Abstract
Family plays an important role in the lives of injecting drug users (IDUs) in Vietnam. This study examined the preliminary outcomes of an intervention targeting IDUs and their family members in Vietnam. Eighty-three families, including 83 IDUs and 83 family members, were recruited from 4 communes in Phú Tho Province, Vietnam. The 4 communes were randomized to either an intervention condition or a standard care condition. The IDUs and their family members in the intervention condition completed 4 group sessions, with the aims to improve their mental health and family relations and to promote positive behavioral change. The intervention effect was evaluated at baseline and 3- and 6-month follow-up assessments. A significant reduction in depressive symptoms and improvement in family functioning were reported for IDUs in the intervention group compared with those in the standard care group. The family members in the intervention group reported better coping skills at 3 months, fewer depressive symptoms at 6 months, and improved family function at both 3 and 6 months compared with those in the standard care group. However, no significant intervention effect was observed for IDUs in terms of drug-using behavior. This study demonstrates the feasibility and preliminary outcomes of an intervention that simultaneously targets IDUs and their family members in Vietnam. Study findings highlight the importance of including family members and enhancing their role in drug use intervention efforts.
Keywords: injecting drug users, family members, intervention, Vietnam
Located in the Golden Triangle, a hotbed of opium production, Vietnam is experiencing a severe epidemic of drug use (Hoffman, Nguyen, Kershaw, & Niccolai, 2011). In 2009, it was estimated that there were about 150,000 drug users in the country, 83% of whom were injection heroin users (Ministry of Labor Invalid and Social Affairs of Vietnam, 2010). A high level (47–81%) of needle sharing among injecting drug users (IDUs) has been observed across different provinces (Hammett et al., 2012; Hoa & Doussantousse, 2001; Tuan et al., 2007; Tuan, Long, Vinh, & Detels, 2001). The epidemic of drug use has become a serious challenge in Vietnam and deserves immediate attention (Nguyen & Scannapieco, 2008).
In Vietnam, families play an important role and exert the most important contextual influence in the lives of IDUs (Go et al., 2011). Most IDUs have daily family contact or live in their parents’ home, so the family is the principal source of support for IDUs (Ogden & Nyblade, 2005; Rudolph et al., 2012; Salter et al., 2010). Drug-using behavior and its consequences significantly impact not only the physical and mental health of individual IDUs, but also the well-being of the family as a whole. Therefore, interventions targeting family members and IDUs have been identified as a public health priority (Hammett et al., 2006).
Despite a great deal of attention to the IDU population in Vietnam (Hammett et al., 2006, 2012; Khoat, West, Valdiserri, & Phan, 2003; Ngo, Schmich, Higgs, & Fischer, 2009), little research has been done for interventions targeted specifically to IDUs and their families. The current study is a 2-year intervention pilot targeting IDUs and their family members in Vietnam. The primary focus is to examine whether the intervention will improve mental health and family well-being of IDUs and their family members.
Method
Study Design and Participants
The intervention pilot was conducted from August 2011 to February 2012 in Phú Tho Province, one of the poorest provinces in northern Vietnam. Four communes (a community-level subdivision) were randomly selected from all communes in the province. The four selected communes are all in urban areas, and they were matched into two pairs based on geographic area and number of IDUs. After the baseline assessment, the two communes in each pair were randomized to either an intervention or a standard care condition. The distance between the intervention and standard care communes was far enough to avoid contamination. The study was approved by the Institutional Review Boards of the University of California, Los Angeles, and the Vietnam National Institute of Hygiene and Epidemiology.
All IDU participants were recruited from commune health centers (CHCs) in each of the selected communes. In Vietnam, service providers in the CHC provide curative and preventive health services, such as referrals for HIV testing, counseling, and preventive education to IDUs in the community (World Health Organization, 2010). They have developed direct working relationships with IDUs in their communes through their routine practices. The CHC providers introduced the project through verbal explanation and a printed flier to IDUs, who were then referred to a study recruiter. The recruiter met with prospective IDUs who were interested in participating and screened them individually for eligibility. The inclusion criteria were age 18 or older, a history of injecting drug use, residence in the participating commune, and willingness to invite a family member to participate in the study. Upon enrolling, IDUs and, with their consent, family members were recruited. The inclusion criteria for family member participants were age 18 or older, immediate or extended family member of the recruited IDU and living with the IDU, and previous knowledge of the drug use status of the IDU participant. When recruiting IDUs and family members, the recruitment staff followed standardized scripts to explain the purpose of the study, procedures, its voluntary nature, and potential risks and benefits. Written informed consent was obtained. A total of 78% of the prospective participants contacted agreed to participate in the study.
Intervention
The intervention, entitled “Intervention V,” was developed based on fieldwork with local commune stakeholders, service providers, and IDUs and their family members in Vietnam. Intervention topics and contents were designed to reflect the challenges faced by the target population. Four intervention sessions were delivered separately for IDUs and family members, each in a group format with 10 participants, over the course of 4 consecutive weeks. Sessions for IDU and family members shared common topics and themes, including (1) my family, (2) my responsibility, (3) my support, and (4) my community. Session 1 focused on the importance of family support, and addressed healthy family routines and caregiving; Session 2 aimed to overcome family challenges, manage negative emotion, and learn coping skills; Session 3 emphasized the development of realistic goals and supporting positive behavioral changes; and Session 4 encouraged breaking barriers of societal stigma in order to integrate into their community. Interactive activities such as games, pair-share, and role-play were included to encourage participants’ full involvement. Although the theme and format of IDUs’ and family member’s sessions were similar, there were different focuses and contents for the two populations. The IDU sessions emphasized making positive behavior change for the well-being of the family, and the intervention for family members focused on dealing with the burden of being a caregiver and providing positive support for the IDUs. Homework activities were assigned at the end of each session for the IDUs and family members to work on together to strengthen the interaction between IDUs and their family members. Two booster sessions were conducted 2 months and 4 months after the initial group sessions to reinforce the intervention effort.
A local team of facilitators delivered the intervention to ensure regional relevancy and sustainability. The facilitation team consisted of health educators from provincial AIDS committees and local commune health workers with experience interacting with IDUs and their family members. Most facilitators had associate or undergraduate medical degrees, and all facilitators went through extensive training on research ethics, facilitation skills, intervention principles and delivery, session-by-session content flow and practice, and procedures for emergency situations. All intervention sessions were delivered in the native language and incorporated local cultural elements. Project evaluators observed all group sessions to ensure the fidelity of the intervention.
Assessments and Follow-Ups
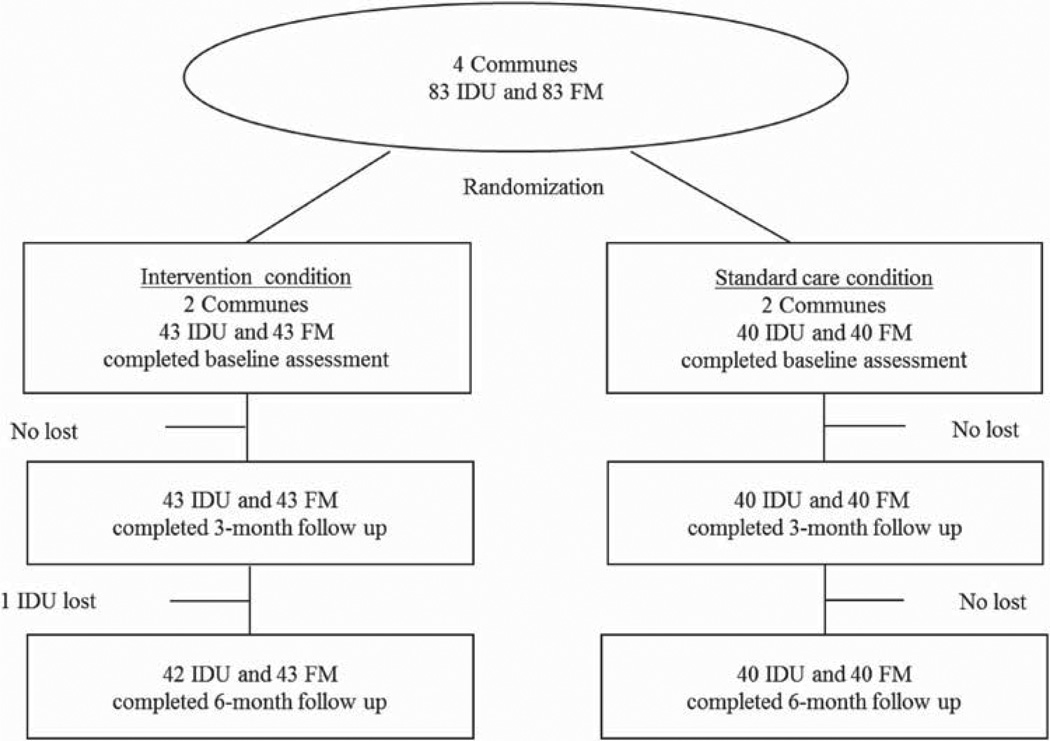
The intervention outcomes were evaluated at baseline and 3-and 6-month follow-ups. The assessments were administered face-to-face by trained interviewers in a private location. Each assessment took about 45 to 60 min. Participants were paid 80,000 dong (about U.S. $5) for each assessment. The follow-up rate was 100% for family members and 98% for IDUs. No significant difference was observed in attrition rate between the intervention conditions (see Figure 1).
Figure 1.
Study flow chart. FM = family member; IDU = injecting drug user.
Several measurement scales were used in the study. Depressive symptoms reported by IDUs and family members were measured by using a short version of the Zung Self-Rating Depression Scale (Zung, 1965). This 10-item instrument was adapted from the original 20-item questionnaire and was successfully used in China (Li, Liang, Ding, & Ji, 2011). The participants were asked how often they feel a particular sentiment (e.g., “I feel down-hearted and blue”) in 10 situations. Response categories ranged from 1 (α little of the time) to 4 (most of the time). A higher overall score indicates a higher level of depressive symptoms (α = .84 for IDU and .75 for family members). Family functioning was reported by IDUs and family members using the Family Functioning Scale (Bloom, 1985; Bloom & Naar, 1994). Three subscales (Family Cohesion, Family Conflict, and Family Sociability) were adapted from the original 15 subscales. The three subscales contained 15 items. Participants evaluated how true each item was for their family on a 4-point scale from 1 (very untrue) to 4 (very true). With some items being reverse-coded, a higher score indicates better family functioning (α = .84 for IDU and .86 for family members). Family members’ level of coping was measured using the Brief COPE Scale (Carver, 1997). Four of 14 subscales were chosen from the original instrument (Active Coping, Planning, Positive Framing, and Acceptance), with two items for each subscale. Responses ranged from 1 (not at all) to 4 (a lot), and a higher score indicates better coping (α = .88).
Drug-using behavior was calculated with the Addiction Severity Index (McLellan et al., 1992). IDUs were queried on the frequency of their illicit substance use (e.g., heroin, other opiates/analgesics, amphetamine, cocaine, hallucinogens) in the previous 30 days. The perceived severity of their drug-using problem was also measured. Based on the combination of these responses, a drug composite score was constructed, with a higher score indicating more severe drug-using behavior (McGahan, Griffith, Parente, & McLellan, 1986). In addition, we also collected IDU and family member background information, including gender, age, education, marital status, and employment status. Duration of drug use and HIV status of IDUs were also self-reported.
Data Analysis
Background characteristics of IDUs and family members were reported for the intervention and standard care groups. The data for IDUs and family members were analyzed separately. Baseline differences between the intervention and standard care groups were analyzed using t tests, and an intent-to-treat approach was used to analyze intervention effects. Plots of means over time for the outcome measures were generated to graphically examine the outcome at different assessment points. We estimated mixed-effect models to fit each participant’s outcome measures with the intervention effect, and covariates included IDU and family member background characteristics, group (standard care vs. intervention), visit (baseline, 3-, or 6-month follow-up), and Group × Visit interaction. The models also included commune-level random effects to account for dependence within communes and a first-order autoregressive covariance structure to account for repeated observations within each participant. To examine the changes (improvement or reduction) in outcome measure between the intervention and standard care groups at the follow-up assessments, we presented the comparison of interest through model contrasts (i.e., the estimated baseline differences and intervention effects at each follow-up after adjusting for IDU and family member characteristics). The results from F tests for the main effects (group and visit effects) and the interaction term were reported. Statistical analyses were conducted using SAS for Windows (Version 9.2).
Results
Participant Characteristics
In total, 83 pairs of IDUs and their family members were included in our study; 43 pairs were in the intervention condition and 40 pairs in the standard care condition. No baseline differences were observed for gender, age, marital status, or employment status of IDUs. Fewer IDUs (15.0%) in the standard care group had 9 years or less education than IDUs in the intervention group (46.5%, p = .0020). One fourth (n = 23, 27.7%) of IDUs reported excessive alcohol drinking during their lifetime. Heroin was the primary substance abused by all participants; two participants reported cocaine use, one reported amphetamine use, and two reported cannabis use in their lifetime. Two (2.4%) participants reported using more than one substance per day during their lifetime. Half (n = 20, 50.0%) of the IDUs in the standard care and 26 (60.5%) in the intervention group reported 10 years or longer history of drug use. Seven IDU participants in the intervention group (16.3%) and another seven in the standard care group (17.5%) were HIV positive at baseline. All of the family members in the standard care group and 81.4% in the intervention were women (p = .0037). About 40% of the family members were spouses, 33.7% were parents, and 12.0% were siblings. Family members in the intervention group were younger (p = .0375) and less likely to be unemployed (p = .0031) than those in the standard care condition. Family members’ marital status and education level were comparable across the two intervention groups (see Table 1).
Table 1.
Numbers (Percentages) of Baseline Demographic and Background Characteristics
| IDU |
Family member |
|||||
|---|---|---|---|---|---|---|
| Characteristic | Standard care |
Intervention | p | Standard care |
Intervention | p |
| Number of participants | 40 | 43 | 40 | 43 | ||
| Gender | 1.0000 | .0037b | ||||
| Male | 40 (100) | 43 (100) | 0 | 8 (18.6) | ||
| Age (years) | .5026 | .0375b | ||||
| ≤30 | 15 (37.5) | 11 (25.6) | 16 (40.0) | 10 (23.8) | ||
| 31–40 | 19 (47.5) | 24 (55.8) | 3 (7.5) | 12 (28.6) | ||
| ≥41 | 6 (15.0) | 8 (18.6) | 21 (52.5) | 20 (47.6) | ||
| Marital status | .8540 | .1309 | ||||
| Single | 16 (40.0) | 15 (34.9) | 2 (5.0) | 3 (7.0) | ||
| Married/living as married | 22 (55.0) | 25 (58.1) | 29 (72.5) | 37 (86.1) | ||
| Divorced/separated or widowed | 2 (5.0) | 3 (7.0) | 9 (22.5) | 3 (7.0) | ||
| Education (years) | .0020a | .2313 | ||||
| ≤9 | 6 (15.0) | 20 (46.5) | 18 (45.0) | 19 (47.5) | ||
| 10–12 | 27 (67.5) | 22 (51.2) | 10 (25.0) | 15 (37.5) | ||
| ≥13 | 7 (17.5) | 1 (2.3) | 12 (30.0) | 6 (15.0) | ||
| Currently unemployed | 9 (22.5) | 14 (32.6) | .3063 | 23 (57.5) | 11 (25.6) | .0031b |
| Duration of drug use (years) | ||||||
| ≥10 | 20 (50.0) | 26 (60.5) | .3378 | |||
| HIV status | ||||||
| Positive | 7 (17.5) | 7 (16.3) | .8820 | |||
Note. IDU = injecting drug user.
A significant group difference was found for IDUs.
A significant group difference was found for family members.
Outcome Measures at Baseline and Follow-Up Assessments
Figure 2 presents the means (±2 SD) of outcome measures among IDUs and family members at baseline and 3- and 6-month assessments. For IDUs, levels of drug composite score, depressive symptoms, and family functioning were comparable between the standard care and intervention groups at baseline. The drug scores of the two intervention conditions remained stable at baseline and follow-up assessments. However, the level of depressive symptoms among IDUs in the intervention group reduced from 17.98 at baseline to 14.81 at 3 months and 15.45 at 6 months. The levels of family functioning increased from 44.53 at baseline to 48.51 at 3 months and 47.19 at 6 months. Such desirable changes were not observed among IDUs in the standard care condition. The outcome measures for family members were comparable at baseline. Family members in the intervention group demonstrated increased levels of coping at 3 and 6 months (28.88 at baseline; 30.98 at 3 months; 30.86 at 6 months), reduced depressive symptoms (17.95 at baseline; 14.81 at 3 months; 13.26 at 6 months), and improved family functioning (47.70 at baseline; 51.93 at 3 months; 51.44 at 6 months). The positive trends in the outcome measures were not evident for family members in the standard care group (see Figure 2).
Figure 2.
Plots of means (±2 SD) at baseline and follow-up points for IDUs and family members. FM = family member; IDU = injecting drug user.
Mixed-Effect Models of Outcome Measures
Tables 2 and 3 present the estimated intervention effects (differences in improvement or reduction in outcome measures between the intervention and standard care groups) from the mixed-effect regression models, controlling for participants’ background characteristics. For IDUs, no significant intervention effect was observed on the drug composite score. Compared with the standard care group, a significant reduction in depressive symptoms was seen at 3 months in the intervention group (estimated difference in reduction from baseline between intervention and standard care = 5.118, SE = 1.007, p < .0001); the estimated difference in reduction became smaller at 6 months (estimated difference in reduction = 3.674, SE = 1.019, p = .0004) after controlling for age, marital status, education, employment, years of drug use, and HIV status. The level of depressive symptoms in IDUs was negatively associated with being married or living as married (p = .0422) and more education (p = .0232). A significantly higher improvement in family functioning was shown at 3 months (estimated difference in improvement = 4.923, SE = 1.042, p < .0001) and 6 months (estimated difference in improvement = 3.075, SE = 1.202, p = .0115) for the intervention group after controlling for the same set of selected covariates.
Table 2.
Results From Mixed-Effects Regression Models-Injecting Drug Users (IDUs)
| Drug composite score |
Depressive symptoms |
Family functioning |
|||||||
|---|---|---|---|---|---|---|---|---|---|
| Parameter | Est. | SE | p | Est. | SE | p | Est. | SE | p |
| IDU characteristics | |||||||||
| Age | −0.0006 | 0.0015 | .6632 | 0.0191 | 0.0779 | .8070 | 0.0157 | 0.0679 | .8179 |
| Married | −0.0228 | 0.0170 | .1820 | − 1.8452 | 0.9006 | .0422 | −0.8605 | 0.7808 | .2722 |
| Education | −0.0097 | 0.0035 | .0069 | −0.4437 | 0.1933 | .0232 | 0.0584 | 0.1736 | .7370 |
| Unemployed | 0.0125 | 0.0144 | .3842 | 1.5433 | 0.8338 | .0662 | −0.1910 | 0.8249 | .8172 |
| Years of use | −0.0018 | 0.0019 | .3405 | −0.1222 | 0.1006 | .2266 | 0.0170 | 0.0886 | .8482 |
| HIV positive | −0.0216 | 0.0187 | .2506 | −0.3648 | 1.0178 | .7205 | 0.9022 | 0.9163 | .3264 |
| Main effecta | |||||||||
| Intervention | .0368 | .0077 | <.0001 | ||||||
| Visit | .5817 | .1963 | .0024 | ||||||
| Visit × Interventiona | .6788 | <.0001 | <.0001 | ||||||
| Baseline comparisonb | −0.0294 | 0.0198 | .1400 | 0.3794 | 1.0806 | .7260 | 1.5948 | 1.0151 | .1183 |
| Intervention effectc | |||||||||
| 3 months | −0.0150 | 0.0174 | .3896 | −5.1179 | 1.0070 | <.0001 | 4.9230 | 1.0424 | <.0001 |
| 6 months | −0.0090 | 0.0161 | .5810 | −3.6738 | 1.0191 | .0004 | 3.0753 | 1.2021 | .0115 |
p value from F test. The significances of the main effects were not of interest.
Estimated difference in IDU outcome measure at baseline between intervention and standard care through model contrasts.
Intervention effect = estimated difference in changes from baseline between intervention and standard care through model contrasts.
Table 3.
Results From Mixed-Effects Regression Models-Family Members
| Coping |
Depressive symptoms |
Family functioning |
|||||||
|---|---|---|---|---|---|---|---|---|---|
| Parameter | Est. | SE | p | Est. | SE | p | Est. | SE | p |
| Family member characteristics | |||||||||
| Male | −0.9560 | 0.9337 | .3075 | −1.2722 | 1.0886 | .2444 | −0.8775 | 1.3552 | .5183 |
| Age | 0.0540 | 0.0231 | .0205 | 0.1095 | 0.0268 | <.0001 | −0.0315 | 0.0334 | .3463 |
| Married | 0.7817 | 0.6353 | .2204 | 0.1589 | 0.7297 | .2879 | −1.4733 | 0.9139 | .1090 |
| Education | 0.1015 | 0.0786 | .1995 | −0.0854 | 0.0916 | .3524 | 0.1555 | 0.1141 | .1751 |
| Unemployed | −0.4156 | 0.5984 | .4884 | −0.2971 | 0.6775 | .6616 | 1.2591 | 0.8533 | .1421 |
| Main effecta | |||||||||
| Intervention | .0146 | <.0001 | <.0001 | ||||||
| Visit | <.0001 | <.0001 | .0002 | ||||||
| Visit × Interventiona | .0789 | .0002 | .0005 | ||||||
| Baseline comparisonb | 0.6613 | 0.7436 | .3752 | −1.0840 | 0.8506 | .2045 | 2.0689 | 1.0665 | .0542 |
| Intervention effectc | |||||||||
| 3 months | 1.7347 | 0.7942 | .0305 | −1.5364 | 0.8720 | .0801 | 3.9450 | 1.1113 | .0005 |
| 6 months | 0.4936 | 0.8026 | .5395 | −3.6815 | 0.8825 | <.0001 | 3.8496 | 1.1242 | .0008 |
p value from F test. The significances of the main effects were not of interest.
Estimated difference in family member’s outcome measure at baseline between intervention and standard care through model contrasts.
Intervention effect = estimated difference in changes from baseline between intervention and standard care through model contrast.
For family members, after controlling for gender, age, education, marital status, and employment status, we found a significantly improved level of coping at 3 months for the intervention group (estimated difference in improvement = 1.735, SE = 0.794, p = .0305). However, the estimated difference in reduction became insignificant at 6 months. The intervention effect of depressive symptoms was insignificant at 3 months, and was strengthened to a significant level at 6 months (estimated difference in reduction = 3.682, SE = 0.8826, p < .0001). The intervention effect in family functioning was significant at both 3 months (estimated difference in improvement = 3.945, SE = 1.111, p = .0005) and 6 months (estimated difference in improvement = 3.850, SE = 1.124, p = .0008). Older family members were associated with better coping (p = .0205) and a higher level of depressive symptom (p < .0001).
Discussion
The intervention piloted in this study is the first in Vietnam to focus on mental health and family relations for both IDUs and their family members. The intervention was well received by the participating IDUs and their family members, as reflected by the near 100% participation in the multiple sessions and the high follow-up rate. Local service providers and intervention facilitators also spoke highly about the strategies and approaches used in the intervention. The providers affirmed that they had learned new perspectives and techniques to interact with IDUs and their family members, and asserted the need to more effectively involve family members in future drug use control and treatment strategies. Our intervention pilot could potentially serve as a model to provide a continuum of services beyond drug rehabilitation centers in Vietnam.
Of the various challenges associated with drug use behaviors, mental health is one of the most critical to acknowledge. Hence, it is very encouraging to see promising outcomes in both depressive symptoms and family functioning for the IDU participants in this study. On the other hand, our intervention pilot failed to show intervention outcomes for IDU drug-using behavior, which reflects the difficulties in changing addictive behavior with a short, four-session intervention. This finding reinforces the need for combination prevention strategies to promote positive behavioral change among IDUs. Continued attention is also needed to develop harm-reduction strategies, including availability of clean syringes and opioid substitution therapy.
In a family-oriented culture such as Vietnam, it is useful to consider the impact of drug use on the collective (family) rather than its traditional framing as the challenge of a single individual. Results from this study reinforce the link between family experience and individual drug use. Participation in this intervention pilot provided family members of IDUs with improved skills to cope with an adverse situation, reduced depressive symptoms, and enhanced family functioning. Future intervention programs should explore additional avenues for exploiting the power of family to address the challenges associated with drug use.
There are some limitations to be noted. First, given the pilot nature of this study, the sample size was small and the follow-up period was short. Therefore, the study results did not provide conclusive evidence of the intervention’s efficacy, especially for drug-using behavior. Also, because of the limited sample size, some imbalances in background characteristics were found between intervention conditions. Second, the outcome measures relied on self-reported data, so issues related to social-desirability bias and recall bias could be raised. Also, some differences in outcome measures between groups, although showing an encouraging trend, may not be clinically significant in nature. Third, caution must be used in generalizing the findings to IDUs in other geographic areas, IDUs who refused to participate or who did not receive routine health care, or IDUs whose drug-using status is not known to commune service providers. Finally, there was a lack of control activity provided to the standard care group, so it is difficult to differentiate the intervention effect from the change due to attention received by the intervention group. Despite these limitations, we believe that the findings presented here indicate the positive effects of Intervention V for IDUs and their family members. It is necessary for future program developers to recognize the importance of family members in the well-being of IDUs and broaden their role in harm reduction and HIV-prevention programs to achieve a sustainable intervention impact in drug use control and prevention.
Acknowledgments
This study was funded by National Institute on Drug Abuse Grant R34DA029493. We thank the project team members in Hanoi and Phú Tho, Vietnam, for their contributions to this study.
Contributor Information
Li Li, Semel Institute for Neuroscience and Human Behavior, Center for Community Health, University of California, Los Angeles.
Nguyen Tran Hien, National Institute of Hygiene and Epidemiology, Hanoi, Vietnam.
Chunqing Lin, Semel Institute for Neuroscience and Human Behavior, Center for Community Health, University of California, Los Angeles.
Nguyen Anh Tuan, National Institute of Hygiene and Epidemiology.
Le Anh Tuan, National Institute of Hygiene and Epidemiology.
Shu C. Farmer, Semel Institute for Neuroscience and Human Behavior, Center for Community Health, University of California, Los Angeles
Roger Detels, School of Public Health, University of California, Los Angeles.
References
- Bloom BL. A factor analysis of self-report measures of family functioning. Family Process. 1985;24:225–239. doi: 10.1111/j.1545-5300.1985.00225.x. [DOI] [PubMed] [Google Scholar]
- Bloom BL, Naar S. Self-report measures of family functioning: Extensions of a factorial analysis. Family Process. 1994;33:203–216. doi: 10.1111/j.1545-5300.1994.00203.x. [DOI] [PubMed] [Google Scholar]
- Carver CS. You want to measure coping but your protocol’s too long: Consider the Brief COPE. International Journal of Behavioral Medicine. 1997;4:92–100. doi: 10.1207/s15327558ijbm0401_6. [DOI] [PubMed] [Google Scholar]
- Go VF, Frangakis C, Van Nam L, Sripaipan T, Bergenstrom A, Li F, Quan VM. Characteristics of high-risk HIV-positive IDUs in Vietnam: Implications for future interventions. Substance Use & Misuse. 2011;46:381–389. doi: 10.3109/10826084.2010.505147. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hammett TM, Kling R, Johnston P, Liu W, Ngu D, Friedmann P, Jarlais DC. Patterns of HIV prevalence and HIV risk behaviors among injection drug users prior to and 24 months following implementation of cross-border HIV prevention interventions in northern Vietnam and southern China. AIDS Education and Prevention. 2006;18:97–115. doi: 10.1521/aeap.2006.18.2.97. [DOI] [PubMed] [Google Scholar]
- Hammett TM, Kling R, Van NT, Son DH, Binh KT, Oanh KT. HIV prevention interventions for female sexual partners for injection drug users in Hanoi, Vietnam: 24-month evaluation results. AIDS and Behavior. 2012;16:1164–1172. doi: 10.1007/s10461-011-0062-4. [DOI] [PubMed] [Google Scholar]
- Hoa NT, Doussantousse S. The life and times of the Hanoi drug user: Some recent insight from field research. Hanoi, Vietnam: UNAIDS Vietnam Country Office; 2001. [Google Scholar]
- Hoffman L, Nguyen HTT, Kershaw TS, Niccolai LM. Dangerous subtlety: Relationship-related determinants of consistency of condom use among female sex workers and their regular, noncommercial partners in Hai Phong, Viet Nam. AIDS and Behavior. 2011;15:1372–1380. doi: 10.1007/s10461-010-9819-4. [DOI] [PubMed] [Google Scholar]
- Khoat DV, West GR, Valdiserri RO, Phan NT. Peer education for HIV prevention in the Socialist Republic of Vietnam: A national assessment. Journal of Community Health. 2003;28:1–17. doi: 10.1023/a:1021321704417. [DOI] [PubMed] [Google Scholar]
- Li L, Liang LJ, Ding YY, Ji GP. Facing HIV as a family: Predicting depressive symptoms with correlated responses. Journal of Family Psychology. 2011;25:202–209. doi: 10.1037/a0022755. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McGahan PL, Griffith JA, Parente R, McLellan AT. Addiction Severity Index Composite Scores manual. Philadelphia, PA: Department of Veterans Affairs Medical Center; 1986. [Google Scholar]
- McLellan AT, Kushner H, Metzger D, Peters R, Smith I, Grissom G, Argeriou M. The fifth edition of the Addiction Severity Index. Journal of Substance Abuse Treatment. 1992;9:199–213. doi: 10.1016/0740-5472(92)90062-s. [DOI] [PubMed] [Google Scholar]
- Ministry of Labor Invalid and Social Affairs of Vietnam. Overview of the impact of policies on drug rehabilitation treatment on its implementation in Vietnam. Hanoi, Vietnam: Author; 2010. [Google Scholar]
- Ngo AD, Schmich L, Higgs P, Fischer A. Qualitative evaluation of peer-based needle syringe programme in Vietnam. International Journal of Drug Policy. 2009;20:179–182. doi: 10.1016/j.drugpo.2007.12.009. [DOI] [PubMed] [Google Scholar]
- Nguyen VT, Scannapieco M. Drug abuse in Vietnam: A critical review of the literature and implications for future research. Addiction. 2008;103:535–543. doi: 10.1111/j.1360-0443.2007.02122.x. [DOI] [PubMed] [Google Scholar]
- Ogden J, Nyblade L. Common at its core: HIV-related stigma across contexts. Washington, DC: International Center on Research for Women; 2005. [Google Scholar]
- Rudolph AE, Davis WW, Quan VM, Ha TV, Minh NL, Gregowski A, Go V. Perceptions of community- and family-level injection drug user (IDU)- and HIV-related stigma, disclosure decisions and experiences with layered stigma among HIV-positive IDUs in Vietnam. AIDS Care. 2012;24:239–244. doi: 10.1080/09540121.2011.596517. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Salter ML, Go VF, Minh NL, Gregowski A, Ha TV, Rudolph A, Quan VM. Influence of perceived secondary stigma and family on the response to HIV infection among injection drug users in Vietnam. AIDS Education and Prevention. 2010;22:558–570. doi: 10.1521/aeap.2010.22.6.558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tuan NA, Fylkesnes K, Thang BD, Hien NT, Long NT, Kinh NV, O’Farrell N. Human immunodeficiency virus (HIV) infection patterns and risk behaviours in different population groups and provinces in Viet Nam. Bulletin of the World Health Organization. 2007;85:35–41. doi: 10.2471/BLT.05.026153. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tuan NA, Long TH, Vinh QP, Detels R. Risk factors for HIV-1 seropositivity in drug users under 30 years old in Haiphong, Vietnam. Addiction. 2001;96:405–413. doi: 10.1046/j.1360-0443.2001.9634055.x. [DOI] [PubMed] [Google Scholar]
- World Health Organization. Good practice in Asia: Targeted HIV prevention for injecting drug users and sex workers. 2010 Retrieved from http://www.who.int/hiv/pub/idu/good_practice_aisa_idu.pdf.
- Zung WW. A self-rating depression scale. Archives of General Psychiatry. 1965;12:63–70. doi: 10.1001/archpsyc.1965.01720310065008. [DOI] [PubMed] [Google Scholar]