Abstract
Background
Electronic activity monitors (such as those manufactured by Fitbit, Jawbone, and Nike) improve on standard pedometers by providing automated feedback and interactive behavior change tools via mobile device or personal computer. These monitors are commercially popular and show promise for use in public health interventions. However, little is known about the content of their feedback applications and how individual monitors may differ from one another.
Objective
The purpose of this study was to describe the behavior change techniques implemented in commercially available electronic activity monitors.
Methods
Electronic activity monitors (N=13) were systematically identified and tested by 3 trained coders for at least 1 week each. All monitors measured lifestyle physical activity and provided feedback via an app (computer or mobile). Coding was based on a hierarchical list of 93 behavior change techniques. Further coding of potentially effective techniques and adherence to theory-based recommendations were based on findings from meta-analyses and meta-regressions in the research literature.
Results
All monitors provided tools for self-monitoring, feedback, and environmental change by definition. The next most prevalent techniques (13 out of 13 monitors) were goal-setting and emphasizing discrepancy between current and goal behavior. Review of behavioral goals, social support, social comparison, prompts/cues, rewards, and a focus on past success were found in more than half of the systems. The monitors included a range of 5-10 of 14 total techniques identified from the research literature as potentially effective. Most of the monitors included goal-setting, self-monitoring, and feedback content that closely matched recommendations from social cognitive theory.
Conclusions
Electronic activity monitors contain a wide range of behavior change techniques typically used in clinical behavioral interventions. Thus, the monitors may represent a medium by which these interventions could be translated for widespread use. This technology has broad applications for use in clinical, public health, and rehabilitation settings.
Keywords: electronic activity monitor, mobile, mhealth, physical activity, behavior change technique
Introduction
Background
Insufficient physical activity is a major worldwide public health problem. Even small increases in activity at a population level could have far-reaching positive impacts on chronic diseases such as diabetes, cardiovascular diseases, and several cancers [1-4]. Despite evidence supporting improved health outcomes from regular physical activity, population levels of physical activity remain low [5], and inactivity is prevalent [6].
Behavioral physical activity interventions are typically successful in increasing activity levels [7-9], but these interventions are costly and require professional expertise in delivering behavior change techniques (BCTs). Electronic activity monitors show promise as a delivery medium, as they can replicate most aspects of pedometer-based interventions while providing options for individually tailored intervention content. These monitors measure physical activity (and sometimes other health and behavior indicators such as heart rate) and interface with a computer or mobile app to provide extensive feedback tools. The feedback can be as or more rich and individualized than that provided in a clinical study, often including multiple charts, social comparisons, and indicators of progress towards individual goals. Initial intervention results using these monitors have been very promising, showing increases in physical activity and decreases in weight for two monitor brands [10-13].
The market for wearable technology activity monitors is large and growing quickly. Numerous options are currently available for use by consumers and researchers [14]. However, little is known about how these monitors differ from one another, what options they provide in their apps, and how these options may impact their effectiveness. The low cost, wide reach, and apparent effectiveness of electronic activity monitors make them appealing for recommendation by practitioners, but the growing number of options precludes practitioners’ ability to provide informed recommendations to patients. Similarly, individuals interested in using a monitor to change their behavior must rely on review websites or word of mouth to compare the variety of options. Information about the functionality of the devices and the content of their companion apps could provide guidance in choosing options most similar to standard intervention practices and best suited to individual preferences and needs.
Behavior Change Techniques and Content Analyses
There is no consensus as to the best method for analyzing content of new media. A common method has been to use health behavior theory to create codes and/or percentage scores of the number of theoretical constructs represented. This process has been used with active video games [15], exercise apps [16], and weight loss apps [17].
A more involved method uses recently developed systematic taxonomies of BCTs to code for content that matches components of traditional behavioral interventions. Behavior change techniques are “observable, replicable, and irreducible component[s] of an intervention designed to alter or redirect causal processes that regulate behavior” [18]. A general hierarchical taxonomy of 93 BCTs has recently been published [18], and a similar taxonomy specific to physical activity and dietary interventions is also available [19]. These validated taxonomies likely provide a more informational and rigorous coding tool than previously used theory-based instruments.
In addition to describing the content of biomedical media, there is also a need to determine the extent to which the behavior change strategies are evidence-based. Several recent analyses have reviewed mobile apps using different sources for their evidence base. Sources have included the Expert Committee for Pediatric Obesity Prevention [20], the Health Education Curriculum Analysis Tool [21], best practices such as those used by the Diabetes Prevention Program [22,23], and clinical recommendations from the American Association of Diabetes Educators [24] and US Public Health Service [25,26].
Although no compendium of evidence-based best practices exists for exercise and weight loss behavioral interventions, several meta-analyses and meta-regressions have provided a general idea of the BCTs typically associated with successful change [27-29]. Investigating the prevalence of these techniques in particular may provide insight into future directions for research and development.
Further, determining how evidence-based BCTs are implemented may also improve standard coding methods. Preliminary evidence suggests that for several of the most common and effective techniques, fidelity to theory-based recommendations in their implementation enhances their effectiveness [30-32]. Thus, more in-depth analysis of implementation would provide valuable additional information, particularly for practitioners and those developing theory-based interventions.
Content Analysis and Electronic Activity Monitors
There has been a call for study of health apps [33-35], due to their widespread use and the absence of guidelines for determining their adherence to standard practices. In addition to standalone apps, for which there are now several published content analyses [16,17,20-22,24,25], we believe that there is a need to study electronic activity monitors and their companion apps. Development of a tool for coding the content of these apps would provide valuable information for practitioners, consumers, and researchers, and could also be used to create a decision aid for determining an appropriate match of monitoring system to individual or research/clinical intervention.
The purpose of this study was to systematically investigate currently available commercial electronic activity monitors to (1) characterize their behavior change techniques, (2) determine the extent to which they include techniques associated with successful outcomes, and (3) compare implementation of several critical techniques to theory-based and evidence-based recommendations.
Methods
Activity Monitor Inclusion Criteria and Descriptions
Monitors were included based on three sources: review listings on CNET for wearable technology, listings in the “Health and Fitness” accessories section of the Apple Store (specifically, the Apple Web-based store that sells physical objects like iPods and MacBooks, not the online-only Apple App Store that sells apps), and a search of the Amazon site for “activity monitor”. Inclusion criteria included (1) continuous monitoring of some kind of physical activity outcome (eg, continuous measurement of steps or minutes of activity rather than discrete measurement of exercise periods), (2) the most recent iteration in a similar series of products released by the same company (eg, Fitbit Force rather than Fitbit Flex), and (3) provision of feedback via a separate mobile device or personal computer interface. Additional monitors were included based on prior knowledge or suggestion of expert colleagues if they fit inclusion criteria but were not present in the three listings above (eg, Ibitz, Lumo). Descriptions of included monitors are provided in Table 1. More in-depth descriptions of each monitor with screenshots from their Web/mobile apps can be found in Multimedia Appendix 1.
Table 1.
Monitor names and descriptions.
| Brand | Model | Where worn | Display/ compatibility | Measures | Possible measuresa | Food/Weight tracking |
| Basis |
|
Wrist | Display, personal computer, iOSb, Android | PAc, Steps, Heart rate, Skin temperature, Perspiration, Sleep |
|
|
| BodyMedia | Fit | Upper arm | Personal computer, iOS, Android | PA, Steps, Sleep | Heart rate, Weight | Food, Weight, Balance |
| Fitbit | Force | Wrist | Display, personal computer, iOS, Android | PA, Steps, Sleep, Stairs, Distance, Calories | Weight | Food, Weight, Balance |
| Fitbug | Orb | Multiple | Personal computer, iOS, Android | Steps, Distance, Calories, Sleep | Weight | Food, Weight, Balance |
| Gruve |
|
Waist | Personal computer | Calories, Activity zones |
|
|
| Ibitz | Unity | Waist | iOS | Steps, Distance, Calories |
|
Weight |
| Jawbone | Up24 | Wrist | iOS, Android | PA, Steps, Sleep, SBd |
|
Food, Weight, Balance |
| Lumo | Back | Waist | iOS, Android | Posture, Steps, Calories, Distance, SB, Sleep |
|
|
| Misfit | Shine | Multiple | iOS, Android | Steps, Calories, Distance, PA, Sleep, “Points” |
|
Food, Weight |
| Nike | Fuelband SE | Wrist | Display, personal computer, iOS, Android | PA, Steps, “Hours won”, Calories, “Nikefuel” |
|
|
| Polar | Loop | Wrist | Display, personal computer, iOS, Android | PA, Steps, Calories, SB, Sleep | Heart rate |
|
| Striiv | Play | Waist | Display, personal computer, iOS, Android | PA, Steps, Stairs, Distance, Calories |
|
Weight |
| Withings | Pulse | Multiple | Display, personal computer, iOS, Android | PA, Steps, Sleep, Resting heart rate | Weight, Blood pressure | Weight |
aThese objective measures are tracked simultaneously by the app. Additional measurement tools must be purchased.
biOS: Apple iPhone/iPad/iPod operating system.
cPA: physical activity.
dSB: sedentary behavior.
Coding Tool and Procedure
Coding procedures for this study were based on the taxonomies of BCTs created by Michie et al [18,19]. The most recent hierarchical list was used, with published definitions guiding coding for each technique.
A tentative list of BCTs associated with successful physical activity change was created based on several recently published meta-analyses [27,28], meta-regressions [29], and systematic reviews [36-38] as well as recommendations from the US Preventive Services Task Force [39] (see Table 2).
Table 2.
Behavior change techniques associated with physical activity change.
| BCT # | Behavior change technique | Source |
| 8.1 | Prompt practice | [28,37,38] |
| 2.3 | Prompt self-monitoring of behavior | [29,36,37,39] |
| 1.1 | Goal-setting/intention formation | [29,36-39] |
| 1.2 | Barrier identification/problem solving | [38,39] |
| 2.2 | Provide feedback on performance | [29] |
| 1.5 | Prompt review of behavioral goals | [29] |
| 5.1 | Provide information on consequences of behavior in general | [27] |
| 1.4 | Action planning | [27] |
| 10.3 | Prompt rewards contingent on effort or progress towards behavior | [27,28] |
| 6.2 | Facilitate social comparison | [27,40] |
| 4.1 | Provide instruction | [27,36] |
| 15.4 | Self-talk | [39] |
| 10.9 | Self-rewards | [39] |
| 3 | Social support | [39] |
| 7.1 | Teach to use prompts/cues | [28] |
Fidelity to implementation recommendations for three of the BCTs was measured based on Rovniak et al’s listing of recommendations for operationalizing mastery procedures from Social Cognitive Theory [30]. These are standard theory-based recommendations, but many of them also have demonstrated efficacy in randomized trials when compared to conditions that did not follow the recommendation(s) [30,32,41]. The full list of recommendations can be seen in the Results section.
Two trained coders (EL and ZL) wore each of the monitors for at least one 1-week period between November 11, 2013, and February 8, 2014. At least one coder wore each of the devices for 2 or more weeks. The coders downloaded and used personal computer apps and/or iPhone apps for each monitor. In cases where additional payment was required to access content (eg, a monthly subscription to use the BodyMedia device, a yearly subscription to access the full Fitbit website), we coded based on full access to all behavioral tools. Interrater reliability between the 2 coders was high (89%), with a kappa statistic of .55. An assistant coder also wore each monitor for 1 week and provided a full set of codes for each monitor. The 3 reviewers met to discuss any discrepancies, using the third coder’s results to help inform final decisions. The third set of codes informed final decisions in case of discrepancies. To update results, the 2 coders met once again in July 2014 to code 1 week’s worth of data on the monitors whose apps were updated since the previous data collection period. Coders also checked Web versions of apps where necessary. The same coding procedure was followed to determine whether additional techniques had been added.
Where functionality existed whereby a technique could be used but would not necessarily be used by default, we coded that technique as being present. For example, “friends” and “teams” are available for social support/social comparison in many apps, but users must add the friends themselves in order to take advantage of these tools. Further specific information on coder interpretation is available in Multimedia Appendix 2.
Results
Table 3 displays the number of monitor systems found to include each BCT. Techniques from the taxonomy that were not found in any of the systems were not included in the table. The most common techniques were those that were necessarily a part of each system: self-monitoring of behavior, feedback based on that monitoring, and the addition of a monitor to the user’s environment, behavioral goal-setting, and emphasizing a discrepancy between current behavior and goal behavior. Discrepancies were typically shown via visual progress indicators, such as progress bars, pie charts, bar charts, and line charts. Charts were often color-coded to indicate proximity to the goal, which was typically set to a default of 10,000 steps per day.
Table 3.
Behavior change techniques present in monitoring systems, by number of systems (N=13).
| BCT category | BCT | Monitors, n |
| Goals and planning | Goal setting (behavior)a | 13 |
| Problem solvinga | 1 | |
| Goal setting (outcome) | 8 | |
| Action planninga | 5 | |
| Review behavior goal(s)a | 10 | |
| Discrepancy between current behavior and goal | 13 | |
| Review outcome goal(s) | 7 | |
| Commitment | 4 | |
| Feedback and monitoring | Feedback on behaviora | 13 |
| Self-monitoring of behaviora | 13 | |
| Self-monitoring of outcome(s) of behavior | 8 | |
| Biofeedback | 2 | |
| Feedback on outcome(s) of behavior | 8 | |
| Social support | Social support (unspecified)a | 8 |
| Social support (practical) | 2 | |
| Social support (emotional) | 4 | |
| Shaping knowledge | Instruction on how to perform the behaviora | 2 |
| Information about antecedents | 1 | |
| Natural consequences | Information about health consequencesa | 6 |
| Information about social and environmental consequencesa | 1 | |
| Monitoring of emotional consequences | 4 | |
| Information about emotional consequencesa | 1 | |
| Comparison of behavior | Social comparisona | 8 |
| Associations | Prompts/cues | 7 |
| Repetition and substitution | Behavior substitution | 1 |
| Habit formation | 1 | |
| Graded tasks | 3 | |
| Comparison of outcomes | Credible source | 2 |
| Reward and threat | Non-specific reward | 6 |
| Social reward | 8 | |
| Reward (outcome) | 1 | |
| Antecedents | Adding objects to the environment | 13 |
| Scheduled consequences | Situation-specific reward | 3 |
| Reward incompatible behavior | 1 | |
| Self-belief | Focus on past successes | 7 |
aThis BCT was identified in the literature as associated with successful intervention.
Six techniques were present in half or more of the monitoring systems. Reviewing behavioral goals (10/13 systems) was coded when systems allowed and/or encouraged users to adjust their goals over time. Social support, social comparison, and social reward were also common (8/13 systems). Tools that allowed social support included friending systems and groups, commenting and emoticon systems for communication with others, and the ability to exercise with others virtually in real time. Social comparison was typically found in the form of lists (leaderboards), charts, and direct statements of comparison to other users. Social rewards consisted primarily of opportunities to share accomplishments and progress via social networks. Prompts or cues were found in seven systems. These were typically inactivity or idle alerts. Systems that alerted via a monitor used vibration or flashing lights to attract attention, while those that alerted via mobile device used push notifications. Seven systems also demonstrated a focus on past success, operationalized here as weekly/monthly/yearly emails discussing progress towards goals. Other techniques were found in fewer than half of the systems.
Figure 1 displays examples of screens from the Fitbit (left) and Jawbone (right) apps. See Multimedia Appendix 1 for further examples of the BCTs discussed below, each taken from one of the studied Web/mobile apps. The full listing of BCTs found in each monitoring system is presented in Multimedia Appendix 2.
Figure 1.
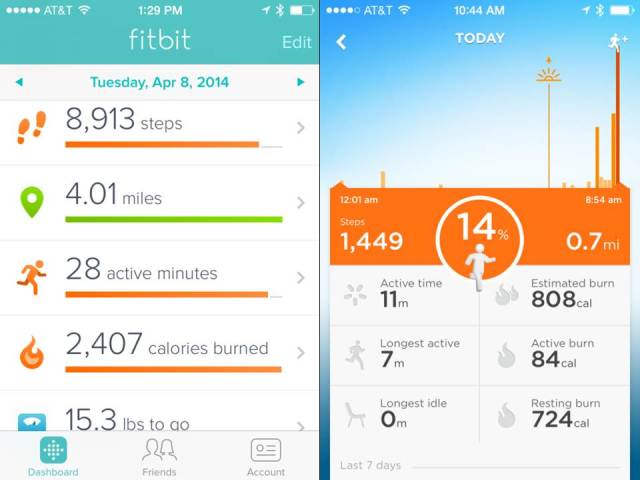
Example screen shots from Fitbit and Jawbone.
Several of the more common techniques were among those found in the literature to be associated with physical activity (shown broken down by monitor system in Multimedia Appendix 3). Goal-setting, self-monitoring, and feedback were found in all of the systems. Social comparison, review of behavioral goals, social support, and social rewards were present in more than half of the monitoring systems. However, several techniques associated with successful interventions were less common. Information about consequences of the behavior and non-specific rewards were each found in six systems. Instruction on performance of the behavior, action planning, and problem solving were rare. Prompting practice, self-rewards, and self-talk were not found.
Table 4 displays theory-based recommendations for goal-setting, self-monitoring, and feedback. Overall, these recommendations were mostly followed by most of the systems. The recommendations less likely to be followed included breaking long-term goals into short-term goals (few systems included both types of goal), progression from easier to more difficult goals, tracking personally valued information, emphasizing performance successes, and comparing performance to norms of similar groups.
Table 4.
Fidelity of monitoring systems to recommendations for goal-setting, self-monitoring, and feedback.
| Technique | Recommendation | Monitors, n |
| Goal-setting | Specific | 13 |
| Measurable | 13 | |
| Moderately challenging | 13 | |
| Long-term goals broken into short-term goals | 6 | |
| Easier goals successfully accomplished before attempting more difficult ones | 3 | |
| Self-monitoring | Conducted regularly | 13 |
| Conducted close in time to target activity | 13 | |
| Track precise information | 13 | |
| Track personally valued information | 6 | |
| Emphasize performance successes | 9 | |
| Focus on behavior modifiable by deliberate effort | 13 | |
| Feedback | Specific | 13 |
| Give a clear idea of how well participant is doing | 13 | |
| Compare performance to past accomplishments | 13 | |
| Compare performance to norms of similar groups | 5 | |
| Compare performance to precise goals | 13 |
Discussion
Principal Findings
Electronic activity monitor systems include a variety of evidence-based BCTs, many of which conform to recommendations for their implementation. The most commonly found techniques were integral to the nature of the monitor: self-monitoring, feedback provision, adding objects to the environment, and goal-setting. Tools that provided or encouraged review of behavioral goals, social support, social comparison, prompts/cues, rewards, and a focus on past success were also common, found in more than half of the systems. Most of the interactive tools for goal-setting, self-monitoring, and feedback conformed to theory-based recommendations. Unfortunately, several techniques associated with successful physical activity intervention were uncommon or absent from the monitor systems, including practice, action planning, and problem solving.
Behavior Change Techniques and eHealth/mHealth
Several recently published articles have provided an overview of the current state of mobile apps for physical activity and weight loss. The results suggest that most apps do not include many BCTs that are thought to be essential to behavioral intervention. For example, one study found that 28% of pediatric obesity prevention apps included goal-setting [20], and a broader study of physical activity apps found that 44% included monitoring of some kind [21]. A study that compared weight loss apps to components of the widely used and validated Diabetes Prevention Program reported better results, with 90% or more including weight loss goals and dietary goals. However, only 20% included a physical activity goal, and fewer than 5% included problem-solving or habit formation [22]. A sample of diabetes apps were found to include a median of only two out of seven self-management behaviors recommended by the American Association of Diabetes Educators [24]. An analysis of fitness video games found greater percentages that included these techniques, such as feedback (17/18), rewards of some kind (16/18), and practice (15/18) [15]. Two content analyses of physical activity apps that used taxonomies of 23 and 26 BCTs, respectively, found that the apps included an average of 5/23 and 8/26 [42,43].
Of the activity monitor apps analyzed here, all 13 included monitoring and goal-setting. Although weight loss was not the primary purpose of most of these systems, 62% (8 /13) included weight loss goals. The prevalence of problem solving (1/13) and habit formation (1/13) was similar to that found in the other apps. As might be expected by the nature of fitness video games versus activity monitor apps, practice was much more prevalent in the video games than in the monitor systems. Rewards were fairly common in the monitor systems (6/13), but not as common as in true video games. These rewards were typical of “gamified” reward systems, including badges and achievements.
The three systems with the most techniques coded (Jawbone, Fitbit, and Nike) included 27, 20, and 19 techniques, respectively, out of the 93 possible. The absolute number of techniques found in a monitoring system may not be informative; in fact, a system with fewer but more effective techniques may ultimately produce a greater impact than a system with more numerous but less effective ones. Further, there exist several iterations of the behavior change taxonomy, ranging from 26 techniques to 93. The total number of possible techniques to be coded makes comparison across studies difficult. A recent meta-analysis of walking and cycling interventions reported that the interventions studied included a mean of approximately six BCTs, ranging from 0-12 out of a possible 26 [36]. A similar study of physical activity interventions among overweight/obese adults found 3-12 techniques out of a possible 40 [38]. The number of techniques found in the monitoring systems studied here ranged from 9-27 out of 93, with most including 12 or more. Upon recalculation using only those techniques that also exist in the 40-item taxonomy [19], we found that the activity monitor systems included 6-12 out of 40 techniques, with an average of 9 techniques per system. Recalculation using the original 26-item taxonomy found an average of 8 techniques out of 26 (range 6-12). Thus, although exact comparison is impossible due to differences in taxonomies over time, it appears that the monitors include a similar number of techniques as can be found in behavioral interventions and a potentially greater number of techniques than found in standard physical activity mobile apps.
Across multiple meta-analyses of physical activity interventions, several techniques were reported to occur in more than half of studied interventions: self-monitoring of behavior, goal-setting, providing instruction, problem solving, and prompting practice [27,28,36,44]. Self-monitoring and goal-setting were also common among the monitoring systems, but instruction, problem solving, and practice were very uncommon. Though the basic content of physical activity interventions and activity monitor systems (self-regulatory techniques such as self-monitoring, goal-setting, and feedback) are the same, monitor systems differ greatly from traditional interventions in the other implemented techniques.
Adherence to Theoretical and Empirical Best Practices
Of the 14 BCTs identified as potentially effective based on their success in previous interventions, five were widely represented across the devices: goal-setting (behavior), review of behavioral goals, feedback of behavior, self-monitoring of behavior, and rewards. Problem solving, action planning, commitment, instruction on how to perform the behavior, and behavioral practice were rare. It may be that these less common techniques are not prioritized by developers or consumers, or perhaps they are more difficult to implement. Problem solving was found in one app, but it provided only generalized tips to overcome problems (some specific to detected behavior and some discussed as common problems). Individualized problem solving would likely be a complex undertaking that would require self-report of barriers and a system for providing automated counseling. Such a system might increase app size unacceptably or be difficult to program. Action planning and commitment occurred in the context of specific challenges that users pledged or committed to undertaking. Gamification such as this appears to be a promising avenue for implementing less common BCTs.
A recent study used classification and regression trees to statistically investigate the effectiveness of combinations of BCTs [45]. The investigators found that a combination of techniques that are now called goal-setting and providing information about consequences was most successful (the analysis used a previous iteration of this taxonomy with slightly different names). They also found that interventions using feedback provision in the absence of review of behavioral goals or information about consequences were the least effective of those studied. Self-monitoring and feedback provision are the backbone of monitor systems, but many systems do not include any kind of information provision regarding specific consequences of behavior. It may be that these bare-bones apps that focus on function do not provide sufficient motivation to encourage consistent activity over time.
Several previous studies have scored apps based on their adherence to theoretical constructs. For a general study of several types of health apps, the mean score found was approximately 8/100, with the highest-scored app receiving 14/100 [17]. For a similar study specific to physical activity apps, the mean score was approximately 10/100, with the highest-scored app rated 28 [16]. It would appear that the activity monitor apps included in this analysis follow theory (here, specifically Social Cognitive Theory) more closely than apps that are not associated with activity monitors. It may be that activity monitors by definition provide behavioral tools that are suggested by Social Cognitive Theory, such as regular, instant, and precise feedback.
The above information leads to the question of what the ideal monitor and monitoring system might include. It is not surprising that two of the most well-known and popular monitors, from Fitbit and Jawbone, were highly adherent to theoretical principles (Fitbit) and evidence-based principles (Jawbone). The Jawbone Up24 was particularly impressive for including all but one of the best practice techniques investigated. However, despite their utility in previous clinical and community interventions, we do not yet know whether these techniques work well in concert and in the context of a wearable device and monitoring app.
Regardless of the number or effectiveness of BCTs included, success for an individual is likely highly influenced by individual preferences and practical issues. For example, the Misfit Shine is the only waterproof monitor of those tested and thus would likely be the most effective for someone who prefers to swim. The BodyMedia, Fitbit, Fitbug, and Jawbone systems provided energy balance information including food logs, which may make them more suitable for weight loss attempts than systems that monitored only activity and weight (although several other monitors can link to other apps that provide this service). Little is known about the reliability and validity of these devices, which could also influence user preferences. Because of the complicated series of variables that potentially influence effectiveness, a decision aid similar to those used in patient-centered outcomes research would be a logical next step for helping potential users choose a monitor in light of their preferences for techniques, game and social functions, appearance, and usability.
Clinical Applications
There exists a large and growing amount of literature demonstrating the utility of Internet- and technology-enhanced (generally called eHealth) energy balance interventions. Although several reviews have found that computer-mediated or telephone-mediated weight loss interventions were less powerful than traditional face-to-face interventions [46,47], a recent meta-regression did not find a significant effect of in-person contact on weight loss at 12 months [40]. Thus, it is currently unclear whether technology-mediated interventions can consistently replicate the effectiveness of standard clinical interventions. Activity monitor apps by definition include self-monitoring and individualized feedback, which are associated with greater effectiveness in technology-based trials [46]. These monitors may be a medium by which more effective tools can be integrated into self-directed, distance interventions.
Although little is known about the efficacy of electronic activity monitors, several clinical trials have provided preliminary data. To our knowledge, three trials have tested BodyMedia’s SenseWear armband, a clinical/research grade armband that is very similar to the commercially available BodyMedia Fit armband. An early study found that adding continuous use of the armband to a 12-week standard behavioral weight loss program produced additional weight loss of approximately 2 kilograms [10]. This finding was not statistically significant in this small sample, but it may be clinically significant if distributed over a large population with respect to disease prevention and health cost reduction. A later study compared a 6-month standard behavioral weight loss (SBWL) program, SBWL plus the armband system, and the armband system alone and found a 5-kilogram difference between SBWL plus armband and SBWL [12]. A 9-month study found a 3-kilogram difference between a SBWL and SBWL plus armband group; however, this difference was not statistically significant [11].
Beyond these more typical implementations for clinical weight loss interventions, electronic activity monitors may also be a useful measure of patient-reported outcomes. Some researchers have begun using patterns of patient ambulation during and after hospitalization as a proxy measure for health, as these patterns can predict readmission [48] and other health outcomes such as quality of life and functional status [49]. Consistent, objective measures provided by these monitors could allow clinicians to identify at-risk individuals for secondary prevention and rehabilitation interventions. The CYCORE (Cyberinfrastructure for Comparative Effectiveness Research) project has demonstrated initial feasibility and acceptability of a system of home-based sensors, including activity monitors, that transmit information to oncologists for early detection of dehydration among head and neck cancer patients [50]. They could also be used to help determine appropriate lengths for hospital stays and to monitor functional independence post-release [51].
Health care professionals’ preferences likely will play a role in how successful a given system is for users who are prescribed the device. Physicians, interventionists, and counselors may find that some of the companion apps are easier to integrate into their personal approach to patient care than others. Ease of surveillance may also play a role in provider choice of monitors. Some monitors more easily lend themselves to various types of surveillance, either by allowing “friends” to view user data, by partnering with other apps that allow for practitioner or friend surveillance, or by allowing users to export their data to third parties. Official methods of transmitting data to practitioners securely do not appear to currently exist in these apps. However, upcoming health information aggregator apps like those made by Apple and Google may provide a method for automatically updating physicians in the future.
Public Health and Community Applications
From a public health perspective, electronic activity monitors hold promise for large-scale, cost-effective activity and energy balance interventions. Much like previous studies of Internet-based behavioral weight loss interventions, monitor-based interventions may be less powerful than standard face-to-face programs [10,12,52]. However, they may also have a greater public health impact due to greater reach, adoption, implementation, and/or maintenance [53]. Initial investigations of the BodyMedia armband have found that it provides a more cost-effective weight loss intervention than standard behavioral weight loss interventions or combinations of the two [52].
Some of the monitors demonstrated a greater emphasis on energy balance, providing tools for monitoring intake, comparing intake to expenditure, and monitoring weight loss (eg, BodyMedia, Fitbit, Fitbug). The apps for BodyMedia, Fitbit, Fitbug, and Withings communicated with smart scales, which automatically uploaded weight measurements to the apps. These monitors and their apps provide interactive tools that mimic a large proportion of the techniques of behavioral weight loss interventions that require skilled interventionist time. These tools could reduce the time needed by interventionists for counseling by creating automated feedback.
Several of the monitoring systems included measurement and cues related to sedentary behavior. Preliminary studies that provided feedback based on baseline analyses of sedentary behavior (using research-grade monitors) produced promising results [54,55]. The existence of commercial monitors that can provide continuous real-time feedback related to sedentary behavior as well as physical activity increases the options available to interventionists. Lumo (sit time, stand ups), Polar (resting, sitting, and low intensities), and Jawbone (longest idle period) monitors measured sedentary behavior and provided mobile phone reminder alerts when sedentary periods extended past a pre-set threshold. These monitors and others that adopt this functionality could be used to implement larger-scale and lower-cost sedentary behavior interventions than those in the past [53].
Rehabilitation Applications
Electronic activity monitors have the potential to significantly improve objective measurement of physical activity for people with chronic diseases and disabilities who receive physical therapy, occupational therapy, and other types of rehabilitation services. While much has been written about the use of pedometers [56,57], accelerometers [56,58,59], and self-report questionnaires [59,60] to measure physical activity for rehabilitation patients, very little has been published expanding to other types of physical activity measurement for these populations. One exception is the development of wearable sensors, such as those described by Bonato et al [61]; however, widespread adoption and testing of wearable technology devices is not evident in the peer-reviewed literature. However, there is agreement among researchers that an effective means of quantifying physical activity is needed. Electronic activity monitors have the potential to offer a solution for gaps in current monitoring systems. For example, these monitors offer researchers and consumers the opportunity to gather physical activity data in real-world conditions such as home and community settings. They also have the capacity to provide real-world behavioral motivation using prompts and intensity measures that are variable or absent in current monitoring methods. Talkowski et al have pointed out the need for accurate physical activity intensity measures that are not currently being accurately evaluated [60]. These authors note that the number of hours of therapy is often a proxy for estimating the intensity of a rehabilitation program, whereas the length of time in therapy may not offer a uniform intensity across patients and over time. An electronic physical activity monitor would provide an objective measure of treatment intensity.
Potential for Unintended Consequences
Though numerous positive applications of these electronic activity monitors exist, there is always the possibility for unintended adverse consequences or ethical dilemmas. The potential for sharing of global positioning system (GPS) location data and personal health information produces clear privacy concerns. Surveillance of the collected data by health care providers may also lead to situations where intervention is deemed ethically necessary. Clear protocols will be necessary to guide provider behavior in such cases and to reduce risks associated with potential privacy breaches.
Because these monitors are commercially available, they can be used by individuals without consultation with medical or public health professionals. Although this widespread availability has benefits for accessibility, it might also increase the risk of negative outcomes if potentially dangerous activity programs are begun without professional oversight. The default activity goals may be inappropriate for older adults, individuals with disabilities or chronic conditions, or children [62]. Though some apps allow users to change their goals, or set goals for them based on a baseline measurement period, others provide pre-set goals that cannot be adjusted. These goals may provoke inappropriately intense activity that could lead to injury.
The validity and reliability of these monitors’ step estimates is as yet unclear. Substantial literature surrounding the validity of the research grade BodyMedia armband exists (eg, [63,64]), but it is not clear whether differences between the research and commercial versions may affect energy expenditure estimates. There is preliminary evidence that one of the Fitbit monitors (worn on the waist) may produce valid estimates of steps, but distance output is inaccurate [65]. Another study found that older Fitbit monitors underestimated energy expenditure [66]. Little is known about newer, wrist-worn monitors or how monitors may differ (both from other commercial monitors and compared to gold standard measures).
Limitations
As a content analysis, this project was by definition preliminary and exploratory. Thus, our conclusions are tentative and require further study. In particular, our coding related to theory-based recommendations and our designation of specific techniques as potentially more effective than others are intended to be first steps towards formal tests as to the true impact of various recommendations or techniques. Only research with human subjects—from small qualitative investigations to large-scale randomized trials—can investigate hypotheses related to feasibility, acceptability, and effectiveness.
The systems tested here were those that measure continuous lifestyle activity that were available for purchase in late 2013. Monitors that had been discontinued (eg, Motorola MOTOACTV and Larklife) could not be tested, nor could a large number of monitors expected to be released in 2014. Follow-up tests should be conducted to include these newer monitors and compare them to earlier models. Also, we did not include monitors that focused specifically on bouts of physical activity (eg, heart rate monitors by Garmin, Polar, Mio) or mobile phone apps that measured activity using GPS or accelerometry within the phone (eg, RunKeeper, phone-based pedometer apps). Our focus on products compatible with Apple iOS, which occurred for practical reasons, may have also led to missing some monitors only available for Android devices if they were not also listed on Amazon or CNET lists. To represent the full range of available options and for use in possible future decision aids, further testing of all these monitoring systems will be necessary.
We chose to use the latest and broadest taxonomy available, which likely contributed to the greater number of techniques found in these systems. Many of the techniques in the larger taxonomy are not used in physical activity intervention (eg, many of the associations techniques are more appropriate for addiction-related interventions) and likely should not be included in activity monitor apps. It is also possible that some techniques are counterproductive or only productive in conjunction with specific other techniques. Even otherwise appropriate techniques, such as behavioral practice, may be unnecessary when the activity being promoted is an activity of daily living like walking. Which techniques are most efficacious is, of course, an empirical question not yet answered.
Finally, coding of ever-changing apps is quite difficult. Some interrater disagreement occurred because only one of the 3 testers engaged in a behavior that triggered use of a specific technique. As all monitors were tested using personal computers and iOS mobile devices, the experiences of Android users may differ from our experiences. Regular app updates also led to differential coding. Although we updated our results prior to publication, it is likely that more techniques will be included across the 13 systems and new systems will be available in the near future.
Conclusions
Electronic activity monitors include many different empirically tested behavior change techniques that are commonly implemented in clinical interventions. Many of these techniques are associated with successful physical activity and/or weight loss, and implementation of most of the techniques adhered closely to theory-based recommendations.
This content analysis provides preliminary information on the extent and type of technique implementation, thus laying a foundation for clinical, public health, and rehabilitation applications. Future studies are needed to further investigate new types of electronic activity monitors and to test their feasibility, acceptability, and ultimately their public health impact.
Acknowledgments
Dr Lyons is supported by a research career development award (K12HD052023: Building Interdisciplinary Research Careers in Women’s Health Program) from the Office of Research on Women’s Health, the Office of the Director, the National Institute of Allergy and Infectious Diseases, and the Eunice Kennedy Shriver National Institute of Child Health and Human Development at the National Institutes of Health. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Dr Lyons is also supported by a Beginning Grant-in-Aid from the American Heart Association (13BGIA17110021). Dr Rowland is supported by a field-initiated grant (H133G080120) from the National Institute on Disability and Rehabilitation Research.
This study was conducted with the support of the Institute for Translational Sciences, supported in part by a Clinical and Translational Science Award (UL1TR000071) from the National Center for Advancing Translational Sciences, National Institutes of Health, and from the Sealy Center on Aging and Claude D Pepper Older Americans Independence Center (P30AG024832) at the University of Texas Medical Branch. This publication was also funded in part by the US Agency for Healthcare Research and Quality through Grant R24HS22134.
The authors would like to acknowledge the assistance of Eloisa Martinez, who served as third coder and provided additional research assistance with this project. Sedonia Holmes and Kelley Prevou also provided administrative and organizational assistance.
Abbreviations
- BCTs
behavior change techniques
- GPS
global positioning systems
- iOS
Apple iPhone/iPad/iPod operating system
- SBWL
standard behavioral weight loss
Multimedia Appendix 1
Screenshot examples of behavior change techniques.
Multimedia Appendix 2
Behavior change techniques by monitor.
Multimedia Appendix 3
Potentially effective techniques by monitor system.
Footnotes
Conflicts of Interest: None declared.
References
- 1.Sattelmair J, Pertman J, Ding EL, Kohl HW, Haskell W, Lee IM. Dose response between physical activity and risk of coronary heart disease: a meta-analysis. Circulation. 2011 Aug 16;124(7):789–95. doi: 10.1161/CIRCULATIONAHA.110.010710. http://circ.ahajournals.org/cgi/pmidlookup?view=long&pmid=21810663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Woodcock J, Franco OH, Orsini N, Roberts I. Non-vigorous physical activity and all-cause mortality: systematic review and meta-analysis of cohort studies. Int J Epidemiol. 2011 Feb;40(1):121–38. doi: 10.1093/ije/dyq104. http://ije.oxfordjournals.org/cgi/pmidlookup?view=long&pmid=20630992. [DOI] [PubMed] [Google Scholar]
- 3.Friedenreich CM, Neilson HK, Lynch BM. State of the epidemiological evidence on physical activity and cancer prevention. Eur J Cancer. 2010 Sep;46(14):2593–604. doi: 10.1016/j.ejca.2010.07.028. [DOI] [PubMed] [Google Scholar]
- 4.Roque FR, Hernanz R, Salaices M, Briones AM. Exercise training and cardiometabolic diseases: focus on the vascular system. Curr Hypertens Rep. 2013 Jun;15(3):204–14. doi: 10.1007/s11906-013-0336-5. [DOI] [PubMed] [Google Scholar]
- 5.Hansen BH, Kolle E, Dyrstad SM, Holme I, Anderssen SA. Accelerometer-determined physical activity in adults and older people. Med Sci Sports Exerc. 2012 Feb;44(2):266–72. doi: 10.1249/MSS.0b013e31822cb354. [DOI] [PubMed] [Google Scholar]
- 6.Moore LV, Harris CD, Carlson SA, Kruger J, Fulton JE. Trends in no leisure-time physical activity--United States, 1988-2010. Res Q Exerc Sport. 2012 Dec;83(4):587–91. doi: 10.1080/02701367.2012.10599884. [DOI] [PubMed] [Google Scholar]
- 7.Kang M, Marshall SJ, Barreira TV, Lee JO. Effect of pedometer-based physical activity interventions: a meta-analysis. Res Q Exerc Sport. 2009 Sep;80(3):648–55. doi: 10.1080/02701367.2009.10599604. [DOI] [PubMed] [Google Scholar]
- 8.Müller-Riemenschneider F, Reinhold T, Nocon M, Willich SN. Long-term effectiveness of interventions promoting physical activity: a systematic review. Prev Med. 2008 Oct;47(4):354–68. doi: 10.1016/j.ypmed.2008.07.006. [DOI] [PubMed] [Google Scholar]
- 9.Vaes AW, Cheung A, Atakhorrami M, Groenen MT, Amft O, Franssen FM, Wouters EF, Spruit MA. Effect of 'activity monitor-based' counseling on physical activity and health-related outcomes in patients with chronic diseases: A systematic review and meta-analysis. Ann Med. 2013 Sep;45(5-6):397–412. doi: 10.3109/07853890.2013.810891. [DOI] [PubMed] [Google Scholar]
- 10.Polzien KM, Jakicic JM, Tate DF, Otto AD. The efficacy of a technology-based system in a short-term behavioral weight loss intervention. Obesity (Silver Spring) 2007 Apr;15(4):825–30. doi: 10.1038/oby.2007.584. [DOI] [PubMed] [Google Scholar]
- 11.Shuger SL, Barry VW, Sui X, McClain A, Hand GA, Wilcox S, Meriwether RA, Hardin JW, Blair SN. Electronic feedback in a diet- and physical activity-based lifestyle intervention for weight loss: a randomized controlled trial. Int J Behav Nutr Phys Act. 2011;8:41. doi: 10.1186/1479-5868-8-41. http://www.ijbnpa.org/content/8//41. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Pellegrini CA, Verba SD, Otto AD, Helsel DL, Davis KK, Jakicic JM. The comparison of a technology-based system and an in-person behavioral weight loss intervention. Obesity (Silver Spring) 2012 Feb;20(2):356–63. doi: 10.1038/oby.2011.13. http://europepmc.org/abstract/MED/21311506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Barwais FA, Cuddihy TF, Tomson LM. Physical activity, sedentary behavior and total wellness changes among sedentary adults: a 4-week randomized controlled trial. Health Qual Life Outcomes. 2013;11:183. doi: 10.1186/1477-7525-11-183. http://www.hqlo.com/content/11//183. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Lowe SA, Ólaighin G. Monitoring human health behaviour in one's living environment: a technological review. Med Eng Phys. 2014 Feb;36(2):147–68. doi: 10.1016/j.medengphy.2013.11.010. [DOI] [PubMed] [Google Scholar]
- 15.Lyons EJ, Hatkevich C. Prevalence of behavior changing strategies in fitness video games: theory-based content analysis. J Med Internet Res. 2013;15(5):e81. doi: 10.2196/jmir.2403. http://www.jmir.org/2013/5/e81/ [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Cowan LT, Van Wagenen SA, Brown BA, Hedin RJ, Seino-Stephan Y, Hall PC, West JH. Apps of steel: are exercise apps providing consumers with realistic expectations?: a content analysis of exercise apps for presence of behavior change theory. Health Educ Behav. 2013 Apr;40(2):133–9. doi: 10.1177/1090198112452126. [DOI] [PubMed] [Google Scholar]
- 17.Azar KM, Lesser LI, Laing BY, Stephens J, Aurora MS, Burke LE, Palaniappan LP. Mobile applications for weight management: theory-based content analysis. Am J Prev Med. 2013 Nov;45(5):583–9. doi: 10.1016/j.amepre.2013.07.005. [DOI] [PubMed] [Google Scholar]
- 18.Michie S, Richardson M, Johnston M, Abraham C, Francis J, Hardeman W, Eccles MP, Cane J, Wood CE. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: building an international consensus for the reporting of behavior change interventions. Ann Behav Med. 2013 Aug;46(1):81–95. doi: 10.1007/s12160-013-9486-6. [DOI] [PubMed] [Google Scholar]
- 19.Michie S, Ashford S, Sniehotta FF, Dombrowski SU, Bishop A, French DP. A refined taxonomy of behaviour change techniques to help people change their physical activity and healthy eating behaviours: the CALO-RE taxonomy. Psychol Health. 2011 Nov;26(11):1479–98. doi: 10.1080/08870446.2010.540664. [DOI] [PubMed] [Google Scholar]
- 20.Schoffman DE, Turner-McGrievy G, Jones SJ, Wilcox S. Mobile apps for pediatric obesity prevention and treatment, healthy eating, and physical activity promotion: just fun and games? Transl Behav Med. 2013 Sep;3(3):320–5. doi: 10.1007/s13142-013-0206-3. http://europepmc.org/abstract/MED/24073184. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.West JH, Hall PC, Hanson CL, Barnes MD, Giraud-Carrier C, Barrett J. There's an app for that: content analysis of paid health and fitness apps. J Med Internet Res. 2012;14(3):e72. doi: 10.2196/jmir.1977. http://www.jmir.org/2012/3/e72/ [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Pagoto S, Schneider K, Jojic M, DeBiasse M, Mann D. Evidence-based strategies in weight-loss mobile apps. Am J Prev Med. 2013 Nov;45(5):576–82. doi: 10.1016/j.amepre.2013.04.025. [DOI] [PubMed] [Google Scholar]
- 23.Breton ER, Fuemmeler BF, Abroms LC. Weight loss-there is an app for that! But does it adhere to evidence-informed practices? Transl Behav Med. 2011 Dec;1(4):523–9. doi: 10.1007/s13142-011-0076-5. http://europepmc.org/abstract/MED/24073074. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Breland JY, Yeh VM, Yu J. Adherence to evidence-based guidelines among diabetes self-management apps. Transl Behav Med. 2013 Sep;3(3):277–86. doi: 10.1007/s13142-013-0205-4. http://europepmc.org/abstract/MED/24073179. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Abroms LC, Padmanabhan N, Thaweethai L, Phillips T. iPhone apps for smoking cessation: a content analysis. Am J Prev Med. 2011 Mar;40(3):279–85. doi: 10.1016/j.amepre.2010.10.032. http://europepmc.org/abstract/MED/21335258. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Abroms LC, Lee Westmaas J, Bontemps-Jones J, Ramani R, Mellerson J. A content analysis of popular smartphone apps for smoking cessation. Am J Prev Med. 2013 Dec;45(6):732–6. doi: 10.1016/j.amepre.2013.07.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Williams SL, French DP. What are the most effective intervention techniques for changing physical activity self-efficacy and physical activity behaviour--and are they the same? Health Educ Res. 2011 Apr;26(2):308–22. doi: 10.1093/her/cyr005. http://her.oxfordjournals.org/cgi/pmidlookup?view=long&pmid=21321008. [DOI] [PubMed] [Google Scholar]
- 28.Olander EK, Fletcher H, Williams S, Atkinson L, Turner A, French DP. What are the most effective techniques in changing obese individuals' physical activity self-efficacy and behaviour: a systematic review and meta-analysis. Int J Behav Nutr Phys Act. 2013;10:29. doi: 10.1186/1479-5868-10-29. http://www.ijbnpa.org/content/10//29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Michie S, Abraham C, Whittington C, McAteer J, Gupta S. Effective techniques in healthy eating and physical activity interventions: a meta-regression. Health Psychol. 2009 Nov;28(6):690–701. doi: 10.1037/a0016136. [DOI] [PubMed] [Google Scholar]
- 30.Rovniak LS, Hovell MF, Wojcik JR, Winett RA, Martinez-Donate AP. Enhancing theoretical fidelity: an e-mail-based walking program demonstration. Am J Health Promot. 2005;20(2):85–95. doi: 10.4278/0890-1171-20.2.85. [DOI] [PubMed] [Google Scholar]
- 31.Turner-McGrievy GM, Campbell MK, Tate DF, Truesdale KP, Bowling JM, Crosby L. Pounds Off Digitally study: a randomized podcasting weight-loss intervention. Am J Prev Med. 2009 Oct;37(4):263–9. doi: 10.1016/j.amepre.2009.06.010. http://europepmc.org/abstract/MED/19765496. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Pearson ES. Goal setting as a health behavior change strategy in overweight and obese adults: a systematic literature review examining intervention components. Patient Educ Couns. 2012 Apr;87(1):32–42. doi: 10.1016/j.pec.2011.07.018. [DOI] [PubMed] [Google Scholar]
- 33.Powell AC, Landman AB, Bates DW. In search of a few good apps. JAMA. 2014 May 14;311(18):1851–2. doi: 10.1001/jama.2014.2564. [DOI] [PubMed] [Google Scholar]
- 34.Eng DS, Lee JM. The promise and peril of mobile health applications for diabetes and endocrinology. Pediatr Diabetes. 2013 Jun;14(4):231–8. doi: 10.1111/pedi.12034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Goyal S, Cafazzo JA. Mobile phone health apps for diabetes management: current evidence and future developments. QJM. 2013 Dec;106(12):1067–9. doi: 10.1093/qjmed/hct203. http://qjmed.oxfordjournals.org/cgi/pmidlookup?view=long&pmid=24106313. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Bird EL, Baker G, Mutrie N, Ogilvie D, Sahlqvist S, Powell J. Behavior change techniques used to promote walking and cycling: a systematic review. Health Psychol. 2013 Aug;32(8):829–38. doi: 10.1037/a0032078. http://europepmc.org/abstract/MED/23477577. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Greaves CJ, Sheppard KE, Abraham C, Hardeman W, Roden M, Evans PH, Schwarz P, IMAGE Study Group Systematic review of reviews of intervention components associated with increased effectiveness in dietary and physical activity interventions. BMC Public Health. 2011;11:119. doi: 10.1186/1471-2458-11-119. http://www.biomedcentral.com/1471-2458/11/119. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Bélanger-Gravel A, Godin G, Vézina-Im LA, Amireault S, Poirier P. The effect of theory-based interventions on physical activity participation among overweight/obese individuals: a systematic review. Obes Rev. 2011 Jun;12(6):430–9. doi: 10.1111/j.1467-789X.2010.00729.x. [DOI] [PubMed] [Google Scholar]
- 39.Task Force on Community Preventive Services Recommendations to increase physical activity in communities. Am J Prev Med. 2002 May;22(4 Suppl):67–72. doi: 10.1016/s0749-3797(02)00433-6. [DOI] [PubMed] [Google Scholar]
- 40.Hartmann-Boyce J, Johns DJ, Jebb SA, Aveyard P, Behavioural Weight Management Review Group Effect of behavioural techniques and delivery mode on effectiveness of weight management: systematic review, meta-analysis and meta-regression. Obes Rev. 2014 Jul;15(7):598–609. doi: 10.1111/obr.12165. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Burke LE, Sereika SM, Music E, Warziski M, Styn MA, Stone A. Using instrumented paper diaries to document self-monitoring patterns in weight loss. Contemp Clin Trials. 2008 Mar;29(2):182–93. doi: 10.1016/j.cct.2007.07.004. http://europepmc.org/abstract/MED/17702667. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Middelweerd A, Mollee JS, van der Wal C, Brug J, Te Velde SJ. Apps to promote physical activity among adults: a review and content analysis. Int J Behav Nutr Phys Act. 2014 Jul 25;11(1):97. doi: 10.1186/s12966-014-0097-9. http://www.ijbnpa.org/content/11/1/97. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Direito A, Dale LP, Shields E, Dobson R, Whittaker R, Maddison R. Do physical activity and dietary smartphone applications incorporate evidence-based behaviour change techniques? BMC Public Health. 2014;14:646. doi: 10.1186/1471-2458-14-646. http://www.biomedcentral.com/1471-2458/14/646. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Ashford S, Edmunds J, French DP. What is the best way to change self-efficacy to promote lifestyle and recreational physical activity? A systematic review with meta-analysis. Br J Health Psychol. 2010 May;15(Pt 2):265–88. doi: 10.1348/135910709X461752. [DOI] [PubMed] [Google Scholar]
- 45.Dusseldorp E, van Genugten L, van Buuren S, Verheijden MW, van Empelen P. Combinations of Techniques That Effectively Change Health Behavior: Evidence From Meta-CART Analysis. Health Psychol. 2013 Nov 25;:-. doi: 10.1037/hea0000018. [DOI] [PubMed] [Google Scholar]
- 46.Wieland LS, Falzon L, Sciamanna CN, Trudeau KJ, Brodney S, Schwartz JE, Davidson KW. Interactive computer-based interventions for weight loss or weight maintenance in overweight or obese people. Cochrane Database Syst Rev. 2012;8:CD007675. doi: 10.1002/14651858.CD007675.pub2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Reed VA, Schifferdecker KE, Rezaee ME, O'Connor S, Larson RJ. The effect of computers for weight loss: a systematic review and meta-analysis of randomized trials. J Gen Intern Med. 2012 Jan;27(1):99–108. doi: 10.1007/s11606-011-1803-9. http://europepmc.org/abstract/MED/21805218. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Fisher SR, Kuo YF, Sharma G, Raji MA, Kumar A, Goodwin JS, Ostir GV, Ottenbacher KJ. Mobility after hospital discharge as a marker for 30-day readmission. J Gerontol A Biol Sci Med Sci. 2013 Jul;68(7):805–10. doi: 10.1093/gerona/gls252. http://europepmc.org/abstract/MED/23254776. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Ferriolli E, Skipworth RJ, Hendry P, Scott A, Stensteth J, Dahele M, Wall L, Greig C, Fallon M, Strasser F, Preston T, Fearon KC. Physical activity monitoring: a responsive and meaningful patient-centered outcome for surgery, chemotherapy, or radiotherapy? J Pain Symptom Manage. 2012 Jun;43(6):1025–35. doi: 10.1016/j.jpainsymman.2011.06.013. [DOI] [PubMed] [Google Scholar]
- 50.Peterson SK, Shinn EH, Basen-Engquist K, Demark-Wahnefried W, Prokhorov AV, Baru C, Krueger IH, Farcas E, Rios P, Garden AS, Beadle BM, Lin K, Yan Y, Martch SL, Patrick K. Identifying early dehydration risk with home-based sensors during radiation treatment: a feasibility study on patients with head and neck cancer. J Natl Cancer Inst Monogr. 2013 Dec;2013(47):162–8. doi: 10.1093/jncimonographs/lgt016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Appelboom G, Yang AH, Christophe BR, Bruce EM, Slomian J, Bruyère O, Bruce SS, Zacharia BE, Reginster JY, Connolly ES. The promise of wearable activity sensors to define patient recovery. J Clin Neurosci. 2014 Jul;21(7):1089–93. doi: 10.1016/j.jocn.2013.12.003. [DOI] [PubMed] [Google Scholar]
- 52.Archer E, Groessl EJ, Sui X, McClain AC, Wilcox S, Hand GA, Meriwether RA, Blair SN. An economic analysis of traditional and technology-based approaches to weight loss. Am J Prev Med. 2012 Aug;43(2):176–82. doi: 10.1016/j.amepre.2012.04.018. [DOI] [PubMed] [Google Scholar]
- 53.Mayrsohn B, Khalil G. Games for Health. In: Krohn R, Metcalf D, editors. mHealth Innovation: Best Practices from the Mobile Frontier. Chicago, IL: HIMSS; 2014. pp. 85–94. [Google Scholar]
- 54.Fitzsimons CF, Kirk A, Baker G, Michie F, Kane C, Mutrie N. Using an individualised consultation and activPAL™ feedback to reduce sedentary time in older Scottish adults: results of a feasibility and pilot study. Prev Med. 2013 Nov;57(5):718–20. doi: 10.1016/j.ypmed.2013.07.017. [DOI] [PubMed] [Google Scholar]
- 55.Gardiner PA, Eakin EG, Healy GN, Owen N. Feasibility of reducing older adults' sedentary time. Am J Prev Med. 2011 Aug;41(2):174–7. doi: 10.1016/j.amepre.2011.03.020. [DOI] [PubMed] [Google Scholar]
- 56.Berlin JE, Storti KL, Brach JS. Using activity monitors to measure physical activity in free-living conditions. Phys Ther. 2006 Aug;86(8):1137–45. http://www.ptjournal.org/cgi/pmidlookup?view=long&pmid=16879047. [PubMed] [Google Scholar]
- 57.Coleman KL, Smith DG, Boone DA, Joseph AW, del Aguila MA. Step activity monitor: long-term, continuous recording of ambulatory function. J Rehabil Res Dev. 1999 Jan;36(1):8–18. [PubMed] [Google Scholar]
- 58.Murphy SL. Review of physical activity measurement using accelerometers in older adults: considerations for research design and conduct. Prev Med. 2009 Feb;48(2):108–14. doi: 10.1016/j.ypmed.2008.12.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Henderson CJ, Lovell DJ, Specker BL, Campaigne BN. Physical activity in children with juvenile rheumatoid arthritis: quantification and evaluation. Arthritis Care Res. 1995 Jun;8(2):114–9. doi: 10.1002/art.1790080210. [DOI] [PubMed] [Google Scholar]
- 60.Talkowski JB, Lenze EJ, Munin MC, Harrison C, Brach JS. Patient participation and physical activity during rehabilitation and future functional outcomes in patients after hip fracture. Arch Phys Med Rehabil. 2009 Apr;90(4):618–22. doi: 10.1016/j.apmr.2008.10.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Bonato P. Advances in wearable technology and applications in physical medicine and rehabilitation. J Neuroeng Rehabil. 2005 Feb 25;2(1):2. doi: 10.1186/1743-0003-2-2. http://www.jneuroengrehab.com/content/2/1/2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Tudor-Locke C, Craig CL, Aoyagi Y, Bell RC, Croteau KA, De Bourdeaudhuij I, Ewald B, Gardner AW, Hatano Y, Lutes LD, Matsudo SM, Ramirez-Marrero FA, Rogers LQ, Rowe DA, Schmidt MD, Tully MA, Blair SN. How many steps/day are enough? For older adults and special populations. Int J Behav Nutr Phys Act. 2011;8:80. doi: 10.1186/1479-5868-8-80. http://www.ijbnpa.org/content/8//80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Berntsen S, Hageberg R, Aandstad A, Mowinckel P, Anderssen SA, Carlsen KH, Andersen LB. Validity of physical activity monitors in adults participating in free-living activities. Br J Sports Med. 2010 Jul;44(9):657–64. doi: 10.1136/bjsm.2008.048868. [DOI] [PubMed] [Google Scholar]
- 64.Cole PJ, LeMura LM, Klinger TA, Strohecker K, McConnell TR. Measuring energy expenditure in cardiac patients using the Body Media Armband versus indirect calorimetry. A validation study. J Sports Med Phys Fitness. 2004 Sep;44(3):262–71. [PubMed] [Google Scholar]
- 65.Takacs J, Pollock CL, Guenther JR, Bahar M, Napier C, Hunt MA. Validation of the Fitbit One activity monitor device during treadmill walking. J Sci Med Sport. 2013 Oct 31;:-. doi: 10.1016/j.jsams.2013.10.241. [DOI] [PubMed] [Google Scholar]
- 66.Dannecker KL, Sazonova NA, Melanson EL, Sazonov ES, Browning RC. A comparison of energy expenditure estimation of several physical activity monitors. Med Sci Sports Exerc. 2013 Nov;45(11):2105–12. doi: 10.1249/MSS.0b013e318299d2eb. [DOI] [PMC free article] [PubMed] [Google Scholar]


