Abstract
Southeast Asian women in California have high cervical cancer incidence and mortality rates, but low levels of Pap screening. No published reports have addressed screening among Thai women. Entertainment-education (EE) is a useful strategy for low-literacy, culturally diverse populations. This quasi-experimental study determined whether a soap-opera-themed, Thai-language EE video was superior to a print handout for increasing knowledge, attitudes, and behavioral intention toward Pap testing. No uniform differences were found between the intervention group (video) and the control group (brochure). Both educational modalities appeared to result in selected increases in knowledge and attitudes.
Keywords: Entertainment-Education, Cervical Cancer Screening, Thai Women, Pap screening
Introduction
One of the least understood groups of Southeast Asians in the US are Thai Americans. There were over 160,000 Thais in the US in 2000, representing a 65 % increase in size from a decade ago. California is home to the largest Thai American population in the country, with approximately 60,000 Thai Americans living in the Hollywood area alone. According to the 2000 census, educational levels are very low for Southeast Asian populations, with only 25 % of Thai females having obtained a college degree. In the Los Angeles and Orange County areas, close to 100 % of the Southeast Asians speak an Asian language at home and about 70–78 % do not speak English very well. Per capita income of Thai Americans was $12,544, and 12.5 % live below the poverty level (http://www.census.gov/main/www.cen2000).
No published reports to date have addressed Pap testing levels among Thai women in the US. However, unpublished data collected in 2003 in California found that, while 91 % of Thai women age 35+years old had ever had a Pap test, only 54 % reported that they obtained their exams yearly (Tsau J, Tanjasiri, SP. Cervical cancer screening among Thai women in northern California. Unpublished manuscript, 2003). Recent studies suggest Asian American populations represent underserved populations for cancer control because of their unique combination of cultural influences (such as their beliefs about the meaning and cause of cancer) [1] and structural barriers (such as lack of health insurance and low income) [2]. Health literacy, defined as an individual's ability to “obtain, process, and understand basic health information and services” [3–5] is also a major concern for Thai American women.
Unquestionably, there is an enormous need in the field for culturally sensitive educational strategies tailored to reach low-literacy and culturally diverse populations, such as Thai Americans [6]. The entertainment-education communication strategy represents a potentially useful format for such a purpose. Entertainment-education (EE) is defined as “the process of purposely designing and implementing a media message to both entertain and educate, in order to increase audience members’ knowledge about an educational issue, create favorable attitudes, shift social norms and change overt behavior” [7].
One of the shortcomings of a one-time, soap-opera-themed EE intervention is its inherent dependence on repetitive exposure. Nariman suggests that the EE strategy is most effective “when applied in a repetitious form of entertainment” [8]. While this study attempted to balance this shortcoming through group discussion between participants and the health educator using the video characters’ attitudes and knowledge to facilitate such discussion, logistical constraints in workplace sites compromised this important aspect of the study design (see “Discussion” below).
Materials and Methods
Study Design
This was a 2-year (2004–2006) quasi-experimental study to design, develop, and test the effectiveness of a culturally appropriate intervention in the form of a 7-min soap-opera-themed video to increase cervical cancer knowledge and promote positive attitudes and screening behavior among Thai women in Los Angeles and Orange Counties, California. We hypothesized that women who were shown the EE video would have higher levels of cervical cancer and Pap testing knowledge, more positive attitudes, and behavioral intention changes compared with women who were given a print handout. Approval of our institution's Internal Review Board for research with human subjects was obtained. Pretest and posttest measures (the latter immediately after the intervention as well as at 3-month follow-up) were used to assess changes in cervical cancer and Pap test knowledge, attitudes, and beliefs. Follow-up was done primarily by telephone, with some face-to-face.
Intervention Development and Implementation
Presenting health messages in an EE drama format demands creativity and cultural sensibilities. Scripting of the intervention for this study addressed three of the six major challenges in keeping EE interventions credible and entertaining cited by staff from Johns Hopkins University's Center for Communication Programs (JHU/CCP), which has assisted over the past 20 years in some 125 EE programs in 40 countries worldwide: (1) high quality and emotionally resonant content; (2) health messages woven into program naturally, gradually, and subtly; (3) research-based content. The other three challenges pertained to comprehensive campaigns around mass-mediated, ongoing serial-type interventions well beyond the scope of this study [9].
The video script was drafted in English by two bilingual Thai–English health educators, with input from the non-Thai researchers on the study. Building on Bandura's social modeling theory [10], the researchers emphasized three character roles: positive, negative, and transitional role models, with the transitional character changing from negative to positive after adopting the desired behavior change (Pap testing). Using the Transtheoretical Model and the EE communication strategy, the script also avoided detailed medical information, with an emphasis on credible characters delivering a message within the dramatic context of a soap opera. Next, the video script was shown to a Thai physician, staff at Thai health clinics, and a Thai filmmaker for their input. The script was modified several times, with the final version translated into Thai by the two bilingual health educators.
A Thai filmmaker used broadcast-quality production methods and Thai actors and actresses. The main character, the negative role model who becomes the transitional role model and then a positive role model, is a mother who continually ignores abdominal pain until her friend, the positive role model, insists she see her doctor and also have a Pap test. After diagnosis of an infection, the main character discusses the Pap test and cervical cancer with her doctor, has a test, and ultimately receives a negative report (her reward).
Two Thai community educators went to organizational sites within the community to present programs. Using a facilitation guide, both educators engaged in group discussions with participants following presentation of the two interventions. The print handouts, which contained the same basic information as the doctor told the main character in the video, were reviewed with participants to ensure they could read and understand the information. Pap testing recommendations followed the American Cancer Society guidelines for pap testing. Group discussions covered specific points with attempts to keep all discussions to similar lengths, though interruptions and other logistical constraints made this difficult (see, “Discussion” below).
Participant Recruitment
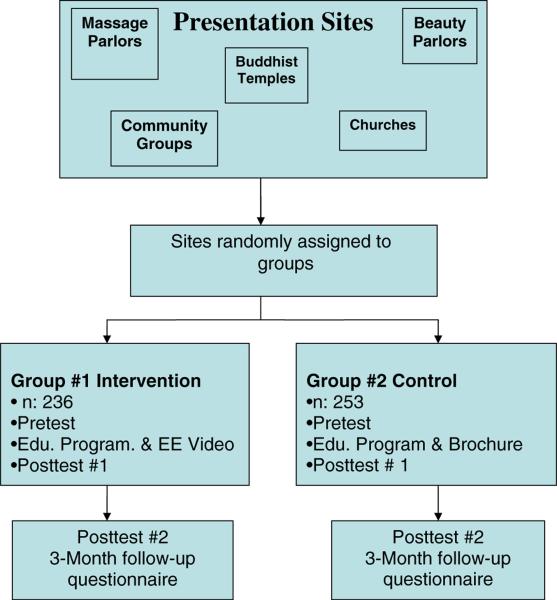
Thai women aged 18 years and older were recruited by two Thai community health educators experienced in cancer control education for the Thai community in Los Angeles and Orange Counties. Based upon input from the educators, an organizational recruitment plan was developed with sites for recruitment including beauty salons, Thai markets, massage parlors with Thai women employees, and Thai temples. Sites were pre-identified and then randomly assigned to receive either the video intervention or a one-page Thai-language print handout on cervical cancer and Pap tests, both followed by a facilitated discussion with the health educator (see Fig. 1). At the time of recruitment, all women received a written informed consent form in the Thai language with the educators explaining the form personally. Only participants who signed the form were included in the study. The form indicated that participants would receive a cash incentive to participate.
Fig. 1.
Study design
Data Management and Analyses
Pretest and posttest data for both groups were coded and entered into SPSS version 14.0 by the authors. Stages of readiness were defined and coded as follows: precontemplation: not planning to have a Pap within the next year; contemplation: off schedule (never had a Pap test or not had one for 3 years) but planned to have one within a year; action: on schedule (had a Pap test within the last 3 years), and planning to have one within the next year. Positive change in stage was defined as either moving one stage or more (e.g., precont-emplation to contemplation) or staying the same stage.
Data analyses included univariate frequencies and chi square tests for statistically significant differences in proportions between intervention and control groups, and within groups between pretest and posttest questionnaires. Multivariate logistic regression was used to determine whether changes in stage of readiness differed significantly by group, controlling for demographic differences between groups. The remainder of this paper reports on the results from the pretest and first posttest questionnaires of the study.
Results
A total of 504 women were approached to participate in this study, of which 498 agreed (98.8 %). Of the 498 women who participated (and completed a pretest and posttest questionnaire), 236 were participants in group 1 (intervention) and 253 in group 2 (control). As shown in Table 1, average age of participants was in the forties, with the overwhelming majority native-born Thais with very minimal English skills. Reading fluency (in Thai) was not differentiated from speaking fluency, as most Thais in California are first-generation, thus concordance between reading and speaking was assumed. Nearly half were married and reported a family income of $12,000 or less yearly. Well over half in the control group had health insurance while well over half in the intervention group did not; however, in spite of lower health insurance rates, a larger majority of intervention group women reported ever having a Pap test. The overwhelming majority of women in both groups were in the contemplation stage. Besides language ability and health insurance, no significant differences were found between groups.
Table 1.
Demographics of study participants at present
| Group 1, intervention (n = 236) | Group 2, control (n = 253) | P valuea | Total (n = 489) | |
|---|---|---|---|---|
| Place of birth | ||||
| Thailand | 94.4 | 96.7 | ns | 95.7 |
| Other | 5.6 | 3.3 | 4.3 | |
| Speak Thai | ||||
| Fluently/well | 85.7 | 92.8 | 0.022 | 89.6 |
| Fair/poor/not at all | 14.3 | 7.2 | 10.4 | |
| Language most comfortable | ||||
| Only/mostly English | 1.3 | 1.2 | ns | 1.2 |
| Both | 29.6 | 32.0 | 30.8 | |
| Only/mostly Thai | 69.1 | 66.8 | 67.9 | |
| Marital status | ||||
| Married | 41.7 | 49.0 | ns | 45.5 |
| Divorced/separated | 16.2 | 14.5 | 15.3 | |
| Long-term relationship | 7.0 | 3.2 | 5.0 | |
| Single | 18.0 | 21.3 | 19.7 | |
| Widowed | 17.1 | 12.0 | 14.5 | |
| Age group | ||||
| 18-25, years | 8.7 | 8.0 | 8.4 | |
| 26-35, years | 8.3 | 12.4 | 10.4 | |
| 36-45, years | 17.9 | 20.0 | 19.0 | |
| 46-55, years | 32.8 | 26.0 | 29.2 | |
| 56-65, years | 19.7 | 20.4 | 20.0 | |
| 66-75, years | 8.7 | 9.2 | 9.0 | |
| 75+, years | 3.9 | 4.0 | ns | 4.0 |
| Family income | ||||
| <$500/month | 17.3 | 10.4 | ns | 13.8 |
| $500-999 | 32.0 | 31.7 | 31.8 | |
| $1,000-1,499 | 15.1 | 14.2 | 14.6 | |
| $1,500-1,999 | 10.7 | 13.3 | 12.0 | |
| $2,000-2,499 | 6.2 | 8.8 | 7.5 | |
| $2,500-2,999 | 4.4 | 2.9 | 3.7 | |
| $3,000+ | 14.2 | 18.8 | 16.6 | |
| Have health insurance | ||||
| Yes | 41.2 | 58.3 | 0.000 | 50.1 |
| No | 58.8 | 41.7 | 49.9 | |
| Ever had a Pap test | ||||
| Yes | 87.5 | 77.7 | ns | 80.9 |
| No | 15.5 | 22.3 | 19.1 | |
| Stage of readiness | ||||
| Precontemplation | 24.1 | 33.9 | 0.041 | 29.3 |
| Contemplation | 26.3 | 26.3 | 26.3 | |
| Action | 49.6 | 39.8 | 44.4 |
Chi square analysis, alpha≤0.05
Table 2 shows changes in knowledge, attitudes, and behavioral intention measures. Unfortunately, we saw no uniform differences between the two groups. Surprisingly, of the 28 items measured, only five showed significant changes for both groups. There were significant increases in knowledge of correct age to start Pap tests (group 1, p<0.0000; group 2, p<0.046). Increases were also significant in one knowledge item: “sex at an early age” (group 1, p<0.000; group 2, p<0.020). Significant increases in attitudes toward Pap tests were seen in “not embarrassed to get Pap” (group 1, p<0.059; group 2, p<0.024). Two items in attitudes toward cervical cancer showed significant increases in both groups: “Pap tests help prevent cervical cancer” (group 1 p<0.038; group 2 p<0.010) and “cervical cancer not punishment from spirits” (group 1 p<0.058; group 2 p<0.000).
Table 2.
Changes in attitudes and behaviors (pretest vs. posttest) by group (includes only women who completed both pretest and posttest 1; percentages are those who answered “yes”)
| Group 1, intervention (n = 236) |
Group 2, control (n = 253) |
|||||
|---|---|---|---|---|---|---|
| Pretest | Posttest | P valuea | Pretest | Posttest | P valuea | |
| Knows correct age to start Pap tests | 14.5 | 54.2 | 0.000 | 8.9 | 15.0 | 0.046 |
| Knows correct frequency for Pap tests | 87.4 | 88.4 | ns | 80.0 | 88.0 | 0.015 |
| Very comfortable talking about Pap tests with family/friends | 63.7 | 69.3 | ns | 63.9 | 36.1 | ns |
| Plan to get a Pap test within year | 75.9 | 78.6 | ns | 66.1 | 73.3 | 0.033 |
| Stages of readiness | ||||||
| Precontemplation | 24.1 | 21.4 | ns | 33.9 | 26.7 | ns |
| Contemplation | 26.3 | 23.3 | 26.3 | 27.1 | ||
| Action | 49.6 | 55.3 | 39.8 | 46.3 | ||
| Knowledge of risk factors for cervical cancer | ||||||
| Getting older | 73.3 | 73.7 | ns | 77.1 | 80.2 | ns |
| Using birth control pills | 93.6 | 85.2 | .004 | 92.9 | 96.0 | ns |
| Sex at early age | 84.7 | 95.3 | .000 | 91.7 | 96.8 | 0.020 |
| Many sex partners | 74.6 | 73.3 | ns | 75.9 | 80.2 | ns |
| Husband having many sex partners | 82.2 | 80.9 | ns | 77.1 | 96.8 | 0.000 |
| Attitudes towards Pap testsb | ||||||
| Not embarrassed to get Pap | 67.1 | 75.5 | 0.059 | 71.2 | 80.2 | 0.024 |
| Not afraid to get Pap | 81.2 | 78.7 | ns | 82.8 | 87.4 | ns |
| Need Pap after menopause | 85.5 | 89.2 | ns | 86.6 | 90.0 | ns |
| Need Pap after childbearing | 91.9 | 91.6 | ns | 94.1 | 94.7 | ns |
| Not too old to need Pap | 90.6 | 92.8 | ns | 87.8 | 85.5 | 0.002 |
| Pap results are accurate | 68.9 | 81.5 | 0.002 | 73.9 | 79.9 | ns |
| Pap even if not sexually active | 87.2 | 90.2 | ns | 88.8 | 91.6 | ns |
| Pap is important | 89.7 | 89.9 | ns | 89.8 | 91.3 | ns |
| Not too busy to get Pap | 91.4 | 93.5 | ns | 93.6 | 94.7 | ns |
| Family not more important | 91.2 | 91.1 | ns | 90.7 | 94.4 | ns |
| Have time for Pap | 90.2 | 94.1 | ns | 88.7 | 91.9 | ns |
| Know where to go for Pap | 82.6 | 97.4 | ns | 86.4 | 91.0 | ns |
| Attitudes toward cervical cancer | ||||||
| Would rather know if hadb | 88.1 | 91.7 | ns | 92.0 | 93.7 | ns |
| Cervical cancer (CC) is not rare so worryb | 74.1 | 80.6 | ns | 68.1 | 87.4 | 0.000 |
| Pap tests help prevent CC | 63.3 | 72.4 | 0.038 | 53.8 | 65.2 | 0.010 |
| CC not punishment from spiritsb | 80.3 | 87.0 | 0.058 | 68.3 | 90.1 | 0.000 |
| CC can be cured | 82.1 | 82.3 | ns | 86.1 | 79.3 | 0.044 |
| I can do things to prevent CCb | 79.1 | 78.8 | ns | 82.5 | 86.7 | ns |
| CC is not because of my fateb | 86.2 | 89.4 | ns | 92.1 | 94.6 | ns |
ns indicates no significant difference between groups
Chi square analyses (paired analyses), alpha≤0.05
Items inverted to report on “positive” attitudes
With regard to stages of readiness, the proportion of women in precontemplation decreased and the proportion in action increased in both groups (see Table 2). Between pretest and posttest, 57.6 % of women in the intervention group had a positive change in their stage of readiness compared with 53.8 % in the control group. However, no statistically significant differences were found by group after controlling for health insurance and Thai speaking ability (data not shown). Data for follow-up are not shown because there were no significant changes.
By way of explanation for several specific findings (listed below), the educators suggested that most participants had seldom or never talked about cancer before and after learning more about the disease were uncomfortable or fearful: Group 1 participants showed a slight increase in being afraid of getting a Pap test; group 2 participants showed a decrease in being comfortable in talking about Pap tests with family and friends. Among participants who indicated they had a Pap test, no information regarding follow-up Pap tests was obtained as this was beyond the scope of this study.
Discussion
This study was the first of its kind to test the effects of an EE video intervention on cancer-related impacts among Thai American women. The purpose of this study was to determine whether an EE video was superior to an informational print handout for increasing knowledge, positive attitudes, and behavioral intention regarding Pap testing. The biggest surprise in this study was the lack of uniform differences between the intervention and control groups; both educational modalities appeared to result in selected increases in cervical cancer and Pap testing knowledge and attitudes. These results suggest that either modality can successfully educate Thai women, supporting the need for any form of education in this underserved population.
Women in both groups increased their stages of readiness, although these increases did not differ significantly by group. Both modalities appeared to work equally well in moving women from precontemplation to contemplation and action. The lack of increased influence of the EE intervention points to the question of whether the intervention reached the threshold necessary to motivate women to intend to get a Pap test. Our findings underscore the importance of learning more about the unique cultural and contextual characteristics of Thai American women in order to more carefully target and tailor Pap testing messages for this population.
Several logistical constraints also presented limitations in this study. Intervention locations were a significant problem. A pronounced shift in workplaces and conditions was identified, with many lower-income Thai women previously employed in the garment industry having moved to jobs in massage parlors, creating time constraints and difficult conditions for presentation of the program. Owners of the parlors were very reluctant to allow employees time to participate. Of those who participated, many were so concerned about time away from their job they did not participate in any discussion, asked no questions, were not attentive to the video, and were interrupted during the program.
It is suggested these conditions particularly negated any benefit from the group discussion so vital to the EE strategy (see last paragraph of “Introduction”). Video intervention group participants had little or no opportunity for necessary parasocial interaction, preventing a full discussion of the characters, their behavior, and relating situations in the video to real-life. These problems may explain the lack of effects from the video intervention. Thus, we see that, while workplace education has advantages, it also has limitations which can negatively impact interventions such as the EE video. (Note: Copies of the EE video were distributed widely to health educators/providers in the Thai community.) Participants did not express any preference for either intervention.
Future studies of underserved populations should build upon our organizational recruitment and assignment approach to better control for differences in site characteristics. Despite the fact that our original hypothesis was not supported, results supported the importance of engaging Thai American women in community-based educational efforts. Such efforts, in the form of print handouts or video, can significantly increase their knowledge of and positive attitudes toward cervical cancer screening. Indeed, given the significant resource needs to produce audiovisual modes of education, it is very encouraging to find that written forms of information are equally as educational. This may be particularly true when presented by trusted bilingual, bicultural educators who may promote not only cognitive increases but also affective support for cancer early detection methods [11].
Future studies should also be extended to include knowledge, positive attitudes, and behavioral intention in regard to cervical cancer prevention now possible through the use of two vaccines (Cervarix and Gardasil) to protect women against the types of human papilloma virus that can cause cervical cancers (http://www.cdc.gov/hpv/vaccine.html).
Supplementary Material
Acknowledgments
This study was supported by NCI grant #55764. The authors gratefully acknowledge the invaluable contributions of Jackie Tran, Waraporn “Nid” Tiaprasith, Srinapha “Noi” Vasunilashorn, Dr. Michele Mouttapa, and all the study participants.
Footnotes
Publisher's Disclaimer: Your article is protected by copyright and all rights are held exclusively by Springer Science+Business Media, LLC. This e-offprint is for personal use only and shall not be self-archived in electronic repositories. If you wish to self-archive your work, please use the accepted author's version for posting to your own website or your institution's repository. You may further deposit the accepted author's version on a funder's repository at a funder's request, provided it is not made publicly available until 12 months after publication.
Electronic supplementary material
The online version of this article (doi:10.1007/s13187-012-0369-5) contains supplementary material, which is available to authorized users.
References
- 1.Jenkins CNH, Kagawa-Singer M. Cancer. In: Zane NWS, Takeuchi DT, Young KNJ, editors. Confronting critical health issues of Asian and Pacific Islander Americans. Thousand Oaks. Sage; 2003. pp. 105–147. [Google Scholar]
- 2.Babey SH, Pence NA, Etzioni DA, et al. Cancer screening in California: racial and ethnic disparities persist. UCLA Center for Health Policy Research; Los Angeles: 2003. [PubMed] [Google Scholar]
- 3.Davis TC, Williams MV, Marin E, et al. Health literacy and cancer communication. CA: A CA J Clin. 2000;52:134–149. doi: 10.3322/canjclin.52.3.134. [DOI] [PubMed] [Google Scholar]
- 4.Freimuth VS, Mettger W. Is there a hard-to-reach audience? Public Health Rep. 1990;105(3):232–239. [PMC free article] [PubMed] [Google Scholar]
- 5.Roter DL, Rudd RE, Comings J. Patient literacy: a barrier to quality of care. J Gen Int Med. 1989;13:850–851. doi: 10.1046/j.1525-1497.1998.00250.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Mead CD. Producing videotapes for cancer education: methods and examples. Onc Nurs Forum. 1996;23:837–846. [PubMed] [Google Scholar]
- 7.Singhal A, Cody M, Rogers E, et al., editors. Entertainment-education and social change: history, research, and practice. Lawrence Erlbaum Associates; Mahwah, NJ: 2004. pp. 153–176. [Google Scholar]
- 8.Nariman HN. Soap operas for social change: toward a methodology for entertainment-education television. Praeger; Westport: 1993. [Google Scholar]
- 9.Piotrow PT, de Fossard E. Entertainment-education as a public health intervention. In: Singhal A, Cody MJ, Rogers E, et al., editors. Entertainment-education and social change: history, research, and practice. Lawrence Erlbaum Associates; Mahwah, NJ: 2004. p. 55. [Google Scholar]
- 10.Bandura A. Social learning theory. Prentice-Hall; Englewood Cliffs, NJ: 1977. [Google Scholar]
- 11.Nguyen TU, Tanjasiri SP, Kagawa-Singer M, et al. Community health navigators for breast- and cervical-cancer screening among Cambodian and Laotian women: intervention strategies and relationship-building processes. Health Promot Pract. 2008;9:356–367. doi: 10.1177/1524839906290251. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.