Abstract
Background
The population ≥65 years is rapidly increasing but remarkably little is known about the natural history of abdominal pain with aging.
Aim
To prospectively evaluate the natural history of abdominal pain (severity and frequency) in a US population, and evaluate potential risk factors (including somatization) for the onset and disappearance of abdominal pain with increasing age.
Methods
Between 1988 and 2004, valid self-report questionnaires that recorded gastrointestinal symptoms including severity and frequency of abdominal pain were mailed to randomly selected cohorts of community residents followed over time. This study identified all respondents who answered abdominal pain questions at an initial and follow-up survey.
Results
1913 subjects were included (mean age in years at first survey: 48±12 (SD), mean age at second survey: 59±13 (SD); 53% female). The onset and disappearance rate of abdominal pain over the follow up were 14% (95% CI, 13,16) and 47% (43,50), respectively. The rates of increasing vs. decreasing abdominal pain score were 18% (16,20) vs. 22% (20,23), respectively. While younger age at initial survey was associated with onset of abdominal pain (vs. subjects without abdominal pain, [OR 0.9 (0.7,1.0)], older age at initial survey and times between surveys were associated with the disappearance of abdominal pain (vs. subjects with abdominal pain, [OR 1.2 (1.0,1.5)]. Female gender [OR 1.4 (1.0,2.1)], higher somatization scores and larger changes in somatization score [OR 5.3 (3.2,8.7)] were positively associated with the onset of abdominal pain.
Conclusions
Increasing age is associated with the disappearance of abdominal pain in the community.
BACKGROUND
The population aged 65 years and older is rapidly increasing in North America, Europe and elsewhere.1, 2 Aging has variable effects on the gastrointestinal tract3, 4 but is linked to altered gastrointestinal function, such as delayed gastric emptying,5 altered colonic transit time,6 or changes on gut microbiota.7 However, surprisingly, little is known about the natural history of gastrointestinal symptoms with aging, most notably abdominal pain.
Based on cross sectional evidence, the prevalence of irritable bowel syndrome and dyspepsia may decrease with age,8, 9 in contrast to the prevalence of constipation and fecal incontinence which have been reported to increase with advancing age.6, 10 Chronic abdominal pain is the central symptom of irritable bowel syndrome8 as well as one of the major symptom components of functional dyspepsia.11 Whether the apparent decrease in IBS and dyspepsia with age is explained by the disappearance of abdominal pain is unknown.
Gururatsakul et al.12 have observed that abdominal pain and nausea during a standardized nutrient challenge were significantly but inversely correlated with age. Thus, we aimed to prospectively evaluate the natural history of chronic abdominal pain (both severity and frequency) in a US population and evaluate potential risk factors (including somatization) for the onset and disappearance of abdominal pain with increasing age.
METHODS
This study is a retrospective data analysis from a prospective population-based cohort study of subjects who were sent an initial GI symptom survey between 1988 and 1994 and then subsequent surveys up until 2004. Data from the individual cross sectional cohorts have been previously published in part,13–22 and each survey, which measured the severity and frequency of abdominal pain experienced during the past year in a standardized and validated questionnaire, was included in the current study. This study was approved by the Institutional Review Boards of the Mayo Clinic and the Olmsted Medical Center.
Subjects
The Olmsted County population comprises approximately 120,000 persons of which 90% are white; sociodemographically, the community is similar to the U.S. white population.23, 24 Eighty percent of the Olmsted County population resides within five miles of Rochester, and County residents receive their medical care almost exclusively from two group practices: Mayo Clinic and Olmsted Medical Center. Mayo Clinic has maintained a common medical record system with its two affiliated hospitals (St. Marys and Rochester Methodist) for over 100 years. Recorded diagnoses and surgical procedures are indexed, including the diagnoses made for outpatients seen in office or clinic consultations, emergency room visits or nursing home care, as well as the diagnoses recorded for hospital inpatients, at autopsy examination or on death certificates.23, 24 The system was further developed by the Rochester Epidemiology Project, which created similar indices for the records of other providers of medical care to local residents, most notably the Olmsted Medical Group and its affiliated Olmsted Community Hospital (Olmsted Medical Center). Annually, over 80% of the entire population is attended by one or both of these two practices, and nearly everyone is seen at least once during any given four-year period.23, 24 Therefore, the Rochester Epidemiology Project medical records linkage system also provides what is essentially an enumeration of the population from which representative samples can be drawn. As part of previous investigations,16–22 we utilized the enumeration of the Olmsted County population as described above to randomly select age- (five year intervals) and sex-stratified random samples of Olmsted County adult residents. The initial two cohorts were young to middle aged (20–50 and 30–65 years); then two elderly cohorts (age >65) were identified. These samples ranged in size from 800 to 2200 residents. They were mailed valid self-report symptom questionnaires from November 1988 to June 1994, i.e., the ‘baseline’ or initial survey. At the outset, the complete (inpatient and outpatient) medical records of the individuals enumerated in the sample were reviewed. Subjects were excluded if they had significant illnesses which might cause gastrointestinal symptoms or impair their ability to complete the questionnaire (e.g. metastatic cancer, major stroke), had a major psychotic episode, mental retardation or dementia, or had a history of major abdominal surgery.
Further, revised versions of the study questionnaire and an explanatory letter were then mailed to the original cohort in a follow-up survey during 2003–2004. Identical validated questions about abdominal pain were included in all surveys. Subjects who had died, moved from Olmsted County, or denied authorization to use their medical records for research, as required by Minnesota law, were excluded from these mailings but passive non-responders to the initial surveys were included. Reminder letters were mailed at 2, 4 and 7 weeks. Subjects who indicated at any point that they did not wish to complete the survey were not contacted further. Otherwise, non-responders were contacted by telephone at 10 weeks to request their participation and verify their residence within the country.
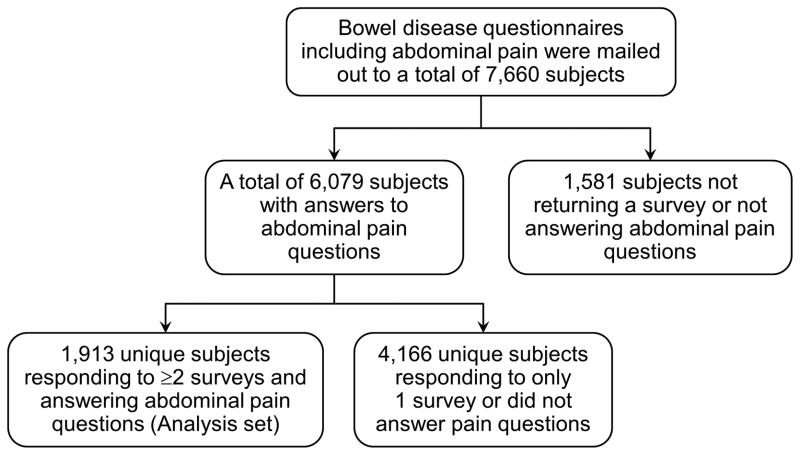
Among a total of 6079 respondents who answered abdominal pain questions at the previous cohort study over the follow up, a total of 1913 subjects, who responded to a minimum of 2 surveys, were eligible for the current study (Figure 1).
Figure 1.
Flow chart for the current study
Questionnaire
The Talley Bowel Disease Questionnaire (BDQ)18, 19, 22 was designed as a self-report instrument to measure symptoms experienced over the prior year and to collect the past medical history. Previous testing has shown this instrument to be reliable, with a median kappa statistic for symptom items of 0.78 (range, 0.52–1.00); reliability was assessed by asking subjects to complete the survey on two occasions two weeks apart in the outpatient setting. It has also been demonstrated to have adequate content, predictive and construct validity.18, 19, 22 The original BDQ contained 46 gastrointestinal symptom-related items including severity and frequency of abdominal pain questions; 25 items that measure past illness, health care use, and sociodemographic variables; and a valid measure of non-gastrointestinal somatic complaints, the Somatic Symptom Checklist (SSC).25 The SSC consists of 12 non-GI symptoms or illnesses. Respondents are instructed to indicate how often each symptom occurred (on a scale of 0, indicating not a problem, to 4, indicating occurs daily) and how bothersome each was (on a scale of 0, not a problem, to 4, extremely bothersome when occurs) during the past year, using separate 5-point scales. Further, the original BDQ was modified and tested for the elderly26 and derivatives created for specific conditions.27–30 These versions were also tested before implementation. Modifications of the original bowel disease questionnaire were used for the follow-up mailings.
Definition of abdominal pain
Frequency of abdominal pain was measured by frequent (at least weekly), infrequent (less than weekly), and none. In addition, severity of abdominal pain was assessed by severe, moderate, mild, or none.
An abdominal pain category in the prior year was generated combining frequency and severity of abdominal pain into 5 categories for the current study (yielding grades 0–4):
0 = no abdominal pain
1 = mild and infrequent abdominal pain
2 = mild and frequent, or moderate and infrequent abdominal pain
3 = moderate and frequent, or severe and infrequent abdominal pain
4 = severe and frequent abdominal pain
We have previously shown that response bias was minimal in our Olmsted County cohorts mailed the BDQ.31
Statistical analysis
The proportions of subjects with onset and disappearance of abdominal pain were estimated along with 95% CIs based on the binomial distribution. The association between age and changes (improved, worsened, remained the same [reference category]) in reported abdominal pain score, disappearance of abdominal pain, and, separately, onset of abdominal pain were analyzed using logistic regression models, which adjusted for gender, SSC score, and time between surveys. The odds ratios (95% CIs) for improvement, worsening, onset, and disappearance were computed from the estimated coefficients in the logistic regression models.
RESULTS
A total of 1913 subjects were eligible for analysis. (Mean age at first survey: 48 ± 12 (SD), mean age at second survey: 59 ± 13 (SD); 53% female).
Changes of abdominal pain over the follow-up
The overall, age and gender specific proportions (%) of subjects reporting specific abdominal pain according to their characteristics (severity and frequency) on the initial and final surveys are given in Table 1. The overall proportion (%) of any abdominal pain (mild, moderate, or severe abdominal pain) in the initial survey was 36% (95% CI: 34, 38) and 31% (95% CI: 29, 33) in the final survey. Also, the overall proportion (%) of severe abdominal pain was 5% (95% CI: 4, 6) in the initial survey and 4% (95% CI: 3, 5) in the final survey. The proportion (%) reporting frequent abdominal pain was 9% (95% CI: 8, 11) initially and 11% (95% CI: 10, 12) in the final survey. The median (range) between initial and final surveys was 11.0 years (0.9 to 15.3 years).
Table 1.
Abdominal pain by severity and frequency on initial and final survey
| Abdominal pain | Initial Survey | Final Survey | ||||
|---|---|---|---|---|---|---|
|
| ||||||
| Male | Female | Overall | Male | Female | Overall | |
|
| ||||||
| Severity | ||||||
| None | 586 (65%) | 636 (63%) | 1222 (64%) | 664 (73%) | 661(66%) | 1325 (69%) |
| Mild | 108 (12%) | 90 (9%) | 198 (10%) | 75 (8%) | 69 (7%) | 144 (8%) |
| Moderate | 170 (19%) | 229 (23%) | 399 (21%) | 133 (15%) | 237 (24%) | 370 (19%) |
| Severe | 40 (4%) | 54 (5%) | 94(5%) | 32 (4%) | 42 (4%) | 74 (4%) |
|
| ||||||
| Frequency | ||||||
| None | 586 (65%) | 636(63%) | 1222 (64%) | 664(73%) | 661(66%) | 1325 (69%) |
| Infrequent | 237 (26%) | 276 (27%) | 513 (27%) | 158(18%) | 221(22%) | 379 (20%) |
| Frequent | 81 (9%) | 97 (10%) | 178 (9%) | 82(9%) | 127(13%) | 209 (11%) |
Transitions over the follow-up
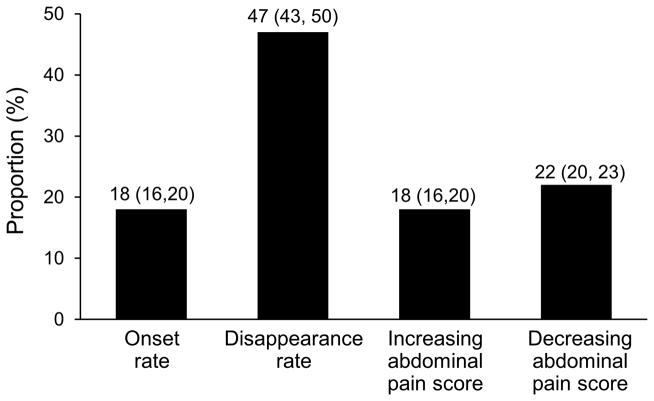
Table 2 shows the onset and disappearance rate of any abdominal pain as well as the rate of increasing and decreasing abdominal pain category. Of those subjects who did not report abdominal pain in any form in their initial survey (n=1222), 18% (95% CI: 16, 20; n=219) reported abdominal pain in their final survey. Among those subjects who reported any abdominal pain, the disappearance rate at the final survey was 47% (95% CI: 43, 50). Notably, about 18% (95% CI: 16, 20) of the respondents reported an increase in their abdominal pain category between initial and final survey, while 22% (95% CI: 20, 23) of the respondents had a decrease of their abdominal category between initial and final survey. Figure 2 shows overall transitions of abdominal pain categories between initial and final survey. Overall, 1160 (61%) of the 1913 reported the same pain category while 39% reported different abdominal pain categories on their last survey compared to their initial survey. Approximately 47% of those reporting some abdominal pain on their initial survey reported no pain on their last survey, and 23% of subjects reporting some abdominal pain on their initial survey reported the same pain category on their last survey. The remaining subjects changed their abdominal pain category, 18% reporting an increased category and 13% reporting a decreased category from their initial to last survey.
Table 2.
Number of patients in initial and final survey according to abdominal pain score
| Abdominal Pain Score on Initial Survey | Abdominal Pain Score on Final Survey | Total | ||||
|---|---|---|---|---|---|---|
| 0 | 1 | 2 | 3 | 4 | ||
| 0 | 1003 | 43 | 110 | 60 | 6 | 1222 |
| 1 | 87 | 30 | 32 | 13 | 3 | 165 |
| 2 | 162 | 24 | 77 | 55 | 7 | 325 |
| 3 | 57 | 12 | 39 | 42 | 13 | 163 |
| 4 | 16 | 1 | 8 | 5 | 8 | 38 |
| Total | 1325 | 110 | 266 | 175 | 37 | 1913 |
Figure 2.
Proportion (%) of onset, disappearance, increasing abdominal score, and decreasing abdominal score with aging. The values in parentheses are the 95% Confidence Intervals.
Logistic regression models
Table 3 summarizes the multiple variable logistic regression models for onset or disappearance. Younger age at initial survey was associated with the onset of abdominal pain (vs. subjects without abdominal pain [OR, 0.9 (0.7, 1.0)]). Moreover, female gender, higher SSC scores and larger changes in SSC score were positively associated with the onset of abdominal pain. Older age at initial survey, lower SSC score, time between surveys and smaller changes in SSC score were associated with the disappearance of abdominal pain compared to subjects with abdominal pain at both initial and last surveys.
Table 3.
Multiple variable logistic modeling for transitions (Odds Ratio, 95% CI)
| Onset No/Yes vs. No/No* n=1222 |
Disappearance Yes/No vs. Yes/Yes+ n=691 |
|||
|---|---|---|---|---|
| Age at first survey (per 10 years) | 0.9 (0.7,1.0) | p=0.06 | 1.2 (1.0,1.5) | p=0.02 |
| Female | 1.4 (1.0,2.1) | p=0.08 | 1.0 (0.7,1.5) | p=0.995 |
| SSC at first survey | 5.3 (3.2,8.7) | p<0.001 | 0.3 (0.2,0.6) | p<0.001 |
| Time between surveys (last – first survey) | 0.9 (0.5,1.5) | p=0.61 | 1.6 (1.0,2.5) | p=0.04 |
| Change in SSC (last – first survey) | 2.1 (1.4,3.2) | p<0.001 | 0.4 (0.3,0.7) | p=0.001 |
No/Yes=no abdominal pain reported on 1st survey but reported at the follow-up survey, No/No=no abdominal pain symptoms at first and follow-up survey;
Yes/no =abdominal pain reported on 1st survey but not at the follow-up survey, Yes/yes=abdominal pain at 1st survey and the follow-up survey
SSC- somatic symptom score
DISCUSSION
In this study, we describe changes in abdominal pain including onset and disappearance with advancing age over a median of 11-years in a U.S. population-based cohort. This is the longest follow-up population-based study of subjects with abdominal pain to our knowledge. It confirms that frequent abdominal pain is highly prevalent, affecting about 10% in the community. Frequent abdominal pain had a stable prevalence over the follow up, whereas the prevalence of any abdominal pain decreased with advancing age. In addition, about 1/4 of subjects changed their abdominal pain scores over time. Notably, the onset rate of abdominal pain over the follow up (18% [95% CI=16, 20]) was lower compared to the disappearance rate over the same period (47% [95% CI=43, 50]).
Abdominal pain is one of the most common gastrointestinal symptoms in the community.15, 32 Based on a multinational survey, Quigley et al.32 showed that the prevalence of abdominal pain was high but varied in different countries between 10% and 46%. We also showed that the prevalence of any abdominal pain in a U.S. sample was about 30% consistent with these international data. Notably, we found that the overall prevalence of any abdominal pain decreased over the follow up. Agreus et al.9 studied the natural history of functional abdominal disorder over 7 years using multiple surveys; they observed a decrease of prevalence over time for overall abdominal pain or discomfort and for dyspepsia, but the prevalence of IBS increased significantly over 7 years. Recently, Gururatsakul et al.12 showed an inverse relationship between the symptom responses to a standardized nutrient challenge and age in healthy volunteer. Their results suggest that elderly people have decreased gastric visceral sensation compared with younger people. Other studies33–37 have suggested an association between aging and increased visceral pain thresholds in other part of body. Lagier et al.33 studied the influence of age on rectal sensory thresholds and tone in 12 healthy subjects, and they found that rectal sensory thresholds were significantly higher in aged subjects without differences in rectal compliance. In another study, Lasch et al.34 showed that elderly subjects had significantly higher pain thresholds to intraesophageal balloon distention than younger subjects. In addition, pain thresholds, somatosensory thresholds, or thermal thresholds have shown an increase in the elderly.35, 36 Gomez-Pinilla et al.38 showed that the number of interstitial cells of Cajal (ICC) bodies and volume in both the stomach and colon significantly decreased with age, at a rate of 13% per decade. It is conceivable that decreases in ICC numbers with aging may contribute to slowing of gastrointestinal motility in turn influencing symptom presentation, although this is unlikely to lessen pain. All together these data support our observations of a decrement in the prevalence of abdominal pain with advancing age.
More intriguing are the findings in the current study of potential predictors for onset and separately disappearance of abdominal pain over the follow up. While older age at first survey was associated with disappearance of abdominal pain, younger age at first survey was associated with onset of abdominal pain. We also found that female gender at initial survey was associated with the onset of abdominal pain compared to no abdominal pain group at first and follow-up survey. Many forms of chronic visceral pain including irritable bowel syndrome have been reported to be more prevalent in women.39–41 This may be explained by increasing visceral sensitivity with perhaps a role for estrogens in the modulation of pain perception.41
Another intriguing finding of the current study is the potential role of somatization on onset and disappearance of abdominal pain. We found that higher somatization score at initial survey was associated with the onset of abdominal pain. Somatization has long been considered to be a significant risk factor for developing functional gastrointestinal disorders.42–44 Sayuk et al.44 reported an increase in the number of current somatic symptoms in outpatients with functional bowel disorders compared to those having structural gastrointestinal disease. Moreover, we found that a lower somatization score at initial survey was associated with the disappearance of abdominal pain over time compared to the persistent abdominal pain group. Choung et al.42 showed that no almost subjects in the community with IBS was free of psychological distress and/or somatic symptoms. Thus, it is conceivable that somatization plays an important role in developing or resolving abdominal pain over time.
The longitudinal design over a decade or more is the greatest methodological strength of the current study. A large community cohort was followed using the same validated instrument asking about abdominal pain over the follow up. Moreover, the investigation of a random community sample in the current study that was not seeking health care for their abdominal pain problems should have minimized selection bias. This study also had limitations. Although a very high response rate initially was obtained (82%), which is likely to avoid significant responder bias, we had about a 50% response rate to the follow-up surveys. The lower response rate at the follow-up survey might have affected the study result; however, those who responded to all three surveys were similar to the original sample (Table 1). Moreover, the BDQ had been extensively tested and found to be reliable and valid; the median kappa statistic for symptom items is 0.78 (range 0.52–1.00).19, 29, 45 Further, we have shown that systematic bias in GI survey responders in Olmsted County is essentially absent.31 Thus, non-respondents unlikely affected the results in the current study. As this was a random population-based study and we excluded at baseline known organic disease, we would expect only a small minority of cases on follow up with pain would have organic disease and most would fall into the functional GI diagnosis category. Finally, the current data cannot be generalized to the entire US population because the racial composition of this community is predominantly white.24
In summary, these data confirm the high prevalence of abdominal pain in the community. The overall prevalence of abdominal pain decreased over time, but notably the prevalence of severe abdominal pain was stable over time. Aging and somatization are important factors for determining the onset or disappearance of abdominal pain.
Acknowledgments
The authors wish to thank Lori R. Anderson for her assistance in the preparation of the manuscript.
Study data were obtained from the Rochester Epidemiology Project, which is supported by the National Institute on Aging of the National Institutes of Health under Award Number R01 AG034676.
Footnotes
The content of this manuscript is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Disclosures: No conflict of interest to disclose for all authors.
Guarantor of the article: Nicholas J. Talley, M.D., Ph.D.
Specific Author Contributions: Rok Seon Choung, Alan R. Zinsmeister. Richard Locke III, and Nicholas J. Talley participated in the design, analysis, and writing of the manuscript. Alan R. Zinsmeister and Cathy D. Schleck provided the statistical analysis and assisted in writing the manuscript.
All authors have approved the final version of the manuscript.
References
- 1.Kowal P, Williams SR, Chatterji S. Challenge of ageing populations. Ageing alongside and outside EU borders. BMJ. 2011;343:d4885. doi: 10.1136/bmj.d4885. [DOI] [PubMed] [Google Scholar]
- 2.Fahy N, McKee M, Busse R, et al. How to meet the challenge of ageing populations. BMJ. 2011;342:d3815. doi: 10.1136/bmj.d3815. [DOI] [PubMed] [Google Scholar]
- 3.Bhutto A, Morley JE. The clinical significance of gastrointestinal changes with aging. Curr Opin Clin Nutr Metab Care. 2008;11:651–60. doi: 10.1097/MCO.0b013e32830b5d37. [DOI] [PubMed] [Google Scholar]
- 4.Grande L, Lacima G, Ros E, et al. Deterioration of esophageal motility with age: a manometric study of 79 healthy subjects. Am J Gastroenterol. 1999;94:1795–801. doi: 10.1111/j.1572-0241.1999.01208.x. [DOI] [PubMed] [Google Scholar]
- 5.Klingensmith WC, 3rd, Rhea KL, Wainwright EA, et al. The gastric emptying study with oatmeal: reference range and reproducibility as a function of age and sex. J Nucl Med Technol. 2010;38:186–90. doi: 10.2967/jnmt.110.077065. [DOI] [PubMed] [Google Scholar]
- 6.Wiskur B, Greenwood-Van Meerveld B. The aging colon: the role of enteric neurodegeneration in constipation. Curr Gastroenterol Rep. 2010;12:507–12. doi: 10.1007/s11894-010-0139-7. [DOI] [PubMed] [Google Scholar]
- 7.Claesson MJ, Jeffery IB, Conde S, et al. Gut microbiota composition correlates with diet and health in the elderly. Nature. 2012;488:178–84. doi: 10.1038/nature11319. [DOI] [PubMed] [Google Scholar]
- 8.Longstreth GF, Thompson WG, Chey WD, et al. Functional bowel disorders. Gastroenterology. 2006;130:1480–91. doi: 10.1053/j.gastro.2005.11.061. [DOI] [PubMed] [Google Scholar]
- 9.Agreus L, Svardsudd K, Talley NJ, et al. Natural history of gastroesophageal reflux disease and functional abdominal disorders: a population-based study. Am J Gastroenterol. 2001;96:2905–14. doi: 10.1111/j.1572-0241.2001.04680.x. [DOI] [PubMed] [Google Scholar]
- 10.Camilleri M, Cowen T, Koch TR. Enteric neurodegeneration in ageing. Neurogastroenterol Motil. 2008;20:418–29. doi: 10.1111/j.1365-2982.2008.01134.x. [DOI] [PubMed] [Google Scholar]
- 11.Tack J, Talley NJ, Camilleri M, et al. Functional gastroduodenal disorders. Gastroenterology. 2006;130:1466–79. doi: 10.1053/j.gastro.2005.11.059. [DOI] [PubMed] [Google Scholar]
- 12.Gururatsakul M, Holloway RH, Adam B, et al. The ageing gut: diminished symptom response to a standardized nutrient stimulus. Neurogastroenterol Motil. 22:246–e77. doi: 10.1111/j.1365-2982.2009.01413.x. [DOI] [PubMed] [Google Scholar]
- 13.Choung RS, Locke GR, 3rd, Schleck CD, et al. Cumulative incidence of chronic constipation: a population-based study 1988–2003. Aliment Pharmacol Ther. 2007;26:1521–8. doi: 10.1111/j.1365-2036.2007.03540.x. [DOI] [PubMed] [Google Scholar]
- 14.Choung RS, Locke GR, 3rd, Zinsmeister AR, et al. Epidemiology of slow and fast colonic transit using a scale of stool form in a community. Aliment Pharmacol Ther. 2007;26:1043–50. doi: 10.1111/j.1365-2036.2007.03456.x. [DOI] [PubMed] [Google Scholar]
- 15.Halder SL, Locke GR, 3rd, Schleck CD, et al. Natural history of functional gastrointestinal disorders: a 12-year longitudinal population-based study. Gastroenterology. 2007;133:799–807. doi: 10.1053/j.gastro.2007.06.010. [DOI] [PubMed] [Google Scholar]
- 16.Talley NJ, Fleming KC, Evans JM, et al. Constipation in an elderly community: a study of prevalence and potential risk factors. Am J Gastroenterol. 1996;91:19–25. [PubMed] [Google Scholar]
- 17.Talley NJ, O’Keefe EA, Zinsmeister AR, et al. Prevalence of gastrointestinal symptoms in the elderly: a population-based study. Gastroenterology. 1992;102:895–901. doi: 10.1016/0016-5085(92)90175-x. [DOI] [PubMed] [Google Scholar]
- 18.Talley NJ, Phillips SF, Melton J, 3rd, et al. A patient questionnaire to identify bowel disease. Ann Intern Med. 1989;111:671–4. doi: 10.7326/0003-4819-111-8-671. [DOI] [PubMed] [Google Scholar]
- 19.Talley NJ, Phillips SF, Wiltgen CM, et al. Assessment of functional gastrointestinal disease: the bowel disease questionnaire. Mayo Clin Proc. 1990;65:1456–79. doi: 10.1016/s0025-6196(12)62169-7. [DOI] [PubMed] [Google Scholar]
- 20.Talley NJ, Weaver AL, Zinsmeister AR, et al. Onset and disappearance of gastrointestinal symptoms and functional gastrointestinal disorders. Am J Epidemiol. 1992;136:165–77. doi: 10.1093/oxfordjournals.aje.a116483. [DOI] [PubMed] [Google Scholar]
- 21.Talley NJ, Weaver AL, Zinsmeister AR, et al. Functional constipation and outlet delay: a population-based study. Gastroenterology. 1993;105:781–90. doi: 10.1016/0016-5085(93)90896-k. [DOI] [PubMed] [Google Scholar]
- 22.Talley NJ, Zinsmeister AR, Van Dyke C, et al. Epidemiology of colonic symptoms and the irritable bowel syndrome. Gastroenterology. 1991;101:927–34. doi: 10.1016/0016-5085(91)90717-y. [DOI] [PubMed] [Google Scholar]
- 23.Melton LJ., 3rd History of the Rochester Epidemiology Project. Mayo Clin Proc. 1996;71:266–74. doi: 10.4065/71.3.266. [DOI] [PubMed] [Google Scholar]
- 24.Melton LJ., 3rd The threat to medical-records research. N Engl J Med. 1997;337:1466–70. doi: 10.1056/NEJM199711133372012. [DOI] [PubMed] [Google Scholar]
- 25.Attanasio V, Andrasik F, Blanchard EB, et al. Psychometric properties of the SUNYA revision of the Psychosomatic Symptom Checklist. J Behav Med. 1984;7:247–57. doi: 10.1007/BF00845390. [DOI] [PubMed] [Google Scholar]
- 26.O’Keefe EA, Talley NJ, Tangalos EG, et al. A bowel symptom questionnaire for the elderly. J Gerontol. 1992;47:M116–21. doi: 10.1093/geronj/47.4.m116. [DOI] [PubMed] [Google Scholar]
- 27.Locke GR, Talley NJ, Weaver AL, et al. A new questionnaire for gastroesophageal reflux disease. Mayo Clin Proc. 1994;69:539–47. doi: 10.1016/s0025-6196(12)62245-9. [DOI] [PubMed] [Google Scholar]
- 28.Reilly WT, Talley NJ, Pemberton JH, et al. Validation of a questionnaire to assess fecal incontinence and associated risk factors: Fecal Incontinence Questionnaire. Dis Colon Rectum. 2000;43:146–53. doi: 10.1007/BF02236971. discussion 153–4. [DOI] [PubMed] [Google Scholar]
- 29.Rey E, Locke GR, 3rd, Jung HK, et al. Measurement of abdominal symptoms by validated questionnaire: a 3-month recall timeframe as recommended by Rome III is not superior to a 1-year recall timeframe. Aliment Pharmacol Ther. 31:1237–47. doi: 10.1111/j.1365-2036.2010.04288.x. [DOI] [PubMed] [Google Scholar]
- 30.Locke GR, 3rd, Pemberton JH, Phillips SF. American Gastroenterological Association Medical Position Statement: guidelines on constipation. Gastroenterology. 2000;119:1761–6. doi: 10.1053/gast.2000.20390. [DOI] [PubMed] [Google Scholar]
- 31.Choung RS, Locke GR, Schleck CD, et al. A low response rate does not necessarily indicate non-response bias in gastroenterology survey research: a population-based study. Journal of Public Health. 2013;21:87–95. [Google Scholar]
- 32.Quigley EM, Locke GR, Mueller-Lissner S, et al. Prevalence and management of abdominal cramping and pain: a multinational survey. Aliment Pharmacol Ther. 2006;24:411–9. doi: 10.1111/j.1365-2036.2006.02989.x. [DOI] [PubMed] [Google Scholar]
- 33.Lagier E, Delvaux M, Vellas B, et al. Influence of age on rectal tone and sensitivity to distension in healthy subjects. Neurogastroenterol Motil. 1999;11:101–7. doi: 10.1046/j.1365-2982.1999.00145.x. [DOI] [PubMed] [Google Scholar]
- 34.Lasch H, Castell DO, Castell JA. Evidence for diminished visceral pain with aging: studies using graded intraesophageal balloon distension. Am J Physiol. 1997;272:G1–3. doi: 10.1152/ajpgi.1997.272.1.G1. [DOI] [PubMed] [Google Scholar]
- 35.Lautenbacher S, Kunz M, Strate P, et al. Age effects on pain thresholds, temporal summation and spatial summation of heat and pressure pain. Pain. 2005;115:410–8. doi: 10.1016/j.pain.2005.03.025. [DOI] [PubMed] [Google Scholar]
- 36.Huang HW, Wang WC, Lin CC. Influence of age on thermal thresholds, thermal pain thresholds, and reaction time. J Clin Neurosci. 17:722–6. doi: 10.1016/j.jocn.2009.10.003. [DOI] [PubMed] [Google Scholar]
- 37.Rayner CK, MacIntosh CG, Chapman IM, et al. Effects of age on proximal gastric motor and sensory function. Scand J Gastroenterol. 2000;35:1041–7. doi: 10.1080/003655200451153. [DOI] [PubMed] [Google Scholar]
- 38.Gomez-Pinilla PJ, Gibbons SJ, Sarr MG, et al. Changes in interstitial cells of cajal with age in the human stomach and colon. Neurogastroenterol Motil. 2011;23:36–44. doi: 10.1111/j.1365-2982.2010.01590.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Talley NJ, Zinsmeister AR, Melton LJ., 3rd Irritable bowel syndrome in a community: symptom subgroups, risk factors, and health care utilization. Am J Epidemiol. 1995;142:76–83. doi: 10.1093/oxfordjournals.aje.a117548. [DOI] [PubMed] [Google Scholar]
- 40.Robinson ME, Riley JL, 3rd, Myers CD, et al. Gender role expectations of pain: relationship to sex differences in pain. J Pain. 2001;2:251–7. doi: 10.1054/jpai.2001.24551. [DOI] [PubMed] [Google Scholar]
- 41.Sanoja R, Cervero F. Estrogen-dependent changes in visceral afferent sensitivity. Auton Neurosci. 153:84–9. doi: 10.1016/j.autneu.2009.07.001. [DOI] [PubMed] [Google Scholar]
- 42.Choung RS, Locke GR, 3rd, Zinsmeister AR, et al. Psychosocial distress and somatic symptoms in community subjects with irritable bowel syndrome: a psychological component is the rule. Am J Gastroenterol. 2009;104:1772–9. doi: 10.1038/ajg.2009.239. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Koloski NA, Boyce PM, Talley NJ. Somatization an independent psychosocial risk factor for irritable bowel syndrome but not dyspepsia: a population-based study. Eur J Gastroenterol Hepatol. 2006;18:1101–9. doi: 10.1097/01.meg.0000231755.42963.c6. [DOI] [PubMed] [Google Scholar]
- 44.Sayuk GS, Elwing JE, Lustman PJ, et al. High somatic symptom burdens and functional gastrointestinal disorders. Clin Gastroenterol Hepatol. 2007;5:556–62. doi: 10.1016/j.cgh.2006.11.024. [DOI] [PubMed] [Google Scholar]
- 45.Locke GR, 3rd, Zinsmeister AR, Fett SL, et al. Overlap of gastrointestinal symptom complexes in a US community. Neurogastroenterol Motil. 2005;17:29–34. doi: 10.1111/j.1365-2982.2004.00581.x. [DOI] [PubMed] [Google Scholar]