Abstract
Background/Aims
Hypnotherapy is considered as a promising intervention for irritable bowel syndrome (IBS), but the evidence is still limited. The aims of this study were to conduct a systematic review and meta-analysis to estimate the efficacy of hypnotherapy for the treatment of IBS.
Methods
A literature search was performed using MEDLINE (PubMed), Embase, PsycINFO and the Cochrane Central Register of Controlled Trials (CENTRAL database). Only randomized controlled trials that compared hypnotherapy with any other conventional treatment or no treatment in patients with IBS were included. Studies had to report outcomes as IBS symptom score or quality of life. The mean change in outcome score was used to pool these outcomes for the meta-analysis. Data were synthesized using the standardized mean difference for continuous data.
Results
Seven randomized controlled trials (6 papers) involving 374 patients with IBS were identified. Performance bias was high in all trials because it was impossible to blind participants and therapists in this type of intervention. The outcomes in this meta-analysis were evaluated at 3 months for short-term effects and at 1 year for long-term effects. The change in abdominal pain score at 3 months was significant in the hypnotherapy group (standardized mean difference, −0.83; 95% CI, −1.65 to −0.01). Three of the 4 trials showed greater improvement in overall gastrointestinal symptoms in the hypnotherapy group.
Conclusions
This study provides clearer evidence that hypnotherapy has beneficial short-term effects in improving gastrointestinal symptoms of patients with IBS.
Keywords: Gastrointestinal diseases, Hypnosis, Irritable bowel syndrome, Meta-analysis, Review
Introduction
Irritable bowel syndrome (IBS) is a chronic functional gastrointestinal disorder characterized by recurrent abdominal pain or discomfort associated with altered bowel movements.1 IBS can be diagnosed only when there is no objective evidence of an underlying organic disorder.2 It is one of the most common bowel disorders diagnosed by gastroenterologists.3 The impact of IBS on quality of life (QOL) is as strong as that observed in other serious disorders such as congestive heart failure or chronic renal failure.4,5
Treatment options include reassurance, dietary modification, and pharmacological treatment. Current pharmacological treatments such as bulking agents, antispasmodics, and antidepressants focus mainly on controlling the symptoms of IBS. However, both pharmacological and conventional options are unsatisfactory in general.6–8
Many IBS patients have psychological symptoms such as anxiety and depression,9 which provide a fundamental rationale for psychological treatment. A number of studies have been conducted to evaluate the effects of psychological treatment for IBS.10 Among them, hypnotherapy has gained popularity after the first randomized controlled trial (RCT) in 1984 demonstrating notable benefits of hypnotherapy.11 Several additional studies have also reported benefits of hypnotherapy in treating gastrointestinal symptoms and QOL of IBS patients.12–16
Previous systematic reviews to prove that there are statistically significant benefits have been based on pooled results of research on the effectiveness of hypnotherapy for IBS patients.17,18 These reviews concluded that, although a number of studies have shown a beneficial effect of hypnotherapy, insufficient evidence existed to recommend widespread use because of limitations in the sample sizes and methodological flaws. From these conclusions, the National Institute for Health and Clinical Excellence guidelines noted that hypnotherapy is a promising intervention for IBS but the evidence remains to be limited.19 These uncertainties justify a systematic review and meta-analysis to determine whether hypnotherapy has significant beneficial effects in the treatment of IBS. Well-designed RCTs have been conducted, but there is no ongoing RCT; this prompted us to update the previous review. We conducted a comprehensive review of RCTs to estimate the efficacy of hypnotherapy for the treatment of IBS.
Materials and Methods
Eligibility Criteria
The inclusion criteria in this study were specified in advance and followed the population, intervention, comparison and outcome(s) (PICO) study design: patients who had been diagnosed with IBS as the population of interest, given hypnotherapy as an intervention, or given any other conventional treatment or no treatment for comparison. Outcomes were overall gastrointestinal symptoms, individual gastrointestinal symptoms (abdominal pain, constipation and diarrhea) and QOL, which were measured as scores. Any studies that reported at least one of these outcomes were included. Only RCTs were included in this meta-analysis to provide more unbiased information than that obtained from other study designs. There was no limitation on publication language, study size or study setting. Patients were not otherwise restricted by age or ethics. Studies that included a comparison between different types of hypnotherapy were excluded.
Search Strategy
A literature search was conducted using MEDLINE (PubMed), Embase, PsycINFO, and the Cochrane Central Register of Controlled Trials (CENTRAL database) from January 15, 2013. The search was performed using the Medical Subject Headings (MeSH): “colonic diseases,” “colonic diseases, functional,” “irritable bowel syndrome,” and “hypnosis.” Other free-text search terms used were “irritable bowel syndrome,” “hypnotherapy,” “hypnosis,” “mesmerism,” “imagery” and “autohypnosis.” Search terms were adapted according to each particular database. The strategy was refined further by a local health care librarian to ensure a good balance of sensitivity and specificity. Electronic searches were supplemented by manually searching the bibliographies of eligible clinical trials and previous systematic reviews.
Study Selection and Data Extraction
Two authors (H.H.L. and Y.Y.C.) independently screened the titles and abstracts of the papers identified by the initial search for relevance to this review. We retrieved the full text for any citation deemed potentially eligible at this stage. Two authors then separately assessed full articles using predetermined inclusion criteria to exclude irrelevant articles. Any disagreements regarding study inclusion were resolved by discussion. Data from the included studies were extracted by 2 authors to a Microsoft Excel spreadsheet (XP Professional; Microsoft Corp, Redmond, WA, USA). Conflicts in data extraction were resolved by consensus after referring back to the original article.
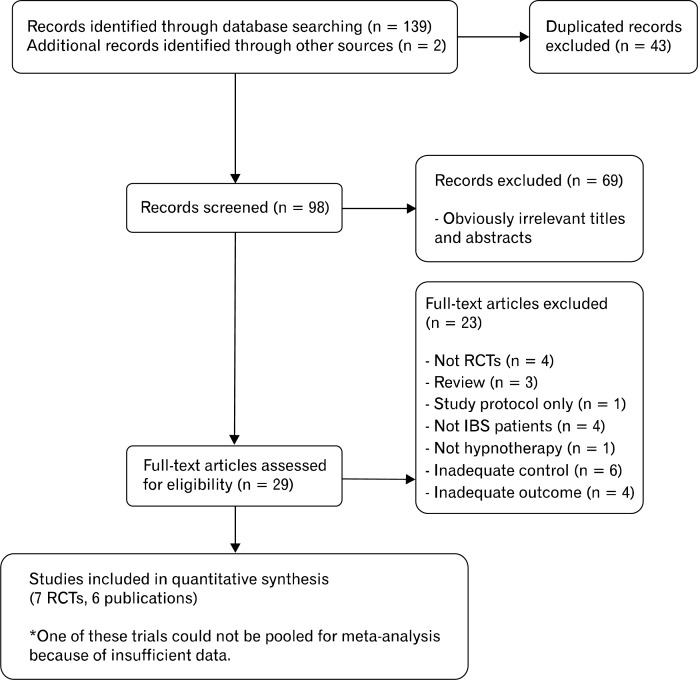
Searches of 4 of the electronic bibliographic databases initially identified 139 potentially relevant citations. Two additional studies were found by cross-referencing. Our search strategy identified 98 citations after removing duplicates, 30 of which were retrieved for full-text assessment, and a total of 7 RCTs ultimately fulfilled our inclusion criteria (Fig. 1).11,20–24 One study reported 2 RCTs being conducted on different settings in one publication.20 One of the studies that we initially excluded was published only in abstract form. As we were conducting our meta-analysis, advance online publication of this study was reported in February 2013, so we have included it in our review.24 Agreement between authors for trial eligibility was substantial (k statistic = 0.79).
Figure 1.
Flow diagram of studies identified in the systematic review. IBS, irritable bowel syndrome; RCT, randomized controlled trial.
Quality Assessment
Two authors independently assessed the methodological quality of the included trials using the risk of bias tool recommended by the Cochrane Collaboration.25 This included random sequence generation, allocation concealment, blinding of participants and personnel, blinding of outcome assessment, assessment of incomplete data outcome, selective reporting and other sources of bias. For each trial, the risk of bias was reported as “low risk,” “unclear risk” or “high risk.” Disagreement was resolved by discussion.
Data Analysis
All the assessed outcomes were continuous variables. Although the studies included in our review reported similar outcomes, various measurement instruments were applied to calculate the scores. The mean change in the outcome score was calculated and used to compare these outcomes by subtracting the baseline score from the score after treatment. The standard deviation (SD) is needed for use of the change score in a meta-analysis. One trial presented the standard deviation of the changes in their report.20 From these data, we calculated the correlation coefficient by using the following formula.
We also used the following formula to calculate the SD of the change by using the correlation coefficient in the studies that did not report this value.
To combine the different scales, we used the standardized mean difference (SMD) rather than the actual means because the SMD does not depend on the measurement scale. To evaluate the magnitude of the effect size calculated by SMD, Cohen’s categories were used with 0.0–0.2 = not a substantial effect size, > 0.2–0.5 = a small effect size, > 0.5–0.8 = a medium effect size, and > 0.8 = a large effect size.26
Meta-analysis was performed using the software Review Manager version 5.2.3 (RevMan for Windows 7; the Nordic Cochrane Center, Copenhagen, Denmark) provided by the Cochrane Collaboration. Meta-analysis was performed using a fixed-effects model and a random-effects model for each outcome, and the analyses were compared. A P-value < 0.05 was considered significant.
Statistical heterogeneity among studies was assessed using the χ2 test, defining a significant heterogeneity as a P-value < 0.1, and was quantified by measuring I2. An I2 value > 50% suggested significant statistical heterogeneity. The fixed-effects model of meta-analysis was used in the case of statistical homogeneity, whereas in the case of statistical heterogeneity, the random-effects model was applied. Analysis and reporting followed the Preferred Reporting Items for Systematic reviews and Meta-analyses (PRISMA) guidelines.27 Forest plots of SMDs for the assessed outcomes with 95% confidence intervals (CIs) and funnel plots were generated. The latter were assessed for evidence of asymmetry and therefore possible reporting bias or publication bias.
Results
Description of Included Studies
The characteristics of the included studies are shown in Table 1. A total of 374 patients (74 men and 300 women) were included in this meta-analysis: 191 patients were in the hypnotherapy group and 183 patients were in the control group. Gut-directed hypnotherapy (GDH) was applied to the patients as an intervention in all 7 trials. The frequency of this intervention varied from 5 to 12 sessions, and the duration of each session varied from 30 to 60 minutes. Three of the included trials used the Manchester protocol for GDH.20,24,28 Moser et al delivered GDH in group sessions.24 Four trials performed GDH with usual medical therapy or supportive talks and medical treatment.20,23,24 Various methods were used for the control groups. Four trials monitored symptoms only in the control group,20–23 and others provided supportive and medical therapy. All trials included as outcomes IBS-related gastrointestinal symptoms. QOL was assessed in 4 trials.20,23,24 No adverse events were reported in any trial.
Table 1.
Characteristics of Included Studie
| Author (yr) | Country (setting) | Population | Definition of IBS | Exclusion criteria | Age (range, yr) | Sex (M:F) | No. of patients (intervention: control) | Intervention | Control | Allowed other medication | Outcomes | Scale |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Whorwell et al11 (1984) | UK (university hospital) | Refractory IBS, at least 1 year | Abdominal pain, a disordered bowel habit, and abdominal distention (predated the Rome criteria) | Organic GI disease, psychiatric disorder | 24–53 | 4:26 | 15:15 | GDH: 7 sessions of 30 min+ autohypnosis | Placebo with supportive psychotherapy : 7 sessions of 30 min | NA | Abdominal pain Abdominal distension Bowel habit General wellbeing |
4-graded Likert scale (none [0] to severe [3]) 4-graded Likert scale (no improvement [0] to maximum improvement [3]) |
| Galovski et al21 (1998) | USA | Refractory IBS, at least 6 months | Rome I, diagnosed by physician or gastroenterologist | Psychiatric disorder, language barrier | 23–58 | 2:9 | 5:6 | GDH: 12 sessions of 30–60 min | Symptom monitoring | NA | CPSR | 5-graded Likert scale (symptom absent [0] to debilitating symptom [4]) |
| Palsson et al22 (2002) | USA | Refractory IBS, at least 1 year | Rome I | Abdominal surgery history, organic GI disease, psychotropic medication | Mean 39.1 | 9:15 | 15:9 | GDH: 7 sessions of 45 min | Symptom monitoring | NA | Abdominal pain Bloating Proportion of hard or loose stools Bowel movements per day |
5-graded Likert scale (none [0] to incapacitating [4]) 4-graded Likert scale (hard, firm, soft and watery) |
| Roberts et al23 (2006) | UK | Refractory IBS, at least 6 months | Diagnosed by general practitioner (criteria used IBS diagnosis not specified) | Atypical GI symptoms Aged over 65 years |
18–65 | 12:69 | 40:41 | GDH: 5 sessions of 30 min | Symptom monitoring | Usual medical therapy | IBS-specific QOL (8 dimensions: dysphoria, interference with activity, body image, health worry, food avoidance, social reaction, sexual function and relationships) Full symptom score (3 dimensions: pain, constipation and diarrhea) |
0–100 scale (increasing scores denoting more severe symptoms) |
| Lindfors et al20 (2012) study 1 | Sweden (university hospital) | Refractory IBS | Rome II | Organic GI disease, severe co-existing disease, psychotropic drugs or antidepressants | 21–68 | 19:71 | 45:45 | GDH (Manchester protocol): 12 sessions of 60 min+ autohypnosis | Dietary advice Information about relaxation training Education Nursing support by telephone |
Antidiarrheals, bulking agents, spasmolytics | GI-symptom questionnaire (2 domains: sensory symptoms score [pain, bloating and gas] and bowel habit score [loose stools, urgency, hard stools and incomplete evacuation]) IBS-QOL (9 dimensions: emotional functioning, mental health, sleep, energy, physical functioning, diet, social role, physical role and sexual relations) The HAD scale (14 items, with 7 items relating to anxiety and 7 items related to depression) |
7-graded Likert scale (none [1] to very severe [7]): total symptom severity score (7–49) 0–100 scale (100 representing the best possible QOL) 4-graded Likert scale (0–3) |
| Lindfors et al20 (2012) study 2 | Sweden (county hospital) | Refractory IBS | Rome II | Organic GI disease, severe co-existing disease, psychotropic drugs or antidepressants | 21–60 | 9:39 | 25:23 | GDH (Manchester protocol): 12 sessions of 60 min+ autohypnosis | Symptom monitoring | Antidiarrheals, bulking agents, spasmolytics | GSRS-IBS (5 domains: pain, bloating, constipation, diarrhea and satiety) SF-36 The HAD scale |
7-graded Likert scale (no discomfort [1] to very severe discomfort [7]) 0–100 scale (100 representing the best possible QOL) 4-graded Likert scale (0–3) |
| Moser et al24 (2013) | Austria (university hospital) | Refractory IBS | Rome III | Pregnancy, bowel surgery, mental retardation, language barrier, psychiatric disease, recent unstable dose of antidepressants | 18–70 | 19:71 | 46:44 | GDH (Manchester protocol): 10 sessions of 45 min+ autohypnosis + SMT | SMT: 10 sessions of 45 min | Spasmolytics, antidiarrheals | IBS impact scale (5 domains: fatigue, impact on daily activities, sleep disturbance, emotional distress and eating habits) IBS single symptoms (abdominal pain, diarrhea, constipation and flatulence) SF-36 The HAD scale |
7-graded Likert scale (decreases with increasing IBS symptom severity) 0–100 scale (increasing scores denoting more severe symptoms) 0–100 scale (100 representing the best possible QOL) 4-graded Likert scale (0–3) |
Risk of Bias
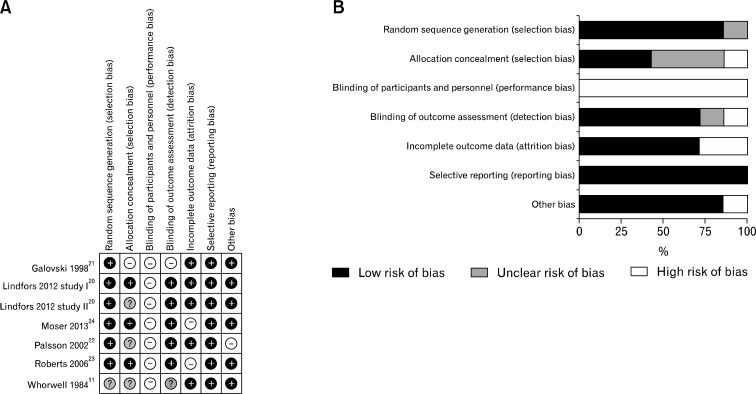
The quality of RCTs included in our review was assessed by the Cochrane risk of bias tool (Fig. 2). Selection bias was shown in one trial because its method was not optimal for ensuring adequate allocation concealment.21 Performance bias was high in all trials because it was not possible to blind participants and therapists in this type of intervention. Attrition bias was high in 2 trials.23,24 Other type of bias was high in one trial. Four trials used intention-to-treat analysis,11,20,24 and the others did not.
Figure 2.
Assessment of risk of bias in this meta-analysis. Risk of bias summary. (A) Summary of risk of bias for each trial assessed by Cochrane Collaboration’ tool, plus sign was for a judgment of Yes or low risk of bias, minus sign was for a judgment of No or high risk of bias, and question mark was for a judgment of Unclear, or uncertain risk of bias, which meant there was insufficient information to permit a judgment of Yes or No. Risk of bias graph. (B) Risk of bias graph about each risk of bias item presented as percentages across all included studies.
Effects
The data for 6 of the 7 included RCTs were pooled for analysis.20–24 The data of one study were not available for analysis after we tried unsuccessfully to correspond with the author.11
The outcomes were evaluated at 3 months for short-term effects. In the cases of short-term effects, although some studies reported their results at 2 or 4 months, we regarded them as the same period as 3 months. The long-term outcomes were measured at 1 year.
Abdominal pain
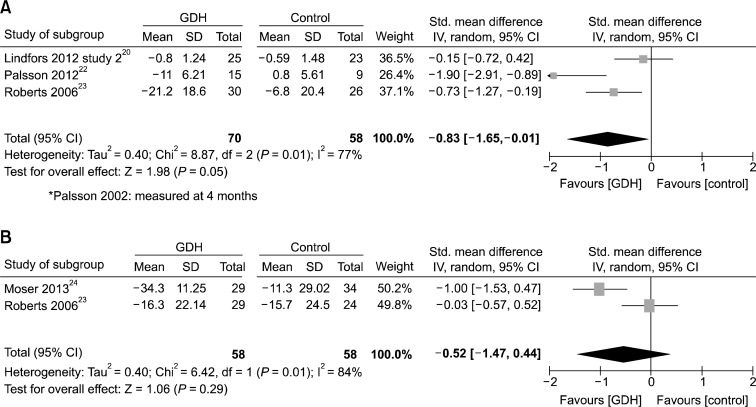
Four RCTs reported an abdominal pain change score.20, 22–24 Three reported it at 3 months,20,22,23 which showed a significant difference in favor of the GDH group (SMD −0.83; 95% CI, −1.65 to −0.01; P = 0.050) (Fig. 3A). The random-effects model was used because there was considerable heterogeneity (I2 = 77%, P = 0.010). Based on Cohen’s categories, the effect size of the abdominal pain change score at 3 months was large. The abdominal pain change score at 1 year was reported by 2 of the 4 RCTs.23,24 Meta-analysis using the fixed-effects model showed a significant difference in favor of the GDH group (SMD, −0.53; 95% CI, −0.90 to −0.15; P = 0.006). However, there was considerable heterogeneity (I2 = 84%, P = 0.010). When the random-effects model was used, there was no significant difference (SMD, −0.52; 95% CI, −1.47 to 0.44; P = 0.290) (Fig. 3B).
Figure 3.
Forest plots of abdominal pain change score. (A) Meta-analysis of 3 months results. (B) Meta-analysis of 1-year results. GDH, gut-directed hypnotherapy; Std., standardized.
Constipation and diarrhea
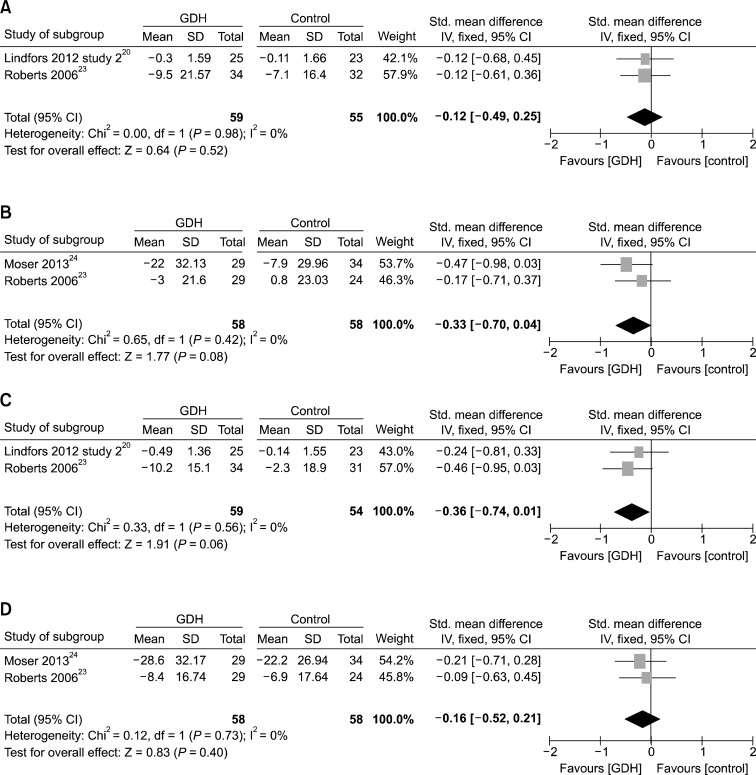
The constipation change score was reported by 3 RCTs.20,23,24 Two of these 3 trials reported this score at 3 months,20,23 and this value did not change significantly (SMD, −0.12; 95% CI, −0.49 to 0.25; P = 0.520) (Fig. 4A). The constipation change score at 1 year was reported by 2 of the 3 RCTs.23,24 Meta-analysis showed no significant difference (SMD, −0.33; 95% CI, −0.70 to 0.04; P = 0.080) (Fig. 4B). Meta-analysis of the diarrhea change score at 3 months was reported by 2 RCTs,20,23 and there was no significant difference (SMD, −0.36; 95% CI, −0.74 to 0.01; P = 0.060) (Fig. 4C). The diarrhea change score at 1 year was reported by 2 RCTs,23,24 and the meta-analysis showed no significant difference (SMD, −0.16; 95% CI, −0.52 to 0.21; P = 0.400) (Fig. 4D).
Figure 4.
Forest plots of constipation change score at 3 months (A) and 1 year (B), diarrhea change score at 3 months (C) and 1 year (D). GDH, gut-directed hypnotherapy; Std., standardized.
Overall gastrointestinal symptoms
Four trials attempted to measure the overall gastrointestinal symptom score in IBS patients (Table 2). Different studies used different assessment tools, and these studies were not eligible to be combined for the meta-analysis. Three trials showed that the hypnotherapy group had greater improvement in the overall gastrointestinal symptom score at 3 months compared with the control group, whereas the difference in the symptom score did not differ significantly between the 2 groups in the other trial. Only one trial reported the result at 1 year, and there was no significant difference between the hypnotherapy group and control group.23 The studies by Lindfors et al20 (studies 1 and 2 in Table 2) did not report the overall gastrointestinal symptom scores at 12 months in the control group because it was considered unethical to not allow the controls to receive hypnotherapy available in their clinical settings. Thus, we could not compare the change in overall gastrointestinal symptom scores at 12 months between the hypnotherapy and control groups.
Table 2.
Change in Overall Gastrointestinal Symptom Score
| Author (yr) | Outcome measurement | 3 months | P-value | 12 months | P-value | ||
|---|---|---|---|---|---|---|---|
|
|
|
||||||
| Intervention (SD) | Control (SD) | Intervention (SD) | Control (SD) | ||||
| Galovski et al21 (1998) | CPSRa | −0.55 (0.53) | 0.32 (0.49) | 0.00047 | NA | NA | NA |
| Roberts et al23 (2006) | Full symptom score | −13.00 (10.50) | −4.5 (13.90) | 0.008 | −9.10 (14.00) | −6.40 (14.70) | 0.440 |
| Lindfors et al20 (2012) study 1 | GI-symptom questionnaire | −4.50 (8.60) | −0.80 (7.30) | < 0.05 | NA | NA | NA |
| Lindfors et al20 (2012) study 2 | GSRS-IBS | −0.43 (0.90) | −0.10 (1.00) | 0.220 | NA | NA | NA |
CPSR was measured at right after end of treatment.
SD, standard deviation; CPSR, composite primary symptom reduction; NA, not allowed; GSRS, gastrointestinal symptom rating scale; IBS, irritable bowel syndrome.
Quality of life
Four RCTs measured QOL.20,23,24 Two used a generic health-related QOL measure (short-form 36 health survey [SF-36]).20,24 Study 2 of Lindfors et al20 showed no significant differences in SF-36 scores between the GDH group and control group. Moser et al24 reported a significant improvement in QOL scores at 3 months and 1 year in 4 dimensions (role physical, general health, vitality and social functioning) and at 1 year in 3 more dimensions (physical functioning, bodily pain and mental health) compared with the control groups.
Three trials used disease-specific QOL instruments.20,23,24 Roberts et al used an IBS-specific QOL measure13 and found no significant difference in QOL scores between the hypnotherapy and control groups at 3 months and 1 year.23 Study 1 of Lindfors et al20 used an IBS-specific QOL measure29 and reported a significant improvement at 3 months in the GDH group in the dimensions of mental health, sleep, energy and social role versus baseline.20 This improvement was maintained significantly at 1 year, and additional improvement in emotional functioning was identified. However, there was no significant difference in the changes in QOL at 3 months between the GDH group and control group. Moser et al24 used an IBS-impact scale, a disease-specific documentation of the impact of IBS on patients’ lives.30 In this study, the hypnotherapy group showed a significant improvement in IBS-impact scale scores at 3 months and 1 year compared with the control group.
Discussion
We reviewed 7 RCTs with a total of 374 patients that compared hypnotherapy with various control treatments to examine whether hypnotherapy as treatment for IBS would have significant beneficial effects on gastrointestinal symptoms and QOL. This review is the first study to conduct a meta-analysis of the efficacy of hypnotherapy in IBS patients. This meta-analysis revealed that hypnotherapy significantly improved abdominal pain, at least at short-term follow-up. Hypnotherapy also provided benefit for overall gastrointestinal symptoms. However, evidence for the long-term efficacy of hypnotherapy is lacking because of an insufficient number of studies.
Our search strategy was comprehensive in that we used 4 databases, distinct inclusion criteria and the Cochrane risk of bias tool for each trial. The previous reviews included insufficient evidences because of the small number of RCTs and methodological flaws.17,18 Our study provides more reliable evidence by including 3 recent well-designed RCTs.
Randomization is especially important in trials of fluctuating diseases such as IBS, since recruitment of patients to a trial usually occurs during a period of increased symptomatology.17 The current study included only RCTs whose aim was to establish the effectiveness of hypnotherapy. The calculation of a summary measure of effect had been difficult because of heterogeneity in the outcome measures in the previous reviews. Likert scales of different grades were used to obtain scores for abdominal pain and symptoms of defecatory dysfunction in individual trials. In this meta-analysis, we used the SMD as a summary statistic for studies that assessed the same outcome but measured it with different methods.
In this meta-analysis, the potential benefits of hypnotherapy in treating constipation and diarrhea were not verified because of insufficient power and internal validity. In addition, patient-reported ratings of changes in bowel habits were not able to delineate adequately whether any benefits were achieved in all of the important subconcepts (i.e., urgency, stool consistency and stool frequency). Further trials should include a predefined definition and grade for bowel habits such as the British stool scale to evaluate benefits precisely.31
GDH involves hypnotic induction by using a variety of techniques, including progressive relaxation, followed by creating imagery related to symptom control and normalization of gut function. The mechanism through which hypnotherapy improves abdominal pain in IBS patients is not well understood. Hypnotic reduction of somatic pain is thought to reduce the activation of certain areas of the brain, which appears to be exaggerated in IBS.32 It is also assumed that hypnotherapy normalizes visceral sensation, decreases colonic phasic contractions, and reverses negative thoughts of IBS patients about their condition.33–35
Although 3 more RCTs were added in this meta-analysis after the last systematic review, the number of included studies was too small to draw firm conclusions. The control groups varied somewhat between studies, from no treatment to supportive therapy; however, separate comparisons of the different control treatments were not conducted because of the limited number of included trials. Difficulties in blinding because of the nature of the intervention also contribute to the potential for performance bias.
In conclusion, hypnotherapy may be a useful and safe therapeutic option for refractory IBS in short term. More high-quality RCTs are needed for evaluating the long-term efficacy of hypnotherapy. All of the included studies targeted refractory IBS; therefore, the beneficial effects of hypnotherapy cannot be generalized to all IBS patients.
Footnotes
Financial support: None.
References
- 1.Thompson WG, Longstreth GF, Drossman DA, Heaton KW, Irvine EJ, Muller-Lissner SA. Functional bowel disorders and functional abdominal pain. Gut. 1999;45(suppl 2):II43–II47. doi: 10.1136/gut.45.2008.ii43. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Karabulut GS, Beşer OF, Erginöz E, Kutlu T, Cokuğraş FÇ, Erkan T. The Incidence of Irritable Bowel Syndrome in Children Using the Rome III Criteria and the Effect of Trimebutine Treatment. J Neurogastroenterol Motil. 2013;19:90–93. doi: 10.5056/jnm.2013.19.1.90. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Agrawal A, Whorwell PJ. Irritable bowel syndrome: diagnosis and management. BMJ. 2006;332:280–283. doi: 10.1136/bmj.332.7536.280. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Whitehead WE, Burnett CK, Cook EW, 3rd, Taub E. Impact of irritable bowel syndrome on quality of life. Dig Dis Sci. 1996;41:2248–2253. doi: 10.1007/BF02071408. [DOI] [PubMed] [Google Scholar]
- 5.Gralnek IM, Hays RD, Kilbourne A, Naliboff B, Mayer EA. The impact of irritable bowel syndrome on health-related quality of life. Gastroenterology. 2000;119:654–660. doi: 10.1053/gast.2000.16484. [DOI] [PubMed] [Google Scholar]
- 6.Quartero AO, Meineche-Schmidt V, Muris J, Rubin G, de Wit N. Bulking agents, antispasmodic and antidepressant medication for the treatment of irritable bowel syndrome. Cochrane Database Syst Rev. 2005;(2):CD003460. doi: 10.1002/14651858.CD003460.pub2. [DOI] [PubMed] [Google Scholar]
- 7.Francis CY, Whorwell PJ. Bran and irritable bowel syndrome: time for reappraisal. Lancet. 1994;344:39–40. doi: 10.1016/s0140-6736(94)91055-3. [DOI] [PubMed] [Google Scholar]
- 8.Poynard T, Naveau S, Mory B, Chaput JC. Meta-analysis of smooth muscle relaxants in the treatment of irritable bowel syndrome. Aliment Pharmacol Ther. 1994;8:499–510. doi: 10.1111/j.1365-2036.1994.tb00322.x. [DOI] [PubMed] [Google Scholar]
- 9.Drossman DA, Camilleri M, Mayer EA, Whitehead WE. AGA technical review on irritable bowel syndrome. Gastroenterology. 2002;123:2108–2131. doi: 10.1053/gast.2002.37095. [DOI] [PubMed] [Google Scholar]
- 10.Lackner JM, Mesmer C, Morley S, Dowzer C, Hamilton S. Psychological treatments for irritable bowel syndrome: a systematic review and meta-analysis. J Consult Clin Psychol. 2004;72:1100–1113. doi: 10.1037/0022-006X.72.6.1100. [DOI] [PubMed] [Google Scholar]
- 11.Whorwell PJ, Prior A, Faragher EB. Controlled trial of hypno-therapy in the treatment of severe refractory irritable-bowel syndrome. Lancet. 1984;2:1232–1234. doi: 10.1016/s0140-6736(84)92793-4. [DOI] [PubMed] [Google Scholar]
- 12.Whorwell PJ, Prior A, Colgan SM. Hypnotherapy in severe irritable bowel syndrome: further experience. Gut. 1987;28:423–425. doi: 10.1136/gut.28.4.423. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Harvey RF, Hinton RA, Gunary RM, Barry RE. Individual and group hypnotherapy in treatment of refractory irritable bowel syndrome. Lancet. 1989;1:424–425. doi: 10.1016/s0140-6736(89)90013-5. [DOI] [PubMed] [Google Scholar]
- 14.Houghton LA, Heyman DJ, Whorwell PJ. Symptomatology, quality of life and economic features of irritable bowel syndrome - the effect of hypnotherapy. Aliment Pharmacol Ther. 1996;10:91–95. doi: 10.1111/j.1365-2036.1996.tb00181.x. [DOI] [PubMed] [Google Scholar]
- 15.Gonsalkorale WM, Houghton LA, Whorwell PJ. Hypnotherapy in irritable bowel syndrome: a large-scale audit of a clinical service with examination of factors influencing responsiveness. Am J Gastroenterol. 2002;97:954–961. doi: 10.1111/j.1572-0241.2002.05615.x. [DOI] [PubMed] [Google Scholar]
- 16.Gonsalkorale WM, Miller V, Afzal A, Whorwell PJ. Long term benefits of hypnotherapy for irritable bowel syndrome. Gut. 2003;52:1623–1629. doi: 10.1136/gut.52.11.1623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Wilson S, Maddison T, Roberts L, Greenfield S, Singh S, Birmingham IBS Research Group Systematic review: the effectiveness of hypnotherapy in the management of irritable bowel syndrome. Aliment Pharmacol Ther. 2006;24:769–780. doi: 10.1111/j.1365-2036.2006.03028.x. [DOI] [PubMed] [Google Scholar]
- 18.Webb AN, Kukuruzovic RH, Catto-Smith AG, Sawyer SM. Hypnotherapy for treatment of irritable bowel syndrome. Cochrane Database Syst Rev. 2007;(4):CD005110. doi: 10.1002/14651858.CD005110.pub2. [DOI] [PubMed] [Google Scholar]
- 19.National Collaborating Center for Nursing and Supportive Care (UK) Irritable bowel syndrome in adults: diagnosis and management of irritable bowel syndrome in primary care. London: Royal College of Nursing (UK); 2008. [PubMed] [Google Scholar]
- 20.Lindfors P, Unge P, Arvidsson P, et al. Effects of gut-directed hypnotherapy on IBS in different clinical settings-results from two randomized, controlled trials. Am J Gastroenterol. 2012;107:276–285. doi: 10.1038/ajg.2011.340. [DOI] [PubMed] [Google Scholar]
- 21.Galovski TE, Blanchard EB. The treatment of irritable bowel syndrome with hypnotherapy. Appl Psychophysiol Biofeedback. 1998;23:219–232. doi: 10.1023/a:1022209631047. [DOI] [PubMed] [Google Scholar]
- 22.Palsson OS, Turner MJ, Johnson DA, Burnett CK, Whitehead WE. Hypnosis treatment for severe irritable bowel syndrome: investigation of mechanism and effects on symptoms. Dig Dis Sci. 2002;47:2605–2614. doi: 10.1023/a:1020545017390. [DOI] [PubMed] [Google Scholar]
- 23.Roberts L, Wilson S, Singh S, Roalfe A, Greenfield S. Gut-directed hypnotherapy for irritable bowel syndrome: piloting a primary care-based randomised controlled trial. Br J Gen Pract. 2006;56:115–121. [PMC free article] [PubMed] [Google Scholar]
- 24.Moser G, Trägner S, Gajowniczek EE, et al. Long-term success of GUT-directed group hypnosis for patients with refractory irritable bowel syndrome: a randomized controlled trial. Am J Gastroenterol. 2013;108:602–609. doi: 10.1038/ajg.2013.19. [DOI] [PubMed] [Google Scholar]
- 25.Higgins JPT, Green S. Cochrane handbook for systematic reviews of interventions: version 5.1.0. 2011 Available from URL: http://www.cochrane-handbook.org (accessed 26 January, 2014.
- 26.Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed. Hillsdale (NJ): Lawrence Erlbaum Associates; 1988. [Google Scholar]
- 27.Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–269. doi: 10.7326/0003-4819-151-4-200908180-00135. [DOI] [PubMed] [Google Scholar]
- 28.Vlieger AM, Menko-Frankenhuis C, Wolfkamp SC, Tromp E, Benninga MA. Hypnotherapy for children with functional abdominal pain or irritable bowel syndrome: a randomized controlled trial. Gastroenterology. 2007;133:1430–1436. doi: 10.1053/j.gastro.2007.08.072. [DOI] [PubMed] [Google Scholar]
- 29.Hahn BA, Kirchdoerfer LJ, Fullerton S, Mayer E. Evaluation of a new quality of life questionnaire for patients with irritable bowel syndrome. Aliment Pharmacol Ther. 1997;11:547–552. doi: 10.1046/j.1365-2036.1997.00168.x. [DOI] [PubMed] [Google Scholar]
- 30.Longstreth GF, Bolus R, Naliboff B, et al. Impact of irritable bowel syndrome on patients’ lives: development and psychometric documentation of a disease-specific measure for use in clinical trials. Eur J Gastroenterol Hepatol. 2005;17:411–420. doi: 10.1097/00042737-200504000-00004. [DOI] [PubMed] [Google Scholar]
- 31.Lewis SJ, Heaton KW. Stool form scale as a useful guide to intestinal transit time. Scand J Gastroenterol. 1997;32:920–924. doi: 10.3109/00365529709011203. [DOI] [PubMed] [Google Scholar]
- 32.Rainville P, Duncan GH, Price DD, Carrier B, Bushnell MC. Pain affect encoded in human anterior cingulate but not somatosensory cortex. Science. 1997;277:968–971. doi: 10.1126/science.277.5328.968. [DOI] [PubMed] [Google Scholar]
- 33.Whorwell PJ, Houghton LA, Taylor EE, Maxton DG. Physiological effects of emotion: assessment via hypnosis. Lancet. 1992;340:69–72. doi: 10.1016/0140-6736(92)90394-i. [DOI] [PubMed] [Google Scholar]
- 34.Lea R, Houghton LA, Calvert EL, et al. Gut-focused hypnotherapy normalizes disordered rectal sensitivity in patients with irritable bowel syndrome. Aliment Pharmacol Ther. 2003;17:635–642. doi: 10.1046/j.1365-2036.2003.01486.x. [DOI] [PubMed] [Google Scholar]
- 35.Gonsalkorale WM, Toner BB, Whorwell PJ. Cognitive change in patients undergoing hypnotherapy for irritable bowel syndrome. J Psychosom Res. 2004;56:271–278. doi: 10.1016/S0022-3999(03)00076-X. [DOI] [PubMed] [Google Scholar]