Abstract
OBJECTIVES:
To examine hospitalizations and length of stay (LOS) for infants aged <1 year in rural and urban counties, hypothesizing that infants living in rural counties experience significantly different hospital use compared with urban infants.
METHODS:
Birth certificates for infants born in California hospitals between 1993 and 2005 and surviving to discharge were linked to hospital discharge records and death certificates during the first year of life, resulting in a study population of >6.4 million. Hospitalizations, cumulative LOS, readmission rates, and mortality were compared by using univariate and multivariable analysis for infants living in small rural, large rural, small urban, and large urban counties. Odds of hospitalization and cumulative LOS were also examined for common infant diagnoses.
RESULTS:
Infants living in increasingly rural counties experienced decreasing rates of hospitalization and decreasing number of hospitalized days during the first year of life. Infants living in small rural counties experienced 370 hospital days per 1000 infants compared with 474 hospital days per 1000 infants living in large urban counties. In multivariable analysis, infants in large urban counties experienced increased odds of hospitalization (odds ratio: 1.20 [95% confidence interval: 1.06–1.36]) and increased hospitalized days (incidence risk ratio: 1.17 [95% confidence interval: 1.06–1.29]) compared with infants in small rural counties. For most common diagnoses, urban residence was associated with either increased odds of hospitalization or increased cumulative LOS.
CONCLUSIONS:
Infants living in rural California counties experienced decreased hospital utilization, including decreased hospitalization and decreased LOS, compared with infants living in urban counties.
KEY WORDS: hospitalization, infant, length of stay, readmission, rural, urban
What’s Known on This Subject:
Patients living in rural versus urban counties encounter different health care environments. Whether these differences result in different health care utilization for rural versus urban infants is not known.
What This Study Adds:
In this study, infants living in rural California counties were hospitalized less often than infants living in urban counties. Among those hospitalized, infants living in rural counties were hospitalized for fewer cumulative days than infants residing in urban counties.
Children living in rural communities encounter different health care environments than children living in urban communities, including differences in access to care1–5 and provider practices.6,7 Previous studies investigating whether these differences result in different hospital utilization found conflicting results for pediatric hospitalization rates8–11 and no data for pediatric length of stay (LOS), because LOS studies have examined rural hospitals rather than rural patients.12,13 Even less is known about hospital utilization among rural infants, with studies generally excluding the youngest of children. Given the relatively high rates of hospitalization during the first year of life, understanding hospitalization patterns for infants across communities is an important public health issue.
This study’s goal was to compare inpatient utilization data, including hospitalization and LOS, for infants aged <1 year in rural and urban communities. We also examined whether differences in hospital utilization were associated with readmissions after discharge or inpatient mortality. We hypothesized that infants living in rural settings would experience significantly different hospitalization rates and LOS compared with urban infants.
Methods
Study Population and Data Collection
Birth certificate data for all infants born in California between 1993 and 2005 were linked to death certificate data and discharge records for any hospitalization during the first year of life by the Office of Statewide Health Planning and Development by using previously described methods.14 More than 98% of records were successfully linked. This database has been the basis of multiple previous studies.15–18 Infants were excluded if they did not survive to discharge from birth hospitalization, if gestational age was <24 weeks or >42 weeks, or if birth weight was >5 standard deviations (SDs) from expected birth weight for gestational age due to concern for data error. Gestational age was determined by best estimation of the obstetrician as recorded on the birth certificate record. In total, 382 161 infants met these exclusion criteria. In addition, 10 582 infants with birth hospitalization exceeding 90 days were excluded to allow an adequate observational period before first birthday.
This study was approved by The Children’s Hospital of Philadelphia Institutional Review Board and the institutional review board of the Department of Health in California.
Variable and Outcomes Definitions
Outcomes
The primary outcome was any hospitalization between discharge from birth hospitalization and day 365 of life. Secondary outcomes included the cumulative time an infant was hospitalized after birth hospitalization during the first year of life; infant mortality; and readmission within 7, 14, and 28 days of discharge from previous nonbirth hospitalization. For clarity, “birth hospitalization” indicates birth hospitalization; “hospitalization” indicates any nonbirth hospitalization; and “readmission” indicates hospitalization occurring within specified commonly studied intervals after a nonbirth hospitalization. Infant mortality was abstracted from death certificate data.
Hospitalizations and cumulative LOS associated with the most common diagnoses in this population were examined, including bronchiolitis, cellulitis, convulsions/seizures, croup, dehydration and gastroenteritis, temperature instability, hyperbilirubinemia, pneumonia, pyloric stenosis (PS), gastroesophageal reflux (GER), sepsis, urinary tract infection (UTI), and viral illness. The Appendix lists International Classification of Diseases, Ninth Revision codes used to identify these conditions. These 13 diagnostic categories accounted for 63% of the principal diagnoses for all hospitalizations in the cohort. Hospitalization is nondiscretionary for 2 of these diagnoses (sepsis and PS), whereas the decision to hospitalize infants for the remaining conditions may include more subjective assessment of medical and social circumstances.19,20 This second group of diagnoses potentially overlaps with the concept of ambulatory care–sensitive hospitalizations, which have been studied as a marker for quality and accessibility of ambulatory care in the adult literature21–24 but have not been validated to the same degree for infants. For this reason, we focused instead on this more complete list of conditions derived from the most common hospitalizations within our study population.
Predictive Factors
Infant residential counties were categorized according to the United States Department of Agriculture 2003 Rural–Urban Continuum Codes,25 which categorize metropolitan areas according to size and rural areas according to size and proximity to metropolitan areas. For our analysis, counties were grouped into the following 4 categories: large urban (metropolitan area with population >1 million); small urban (metropolitan area with population <1 million); large rural (nonmetropolitan area with urban population >20 000); and small rural (nonmetropolitan area with urban population <20 000). Hospitalizations were analyzed based on the county in which each infant resided rather than the county in which the hospitalization occurred.
Additional predictive factors were included based on their association with increased hospitalization or increased potentially preventable hospitalization26–31 or as a marker of chronic illness. These factors included birth factors, such as multiple gestation birth, gestational age, and small for gestational age (SGA); maternal sociodemographic data, including age, race, education, parity, trimester of prenatal care initiation, insurance, and median income of the residential zip code; and infant gender.
Data Analysis
Analysis was performed by using Stata version 10 (Stata Corp, College Station, TX). For univariate analysis, the Kruskal-Wallis 1-way analysis of variance was used for continuous variables and the χ2 test for categorical variables. The χ2 test for trends was used to analyze univariate outcomes across county types. Statistical significance was set at <.05 after use of the Bonferroni correction for multiple comparisons. For multivariable analysis, we constructed logistic regression models to determine the odds that infants of different county types would experience ≥1 hospitalization during the first year of life after controlling for infant and maternal characteristics and for clustering by residential county using robust standard error (SE) calculation. Independent variables were included in the multivariable models if inclusion improved the likelihood ratio of the new model at a significance level of 10%32 or based on a priori determination of relevant variables. Among infants who were hospitalized, cumulative LOS was analyzed by using Poisson regression models. Data were analyzed for all hospitalizations as well as for specific diagnoses. The impact of specific events (Children’s Health Insurance Program [CHIP]) legislation, pneumococcal conjugate vaccine development, and new hyperbilirubinemia and UTI guidelines) on the risk of hospitalization and LOS was examined through the addition of interaction terms between time period after each event and geographic location. These interaction terms were reported if they resulted in a new model that was statistically different from the original base model at a .05 level.
Results
After exclusion criteria were applied, this study included 6 419 257 infants. Table 1 reports baseline characteristics at birth hospitalization discharge. Compared with infants in large and small urban areas, more infants in large and small rural counties were born to white mothers and received federal insurance.
TABLE 1.
Infant and Maternal Characteristics According to Rurality of County
| Characteristic | Small Rural (n = 37 183) | Large Rural (n = 59 949) | Small Urban (n = 1 337 509) | Large Urban (n = 4 984 616) | P Value |
|---|---|---|---|---|---|
| Gestational age, median (IQR), wk | 39 (38–40) | 39 (38–40) | 39 (38–40) | 39 (38–40) | .0001 |
| Gestational age, wk | <.001 | ||||
| 24–28 | 118 (0.3) | 271 (0.5) | 6069 (0.5) | 19 812 (0.4) | |
| 29–33 | 622 (1.7) | 1185 (2.0) | 32 564 (2.4) | 113 379 (2.3) | |
| 34–36 | 2563 (6.9) | 4471 (7.5) | 110 862 (8.3) | 397 506 (8.0) | |
| 37–42 | 33 880 (91.1) | 54 022 (90.1) | 1 188 014 (88.8) | 4 453 919 (89.4) | |
| Birth weight, median (IQR), g | 3402 (3078–3736) | 3430 (3090–3770) | 3400 (3062–3719) | 3374 (3040–3696) | .0001 |
| SGA | 3052 (8.2) | 4623 (7.7) | 107 378 (8.0) | 438 653 (8.8) | <.001 |
| Multiple gestation | 819 (2.2) | 1620 (2.7) | 33 622 (2.5) | 136 615 (2.7) | <.001 |
| Female infant | 18 207 (49.0) | 29 118 (48.6) | 653 109 (48.8) | 2 432 894 (48.8) | .583 |
| Maternal age <20 y | 5135 (13.8) | 7883 (13.2) | 182 190 (13.6) | 496 087 (9.95) | <.001 |
| Nonprimiparous mother | 23 361 (62.8) | 36 325 (60.6) | 846 962 (63.3) | 3 028 650 (60.8) | <.001 |
| Maternal parity, median (IQR), number | 2 (1–3) | 2 (1–3) | 2 (1–3) | 2 (1–3) | .0001 |
| Race | <.001 | ||||
| Hispanic | 6986 (18.8) | 9060 (15.1) | 610 848 (45.7) | 2 229 238 (44.7) | |
| White | 27 291 (73.4) | 46 559 (77.7) | 564 627 (42.2) | 1 707 501 (34.3) | |
| Other | 2906 (7.8) | 4330 (7.2) | 162 034 (12.1) | 1 047 877 (21.0) | |
| Maternal education | <.001 | ||||
| Completed high school or less | 24 291 (65.33) | 36 569 (61.0) | 857 888 (64.1) | 2 860 956 (57.4) | |
| Completed ≥1 y of college | 12 892 (34.7) | 23 380 (39.0) | 479 621 (35.9) | 2 123 660 (42.6) | |
| Trimester of prenatal care initiation | <.001 | ||||
| 1st | 28 616 (77.0) | 45 734 (76.3) | 1 057 136 (79.0) | 4 203 972 (84.3) | |
| 2nd | 6923 (18.6) | 10 944 (18.3) | 208 429 (15.6) | 606 652 (12.2) | |
| 3rd | 1644 (4.4) | 3271 (5.5) | 71 944 (5.4) | 173 992 (3.49) | |
| Insurance | <.001 | ||||
| Private | 15 614 (42) | 24 990 (41.7) | 625 270 (46.8) | 2 708 585 (54.4) | |
| Federal | 20 144 (54.2) | 31 745 (53.0) | 677 844 (50.7) | 2 120 521 (42.6) | |
| Uninsured | 1417 (3.8) | 3211 (5.4) | 34 209 (2.6) | 154 104 (3.1) | |
| Median income of infant neighborhood, median (IQR), $ | 34 012 | 33 793 | 38 711 | 45 137 | .0001 |
| (31 171–38 386) | (28 634–37 714) | (32 573–49 124) | (35 403–60 229) |
Data are presented as number (%), unless otherwise noted.
Overall Hospital Use
Table 2 reports hospitalization outcomes according to infant residence. Percentage of infants experiencing hospitalization decreased significantly as communities become more rural (9.8% of infants in large urban counties vs 8.9% in small rural counties; P < .0001). The additional 0.9% of infants hospitalized from large urban counties translated into 46 000 additional hospitalized infants over the study period. In addition to more hospitalizations, living in increasingly urban counties was associated with higher percentages of hospitalizations lasting ≥3 days (P < .0001).
TABLE 2.
Hospitalization, LOS, Readmissions, and Death
| Outcome | Small Rural | Large Rural | Small Urban | Large Urban |
|---|---|---|---|---|
| Among total population | n = 37 183 | n = 59 949 | n = 1 337 509 | n = 4 984 616 |
| Hospitalized, n (%)a | 3302 (8.9) | 5681 (9.5) | 138 258 (10.3) | 490 101 (9.8) |
| Cumulative length of stay >3 d, n (%)a | 1416 (3.8) | 2694 (4.5) | 71 154 (5.3) | 271 084 (5.4) |
| Death during Hospitalization, n (%) | 4 (0.01) | 9 (0.02) | 157 (0.01) | 719 (0.01) |
| No. of hospitalizations per 1000 infantsb | 106 | 113 | 127 | 119 |
| No. of hospital days per 1000 infantsb | 370 | 417 | 472 | 474 |
| Among those hospitalized | n = 3302 | n = 5681 | n = 138 258 | n = 490 101 |
| Days at home before first hospitalization, median (IQR)a | 38 (4–142) | 37 (4–139) | 54 (15–158) | 55 (16–163) |
| Cumulative length of stay >3 d, n (%)a | 1416 (42.9) | 2694 (47.4) | 71 154 (51.5) | 271 084 (55.3) |
| Cumulative LOS in days, median (IQR)a | 2 (1–4) | 2 (2–4) | 3 (2–4) | 3 (2–5) |
| Readmit within 7 d of discharge, n (%)a | 299 (9.1) | 494 (8.7) | 14 654 (10.6) | 47 767 (9.8) |
| Readmit within 14 d of discharge, n (%)a | 315 (9.5) | 526 (9.3) | 15 391 (11.1) | 50 209 (10.2) |
| Readmit within 28 d of discharge, n (%)a | 330 (10.0) | 560 (9.9) | 16 446 (11.9) | 53 744 (11.0) |
Rows where P value was significant at a 5% level based on χ2 test for trends.
Rows where no statistical test performed.
Despite fewer hospitalizations and fewer prolonged hospitalizations for infants living in more rural counties, there was no statistically significant trend in infant deaths for infants from rural versus urban areas. In addition, living in increasingly rural counties was associated with fewer readmissions within 7, 14, and 28 days of hospitalization compared with infants from more urban areas (P < .0001).
Overall, infants from large urban communities experienced 119 hospitalizations and 474 hospital days per 1000 infants. In contrast, infants from small rural communities experienced 106 hospitalizations and 370 hospital days per 1000 infants. Infants from small urban counties had hospitalization rates and hospital days similar to large urban counties, whereas infants from large rural counties experienced hospitalization rates and hospital days intermediate to rural and urban extremes.
When hospitalized, patients from small rural counties were usually hospitalized within small rural counties (51% of nonbirth hospitalizations), whereas almost all patients from large urban counties experiencing hospitalization were hospitalized within large urban counties (99.7% of nonbirth hospitalizations). Transfers to large urban hospitals (from any hospital including another large urban hospital) occurred in 7.1% of hospitalizations of infants from small rural areas compared with 5.4% of hospitalizations of infants from large urban areas.
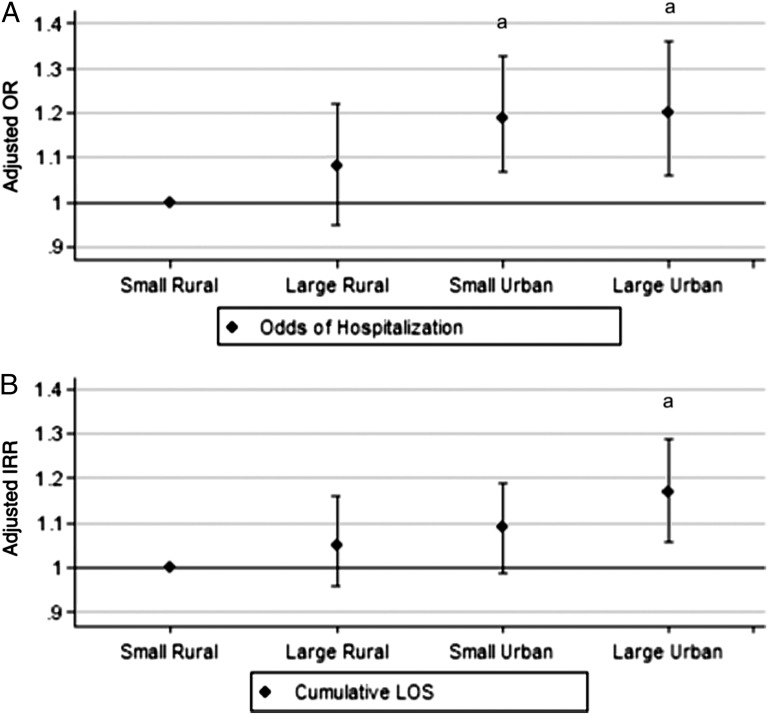
In multivariable analysis (Fig 1), living in increasingly urban counties was associated with increasing odds of hospitalization, with the largest odds ratio (OR) associated with living in large urban counties (OR: 1.20 [95% confidence interval [CI]: 1.06–1.36]). In multivariable analysis of LOS among those hospitalized, living outside of a rural county was associated with more hospital days, with infants from large urban settings experiencing 17% more hospital days than infants from small rural communities (95% CI: 1.06–1.29).
FIGURE 1.
Adjusted ORs for odds of hospitalization (A) and adjusted IRRs for cumulative LOS (B) according to county size. Results adjusted for gestational age, SGA, multiple gestations, gender, maternal age, race, parity, maternal education, insurance, neighborhood median income, and birth year, compared with small rural reference group after adjusting for clustering by residential county. aSignificant at 5% level after correcting for multiple comparisons through Bonferroni correction.
As a secondary analysis, infants from any rural county were compared with infants from any urban county; this combined group of rural infants still had decreased odds of hospitalization (OR: 0.88 [95% CI: 0.79–0.98]) and decreased cumulative LOS (incidence risk ratio [IRR]: 0.90 [95% CI: 0.85–0.96]) compared with the urban infants. We also explored a variable indicating birth hospitalization >7 days, which did not significantly change the association between geography and hospitalization risk or LOS.
Specific Diagnoses
For most diagnoses, the trend of increased hospitalizations and/or increased LOS for infants in increasingly urban areas persisted, although not always to a statistically significant degree (Fig 2). The increased odds of hospitalization for infants from large urban counties compared with small rural counties were most notable for cellulitis, dehydration, convulsions, GER, UTI, and viral infections. Large urban residence was associated with statistically significant increased LOS among infants hospitalized for dehydration, bronchiolitis, pneumonia, temperature instability, and hyperbilirubinemia compared with the small rural reference group.
FIGURE 2.
Adjusted ORs for odds of hospitalization and IRR for cumulative LOS of specific diagnoses in large urban compared with small rural areas. Results adjusted for gestational age, SGA, multiple gestations, gender, maternal age, race, parity, maternal education, insurance, neighborhood median income, and birth year, compared with small rural reference group after adjusting for clustering by residential county. aSignificant at 5% level after correcting for multiple comparisons through Bonferroni correction. Temp, temperature; Hyperbili, hyperbilirubinemia.
Compared with small rural counties, residence in large urban counties was associated with increased odds of hospitalization for sepsis (OR: 1.60 [95% CI: 1.17–2.20]) and PS (OR: 1.43 [95% CI: 1.02–1.99]), although this second value did not maintain statistical significance after adjusting for multiple comparisons. When hospitalized for either sepsis or PS, there was no significant difference in LOS for infants from large urban areas compared with the small rural reference group.
Living in large urban counties was associated with decreased odds of hospitalization for hyperbilirubinemia relative to infants in small rural counties (OR: 0.41 [95% CI: 0.30–0.56]). When hospitalized for hyperbilirubinemia, infants in large urban counties had increased LOS relative to infants in small rural counties.
In additional analysis, CHIP legislation interacted significantly with county type, with odds of hospitalization for infants from large urban counties being larger before CHIP (OR: 1.26 [95% CI: 1.07–1.47]) than after CHIP (OR: 1.16 [95% CI: 1.02–1.32]) relative to the rural reference group. Other studied events did not interact significantly with county type.
Discussion
In our study of >6 million infants born in California between 1993 and 2005, infants from small rural counties had decreased inpatient utilization, including lower hospitalization rates and fewer hospitalized days, than infants from large urban counties during their first year of life. Our findings persisted after controlling for several potential infant, maternal, and economic confounders. These findings were consistent with our hypothesis of different hospital utilization for infants from rural and urban counties and with 1 previous study of hospitalizations8 but are at odds with other studies.9–11 Possible explanations for differences from previous studies include our focus on infants or our study’s increased power. Our study differed in design from the few previous pediatric studies of LOS in rural areas12,13 by examining LOS according to residential county, focusing on infants, and using population rather than hospital data, which allowed analysis of hospitalization rates along with LOS. Examining specific diagnoses found that urban residence was associated with increased odds of hospitalization for many diagnoses and increased cumulative LOS for most of the remaining diagnoses. We did not identify adverse consequences of decreased inpatient utilization in rural patients such as increased mortality or increased readmissions relative to urban patients. Numerous factors may contribute to the observed differences, including access to care, quality of care, physician decision-making, and disease burden.
Access is a known issue in rural communities, with studies reporting decreased access to pediatricians1,2,5 and generalists3,4 in rural settings. However, studies of the impact of physician supply and distance from hospitals have not consistently shown an effect on hospitalization rates.12,21,23,33–39 Other dimensions of access include patient perception of access (which may be better in rural communities40 and may impact hospitalization rates23) and parental choice in accessing care (since patient care-seeking behavior has been associated with variations in care41 and location of presentation may influence hospitalization rates.42) In addition, financial access may influence odds of hospitalization, as suggested by our finding of decreased differences in odds of hospitalization after CHIP implementation. If barriers to needed care in rural areas alone accounted for decreased hospitalizations, we might expect the smaller cohort of hospitalized patients from rural areas to have more severe disease, potentially reflected in longer LOS or increased mortality. Our findings suggest that decreased ability to access care does not adequately explain decreased utilization in rural areas.
Quality of care at presentation site may also affect hospitalization rates.43 Studies have suggested that receipt of recommended ambulatory care may differ between rural and urban settings.6,7 We did not, however, observe significant change in the effect of geography on hospitalization risk or LOS after the introduction of specific management guidelines. Although unstudied, rural patients may experience increased continuity of care due to the more limited number of providers in their communities. If this were the case, we might expect reduced hospitalization and LOS because increased physician continuity has been associated with decreased emergency department utilization,44 increased patient satisfaction,45 and fewer avoidable hospitalizations,46,47 whereas increased fragmentation of inpatient care has been associated with longer LOS.48 Previous work has identified the difficulties of continuity of care when rural patients are hospitalized outside of their community,49,50 but less is known about continuity of outpatient and inpatient care within rural communities.
In addition, physicians may approach hospitalization decisions differently in rural versus urban communities. Previous work has shown that hospitalization thresholds can shift over time,51 and they may shift over space as well. In our study, patients were most commonly hospitalized in counties of sizes congruent with the patient’s own county. Although previous studies have suggested that physician practice style and risk attitudes may not contribute as much to different hospitalization rates as expected,41,52,53 the potential for admission thresholds and LOS to vary systematically across regions with different access to ambulatory and tertiary care (eg, urban versus rural settings) has not been adequately explored.
Finally, disease burden may actually differ between rural and urban communities. Prior studies of disease burden have reported increased severity of presentation in urban children with asthma54,55 and increased rates of rotavirus hospitalization in urban communities.56 Although consistent with the direction of our findings, it is difficult with these diagnoses to know whether increased hospitalizations reflects increased incidence, increased severity, or altered hospitalization thresholds. Within our study, PS and sepsis are 2 diagnoses in which every case should result in hospitalization, such that hospitalization rates should reflect disease burden without the influence of other factors. Our finding, then, of increased odds of hospitalization for infants living in urban counties for sepsis and PS does suggest increased incidence (although our finding for PS did not remain significant), especially in the setting of similar LOS among those hospitalized. Regional differences in incidence of PS have been noted previously,57,58 although not with the same urban/rural distinction.
Hyperbilirubinemia was the 1 diagnosis in which large urban residence was associated with decreased odds of hospitalization. Hyperbilirubinemia might behave differently than other diagnoses in rural versus urban communities due to different access to home nursing and home phototherapy, different breastfeeding rates, or different adherence to guidelines, although we were unable to find studies reporting rural–urban differences in these factors or a significant interaction with guideline release in our data. Of note, among those hospitalized, large urban residence was still associated with longer cumulative LOS.
This study has potential limitations that should be noted. First, earlier work has demonstrated different hospitalization rates even between multiple large urban centers.59 Thus, the degree to which our findings can be generalized beyond the study region is unclear. In particular, different racial and ethnic composition in other rural areas of the United States may limit generalizability of our findings. Generalizability may be further limited by our exclusion of infants with prolonged birth hospitalizations (>90 days). However, this study included >6 million infants born over 12 years within a large, geographically diverse state, and represents the largest current report of hospital utilization among rural and urban infants. In addition, administrative data sets have the potential for inaccuracies in coding, but we would not expect systematic bias in such errors. Also, although we were able to control for many infant and maternal characteristics at the level of the individual patient, this study did not include additional geographic characteristics, such as the location of pediatricians, family practitioners, hospitals, emergency departments, pediatric centers, and rural health centers, as this was beyond the scope of our analysis. Similarly, although we could determine transfers between hospitals after hospitalization, we did not have data on preceding clinic or emergency department visits or potential transfers between emergency departments before hospitalization. This additional information would help us better understand the flow of patients through rural and urban sites of care and further understand the observed differences in health care utilization among rural and urban patients.
Conclusions
Infants living in rural California counties experienced decreased hospital utilization, including decreased hospitalization and decreased LOS. Decreased inpatient utilization by rural infants persisted after controlling for potential confounders and was not associated with increased hospital mortality or increased readmission rates. Increasing rurality was associated with decreased hospital utilization for the majority of diagnoses, with either decreased odds of hospitalization or cumulative LOS observed. The reason for (and implications of) these differences requires further study.
APPENDIX.
ICD-9 Codes
| Diagnosis Category | ICD-9 Codes |
|---|---|
| Bronchiolitis | 466.0, 466.1, 466.11, 466.19, 480.1, 485, 490, 079.6 |
| Cellulitis | 681.00, 681.10, 681.9, 682.0, 682.1, 682.2, 682.3, 682.4, 682.5, 682.6, 682.7, 682.8, 682.9, 771.4 |
| Convulsions | 779.0, 780.3, 780.31, 780.39 |
| Croup | 464.4 |
| Dehydration/gastroenteritis | 008.8, 008.61, 276.5, 276.51, 276.52, 558.9, 775.5 |
| GER | 530.81 |
| Hyperbilirubinemia | 773.0, 773.1, 773.2, 774.0, 774.1, 774.2, 774.30, 774.39, 774.5, 774.6, 782.4 |
| Pneumonia | 480.2, 480.8, 480.9, 481, 482.0, 482.1, 482.2, 482.30, 482.31, 482.32, 482.39, 482.4, 482.40, 482.41, 482.49, 482.81, 482.82, 482.83, 482.89, 482.9, 483.0, 483.1, 483.8, 486, 487.0, 003.22 |
| PS | 537.0, 750.5 |
| Sepsis | 003.1, 038.0, 038.1, 038.1, 038.10, 038.10, 038.11, 038.19, 038.2, 038.3, 038.40, 038.41, 038.42, 038.43, 038.44, 038.49, 038.8, 038.9, 771.81, 771.83, 785.52, 790.7, 995.91, 995.92 |
| Temperature instability | 778.4, 780.6 |
| UTI | 590.10, 590.80, 599.0, 771.82 |
| Virus | 079.99, 465.9 |
ICD-9, International Classification of Diseases, Ninth Revision.
Acknowledgment
We acknowledge Corinne Ahlberg, MS, for her assistance with database management.
Glossary
- CHIP
Children’s Health Insurance Program
- CI
confidence interval
- GER
gastroesophageal reflux
- IRR
incidence risk ratio
- IQR
interquartile range
- LOS
length of stay
- OR
odds ratio
- PS
pyloric stenosis
- SGA
small for gestational age
- UTI
urinary tract infection
Footnotes
Dr Ray conceived and designed the study, analyzed and interpreted the data, wrote and revised the manuscript, and approved of the final version for publication; and Dr Lorch supervised study design, analysis, and interpretation; acquired the original data set; critically revised the manuscript; and approved of the final version for publication.
Dr Ray’s current affiliation is Division of General Academic Pediatrics, Children’s Hospital of Pittsburgh, Pittsburgh, PA
FINANCIAL DISCLOSURE: The authors have indicated they have no financial relationships relevant to this article to disclose.
FUNDING: This study was funded in part by the Maternal and Child Health Bureau (R40 MC05474-01-00) and the Agency for Healthcare Research and Quality (R01 HS 015696).
References
- 1.Randolph GD, Pathman DE. Trends in the rural-urban distribution of general pediatricians. Pediatrics. 2001;107(2). [DOI] [PubMed] [Google Scholar]
- 2.Melzer SM, Grossman DC, Rivara FP. Physician experience with pediatric inpatient care in Washington State. Pediatrics. 1996;97(1):65–70 [PubMed] [Google Scholar]
- 3.Hart LG, Salsberg E, Phillips DM, Lishner DM. Rural health care providers in the United States. J Rural Health. 2002;18(suppl):211–232 [DOI] [PubMed] [Google Scholar]
- 4.Himes CL, Rutrough TS. Differences in the use of health services by metropolitan and nonmetropolitan elderly. J Rural Health. 1994;10(2):80–88 [DOI] [PubMed] [Google Scholar]
- 5.Shipman SA, Lan J, Chang CH, Goodman DC. Geographic maldistribution of primary care for children. Pediatrics. 2011;127(1):19–27 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Rosenblatt RA, Baldwin LM, Chan L, et al. Improving the quality of outpatient care for older patients with diabetes: lessons from a comparison of rural and urban communities. J Fam Pract. 2001;50(8):676–680 [PubMed] [Google Scholar]
- 7.Bronstein JM, Johnson VA, Fargason CA, Jr. How rural physicians compare on cost and quality measures for Medicaid ambulatory care episodes. J Rural Health. 1997;13(2):126–135 [DOI] [PubMed] [Google Scholar]
- 8.Goodman DC, Stukel TA, Chang CH. Trends in pediatric asthma hospitalization rates: regional and socioeconomic differences. Pediatrics. 1998;101(2):208–213 [DOI] [PubMed] [Google Scholar]
- 9.Garg A, Probst JC, Sease T, Samuels ME. Potentially preventable care: ambulatory care-sensitive pediatric hospitalizations in South Carolina in 1998. South Med J. 2003;96(9):850–858 [DOI] [PubMed] [Google Scholar]
- 10.Knudson A, Casey M, Burlew M, Davidson G. Disparities in pediatric asthma hospitalizations. J Public Health Manag Pract. 2009;15(3):232–237 [DOI] [PubMed] [Google Scholar]
- 11.Laditka JN, Laditka SB, Probst JC. Health care access in rural areas: evidence that hospitalization for ambulatory care-sensitive conditions in the United States may increase with the level of rurality. Health Place. 2009;15(3):731–740 [DOI] [PubMed] [Google Scholar]
- 12.Lorch SA, Zhang X, Rosenbaum PR, Evan-Shoshan O, Silber JH. Equivalent lengths of stay of pediatric patients hospitalized in rural and nonrural hospitals. Pediatrics. 2004;114(4). Available at: www.pediatrics.org/cgi/content/full/114/4/e400 [DOI] [PubMed] [Google Scholar]
- 13.Odetola FO, Gebremariam A, Freed GL. Patient and hospital correlates of clinical outcomes and resource utilization in severe pediatric sepsis. Pediatrics. 2007;119(3):487–494 [DOI] [PubMed] [Google Scholar]
- 14.Herrchen B, Gould JB, Nesbitt TS. Vital statistics linked birth/infant death and hospital discharge record linkage for epidemiological studies. Comput Biomed Res. 1997;30(4):290–305 [DOI] [PubMed] [Google Scholar]
- 15.Goyal NK, Fager C, Lorch SA. Adherence to discharge guidelines for late-preterm newborns. Pediatrics. 2011;128(1):62–71 [DOI] [PubMed] [Google Scholar]
- 16.Srinivas SK, Fager C, Lorch SA. Evaluating risk-adjusted cesarean delivery rate as a measure of obstetric quality. Obstet Gynecol. 2010;115(5):1007–1013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Tucker Edmonds B, Fager C, Srinivas S, Lorch S. Predictors of cesarean delivery for periviable neonates. Obstet Gynecol. 2011;118(1):49–56 [DOI] [PubMed] [Google Scholar]
- 18.Tucker Edmonds B, Fager C, Srinivas S, Lorch SA. Racial and ethnic differences in use of intubation for periviable neonates. Pediatrics. 2011;127(5). Available at: www.pediatrics.org/cgi/content/full/127/5/e1120 [DOI] [PubMed] [Google Scholar]
- 19.American Academy of Pediatrics Subcommittee on Diagnosis and Management of Bronchiolitis . Diagnosis and management of bronchiolitis. Pediatrics. 2006;118(4):1774–1793 [DOI] [PubMed] [Google Scholar]
- 20.Bradley JS, Byington CL, Shah SS, et al. Pediatric Infectious Diseases Society and the Infectious Diseases Society of America . The management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clin Infect Dis. 2011;53(7):e25–e76 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Basu J, Friedman B, Burstin H. Primary care, HMO enrollment, and hospitalization for ambulatory care sensitive conditions: a new approach. Med Care. 2002;40(12):1260–1269 [DOI] [PubMed] [Google Scholar]
- 22.Homer CJ, Szilagyi P, Rodewald L, et al. Does quality of care affect rates of hospitalization for childhood asthma? Pediatrics. 1996;98(1):18–23 [PubMed] [Google Scholar]
- 23.Bindman AB, Grumbach K, Osmond D, et al. Preventable hospitalizations and access to health care. JAMA. 1995;274(4):305–311 [PubMed] [Google Scholar]
- 24.Parchman ML, Culler S. Primary care physicians and avoidable hospitalizations. J Fam Pract. 1994;39(2):123–128 [PubMed] [Google Scholar]
- 25.United States Department of Agriculture. 2003 Rural-Urban Continuum Codes. Available at: www.ers.usda.gov/Data/RuralUrbanContinuumCodes/. Accessed October 14, 2010
- 26.Weissman JS, Gatsonis C, Epstein AM. Rates of avoidable hospitalization by insurance status in Massachusetts and Maryland. JAMA. 1992;268(17):2388–2394 [PubMed] [Google Scholar]
- 27.Basu J, Friedman B, Burstin H. Managed care and preventable hospitalization among Medicaid adults. Health Serv Res. 2004;39(3):489–510 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Howard DL, Hakeem FB, Njue C, Carey T, Jallah Y. Racially disproportionate admission rates for ambulatory care sensitive conditions in North Carolina. Public Health Rep. 2007;122(3):362–372 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Pappas G, Hadden WC, Kozak LJ, Fisher GF. Potentially avoidable hospitalizations: inequalities in rates between US socioeconomic groups. Am J Public Health. 1997;87(5):811–816 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Chamberlain JM, Joseph JG, Patel KM, Pollack MM. Differences in severity-adjusted pediatric hospitalization rates are associated with race/ethnicity. Pediatrics. 2007;119(6). Available at: www.pediatrics.org/cgi/content/full/119/6/e1319 [DOI] [PubMed] [Google Scholar]
- 31.Agabiti N, Pirani M, Schifano P, et al. Italian Study Group on Inequalities in Health Care . Income level and chronic ambulatory care sensitive conditions in adults: a multicity population-based study in Italy. BMC Public Health. 2009;9:457. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Sun GW, Shook TL, Kay GL. Inappropriate use of bivariable analysis to screen risk factors for use in multivariable analysis. J Clin Epidemiol. 1996;49(8):907–916 [DOI] [PubMed] [Google Scholar]
- 33.Laditka JN, Laditka SB, Probst JC. More may be better: evidence of a negative relationship between physician supply and hospitalization for ambulatory care sensitive conditions. Health Serv Res. 2005;40(4):1148–1166 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Grumback K, Vranizan K, Bindman AB. Physician supply and access to care in urban communities. Health Aff (Millwood). 1997;16(1):71–86 [DOI] [PubMed] [Google Scholar]
- 35.Friedman B, Basu J. Health insurance, primary care, and preventable hospitalization of children in a large state. Am J Manag Care. 2001;7(5):473–481 [PubMed] [Google Scholar]
- 36.Probst JC, Laditka JN, Laditka SB. Association between community health center and rural health clinic presence and county-level hospitalization rates for ambulatory care sensitive conditions: an analysis across eight US states. BMC Health Serv Res. 2009;9:134. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Epstein AJ. The role of public clinics in preventable hospitalizations among vulnerable populations. Health Serv Res. 2001;36(2):405–420 [PMC free article] [PubMed] [Google Scholar]
- 38.Goodman DC, Fisher ES, Gittelsohn A, Chang CH, Fleming C. Why are children hospitalized? The role of non-clinical factors in pediatric hospitalizations. Pediatrics. 1994;93(6 pt 1):896–902 [PubMed] [Google Scholar]
- 39.Henneman PL, Garb JL, Capraro GA, Li H, Smithline HA, Wait RB. Geography and travel distance impact emergency department visits. J Emerg Med. 2011;40(3):333–339 [DOI] [PubMed] [Google Scholar]
- 40.Stearns SC, Slifkin RT, Edin HM. Access to care for rural Medicare beneficiaries. J Rural Health. 2000;16(1):31–42 [DOI] [PubMed] [Google Scholar]
- 41.Escarce JJ. Would eliminating differences in physician practice style reduce geographic variations in cataract surgery rates? Med Care. 1993;31(12):1106–1118 [DOI] [PubMed] [Google Scholar]
- 42.Chamberlain JM, Patel KM, Pollack MM. Association of emergency department care factors with admission and discharge decisions for pediatric patients. J Pediatr. 2006;149(5):644–649 [DOI] [PubMed] [Google Scholar]
- 43.Lorch SA, Baiocchi M, Silber JH, Even-Shoshan O, Escobar GJ, Small DS. The role of outpatient facilities in explaining variations in risk-adjusted readmission rates between hospitals. Health Serv Res. 2010;45(1):24–41 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Ionescu-Ittu R, McCusker J, Ciampi A, et al. Continuity of primary care and emergency department utilization among elderly people. CMAJ. 2007;177(11):1362–1368 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Donahue KE, Ashkin E, Pathman DE. Length of patient-physician relationship and patients’ satisfaction and preventive service use in the rural south: a cross-sectional telephone study. BMC Fam Pract. 2005;6:40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Cheng SH, Chen CC, Hou YF. A longitudinal examination of continuity of care and avoidable hospitalization: evidence from a universal coverage health care system. Arch Intern Med. 2010;170(18):1671–1677 [DOI] [PubMed] [Google Scholar]
- 47.Tom JO, Tseng CW, Davis J, Solomon C, Zhou C, Mangione-Smith R. Missed well-child care visits, low continuity of care, and risk of ambulatory care-sensitive hospitalizations in young children. Arch Pediatr Adolesc Med. 2010;164(11):1052–1058 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Epstein K, Juarez E, Epstein A, Loya K, Singer A. The impact of fragmentation of hospitalist care on length of stay. J Hosp Med. 2010;5(6):335–338 [DOI] [PubMed] [Google Scholar]
- 49.Farrell SP, Koch JR, Blank M. Rural and urban differences in continuity of care after state hospital discharge. Psychiatr Serv. 1996;47(6):652–654 [DOI] [PubMed] [Google Scholar]
- 50.Biem HJ, Hadjistavropoulos H, Morgan D, Biem HB, Pong RW. Breaks in continuity of care and the rural senior transferred for medical care under regionalisation. Int J Integr Care. 2003;3:e03. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Russo MJ, McConnochie KM, McBride JT, Szilagyi PG, Brooks AM, Roghmann KJ. Increase in admission threshold explains stable asthma hospitalization rates. Pediatrics. 1999;104(3 pt 1):454–462 [DOI] [PubMed] [Google Scholar]
- 52.Komaromy M, Lurie N, Osmond D, Vranizan K, Keane D, Bindman AB. Physician practice style and rates of hospitalization for chronic medical conditions. Med Care. 1996;34(6):594–609 [DOI] [PubMed] [Google Scholar]
- 53.Baldwin RL, Green JW, Shaw JL, et al. Physician risk attitudes and hospitalization of infants with bronchiolitis. Acad Emerg Med. 2005;12(2):142–146 [DOI] [PubMed] [Google Scholar]
- 54.Bai Y, Hillemeier MM, Lengerich EJ. Racial/ethnic disparities in symptom severity among children hospitalized with asthma. J Health Care Poor Underserved. 2007;18(1):54–61 [DOI] [PubMed] [Google Scholar]
- 55.McConnochie KM, Russo MJ, McBride JT, Szilagyi PG, Brooks AM, Roghmann KJ. Socioeconomic variation in asthma hospitalization: excess utilization or greater need? Pediatrics. 1999;103(6). Available at: www.pediatrics.org/cgi/content/full/103/6/e75. [DOI] [PubMed] [Google Scholar]
- 56.Bucher B, Aebi C. Population-based epidemiology of rotavirus hospitalisations in Switzerland. Swiss Med Wkly. 2006;136(45–46):726–731 [DOI] [PubMed] [Google Scholar]
- 57.Hedbäck G, Abrahamsson K, Husberg B, Granholm T, Odén A. The epidemiology of infantile hypertrophic pyloric stenosis in Sweden 1987-96. Arch Dis Child. 2001;85(5):379–381 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.To T, Wajja A, Wales PW, Langer JC. Population demographic indicators associated with incidence of pyloric stenosis. Arch Pediatr Adolesc Med. 2005;159(6):520–525 [DOI] [PubMed] [Google Scholar]
- 59.Perrin JM, Homer CJ, Berwick DM, Woolf AD, Freeman JL, Wennberg JE. Variations in rates of hospitalization of children in three urban communities. N Engl J Med. 1989;320(18):1183–1187 [DOI] [PubMed] [Google Scholar]