Abstract
Introduction
Preterm premature rupture of membranes (PPROM) complicates 1–5 % of all pregnancies and is the major contributory factor for perinatal morbidity and mortality. Micronutrient deficiency (vitamin C) is associated with increased risk of PPROM. This study was conducted to establish the association between maternal plasma vitamin C concentration in women with PPROM and women without PPROM and to study the difference in maternal morbidity, neonatal morbidity, and mortality.
Methods
A prospective study was conducted where 40 women (20 in each study and control group) with singleton pregnancies between 28 and 37 weeks gestation were recruited. Women with anemia, diabetes, UTI, RTI, vaginal infection, bleeding, h/o PPROM in previous pregnancy, polyhydramnios, and smoker were excluded from the study. Maternal plasma vitamin C levels were measured.
Results
Ascorbic acid levels were low in women with PPROM 0.41 ± 0.08 versus 0.84 ± 0.19 mg/dl. There is a linear decline in plasma vitamin C levels as the pregnancy advances. Inverse relationship was observed between duration of rupture of membranes and vitamin C levels. There was a significant difference in maternal morbidity, neonatal morbidity, and mortality.
Conclusion
Ascorbic acid concentration was low in women with PPROM. Thus, vitamin C supplementation should be made mandatory along with iron and calcium to antenatal women to avoid the complications of PPROM.
Introduction
Preterm premature rupture of membranes (PPROM) complicates 1–3 % of all pregnancies and is the major contributory factor for perinatal morbidity and mortality. Approximately, 40 % of preterm births are associated with PPROM [1, 2].
The cause of PPROM is unknown but the pathophysiology appears to be multifactorial. Recent evidence suggests that membrane rupture is also related to biochemical processes such as abnormalities in collagen structure and formation as well as increased oxidative stress [3].
Micronutrient deficiency that leads to abnormal collagen structure has been associated with increased risk of PPROM [3, 4]. The micronutrient vitamin C is an effective water soluble antioxidant that scavenges several reactive oxygen species, thus reducing oxidative stress. It also acts as an enzymatic cofactor to the enzymes lysyl hydroxylase and prolyl hydroxylase, which is required for synthesis of hydroxyproline and hydroxylysine. Collagen requires hydroxyproline bridges across the triple helix to provide stability to it. Ascorbic acid also causes downregulation of the metalloproteinase-2 and biosynthesis of collagen where it is required for the formation of triple helical structure of collagen.
Thus, ascorbic acid participates in the equilibrium between synthesis and degradation of collagen and this may be critical in reducing the occurrence of preterm PROM [5, 6].
Daily supplementation of 100 mg/day vitamin C after 20 weeks gestation effectively reduces the incidence of PROM [7].
We conducted a study to compare the serum vitamin C levels in women with preterm PROM and women without PPROM.
Objective
To establish the association between maternal plasma vitamin C concentration in women with PPROM and women without PPROM and also to study the difference in maternal & perinatal morbidity and mortality in both the groups.
Methods
Prospective randomised study was conducted in our institution for a period of 1 year from Dec 2011 to 2012, where 40 women with singleton pregnancies between 28 and 37 weeks were recruited.
Study group included 20 antenatal women with history of PPROM and fulfilled the inclusion and exclusion criteria.
Control group also included 20 pregnant women without PPROM following every recorded case of PPROM and matched for gestational age.
Inclusion criteria
Women who were willing to participate in the study and gave written consent to complete the study.
Exclusion criteria
Women with anemia, diabetes, UTI, RTI, vaginal infection, polyhydramnios, smoker, h/o PPROM in previous pregnancy, and evidence of chorioamnionitis in current pregnancy were excluded from the study.
A general physical and abdominal examination was done. Sterile per speculum examination along with nitrazine test and ferning test was carried out to confirm PPROM. Vaginal swab culture was obtained.
After 6–8 h fasting, maternal 5 ml venous blood samples were collected in EDTA vial to estimate vitamin C concentration from both the groups. Vitamin C cut off limit taken as 0.6 mg/dl [8], and all the patients were followed till the delivery.
Results
There were no statistically significant difference in age and parity among both the groups. 50 % versus 60 % of women belonged to 20–25 years of age in study and control groups, respectively (Table 1).
Table 1.
Age distribution
| Age group (years) | Study group | Control group |
|---|---|---|
| 20–25 | 10 (50 %) | 12 (60 %) |
| 26–31 | 10 (50 %) | 7 (35 %) |
| 32–37 | 0 | 1 (5 %) |
| Total | 20 | 20 |
65 % women in study group compared to 50 % in control group were multigravidas (Table 2).
Table 2.
Parity distribution
| Parity | Study group | Control group |
|---|---|---|
| Primigravida | 7 (35 %) | 10 (50 %) |
| Multigravida | 13 (65 %) | 10 (50 %) |
| Total | 20 | 20 |
Majority (30 %) of women reported within 6–12 h of rupture of membranes (Table 3).
Table 3.
Duration of rupture of membranes
| Duration (hrs) | Study group (n = 20) |
|---|---|
| <6 | 1 (5 %) |
| 6–12 | 6 (30 %) |
| 12–24 | 5 (25 %) |
| 24–48 | 5 (25 %) |
| >48 | 3 (15 %) |
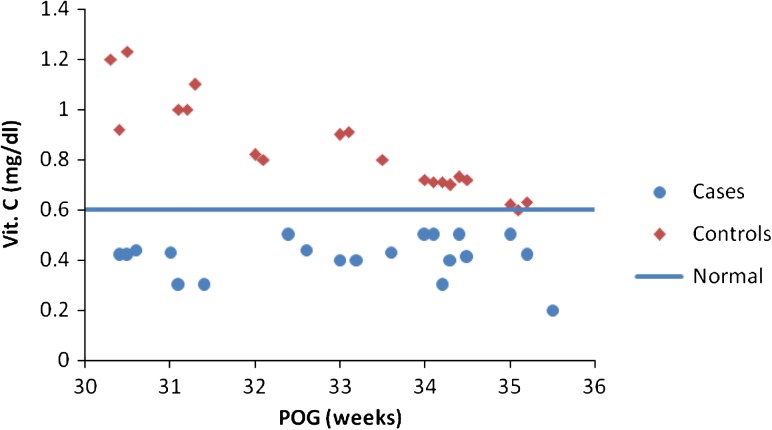
Ascorbic acid levels were low in women with PPROM. There was a statistically significant difference in vitamin C levels in both the groups, and the mean was 0.41 ± 0.08 versus 0.84 ± 0.19 mg/dl in controls (t test .000 SS). There is a linear decline in Plasma vitamin C levels as the pregnancy advances (Fig. 1).
Fig. 1.
Comparison of vitamin C levels at different POG in both the groups
Inverse relationship was observed between duration of PPROM and vitamin C levels (Table 4).
Table 4.
Relation of vitamin C and duration of PPROM in both the groups
| Duration of PPROM | Plasma vitamin C levels |
|---|---|
| <48 h | 0.2–0.5 mg/dl |
| >48 h | 0.1 mg/dl |
There was a significant difference in the mode of deliveries, and 55 % of women underwent LSCS in the study group VS 20 % in the control group (Pearson Chi-square test 0.022 SS). Maternal morbidity was increased in the study group as three (15 %) women had wound dehiscence and prolonged hospital stay. NICU stay beyond 24 h was 60 % versus 15 % in the study and control groups, respectively. Early neonatal deaths were more in the study group 25 % probably due to prematurity and low birth weight (Table 5).
Table 5.
Maternal and fetal outcome in both the groups
| Study group | Control group | |
|---|---|---|
| Mode of deliveries | ||
| LSCS | 11 (55 %) | 4 (20) % |
| NVD | 09 (45 %) | 16 (80) % |
| Wound dehiscence | 3 (15 %) | 0 |
| NICU admissions | 12 (60 %) | 3 (15 %) |
| Mean NICU (days) | 9.42 ± 4.89 | 6.33 ± 3.1 |
| Early neonatal death | 5 (25 %) | 2 (10 %) |
Discussion
The main cause of PROM with different pathologies is disorder in collagen metabolism. Reduction in collagen content of membranes decreases their stability and causes rupture of membranes. Vitamin C supplementation during pregnancy can prevent PROM as it regulates the metabolism of membrane’s collagen and augment their resistance.
The association between vitamin C and the preventable devastating consequences of preterm PROM and prematurity encouraged us to study the plasma levels of ascorbic acid in women with and without rupture of membranes. This may be necessary to develop health strategies aimed at improving outcome by predicting and preventing PPROM.
Osakhuwuomwan JA et al. [8] reported that plasma vitamin c decreases with increasing gestational age, and its levels were low in women with PPROM compared to the women without PPROM 0.53 ± 0.05 versus 0.58 ± 0.05 mg/dl. Our study also observed a decreasing trend of vitamin C as the pregnancy advances and vitamin C levels in women with PPROM and without PPROM was 0.41 ± 0.08 versus 0.84 ± 0.19 mg/dl.
Barett BM et al. [9] conducted a study and concluded that PROM patients had lower ratios of ascorbic acid in amniotic fluid than controls and lower ratios of amniotic fluid to serum ascorbic acid (p < 0.0001). Our study also showed lower ascorbic acid concentration in PROM women compared to the controls (0.41 ± 0.08 Vs 0.84 ± 0.19).
Tejero E et al. [10] and Awolelu CO et al. [11] concluded no significant difference in the study and the control groups, which is contradictory to our study.
Mehrangiz et al. [12] reported that vitamin c supplementation prevents early rise of serum estriol, and its levels were low in women without PROM as compared to women receiving placebo (p = 0.044).
Conclusion
Vitamin C concentrations were low in PPROM patients, and also its concentration declines as the pregnancy advances. However, large multicenter clinical trials are required to further test this association of ascorbic acid and PPROM. Vitamin C supplementation should be made mandatory along with iron and calcium to antenatal women to avoid the preventable complications of PPROM.
Richa Sharma
have done M.B.B.S from ST.Johns”s Medical College Bangalore and M.S from KMC Mangalore (M.A.H.E).Joined U.C.M.S –GTB Hospital Delhi, as senior resident and currently working as assistant professor on permanent post with seven and half yrs of post M.D experience.My areas of interests are high risk pregnancy and infertility. I like to present papers on the above topics in the conferences and would be greatful to be the speaker for these topics in the conferences and workshops.
References
- 1.Mercer B, Milluzi C, Collin M. Periviable birth at 20–26 weeks of gestation. Proximate causes, previous obstetric history and recurrence risk. Am J Obstet Gynecol. 2005;193(3pt2):1175–1180. doi: 10.1016/j.ajog.2005.05.040. [DOI] [PubMed] [Google Scholar]
- 2.Mercer BM. Preterm PROM diagnosis and management. Clin Perinatol. 2004;31(4):765–782. doi: 10.1016/j.clp.2004.06.004. [DOI] [PubMed] [Google Scholar]
- 3.Parry S, Strauss JF. Mechanism of disease premature rupture of membranes. N Engl J Med. 1998;338:663–670. doi: 10.1056/NEJM199803053381006. [DOI] [PubMed] [Google Scholar]
- 4.McParland PC, Taylor DJ. Preterm prelabour rupture of membranes. In: Boonar J, Dinlop W (Ed). Recent Advances in Obstet and Gynecol; 2005. p. 27–38.
- 5.Shan TT, Defranco EA, Stamillo DM, et al. A population based study of race specific risk of PPROM. Am J Obstet Gynecol. 2008;198(4):373. doi: 10.1016/j.ajog.2008.05.011. [DOI] [PubMed] [Google Scholar]
- 6.Woods JR, Plessinger MA, Miller RK. Vitamin C and E missing links in preventing PPROM? Am J Obstet Gynecol. 2001;185(1):5–10. doi: 10.1067/mob.2001.115868. [DOI] [PubMed] [Google Scholar]
- 7.Casanueva E, Ripoll C, Tolentino M, et al. Vitamin C supplementation to prevent premature rupture of the chorioamniotic membranes: a randomized trial. Am J Clin Nutr. 2005;81:859–863. doi: 10.1093/ajcn/81.4.859. [DOI] [PubMed] [Google Scholar]
- 8.Osaikhuwuomwen JA, Okpere EE, Okonkwo CA, et al. Plasma vitamin C levels and risk of preterm prelabour rupture of membrane. Arch Gynecol Obstet. 2011;284(4):595. doi: 10.1007/s00404-010-1741-5. [DOI] [PubMed] [Google Scholar]
- 9.Barett BM, Sowell A, Gunter E, et al. Potential role of ascorbic acid and beta carotene in the prevention of PROM. Int J Vitam Nutr Res. 1994;64(3):192–197. [PubMed] [Google Scholar]
- 10.Tejero E, Perichart O, Pfeffer F, et al. Collagen synthesis during pregnancy, vitamin C availability and risk of premature rupture of foetal membranes. Int J Gynaecol Obstet. 2003;81:29–34. doi: 10.1016/S0020-7292(02)00400-9. [DOI] [PubMed] [Google Scholar]
- 11.Awoyelu CO, Agharanya JC, Oguntibeju OO. Ascorbic acid status in third trimester of pregnancy at delivery and in cord blood. Indian J Clin Biochem. 2004;19(1):54–56. doi: 10.1007/BF02872390. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Zamani M, Goodarzi MT, Lavasani NS, et al. Effects of ascorbic Acid on serum level of unconjugated estriol and its relationship with preterm premature rupture of membrane: a double-blind randomized controlled clinical trial. Iran J Med Sci. 2013;38(3):227–232. [PMC free article] [PubMed] [Google Scholar]