Abstract
We report a rare case of a young man with hereditary multiple exostoses (HME) who presented with severe pain in the hips, requiring bilateral total hip arthroplasty (THA), along with excision of the exostoses. The reported incidence of exostoses around the hip has been reported from 30% in some series to 90% in other studies of HME. These patients may remain asymptomatic, but if not, their symptoms are usually related to the presence of the exostoses itself and the possibility of hip osteoarthrosis is frequently overlooked. This may account for a low incidence of THA for this condition. Surgical management often remains challenging as such lesions are not commonly encountered in the clinical practice and are often very difficult to treat.
Background
Bilateral hip lesions in hereditary multiple exostoses (HME) are rare and complex.1–4 They may be associated with premature osteoarthrosis (OA) of the hip. The treatment of multiple exostoses with OA should not only involve removing the exostoses but must also address the OA with total hip arthroplasty (THA) in severe and symptomatic cases. We performed bilateral THA in our young patient. The surgery was challenging and complex due to disturbed anatomy.
Case presentation
A 27-year-old man presented with bilateral hip pain and difficulty in walking for the past 1.5 years. The pain was severe enough to prevent him from walking and performing activities of daily living independently. It first developed in the left hip and subsequently also affected the right hip. It was insidious in onset and mild in intensity initially, but gradually progressed to severe and constant pain. The patient had multiple bony swellings over his body since childhood, which had grown gradually as he matured. He also had a family history of similar swellings in his younger brother and mother. There were no associated comorbid medical problems noted.
On examination, the patient was short statured (figure 1) with a thin build; he walked with a waddling gait. There were multiple hard bony swellings over his hips, proximal tibia, distal femur, scapula and proximal humerus. Both hips had limited range of motion with bilateral fixed flexion deformity of 30° and bilateral fixed external rotational deformity (20°). There was a large hard bony swelling (2″×3″) present in the right inguinal and left iliac region. The right lower limb was longer than the left by 1 cm.
Figure 1.

Multiple bony swellings (exostoses) over the scapulae, pelvis and arm.
Investigations
Anteroposterior X-ray of the pelvis showed exophytic bony growth in the femur and pelvic bone with degenerative changes in the hips and coxa valga, decreased centre edge angle and increased neck head width ratio (figure 2). CT of the pelvis confirmed exophytic growth with cartilaginous cap in the femur and pelvic bones (figures 3 and 4) and significant secondary OA changes in the hips.
Figure 2.

Anteroposterior X-ray of the pelvis showing exophytic growth in bilateral femur and pelvis.
Figure 3.

CT of the pelvis showing exostoses in bilateral femur and pelvis.
Figure 4.

CT scan showing osteoarthrosis changes in bilateral hips.
Differential diagnosis
Loose bodies
Chondrosarcoma
Heterotopic ossification
Multiple epiphysial dysplasia
Treatment
The left hip was operated on first, using an anterolateral approach (modified Hardinges), where excision of exostoses from the femur and acetabulum was carried out; the arthritic hip was replaced with uncemented prosthesis using a 36 mm head with 58 mm cross-linked polyethylene acetabular cup (Stryker). One week later, the right hip was operated on, using an anterior approach. The osteochondromas were first excised from the pelvis through an anterior ilioinguinal approach; subsequently the THA was performed using a modified Smith Peterson approach. An uncemented THA using SROM prosthesis (Depuy) was carried out. A corrective femoral osteotomy was required in the upper third of the femur to accommodate the femoral stem of the prosthesis (figure 5). This osteotomy was fixed using one eight-hole low-contact dynamic compression plate.
Figure 5.
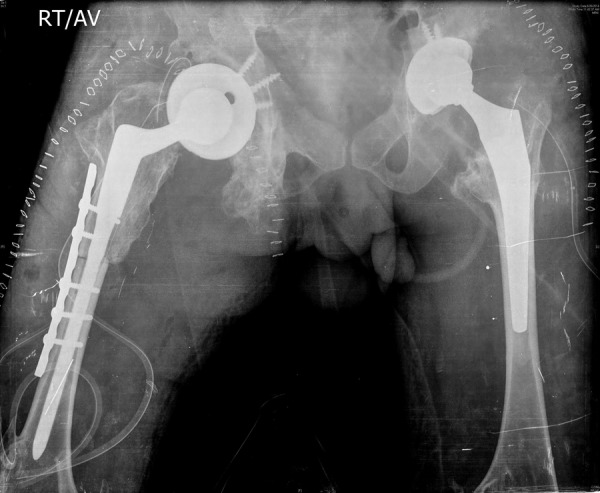
Bilateral total hip arthroplasty showing revision of the left hip femoral stem (with larger stem and longer neck length).
The left hip was found to be dislocated after right hip arthroplasty (figure 6). After closed reduction the hip was found unstable, hence an open reduction with revision to a larger stem size 2–3 (with improved version) and longer neck length, from size +5 to +10, was made. A boot and bar cast was applied on the left leg for 3 weeks, to prevent dislocation.
Figure 6.

X-ray of the pelvis of bilateral hip arthroplasty showing dislocated left hip and uncemented S-ROM right hip with femoral osteotomy fixed with low-contact dynamic compression plate.
Outcome and follow-up
At follow-up, after 12 months both hips were found stable (figure 7), and the osteotomy on the right side had healed. The patient was mobilising with full weight bearing. Harris hip score improved from 15 preoperatively to 78 postoperatively on the right side and 18–86 on the left side.
Figure 7.

Twelve months’ follow-up X-ray of both hips showing well-reduced hips and healed right femoral osteotomy.
Discussion
HME are a type of skeletal dysplasia characterised by the presence of multiple exostoses.5 This uncommon condition has an incidence of 1 in 50 000 population, with autosomal dominant inheritance of variable penetrance.6 7 The exostoses in HME are usually diagnosed in the first decade of life in affected individuals (80%). These cases are discovered relatively early due to their positive family history.1 Exostoses may develop in any bone preformed in cartilage but are usually found on metaphysis of a long bone near the physis and are most commonly seen on the distal femur, proximal tibia and proximal humerus.5 Deep-seated osteochondromas in areas such as the proximal femur or pelvis are not easily diagnosed as they rarely cause symptoms.7
The presence and severity of symptoms in the hip are related to the location of osteochondromas.8 Lesions in the medial femur and periacetabular region cause more pain as they alter the hip parameters and its development resulting in acetabular dysplasia and coxa valga. Acetabular dysplasia and coxa valga occur in approximately 25% of patients with HME.9 10 The femoral head itself does not appear to be primarily affected, hence findings of coxa valga may require intervention as varus osteotomy, which may delay arthritis.1 As compared to medial and periacetabular lesions, lateral femoral lesions occur less often and also cause less pain and discomfort, and do not alter the hip geometry.8
The reported view about the association of symptoms to hip pathology in HME has changed over the years. Previously, pain and limitation in hip movement were related to mechanical restriction by exostoses around the femoral neck.4 However, more recently, it has been recognised that other hip pathologies due to skeletal dysplasia are also responsible for causing symptoms. These include coxa valga, acetabular dysplasia and partial uncoverage of femoral head.10 11 Scarborough and Moreau12 had attributed premature osteoarthritis to acetabular dysplasia and coxa valga. Since then, the concept of premature osteoarthritis of the hip as a result of abnormalities of the proximal femur and acetabulum has gained importance as a cause of hip symptoms in patients of HME.
Total hip replacement has seldom been reported as a treatment for hip involvement in HME. There are only a few reports present in which THA was performed for the condition.4 13 14 15 It has been recognised that THA is a technically difficult procedure in HME due to distorted hip anatomy, such as coxa valga, acetabular dysplasia, short stature and limb length discrepancy, which creates difficulty in placing properly sized implants.15 THA for severe hip involvement in HME leads to good symptomatic relief with improvement in Harris hip scores and good functional outcome.13 We believe that THA (in association with removal of most accessible and symptomatic osteochondromas) can offer a one stage and definitive solution to treat osteochondroma associated with secondary OA due to HME.
Patient's perspective.
I was feeling hopeless due to the complex nature of my problem and as no definitive treatment was offered to me. I was suffering with severe agonising pain in the hips. However, after bilateral hip surgery, I felt as if a new lease of life had been given to me.
Learning points.
Hereditary multiple exostosis is a rare developmental disorder which also affects the hips.
Premature osteoarthrosis of the hip can be a presenting symptom in multiple hereditary exostoses.
Total hip arthroplasty can be a definitive procedure to treat hip arthritis in hereditary multiple exostoses.
Footnotes
Contributors: All the authors have contributed in writing this manuscript.
Competing interests: None.
Patient consent: Obtained.
Provenance and peer review: Not commissioned; externally peer reviewed.
References
- 1.Steiber JR, Dormans JP. Manifestation of hereditary multiple exostoses. J Am Acad Orthop Surg 2005;13:110–20. [DOI] [PubMed] [Google Scholar]
- 2.Saglik Y, Altay M, Unal VS et al. Manifestations and management of osteochondromas: a retrospective analysis of 382 patients. Acta Orthop Belg 2006;72:748–55. [PubMed] [Google Scholar]
- 3.Felix NA, Mazur JM, Loveless EA. Acetabular dysplasia associated with multiple hereditary exostoses. A case report. J Bone Joint Surg Br 2000;82:555–7. 10.1302/0301-620X.82B4.9894 [DOI] [PubMed] [Google Scholar]
- 4.Singh V, Carter S. Total hip replacement in diaphyseal aclasis: a case report. Int J Orthop Surg 2007;5:10. [Google Scholar]
- 5.Heck RK., Jr Campbell Operative Orthopaedics. 11th edn, 2008 chap 20:860–2. [Google Scholar]
- 6.Makhdom AM, Jiang F, Hamdy RC et al. Hip joint osteochondroma: systemic review of literature and report of further three cases. Adv Orthop 2014;2014:180254 10.1155/2014/180254 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Porter DE, Benson MK, Hosney GA. The hip in hereditary multiple exostoses. J Bone Joint Surgery[Br] 2001;83-B:988–95. 10.1302/0301-620X.83B7.10779 [DOI] [PubMed] [Google Scholar]
- 8.El-Fiky TA, Chow W, Li YH et al. Herditary multiple exostoses of the hip. J Orthop Surg (Hong Kong) 2009;17:161–5. [DOI] [PubMed] [Google Scholar]
- 9.Malagon V. Development of hip dysplasia in hereditary multiple exostoses. J Paed Orthop 2001;21:205–11. [PubMed] [Google Scholar]
- 10.Shapiro F, Simon S, Glimcher MJ. Hereditary multiple exostoses: anthropometric, roentgenographic and clinical aspects. J Bone Joint Surg[Am] 1979;61-A:815–24. [PubMed] [Google Scholar]
- 11.Weiner DS, Hoyt WA Jr. The development of the upper end of the femur in hereditary multiple exostoses. Clin Orthop Relat Res 1978;137:187–90. [PubMed] [Google Scholar]
- 12.Scarborough MT, Moreau G. Benign cartilage tumors. Orthop Clin North Am 1996;27:583–9. [PubMed] [Google Scholar]
- 13.Moran M, Kreig AH, Boyle RA et al. Bilateral total hip arthroplasty in severe hereditary multiple exostoses: a report of two cases. Hip Int 2009;19:279–82. [DOI] [PubMed] [Google Scholar]
- 14.Annapureddy SR, Chapman TWL, Charnley GJ. Dual aetiology hip pain requiring total hip arthroplasty in hereditary multiple exostoses: a case report and review of the literature. Hip Int 2002;12:397–9. [DOI] [PubMed] [Google Scholar]
- 15.Mesfin A, Goddard MS, Tuakli-Wosornu YA et al. Total hip and knee arthroplasty in patients with hereditary multiple exostoses. Orthopedics 2012;35:e1807–10. 10.3928/01477447-20121120-29 [DOI] [PubMed] [Google Scholar]


