Abstract
Orthorexia nervosa describes a pathological obsession with proper nutrition that is characterized by a restrictive diet, ritualized patterns of eating, and rigid avoidance of foods believed to be unhealthy or impure. Although prompted by a desire to achieve optimum health, orthorexia may lead to nutritional deficiencies, medical complications, and poor quality of life. Despite its being a distinct behavioral pattern that is frequently observed by clinicians, orthorexia has received very little empirical attention and is not yet formally recognized as a psychiatric disorder. In this review, we synthesize existing research to identify what is known about the symptoms, prevalence, neuropsychological profile, and treatment of orthorexia. An examination of diagnostic boundaries reveals important points of symptom overlap between orthorexia and anorexia nervosa, obsessive–compulsive disorder (OCD), obsessive–compulsive personality disorder (OCPD), somatic symptom disorder, illness anxiety disorder, and psychotic spectrum disorders. Neuropsychological data suggest that orthorexic symptoms are independently associated with key facets of executive dysfunction for which some of these conditions already overlap. Discussion of cognitive weaknesses in set-shifting, external attention, and working memory highlights the value of continued research to identify intermediate, transdiagnostic endophenotypes for insight into the neuropathogenesis of orthorexia. An evaluation of current orthorexia measures indicates a need for further psychometric development to ensure that subsequent research has access to reliable and valid assessment tools. Optimized assessment will not only permit a clearer understanding of prevalence rates, psychosocial risk factors, and comorbid psychopathology but will also be needed to index intervention effectiveness. Though the field lacks data on therapeutic outcomes, current best practices suggest that orthorexia can successfully be treated with a combination of cognitive-behavioral therapy, psychoeducation, and medication.
Keywords: orthorexia nervosa, diagnosis, psychometrics, neuropsychology, endophenotypes, treatment
Introduction
Orthorexia nervosa, literally meaning “proper appetite”, is a pathological fixation with healthy food that has aptly been described as “a disease disguised as a virtue”.1 Although not yet officially recognized as a psychiatric diagnosis, orthorexia is often associated with significant impairment, as what starts as an attempt to attain optimum health through attention to diet may lead to malnourishment, loss of relationships, and poor quality of life. Relative to other styles of unhealthy eating, orthorexia has been largely neglected by the scientific community even though its behavioral pattern is frequently observed by eating disorder specialists.2 In this review, we describe what is known about the symptoms, epidemiology, and assessment of orthorexia, including a discussion of its diagnostic boundaries and neuropsychological profile. We also highlight what remains unknown about this problematic eating pattern and suggest multiple avenues for additional research.
Symptoms of orthorexia
First coined by Bratman and Knight in 1997, the term orthorexia nervosa describes individuals with an obsession for proper nutrition who pursue this obsession through a restrictive diet, a focus on food preparation, and ritualized patterns of eating. Orthorexic individuals are typically concerned by the quality, as opposed to the quantity, of food in one’s diet,3 spending considerable time scrutinizing the source (eg, whether vegetables have been exposed to pesticides; whether dairy products came from hormone-supplemented cows), processing (eg, whether nutritional content was lost during cooking; whether micro-nutrients, artificial flavoring, or preservatives were added), and packaging (eg, whether food may contain plastic-derived carcinogenic compounds; whether labels provide enough information to judge the quality of specific ingredients) of foods that are then sold in the marketplace.4 The fixation on food quality – a combination of the nutritional value of food as well its perceived purity – is prompted by a desire to maximize one’s own physical health and well-being, rather than religious beliefs or concerns for sustainable agriculture, environmental protection, or animal welfare. Such preoccupation with health from food may elicit eating patterns that are especially complex (eg, internalized rules governing which foods can be combined at one sitting or at certain times of day) and/or require unusually long periods of time to execute (eg, beliefs that maximal digestion of one food type occurs a certain amount of time after ingestion of another food type). Outside of meals, extra time is spent researching and cataloging food, weighing and measuring food, and planning future meals, with additional, intrusive, food-related thoughts occurring outside of these circumscribed periods.1 Diagnostic criteria, as suggested by Moroze et al,5 are shown in Table 1.
Table 1.
Orthorexia nervosa diagnostic criteria proposed by Moroze et al5
| Criterion A: Obsessional preoccupation with eating “healthy foods,” focusing on concerns regarding the quality and composition of meals. (Two or more of the following.) |
| • Consuming a nutritionally unbalanced diet owing to preoccupying beliefs about food “purity.” |
| • Preoccupation and worries about eating impure or unhealthy foods and of the effect of food quality and composition on physical or emotional health or both. |
| • Rigid avoidance of foods believed by the patient to be “unhealthy,” which may include foods containing any fat, preservatives, food additives, animal products, or other ingredients considered by the subject to be unhealthy. |
| • For individuals who are not food professionals, excessive amounts of time (eg., 3 or more hours per day) spent reading about, acquiring, and preparing specific types of foods based on their perceived quality and composition. |
| • Guilty feelings and worries after transgressions in which “unhealthy” or “impure” foods are consumed. |
| • Intolerance to other’s food beliefs. |
| • Spending excessive amounts of money relative to one’s income on foods because of their perceived quality and composition. |
| Criterion B: The obsessional preoccupation becomes impairing by either of the following: |
| • Impairment of physical health owing to nutritional imbalances (eg., developing malnutrition because of an unbalanced diet). |
| • Severe distress or impairment of social, academic, or vocational functioning owing to obsessional thoughts and behaviors focusing on patient’s beliefs about “healthy” eating. |
| Criterion C: The disturbance is not merely an exacerbation of the symptoms of another disorder such as obsessive-compulsive disorder or of schizophrenia or another psychotic disorder. |
| Criterion D: The behavior is not better accounted for by the exclusive observation of organized orthodox religious food observance or when concerns with specialized food requirements are in relation to professionally diagnosed food allergies or medical conditions requiring a special diet. |
Notes: Reprinted from Psychosomatics, Moroze RM, Dunn TM, Craig Holland J, et al, Microthinking about micronutrients: a case of transition from obsessions about healthy eating to near-fatal “orthorexia nervosa” and proposed diagnostic criteria, In press March 19, 2014, with permission from Elsevier.5
With regard to the consequences of this extreme style of eating, orthorexic individuals may experience nutritional deficiencies due to omission of entire food groups,6 and, although long-term empirical studies are lacking, there is anecdotal evidence that this kind of dietary extremism can lead to the same medical complications that one sees with severe anorexia: osteopenia, anemia, hyponatremia, metabolic acidosis, pancytopenia, testosterone deficiency, and bradycardia.1,5,7 Psychologically, orthorexic individuals experience intense frustration when their food-related practices are disrupted or thwarted, disgust when food purity is seemingly compromised, and guilt and self-loathing when they commit food transgressions,8 all of which is superimposed on chronic worry about imperfection and nonoptimal health. Indeed, dietary violations may prompt a desire for self-punishment, manifested by an even stricter diet, or purification via supposedly cleansing fasts.1 Moreover, orthorexic individuals are at risk for social isolation, as they may believe that they can only maintain healthy eating while alone and in control of one’s surroundings and may adopt a stance of moral superiority about their food habits such that they do not wish to interact with others who are unlike them.8
Diagnostic boundaries
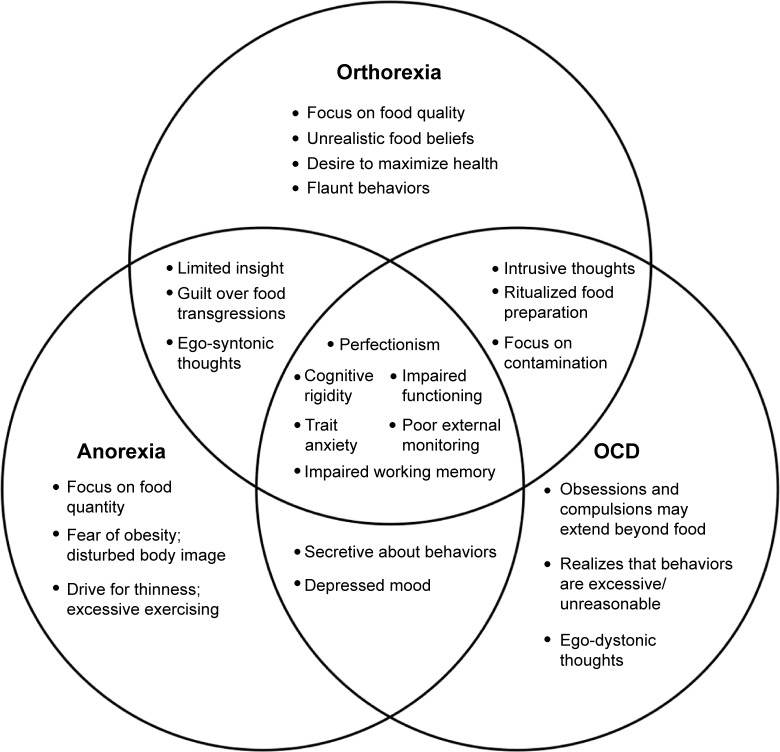
Many of the features described above echo symptoms of anorexia nervosa and obsessive–compulsive disorder (OCD), conditions that are themselves highly comorbid and have functionally similar clinical presentations,9 prompting debate as to whether orthorexia is a unique disorder or a subset of anorexia or OCD (Figure 1). Orthorexia and anorexia share common traits of perfectionism, high trait anxiety, and a high need to exert control,10 in addition to the potential for significant weight loss.4 Both orthorexic and anorexic individuals are achievement-oriented, valuing adherence to their diet as a marker of self-discipline and construing deviation from the diet as a failure of self-control. Both have limited insight into their condition and often deny the functional impairments associated with their disorder.1 With regard to overlap with OCD, orthorexic individuals manifest certain obsessive– compulsive tendencies: recurrent, intrusive thoughts about food and health at inappropriate times, inflated concern over contamination and impurity, and a strong need to arrange food and eat in a ritualized manner.1,11 Similar to those with OCD, orthorexic individuals have limited time for other activities, as adherence to a strict eating style interferes with normal routines.4
Figure 1.
Venn diagram showing unique and overlapping features of orthorexia nervosa, anorexia nervosa, and obsessive–compulsive disorder (OCD).
Yet, there are notable points of departure between orthorexia and these other conditions as well. The most significant difference between orthorexia and anorexia is the motivation for disordered eating. In anorexia, individuals are preoccupied with body image and fear of obesity, altering their eating patterns in order to lose weight. In orthorexia, individuals adopt eating habits given a desire to be healthy, natural, or pure,1,12 entertaining unrealistic, if not magical, beliefs about certain foods.13 Anorexic individuals tend to hide their behaviors, whereas orthorexic individuals are more likely to flaunt their habits.1 With regard to OCD, the most significant difference is that the content of obsessions in orthorexia is perceived as ego-syntonic, rather than ego-dystonic.8
Beyond these two disorders, orthorexia shares overlapping features with several other diagnostic categories, including obsessive–compulsive personality disorder (OCPD). Within the OCPD syndrome, which itself belongs to the cluster of personality disorders characterized by fear and behavioral inhibition,14 notable similarities to orthorexia include perfectionism, rigid thinking, excessive devotion, hypermorality, and a preoccupation with details and perceived rules. While no studies to date have examined the rates of co-occurrence between OCPD and orthorexia, the comorbidity between OCPD and OCD and between OCPD and eating disorders has been extensively studied. Data concerning the former are mixed, with some studies suggesting a low degree of association between OCPD and OCD15,16 and others indicating significant and specific associations.17,18 Concerning the latter relationship, there is some evidence that OCPD, rather than OCD, has a close link with eating disorders,19 particularly to anorexia.20 Other research has shown that the presence of OCPD traits positively predicts development of pathological eating habits.21,22
Features of orthorexia may also bear resemblance to health-related anxiety seen in the somatoform disorders. Although the 5th edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5)23 introduced significant changes to the nomenclature and scope of the somatoform conditions relative to the DSM-IV-TR edition, the potential relevance of orthorexia to these conditions, namely somatic symptom disorder and illness anxiety disorder, is noteworthy. With the former, individuals experience one or more chronic somatic symptoms – whether or not medically unexplainable – about which they are excessively preoccupied or fearful, prompting frequent use of traditional and sometimes nontraditional health care services. With the latter, individuals experience heightened bodily sensations and are intensely anxious about the possibility of an undiagnosed illness, often devoting excessive time and energy to these health concerns. In each condition, the preoccupation with illness might engender a secondary preoccupation with food and diet as a route by which to combat real or perceived illness; in this scenario, an individual would be most likely to turn toward compensatory dietary management upon dissatisfaction with the traditional medical establishment or upon specific advice from health care professionals to manage illness with diet. While there are no empirical studies to date that specifically describe orthorexia as an associated feature of these somatoform conditions, health anxiety is known to be positively correlated with food and diet preoccupation,24 and there is evidence that health anxiety prompts significant, problematic changes in eating patterns.25
Lastly, although robust empirical data are lacking on this topic, there remains the possibility that orthorexia can signal more severe psychopathology in the form of a psychotic spectrum condition. To date, there is one case study of an adult woman whose orthorexic eating habits represented the prodromal phase of schizophrenia.26 While the comorbidity of schizophrenia and eating disorders is generally estimated to be low,27 the numerous case reports of anorexia preceding first episode psychosis have prompted theories that a) the obsessional features of anorexia have the potential to devolve into more precise delusions over time and that b) nutritional deficiency from food restriction may itself trigger psychosis. As orthorexia is a recently-documented construct, prospective analysis is needed to determine the extent to which orthorexia elevates the risk for subsequent development of schizophrenia, delusional disorder, and related conditions. At a theoretical level, the feature of orthorexia of greatest relevance to the psychosis spectrum is food-related magical thinking (Table 2), erroneous beliefs that are based on intuitive laws of contagion (ie, the notion that objects that have been in real or imagined contact continue to influence each other over time or space) or similarity (ie, the notion that superficial resemblances between objects or concepts are actually deeply meaningful).13,28 Regardless of whether their origin is culturally or religiously accepted, magical beliefs about food are of medical concern when food exclusion and food refusal lead to severe nutritional deficiency.29 From a psychiatric perspective, elevated magical ideation, regardless of its content, is a common symptom of schizotypal personality disorder and a good predictor of future psychosis.30
Table 2.
Examples of erroneous food beliefs associated with certain food movements
| • Approximately 70% of our food should be high in water content since our bodies are 70% water (living water diet) |
| • Chewing food too quickly impedes stomach digestion of proteins and the absorption of amino acids (raw foodism) |
| • Eating yellow food focuses one’s energy on productive activities and strengthens the spiritual center (chakra-focused eating) |
| • Eating unprocessed plant-based food increases one’s spiritual frequency and helps one connect to the divine (veganism) |
| • Eating fruit on an empty stomach 30–60 minutes before a meal primes the stomach for nutrition absorption (trophology) |
| • Eating food associated with one’s blood type prevents disease and enhances energy and well-being (blood type diet) |
| • To avoid bodily degeneration and illness, no more than 30% of the diet should consist of acidic foods (alkaline diet) |
| • Eating at the wrong time of day disturbs the autonomic nervous system, hindering one’s ability to manage stress (warrior diet) |
Epidemiology and assessment
Data concerning the epidemiology of orthorexia, like that of any other condition, are shaped by the sensitivity and specificity of assessment instruments. The fact that there are no thoroughly vetted measures of orthorexia with clear psychometric properties makes it difficult to obtain trustworthy estimates of its prevalence. In their original treatise on orthorexia, Bratman and Knight1 proposed a simple 10-item dichotomous rating scale by which to assess orthorexia, but this measure has not received much traction in the literature. Instead, researchers have relied primarily on a modification of this scale called the ORTO-1531 and, to a lesser degree, the ORTO-1110 and ORTO-11-Hu32 to measure the prevalence of orthorexia in various populations.3,6,32 There is debate, however, as to the reliability and validity of these measures.
The ORTO-15 is a 15-item measure that assesses beliefs about the perceived effects of eating healthy food (eg, “Do you think that consuming healthy food may improve your appearance?”), attitudes governing food selection (eg, “Are your eating choices conditioned by your worry about your health status?”), habits of food consumption (eg, “At present, are you alone when having meals?”), and the extent to which food concerns influence daily life (eg, “Does the thought about food worry you for more than 3 hours a day?”).31 Responses are scored on a 4-point scale and totaled, with scores below 40 considered indicative of orthorexia and higher scores purportedly reflecting normal eating behavior. With regard to its psychometric properties, Donini et al31 report sensitivity, specificity, and predictive validity values for the ORTO-15 using this threshold in an Italian adult sample. However, the lack of established diagnostic criteria makes it difficult to gauge the appropriateness of any self-report measure, as epidemiological research is predicated on the existence of a gold standard approach for ascertaining true from false positives and true from false negatives. Beyond this, the ORTO-15 has been criticized for potentially problematic internal consistency. In four different samples of American undergraduate students, reported Cronbach’s alpha coefficients have ranged from an unacceptable low of 0.1433 to respectable highs above 0.70.34–36 While this one instance of poor overall internal consistency may represent an isolated methodological design flaw, it is also worth noting that low internal reliability may signal an orthogonal multifactorial latent structure. Indeed, factor analytic work on the ORTO-15 has suggested both two-33,37 and three-factor31,38 solutions. However, in these studies, these factors did not collectively explain a large proportion of the variance observed across the ORTO-15 items.
Some researchers have eliminated items from the ORTO-15 in an effort to strengthen its reliability and validity. For example, when adapting the ORTO-15 for use in a Hungarian population, Varga et al32 eliminated four items from the measure to improve its consistency, resulting in the ORTO-11-Hu. Although more research is needed, the ORTO-11-Hu appears to have good internal reliability (Cronbach’s α =0.82) when used in a Hungarian population. Similarly, Arusoğlu et al39 eliminated four items from the ORTO-15 for use in a Turkish population, achieving an 11-item version with an internal validity coefficient of 0.62. Notably, the items eliminated from the ORTO-15 for the Hungarian adaptation were different from the items eliminated for the Turkish adaptation. While it is possible, as Varga et al32 suggest, that cultural differences account for contradictory internal consistency values across samples, it is also possible that the ORTO-15 is simply not a reliable measure of orthorexia.
Another serious point of concern regarding the ORTO-15 is the fact that it does not account for the obsessive–compulsive symptoms that people with orthorexia experience, such as intrusive food related thoughts, concerns with contamination and impurity, and the tendency to eat in a ritualized manner. This flaw prompted the researchers who developed the ORTO-15 to only label a study participant as orthorexic if the participant exhibited both “health fanatic behavior” (as determined by ORTO-15 score) and an “altered MMPI”.31 Participants who met this latter criterion were men who scored less than 66 and women who scored less than 65 on Scale 7 of the Minnesota Multiphasic Personality Inventory, which accounts for obsessive behavior.31 Yet in various other studies,3,6,32,34 researchers have used the ORTO-15 as the sole measure of orthorexia, raising concerns about the accuracy of their results.
Based on the flaws in the ORTO-15 as well as the many differences across orthorexia studies in terms of methodology and sample characteristics, a clear picture of the prevalence of orthorexia has yet to emerge. Existing estimates of orthorexia range from 6.9%4 to 57.6%12 in the general population, with rates as high as 81.8% in specific populations.3 Furthermore, it is unclear whether orthorexia is more prevalent among women or men. Some studies12,34 report that the rates of orthorexia are higher in women than men, whereas other studies report the reverse pattern.4,10 Yet other studies report comparable rates across the sexes.6,33 Similar contradictions exist regarding the prevalence of orthorexia based on age,4,10,12,32,33 education level,3,4,12,33 body mass index,3,4,10,32,33 smoking status,3,10,32,33 and alcohol consumption.3,32,33 Additional epidemiology research is needed in conjunction with improvements in the psychometrics of orthorexia measures. Psychometric problems aside, it may be the case that individuals who are focused on nutrition and health for one’s career or leisure activities – such as those involved in healthcare,6,10,11,32,40 the performing arts,3 and athletics41 – may be at an elevated risk for developing orthorexia. Given that these individuals are likely to be particularly sensitive to issues surrounding health and nutrition,6 may feel pressure to be role models for health,3 and might have tendencies toward perfectionism, it is important to continue to examine the prevalence of orthorexia within these particular populations.
Overall, the methodological issues concerning the existing scales have not gone unnoticed, and researchers have taken preliminary steps to develop a new measure, the Eating Habits Questionnaire (EHQ), to identify individuals with behaviors, cognitions, and feelings that may indicate a problematic fixation on healthy eating.40 The EHQ is a 21-item measure that contains three subscales that measure knowledge of healthy eating (eg, “I know more about healthy eating than do other people”), problems associated with healthy eating (eg, “I spend more than 3 hours a day thinking about healthy food”), and feelings associated with healthy eating (eg, “I feel control when I eat healthily”); initial analyses suggest good convergent and divergent validity in that the EHQ subscales correlated strongly with measures of maladaptive eating behaviors and attitudes rather than with measures of personality, social desirability, and general psychopathology. Preliminary evidence suggests that the EHQ is reliable, with the three subscales showing strong internal consistency (Cronbach’s α =0.82, 0.90, and 0.86, respectively).40 While the psychometric properties appear promising, it should be noted that the EHQ is not necessarily a comprehensive measure of orthorexia symptoms. Although certain items do probe the obsessive nature of food-related cognitions, there is no assessment of compulsive behaviors that one might expect in the syndrome.
Neuropsychological profile
To date, most of the research concerning orthorexia has focused on the emotional and physical sequelae of the condition rather than on the underlying brain–behavior relationships. One study,34 however, used standardized clinical neuropsychological assessment to characterize the cognitive profile of orthorexia, targeting the cognitive domains known to be affected in anorexia and OCD, including attention, verbal long-term memory, visuospatial functioning, and executive functioning,42–45 as candidate areas of inquiry. Using a nonclinical sample of undergraduate students, highly orthorexic participants (defined as those scoring <40 on the ORTO-15) performed worse in domains of set-shifting, external attention, and working memory (WM) relative to nonorthorexic participants, even after controlling for scores on measures of anorexia and OCD. In effect, orthorexia was independently associated with key facets of executive dysfunction for which anorexia and OCD profiles already overlap.
Set-shifting involves flexible problem-solving and the ability to move freely from one situation or set of thoughts to another as needed. Impoverished set-shifting, or cognitive rigidity, might readily explain the inflexible, rule-bound approach that orthorexic individuals take toward food selection, preparation, and consumption.34 Indeed, an unfortunate positive feedback loop might develop such that one’s exposure to varied, stimulating daily activities declines in order to fulfill time-intensive and complex food rules, prompting yet further decline in set-shifting skills from lack of applicative practice.34 Cognitive inflexibility is also a hallmark feature of anorexia46 and OCD.47
External attention refers to the ability to focus on the external environment, including awareness of one’s social impact on other people. As many orthorexic behaviors signal an extreme focus on the self, specifically on obtaining bodily health and/or purity, and given evidence that focusing attention inward is associated with impaired processing of external cues,48 it is not surprising for orthorexic individuals to have difficulty with external attention.34 Reviews of the clinical literature suggest that individuals with psychological disorders generally exhibit excessive self-focused attention and that this pattern produces additional dysfunctional effects, such as intensification of emotional states, reduction in effortful coping, and impairment in task performance.49,50 For example, anorexic individuals seem to privilege inward perceptual, cognitive, and emotional information as opposed to external information51 and, furthermore, demonstrate impaired external sustained attention.52 Similarly, individuals with OCD exhibit increased awareness of and monitoring of their thoughts53 as well as heightened self-preoccupation and rumination.54 Recent neuroimaging data55 provide evidence of disrupted functional connectivity in OCD between large-scale brain networks supporting internal and external attention, potentially explaining the difficulty among individuals with OCD to disengage from internally-generated thoughts when performing tasks requiring external attention. Similar neuroimaging studies are needed to determine if orthorexic individuals exhibit analogous patterns.
As a construct, WM refers to the ability to hold information online for brief periods of time in the service of another task. As a finite and depletable set of resources, WM operations can be easily disrupted by attention to task-irrelevant stimuli, whether internal or external;56 it is possible, for example, that ongoing preoccupation with food- and health-related images or thoughts weakens WM in orthorexia,34 as similar findings have been reported in the eating disorders literature. Evidence suggests that food-related thoughts reduce WM capacity in dieters,57 and dysfunction has been reported in anorexic patients particularly in the visuospatial sketch pad and central executive components of WM.58 With regard to OCD, there is meta-analytic evidence59 to implicate WM as the link between executive dysfunction and long-term memory impairment such that repetitive, intrusive thoughts interfere with episodic binding during WM. As WM is a multifaceted cognitive domain, future research on orthorexia should attempt to dissociate the executive (eg, cognitive control) from nonexecutive (eg, storage) elements in order to provide a more nuanced analysis of WM dysfunction and to help disambiguate the brain pathways that underlie the dysfunction.
Beyond this one exploratory neuropsychological investigation of orthorexia, there is no published research on the genetic, neuroanatomical, neurochemical, or psychophysiological correlates of the orthorexic syndrome. Given the theoretical overlap with anorexia and OCD, we might look to the literature concerning the neuropathophysiology of these latter conditions to outline logical starting points for this kind of research. Furthermore, additional mapping of the behavioral and cognitive endophenotypes in orthorexia with experimental neuropsychological methodologies will provide useful clues about proximal biological contributors, in essence providing a “top-down deconstruction”60 of outwardly complex behavior to simpler component processes. Intermediate endophenotypes may provide better insight into underlying etiology than can symptom-level clinical categories61 which, given the perplexities surrounding the differential diagnosis of orthorexia, will be advantageous for advancing our understanding of orthorexia more quickly. In other words, we might be better served to shift our research focus away from achieving precise categorical boundaries among orthorexia and related conditions to, instead, continuing to characterize the dimensional endophenotypes that best explain the orthorexic phenomenon, recognizing that such dimensions will likely be transdiagnostic in nature. A deeper appreciation of these endophenotypes may generate ideas for novel approaches to both the prevention and treatment of orthorexia and its diagnostic cousins.
Treatment and management
To date, there are no studies of treatment effectiveness for orthorexia, although suggestions for best practices have been offered. The ideal intervention involves a multidisciplinary team that includes physicians, psychotherapists, and dieticians62,63 such that a combination of medication, cognitive-behavioral therapy, and psychoeducation8 can be applied with close monitoring in outpatient settings. In cases of significant weight loss and malnourishment, an inpatient setting with physicians experienced in refeeding syndrome5 would be indicated.
With regard to psychotropic medication, serotonin reuptake inhibitors are reportedly helpful for orthorexia,8 which makes sense given evidence of their efficacy for both anorexia and OCD.64 Others have successfully used antipsychotics such as olanzapine to decrease the obsessive nature of magical food-related thinking.5 It should be noted, however, that orthorexic individuals may be apt to reject pharmaceuticals as “non-natural” substances.8 When considering psychotherapy, interventions should be individualized based on the symptoms that are prominent for a given patient,39 recognizing that treatment goals should focus not only on what patients eat but also on how they shop for, prepare, and feel about the food they consume.63 Exposure and response prevention, potentially in conjunction with habit reversal training,65 may be most successful for treating obsessive and compulsive aspects of orthorexia. Cognitive restructuring is likely to be beneficial for dichotomous thinking, overgeneralization, catastrophization, and other cognitive distortions surrounding food, eating, and health66 as well as associated problematic traits such as perfectionism. Various forms of relaxation training may assist with pre- and postprandial anxiety67 and other manifestations of health anxiety.68,69 Moreover, behavior modification strategies may be useful to expand one’s food repertoire, increase socialization during meals, and diversify leisure activities to include nonfood themes. Lastly, psychoeducation about empirically-validated dietetic science may help disabuse orthorexic patients of false food beliefs.62 However, research indicates that nutrition and health education, while obviously needing to contain objective concepts about nutrients and physiology, should also recognize the deeply emotional aspects of food beliefs and food choices so as to incorporate affective approaches to patient counseling.28 Asking severely orthorexic patients to abandon false food beliefs is really a request to discard a deeply held ideology; as discussed by Lindeman et al,13 ideologies, whether comprised of reality-grounded or magical beliefs, provide structure and order to one’s life, reducing anxiety by providing a means to exert control over the environment. Psychoeducation, to the extent that it challenges an entrenched belief system, should be undertaken with an appreciation of its potential for significant emotional upheaval in the patient.
Conclusion
Unchecked by any scientific regulatory process, the sharp rise in healthy lifestyle-related propaganda through book, magazine, and electronic formats, further bolstered by a rapid exchange of ideas through social media, means that the average individual is regularly bombarded by advice and admonitions about diet and health. Despite the great potential for misinformation, those who utilize the Internet, for example, to search for health-related information tend not to attend to the validity or recency of the source and often misjudge the trustworthiness of the information.70 For those already predisposed to health anxiety, research indicates that searching online for health information exacerbates this anxiety, a phenomenon dubbed “cyberchondria”.71 As orthorexia presents as a cluster of symptoms that is almost a parody of trends in popular culture toward healthy living, it is difficult to pinpoint when concern over the healthfulness and integrity of one’s diet reaches pathological proportions.63 Yet, in a recent survey of psychologists, psychiatrists, nurses, and social workers, two-thirds reported having observed patients in their practice presenting with clinically significant orthorexia; importantly, two-thirds of clinicians also indicated that the syndrome deserves more scientific attention.2
With the acknowledgment that further research into orthorexia may serve to reify a culturally-constructed condition,72 the information reviewed in the preceding sections leaves us with more questions than firm answers (Table 3). Proper diagnostic recognition, as begun by Moroze et al,5 is a precursory step toward the creation of gold standard assessment instruments needed for appropriate identification of orthorexic individuals,63 and with that will come advances in our understanding of etiology, treatment, and prevention.
Table 3.
Questions for future research
| • What additional comorbidities beyond anorexia and obsessive–compulsive disorder (OCD) are common in orthorexia and complicate treatment? |
| • How can existing orthorexia scales be modified to improve their psychometric properties? What additional measures should be used in conjunction with orthorexia scales for a comprehensive view of patient pathology? |
| • What cultural factors might explain the differences in prevalence rates across geographic regions? |
| • Are there meaningful subtypes of orthorexia, each with its unique set of external correlates? |
| • Are the cognitive weaknesses associated with orthorexia precursory, developmental risk factors or secondary sequelae? |
| • Which behavioral endophenotypes explain the greatest percentage of variance in orthorexic symptoms? |
| • What is the neuropathogenesis of orthorexia, and how can knowledge about the associated genetics, anatomy, chemistry, and physiology be applied to prevention and management practices? |
| • What is the effectiveness of various psychotherapy techniques for orthorexia? How can assessment be used to optimize treatment? |
Footnotes
Disclosure
The authors report no conflicts of interest in this work.
References
- 1.Bratman S, Knight D. Health Food Junkies: Orthorexia Nervosa– Overcoming the Obsession With Healthful Eating. New York, NY: Broadway; 2000. [Google Scholar]
- 2.Vandereycken W. Media hype, diagnostic fad, or genuine disorder? Professionals’ opinions about night eating syndrome, orthorexia, muscle dysmorphia, and emetophobia. Eat Disord. 2011;19(2):145–155. doi: 10.1080/10640266.2011.551634. [DOI] [PubMed] [Google Scholar]
- 3.Aksoydan E, Camci N. Prevalence of orthorexia nervosa among Turkish performance artists. Eat Weight Disord. 2009;14(1):33–37. doi: 10.1007/BF03327792. [DOI] [PubMed] [Google Scholar]
- 4.Donini LM, Marsili D, Graziani MP, et al. Orthorexia nervosa: a preliminary study with a proposal for diagnosis and an attempt to measure the dimension of the phenomenon. Eat Weight Disord. 2004;9(2):151–157. doi: 10.1007/BF03325060. [DOI] [PubMed] [Google Scholar]
- 5.Moroze RM, Dunn TM, Craig Holland J, et al. Microthinking about micronutrients: a case of transition from obsessions about healthy eating to near-fatal “orthorexia nervosa” and proposed diagnostic criteria. Psychosomatics. 2014 Mar 19; doi: 10.1016/j.psym.2014.03.003. Epub. [DOI] [PubMed] [Google Scholar]
- 6.Bosi ATB, Çamur D, Güler Ç. Prevalence of orthorexia nervosa in resident medical doctors in the faculty of medicine. Appetite. 2007;49(3):661–666. doi: 10.1016/j.appet.2007.04.007. [DOI] [PubMed] [Google Scholar]
- 7.Park SW, Kim JY, Go GJ, et al. Orthorexia nervosa with hyponatremia, subcutaneous emphysema, pneumomediastimum, pneumothorax, and pancytopenia. Electrolyte Blood Press. 2011;9(1):32–37. doi: 10.5049/EBP.2011.9.1.32. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Mathieu J. What is orthorexia? J Am Diet Assoc. 2005;105(10):1510–1512. doi: 10.1016/j.jada.2005.08.021. [DOI] [PubMed] [Google Scholar]
- 9.Altman SE, Shankman SA. What is the association between obsessive–compulsive disorder and eating disorders? Clin Psychol Rev. 2009;29(7):638–646. doi: 10.1016/j.cpr.2009.08.001. [DOI] [PubMed] [Google Scholar]
- 10.Fidan T, Ertekin V, Işikay S, et al. Prevalence of orthorexia among medical students in Erzurum, Turkey. Compr Psychiatry. 2010;51(1):49–54. doi: 10.1016/j.comppsych.2009.03.001. [DOI] [PubMed] [Google Scholar]
- 11.Kinzl JF, Hauer K, Traweger C, et al. Orthorexia nervosa in dieticians. Psychother Psychosom. 2006;75(6):395–396. doi: 10.1159/000095447. [DOI] [PubMed] [Google Scholar]
- 12.Ramacciotti CE, Perrone P, Coli E, et al. Orthorexia nervosa in the general population: a preliminary screening using a self-administered questionnaire (ORTO-15) Eat Weight Disord. 2011;16(2):e127–e130. doi: 10.1007/BF03325318. [DOI] [PubMed] [Google Scholar]
- 13.Lindeman M, Keskivaara P, Roschier M. Assessment of magical beliefs about food and health. J Health Psychol. 2000;5(2):195–209. doi: 10.1177/135910530000500210. [DOI] [PubMed] [Google Scholar]
- 14.Emmelkamp PMG, Kamphius JH. Personality Disorders. London, UK: Taylor & Francis; 2007. [Google Scholar]
- 15.Mancebo M, Eisen J, Grant J, et al. Obsessive compulsive personality disorder and obsessive compulsive disorder: clinical characteristics, diagnostic difficulties, and treatment. Ann Clin Psychiatry. 2005;17(4):197–204. doi: 10.1080/10401230500295305. [DOI] [PubMed] [Google Scholar]
- 16.Wu KD, Clark LA, Watson D. Relations between obsessive-compulsive disorder and personality: beyond Axis I-Axis II comorbidity. J Anxiety Disord. 2006;20(6):695–717. doi: 10.1016/j.janxdis.2005.11.001. [DOI] [PubMed] [Google Scholar]
- 17.Gordon OM, Salkovskis PM, Oldfield VB, et al. The association between obsessive compulsive disorder and obsessive compulsive personality disorder: prevalence and clinical presentation. Br J Clin Psychol. 2013;52(3):300–315. doi: 10.1111/bjc.12016. [DOI] [PubMed] [Google Scholar]
- 18.Starcevic V, Berle D, Brakoulias V, et al. Obsessive–compulsive personality disorder co-occurring with obsessive-compulsive disorder: conceptual and clinical implications. Aust N Z J Psychiatry. 2013;47(1):65–73. doi: 10.1177/0004867412450645. [DOI] [PubMed] [Google Scholar]
- 19.Halmi KA, Tozzi F, Thornton LM, et al. The relation among perfectionism, obsessive-compulsive personality disorder, and obsessive-compulsive disorder in individuals with eating disorders. Int J Eat Disord. 2005;38(4):371–374. doi: 10.1002/eat.20190. [DOI] [PubMed] [Google Scholar]
- 20.Serpell L, Livingstone A, Neiderman M, et al. Anorexia nervosa: obsessive-compulsive disorder, obsessive-compulsive personality disorder, or neither? Clin Psychol Rev. 2002;22(5):647–669. doi: 10.1016/s0272-7358(01)00112-x. [DOI] [PubMed] [Google Scholar]
- 21.Lilenfeld LRR, Jacobs CH, Woods AM, et al. A prospective study of obsessive-compulsive and borderline personality traits, race, and disordered eating. Eur Eat Disord Rev. 2008;16(2):124–132. doi: 10.1002/erv.842. [DOI] [PubMed] [Google Scholar]
- 22.Anderluh MB, Tchanturia K, Rabe-Hesketh S, et al. Childhood obsessive-compulsive personality traits in adult women with eating disorders: defining a broader eating disorder phenotype. Am J Psychiatry. 2003;160(2):242–247. doi: 10.1176/appi.ajp.160.2.242. [DOI] [PubMed] [Google Scholar]
- 23.American Psychiatric Association . Diagnostic and statistical manual of mental disorders. 5th ed. Arlington, VA: American Psychiatric Publishing; 2013. [Google Scholar]
- 24.Hadjistavropoulos H, Lawrence B. Does anxiety about health influence eating patterns and shape-related body checking among females? Pers Individ Dif. 2007;43(2):319–328. [Google Scholar]
- 25.Quick VM, McWilliams R, Byrd-Bredbenner C. Case–control study of disturbed eating behaviors and related psychographic characteristics in young adults with and without diet-related chronic health conditions. Eat Behav. 2012;13(3):207–213. doi: 10.1016/j.eatbeh.2012.02.003. [DOI] [PubMed] [Google Scholar]
- 26.Saddichha S, Babu GN, Chandra P. Orthorexia nervosa presenting as prodrome of schizophrenia. Schizophr Res. 2012;134(1):110. doi: 10.1016/j.schres.2011.10.017. [DOI] [PubMed] [Google Scholar]
- 27.Miotto P, Pollini B, Restaneo A, et al. Symptoms of psychosis in anorexia and bulimia nervosa. Psychiatry Res. 2010;175(3):237–243. doi: 10.1016/j.psychres.2009.03.011. [DOI] [PubMed] [Google Scholar]
- 28.Aarnio K, Lindeman M. Magical food and health beliefs: a portrait of believers and functions of the beliefs. Appetite. 2004;43(1):65–74. doi: 10.1016/j.appet.2004.03.002. [DOI] [PubMed] [Google Scholar]
- 29.Geddavalasa L. Food preferences and taboos during antenatal period among the tribal women of north coastal Andhra Pradesh. J Community Nutr Health. 2013;2(2):32–37. [Google Scholar]
- 30.Gooding DC, Tallent KA, Matts CW. Clinical status of at-risk individuals 5 years later: Further validation of the psychometric high-risk strategy. J Abnorm Psychol. 2005;114(1):170–175. doi: 10.1037/0021-843X.114.1.170. [DOI] [PubMed] [Google Scholar]
- 31.Donini LM, Marsili D, Graziani MP, et al. Orthorexia nervosa: validation of a diagnosis questionnaire. Eat Weight Disord. 2005;10(2):e28–e32. doi: 10.1007/BF03327537. [DOI] [PubMed] [Google Scholar]
- 32.Varga M, Thege BK, Dukay-Szabó S, et al. When eating healthy is not healthy: Orthorexia nervosa and its measurement with the ORTO-15 in Hungary. BMC Psychiatry. 2014;14:59. doi: 10.1186/1471-244X-14-59. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.McInerney-Ernst EM. Orthorexia Nervosa: Real Construct or Newest Social Trend? USA: ProQuest Information & Learning; 2012. [Accessed December 15, 2014]. Available from: http://hdl.handle.net/10355/11200. [Google Scholar]
- 34.Koven NS, Senbonmatsu R. A neuropsychological evaluation of orthorexia nervosa. Open J Psychiatry. 2013;3:214–222. [Google Scholar]
- 35.Lewis D. Understanding Prevalence and Attitudes: Dietary and Exercise Behaviors Among African American Collegiate Athletes [dissertation] USA: ProQuest Information & Learning; 2013. [Accessed December 15, 2014]. Available from: http://gradworks.umi.com/35/40/3540007.html. [Google Scholar]
- 36.Meister SE. The Occurrence of Highly Sensitive Attitudes and Behaviors Toward Eating Among Undergraduate Students at A Midwestern University [thesis] USA: ProQuest Information & Learning; 2010. [Accessed December 15, 2014]. Available from: http://gradworks.umi.com/14/80/1480729.html. [Google Scholar]
- 37.Brytek-Matera A, Krupa M, Poggiogalle E, et al. Adaptation of the ORTHO-15 test to Polish women and men. Eat Weight Disord. 2014;19(1):69–76. doi: 10.1007/s40519-014-0100-0. [DOI] [PubMed] [Google Scholar]
- 38.Alvarenga MS, Martins MCT, Sato KSCJ, et al. Orthorexia nervosa behavior in a sample of Brazilian dietitians assessed by the Portuguese version of ORTO-15. Eat Weight Disord. 2012;17(1):e29–e35. doi: 10.1007/BF03325325. [DOI] [PubMed] [Google Scholar]
- 39.Arusoğlu G, Kabakçi E, Köksal G, et al. Ortoreksiya Nervoza ve Orto-11’in Türkçeye Uyarlama Çalış ması [Orthorexia nervosa and adaptation of ORTO-11 into Turkish] Türk Psikiyatri Dergisi. 2008;19(3):283–291. Turkish. [PubMed] [Google Scholar]
- 40.Gleaves DH, Graham EC, Ambwani S. Measuring “orthorexia”: development of the Eating Habits Questionnaire. Int J Educ Psychol Assess. 2013;12(2):1–18. [Google Scholar]
- 41.Segura-García C, Papaianni MC, Caglioti F, et al. Orthorexia nervosa: a frequent eating disordered behavior in athletes. Eat Weight Disord. 2012;17(4):e223–e233. doi: 10.3275/8272. [DOI] [PubMed] [Google Scholar]
- 42.Kingston K, Szmukler G, Andrewes D, et al. Neuropsychological and structural brain changes in anorexia nervosa before and after refeeding. Psychol Med. 1996;26(1):15–28. doi: 10.1017/s0033291700033687. [DOI] [PubMed] [Google Scholar]
- 43.Steinglass JE, Walsh BT, Stern Y. Set shifting deficit in anorexia nervosa. J Int Neuropsychol Soc. 2006;12(3):431–435. doi: 10.1017/s1355617706060528. [DOI] [PubMed] [Google Scholar]
- 44.Fontenelle LF, Mendlowicz MV, Mattos P, et al. Neuropsychological findings in obsessive-compulsive disorder and its potential implications for treatment. Curr Psychiatry Rev. 2006;2(1):11–26. [Google Scholar]
- 45.Chamberlain SR, Blackwell AD, Fineberg NA, et al. The neuropsychology of obsessive compulsive disorder: the importance of failures in cognitive and behavioural inhibition as candidate endophenotypic markers. Neurosci Biobehav Rev. 2005;29(3):399–419. doi: 10.1016/j.neubiorev.2004.11.006. [DOI] [PubMed] [Google Scholar]
- 46.Abbate-Dage G, Buzzichelli S, Amianto F, et al. Cognitive flexibility in verbal and nonverbal domains and decision making in anorexia nervosa patients: a pilot study. BMC Psychiatry. 2011;11(1):162–169. doi: 10.1186/1471-244X-11-162. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Gu B-M, Park J-Y, Kang D-H, et al. Neural correlates of cognitive inflexibility during task-switching in obsessive-compulsive disorder. Brain. 2008;131(1):155–164. doi: 10.1093/brain/awm277. [DOI] [PubMed] [Google Scholar]
- 48.Clark DM. A cognitive perspective on social phobia. In: Crozier WR, Alden LE, editors. The Essential Handbook of Social Anxiety for Clinicians. New York, NY: John Wiley & Sons; 2005. pp. 193–218. [Google Scholar]
- 49.Ingram RE. Self-focused attention in clinical disorders: review and a conceptual model. Psychol Bull. 1990;107(2):156–176. doi: 10.1037/0033-2909.107.2.156. [DOI] [PubMed] [Google Scholar]
- 50.Wells A, Matthews G. Attention and Emotion: A Clinical Perspective. Hillsdale, NJ: Lawrence Erlbaum Associates; 1994. [Google Scholar]
- 51.Zucker N, Wagner HR, Merwin R, et al. Self-focused attention in anorexia nervosa. Int J Eat Disord. 2014 Jun 5; doi: 10.1002/eat.22307. Epub. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Fowler L, Blackwell A, Jaffa A, et al. Profile of neurocognitive impairments associated with female in-patients with anorexia nervosa. Psychol Med. 2006;36(4):517–527. doi: 10.1017/S0033291705006379. [DOI] [PubMed] [Google Scholar]
- 53.Kikul J, Van Allen TS, Exner C. Underlying mechanisms of verbal memory deficits in obsessive-compulsive disorder and major depression – the role of cognitive self-consciousness. J Behav Ther Exp Psychiatry. 2012;43(3):863–870. doi: 10.1016/j.jbtep.2011.12.009. [DOI] [PubMed] [Google Scholar]
- 54.O’Kearney R, Nicholson C. Can a theory of mind disruption help explain OCD related metacognitive disturbances? Behav Change. 2008;25(2):55–70. [Google Scholar]
- 55.Stern ER, Fitzgerald KD, Welsh RC, et al. Resting-state functionality connectivity between fronto-parietal and default mode networks in obsessive-compulsive disorder. PLoS ONE. 2012;7(5):e36356. doi: 10.1371/journal.pone.0036356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Anticevic A, Repovs G, Barch DM. Resisting emotional interference: brain regions facilitating working memory performance during negative distraction. Cogn Affect Behav Neurosci. 2010;10(2):159–173. doi: 10.3758/CABN.10.2.159. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Kemps E, Tiggemann M. Working memory performance and preoccupying thoughts in female dieters: Evidence for a selective central executive impairment. Br J Clin Psychol. 2005;44(3):357–366. doi: 10.1348/014466505X35272. [DOI] [PubMed] [Google Scholar]
- 58.Kemps E, Tiggemann M, Wade T, et al. Selective working memory deficits in anorexia nervosa. Eur Eat Disord Rev. 2006;14(2):97–103. [Google Scholar]
- 59.Harkin B, Kessler K. The role of working memory in compulsive checking and OCD: A systematic classification of 58 experimental findings. Clin Psychol Rev. 2011;31(6):1004–1021. doi: 10.1016/j.cpr.2011.06.004. [DOI] [PubMed] [Google Scholar]
- 60.Chen EYH, Wong GHY, Hui CLM, et al. Phenotyping psychosis: room for neurocomputational and content-dependent cognitive endophenotypes? Cogn Neuropsychiatry. 2009;14(4–5):451–472. doi: 10.1080/13546800902965695. [DOI] [PubMed] [Google Scholar]
- 61.Gottesman II, Gould TD. The endophenotype concept in psychiatry: etymology and strategic intentions. Am J Psychiatry. 2003;160(4):636–645. doi: 10.1176/appi.ajp.160.4.636. [DOI] [PubMed] [Google Scholar]
- 62.Bartrina JA. Ortorexia o la obsesión por la dieta saludable [Orthorexia or when a healthy diet becomes an obsession] Archivos Latinoamericanos de Nutrición. 2007;57(4):313–315. Spanish. [PubMed] [Google Scholar]
- 63.Borgida A. In sickness and in Health: Orthorexia Nervosa, The Study of Obsessive Healthy Eating [dissertation] USA: ProQuest Information and Learning; 2012. [Accessed December 15, 2014]. pp. 6376–6376. Available from: http://gradworks.umi.com/34/67/3467161.html. [Google Scholar]
- 64.Simpson HB, Wetterneck CT, Cahill SP, et al. Treatment of obsessive-compulsive disorder complicated by comorbid eating disorders. Cogn Behav Ther. 2013;42(1):64–76. doi: 10.1080/16506073.2012.751124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Sulkowski ML, Jacob ML, Storch EA. Exposure and response prevention and habit reversal training: commonalities, differential use, and combined applications. J Contemp Psychother. 2013;43(3):179–185. [Google Scholar]
- 66.Abbott M. Restructuring cognitive distortions. In: Robert-McComb JJ, editor. Eating Disorders in Women and Children: Prevention, Stress Management, and Treatment. Boca Raton, FL: CRC Press; 2001. pp. 273–282. [Google Scholar]
- 67.Shapiro JR, Pisetsky EM, Crenshaw W, et al. Exploratory study to decrease postprandial anxiety: just relax! Int J Eat Disord. 2008;41(8):728–733. doi: 10.1002/eat.20552. [DOI] [PubMed] [Google Scholar]
- 68.Schröder A, Heider J, Zaby A, et al. Cognitive behavioral therapy versus progressive muscle relaxation training for multiple somatoform symptoms: results of a randomized controlled trial. Cogn Ther Res. 2013;37(2):296–306. [Google Scholar]
- 69.Barsky AJ, Ahern DK, Bauer MR, et al. A randomized trial of treatments for high-utilizing somatizing patients. J Gen Inter Med. 2013;28(11):1396–1404. doi: 10.1007/s11606-013-2392-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Morahan-Martin JM. How Internet users find, evaluate, and use online health information: a cross-cultural review. Cyberpsychol Behav. 2004;7(5):497–510. doi: 10.1089/cpb.2004.7.497. [DOI] [PubMed] [Google Scholar]
- 71.Muse K, McManus F, Leung C, et al. Cyberchondriasis: fact or fiction? A preliminary examination of the relationship between health anxiety and searching for health information on the Internet. J Anxiety Disord. 2012;26(1):189–196. doi: 10.1016/j.janxdis.2011.11.005. [DOI] [PubMed] [Google Scholar]
- 72.Frances A. Saving Normal: An Insider’s Revolt Against Out-Of-Control Psychiatric Diagnosis, DSM-5, Big Pharma, and The Medicalization of Ordinary Life. New York, NY: William Morrow & Co; 2013. [Google Scholar]