Abstract
Disabling the function of immune checkpoint molecules can unlock T-cell immunity against cancer, yet despite remarkable clinical success with monoclonal antibodies (mAb) that block PD-1 or CTLA-4, resistance remains common and essentially unexplained. To date, pancreatic carcinoma is fully refractory to these antibodies. Here, using a genetically engineered mouse model of pancreatic ductal adenocarcinoma in which spontaneous immunity is minimal, we found that PD-L1 is prominent in the tumor microenvironment, a phenotype confirmed in patients; however, tumor PD-L1 was found to be independent of IFNγ in this model. Tumor T cells expressed PD-1 as prominently as T cells from chronically infected mice, but treatment with αPD-1 mAbs, with or without αCTLA-4 mAbs, failed in well-established tumors, thus recapitulating clinical results. Agonist αCD40 mAbs with chemotherapy induced T-cell immunity and reversed the complete resistance of pancreatic tumors to αPD-1 and αCTLA-4. The combination of αCD40/chemotherapy plus αPD-1 and/or αCTLA-4 induced regression of subcutaneous tumors, improved overall survival, and conferred curative protection from multiple tumor rechallenges, consistent with immune memory not otherwise achievable. Combinatorial treatment nearly doubled survival of mice with spontaneous pancreatic cancers although no cures were observed. Our findings suggest that in pancreatic carcinoma, a non-immunogenic tumor, baseline refractoriness to checkpoint inhibitors can be rescued by the priming of a T-cell response with αCD40/chemotherapy.
Keywords: Pancreatic cancer, PD-1, CTLA-4, immunotherapy, CD40
INTRODUCTION
Pancreatic ductal adenocarcinoma (PDA) is a lethal and aggressive disease with the lowest 5-year patient survival rates of any tumor type routinely tracked (6%). The incidence of PDA is rising, and it is projected to become the second leading cause of cancer death in the United States by 2025 (1). PDA is distinguished by a dense desmoplastic stroma, rich in fibroblasts, extracellular matrix, and inflammatory leukocytes (but few infiltrating effector T cells). Although new combination chemotherapies are increasingly effective for PDA (2,3), tumor response rates remain low and durability is short.
T cells are key mediators of antitumor immunity and regulate the outcome of tumor immune surveillance (4). Critical to this regulation are lymphocyte inhibitory receptors such as programmed cell death protein 1 (PD-1) and cytotoxic T-lymphocyte-associated antigen 4 (CTLA-4), which restrain T-cell antitumor immunity (5-8). Monoclonal antibodies (mAb) that block PD-1 or CTLA-4 induce T cell-dependent tumor regression in many experimental systems (7,8). Unprecedented rates of tumor regressions have been observed in patients with melanoma and multiple carcinomas following treatment with mAbs against CTLA-4, PD-1, or programmed death-ligand 1 (PD-L1), a ligand for PD-1 (9-14). PD-1 engagement inhibits T-cell function primarily during the T-cell effector phase (15-17). Its main ligands are PD-L1 and programmed death-ligand 2 (18). PD-L1 is expressed on tumor cells as well as on tumor-associated leukocytes, and antibody blockade of either PD-1 or PD-L1 can restore antitumor immunity in murine cancer models (19-21). CTLA-4 is a crucial immune checkpoint regulator expressed on T cells; loss of CTLA-4 leads to rampant lymphoproliferation, autoimmunity, and death in mice (22). Expression of CTLA-4 is found on effector T cells but especially regulatory T cells (Treg); CTLA-4 blockade in murine tumor models both inhibits negative signaling in effector cells and depletes Tregs (23-25).
Mechanisms of PD-1 or CTLA-4 resistance are poorly understood. Pre-existing T-cell antitumor immunity has been hypothesized as a prerequisite (26-29). The majority of cancer patients treated with these agents alone do not respond clinically, and some tumor types, such as PDA, are fully refractory (12,30,31). Although combinations of αPD-1 and αCTLA-4 may improve tumor response rates in melanoma, a large fraction of patients still fail to respond (32). Tumor PD-L1 expression in some tumors correlates spatially with the presence of infiltrating CD8+ T cells, suggesting that tumor cells upregulate PD-L1 in response to immune pressure, a hypothesis termed adaptive immune resistance (33-35). CD8+ T cell-derived IFNγ may drive PD-L1 expression in malignant cells (18,36). These data suggest that the efficacy of checkpoint inhibitors may require the presence of an endogenous antitumor T-cell response. In fact, the augmentation of antitumor T-cell responses with vaccines, peritumoral poly(I:C), or intratumoral oncolytic virus has been shown to improve baseline responses to checkpoint inhibitors in murine models (21,27,37,38).
In the studies reported here, we tested the hypothesis that failed immune recognition or poor T-cell priming underlies weak clinical responses to checkpoint therapy in pancreatic cancer, i.e. induction of T-cell immunity is required to potentiate tumor regressions not otherwise achievable with checkpoint blockade alone. We studied the KPC mouse model of spontaneous PDA in which expression of oncogenic KrasG12D and mutant p53 is targeted to the pancreas by Cre recombinase under the control of the pancreas-specific promoter Pdx-1 (39). This model recapitulates the molecular, histologic and immune parameters of the human disease (39-43). Analysis of human PDA was performed to confirm the clinical relevance of our findings in the murine model. We induced T-cell immunity using an agonistic αCD40 in combination with chemotherapy (44,45), and studied the impact of αPD-1/αCTLA4 mAbs.
MATERIALS AND METHODS
Mice
All animal protocols were reviewed and approved by the Institutional Animal Care and Use Committee of the University of Pennsylvania. KrasLSL-G12D/+, Trp53LSL-R172H/+, Pdx1-Cre (KPC) mice (39), and KrasLSL-G12D/+, Trp53LSL-R172H/+, Pdx1-Cre, LSL-Rosa-YFP (KPC-Y) mice (46) were backcrossed 10 generations on the C57BL/6 background. Six- to eight-week-old female C57BL/6 and B6.129S7-Ifngtm1Ts/J (IFNγ ko) mice used for implantable tumor studies were from Jackson Laboratories.
Cell Lines
PDA cell lines from KPC or KPC-Y mice were derived from single-cell suspensions of PDA tissue as previously described (42). Dissociated cells were plated in a 6-well dish with serum free DMEM. After 2 weeks, media was changed to DMEM + 10% FCS. After 4-10 passages, cells were used in experiments. The cell lines were tested and confirmed to be mycoplasma-free. No other authentication assays were performed.
In vivo Mouse Studies
For implantable tumor experiments, PDA tumor cells (5×105) were injected subcutaneously in PBS into the flanks of mice and allowed to grow 9-11 days until tumor volumes averaged 30-100mm3. Mice were then enrolled into treatment groups such that cohorts were balanced for baseline tumor size. Mice were treated intraperitoneally (i.p.) with αPD-1 (RMP1-14, BioXcell; 200μg per dose) on days 0, 3, 6, 9, 12, 15, 18, and 21 (after enrollment) and/or αCTLA-4 (9H10, BioXcell; 200μg per dose) on days 0, 3, and 6. All antibodies were endotoxin free. Clinical grade gemcitabine (Eli Lilly) was purchased through the Hospital of the University of Pennsylvania Pharmacy; clinical grade nab-paclitaxel was either purchased or a kind gift from Celgene. Chemotherapy vials were resuspended and diluted in sterile PBS, and injected i.p. at 120 mg/kg (for each chemotherapeutic) on day 1. As a control for the human albumin component of nab-paclitaxel, control cohorts were treated with human albumin at the same dose as the albumin component of nab-paclitaxel (108 mg/kg) on day 1 (Sigma Life Science). All antibodies were given i.p. Agonistic αCD40 (FGK45, BioXcell; 100μg) was given on day 3. For T-cell depletion studies, αCD8 (2.43, BioXcell; 200μg per dose) and αCD4 mAbs (GK1.5, BioXcell; 200μg per dose) were injected twice weekly for the duration of the experiment, starting on day 0 (day of enrollment). For isotype controls, rat IgG2a (2A3, BioXcell; 100μg) and rat IgG2b (LTF-2, BioXcell; 200μg per dose) were used. This approach achieved >98% depletion of CD8+ and CD4+ T cells in peripheral blood and tumor tissue compared to that of control mice, as monitored by flow cytometry. For macrophage depletion studies, clodronate encapsulated liposomes (CEL) or PBS encapsulated liposomes (PEL, both at 12μl/g; purchased from Dr. Nico van Rooijen, Vrije Universiteit, Amsterdam, the Netherlands) were used i.p. starting on day -1 and repeated every 4 days for the duration of the experiment; in these experiments, 2.5×105 PDA cells were implanted. For tumor rechallenge studies, αCD8 or isotype control antibodies were injected i.p. the day before the second rechallenge and continued twice weekly until day 60 or the mouse was sacrificed for tumor burden. To monitor growth of subcutaneous tumors, tumor diameters were measured by calipers and volume calculated by 0.5 × L × W2 in which L is the longest diameter and W is the perpendicular diameter. Endpoint criteria for the survival studies included tumor volume exceeding 1,000 mm3 or tumor ulceration. Mice that died suddenly or developed vestibular signs, as described in Supplementary Fig. S8, with minimal tumor burden were censored on the day of death or euthanasia.
For studies using the KPC model, young KPC mice were monitored by abdominal palpation and/or ultrasonography (Vevo 2100 Imaging System with 55MHz MicroScan transducer, Visual Sonics) for the development of pancreatic tumors. Mice with ultrasound diagnosed tumors of volume 30-150 mm3 were enrolled and block randomized into treatment groups. Tumors were visualized and reconstructed for quantifying tumor volume using the integrated Vevo Workstation software package. Baseline tumor volume was not significantly different across cohorts. KPC mice were treated with the same dose and schedule of antibodies and chemotherapeutics as noted above in the subcutaneous model. Mice were censored from study if they developed a secondary malignancy (n=1). Endpoint criteria included tumor volume exceeding 1,000 mm3 (by ultrasonography), severe cachexia, or extreme weakness and inactivity.
For viral studies, C57BL/6 mice were infected intravenously with 4×106 PFU of LCMV clone 13, which was propagated, titrated and used as previously described (15). Mice were sacrificed on day 30 post infection and tissues harvested for analyses.
Collection of Tissue Samples from Mice
The entire pancreas (KPC) or subcutaneous tumor was washed in PBS, minced into small fragments, and incubated in collagenase solution (1 mg/ml collagenase V in DMEM) at 37°C for 45 min. Dissociated cells were passed through a 70 μM cell strainer twice and washed three times in DMEM. Spleens and lymph nodes were homogenized and passed through a 70 μM cell strainer to achieve single cell suspensions. For spleens, red blood cells were lysed using ACK Lysis Buffer (BioWhittaker).
Antibodies, Flow cytometry, In vitro IFNγ stimulation of tumor cells, and Toxicology are described in Supplementary Methods.
Patient Samples and Analysis
Formalin-fixed, paraffin-embedded tissue samples were prepared after surgical resection of patients with resectable pancreatic carcinoma according to an IRB-approved protocol, as noted in Supplementary Methods.
Statistical Analysis
Differences between two groups were analyzed by two-tailed Student’s T test. Differences between three or more groups were analyzed by one-way ANOVA with Bonferonni’s multiple comparison test used as a post hoc test to assess differences between any two groups. Tumor growth curves were analyzed by two-way ANOVA, with Tukey multiple comparisons of means used as a post hoc test to assess differences between any two groups. Survival curves were assessed by Log-rank (Mantel-Cox). Correlation between two groups was assessed by Spearman’s Rank Correlation Coefficient. All statistical analyses were performed on GraphPad Prism 6 (GraphPad) except 2-way ANOVA and related post hoc testing which were performed on R Statistical Software (R Core Team). p≤0.05 denotes differences that are statistically significant.
RESULTS
PD-1/PD-L1 axis is highly expressed in murine and human PDA
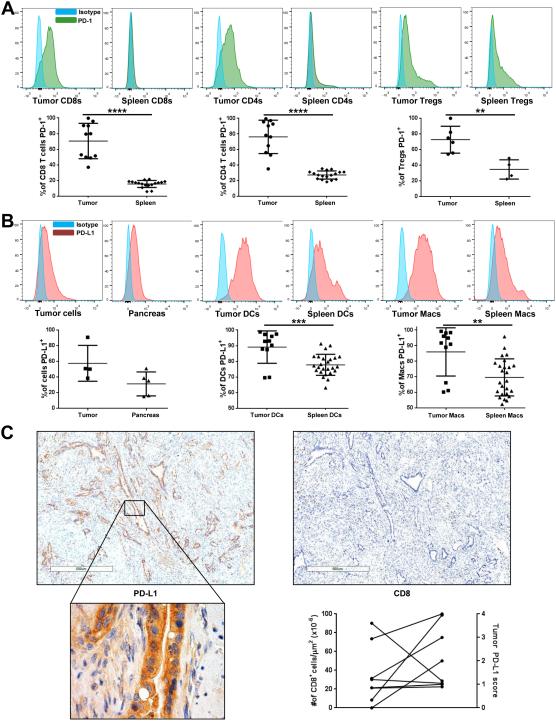
We interrogated the expression of PD-1 and PD-L1 using the KPC spontaneous genetic model of PDA. Within the microenvironment of KPC tumors, few infiltrating T cells were observed, as previously reported (41,42), but these T cells prominently expressed PD-1 in all subsets including CD8+, CD4+, and regulatory (Foxp3+) T cells. For each subset, PD-1 expression was significantly higher in the tumor than in the corresponding populations in the spleens of the same tumor-bearing mice (Fig. 1A). In the absence of a distinct marker for pancreatic epithelial cells in the KPC model, we identified tumor cells with negative gating, excluding leukocytes (CD45), endothelial cells (CD31) and mesenchymal populations (CD90) by flow cytometry of single-cell suspensions of KPC tumors. KPC pancreatic tumor cells exhibited moderate expression of PD-L1 on more than 40% of the identified tumor cells (Fig. 1B). PD-L1 was also expressed by 10%-50% of normal pancreatic epithelial cells identified in tumor-free wild-type mice. Dendritic cells (DC) and macrophages in the KPC tumor microenvironment expressed very high levels of PD-L1, statistically significantly higher compared to PD-L1 expression of these same antigen-presenting cell (APC) populations in the spleens of KPC mice (Fig. 1B).
Figure 1. Expression of PD-1 and PD-L1 in murine and human PDA.
(A) Representative histograms and quantification of PD-1 expression on tumor-infiltrating CD8+ (gated on live, CD45+, CD3+, CD8+), CD4+ (gated on live, CD45+, CD3+, CD4+), or regulatory (Tregs; gated on live, CD45+, CD3+, CD4+, FoxP3+) T cells in tumors (n=6-11) or spleens (n=4-17) from tumor-bearing KPC mice. **p≤ 0.01, ****p≤ 0.0001.
(B) Representative histograms and quantification of PD-L1 expression on tumor cells, normal pancreatic epithelial cells (gated on live, CD45neg, CD31neg, CD90neg), dendritic cells (DCs; gated on live, CD45+, F4/80neg, CD19neg, CD11c+), and macrophages (Macs; gated on live, CD45+, F4/80+) in tumors (n=4-11) or spleens (n=25) from tumor-bearing KPC mice; and normal pancreata (n=5) from healthy C57BL/6 mice. **p≤ 0.01, ***p≤ 0.001.
(C) Histology and quantification of PD-L1 expression and CD8+ T-cell infiltration in human pancreatic cancer sections. Left two panels, PD-L1 expression on malignant cells of a PDA tumor (PD-L1 expression score of 4+ (intense), see Materials and Methods and Supplementary Fig. S1; 40x and 400x magnification for top and bottom panels, respectively). Right top panel, CD8 expression in serial section of the tumor in left panel, demonstrating few tumor-infiltrating CD8+ T cells (40x magnification). Right bottom panel, plot describing correlation between intratumoral CD8 count and tumor PD-L1 score (n=8). p=0.69.
To assess whether these findings in the KPC model were consistent with human PDA, we examined human PDA samples for PD-L1 expression. In primary tumors from patients with resected PDA, we observed moderate to intense expression of PD-L1 on tumor and mononuclear cells in 4 of 8 (50%) resection specimens (Fig. 1C and Supplementary Fig. S1). We also observed that T cells in human PDA were relatively rare within malignant foci (mean ratio of CD8+ T cells per μm2 of tumor vs. non-tumor areas was 0.065 ± 0.052, range of 0.000-0.170) – again consistent with the KPC model (42). PD-L1 expression on tumor cells in human samples did not correspond spatially with the presence of CD8+ T cells; there was no statistical correlation between intensity or extent of tumor PD-L1 expression and intratumoral CD8+ T-cell infiltration (p=0.69) (Fig. 1C). For example, of the two tumors with the most intratumoral CD8+ T cells, one had intense and the other had minimal PD-L1 expression (Fig. 1C). These data in human PDA are in contrast to the correspondence of tumor PD-L1 expression and T-cell infiltration previously reported for tumors from patients with melanoma or kidney or head and neck carcinoma (HNSCC) (33-35).
PD-1 is as highly expressed in murine PDA as it is in chronic LCMV infection
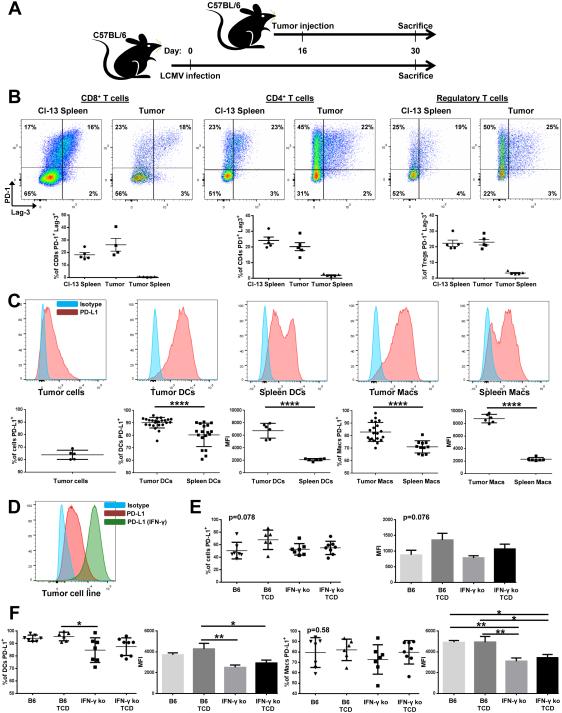
To evaluate the potential role of the PD-1/PD-L1 axis in mediating immune suppression in PDA, we first generated a PDA cell line from a backcrossed KPC mouse and established subcutaneous PDA tumors in immune competent C57BL/6 mice. Histopathologic examination of established tumors from this model showed recapitulation of both the cellular and extracellular components of spontaneous KPC tumors, with prominent deposition of a dense desmoplastic stroma and comparable populations of infiltrating immunosuppressive leukocytes, including F4/80+ macrophages (data not shown). We then examined expression of PD-1 on T cells from subcutaneous tumor-bearing mice but did so by simultaneously examining PD-1 expression on T cells from a parallel cohort of mice in which chronic lymphocytic choriomeningitis viral (LCMV) infection had been established with LCMV clone 13 (Fig. 2A). In many ways, this model of chronic LCMV infection has served as a gold standard for understanding the transcriptional basis and phenotype of exhausted CD4+ and CD8+ T cells (15,16,47-50). Two of the most highly upregulated genes mechanistically linked to T-cell exhaustion in response to chronic infection in this model are PD-1 and Lag-3 (15). We therefore compared coexpression of these markers on intratumoral and splenic T cells in mice bearing established subcutaneous PDA tumors with splenic T cells from mice with chronic LCMV (Fig. 2A). Intratumoral CD8+, CD4+, and regulatory T cells co-expressed PD-1 and Lag-3 at levels comparable to the same T-cell populations in LCMV-infected mice (Fig. 2B). This phenotype was restricted to the tumor, as splenic T cells from tumor-bearing mice did not co-express PD-1 or Lag-3. Thus, T-cell expression of PD-1 is as prominent in the PDA tumor microenvironment as it is in chronic LCMV infection.
Figure 2. PD-1/PD-L1 axis is highly expressed and is not IFNγ-dependent in a subcutaneous murine model of PDA.
(A) Experimental design for establishment of subcutaneous PDA tumors or chronic LCMV clone 13 (Cl-13) infection simultaneously in 2 cohorts of C57BL/6 mice.
(B) Representative flow plots and quantification of co-expression of PD-1 and Lag-3 on CD8+ (gated on live, lymphocytes, B220neg, NK1.1neg, CD8+), CD4+ (gated on live, lymphocytes, B220neg, NK1.1neg, CD4+) and regulatory (Tregs; gated on live, lymphocytes, B220neg, NK1.1neg, CD4+, FoxP3+) T cells from spleens of mice infected with LCMV Cl-13 (day 30) or the tumors and spleens of mice bearing PDA tumors (day 14).
(C) Representative histograms and quantification of PD-L1 expression on tumor cells, dendritic cells (DC), and macrophages (Mac) in subcutaneous PDA tumors or spleens from the same mice (day 14), gated as in Figure 1B. (MFI=mean fluorescence intensity). ****p≤ 0.0001. See also Supplementary Fig. S2.
(D) Histogram of KPC-derived PDA cell line interrogated for PD-L1 expression in vitro with or without IFNγ in the culture, representative of 3 experiments.
(E) Quantification and MFI of PD-L1 expression on tumor cells from subcutaneous PDA tumors established in either C57BL/6 (B6) or IFNγ−/− (IFNγ ko) mice with or without CD4+ and CD8+ T-cell depletion (TCD) (day 16; n=6-8 mice per cohort).
(F) Quantification and MFI of PD-L1 expression on dendritic cells and macrophages in subcutaneous PDA tumors grown in either B6 or IFN-γ ko mice with or without TCD (day 16; n=6-8 mice per cohort). One-way ANOVA: %DCs PD-L1+, p=0.015; DC PD-L1 MFI, p=0.0039; %Macs PD-L1+, p=0.58; Macs PD-L1 MFI, p=0.0007. Post hoc test p values are indicated where statistically significant as *p≤ 0.05, **p≤ 0.01.
In the subcutaneous PDA model, about 60% to 70% of tumor cells isolated from established tumors expressed PD-L1 (Fig. 2C), similar to the expression of PD-L1 on this cell line grown in vitro (Fig. 2D). These findings were confirmed using a YFP+ tumor cell line established from a pancreatic tumor isolated from a KPC-Y genetically engineered mouse; in this model, YFP serves as a validated lineage tracer for pancreatic epithelium (46). After subcutaneous tumor implantation and growth in syngeneic hosts, we found that on average 66.7% of YFP+ tumors cells expressed PD-L1, as measured by flow cytometry (Supplementary Fig. S2). Moreover, high levels of PD-L1 on both DCs and macrophages were observed in the tumor microenvironment of the KPC subcutaneous tumors (Fig. 2C), mirroring PD-L1 expression on these APC subsets in spontaneous tumors of KPC mice. Both a higher percentage of PD-L1+ APCs and a higher (~3-4-fold) mean fluorescence intensity (MFI) of PD-L1 was observed compared to that of the corresponding APC populations in the spleens of the same mice (Fig. 2C). These data indicate that PD-L1 expression is prevalent in the PDA microenvironment.
Tumor PD-L1 expression in PDA is not IFNγ-dependent
PD-L1 expression in human melanoma and HNSCC correlates spatially with T-cell infiltration (33,35), and in melanoma, tumor expression of PD-L1 is dynamically upregulated in response to IFNγ secreted by infiltrating CD8+ T cells (36). To determine whether this same mechanism is responsible for PD-L1 expression in PDA, we assessed the ability of our PDA cell line to upregulate PD-L1 in response to IFNγ; in vitro, IFNγ stimulation resulted in increased expression of PD-L1 by PDA cells (Fig. 2D). In vivo, we evaluated tumor and APC PD-L1 expression in the presence or absence of T cells and IFNγ. Subcutaneous PDA tumors were established in mice that were genetically lacking IFNγ, systemically depleted of CD4+ and CD8+ T cells, or both. Tumor growth rate in vivo was the same for each condition compared to that of control (data not shown). Analysis of these tumors showed no significant change in tumor PD-L1 expression (either percentage or MFI) with regard to IFNγ or T-cell status (Fig. 2E). Analysis of the APC populations in these tumors indicated that IFNγ plays a minor role in the regulation of PD-L1 expression on intratumoral DCs and macrophages. Small but statistically significant differences were observed in the percentage and MFI of PD-L1 expression on intratumoral APCs between IFNγ-sufficient and IFNγ-deficient hosts (Fig. 2F). In contrast, the presence or absence of T cells did not affect PD-L1 expression by APCs regardless of host IFNγ status (Fig. 2F), recapitulating the lack of correspondence between CD8+ T cells and PD-L1 expression in human PDA (Fig. 1C).
T-cell stimulation with CD40/gemcitabine/nab-paclitaxel converts PDA from being fully refractory to highly sensitive to checkpoint blockade
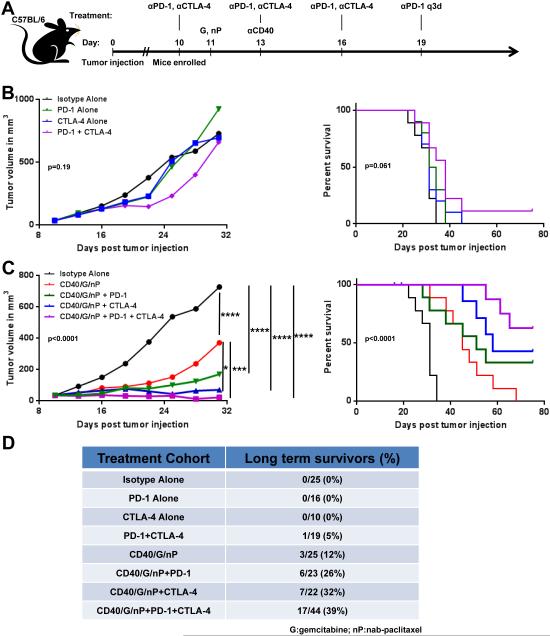
We then tested the antitumor in vivo efficacy of PD-1-blocking mAbs either with or without CTLA-4 blocking mAbs (Fig. 3A). CTLA-4 is expressed at higher levels on intratumoral CD8+ and CD4+ T-cell populations (including Treg) when compared to that of splenic populations, suggesting that blockade of this negative checkpoint may improve antitumor immunity (Supplementary Fig. S3). Even with αCTLA-4, αPD-1 did not impact tumor growth or survival (Fig. 3B), even though a comparable αPD-1 dosing schedule reproducibly improves clinical outcomes in mice chronically infected with LCMV clone 13 (50,51). This lack of antitumor efficacy is similar to the lack of responses observed to date in patients with advanced PDA treated with αPD-L1 or αCTLA-4 (12,30,31).
Figure 3. T-cell stimulation with αCD40/gemcitabine/nab-paclitaxel potentiates efficacy of checkpoint blockade in murine model of PDA.
(A) Experimental design for experiments of subcutaneous PDA tumors treated with checkpoint inhibitors and αCD40/chemotherapy, as further described in Materials and Methods. (G=gemcitabine; nP=nab-paclitaxel; q3d= antibody administered every 3 days).
(B) Tumor growth and survival analyses of mice bearing subcutaneous PDA tumors treated as indicated (n=9-10 per cohort; results for control and αPD-1+αCTLA-4 cohorts representative of 3 independent experiments). See also Supplementary Fig. S7.
(C) Tumor growth and survival analyses of mice bearing subcutaneous PDA tumors treated as indicated (n=9-10 per cohort; findings representative of 3 independent experiments). Two-way ANOVA: p≤0.0001. Post hoc test p values indicated where statistically significant as *p≤ 0.05, ***p≤ 0.001, ****p≤ 0.0001. See also Supplementary Fig. S7.
(D) Percentage of mice bearing subcutaneous PDA tumors treated with indicated regimens that rejected their tumors and survived tumor-free long-term (median follow-up of 42 days, range 23 to 222 days). Data compiled from 5 independent experiments.
These same reagents have shown efficacy in patients with other malignancies; one possible distinction may be the presence of an antitumor immune response at baseline in subsets of these patients (28,52). We therefore hypothesized that the induction of a T-cell response would be required to overcome refractoriness to αPD-1 and αCTLA-4 in PDA and achieve clinical benefit. Agonist αCD40 antibody facilitates cancer vaccines (53) and can synergize with chemotherapy-induced immunogenic cell death to initiate a T cell-dependent antitumor regression, providing a vaccine effect in model systems for which a tumor-rejection antigen is not characterized (45,54). APCs in KPC-derived subcutaneous tumors express CD40 (Supplementary Fig. S4), as we have previously shown (42). Here, we studied gemcitabine and nab-paclitaxel because this combination was recently approved by the FDA for the treatment of metastatic PDA (3), and gemcitabine has been shown to cooperate immunologically with αCD40 (45). Treatment of mice with established subcutaneous PDA tumors with αCD40/chemotherapy altered the phenotype of tumor-infiltrating T cells although the percent of T cells infiltrating the tumors did not change. There were statistically significantly fewer CD8+ T cells that co-expressed the inhibitory PD-1 and Lag-3 markers in treated tumors and more proliferating CD4+ and CD8+ T cells were found in the tumors of treated mice compared to that of controls (Supplementary Fig. S5).
The combination of gemcitabine and nab-paclitaxel at the maximum tolerated dose did not induce regression of established subcutaneous PDA tumors; however, the addition of αCD40 to this chemotherapy regimen inhibited tumor growth and improved survival compared to control-treated tumor-bearing mice (Fig. 3C). These effects were macrophage-independent as CEL failed to abrogate the effect (Supplementary Fig. S6). Given that we have previously observed that αCD40 plus chemotherapy in the subcutaneous KPC model manifests an antitumor effect that is T-cell dependent (55), we added αPD-1, αCTLA-4, or both to treatment with αCD40/chemotherapy in an effort to enhance T-cell immunity. The addition of αPD-1, αCTLA-4, or both to αCD40/chemotherapy enhanced tumor growth inhibition, and led to an increase in survival in mice bearing subcutaneous PDA tumors (Fig. 3C). Moreover, these combinations led to complete rejection of established tumors and long-term tumor-free survival in significant proportions of mice treated with the combined regimen (Fig. 3D). Treatment with αPD-1 and αCTLA-4 did not alter CD40 expression on APCs in the tumor microenvironment (Supplementary Fig. S4). The highest rates of tumor regression were observed in mice treated with both αPD-1 and αCTLA-4, with 39% (17 of 44) of mice achieving long-term complete remission and survival after treatment with all three antibodies plus chemotherapy (Fig. 3D). Tumor growth was delayed in nearly all mice treated with αCD40/chemotherapy and αPD-1/αCTLA-4, even in those mice not completely rejecting their tumors, suggesting that the tumor response rate is even higher than the tumor rejection rate in this model (Supplementary Fig. S7). Although treatment was well tolerated in the vast majority of mice, in 6.3% of mice treated with αCD40/chemotherapy and at least one checkpoint blocking mAb we noted clinical deterioration consistent with an infectious syndrome (Supplementary Fig. S8).
Rejection of PDA tumors by αCD40/chemotherapy and checkpoint blockade is T cell-mediated
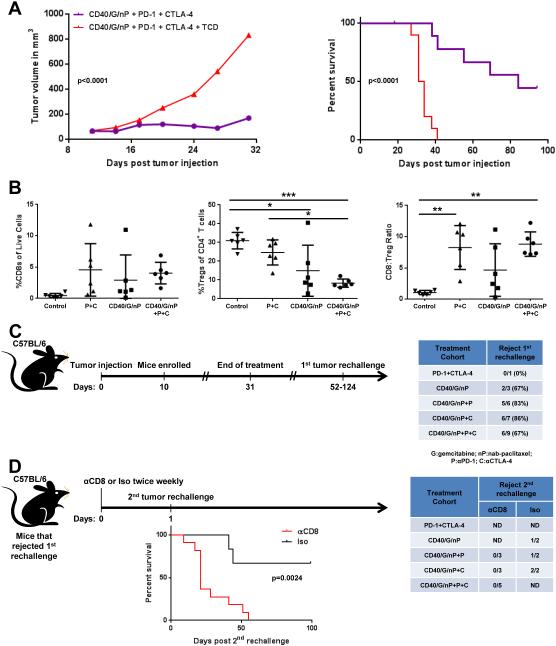
To determine whether the antitumor effect we observed was T cell-mediated, we repeated the study with a cohort of mice depleted of CD4+ and CD8+ T cells, starting on the day prior to the initiation of therapy. In the absence of T cells, the treatment did not inhibit tumor growth or afford survival advantage, and no T cell-depleted mice rejected the tumor or survived long-term (Fig. 4A).
Figure 4. Rejection of PDA tumors after αCD40/chemotherapy and checkpoint blockade is T cell-mediated.
(A) Tumor growth and survival analyses of mice bearing subcutaneous PDA tumors treated as indicated (n=9-10 per cohort; G=gemcitabine; nP=nab-paclitaxel; TCD=CD4/CD8 depletion).
(B) Flow cytometric analysis of subcutaneous PDA tumors treated as indicated (day 18 after tumor injection, day 7 after αCD40 treatment; P=αPD-1; C=αCTLA-4). One way ANOVA %CD8s of live cells: p=0.17; one-way ANOVA %Tregs of CD4+ T cells: p=0.0004; one-way ANOVA CD8:Treg Ratio: p=0.0005. Post hoc test p values indicated where statistically significant as *p≤ 0.05, **p≤ 0.01, ***p≤ 0.001.
(C) Experimental design for 1st tumor rechallenge experiments. Table quantifies fraction and percentage of mice that rejected tumor rechallenge in mice that had rejected the initial tumor implantation and were tumor-free for at least 43 days. Data compiled from 3 independent experiments.
(D) Experimental design for 2nd tumor rechallenge experiment. The 2nd rechallenge occurred on day 31-49 after the first rechallenge. Table quantifies fraction and percentage of mice that rejected the 2nd tumor rechallenge in mice that had rejected a 1st tumor rechallenge. Host mice in this experiment were either treated with αCD8 (n=11) or isotype (Iso; n=6) antibodies. Survival analysis of mice after the 2nd rechallenge with or without CD8 depletion is shown. Data compiled from 2 independent experiments.
To understand the effect of our treatment on intratumoral T-cell populations, we treated cohorts of tumor-bearing mice with αPD-1/αCTLA-4, αCD40/chemotherapy, both, or neither (control), and sacrificed mice one week after treatment with αCD40 (or control) to analyze tumors for T-cell infiltration. Tumors from mice treated with αPD-1/αCTLA-4 plus αCD40/chemotherapy had a significantly increased (7-fold) CD8:Treg ratio compared to that of control-treated mice (Fig. 4B). This phenotype was also seen in some of the mice treated with αCD40/chemotherapy or αPD-1/αCTLA-4, although neither one of these two groups exhibited as consistent an increase in the CD8:Treg ratio as the mice treated with αPD-1/αCTLA-4 plus αCD40/chemotherapy (Fig. 4B). The CTLA-4 mAb clone 9H10 partly mediates its antitumor effect by depletion of Tregs, which express CTLA-4 (24); however, we observed that mice treated with αPD-1/αCTLA-4 alone did not have a significantly decreased percentage of Tregs among CD4+ T cells (Fig. 4B) or among total CD45+ cells. Rather, the administration of αCD40/chemotherapy (either with or without αPD-1/αCTLA-4) was associated with a significant decrease in Treg percentages compared to that of control treated mice; all groups treated with immunotherapy demonstrated a slight increase in the CD8+ T-cell infiltrate, although the changes were not statistically significant (Fig. 4B). These data suggest that αCD40/chemotherapy changes the immune microenvironment in this PDA model and leads to a decreased percentage of Tregs and increased CD8:Treg ratio, an effect that is augmented further with the addition of checkpoint blockade. The greatest changes in Treg percentage and CD8:Treg ratio were associated with the highest rates of complete remission and long-term survival across cohorts reported in Fig. 3D.
To test whether mice that had completely rejected established PDA tumors had developed immune memory, we rechallenged cohorts of mice that were in long-term complete remission with the same number of cells of the same PDA tumor line but on the opposite flank (Fig. 4C). We observed that 67% to 86% of such mice rejected the PDA tumor cells implanted on the opposite flank without any additional therapy (Fig. 4C), consistent with those mice having developed immunologic memory. Because the most likely effector memory T-cell population mediating this effect is a CD8+ T cell, we further studied mice that had rejected both the initial tumor and the first rechallenge on the opposite flank, and either depleted these mice of CD8+ T cells or administered an isotype control antibody that did not deplete CD8+ T cells. All mice were then rechallenged with the same number of cells of the same cell line on the original flank. All mice depleted of CD8+ T cells rapidly developed progressively growing tumors at the site of the second rechallenge, whereas 4 of 6 isotype-treated mice rejected this second tumor rechallenge (Fig. 4D). This effect translated into a statistically significant difference in overall survival after the second rechallenge (Fig. 4D).
αCD40/chemotherapy cooperates with PD-1 blockade to improve survival of mice with established tumors in the KPC genetic model of PDA
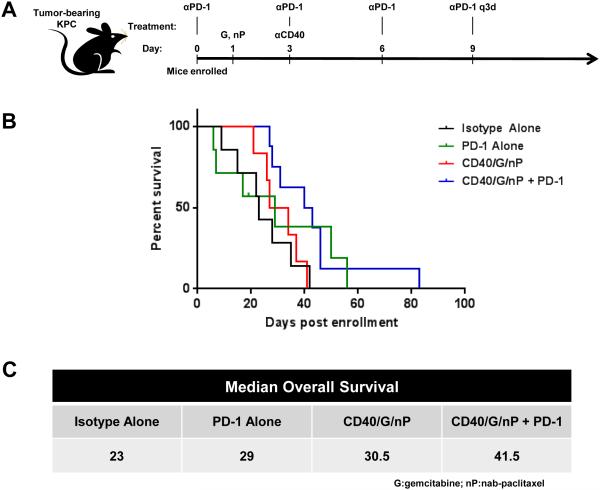
Having observed that the induction of T-cell immunity via αCD40/chemotherapy potentiates the efficacy of checkpoint inhibitors in the subcutaneous model of PDA, we then tested this approach in the autochthonous KPC model of PDA. Observations in the KPC model have previously been shown to predict clinical responses in PDA patients treated with the same or homologous agent (42,56-58). We therefore performed a randomized, controlled study of checkpoint inhibition in combination with αCD40/chemotherapy in cohorts of tumor-bearing KPC mice. Given the striking expression of PD-1 and PD-L1 in the KPC tumor microenvironment, we chose to test our hypothesis using the αPD-1 mAb. Mice diagnosed with pancreatic tumors of 30 mm3-150 mm3 were randomized to treatment with αCD40 plus gemcitabine/nab-paclitaxel, αPD-1, αCD40/chemotheray plus αPD-1, or control (as described in Materials and Methods and summarized in Fig. 5A), using the same dose and schedule as used for mice in the subcutaneous PDA studies. We observed a statistically significant increase in overall survival for mice receiving αCD40/chemotherapy plus αPD-1 compared to that of control (p=0.015, log-rank Mantel-Cox) (Fig. 5B). The effect was large: combination treatment nearly doubled the median overall survival from 23 days in the control arm to 41.5 days in the experimental arm with a hazard ratio of 0.334 (0.0584-0.657, 95% confidence interval). Neither PD-1 alone nor αCD40/chemotherapy significantly improved overall survival. These data suggest that as predicted by our findings in the subcutaneous PDA model, the induction of a T-cell response is needed for the αPD-1 antitumor effects in PDA.
Figure 5. Combination of αCD40/chemotherapy and PD-1 blockade improves survival in KPC genetic model of PDA.
(A) Experimental design for randomized, controlled study in tumor-bearing KPC mice, treated with αCD40/chemotherapy and αPD-1, as described in Materials and Methods. G=gemcitabine; nP=nab-paclitaxel; q3d= antibody administered every 3 days.
(B) Overall survival analysis of tumor-bearing KPC mice treated as indicated (n=6-8 per cohort). αPD-1 alone vs. isotype alone p=0.39; CD40/G/nP vs. isotype alone p=0.76; CD40/G/nP + αPD-1 vs. isotype alone p=0.015.
(C) Median overall survival of tumor-bearing KPC mice as indicated.
DISCUSSION
The clinical success of checkpoint inhibitors, including FDA approval of ipilimumab and pembrolizumab for melanoma, has prompted investigations to replicate these results more broadly in oncology. Early findings, however, suggest that many tumors are resistant, with pancreatic carcinoma appearing completely refractory to monotherapy with checkpoint blockade (12,30,31). Here, using a genetically engineered mouse model of PDA, which like human PDA exhibits minimal spontaneous immunity, we demonstrate that despite robust expression of PD-1 and PD-L1 in the tumor microenvironment, treatment with αPD-1 with or without αCTLA-4 has minimal antitumor impact, replicating that in PDA patients treated with analogous agents (12,30,31). However, in the context of αCD40/chemotherapy, we demonstrate that the induction of T-cell immunity converts PDA from a tumor that is completely refractory to αPD-1 and/or αCTLA-4 into one in which checkpoint blockade controls tumor growth and significantly improves survival in a CD8+ T cell-dependent manner. In particular, the combined regimen of αCD40/chemotherapy plus αPD-1 nearly doubles the median overall survival in genetically engineered KPC mice with pre-established spontaneous pancreatic tumors. Moreover, the capability of the treated mice to reject second and third subcutaneous tumor challenges in a CD8+ T cell-dependent fashion thereby rendering long-term survival, suggests that the combined regimen induced the establishment of antitumor immune memory with curative potential. These findings indicate that poorly immunogenic tumors, epitomized by the KPC pancreatic tumor model, can nevertheless be controlled by the adaptive immune system provided a dual approach of therapeutic T-cell induction and checkpoint blockade is utilized.
Immunologically, the PDA tumor microenvironment is considered especially suppressive, but increasingly, there is an appreciation from studies in KPC and other PDA models of an underlying sensitivity of PDA tumor cells to T-cell cytotoxicity (59). Unlike melanoma, PDA does not commonly present with a robust tumor infiltration of CD8+ T cells (60-63). In genetically engineered mouse models of PDA, a prominent network of immunosuppression is dominant even at the earliest stages of disease (40-43,64). We demonstrated that PD-1 is as prominent in the KPC tumor microenvironment as it is systemically in mice chronically infected with LCMV (50). We propose therefore, that the lack of responses to treatment with checkpoint inhibitors in KPC mice likely reflects a tumor microenvironment without an underlying antitumor T-cell response.
The lack of PDA immunogenicity does not necessarily indicate an inherent lack of antigenicity of PDA tumors cells; indeed, PDA cells might be unexpectedly sensitive to T-cell killing because they have not been exposed to Darwinian-like T-cell selective pressure in vivo. Without T-cell pressure, T-cell escape and classical immunoediting may not be necessary for pancreatic tumor growth as it is for highly immunogenic tumors (4,59). Thus, in this study we interpret the antitumor effects of αCD40/chemotherapy plus αPD-1/αCTLA-4 as a strategy that overcomes acquired immune privilege in PDA. Other pathways and cells in the PDA tumor microenvironment may also be “targetable” as part of novel immunotherapeutic approaches (43,65,66).
Despite the 80% increased overall survival observed in KPC mice treated with αCD40/chemotherapy and αPD-1 compared to that of the controls, all mice succumbed to their disease. It is worth noting that there are no published reports of cures of KPC mice bearing established invasive tumors. A few groups have reported improved overall survival (without cures) with treatment in this model, including the recent demonstration that the vitamin D analogue calcipotriol improves survival by 57% (57,67,68). Given the difference we observed in the response to treatment between the subcutaneous and KPC PDA models, we hypothesize that there is additional complexity in the tumor microenvironment of spontaneous KPC tumors which limits therapeutic responses. Potential other immunosuppressive pathways contributing to treatment resistance include myeloid-derived suppressor cells (MDSC), macrophages, and fibroblast-activating protein+ (FAP+) mesenchymal cells, among others (43,65,66,69).
Our observations that αCD40/chemotherapy converts PDA from a tumor fully refractory to checkpoint inhibition to one that is sensitive are important in the context of prior efforts to extend the therapeutic range of αPD-1 and αCTLA-4. Our goal was to use a murine model that reproduces the lack of clinical effect observed to date with αPD-1 and αCTLA-4 in PDA, in contrast to many tumor models that exhibit baseline levels of responsiveness to αCTLA-4, αPD-1, αPD-L1 or combinations of these agents. For example, in models of colon carcinoma, melanoma, ovarian cancer, bladder cancer, and neuroblastoma, checkpoint therapy alone inhibits tumor growth, improves survival, and occasionally mediates complete rejection (21,70-73). In studies using the Panc02 subcutaneous PDA model, tumor rejection was observed in 50% of mice after treatment with αCTLA-4 (74), and treatment with αPD-L1 (with or without gemcitabine) leads to significant decreases in tumor growth (75), findings not representative of the clinical record of these agents in patients with PDA (12,30,31) and possibly related to Panc02 being a carcinogen-induced and likely hypermutated tumor [whereas human PDA is not a hypermutated tumor (76)]. Previous work in these types of models demonstrates that T-cell stimulatory therapies can improve baseline effects of checkpoint blockade (21,27,37,38). In PDA, the stimulation of a T-cell response using αCD40/chemotherapy is able to transform a tumor that is refractory to checkpoint inhibition into a sensitive one, rather than only improving upon baseline activity of checkpoint mAbs.
In the absence of a defined tumor antigen in our KPC model, we therapeutically induced T cells with chemotherapy followed by an agonist αCD40 (45). Although other agents may also synergize with αCD40 (77), gemcitabine in particular cooperates with αCD40 (45). Here, we added nab-paclitaxel given the recent regulatory clinical approval of the combination. We have previously demonstrated in KPC mice with spontaneous tumors that αCD40 can reprogram macrophages to mediate (T cell-independent) stromal involution and short-term decreases in tumor volume without improvement in overall survival (42); here, we found that a one-time treatment with chemotherapy followed by αCD40 enabled a macrophage-independent T-cell response, engendering immune memory and durable complete remissions in a large fraction of mice harboring subcutaneous PDA tumors – and extending survival in KPC mice with spontaneous tumors. Both the use of nab-paclitaxel and the subcutaneous setting may be responsible for the differences in these observations, the subject of current investigations. Although of interest, we could not evaluate in Fc receptor-null mice whether Treg changes from αPD-1/αCTLA-4 were Fc receptor-dependent because the effects of agonistic αCD40 are lost in such mice (78).
In certain human cancers, tumor cell PD-L1 expression co-localizes with lymphocytic immune infiltrates, suggesting adaptive resistance by the tumor and the potential root of sensitivity to αPD-1 (33-35,79). In the case of melanoma, tumor cell PD-L1 expression has been demonstrated to be dependent on CD8+ T cells and the secretion of IFNγ (36). In contrast, we found in our PDA mouse models harboring minimal intratumoral T cells, tumor cells express PD-L1 at moderate levels and tumor-associated DCs and macrophages express high levels of this inhibitory ligand. We further observed that PD-L1 expression in murine PDA is not dependent on T cells or IFNγ, indicating that PD-L1 tumor expression does not appear to be an adaptive response to immune pressure. These findings in the KPC model are corroborated by our observations in human PDA in which there was no spatial correlation between tumor PD-L1 expression and the presence of intratumoral CD8+ T cells. Tumor PD-L1 expression has been reported to be regulated by oncogenes such as EGFR (80), suggesting that the regulation of PD-L1 in PDA may differ from the regulation of PD-L1 in other solid malignancies.
In summary, induction of T-cell immunity reduces resistance to PD-1 and CTLA-4 blockade and improves survival in pancreatic carcinoma. It is notable that four out of the five reagents that we used in these studies have an FDA-approved human homologue (gemcitabine, nab-paclitaxel, αPD-1, αCTLA-4) which should facilitate clinical translation.
Supplementary Material
ACKNOWLEDGEMENTS
RW designed study concept, designed and performed experiments, analyzed data, and wrote and edited the manuscript. KTB, RAE, PMO, ARLM, DLB, and CC designed and performed experiments, analyzed data, and edited the manuscript. BZS, EEF and EJW designed experiments, analyzed data, and edited the manuscript. RHV designed study concept, designed experiments, analyzed data, wrote and edited the manuscript, and supervised the study. We thank Amy Ziober, Michael Feldman, Erin Dekleva, Tim Chao, Andrew Rech, Mark Diamond, Steve Albelda, Jim Riley, Ellen Pure, and Anil Rustgi (Penn) and Dafna Bar-Sagi (New York University) for helpful discussions.
Funding: NIH grants: R01 CA169123 (R.H.V. and B.Z.S.), T32 CA009140 (R.W.), T32 HL007439 (K.T.B.), T32 HL007775 (D.L.B), P30 CA016520 (R.H.V.), U19 AI 082630, P01 AI112521 (E.J.W.)
Stand Up To Cancer (R.H.V.)
Pancreatic Action Cancer Network-AACR (R.H.V.)
Translational Center of Excellence in Pancreatic Cancer of the Abramson Cancer Center (R.H.V., C.C., E.E.F.)
Footnotes
The authors declare no conflict of interest.
REFERENCES
- 1.Rahib L, Smith BD, Aizenberg R, Rosenzweig AB, Fleshman JM, Matrisian LM. Projecting cancer incidence and deaths to 2030: the unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res. 2014;74:2913–21. doi: 10.1158/0008-5472.CAN-14-0155. [DOI] [PubMed] [Google Scholar]
- 2.Conroy T, Desseigne F, Ychou M, Bouché O, Guimbaud R, Bécouarn Y, et al. FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. N Engl J Med. 2011;364:1817–25. doi: 10.1056/NEJMoa1011923. [DOI] [PubMed] [Google Scholar]
- 3.Hoff von DD, Ervin T, Arena FP, Chiorean EG, Infante J, Moore M, et al. Increased survival in pancreatic cancer with nab-paclitaxel plus gemcitabine. N Engl J Med. 2013;369:1691–703. doi: 10.1056/NEJMoa1304369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Schreiber RD, Old LJ, Smyth MJ. Cancer immunoediting: integrating immunity's roles in cancer suppression and promotion. Science. 2011;331:1565–70. doi: 10.1126/science.1203486. [DOI] [PubMed] [Google Scholar]
- 5.Odorizzi PM, Wherry EJ. Inhibitory receptors on lymphocytes: insights from infections. J Immunol. 2012;188:2957–65. doi: 10.4049/jimmunol.1100038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Sznol M, Chen L. Antagonist antibodies to PD-1 and B7-H1 (PD-L1) in the treatment of advanced human cancer. Clin Cancer Res. 2013;19:1021–4. doi: 10.1158/1078-0432.CCR-12-2063. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Page DB, Postow MA, Callahan MK, Allison JP, Wolchok JD. Immune Modulation in Cancer with Antibodies. Annu Rev Med. 2014;65:185–202. doi: 10.1146/annurev-med-092012-112807. [DOI] [PubMed] [Google Scholar]
- 8.Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat. Rev. Cancer. 2012;12:252–64. doi: 10.1038/nrc3239. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Powles T, Eder JP, Fine GD, Braiteh FS, Loriot Y, Cruz C, et al. MPDL3280A (anti-PD-L1) treatment leads to clinical activity in metastatic bladder cancer. Nature. 2014;515:558–62. doi: 10.1038/nature13904. [DOI] [PubMed] [Google Scholar]
- 10.Herbst RS, Soria J, Kowanetz M, Fine GD, Hamid O, Gordon MS, et al. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature. 2014;515:563–7. doi: 10.1038/nature14011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Hodi FS, O'Day SJ, McDermott DF, Weber RW, Sosman JA, Haanen JB, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010;363:711–23. doi: 10.1056/NEJMoa1003466. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Brahmer JR, Tykodi SS, Chow LQM, Hwu W, Topalian SL, Hwu P, et al. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med. 2012;366:2455–65. doi: 10.1056/NEJMoa1200694. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med. 2012;366:2443–54. doi: 10.1056/NEJMoa1200690. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Hamid O, Robert C, Daud A, Hodi FS, Hwu W, Kefford R, et al. Safety and tumor responses with lambrolizumab (anti-PD-1) in melanoma. N Engl J Med. 2013;369:134–44. doi: 10.1056/NEJMoa1305133. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Blackburn SD, Shin H, Haining WN, Zou T, Workman CJ, Polley A, et al. Coregulation of CD8+ T cell exhaustion by multiple inhibitory receptors during chronic viral infection. Nat Immunol. 2009;10:29–37. doi: 10.1038/ni.1679. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Crawford A, Angelosanto J, Kao C, Doering T, Odorizzi P, Barnett B, et al. Molecular and transcriptional basis of CD4+ T cell dysfunction during chronic infection. Immunity. 2014;40:289–302. doi: 10.1016/j.immuni.2014.01.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Nishimura H, Okazaki T, Tanaka Y, Nakatani K, Hara M, Matsumori A, et al. Autoimmune dilated cardiomyopathy in PD-1 receptor-deficient mice. Science. 2001;291:319–22. doi: 10.1126/science.291.5502.319. [DOI] [PubMed] [Google Scholar]
- 18.Keir ME, Butte MJ, Freeman GJ, Sharpe AH. PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol. 2008;26:677–704. doi: 10.1146/annurev.immunol.26.021607.090331. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Curiel TJ, Wei S, Dong H, Alvarez X, Cheng P, Mottram P, et al. Blockade of B7-H1 improves myeloid dendritic cell-mediated antitumor immunity. Nat Med. 2003;9:562–7. doi: 10.1038/nm863. [DOI] [PubMed] [Google Scholar]
- 20.Dong H, Strome SE, Salomao DR, Tamura H, Hirano F, Flies DB, et al. Tumor-associated B7-H1 promotes T-cell apoptosis: a potential mechanism of immune evasion. Nat Med. 2002;8:793–800. doi: 10.1038/nm730. [DOI] [PubMed] [Google Scholar]
- 21.Duraiswamy J, Kaluza KM, Freeman GJ, Coukos G. Dual blockade of PD-1 and CTLA-4 combined with tumor vaccine effectively restores T-cell rejection function in tumors. Cancer Res. 2013;73:3591–603. doi: 10.1158/0008-5472.CAN-12-4100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Tivol EA, Borriello F, Schweitzer AN, Lynch WP, Bluestone JA, Sharpe AH. Loss of CTLA-4 leads to massive lymphoproliferation and fatal multiorgan tissue destruction, revealing a critical negative regulatory role of CTLA-4. Immunity. 1995;3:541–7. doi: 10.1016/1074-7613(95)90125-6. [DOI] [PubMed] [Google Scholar]
- 23.Peggs KS, Quezada SA, Chambers CA, Korman AJ, Allison JP. Blockade of CTLA-4 on both effector and regulatory T cell compartments contributes to the antitumor activity of anti-CTLA-4 antibodies. J Exp Med. 2009;206:1717–25. doi: 10.1084/jem.20082492. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Simpson TR, Li F, Montalvo-Ortiz W, Sepulveda MA, Bergerhoff K, Arce F, et al. Fc-dependent depletion of tumor-infiltrating regulatory T cells co-defines the efficacy of anti-CTLA-4 therapy against melanoma. J Exp Med. 2013;210:1695–710. doi: 10.1084/jem.20130579. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Selby MJ, Engelhardt JJ, Quigley M, Henning KA, Chen T, Srinivasan M, Korman AJ. Anti-CTLA-4 antibodies of IgG2a isotype enhance antitumor activity through reduction of intratumoral regulatory T cells. Cancer Immunol Res. 2013;1:32–42. doi: 10.1158/2326-6066.CIR-13-0013. [DOI] [PubMed] [Google Scholar]
- 26.Kvistborg P, Philips D, Kelderman S, Hageman L, Ottensmeier C, Joseph-Pietras D, et al. Anti-CTLA-4 therapy broadens the melanoma-reactive CD8+ T cell response. Sci Transl Med. 2014;6:254ra128. doi: 10.1126/scitranslmed.3008918. [DOI] [PubMed] [Google Scholar]
- 27.Zamarin D, Holmgaard RB, Subudhi SK, Park JS, Mansour M, Palese P, et al. Localized oncolytic virotherapy overcomes systemic tumor resistance to immune checkpoint blockade immunotherapy. Sci Transl Med. 2014;6:226ra32. doi: 10.1126/scitranslmed.3008095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Gajewski TF, Louahed J, Brichard VG. Gene signature in melanoma associated with clinical activity: a potential clue to unlock cancer immunotherapy. Cancer J. 2010;16:399–403. doi: 10.1097/PPO.0b013e3181eacbd8. [DOI] [PubMed] [Google Scholar]
- 29.Ji R, Chasalow SD, Wang L, Hamid O, Schmidt H, Cogswell J, et al. An immune-active tumor microenvironment favors clinical response to ipilimumab. Cancer Immunol Immunother. 2011;61:1019–31. doi: 10.1007/s00262-011-1172-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Royal RE, Levy C, Turner K, Mathur A, Hughes M, Kammula US, et al. Phase 2 trial of single agent Ipilimumab (anti-CTLA-4) for locally advanced or metastatic pancreatic adenocarcinoma. J Immunother. 2010;33:828–33. doi: 10.1097/CJI.0b013e3181eec14c. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Le DT, Lutz E, Uram JN, Sugar EA, Onners B, Solt S, et al. Evaluation of ipilimumab in combination with allogeneic pancreatic tumor cells transfected with a GM-CSF gene in previously treated pancreatic cancer. J Immunother. 2013;36:382–9. doi: 10.1097/CJI.0b013e31829fb7a2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Wolchok JD, Kluger H, Callahan MK, Postow MA, Rizvi NA, Lesokhin AM, et al. Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med. 2013;369:122–33. doi: 10.1056/NEJMoa1302369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Taube JM, Anders RA, Young GD, Xu H, Sharma R, McMiller TL, et al. Colocalization of inflammatory response with B7-h1 expression in human melanocytic lesions supports an adaptive resistance mechanism of immune escape. Sci Transl Med. 2012;4:127ra37. doi: 10.1126/scitranslmed.3003689. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Taube JM, Klein A, Brahmer JR, Xu H, Pan X, Kim JH, et al. Association of PD-1, PD-1 ligands, and other features of the tumor immune microenvironment with response to anti-PD-1 therapy. Clin Can Res. 2014;20:5064–74. doi: 10.1158/1078-0432.CCR-13-3271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Lyford-Pike S, Peng S, Young GD, Taube JM, Westra WH, Akpeng B, et al. Evidence for a role of the PD-1:PD-L1 pathway in immune resistance of HPV-associated head and neck squamous cell carcinoma. Cancer Res. 2013;73:1733–41. doi: 10.1158/0008-5472.CAN-12-2384. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Spranger S, Spaapen RM, Zha Y, Williams J, Meng Y, Ha TT, et al. Up-regulation of PD-L1, IDO, and T(regs) in the melanoma tumor microenvironment is driven by CD8(+) T cells. Sci Transl Med. 2013;5:200ra116. doi: 10.1126/scitranslmed.3006504. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Bald T, Landsberg J, Lopez-Ramos D, Renn M, Glodde N, Jansen P, et al. Immune cell-poor melanomas benefit from PD-1 blockade after targeted type I IFN activation. Cancer Discov. 2014;4:674–87. doi: 10.1158/2159-8290.CD-13-0458. [DOI] [PubMed] [Google Scholar]
- 38.Zhou Q, Xiao H, Liu Y, Peng Y, Hong Y, Yagita H, et al. Blockade of programmed death-1 pathway rescues the effector function of tumor-infiltrating T cells and enhances the antitumor efficacy of lentivector immunization. J Immunol. 2010;185:5082–92. doi: 10.4049/jimmunol.1001821. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Hingorani SR, Wang L, Multani AS, Combs C, Deramaudt TB, Hruban RH, et al. Trp53R172H and KrasG12D cooperate to promote chromosomal instability and widely metastatic pancreatic ductal adenocarcinoma in mice. Cancer Cell. 2005;7:469–83. doi: 10.1016/j.ccr.2005.04.023. [DOI] [PubMed] [Google Scholar]
- 40.Clark CE, Hingorani SR, Mick R, Combs C, Tuveson DA, Vonderheide RH. Dynamics of the immune reaction to pancreatic cancer from inception to invasion. Cancer Res. 2007;67:9518–27. doi: 10.1158/0008-5472.CAN-07-0175. [DOI] [PubMed] [Google Scholar]
- 41.Clark CE, Beatty GL, Vonderheide RH. Immunosurveillance of pancreatic adenocarcinoma: insights from genetically engineered mouse models of cancer. Cancer Lett. 2008;279:1–7. doi: 10.1016/j.canlet.2008.09.037. [DOI] [PubMed] [Google Scholar]
- 42.Beatty GL, Chiorean EG, Fishman MP, Saboury B, Teitelbaum UR, Sun W, et al. CD40 agonists alter tumor stroma and show efficacy against pancreatic carcinoma in mice and humans. Science. 2011;331:1612–6. doi: 10.1126/science.1198443. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Bayne L, Beatty G, Jhala N, Clark C, Rhim A, Stanger B, et al. Tumor-derived granulocyte-macrophage colony-stimulating factor regulates myeloid inflammation and T cell immunity in pancreatic cancer. Cancer Cell. 2012;21:822–35. doi: 10.1016/j.ccr.2012.04.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Elgueta R, Benson MJ, de Vries VC, Wasiuk A, Guo Y, Noelle RJ. Molecular mechanism and function of CD40/CD40L engagement in the immune system. Immunol Rev. 2009;229:152–72. doi: 10.1111/j.1600-065X.2009.00782.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Nowak AK, Robinson BWS, Lake RA. Synergy between chemotherapy and immunotherapy in the treatment of established murine solid tumors. Cancer Res. 2003;63:4490–6. [PubMed] [Google Scholar]
- 46.Rhim AD, Mirek ET, Aiello NM, Maitra A, Bailey JM, McAllister F, et al. EMT and dissemination precede pancreatic tumor formation. Cell. 2012;148:349–61. doi: 10.1016/j.cell.2011.11.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Paley MA, Kroy DC, Odorizzi PM, Johnnidis JB, Dolfi DV, Barnett BE, et al. Progenitor and terminal subsets of CD8+ T cells cooperate to contain chronic viral infection. Science. 2012;338:1220–5. doi: 10.1126/science.1229620. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Doering TA, Crawford A, Angelosanto JM, Paley MA, Ziegler CG, Wherry EJ. Network analysis reveals centrally connected genes and pathways involved in CD8+ T cell exhaustion versus memory. Immunity. 2012;37:1130–44. doi: 10.1016/j.immuni.2012.08.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Wherry EJ, Ha S, Kaech SM, Haining WN, Sarkar S, Kalia V, et al. Molecular signature of CD8+ T cell exhaustion during chronic viral infection. Immunity. 2007;27:670–84. doi: 10.1016/j.immuni.2007.09.006. [DOI] [PubMed] [Google Scholar]
- 50.Barber DL, Wherry EJ, Masopust D, Zhu B, Allison JP, Sharpe AH, et al. Restoring function in exhausted CD8 T cells during chronic viral infection. Nature. 2006;439:682–7. doi: 10.1038/nature04444. [DOI] [PubMed] [Google Scholar]
- 51.Blackburn SD, Shin H, Freeman GJ, Wherry EJ. Selective expansion of a subset of exhausted CD8 T cells by PD-L1 blockade. Proc Natl Acad Sci U S A. 2008;105:15016–21. doi: 10.1073/pnas.0801497105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Galon J, Angell H, Bedognetti D, Marincola F. The continuum of cancer immunosurveillance: prognostic, predictive, and mechanistic signatures. Immunity. 2013;39:11–26. doi: 10.1016/j.immuni.2013.07.008. [DOI] [PubMed] [Google Scholar]
- 53.Cho H, Celis E. Optimized peptide vaccines eliciting extensive CD8 T-cell responses with therapeutic antitumor effects. Cancer Res. 2009;69:9012–9. doi: 10.1158/0008-5472.CAN-09-2019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Buhtoiarov IN, Sondel PM, Wigginton JM, Buhtoiarova TN, Yanke EM, Mahvi DA, et al. Anti-tumour synergy of cytotoxic chemotherapy and anti-CD40 plus CpG-ODN immunotherapy through repolarization of tumour-associated macrophages. Immunology. 2010;132:226–39. doi: 10.1111/j.1365-2567.2010.03357.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Vonderheide RH, Bajor DL, Winograd R, Evans RA, Bayne LJ, Beatty GL. CD40 immunotherapy for pancreatic cancer. Cancer Immunol Immunother. 2013;62:949–54. doi: 10.1007/s00262-013-1427-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Shepard HM, Jacobetz MA, Chan DS, Neesse A, Bapiro TE, Cook N, et al. Hyaluronan impairs vascular function and drug delivery in a mouse model of pancreatic cancer. Gut. 2012;62:112–20. doi: 10.1136/gutjnl-2012-302529. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Provenzano P, Cuevas C, Chang A, Goel V, Von Hoff D, Hingorani S. Enzymatic targeting of the stroma ablates physical barriers to treatment of pancreatic ductal adenocarcinoma. Cancer Cell. 2012;21:418–29. doi: 10.1016/j.ccr.2012.01.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Rhim A, Oberstein P, Thomas D, Mirek E, Palermo C, Sastra S, et al. Stromal elements act to restrain, rather than support, pancreatic ductal adenocarcinoma. Cancer Cell. 2014;25:735–47. doi: 10.1016/j.ccr.2014.04.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Vonderheide RH, Bayne LJ. Inflammatory networks and immune surveillance of pancreatic carcinoma. Curr. Opin. Immunol. 2013;25:200–5. doi: 10.1016/j.coi.2013.01.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Hiraoka N, Onozato K, Kosuge T, Hirohashi S. Prevalence of FOXP3+ regulatory T cells increases during the progression of pancreatic ductal adenocarcinoma and its premalignant lesions. Clin Can Res. 2006;12:5423–34. doi: 10.1158/1078-0432.CCR-06-0369. [DOI] [PubMed] [Google Scholar]
- 61.De Monte L, Reni M, Tassi E, Clavenna D, Papa I, Recalde H, et al. Intratumor T helper type 2 cell infiltrate correlates with cancer-associated fibroblast thymic stromal lymphopoietin production and reduced survival in pancreatic cancer. J Exp Med. 2011;208:469–78. doi: 10.1084/jem.20101876. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Fukunaga A, Miyamoto M, Cho Y, Murakami S, Kawarada Y, Oshikiri T, et al. CD8+ tumor-infiltrating lymphocytes together with CD4+ tumor-infiltrating lymphocytes and dendritic cells improve the prognosis of patients with pancreatic adenocarcinoma. Pancreas. 2004;28:e26–31. doi: 10.1097/00006676-200401000-00023. [DOI] [PubMed] [Google Scholar]
- 63.Bernstorff von W, Voss M, Freichel S, Schmid A, Vogel I, Jöhnk C, et al. Systemic and local immunosuppression in pancreatic cancer patients. Clin Can Res. 2001;7:925s–32s. [PubMed] [Google Scholar]
- 64.Zhang Y, Yan W, Mathew E, Bednar F, Wan S, Collins MA, et al. CD4+ T lymphocyte ablation prevents pancreatic carcinogenesis in mice. Cancer Immunol Res. 2014;2:423–35. doi: 10.1158/2326-6066.CIR-14-0016-T. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Feig C, Jones JO, Kraman M, Wells RJB, Deonarine A, Chan DS, et al. Targeting CXCL12 from FAP-expressing carcinoma-associated fibroblasts synergizes with anti-PD-L1 immunotherapy in pancreatic cancer. Proc Natl Acad Sci U S A. 2013;110:20212–7. doi: 10.1073/pnas.1320318110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Zhu Y, Knolhoff BL, Meyer MA, Nywening TM, West BL, Luo J, et al. CSF1/CSF1R blockade reprograms tumor-infiltrating macrophages and improves response to T-cell checkpoint immunotherapy in pancreatic cancer models. Cancer Res. 2014;74:5057–69. doi: 10.1158/0008-5472.CAN-13-3723. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Sherman MH, Yu RT, Engle DD, Ding N, Atkins AR, Tiriac H, et al. Vitamin d receptor-mediated stromal reprogramming suppresses pancreatitis and enhances pancreatic cancer therapy. Cell. 2014;159:80–93. doi: 10.1016/j.cell.2014.08.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Olive KP, Jacobetz MA, Davidson CJ, Gopinathan A, McIntyre D, Honess D, et al. Inhibition of Hedgehog signaling enhances delivery of chemotherapy in a mouse model of pancreatic cancer. Science. 2009;324:1457–61. doi: 10.1126/science.1171362. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Pylayeva-Gupta Y, Lee K, Hajdu C, Miller G, Bar-Sagi D. Oncogenic Kras-induced GM-CSF production promotes the development of pancreatic neoplasia. Cancer Cell. 2012;21:836–47. doi: 10.1016/j.ccr.2012.04.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Curran MA, Montalvo W, Yagita H, Allison JP. PD-1 and CTLA-4 combination blockade expands infiltrating T cells and reduces regulatory T and myeloid cells within B16 melanoma tumors. Proc Natl Acad Sci U S A. 2010;107:4275–80. doi: 10.1073/pnas.0915174107. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Leach DR, Krummel MF, Allison JP. Enhancement of antitumor immunity by CTLA-4 blockade. Science. 1996;271:1734–6. doi: 10.1126/science.271.5256.1734. [DOI] [PubMed] [Google Scholar]
- 72.Mangsbo SM, Sandin LC, Anger K, Korman AJ, Loskog A, Tötterman TH. Enhanced tumor eradication by combining CTLA-4 or PD-1 blockade with CpG therapy. J Immunother. 2010;33:225–35. doi: 10.1097/CJI.0b013e3181c01fcb. [DOI] [PubMed] [Google Scholar]
- 73.Williams EL, Dunn SN, James S, Johnson PW, Cragg MS, Glennie MJ, et al. Immunomodulatory monoclonal antibodies combined with peptide vaccination provide potent immunotherapy in an aggressive murine neuroblastoma model. Clin Can Res. 2013;19:3545–55. doi: 10.1158/1078-0432.CCR-12-3226. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Sandin LC, Eriksson F, Ellmark P, Loskog AS, Tötterman TH, Mangsbo SM. Local CTLA4 blockade effectively restrains experimental pancreatic adenocarcinoma growth in vivo. Oncoimmunology. 2014;3:e27614. doi: 10.4161/onci.27614. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Nomi T, Sho M, Akahori T, Hamada K, Kubo A, Kanehiro H, et al. Clinical significance and therapeutic potential of the programmed death-1 ligand/programmed death-1 pathway in human pancreatic cancer. Clin Can Res. 2007;13:2151–7. doi: 10.1158/1078-0432.CCR-06-2746. [DOI] [PubMed] [Google Scholar]
- 76.Jones S, Zhang X, Parsons DW, Leary RJ, Angenendt P, Mankoo P, et al. Core signaling pathways in human pancreatic cancers revealed by global genomic analyses. Science. 2008;321:1801–6. doi: 10.1126/science.1164368. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Ho P, Meeth KM, Tsui Y, Srivastava B, Bosenberg MW, Kaech SM. Immune-based antitumor effects of BRAF inhibitors rely on signaling by CD40L and IFNγ. Cancer Res. 2014;74:3205–3217. doi: 10.1158/0008-5472.CAN-13-3461. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Richman LP, Vonderheide RH. Role of crosslinking for agonistic CD40 monoclonal antibodies as immune therapy of cancer. Cancer Immunol Res. 2014;2:19–26. doi: 10.1158/2326-6066.CIR-13-0152. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Velcheti V, Schalper KA, Carvajal DE, Anagnostou VK, Syrigos KN, Sznol M, et al. Programmed death ligand-1 expression in non-small cell lung cancer. Lab. Invest. 2013;94:107–16. doi: 10.1038/labinvest.2013.130. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Akbay EA, Koyama S, Carretero J, Altabef A, Tchaicha JH, Christensen CL, et al. Activation of the PD-1 pathway contributes to immune escape in EGFR-driven lung tumors. Cancer Discov. 2013;3:1355–63. doi: 10.1158/2159-8290.CD-13-0310. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.