Abstract
Background
Reperfusion in ischemia is believed to generate cytotoxic oxidative stress, which mediates reperfusion injury. These stress conditions can initiate lipid peroxidation and damage to proteins, as well as promote DNA strand breaks. As biliverdin and bilirubin produced by heme oxygenase isoform 1 (HO-1) have antioxidant properties, the production of both antioxidants by HO-1 may help increase the resistance of the ischemic brain to oxidative stress. In the present study, the survival effect of HO-1 was confirmed using hemin.
Methods
To confirm the roles of HO-1, carbon monoxide, and cyclic guanosine monophosphate further in the antioxidant effect of HO-1 and bilirubin, cells were treated with cycloheximide, desferoxamine, and zinc deuteroporphyrin IX 2,4 bis glycol, respectively.
Results
HO-1 itself acted as an antioxidant. Furthermore, iron, rather than carbon monoxide, was involved in the HO-1-mediated survival effect. HO-1 activity was also important in providing bilirubin as an antioxidant.
Conclusion
Our results suggested that HO-1 helped to increase the resistance of the ischemic brain to oxidative stress.
Keywords: Heme, Oxygenases, Bilirubin, Iron, Carbon monoxide
INTRODUCTION
Heme oxygenase (HO) catalyzes the initial reaction, and subsequent rate limiting step, in heme catabolism. There are three different types of HO isoforms, HO-1, HO-2, and HO-3, although HO-3 is not catalytically active and is thought to be a pseudogene derived from HO-2 transcripts [1]. Initially, HO was thought to be only an enzyme that catalyzed the initial step in the destruction of senescent erythrocytes seen in all systemic organs. In subsequent studies, HO was also shown to undergo adaptive regulation in response to stress. Following the discovery of this stress-related upregulation, two different isoforms of the HO enzyme, HO-1 and HO-2, were identified in 1968. Once the two different isoforms were identified, it was determined that the observed stress-related upregulation was due to a 32-kDa protein, HO-1, and that the 36-kDa isoform, HO-2, was not upregulated during times of stress.
While HO-2 is constitutively expressed, HO-1 is normally expressed at low levels in most tissues; however, it is highly inducible by a variety of stimuli including growth factors, oxidative stress, dietary antioxidants, or disease states [2]. HO-1 is mainly expressed in the liver and spleen, and is not expressed in the brain under normoxic conditions [3]. Indeed, HO-1 may be among the most critical cytoprotective mechanisms activated during times of cellular stress such as inflammation, ischemia, hypoxia, hyperoxia, hyperthermia, or radiation [4], and is thought to play a key role in maintaining antioxidant/oxidant homeostasis. In particular, HO-1 is induced by hypoxia via a mechanism independent of hypoxia-inducible factors [5]. Moreover, the induction of HO-1 during conditions of cerebral oxidative stress is critical in neuroprotection [6]. Although HO-1 is an HO enzyme, it is also known as HSP32, a member of a family of proteins referred to as heat shock proteins [7,8].
The upregulation of HO-1 during times of oxidative and heat stress implied an antioxidant role. However, it was unclear whether HO-1 had inherent antioxidant properties, or whether its protective effect was a result of its catalytic products. HO uses molecular oxygen, nicotinamide adenine dinucleotide phosphate, and cytochrome P-450 reductase to catalyze the oxidative cleavage of the heme molecule, producing carbon monoxide (CO), biliverdin (subsequently converted to bilirubin by biliverdin reductase), and iron.
The ferric ion (Fe3+) is one of the products of the heme degradation reaction. Therefore, the production of free iron from the catabolism of heme could give rise to toxic hydroxyl radicals through a reaction known as the Fenton reaction, which involves hydrogen peroxide and superoxide. However, ferritin is thought to be induced to bind and sequester free iron, thus functioning as an antioxidant by preventing the production of toxic hydroxyl radicals [9].
There has also been evidence to suggest that bilirubin, another product of the heme oxygenase catalyzed reaction, can function as an antioxidant. It has been shown in vitro that bilirubin scavenges peroxyl radicals as efficiently as α-tocopherol, which is regarded as the most potent antioxidant of lipid peroxidation. Therefore, the redox cycling of bilirubin may scavenge reactive oxygen species, protecting cells from oxidative stress. Furthermore, bilirubin reacts with peroxyl radicals to form biliverdin [10].
CO is another product of heme catabolism, and has been implicated as a diffusible second messenger to activate soluble guanylyl cyclase. Since the discovery of the role of nitric oxide (NO) in the central nervous system as a second messenger, research has been conducted in an attempt to elucidate a similar role for CO. Like NO, CO can bind to the iron in the heme present in guanylyl cyclase and activate the enzyme. As was the case with NO, exogenous CO has also been shown to inhibit platelet aggregation due to the activation of soluble guanylyl cyclase [11]. The colocalization of 5-aminolevulinic acid synthase with HO-2 in the brain also indicates that the machinery for porphyrin synthesis and CO production occur together, as would be required for an endogenous second messenger [12].
The present study examined the function of HO-1 in rat brain endothelial microvessel cells (RBE4). This cell line was selected for this study because it provides an excellent model to study brain endothelial cells, which constitute the blood-brain barrier. Molecular biology methodologies were used to evaluate the functional roles of HO-1, bilirubin, and ferritin induction in cytoprotection.
METHODS
Cells
RBE4 cells were immortalized using the adenovirus E1A gene without oncogenic transformation. Transfection was carried out using a calcium phosphate precipitation procedure on endothelial microvessel cells. Each line was packaged with trypsin-ethylenediaminetetraacetic acid and RBE4 medium, which was composed of 500 mL of Dulbecco's Modified Eagle's Medium (DMEM; obtained from Gibco, Grand Island, NY), 55 mL of fetal bovine serum (Gibco), 11 mL of HEPES (Sigma, St. Louis, MO, USA), 146 g of L-glutamine, 167 g of geneticin (Sigma) and 55 µL of basic fibroblast growth factor (Biomedical Technologies, Stoughton, MA, USA). Trypsin (4 mL) was added to each 10-cm2 dish and the dishes were incubated for 5 minutes. Cells were washed into a 50-mL conical tube and then the dish was washed again with 4 mL of DMEM. The conical tube was then centrifuged at 1,500 rpm for 5 minutes. The supernatant was aspirated and the pellet was resuspended in RBE4 medium based on the desired dilution factor. Cell lines were diluted at concentrations of 1:3 to 1:6 with RBE4 medium.
Viability assays
Certain cell lines were frozen in liquid nitrogen to allow for their use at a later time. Two 10-cm2 dishes at 100% confluence were frozen per vial diluted with freeze medium. The freeze medium consisted of 10% dimethyl sulfoxide and 90% DMEM. Cells were trypsinized and centrifuged. Each pellet was resuspended in 500 µL of DMEM and transferred to a vial. Each vial was chilled on ice for 5 minutes, and then another 500 µL of ice-cold freeze media was added to each vial. The vials were then stored at -20℃ for 1 hour prior to storage at -70℃ for 4 to 15 hours, after which vials were put into liquid nitrogen.
Cell lines were passaged on 10-cm2 dishes and 3-(4,5-dim-ethylthiazolyl-2)-2,5-diphenyltetrazoliµM bromide (MTT) experiments were conducted on 24-well plates. The plates were coated with fibronectin to allow for the growth of cells. The experiments were comprised of three stages: induction, sensitization, and hydrogen peroxide. The induction phase was initiated at time 0 and continued for 1 hour. The sensitization phase occurred at 16 hours and was followed by the hydrogen peroxide phase, where the cell monolayers received 500 µM of H2O2 at 17 hours. Hydrogen peroxide was applied for 1.5 hours before the 10% MTT solution (diluted with DMEM) was placed on the cells for 3 hours. A solubilization buffer was then applied to the cells overnight. The next day, wells were measured in a spectrophotometer at 575 and 675 nm. The average of the differences between the 575 and 675 nm readings from triplicate sets was divided by the control reading. This quotient represented the percentage of cells that survived.
Chemicals
Cells underwent oxidative stress in the peroxide phase due to the addition of 0.5 mL of 500 µM hydrogen peroxide to each well. The induction and sensitization phases represented times during which various known compounds were introduced into the medium to test several hypotheses regarding the antioxidant role of heme oxygenase. The experiments were conducted using different concentrations of zinc deuteroporphyrin IX 2,4 bis glycol (ZnBG, Porphyrin Products Inc., Logan, UT, USA), bilirubin (Porphyrin Products Inc.), cycloheximide (Sigma), desferoxamine (Sigma), and hemin (Sigma).
The MTT cell proliferation kit I (Boehringer Mannheim, Mannheim, Germany) was used to evaluate the viability of the RBE4 cells. The MTT kit was selected to quantify cell viability because it provides a colorimetric assay that can be run expediently on a large nµMber of cell monolayers and does not rely on cell counting. This colorimetric assay is based upon the cleavage of the tetrazoliµM salt, MTT, to purple formazin crystals by dehydrogenase activity in active mitochondria.
Tests were run to determine whether the variables used in the MTT assay experiments affected the cleavage of the tetrazoliµM salt, which could skew the data. Specific concentrations of bilirubin, hemin, ZnBG, cycloheximide, and desferoxamine were placed on cells during the last 10 minutes of the sensitization phase. Nothing was placed on the cells during the induction phase. Subsequently, cells underwent the aforementioned procedure, and it was determined that none of the variables of the experiments affected the cleavage of the salt.
Statistical analysis
All data are presented as the means±standard errors of the means. One-way analysis of variance was conducted and followed by Dunnett's post hoc test.
RESULTS
Heme oxygenase-1 promoted rat brain microvessel endothelial cell survival under oxidative stress mainly through bilirubin
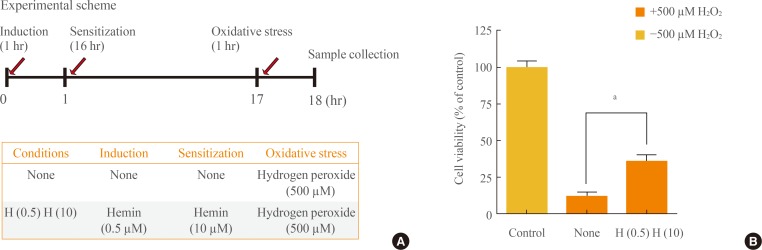
To study the role of HO activity in the protective effects observed under conditions of oxidative stress, we employed in vitro models with hemin, which is the HO-1 substrate for induction and sensitization under oxidative stress attributable to hydrogen peroxide (500 µM H2O2) (Fig. 1A). Cell death was prevented by treatment with hemin (none vs. hemin [10 µM]; 11.58 vs. 36.32) (Fig. 1B). The results of the cell viability assay suggested that inducible HO-1 played an important role in the survival of RBE4 cells under oxidative stress.
Fig. 1.
Protective effects of heme under conditions of oxidative stress. (A) Experimental scheme for induction, sensitization, and oxidative stress. The "H (0.5) H (10)" condition was induction by hemin (0.5 µM) and sensitization by hemin (10 µM), while the "none" condition was no induction and no sensitization. (B) Cells untreated by H2O2 were used as a positive control. Before oxidative stress was applied (500 µM H2O2), cells were inducted and sensitized according to the experimental scheme. Data are mean±SEM of three separate experiments. Analyses performed were one-way analysis of variance followed by Dunnett's post hoc test. aP<0.01 denote statistical significance.
Iron was necessary for the antioxidant effects of HO-1 activity
HO appears to exert most of its actions via enzymatic activity and the generation of various enzymatic byproducts that act on multiple pathways. For example, HO can promote: 1) the generation of biliverdin and its subsequent reduction to bilirubin, 2) the release of CO, and 3) the release and safe disposal of iron. These actions modulate various pathways with a high degree of overlap and/or crossover, which may help to ensure the induction of the desired biological effects [13].
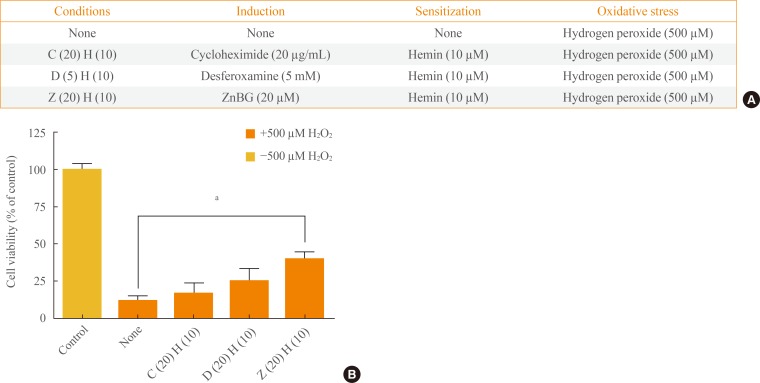
To confirm the roles of HO-1, CO, and cyclic guanosine monophosphate (cGMP) in the antioxidant effects of HO-1 induced by hemin, we treated cells with cycloheximide, desferoxamine, and ZnBG, respectively, in the induction phase of experiments for 1 hour (Fig. 2A). After the induction phase, hemin was used in the sensitization phase for 16 hours. Study results revealed that the HO-1 activity induced by hemin was blocked by cycloheximide, an inhibitor of protein biosynthesis. Furthermore, cycloheximide induction completely blocked the survival effect of HO-1. Conversely, ZnBG, which is an inhibitor of heme oxygenase induction, did not block the survival effect of HO-1 following hemin induction (cycloheximide induction vs. ZnBG induction; 16.5 vs. 39.6) (Fig. 2B). Desferoxamine, which binds specifically to iron and removes the relevant effect of iron induction, only partially blocked the survival effect of HO-1. Study results indicated that iron, not CO, was involved in the survival effects attributable to HO-1.
Fig. 2.
The antioxidant effects of heme oxygenase isoform 1 activity require iron. (A) Experimental scheme for induction, sensitization, and oxidative stress. The "C (20) H (10)," "D (5) H (10)," and "Z (20) H (10)" conditions were induction by cycloheximide (20 ng/mL), desferoxamine (5 nM), and ZnBG (20 µM), respectively, with sensitization by hemin (10 µM) in each case, while the "none" condition was no induction and no sensitization. (B) Cells untreated by H2O2 were used as a positive control. Before oxidative stress was applied (500 µM H2O2), cells were inducted and sensitized according to the experimental scheme. Data are mean±SEM of three separate experiments. Analyses performed were one-way analysis of variance followed by Dunnett's post hoc test. aP<0.01 denote statistical significance.
HO-1 was necessary for the antioxidant effects of bilirubin
Bilirubin acts as a scavenger against reactive oxygen species via its own oxidation [14,15,16]. Indeed, bilirubin is a powerful antioxidant that can inhibit the oxidation of low-density lipoprotein and other lipids [17], scavenge oxygen radicals [18], and counteract oxidative stress in general [19]. The production of bilirubin could participate in an amplification cycle via its oxidization into biliverdin and then reduction back into bilirubin by biliverdin reductase [20].
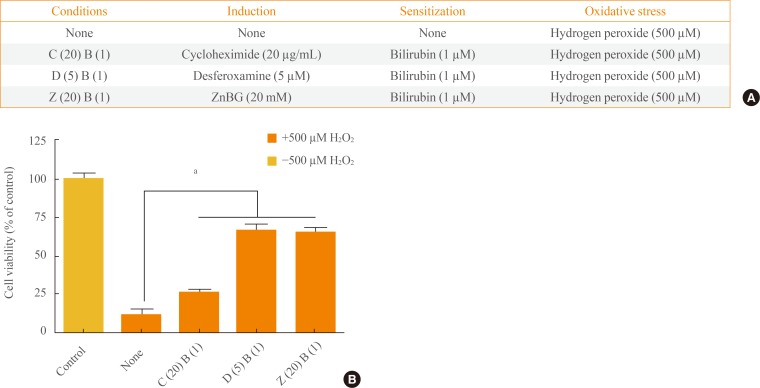
To confirm the roles of HO-1, CO, and cGMP in the antioxidant effect of bilirubin, we used cycloheximide, desferoxamine, and ZnBG, respectively, during the induction phase of the experiments for 1 hour. After the induction phase, bilirubin was used in the sensitization phase for 16 hours (Fig. 3A). Cycloheximide induction partially blocked the survival effect of bilirubin, suggesting that HO-1 played an important role in the antioxidant effect of bilirubin. Furthermore, bilirubin did not require CO or cGMP to increase cell viability (Fig. 3B). Study results indicated that HO-1 required heme and iron to produce the observed survival effect. However, bilirubin, as an HO-1 effector for oxidative stress, did not require CO or cGMP.
Fig. 3.
The antioxidant effects of bilirubin require heme oxygenase isoform 1 activity. (A) Experimental scheme for induction, sensitization, and oxidative stress. The "C (20) B (10)," "D (5) B (10)," and "Z (20) B (10)" conditions were induction by cycloheximide (20 ng/mL), desferoxamine (5 nM), and ZnBG (20 µM), respectively, with sensitization by bilirubin (1 µM) in each case, while the "none" condition was no induction and no sensitization. (B) Cells untreated by H2O2 were used as a positive control. Before oxidative stress was applied (500 µM H2O2), cells were inducted and sensitized according to the experimental scheme. Data are mean±SEM of three separate experiments. Analyses performed were one-way analysis of variance followed by Dunnett's post hoc test. aP<0.001 denote statistical significance.
DISCUSSION
The present study examined the anti-oxidative effects of HO-1 using rat brain endothelial cells. Study results showed that the HO-1 itself acted as an antioxidant. Additionally, iron, but not CO, was demonstrated to be involved in the survival effect mediated by HO-1. The HO-1 activity was also shown to be important in providing bilirubin as an antioxidant.
Ferric ions participated in the Fenton reaction to protect cells and allowed for a comparison of the protection afforded by hemin induction. The importance of iron in inducing ferritin for cytoprotection was also demonstrated when desferoxaminexamine was added during the induction phase.
HO-1 has been shown to be a critical gene in the cellular response against pro-oxidative stimuli. When considering the cellular response as a whole, HO-1 seems to act as a hub of gene-gene interactions that modulate the triggering and activation of several protective molecular pathways.
Basal HO-1 mRNA expression levels in response to injurious stimuli appear to be more important than the degree of upregulation or fold induction for protection against those stimuli in the vasculature. In some circumstances, the levels of HO-1 protein and HO functional activity may not be concordant, which could be due to post-translational modifications.
HO-1 has been shown to be induced inside as well as outside of areas of cerebral infarction. In particular, HO-1 has been shown to be induced in the endothelial cells within areas of infarction and in glia. More specifically, HO-1 was induced primarily in glial cells in noninfarcted areas of the cortex inside as well as outside the middle cerebral artery distribution. The cells most resistant to cerebral infarction, the endothelial cells, expressed HO-1-inducible stress genes in areas of infarction 24 hours after ischemic injuries. Because HO-1-inducible genes have heat shock elements within their promoters, it is possible that the presence of oxidative stimulus for stress related protein induction within the injured endothelial cells [21]. It is not known whether the endothelial cells within the infarction survive, but they may do so due to the synthesis of HO-1, which could serve to protect them from further injury and therefore enable them to survive the ischemic insult [22].
HO-1 is influenced by oxidative stress in cells, as the depletion of glutathione (GSH) and ascorbic acid induce HO-1 [23]. Reperfusion in focal ischemia is believed to generate cytotoxic free radicals that mediate reperfusion injury [24]. Reactive oxygen species can initiate lipid peroxidation and damage to proteins, as well as promote DNA strand breaks. Although there are a number of pathways and enzymes in the brain that detoxify and inactivate free radicals, these antioxidants, including GSH and ascorbic acid, can be quickly overwhelmed following reperfusion injury. Because the biliverdin and bilirubin produced by HO-1 and HO-2 have antioxidant properties [4,24], the production of both antioxidants by HO-1 may help increase the resistance of the ischemic brain to oxidative stress.
ACKNOWLEDGMENTS
This work was supported by the DGIST R&D Program of the ministry of science, ICT & Future Planning, Science and Technology of Korea (14-BD-0402).
Footnotes
No potential conflict of interest relevant to this article was reported.
References
- 1.Hayashi S, Omata Y, Sakamoto H, Higashimoto Y, Hara T, Sagara Y, Noguchi M. Characterization of rat heme oxygenase-3 gene. Implication of processed pseudogenes derived from heme oxygenase-2 gene. Gene. 2004;336:241–250. doi: 10.1016/j.gene.2004.04.002. [DOI] [PubMed] [Google Scholar]
- 2.Calabrese V, Butterfield DA, Scapagnini G, Stella AM, Maines MD. Redox regulation of heat shock protein expression by signaling involving nitric oxide and carbon monoxide: relevance to brain aging, neurodegenerative disorders, and longevity. Antioxid Redox Signal. 2006;8:444–477. doi: 10.1089/ars.2006.8.444. [DOI] [PubMed] [Google Scholar]
- 3.Sun Y, Rotenberg MO, Maines MD. Developmental expression of heme oxygenase isozymes in rat brain. Two HO-2 mRNAs are detected. J Biol Chem. 1990;265:8212–8217. [PubMed] [Google Scholar]
- 4.Choi AM, Alam J. Heme oxygenase-1: function, regulation, and implication of a novel stress-inducible protein in oxidant-induced lung injury. Am J Respir Cell Mol Biol. 1996;15:9–19. doi: 10.1165/ajrcmb.15.1.8679227. [DOI] [PubMed] [Google Scholar]
- 5.Wood SM, Wiesener MS, Yeates KM, Okada N, Pugh CW, Maxwell PH, Ratcliffe PJ. Selection and analysis of a mutant cell line defective in the hypoxia-inducible factor-1 alpha-subunit (HIF-1alpha). Characterization of hif-1alpha-dependent and -independent hypoxia-inducible gene expression. J Biol Chem. 1998;273:8360–8368. doi: 10.1074/jbc.273.14.8360. [DOI] [PubMed] [Google Scholar]
- 6.Parfenova H, Carratu P, Tcheranova D, Fedinec A, Pourcyrous M, Leffler CW. Epileptic seizures cause extended postictal cerebral vascular dysfunction that is prevented by HO-1 overexpression. Am J Physiol Heart Circ Physiol. 2005;288:H2843–H2850. doi: 10.1152/ajpheart.01274.2004. [DOI] [PubMed] [Google Scholar]
- 7.Ewing JF, Maines MD. Rapid induction of heme oxygenase 1 mRNA and protein by hyperthermia in rat brain: heme oxygenase 2 is not a heat shock protein. Proc Natl Acad Sci U S A. 1991;88:5364–5368. doi: 10.1073/pnas.88.12.5364. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Dwyer BE, Nishimura RN, De Vellis J, Yoshida T. Heme oxygenase is a heat shock protein and PEST protein in rat astroglial cells. Glia. 1992;5:300–305. doi: 10.1002/glia.440050407. [DOI] [PubMed] [Google Scholar]
- 9.Eisenstein RS, Garcia-Mayol D, Pettingell W, Munro HN. Regulation of ferritin and heme oxygenase synthesis in rat fibroblasts by different forms of iron. Proc Natl Acad Sci U S A. 1991;88:688–692. doi: 10.1073/pnas.88.3.688. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Baranano DE, Snyder SH. Neural roles for heme oxygenase: contrasts to nitric oxide synthase. Proc Natl Acad Sci U S A. 2001;98:10996–11002. doi: 10.1073/pnas.191351298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Zakhary R, Gaine SP, Dinerman JL, Ruat M, Flavahan NA, Snyder SH. Heme oxygenase 2: endothelial and neuronal localization and role in endotheliuM-dependent relaxation. Proc Natl Acad Sci U S A. 1996;93:795–798. doi: 10.1073/pnas.93.2.795. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Verma A, Hirsch DJ, Glatt CE, Ronnett GV, Snyder SH. Carbon monoxide: a putative neural messenger. Science. 1993;259:381–384. doi: 10.1126/science.7678352. [DOI] [PubMed] [Google Scholar]
- 13.Maines MD. Heme oxygenase: function, multiplicity, regulatory mechanisms, and clinical applications. FASEB J. 1988;2:2557–2568. [PubMed] [Google Scholar]
- 14.Dore S, Snyder SH. Neuroprotective action of bilirubin against oxidative stress in primary hippocampal cultures. Ann N Y Acad Sci. 1999;890:167–172. doi: 10.1111/j.1749-6632.1999.tb07991.x. [DOI] [PubMed] [Google Scholar]
- 15.Dore S, Takahashi M, Ferris CD, Zakhary R, Hester LD, Guastella D, Snyder SH. Bilirubin, formed by activation of heme oxygenase-2, protects neurons against oxidative stress injury. Proc Natl Acad Sci U S A. 1999;96:2445–2450. doi: 10.1073/pnas.96.5.2445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Stocker R, Keaney JF., Jr Role of oxidative modifications in atherosclerosis. Physiol Rev. 2004;84:1381–1478. doi: 10.1152/physrev.00047.2003. [DOI] [PubMed] [Google Scholar]
- 17.Stocker R. Lipoprotein oxidation: mechanistic aspects, methodological approaches and clinical relevance. Curr Opin Lipidol. 1994;5:422–433. [PubMed] [Google Scholar]
- 18.Stocker R, Yamamoto Y, McDonagh AF, Glazer AN, Ames BN. Bilirubin is an antioxidant of possible physiological importance. Science. 1987;235:1043–1046. doi: 10.1126/science.3029864. [DOI] [PubMed] [Google Scholar]
- 19.Schwertner HA. Association of smoking and low serμM bilirubin antioxidant concentrations. Atherosclerosis. 1998;136:383–387. doi: 10.1016/s0021-9150(97)00232-3. [DOI] [PubMed] [Google Scholar]
- 20.Baranano DE, Rao M, Ferris CD, Snyder SH. Biliverdin reductase: a major physiologic cytoprotectant. Proc Natl Acad Sci U S A. 2002;99:16093–16098. doi: 10.1073/pnas.252626999. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Kinouchi H, Sharp FR, Hill MP, Koistinaho J, Sagar SM, Chan PH. Induction of 70-kDa heat shock protein and hsp70 mRNA following transient focal cerebral ischemia in the rat. J Cereb Blood Flow Metab. 1993;13:105–115. doi: 10.1038/jcbfm.1993.13. [DOI] [PubMed] [Google Scholar]
- 22.Welch WJ, Suhan JP. Cellular and biochemical events in mammalian cells during and after recovery from physiological stress. J Cell Biol. 1986;103:2035–2052. doi: 10.1083/jcb.103.5.2035. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Srisook K, Cha YN. Super-induction of HO-1 in macrophages stimulated with lipopolysaccharide by prior depletion of glutathione decreases iNOS expression and NO production. Nitric Oxide. 2005;12:70–79. doi: 10.1016/j.niox.2004.12.002. [DOI] [PubMed] [Google Scholar]
- 24.Nimura T, Weinstein PR, Massa SM, Panter S, Sharp FR. Heme oxygenase-1 (HO-1) protein induction in rat brain following focal ischemia. Brain Res Mol Brain Res. 1996;37:201–208. doi: 10.1016/0169-328x(95)00315-j. [DOI] [PubMed] [Google Scholar]