Abstract
Saw palmetto extract (SPE), an extract from the ripe berries of the American dwarf palm, has been widely used as a therapeutic remedy for urinary dysfunction due to benign prostatic hyperplasia (BPH) in Europe. Numerous mechanisms of action have been proposed for SPE, including the inhibition of 5α-reductase. Today, α1-adrenoceptor antagonists and muscarinic cholinoceptor antagonists are commonly used in the treatment of men with voiding symptoms secondary to BPH. The improvement of voiding symptoms in patients taking SPE may arise from its binding to pharmacologically relevant receptors in the lower urinary tract, such as α1-adrenoceptors, muscarinic cholinoceptors, 1,4-dihyropyridine receptors and vanilloid receptors. Furthermore, oral administration of SPE has been shown to attenuate the up-regulation of α1-adrenoceptors in the rat prostate induced by testosterone. Thus, SPE at clinically relevant doses may exert a direct effect on the pharmacological receptors in the lower urinary tract, thereby improving urinary dysfunction in patients with BPH and an overactive bladder. SPE does not have interactions with co-administered drugs or serious adverse events in blood biochemical parameters, suggestive of its relative safety, even with long-term intake. Clinical trials (placebo-controlled and active-controlled trials) of SPE conducted in men with BPH were also reviewed. This review should contribute to the understanding of the pharmacological effects of SPE in the treatment of patients with BPH and associated lower urinary tract symptoms (LUTS).
Keywords: saw palmetto extract, pharmacological effects, lower urinary tract receptors
Introduction
Benign prostatic hyperplasia (BPH) and associated lower urinary tract symptoms (LUTS) are very common disorders in aging men. The prevalence of histopathologic BPH is age dependent, with initial development usually occurring after 40 years of age1. By 60 years of age, its prevalence is greater than 50% and by age 85, the prevalence is as high as 90%. Similar to histological evidence, the prevalence of bothersome symptoms also increases with age. The two main forms of internationally accepted medical treatment for BPH are inhibitors of 5α-reductase, such as finasteride and α1-adrenoceptor antagonists, with the latter being more effective2. In addition to these medications, the ripe berries of the American dwarf palm (Serenoa repens, saw palmetto) have been traditionally used to treat genitourinary problems; to enhance sperm production, breast size, or libido; and as a mild diuretic3. In many European countries, phytotherapeutic agents, including saw palmetto, are very popular. Phytotherapeutic agents represent nearly half of the medications dispensed for the treatment of BPH in Italy, compared with 5% for α-blockers and 5% for 5α-reductase inhibitors4. In Germany and Austria, phytotherapy is the first-line treatment for mild to moderate lower urinary tract symptoms and represents more than 90% of all drugs prescribed for the treatment of BPH4, 5, 6. Saw palmetto is a dwarf palm tree of the family Arecaceae and is indigenous to the southeastern parts of the United States. Saw palmetto berries have traditionally been used by American Indians to cure genitourinary disturbances, relieve mucous membrane irritations, increase testicular function, or increase breast size5, 6. In the United States, the use of phytotherapy for LUTS has grown rapidly, and approximately 2.5 million men used saw palmetto extract (SPE), although a guideline panel did not recommend phytotherapy as a treatment for BPH7, 8. In Japan, SPE is not a prescribed medication; however, it has been receiving increasing attention recently among patients with BPH.
The mechanisms of pharmacological action of SPE were not fully understood, although numerous proposals have been made, including inhibition of 5α-reductase, anti-androgenic effects, anti-proliferative effects, anti-inflammatory effects and anti-edema effects6. However, most of these pharmacological effects were observed at relatively high concentrations or large doses of SPE9, 10, and it is uncertain whether the reported modes of action of SPE are therapeutically relevant11, 12. As described above, α1-adrenoceptor antagonists are commonly used in the treatment of men with voiding symptoms (urinary obstruction, pollakiuria and urinary incontinence) secondary to BPH. Goepel et al13 have shown that SPE might have α1-adrenoceptor inhibitory properties. SPE significantly affects pharmacological receptors, such as the α1-adrenoceptor and the muscarinic receptor in the lower urinary tract, to relieve the irritative and obstructive symptoms of dysuria due to BPH and LUTS14. In addition to traditionally used medications, like α1-adrenoceptor antagonists, antimuscarinics, 5α-reductase inhibitors, and phytotherapy, several new therapeutic agents, such as selective β3-adrenoceptor agonists, are potentially useful for treating LUTS suggestive of BPH, particularly for storage symptoms secondary to outflow obstruction15. Thus, the effects of SPE on these receptors in the lower urinary tract might be pharmacologically relevant.
To date, more than 11 placebo-controlled trials and 4 active-controlled trials with SPE in men with BPH have been conducted. Most of these were reported in the 1980s. Patient numbers were usually limited and the evaluation periods were relatively short, so it would be difficult to evaluate the effect of SPE and ascertain the efficacy of SPE in BPH patients. However, some placebo-controlled studies and comparisons to α1-blockers have recently been conducted with relatively long-term treatments and sufficient numbers of patients8, 16, 17.
Herbal products, including SPE, are often used with other prescription medications, and most patients with BPH are aged men. Elderly individuals frequently take dietary supplements with prescription drugs, and such a tendency will continue to increase in the near future. In such cases, a major concern is adverse events caused by a large excess intake or interactions between dietary supplements and drugs. Thus, the safety, as well as the efficacy, of these natural products and of their active ingredients remains to be analyzed at a scientific level. This review introduces newly revealed pharmacological actions of SPE, as well as some well-known mechanisms of action of SPE, and also summarizes clinical trials of SPE in comparison with currently used medicines.
Chemical composition
SABALSELECTTM, manufactured by Indena SpA. (Milano, Italy), was used for the animal experiments14, 18, 19. Indena SpA. explains the extraction of saw palmetto in the brochure as follows: the fruits of S repens are extracted with supercritical CO2. This extractive procedure, conducted at 45 °C/220 bar, directly produces a pharmacological product (SABALSELECTTM), which can be used without further purification. Table 1 shows the chemical composition of SABALSELECTTM. It consists of fatty acids, alcohols and sterols (Brochure of SabalselectTM: Indena SpA). Habib and Wyllie20 reported that the contents of different brands of SPE were markedly different; for example, free fatty acids ranged from 40.7% to 80.7% (mean %), methyl and ethyl esters from 1.5% to 16.7% (mean %), and glycerides from 6.8% to 52.2% (mean %). In the United States, herbal products are regulated under the Dietary Supplement Health and Education Act (DSHEA); however, approval for launching products onto the market is not required except in cases of a new dietary ingredient. Therefore, herbal products that existed before October 15, 1994, can remain with different ingredients21. Levin and Das22 issued a warning that each preparation must be considered individually because of differences in extraction techniques, preparation of products, composition, and biological activities.
Table 1. Chemical composition of SPE (Brochure of SabalselectTM: Indena SpA. http://www.indena.it/pdf/sabalselect.pdf).
| Fatty acids | Content (%) | Fatty alcohols and sterols | Content (%) |
|---|---|---|---|
| Total fatty acids | 93.5 | Fatty alcohols | 0.20 |
| Hexacosanol | 0.017 | ||
| Saturated | 59.8 | Octacosanol | 0.146 |
| Caproic acid | 1.5 | Tetracosanol | 0.004 |
| Caprylic acid | 2.3 | Triacontanol | 0.003 |
| Capric acid | 2.5 | ||
| Lauric acid | 30.2 | Sterols | 0.32 |
| Myristic acid | 12.0 | Campesterol | 0.07 |
| Palmitic acid | 9.5 | Stigmasterol | 0.03 |
| Stearic acid | 1.8 | β-Sitosterol | 0.22 |
| Unsaturated | 33.7 | ||
| Oleic acid | 28.5 | ||
| Linoleic acid | 4.6 | ||
| Linolenic acid | 0.6 |
Pharmacological properties
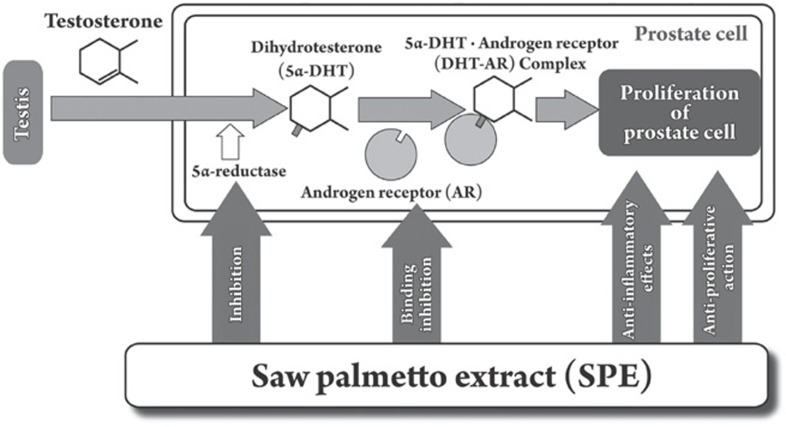
BPH causes dysuria and residual urine via a mechanical stoppage due to hypertrophy of prostatic tissue and via a functional stoppage caused by α1-adrenoceptor hypertonia of prostatic smooth muscle. Previous studies have demonstrated that SPE had a number of pharmacological effects: 1) an anti-androgenic effect — inhibition of 5α-reductase I and II and inhibition of binding of dihydrotestosterone (DHT) to the cytosolic androgen receptors, 2) an anti-inflammatory effect, 3) an anti-proliferative effect, (Figure 1), and 4) significant binding of pharmacological receptors existing in the lower urinary tract.
Figure 1.
Mechanisms of pharmacological action of saw palmetto extract (SPE). They include antiandrogenic effects, such as inhibition of 5α-reductase I and II and inhibition of binding of dihydrotestosterone (DHT) to the cytosolic androgen receptors, anti-proliferative effects and anti-inflammatory effects.
Anti-androgenic effects
The development and growth of the prostate gland depend on androgen stimulation23, 24. DHT is one of several factors regulating this development and growth24, 25 and is converted from testosterone by 5α-reductase. This enzyme has two isoforms (5α-reductase 1 and 2)25. The respective roles of these 5α-reductases in BPH development have not yet been elucidated26. SPE inhibited both isozymes in a noncompetitive manner27, 28, 29, whereas finasteride inhibited only 5α-reductase 2 in a competitive manner25. Among the many components of SPE, lauric acid and linoleic acid showed inhibition of both isozymes, oleic acid was active only against 5α-reductase 1 and myristic acid was active only against 5α-reductase 2. However, palmitic acid, stearic acid, esterified fatty acids, sterols, and alcohols were inactive against both30.
Di Silverio et al26 reported a significant decrease in DHT and increase in testosterone in the periurethral region of prostate tissue from BPH patients receiving Permixon® (320 mg/day) for 3 months and thus suggested that SPE could inhibit 5α-reductase in the human prostate in vivo. Sultan et al9 investigated the interaction of SPE with the intercellular androgen-receptor complex. SPE inhibited [3H]dihydrotestosterone from binding to its receptor. The affinity of SPE was higher for cytosol receptors than for nuclear receptors. Competitive interference with the binding of [3H]methyltrienolone to cytosolic androgen receptors was also shown in rat prostate cells31.
Anti-inflammatory effects
Inflammation was frequently observed in hormonally induced hypertrophied prostates of dogs32 and in a study of human BPH33. Mahapokai et al32 concluded that the development of hyperplasia preceded inflammatory infiltration. An anti-inflammatory effect was indicated as one of the mechanisms of action of SPE. In fact, it is plausible that SPE affects several inflammatory mediators. SPE showed anti-inflammatory and anti-edematous effects in vivo34. The production of 5-lipoxygenase metabolites was inhibited by SPE (Permixon®) at a concentration of 5 μg/mL35. Breu et al34 demonstrated that acid lipophilic compounds of SPE inhibited the biosynthesis of cyclooxygenase and 5-lipoxygenase metabolites with the same intensity as SPE.
Vela Navarrete et al36 conducted a multicenter open pilot clinical study to make a comparison between a control group and an SPE (Permixon®) group in BPH patients. After 3 months of treatment with SPE, the patients showed an improvement in their International Prostate Symptom Score (IPSS). Also, significant decreases in the levels of interleukin-1β (IL-1β) and tumor necrosis factor (TNF)-α were observed after the SPE treatment. Thus, SPE was shown to exert an anti-inflammatory effect.
Anti-proliferative effects
Maintenance of a constant number of cells is one of the basic functions of homeostasis. In normal adult prostate, the delicate balance between apoptosis and proliferation is well regulated and these indices are low. In contrast, in a prostate with BPH this equilibrium may not be maintained37, 38, 39, 40. Kyprianou et al37 showed a statistically significant elevation in TGF-β, a negative growth factor able to induce apoptosis under physiological conditions, in the epithelial cells of BPH tissue compared with the normal prostate and a statistically significant increase in the intensity of immunoreactivity for bcl-2 and the number of positive epithelial cells in BPH specimens relative to normal prostate. Claus et al41 also indicated stromal growth in BPH due to cell proliferation in the absence of apoptosis. Vacherot et al40 revealed that proliferation exceeded apoptosis in the stroma and epithelium of human BPH tissues. Although the rate of apoptosis did not differ between normal prostate and BPH tissue, the proliferative index was significantly higher in BPH tissue than in normal prostate in both the stroma and the epithelium. Furthermore, comparisons of the proliferative indices and apoptotic indices between the BPH tissues after 3 months of SPE (Permixon®) administration and those without SPE administration showed that in both the stroma and the epithelium, the proliferative index showed a significant decrease in SPE-treated BPH tissue relative to untreated tissue and the apoptotic index showed a significant increase in the SPE-treated BPH tissue.
Vacher et al42 showed that SPE reduced the basal activity of K+channels and protein kinase C in Chinese hamster ovary cells and that pretreatment with SPE abolished the effects of prolactin. Furthermore, it was demonstrated that SPE (Permixon®) inhibited the effects of prolactin and androgens on prostate growth in the rat lateral prostate23. Thus, SPE might block prolactin-induced prostate growth by inhibiting several steps of prolactin receptor signal transduction.
Effects on pharmacological receptors in the lower urinary tract
In vitro effects
Goepel et al13 have shown that SPE displaced an α1-adrenoceptor radioligand to bind to human prostatic and cloned human α1-adrenoceptors in a noncompetitive manner and concomitantly suppressed the agonist-induced formation of [3H]-inositol phosphate. We evaluated the in vitro and in vivo binding of SPE to autonomic receptors in the lower urinary tract14, 18, 19. The in vitro experiment has shown that SPE inhibited the specific binding of [3H]prasozin (α1-adreceptor), [3H]N-methylscopolamine (NMS, muscarinic receptor) and (+)-[3H]PN 200-110 (1,4-dihydropyridine receptors), but not [3H]αβ-MeATP (purinergic receptor), in the prostate, bladder and other tissues of rats in a concentration-dependent manner. Our recent study has shown that SPE competitively inhibited specific binding of [3H]prasozin and [3H]NMS in human prostate and bladder (Yamada et al, unpublished data). Thus, it is suggested that SPE binds to α1-adrenergic, muscarinic and 1,4-dihydropyridine receptors, but not to purinergic receptors14, 18, 19. Based on IC50 values (Table 2), the binding activity of SPE for muscarinic receptors was shown to be 2-4 times greater than that for α1-adrenergic and 1,4-dihydropyridine receptors. The affinity of SPE for these receptors was comparable to the in vitro pharmacological potency of this extract [eg, inhibition of 5α-reductase (IC50: 71 μg/mL), anti-inflammatory effect (IC50 of cyclooxygenase and 5-lipoxygenase: 28.1 and 18.0 μg/mL, respectively), and anti-androgenic effect (IC50: 1004 μg/mL)]34, 43 reported previously. Furthermore, Scatchard analysis has revealed that SPE caused a significant decrease in the maximal number of binding sites (Bmax values) of [3H]prazosin, [3H]NMS and (+)-[3H]PN 200-110 in the prostate or bladder of rats (45%, 45% and 33%, respectively)18, 19. Therefore, it could be presumed that SPE binds non-competitively to α1-adrenergic, muscarinic and 1,4-dihydropyridine receptors in rat tissues. Such insurmountable antagonism by SPE was previously noted in human prostatic and cloned α1-adrenoceptors13.
Table 2. IC50 values for in vitro inhibition by SPE of specific binding of [3H]prazosin, [3H]NMS, and (+)-[3H]PN 200–110 in rat tissues.
| Radioligands | IC50 values (μg/mL) |
|---|---|
| (Mean±SEM, n=4–9) | |
| Specific [3H]prazosin binding | |
| Prostate | 169±24 |
| Spleen | 188±47 |
| Specific [3H]NMS binding | |
| Bladder | 40.0±4.1 |
| Submaxillary gland | 52.3±4.4 |
| Specific (+)-[3H]PN 200-110 binding | |
| Bladder | 97.3±17.1 |
Vanilloids exert their activity through the transient receptor potential vanilloid subtype 1 (TRPV1), a nonselective cation channel. TRPV1 has been shown to be located in urinary bladder epithelial cells44. The urothelial TRPV1 may play a role in concert with TRPV1 nerve fibers45. Thus, TRPV1 may play a significant role in the pathophysiology of bladder disease. Our recent study has also shown that SPE significantly inhibited the capsaicin-induced Ca2+ influx in HEK293VR11 cells expressing TRPV1 receptors46. Furthermore, SPE inhibited specific binding of [3H]resineferatoxin in HEK293VR11 cells in a concentration-dependent manner. Thus, it is assumed that SPE inhibits the activation of TRPV1 in the bladder.
In vivo effects
Suzuki et al18, 19 examined the effects of oral administration of SPE on autonomic receptors in rats. Repeated oral administration of SPE (SABALSELECT™) for 4 weeks produced a significant decrease of muscarinic receptor (specific [3H]NMS binding) sites in the rat bladder and submaxillary gland18, 19. Notably, such a reduction in the number of [3H]NMS binding sites was observed at relatively low doses (0.6, 6 mg·kg−1·d−1) of SPE in the bladder and only at a high dose (60 mg·kg−1·d−1) in the submaxillary gland19. On the other hand, a significant enhancement of α1-adrenoceptor (specific [3H]prazosin binding) sites was observed in rat prostate after repeated treatment with the low dose (6 mg· kg−1·d−1) of SPE, but not in the submaxillary gland, spleen and heart. The in vitro experiment showed that SPE exhibited little tissue selectivity in the binding of each receptor. These data suggest that SPE administered orally specifically affects muscarinic and α1-adrenoceptors in the lower urinary tract. Although there is no clear explanation for such selectivity, the most plausible reason may be the preferential distribution of receptor-binding constituents in the lower urinary tract after the systemic administration of SPE. SPE contains a complex mixture of free fatty acids and their esters, small quantities of phytosterols (eg, β-sitosterol), aliphatic alcohols and various polyprenic compounds47. A systemic distribution study in rats administered [14C]oleic acid or [14C]sitosterol-supplemented SPE has shown that these components are accumulated to a greater extent in the prostate than in other tissues48. Because the prostate is particularly rich in free fatty acids, it would be expected that greater amounts of lipophilic substances accumulate in the prostate than in other tissues.
Repeated administration of SPE (100, 320 mg/kg) for 30 days inhibited prostatic hyperplasia induced by sulpiride in rats23 and repeated administration of SPE (50 mg/kg) for 60 days also inhibited prostate hyperplasia induced by testosterone10. Our previous study has shown that repeated treatment with testosterone for 4 weeks resulted in significantly increased (1.7–1.8 times) prostate weight in rats18. However, repeated oral administration of SPE (6 and 60 mg·kg−1·d−1) failed to significantly decrease tissue weight in any region of hypertrophied prostates of rats induced by the testosterone treatment. The reason why our data could not reproduce previous results might be the lower dosage and shorter treatment period. In agreement with the observation by Suzuki et al18, Rhodes et al49 noted that even high doses (180, 1800 mg/day) of SPE had no effect on prostatic hyperplasia in rats induced by testosterone treatment. The dosages (6 or 60 mg/kg) were comparable (320 mg/day) or 10 times higher than the dosage used for the treatment for BPH in humans.
Repeated treatment with testosterone in rats induced a significant (62%) increase in prostatic α1-adrenoceptor receptor sites. Such enhancement of prostatic α1-adrenoceptor density in testosterone-treated rats was alleviated by the concomitant administration of SPE (SABALSELECTTM, 6 mg/kg)18. Thus, oral administration of SPE has been suggested to attenuate up-regulation of α1-adrenoceptors in rat prostate induced by testosterone. It may be concluded that SPE at a clinically relevant dose exerts a direct effect on the pharmacological receptors in the lower urinary tract, thereby improving urinary dysfunction in patients with BPH and overactive bladders (OAB).
Effects on hepatic drug-metabolizing enzymes and blood biochemical values
Although the usage of medical herbs has grown quickly as a complementary and alternative medicine, scientific knowledge of the efficacy and safety of herbs is still lacking. Furthermore, the potential for interactions between herbs and drugs should be a concern because all herbs contain a large number of constituents50, 51, 52, 53. The proposed interactions would affect the pharmacokinetics and pharmacodynamics of drugs: absorption in the small intestine, metabolism in the intestine and liver, distribution to target organs, transport across cell membranes, and binding to specific receptors. Among these interactions, induction and inhibition of hepatic drug-metabolizing enzymes by herbal medicines or dietary compounds have been investigated. Suzuki et al18 have shown that repeated oral administration of SPE in rats had little significant influence on the content and activities of hepatic drug-metabolizing enzymes. Markowitz et al54 reported that SPE (320 mg/day for 14 days) for the treatment of lower urinary tract symptoms suggestive of BPH did not alter plasma concentrations of probe drugs for cytochrome P-450 (CYP)2D6 and CYP3A4 activity in normal volunteers. Therefore, it is unlikely that SPE at generally recommended doses alters the disposition of co-administered drugs. Also, repeated oral administration of SPE in rats had little effect on blood biochemical parameters, except for a slight increase in the albumin value, suggestive of relative safety even with long-term intake18.
Clinical trials
Clinical trials conducted with SPE in men with BPH are summarized in Table 355, 56, 57. There have been more than 11 placebo-controlled trials8, 17, 58, 59, 60, 61, 62, 63, 64, 65, 66 and 4 active-controlled trials11, 15, 67, 68.
Table 3. Effect of SPE on IPSS, peak urinary flow rate (Qmax) and mean values of urinary frequency (nocturia) in men with BPH in clinical trials.
| Study | Group | Dose | Duration | IPSS | Qmax | Nocturia | |||
|---|---|---|---|---|---|---|---|---|---|
| n | change | n | change | n | change | ||||
| Placebo-controlled study | |||||||||
| Bent S et al8 | SPE | 160*2 | 12m | 112 | −0.68# | 112 | 0.42 | ||
| Placebo | Placebo | 113 | −0.72# | 113 | −0.01 | ||||
| Willetts KE et al17 | SPE | 160*2 | 12m | 46 | 1.5 | ||||
| Placebo | Placebo | 47 | 4.4 | ||||||
| Gerber GS et al58 | SPE | 160*2 | 6m | 41 | −4.4 | 41 | 1.0 | ||
| Placebo | Placebo | 44 | −2.2 | 44 | 1.4 | ||||
| Marks LS et al59 | SPE (blend) | 106*3 | 6m | 21 | −2.24 | 21 | 1.27 | ||
| Placebo | Placebo | 23 | −1.39 | 23 | 0.09 | ||||
| Descotes JL et al60 | SPE | 160*2 | 1m | 82 | 3.42 | 82 | −0.67 | ||
| Placebo | Placebo | 94 | 1.06 | 94 | −0.32 | ||||
| Reece SH et al61 | SPE | 160*2 | 3m | 33 | 2.35 | 33 | −1.0 | ||
| Placebo | Placebo | 37 | 2.3 | 37 | −1.0 | ||||
| Cukier J et al62 | SPE | 2*80*2 | 2–3m | 43 | −1.1 | ||||
| Placebo | Placebo | 47 | −0.5 | ||||||
| Tasca A et al63 | SPE | 160*2 | 3m | 14 | 3.3 | 14 | −2.6 | ||
| Placebo | Placebo | 13 | 0.6 | 13 | −1.2 | ||||
| Champault G et al64 | SPE | 2*80*2 | 1m | 46 | 2.7 | 47 | −1.4 | ||
| Placebo | Placebo | 39 | 0.25 | 41 | −0.5 | ||||
| Boccafoschi C et al65 | SPE | 160*2 | 2m | 11 | 4.13 | 11 | −2.2 | ||
| Placebo | Placebo | 11 | 1.96 | 11 | −1.0 | ||||
| Emili E et al66 | SPE | 160*2 | 1m | 15 | 3.37 | 15 | −1.6 | ||
| Placebo | Placebo | 15 | 0.2 | 15 | −0.4 | ||||
| Active-controlled study | |||||||||
| Debruyne F et al16 | SPE | 320*1 | 12m | 350 | −4.4 | 1.79 | |||
| Tamsulosin | 0.4*1 | 354 | −4.4 | 1.89 | |||||
| Carraro JC et al11 | SPE | 160*2 | 6m | 464 | −5.8 | 2.68 | 464 | −0.74 | |
| Finasteride | 5 | 477 | −6.2 | 3.26 | 477 | −0.69 | |||
| Grasso M et al67 | SPE | 160*2 | 0.75m | 31 | 2.8 | 32 | −1.0 | ||
| Alfuzosin | 7.5 | 32 | 4.7 | 31 | −0.9 | ||||
| Adriazola Semino et al68 | SPE | 160*2 | 3m | 20 | 1.5 | 20 | −0.2 | ||
| Prazosin | 22 | 0.47 | 22 | −0.4 | |||||
AUASI: American Urological Association Symptom Index
Placebo-controlled trials
As shown in Table 3, all placebo-controlled trials were conducted with SPE (320 mg/day) and placebo. Most of them were reported in the 1980s; the patient number was usually limited and the evaluation period was relatively short. More recently, two new and relatively large-scale placebo-controlled trials were conducted. One was reported by Willetts et al17 and the other by Bent et al8. A double-blind placebo-controlled trial was held in Australia from January 1999 to March 200017. One hundred men with symptomatic BPH, aged <80 years with a maximal urinary flow rate of 5–15 mL/s, were included in the trial and were randomized to a group receiving SPE (160 mg twice a day) or placebo. The treatment period was 12 weeks. The primary outcomes were changes in IPSS, maximal urinary flow rate, and the Rosen International Index of Erectile Function (IIEF). The IPSS score decreased over time in both treatment groups; however, there was no significant difference after 12 weeks of treatment between the groups. There were no significant differences between the two treatment groups in the quality of life (QOL) score, the maximal urinary flow rate, and the IIEF score. On the other hand, each treatment group showed a significant improvement between week 0 and week 12. This trial was double-blind placebo-controlled, with high compliance and a low withdrawal rate; therefore, it could be regarded as a well-controlled trial. However, some of the results were unexpected, especially for the IPSS score and urine flow rates. The authors considered that it might be ascribable to a low IPSS at baseline, a small number of patients, and a relatively short trial period.
The other clinical trial was held in the United States from July 2001 to May 20048. It was a double-blind placebo-controlled trial lasting 14 months (2 months screening, 12 months treatment). Two hundred twenty-five men aged >49 years, with a maximum urinary flow rate of <15 mL/s, were randomly assigned to receive SPE (160 mg twice a day) or placebo. The primary outcomes were changes in the American Urological Association Symptom Index (AUASI) and the maximal urinary flow rate. Secondary outcomes were changes in prostate size, residual urinary volume after voiding, QOL, laboratory values, and the rate of reported adverse effects8. No significant differences between the SPE and placebo groups were observed in the change in AUASI scores (mean difference: 0.04 point), maximal urinary flow rate (mean difference: 0.43 mL/s), prostate size, residual volume after voiding, QOL or serum prostate-specific antigen (PSA) levels during the one-year trial. The incidence of side effects was similar in the two groups. During the single-blind, placebo run-in period, there was a small but significant decrease in the AUASI score. Bent et al8 considered the discrepancy between their results and results from previous trials and questioned the adequacy of blinding, whether certain attributes of participants were taken into account, and specification of the SPE preparations of the previous trials.
Active-controlled trials
Four active-controlled trials have been conducted with SPE in men with BPH (Table 3). Just as the placebo-controlled trials, half of the trials enrolled very limited numbers of patients and had very short evaluation periods. Two active-controlled trials recruited enough patients and had relatively long treatment periods (6 and 12 months).
One of these studies was a 6-month, double-blind, randomized trial that compared the effects of SPE (160 mg twice daily, Permixon®) with that of a 5α-reductase inhibitor (5 mg finasteride) in 1,098 men with moderate BPH using IPSS as the primary outcome11. Both SPE and finasteride decreased the IPSS (−37% and −39%, respectively), improved QOL (by 38% and 41%) and increased peak urinary flow rate (+25% and +30%). Prostate volume (−18%) and serum PSA levels (−41%) were markedly decreased by finasteride. On the other hand, SPE improved symptoms with little effect on prostate volume and no change in PSA levels. SPE fared better than finasteride in a sexual function questionnaire and resulted in fewer complaints of decreased libido and impotence. Both treatments relieved the symptoms of BPH in about two thirds of the patients but, unlike finasteride, SPE had little effect on so-called androgen-dependent parameters. This suggests that other pathways are also involved in the symptomatology of BPH.
The other trial was a comparison of SPE (Permixon®) with tamsulosin16. Eight hundred and eleven men with symptomatic BPH were recruited and 704 patients were randomized to receive either tamsulosin (0.4 mg/d) or SPE (320 mg/d). At 12 months, IPSS decreased by 4.4% in each group and no differences were observed in either irritative or obstructive symptom improvements. The increase in maximal urinary flow rate was similar in both treatment groups. The mean prostate volume decreased by 0.99 mL in the SPE group, whereas it increased by 0.22 mL in the tamsulosin group. PSA remained stable, whereas prostate volume decreased slightly in SPE-treated patients. The tamsulosin group showed no significant changes in total PSA. The two compounds were well tolerated; however, evacuation disorders occurred more frequently in the tamsulosin group. This trial demonstrated that SPE and tamsulosin were equivalent in the medical treatment of LUTS in men with BPH during and up to 12 months of therapy.
Debruyne et al69 conducted a subset analysis of the trial mentioned above. One hundred twenty-four patients with severe LUTS (IPSS>19) were stratified: 59 and 65 patients had been randomized to the tamsulosin and SPE groups, respectively. At 12 months, total IPSS decreased by 7.8% with SPE and 5.8% with tamsulosin; the irritative symptoms were improved significantly more with SPE. The superiority of SPE in reducing irritative symptoms appeared only 3 months into treatment and was maintained up to month 12. Further analyses were conducted with the most severely symptomatic patients. In this subgroup, the between-group difference was maximal as soon as month 3 and was maintained up to month 12 for both irritative and obstructive IPSS. For the irritative symptoms, the difference between groups was statistically significant over this period. Although the number of patients decreased, the between-group difference was still statistically significant over this period for the irritative symptoms.
Adverse effects of SPE are rare and usually mild. They include constipation, decreased libido, diarrhea, headache, hypertension, nausea, urine retention and pancreatitis3, 70. In all randomized clinical trials in the meta-analysis3, withdrawal rates (a rough indicator of patient acceptance) were 9.1% for SPE, 11.2% for finasteride and 7.0% for placebo. No herb-drug interactions have been described54, 71. However, in high throughput screening, SPE showed potent inhibition of the metabolic activity of CYP3A4, 2D6, and 2C972.
Conclusions
BPH and associated LUTS are common disorders in aging men. Plant extracts are widely used in the treatment of BPH and related LUTS. In fact, SPE has been widely used as a therapeutic remedy for BPH in Europe. In the United States and Japan, SPE is not a prescribed medication; however, it has received attention from patients with BPH.
It is suggested that SPE has various pharmacological mechanisms (eg, inhibition of 5α-reductase, anti-androgenic effects, anti-proliferative effects, anti-inflammatory effects, and anti-edema effects). In addition, SPE may have α1-adrenoceptor inhibitory properties. In addition to the α1-adrenoceptor binding, we found significant binding to the muscarinic and 1,4-dihydropyridine receptors as novel mechanisms of pharmacological action of SPE in the lower urinary tract (Figure 2). Also, there is a possibility that SPE affects vanilloid receptor activity in the bladder. Anticholinergic agents are widely used for the treatment of OAB; therefore, inhibition of muscarinic receptors could be a novel pharmacological effect of SPE on the lower urinary tract for relief of irritative and obstructive symptoms of dysuria in BPH and LUTS. It is unlikely that the usefulness of SPE is limited by notable interactions with coadministered drugs or serious adverse events. Thus, this review may significantly contribute to the further understanding of the pharmacological effects of SPE in the treatment of patients with BPH and LUTS.
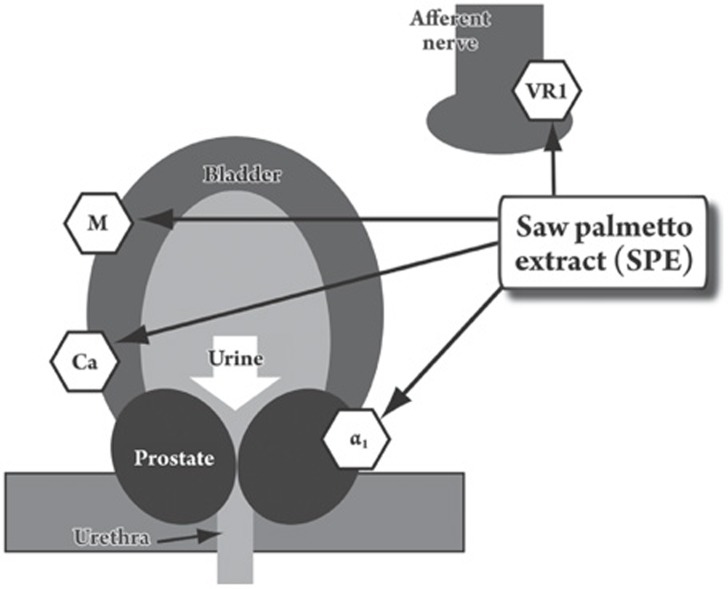
Figure 2.
Proposed binding activities of saw palmetto extract (SPE) for pharmacological receptors in the lower urinary tract (bladder and prostate). M: muscarinic receptor, VR1: vanilloid receptor, Ca: 1,4-dihydropyridine receptor, α1: α1-adrenoceptor.
The constituents of different preparations of SPE differed markedly. The efficacy of SPE likely depends on the ingredients. Hence, it would be ideal to identify the active ingredients and to establish the optimal preparation in terms of efficacy and safety, or it should be recognized that the efficacy and the safety of SPE could differ according to brand.
Considering that recent clinical trials, which were relatively large and well-controlled, did not demonstrate the superiority of SPE to placebo, the clinical potency of SPE has been questioned. However, the facts that several clinical studies showed the superiority of SPE over placebo and its comparability to prescribed medications and that many patients appear to reap benefits from SPE should be considered. Hence, it is anticipated that some suitably designed clinical studies (adequacy of blinding, treatment period, patient numbers, patient characteristics, etc) will be conducted and we could ascertain the real potential of SPE for patients with BPH.
References
- Roehrborn CG, Rosen RC. Medical therapy options for aging men with benign prostatic hyperplasia: focus on alfusozin 10 mg once daily. Clin Interv Aging. 2008;3:511–24. doi: 10.2147/cia.s3635. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lepor H, Williford WO, Barry MJ, Brawer MK, Dixon CM, Gormley G, et al. The efficacy of terazosin, finasteride, or both in benign prostatic hyperplasia. Veterans Affairs Cooperative Studies Benign Prostatic Hyperplasia Study Group. N Engl J Med. 1996;335:533–9. doi: 10.1056/NEJM199608223350801. [DOI] [PubMed] [Google Scholar]
- Ernst E. The risk-benefit profile of commonly used herbal therapies: Ginkgo, St John's Wort, Ginseng, Echinacea, Saw palmetto, and Kava. Ann Intern Med. 2002;136:42–53. doi: 10.7326/0003-4819-136-1-200201010-00010. [DOI] [PubMed] [Google Scholar]
- Wilt TJ, Ishani A, Stark G, MacDonald R, Lau J, Mulrow C. Saw palmetto extracts for treatment of benign prostatic hyperplasia: a systematic review. JAMA. 1998;280:1604–9. doi: 10.1001/jama.280.18.1604. [DOI] [PubMed] [Google Scholar]
- Lowe FC, Ku JC. Phytotherapy in treatment of benign prostatic hyperplasia: a critical review. Urology. 1996;48:12–20. doi: 10.1016/s0090-4295(96)00077-5. [DOI] [PubMed] [Google Scholar]
- Koch E. Extracts from fruits of saw palmetto (Sabal serrulata) and roots of stinging nettle (Urtica dioica): viable alternatives in the medical treatment of benign prostatic hyperplasia and associated lower urinary tracts symptoms. Planta Med. 2001;67:489–500. doi: 10.1055/s-2001-16496. [DOI] [PubMed] [Google Scholar]
- McNaughton-Collins M, Barry MJ. Managing patients with lower urinary tract symptoms suggestive of benign prostatic hyperplasia. Am J Med. 2005;118:1331–9. doi: 10.1016/j.amjmed.2004.12.033. [DOI] [PubMed] [Google Scholar]
- Bent S, Kane C, Shinohara K, Neuhaus J, Hudes ES, Goldberg H, et al. Saw palmetto for benign prostatic hyperplasia. N Engl J Med. 2006;354:557–66. doi: 10.1056/NEJMoa053085. [DOI] [PubMed] [Google Scholar]
- Sultan C, Terraza A, Devillier C, Carilla E, Briley M, Loire C, et al. Inhibition of androgen metabolism and binding by a liposterolic extract of “Serenoa repens B” in human foreskin fibroblasts. J Steroid Biochem. 1984;20:515–9. doi: 10.1016/0022-4731(84)90264-4. [DOI] [PubMed] [Google Scholar]
- Paubert-Braquet M, Richardson FO, Servent-Saez N, Gordon WC, Monge MC, Bazan NG, et al. Effect of Serenoa repens extract (Permixon) on estradiol/testosterone-induced experimental prostate enlargement in the rat. Pharmacol Res. 1996;34:171–9. doi: 10.1006/phrs.1996.0085. [DOI] [PubMed] [Google Scholar]
- Carraro JC, Raynaud JP, Koch G, Chisholm GD, Di Silverio F, Teillac P, et al. Comparison of phytotherapy (Permixon) with finasteride in the treatment of benign prostate hyperplasia: a randomized international study of 1 098 patients Prostate 199629231–40.discussion 241–2. [DOI] [PubMed] [Google Scholar]
- Gerber GS, Zagaja GP, Bales GT, Chodak GW, Contreras BA. Saw palmetto (Serenoa repens) in men with lower urinary tract symptoms: effects on urodynamic parameters and voiding symptoms. Urology. 1998;51:1003–7. doi: 10.1016/s0090-4295(98)00143-5. [DOI] [PubMed] [Google Scholar]
- Goepel M, Hecker U, Krege S, Rubben H, Michel MC. Saw palmetto extracts potently and noncompetitively inhibit human alpha1-adrenoceptors in vitro. Prostate. 1999;38:208–15. doi: 10.1002/(sici)1097-0045(19990215)38:3<208::aid-pros5>3.0.co;2-4. [DOI] [PubMed] [Google Scholar]
- Oki T, Suzuki M, Nishioka Y, Yasuda A, Umegaki K, Yamada S. Effects of saw palmetto extract on micturition reflex of rats and its autonomic receptor binding activity. J Urol. 2005;173:1395–9. doi: 10.1097/01.ju.0000146273.26591.f5. [DOI] [PubMed] [Google Scholar]
- Andersson KE. LUTS treatment: future treatment options. Neurourol Urodyn. 2007;26:934–47. doi: 10.1002/nau.20500. [DOI] [PubMed] [Google Scholar]
- Debruyne F, Koch G, Boyle P, Da Silva FC, Gillenwater JG, Hamdy FC, et al. Comparison of a phytotherapeutic agent (Permixon) with an alpha-blocker (Tamsulosin) in the treatment of benign prostatic hyperplasia: a 1-year randomized international study Eur Urol 200241497–506.discussion 506–7. [PubMed] [Google Scholar]
- Willetts KE, Clements MS, Champion S, Ehsman S, Eden JA. Serenoa repens extract for benign prostate hyperplasia: a randomized controlled trial. BJU Int. 2003;92:267–70. doi: 10.1046/j.1464-410x.2003.04316.x. [DOI] [PubMed] [Google Scholar]
- Suzuki M, Oki T, Maruyama S, Takagi Y, Umegaki K, Nishioka Y, et al. Pharmacological effects of Saw Palmetto Extract on urodynamic functions and automic receptors in lower urinary tract of rats. Jpn Neurogenic Bladder Soc. 2005;16:191–201. [Google Scholar]
- Suzuki M, Oki T, Sugiyama T, Umegaki K, Uchida S, Yamada S. Muscarinic and alpha 1-adrenergic receptor binding characteristics of saw palmetto extract in rat lower urinary tract. Urology. 2007;69:1216–20. doi: 10.1016/j.urology.2007.02.038. [DOI] [PubMed] [Google Scholar]
- Habib FK, Wyllie MG. Not all brands are created equal: a comparison of selected components of different brands of Serenoa repens extract. Prostate Cancer Prostatic Dis. 2004;7:195–200. doi: 10.1038/sj.pcan.4500746. [DOI] [PubMed] [Google Scholar]
- Marks LS, Tyler VE. Saw palmetto extract: newest (and oldest) treatment alternative for men with symptomatic benign prostatic hyperplasia. Urology. 1999;53:457–61. [PubMed] [Google Scholar]
- Levin RM, Das AK. A scientific basis for the therapeutic effects of Pygeum africanum and Serenoa repens. Urol Res. 2000;28:201–9. doi: 10.1007/s002409900098. [DOI] [PubMed] [Google Scholar]
- Van Coppenolle F, Le Bourhis X, Carpentier F, Delaby G, Cousse H, Raynaud JP, et al. Pharmacological effects of the lipidosterolic extract of Serenoa repens (Permixon) on rat prostate hyperplasia induced by hyperprolactinemia: comparison with finasteride. Prostate. 2000;43:49–58. doi: 10.1002/(sici)1097-0045(20000401)43:1<49::aid-pros7>3.0.co;2-j. [DOI] [PubMed] [Google Scholar]
- Steers WD.5alpha-reductase activity in the prostate Urology 20015817–24.discussion 24 [DOI] [PubMed] [Google Scholar]
- Delos S, Iehle C, Martin PM, Raynaud JP. Inhibition of the activity of ‘basic' 5 alpha-reductase (type 1) detected in DU 145 cells and expressed in insect cells. J Steroid Biochem Mol Biol. 1994;48:347–52. doi: 10.1016/0960-0760(94)90074-4. [DOI] [PubMed] [Google Scholar]
- Di Silverio F, Monti S, Sciarra A, Varasano PA, Martini C, Lanzara S, et al. Effects of long-term treatment with Serenoa repens (Permixon) on the concentrations and regional distribution of androgens and epidermal growth factor in benign prostatic hyperplasia. Prostate. 1998;37:77–83. doi: 10.1002/(sici)1097-0045(19981001)37:2<77::aid-pros3>3.0.co;2-i. [DOI] [PubMed] [Google Scholar]
- Iehle C, Delos S, Guirou O, Tate R, Raynaud JP, Martin PM. Human prostatic steroid 5 alpha-reductase isoforms — a comparative study of selective inhibitors. J Steroid Biochem Mol Biol. 1995;54:273–9. doi: 10.1016/0960-0760(95)00134-l. [DOI] [PubMed] [Google Scholar]
- Weisser H, Tunn S, Behnke B, Krieg M. Effects of the sabal serrulata extract IDS 89 and its subfractions on 5 alpha-reductase activity in human benign prostatic hyperplasia. Prostate. 1996;28:300–6. doi: 10.1002/(SICI)1097-0045(199605)28:5<300::AID-PROS5>3.0.CO;2-F. [DOI] [PubMed] [Google Scholar]
- Palin MF, Faguy M, LeHoux JG, Pelletier G. Inhibitory effects of Serenoa repens on the kinetic of pig prostatic microsomal 5alpha-reductase activity. Endocrine. 1998;9:65–9. doi: 10.1385/ENDO:9:1:65. [DOI] [PubMed] [Google Scholar]
- Raynaud JP, Cousse H, Martin PM. Inhibition of type 1 and type 2 5alpha-reductase activity by free fatty acids, active ingredients of Permixon. J Steroid Biochem Mol Biol. 2002;82:233–9. doi: 10.1016/s0960-0760(02)00187-5. [DOI] [PubMed] [Google Scholar]
- Carilla E, Briley M, Fauran F, Sultan C, Duvilliers C. Binding of Permixon, a new treatment for prostatic benign hyperplasia, to the cytosolic androgen receptor in the rat prostate. J Steroid Biochem. 1984;20:521–3. doi: 10.1016/0022-4731(84)90265-6. [DOI] [PubMed] [Google Scholar]
- Mahapokai W, van den Ingh TS, van Mil F, van Garderen E, Schalken JA, Mol JA, et al. Immune response in hormonally-induced prostatic hyperplasia in the dog. Vet Immunol Immunopathol. 2001;78:297–303. doi: 10.1016/s0165-2427(01)00236-7. [DOI] [PubMed] [Google Scholar]
- Steiner G, Gessl A, Kramer G, Schollhammer A, Forster O, Marberger M. Phenotype and function of peripheral and prostatic lymphocytes in patients with benign prostatic hyperplasia. J Urol. 1994;151:480–4. doi: 10.1016/s0022-5347(17)34998-4. [DOI] [PubMed] [Google Scholar]
- Breu W, Hagenlocher M, Redl K, Tittel G, Stadler F, Wagner H. Anti-inflammatory activity of sabal fruit extracts prepared with supercritical carbon dioxide. In vitro antagonists of cyclooxygenase and 5-lipoxygenase metabolism. Arzneimittelforschung. 1992;42:547–51. [PubMed] [Google Scholar]
- Paubert-Braquet M, Mencia Huerta JM, Cousse H, Braquet P. Effect of the lipidic lipidosterolic extract of Serenoa repens (Permixon) on the ionophore A23187-stimulated production of leukotriene B4 (LTB4) from human polymorphonuclear neutrophils. Prostaglandins Leukot Essent Fatty Acids. 1997;57:299–304. doi: 10.1016/s0952-3278(97)90548-2. [DOI] [PubMed] [Google Scholar]
- Vela Navarrete R, Garcia Cardoso JV, Barat A, Manzarbeitia F, Lopez Farre A. BPH and inflammation: pharmacological effects of Permixon on histological and molecular inflammatory markers. Results of a double blind pilot clinical assay. Eur Urol. 2003;44:549–55. doi: 10.1016/s0302-2838(03)00368-3. [DOI] [PubMed] [Google Scholar]
- Kyprianou N, Tu H, Jacobs SC. Apoptotic versus proliferative activities in human benign prostatic hyperplasia. Hum Pathol. 1996;27:668–75. doi: 10.1016/s0046-8177(96)90396-2. [DOI] [PubMed] [Google Scholar]
- Cardillo M, Berchem G, Tarkington MA, Krajewski S, Krajewski M, Reed JC, et al. Resistance to apoptosis and up regulation of Bcl-2 in benign prostatic hyperplasia after androgen deprivation. J Urol. 1997;158:212–6. doi: 10.1097/00005392-199707000-00073. [DOI] [PubMed] [Google Scholar]
- Colombel M, Vacherot F, Diez SG, Fontaine E, Buttyan R, Chopin D. Zonal variation of apoptosis and proliferation in the normal prostate and in benign prostatic hyperplasia. Br J Urol. 1998;82:380–5. doi: 10.1046/j.1464-410x.1998.00752.x. [DOI] [PubMed] [Google Scholar]
- Vacherot F, Azzouz M, Gil-Diez-De-Medina S, Colombel M, De La Taille A, Lefrere Belda MA, et al. Induction of apoptosis and inhibition of cell proliferation by the lipido-sterolic extract of Serenoa repens (LSESr, Permixon®) in benign prostatic hyperplasia. Prostate. 2000;45:259–66. doi: 10.1002/1097-0045(20001101)45:3<259::aid-pros9>3.0.co;2-g. [DOI] [PubMed] [Google Scholar]
- Claus S, Berges R, Senge T, Schulze H. Cell kinetic in epithelium and stroma of benign prostatic hyperplasia. J Urol. 1997;158:217–21. doi: 10.1097/00005392-199707000-00074. [DOI] [PubMed] [Google Scholar]
- Vacher P, Prevarskaya N, Skryma R, Audy MC, Vacher AM, Odessa MF, et al. The lipidosterolic extract from serenoa repens interferes with prolactin receptor signal transduction. J Biomed Sci. 1995;2:357–65. doi: 10.1007/BF02255223. [DOI] [PubMed] [Google Scholar]
- Koch E. Pharmakologie und Wirkmechanismus von Extrakten aus Sabalfrüchten (Sabal fructus), Brennesselwurzeln (Urtica radix) und Kürbissamen (Cucurbitae peponis semen) bei der Behandlung der benignen Prostatahyperplasie. Phytopharmaka in Forschung und klinischer Anwendung. 1995.
- Birder LA, Kanai AJ, de Groat WC, Kiss S, Nealen ML, Burke NE, et al. Vanilloid receptor expression suggests a sensory role for urinary bladder epithelial cells. Proc Natl Acad Sci USA. 2001;98:13396–401. doi: 10.1073/pnas.231243698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Apostolidis A, Brady CM, Yiangou Y, Davis J, Fowler CJ, Anand P. Capsaicin receptor TRPV1 in urothelium of neurogenic human bladders and effect of intravesical resiniferatoxin. Urology. 2005;65:400–5. doi: 10.1016/j.urology.2004.10.007. [DOI] [PubMed] [Google Scholar]
- Ito Y, Kageyama A, Iwasaki Y, Watanabe T, Yamada S.Effects of propiverine and oxybutynin to treat overactive bladder, on vanilloid receptor (transient receptor potential vanilloid subtype 1: TRPV1) Jpn Neurogenic Bladder Soc; in press. [Google Scholar]
- Plosker GL, Brogden RN.Serenoa repens (Permixon). A review of its pharmacology and therapeutic efficacy in benign prostatic hyperplasia Drugs Aging 19969379–95. [DOI] [PubMed] [Google Scholar]
- Chevalier G, Benard P, Cousse H, Bengone T. Distribution study of radioactivity in rats after oral administration of the lipido/sterolic extract of Serenoa repens (Permixon) supplemented with [1-14C]-lauric acid, [1-14C]-oleic acid or [4-14C]-beta-sitosterol. Eur J Drug Metab Pharmacokinet. 1997;22:73–83. doi: 10.1007/BF03189787. [DOI] [PubMed] [Google Scholar]
- Rhodes L, Primka RL, Berman C, Vergult G, Gabriel M, Pierre-Malice M, et al. Comparison of finasteride (Proscar), a 5 alpha reductase inhibitor, and various commercial plant extracts in in vitro and in vivo 5 alpha reductase inhibition. Prostate. 1993;22:43–51. doi: 10.1002/pros.2990220107. [DOI] [PubMed] [Google Scholar]
- Izzo AA, Ernst E. Interactions between herbal medicines and prescribed drugs: a systematic review. Drugs. 2001;61:2163–75. doi: 10.2165/00003495-200161150-00002. [DOI] [PubMed] [Google Scholar]
- Williamson EM. Synergy and other interactions in phytomedicines. Phytomedicine. 2001;8:401–9. doi: 10.1078/0944-7113-00060. [DOI] [PubMed] [Google Scholar]
- Sugiyama T, Kubota Y, Shinozuka K, Yamada S, Wu J, Umegaki K. Ginkgo biloba extract modifies hypoglycemic action of tolbutamide via hepatic cytochrome P450 mediated mechanism in aged rats. Life Sci. 2004;75:1113–22. doi: 10.1016/j.lfs.2004.02.020. [DOI] [PubMed] [Google Scholar]
- Uchida S, Yamada H, Li XD, Maruyama S, Ohmori Y, Oki T, et al. Effects of Ginkgo biloba extract on pharmacokinetics and pharmacodynamics of tolbutamide and midazolam in healthy volunteers. J Clin Pharmacol. 2006;46:1290–8. doi: 10.1177/0091270006292628. [DOI] [PubMed] [Google Scholar]
- Markowitz JS, Donovan JL, Devane CL, Taylor RM, Ruan Y, Wang JS, et al. Multiple doses of saw palmetto (Serenoa repens) did not alter cytochrome P450 2D6 and 3A4 activity in normal volunteers. Clin Pharmacol Ther. 2003;74:536–42. doi: 10.1016/j.clpt.2003.08.010. [DOI] [PubMed] [Google Scholar]
- Boyle P, Robertson C, Lowe F, Roehrborn C. Meta-analysis of clinical trials of permixon in the treatment of symptomatic benign prostatic hyperplasia. Urology. 2000;55:533–9. doi: 10.1016/s0090-4295(99)00593-2. [DOI] [PubMed] [Google Scholar]
- Boyle P, Robertson C, Lowe F, Roehrborn C. Updated meta-analysis of clinical trials of Serenoa repens extract in the treatment of symptomatic benign prostatic hyperplasia. BJU Int. 2004;93:751–6. doi: 10.1111/j.1464-410X.2003.04735.x. [DOI] [PubMed] [Google Scholar]
- Gerber GS, Fitzpatrick JM. The role of a lipido-sterolic extract of Serenoa repens in the management of lower urinary tract symptoms associated with benign prostatic hyperplasia. BJU Int. 2004;94:338–44. doi: 10.1111/j.1464-410X.2004.04962.x. [DOI] [PubMed] [Google Scholar]
- Gerber GS, Kuznetsov D, Johnson BC, Burstein JD.Randomized, double-blind, placebo-controlled trial of saw palmetto in men with lower urinary tract symptoms Urology 200158960–4.discussion 964–5. [DOI] [PubMed] [Google Scholar]
- Marks LS, Partin AW, Epstein JI, Tyler VE, Simon I, Macairan ML, et al. Effects of a saw palmetto herbal blend in men with symptomatic benign prostatic hyperplasia. J Urol. 2000;163:1451–6. [PubMed] [Google Scholar]
- Descotes JL, Rambeaud JJ, Deschaseauz P, Faure G. Placebo-controlled evaluation of the efficacy and tolerability of Permixon in benign prostatic hyperplasia after exclusion of placebo responders. Clin Drug Investig. 1995;9:291–7. [Google Scholar]
- Reece SH, Memon A, Smart CJ, Dewbury K. The value of permixon in benign prostatic hypertrophy. Br J Urol. 1986;58:36–40. doi: 10.1111/j.1464-410x.1986.tb05424.x. [DOI] [PubMed] [Google Scholar]
- Cukier J, Ducasso J, Le Guillou M, Leriche A, Lobel B, Toubol J. Permixon versus placebo: resultats d'une ‘etude multicentrique. CR Ther Pharmacol Clin. 1985;4:15–21. [Google Scholar]
- Tasca A, Barulli M, Cavazzana A, Zattoni F, Artibani W, Pagano F.Treatment of obstructive symptomatology caused by prostatic adenoma with an extract of Serenoa repens. Double-blind clinical study vs placebo Minerva Urol Nefrol 19853787–91. [PubMed] [Google Scholar]
- Champault G, Patel JC, Bonnard AM. A double-blind trial of an extract of the plant Serenoa repens in benign prostatic hyperplasia. Br J Clin Pharmacol. 1984;18:461–2. doi: 10.1111/j.1365-2125.1984.tb02491.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boccafoschi C, Annoscia S. Comparison of Serenoa repens extract with placebo by controlled clinical trial in patients with prostatic adenomatosis. Urologia. 1983;50:1257–68. [Google Scholar]
- Emili E, Cingo M, Petrone U. Risulti clinici su un nueovo farmaco nella terapia dell-ipertrofia della prostate (Permixon®) Urologia. 1983;50:1042–9. [Google Scholar]
- Grasso M, Montesano A, Buonaguidi A, Castelli M, Lania C, Rigatti P, et al. Comparative effects of alfuzosin versus Serenoa repens in the treatment of symptomatic benign prostatic hyperplasia. Arch Esp Urol. 1995;48:97–103. [PubMed] [Google Scholar]
- Adriazola Semino M, Lozano Ortega JL, Garcia Cobo E, Tejeda Banez E, Romero Rodriguez F.Symptomatic treatment of benign hypertrophy of the prostate. Comparative study of prazosin and serenoa repens Arch Esp Urol 199245211–3. [PubMed] [Google Scholar]
- Debruyne F, Boyle P, Calais Da Silva F, Gillenwater JG, Hamdy FC, Perrin P, et al. Evaluation of the clinical benefit of permixon and tamsulosin in severe BPH patients-PERMAL study subset analysis. Eur Urol. 2004;45:773–9. doi: 10.1016/j.eururo.2004.01.015. [DOI] [PubMed] [Google Scholar]
- Jibrin I, Erinle A, Saidi A, Aliyu ZY. Saw palmetto-induced pancreatitis. South Med J. 2006;99:611–2. doi: 10.1097/01.smj.0000215642.76198.44. [DOI] [PubMed] [Google Scholar]
- Gurley BJ, Gardner SF, Hubbard MA, Williams DK, Gentry WB, Carrier J, et al. In vivo assessment of botanical supplementation on human cytochrome P450 phenotypes: Citrus aurantium, Echinacea purpurea, milk thistle, and saw palmetto. Clin Pharmacol Ther. 2004;76:428–40. doi: 10.1016/j.clpt.2004.07.007. [DOI] [PubMed] [Google Scholar]
- Yale SH, Glurich I. Analysis of the inhibitory potential of Ginkgo biloba, Echinacea purpurea, and Serenoa repens on the metabolic activity of cytochrome P450 3A4, 2D6, and 2C9. J Altern Complement Med. 2005;11:433–9. doi: 10.1089/acm.2005.11.433. [DOI] [PubMed] [Google Scholar]