Abstract
Background
The global pandemic of obesity has become a disastrous public health issue that needs urgent attention. Previous studies have concentrated in high-income urban settings and few cover low-income rural settings especially nomadic residents in mountain areas. This study focused on low-income rural and nomadic minority people residing in China’s far west and investigated their prevalence and ethnic differences of obesity.
Methods
A questionnaire-based survey and physical examination of 8,036 individuals were conducted during 2009–2010, using stratified cluster random sampling method in nomadic Kazakhs and rural Uyghur residents (≥18 years old) in 18 villages, Xinjiang, China, about 4,407 km away from capital Beijing. Obesity was defined by BMI and WC.
Results
The overall prevalence of general and abdominal obesity in Kazakh adults were 18.3% and 60.0%, respectively and in Uyghur, 7.6% and 54.5%, respectively. Female’s prevalence of obesity was higher than male’s for general obesity (45–54 age group in Uyghur, P = 0.041) and abdominal obesity (≥55 years in Kazakhs, P55∼ = 0.010, P65∼ = 0.001; and ≥18 years in Uyghurs, P<0.001). Kazakh’s prevalence of obesity was higher than Uyghur’s (general obesity: ≥35 years, P<0.001; abdominal obesity: ≥25 years in males and ≥65 years in females, P<0.01). The prevalence of obesity increased after 18 years old and subsequently decreased after 55 years old. Meat consumption, older age, and female gender had a higher risk of obesity in these two minorities.
Conclusions
Both general and abdominal obesity were common in rural ethnic Kazakhs and Uyghurs. The prevalence rates were different in these two minorities depending on ethnicity, gender, and age. Kazakhs, females and elderly people may be prioritized in prevention of obesity in western China. Because of cost-effectiveness in measuring BMI and WC, we recommend that BMI and WC be integrated into local preventive policies in public health toward screening obesity and related diseases in low-income rural minorities.
Introduction
Obesity has become a global pandemic affecting 200 million men and nearly 300 million women worldwide posting great public health threats to all nations and all races [1]. According to the World Health Organization (WHO), the worldwide prevalence of obesity (body mass index (BMI) ≥30 kg/m2) was almost doubled between 1980 and 2008 with estimated 502 million adults being obese globally by 2008 [2]–[5].
China is a multi-ethnic country and there are more than 10 ethnic groups in Xinjiang Uyghur Autonomous Region, where Kazakhs and Uyghurs are two large inhabitant minority groups. Due to limited resources in public health and poor transportation, there have not been serious investigations to analyze local public health needs including prevalence of obesity and related diseases such as diabetes and cardiovascular diseases. On the other hand, due to differences in religion, culture, lifestyle, diet, and genetic background in these ethnic groups, characterizing the prevalence of obesity may reveal valuable information for making appropriate policies in preventive public health for inhabitant residents in Xinjiang.
In terms of screening for obesity, BMI and waist circumference (WC) measurements are two cost-effective and yet practical indices to identify general and abdominal obesity. It has been reported that in some populations, mean WC increases more rapidly than mean BMI [6]–[10]. It is suggested that using BMI in combination with WC allows more accurate monitoring of obesity.
Studies have shown that prevalence of obesity varies depending on populations and areas [6], [7], [11]–[13]. However, the information is gathered mainly from high-income and urban settings and little is from low-income rural settings. Using BMI and WC, this study has focused on studying two local minority groups, namely Kazakh and Uyghur people, to investigate the prevalence of obesity and possible differences between ethnic groups residing in far western China. Our findings presented may have important implications in preventive public health for medically underserved Muslim minorities.
Methods
Ethics Statement
The Institutional Ethics Review Board (IERB) at the First Affiliated Hospital of Shihezi University School of Medicine approved the study (IERB No. SHZ2010LL01). Standard university hospital guidelines including informed consent, voluntary participation, confidentiality, and anonymity were followed. All participants gave written informed consent before the study began.
Settings and Study Population
The survey was conducted from 2009 to 2010 in Yili (Kazakh) and Kashi (Uyghur) prefectures, respectively, about 4,407 km (2,739 miles) away from Beijing, where approximately 98% of the population are minority Muslim Kazakhs or Uyghurs. Multistage (prefecture-county-township-village) stratified cluster random sampling method was used to select participants. At beginning, we chose these two representative prefectures (Yili and Kashi) according to geographical distributions of the minority populations in Xinjiang, a province in China’s northwest. We randomly selected one county in each prefecture and one township from each county (Nalati Township in Xinyuan County and Jiangbazi Township in Jiashi County). At the last stage, stratified sampling method was used to draw corresponding villages in each township (6 villages in Nalati Township and 12 villages in Jiangbazi Township). We interviewed local Kazakhs and Uyghurs aged 18 years or older residing in the village for at least 6 months. We successfully interviewed a total of 8,036 individuals (3,920 Kazakhs and 4,116 Uyghurs, respectively). The overall response rate was 89.3% (87.1% for Kazakhs and 91.5% for Uyghurs, respectively).
Questionnaire Survey
A self-developed questionnaire was applied to collect detailed information from all respondents during face-to-face interview. The questionnaire consisted of demographic information of respondents (such as age, gender, ethnicity, education level, and marital status, etc.) and personal lifestyles (such as smoking, alcohol intake, physical activity, and dietary habits, etc.).
Physical Examinations
Anthropometric measurements of height, weight and WC were obtained using a standard protocol for participants during the interview and physical examinations [14]. Height was measured to the nearest 0.1 centimeter (cm), without shoes, with the participant’s back square against the wall tape, eyes looking straight ahead with a right-angle triangle resting on the scalp and against the wall. Weight was measured with a lever balance to the nearest 0.1 kilogram (kg) in light undergarments without shoes. WC was defined as the midpoint between the lower rib and upper margin of the iliac crest, measured by a ruler tape with an insertion buckle at one end. WC was measured to the nearest 0.1 cm. Body mass index (BMI) was calculated by dividing weight (in kilograms) by height (in meters) squared (kg/m2).
Definitions
To ensure comparability with other studies, our study incorporated the criteria recommended by the Working Group on Obesity in China (WGOC) (General obesity: BMI ≥28 kg/m2; Abdominal obesity: WC ≥85 cm for men and ≥80 cm for women) [15]. The WHO classifications for Europids (General obesity: BMI ≥30 kg/m2; Abdominal obesity: WC ≥102 cm for men and ≥88 cm for women) [16].
Statistical Analysis
A databank was created using EpiData software (EpiData Association, Odense, Denmark, http://www.epidata.dk/). Data were then analyzed using SPSS (Statistical Program for Social Sciences, version 17.0, 2008). Continuous variables were presented as means ± standard deviations (M±SD) and analyzed using t-test. Categorical variables were expressed as numbers or percentages and analyzed using the Chi-square test and trend test. Adjusted odds ratio (OR) with associated 95% confidence interval (95% CI) for general obesity, and abdominal obesity were calculated from multivariate logistic regression. The official 2000 census data of China was used to calculate age-standardized rates [17]. All statistical tests were two-sided and differences were considered statistically significant when P value <0.05.
Results
Basic Characteristics of the Study Populations
Among 3,920 Kazakh adults, there were 1,551 men (39.6%) and 2,369 women (60.4%) with an average age of (44.19±13.24) years. Among 4,116 Uyghur adults, there were 2,036 men (49.5%) and 2,080 women (50.5%) with an average age of (43.56±17.69) years. The average age, BMI, WC and gender differed significantly among ethnicities (P<0.001 for each comparison). Kazakh adults had greater BMI and WC compared to corresponding Uyghur adults ( Table 1 ).
Table 1. Baseline characteristics of the study population.
| Characteristic | Kazakh | Uyghur | Total | ||||||
| Male | Female | Total | Male | Female | Total | Male | Female | Total | |
| n | 1551 | 2369 | 3920 | 2036 | 2080 | 4116 | 3587 | 4449 | 8036 |
| Age (years)* | 45.10(13.50) | 43.60(13.03) | 44.19(13.24) | 44.17(17.16) | 42.96(18.19) | 43.56(17.69) | 44.57(15.69) | 44.30(15.66) | 43.87(15.68) |
| BMI (kg/m2)* | 24.55(4.14) | 24.17(4.35) | 24.32(4.27) | 22.98(3.12) | 22.70(3.66) | 22.84(3.40) | 23.66(3.68) | 23.48(3.10) | 23.56(3.92) |
| WC (cm)* | 88.37(12.19) | 83.89(12.16) | 85.66(12.36) | 84.95(12.16) | 83.55(25.78) | 84.25(19.44) | 86.44(10.71) | 83.73(19.73) | 84.94(16.39) |
Note: BMI = body mass index, WC = waist circumference, SD = standard deviation. * = Data were expressed as mean (SD).
Prevalence of General Obesity and Abdominal Obesity (by WGOC Criteria)
Table 2 shows the gender- and age-specific prevalence rates of general obesity and abdominal obesity in these two ethnic groups based on the WGOC criteria for BMI and WC classifications. The prevalence of general obesity in Uyghur women was significantly greater than that in Uyghur men in the 45–54 age group (χ2 = 4.156, P = 0.041). The prevalence of abdominal obesity in Kazakh women was significantly higher than that in Kazakh men in the 55–64 and ≥65 age groups (χ2 55− = 6.607, P = 0.010; χ2 65− = 10.779, P = 0.001), respectively. The prevalence of abdominal obesity in Uyghur women was significantly higher than that in Uyghur men in all age groups (≥18 years, P<0.001). It was interesting to note that the prevalence of both general and abdominal obesity increased regardless of gender and ethnicity (including Kazakhs and Uyghurs) after 18 years and subsequently decreased after 55 years old. The prevalence of general obesity peaked at 55–64 years of age among Kazakh adults (χ2male = 61.397, P<0.001; χ2female = 155.032, P<0.001). Among Uyghur adults, the prevalence of general obesity peaked at 35–44 years of age in men and at 45–54 years in women (χ2male = 32.059, P<0.001; χ2female = 40.576, P<0.001). The prevalence rate of abdominal obesity among Kazakh adults peaked at 55–64 years of age in men and at ≥65 years of age in women (χ2male = 163.483, P<0.001; χ2female = 320.470, P<0.001). The prevalence of abdominal obesity among Uyghur adults peaked at 45–54 years of age in men and at 55–64 years of age in women (χ2male = 152.084, P<0.001; χ2female = 152.988, P<0.001).
Table 2. Prevalence of general obesity and abdominal obesity in Kazakh and Uyghur rural adults according to gender and age categories#–WGOC Criteria ## .
| Age(years) | General obesity | Abdominal obesity | ||||||||||
| Kazakh | Uyghur | Kazakh | Uyghur | |||||||||
| Male | Female | Total | Male | Female | Total | Male | Female | Total | Male | Female | Total | |
| 18–24 | 1(1.0) | 3(1.6) | 4(1.4) | 4 (1.5) | 11 (3.8) | 15 (2.7) | 15(15.6) | 42(22.0) | 57(19.9) | 55(20.3) * | 129 (44.9) | 184(33.0) |
| 25–34 | 26(9.0) | 27(6.4) | 53(7.4) | 25 (5.6) | 18 (4.1) | 43 (4.8) | 122(42.1) | 185 (43.7) | 307(43.1) | 147 (32.7) * | 207 (46.7) | 354(39.6) |
| 35–44 | 61 (17.0) | 94 (14.6) | 155 (15.5) | 49 (11.3) | 51 (10.0) | 100 (10.6) | 194(54.2) | 361 (56.1) | 555(55.4) | 227 (52.2)* | 371 (72.6) | 598(63.2) |
| 45–54 | 85(22.2) | 148 (24.5) | 233 (23.6) | 29 (9.6)* | 51 (14.9) | 80 (12.4) | 268(70.0) | 437 (72.2) | 705(71.4) | 178 (58.9)* | 257 (75.1) | 435(67.5) |
| 55–64 | 88 (28.1) | 115 (31.9) | 203 (30.1) | 19 (6.6) | 27 (9.2) | 46 (7.9) | 229(73.2)* | 294 (81.4) | 523(77.6) | 167 (57.8) * | 220 (75.3) | 387(66.6) |
| ≥65 | 25 (22.5) | 43 (29.7) | 68(26.6) | 14 (4.8) | 14 (6.8) | 28 (5.7) | 79(71.2)* | 127 (87.6) | 206(80.5) | 151 (52.2)* | 136 (66.3) | 287(58.1) |
| Overall | 286 (18.4) | 430 (18.2) | 716 (18.3) | 140 (6.9) | 172 (8.3) | 312 (7.6) | 907(58.5) | 1446 (61.0) | 2353(60.0) | 925 (45.4) | 1320 (63.5) | 2245(54.5) |
| χ2trend | 52.40 | 146.04 | 193.63 | 1.70 | 11.09 | 10.41 | 137.98 | 309.24 | 437.07 | 101.08 | 84.64 | 168.190 |
| P value | <0.001 | <0.001 | <0.001 | 0.192 | 0.001 | 0.001 | <0.001 | <0.001 | <0.001 | <0.001 | <0.001 | <0.001 |
Note: # = Data were expressed as n (%). Descriptive characteristics were compared by χ2 test and trend test.
= General obesity: BMI ≥28 kg/m2; Abdominal obesity: WC ≥85 cm for men and ≥80 cm for women.
* = P<0.05 versus female from the same ethnic group and age.
Ethnic Differences in Prevalence for General Obesity and Abdominal Obesity between Kazakh and Uyghur Adults (by WGOC Criteria)
The prevalence rates of general obesity in males, females and overall in Kazakh adults were 14.9%, 15.3%, and 15.0%, respectively and of abdominal obesity, 55.1%, 55.9%, and 53.9%, respectively. The corresponding prevalence rates in Uyghur adults were 6.9%, 7.8%, and 7.4%, respectively for general obesity and 43.7%, 61.3%, and 52.7%, respectively for abdominal obesity. Table 2 shows that the prevalence rates of general obesity in both male and female Kazakhs were significantly greater than those of corresponding male and female Uyghurs in the age groups of ≥35 years (P<0.001 for both comparisons). The prevalence rates of abdominal obesity were the same in Kazakh and Uyghur adults (≥25 years in males, P<0.01; ≥65 years in females, P<0.01).
Comparisons of Prevalence Rates of General Obesity and Abdominal Obesity Using WGOC or WHO Criteria
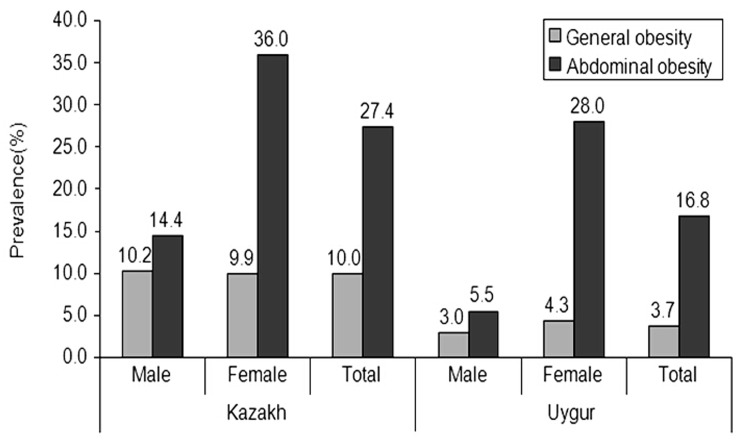
According to the WHO standards, the prevalence rates of general obesity and abdominal obesity among males, females and both sexes in Kazakh adults were 10.2%, 9.9%, and 10.0%, respectively for general obesity, and 14.4%, 36.0%, and 27.4% respectively for abdominal obesity. The corresponding prevalence rates in Uyghur adults were 3.0%, 4.3%, and 3.7%, respectively for general obesity and 5.5%, 28.0%, and 16.8%, respectively for abdominal obesity ( Figure 1 ). For both general and abdominal obesity, the prevalence rates according to the WHO standards were lower than those according to the WGOC standards (P<0.001 for either comparison). Further, the prevalence of abdominal obesity was higher than that of general obesity (P<0.001 for either comparison).
Figure 1. Prevalence of general obesity and abdominal obesity in rural Kazakh and Uyghur adult men and women based on the WHO Criteria.
(General obesity: BMI ≥30 kg/m2; Abdominal obesity: WC ≥102 cm for men, and ≥88 cm for women).
Factors Associated with Differential Prevalence of Obesity in Kazakh and Uyghur Rural Adults
As shown in Table 3, we analyzed factors that may be associated with observed differences in prevalence of obesity as defined by BMI-obesity and abdominal obesity (WGOC criteria) in rural Kazakh and Uyghur Adults using multiple logistic regression analysis. Among Kazakhs, meat consumption of ≥2 kg, older age, female gender, smoking, and drinking appeared to render a higher risk of obesity. On the other hand, consumption of 1–3 plates of vegetables was associated with a lowered risk of obesity. In Uyghur adults, however, meat consumption of at 1 kg, older age, female gender were associated with an increased risk of obesity while consumption of 1–3 plates of fruits and higher levels of education received were each associated with a lower prevalence of obesity.
Table 3. Factors associated with the difference prevalence of obesity from multivariate logistic regression models in Kazakh and Uyghur rural adults*.
| Variables | Kazakh | Uyghur | ||||
| P value | OR value | OR 95% CI | P value | OR value | OR 95% CI | |
| Meat | ||||||
| No or <1 kg per month | 0.004 | 1.000 | <0.001 | 1.000 | ||
| 1–2 kg per month | 0.721 | 0.936 | 0.650∼1.346 | <0.001 | 1.463 | 1.259∼1.700 |
| ≥2 kg per month | 0.043 | 1.467 | 1.031∼2.124 | <0.001 | 1.621 | 1.337∼1.965 |
| Sex | ||||||
| Male | <0.001 | 1.000 | <0.001 | 1.000 | ||
| Female | 0.001 | 1.615 | 1.214∼2.148 | <0.001 | 2.878 | 2.479∼3.341 |
| Age | ||||||
| 18–24 | <0.001 | 1.000 | <0.001 | 1.000 | ||
| 25–34 | <0.001 | 3.422 | 1.980∼5.916 | 0.006 | 1.384 | 1.098∼1.744 |
| 35–44 | <0.001 | 6.342 | 3.667∼10.970 | <0.001 | 3.818 | 3.032∼4.808 |
| 45–54 | <0.001 | 10.617 | 5.900∼19.105 | <0.001 | 4.529 | 3.518∼5.831 |
| 55–64 | <0.001 | 10.722 | 5.662∼20.303 | <0.001 | 4.405 | 3.404∼5.701 |
| ≥65 | <0.001 | 22.726 | 9.793∼52.739 | <0.001 | 3.425 | 2.631∼4.459 |
| Vegetables | ||||||
| No or <1 plate per week | 0.108 | 1.000 | / | / | / | |
| 1–3 plates per week | 0.019 | 0.327 | 0.128∼0.834 | / | / | / |
| 4–6 plates per week | 0.565 | 0.909 | 0.658∼1.257 | / | / | / |
| ≥7 plates per week | 0.276 | 0.850 | 0.635∼1.138 | / | / | / |
| Smoking | ||||||
| No | <0.001 | 1.000 | ||||
| Yes | 0.010 | 1.472 | 1.096∼1.977 | / | / | / |
| Drinking | ||||||
| No | <0.001 | 1.000 | ||||
| Yes | <0.001 | 2.578 | 1.601∼4.153 | / | / | / |
| Fruit | ||||||
| No or <1 plate per week | / | / | / | 0.073 | 1.000 | |
| 1–3 plates per week | / | / | / | 0.046 | 0.814 | 0.665∼0.997 |
| ≥4 plates per week | / | / | / | 0.058 | 0.866 | 0.745∼1.005 |
| Education | ||||||
| Illiteracy | / | / | / | <0.001 | 1.000 | |
| Primary school | / | / | / | <0.001 | 0.606 | 0.493∼0.746 |
| Junior high school | / | / | / | <0.001 | 0.350 | 0.276∼0.443 |
| ≥ Senior high school | / | / | / | <0.001 | 0.374 | 0.249∼0.562 |
Note: OR = odd ratio, CI = confidence interval. / = Data not available. * = Obesity was combined with general obesity and abdominal obesity.
Discussion and Conclusions
Obesity is a serious chronic disease itself and a significant risk factor for many other diseases such as diabetes and cardiovascular diseases [18]–[19]. Rapid economic growth in China has led to significant changes in life style, including diet and physical activity, which in turn lead to an increase in prevalence of obesity [20]–[22]. Based on the data provided by the China Health and Nutrition Survey (CHNS), the prevalence of general obesity increased 168% from 1993 to 2009 (4.0% in 1993 and 10.7% in 2009) and the prevalence of abdominal obesity increased 101% during the same period (18.6% in 1993 and 37.4% in 2009) [23]. Similar trends in the prevalence of obesity have been observed among US, Spain and Brazil adults [24]–[26]. These observations indicate an urgency to study and prevent this global public health issue of obesity pandemic.
The current study has intended to investigate the epidemiologic features of general and abdominal obesity in rural Kazakh and Uyghur adults in northwest China. Based on WHO criteria, we have found that, in Kazakhs, the overall prevalence rates of general and abdominal obesity in the studied population are as high as 10.0% (general obesity) and 27.4% (abdominal obesity), respectively. In Uyghurs, the prevalence of general obesity has reached 3.7% and that of abdominal obesity, 16.8%, respectively. Using the Chinese WGOC criteria, the corresponding prevalence rates of general obesity in Kazakhs are 18.3%, and abdominal obesity, 60.0%, respectively and the prevalence of general obesity in Uyghurs is 7.6% and abdominal obesity, 54.5%, respectively. As shown in Table 4, the prevalence rates of general and abdominal obesity in rural Chinese Kazakh and Uyghur adults are lower than in urban adults in several developed countries [24]–[26], but are higher than Chinese Han adults no matter in urban or rural areas (general obesity in Uyghur was excepted) [23], [27], especially abdominal obesity. The prevalence rates of general obesity and abdominal obesity in these two minorities are more than doubled as compared with those of majority Han Chinese. Our results of general obesity are consistent with the observations by our colleagues in Kashi Prefecture [28].
Table 4. A comparison of general obesity and abdominal obesity from selected ethnic groups within China and in the world.
| Ethnicity | Residency | N | Age(years) | GO (%) | AO (%) | Reference |
| Kazakh | Xinyuan rural, China | 3,920 | ≥18 | 18.3 | 60.0 | this study* |
| Uyghur | Jiashi rural, China | 4,116 | ≥18 | 7.6 | 54.5 | this study* |
| Han | Urban & rural, China | 9,365 | ≥18 | 10.7 | 37.4 | [23]* |
| Kazakh | Xinyuan rural, China | 3,920 | ≥18 | 10.0 | 27.4 | this study# |
| Uyghur | Jiashi rural, China | 4,116 | ≥18 | 3.7 | 16.8 | this study# |
| American | Urban, USA | 22,872 | ≥20 | 33.6 | 52.9 | [24] # |
| Spanish | Urban, Spain | 12,883 | ≥18 | 22.9 | 36.0 | [25] # |
| Brazilian | Urban, Brazil | 2,448 | ≥20 | 26.1 | 30.0 | [26] # |
| Han | Urban, China | 25,196 | 18–74 | 5.2 | 12.2 | [27] # |
Note: GO = general obesity, AO = abdominal obesity. * = Using WGOC standard (General obesity: BMI ≥28 kg/m2; Abdominal obesity: WC ≥85 cm for men and ≥80 cm for women), # = Using WHO standard (General obesity: BMI ≥30 kg/m2; Abdominal obesity: WC ≥102 cm for men and ≥88 cm for women). Han = Chinese ethnic Han majority.
Gender and age are strongly associated with the prevalence of obesity. Reynolds et al. [29] have reported that women have higher prevalence of obesity than men no matter which cut-offs are used. Wang H et al. [27] have observed that the prevalence of general and abdominal obesity is initially increased and then decreased with age. Our current study has demonstrated similar trends in rural Chinese Kazakh and Uyghur adults, in keeping with previous findings [27]. The gender difference in developing obesity may be due to differences in body composition or sex steroid hormone levels between men and women [30], [31]. Differences in pattern of labor (working outside for men and doing housework for women), levels of physical activity, and social status may also play important roles in the gender difference in developing obesity [32]. Decreased physical activity with age [33], and the survivor effect as those people died at an earlier age due to obesity-related diseases may be closely associated with the subsequent decline in obesity prevalence with age [34]. The gender and age differences in obesity occurrence in rural Chinese Kazakh and Uyghur adults suggest that female and elderly populations should be prioritized in preventive public health in far western China. On the other hand, our findings that females are at a higher risk of obesity may have important implications in national screening programs, such as screening for breast cancer and for cervical cancer currently performed in China, in which a simple addition of measuring BMI and/or WC would give participant women an opportunity for diagnosis of obesity. Furthermore, those women diagnosed as having obesity may be offered chance to be screened for obesity-related diseases such diabetes and cardiovascular diseases.
Our current data show that the prevalence of both general and abdominal obesity in Kazakh adults is higher than Uyghur adults by any definition. Similarly, ethnic differences in the prevalence of obesity have been reported in the US, UK, Norway, and Netherlands [6], [7], [10], [35]–[37]. Kazakhs are nomadic and resides in mountainous areas where outdoor activities are impractical in cold winter season. The primary foods these two minorities consume are wheat, beef, mutton, and dairy products, which contain high fat. Living in plains, Uyghurs drink and smoke less, but consume more fruits and vegetables than Kazakhs. Results by multiple logistic regression analysis let us to suggest that ethnic differences in the prevalence of obesity between Kazakhs and Uyghurs may be due to many factors including age, sex, education, smoking, drinking, vegetables, meat, fruits that are different from other geographic regions in China. On the other hand, molecular studies have demonstrated that Kazakh and Uygur populations reside at borders with countries where Caucasian and Asian peoples are mixed [38]. For example, Uyghurs have a mixture of 60% European ancestry and 40% East Asian ancestry [39], which may explain, at least in part, the genetic influence on the two studied minorities whose abdominal obesity rate is higher than Asians (Han Chinese) but lower than Europeans (Table 4).
Xi B et al. have reported that approximately two-thirds of individuals with obesity may be missed if screening by BMI alone, and WC measurement can provide additional information beyond that provided by BMI for accurate prediction of obesity-associated complications [23]. In this study, the prevalence rate of abdominal obesity is greater than that of general obesity in both rural Kazakh and Uyghur adults may echo those previous findings. Therefore, it is important to use a comprehensive program, including both BMI and WC, to evaluate prevalence, trends, and public health significance of obesity as previously suggested [40]. Furthermore, many studies have suggested that, comparing with Caucasians, Asians have more central distribution of body fat under a given BMI [41], [42], which can magnify the numerical differences between the two types of obesity. Although all types of obesity are significantly increased in Chinese adults, the increase in abdominal obesity is the most significant and such unbalanced increase may further widen the prevalence gap between general obesity and abdominal obesity in Chinese [23]. Moreover, rural adults are more likely to be overweight or obese than urban adults [43], implicating a serious challenge to public health policies in preventing obesity because there would be much limited resources in rural settings especially in rural areas where ethnic minorities reside.
Although this study did not collect social-economic and environmental variables which would have impact on obesity and our study could not establish causal relations due to a cross-sectional design, our study maintained a large sample size in two major minorities in northwest China, which allowed exploring the prevalence of obesity over a range of demographic groups. These findings provide important demographic insights into the growing problem of obesity in rural Kazakh and Uyghur populations.
In both Yili and Kashi Prefectures, most Kazakhs and Uyghurs reside in low-income rural communities where public health resources are limited. For example, in Uyghur concentrated Jiashi county, more than 92% of Uyghurs live on US$1.00 per day or less, a sharp contrast to the national average of 15.9% of people living on US$1.00 per day in 2005 [28], [44]. As chronic diseases such as type 2 diabetes and cardiovascular diseases are common in these low-income rural communities, our data presented here strongly support a cost-effective, two-step screening strategy: first to screen for obesity using the simplest BMI and then to screen persons with obesity for diabetes and cardiovascular diseases using more sophisticated measures [28]. Going one step further to see an immediate impact of this two-step screening strategy on public health, we would like to recommend that BMI and WC examinations be incorporated into the currently running national screening programs for cervical cancer and breast cancer in China. In addition, this two-step screening strategy may also be beneficial in routine health screening in most healthcare organizations by which a large number of obese individuals may be detected and offered preventive measures before they progress to diabetes and/or cardiovascular diseases. In this context, place our observations and recommendations over the making of appropriate policies in public health would not only benefit low-income populations but also help middle-income individuals choose suitable strategies for disease prevention.
Data Availability
The authors confirm that all data underlying the findings are fully available without restriction. All relevant data are within the article's Supporting Information files.
Funding Statement
This research was supported by the National Key Technology R&D Program of China (Grant No. 2009BAI82B04). The funder had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
References
- 1. World Health Organization (WHO) (2013) Obesity and overweight. WHO Fact Sheet No. 311: 2013. [Google Scholar]
- 2.WHO (2012) World health statistics. Geneva: World Health Organization, 2012.
- 3. Kaidar-Person O, Bar-Sela G, Person B (2011) The two major epidemics of the twenty-first century: Obesity and cancer. Obes Surg 21: 1792–1797. [DOI] [PubMed] [Google Scholar]
- 4.WHO (2008) Global strategy on diet, physical activity and health: a framework to monitor and evaluate implementation. Geneva: World Health Organization, 2008.
- 5. Finucane MM, Stevens GA, Cowan MJ, Danaei G, Lin JK, et al. (2011) National, regional, and global trends in body-mass index since 1980: Systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9.1 million participants. Lancet 377: 557–567. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Flegal KM, Carroll MD, Kit BK, Ogden CL (2012) Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999–2010. JAMA 307: 491–497. [DOI] [PubMed] [Google Scholar]
- 7. Flegal KM, Carroll MD, Ogden CL, Curtin LR (2010) Prevalence and trends in obesity among US adults, 1999–2008. JAMA 303: 235–241. [DOI] [PubMed] [Google Scholar]
- 8. Elobeid MA, Desmond RA, Thomas O, Keith SW, Allison DB (2007) Waist circumference values are increasing beyond those expected from BMI increases. Obesity (Silver Spring) 15: 2380–2383. [DOI] [PubMed] [Google Scholar]
- 9. Ko GT, Tang JS, Chan JC (2010) Worsening trend of central obesity despite stable or declining body mass index in Hong Kong Chinese between 1996 and 2005. Eur J Clin Nutr 64: 549–552. [DOI] [PubMed] [Google Scholar]
- 10. Ford ES, Li C, Zhao G, Tsai J (2011) Trends in obesity and abdominal obesity among adults in the United States from 1999–2008. Int J Obes (Lond) 35: 736–743. [DOI] [PubMed] [Google Scholar]
- 11. McLellan F (2002) Obesity rising to alarming levels around the world. Lancet 359: 1412. [DOI] [PubMed] [Google Scholar]
- 12. Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, et al. (2006) Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 295: 1549–1555. [DOI] [PubMed] [Google Scholar]
- 13. Gao Y, Ran XW, Xie XH, Lu HL, Chen T, et al. (2006) Prevalence of overweight and obesity among Chinese Yi nationality: A cross-sectional study. BMC Public Health 11: 919. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. WHO (2000) Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser 894: 1–253. [PubMed] [Google Scholar]
- 15. Chen C, Lu FC (2004) Department of Disease Control Ministry of Health, People’s Republic China (2004) The guidelines for prevention and control of overweight and obesity in Chinese adults. Biomed Environ Sci 17: 1–36. [PubMed] [Google Scholar]
- 16. WHO (2003) Diet, nutrition and the prevention of chronic diseases. World Health Organ Tech Rep Ser 916: 1–149. [PubMed] [Google Scholar]
- 17.Population Census Office under the State Council of China, National Bureau of Statistics of China (2002) Tabulation on the 2000 population census of People’s Republic of China. Beijing: China Statistics Press.
- 18. Lorig K, Ritter PL, Plant K, Laurent DD, Kelly P, et al. (2013) The South Australia Health Chronic Disease Self-Management Internet Trial. Health Educ Behav 40: 67–77. [DOI] [PubMed] [Google Scholar]
- 19. Hamer M, Stamatakis E (2012) Metabolically healthy obesity and risk of all-cause and ardiovascular disease mortality. J Clin Endocrinol Metab 97: 2482–2488. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Hou X, Jia W, Bao Y, Lu H, Jiang S, et al. (2008) Risk factors for overweight and obesity, and changes in body mass index of Chinese adults in Shanghai. BMC Publ Health 8: 389. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Chen CM (2008) Overview of obesity in Mainland China. Obes Rev 9: 14–21. [DOI] [PubMed] [Google Scholar]
- 22. Wang Y, Mi J, Shan XY, Wang QJ, Ge KY (2007) Is China facing an obesity epidemic and the consequences? The trends in obesity and chronic disease in China. Int J Obesity 31: 177–188. [DOI] [PubMed] [Google Scholar]
- 23. Xi B, Liang Y, He T, Reilly KH, Hu Y, et al. (2012) Secular trends in the prevalence of general and abdominal obesity among Chinese adults, 1993–2009. Obes Rev 13: 287–296. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Ford ES, Li C, Zhao G, Tsai J (2011) Trends in obesity and abdominal obesity among adults in the United States from 1999–2008. Int J Obes (Lond) 35: 736–743. [DOI] [PubMed] [Google Scholar]
- 25. Gutiérrez-Fisac JL, Guallar-Castillón P, León-Muñoz LM, Graciani A, Banegas JR, et al. (2012) Prevalence of general and abdominal obesity in the adult population of Spain, 2008–2010: The ENRICA study. Obes Rev 13: 388–392. [DOI] [PubMed] [Google Scholar]
- 26. Linhares Rda S, Horta BL, Gigante DP, Dias-da-Costa JS, Olinto MT (2012) Distribution of general and abdominal obesity in adults in a city in southern Brazil. Cad Saude Publica 28: 438–447. [DOI] [PubMed] [Google Scholar]
- 27. Wang H, Wang J, Liu MM, Wang D, Liu YQ, et al. (2012) Epidemiology of general obesity, abdominal obesity and related risk factors in urban adults from 33 communities of Northeast China: The CHPSNE study. BMC Public Health 12: 967. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Cong L, Zhan JQ, Yang L, Zhang W, Li SG, et al. (2014) Overweight and Obesity among Low-Income Muslim Uyghur Women in Far Western China: Correlations of Body Mass Index with Blood Lipids and Implications in Preventive Public Health. PLoS One 9: e90262. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Reynolds K, Gu D, Whelton PK, Wu X, Duan X, et al. (2007) Prevalence and risk factors of overweight and obesity in China. Obesity (Silver Spring) 15: 10–18. [DOI] [PubMed] [Google Scholar]
- 30. Kim J, Wang Z, Heymsfield SB, Baumgartner RN, Gallagher D (2002) Total-body skeletal muscle mass: estimation by a new dual-energy X-ray absorptiometry method. Am J Clin Nutr 76: 378–383. [DOI] [PubMed] [Google Scholar]
- 31. Baghaei F, Rosmond R, Westberg L, Hellstrand M, Eriksson E, et al. (2003) The YP19 gene and associations with androgens and abdominal obesity in premenopausal women. Obes Res 11: 578–585. [DOI] [PubMed] [Google Scholar]
- 32. Chau JY, van der Ploeg HP, Merom D, Chey T, Bauman AE (2012) Cross-sectional associations between occupational and leisure-time sitting, physical activity and obesity in working adults. Prev Med 54: 195–200. [DOI] [PubMed] [Google Scholar]
- 33. Martínez-Ros MT, Tormo MJ, Navarro C, Chirlaque MD, Pérez-Flores D (2001) Extremely high prevalence of overweight and obesity in Murcia, a Mediterranean region in south-east Spain. Int J Obes Relat Metab Disord 25: 1372–1380. [DOI] [PubMed] [Google Scholar]
- 34.National Heart Lung and Blood Institute (1998) Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults–The Evidence Report. National Institutes of Health. Obes Res Suppl 2: 51S–209S. [PubMed]
- 35. Kershaw KN, Albrecht SS, Carnethon MR (2013) Racial and ethnic residential segregation, the neighborhood socioeconomic environment, and obesity among Blacks and Mexican Americans. Am J Epidemiol 177: 299–309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Nystad T, Melhus M, Brustad M, Lund E (2010) Ethnic differences in the prevalence of general and central obesity among the Sami and Norwegian populations: The SAMINOR study. Scand J Public Health 38: 17–24. [DOI] [PubMed] [Google Scholar]
- 37. Agyemang C, Kunst A, Bhopal R, Zaninotto P, Nazroo J, et al. (2011) Dutch versus English advantage in the epidemic of central and generalised obesity is not shared by ethnic minority groups: comparative secondary analysis of cross-sectional data. Int J Obes (Lond) 35: 1334–1346. [DOI] [PubMed] [Google Scholar]
- 38. Katsuyama Y, Inoko H, Imanishi T, Mizuki N, Gojobori T, et al. (1998) Genetic relationships among Japanese, northern Han, Hui, Uygur, Kazakh, Greek, Saudi Arabian, and Italian populations based on allelic frequencies at four VNTR (D1S80, D4S43, COL2A1, D17S5) and one STR (ACTBP2) loci. Hum Hered 48: 126–37. [DOI] [PubMed] [Google Scholar]
- 39. Xu S, Huang W, Qian J, Jin L (2008) Analysis of genomic admixture in Uyghur and its implication in mapping strategy. American Journal of Human Genetics 82: 883–894. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Kwan ML, John EM, Caan BJ, Lee VS, Bernstein L, et al. (2014) Obesity and mortality after breast cancer by race/ethnicity: the california breast cancer survivorship consortium. Am J Epidemiol 179: 95–111. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Deurenberg P, Yap M, van Staveren WA (1998) Body mass index and percent body fat: A meta analysis among different ethnic groups. Int J Obes Relat Metab Disord 22: 1164–1171. [DOI] [PubMed] [Google Scholar]
- 42. Chang CJ, Wu CH, Chang CS, Yao WJ, Yang YC, et al. (2003) Low body mass index but high percent body fat in Taiwanese subjects: Implications of obesity cutoffs. Int J Obes Relat Metab Disord 27: 253–259. [DOI] [PubMed] [Google Scholar]
- 43. Tian H, Xie H, Song G, Zhang H, Hu G (2009) Prevalence of overweight and obesity among 2.6 million rural Chinese adults. Prev Med 48: 59–63. [DOI] [PubMed] [Google Scholar]
- 44. Zhang WJ, Li F, Wang YH, Simayi D, Saimaiti A, et al. (2013) The case for semi-mandatory HPV vaccination in China. Nature Biotechnology 31: 590–1. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The authors confirm that all data underlying the findings are fully available without restriction. All relevant data are within the article's Supporting Information files.