Abstract
We report a 55-year-old male who developed advanced hepatic metastasis and peritoneal carcinomatosis after resection of remnant gastric cancer resection 3 mo ago. The patient only received epidermal growth factor (EGF) receptor antibody (Cetuximab) plus recombinant human endostatin (Endostar). Anti-tumor activity was assessed by 18F-fluorodeoxyglucose (18F-FDG) positron emission tomography/computer tomography (PET/CT) at baseline and then every 4 wk. The case illustrates that 18FDG-PET/CT could make an early prediction of the response to Cetuximab plus Endostar in such clinical situations. 18FDG-PET/CT is a useful molecular imaging modality to evaluate the biological response advanced hepatic metastasis and peritoneal carcinomatosis to Cetuximab plus Endostar in patients after remnant gastric cancer resection.
Keywords: Hepatic metastasis, Remnant gastric cancer, Cetuximab, Recombinant human endostatin, 18F-fluorodeoxyglucose, Positron emission tomography/computer tomography
INTRODUCTION
The activity of epidermal growth factor (EGF) and its receptor (EGFR) has been identified as the key driver in the process of cell growth and replication. There is now a body of evidence that EGFR-mediated drive is increased in a wide variety of solid tumors, including non-small cell lung cancer, prostate cancer, breast cancer, gastric cancer, colon cancer, ovarian cancer and tumors of the head and neck[1]. EGFR antibody (Cetuximab, Erbitux, Merck and Imclone Systems) has been approved by the Food and Drug Administration (FDA)[2] for use in treatment of colorectal cancer. Angiogenesis is the formation of new capillaries from existing blood vessels. The recognition of tumor angiogenesis as a therapeutically useful target is based on experimental evidence that tumor growth and progression are dependent on new blood vessel formation. Endostatin has been shown to inhibit potently angiogenesis in vitro and in vivo and Endostar (Medgenn Bioengineering Co. Ltd. Yantai, Shandong, P. R.China.) has been approved by the State Food and Drug Administration (SFDA)[3]. In this case, we used 18FDG-PET/CT to monitor the early response of advanced hepatic metastasis and peritoneal carcinomatosis to Cetuximab plus Endostar in patients after remnant gastric cancer resection.
CASE REPORT
A 55-year-old male, with a history of subtotal gastrectomy for gastric ulcer 20 years ago, received remnant gastric cancer resection 3 mo ago. Immunohistochemistry revealed adenocarcinoma of the stomach with expression of EGFR. Episodes of fever above 40°C appeared without evidence of infection and mild jaundice developed with weight loss of 10 kg within 1 mo. A palpable liver and tenderness of the left upper abdominal quadrant were found during physical examination. Laboratory findings during the first admission showed 55 g/L HGB, 41.4 μmol/L TBIL, 12.9 μmol/L DBIL, and 28.5 μmol/L IBIL. Advanced hepatic metastasis and peritoneal carcinomatosis were confirmed by 18F-fluorodeoxyglucose positron emission tomography/computer tomography (18F-FDG PET/CT) and biopsy guided by 18F-FDG PET/CT. These findings were supportive for tumor-associated cachexia because his overall performance status was significantly reduced (Karnofsky index: 40%). Conventional chemotherapy was not considered the first choice of treatment for the patient. After giving informed consent, the patient received Cetuximab weekly at 400 mg/m2 iv loading dose, followed by at 250 mg/m2 iv maintenance dose for 8 wk, together with but separately used Endostar daily at 15 mg iv loading dose and maintenance dose for over 8 wk. Anti-tumor activity was assessed by 18F-FDG PET/CT at baseline and then every 4 wk. During the 8-wk follow-up period of time, 18F-FDG PET/CT was performed 3 times to monitor the treatment response. His temperature returned to normal slowly after 4 wk of treatment. Cetuximab exhibited only mild skin toxicity, and hepatic metastasis and peritoneal carcinomatosis lesions had a partial response to Cetuximab treatment (> 30% reduction, according to RECIST) after 4 wk (Figure 1 and Figure 2). Main laboratory tests showed 70 g/L HGB, 21.4 μmol/L TBIL, 13.9 μmol/L DBIL, 16.5 μmol/L IBIL. Karnofsky index was 70%. Due to responses to the treatment without serious complications, after the second treatment cycle, hepatic metastases were almost completely gone on the third 18F-FDG PET/CT (Figures 1 and 2). However, a few metastatic lymphoid nodes in the abdomen could be detected (Figure 3). In parallel, main laboratory tests showed 90 g/L HGB, 20.4 μmol/L TBIL, 12.9 μmol/L DBIL, 15.5 μmol/L IBIL. Karnofsky index was 80%. Due to the confirmed responses to the treatment, the third cycle of treatment was going on when this paper was completed.
Figure 1.
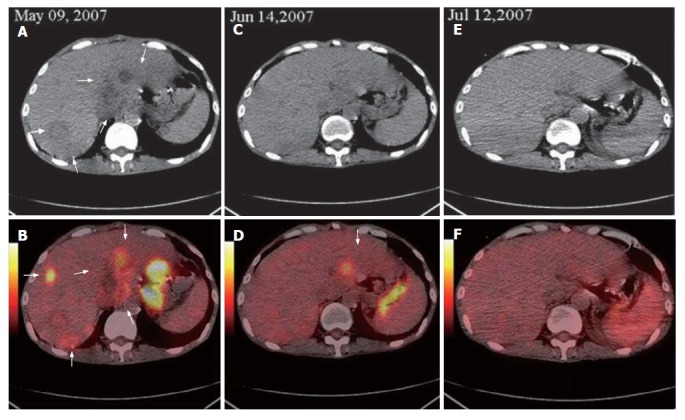
Base line FDG PET/CT detecting a highly metabolic metastasis in liver (white arrows, A and B), second FDG PET/CT demonstrating the decreased number and metabolism level of liver metastases and one highly metabolic metastasis in the left lobe of liver (white arrows, C and D), third FDG PET/CT displaying no lesion at the same position (E and F).
Figure 2.
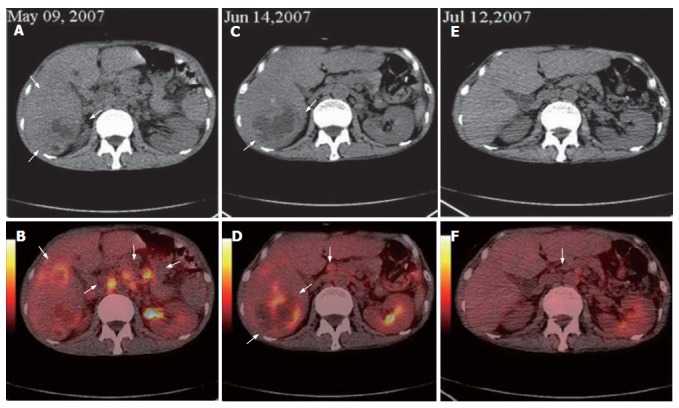
Base line FDG PET/CT detecting huge metastases in the right lobe of liver and highly metastatic lymphoid nodes in abdomen (white arrows, A and B), second FDG PET/CT demonstrating huge metastases in the right lobe of liver and the decreased number, size and metabolism level of metastatic lymphoid nodes (white arrows, C and D), third FDG PET/CT displaying the disappeared huge metastases in the right lobe of liver and the normal size of metastatic lymphoid nodes (E and F).
Figure 3.
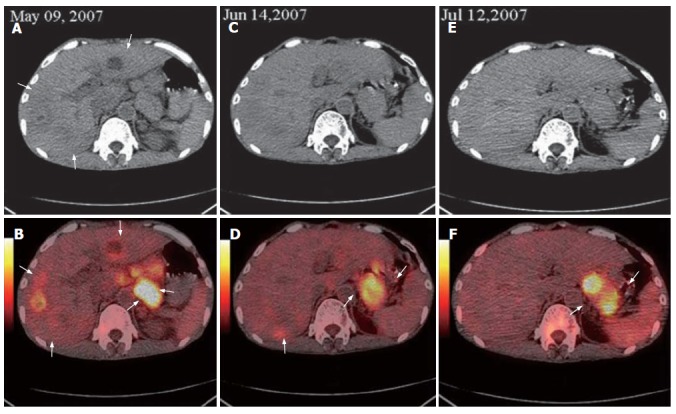
Base line FDG PET/CT detecting multi high metastases in both lobes of liver and highly metastatic lymphoid nodes in abdomen (white arrows, A and B), second FDG PET/CT demonstrating multi high metastases in the liver and the decreased number, size and metabolism level of metastatic lymphoid nodes (white arrows, C and D), third FDG PET/CT displaying disappeared liver metastasis and metastatic lymphoid nodes (E and F).
DISCUSSION
Multiple cellular pathways involved in the growth and metastatic potential of tumors may create heterogeneity, redundancy, and the potential for tumors to bypass signaling pathway blockade, resulting in primary or acquired resistance. Combined therapies are more effective in inhibiting different signaling pathways and can overcome tumor resistance[4]. Vascular endothelial growth factor (VEGF) and EGFR inhibitors have become the key components of therapies for several tumor types. There is a close relationship between these two factors. VEGF signaling is up-regulated by EGFR expression while VEGF up-regulation independent of EGFR signaling seems to contribute to resistance to EGFR inhibition. Therefore, inhibition of both pathways improves anti-tumor efficacy and overcomes resistance to EGFR inhibition[5].
EGFR belongs to a family of receptors known as the ErbB family (ErbB tyrosine kinase receptors), which comprises four proteins encoded by the c-erbB proto-oncogene. EGFR can activate a cascade of multiple signaling pathways that facilitate tumor growth process[6]. The EGFR signaling pathway regulates cell differentiation, proliferation, migration, angiogenesis, and apoptosis, all of which are down regulated in cancer cells. In a study, EGFR immunoreactivity was detected in one (3.8%) of the 26 early gastric carcinomas and in 33 (34.4%) of the 96 advanced gastric carcinomas, respectively, the incidence of expression between the two groups was significantly different[7]. In gastric cancer, the management of peritoneal dissemination in the peritoneal cavity is extremely important. However, peritoneal dissemination in the final stage of gastric cancer remains untreatable. VEGF is correlated with peritoneal metastasis from gastric cancer, and has been reported as a useful indicator of peritoneal recurrence[8].
Cetuximab is a chimeric IgG1 monoclonal antibody and binds to EGFR with a high specificity and a higher affinity than either EGF or TGF-α, thus blocking ligand-induced phosphorylation of EGFR. Second line therapies with Cetuximab for colorectal cancer after failure of first-line regimes have shown a response rate of 17%-23% and an overall survival (median) of 8.6 mo[9]. Endostar is a new recombinant human endostatin developed by Medgenn Bioengineering Co. Ltd (Yantai, Shandong, China) in 2005. A preclinical study indicated that endostar could inhibit tumor endothelial cell proliferation, angiogenesis and tumor growth, and results from prospective trials addressing the response of colorectal cancer to Cetuximab containing regimes have confirmed its efficacy in clinical practice[10].
Modern cancer care is critically dependent on imaging technologies, which are used to detect early tumors and guide their therapy or surgery[11]. Molecular imaging technologies provide information about the functional or metabolic characteristics of malignancies, tumor stage and therapeutical response, and tumor recurrence, whereas conventional imaging technologies predominantly assess the tumor’s anatomical or morphologic features including its size, density, and shape, etc. Since conventional imaging technologies reveal morphology of lesions with nonspecific features, differentiation between malignant and benign lesions could be improved by molecular imaging. As our knowledge about the molecular basis of cancer increases, imaging methods that provide clinicians with telling details about the molecular environments of patients’ tissues are needed. By using standard anatomic imaging technologies combined with molecular imaging technologies such as PET/CT, we can detect disease processes at the anatomic, physiologic, metabolic, and molecular levels, thereby, allowing earlier detection of diseases, monitoring of therapies, and better prognostication of disease progression[12].
The precise tailoring of treatment for patients with cancer is a challenge. PET/CT and SPECT/CT help achieve better results[13]. PET with the glucose analog 18F-FDG is increasingly used to monitor the effectiveness of therapy for patients with malignant lymphomas and solid tumors. Quantitative assessment of therapy-induced changes in tumor 18F-FDG uptake can predict tumor response and patient outcome early in the course of therapy. Treatment may be adjusted according to the chemosensitivity and radiosensitivity of tumor tissue in an individual patient. Thus, 18F-FDG PET has a potential to reduce the side effects and costs of ineffective therapy[14]. The use of integrated PET/CT instead of PET in treatment monitoring poses some methodologic challenges against the quantitative analysis of PET scans. However, it may provide the opportunity to integrate morphologic and functional information. This integration may define new parameters for assessment of tumor response and facilitate the use of PET in studies as well as in clinical practice[14]. In our case, a partial response (> 30% reduction, according to RECIST) of hepatic metastasis and peritoneal carcinomatosis lesions was achieved after 4 wk of treatment with Cetuximab plus Endostar.
In conclusion, our case demonstrates that molecular imaging could monitor molecular treatment and combination of EGFR-specific antibodies with VEGF-specific antibodies may be a promising treatment modality. Further prospective trials are mandatory to confirm its effects and discriminate Cetuximab-induced response from Endostar-associated response. The potential of this novel approach to anticancer therapy should be elucidated in large clinical trials.
Footnotes
S- Editor Liu Y L- Editor Wang XL E- Editor Wang HF
References
- 1.Shelton JG, Steelman LS, Abrams SL, Bertrand FE, Franklin RA, McMahon M, McCubrey JA. The epidermal growth factor receptor gene family as a target for therapeutic intervention in numerous cancers: what's genetics got to do with it? Expert Opin Ther Targets. 2005;9:1009–1030. doi: 10.1517/14728222.9.5.1009. [DOI] [PubMed] [Google Scholar]
- 2. Available from: http: //www.fda.gov/cder/drug/infopage/erbitux/default.htm.
- 3. Available from: http: //app1.sfda.gov.cn/webportal/portal.po? UID=DWV1_WOUID_URL_11635827&POpType=DBSearch&DBSearch=DJSearch&DJSearch=DJDetailPg& DJDetailPg=MTcyNTEx&selDbName=PLDB_TBL_TABLE7&tblCol=OID&Ptype1_sld=0&Ptype2_sld=0& Ptype3_sld=0.
- 4.Tabernero J. The role of VEGF and EGFR inhibition: implications for combining anti-VEGF and anti-EGFR agents. Mol Cancer Res. 2007;5:203–220. doi: 10.1158/1541-7786.MCR-06-0404. [DOI] [PubMed] [Google Scholar]
- 5.Ciardiello F, Bianco R, Caputo R, Caputo R, Damiano V, Troiani T, Melisi D, De Vita F, De Placido S, Bianco AR, et al. Antitumor activity of ZD6474, a vascular endothelial growth factor receptor tyrosine kinase inhibitor, in human cancer cells with acquired resistance to antiepidermal growth factor receptor therapy. Clin Cancer Res. 2004;10:784–793. doi: 10.1158/1078-0432.ccr-1100-03. [DOI] [PubMed] [Google Scholar]
- 6.Becker JC, Muller-Tidow C, Serve H, Domschke W, Pohle T. Role of receptor tyrosine kinases in gastric cancer: new targets for a selective therapy. World J Gastroenterol. 2006;12:3297–3305. doi: 10.3748/wjg.v12.i21.3297. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Takehana T, Kunitomo K, Suzuki S, Kono K, Fujii H, Matsumoto Y, Ooi A. Expression of epidermal growth factor receptor in gastric carcinomas. Clin Gastroenterol Hepatol. 2003;1:438–445. doi: 10.1016/s1542-3565(03)00219-2. [DOI] [PubMed] [Google Scholar]
- 8.Aoyagi K, Kouhuji K, Yano S, Miyagi M, Imaizumi T, Takeda J, Shirouzu K. VEGF significance in peritoneal recurrence from gastric cancer. Gastric Cancer. 2005;8:155–163. doi: 10.1007/s10120-005-0329-4. [DOI] [PubMed] [Google Scholar]
- 9.Cunningham D, Humblet Y, Siena S, Khayat D, Bleiberg H, Santoro A, Bets D, Mueser M, Harstrick A, Verslype C, et al. Cetuximab monotherapy and cetuximab plus irinotecan in irinotecan-refractory metastatic colorectal cancer. N Engl J Med. 2004;351:337–345. doi: 10.1056/NEJMoa033025. [DOI] [PubMed] [Google Scholar]
- 10.Wang JW, Sun Y, Liu YY, Yu QT, Zhang YP, Li K, Zhu YZ, Zhou QH, Hou M, Guan ZZ, et al. Results of randomized, multicenter, double-blind phase III trial of rh-endostatin (YH-16) in treatment of advanced non-small cell lung cancer patients. Zhongguo Feiai Zazhi. 2005;4:283–290. doi: 10.3779/j.issn.1009-3419.2005.04.07. [DOI] [PubMed] [Google Scholar]
- 11.Weissleder R. Molecular imaging in cancer. Science. 2006;312:1168–1171. doi: 10.1126/science.1125949. [DOI] [PubMed] [Google Scholar]
- 12.Hoffman JM, Gambhir SS. Molecular imaging: the vision and opportunity for radiology in the future. Radiology. 2007;244:39–47. doi: 10.1148/radiol.2441060773. [DOI] [PubMed] [Google Scholar]
- 13.Shu CJ, Guo S, Kim YJ, Shelly SM, Nijagal A, Ray P, Gambhir SS, Radu CG, Witte ON. Visualization of a primary anti-tumor immune response by positron emission tomography. Proc Natl Acad Sci USA. 2005;102:17412–17417. doi: 10.1073/pnas.0508698102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Sasaki R, Komaki R, Macapinlac H, Erasmus J, Allen P, Forster K, Putnam JB, Herbst RS, Moran CA, Podoloff DA, et al. [18F]fluorodeoxyglucose uptake by positron emission tomography predicts outcome of non-small-cell lung cancer. J Clin Oncol. 2005;23:1136–1143. doi: 10.1200/JCO.2005.06.129. [DOI] [PubMed] [Google Scholar]
- 15.Gillies RJ. Noninvasive imaging of anticancer therapy. Mol Cancer Ther. 2003;2:333–334. [PubMed] [Google Scholar]


