Abstract
Objective. To analyse the prevalence of GAD and other anxiety disorders, as well as sensitivity and specificity of GAD-7 among high utilizers of health care. Setting. Four municipal health centres in Northern Finland. Subjects. A psychiatric interview was conducted for 150 high utilizers of health care. Main outcome measures. Prevalence of GAD as well as sensitivity and specificity of GAD-7. Results. The prevalence of GAD was 4% in this study group of Finnish high utilizers of health care. The sensitivity of GAD-7 was 100.0% (95% CI 54.1–100.0) and the specificity of GAD-7 was 82.6% (95% CI 75.4–88.4) with a cut-off point of 7 or more. Conclusion. GAD is rather common among high utilizers of primary care, although the prevalence of 4% is lower than that previously reported. GAD-7 is a valid and useful tool for detecting GAD among primary health care patients.
Key Words: Anxiety disorders, Finland, generalized anxiety disorder, general practice, high utilizers of health care, panic disorder, screening
Generalized anxiety disorder (GAD) is one of the most common psychiatric disorders in the general population associated with high use of health care services.
The prevalence of GAD was 4% in this study group of Finnish high utilizers of health care.
The Finnish translations of GAD-7 and GAD-2 are valid and useful tools for screening GAD among the primary health care patients.
Introduction
Generalized anxiety disorder (GAD) is highly prevalent in the general population with a current prevalence of 2–3% and a lifetime prevalence of over 5% [1–3]. According to international studies, GAD is especially frequent among primary care attenders with an 8% prevalence [3,4]. In Finland, the age-standardized prevalence rate of GAD among primary health care patients has been reported to be 4.1% for males and 7.1% for females [5]. Patients with GAD often present with somatic and sleeping problems and only rarely complain of anxiety symptoms directly, which makes detecting of this disease challenging [1]. Therefore, it is no surprise that GAD is poorly detected by health care professionals [6]. Earlier studies have shown patients with GAD to have a high rate of primary care visits [6]. In an American primary care study, 51% of high utilizers were identified as distressed by their physician, or had elevated scores on the SCL (Symptom Checklist-90-R) anxiety and depression scales or SCL somatization scale. Among these distressed high utilizers, 21.8% had GAD based on the DSM-III-R Diagnostic Interview Schedule [7].
A seven-item generalized anxiety disorder scale (GAD-7) instrument has been shown to be a valid and efficient tool for the screening of GAD with a sensitivity of 89% and specificity of 82% [8]. GAD-7 and GAD-2, a short version of the tool comprising of the first two questions of GAD-7, has been validated in different populations and patient groups [8–15]. Both GAD-7 and GAD-2 have also been efficient in screening for other anxiety disorders, including panic disorder, posttraumatic stress disorder, and social anxiety disorder, although results for GAD have been most convincing [10].
Our aim was to investigate the prevalence of GAD and other anxiety disorders among Finnish primary care high utilizers. Secondly we aimed to study the sensitivity and specificity of the Finnish translation of GAD-7.
Material and methods
Study sample
The study was conducted in four municipal health centres (Ii, Pudasjärvi, Utajärvi, Vaala) in Northern Finland.
The data on high utilizers of health care were collected retrospectively from the medical records of municipal health centres and medical reports from outpatient visits to Oulu University Hospital (providing secondary health care facilities for all of the municipal health centres participating in this study) before two years of study in 2006–2008. The patients’ inclusion criteria were being at least 18 years of age and having ≥ 8 visits per year to the general practitioner (GP) in the local health centre or ≥ 4 visits per year to the university hospital. The total number of all frequent attenders (FA) in the selected health centres during 1 August 2006–31 July 2008 was 3319 (see Figure 1).
Figure 1.

Flow chart demonstrating participation in the study.
Exclusion criteria included visits due to pregnancy or delivery, serial treatment for the same illness, terminal hospice, cancer palliative care, psychotic illness, dementia, mental retardation, inability to give informed consent, and other study intervention at the same time or just prior to this study.
All the participating health centres had a nurse as a case manager, who telephoned the identified FA and invited him/her to a consultation. The case manager verified patients’ eligibility for the study, requested their written informed consent for the study, and helped in filling in a semi-structured postal questionnaire, which was sent to the participants in October 2008 to May 2009.
The group for the case management intervention consisted of 286 patients (Ii = 61, Pudasjärvi = 90, Utajärvi = 56, Vaala = 79). In 2012, case managers called the patients still living in the area and asked about their willingness to participate in a psychiatric interview. Before the clinical interview, a new written informed consent was obtained and patients filled in the Finnish translation of the seven-item generalized anxiety disorder scale (GAD-7) (8), as well as a self-questionnaire concerning their lifetime psychiatric diagnoses and medications. A trained general practitioner carried out Mini International Neuropsychiatric Interview 5.0.0 Finnish version (MINI) with those 150 patients who gave written informed consent.
The group of patients attending the MINI interview did not differ significantly from the group not attending the interview regarding the following variables carried out earlier during the whole study project: quality of life measured by 15D, hypochondria measured by the Whiteley Index (WI), daily functioning measured by the Frenchay Activities Index (FAI), somatization measured by the somatization scale of the Symptom Checklist-90-R, orientation measured by the Sense of Coherence Scale (SOC), and mood measured by Raitasalo's modification of the short form of the Beck Depression Inventory (RBDI).
GAD-7 is a brief self-questionnaire developed based on the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) symptom criteria for GAD (8). It asks how often the patient has been bothered by seven different symptoms of anxiety during the last two weeks with response options such as: “not at all”, “several days”, “more than half the days”, and “nearly every day” scored as 0, 1, 2, and 3, respectively (8). The Finnish translation of GAD-7 has been done by Finnish psychiatry professionals.
Statistical methods
Results were expressed as means with standard deviation (SD) and 95% confidence intervals (CIs), and as medians with interquartile range (IQR). Statistical comparison between the groups was performed by t-test or chi-squared test, when appropriate.
Receiver-operating characteristic (ROC) curves were constructed to obtain the area under the curve (AUC), which is a criterion for test quality. We defined the best cut-off value as the value with the highest accuracy that maximizes Youden's index. Sensitivity, specificity, positive predictive value, likelihood ratio, Youden's index, and their 95% CI values were calculated.
Results
Demographic characteristics of the study population are presented in Table I. Our study population consisted of 46 (30.7%) males and 104 (69.3%) females. The mean age of our study population was 62.7 (SD 13.0) years. The prevalence of GAD according to the DSM-IV (obtained by the MINI) among our study population was 4.0% (1.5–8.5). According to patient questionnaires enquiring about lifetime psychiatric diagnoses, none of these GAD diagnoses was previously detected. The prevalence of panic disorder and other anxiety disorders was 6.7 (3.2–11.9) and 6.7 (3.2–11.9), respectively.
Table I.
Demographic characteristics of study population (n = 150).
| Demographic characteristic | n | % |
| Sex: | ||
| Male | 46 | 30.7 |
| Female | 104 | 69.3 |
| Education: | ||
| Less than comprehensive school | 16 | 10.8 |
| Comprehensive school | 57 | 38.5 |
| Matriculation examination | 2 | 1.4 |
| Vocational examination | 52 | 35.1 |
| College | 20 | 13.5 |
| Academic degree | 1 | 0.7 |
| Occupation: | ||
| Entrepreneur | 9 | 6.0 |
| Farmer | 22 | 14.8 |
| Employee | 95 | 63.8 |
| Senior salaried employee | 16 | 10.7 |
| Student or domestic work | 7 | 4.7 |
| Working status: | ||
| Full-time occupation | 27 | 18.0 |
| Part-time occupation | 3 | 2.0 |
| Sick leave | 8 | 5.3 |
| Disability pension | 36 | 24.0 |
| Other pension | 60 | 40.0 |
| Unemployed | 9 | 6.0 |
| Student | 3 | 2.0 |
| Other | 4 | 2.7 |
Table II presents the measures of validity (sensitivity, specificity, and positive likelihood ratios) for different cut-off points of the GAD-7 and GAD-2 in patients with GAD, panic disorder, and other anxiety disorders. In GAD, Youden's index was the highest (0.83) for the cut-off point 7 or more for GAD-7. The sensitivity and specificity parameters for this cut-off point were 100.0% (95% CI 54.1%–100%) and 82.6% (95% CI 75.4%–88.4%), respectively; its positive likelihood ratio was 5.8 (95% CI 4.0–8.2).
Table II.
Sensitivity, specificity, and positive likelihood ratio of the Generalized Anxiety Disorder-7 (GAD-7) and GAD-2 scales.
| Cut-off point | Generalized anxiety disorder (n = 6 [4.0%]) |
Panic disorder (n = 10 [6.7%]) |
Other anxiety disorder (n = 10 [6.7%]) |
| GAD-7 score | |||
| ≥ 5 | |||
| Sensitivity (95% CI) | 1.00 (0.54–1.00) | 0.70 (0.35–0.94) | 0.80 (0.44–0.98) |
| Specificity (95% CI) | 0.73 (0.65–0.80) | 0.73 (0.65–0.80) | 0.74 (0.66–0.81) |
| Positive LR (95% CI) | 3.69 (2.82–4.83) | 2.58 (1.58–4.20) | 3.03 (2.00–4.59) |
| ≥ 6 | |||
| Sensitivity (95% CI) | 1.00 (0.54–1.00) | 0.70 (0.35–0.93) | 0.70 (0.35–0.93) |
| Specificity (95% CI) | 0.79 (0.72–0.86) | 0.79 (0.72–0.86) | 0.79 (0.72–0.86) |
| Positive LR (95% CI) | 4.80 (3.49–6.60) | 3.38 (2.01–5.68) | 3.38 (2.01–5.68) |
| ≥ 7 | |||
| Sensitivity (95% CI) | 1.00 (0.54–1.00) | 0.60 (0.26–0.88) | 0.60 (0.26–0.88) |
| Specificity (95% CI) | 0.83 (0.75–0.88) | 0.82 (0.75–0.88) | 0.82 (0.75–0.88) |
| Positive LR (95% CI) | 5.76 (4.03–8.23) | 3.36 (1.81–6.24) | 3.36 (1.81–6.24) |
| ≥ 8 | |||
| Sensitivity (95% CI) | 0.83 (0.36–0.99) | 0.40 (0.12–0.74) | 0.50 (0.19–0.81) |
| Specificity (95% CI) | 0.88 (0.82–0.93) | 0.87 (0.80–0.92) | 0.88 (0.81–0.93) |
| Positive LR (95% CI) | 7.06 (3.98–12.50) | 3.11 (1.30–7.45) | 4.12 (1.92–8.83) |
| ≥ 9 | |||
| Sensitivity (95% CI) | 0.83 (0.36–0.99) | 0.40 (0.12–0.74) | 0.40 (0.12–0.74) |
| Specificity (95% CI) | 0.94 (0.89–0.97) | 0.93 (0.87–0.97) | 0.93 (0.87–0.97) |
| Positive LR (95% CI) | 13.3 (6.45–27.6) | 5.60 (2.13–14.70) | 5.60 (2.13–14.70) |
| ≥ 10 | |||
| Sensitivity (95% CI) | 0.67 (0.22–0.96) | 0.40 (0.12–0.74) | 0.40 (0.12–0.74) |
| Specificity (95% CI) | 0.95 (0.90–0.98) | 0.95 (0.90–0.98) | 0.95 (0.90–0.98) |
| Positive LR (95% CI) | 13.7 (5.48–34.3) | 8.00 (2.81–22.80) | 8.00 (2.81–22.80) |
| GAD-2 score | |||
| ≥ 2 | |||
| Sensitivity (95% CI) | 0.83 (0.36–0.99) | 0.50 (0.19–0.81) | 0.60 (0.26–0.88) |
| Specificity (95% CI) | 0.75 (0.67–0.82) | 0.74 (0.66–0.81) | 0.75 (0.67–0.82) |
| Positive LR (95% CI) | 3.33 (2.11–5.26) | 1.94 (0.98–3.84) | 2.40 (1.34–4.29) |
| ≥ 3 | |||
| Sensitivity (95% CI) | 0.83 (0.36–0.99) | 0.30 (0.07–0.65) | 0.20 (0.03–0.56) |
| Specificity (95% CI) | 0.90 (0.84–0.95) | 0.89 (0.82–0.93) | 0.88 (0.81–0.93) |
| Positive LR (95% CI) | 8.57 (4.64–15.80) | 2.63 (0.92–7.52) | 1.65 (0.44–6.15) |
| ≥ 4 | |||
| Sensitivity (95% CI) | 0.67 (0.22–0.96) | 0.20 (0.03–0.56) | 0.10 (0.03–0.45) |
| Specificity (95% CI) | 0.95 (0.90–0.98) | 0.94 (0.88–0.97) | 0.93 (0.87–0.97) |
| Positive LR (95% CI) | 13.7 (5.48–34.30) | 3.11 (0.78–12.50) | 1.40 (0.20–9.87) |
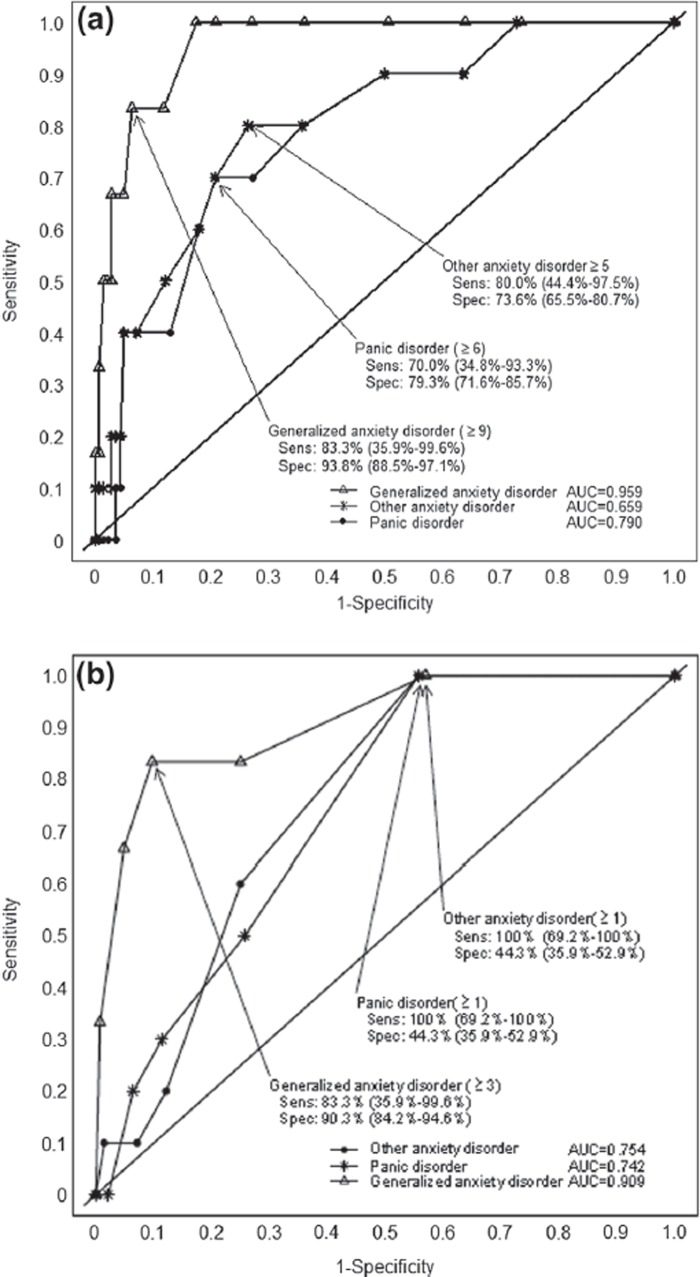
In panic disorder and other anxiety disorders, Youden's index was the highest (0.49 and 0.53, respectively) for the cut-off points 6 and 5, respectively. In panic disorder, the sensitivity and specificity parameters for this cut-off point of 6 or more were 70.0% (95% CI 34.8%–93.3%) and 79.3% (95% CI 71.6%–85.7%), respectively. Its positive likelihood ratio was 3.4 (95% CI 2.01–5.68). The sensitivity and specificity for other anxiety disorders with the cut-off point of 5 or more were 80.0% (95% CI 44.4%–97.5%), 73.6% (95% CI 65.5%–80.7%), respectively. The positive likelihood ratio was 3.0 (95% CI 2.00–4.59).
For the GAD-2 scale, Youden's index was highest with a cut-off point ≥ 3 in GAD, ≥ 1 in panic disorder, and ≥ 1 in other anxiety disorders. The corresponding sensitivity, specificity, and positive likelihood ratios are presented in Table II.
In ROC analysis (Figure 2a), for GAD-7, the area under the curve in GAD, panic disorder, and other anxiety disorders was 0.96 (95% CI 0.91–1.00), 0.79 (95% CI 0.65–9.93), and 0.81 (95% CI 0.67–0.95), respectively. The corresponding figures for GAD-2 were 0.91 (95% CI 0.78-1.0), 0.74 (95% CI 0.63–0.85), and 0.75 (95% CI 0.65–0.86), respectively (Figure 2b). Table III summarises this data.
Figure 2.
ROC for GAD, panic disorder and other anxiety disorder using a) GAD-7 and b) GAD-2.
Table III.
Comparison of Generalized Anxiety Disorder (GAD)-7 and (GAD)-2 scales by receiving-operating characteristic curve analysis.
| AUC (95% CI) | Comparison of GAD-7 and GAD-2 AUC | |||
| Anxiety disorder | GAD-7 | GAD-2 | Chi-square | p-value |
| Generalized anxiety disorder | 0.96 (0.91–1.00) | 0.91 (0.78–1.00) | 1.28 | 0.26 |
| Panic disorder | 0.79 (0.65–0.93) | 0.74 (0.63–0.85) | 0.98 | 0.32 |
| Other anxiety disorder | 0.81 (0.67–0.95) | 0.75 (0.65–0.86) | 0.73 | 0.39 |
Discussion
Statement of principal findings
To the best of our knowledge, this was the first study investigating the prevalence of GAD in primary care in Finland by using a structured and validated psychiatric interview (MINI). The prevalence of GAD was 4%. It should be noted that all of the GAD diagnoses were undetected according to the self-questionnaires. We also showed that GAD-7 and GAD-2 are valid instruments for detecting GAD in primary health care patients.
Strengths and weaknesses of the study
The strength of our study was that it was among the first globally investigating the prevalence of GAD among high utilizers of health care. Second, the diagnoses were based on a psychiatric interview with the help of a semi-structured and validated instrument (MINI). What is more, this study also has practical implications by showing the validity of the Finnish version of GAD-7 as a screening tool for GAD and other anxiety disorders among primary care patients.
Our study also has some limitations. A small sample size limits the generalization of our results. Not all the patients from the original sample of 286 high utilizers participated in the psychiatric interview. It is notable, however, that the patients not attending the psychiatric interview do not differ significantly from our final study population with regard to variables such as quality of life, somatization, mood, and daily functioning. Therefore, the group of patients included in the psychiatric interviews is representative of the total sample of 286 patients.
The health care utilization data were determined four years prior to psychiatric interviews, which means that not necessarily the whole study population were high utilizers at the point of interview. However, earlier studies indicate that up to 40% of high utilizers of health care still remain high utilizers in the following year (16).
Comparison with existing literature
Earlier studies indicated a higher prevalence of GAD than that observed in this investigation because in a European study primary care attenders have been reported to have a prevalence of 8% [3,4]. In Finland, the prevalence of current GAD among primary care attenders was 4.1% for males and 7.1% for females in an earlier study based on self-questionnaires [5]. In a population study, the 12-month prevalence of GAD in Finland was 1.3% based on CIDI interview [17].
Only a few earlier studies exist investigating the prevalence of GAD specifically among high utilizers of health care, and major methodological differences make comparison of these difficult. An American study investigated the prevalence of GAD among distressed high utilizers of health care and reported a prevalence of 21.8% for GAD [7]. The high prevalence is explained by their approach of focusing only on distressed high utilizers of health care. A Canadian study based on the self-reported worry and anxiety questionnaire (WAQ) showed that patients with five or more yearly physician consultations were 3.95 times more likely to have positive results for GAD with a rate of 35.2% (18). Our study was based on a structured psychiatric interview giving a reliable diagnosis rather than symptoms only. The detected prevalence of 4% in this study is close to what had been detected earlier among all primary care attenders, and it is possible that a smaller proportion of patients with GAD have attended the present study due to their anxiety.
GAD-7 is a new tool that is designed for screening for GAD and other anxiety disorders in primary care. Our data shows that the Finnish translation of GAD-7 and its shorter version, GAD-2, are valid tools with high sensitivity and specificity for GAD. The highest Youden's index was obtained with a cut-off point of 7. This is lower than in the original study, in which the cut-off point was defined as a total score of 10 (8). Additional data are needed to further define the optimal cut-off point for the Finnish version. GAD-7 and GAD-2 are also valuable for detecting panic disorder and other anxiety disorders, although sensitivity and specificity are lower than for GAD. This is in line with earlier studies (10).
Implications for clinical practice and future research
GAD is a severe condition with a major negative effect on functioning and quality of life [19]. Based on our data here and earlier reports, GAD is rather prevalent among primary care patients, especially those with frequent visits. Therefore, it is important that the condition is recognized by health care professionals. GAD-7 is a valid and useful tool for screening for GAD and other anxiety disorders in primary health care. Additional studies are needed to further elucidate the psychometric properties of GAD-7.
Conclusions
GAD and also other anxiety disorders are rather common among high utilizers of health care. The Finnish version of GAD-7 is a valid instrument for detecting GAD in primary health care.
Acknowledgments
Ethical considerations
The procedures followed in this study were in accordance with the Helsinki Declaration of 1975 as revised in 1983. This study has been approved by the ethics committee of Northern Ostobothnia health district.
Declaration of interest
The authors alone are responsible for the content and writing of the paper.
Tero Kujanpää has been granted financial support for this project from Northern Finland health care support foundation and he has been reimbursed by Orion Oy for attending a conference. Tero Ylisaukko-oja is a shareholder of Genecodebook Oy and MedEngine Oy, and has worked as a consultant for Pfizer Oy, Oy Bristol-Myers Squibb (Finland) Ab, Otsuka Pharmaceutical Scandinavia AB, Oy Takeda-Leiras Pharmaceuticals AB, and Teva Finland Oy. Markku Timonen was reimbursed by Oy Bristol-Myers Squibb (Finland) Ab, H. Lundbeck A/S, Pfizer Oy, and Servier Finland Oy for attending four conferences, was paid by Astra Zeneca, Oy Bristol-Myers Squibb (Finland) Ab, Eli Lilly, Pfizer Oy, and Servier Finland Oy for speaking on different educational occasions, has received advisory panel payments from H. Lundbeck A/S and Pfizer Oy for four meetings, and is a minor shareholder in Valkee Ltd. There are no other relationships or activities that could appear to have influenced the submitted work.
References
- 1.Wittchen HU, Hoyer J. Generalized anxiety disorder: Nature and course. J Clin Psychiatry. 2001;62((Suppl 11)):15–19. discussion 20–1. [PubMed] [Google Scholar]
- 2.Wittchen HU, Zhao S, Kessler RC, Eaton WW. DSM-III-R generalized anxiety disorder in the National Comorbidity Survey. Arch Gen Psychiatry. 1994;51:355–64. doi: 10.1001/archpsyc.1994.03950050015002. [DOI] [PubMed] [Google Scholar]
- 3.Maier W, Gansicke M, Freyberger HJ, Linz M, Heun R, Lecrubier Y. Generalized anxiety disorder (ICD-10) in primary care from a cross-cultural perspective: A valid diagnostic entity? Acta Psychiatr Scand. 2000;101:29–36. doi: 10.1034/j.1600-0447.2000.101001029.x. [DOI] [PubMed] [Google Scholar]
- 4.Lieb R, Becker E, Altamura C. The epidemiology of generalized anxiety disorder in Europe. Eur Neuropsychopharmacol. 2005;15:445–52. doi: 10.1016/j.euroneuro.2005.04.010. [DOI] [PubMed] [Google Scholar]
- 5.Munk-Jorgensen P, Allgulander C, Dahl AA, Foldager L, Holm M, Rasmussen I, et al. Prevalence of generalized anxiety disorder in general practice in Denmark, Finland, Norway, and Sweden. Psychiatr Serv. 2006;57:1738–44. doi: 10.1176/ps.2006.57.12.1738. [DOI] [PubMed] [Google Scholar]
- 6.Wittchen HU, Kessler RC, Beesdo K, Krause P, Hofler M, Hoyer J. Generalized anxiety and depression in primary care: Prevalence, recognition, and management. J Clin Psychiatry. 2002;63((Suppl 8)):24–34. [PubMed] [Google Scholar]
- 7.Katon W, Von Korff M, Lin E, Lipscomb P, Russo J, Wagner E, et al. Distressed high utilizers of medical care. DSM-III-R diagnoses and treatment needs. Gen Hosp Psychiatry. 1990;12:355–62. doi: 10.1016/0163-8343(90)90002-t. [DOI] [PubMed] [Google Scholar]
- 8.Spitzer RL, Kroenke K, Williams JB, Lowe B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch Intern Med. 2006;166:1092–7. doi: 10.1001/archinte.166.10.1092. [DOI] [PubMed] [Google Scholar]
- 9.Garcia-Campayo J, Zamorano E, Ruiz MA, Pardo A, Perez-Paramo M, Lopez-Gomez V, et al. Cultural adaptation into Spanish of the generalized anxiety disorder-7 (GAD-7) scale as a screening tool. Health & Quality of Life Outcomes. 2010;8:8. doi: 10.1186/1477-7525-8-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Kroenke K, Spitzer RL, Williams JB, Monahan PO, Lowe B. Anxiety disorders in primary care: Prevalence, impairment, comorbidity, and detection. Ann Intern Med. 2007;146:317–25. doi: 10.7326/0003-4819-146-5-200703060-00004. [DOI] [PubMed] [Google Scholar]
- 11.Donker T, van Straten A, Marks I, Cuijpers P. Quick and easy self-rating of Generalized Anxiety Disorder: Validity of the Dutch web-based GAD-7, GAD-2 and GAD-SI. Psychiatry Res. 2011;188:58–64. doi: 10.1016/j.psychres.2011.01.016. [DOI] [PubMed] [Google Scholar]
- 12.Sidik SM, Arroll B, Goodyear-Smith F. Validation of the GAD-7 (Malay version) among women attending a primary care clinic in Malaysia. J Prim Health Care. 2012;4:5–11. [PubMed] [Google Scholar]
- 13.Ruiz MA, Zamorano E, Garcia-Campayo J, Pardo A, Freire O, Rejas J. Validity of the GAD-7 scale as an outcome measure of disability in patients with generalized anxiety disorders in primary care. J Affect Disord. 2011;128:277–86. doi: 10.1016/j.jad.2010.07.010. [DOI] [PubMed] [Google Scholar]
- 14.Christensen H, Batterham PJ, Grant JB, Griffiths KM, Mackinnon AJ. A population study comparing screening performance of prototypes for depression and anxiety with standard scales. BMC Med Res Methodol. 2011;11:154. doi: 10.1186/1471-2288-11-154. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Lowe B, Decker O, Muller S, Brahler E, Schellberg D, Herzog W, et al. Validation and standardization of the Generalized Anxiety Disorder Screener (GAD-7) in the general population. Med Care. 2008-;46:266–74. doi: 10.1097/MLR.0b013e318160d093. [DOI] [PubMed] [Google Scholar]
- 16.Vedsted P, Christensen MB. Frequent attenders in general practice care: A literature review with special reference to methodological considerations. Public Health. 2005;119:118–37. doi: 10.1016/j.puhe.2004.03.007. [DOI] [PubMed] [Google Scholar]
- 17.Pirkola SP, Isometsa E, Suvisaari J, Aro H, Joukamaa M, Poikolainen K, et al. DSM-IV mood-, anxiety- and alcohol use disorders and their comorbidity in the Finnish general population: Results from the Health 2000 Study. Soc Psychiatry Psychiatr Epidemiol. 2005;40:1–10. doi: 10.1007/s00127-005-0848-7. [DOI] [PubMed] [Google Scholar]
- 18.Belanger L, Ladouceur R, Morin CM. Generalized anxiety disorder and health care use. Can Fam Physician. 2005;51:1362–3. [PMC free article] [PubMed] [Google Scholar]
- 19.Henning ER, Turk CL, Mennin DS, Fresco DM, Heimberg RG. Impairment and quality of life in individuals with generalized anxiety disorder. Depression & Anxiety. 2007;24:342–9. doi: 10.1002/da.20249. [DOI] [PubMed] [Google Scholar]