the 90th percentile of WC or adult cutoff if lower.39 In adults, overweight and obesity were defined as BMI ⩾25 and ⩾30 kg m−2, respectively. Central obesity was defined as WC ⩾90 cm for male or 80 cm for female.39
Statistical analysis
All statistical analyses were performed using SPSS for Windows v.18 (SPSS, Chicago, IL, USA). Two-tailed P-values <0.05 were considered statistically significant.
Data are presented as percentage (n), mean±s.d. or geometric mean (95% CI) (where appropriate). FPI, HOMA-IR, HOMA-β, insulin concentrations during OGTT at 0, 15, 30, 60 and 120 min, insulin AUC during OGTT at 0–120 min, insulinogenic index, ISI, DI, TG and ACR were log transformed due to skewed distributions. Each cardiometabolic trait was winsorized separately in adult and adolescent cohorts by replacing the extreme values with four s.d. from the mean. In total, 0.25% and 0.31% of data in adolescents and adults were replaced, respectively.
Within each cohort, associations between cardiometabolic risk factors and PH categories were tested by multiple linear regression analysis, adjusted for sex and age. Three dummy variables were used to code for the PH categories (paternal, maternal and biparental history of diabetes) and each group was compared with the group without diabetic parent. We conducted the logistic regression analysis to estimate the ORs with 95% CIs for dichotomous traits (overweight or obesity and central obesity). To combine the results from the two cohorts, meta-analyses under fixed- and random-effects models were performed by weighting the β-coefficient of each study using the inverse of their variance. Cochran's Q statistic and I2 index were used to assess heterogeneity of effects across cohorts. The Q test informs us about the presence versus the absence of heterogeneity, whereas I2 index quantifies the degree of heterogeneity in meta-analysis. I2 values around 25, 50 and 75% would mean low, medium and high heterogeneity, respectively. Multiple testing of phenotypic traits was corrected by a sharper Bonferroni procedure suggested by Hochberg.40
Results
Cohort description
The demographic characteristics of the participants are summarized in Table 1. Among 2026 adolescents, 1861 (91.86%) subjects had no PH of diabetes, whereas 95 (4.69%) had a diabetic father, 69 (3.41%) had a diabetic mother and 1 (0.05%) had two diabetic parents. In this cohort, the prevalence of T2D, obesity and central obesity were 0.05%, 13.0% and 7.4%, respectively. Among 555 adults, 411 (74.05%) subjects had no PH of diabetes, whereas 45 (8.11%) had a diabetic father, 84 (15.14%) had a diabetic mother and 15 (2.70%) had two diabetic parents. In this cohort, the prevalence of T2D, obesity and central obesity were 6.8%, 32.3% and 24.5%, respectively. Tables 2 and 3 show the cardiometabolic characteristics of the individuals stratified by parental diabetes status.
Table 1. Demographic characteristics of 2026 and 555 Chinese adolescents and adults, respectively.
| Adolescents | Adults | |
|---|---|---|
| N | 2026 | 555 |
| Sex (male %) | 45.5% (922) | 48.3% (268) |
| Age (years) | 15.6±2.0 | 43.5±8.2 |
| Parental history of diabetes | ||
| No parental history (%) | 91.86% (1861) | 74.05% (411) |
| Paternal history (%) | 4.69% (95) | 8.11% (45) |
| Maternal history (%) | 3.41% (69) | 15.14% (84) |
| Biparental history (%) | 0.05% (1) | 2.70% (15) |
| Proportion of participants with OGTT data (%) | 13.8% (279) | 100.0% (555) |
| Type 2 diabetes (%) | 0.05% (1) | 6.8% (38) |
| Overweight or obesity (%) | 13.0% (264) | 32.3% (179) |
| Central obesity (%) | 7.4% (150) | 24.5% (136) |
Abbreviation: OGTT, oral glucose tolerance test.
Data were expressed as % (n) or mean±s.d.
Table 2. Clinical and cardiometabolic characteristic of adolescents and adults stratified by parental history (yes/no).
|
Adolescents |
Adults |
Meta-analysis |
||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
Parental diabetic history |
Padjusted |
Parental diabetic history |
Padjusted | Pfixed | Prandom |
Heterogeneity test |
||||
| No | Yes | No | Yes | PQ | I2 | |||||
| N | 1861 | 165 | — | 411 | 144 | — | — | — | — | — |
| Sex (male %) | 44.8% (833) | 53.9% (89) | 0.0239 | 199 (48%) | 69 (48%) | 0.9174 | — | — | — | — |
| Age (years) | 15.55±2.04 | 15.76±2.08 | 0.1265 | 43.9±8.35 | 42.51±7.74 | 0.0807 | — | — | — | — |
| Obesity traits | ||||||||||
| Body height (cm) | 161.4±8.3 | 162.3±9.6 | 0.7238 | 161.6±8.1 | 160.4±8.8 | 0.0108 | 0.0440 | 0.2009 | 0.1058 | 0.6177 |
| Body weight (kg) | 52.1±11.2 | 55.3±12.9 | 0.0081 | 61.8±10.9 | 63±12.6 | 0.1988 | 0.0048 | 0.0048 | 0.3908 | 0.0000 |
| Body mass index (kg m−2) | 19.9±3.4 | 20.9±3.9 | 0.0013 | 23.6±3.3 | 24.4±4 | 0.0071 | 2.6 × 10−5 | 2.6 × 10−5 | 0.9882 | 0.0000 |
| Waist circumference (cm) | ||||||||||
| Male | 71.2±8.5 | 72.8±9.3 | 0.1382 | 83.8±8.2 | 85.5±9.5 | 0.1378 | 0.0370 | 0.0370 | 0.7954 | 0.0000 |
| Female | 65.6±6.6 | 67.5±8 | 0.0219 | 74.1±8.3 | 74.9±9.2 | 0.3339 | 0.0150 | 0.0150 | 0.5939 | 0.0000 |
| Hip circumference (cm) | 88.9±7.7 | 90.4±8.8 | 0.0693 | 93.7±5.8 | 94.6±7.1 | 0.1562 | 0.0224 | 0.0224 | 0.7465 | 0.0000 |
| Waist–hip ratio | 0.77±0.05 | 0.78±0.05 | 0.0122 | 0.84±0.07 | 0.84±0.08 | 0.1768 | 0.0045 | 0.0045 | 0.8264 | 0.0000 |
| Body fat percentage (%) | 21.2±6.9 | 21.9±7.9 | 0.0292 | 27.5±6.6 | 28.6±7.5 | 0.0565 | 0.0037 | 0.0037 | 0.9854 | 0.0000 |
| Glucose-related traits | ||||||||||
| Fasting plasma glucose (mmol l−1) | 4.7±0.35 | 4.72±0.36 | 0.5558 | 4.96±0.62 | 5.18±0.75 | 2.1 × 10−4 | 0.0381 | 0.2760 | 0.0016 | 0.9001 |
| Fasting plasma insulin (pmol l−1) | 46.8 (45.8–47.7) | 49.8 (46.4–53.4) | 0.0377 | 44.4 (41.3–47.8) | 53.6 (47.9–60.1) | 0.0113 | 0.0028 | 0.0314 | 0.1753 | 0.4555 |
| HOMA-IR | 1.62 (1.59–1.66) | 1.73 (1.61–1.87) | 0.0393 | 1.62 (1.51–1.75) | 2.05 (1.82–2.31) | 0.0023 | 0.0013 | 0.0638 | 0.0675 | 0.7009 |
| HOMA-β | 135.8 (132.8–139) | 143.5 (133.1–154.7) | 0.1113 | 109 (100.9–117.8) | 115.5 (102.1–130.6) | 0.6061 | 0.0993 | 0.0993 | 0.7663 | 0.0000 |
| 2-h glucose (mmol l−1)a | 6.05±1.61 | 6.15±1.5 | 0.6928 | 6.39±2.31 | 6.79±2.75 | 0.0488 | 0.0732 | 0.0732 | 0.3577 | 0.0000 |
| 2-h insulin (pmol l−1)a | 460.8 (415.9–510.5) | 492 (376–643.8) | 0.6031 | 271.4 (252.8–291.5) | 313.7 (276.3–356.3) | 0.0535 | 0.0495 | 0.0495 | 0.6937 | 0.0000 |
| Glucose AUC during OGTT at 0–120 mina | 814.9±160.9 | 835.7±140.3 | 0.4652 | 893.8±224 | 954.5±263.4 | 0.0027 | 0.0045 | 0.0318 | 0.2151 | 0.3492 |
| Insulin AUC during OGTT at 0–120 mina | 59702 (55381–64360) | 56779 (45538–70795) | 0.7045 | 36227 (34372–38182) | 40664 (36720–45032) | 0.0587 | 0.1274 | 0.3453 | 0.2353 | 0.2899 |
| Insulinogenic indexa | 32 (29–35.4) | 27.6 (21–36.1) | 0.3145 | 13.2 (12.2–14.3) | 12.8 (10.9–15.1) | 0.5342 | 0.3028 | 0.3028 | 0.5594 | 0.0000 |
| Insulin sensitivity indexa | 68.2 (62.7–74.3) | 63.3 (49.8–80.4) | 0.4803 | 93.8 (88.4–99.6) | 77 (69.2–85.6) | 0.0014 | 0.0015 | 0.0015 | 0.4284 | 0.0000 |
| Oral disposition indexa | 17.64 (15.9–19.57) | 12.64 (10.36–15.43) | 0.0294 | 8.46 (7.65–9.36) | 6.21 (5.15–7.48) | 0.0015 | 1.1 × 10−4 | 1.1 × 10−4 | 0.9682 | 0.0000 |
| Blood pressure | ||||||||||
| Systolic blood pressure (mm Hg) | 116.8±12.6 | 118.4±13.8 | 0.3760 | 117±17.8 | 119.3±19 | 0.0387 | 0.0654 | 0.1319 | 0.1947 | 0.4055 |
| Diastolic blood pressure (mm Hg) | 72.6±9.2 | 71.8±9.9 | 0.3419 | 75.5±10.7 | 77.1±11.7 | 0.0419 | 0.6244 | 0.6748 | 0.0281 | 0.7926 |
| Lipid profile | ||||||||||
| Total cholesterol (mmol l−1) | 4.17±0.7 | 4.19±0.72 | 0.5544 | 5.21±0.93 | 5.32±0.98 | 0.0849 | 0.1500 | 0.1842 | 0.2624 | 0.2038 |
| Triglycerides (mmol l−1) | 0.76 (0.75–0.77) | 0.77 (0.73–0.82) | 0.4085 | 1.07 (1.01–1.12) | 1.18 (1.08–1.29) | 0.0183 | 0.0465 | 0.1481 | 0.1275 | 0.5696 |
| HDL cholesterol (mmol l−1) | 1.6±0.31 | 1.6±0.32 | 0.9900 | 1.59±0.42 | 1.53±0.4 | 0.0970 | 0.3504 | 0.4095 | 0.1691 | 0.4713 |
| LDL cholesterol (mmol l−1) | 2.2±0.6 | 2.21±0.65 | 0.6292 | 3.06±0.84 | 3.19±0.85 | 0.0351 | 0.1275 | 0.2445 | 0.1234 | 0.5788 |
| Cardiovascular risk factor | ||||||||||
| Albumin-creatinine ratio | 0.61 (0.58–0.64) | 0.58 (0.49–0.68) | 0.7971 | 0.81 (0.73–0.89) | 0.88 (0.73–1.08) | 0.2856 | 0.6159 | 0.6159 | 0.3280 | 0.0000 |
Abbreviations: AUC, areas under the curve; HDL, high-density lipoprotein; HOMA-IR, homoeostasis model assessment of insulin resistance; HOMA-β, homoeostasis model assessment of β-cell function; LDL, low-density lipoprotein; OGTT, oral glucose tolerance test.
Data were expressed as n, %, mean±s.d. or geometric mean (95% confidence interval).
Padjusted refers to P-value obtained from linear regression adjusted by sex and age.
Pfixed and Prandom refer to P-value obtained from meta-analysis using fixed- and random-effect model, respectively.
PQ refers to P-value of Cochran's Q statistics in heterogeneity test.
I2 index is used to quantify the degree of heterogeneity of β-coefficient. I2 values around 25, 50 and 75% would mean low, medium and high heterogeneity.
Indicates only a subset of samples (285 adolescents and 555 adults) who were included in the analysis.
Table 3. Clinical and cardiometabolic characteristic of adolescents and adults stratified by parental history categories.
| Phenotype | Parental history categories |
Adolescent |
Adults |
Meta-analysis |
|||||
|---|---|---|---|---|---|---|---|---|---|
| Value | Padjusted | Value | Padjusted | Pfixed | Prandom | PQ | I2 | ||
| N | No parental | 1861 (91.86%) | — | 411 (74.05%) | — | — | — | — | — |
| Paternal | 95 (4.69%) | — | 45 (8.11%) | — | — | — | — | — | |
| Maternal | 69 (3.41%) | — | 84 (15.14%) | — | — | — | — | — | |
| Both | 1 (0.05%) | — | 15 (2.70%) | — | — | — | — | — | |
| Sex (male %) | No parental | 833 (44.8%) | — | 199 (48%) | — | — | — | — | — |
| Paternal | 55 (57.9%) | 0.0130 | 23 (51%) | 0.7316 | — | — | — | — | |
| Maternal | 34 (49.3%) | 0.4597 | 39 (46%) | 0.7395 | — | — | — | — | |
| Both | — | — | 7 (47%) | 0.8939 | — | — | — | — | |
| Age (years) | No parental | 15.55±2.04 | — | 43.9±8.35 | — | — | — | — | — |
| Paternal | 15.88±2.13 | 0.0649 | 42.04±7.35 | 0.1373 | — | — | — | — | |
| Maternal | 15.6±2.03 | 0.7743 | 43.26±7.99 | 0.5398 | — | — | — | — | |
| Both | — | — | 39.67±7.12 | 0.0505 | — | — | — | — | |
| Obesity traits | |||||||||
| Body height (cm) | No parental | 161.4±8.3 | Reference | 161.6±8.1 | Reference | — | — | — | — |
| Paternal | 162.7±9.7 | 0.6420 | 160.9±7.7 | 0.1312 | 0.1999 | 0.1999 | 0.3541 | 0.0000 | |
| Maternal | 161.9±9.5 | 0.9869 | 160.1±9.1 | 0.0434 | 0.1289 | 0.2875 | 0.1805 | 0.4423 | |
| Both | — | — | 160.4±10.6 | 0.2393 | — | — | — | — | |
| Body weight (kg) | No parental | 52.1±11.2 | Reference | 61.8±10.9 | Reference | — | — | — | — |
| Paternal | 54.9±13.8 | 0.2115 | 63±10.3 | 0.6155 | 0.1924 | 0.1924 | 0.7335 | 0.0000 | |
| Maternal | 55.9±11.7 | 0.0083 | 63.6±14 | 0.0727 | 0.0020 | 0.0020 | 0.4299 | 0.0000 | |
| Both | — | — | 59.5±10.9 | 0.3407 | — | — | — | — | |
| Body mass index (kg m−2) | No parental | 19.9±3.4 | Reference | 23.6±3.3 | Reference | — | — | — | — |
| Paternal | 20.6±4 | 0.1224 | 24.3±3.6 | 0.1480 | 0.0367 | 0.0367 | 0.7275 | 0.0000 | |
| Maternal | 21.2±3.7 | 0.0016 | 24.7±4.2 | 0.0042 | 2.0 × 10−5 | 2.0 × 10−5 | 0.8105 | 0.0000 | |
| Both | — | — | 23.1±3.2 | 0.7137 | — | — | — | — | |
| Waist circumference | |||||||||
| Male (cm) | No parental | 71.2±8.5 | Reference | 83.8±8.2 | Reference | — | — | — | — |
| Paternal | 72.2±8.9 | 0.6683 | 82.7±7 | 0.5537 | 0.9611 | 0.9611 | 0.4653 | 0.0000 | |
| Maternal | 73.9±9.9 | 0.0550 | 87.8±10.4 | 0.0066 | 0.0010 | 0.0010 | 0.5472 | 0.0000 | |
| Both | — | — | 81.9±8.5 | 0.6483 | — | — | — | — | |
| Female (cm) | No parental | 65.6±6.6 | Reference | 74.1±8.3 | Reference | — | — | — | — |
| Paternal | 67.7±8.2 | 0.0554 | 76.7±11.5 | 0.0745 | 0.0107 | 0.0107 | 0.5503 | 0.0000 | |
| Maternal | 67.2±8 | 0.1923 | 74.9±8.4 | 0.5364 | 0.1626 | 0.1626 | 0.7129 | 0.0000 | |
| Both | — | — | 69.6±5.1 | 0.2156 | — | — | — | — | |
| Hip circumference (cm) | No parental | 88.9±7.7 | Reference | 93.71±5.83 | Reference | — | — | — | — |
| Paternal | 90.2±9.3 | 0.3157 | 94.36±6.6 | 0.6054 | 0.2703 | 0.2703 | 0.8074 | 0.0000 | |
| Maternal | 90.5±8.3 | 0.1078 | 95.16±7.61 | 0.0482 | 0.0108 | 0.0108 | 0.9690 | 0.0000 | |
| Both | — | — | 92.3±5.1 | 0.3331 | — | — | — | — | |
| Waist–hip ratio | No parental | 0.77±0.05 | Reference | 0.8±0.1 | Reference | — | — | — | — |
| Paternal | 0.78±0.04 | 0.0651 | 0.8±0.1 | 0.4977 | 0.0510 | 0.0510 | 0.8090 | 0.0000 | |
| Maternal | 0.78±0.06 | 0.0717 | 0.85±0.08 | 0.0736 | 0.0116 | 0.0116 | 0.7682 | 0.0000 | |
| Both | — | — | 0.81±0.07 | 0.3082 | — | — | — | — | |
| Body fat percentage (%) | No parental | 21.2±6.9 | Reference | 27.5±6.6 | Reference | — | — | — | — |
| Paternal | 21.3±8.3 | 0.3101 | 28.1±7.8 | 0.3868 | 0.1843 | 0.1843 | 0.8927 | 0.0000 | |
| Maternal | 22.7±7.2 | 0.0295 | 29.1±7.5 | 0.0372 | 0.0026 | 0.0026 | 0.8841 | 0.0000 | |
| Both | — | — | 27.3±6.1 | 0.8967 | — | — | — | — | |
| Glucose-related traits | |||||||||
| Fasting plasma glucose (mmol l−1) | No parental | 4.7±0.35 | Reference | 4.96±0.62 | Reference | — | — | — | — |
| Paternal | 4.75±0.36 | 0.1505 | 5.15±0.69 | 0.0461 | 0.0427 | 0.1580 | 0.1620 | 0.4886 | |
| Maternal | 4.68±0.35 | 0.5541 | 5.18±0.82 | 0.0026 | 0.3461 | 0.4565 | 0.0033 | 0.8838 | |
| Both | — | — | 5.23±0.56 | 0.0560 | — | — | — | — | |
| Fasting plasma insulin (pmol l−1) | No parental | 46.8 (45.8–47.7) | Reference | 44.4 (41.3–47.8) | Reference | — | — | — | — |
| Paternal | 47.7 (43.7–52.1) | 0.4590 | 46.3 (38.3–56.1) | 0.8039 | 0.4357 | 0.4357 | 0.9584 | 0.0000 | |
| Maternal | 52.8 (47.2–59) | 0.0122 | 59.8 (51.6–69.4) | 7.8 × 10−4 | 1.1 × 10−4 | 0.0178 | 0.0958 | 0.6395 | |
| Both | — | — | 45 (30.3–66.8) | 0.9490 | — | — | — | — | |
| HOMA-IR | No parental | 1.62 (1.59–1.66) | Reference | 1.62 (1.51–1.75) | Reference | — | — | — | — |
| Paternal | 1.68 (1.53–1.84) | 0.3453 | 1.77 (1.44–2.16) | 0.5560 | 0.2727 | 0.2727 | 0.8515 | 0.0000 | |
| Maternal | 1.82 (1.62–2.05) | 0.0222 | 2.29 (1.96–2.67) | 2.1 × 10−4 | 1.2 × 10−4 | 0.0444 | 0.0382 | 0.7671 | |
| Both | — | — | 1.73 (1.14–2.64) | 0.8010 | — | — | — | — | |
| HOMA-β | No parental | 135.8 (132.8–139) | Reference | 109 (100.9–117.8) | Reference | — | — | — | — |
| Paternal | 132.7 (119.8–147.1) | 0.8636 | 101.1 (82.4–124) | 0.4317 | 0.6347 | 0.6347 | 0.5156 | 0.0000 | |
| Maternal | 157.3 (141.1–175.3) | 0.0093 | 129.2 (109.6–152.4) | 0.0877 | 0.0019 | 0.0019 | 0.9499 | 0.0000 | |
| Both | — | — | 91 (63.8–129.9) | 0.2390 | — | — | — | — | |
| 2-h glucosea (mmol l−1) | No parental | 6.05±1.61 | Reference | 6.39±2.31 | Reference | — | — | — | — |
| Paternal | 5.85±1.24 | 0.7081 | 6.04±2.6 | 0.4750 | 0.4389 | 0.4389 | 0.8190 | 0.0000 | |
| Maternal | 6.52±1.73 | 0.3097 | 7.17±2.79 | 0.0055 | 0.0041 | 0.0041 | 0.4661 | 0.0000 | |
| Both | — | — | 6.97±2.67 | 0.2277 | — | — | — | — | |
| 2-h insulina (pmol l−1) | No parental | 460.8 (415.9–510.5) | Reference | 271.4 (252.8–291.5) | Reference | — | — | — | — |
| Paternal | 409.2 (302.1–554.3) | 0.6941 | 270.9 (219.1–335) | 0.9497 | 0.7959 | 0.7959 | 0.7616 | 0.0000 | |
| Maternal | 613.8 (390.4–964.9) | 0.2193 | 348.8 (295.2–412.1) | 0.0057 | 0.0024 | 0.0024 | 0.9633 | 0.0000 | |
| Both | — | — | 269.3 (172.7–419.9) | 0.9047 | — | — | — | — | |
| Glucose AUC during OGTT at 0–120 mina | No parental | 814.9±160.9 | Reference | 893.8±224 | Reference | — | — | — | — |
| Paternal | 817±134.7 | 0.8978 | 901.7±247.3 | 0.6728 | 0.6912 | 0.6912 | 0.8468 | 0.0000 | |
| Maternal | 858.1±148.1 | 0.3296 | 974.9±269.3 | 0.0022 | 0.0019 | 0.0019 | 0.3891 | 0.0000 | |
| Both | — | — | 999.5±270.6 | 0.0361 | — | — | — | — | |
| Insulin AUC during OGTT at 0–120 mina | No parental | 59702 (55381–64360) | Reference | 36227 (34372–38182) | Reference | — | — | — | — |
| Paternal | 50525 (40950–62340) | 0.3569 | 40645 (33874–48770) | 0.2762 | 0.6612 | 0.9291 | 0.1740 | 0.4588 | |
| Maternal | 65970 (43200–100743) | 0.6458 | 42057 (36831–48025) | 0.0319 | 0.0307 | 0.0307 | 0.6810 | 0.0000 | |
| Both | — | — | 33719 (24145–47090) | 0.4542 | — | — | — | — | |
| Insulinogenic indexa | No parental | 32 (29–35.4) | Reference | 13.2 (12.2–14.3) | Reference | — | — | — | — |
| Paternal | 27.4 (19.5–38.4) | 0.4985 | 15.4 (11.7–20.4) | 0.3373 | 0.6863 | 0.7705 | 0.2697 | 0.1793 | |
| Maternal | 27.8 (17.6–44.1) | 0.4254 | 12.6 (10.3–15.5) | 0.5838 | 0.4084 | 0.4084 | 0.6139 | 0.0000 | |
| Both | — | — | 8.1 (4.5–14.7) | 0.0114 | — | — | — | — | |
| Insulin sensitivity indexa | No parental | 68.2 (62.7–74.3) | Reference | 93.8 (88.4–99.6) | Reference | — | — | — | — |
| Paternal | 74.2 (57–96.5) | 0.8120 | 85.4 (71.5–101.9) | 0.3830 | 0.5361 | 0.5361 | 0.5091 | 0.0000 | |
| Maternal | 51.6 (33.9–78.4) | 0.1701 | 70.9 (61.8–81.4) | 2.0 × 10−4 | 6.9 × 10−5 | 6.9 × 10−5 | 0.8594 | 0.0000 | |
| Both | — | — | 88.8 (60.3–130.7) | 0.7915 | — | — | — | — | |
| Oral disposition indexa | No parental | 17.6 (15.9–19.6) | Reference | 8.46 (7.65–9.36) | Reference | — | — | — | — |
| Paternal | 14 (11–18) | 0.2193 | 8.54 (6.1–11.95) | 0.9802 | 0.4158 | 0.4158 | 0.3552 | 0.0000 | |
| Maternal | 11 (8–15.2) | 0.0458 | 5.55 (4.4–7) | 5.7 × 10−4 | 6.3 × 10−5 | 6.3 × 10−5 | 0.9445 | 0.0000 | |
| Both | — | — | 4.66 (2.38–9.16) | 0.0178 | — | — | — | — | |
| Blood pressure | |||||||||
| Systolic blood pressure (mm Hg) | No parental | 116.8±12.6 | Reference | 117±17.8 | Reference | — | — | — | — |
| Paternal | 118.9±14 | 0.4134 | 114.2±17.9 | 0.5031 | 0.6635 | 0.6635 | 0.3351 | 0.0000 | |
| Maternal | 118.1±13.3 | 0.5032 | 121.9±19.4 | 0.0044 | 0.0237 | 0.1744 | 0.0605 | 0.7162 | |
| Both | — | — | 119.4±18 | 0.2091 | — | — | — | — | |
| Diastolic blood pressure (mm Hg) | No parental | 72.6±9.2 | Reference | 75.5±10.7 | Reference | — | — | — | — |
| Paternal | 72.2±9.7 | 0.7737 | 73.8±10.2 | 0.3681 | 0.4725 | 0.4725 | 0.5387 | 0.0000 | |
| Maternal | 71.3±10.4 | 0.2821 | 79±12.1 | 0.0014 | 0.1548 | 0.6080 | 0.0021 | 0.8940 | |
| Both | — | — | 76.1±11.6 | 0.5041 | — | — | — | — | |
| Lipid profile | |||||||||
| Total cholesterol (mmol l−1) | No parental | 4.17±0.7 | Reference | 5.21±0.93 | Reference | — | — | — | — |
| Paternal | 4.23±0.73 | 0.2548 | 5.17±0.91 | 0.9495 | 0.2990 | 0.2990 | 0.6369 | 0.0000 | |
| Maternal | 4.13±0.71 | 0.6784 | 5.37±1.02 | 0.0864 | 0.4542 | 0.5534 | 0.1095 | 0.6097 | |
| Both | — | — | 5.46±0.95 | 0.1044 | — | — | — | — | |
| Triglycerides (mmol l−1) | No parental | 0.76 (0.75–0.77) | Reference | 1.07 (1.01–1.12) | Reference | — | — | — | — |
| Paternal | 0.76 (0.71–0.82) | 0.6747 | 1.11 (0.95–1.29) | 0.5535 | 0.5171 | 0.5171 | 0.7423 | 0.0000 | |
| Maternal | 0.79 (0.72–0.88) | 0.3486 | 1.27 (1.12–1.43) | 0.0019 | 0.0073 | 0.1144 | 0.0656 | 0.7050 | |
| Both | — | — | 0.94 (0.76–1.15) | 0.5206 | — | — | — | — | |
| HDL cholesterol (mmol l−1) | No parental | 1.6±0.31 | Reference | 1.59±0.42 | Reference | — | — | — | — |
| Paternal | 1.64±0.32 | 0.1688 | 1.51±0.34 | 0.2617 | 0.4943 | 0.9986 | 0.1010 | 0.6282 | |
| Maternal | 1.54±0.3 | 0.1040 | 1.5±0.43 | 0.0413 | 0.0107 | 0.0107 | 0.5793 | 0.0000 | |
| Both | — | — | 1.72±0.4 | 0.1742 | — | — | — | — | |
| LDL cholesterol (mmol l−1) | No parental | 2.2±0.6 | Reference | 3.06±0.84 | Reference | — | — | — | — |
| Paternal | 2.22±0.67 | 0.5528 | 3.14±0.8 | 0.3705 | 0.3522 | 0.3522 | 0.5901 | 0.0000 | |
| Maternal | 2.19±0.62 | 0.9907 | 3.2±0.88 | 0.0857 | 0.2957 | 0.3828 | 0.1714 | 0.4653 | |
| Both | — | — | 3.28±0.87 | 0.1410 | — | — | — | — | |
| Cardiovascular risk factor | |||||||||
| Albumin-creatinine ratio | No parental | 0.61 (0.58–0.64) | Reference | 0.81 (0.73–0.89) | Reference | — | — | — | — |
| Paternal | 0.59 (0.47–0.73) | 0.9103 | 0.62 (0.49–0.78) | 0.1625 | 0.4879 | 0.5028 | 0.2226 | 0.3277 | |
| Maternal | 0.56 (0.43–0.73) | 0.5823 | 1.07 (0.79–1.45) | 0.0233 | 0.1983 | 0.5440 | 0.0505 | 0.7386 | |
| Both | — | — | 0.88 (0.66–1.17) | 0.6263 | — | — | — | — | |
Abbreviations: AUC, areas under the curve; HDL, high-density lipoprotein; HOMA-IR, homoeostasis model assessment of insulin resistance; HOMA-β, homoeostasis model assessment of β-cell function; LDL, low-density lipoprotein; OGTT, oral glucose tolerance test.
Data were expressed as n, %, mean±s.d. or geometric mean (95% confidence interval).
Padjusted refers to P-value obtained from linear regression adjusted by sex and age.
Pfixed and Prandom refer to P-value obtained from meta-analysis using fixed- and random-effect model, respectively.
PQ refers to P-value of Cochran's Q statistics in heterogeneity test.
I2 index is used to quantify the degree of heterogeneity of β-coefficient. I2 values around 25, 50 and 75% would mean low, medium and high heterogeneity.
Each group (paternal, maternal and both parental history of diabetes) was compared with the reference group (no parental history of diabetes) in linear regression analysis.
Indicates only a subset of samples (285 adolescents and 555 adults) who were included in the analysis.
Effect of PH of diabetes on cardiometabolic risk factors
Of the adolescents, a positive PH of diabetes was significantly associated with higher BW, BMI, WC in female, WHR, FAT, FPI, HOMA-IR but lower DI (0.0013<P<0.0393) (Table 2). Among adults, a positive parental diabetes was associated with higher BMI, FPG, FPI, HOMA-IR, 2-h glucose, glucose AUC during OGTT at 0-120 min (Figure 1 and Supplementary Table 1), SBP, DBP, TG, low-density lipoprotein cholesterol and lower body height, ISI and DI (2.1 × 10−4<P<0.0488) (Table 2). In the meta-analysis, we observed significant associations for body height, BW, BMI, WC in male and female, HC, WHR, FAT, FPI, HOMA-IR, 2-h insulin, glucose AUC at OGTT 0–120 min, ISI, DI and TG (2.6 × 10−5<P<0.0495) under the absence of heterogeneity between the two cohorts (P>0.05 in Q test) (Table 2). The differences in BMI, HOMA-IR, ISI and DI still remained significant after correction of multiple comparisons.
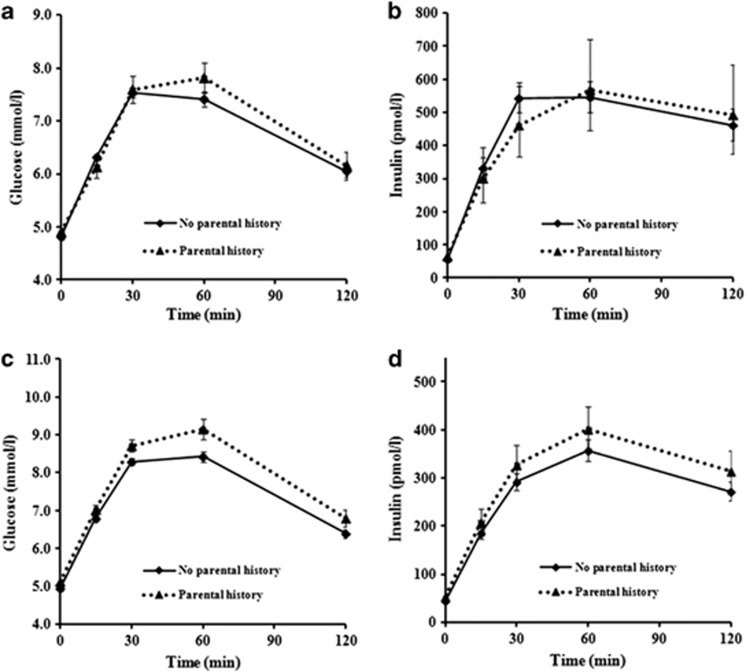
Figure 1.
Plasma glucose and insulin concentrations at 0, 15, 30, 60 and 120 min during oral glucose tolerance test (OGTT) in (a, b) adolescents (n=279) and (c, d) adults (n=555) stratified by parental history (yes/no). Data were expressed as mean±s.e. Associations between glucose/insulin concentrations and parental history for each time point during OGTT were shown in Supplementary Table 1.
Paternal and maternal transmission of cardiometabolic risk factors
Next, we examined the paternal and maternal transmission effect on cardiometabolic traits. Adolescents with a maternal history of diabetes had significantly higher BW, BMI, FAT, FPI, HOMA-IR and HOMA-β but lower DI (0.0016<P<0.0458) compared with those without PH of diabetes (Table 3). Likewise, adults with a maternal history of diabetes had higher BMI, WC in male, HC, FAT, FPG, FPI, HOMA-IR, 2-h glucose, 2-h insulin, glucose and insulin AUC during OGTT at 0–120 min (Figure 2 and Supplementary Table 2), SBP, DBP, TG and ACR, but lower body height, ISI, DI and HDL, (2.0 × 10−4<P<0.0482), compared with individuals with no parental diabetes (Table 3). In the meta-analysis, there were significant associations for positive maternal history of diabetes with higher BW, BMI, WC in male, HC, WHR, FAT, FPI, HOMA-IR, HOMA-β, 2-h glucose, 2-h insulin, glucose and insulin AUC during OGTT at 0–120 min, SBP and TG, as well as lower ISI, DI and HDL (2.0 × 10−5<P<0.0444) (Table 3). Conversely, a paternal history of diabetes had no effect on any of the cardiometabolic traits, except for the higher FPG levels in adults (P=0.0461), as well as higher BMI (P=0.0367), WC in female (P=0.0107) and FPG (P=0.0427) in the combined analysis (Table 3). Associations between maternal history of diabetes and BMI, WC in male, FPI, ISI and DI remained significant after considering multiple testing. When we compared the cardiometabolic traits between offspring with diabetic mother to diabetic father, significant associations were still observed for higher WC in male, FPI, HOMA-IR, HOMA-β, 2-h glucose, 2-h insulin, SBP, DBP, ACR, as well as lower ISI, DI and HDL in either individual or combined cohorts (Supplementary Table 3). Among adults, we also found that offspring with two diabetic parents have more impaired β-cell function indicated by the increased glucose AUC during OGTT at 0–120 min (Figure 2 and Supplementary Table 2) and the reduced insulinogenic index and DI compared with those without parental diabetes (Table 3).
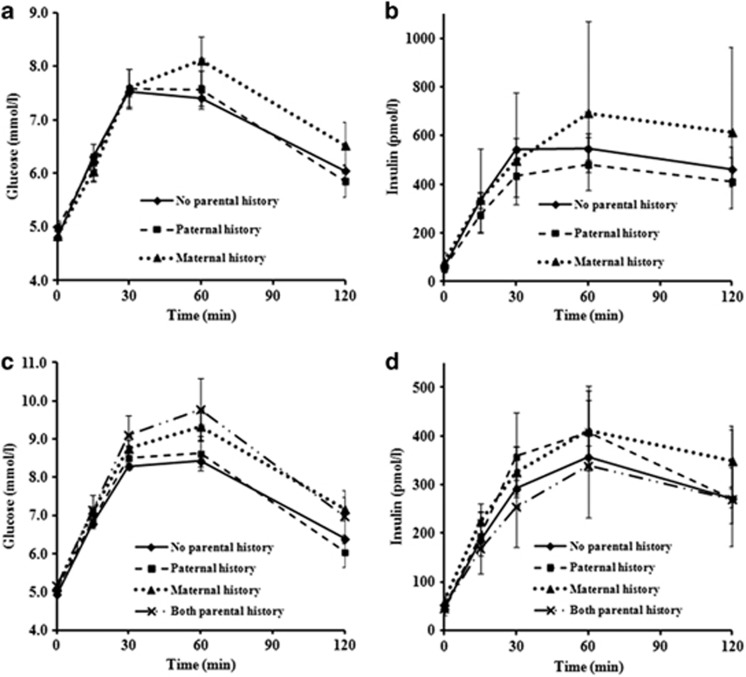
Figure 2.
Plasma glucose and insulin concentrations at 0, 15, 30, 60 and 120 min during oral glucose tolerance test (OGTT) in (a, b) adolescents (n=279) and (c, d) adults (n=555) according to parental history categories of diabetes. Data were expressed as mean±s.e. Associations between glucose/insulin concentrations and parental history categories for each time point during OGTT were shown in Supplementary Table 2.
Associations of obesity and central obesity with PH
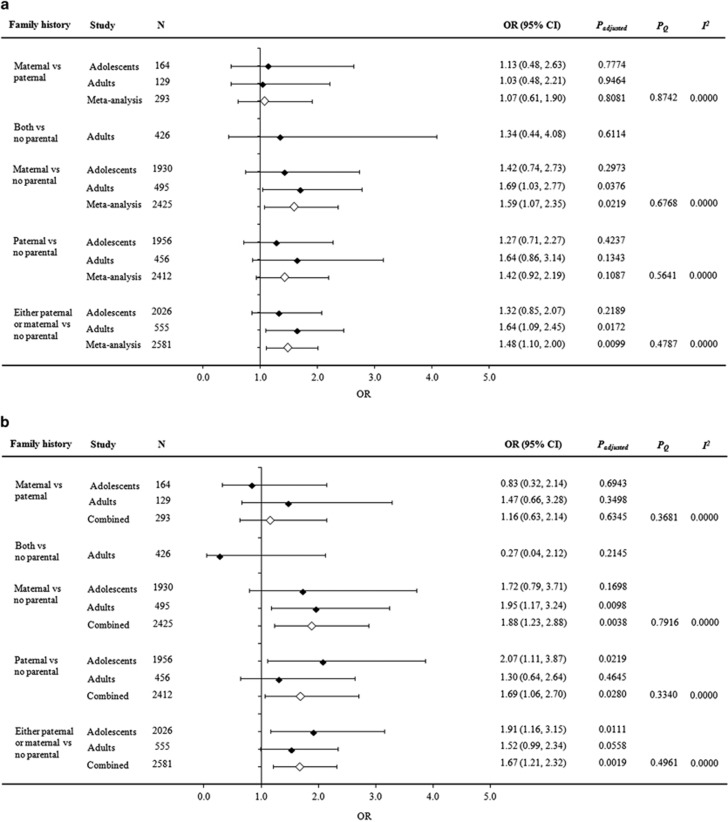
Lastly, we investigated the transmission pattern of obesity and central obesity according to the diabetes status of parents. Subjects with at least one diabetic parent are more obese (OR (95% CI)=1.48 (1.10–2.00) in overall) and centrally obese (OR (95% CI)=1.67 (1.21–2.32) in overall) than those without parental diabetes (Figures 3a and b). In addition, subjects with diabetic father had increased odds of central obesity of 1.69 (95% CI=1.06–2.70 in overall), whereas subjects with diabetic mother had ORs of 1.59 (95% CI=1.07–2.35 in overall) and 1.88 (95% CI=1.23–2.88 in overall) for obesity and for central obesity, respectively, compared with offspring without PH of diabetes (Figures 3a and b).
Figure 3.
Association of degrees of parental history with risk of (a) overweight or obesity and (b) central obesity adjusted for sex, age and/or study. Reference groups were individuals with no reported parental history of diabetes or with paternal history of diabetes in testing maternal versus paternal history of diabetes.
Discussion
T2D has been recognized as a familial disease, passed through from one generation to the next. Recently, several Caucasian studies have indicated that the gender of a diabetic parent may be an important factor in the transmission of the disease to the offspring.14, 15, 17, 24 In our previous study, we have found evidence for familial clustering of diabetes and maternal influence on increasing total cholesterol level in Chinese patients with T2D.6 Here we further investigated the effect of parental diabetes on the cardiometabolic traits, which are useful predictors for the development of T2D, in two Chinese cohorts consisting of 2026 adolescents and 555 adults.
In this study, we have confirmed that a positive PH of diabetes conferred increased risk of cardiometabolic abnormalities, including obesity, central obesity, hyperinsulinaemia, hyperglycaemia, insulin resistance, impaired first-phase insulin response, hypertension and dyslipidaemia, in Chinese. Our findings are in line with most of the earlier studies in other populations, which demonstrated familial aggregation of diabetes and related phenotypes.3, 4, 5, 6, 7, 8, 9, 41 For example, Abbasi et al.41 reported that PH of diabetes is associated with higher BMI, WC, HC and BP, whereas a Korean study found that offspring with parental diabetes have increased risk for abnormal glucose homoeostasis, compared with offspring without PH.5 On the other hand, a study conducted in Italy showed that T2D patients with parental diabetes were younger at diagnosis and more likely to be insulin-treated than those without familial diabetes.10 In the EPIC-InterAct study,3 a higher frequency of positive FH was observed among T2D patients with more risk alleles in a genetic score. Nevertheless, the genetic score alone explains only 2% of the FH-associated risk of T2D,3 suggesting that more genes and/or interactions between them have yet to be detected. Taken together, these suggest that positive PH of diabetes in fact reflects the interaction between genetic and shared environmental/lifestyle factors.
Of note, we found that the effect of parental diabetes is largely confined to the maternal side. Our results demonstrated a predominance of maternal influence on the cardiometabolic risk, which strongly support the clinical observations of a greater risk of T2D transmission from the mother than from the father.6, 10, 11, 14, 15, 16, 17, 18, 19, 20, 22, 26, 27, 41 Despite consistent findings from these studies, it is worth noting that the Framingham study and a few others have failed to detect such an effect.5, 7, 28, 42, 43 We noted in our study that when compared with either the group without parental diabetes or the group with paternal diabetes, offspring with maternal diabetes were more obese, more centrally obese and insulin resistant, had higher glucose levels and BP, and worse lipid profiles in the present study. Recently, similar findings have been also reported by Tan et al.,8 Groop et al.,18 Ekoe et al.,44 Kasperska-Czyzyk et al.,45 Bjornholt et al.16 and Sasaki et al.46 In addition, we found that positive maternal history of diabetes was associated with impaired first-phase insulin secretion (at 0–30 min during OGTT). Interestingly, our finding is in agreement with the observation reported by Praveen et al.,47 Otabe et al.48 and Kasperska-Czyzyk et al.45 that maternal diabetes was associated with a trend towards lower DI (0–120 min) and β-cell dysfunction.
Several possible mechanisms have been proposed to explain the greater effect of maternal diabetes than paternal diabetes. Recent data reported by Harder et al. and Omar et al.49, 50 observed a higher prevalence of T2D on the maternal-grandmaternal line than on the paternal-grandpaternal line among the T2D patients. Several studies also showed that a younger onset of maternal diabetes (that is, diabetes present in women of child-bearing age) was associated with an increased risk of impaired glucose tolerance or T2D in the offspring.3, 7, 51 Furthermore, the classical study in Pima Indians by Pettitt et al. had noted the deleterious effect of gestational diabetes on the offspring, including obesity and abnormal glucose tolerance, which in turn may contribute to pass on the risk for developing the same problems through subsequent generations. Taken together, these findings point towards a genetic background of T2D contributed by mutations or deletions of maternally inherited mitochondrial DNA. Other potential mechanisms include epigenetic changes, the role of imprinted genes whose expression is determined by the parent that contributed them, as well as postnatal lifestyle, which may be preferentially influenced by the mother. Interestingly, there is evidence also suggesting the importance of the intrauterine environment (that is, maternal nutrition) and maternal weight gain during pregnancy for the development of T2D in the offspring.24 Although the maternal diabetes status defined in the present study was not necessarily diagnosed before or during pregnancy, a mother who is diagnosed with diabetes after pregnancy is more likely to be prediabetic or insulin resistant at the time of her pregnancy and perhaps present an abnormal intrauterine environment to their offspring.
In this study, the maternal history of diabetes was consistently associated with obesity, insulin resistance and loss of first-phase insulin secretion in both adolescents and adults. We further noted adverse effects of maternal diabetes on BP, lipid profiles and ACR in adults, although we failed to observe the same in adolescents. This may be due to the stronger influence of confounding factors, such as age or lifestyle, compared with that of the intrauterine environment or genetic factors. In addition, due to the younger age of parents of the adolescents, the prevalence of maternal diabetes in adolescents is much lower than that in adult offspring (3.41% versus 15.14%). This may also explain the absence of associations in adolescents.
The strengths of this study include the inclusion of two representative samples in Chinese adolescents and adults, as well as the detailed clinical assessment of the cardiometabolic risk factors. However, some limitations of this study need to be considered. First, the PH of diabetes collected from questionnaires is self-reported and this collection method did not allow for confirming the diabetes status of parents. Potential censoring and report biases suggested by Cox52 could contribute to the excess maternal transmission observed in the present study. Therefore, we test for potential biases by comparing the cardiometabolic risk factors among responders and non-responders in adolescents (we did not test for the biases in adults because of the high response rate). We found that the cardiometabolic traits of the non-responders did not differ from those of responders, except for BMI and WHR (Supplementary Table 4). In addition, we observed similar proportion of unknown paternal status and unknown maternal status (12.6% versus 12.3%) in adolescents. Compared with adults, the difference in the proportion of affected fathers and mothers was smaller in adolescents (affected father versus affected mother 4.69% versus 3.41% in adolescents and 8.11% versus 15.14% in adults), those for whom both parents were most likely to be living. However, we observed a consistent effect of maternal diabetes on cardiometabolic risk factors in both cohorts. On the whole, these results indicate that our data is a representative sample of the Hong Kong Chinese population. Moreover, our study could be further improved by obtaining parental BMI, diagnosed age of diabetes, history of gestational diabetes and information of sharing familial environment, which may help to dissect the underlying mechanism of the association between maternal diabetes and T2D.
In conclusion, we showed that a positive PH of diabetes confers increased risk of cardiometabolic abnormalities in Chinese adolescents and adults, concordant with Caucasian studies. This effect is more pronounced in offspring with maternal history of diabetes, who are more obese, insulin resistant but also had impaired first-phase insulin secretion. Our studies highlight the need for public health schemes including targeted screening, lifestyle modifications and early intervention in offspring with parental diabetes, which may help to circumvent the vicious cycle of cardiometabolic defects through generations.
Acknowledgments
We are grateful to all study participants. We thank the Chinese University of Hong Kong Information Technology Services Centre for providing computing resources. Special thanks are extended to all nursing and medical staff at the PWH Diabetes and Endocrine Centre for their dedication and professionalism. This study was supported by the Hong Kong Foundation for Research and Development in Diabetes established under the auspices of the Chinese University of Hong Kong, the Liao Wun Yuk Diabetes Research Memorial Fund, the Hong Kong Governments Research Grant Committee Central Allocation Scheme (CUHK 1/04C), Research Grants Council Earmarked Research Grant (CUHK4055/01M, CUHK4727/07M), General Research Fund (CU471713), the Innovation and Technology Fund (ITS/088/08 and ITS/487/09FP), the Focused Investment Fund of the Chinese University, the Research Fund of the Department of Medicine and Therapeutics, and the Diabetes and Endocrine Research Fund of the Chinese University of Hong Kong.
The authors declare no conflict of interest.
Footnotes
Supplementary Information accompanies this paper on the Nutrition & Diabetes website (http://www.nature.com/nutd)
Supplementary Material
References
- Wong KC, Wang Z. Prevalence of type 2 diabetes mellitus of Chinese populations in Mainland China, Hong Kong, and Taiwan. Diabetes Res Clin Pract. 2006;73:126–134. doi: 10.1016/j.diabres.2006.01.007. [DOI] [PubMed] [Google Scholar]
- Stumvoll M, Goldstein BJ, van Haeften TW. Type 2 diabetes: principles of pathogenesis and therapy. Lancet. 2005;365:1333–1346. doi: 10.1016/S0140-6736(05)61032-X. [DOI] [PubMed] [Google Scholar]
- InterAct Consortium The link between family history and risk of type 2 diabetes is not explained by anthropometric, lifestyle or genetic risk factors: the EPIC-InterAct study. Diabetologia. 2013;56:60–69. doi: 10.1007/s00125-012-2715-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hagura R, Matsuda A, Kuzuya T, Yoshinaga H, Kosaka K. Family history of diabetic patients in Japan. Diabetes Res Clin Pract. 1994;24 (Suppl:S69–S73. doi: 10.1016/0168-8227(94)90230-5. [DOI] [PubMed] [Google Scholar]
- Kim DJ, Cho NH, Noh JH, Lee MS, Lee MK, Kim KW. Lack of excess maternal transmission of type 2 diabetes in a Korean population. Diabetes Res Clin Pract. 2004;65:117–124. doi: 10.1016/j.diabres.2003.11.020. [DOI] [PubMed] [Google Scholar]
- Lee SC, Pu YB, Chow CC, Yeung VT, Ko GT, So WY, et al. Diabetes in Hong Kong Chinese: evidence for familial clustering and parental effects. Diabetes Care. 2000;23:1365–1368. doi: 10.2337/diacare.23.9.1365. [DOI] [PubMed] [Google Scholar]
- Meigs JB, Cupples LA, Wilson PW. Parental transmission of type 2 diabetes: the Framingham Offspring Study. Diabetes. 2000;49:2201–2207. doi: 10.2337/diabetes.49.12.2201. [DOI] [PubMed] [Google Scholar]
- Tan JT, Tan LS, Chia KS, Chew SK, Tai ES. A family history of type 2 diabetes is associated with glucose intolerance and obesity-related traits with evidence of excess maternal transmission for obesity-related traits in a South East Asian population. Diabetes Res Clin Pract. 2008;82:268–275. doi: 10.1016/j.diabres.2008.08.005. [DOI] [PubMed] [Google Scholar]
- Vaag A, Lehtovirta M, Thye-Ronn P, Groop L. Metabolic impact of a family history of Type 2 diabetes. Results from a European multicentre study (EGIR) Diabet Med. 2001;18:533–540. doi: 10.1046/j.1464-5491.2001.00496.x. [DOI] [PubMed] [Google Scholar]
- Bo S, Cavallo-Perin P, Gentile L, Repetti E, Pagano G. Influence of a familial history of diabetes on the clinical characteristics of patients with Type 2 diabetes mellitus. Diabet Med. 2000;17:538–542. doi: 10.1046/j.1464-5491.2000.00330.x. [DOI] [PubMed] [Google Scholar]
- Papazafiropoulou A, Sotiropoulos A, Skliros E, Kardara M, Kokolaki A, Apostolou O, et al. Familial history of diabetes and clinical characteristics in Greek subjects with type 2 diabetes. BMC Endocr Disord. 2009;9:12. doi: 10.1186/1472-6823-9-12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Martin AO, Simpson JL, Ober C, Freinkel N. Frequency of diabetes mellitus in mothers of probands with gestational diabetes: possible maternal influence on the predisposition to gestational diabetes. Am J Obstet Gynecol. 1985;151:471–475. doi: 10.1016/0002-9378(85)90272-8. [DOI] [PubMed] [Google Scholar]
- Aerts L, Holemans K, Van Assche FA. Maternal diabetes during pregnancy: consequences for the offspring. Diabetes Metab Rev. 1990;6:147–167. doi: 10.1002/dmr.5610060303. [DOI] [PubMed] [Google Scholar]
- Alcolado JC, Alcolado R. Importance of maternal history of non-insulin dependent diabetic patients. BMJ. 1991;302:1178–1180. doi: 10.1136/bmj.302.6786.1178. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Benrahma H, Arfa I, Charif M, Bounaceur S, Eloualid A, Boulouiz R, et al. Maternal effect and familial aggregation in a type 2 diabetic Moroccan population. J Community Health. 2011;36:943–948. doi: 10.1007/s10900-011-9393-3. [DOI] [PubMed] [Google Scholar]
- Bjornholt JV, Erikssen G, Liestol K, Jervell J, Thaulow E, Erikssen J. Type 2 diabetes and maternal family history: an impact beyond slow glucose removal rate and fasting hyperglycemia in low-risk individuals? Results from 22.5 years of follow-up of healthy nondiabetic men. Diabetes Care. 2000;23:1255–1259. doi: 10.2337/diacare.23.9.1255. [DOI] [PubMed] [Google Scholar]
- De Silva SN, Weerasuriya N, De Alwis NM, De Silva MW, Fernando DJ. Excess maternal transmission and familial aggregation of Type 2 diabetes in Sri Lanka. Diabetes Res Clin Pract. 2002;58:173–177. doi: 10.1016/s0168-8227(02)00152-3. [DOI] [PubMed] [Google Scholar]
- Groop L, Forsblom C, Lehtovirta M, Tuomi T, Karanko S, Nissen M, et al. Metabolic consequences of a family history of NIDDM (the Botnia study): evidence for sex-specific parental effects. Diabetes. 1996;45:1585–1593. doi: 10.2337/diab.45.11.1585. [DOI] [PubMed] [Google Scholar]
- Karter AJ, Rowell SE, Ackerson LM, Mitchell BD, Ferrara A, Selby JV, et al. Excess maternal transmission of type 2 diabetes. The Northern California Kaiser Permanente Diabetes Registry. Diabetes Care. 1999;22:938–943. doi: 10.2337/diacare.22.6.938. [DOI] [PubMed] [Google Scholar]
- Klein BE, Klein R, Moss SE, Cruickshanks KJ. Parental history of diabetes in a population-based study. Diabetes Care. 1996;19:827–830. doi: 10.2337/diacare.19.8.827. [DOI] [PubMed] [Google Scholar]
- Lin RS, Lee WC, Lee YT, Chou P, Fu CC. Maternal role in type 2 diabetes mellitus: indirect evidence for a mitochondrial inheritance. Int J Epidemiol. 1994;23:886–890. doi: 10.1093/ije/23.5.886. [DOI] [PubMed] [Google Scholar]
- Mitchell BD, Valdez R, Hazuda HP, Haffner SM, Monterrosa A, Stern MP. Differences in the prevalence of diabetes and impaired glucose tolerance according to maternal or paternal history of diabetes. Diabetes Care. 1993;16:1262–1267. doi: 10.2337/diacare.16.9.1262. [DOI] [PubMed] [Google Scholar]
- Otabe S, Nakayama H, Fukutani T, Yuan X, Wada N, Hashinaga T, et al. Excessive maternal transmission of diabetes in Japanese families with young-onset type 2 diabetes and insulin secretion defect according to clinical features. Acta Diabetol. 2009;47 (Suppl 1:133–138. doi: 10.1007/s00592-009-0152-1. [DOI] [PubMed] [Google Scholar]
- Pettitt DJ, Bennett PH, Saad MF, Charles MA, Nelson RG, Knowler WC. Abnormal glucose tolerance during pregnancy in Pima Indian women. Long-term effects on offspring. Diabetes. 1991;40 (Suppl 2:126–130. doi: 10.2337/diab.40.2.s126. [DOI] [PubMed] [Google Scholar]
- Riley MD, Blizzard CL, McCarty DJ, Senator GB, Dwyer T, Zimmet P. Parental history of diabetes in an insulin-treated diabetes registry. Diabet Med. 1997;14:35–41. doi: 10.1002/(SICI)1096-9136(199701)14:1<35::AID-DIA296>3.0.CO;2-I. [DOI] [PubMed] [Google Scholar]
- Thomas F, Balkau B, Vauzelle-Kervroedan F, Papoz L. Maternal effect and familial aggregation in NIDDM. The CODIAB Study. CODIAB-INSERM-ZENECA Study Group. Diabetes. 1994;43:63–67. doi: 10.2337/diab.43.1.63. [DOI] [PubMed] [Google Scholar]
- Young CA, Kumar S, Young MJ, Boulton AJ. Excess maternal history of diabetes in Caucasian and Afro-origin non-insulin-dependent diabetic patients suggests dominant maternal factors in disease transmission. Diabetes Res Clin Pract. 1995;28:47–49. doi: 10.1016/0168-8227(94)01058-8. [DOI] [PubMed] [Google Scholar]
- Mitchell BD, Kammerer CM, Reinhart LJ, Stern MP, MacCluer JW. Is there an excess in maternal transmission of NIDDM. Diabetologia. 1995;38:314–317. doi: 10.1007/BF00400636. [DOI] [PubMed] [Google Scholar]
- Thorand B, Liese AD, Metzger MH, Reitmeir P, Schneider A, Lowel H. Can inaccuracy of reported parental history of diabetes explain the maternal transmission hypothesis for diabetes. Int J Epidemiol. 2001;30:1084–1089. doi: 10.1093/ije/30.5.1084. [DOI] [PubMed] [Google Scholar]
- Viswanathan M, McCarthy MI, Snehalatha C, Hitman GA, Ramachandran A. Familial aggregation of type 2 (non-insulin-dependent) diabetes mellitus in south India; absence of excess maternal transmission. Diabet Med. 1996;13:232–237. doi: 10.1002/(SICI)1096-9136(199603)13:3<232::AID-DIA27>3.0.CO;2-7. [DOI] [PubMed] [Google Scholar]
- Ng MC, Park KS, Oh B, Tam CH, Cho YM, Shin HD, et al. Implication of genetic variants near TCF7L2, SLC30A8, HHEX, CDKAL1, CDKN2A/B, IGF2BP2, and FTO in type 2 diabetes and obesity in 6,719 Asians. Diabetes. 2008;57:2226–2233. doi: 10.2337/db07-1583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ozaki R, Qiao Q, Wong GW, Chan MH, So WY, Tong PC, et al. Overweight, family history of diabetes and attending schools of lower academic grading are independent predictors for metabolic syndrome in Hong Kong Chinese adolescents. Arch Dis Child. 2007;92:224–228. doi: 10.1136/adc.2006.100453. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ko GT, Chan JC, Chan AW, Wong PT, Hui SS, Tong SD, et al. Association between sleeping hours, working hours and obesity in Hong Kong Chinese: the 'better health for better Hong Kong' health promotion campaign. Int J Obes (Lond) 2007;31:254–260. doi: 10.1038/sj.ijo.0803389. [DOI] [PubMed] [Google Scholar]
- Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28:412–419. doi: 10.1007/BF00280883. [DOI] [PubMed] [Google Scholar]
- Phillips DI, Clark PM, Hales CN, Osmond C. Understanding oral glucose tolerance: comparison of glucose or insulin measurements during the oral glucose tolerance test with specific measurements of insulin resistance and insulin secretion. Diabet Med. 1994;11:286–292. doi: 10.1111/j.1464-5491.1994.tb00273.x. [DOI] [PubMed] [Google Scholar]
- Matsuda M, DeFronzo RA. Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes Care. 1999;22:1462–1470. doi: 10.2337/diacare.22.9.1462. [DOI] [PubMed] [Google Scholar]
- Gastaldelli A, Ferrannini E, Miyazaki Y, Matsuda M, DeFronzo RA. Beta-cell dysfunction and glucose intolerance: results from the San Antonio metabolism (SAM) study. Diabetologia. 2004;47:31–39. doi: 10.1007/s00125-003-1263-9. [DOI] [PubMed] [Google Scholar]
- Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320:1240–1243. doi: 10.1136/bmj.320.7244.1240. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zimmet P, Alberti KG, Kaufman F, Tajima N, Silink M, Arslanian S, et al. The metabolic syndrome in children and adolescents - an IDF consensus report. Pediatr Diabetes. 2007;8:299–306. doi: 10.1111/j.1399-5448.2007.00271.x. [DOI] [PubMed] [Google Scholar]
- Hochberg Y. A sharper Bonferroni procedure for multiple tests of significance. Biometrika. 1988;75:800–802. [Google Scholar]
- Abbasi A, Corpeleijn E, van der Schouw YT, Stolk RP, Spijkerman AM, van der AD, et al. Maternal and paternal transmission of type 2 diabetes: influence of diet, lifestyle and adiposity. J Intern Med. 2011;270:388–396. doi: 10.1111/j.1365-2796.2011.02347.x. [DOI] [PubMed] [Google Scholar]
- Knowler WC, Pettitt DJ, Savage PJ, Bennett PH. Diabetes incidence in Pima indians: contributions of obesity and parental diabetes. Am J Epidemiol. 1981;113:144–156. doi: 10.1093/oxfordjournals.aje.a113079. [DOI] [PubMed] [Google Scholar]
- McCarthy M, Cassell P, Tran T, Mathias L, t Hart LM, Maassen JA, et al. Evaluation of the importance of maternal history of diabetes and of mitochondrial variation in the development of NIDDM. Diabet Med. 1996;13:420–428. doi: 10.1002/(SICI)1096-9136(199605)13:5<420::AID-DIA97>3.0.CO;2-W. [DOI] [PubMed] [Google Scholar]
- Ekoe JM, Thomas F, Balkau B, Eschwege E, Delisle H. Effect of maternal diabetes on the pattern of selected insulin resistance syndrome parameters in normal glucose tolerant subjects of two Algonquin Indian communities in Quebec. Diabetes Care. 1996;19:822–826. doi: 10.2337/diacare.19.8.822. [DOI] [PubMed] [Google Scholar]
- Kasperska-Czyzyk T, Jedynasty K, Bowsher RR, Holloway DL, Stradowska I, Stepien K, et al. Difference in the influence of maternal and paternal NIDDM on pancreatic beta-cell activity and blood lipids in normoglycaemic non-diabetic adult offspring. Diabetologia. 1996;39:831–837. doi: 10.1007/s001250050517. [DOI] [PubMed] [Google Scholar]
- Sasaki K, Yoshida A, Ohta H, Aizawa Y, Kojima A, Chiba H, et al. Maternal and paternal family history of type 2 diabetes differently influence lipid parameters in young nondiabetic Japanese women. Environ Health Prev Med. 2012;18:104–109. doi: 10.1007/s12199-012-0296-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Praveen EP, Sahoo J, Khurana ML, Kulshreshtha B, Khadgawat R, Gupta N, et al. Insulin sensitivity and beta-cell function in normoglycemic offspring of individuals with type 2 diabetes mellitus: Impact of line of inheritance. Indian J Endocrinol Metab. 2012;16:105–111. doi: 10.4103/2230-8210.91204. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Otabe S, Nakayama H, Fukutani T, Yuan X, Wada N, Hashinaga T, et al. Excessive maternal transmission of diabetes in Japanese families with young-onset type 2 diabetes and insulin secretion defect according to clinical features. Acta Diabetol. 2010;47 (Suppl 1:133–138. doi: 10.1007/s00592-009-0152-1. [DOI] [PubMed] [Google Scholar]
- Harder T, Plagemann A. A role for gestational diabetes in the excess maternal transmission of type 2 diabetes. Diabetes Care. 2000;23:431–432. doi: 10.2337/diacare.23.3.431. [DOI] [PubMed] [Google Scholar]
- Omar MA, Motala AA, Seedat MA, Pirie F. The significance of a positive family history in South African Indians with non-insulin-dependent diabetes (NIDDM) Diabetes Res Clin Pract. 1996;34 (Suppl:S13–S16. doi: 10.1016/s0168-8227(96)90003-0. [DOI] [PubMed] [Google Scholar]
- Franks PW, Looker HC, Kobes S, Touger L, Tataranni PA, Hanson RL, et al. Gestational glucose tolerance and risk of type 2 diabetes in young Pima Indian offspring. Diabetes. 2006;55:460–465. doi: 10.2337/diabetes.55.02.06.db05-0823. [DOI] [PubMed] [Google Scholar]
- Cox NJ. Maternal component in NIDDM transmission. How large an effect. Diabetes. 1994;43:166–168. doi: 10.2337/diab.43.1.166. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.