Abstract
Background
Compliance with methadone maintenance treatment (MMT) in China is poor.
Objective
To evaluate the effects of adjunctive contingency management (CM) on the efficacy of methadone maintenance treatment (MMT) in patients with opioid dependence.
Hypothesis
A 12-week prize-based contingency management (CM) intervention can increase the retention and compliance of heroin abusers to standardized MMT programs in Shanghai.
Methods
160 heroin-dependent patients from three voluntary MMT clinics in Shanghai were randomly assigned to a treatment as usual group (MMT, n=80) and an intervention group (MMT+CM, n=80). Daily use of methadone was recorded and urine drug tests were conducted weekly during the first 12 weeks and then at week 16, week 20 and week 24.
Results
The 12-week retention rates for the intervention (MMT+CM) and treatment-as-usual (MMT) groups were both quite high: 87.5% and 86.2%, respectively. The average durations of using methadone in the two groups were equal (70 days versus 71 days, respectively). There was a non-significant increase in the mean longest drug-free period (7.4 weeks versus 6.5 weeks) and in the mean number of negative urine tests (7.9 versus 7.6). Secondary analysis of the 24-week outcomes (12 weeks after termination of the adjunctive CM treatment) also found no significant differences between the groups. Among those who remained in the program the severity of addiction as assessed by the Addiction Severity Index decreased dramatically over the 24 weeks but, again, there were no significant differences in the addiction measures between those in the intervention group and those in the treatment-as-usual group.
Conclusion
Prize-based CM is not effective in improving the retention and compliance of heroin abusers to MMT in Shanghai. The main reasons for failure to replicate western studies were the unexpectedly high baseline rates of compliance in this sample (86%) and the relatively weak financial incentives provided by the CM program. CM programs are context dependent so a careful preliminary situational analysis is needed to determine their potential effectiveness at a particular site and to identify the types of incentives (prizes) that will effectively encourage behavioral change in the target participants.
Keywords: Heroin dependence, Methadone maintenance treatment, Behavior contingency management, Survival analysis
Abstract
背景
为了应对海洛因依赖的严重后果,我国开展了美沙酮维持治疗(methadone maintenance treatment,MMT)项目,但是MMT依从性差。
目的
评估在美沙酮维持治疗中行为列联管理(contingency management,CM)对阿片类药物依赖者的作用。
假设
在上海市常规MMT项目基础上结合以奖励机制为基础的CM干预共12周,可提高MMT治疗依从性和增加操守程度。
方法
来自于3个自愿戒毒MMT门诊的160名海洛因依赖者被随机分入常规治疗组(MMT,n=80)和干预组(MMT+CM,n=80),在前12周每周评估患者的服药行为并进行尿液的毒品检测,随后在第16、20和24周分别进行上述评估检测。
结果
干预组和常规治疗组完成12周治疗的比例都很高,分别为87.5%和86.2%。12周中,两组服用美沙酮的平均天数差异无统计学意义[70(2.9)d与71(2.7)d],两组未吸海洛因的最长时间(分别为7.4周与6.5周)以及尿检阴性的次数(分别为7.9次与7.6次)也没有明显差异。同样,根据24周的分析提示两组间差异也无统计学意义。用成瘾严重程度指数评估成瘾程度,24周内两组完成随访者的成瘾严重程度都显著下降,但是两组间比较同样无明显差异。
结论
在我国上海的MMT门诊,以奖励机制为基础的行为列联管理干预并未起到提高治疗依从性和促进保持操守的作用。这与西方研究结果不同。究其原因,一是基线依从性高(86%),二是CM项目提供的奖励相对少。在CM项目中奖励与场景是相关的,因而需要对场景进行仔细的分析,了解在特定场景采用什么特定的奖励措施,以便鼓励目标人群改变行为。
1. Introduction
Heroin is the main drug of abuse in China: 0.978 million of the 1.335 million drug addicts registered by the national public security system in China (73.2%) are addicted to heroin[1]. To address this problem the Ministry of Health, the Ministry of Public Security and the State Food and Drug Administration jointly run a Methadone Maintenance Treatment (MMT) program that included 668 clinics in 27 provinces by the end of 2010. Since the program started in March 2004, 236 000 individuals have received treatment and 110 000 have been stabilized[2]. In Shanghai there were over 40 000 registered drug addicts by the end of 2010 but the MMT program (which started in September 2006) only has 14 clinics that have treated a total of 5 000 patients among whom only 2 000 had been stabilized on daily methadone maintenance. Thus, despite government efforts in this area, the coverage of the MMT programs is quite limited and the retention of individuals who get into the programs is poor[2].
Previous studies identified potential reasons for the poor results of MMT in China: the relatively low dosages of methadone employed, the inconvenience for patients, concerns of patients about being supervised by public security personnel, and so forth[3], [4]. Another possible reason for the poor retention and compliance in MMT programs in China is the lack of systematic social and psychological interventions as adjunctive treatments for MMT. Studies in other countries report that contingency management (CM), one of the most frequently used psychosocial intervention methods for patients with schizophrenia[5], is helpful for increasing retention and compliance to MMT programs. This technique uses behavioral reinforcement techniques based on Skinner's Operational Conditioned Reflex theory and “reinforced contingency” principle. Several studies in other countries involving the “goldfish bowl” ballot method of CM find that this version of CM is relatively easy and economical to implement and has good results[6]. The present study is a randomized controlled trail that assesses the benefit of adjunctive CM using the goldfish bowl ballot method in improving the retention and efficacy of MMT in Shanghai. We hypothesize that a 12-week CM intervention will significantly increase the retention and compliance of patients enrolled in a standardized MMT program.
2. Subjects and methods
The results presented are part of the China-United States cooperation project entitled “Research about improving the compliance and efficacy of methadone maintenance treatment in China” that was approved by the ethics committee of the University of California at Los Angeles (UCLA IRB #: G08-03-087-01).
2.1. Subjects
Based on outpatient records of the MMT programs in Shanghai we estimated that the retention rate in these programs is about 40%. Other reports suggest that CM can result in a 30% improvement in retention[7]–[9]. Assuming α=0.05 and β=0.10, the sample size required for comparing rates of retention in two groups (treatment as usual group vs. intervention group) is 80 subjects per group[10].
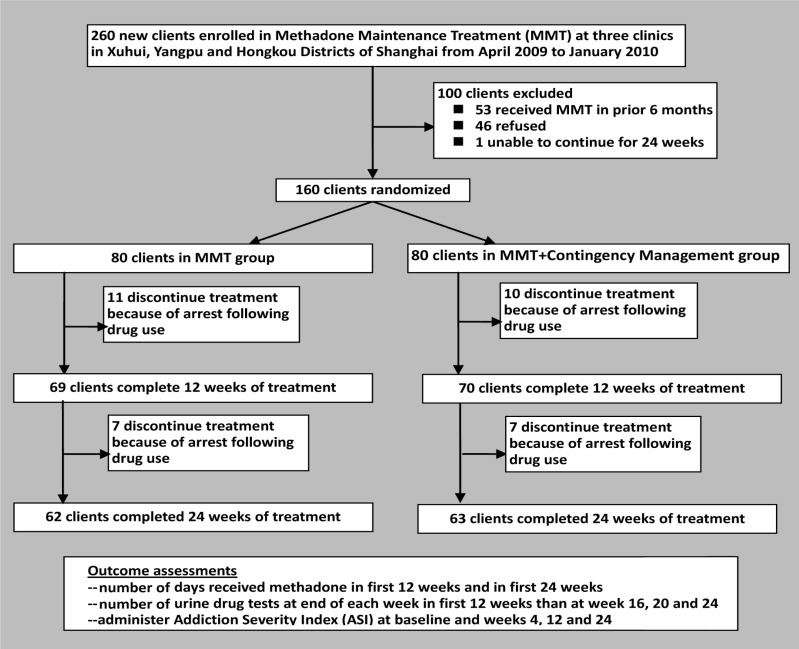
The enrollment and follow-up of patients is shown in Figure 1. Newly enrolled clients at three MMT clinics in the Xuhui, Yangpu and Hongkou Districts of Shanghai from April 2009 to January 2010 who provided written informed consent, met DSM-IV criteria for heroin dependence, had no other serious mental disorders and had not received MMT treatment in the last six months were enrolled in the study.
Figure 1. Flowchart of enrollment and follow-up of subjects in the study.
The diagnosis of heroin dependence was determined by a psychiatrist who administered the Mini International Neuropsychiatric Interview[11],[12]. After fully explaining the project, eligible subjects were asked to provide written content. Those that consented were randomized using simple randomization tables for each of the three sites generated by the SPSS software package (SEED: 210002); 80 subjects were assigned to the treatment as usual group (MMT) and 80 to the intervention group (MMT+CM). Prior to assignment the evaluating clinicians were blind to the potential assignment of each patient.
2.2. Intervention methods and procedures
The standardized MMT involved daily visits to the clinic, administration of methadone in the clinic at the dosage determined by the treating physician (based on the client's condition), regular urine and blood testing, and monitoring in the community by specialized drug-monitoring social workers. The cost of this treatment was 10 Chinese Yuan ($1.60 US) per visit, for a maximum of 300 Chinese Yuan ($48 US) per month. None of the health insurance packages available in Shanghai cover this cost so the clients had to pay this fee themselves. (The mean per capita income in Shanghai at the time was 3 898 Chinese Yuan per month.) All clinic visits were recorded and urines were tested for opiates weekly for the first 12 weeks and then at week 16, 20 and 24 after initiation of treatment. The results of the drug tests were discussed with the clients who were encouraged to utilize the MMT treatments regularly and to keep their urine results negative.
The intervention group received the standardized MMT described above and simultaneously received a 12-week behavior contingency management intervention. Small financial rewards (that could be used to pay the daily MMT cost or, less commonly, were converted into daily necessities like shampoo, towels, etc.) were provided based on an algorithm developed by the Yunan Province Drug Abuse Institute and computerized by the current research team. Patients participated in raffles, with the winner of the raffle receiving a reward. The size of the reward and/or the number of drawings an individuals could make increased based on the number of times the client continuously received MMT or had sequential negative urine drug tests. After each urine test the results were discussed with the subject and motivational interviewing methods were used to encourage continued participation and compliance with the MMT program. The average value of the total awards provided to intervention group clients over the 12 weeks was 527 Chinese Yuan ($83.60 US) and the range in value was from 342 to 2 745 Chinese Yuan ($54.30 US∼$435.80 US).
2.3. Evaluation of the severity of addiction
A Chinese translation of the Addiction Severity Index (ASI) that has good reliability and validity in China[13],[14] was used to assess the severity of addiction at enrollment and at weeks 4, 12 and 24 after enrollment. This is an 55-item scale that assesses seven dimensions of addiction: physical condition, employment status, drug usage, alcohol abuse, criminal activities, family relationships, and mental status. The scale, which takes about 30 minutes to complete, was administered by interviewers who were trained in the administration of the scale prior to the start of the study. A complex algorithm is applied to the scores of the 55 items in the scale to compute composite scores (between 0 and 1, with higher scores representing more severe addiction) for each of the seven dimensions[15]. Studies in other countries find that the ASI has good reliability and validity[16]. The reliability and validity of the Chinese version of the instrument has also been assessed[14]. The internal consistency of the seven dimensions was judged to be acceptable (alpha=0.44∼0.79), the test-retest reliability was good (ICC=0.68∼0.84), and the inter-rater reliability was good (ICC=0.87∼0.98).
To minimize the risk of biased results, as much as possible the persons who conducted the urine tests and completed the evaluation of the ASI were different from those who provided the CM intervention. But subjects may talk about the CM intervention during the assessment so it was not possible to completely ‘blind’ the evaluators to the treatment group of the subjects.
2.4. Statistical methods
‘Retention’ was defined as the number of days over the first 12 weeks of treatment that the subject attended the clinic and received methadone. Compliance (i.e., remaining drug-free) was defined in two ways: the longest continuous period (in weeks) of negative urine tests in the first 12-weeks of treatment and the total number of negative urine tests over the first 12 weeks of treatment. An intention to treat (ITT) analysis was employed so subjects who dropped out of the MMT or did not appear for the urine tests were assumed to have positive urine tests. The seven dimension scores of the ASI were used as secondary measures of efficacy. An ITT analysis was NOT used for the analysis of ASI results because most persons who dropped out of the program did so because they had started taking drugs again and were remanded to a compulsory treatment facility; it was not, therefore, considered appropriate to use their last ASI result (when they were drug free) to impute subsequent results.
Statistical analyses were conducted using version 15.0 of the SPSS software package. Chi-square tests and t-tests were used to compare characteristics of the members of the two groups. Survival analyses with ‘dropout’ as the outcome measure (defined as seven consecutive days without methadone) were used to compare the compliance with MMT between the two groups at both 12 weeks and 24 weeks. Backwards stepwise logistic regression was used to identify those factors associated with dropping out from MMT. Analysis of covariance was used to compare the longest retention of drug-free status between the groups. Generalized Estimating Equations (GEE) were used to compare changes in the seven ASI dimension scores over the four time periods (baseline and at weeks 4, 12 and 24).
3. Results
3.1. Characteristics of the subjects
The basic characteristics of the 160 enrolled subjects are shown in Table 1. Almost 80% were male. They had started abusing drugs in their late twenties and had, on average, a nine-year history of abuse. Most of them had had prior mandatory treatments for abuse and 41 (25.6%) had spent time in prison for criminal offenses. Despite the random assignment to groups, subjects in the intervention group were more likely to be divorced or separated, to have a later age of onset of drug abuse and to have a shorter duration of drug abuse than subjects in the treatment as usual group; these three variables were adjusted for in the subsequent analyses.
Table 1. Characteristics of the subjects.
| Characteristic | Total (n=160) | MMT+CM group (n=80) | MMT group (n=80) | p-values | |
| Age | M (SD), years | 38.9 (8.9) | 37.7 (7.8) | 38.0 (10.0) | 0.234 |
| Gender, | Male, n,% | 125 (78.1%) | 65 (81.3%) | 60 (75.0%) | 0.339 |
| Nationality | Han, n,% | 157 (98.1%) | 78 (97.5%) | 79 (98.8%) | 0.553 |
| Marital status | Married, n,% | 58 (36.3%) | 25 (31.3%) | 33 (41.3%) | 0.048 |
| Unmarried, n,% | 77 (48.1%) | 37 (46.3%) | 40 (50.0%) | ||
| Other, n,% | 25 (15.6%) | 18 (22.5%) | 7 (8.8%) | ||
| Education | Years formal schooling, M (SD) | 10.1 (1.8) | 10.3 (1.6) | 9.9 (1.9) | 0.178 |
| Level of education | 0.398 | ||||
| Below junior high school, n,% | 91 (56.9%) | 42 (52.5%) | 49 (61.3%) | ||
| Senior high school and above, n,% | 69 (43.1%) | 38 (47.6%) | 31 (38.8%) | ||
| Employment | Full-time or part-time, n,% | 53 (33.8%) | 31 (39.3%) | 22 (28.2%) | 0.107 |
| Unemployed, n,% | 100 (63.7%) | 48 (60.8%) | 52 (66.7%) | ||
| Incarcerated, n,% | 4 (2.5%) | 0 (0%) | 4 (5.1%) | ||
| Legal status | Number of compulsory treatments, M (SD) | 2.3 (1.8) | 2.1 (1.9) | 2.5 (1.9) | 0.180 |
| Prison time*, M (SD), months | 11.2 (29.4) | 11.9 (34.2) | 10.5 (23.8) | 0.758 | |
| Number of criminal offense, M (SD) | 0.5 (1.1) | 0.5 (1.0) | 0.5 (1.2) | 0.887 | |
| Physical conditions | Chronic physical diseases, n,% | 30 (18.7%) | 13 (16.3%) | 17 (21.2%) | 0.418 |
| HCV positive, n,% | 103 (65.6%) | 50 (64.1%) | 53 (67.1%) | 0.694 | |
| Drug use | Age of initial drug abuse, M (SD), years | 28.2 (7.8) | 29.5 (7.6) | 26.8 (7.8) | 0.027 |
| Duration for drug abuse, M (SD), years | 8.9 (6.3) | 7.7 (4.2) | 10.1 (7.7) | 0.017 | |
| Average dose, M (SD), g | 0.8 (0.5) | 0.8 (0.4) | 0.9 (0.6) | 0.425 | |
| Main method of drug use: | 0.454 | ||||
| Sniffing, n,% | 26 (18.4%) | 11 (15.9%) | 15 (20.8%) | ||
| Injection, n,% | 115 (81.6%) | 58 (84.1%) | 57 (79.2%) | ||
| Used ATS in last 30 days, n,% | 6 (3.8%) | 3 (3.8%) | 3 (3.8%) | 1.000 | |
MMT= Methadone Maintenance Treatment; CM=Contingency Management; HCV=Hepatitis C; ATS=Amphetamine-type stimulants
*not including incarceration for compulsory drug rehabilitation
3.2. Retention in MMT treatment
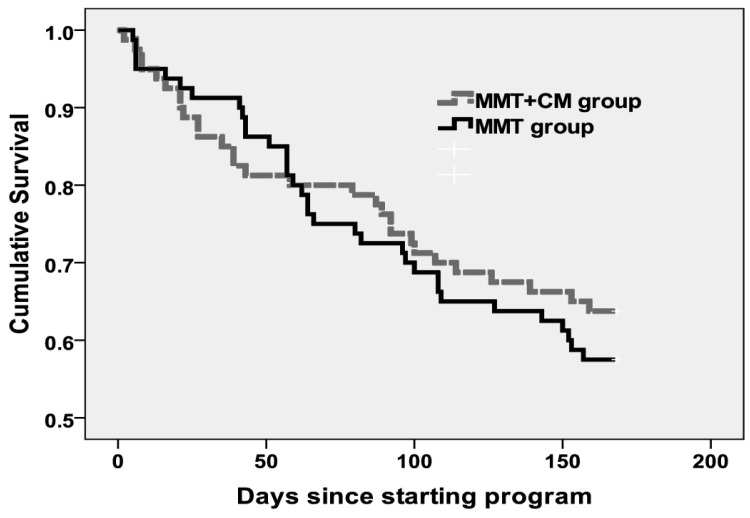
At the end of 12 weeks 69 subjects (86.2%) in the MMT group remained in treatment and 70 subjects (87.5%) in the MMT+CM group remained in treatment (X2=0.05, df=1, p=0.819; power=59%). The survival plot for compliance with MMT treatment of the two groups is shown in Figure 2. Over the first 12 weeks the mean (SD) days of remaining in the program in the MMT and MMT+CM groups were 71.0 (2.7) days and 70.0 (2.9) days, respectively (survival analysis: log-rank X2=0.29, p=0.590, power=54%).
Figure 2. 24-week survival curve of retention in the MMT (Methadone Maintenance Treatment) and MMT+CM (Contingency Management) groups.
By the end of 24 weeks of treatment 62 subjects (77.5%) in the MMT group and 63 subjects (78.8%) in the MMT+CM group remained in treatment (X2=0.04, df=1, p=0.848, power=54%). Over the entire 24-week period the mean days of remaining in the program in the MMT and MMT+CM groups were 129 (6.5) days and 127.3 (6.3) days, respectively (survival analysis: log-rank X2=0.45, p=0.500, power=50%).
The 18 subjects who dropped out of the MMT group over the 24 weeks included 13 (72.2%) males and had a mean age of 41.4 (7.1) years. The 17 subjects who dropped out of the MMT+CM group included 13 (76.5%) males who had a mean age of 37.5 (9.0) years. Backward stepwise logistic regression analysis including all of the demographic and clinical variables listed in Table 1 found no statistical differences in any of these variables between the drop-out subjects in the two groups.
3.3. Compliance as assessed by urine-test results
During the first 12 weeks the mean longest drug-free interval in the MMT and MMT+CM groups were 6.5 (3.9) weeks versus 7.4 (4.4) weeks, respectively (t=1.51, p=0.148, power=68%). Assuming that the urine tests at week 16, week 20 and week 24 represent the drug-use status of the individual in the prior four weeks, the mean longest drug-free interval in the MMT and MMT+CM groups after 24 weeks of treatment were 13.0 (8.1) weeks versus 15.4 (8.1) weeks, respectively (t=1.86, p=0.064; power=79%)
Based on the intention-to-treat analysis which considers missing urine tests positive, the mean number of negative urine samples during the first 12 weeks of treatment (conducted at the end of each of the 12 weeks) was 7.6 (3.6) in the MMT group and 7.9 (4.2) in the MMT+CM group (t=0.44, p=0.658, power=93%). After 24 weeks of treatment the mean number of negative urine tests (out of a total of 15 urine tests) was 9.6 (4.5) in the MMT group and 9.2 (5.5) in the MMT+CM group (t=0.55, p=0.585, power=57%).
3.4. Severity of addiction
Table 2 shows the results for the four administrations of the ASI. The ASI was not assessed in individuals who dropped out of the program so the analysis is based on the results of subjects who remained in the program at each time period. The number of days using heroin in the last month, as reported by the subjects themselves, decreased dramatically over the 24 weeks of treatment. Six of the seven composite dimension score (excluding the alcohol use dimension score) also decreased significantly over the 24 weeks. However, none of these measures showed a main effect for the treatment group or an interaction effect between time and treatment group, so there is no evidence of any difference in these measures between the MMT group and MMT+CM group.
Table 2. Comparisons in addiction-related issues between the two groups.
| Dimension | Time period* | MMT+CM group | MMT group | All subjects | Statistical analysis GEE: F, P |
||
| Temporal main effects | Main effects of CM intervention | Interaction of time and CM intervention | |||||
| Self-report of heroin use in 30 days prior to interview** Mean (SD) days |
Baseline | 26.5(7.1) | 24.6(9.3) | 25.5(8.3) | 1144.51 | 0.79 | 0.57 |
| 4 weeks | 0.9(3.7) | 2.2(6.8) | 1.6(5.5) | <0.001 | 0.375 | 0.449 | |
| 12 weeks | 1.3(5.8) | 0.9(4.5) | 1.1(5.1) | ||||
| 24 weeks | 0.3(1.7) | 0.2(1.0) | 0.2(1.4) | ||||
| Physical condition dimension score Mean (SE of mean) |
Baseline | 0.14(0.02) | 0.15(0.02) | 0.15(0.02) | 7.15 | 0.01 | 0.00 |
| 4 weeks | 0.07(0.02) | 0.09(0.02) | 0.08(0.02) | 0.008 | 0.911 | 0.983 | |
| 12 weeks | 0.10(0.02) | 0.08(0.02) | 0.09(0.02) | ||||
| 24 weeks | 0.07(0.03) | 0.09(0.03) | 0.08(0.02) | ||||
| Employment dimension score Mean (SE of mean) |
Baseline | 0.57(0.02) | 0.56(0.03) | 0.57(0.02) | 12.32 | 0.88 | 0.32 |
| 4 weeks | 0.53(0.03) | 0.59(0.03) | 0.56(0.02) | <0.001 | 0.350 | 0.569 | |
| 12 weeks | 0.50(0.03) | 0.55(0.03) | 0.52(0.02) | ||||
| 24 weeks | 0.51(0.03) | 0.48(0.04) | 0.49(0.02) | ||||
| Alcohol problem dimension score Mean (SE of mean) |
Baseline | 0.03(0.01) | 0.03(0.01) | 0.03(0.01) | 2.00 | 1.77 | 1.57 |
| 4 weeks | 0.02(0.01) | 0.02(0.01) | 0.02(0.00) | 0.158 | 0.183 | 0.210 | |
| 12 weeks | 0.01(0.01) | 0.01(0.00) | 0.01(0.00) | ||||
| 24 weeks | 0.02(0.01) | 0.02(0.01) | 0.02(0.01) | ||||
| Drug problem dimension score Mean (SE of mean) |
Baseline | 0.16(0.01) | 0.15(0.01) | 0.15(0.01) | 243.27 | 0.56 | 1.16 |
| 4 weeks | 0.08(0.01) | 0.08(0.01) | 0.08(0.01) | <0.001 | 0.453 | 0.282 | |
| 12 weeks | 0.05(0.01) | 0.05(0.01) | 0.05(0.01) | ||||
| 24 weeks | 0.03(0.01) | 0.05(0.01) | 0.04(0.01) | ||||
| Legal problems dimension score Mean (SE of mean) |
Baseline | 0.15(0.01) | 0.16(0.01) | 0.16(0.01) | 21.01 | 0.00 | 0.01 |
| 4 weeks | 0.09(0.01) | 0.08(0.01) | 0.08(0.01) | <0.001 | 0.959 | 0.931 | |
| 12 weeks | 0.11(0.01) | 0.11(0.01) | 0.11(0.01) | ||||
| 24 weeks | 0.10(0.01) | 0.09(0.01) | 0.10(0.01) | ||||
| Family status dimension score Mean (SE of mean) |
Baseline | 0.14(0.02) | 0.15(0.02) | 0.14(0.01) | 33.49 | 0.68 | 0.00 |
| 4 weeks | 0.05(0.01) | 0.09(0.01) | 0.07(0.01) | <0.001 | 0.410 | 0.966 | |
| 12 weeks | 0.05(0.01) | 0.09(0.01) | 0.07(0.01) | ||||
| 24 weeks | 0.05(0.01) | 0.06(0.01) | 0.05(0.01) | ||||
| Mental health dimension score Mean (SE of mean) |
Baseline | 0.06(0.01) | 0.08(0.02) | 0.07(0.01) | 10.31 | 0.88 | 0.49 |
| 4 weeks | 0.02(0.01) | 0.02(0.01) | 0.02(0.00) | 0.001 | 0.349 | 0.484 | |
| 12 weeks | 0.02(0.01) | 0.04(0.01) | 0.03(0.01) | ||||
| 24 weeks | 0.03(0.02) | 0.02(0.01) | 0.02(0.01) | ||||
MMT=Methadone Maintenance Treatment; CM=Contingency Management; SD=Standard Deviation; SE=Standard Error
*160 subjects participated in the baseline evaluation (80 in each group); 151 subjects participated in the 4-week evaluation (75 in the MMT+CM group, 76 in the MMT group); 139 subjects participated in the 12-week evaluation (70 in the MMT+CM group and 69 in the MMT group); and 125 subjects participated in the 24-week evaluation (63 in the MMT+CM group and 62 in the MMT group).
** Self-report of heroin use in 30 days prior to interview is one item in the ‘Drug problem’ dimension
4. Discussion
4.1. Major findings
This is the first prospective randomized control trial in China to assess the effectiveness of Contingency Management as an adjunctive treatment for Methadone Maintenance Treatment in individuals addicted to heroin. The sample was relatively large, with 80 subjects in each group. Easily-assessed objective measures were employed as the target outcomes: retention in the MMT program and number of drug-negative weekly urine tests. Rigorous intention-to-treat analysis was employed to compare urine test results between the two groups, assuming all no-shows were positive tests.
The original hypothesis—that a 12-week program of adjunctive CM would improve retention and compliance to MMT—was not confirmed. The 12-week program retention for the intervention (MMT+CM) and treatment-as-usual (MMT) groups were both quite high: 87.5% and 86.2%, respectively. The average duration of methadone use in the two groups over the 12 weeks were equal (70 days versus 71 days, respectively). The mean longest drug-free period in the 12 weeks was slightly, but not significantly, longer in the intervention group (7.4 weeks versus 6.5 weeks). And the mean number of weekly negative urine tests was slightly, but not significantly, higher in the intervention group (7.9 versus 7.6). Secondary analysis of the 24-week outcomes (12 weeks after termination of the CM intervention) also found no significant differences between the groups. Among those who remained in the program the severity of addiction, as assessed by the Addiction Severity Index, decreased dramatically over the 24 weeks but, again, there were no significant differences in the addiction severity measures between those in the intervention group and those in the treatment-as-usual group.
In sum, this rigorous assessment did not find any benefit of the CM technique employed (the goldfish bowl ballot method) in this sample of heroin addicts treated at three MMT centers in Shanghai.
4.2. Limitations
The sample size for the study was predicated on an estimated 12-week retention rate in the MMT programs in Shanghai of 40% and an estimated 30% improvement in retention with adjunctive CM treatment. The actual 12-week retention rate in the treatment-as-usual MMT group was 86%, so the sample size, though relatively large for this type of study, was too small to demonstrate a differences between the groups. Moreover, given this level of retention in the treatment-as-usual group, a 30% improvement is theoretically impossible. Thus the power of some of the analyses was relatively weak and it is possible that the negative results were due to Type II errors. However, the power for the primary analyses were all above 50% (that for the number of negative urine tests was over 90%) and there was no strong trend in the results that suggested that a ‘real’ difference was been obscured by the small sample size. Thus, despite the technically insufficient sample size, the weight of the evidence suggests that given the underlying high rates of MMT program compliance in this setting the CM intervention is not intensive enough to significantly improve on this already quite good level of retention.
The unexpectedly high retention rates of the clients at these three MMT clinics in Shanghai suggests that clients at these clinics may not be representative of heroin users at clinics in other parts of the country. The results could be quite different in centers where there was a much lower underlying rate of retention.
Shanghai is the richest city in the country so the small financial incentives employed may have been insufficient to motivate behavioral change in these subjects. The average total award of 527 Chinese Yuan ($83.60) in the 12-week treatment period is only equal to 4.5% of the average per capita three-month income in Shanghai.
Many of the patients who relapsed were remanded to compulsory inpatient drug treatment programs so they dropped out of the voluntary outpatient MMT clinic program. After incarceration these patients were not longer available to complete the Abuse Severity Index so subsequent severity data points were missing. (Using the severity measures at the last assessment prior to the relapse to impute subsequent values—the ‘last observed value carried forward’ (LOCF) method--would not accurately reflect the condition of the subjects so it was not used.) Thus, the ASI severity measures do not include data on those who had severe relapses so it underestimates the true severity of the abuse in the subjects. Since the number of dropouts increased over the four assessment periods (baseline, four weeks, 12 weeks and 24 weeks) it is possible that some of the reported improvement in the severity measures of abuse over time are cause by the removal of the most severely affected individuals. However the overall proportion of relapses was relatively small (under 15%), the proportions of relapses in the two groups was similar, and there were no differences in the characteristics of individuals who relapsed in the two groups. It therefore seems unlikely that the dropouts lead to biased results.
4.3. Implications
We believe the main reasons our study failed to replicate western studies that have demonstrated the efficacy of CM as an adjunctive treatment for MMT[7]–[9] were the very high baseline retention rates at the three MMT clinics chosen (thus producing a ‘ceiling effect’) and the relatively weak incentives provided by the goldfish bowl ballot method employed. One external factor that may have temporarily increased MMT clinic retention rates in Shanghai was that the study was conducted during the 2010 Shanghai World Exposition. During the exposition the Shanghai public security department was much more diligent than usual in combating drug abuse and drug trafficking. Another factor that could have increased baseline compliance is that the effectiveness of anti-drug social workers in Shanghai has been gradually improving[17] and the community management of all the subjects in the study was being supervised by this cadre of experienced social workers.
Previous work has shown that the long-term effectiveness of CM programs is closely related to the degree of the incentive provided[18], and that well-designed programs can provide incentives that both encourage participants to stop the drug-taking behavior (to get the award) and simultaneously reinforce the alternative behaviors needed to resist drug abuse in the future[19]. In retrospect it is clear that the goldfish bowl ballot program used in our study achieved neither of these objectives. Almost all clients simply used the funds to pay for the MMT rather than trade the vouchers for daily necessities or other rewards, and staff members encouraged this use of the rewards because it was much easier to administer this way. The financial incentive was minimal and there was no real attempt to use this incentive to change the lifestyle problems that were sustaining the drug-taking behavior.
The most important take-home message from the study is that CM programs are context sensitive. They are unlikely to be effective in situations where compliance with MMT is already very high or when the incentive provided is of relatively little value to the participants. At each potential target site a careful preliminary situational analysis is needed to determine the potential effectiveness of an adjunctive CM program and to identify the types of incentives (prizes) that will effectively encourage behavioral change in the target participants.
Footnotes
Conflict of interest: The authors report no conflict of interest related to this paper.
Funding: This project was supported by grants from the National Institute of Health in the USA (R21DA025385) and from the Shanghai Science and Technology Commission (Grant number: 09410707000).
References
- 1.Chinese Ministry of Public Security . 2010 Annual report on drug control in China. Beijing: 2010. http://www.mps.gov.cn/n16/n80209/n80481/n804535/2635494.html. [accessed 11 February, 2012] (in Chinese) [Google Scholar]
- 2.National Working Group on Community–based Methadone Maintenance Treatment for Opium Dependents Scaling-up methadone maintenance treatment program in China. Talk presented at UNETG meeting on 25 February 2009. http://www.unaids.org.cn/download/UNETG-090225-NCAIDS.ppt. [accessed 11 February, 2012] (in Chinese)
- 3.Du C, Liu ZM. Discussion on current situations in the methadone maintenance therapy and related problems in our country. Chinese Magazine of Drug Abuse Prevention and Treatment. 2009;15(6):326–330. (in Chinese) [Google Scholar]
- 4.Zhao CZ, An YQ, Zeng LN, Liang JC, Liu YH, Zhao D, et al. Ideas from the problems discovered in the community methadone maintenance therapy. Chin J Drug Depend. 2009;18(3):232–234. (in Chinese) [Google Scholar]
- 5.Jiang HF, Du J, Zhao M. Applications of behavior contingency management in the treatments on substance abuse. Chinese Journal of Behavioral Medicine and Brain Sciences. 2010;2(19):185–186. (in Chinese) [Google Scholar]
- 6.Petry NM, Alessi SM, Marx J, Austin M, Tardif M. Vouchers versus prizes: contingency management treatment of substance abusers in community settings. J Consult Clin Psychol. 2005;73(6):1005–1014. doi: 10.1037/0022-006X.73.6.1005. [DOI] [PubMed] [Google Scholar]
- 7.Petry NM, Peirce JM, Stitzer ML, Blaine J, Roll JM, Cohen A, et al. Effect of prize-based incentives on outcomes in stimulant abusers in outpatient psychosocial treatment programs: a national drug abuse treatment clinical trials network study. Arch Gen Psychiatry. 2005;62(10):1148–1156. doi: 10.1001/archpsyc.62.10.1148. [DOI] [PubMed] [Google Scholar]
- 8.Preston KL, Umbricht A, Epstein DH. Methadone dose increase and abstinence reinforcement for treatment of continued heroin use during methadone maintenance. Arch Gen Psychiatry. 2000;57(4):395–404. doi: 10.1001/archpsyc.57.4.395. [DOI] [PubMed] [Google Scholar]
- 9.Robles E, Stitzer ML, Strain EC, Bigelow GE, Silverman K. Voucher-based reinforcement of opiate abstinence during methadone detoxification. Drug Alcohol Depend. 2002;65(2):179–189. doi: 10.1016/s0376-8716(01)00160-0. [DOI] [PubMed] [Google Scholar]
- 10.Shi JP. The methods of sample size estimation in clinical study. Chinese Journal of Clinical Rehabilitation. 2003;7(10):1569–1571. (in Chinese) [Google Scholar]
- 11.Sheehan DV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, Weiller E, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. 1998;59(suppl 20):22–33. [PubMed] [Google Scholar]
- 12.Si TM, Shu L, Dang WM, Se YA, Chen JX, Dong WT, et al. Evaluation of the reliability and validity of Chinese version of the Mini-International Neuropsychiatric Interview in patients with mental disorders. Chinese Mental Health Journal. 2009;23(7):493–497,503. (in Chinese) [Google Scholar]
- 13.Zhao M, Li X, Hao W, Wang ZC, Zhang MY, Xu D, et al. A preliminary study of the reliability and validity of the Addiction Severity Index. Journal of Chinese Medicine Research. 2004;4(8):679–680. (in Chinese) [Google Scholar]
- 14.Luo W, Wu ZY, Wei XL, Jia W, Zhang QC, Li LL, et al. Adaptation and evaluation of Chinese version of Addiction Severity Index-V and its usage for assessing addiction of patients in methadone maintenance treatment clinics. Chin J Drug Depend. 2007;16(5):373–378. (in Chinese) [Google Scholar]
- 15.McGahan PL, Griffith JA, Parente R, McLellan AT. Addiction Severity Index: Composite scores manual. Philadelphia, USA: University of Pennsylvania/Veteran Administration Center for Studies of Addiction; 1986. [Google Scholar]
- 16.Leonhard C, Mulvey K, Gastfriend DR, Shwartz M. The Addiction Severity Index: A field study of internal consistency and validity. J Subst Abuse Treat. 2000;18(2):129–135. doi: 10.1016/s0740-5472(99)00025-2. [DOI] [PubMed] [Google Scholar]
- 17.Sun AQ. Review and prospective for self-organized peer education. Anti-drug Social Work. 2010;4(17):5–8. [Google Scholar]
- 18.Stitzer ML, Vandrey R. Contingency management: utility in the treatment of drug abuse disorders. Clin Pharmacol Ther. 2008;83(4):644–647. doi: 10.1038/sj.clpt.6100508. [DOI] [PubMed] [Google Scholar]
- 19.Higgins ST, Petry NM. Contingency management. Incentives for sobriety. Alcohol Res Health. 1999;23(2):122–127. [PMC free article] [PubMed] [Google Scholar]