Abstract
Objective
To compare the long-term effectiveness of ablation to resection in patients with bilateral hepatic colorectal metastases.
Design
Review of prospective database of 2123 operative cases of hepatic colorectal metastases.
Setting
A large institution with expertise in ablation and resection.
Patients
Patients with bilateral colorectal liver metastases undergoing operation with a curative intent.
Interventions
Radiofrequency or microwave ablation alone or in combination with resection (Com) compared with bilateral resection (Res).
Main Outcome Measures
We compared tumor characteristics, operative, and postoperative outcomes using chi-square or Wilcoxon tests as appropriate and assessed overall survival differences between the two groups using the log-rank test.
Results
During the study period 141 patients were treated with Res and 95 patients Com. The Com group was a significantly poorer prognostic group than the Res group as judged by the Clinical Risk Score (p<0.01). There was no difference in median operative time (Com: 280 min, Res 282; p=0.52), but a lower blood loss (Com: 300 mL, Res 500; p<0.01) and a shorter length of stay (Com: 7 days, Res: 9; p<0.01) was achieved in the Com group. Long term outcome was not significantly different between groups (5-yr overall survival Com: 56%, Res: 49%; p=0.16).
Conclusions
Treatment of bilateral, multiple hepatic metastases with combined resection and ablation is associated with improved perioperative outcomes without compromising long-term survival compared with bilateral resection. Ablative therapies extend the capability of delivering potentially curative treatment for bilateral hepatic colorectal metastases.
Keywords: Hepatic metastases, Colorectal cancer, Ablation, Radiofrequency ablation, Microwave ablation
INTRODUCTION
Resection of colorectal metastases confined to the liver improves the overall survival of patients and offers the potential for cure1-5. Patients with bilateral liver metastases are less likely to be resectable with conventional techniques. Strategies for managing patients with bilateral liver metastases include multiple simultaneous liver resections, staged approaches to resection (with or without portal vein embolization), or attempts at reducing tumor burden using systemic or local chemotherapy6, 7.
In the past decade, ablative techniques have emerged as an option to locally treat liver tumors including colorectal liver metastases. The role of ablation in patients with colorectal liver metastases is unclear. Previous series have suggested that ablation yields an improvement in survival compared with chemotherapy alone for unresectable metastases but is inferior to resection for resectable metastases8. A recent attempt to establish clinical practice guidelines concluded that there was insufficient evidence to base guidelines with wide variability in five year survival (15-55%) and a compelling need for more research to determine the efficacy and utility of ablation9.
Given the challenges to treating patients with bilateral colorectal liver metastases, ablative techniques may increase the number of patients eligible to be treated with a potentially curative intent. The objective of this study was to compare perioperative and long-term outcomes in patients with bilateral colorectal liver metastases treated with ablation (and/or resection) to patients treated with the historical gold standard of bilateral resection.
METHODS
Patients operatively treated for bilateral, multiple colorectal liver metastases between 1999 and 2008 were identified from a prospectively maintained database containing demographic, clinical, operative, pathological, and follow-up data. Prior to 2004, patients with resectable bilateral colorectal metastases underwent bilateral resection in either a one-stage or two-stage approach. Surgeons at our institution began using ablation (primarily RFA) more frequently in 2004. In general, patients with bilateral colorectal metastases undergo bilateral resection if sufficient parenchyma can be safely preserved. Patients with borderline resectable metastases or with unresectable metastases amenable to complete treatment with ablation undergo ablation alone or in combination with resection.
In order to minimize the bias from patient selection that has occurred in the more contemporary time period, we compared patients treated by ablation alone or in combination with resection from 2004-2008 (Com) with cases treated by conventional bilateral resection from 1999-2003 (Res). Some of the patients in this study were included in prior reports on outcomes of metastatic colorectal cancer at our institution. The Institutional Review Board at MSKCC approved this study.
We calculated the Clinical Risk Score (CRS) for each patient included in the analysis10. The CRS is a prediction tool composed of five clinical variables: node-positive primary cancer, disease-free interval less than 12 months, multiple liver metastasis, largest diameter of any liver metastasis greater than 5 cm, and preoperative serum carcinoembryonic antigen level >200 ng/mL. Based on CRS, patients were grouped into two categories: low CRS (0, 1, or 2) and high CRS (3, 4, or 5).
We compared baseline patient and tumor characteristics, operative time, blood loss, length of hospital stay, and 30-day mortality between patients in the two groups using the chi-square for categorical variables or the Wilcoxon test for continuous variables. We assessed overall survival differences between the two groups using the log-rank test. All statistical tests were two sided and we considered p<0.05 indicative of statistically significant differences.
RESULTS
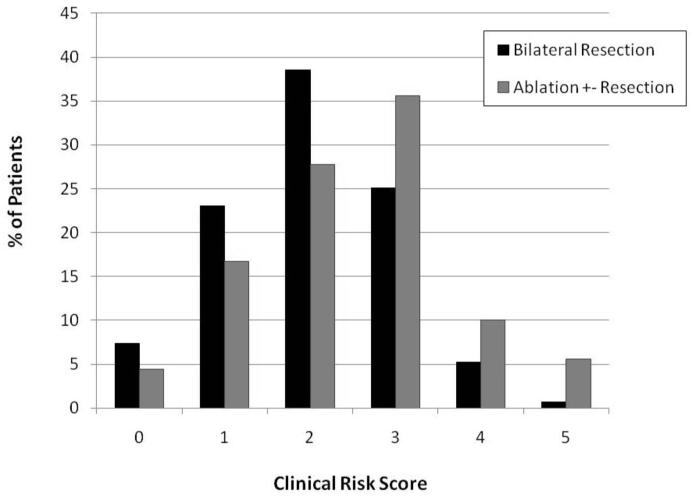
During the defined study periods 141 patients were treated with bilateral resection and 95 patients had ablation, either alone (9) or in combination with resection (86). Median age was 62, with no difference between groups (Table 1). More patients treated with the combined approach had colon primary cancers compared with the resected group, and patients treated with ablation were more likely to undergo simultaneous colorectal resection (23 vs 4%). Patients treated with a combined strategy in general had a higher CRS, primarily attributed to shorter disease free intervals (Figure 1). In contrast, patients treated with resection had higher CEA levels, number of tumors, and size of largest tumor.
Table 1.
Characteristics of patients included in this study
| Bilateral Resection N = 141 |
Ablation ± Resection N = 95 |
p | |
|---|---|---|---|
|
| |||
| Female (%) | 62 (47) | 41 (43) | 0.534 |
|
| |||
| Age [median (IQ Range)] | 61.4 (53.6-69.2) | 63.0 (53.6-71.0) | 0.432 |
|
| |||
| Primary in Colon (%) | 94 (70) | 78 (82) | 0.032 |
|
| |||
| Simultaneous colorectal resection (%) | 6 (4) | 22 (23) | <0.001 |
|
| |||
| Primary Nodal Status (%) | 0.246 | ||
| N0 | 43 (31) | 40 (42) | |
| N1 | 62 (45) | 36 (38) | |
| N2 | 32 (23) | 19 (20) | |
|
| |||
| Disease Free Interval (Months) [median (IQ Range)] |
8.9 (2.4-19.9) | 0 (0-0) | <0.001 |
|
| |||
| CEA (ng/mL) [median (IQ Range)] |
29.2 (7.9-166.3) | 7.9 (2.9-28.3) | <0.001 |
|
| |||
| Number of Tumors [median (IQ Range)] |
4.0 (2.0-5.0) | 3.0 (2.0-4.0) | 0.005 |
|
| |||
| Size of Largest Tumor (cm) [median (IQ Range)] |
4.1 (2.5-6.0) | 2.3 (1.5-3.6) | <0.001 |
|
| |||
| Clinical Risk Score (CRS) > 2 (%) | 42 (31) | 46 (51) | 0.003 |
|
| |||
| Ablation alone | N/A | 9 (9) | N/A |
| Ablation + Resection | 86 (91) | ||
|
| |||
| Radiofrequency Ablation | N/A | 88 (91) | N/A |
| Microwave Ablation | 9 (9) | ||
Figure 1.
Distribution of Clinical Risk Score (CRS) in patients treated with bilateral resection or ablation +- resection (p=0.002).
Operative time was similar between the two groups, while blood loss was significantly greater in patients treated with bilateral resection (Table 2). Three patients (2.1%) died within 30 days of operation in the resection group compared with one patient in the combined group. Median length of stay was 9 days following resection and 7 days following ablation +- resection (p<0.001).
Table 2.
Operative and perioperative outcomes in patients treated with bilateral resection or ablation +- resection.
| Bilateral Resection N = 141 |
Ablation ± Resection N = 95 |
p | |
|---|---|---|---|
| Total operative time (min) [median (IQ Range)] |
282 (238-336) | 280 (219-330) | 0.518 |
| Intraoperative blood loss (mL) [median (IQ Range)] |
500 (300-1000) | 300 (200-420) | <0.001 |
| 30-day mortality (%) | 3 (2) | 1(1) | 0.518 |
| Length of stay (days) [median (IQ Range)] |
9 (7-11) | 7 (6-9) | <0.001 |
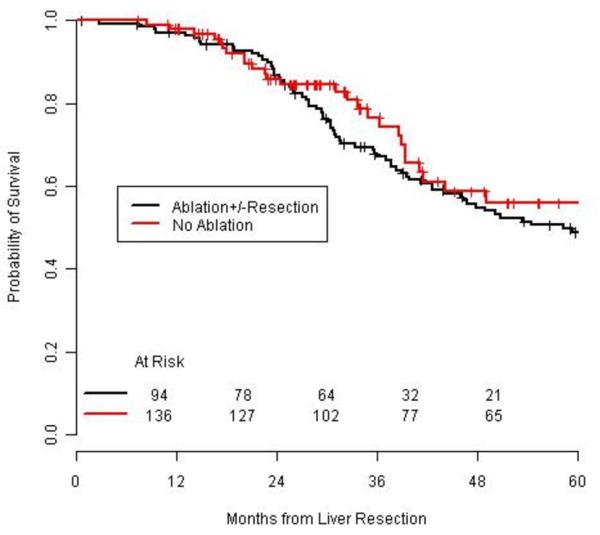
Median follow-up in patients treated with resection was 44 months and in patients treated with the combined approach was 23 months. Overall survival at three years was 67% in the resection group and 77% in the combined group. After five years overall survival was 49% and 56% respectively (p=0.161, Figure 2).
Figure 2.
Overall survival in patients treated with bilateral resection or ablation +- resection (p=0.161).
DISCUSSION
This comparative analysis of patients with bilateral colorectal liver metastases demonstrates the perioperative and longterm safety of a combined ablative strategy compared with the conventional gold-standard of bilateral resection. Patients treated with ablation, either alone or in combination with resection, had less intraoperative blood loss, similar perioperative mortality, shorter length of hospitalization, and similar overall five-year survival.
The long-term survival in patients treated with the combined approach in this study is particularly encouraging given their high-risk clinical characteristics. More than half of patients in the Com group presented with a CRS of three or more, compared with 31% of patients who underwent bilateral resection. This difference was predominantly driven by the shorter disease-free interval in patients who underwent ablation. Indeed, the median disease-free interval in this group was 0, indicating that the majority of patients presented with synchronous liver metastases. In contrast, patients who underwent bilateral resection had larger tumor burden, evidenced by the higher number of metastases, size of largest metastasis, and CEA level. In the more contemporary timeframe patients with high tumor burden were appropriately selected for resection rather than ablation and therefore noticeably absent from this group.
This study is strengthened by the high quality of the data. All patients were treated at a single institution with extensive experience caring for patients with colorectal liver metastases. Data were prospectively collected and follow-up was complete. We chose to focus on overall survival as an indicator of long-term efficacy because it is objective and of most importance to patients.
The conclusions from this study are most limited by the selection bias inherent in this comparison. The optimal study design to address this question would be a prospective, randomized controlled trial. Unfortunately surgeons have been relatively unsuccessful at assessing the efficacy of new technologies with randomized trials and this technology is no exception. Technologies instead are generally introduced into general practice and rapidly adopted as part of standard care. A randomized trial would be particularly difficult to conduct in this setting because the selection of patients for ablation or resection seems intuitive. In general, patients with multiple tumors confined to one region of the liver or with large solitary metastases should undergo resection. Ablation in these settings would be at best inefficient and at worst ineffective. In contrast, ablation may play a role for patients with a limited number of small metastases deep within the hepatic parenchyma. In this scenario, ablation allows for optimal parenchymal preservation and extends potentially curative treatment to patients who might otherwise be deemed unresectable.
We attempted to address the inherent selection bias as much as possible by selecting patients who underwent bilateral resection from the timeframe prior to the adoption of ablation at our institution. As a result, this group represents a broadly representative group of patients with bilateral metastases, rather than patients who were specifically selected not to receive ablation. Although the two groups are not perfectly matched (Table 1), the higher CRS in the ablation group suggests that, if anything, the long-term results should favor the resection group. The comparable long-term survival despite this potential bias is reassuring. Furthermore, although systemic treatment of patients with colorectal liver metastases has improved during this time period, the incremental benefit has been modest with overall survival in the absence of surgery between 20-30% at three years11, 12. The three-year survival in patients who underwent ablation in this study was 77%; three times that of these contemporary patients treated with chemotherapy only. Follow-up in the ablation group was shorter than in the resection group given the different time-periods, so longer follow-up ideally including patterns of recurrence will be beneficial.
This study contributes to the growing body of literature confirming the safety and efficacy of ablation in the treatment of colorectal liver metastases. Abdalla and colleagues from the M.D. Anderson Cancer Center reported their experience in a series of patients with metastases confined to the liver8. With a median follow-up of 21 months, patients who underwent resection achieved better three-year survival than patients who had ablation (73% vs. 40%). However, the authors reserved ablative strategies for patients deemed “unresectable” at the time of laparotomy, making it difficult to compare outcomes in these heterogeneous groups. In a similar study from the Cleveland Clinic, 234 patients who were not candidates for resection underwent laparoscopic ablation13. Five-year survival in this group of patients was only 18%, however a significant proportion of patients had extra-hepatic disease and the majority of patients had been treated extensively with chemotherapy prior to operation. The authors conclude that survival in these patients would be near zero and that the use of ablation in this group achieves a survival advantage. Our study builds on these by limiting inclusion to patients with bilateral liver metastases in whom ablation was more liberally adopted with excellent long-term outcomes. Future research may compare these patients with a larger group of patients treated with ablation alone, perhaps including a percutaneous ablation group.
In summary, treatment of bilateral hepatic colorectal metastases with a combined ablative strategy yields good perioperative outcomes and does not compromise long-term overall survival. Ablative therapies may extend the capability of delivering potentially curative treatment for patients with bilateral hepatic colorectal metastases.
ACKNOWLEDGEMENTS
Paul Karanicolas contributed to the study conception and design, acquisition of data, analysis and interpretation of data, drafting of the manuscript, and critical revisions.
William Jarnagin contributed to the analysis and interpretation of data, and critical revisions of the manuscript.
Mithat Gönen contributed to the study conception and design, acquisition of data, analysis and interpretation of data, drafting of the manuscript, and critical revisions.
Scott Tuorto contributed to the acquisition of data, analysis and interpretation of data, and critical revisions of the manuscript.
Peter Allen contributed to the analysis and interpretation of data, and critical revisions of the manuscript.
Ronald DeMatteo contributed to the analysis and interpretation of data, and critical revisions of the manuscript.
Michael D’Angelica contributed to the analysis and interpretation of data, and critical revisions of the manuscript.
Yuman Fong contributed to the study conception and design, acquisition of data, analysis and interpretation of data, drafting of the manuscript, and critical revisions.
No funding was received for the conduct of this study.
Footnotes
None of the authors have a conflict of interest to declare.
REFERENCES
- 1.Choti MA, Sitzmann JV, Tiburi MF, et al. Trends in long-term survival following liver resection for hepatic colorectal metastases. Ann Surg. 2002;235(6):759–66. doi: 10.1097/00000658-200206000-00002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.House MG, Ito H, Gonen M, et al. Survival after hepatic resection for metastatic colorectal cancer: trends in outcomes for 1,600 patients during two decades at a single institution. J Am Coll Surg. 2010;210(5):744–52. 752–5. doi: 10.1016/j.jamcollsurg.2009.12.040. [DOI] [PubMed] [Google Scholar]
- 3.Nordlinger B, Guiguet M, Vaillant JC, et al. Surgical resection of colorectal carcinoma metastases to the liver. A prognostic scoring system to improve case selection, based on 1568 patients. Association Francaise de Chirurgie. Cancer. 1996;77(7):1254–62. [PubMed] [Google Scholar]
- 4.Scheele J, Stang R, Altendorf-Hofmann A, et al. Resection of colorectal liver metastases. World J Surg. 1995;19(1):59–71. doi: 10.1007/BF00316981. [DOI] [PubMed] [Google Scholar]
- 5.Tomlinson JS, Jarnagin WR, DeMatteo RP, et al. Actual 10-year survival after resection of colorectal liver metastases defines cure. J Clin Oncol. 2007;25(29):4575–80. doi: 10.1200/JCO.2007.11.0833. [DOI] [PubMed] [Google Scholar]
- 6.Gold JS, Are C, Kornprat P, et al. Increased use of parenchymal-sparing surgery for bilateral liver metastases from colorectal cancer is associated with improved mortality without change in oncologic outcome: trends in treatment over time in 440 patients. Ann Surg. 2008;247(1):109–17. doi: 10.1097/SLA.0b013e3181557e47. [DOI] [PubMed] [Google Scholar]
- 7.Kornprat P, Jarnagin WR, Gonen M, et al. Outcome after hepatectomy for multiple (four or more) colorectal metastases in the era of effective chemotherapy. Ann Surg Oncol. 2007;14(3):1151–60. doi: 10.1245/s10434-006-9068-y. [DOI] [PubMed] [Google Scholar]
- 8.Abdalla EK, Vauthey JN, Ellis LM, et al. Recurrence and outcomes following hepatic resection, radiofrequency ablation, and combined resection/ablation for colorectal liver metastases. Ann Surg. 2004;239(6):818–25. doi: 10.1097/01.sla.0000128305.90650.71. discussion 825-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Wong SL, Mangu PB, Choti MA, et al. American Society of Clinical Oncology 2009 clinical evidence review on radiofrequency ablation of hepatic metastases from colorectal cancer. J Clin Oncol. 2010;28(3):493–508. doi: 10.1200/JCO.2009.23.4450. [DOI] [PubMed] [Google Scholar]
- 10.Fong Y, Fortner J, Sun RL, et al. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg. 1999;230(3):309–18. doi: 10.1097/00000658-199909000-00004. discussion 318-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Falcone A, Ricci S, Brunetti I, et al. Phase III trial of infusional fluorouracil, leucovorin, oxaliplatin, and irinotecan (FOLFOXIRI) compared with infusional fluorouracil, leucovorin, and irinotecan (FOLFIRI) as first-line treatment for metastatic colorectal cancer: the Gruppo Oncologico Nord Ovest. J Clin Oncol. 2007;25(13):1670–6. doi: 10.1200/JCO.2006.09.0928. [DOI] [PubMed] [Google Scholar]
- 12.Hurwitz H, Fehrenbacher L, Novotny W, et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med. 2004;350(23):2335–42. doi: 10.1056/NEJMoa032691. [DOI] [PubMed] [Google Scholar]
- 13.Siperstein AE, Berber E, Ballem N, et al. Survival after radiofrequency ablation of colorectal liver metastases. Ann Surg. 2007;246(4):559–567. doi: 10.1097/SLA.0b013e318155a7b6. [DOI] [PubMed] [Google Scholar]