Description
Eighty per cent of primary hyperparathyroidism cases are caused by parathyroid adenoma while nearly 16% of ectopic parathyroid adenomas have been found to be the aetiology.1 A 50-year-old man presented with pain in the back and knees for 4 years. He was initially evaluated elsewhere and was detected to have hypercalcaemia. No other investigations were done at the other facility. He was then evaluated in our institution for the persistence of hypercalcaemia and recently deranged renal function. His blood investigations revealed: serum calcium 12 mg% (normal (N) 8.3–10.4), phosphorus 1.8 mg% (N 2.5–4.6), creatinine 2 mg% (N 0.7–1.4), estimated glomerular filtration rate (eGFR) 56 mL/min/body surface area (BSA), 25(OH)-vitamin-D 20.03 ng/mL (N 20–32) and intact parathyroid hormone (iPTH) 644 pg/mL (N 8–74). An ultrasonography of his abdomen revealed mild nephrocalcinosis bilaterally. His bone mineral density showed a t score of −3 in forearm as compared with spine (−1.2) and neck of femur (−1.6). The ultrasonography of the neck did not show any parathyroid adenoma. He underwent a technetium-99m (99mTc) sestamibi scan as well as a single photon emission CT (SPECT), which revealed an ectopic parathyroid adenoma below the lower pole of the right lobe of thyroid (figures 1 and 2). He underwent a focal parathyroid surgery via the cervical approach and the adenoma was located in the thymus; it was resected and removed. His intact parathyroid hormone (iPTH) and serum calcium levels measured 24 h after surgery, within normal limits. On the day of discharge, his corrected serum calcium level was 8.83 mg%. At present, he is asymptomatic, on regular follow-up and has normal serum calcium levels.
Figure 1.
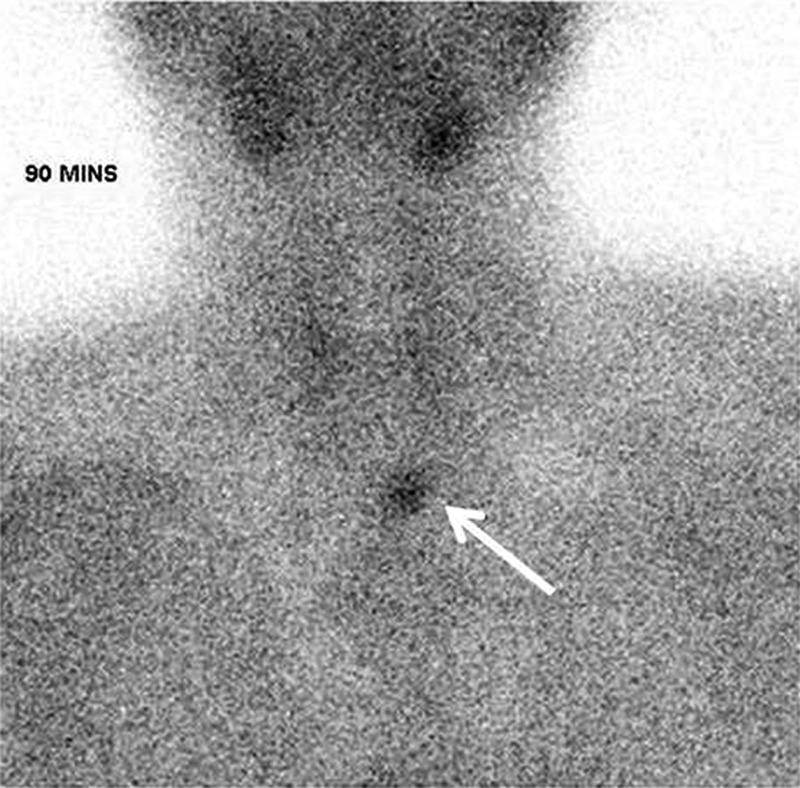
Technetium-99m (99mTc) sestamibi scan showing ectopic parathyroid uptake at 90 min.
Figure 2.
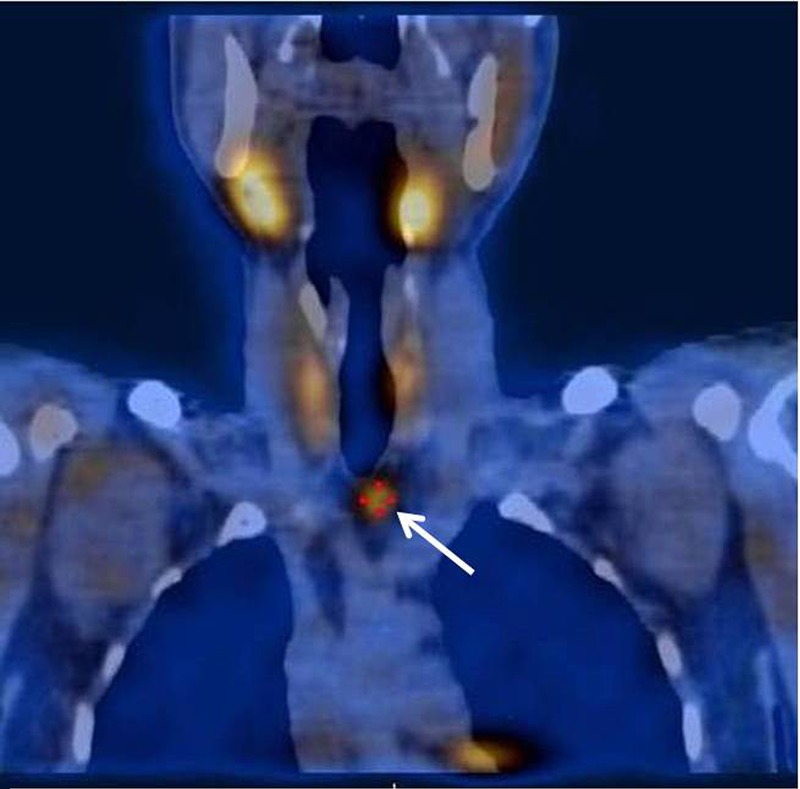
Single photon emission CT showing ectopic parathyroid adenoma below the right lobe of thyroid.
Learning points.
Although 99mTc sestamibi with single photon emission CT scanning has a high accuracy in localising parathyroid adenomas, including those that are ectopic, it may not always be positive in all cases, with a reported sensitivity varying between 70% and 100%.2 3
Accurate preoperative localisation of parathyroid adenomas is essential for the success of the parathyroid surgery.
Focus parathyroid surgery is adequate for cures other than bilateral neck exploration if the parathyroid adenoma is accurately localised. Thereby, it reduces the surgical morbidity and complications.
Footnotes
Contributors: DN and KFJ collected the case details and prepared the manuscript. AJC and RD participated in the treatment of the patient.
Competing interests: None.
Patient consent: Obtained.
Provenance and peer review: Not commissioned; externally peer reviewed.
References
- 1.Noussios G, Anagnostis P, Natsis K. Ectopic parathyroid glands and their anatomical, clinical and surgical implications. Exp Clin Endocrinol Diabetes 2012;120:604–10 [DOI] [PubMed] [Google Scholar]
- 2.Bernà L, Caixàs A, Piera J, et al. Technetium-99m-methoxyisobutylisonitrile in localization of ectopic parathyroid adenoma. J Nucl Med 1996;37:631–3 [PubMed] [Google Scholar]
- 3.Patel CN, Salahudeen HM, Lansdown M, et al. Clinical utility of ultrasound and 99mTc sestamibi SPECT/CT for preoperative localization of parathyroid adenoma in patients with primary hyperparathyroidism. Clin Radiol 2010;65:278–87 [DOI] [PubMed] [Google Scholar]


