Abstract
Reducing HIV and AIDS-related stigma is critical in the fight against HIV/AIDS. Although national campaigns and prevention programs have been implemented across South Africa to address this critical concern (Soul City, 2008; USAIDS, 2007), assessing the impact of these initiatives is difficult as it requires that measurement of HIV/AIDS-related stigma is uniform and comparable nationwide. The appropriateness of existing stigma measures for this task is unclear as measurement of HIV/AIDS related stigma may be qualitatively different across South Africa’s diverse population (Jöreskog, 1971). The current study assesses a theoretically and culturally informed multi-dimensional, HIV/AIDS-related, stigma scale for measurement invariance across a sample drawn from two culturally distinct South African provinces: Limpopo (n = 597) and Western Cape (n = 598). Results suggest measurement invariance across groups for the HIV/AIDS-stigma scale, supporting the scale’s integrity and appropriateness for use across diverse populations.
Keywords: Stigma, HIV/AIDS, South Africa, Scale Development, Measurement
Introduction
HIV/AIDS related stigma is as a major barrier to prevention, testing and treatment of HIV/AIDS in African countries (Kalichman et al., 2005). In some African communities, individuals report greater fear of the social consequences of an HIV/AIDS diagnosis than the disease itself (Lie & Biswalo, 1994). Consequently, measuring stigma in a manner that is culturally appropriate is necessary to enable researchers and community leaders to assess stigma and evaluate interventions aimed at reducing it. Even within one country, the appropriateness of a stigma scale may vary across diverse cultural groups. This study’s aim is to develop a measure of stigma appropriate for use across South Africa’s diverse population.
Methods
Scale Development
Graduate students trained in qualitative methods each conducted six focus groups, usually with 8–9 participants (see Airhihenbuwa et al., 2009 for details on training and analytic procedures). Qualitative data were analyzed using Nvivo 2.0 software and guided survey development.
A pre-test of this survey instrument was conducted with 50 participants, and feedback was solicited through self-report, individual interviews, and group interviews. The majority of the questions were well received by the respondents. Respondents identified specific differences between “shame” and “rejection”; themes that had previously been combined. The survey was changed to reflect these differences. In Year 5, the full survey was developed based on a combination of focus group data and the pre-test survey from years 1–4.
Target population
Six South African postgraduate students from the University of the Western Cape and the University of Limpopo were trained to use the survey instrument to collect data from 200 participants each. Data were collected in the regions of the two partnered universities, which represent regions that are geographically, culturally, and economically unique and thus provide an appropriate contrast for assessing the scales appropriateness in diverse contexts. Preliminary qualitative research suggested we focus on three primary contexts; health care facilities; families of PLWHA; and PLWHA.
Participants
Analyses focus on 1195 South Africans who participated in the study during its final year (year 5). Participants were recruited from either Limpopo province (n = 597), in the north, or Western Cape (n = 598), in the south, and consisted of family/community members, health care workers and PLWHA. The majority of participants was female (69.5%), Christian (86.7%), and identified as African (83.3%). On average, participants were 35.8 years old. Southern participants were more likely to report that someone they knew personally had disclosed their HIV/AIDS status to them (70% vs. 43.2%) and that they knew someone who died from HIV/AIDS (67.1% vs. 46.4%).
Data Collection
Data were collected using the participant’s preferred language. A language specialist, who was not a member of the research team, translated the survey from English into different languages and back to English.
Analytic Methods
The scale consisted of twelve items selected based on their fit with the overall conceptualization of stigma indicated through qualitative research and pilot testing (see Table 1). The number of factors and appropriateness of each item was assessed using principle components and promax rotation in SAS 9.2 for the full sample and subsamples. Factor solutions were identified based on scree plots. Items with loadings of at least 0.40 were included in the solution. Scale reliability was assessed using Cronbach’s Alpha coefficient (α) for each subscales using SAS 9.2.
Table 1.
HIV Stigma Scale Items
| Item # | Item |
|---|---|
| 1 | For people living with HIV and AIDS, government should support organizations that offer assistance to PLWHA. |
| 2 | For people living with HIV and AIDS, government should provide food. |
| 3 | For people living with HIV and AIDS, government should provide housing. |
| 4 | For people living with HIV and AIDS, government should provide ARV treatment. |
| 5 | Given a choice between two well-qualified applicants for a job, I would support hiring an HIV negative person. |
| 6 | I would be ashamed to disclose my status if I ever test positive for HIV. |
| 7 | A person who contracts HIV should be shamed. |
| 8 | A person who contracts HIV should be rejected. |
| 9 | HIV is more of a problem for other religious/spiritual groups than mine. |
| 10 | I support community events that support PLWHA. |
| 11 | I participate in community events to support PLWHA. |
| 12 | I would share meals with members of my family if they lived with HIV and AIDS. |
Possible group differences in the stigma factor solution were analyzed using Lisrel 8.2 by comparing a series of nested models based on Jöreskog’s hierarchy (1971)., in which parameter constraints are applied hierarchically. Confirmatory factor analysis (CFA) assessed the fit of the factor structure for the overall sample ignoring any potential differences between groups. For each factor, items with the highest loading were fixed to 1.0 so that all other parameters could be freely estimated. The factor structure was then assessed for regional subgroups to determine if the factor structure for the overall sample could be applied to the two groups. The fit of each model was assessed using indices of practical fit, because chi-square statistics are known to be highly sensitive to large sample sizes (Bentler, 1990; Bentler & Bonett, 1980; Browne & Cudek, 1993; McDonald & Marsh, 1990; Tucker & Lewis, 1973). The large sample size in the current study (N=1195) would result in a statistically significant χ2 even with slight departure from the perfect model. Instead, RHO (Bentler & Bonett, 1980; Tucker & Lewis, 1973), CFI (Bentler, 1990; McDonald & Marsh, 1990) and RMSEA (Browne & Cudeck, 1993) were used, which have been found to be good indices of practical fit.
Lastly, a model in which factor loadings and factor variances were constrained to be the same for both the north and south groups was compared to a model where the loadings and variances were not constrained to be equal across groups to assess if the factor loadings and variances were the same for the two groups. Model differences were assessed using chi-square difference test and difference tests for the indices of practical fit.
Results
Internal Consistency
The scree plot and eigenvalues from the exploratory factor analysis supported the presence of three factors with item factor loadings ranging from 0.44 to 0.85 on the three factors. The three distinct domains were identified as “government support” (items 1–4); “Shame and Rejection” (items 5–9); and “Individual Support” (items 10–12). The individual subscales were internally consistent with alpha coefficients ranging from 0.67 to 0.80. Chronbach’s alpha is known to be affected by the number of items in a scale (Corina, 1993), thus this level of internal consistency is considered to be acceptable given the low number of items in the subscales and is in line with other stigma scales that have a greater number of items (Kalichman et al., 2005).
Confirmatory Factor Analyses
CFAs were conducted using Lisrel 8.2 to assess goodness of fit for the three-factor model obtained with exploratory factor analyses (Model 0) compared to the one-factor model for the entire sample. Based on the indices analyses χ2 (51) = 536.38, RHO= 0.851, CFI = 0.885, and RMSEA = 0.089, the model was determined to have poor fit. The residual covariance between item 1 and item 4 were estimated to assess possible improvement in model fit. Estimating the additional parameter (TE 4,1) did not impact factor loadings for Shame and Rejection and Individual Support and produced only slight changes in correlations between factors (Δr <.01). Despite the significant chi-square for Model 0a, Model 0a had improved fit with RHO = .913, CFI=.934, and RMSEA = .068. The fit indices suggest that the model fit is acceptable (Hu & Bentler, 1999), and supports the validity of the three-factor model.
Multiple Group Confirmatory Factor Analysis
The factor structure established for the full sample was tested independently for both the north (Model 0N) and south (Model 0S) subsamples. Both models were determined to have acceptable fit based on indices of practical fit. The north and south subsamples were combined in a two group latent variable model (Model 1) that assessed factor structure invariance. Based on indices of practical fit (see Table 2), the two group model was determined to have acceptable fit suggesting that the three factors and the items that make up each factor are the same for both the north and the south subsamples.
Table 2.
Goodness of Fit Results for the two group model (north and south)
| Model
|
Chi-sq
|
df
|
RMSEA1
|
RMSEA2
|
RHO
|
CFI
|
|---|---|---|---|---|---|---|
| Null 0N | 2535.90 | 66 | 0.251 | |||
| Model 0N | 211.43 | 50 | 0.074 | 0.074 | 0.914 | 0.935 |
| Null 0S | 1741.58 | 66 | 0.206 | |||
| Model 0S | 143.56 | 50 | 0.056 | 0.056 | 0.926 | 0.944 |
| Null 1 & 2 | 4277.47 | 132 | 0.230 | |||
| Model 1(LY=PS) | 355.00 | 100 | 0.065 | 0.046 | 0.919 | 0.939 |
| Model 2(LY=IN) | 452.62 | 109 | 0.073 | 0.051 | 0.900 | 0.917 |
| Model2 - M1 | 97.63 | 9 | +0.008 | −0.005 | −0.016 | −0.022 |
Equivalence of Factor Loadings and Variances
In Model 2, all factor loadings were constrained to be equal across groups to test for invariance in the factor patterns between the two groups. Like in the other models, the chi-square was significant; however, Model 2 was judged to have acceptable fit based on indices of practical fit and was statistically significant based on the difference between Model 1 and Model 2 (Table 2). However, the fit of Model 2 was not practically different than Model 1 as change in indices of practical fit was minimal. Therefore, differences in the factor loadings for each group were considered invariant. The invariance of the factor structure (including overall pattern, factor loadings and factor variances) supports the use of the scale for individuals in both the northern and southern regions of South Africa and suggests that the meaning of stigma, as presented in figure 1, is the same across the two groups.
Figure 1.
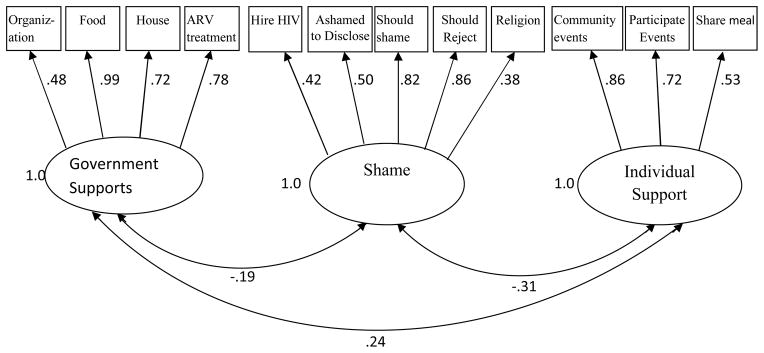
Confirmatory factor analysis model of HIV/AIDS stigma scale for individuals in both the northern and southern regions of South Africa. Results supported a three-factor solution, in which Government Supports, Shame, and Individual Support are correlated. The factor correlations and the factor loadings are included in the model.
Discussion
Although existing stigma scales have used qualitative research and past literature to develop culturally and theoretically informed stigma scales (Kalichman et al., 2005; Zelaya et al., 2008), the current study is the first to our knowledge to be guided a priori by a theoretical framework and demonstrate the equivalence of the developed scale in culturally unique subsamples. This is an important contribution to the field of HIV/AIDS prevention and stigma research as it provides a tool that can be used to assess HIV/AIDS related stigma initiatives across South Africa. Additionally, the multidimensionality of the current scale addresses a previously identified weakness (Kalichman et al., 2005) in existing scales and provides a more comprehensive measure of stigma than prior scales (Kalichman et al., 2005; Visser et al., 2008).
The stricter psychometric approach to evaluating the current scale allows for greater confidence in the use of the scale across South Africa. Prior scales developed for use in South Africa, rely on samples from a single region within South Africa (Kalichman et al., 2005; Visser et al., 2008). Consequently, the appropriateness of these scales in both northern and southern regions of South Africa is unknown. Although these studies did compare the reliability (Kalichman et al., 2005) and factor structure (Visser et al., 2008) of the scales across groups, such tests are not sufficient to ensure that the overall meaning of the scale is consistent across subpopulations. Even when a scale has good reliability and strong factor loadings in pooled analyses, ignoring potential group differences or comparing the two populations may be inappropriate, producing inaccurate results if both the structure and meaning of the scale are not equivalent across groups (Jöreskog, 1971).
Multidimensionality
The domains covered in the current scale, Government Support, Shame and Rejection, and Individual Support, closely parallel prior measures of stigma. For example, Zelaya and colleague’s (2008) scale reports four domains identified in an Indian sample, with association with shame, blame, and judgment and personal support of discriminatory actions or policies against PLWHA reflecting similar aspects of stigma as the Shame and Rejection and Government Support domains in the current scale. In scales developed for use in South Africa, the items included in the Shame and Rejection domain are similar to those included in the uni-dimensional AIDS-Related Stigma Scale (Kalichman et al., 2005) and Visser and colleague’s (2008) Blame and Judgment domain. The consistency of such items in all stigma scales in South Africa suggest that shame, judgment, and rejection are robust and salient aspects of HIV stigma in South Africa. Visser and colleagues’ second domain measured interpersonal distancing. This domain covers some aspects of our Individual Support domain, but is not completely equivalent as the authors intended the scale to be parallel, but hold different meanings for the subpopulations. Differences in the current scale and the Visser and colleagues’ scale may reflect different goals in scale development.
Limitations
Despite the strengths of this study, several limitations should be noted. Although the cultural differences between the north and the south suggest that our sample is diverse and covers a broad range of perspectives, the sampling scheme did not capture all regions of South Africa. Furthermore, purposive sampling was used to recruit participants who were proximate to someone who had HIV/AIDS. Given the prevalence of HIV/AIDS in South Africa, few South Africans would be unexposed to the virus. Nonetheless, these two limitations may limit the generalizability of this study to South Africa as a whole. The instrument’s validity should be assessed prior to generalizing the current findings to populations in different regions, countries, as well as to minors or those who are unexposed to HIV/AIDS. Lastly, although preliminary research suggested few differences in how HIV/AIDS stigma is perceived by family members, PLWHA, and healthcare workers (Airhihenbuwa et al., 2011), future research should examine the equivalence of this scale for these groups.
Acknowledgments
This research was supported by the U.S. National Institutes of Health (R24 MH068180) and by the National Institute on Drug Abuse (T32 DA017629). The authors would like to thank the HIV and AIDS Stigma Project Team at Penn State University, the Human Sciences Research Council, The University of the Western Cape and the University of Limpopo in South Africa.
References
- Airhihenbuwa CO, Okoror TA, Shefer T, Brown D, Iwelunmor J, Smith EA, Adam M, et al. Stigma, Culture, and HIV and AIDS in the Western Cape, South Africa: An Application of the PEN-3 Cultural Model for Community-Based Research. Journal of Black Psychology. 2009;35(4):407–432. doi: 10.1177/0095798408329941. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Airhihenbuwa CO, Shisana O, Zungu NP, BeLue R, Makofani DM, Shefer T, Smith EA, et al. Research capacity building: a US-South African partnership. Global Health Promotion. 2011;18(2):27–35. doi: 10.1177/1757975911404745. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bentler PM. Comparative fit indexes in structural models. Psychological Bulletin. 1990;107(2):238–46. doi: 10.1037/0033-2909.107.2.238. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/2320703. [DOI] [PubMed] [Google Scholar]
- Bentler Peter M, Bonett DG. Significance tests and goodness of fit in the analysis of covariance structures. Psychological Bulletin. 1980;88(3):588–606. doi: 10.1037//0033-2909.88.3.588. [DOI] [Google Scholar]
- Browne MW, Cudeck R. Alternative ways of assessing model fit. In: Bollen KA, Long JS, editors. Testing structural equation models. Newbury Park, CA: Sage; 1993. pp. 136–162. [Google Scholar]
- Cortina J. What is coefficient alpha? An examination of theory and applications. Journal of Applied Psychology. 1993;78(1):98–10. Retrieved from http://psychweb.psy.umt.edu/denis/datadecision/front/cortina_alpha.pdf. [Google Scholar]
- Hu L, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal. 1999;6(1):1–55. doi: 10.1080/10705519909540118. [DOI] [Google Scholar]
- Jöreskog KG. Simultaneous factor analysis in several populations. Psychometrika. 1971;36(4):409–426. Retrieved from http://www.springerlink.com/index/93M1M81738G10337.pdf. [Google Scholar]
- Kalichman SC, Simbayi LC, Jooste S, Toefy Y, Cain D, Cherry C, Kagee A. Development of a brief scale to measure AIDS-related stigma in South Africa. AIDS and Behavior. 2005;9(2):135–43. doi: 10.1007/s10461-005-3895-x. [DOI] [PubMed] [Google Scholar]
- Lie GT, Biswalo PM. Perceptions of the appropriate HIV/AIDS counsellor in arusha and Kilimanjaro Regions of Tanzania: Implications for hospital counselling. AIDS Care. 1994;6(2):139–151. doi: 10.1080/09540129408258625. [DOI] [PubMed] [Google Scholar]
- McDonald RP, Marsh HW. Choosing a multivariate model: Noncentrality and goodness of fit. Psychological Bulletin. 1990;107(2):247–255. doi: 10.1037//0033-2909.107.2.247. [DOI] [Google Scholar]
- Soul City. Soul Buddyz: Evaluation Report 2008. Dunkeld West, South Africa: Soul City: Institute for Health and Development Communication; 2008. [Google Scholar]
- Tucker LR, Lewis C. A reliability coefficient for maximum likelihood factor analysis. Psychometrika. 1973;38(1):1–10. Retrieved from http://www.springerlink.com/index/T73R850283255265.pdf. [Google Scholar]
- USAIDS. Reducing HIV Stigma and Discrimination: A critical part of national AIDS programmes. Geneva: 2007. [Google Scholar]
- Visser MJ, Kershaw T, Makin JD, Forsyth BWC. Development of parallel scales to measure HIV-related stigma. AIDS and Behavior. 2008;12(5):759–71. doi: 10.1007/s10461-008-9363-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zelaya CE, Sivaram S, Johnson SC, Srikrishnan AK, Solomon S, Celentano DD. HIV/AIDS stigma: reliability and validity of a new measurement instrument in Chennai, India. AIDS and Behavior. 2008;12(5):781–8. doi: 10.1007/s10461-007-9331-7. [DOI] [PubMed] [Google Scholar]


