Abstract
Background: The barriers to HIV testing and counselling that migrants encounter can jeopardize proactive HIV testing that relies on the fact that HIV testing must be linked to care. We analyse available evidence on HIV testing and counselling strategies targeting migrants and ethnic minorities in high-income countries. Methods: Systematic literature review of the five main databases of articles in English from Europe, North America and Australia between 2005 and 2009. Results: Of 1034 abstracts, 37 articles were selected. Migrants, mainly from HIV-endemic countries, are at risk of HIV infection and its consequences. The HIV prevalence among migrants is higher than the general population’s, and migrants have higher frequency of delayed HIV diagnosis. For migrants from countries with low HIV prevalence and for ethnic minorities, socio-economic vulnerability puts them at risk of acquiring HIV. Migrants have specific legal and administrative impediments to accessing HIV testing—in some countries, undocumented migrants are not entitled to health care—as well as cultural and linguistic barriers, racism and xenophobia. Migrants and ethnic minorities fear stigma from their communities, yet community acceptance is key for well-being. Conclusions: Migrants and ethnic minorities should be offered HIV testing, but the barriers highlighted in this review may deter programs from achieving the final goal, which is linking migrants and ethnic minorities to HIV clinical care under the public health perspective.
Introduction
Migrant populations, largely from sub-Saharan Africa (SSA), represent a considerable proportion of HIV infections in Europe and are heavily affected by late HIV diagnoses.1,2 A similar situation occurs in ethnic minorities in the USA.3 In 2006, the US Centers for Disease Control and Prevention published their revised recommendations for HIV testing, which aimed for routine voluntary HIV screening for all persons aged 13–64 years in health-care settings independently of HIV risk assessment unless the local HIV prevalence falls below 0.1%. Under the new recommendations, neither pretest counselling nor separate signed consent forms are required.3 Since then, other recommendations have been issued to expand HIV testing and normalize testing.4–8 Although increasing HIV testing at population level is a challenge, doing so in migrants and ethnic minorities may pose additional difficulties. Whereas some barriers to HIV testing are shared by other groups, others, such as administrative,9–12 legal,1,13,14 language14–18 and cultural barriers,9,11,14,16,18–20 are not. Some European Union (EU) countries do not provide HIV care for people of uncertain legal status. Therefore, the lack of any medical benefit for individuals found to have HIV combined with the fear of deportation may hinder public health initiatives promoting testing in migrants.21
The different epidemiological patterns of HIV infection in migrants and ethnic minorities in Europe and the migrants’ unique barriers to HIV testing and care may compromise proactive HIV testing approaches that rely on the statement that HIV testing is linked to care.4,5,22 Given that the translation of policies into practice requires deep knowledge of target populations, we have conducted a systematic review of the literature on HIV testing and counselling targeting migrants living in high-income countries.
Methods
We performed a literature search in PubMed, EMBASE, CRD York database, Cochrane and Web of Knowledge of articles published in English between 2005 and 2009 in Europe, North America and Australia. To be eligible, articles had to include at least one keyword from: (i) ethnic groups, minority groups, transients and immigrants, refugees; (ii) mass screening, diagnosis, AIDS Serodiagnosis, public policy, prevention and control, Centers for Disease Control and Prevention (USA), counselling; and (iii) Acquired immunodeficiency syndrome, HIV, HIV Infections.
After piloting in 14 articles, the final data collection form included information on year and country of the study, ‘migrants’ and ‘ethnic minorities’ definition, setting, study design and sample size. Information on gender, criminalization of HIV transmission and legal consequences of HIV disclosure in migrants with uncertain status was also collected.
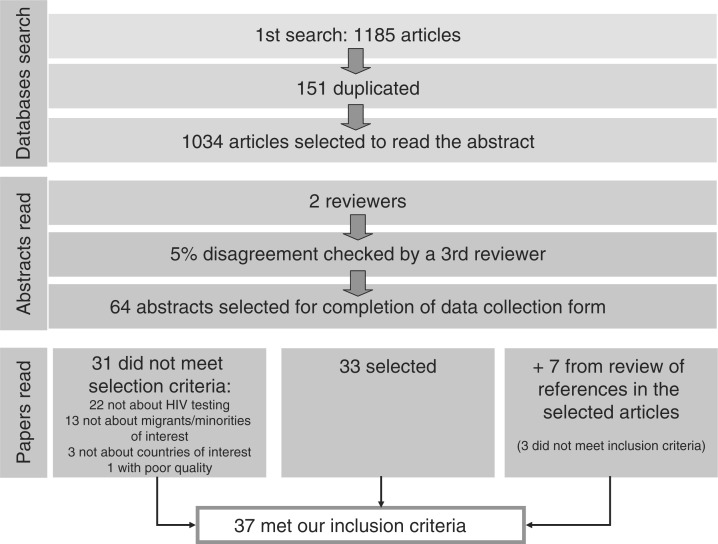
As described in figure 1, 1185 articles were identified; 151 were duplicates. The remaining 1034 abstracts were read, and only abstracts not referring to migrants or ethnic minorities in Europe, USA, Canada and Australia and HIV testing and/or counselling were eliminated at this stage; 970 articles were discarded and 64 selected for full review.
Figure 1.
Flow diagram
Teams of two people read the 64 articles and applied eligibility criteria; 31 articles were rejected because they did not deal with HIV testing (n = 22), they did not deal with migrants or ethnic minorities (n = 13), countries did not meet criteria (n = 3) or they were of poor quality (n = 1). The review of these 64 articles identified seven new manuscripts, from the manuscripts’ references, of which four met inclusion criteria. Final analyses were based on 37 articles.
Results
Most studies were conducted in Anglo-Saxon countries—12 in USA, 4 in Canada, 13 in the UK—and 8 from other European countries. None of the articles was from Australia. The majority (n = 35) was conducted in one country, most (n = 20) with local scope. Studies were conducted in health (n = 15) and community settings (n = 11) (supplementary table). Overall, 25 studies (68%) used quantitative methodology, two combined quantitative and qualitative methodology, six used qualitative methodology and four were literature reviews. Operational definitions for ‘migrant’, ‘race’ or ‘ethnicity’ (understood as concept defining racial/ethnic minorities) were present in all articles; more than one definition was often present; 14 defined migrants based on country of origin, 13 on country of birth and 3 on nationality. With regards to race and ethnicity, eight studies (mostly from USA) defined subjects on self-reported ethnicity and nine on documented ethnicity (n = 7), ethnic origin (n = 1) and race (n = 1).
Migrant populations studied were largely sub-Saharan Africans,10,11,23–26 Latin Americans23 and South Asians20 in EU countries, and Hispanics or Latinos,12,15,17,27–29 Africans16 and Southeast Asians14 in the USA. Three articles from Canada studied asylum seekers, visa applicants and refugees9,30,31, and one from the USA studied adopted foreign children.19 The racial/ethnic minorities were largely ‘Black communities’ in the UK.32–35 One study in the USA refers to generic ‘racial minorities’.36
The 37 studies addressed heterogeneous aspects of HIV testing and counselling in migrants and ethnic minorities, which could be grouped as follows: (i) prevalence and risk factors for HIV infection; (ii) barriers to HIV testing; (iii) HIV testing uptake; (iv) late HIV diagnosis; and (v) interventions to encourage HIV testing.
Prevalence and risk factors for HIV infection in migrants and ethnic minorities
Although our aim was not to systematically review HIV prevalence and risk factors in migrants and ethnic minorities, this topic came up frequently. Although many articles include general references to this issue, studies that report data about differential prevalence of HIV have been included in table 1. The groups identified as having high HIV prevalence were sub-Saharan Africans in Europe, black Africans and black Caribbeans in London and sub-Saharan Africans, Latinos and blacks in USA.
Table 1.
HIV prevalence in migrants and ethnic minorities
| Authors | Country/Date | Sample size | Target population | HIV prevalence/incidence | Design |
|---|---|---|---|---|---|
| Monge-Maillo B et al | Spain (2009) | 2198 | Immigrants referred to the Tropical Medicine Unit of Ramón y Cajal Hospital (Madrid) over a 20-year period | Incidence: total population: 97 (4.4%); sub-Saharan Africans: 82 (5.2%); Latin Americans: 15 (2.4%) | Cross-sectional study |
| Forbes KM et al. | UK (2008) | 30 | Patients attending an outreach clinic for those <25 years between June and October 2007, in an area where black and minority ethnic groups comprise the majority of the local population | There were no cases of HIV | A retrospective case-notes review was undertaken of those attending community-based sexual health services. (Note: not clear if all respondents were from minorities) |
| Zencovich M et al. | Canada (2006) | 634 958 | All applicants in Canada, 15 years of age and older, for permanent residency between 2002 and 2003 | Incidence: 932 (0.146%). Prevalence of 3% among applicants from six African countries (Zimbabwe, Burundi, Rwanda, Uganda, Zambia and Chad) | National data collected by Public Health Agency of Canada |
| Schmid J et al. | Denmark (2005) | Does not know (Unknown) (DK) | Children <16 years in Denmark in 2003 | Incidence: 89 (5.77 per 100 000 children). Of these 89 newly diagnosed: 48% born in Denmark 43% in Africa and 9% in other places | Data from the national surveillance system and HIV-infected children from the Danish Paediatric HIV Cohort Study |
| MacPherson DW et al. | Canada (2006) | 256 970 | Residency applicants <15 years of age between 2002 and 2005 | 36 (0.014%), most of them from Africa (89%) | Data from the Canadian immigration medical examination register |
| Perez-Molina JA et al. | Spain (2009) | 1609 | Immigrants referred to the Tropical Medicine Unit of Ramón y Cajal Hospital (Madrid) during 1997–2006 | 77 (4.8%). By geographic groups: sub-Saharan Africans (5.6%); South-Central Americans (3.2%) | Non-interventional retrospective medical chart review |
| Dougan, S et al. | UK (2005) | 1040 | Men who have sex with men aged 16–44 years in England and Wales in 2002 | Prevalence: 7.4% black and minority ethnic MSM; 3.2% white MSM | Cross-sectional study with the data from the Survey of Prevalent HIV Infections Diagnosed that estimates the number of individuals living with diagnosed HIV infection in England and Wales (E&W) since 1995 |
Epidemiological patterns in countries of origin, together with clinical presentations in countries of destination, led some authors to conclude most HIV infections in migrants are imported. This approach is largely applied to migrants from SSA in Europe (Denmark,37 France,38 Spain18,23 and UK25,32,34) and Canada.9,30,31 Other studies consider some migrants may have acquired HIV in countries of destination because of unfavourable environment to fostering preventive behaviours.11,39,40 Some migrants are described as having high-risk behaviours: multiple sexual partners, low and inconsistent condom use, high alcohol consumption and drug use.17,27–29
Migrant women and ethnic minority men who have sex with men (MSM) are considered especially vulnerable; female migrants suffer disproportionate burden of HIV infection derived from difficulties negotiating condom use28 and sexual exploitation.31 The invisibility of ethnic minority MSM, who go unnoticed by the stigma of being MSM that would involve their country or ethnic group of origin, is thought to be key to their vulnerability to HIV infection; they have high HIV prevalence, unsafe sex39 and high prevalence of late HIV diagnosis.14,35
Barriers to HIV testing in migrants and ethnic minorities
Barriers to HIV testing exist at the structural, health-care provider, health-care user and community levels.
Structural barriers to HIV testing relate to poor living conditions, legal and administrative status and discrimination in countries of destination. High levels of unemployment and poverty in migrants and ethnic minorities, low social status and inequalities are mentioned as barriers to HIV testing and care.10,11,18–20,24 Legal status, which ranks among the highest priorities, and concerns about implications of testing positive are the main barriers in studies from Canada, USA, Spain and the UK. According to these studies, in contexts where an HIV diagnosis may adversely affect visa or residence application or where there is a fear of deportation, migrants are reluctant to be tested.10,11,13 Lack of entitlement to health care for undocumented immigrants is another barrier, largely but not exclusively, mentioned in the USA.13,14,35 Lack of clarity among health-care providers on migrants’ rights to health care is highlighted.24 Regarding stigma and discrimination, African people tested for HIV in London in the 1990s were twice as likely as whites to be concerned about being discriminated against.10 Structural racism is also mentioned by Fakoya et al.,24 who drew attention to the disproportionate number of sub-Saharan Africans prosecuted for allegedly transmitting HIV infection in the UK.
Within health-care structures, communication, language problems and lack of cultural sensitivity and underinvestment in culturally competent services lead to misconceptions about migrants and minority groups by health-care providers.14–18,20 Some migrants and ethnic minorities prefer to visit medical practitioners from their own community.19 Whereas some communities are described as having good knowledge about where to go for HIV testing, for example, sub-Saharan Africans in the UK,11 other studies identify poor knowledge among migrant and ethnic minorities regarding where to get tested for HIV anonymously and free of charge.9–12 Other barriers at health-care user level include the low-priority migrants assigned to health care11,13 and their low perception of HIV risk10,12,14,35,41. Migrants give priority to basic needs, but knowledge of their HIV status ranks low.13 Low HIV risk perception at individual level is mentioned, even in people with community risk awareness.10,12,14,35,41 Researchers note there is often a gap between risk perception and individual risk behaviours14; some studies describe low risk perception among those who test HIV positive.10,11,41
At the community level, cultural and gender norms may dissuade heterosexual men and women and MSM from seeking HIV testing. Loss of status and community support and social isolation after confidentiality gaps are among the main reasons given for not testing.9–13,16,24,26,27,34,41,42 This is a particular concern for individuals who need to bring a relative or friend to help with translation.19 Olshefsky et al.27 report ‘machismo’ as a barrier among Latino men; Foley16 reports that women from SSA have difficulty seeking HIV testing or treatment without partners’ approval and economic support.
HIV testing uptake in migrants and ethnic minorities
Several studies describe an HIV testing uptake in migrants and ethnic minorities to range from 21% to 73% in the USA and from 23% to 64% in Europe12,14,20,29,43 (table 2). Overall, a higher proportion of ethnic minority and migrant women have been tested for HIV compared with men; this is partially owing to women’s acceptance of routine HIV screening during antenatal care.29,33,42,44 However, beyond this, several studies support a gender difference in HIV testing uptake, with migrant men being not only less exposed to HIV testing but also less willing to be tested.24
Table 2.
Uptake of HIV test in migrants and ethnic minorities
| Authors | Country/Date | Sample size | Target population | Test prevalence/test acceptance prevalence | Design |
|---|---|---|---|---|---|
| Forbes KM et al. | UK (2008) | 117 | Outreach clinic for those <25 years in an area where black and minority ethnic groups comprise the majority of the local population | 23% ever tested | A retrospective case-notes review was undertaken of those attending community-based sexual health services. (Note: not clear whether all respondents were from minorities) |
| Conaty SJ et al. | UK (2005) | 443 | Sub-Saharan women in antenatal care | 86% accepted an HIV test | Cross-sectional study. HIV test acceptance. (Note: prevalence calculated by our research team based on presented article data) |
| Fernandez MI et al. | USA (2005) | 244 | Hispanic migrant/seasonal farm workers in southern Miami-Dade County, Florida | 21% (51/244) had been tested for HIV; 39% (94/244) declared they would accept on the day of the interview; 69% (134/193 never tested) declared they would accept if recommended by a provider | Cross-sectional study: questions about HIV test performance and intention to test |
| Sadler KE et al. | UK (2006) | 114 | Black Africans (>16 years old) living in London | 82% (93/114) accepted HIV testing in the survey | Cross-sectional study with offer of HIV test |
| Dowling T et al | USA (2007) | 627 | Participants at black gay, Hispanic gay or gay pride events | 24% (133) of those with unknown or negative HIV status (543) accepted HIV testing | Cross-sectional study with offer of HIV test. (Note: not clear if all respondents were from ethnic minorities. Of all persons willing to be tested, not all were finally tested for several reasons, mainly resource limitations) |
| Ostermann J et al. | USA (2007) | 146 868 | Adult participants in the survey aged 18–64 years | Tested in past 12 months (by ethnicity): white non-Hispanic, 8.1%; black non-Hispanic, 19.0%; Hispanic, 11.7%; Other, 9.6%. Plan to test in next 12 months: white non-Hispanic, 5.2%; black non-Hispanic, 19.8%; Hispanic, 12.7%; Other, 7.1% | Cross-sectional analysis of data from 146 868 participants aged 18–64 years in the 2000–05 National Health Interview Surveys, HIV test in the past |
| Tariq S et al. | UK (2007) | 458 | Cases were defined as the first 125 new Genito-Urinary (GU) clinic attendees who self-identified as South Asian. Controls were defined as subsequent new presentations self-identified as non-South Asian | Ever tested: cases: 60% (148/229); controls: 64% (154/229) | A retrospective case–control study was performed at a GU Clinic in London: HIV test in the past |
| Huang ZJ et al. | USA (2008) | 604 | Self-identified as Cambodian, Laotian or Vietnamese; >18 yearsold and residents in Washington, DC | Ever tested: total sample, 31% (186/604); Laotians, 22% (44/196); Vietnamese, 37% (72/197); Cambodians, 38% (79/211) | Cross-sectional study. Have had an HIV test |
| Southgate J et al. | UK (2008) | 1586 | Pregnant women from ethnic minority groups | Prevalence ratio of HIV test acceptance: white, 91% (1094/1214); black African, 92% (145/158); Asian, 90% (138/153); Chinese, 80% (4/5) | Cross-sectional study. Antenatal HIV screening routinely proposed |
| López Quintero C et al. | USA (2005) | 4261 | Hispanic subgroups living in the USA | Ever tested: total sample, 34% (1444/4261); Puerto Ricans, 44% (197/444); Mexicans, 28% (419/1480); Mexican Americans, 33% (355/1079); Cubans + Cuban Americans, 29% (80/277); Central/South Americans, 41% (259/640); other Hispanics, 39% (133/341) | Cross-sectional study. Have had an HIV test (Note: prevalence by our research team based on presented article data) |
| Dougan S et al. | UK (2005) | 1040 | Black and minority ethnic men who have sex with men in England and Wales | Prevalence ratio of HIV test acceptance: Caribbean, 52% (138/265); Central/South America, 60% (593/993); sub-Saharan African, 54% (473/870); Asia, 56% (417/739) | Cross-sectional study with offer of HIV test |
The context in which testing is offered and who offers the test seem to be important determinants of test acceptance. For example, in a US study, 70% of Hispanic migrant farm workers reported they would accept testing recommended by a health-care provider, with women more likely than men to accept testing.29 In contrast, MSM from ethnic minorities in the USA were more prone to accept HIV testing outside health settings; rapid HIV testing of MSM in racial/ethnic minority groups in settings such as gay pride events is a useful way to enable HIV-infected MSM to learn their HIV status.
Late HIV diagnosis in migrants and ethnic minorities
High prevalence of delayed diagnosis of HIV infection in migrants and ethnic minorities was reported, largely among sub-Saharan Africans in the UK,10,11,13,24,25,40 Spain23 and France38 and among Latinos and Asian Americans in the USA14,27 and Canada.45
López-Quintero et al.12 report Hispanics to be more likely to have delayed HIV diagnoses than whites and Afro-Americans. Prost et al.10 cite the Health Protection Agency and the Mayisha II Study,46 which estimated that by 2005, approximately 21 500 Africans were living with HIV in the UK and that one-third of them were undiagnosed. Fakoya et al.24 report that most people from sub-Sahara diagnosed with HIV in the UK acquired the infection in the countries of origin and tend to present with advanced disease. Also in the UK, Chadborn et al.13 report high prevalence of late diagnosis in heterosexual whites (36%), black Caribbeans (36%) and black Africans (43%). They describe lower rates of delayed diagnosis in women diagnosed through antenatal testing than other people diagnosed elsewhere. For sub-Saharan Africans, late diagnosis was present in 21% of women diagnosed during antenatal care, 44% of women diagnosed elsewhere and 50% of men. In France, although women were less likely to be diagnosed late because of routine prenatal testing, this was not the case among migrants. Acquisition of HIV infection at early ages before arrival to France could underlie these differences.38
Interventions to encourage HIV testing in migrants and ethnic minorities
The literature identified two main approaches to HIV testing: general population approaches in health-care settings and targeted approaches directed to at-risk populations, including migrant and/or ethnic minorities. In both cases, specific interventions to encourage the participation of migrants and ethnic minorities are discussed. Among the targeted approaches, voluntary or compulsory HIV testing strategies are analysed.
Antenatal screening is an example of a population-wide approach; various studies support routine antenatal testing for all pregnant women as an effective strategy for achieving good coverage of HIV testing in migrant and ethnic minorities.42 Regarding preferences of immigrant women, a study in Canada found that women from HIV-endemic countries prefer non-targeted strategies integrated within health services.9 Some countries have taken targeted approaches to HIV testing in antenatal care. For example, Denmark switched from routine to HIV selective antenatal screening in 1995; HIV testing was only offered to women from high prevalence countries since almost all HIV-positive pregnant women identified were migrants or married to migrants from high prevalence countries.37 However, a few HIV-positive babies were born subsequently, resulting in the reintroduction of universal screening.
Health-care provider endorsement was identified as a significant predictor of HIV testing. Some authors recommend mixed approaches; introducing HIV screening in routine medical practice in addition to targeted strategies in place, particularly in areas with high HIV prevalence and a concentration of migrant population.9,29,41,42
Many authors indicated that culturally sensitive HIV testing and counselling interventions are needed to improve institutional access to health services to promote HIV testing among migrants and ethnic minorities.9,11,29 Community partnerships and participation are identified as critical to increase testing uptake. A UK study calls for community involvement in promoting testing along with the benefits of accessing antiretroviral therapy.11 Provision of testing services in client’s language is also mentioned.9,17
Innovative targeted approaches to reach people who might not otherwise use testing services include the provision of HIV rapid testing in non-traditional health-care settings outside normal working hours.29 Provision of point-of-care testing by non-government and community-based organizations and testing by outreach services, mobile clinics and in venues such as barber shops and hair salons, social clubs, sporting events or street corners27,36 are recommended. Offering HIV testing at gay pride events36, saunas41 and other venues was also considered to increase uptake among MSM.
Another approach specifically targeting migrants is screening on arrival in the country. US policy requires HIV testing for asylum seekers,47 and in 2008, when the mentioned article was published, those who were HIV-infected could only obtain temporary admission to the USA. Children who arrive in the USA needing a permanent visa are required to be screened for HIV, hepatitis B and C and tuberculosis, and screening is repeated 6 months after arrival. The implications of HIV test results for visa status are not discussed.19 HIV testing is also mandatory for migrants and asylum seekers entering Canada. Screening includes clinical referral and information that is sensitive to the gender, cultural and linguistic profile of the client.30,31 This approach is reported to have resulted in an increased number of cases of HIV diagnosed in immigrants and uptake of health care in this country.45 A French study recommends offering HIV testing to migrants on arrival to reduce late diagnosis.38
Discussion
This systematic review has found that migrants, largely those from HIV-endemic countries, are at high risk of HIV infection and its consequences.10,11,13,14,23–25,27,38,40,45 Their HIV prevalence is higher than that of the general population, they have a higher frequency of delayed HIV diagnosis and are more vulnerable to the negative effects of disclosure of HIV status.11,16 For migrants from countries where HIV prevalence is low, their socio-economic vulnerability puts them at risk of acquiring HIV in destination countries.11,39,40 In addition to their socio-economic vulnerability and the barriers to HIV testing shared with other groups at risk, migrants have specific legal and administrative impediments to accessing health services10,16,17,24 and thus HIV testing facilities—in some countries, undocumented migrants are not entitled to health care13,14,35—as well as cultural and linguistic barriers,14–18,20 racism and xenophobia10; criminalization of HIV transmission has disproportionately affected migrants from SSA.10 Migrants also fear stigma and discrimination from their communities, fundamental for their well-being in a foreign country.10
Testing migrants for HIV may take place either in the context of general population strategies in health-care settings—such as antenatal testing—or targeted approaches among specific populations. HIV testing uptake in antenatal settings in migrants is high and similar to that of non-migrant women. Women from HIV-endemic countries prefer general population strategies that are integrated within health services.33,42 Overall, a higher proportion of migrant women have been tested for HIV compared with men, partially because of high acceptance of routine antenatal HIV screening, but men, although less exposed to HIV testing, are also less willing to be tested.29 Reaching migrant men, both heterosexual and MSM, is a challenge. The literature shows that migrant MSM are a hard-to-reach group and that ‘machismo’ and homophobia are deterrents to HIV prevention.27 Mandatory HIV testing for migrants and asylum seekers when entering a country, in place in some settings,30,31,47 violates the core principles that HIV testing must be confidential, voluntary and performed with informed consent.
A key aspect—often undermined—is the heterogeneity of migrant populations, which requires tailored strategies for some groups. It is essential to discuss and implement interventions in partnerships with the communities. Test performance in non-traditional settings27,36,41 and during off-hours,29 the use of rapid tests12,29,36 and providing test services from a culturally sensitive perspective appear to be positive interventions. It is remarkable that little information on counselling was retrieved from the literature.
There are a number of study limitations that merit discussion. Although our aim was not to review studies on HIV prevalence and risk factors in migrants and ethnic minorities, these subjects came up in a large number of studies. However, we realize that the search strategy used provides only a partial view on these topics. We are also aware this search covers only articles in English; research in other languages, the grey literature and conference abstracts are not included. The methodology used in this systematic review does not permit a comprehensive assessment of the extent to which mandatory HIV testing is applied to migrants.
There is increasing evidence in recent years of the benefits of HIV testing at the individual and community levels.5,48–52 There is also overwhelming consensus that HIV testing cannot be the final goal, and it is essential to link testing with care, support and treatment so as to ensure a referral pathway for those who test positive. In December 2010, the European Centre for Disease Prevention and Control (ECDC) launched ‘HIV testing: increasing uptake and effectiveness in the European Union’8 in which migrants receive considerable attention. The results from this systematic review may help to design interventions targeting migrants, so that ECDC guidance may influence national recommendations.
Supplementary Data
Supplementary Data are available at EURPUB online.
Funding
This work has been financed by the European Centre for Disease Prevention and Control, the Spanish Network of HIV/AIDS Research [RIS—RD06/0006] and the CIBERESP (Biomedical Research Centre Network for Epidemiology and Public Health).
Conflict of interest: None declared.
Key points.
Migrants, mainly from HIV-endemic countries, are at high risk of HIV infection and its consequences. Their HIV prevalence is higher than in the general population, they have higher frequency of delayed HIV diagnosis and are more vulnerable to the negative effects of disclosure of HIV status. For migrants from countries with low HIV prevalence, socio-economic vulnerability puts them at risk of acquiring HIV in destination countries.
Migrants have specific legal and administrative impediments in accessing health services and HIV testing—in some countries, undocumented migrants are not entitled to health care—as well as cultural and linguistic barriers, racism and xenophobia. Migrants fear stigma from their communities, yet community acceptance is key for well-being.
Although there is increasing evidence of the benefits of HIV testing at both the individual and community levels, the barriers highlighted in this systematic review may prevent programs from achieving the final goal, which is linking migrants and ethnic minorities to HIV clinical care under the public health perspective.
Acknowledgements
The authors are grateful to Jessika Deblonde and Georg Bröring for their valuable input to this work. This work has been financed by the ECDC, the Spanish Network of HIV/AIDS Research [RIS—RD06/0006] and the CIBERESP.
References
- 1.European Centre for Diseases Prevention and Control (ECDC) HIV/AIDS surveillance in Europe 2007. Surveillance report. 2008. Available at: http://ecdc.europa.eu/en/publications/publications/0812_sur_hiv_aids_surveillance_in_europe.pdf (15 January 2012, date last accessed)
- 2.Del Amo J, Perez-Cachafeiro S, Hernando V, et al. Migrant health: Epidemiology of HIV and AIDS in migrant communities and ethnic minorities in EU/EEA countries, Technical report. 2010. Available at: http://www.ecdc.europa.eu/en/publications/Publications/0907_TER_Migrant_health_HIV_Epidemiology_review.pdf (15 January 2012, date last accessed)
- 3.Centers of Disease Control and Prevention. Revised Recommendations for HIV Testing of Adults, Adolescents, and Pregnant Women in Health-Care Settings. 2006. Available at: http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5514a1.htm (15 January 2012, date last accessed) [PubMed]
- 4.World Health Organization (WHO), Joint United Nations Programme on HIV/AIDS (UNAIDS), and UNICEF. Towards universal access. Scaling up priority HIV/AIDS interventions in the health sector. 2009. Available at: http://www.who.int/hiv/pub/tuapr_2009_en.pdf (15 January 2012, date last accessed)
- 5.World Health Organization (WHO) Scaling up HIV testing and counselling in the WHO European Region as an essential component of efforts to achieve universal access to HIV prevention, treatment, care and support. 2010. Available at: http://www.euro.who.int/__data/assets/pdf_file/0007/85489/E93715.pdf (15 January 2012, date last accessed)
- 6.Haute Autorité de Santè (HAS) HIV infection screening in France—Screening Strategies. 2009. Available at: http://www.has-sante.fr/portail/upload/docs/application/pdf/2010-02/hiv_infection_screening_in_france_-_screening_strategies_-_executive_summary_2010-02-26_10-28-32_643.pdf (15 January 2012, date last accessed)
- 7.British HIV Association, British Association of Sexual Health, and HIV British Infection Society. UK National Guidelines for HIV Testing. 2008. Available at: http://www.bhiva.org/documents/Guidelines/Testing/GlinesHIVTest08.pdf (15 January 2012, date last accessed)
- 8.European Centre for Disease Prevention and Control (ECDC) HIV testing: increasing uptake and effectiveness in the European Union. 2010. Available at: http://www.ecdc.europa.eu/en/publications/Publications/101129_GUI_HIV_testing.pdf (15 January 2012, date last accessed)
- 9.Mitra D, Jacobsen MJ, O'Connor A, et al. Assessment of the decision support needs of women from HIV endemic countries regarding voluntary HIV testing in Canada. Patient Educ Couns. 2006;63:292–300. doi: 10.1016/j.pec.2006.04.005. [DOI] [PubMed] [Google Scholar]
- 10.Prost A, Elford J, Imrie J, et al. Social, behavioural, and intervention research among people of sub-saharan African origin living with HIV in the UK and Europe: literature review and recommendations for intervention. AIDS Behav. 2008;12:170–94. doi: 10.1007/s10461-007-9237-4. [DOI] [PubMed] [Google Scholar]
- 11.Burns FM, Imrie JY, Nazroo J, et al. Why the(y) wait? Key informant understandings of factors contributing to late presentation and poor utilization of HIV health and social care services by African migrants in Britain. AIDS Care. 2007;19:102–8. doi: 10.1080/09540120600908440. [DOI] [PubMed] [Google Scholar]
- 12.Lopez-Quintero C, Shtarkshall R, Neumark YD. Barriers to HIV-testing among Hispanics in the United States: analysis of the National Health Interview Survey, 2000. AIDS Patient Care STDS. 2005;19:672–83. doi: 10.1089/apc.2005.19.672. [DOI] [PubMed] [Google Scholar]
- 13.Chadborn TR, Delpech VC, Sabin CA, et al. The late diagnosis and consequent short-term mortality of HIV-infected heterosexuals (England and Wales, 2000-2004) AIDS. 2006;20:2371–9. doi: 10.1097/QAD.0b013e32801138f7. [DOI] [PubMed] [Google Scholar]
- 14.Huang ZJ, Wong FY, De Leon JM, Park RJ. Self-reported HIV testing behaviors among a sample of Southeast Asians in an urban setting in the United States. AIDS Educ Prev. 2008;20:65–77. doi: 10.1521/aeap.2008.20.1.65. [DOI] [PubMed] [Google Scholar]
- 15.Vissman AT, Eng E, Aronson RE, et al. What do men who serve as lay health advisers really do?: immigrant Latino men share their experiences as Navegantes to prevent HIV. AIDS Educ Prev. 2009;21:220–32. doi: 10.1521/aeap.2009.21.3.220. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Foley EE. HIV/AIDS and African immigrant women in Philadelphia: structural and cultural barriers to care. AIDS Care. 2005;17:1030–43. doi: 10.1080/09540120500100890. [DOI] [PubMed] [Google Scholar]
- 17.Levy V, Page-Shafer K, Evans J, et al. HIV-related risk behavior among Hispanic immigrant men in a population-based household survey in low-income neighborhoods of northern California. Sex Transm Dis. 2005;32:487–90. doi: 10.1097/01.olq.0000161185.06387.94. [DOI] [PubMed] [Google Scholar]
- 18.Perez-Molina JA, Lopez-Velez R, Navarro M, et al. Clinicoepidemiological characteristics of HIV-infected immigrants attended at a tropical medicine referral unit. J Travel Med. 2009;16:248–52. doi: 10.1111/j.1708-8305.2009.00308.x. [DOI] [PubMed] [Google Scholar]
- 19.Schwarzwald H. Illnesses among recently immigrated children. Semin Pediatr Infect Dis. 2005;16:78–83. doi: 10.1053/j.spid.2005.12.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Tariq S, Edwards SG, Nalabanda A, et al. Sexual health services for South Asians in London, UK: a case-control study. Int J STD AIDS. 2007;18:563–4. doi: 10.1258/095646207781439676. [DOI] [PubMed] [Google Scholar]
- 21.Platform for International Cooperation and Undocumented Migrants (PICUM) Access to health care for undocumented migrants in Europe. 2007. Available at: http://www.picum.org/sites/default/files/data/Access%20to%20Health%20Care%20for%20Undocumented%20Migrants.pdf (15 January 2012, date last accessed)
- 22.World Health Organization (WHO) Dublin Declaration on Partnership to fight HIV/AIDS in Europe and Central Asia. 2004. Available at: http://www.unicef.org/ceecis/The_Dublin_Declaration.pdf (15 January 2012, date last accessed)
- 23.Monge-Maillo B, Jimenez BC, Perez-Molina JA, et al. Imported infectious diseases in mobile populations, Spain. Emerg Infect Dis. 2009;15:1745–52. doi: 10.3201/eid1511.090718. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Fakoya I, Reynolds R, Caswell G, Shiripinda I. Barriers to HIV testing for migrant black Africans in Western Europe. HIV Med. 2008;9(Suppl 2):23–5. doi: 10.1111/j.1468-1293.2008.00587.x. [DOI] [PubMed] [Google Scholar]
- 25.Prost A, Seruma WS, Fakoya I, et al. HIV voluntary counselling and testing for African communities in London: learning from experiences in Kenya. Sex Transm Infect. 2007;83:547–51. doi: 10.1136/sti.2007.027110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Eisenhut M, Sharma V, Kawsar M, Balachandran T. Knowledge of their children's HIV status in HIV-positive mothers attending a genitourinary medicine clinic in the UK. HIV Med. 2008;9:257–9. doi: 10.1111/j.1468-1293.2008.00556.x. [DOI] [PubMed] [Google Scholar]
- 27.Olshefsky AM, Zive MM, Scolari R, Zuniga M. Promoting HIV risk awareness and testing in Latinos living on the U.S.-Mexico border: the Tu No Me Conoces social marketing campaign. AIDS Educ Prev. 2007;19:422–35. doi: 10.1521/aeap.2007.19.5.422. [DOI] [PubMed] [Google Scholar]
- 28.Ehrlich SF, Organista KC, Oman D. Migrant Latino day laborers and intentions to test for HIV. AIDS Behav. 2007;11:743–52. doi: 10.1007/s10461-006-9182-7. [DOI] [PubMed] [Google Scholar]
- 29.Fernandez MI, Collazo JB, Bowen GS, et al. Predictors of HIV testing and intention to test among Hispanic farmworkers in South Florida. J Rural Health. 2005;21:56–64. doi: 10.1111/j.1748-0361.2005.tb00062.x. [DOI] [PubMed] [Google Scholar]
- 30.Zencovich M, Kennedy K, MacPherson DW, Gushulak BD. Immigration medical screening and HIV infection in Canada. Int J STD AIDS. 2006;17:813–16. doi: 10.1258/095646206779307469. [DOI] [PubMed] [Google Scholar]
- 31.MacPherson DW, Zencovich M, Gushulak BD. Emerging pediatric HIV epidemic related to migration. Emerg Infect Dis. 2006;12:612–17. doi: 10.3201/eid1204.051025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Sadler KE, McGarrigle CA, Elam G, et al. Mayisha II: pilot of a community-based survey of sexual attitudes and lifestyles and anonymous HIV testing within African communities in London. AIDS Care. 2006;18:398–403. doi: 10.1080/09540120600634400. [DOI] [PubMed] [Google Scholar]
- 33.Southgate J, Mital D, Stock A. Are women from high-risk ethnic minority groups more likely to decline antenatal HIV screening? Int J STD AIDS. 2008;19:206–7. doi: 10.1258/ijsa.2007.007230. [DOI] [PubMed] [Google Scholar]
- 34.Flowers P, Davis M, Hart G, et al. Diagnosis and stigma and identity amongst HIV positive Black Africans living in the UK. Psychol Health. 2006;21:109–22. [Google Scholar]
- 35.Boyd AE, Murad S, O'shea S, et al. Ethnic differences in stage of presentation of adults newly diagnosed with HIV-1 infection in south London. HIV Med. 2005;6:59–65. doi: 10.1111/j.1468-1293.2005.00267.x. [DOI] [PubMed] [Google Scholar]
- 36.Dowling T. Rapid HIV testing among racial/ethnic minority men at gay pride events—nine U.S. cities, 2004-2006. MMWR Morb Mortal Wkly Rep. 2007;56:602–4. [PubMed] [Google Scholar]
- 37.Schmid J, Jensen-Fangel S, Valerius NH, et al. Demographics in HIV-infected children in Denmark: results from the Danish Paediatric HIV Cohort Study. Scand J Infect Dis. 2005;37:344–9. doi: 10.1080/00365540510031700. [DOI] [PubMed] [Google Scholar]
- 38.Delpierre C, Dray-Spira R, Cuzin L, et al. Correlates of late HIV diagnosis: implications for testing policy. Int J STD AIDS. 2007;18:312–17. doi: 10.1258/095646207780749709. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Dougan S, Elford J, Rice B, et al. Epidemiology of HIV among black and minority ethnic men who have sex with men in England and Wales. Sex Transm Infect. 2005;81:345–50. doi: 10.1136/sti.2004.012328. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Manzardo C, Trevino B, Prat J, et al. Communicable diseases in the immigrant population attended to in a tropical medicine unit: epidemiological aspects and public health issues. Travel Med Infect Dis. 2008;6:4–11. doi: 10.1016/j.tmaid.2007.11.002. [DOI] [PubMed] [Google Scholar]
- 41.Carnicer-Pont D, de Olalla PG, Cayla JA, AIDS WG HIV infection late detection in AIDS patients of an European city with increased immigration since mid 1990s. Curr HIV Res. 2009;7:237–43. doi: 10.2174/157016209787581427. [DOI] [PubMed] [Google Scholar]
- 42.Ostermann J, Kumar V, Pence BW, Whetten K. Trends in HIV testing and differences between planned and actual testing in the United States, 2000-2005. Arch Intern Med. 2007;167:2128–35. doi: 10.1001/archinte.167.19.2128. [DOI] [PubMed] [Google Scholar]
- 43.Forbes KM, Rahman N, McCrae S, Reeves I. Integrated community-based sexual health services for young people in urban areas: are we meeting the needs of the local community? Int J STD AIDS. 2008;19:713–14. doi: 10.1258/ijsa.2008.008055. [DOI] [PubMed] [Google Scholar]
- 44.Conaty SJ, Cassell JA, Harrisson U, et al. Women who decline antenatal screening for HIV infection in the era of universal testing: results of an audit of uptake in three London hospitals. J Public Health (Oxf) 2005;27:114–17. doi: 10.1093/pubmed/fdh203. [DOI] [PubMed] [Google Scholar]
- 45.Krentz H, Gill MJ. The five-year impact of an evolving global epidemic, changing migration patterns, and policy changes in a regional Canadian HIV population. Health Policy. 2009;90:296–302. doi: 10.1016/j.healthpol.2008.09.016. [DOI] [PubMed] [Google Scholar]
- 46.MAYISHA II Collaborative Group. Assessing the feasibility and acceptability of community based prevalence surveys of HIVamong black Africans in England. London: Health Protection Agency Centre for Infections; 2005. [Google Scholar]
- 47.Jones KG, Jones SG. Lo Siento Pero Usted No Esta Bienvenido: U.S. travel policies and immigration laws for HIV-infected persons. J Assoc Nurses AIDS Care. 2008;19:325–9. doi: 10.1016/j.jana.2008.04.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.European Centre for Diseases Prevention and Control (ECDC) Migrant health: Background note to the ‘ECDC Report on migration and infectious diseases in the EU’. Technical report. Available at: http://www.episouth.org/doc/r_documents/0907_TER_Migrant_health_Background_note.pdf (15 January 2012, date last accessed)
- 49.Das M, Chu PL, Santos GM, et al. Decreases in community viral load are accompanied by reductions in new HIV infections in San Francisco. PLoS.One. 2010;5:e11068. doi: 10.1371/journal.pone.0011068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Porco TC, Martin JN, Page-Shafer KA, et al. Decline in HIV infectivity following the introduction of highly active antiretroviral therapy. AIDS. 2004;18:81–8. doi: 10.1097/01.aids.0000096872.36052.24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Quinn TC, Wawer MJ, Sewankambo N, et al. Viral load and heterosexual transmission of human immunodeficiency virus type 1. N Engl J Med. 2000;342:921–9. doi: 10.1056/NEJM200003303421303. [DOI] [PubMed] [Google Scholar]
- 52.National Institute of Allergy and Infectious Diseases (NIAID) Treating HIV-infected people with antiretrovirals protects partners from infection. 2011. Available at: http://www.niaid.nih.gov/news/newsreleases/2011/Pages/HPTN052.aspx (15 January 2012, date last accessed)