ABSTRACT
Purpose: To determine the comparative effectiveness of consistent cooling using an icing device (DonJoy Iceman, DJO Canada, Mississauga, ON) versus intermittent cooling using an ice bag (usual care) for the first 48 hours after total knee arthroplasty (TKA). Method: A sample of 78 patients (intervention group, n=37; control group, n=34) undergoing primary TKA were randomized to intervention (device) or control (ice) groups. The primary outcome was pain intensity, measured by numerical pain rating scale (NPRS). Secondary outcomes were passive range of motion (PROM), nausea or vomiting, opioid use, blood loss, lower limb function, hospital length of stay, and patient-reported compliance and satisfaction. Results: No significant differences in the primary outcome (pain intensity measured via NPRS) were observed between control and intervention groups. Patients in the intervention group were significantly more satisfied (8.4 vs. 6.0, p=0.002); used the device more consistently, day and night (85.7% vs. 29.6% and 87.6% vs. 30.8%, respectively, p<0.001); and were more likely to recommend this method of cooling (96.8% vs. 68.0%, p=0.004). Conclusion: The study found no additional benefit of consistent cryotherapy using the icing device over intermittent ice bags on postoperative pain, PROM, nausea or vomiting, opioid use, blood loss, lower limb function, or length of stay, despite significant differences in patient-reported compliance and satisfaction.
Key Words: arthroplasty, cryotherapy, knee
RÉSUMÉ
Objet: Déterminer l'efficacité comparative du refroidissement constant au moyen d'un dispositif de refroidissement (DonJoy Iceman, DJO Canada, Mississauga, Ontario) en comparaison du refroidissement intermittent découlant de l'utilisation d'un sac à glace (soins habituels) dans les 48 premières heures suivant l'arthroplastie totale du genou. Méthode: Un échantillon de 78 patients (groupe d'intervention n=37; groupe témoin n=34) ayant subi une première arthroplastie totale du genou ont été randomisés dans des groupes d'intervention (dispositif) ou témoin (glace). Le résultat principal était l'intensité de la douleur, mesurée selon une échelle d'évaluation numérique de la douleur. Les résultats secondaires étaient l'amplitude passive du mouvement, les nausées/vomissements, l'utilisation d'opioïde, la perte de sang, la fonction des membres inférieurs, la durée du séjour à l'hôpital, et la conformité et la satisfaction déclarées par les patients. Résultats: On n'a observé aucune différence significative dans le résultat principal (intensité de la douleur mesurée selon une échelle d'évaluation numérique de la douleur) entre les groupes témoin et d'intervention. Les patients du groupe d'intervention étaient considérablement plus satisfaits (8,4 contre 6, 0, p=0,002); utilisaient le dispositif de façon plus uniforme, le jour et la nuit (85.7% contre 29.6% et 87.6% contre 30.8%, respectivement, p<0,001); et étaient plus susceptibles de recommander cette méthode de refroidissement (96,8% contre 68,0%, p=0,004). Conclusion: L'étude n'a révélé aucun avantage supplémentaire découlant de la cryothérapie constante au moyen d'un dispositif de refroidissement par rapport aux sacs à glace intermittents pour ce qui est de la douleur postopératoire, de l'amplitude passive du mouvement, des nausées/vomissements, de l'utilisation d'opioïdes, de la perte de sang, de la fonction des membres inférieurs ou de la durée du séjour, malgré les différences significatives en matière de conformité et de satisfaction déclarées par les patients.
Mots clés : arthroplastie, cryothérapie, remplacement, genou
Total knee arthroplasty (TKA) is a common major orthopaedic procedure. From April 1, 2010, to March 31, 2011, there were 47,113 acute-care hospitalizations for primary TKA in Canada, of which 6,392 were in British Columbia.1 Immediate consequences after TKA include significant pain,2 swelling,3 limited movement,4 nausea or vomiting,5 and potential blood loss.6 The goal of surgery is to reduce pain, improve function, and maximize knee range of motion (ROM).7
Pain is often severe in the early postoperative period, impeding rehabilitation.8 Mobilization requires pain control, but the side effects associated with narcotics, such as nausea, vomiting, sedation, pruritus, hypotension, and respiratory depression can limit activity, result in longer hospital stays, increase morbidity, and reduce patients' satisfaction.9 Achieving adequate pain control while minimizing side effects is crucial.10 A common method to assist with pain and swelling post-TKA is intermittent cooling using a bag of ice or a device for 24–48 hours after surgery.11
Although an important goal post-TKA is to restore or maximize knee ROM, stiffness is common, and7,11 patient compliance with exercise postoperatively is important to prevent and treat stiffness.7 Gibbons and colleagues12 reported that a significant increase in ROM resulted in successful short-term rehabilitation and that this was best achieved through combined cold and compression rather than compression alone.
Intra- and postoperative bleeding is a risk of TKA. Limiting blood loss reduces associated comorbidities, improves recovery and participation in rehabilitation,13 and minimizes the need for blood transfusions.14 Although compression used for at least 48 hours can provide effective control of intra-articular bleeding,15 cryotherapy has only a small effect on intra-articular bleeding.16
Although applying a bag of ice is a common method of postoperative cryotherapy,17 the frequency, intensity, and duration of application vary, which may contribute to suboptimal care for patients.17 Moreover, this method of cooling carries a risk of precipitating skin and nerve damage.18 Interest has recently grown in using devices that incorporate both cooling and compression; a survey of physiotherapists in the United Kingdom found that 59% of respondents use these devices.17 An example is the DonJoy Iceman (DJO Canada, Mississauga, ON), which uses a semi-closed loop system consisting of a cooler with a pump and tubing connected to a polyethylene cuff.19
Cooling and compression post-trauma are fundamental interventions for managing inflammation, which peaks within the first 48 hours after TKA surgery.3 The physiological benefits of cooling together with compression are decreased secondary cell death (i.e., cells not injured in the initial trauma die as a result of physiological responses to the primary injury, such as acidosis and lysosomal digestion)20 and attenuated pain.21 Previous research with cooling and compression post-TKA has demonstrated reduced pain and blood loss,22–24 but findings are inconsistent with respect to reduced swelling and improved mobility.22–25 Similarly, Markert26 reported inconsistent findings in a review of 11 studies on the use of cryotherapy post-TKA. A Cochrane review by Adie and colleagues16 reported that cryotherapy had a small but perhaps not clinically significant beneficial effect on blood loss, pain, and ROM. Variation in the application of cryotherapy (type, frequency, duration) in the literature makes it difficult to ascertain definitive direction for clinical practice. Moreover, none of the trials reviewed by Adie and colleagues16 included a measure of function, and there was no analysis comparing the relative effectiveness of intermittent cooling with an ice bag versus consistent cooling with a device. The purpose of our study, therefore, was to compare the effects on pain and several secondary outcomes of consistent cooling (using a motorized icing device) with those of intermittent cooling (using an ice bag) for 48 hours post-TKA. We hypothesized that there would be no significant between-group differences in either primary or secondary outcomes.
Methods
Context and population
The study took place at St. Paul's Hospital, a major tertiary care centre, from February 2009 through May 2012, during which 382 TKAs were performed at this centre.27 Eligible participants were adult patients of two orthopaedic surgeons (surgeon A and surgeon B) who underwent primary TKA. Potential participants were excluded if they had preoperative pain requiring daily narcotic use, Raynaud's disease,28 cryoglobinaemia,29 cold urticaria,30–33 and hemoglobinuria.34 The centre's Ethics Review Board approved the study.
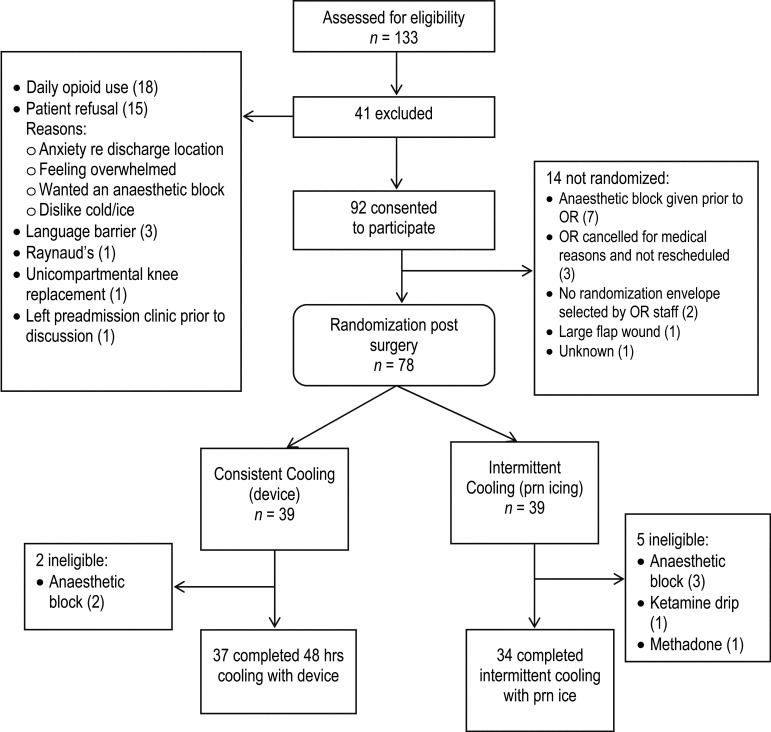
We aimed to recruit 40 participants into each group, based on a priori sample-size calculation, with allowances for potential dropouts. Using a standard deviation of 1.46,35 we estimated that we would need 35 participants in each group to detect a statistically significant 1-point difference in pain scores (or a moderate effect size of 0.68) at an alpha level of 0.05 and power level of 80% (see Figure 1).
Figure 1.
Overview of study participant flow for inclusion.
Procedures
Patients were invited to participate during the preadmission clinic (PAC) visit by a member of the research team, and written informed consent was obtained.
A total of 133 patients were assessed for eligibility; 41 were excluded. Of the 92 who consented, 14 were not randomized (see Figure 1). The remaining 78 were randomized, 39 to each arm (Figure 1), by staff of the operating room (OR), independent of the research team; at the time of incision closure, OR staff chose a sealed opaque envelope containing standardized orders pertinent to intervention versus control. A total of 7 consenting patients were ineligible for the study, the majority because of an intra-operative decision to use a nerve block. The decision to use a nerve block was driven by surgeon and anesthetist preference and was confirmed to be unrelated to patient characteristics. The final intervention group contained 37 participants, and the control group 34.
Blinding
Neither participants nor the care providers who assessed outcomes could be blinded to the intervention because application of the device or ice was visually obvious. However, measured outcomes were extracted from patient charts, using a study-specific data collection form, by a research assistant who was not a member of the research team and was blinded to group allocation.
Intervention
Both groups received identical surgical wound dressings in the OR. For the intervention group, to prevent swelling distal to the device, the surgeons requested that the operated leg be wrapped with an elastic bandage from the toes up to the cuff of the device; stockinette was applied over the knee as a protective barrier between skin and cuff. For the control group, the operated limb was wrapped with an elastic bandage from toes to above the knee for 48 hours after surgery to help control the degree of compression between groups. In the post-anaesthetic recovery room and on the unit, the control group received ice bags at a frequency requested by the patient (usual care) for 48 hours.
For the intervention group, the device was applied by the surgeon in the OR immediately after surgery and remained in place for 48 hours, except for brief periods: after 1 hour, and every 4 hours thereafter, for nursing assessment for skin or nerve damage; during exercise; and during ambulation. Nursing staff were trained at the beginning of the study on how to set up and use the device, and detailed instructions and photographs were secured to all devices for the duration of the study. The temperature setting was determined by piloting with members of the research team and subsequently standardized and secured at the chosen setting, indicated by a blue dot. Because it was not possible to determine the level of cooling with a patient connected to the device, two members of the research team independently ascertained (by running the device unapplied to a limb for 4-hour intervals on 2 consecutive days) that the selected setting resulted in a range of cooling between 2°C and 6°C, as indicated by the thermometer on the device.
Outcome measures
Data collection took place as part of existing standardized postoperative care procedures for TKA. On admission to the orthopaedic ward and every 4 hours thereafter for 48 hours, all patients underwent a nursing assessment including vital signs, skin assessments, opioid use, and numeric pain rating scale (NPRS). Nausea or vomiting was assessed twice a day, passive range of motion (PROM) and hemoglobin once a day, and the Western Ontario and McMaster University Osteoarthritis Index (WOMAC) was administered twice: in the PAC and at 6-week follow-up in the surgeon's office. The patient satisfaction questionnaire was completed immediately after the 48-hour treatment period.
Primary outcome
The primary study outcome was pain, measured via NPRS. Although the study protocol requested that pain be measured on a 10 cm visual analogue scale (VAS), the hospital's standard clinical practice used the NPRS, which was therefore consistently used as the pain score throughout the study. The NPRS 0–10 is the numeric version of the VAS and has been shown to be highly correlated with the VAS, with good test–retest reliability, for both literate and illiterate patients.36 Observations over the period from 24 to 48 hours post-surgery were averaged; data from the first 24 hours were excluded to allow the effects of intra-operative medication to dissipate.
Secondary outcomes
The physiotherapist working on the ward in the morning of postoperative days 1 and 2 assessed the total amount of passive movement between knee extension and flexion using a standard 30.48 centimetre (12 in.) goniometer with 1° increments. Interrater reliability between physiotherapists for this measurement has been established,37 and all physiotherapists were trained and experienced in goniometric assessment of ROM in this patient population. Nausea or vomiting, reported by the patient, was assessed and recorded on the clinical pathway every 12 hours by nursing staff. All doses of opioids were converted to a corresponding equal dose of morphine, calculated as equianalgesic total opioid use for 24–48 hours38 and reported in milligrams (see Table 1). Pain medications were standardized to the extent possible. A single acetaminophen dose (650–975 mg), a long-acting opioid, and a long-acting COX-2 selective non-steroidal anti-inflammatory drug (NSAID) were all prescribed preoperatively. Postoperatively, patients were prescribed 650 milligrams acetaminophen every 6 hours, a long-acting opioid twice daily, a long-acting COX-2 selective NSAID, and an opioid as needed, as allergies and patients' needs permitted. Change in hemoglobin between 24 and 48 hours was recorded as the proxy indicator of blood loss.39 We used the WOMAC to assess function because it is sensitive to change and has been shown to be preferable to other instruments for assessment of osteoarthritis.40,41 The required license for the WOMAC was obtained. We compared the change in overall average score (0–4) and scores on the sub-dimensions (pain, stiffness, physical function) between groups. The mean length of stay (LOS) was determined from hospital records.
Table 1.
Modified Equal Analgesic Conversion Table
| Morphine dose | Is equivalent to |
|---|---|
| 10 mg PO morphine | 2 mg PO hydromorphone |
| 10 mg PO morphine | 1 mg IV/SC hydromorphone |
| 10 mg PO morphine | 0.5 epidural morphine |
| 2 mg PO morphine | 1 mg IV/SC morphine |
| 2 mg PO morphine | 15 mcg IV fentanyl |
| 13.33 mg PO morphine | 10 mg PO oxycodone |
Patient satisfaction was assessed via questionnaire. Participants reported their overall satisfaction by placing an X on a 10 centimetre line (0=extremely unsatisfied, 10=extremely satisfied); the distance was measured in centimetres from the beginning of the line to the centre of the patient's X, using a ruler with 1 millimetre increments. Participants were also asked to report the average proportion of time the ice or device was used (always, 100%; almost always, 75%; half the time, 50%; a little bit of the time, 25%; none of the time, 0%), likes and dislikes, and whether they would recommend the method of cooling. The questionnaire was piloted with 10 TKA patients before its use in the study; no revisions were required as a result of the pilot testing.
Statistical analysis
We described participant characteristics—age, sex, and outcome variables—and calculated means, standard deviations, and proportions for all outcomes. Group differences were tested using two-sided t-tests and χ2 tests. To confirm that the 24–48 hour postoperative period was optimal for capturing postoperative pain without the effect of pain medications administered intra-operatively, we also ran a linear regression for opioid use during the first 0–24 hours. Levels of satisfaction for the intervention and control groups were compared via two-sided t-test. Two independent coders, blinded to group allocation, thematically analyzed participants' comments regarding likes and dislikes. A third coder was not required because there were no discrepancies. Missing data ranged from 0% to 38%; the highest rate of missing data was for WOMAC scores. The primary outcome of pain had 4% missing data. Pairwise deletion was used in the analysis to retain as much data as possible.
Results
Groups were similar at baseline with respect to age, sex, preoperative opioid use, and functional status (see Table 2). For the primary outcome of pain, we found no statistically significant difference between groups (see Table 3). Because medication dosing can be a confounder, in addition to attempting to standardize both pre- and postoperative doses, we calculated equianalgesic total opioid use for all participants (see Table 1).42 Controlling statistically for opioid use in the 0–24 hour period did not change the magnitude or significance of the difference in this period; we therefore report only unadjusted results (i.e., results of t-tests) in Table 3.
Table 2.
Patient Baseline Descriptive Characteristics*
| Mean (SE)* |
||
|---|---|---|
| Characteristic | Control (n=34) | Intervention (n=37) |
| Age, y | 71.5 (1.8) | 70.4 (1.8) |
| Sex, % women | 41.2 | 54.0 |
| Surgeon A/B, % surgeon A | 38.2 | 29.7 |
| Preoperative narcotic use, mg | 8.8 (1.4) | 9.6 (1.0) |
| WOMAC score | ||
| Pain | 1.8 (0.14) | 1.6 (0.13) |
| Stiffness | 2.0 (0.16) | 1.9 (0.15) |
| Function | 1.9 (0.13) | 1.8 (0.14) |
Unless otherwise indicated.
WOMAC=Western Ontario and McMaster University Osteoarthritis Index.
Table 3.
Study Outcomes
| Mean (SE)* |
|||
|---|---|---|---|
| Outcome | Control (n=34) | Intervention (n=37) | p-value |
| Primary outcome | |||
| Pain, NPRS (24–48 h post-op) | 3.6 (0.27) | 3.8 (0.25) | 0.67 |
| Secondary clinical outcomes | |||
| PROM, degrees (48 h postop) | 59.8 (3.1) | 54.0 (2.4) | 0.14 |
| Nausea or vomiting, % yes (24–48 h postop) | 15.6 | 34.3 | 0.08 |
| Opioid use, mg (24–48 h postop) | 42.3 (4.9) | 49.9 (5.8) | 0.33 |
| Change in Hgb, g/L (24–48 h postop) | −8.8 (1.7) | −7.7 (1.8) | 0.68 |
| Change in WOMAC pain | −0.7 (0.23) | −0.4 (0.23) | 0.32 |
| Change in WOMAC stiffness | −0.8 (0.23) | −0.3 (0.24) | 0.14 |
| Change in WOMAC function | −0.6 (0.21) | −0.6 (.17) | 0.95 |
| Length of stay, d | 4.8 (0.39) | 5.8 (0.64) | 0.20 |
| Patient satisfaction | |||
| Patient satisfaction, cm | 6.0 (0.70) | 8.4 (0.36) | 0.002 |
| Patients who recommended “yes,” % | 63.0 | 96.9 | 0.004 |
| Consistency of use | |||
| Average time used during the day, % of participants | <0.001 | ||
| None of the time (0%) | 14.8 | 0 | |
| Little bit of the time (25%) | 25.9 | 8.6 | |
| Half the time (50%) | 29.6 | 5.7 | |
| Almost always (75%) | 22.2 | 17.1 | |
| Always (100%) | 7.4 | 68.6 | |
| Average time used at night, % of participants | <0.001 | ||
| None of the time (0%) | 30.8 | 6.3 | |
| Little bit of the time (25%) | 19.2 | 3.1 | |
| Half the time (50%) | 19.2 | 3.1 | |
| Almost always (75%) | 23.1 | 18.8 | |
| Always (100%) | 7.7 | 68.8 | |
Unless otherwise indicated.
NPRS=Numeric Pain Rating Scale; PROM=passive range of motion; Hgb=hemoglobin; WOMAC=Western Ontario and McMaster University Osteoarthritis Index.
There were no statistically significant between-group differences in the secondary outcomes of nausea or vomiting, opioid use, change in hemoglobin at 24–48 hours after surgery, PROM after 48 hours, WOMAC at 6 weeks, or LOS (see Table 3). These findings, though not statistically significant, may be clinically significant, because better control of nausea and vomiting may permit patients to mobilize to a greater degree. Patients in the intervention group reported greater satisfaction with postoperative cooling, were more likely to recommend the method they received, and used cooling more consistently (see Table 3). The results of the thematic analysis from the patient questionnaire revealed that the intervention group found the device both convenient and comfortable and felt it reduced their pain and swelling. Patients also reported, however, that the device was heavy and that some staff appeared to be unsure as to how to apply it. Although both groups reported that their pain decreased, the decrease reported by the control group was less than that reported by the intervention group. The control group also disliked the ice melting and would have liked ice more often. No adverse events were reported or observed in either group.
Discussion
Our study found that use of consistent cooling with a device did not improve pain, measured by the NPRS, more than intermittent cooling using an ice bag in the 24–48 hour postoperative period. Confidence in the validity of this finding is supported by (1) exclusion of patients who used narcotics daily preoperatively; (2) standardized “equianalgesic” dosing; (3) statistical confirmation that patients withdrawn as a result of nerve blocks were not different from those who remained in the study; and (4) statistical confirmation, using linear regression, that the 24–48 hour postoperative period was optimal for capturing postoperative pain. This finding is consistent with those of previous studies with respect to the lack of significant influence of cryotherapy on pain post-TKR.16,26
Similarly, we found no between-group difference in PROM, nausea or vomiting, or blood loss, which suggests that consistent and intermittent cooling were equally as effective in managing these common consequences of TKA. These findings concur with those reported by Adie and colleagues;16 however, although the four trials included in their meta-analysis compared several different methods of cooling (cold vs. compression, cold compression vs. nothing, and cold compression vs. compression), none included a comparison between ice and a cooling device.16 Our study addresses this gap in the literature. Our findings are particularly intriguing because although the intervention group had much longer and more consistent cooling periods, and thus the magnitude of a therapeutic effect could theoretically have favoured this group, it did not. One potential contributing factor may be a difference in the intervening layer of material between the wound dressing and cooling method: stockinette and the polyethylene cuff for the intervention group and an elastic bandage and plastic bag for the control group. The choice of these intervening layers was dictated by clinical need and therefore could not be standardized between groups. A second potential contributing factor was the difference in the method and degree of sustained compression: For the intervention group, pressure was supplied by the water-filled cuff secured in place with an elastic bandage, whereas the control group had only an elastic bandage. Again, it was not possible to standardize the compression between groups. These two factors illustrate the complexities of undertaking a randomized controlled trial in a clinical setting.
Although there was no significant decrease in pain or opioid use in the intervention group, participants in this group reported higher satisfaction with postoperative cooling, used cooling more consistently, and were more likely to recommend the icing device. Although one could hypothesize that greater satisfaction would be associated with less pain and ultimately better outcomes, our findings do not substantiate this hypothesis. This discrepancy between patient satisfaction and clinical outcomes may indicate that consistent cooling confers an effect that is not measureable by the outcome measures used in this study. The minimal clinically important difference for the NPRS after orthopaedic surgery has been reported as 28.6%, and patients in this study clearly did not report that degree of pain reduction.44 The higher level of satisfaction may also be attributable to greater patient contact with the staff who replaced ice and water in the device and conducted skin checks every 4 hours. Regardless of the underlying potential causes of higher patient-reported satisfaction, our findings provide evidence that the choice of compression and cooling methods may be guided by patient preference rather than by evidence of a definitive beneficial effect on pain, PROM, lower limb function, blood loss, or LOS.
Our results indicate that, given the increasing demands on clinicians and limited resources in acute-care settings, the extra costs and resources associated with providing cooling devices may not be necessary for better patient outcomes following TKA. However, the trend to shorter LOS, though not statistically significant, may provide an opportunity for potential cost savings. Ice is also readily available, less costly, and easy to apply at home,26 all of which are important factors given that most patients undergoing TKA are elderly, with multiple comorbidities.45 All patients in this study were advised to use ice as needed after the 48 hour period, both in hospital and at home; they were not advised to obtain a cooling device. Nevertheless, if patients do choose to use these devices postoperatively, the absence of complications with use of the icing device in our study indicates that when coupled with stockinette and skin assessments every 4 hours, it is a safe treatment option.
Limitations
Our study has several potential limitations. First, because neither patients nor care providers could be blinded to group allocation, subjective measures such as level of pain, level of satisfaction, and treatment recommendation are subject to potential bias. Second, the absence of significant between-group differences may primarily be due to the measures' not being sensitive enough to detect change. Third, the extrapolation of these findings is limited by postoperative pain management protocols; many acute-care organizations now use femoral nerve blocks or femoral nerve catheters post-TKA, but when our study began, this option was not consistently available at our facility, and therefore patients who received blocks were excluded. Our results might have been different if postoperative pain had been decreased with a femoral nerve block. Finally, it is important to acknowledge that these findings may not be generalizable to (1) patients after revision TKA, (2) pain management beyond the 48 hour postoperative period, or (3) other methods of continuous cryotherapy that incorporate different parameters of cooling and compression.
Conclusion
There is no significant difference between the effects of intermittent cooling with an ice bag and those of consistent cooling using a device with respect to pain, blood loss, nausea or vomiting, self-reported function, PROM, or LOS after TKA. The fact that we observed no differences in clinical outcomes despite marked differences in consistency of cooling suggests that the additional costs and resources required to use these devices may not be warranted.
Key Messages
What is already known on this topic
Previous research on the use of cooling after TKA has reported inconsistent findings with respect to reduction of swelling and improved mobility immediately post-TKA and small and likely clinically insignificant effects on blood loss, pain, and ROM.
What this study adds
This study contributes new evidence on the relative effectiveness of continuous cooling using a device versus intermittent cooling using an ice bag by means of a head-to-head comparison of the influence of these methods on previously investigated outcomes (pain, blood loss, lower limb function, ROM, opioid use, and LOS) and also addresses the relative influence of each method on previously underexplored outcomes: duration of cooling and patient satisfaction. Though patients reported significantly greater satisfaction with consistent cooling with the device, there were no significant differences in functional status (as measured by the WOMAC) at 6 week follow-up.
Physiotherapy Canada 2015; 67(1);48–55; doi:10.3138/ptc.2013-78
References
- 1.Canadian Institute for Health Information. Hip and knee replacements in Canada: Canadian Joint Replacement Registry 2013 annual report [Internet] Ottawa: The Institute; c2013. [cited 2013 Aug 13]. Available from: https://secure.cihi.ca/estore/productFamily.htm?locale=en&pf=PFC2209&lang=en&media=0. [Google Scholar]
- 2.Jenstrup MT, Jæger P, Lund J, et al. Effects of adductor-canal-blockade on pain and ambulation after total knee arthroplasty: a randomized study. Acta Anaesthesiol Scand. 2012;56(3):357–64. doi: 10.1111/j.1399-6576.2011.02621.x. http://dx.doi.org/10.1111/j.1399-6576.2011.02621.x. Medline:22221014. [DOI] [PubMed] [Google Scholar]
- 3.Hughes SF, Hendricks BD, Edwards DR, et al. Total hip and knee replacement surgery results in changes in leukocyte and endothelial markers. J Inflamm (Lond) 2010;7(1):2. doi: 10.1186/1476-9255-7-2. http://dx.doi.org/10.1186/1476-9255-7-2. Medline:20148137. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Pivec R, Issa K, Kester M, et al. Long-term outcomes of MUA for stiffness in primary TKA. J Knee Surg. 2013;26(6):405–10. doi: 10.1055/s-0033-1341579. http://dx.doi.org/10.1055/s-0033-1341579. Medline:23512543. [DOI] [PubMed] [Google Scholar]
- 5.Lewis C, Gunta K, Mitchell K, et al. Effectiveness of multimodal pain management protocol in total knee arthroplasty patients. Orthop Nurs. 2012;31(3):153–9. doi: 10.1097/NOR.0b013e3182558d0b. http://dx.doi.org/10.1097/NOR.0b013e3182558d0b. Medline:22622607. [DOI] [PubMed] [Google Scholar]
- 6.Sehat KR, Evans RL, Newman JH. Hidden blood loss following hip and knee arthroplasty. Correct management of blood loss should take hidden loss into account. J Bone Joint Surg Br. 2004;86(4):561–5. Medline:15174554. [PubMed] [Google Scholar]
- 7.Beaver WB, Jr, Fehring TK. Prevention and treatment of stiffness following total knee arthroplasty. Curr Opin Orthop. 2008;19(1):174–5. http://dx.doi.org/10.1097/BCO.0b013e3282f2ccda. [Google Scholar]
- 8.Kullenberg B, Ylipää S, Söderlund K, et al. Postoperative cryotherapy after total knee arthroplasty: a prospective study of 86 patients. J Arthroplasty. 2006;21(8):1175–9. doi: 10.1016/j.arth.2006.02.159. http://dx.doi.org/10.1016/j.arth.2006.02.159. Medline:17162178. [DOI] [PubMed] [Google Scholar]
- 9.Trueblood A, Manning DW. Analgesia following total knee arthroplasty. Curr Opin Orthop. 2007;18(1):76–80. http://dx.doi.org/10.1097/BCO.0b013e3280119635. [Google Scholar]
- 10.White PF. The changing role of non-opioid analgesic techniques in the management of postoperative pain. Anesth Analg. 2005;101(5 Suppl):S5–22. doi: 10.1213/01.ANE.0000177099.28914.A7. http://dx.doi.org/10.1213/01.ANE.0000177099.28914.A7. Medline:16334489. [DOI] [PubMed] [Google Scholar]
- 11.Barry S, Wallace L, Lamb S. Cryotherapy after total knee replacement: a survey of current practice. Physiother Res Int. 2003;8(3):111–20. doi: 10.1002/pri.279. http://dx.doi.org/10.1002/pri.279. Medline:14533367. [DOI] [PubMed] [Google Scholar]
- 12.Gibbons CE, Solan MC, Ricketts DM, et al. Cryotherapy compared with Robert Jones bandage after total knee replacement: a prospective randomized trial. Int Orthop. 2001;25(4):250–2. doi: 10.1007/s002640100227. http://dx.doi.org/10.1007/s002640100227. Medline:11561502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Fechisin J, Scuderi GR. The efficacy of bipolar transcollation in managing blood loss in total knee arthroplasty. Tech Knee Surg. 2011;10(4):206–10. http://dx.doi.org/10.1097/BTK.0b013e31823a230a. [Google Scholar]
- 14.Courtney JB, Cushner F, Long WJ, et al. An effective bloodless surgery protocol. Tech Knee Surg. 2011;10(4):188–97. http://dx.doi.org/10.1097/BTK.0b013e31823b31ea. [Google Scholar]
- 15.Charalambides C, Beer M, Melhuish J, et al. Bandaging technique after knee replacement. Acta Orthop. 2005;76(1):89–94. doi: 10.1080/00016470510030382. http://dx.doi.org/10.1080/00016470510030382. Medline:15788314. [DOI] [PubMed] [Google Scholar]
- 16.Adie S, Kwan A, Naylor JM, et al. Cryotherapy following total knee replacement. Cochrane Database Syst Rev. 2012;2012(9):CD007911. doi: 10.1002/14651858.CD007911.pub2. Medline:22972114. [DOI] [PubMed] [Google Scholar]
- 17.Barry S, Wallace L, Lamb S. Cryotherapy after total knee replacement: a survey of current practice. Physiother Res Int. 2003;8(3):111–20. doi: 10.1002/pri.279. http://dx.doi.org/10.1002/pri.279. Medline:14533367. [DOI] [PubMed] [Google Scholar]
- 18.Moeller JL, Monroe J, McKeag DB. Cryotherapy-induced common peroneal nerve palsy. Clin J Sport Med. 1997;7(3):212–6. doi: 10.1097/00042752-199707000-00011. http://dx.doi.org/10.1097/00042752-199707000-00011. Medline:9262890. [DOI] [PubMed] [Google Scholar]
- 19.DonJoy Global. DonJoy Iceman Classic. Vista, CA: DJO Global; [cited 2013 Aug 25]. [about 2 screens] Available from: https://www.djoglobal.com/products/donjoy/donjoy-iceman-classic. [Google Scholar]
- 20.Merrick MA. Secondary injury after musculoskeletal trauma: a review and update. J Athl Train. 2002;37(2):209–17. Medline:16558673. [PMC free article] [PubMed] [Google Scholar]
- 21.Bleakley CM, McDonough SM, MacAuley DC, et al. Cryotherapy for acute ankle sprains: a randomised controlled study of two different icing protocols. Br J Sports Med. 2006;40(8):700–5, discussion 705. doi: 10.1136/bjsm.2006.025932. http://dx.doi.org/10.1136/bjsm.2006.025932. Medline:16611722. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Webb JM, Williams D, Ivory JP, et al. The use of cold compression dressings after total knee replacement: a randomized controlled trial. Orthopedics. 1998;21(1):59–61. doi: 10.3928/0147-7447-19980101-14. Medline:9474633. [DOI] [PubMed] [Google Scholar]
- 23.Schröder D, Pässler HH. Combination of cold and compression after knee surgery. A prospective randomized study. Knee Surg Sports Traumatol Arthrosc. 1994;2(3):158–65. doi: 10.1007/BF01467918. http://dx.doi.org/10.1007/BF01467918. Medline:7584198. [DOI] [PubMed] [Google Scholar]
- 24.Levy AS, Marmar E. The role of cold compression dressings in the postoperative treatment of total knee arthroplasty. Clin Orthop Relat Res. 1993;(297):174–8. Medline:7902225. [PubMed] [Google Scholar]
- 25.Smith J, Stevens J, Taylor M, et al. A randomized, controlled trial comparing compression bandaging and cold therapy in postoperative total knee replacement surgery. Orthop Nurs. 2002;21(2):61–6. doi: 10.1097/00006416-200203000-00009. http://dx.doi.org/10.1097/00006416-200203000-00009. Medline:11949239. [DOI] [PubMed] [Google Scholar]
- 26.Markert SE. The use of cryotherapy after a total knee replacement: a literature review. Orthop Nurs. 2011;30(1):29–36. doi: 10.1097/NOR.0b013e318205749a. http://dx.doi.org/10.1097/NOR.0b013e318205749a. Medline:21278552. [DOI] [PubMed] [Google Scholar]
- 27.Chu C. Providence Health Care. Orthopedic Surgery Department: number of cases performed at St Paul's Hospital between Jan 1, 2009 and September 30, 2012. Data extracted from Providence Health Care Operating Room Management Information System. [cited 2013 July 17].
- 28.Harvey CK. An overview of cold injuries. J Am Podiatr Med Assoc. 1992;82(8):436–8. doi: 10.7547/87507315-82-8-436. http://dx.doi.org/10.7547/87507315-82-8-436. Medline:1507084. [DOI] [PubMed] [Google Scholar]
- 29.Dispenzieri A, Gorevic PD. Cryoglobulinemia. Hematol Oncol Clin North Am. 1999;13(6):1315–49. doi: 10.1016/s0889-8588(05)70129-5. http://dx.doi.org/10.1016/S0889-8588(05)70129-5. Medline:10626153. [DOI] [PubMed] [Google Scholar]
- 30.Claus-Walker J, Halstead LS, Carter RE, et al. Physiological responses to cold stress in healthy subjects and in subjects with cervical cord injuries. Arch Phys Med Rehabil. 1974;55(11):485–90. Medline:4441259. [PubMed] [Google Scholar]
- 31.Dover G, Borsa PA, McDonald DJ. Cold urticaria following an ice application: a case study. Clin J Sport Med. 2004;14(6):362–4. doi: 10.1097/00042752-200411000-00008. http://dx.doi.org/10.1097/00042752-200411000-00008. Medline:15523210. [DOI] [PubMed] [Google Scholar]
- 32.Knight KL. Cryotherapy in sport injury management. Champaign (IL): Human Kinetics; 1995. [Google Scholar]
- 33.Shelley WB, Caro WA. Cold erythema. A new hypersensitivity syndrome. JAMA. 1962;180(8):639–42. doi: 10.1001/jama.1962.03050210001001. http://dx.doi.org/10.1001/jama.1962.03050210001001. Medline:13911629. [DOI] [PubMed] [Google Scholar]
- 34.Petz LD. Cold antibody autoimmune hemolytic anemias. Blood Rev. 2008;22(1):1–15. doi: 10.1016/j.blre.2007.08.002. http://dx.doi.org/10.1016/j.blre.2007.08.002. Medline:17904258. [DOI] [PubMed] [Google Scholar]
- 35.Pinto PR, McIntyre T, Ferrero R, et al. Risk factors for moderate and severe persistent pain in patients undergoing total knee and hip arthroplasty: a prospective predictive study. PLoS One. 2013;8(9):e73917. doi: 10.1371/journal.pone.0073917. http://dx.doi.org/10.1371/journal.pone.0073917. Medline:24058502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Hawker GA, Mian S, Kendzersja T, et al. Measures of adult pain: Visual analogue scale for pain (VAS pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP) Arthritis Care Res. 2011;63(Suppl 11 S):240–52. doi: 10.1002/acr.20543. http://dx.doi.org/10.1002/acr.20543. [DOI] [PubMed] [Google Scholar]
- 37.Gajdosik RL, Bohannon RW. Clinical measurement of range of motion. Review of goniometry emphasizing reliability and validity. Phys Ther. 1987;67(12):1867–72. doi: 10.1093/ptj/67.12.1867. Medline:3685114. [DOI] [PubMed] [Google Scholar]
- 38.McCaffery M, Pasero C. Pain assessment and pharmacological management. St. Louis (MO): Mosby Inc.; 2011. [Google Scholar]
- 39.Liu J, Cao JG, Wang L, et al. Effect of fibrin sealant on blood loss following total knee arthroplasty: a systematic review and meta-analysis. Int J Surg. 2014;12(2):95–102. doi: 10.1016/j.ijsu.2013.11.011. http://dx.doi.org/10.1016/j.ijsu.2013.11.011. Medline:24316285. [DOI] [PubMed] [Google Scholar]
- 40.Davies AP. Rating systems for total knee replacement. Knee. 2002;9(4):261–6. doi: 10.1016/s0968-0160(02)00095-9. http://dx.doi.org/10.1016/S0968-0160(02)00095-9. Medline:12424032. [DOI] [PubMed] [Google Scholar]
- 41.Tilley S, Thomas N. What knee scoring system? [cited 2013 Aug 13];J Bone Joint Surg. 2010 [4 p.]. Available from: http://www.boneandjoint.org.uk/content/focus/what-knee-scoring-system. [Google Scholar]
- 42.Providence Health Care Connect. Pharmacotherapeutic guidelines. Analgesic dosage equivalences (P&T approved); PHC-equianalgesic potency of opioids [PHC Intranet] Vancouver: Providence Health Care Connect; [cited 2013 Jul 1]. [updated 2012 Nov] [Google Scholar]
- 43.Gippsland Region Palliative Care Consortium Clinical Practice Group. Opioid conversion guidelines [Internet] Warragul, Victoria, Australia: Gippsland Region Palliative Care Consortium; c2011. [cited 2013 Jun 15]. Available from: http://www.gha.net.au/Uploadlibrary/406205172GRPCC-CPG002_1.0_2011-Opioid.pdf. [Google Scholar]
- 44.Sloman R, Wruble AW, Rosen G, et al. Determination of clinically meaningful levels of pain reduction in patients experiencing acute postoperative pain. Pain Manag Nurs. 2006;7(4):153–8. doi: 10.1016/j.pmn.2006.09.001. http://dx.doi.org/10.1016/j.pmn.2006.09.001. Medline:17145489. [DOI] [PubMed] [Google Scholar]
- 45.Frassanito L, Vergari A, Zanghi F, et al. Post-operative analgesia following total knee arthroplasty: comparison of low-dose intrathecal morphine and single-shot ultrasound-guided femoral nerve block: a randomized, single blinded, controlled study. Eur Rev Med Pharmacol Sci. 2010;14(7):589–96. Medline:20707248. [PubMed] [Google Scholar]