Abstract
This review of child disaster mental health intervention studies describes the techniques used in the interventions and the outcomes addressed, and it provides a preliminary evaluation of the field. The interventions reviewed here used a variety of strategies such as cognitive behavioral approaches, exposure and narrative techniques, relaxation, coping skill development, social support, psychoeducation, eye movement desensitization and reprocessing, and debriefing. A diagnosis of posttraumatic stress disorder (PTSD) and/or posttraumatic stress reactions were the most commonly addressed outcomes although other reactions such as depression, anxiety, behavior problems, fear, and/or traumatic grief also were examined. Recommendations for future research are outlined.
Keywords: children, disaster, intervention, outcomes, posttraumatic stress, posttraumatic stress disorder, research, terrorism, therapy, treatment
Introduction
A well-developed research base documenting the deleterious emotional and behavioral effects of disasters and terrorism on children and adolescents1-3 has led to the development, delivery, and evaluation of numerous child disaster mental health interventions. Several review papers describing child trauma interventions, including interventions used in the context of disasters and terrorism, have been published.4-8 Few studies, however, have focused specifically on disasters and terrorism.9-11 This systematic review summarizes the techniques used in child disaster and terrorism interventions, identifies the symptoms and conditions addressed by these interventions, presents a preliminary qualitative evaluation of the evidence base for interventions, and suggests directions for future research.
The Current Review
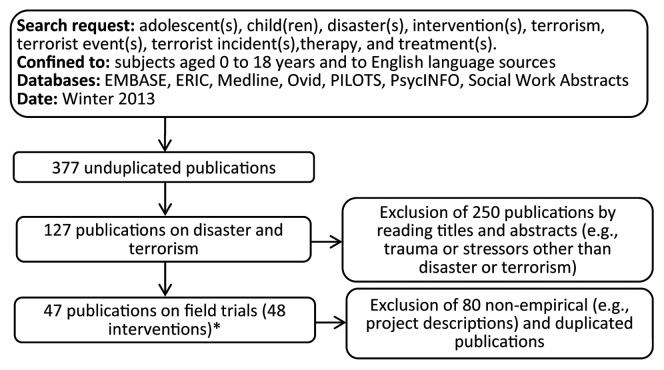
This report was guided by a literature search conducted in the winter of 2013 using EMBASE, ERIC, Medline, Ovid, PILOTS, PsycINFO, and Social Work Abstracts databases. A total of 47 papers were reviewed. One article described a two-stage trial with two different interventions.12 The two interventions were analyzed separately. Hence, the final sample included 48 studies. Figure 1 provides a flowchart of the literature search and results.
Figure 1. Flow diagram of the literature search and research reviewed. *Two stages of one study which described a two-phase trial12 were analyzed separately, resulting in 48 interventions for review.
Five of the selected studies (10.4%), although war-related, were included in the review as the study participants had been exposed to repetitive terrorist attacks.13-17 Three interventions (6.3%) were used in heterogeneous samples of which natural disasters18,19 or terrorism20 were among other traumas (Table 1).
Table 1. Traumatic Events of Studies Included in Current Review.
| Traumatic Event | Frequency Total = 48 (%) |
|---|---|
| Natural disaster | 29 (60.4) |
| Single terrorist attack | 6 (12.5) |
| Chronic terrorism | 5 (10.4) |
| Heterogeneous | 3 (6.3) |
| Technological disaster | 3 (6.3) |
| Hostage | 1 (2.1) |
| Preparedness | 1 (2.1) |
The Samples
As evident in Table 2, the interventions reviewed for this report were provided to children across the age span following a variety of natural and human-caused disasters occurring around the world. Some studies included children representing a wide age range, from 4 or 5 y of age to adolescents or young adults.21-23 One publication reported a case study of a five year old24 and one studied a preschool sample.19 Participants’ disaster exposure was not consistently described and typically was not included in analysis of treatment effects in this body of work. Thus, age and exposure were not examined in the analysis conducted for this report.
Table 2. Description of Studies Included in Current Review.
| Author | Event | Design | Type of Intervention in Treatment Group |
Type of Intervention in Control Group | Sample Size | Age Years/ Grades |
Number of Sessions and Duration of the Intervention |
|---|---|---|---|---|---|---|---|
| Berger and Gelkopf (2009)25 | Indian Ocean tsunami, Sri Lanka (2004) | CRC | Eclectic with CBT | WL | 166 | 9–14/ Elementary school | 12 weekly sessions |
| Berger, Gelkopf and Heineberg (2012)13 | Chronic terrorism including multiple rocket attacks in Sderot, Israel (2000–2008) | CRC | Eclectic with CBT | WL | 154 | 11–13/7–8 | 16 weekly sessions |
| Berger, Pat-Horenczyk and Gelkopf (2007)14 | Chronic terrorism including suicide bombings in Hadera, Israel (2000–2003) | CRC | Eclectic with CBT | WL | 142 | NS/2–6 | 8 sessions |
| Brown, McQuaid et al. (2006)12 (Phase 1: Classroom intervention) | September 11 terrorist attack (2001) | NC | Strict CBT (group) | NA | 62 | 8–13/3–7 | 10 weekly sessions |
| Brown, McQuaid et al. (2006)12 (Phase 2: classroom + individual intervention vs. classroom intervention only) | September 11 terrorist attack (2001) | NRC | Strict CBT (individual) | Strict CBT (group) vs. Strict CBT (group + individual) | 59 | 8–13/3–7 | 10 weekly group sessions in the classroom and 6 individual sessions |
| Brown, Pearlman and Goodman24 (2004) | September 11 terrorist attack (2001) | NC | CBT with Grief Interventions | NA | 1 | 5 | 16 wk |
| Cain et al.21 (2010) | Hurricane Katrina (2005) | NC | PFA | NA | 99 | 5–15/ Elementary and middle school | 6-wk intervention |
| Catani et al.26 (2009) | Indian Ocean tsunami, Sri Lanka (2004) | RC | Narrative and exposure (KIDNET) |
Meditation and relaxation (Med-Relax) | 31 | 8–14/Middle school | 6 sessions completed in 2 wk |
| CATS Consortium (2010)22 | September 11 terrorist attack (2001) | NRC | Strict CBT | Strict CBT | 306 | 5–21/NS | 8–20 sessions for trauma-specific CBT and 4 sessions for brief-CBT skills |
| Chemtob, Nakashima and Carlson (2002)27 | Hurricane Iniki (1992) | RC | EMDR | WL | 32 | 6–12/NS | 3 weekly sessions |
| Chemtob, Nakashima and Hamada (2002)28 | Hurricane Iniki (1992) | RC | Eclectic with no CBT (group) | Eclectic with no CBT (individual) | 248 | 6–12/2–6 | 4 weekly sessions |
| Cohen et al. (2009)29 | Hurricane Katrina (2005) | NC | Strict CBT (CBITS and TF-CBT) |
NA | 2 | 8 and 11 (for case studies)/NS | 10 group sessions and 1–3 individual sessions for CBITS and 12–16 individual sessions for TF-CBT |
| de Roos et al. (2011)23 | Explosion at a fireworks factory in Enschede, Netherlands (2000) | RC | CBT | EMDR | 52 | 4–18/NS | 4 sessions over 4–8 wk |
| Fernandez (2007)30 | Earthquake in Molise, Italy (2002) | NC | EMDR | NA | 22 | 7–11/NS | Average of 6.5 sessions over 1 y |
| Field et al. (1996)31 | Hurricane Andrew (1992) | RC | Massage | Placebo video attention control group | 60 | NS/1–5 | 8 sessions |
| Galante and Foa (1986)32 | Earthquake in Central Italy (1980) | NC | Eclectic with no CBT | NA | 300 | NS/1–4 | 7 sessions |
| Gelkopf and Berger 2009)15 | Chronic terrorism including multiple terror attacks in Beer Sheba, Israel (2000–2006) | RC | Eclectic with CBT | WL | 107 | NS/7–8 | 12 sessions |
| Giannopoulou et al. (2006)33 | Earthquake in Athens, Greece (1999) | NRCa | Strict CBT | WL | 17 | 8–12/NS | 6 weekly sessions |
| Gilboa-Schechtman et al. (2010)20 | Heterogeneous including terrorist attacks, motor vehicle accidents, and sexual and nonsexual assaults in Israel | RC | Exposure therapy (PE-A) | Psychodynamic therapy (TLDP-A) | 38 | 12–18/NS | 12–15 weekly sessions for PE-A and 15–18 sessions for TLDP-A |
| Goenjian et al. (1997)34 | Earthquake in Spitak, Armenia (1988) | NRC | Eclectic with CBT | NTC | 64 | NS/6–7 | 4 group and 2 individual sessions over 3 wk |
| Goenjian et al. (2005)35 | Earthquake in Spitak, Armenia (1988) | NRC | Eclectic with CBT | NTC | 63 | 15–17/NS | 4 group and 2 individual sessions over 3 wk |
| Goodman et al. (2004)36 | September 11 terrorist attack (2001) | NC | Client centered therapy | NA | 1 | 15/High school | 5 mo |
| Hardin et al. (2002)38 | Hurricane Hugo (1989) | CRC | Eclectic with CBT | NTC | 1030 | 13–18/High school | 3 sessions per year for 3 y |
| Jaycox et al. (2010)38 | Hurricane Katrina (2005) | RC | Strict CBT (TF-CBT) |
Strict CBT (CBITS) | 118 | NS/4–8 | 10 group sessions and 1–3 individual sessions for CBITS and 12 individual sessions or conjoint sessions with parent for TF-CBT |
| Karairmak and Aydin (2008)39 | Earthquake in the Marmara region, Turkey (1999) | RC | Cognitive therapy | Placebo attention control group | 20 | NS/NS | 9 sessions over 3 wk |
| Lesmana et al. (2009)40 | Terrorist attack in Bali, Indonesia (2002) | RC | Spiritual hypnosis | NTC | 226 | 6–12/NS | 1 session |
| Mahmoudi-Gharaei et al. (2009)41 | Earthquake in Bam, Iran (2003) | RC | Eclectic with CBT | WL | 85 | 11–18/NS | 4 weekly sessions |
| Mahmoudi-Gharaei et al. (2009)42 | Earthquake in Bam, Iran (2003) | RC | Eclectic with CBT | Art and sport activities; Eclectic with CBT; WL | 161 | 6–11/NS | 4 sessions |
| March et al. (1998)18 | Heterogeneous including car accidents, severe storms, accidental and gunshot injury, severe illness, and fires | NRC | Strict CBT | WL | 17 | 10–15/4–9 | 18 weekly sessions |
| Plummer et al. (2009)43 | Hurricane Katrina (2005) | NC | PFA | NA | 12 | 6–13/ Elementary and middle school |
6 wk |
| Ronan and Johnston (1999)44 |
Volcanic eruptions of Mount Ruapehu, New Zealand (1995) | CRC | Eclectic with CBT | Video based exposure and normalizing condition | 112 | 7–13/NS | 1 session |
| Ronan and Johnston (2003)45 |
Hazard education-preparedness, New Zealand | CRC | Emergency hazard educationb | Usual hazard educationb | 219 | 11–13/NS | 1 class period per day over six weeks for UC and NS for EM |
| Sahin et al. (2011)46 |
Earthquake in the Marmara region, Turkey (1999) |
NRC | Psychoeducation | NTC | 774 | NS/NS | NS |
| Salloum and Overstreet (2008)47 |
Hurricane Katrina (2005) | RC | Eclectic with CBT (individual) | Eclectic with CBT (group) | 56 | 7–12/NS | 10 sessions |
| Salloum and Overstreet (2012)48 |
Hurricane Katrina (2005) | RC | Eclectic with CBT (GTI-CN) |
Eclectic with CBT (GTI-C) |
70 | 6–12/2–6 | 11 sessions |
| Scheeringa et al. (2011)19 | Heterogeneous including Hurricane Katrina (2005), acute injury, and witness to domestic violence | RC | Strict CBT | WL | 64 | 3–6/NS | 12 sessions |
| Shen (2002)49 | Earthquake in Taiwan (1999) | RC | Play therapy | NTC | 30 | 8–12/3–6 | 10 sessions over 4 wk |
| Shooshtary et al. (2008)50 | Earthquake in Bam, Iran (2003) | NRC | Eclectic with CBT | WL | 168 | 11–20/NS | 4 sessions over 4 wk |
| Taylor and Weems (2011)51 | Hurricane Katrina (2005) | NC | Strict CBT | NA | 6 | 8–13/NS | 10 weekly sessions |
| Vijayakumar et al. (2006)52 | Indian Ocean tsunami, Srinivasapuram, India (2004) |
NRC | Eclectic with CBT | NTC | 135 | 11–14/NS | 6 sessions over 6 mo |
| Vila et al. (1999)53 | School hostage crisis in Paris, France (1995) | NRC | Debriefing | NTC | 26 | 6–9.5/1 and 3 | Debriefing at 24 h and 6 wk post event |
| Weems et al. (2009)54 | Hurricane Katrina (2005) | CRC | Eclectic with CBT | NTC | 94 | 13–16/9 | 5 sessions over 4–5 wk |
| Wolmer, Hamiel, Barchas, Slone, Laor (2011)16 | Second Lebanon War (Chronic terrorism) (2006) |
NRC | Eclectic with CBT | WL | 2135 | 8–12/3–6 | 15 weekly modules |
| Wolmer, Hamiel and Laor (2011)17 | Chronic terrorism with preventive intervention before rocket attacks, Operation Cast Lead, Israel (2008–2009) | NRC | Eclectic with CBT | WL | 1488 | NS/4–5 | 14 weekly modules |
| Wolmer, Laor, Dedeoglu et al. (2005)c, 55 | Earthquake in the Marmara region, Turkey (1999) | NRC | Eclectic with CBT | NTC | 287 | 9–17/NS | 8 twice-weekly sessions |
| Wolmer, Laor and Yazgan (2003)56 | Earthquake in the Marmara region, Turkey (1999) | NC | Eclectic with CBT | NA | 202 | NS/1–5 | 8 twice-weekly sessions |
| Yule (1992)57 | Jupiter cruise ship sinking at the Greek port of Piraeus (1988) | NRC | Debriefing and CBT | NTC | 39 | 14–16/NS | 1 session of debriefing and 2 CBT group sessions |
| Yule and Udwin (1991)58 | Jupiter cruise ship sinking at the Greek port of Piraeus (1988) | NC | Debriefing | NA | 24 | 14–16/NS | 1 session of debriefing |
Notes: CBITS, Cognitive Behavioral Intervention for Trauma in Schools; CBT, cognitive behavioral therapy; EMDR, Eye Movement Desensitization and Reprocessing; GTI-C, Grief and Trauma Intervention with Coping Skills; GTI-CN, Grief and Trauma Intervention with Coping Skills and Trauma Narrative Processing; KIDNET, Narrative Exposure Therapy for Children; NA, not applicable; NC, non-controlled study; NRC, non-randomized controlled study; NS, not specified; NTC, non-treatment control; PE-A, Prolonged Exposure Therapy for Adolescents; PFA, Psychological First Aid; RC, randomized controlled study; CRC, cluster-randomized controlled study; TF-CBT, Trauma-Focused Cognitive Behavioral Therapy; TLDP-A, Time-Limited Dynamic Psychotherapy for Adolescents; WL, waitlist; aThe two treatment groups (immediate treatment and delayed treatment) were merged for the analysis; bThe usual hazard education included reading of hazard-related materials and classroom discussions. In addition to the readings and classroom discussions, children in the emergency management education condition were given additional material related to hazard adjustments and guided interactions through homework to be completed with their parents; cWolmer and colleagues55 is a follow-up to an earlier study by the same group.56
Intervention Techniques
The interventions reviewed for this report used a variety of techniques to address children’s disaster reactions, and many interventions utilized multiple techniques. The most commonly used techniques could be characterized as cognitive behavioral in nature. See Table 2. Some interventions used exposure20,54 or narrative22,26,34,48 techniques. Relaxation also was used commonly as one component among others or in combination with other techniques in the interventions studied.12,21,24,33,34,38,39,41-43,48,50,54 For example, Catani and colleagues26 found both narrative exposure and meditation-relaxation interventions to be effective in children following the Indian Ocean tsunami, with no significant difference between the two interventions in any outcome measure. Also, Weems and colleagues54 used relaxation training coupled with gradual exposure to address test anxiety in ninth graders exposed to Hurricane Katrina.
Many interventions incorporated components to enhance coping12,22,43,44,48 and some provided a social support component.14,15,21,35,37,44,48 For example, using a cognitive behavioral approach, Brown and colleagues12 helped children develop a coping “tool box” by teaching them a variety of coping techniques. Berger and Gelkopf25 administered the ERASE Stress intervention which focused on teaching children coping skills to address anger, loss, fears, and other emotions. Some interventions used enhancement of social support as a type of coping skill. For example, ERASE Stress included a session on building social support and asking for help,25 and Salloum and Overstreet48 conceptualized “reconnection” as a coping strategy.
Psychoeducation was incorporated along with other techniques in numerous studies.15,21,22,24,35,46 In some studies, psychoeducation was delivered repeatedly throughout the course of the intervention. For instance, Gelkopf and Berger’s15 ERASE Stress intervention included a psychoeducation component in every session. In other studies, psychoeducation was used only early in the intervention.24 One study examined an intervention in which psychoeducation was the primary component.47
Eye Movement Desensitization and Reprocessing (EMDR)23,27,30 and dual attention tasks associated with EMDR techniques33,50 were included in some studies. Debriefing was the key intervention examined in two studies.53,57 Others included debriefing as one technique in their cognitive behavioral interventions but did not examine the debriefing component separate from other elements of their intervention.41,42,50
Several interventions used techniques not commonly studied. For example, nondirective, non-trauma-focused time-limited dynamic therapy was the control condition in a study of exposure.20 Client centered treatment, involving empathy as an essential aspect of the therapy, was provided by Goodman and colleagues36 in a case study of childhood traumatic grief after the September 11 World Trade Center attacks. One study evaluated massage therapy for classroom behavior problems in children after Hurricane Andrew31 while another study examined spiritual hypnosis for the treatment of posttraumatic stress disorder (PTSD) in children after a terrorist attack.40 Shooshtary and colleagues50 used a kinesthetic technique with “touch, message and movement” in their earthquake intervention.
Symptoms and Conditions Addressed in Interventions
Children’s post-disaster adjustment reflects a wide range of emotional and behavioral reactions. The outcomes typically used in assessing the efficacy of interventions included PTSD and posttraumatic stress reactions, depression, anxiety, functioning, behavior problems, anger, somatic complaints, fear, and traumatic grief. Studies of intervention efficacy have used both pre/post assessment and controlled trials. Summary information on outcomes according to the research design of studies is presented in Table 3 which displays the number of studies using pre/post and control design for each of the major outcomes examined. Table 3 also identifies the number and percentage of studies demonstrating improvement, no change, and worse outcomes using pre/post assessment and those with superior outcomes, no significant differences, and inferior outcomes in controlled trials.
Table 3. Number of Studies by Design for Each Major Outcome.
| Outcome | PTSD | Posttraumatic Stress Reactions | Depression | Anxiety | Functioning | Behavior Problemsc | Somatic complaints | Anger | Fear | Grief | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Total number (%) of studies that measured the outcome (Total = 48) |
16 (33.3) | 41 (85.4) | 20 (41.7) | 17 (35.4) | 10 (20.8) | 9 (18.8) | 6 (12.5) | 4 (8.3) | 4 (8.3) | 4 (8.3) | |
| Number (%) of studies with pre-/post intervention assessment | Improved | 15 (100.0) | 32 (86.5) | 13 (68.4) | 11 (73.3) | 8 (88.9) | 4 (44.4) | 4 (66.7) | 3 (75.0) | 2 (100.0) | 2 (66.7) |
| No Change | 0 (0.0) | 5 (13.5) | 4 (21.1) | 3 (20.0) | 1 (11.1) | 5 (55.6) | 2 (33.3) | 1 (25.0) | 0 (0.0) | 0 (0.0) | |
| Worse | 0 (0.0) | 0 (0.0) | 2 (10.5) | 1 (6.7) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 1 (33.3) | |
| Total | 15a | 37 | 19 | 15 | 9 | 9 | 6 | 4 | 2 | 3 | |
| Number (%) of controlled trials | Superior | 7 (70.0) | 17 (60.7) | 6 (42.9) | 6 (50.0) | 6 (85.7) | 0 (0.0) | 4 (66.7) | 0 (0.00 | 1 (33.3) | 0 (0.0) |
| NSD | 3 (30.0) | 11 (39.3) | 8 (57.1) | 6 (50.0) | 1 (14.3) | 6 (100.0) | 2 (33.3) | 1 (100.0) | 1 (33.3) | 3 (100.0) | |
| Inferior | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 1 (33.3) | 0 (0.0) | |
| Total | 10b | 28 | 14 | 12 | 7 | 6 | 6 | 1 | 3 | 3 |
NSD, Non significant difference; aFor the purpose of this review, an exact McNemar test using the data presented by the authors was performed for a pre-/post assessment of the treatment effect on PTSD diagnosis in the intervention group in six studies where the authors did not perform such evaluation.14,18,20,25,26,38; bFor the purpose of this review, an independent chi-square test using the data presented by the authors was performed for a between-group comparison of the treatment effect on PTSD diagnosis in two studies where the authors did not perform a statistical test for such assessment.14,25; cBehavioral difficulties did not include ADHD or hyperactivity disorder.
As evident in Table 3, posttraumatic stress reactions (n = 41, 85.4%) were the most commonly assessed mental health outcome for the intervention studies included in the present review. PTSD was examined in 16 (33.3%) of the studies. Some studies used terminology such as “caseness”18 or “probable PTSD”22,25 in describing outcomes to acknowledge that an actual diagnosis was not given but that empirically-derived thresholds and patterns were determined for trauma-related symptoms. Rather than focusing exclusively on posttraumatic stress reactions, outcomes must be appropriate for the intervention delivered. For example, Vijayakumar and colleagues52 attributed their failure to find improvement in PTSD symptoms in children who participated in their intervention relative to a non-treatment control to the fact that the largely psychoeducational intervention was not intended to address trauma symptoms. Rather, it focused on other behaviors. The study revealed positive results for two outcomes—desisting smoking and the expression of positive emotions.
Given the high comorbidity of depression with PTSD in traumatized children,3 it is not surprising that many interventions (n = 20, 41.7%) included depression as an outcome measure. Brown and colleagues12 found that depression improved in children who received their September 11 classroom-based intervention. Interestingly, depression worsened in children who received an individualized intervention delivered to those who remained symptomatic following the classroom intervention. The authors suggested that perhaps the social support inherent in the classroom intervention was essential to improvement in depression.12
Behavioral problems were examined in nine studies (18.8%)12,18,19,23,24,36,48,49,52 In addition to oppositional defiant disorder, Scheeringa and colleagues19 assessed ADHD as an outcome finding improvement in symptoms of oppositional defiant disorder but not ADHD symptoms. Vijayakumar and colleagues52 found the opposite—a reduction in hyperactivity but not in oppositional or conduct problems—in their controlled trial of a psychosocial intervention for children after the 2004 Indian Ocean tsunami. Children receiving the intervention were more likely than those in the control group to report that they could resist peer pressure and desist smoking.52
Four studies examined fear32,39,45,57 One study found an activity-based cognitive fear-reduction intervention inferior to a placebo control group that provided structured activities and games in a small sample of children exposed to an earthquake.39 The investigators implicated the brevity of the intervention and the lack of a parent component in the intervention’s failure.39 In general, the benefits of including parents in interventions have been understudied.59
Children and adolescents may experience concomitant trauma and grief symptoms if they lose loved ones as a result of a disaster. In their study of a teacher-mediated intervention for children after an earthquake in Turkey, Wolmer and colleagues56 found improvement in PTSD symptoms while self-reported grief symptoms increased. Explanations for this finding are that the resolution of trauma allowed the grief process to begin, the intervention did not adequately address grief symptoms, and/or reporting bias. Three years later, grief symptoms, as reported by participants’ parents, had improved in the treatment group, but there was no significant difference between the treatment and non-treatment control groups at follow up. The observed improvement in grief symptoms in the treatment group could be artifactual, however, and explained by the difference in informants. Salloum and Overstreet conducted two studies of grief and trauma interventions. In their first study published in 2008,47 they found improvement in children’s self-reported grief after the intervention, with no significant difference between those who received the intervention in individual vs. group format. In their 2012 study, these investigators found significant improvement in self-reported traumatic grief after a grief and trauma intervention that used a coping skills component as well as with one that used both the coping skills component and trauma narrative processing.48
Functional impairment and/or clinically-significant distress is an essential criterion for a diagnosis of PTSD.60 Only ten (20.8%) of the studies in this review examined functioning.13-15,20,24-26,33,36,55 For example, Wolmer and colleagues55 asked teachers who were blind to the children’s participation in the intervention program to assess the children on three domains of daily functioning: academic performance, social behavior, and general conduct in the academic setting. Because it is a key criterion in the diagnosis of many psychological disorders, and because it is closely related to the child’s quality of life, functional impairment should be studied routinely as an outcome. Another three studies examined mental37 or global47,48 distress which are not included in the counts in Table 3.
Course of Recovery in Treatment Samples
The choice of an intervention must be matched to the child’s reactions and to the course of symptom development and recovery following exposure to disasters. La Greca and colleagues61 identified three trajectories of posttraumatic stress symptoms (resilient, recovery, and chronic) in children exposed to Hurricane Andrew over the course of one year with assessments at 3, 7 and 10 mo post disaster, and with no intervention delivered by the authors. Although mean posttraumatic stress symptom scores decreased significantly over time in all three trajectories, the mean posttraumatic stress symptom score for children in the chronic trajectory (20%) remained above the clinical cut-off beyond seven months. Intervention studies speak to the intractable nature of post-disaster pathology. For example, despite demonstrated efficacy for both a clinic- and a school-based cognitive behavioral intervention in children 15 mo after Hurricane Katrina, Jaycox and colleagues38 found that 65% of the children in the school-based group and 43% in the clinic group scored in the “at risk” range of PTSD at a follow-up assessment 10 mo post intervention. Wolmer and colleagues55 noted that symptoms will subside in most children while some will continue to have difficulty even after intervention. The authors suggested that children with moderate or subclinical PTSD, who are at risk due to exposure and/or prior traumatic experiences, be followed and reevaluated over time after the intervention.
While PTSD reactions and anxiety are likely to occur early in the post-disaster course and to continue if untreated, depression may have later onset and may persist.34 The course of symptom development and recovery may affect the response to interventions. For example, Goenjian and colleagues35 failed to demonstrate a change in depression with their earthquake intervention, but depression increased in the control group from pre to post treatment. Brown, McQuaid, and colleagues12 found that the effect of their September 11 classroom intervention on depression was not sustained even for children who received a subsequent individual intervention that was associated with improvement in posttraumatic stress symptoms. Speculating that social support, not a component in the individual intervention, may have accounted for the improvement in depression in the classroom intervention, the researchers called for future research regarding interventions for depression.12 Thus, service providers should consider the trajectory of disaster reactions in selecting interventions. Comprehensive evaluation and intensive and traditional treatment along with enhanced attention to social support may be needed for children who are at elevated risk and for those who suffer enduring clinical problems.
Preliminary Evaluation of the Evidence Base
A preliminary evaluation of the evidence base for child disaster mental health interventions requires a review of the research design of extant studies. An essential next step in intervention development will be to dismantle and evaluate specific intervention components and to compare various intervention techniques and modalities.
Research Design
Clinical practice guidelines have prioritized studies using randomized controlled trials at the highest level in establishing the evidence base for trauma interventions.62-65 The use of control groups makes it possible to determine if observed changes can be attributed to the intervention rather than to unrelated factors such as the mere passage of time.66 Thus, it is encouraging that more than three quarters of the studies (n = 37, 77.1%) in this review used a controlled design. The types of controls included other therapeutic interventions (n = 11, 29.7%), non-treatment controls (n = 11, 29.7%), waitlist controls (n = 12, 32.4%), and placebo controls (n = 2, 5.4%). See Table 2. Following an earthquake, Mahmoudi-Gharaei and colleagues42 compared four group interventions: group behavioral therapy, group behavioral therapy with art and sport interventions, art and sport interventions, and a waitlist control group. While PTSD symptoms did not decrease significantly with any of the interventions, PTSD symptoms increased in the group that received no intervention.
Randomized controlled trials, the gold standard for experimental studies, require a controlled design with participants randomly assigned to treatment arms to balance the groups regarding known and unknown factors that may be associated with treatment outcome. While more than one half (n = 23, 62.2%) of the controlled trials in this review randomly assigned individual participants to treatment groups, greater adoption of random assignment is needed to perform rigorous comparisons between different types of treatments. See Table 2.
Only one study found an inferior result for the intervention condition relative to the control condition.39 Karairmak and Aydin39 reported higher levels of fear in their intervention group compared with the control group post treatment. Fear was the only outcome measured for the trial and no pre/post test results were reported. Additionally, as discussed by the authors, the treatment control, labeled as “placebo,” which included structured activities and games, may have had a therapeutic effect. Moreover, the duration of the intervention may have been too brief to confer benefit, and the involvement of parents may have improved the outcome.39
Dismantling Interventions and Comparing Interventions
Few studies have tried to dismantle interventions to better identify the specific components or techniques responsible for benefit or to better understand the mechanism of action for interventions. In their study of elementary-school children three years post Hurricane Katrina, Salloum and Overstreet48 questioned the need for a structured trauma narrative as part of a coping skill-enhancement trauma and grief intervention though the investigators acknowledged that the children in their study who did not receive the structured trauma narrative did engage in discussion about their experiences. A related issue is the importance of sequencing of intervention components. Future investigations should identify the types and order of techniques, procedures, and activities for children’s optimal recovery.
Relatively few studies have compared interventions. de Roos and colleagues23 compared the effectiveness of EMDR and cognitive behavioral therapy in the treatment of children with trauma-related psychological symptoms after a factory explosion in the Netherlands. Both interventions were effective in reducing the symptoms, and their effects were not statistically different. Analyses revealed, however, that the cognitive behavioral intervention required more treatment sessions than EMDR to obtain similar results.23 Gilboa-Schechtman and colleagues20 found that participants who completed prolonged exposure therapy and those who completed time-limited dynamic therapy experienced a decrease in depressive symptoms, but the exposure group reported more improvement than did the dynamic therapy group after treatment and at six-month follow up. The superiority of exposure was not maintained at 17-mo follow-up, however.20 It is unclear how important the early superior benefits associated with exposure therapy were for the adolescents in this study as key developmental changes and milestones may occur over brief periods of months in youth. Other studies have failed to support one intervention over another26,38,44,47 suggesting that perhaps common factors among interventions (e.g., aspects of the therapeutic relationship, focused attention on the trauma history and reactions, expectation of benefit) may account for at least some of the benefit. Thus, the field awaits studies that dismantle interventions and those that compare interventions to determine which components and mechanisms of action are responsible for general and specific benefits.
Placing Disaster Intervention Studies in the Larger Context of Child Trauma
The American Academy of Child and Adolescent Psychiatry practice parameter on the assessment and treatment of posttraumatic stress disorder (PTSD)62 in children voices support for the use of trauma-focused cognitive behavioral interventions in traumatized children. More formal studies, however, have identified limitations in the extant intervention research for various forms of trauma. For example, in his 2006 review of randomized controlled trials of child trauma interventions, which included primarily cognitive behavioral interventions for sexually abused girls, Stallard7 concluded that “deconstruction studies” are needed to determine the effective ingredients of interventions and to match intervention components to specific symptoms or conditions and the various demographics, experiences, and exposures of the children receiving them. Seeking to match treatment modalities with outcomes in sexually-abused children, a meta-analytic investigation found play therapy most effective for social functioning; cognitive behavioral therapy, abuse-specific, and supportive therapy best for behavior problems; cognitive behavioral therapy, family, and individual therapy most effective for psychological distress; and abuse-specific, cognitive behavioral therapy, and group therapy most effective for low self-concept.67 In a review of psychosocial interventions for traumatized children, Silverman and colleagues6 also found support for cognitive behavioral therapy for PTSD outcomes but called for more rigorous large-scale studies. In a recent Cochrane review, Gillies and colleagues68 (p. 21) also concluded that while there is “fair evidence for the effectiveness of psychological therapies,” especially cognitive behavioral therapy, for the treatment of PTSD in children exposed to a range of traumatic experiences, there is “no clear evidence” that any one therapy is superior to others. Thus, intervention research is needed across all forms of childhood trauma.
Conclusions and Future Directions
The current review using a descriptive approach suggests that a variety of interventions reduce posttraumatic stress, depression, anxiety, behavior problems, traumatic grief, and other psychological, behavioral, and somatic reactions. Most investigations examined posttraumatic stress reactions, depression, and anxiety with fewer studying behavior problems, somatic complaints, anger, traumatic grief, fear, and functional impairment. An overreliance on the assessment of PTSD and posttraumatic stress reactions is imprudent as it fails to address the complexity and the spectrum of stress responses (e.g., internalizing, externalizing, and somatic symptoms) that emerge over the months and years that follow children’s exposure to a disaster and to the ensuing secondary adversities.
The specific techniques responsible for the positive outcomes in the intervention studies examined thus far remain unclear. Numerous investigations found no significant differences in the intervention and control conditions.26,38,44,47,48 It is possible that natural recovery and/or some common factors among interventions accounted for the benefit found with some interventions. Moreover, not every traumatized child requires structured intensive mental health treatment.52,69 Many children exposed to disasters will recover with basic public health interventions such as psychoeducation and social support. Moreover, some children and their families will not desire intervention services after a disaster.69 Because of the diverse posttraumatic trajectories children experience, not every child will benefit from the same set of services. Thus, those planning services must match interventions with the specific reactions and conditions experienced by the children being served and should consider adopting a stepped care approach where some services, such as public health interventions, are provided to all children, and other techniques are offered to children as indicated by their clinical status.12,70 The next generation of research should help to clarify which children require intervention and match specific interventions to children’s needs.
To ascertain the effects of disaster mental health interventions and natural recovery on children’s posttraumatic reactions, it is recommended that studies include control groups as well as other elements of well-designed studies such as clearly defined target symptoms, reliable and valid measures, blinded evaluators, assessor training, replicable interventions, random assignment, and treatment adherence measures.71 This review did not examine the types of controls used or other elements of well-designed studies, but that is also necessary. A host of factors have the potential to influence the results of intervention studies including: (1) characteristics of the children who receive interventions, their disaster exposures and experiences, and their family and social situations; (2) additional factors related to the interventions and the context of service delivery; and (3) other methodological issues. For example, this review did not examine the developmental, cultural, or experiential characteristics of the children studied. Taking an all-hazards approach, the analysis also did not compare interventions used in disaster situations and those used for terrorism. Some, but not all, aspects of the interventions and details of service delivery are covered in a related publication.59 Other methodological issues await evaluation, including the timing of intervention delivery, the effects of attrition from study, and the use and length of follow-up assessment. Future review studies should conduct quantitative assessments of child disaster outcomes.
Acknowledgments
This work was funded in part by the National Institute of Mental Health, the National Institute of Nursing Research, and the Substance Abuse and Mental Health Services Administration (5 R25 MH070569) which established the Child and Family Disaster Research Training and Education Program at the Terrorism and Disaster Center (TDC) at the University of Oklahoma Health Sciences Center. TDC is a partner in the National Child Traumatic Stress Network and is funded by the Substance Abuse and Mental Health Services Administration (1 U79 SM57278).
Points of view in this document are those of the authors and do not necessarily represent the official position of Courtroom Sciences, Inc.; the Duke University Medical Center; the National Child Traumatic Stress Network; the National Institute of Mental Health; the National Institute of Nursing Research; the Substance Abuse and Mental Health Services Administration; the Tulsa Institute of Trauma, Abuse and Neglect; the United States Department of Veterans Affairs; the University of Miami School of Medicine; the University of Oklahoma Health Sciences Center; or the University of Tulsa.
References
- 1.Furr JM, Comer JS, Edmunds JM, Kendall PC. . Disasters and youth: a meta-analytic examination of posttraumatic stress. J Consult Clin Psychol 2010; 78:765 - 80; http://dx.doi.org/ 10.1037/a0021482; PMID: 21114340 [DOI] [PubMed] [Google Scholar]
- 2.Norris FH, Friedman MJ, Watson PJ, Byrne CM, Diaz E, Kaniasty K. . 60,000 disaster victims speak: Part I. An empirical review of the empirical literature, 1981-2001. Psychiatry 2002; 65:207 - 39; http://dx.doi.org/ 10.1521/psyc.65.3.207.20173; PMID: 12405079 [DOI] [PubMed] [Google Scholar]
- 3.Silverman WK, La Greca AM. Children experiencing disasters: Definitions, reactions, and predictors of outcomes. In: La Greca, AM, Silverman WK, Vernberg EM, Roberts MC, eds. Helping Children Cope with Disasters and Terrorism. Washington, DC: American Psychological Association, 2002: 11-33. [Google Scholar]
- 4.Feeny NC, Treadwell KRH, Foa EB, March J. . Posttraumatic stress disorder in youth: A critical review of the cognitive and behavioral treatment outcome literature. Prof Psychol Res Pr 2004; 35:466 - 76; http://dx.doi.org/ 10.1037/0735-7028.35.5.466 [DOI] [Google Scholar]
- 5.Rolfsnes ES, Idsoe T. . School-based intervention programs for PTSD symptoms: a review and meta-analysis. J Trauma Stress 2011; 24:155 - 65; http://dx.doi.org/ 10.1002/jts.20622; PMID: 21425191 [DOI] [PubMed] [Google Scholar]
- 6.Silverman WK, Ortiz CD, Viswesvaran C, Burns BJ, Kolko DJ, Putnam FW, Amaya-Jackson L. . Evidence-based psychosocial treatments for children and adolescents exposed to traumatic events. J Clin Child Adolesc Psychol 2008; 37:156 - 83; http://dx.doi.org/ 10.1080/15374410701818293; PMID: 18444057 [DOI] [PubMed] [Google Scholar]
- 7.Stallard P. . Psychological interventions for post-traumatic reactions in children and young people: a review of randomised controlled trials. Clin Psychol Rev 2006; 26:895 - 911; http://dx.doi.org/ 10.1016/j.cpr.2005.09.005; PMID: 16481081 [DOI] [PubMed] [Google Scholar]
- 8.Wethington HR, Hahn RA, Fuqua-Whitley DS, Sipe TA, Crosby AE, Johnson RL, Liberman AM, Mościcki E, Price LN, Tuma FK, et al. , Task Force on Community Preventive Services. . The effectiveness of interventions to reduce psychological harm from traumatic events among children and adolescents: a systematic review. Am J Prev Med 2008; 35:287 - 313; http://dx.doi.org/ 10.1016/j.amepre.2008.06.024; PMID: 18692745 [DOI] [PubMed] [Google Scholar]
- 9.Forman-Hoffman VL, Zolotor AJ, McKeeman JL, Blanco R, Knauer SR, Lloyd SW, Fraser JG, Viswanathan M. . Comparative effectiveness of interventions for children exposed to nonrelational traumatic events. Pediatrics 2013; 131:526 - 39; http://dx.doi.org/ 10.1542/peds.2012-3846; PMID: 23400617 [DOI] [PubMed] [Google Scholar]
- 10.La Greca AM, Silverman WK. . Treatment and prevention of posttraumatic stress reactions in children and adolescents exposed to disasters and terrorism: What is the evidence?. Child Dev Perspect 2009; 3:4 - 10; http://dx.doi.org/ 10.1111/j.1750-8606.2008.00069.x [DOI] [Google Scholar]
- 11.La Greca AM, Silverman WK. Interventions for youth following disasters and acts of terrorism. In: Kendall PC (ed.) Child and Adolescent Therapy (4th Ed). Cognitive-Behavioral Procedures. NewYork, NY: The Guilford Press, 2011:324-344. [Google Scholar]
- 12.Brown EJ, McQuaid J, Farina L, Ali R, Winnick-Gelles A. . Matching interventions to children’s mental health needs: Feasibility and acceptability of a pilot school-based trauma intervention program. Educ Treat Child 2006; 29:257 - 86 [Google Scholar]
- 13.Berger R, Gelkopf M, Heineberg Y. . A teacher-delivered intervention for adolescents exposed to ongoing and intense traumatic war-related stress: a quasi-randomized controlled study. J Adolesc Health 2012; 51:453 - 61; http://dx.doi.org/ 10.1016/j.jadohealth.2012.02.011; PMID: 23084166 [DOI] [PubMed] [Google Scholar]
- 14.Berger R, Pat-Horenczyk R, Gelkopf M. . School-based intervention for prevention and treatment of elementary-students’ terror-related distress in Israel: a quasi-randomized controlled trial. J Trauma Stress 2007; 20:541 - 51; http://dx.doi.org/ 10.1002/jts.20225; PMID: 17721962 [DOI] [PubMed] [Google Scholar]
- 15.Gelkopf M, Berger R. . A school-based, teacher-mediated prevention program (ERASE-Stress) for reducing terror-related traumatic reactions in Israeli youth: a quasi-randomized controlled trial. J Child Psychol Psychiatry 2009; 50:962 - 71; http://dx.doi.org/ 10.1111/j.1469-7610.2008.02021.x; PMID: 19207621 [DOI] [PubMed] [Google Scholar]
- 16.Wolmer L, Hamiel D, Barchas JD, Slone M, Laor N. . Teacher-delivered resilience-focused intervention in schools with traumatized children following the second Lebanon War. J Trauma Stress 2011; 24:309 - 16; http://dx.doi.org/ 10.1002/jts.20638; PMID: 21618288 [DOI] [PubMed] [Google Scholar]
- 17.Wolmer L, Hamiel D, Laor N. . Preventing children’s posttraumatic stress after disaster with teacher-based intervention: a controlled study. J Am Acad Child Adolesc Psychiatry 2011; 50:340 - 8, e1-2; http://dx.doi.org/ 10.1016/j.jaac.2011.01.002; PMID: 21421174 [DOI] [PubMed] [Google Scholar]
- 18.March JS, Amaya-Jackson L, Murray MC, Schulte A. . Cognitive-behavioral psychotherapy for children and adolescents with posttraumatic stress disorder after a single-incident stressor. J Am Acad Child Adolesc Psychiatry 1998; 37:585 - 93; http://dx.doi.org/ 10.1097/00004583-199806000-00008; PMID: 9628078 [DOI] [PubMed] [Google Scholar]
- 19.Scheeringa MS, Weems CF, Cohen JA, Amaya-Jackson L, Guthrie D. . Trauma-focused cognitive-behavioral therapy for posttraumatic stress disorder in three-through six year-old children: a randomized clinical trial. J Child Psychol Psychiatry 2011; 52:853 - 60; http://dx.doi.org/ 10.1111/j.1469-7610.2010.02354.x; PMID: 21155776 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Gilboa-Schechtman E, Foa EB, Shafran N, Aderka IM, Powers MB, Rachamim L, Rosenbach L, Yadin E, Apter A. . Prolonged exposure versus dynamic therapy for adolescent PTSD: a pilot randomized controlled trial. J Am Acad Child Adolesc Psychiatry 2010; 49:1034 - 42; http://dx.doi.org/ 10.1016/j.jaac.2010.07.014; PMID: 20855048 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Cain DS, Plummer CA, Fisher RM, Bankston TQ. . Weathering the storm: Persistent effects and psychological first aid with children displaced by Katrina. J Child Adolesc Trauma 2010; 3:330 - 43; http://dx.doi.org/ 10.1080/19361521.2010.523063 [DOI] [Google Scholar]
- 22.CATS Consortium. . Implementation of CBT for youth affected by the World Trade Center disaster: matching need to treatment intensity and reducing trauma symptoms. J Trauma Stress 2010; 23:699 - 707; http://dx.doi.org/ 10.1002/jts.20594; PMID: 21171130 [DOI] [PubMed] [Google Scholar]
- 23.de Roos C, Greenwald R, den Hollander-Gijsman M, Noorthoorn E, van Buuren S, de Jongh A. . A randomised comparison of cognitive behavioural therapy (CBT) and eye movement desensitisation and reprocessing (EMDR) in disaster-exposed children. Eur J Psychotraumatol 2011; 2:1 - 11; http://dx.doi.org/ 10.3402/ejpt.v2i0.5694; PMID: 22893815 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Brown EJ, Pearlman MY, Goodman RF. . Facing fears and sadness: cognitive-behavioral therapy for childhood traumatic grief. Harv Rev Psychiatry 2004; 12:187 - 98; http://dx.doi.org/ 10.1080/10673220490509516; PMID: 15371061 [DOI] [PubMed] [Google Scholar]
- 25.Berger R, Gelkopf M. . School-based intervention for the treatment of tsunami-related distress in children: a quasi-randomized controlled trial. Psychother Psychosom 2009; 78:364 - 71; http://dx.doi.org/ 10.1159/000235976; PMID: 19738402 [DOI] [PubMed] [Google Scholar]
- 26.Catani C, Kohiladevy M, Ruf M, Schauer E, Elbert T, Neuner F. . Treating children traumatized by war and Tsunami: a comparison between exposure therapy and meditation-relaxation in North-East Sri Lanka. BMC Psychiatry 2009; 9:22; http://dx.doi.org/ 10.1186/1471-244X-9-22; PMID: 19439099 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Chemtob CM, Nakashima J, Carlson JG. . Brief treatment for elementary school children with disaster-related posttraumatic stress disorder: a field study. J Clin Psychol 2002; 58:99 - 112; http://dx.doi.org/ 10.1002/jclp.1131; PMID: 11748599 [DOI] [PubMed] [Google Scholar]
- 28.Chemtob CM, Nakashima JP, Hamada RS. . Psychosocial intervention for postdisaster trauma symptoms in elementary school children: a controlled community field study. Arch Pediatr Adolesc Med 2002; 156:211 - 6; http://dx.doi.org/ 10.1001/archpedi.156.3.211; PMID: 11876663 [DOI] [PubMed] [Google Scholar]
- 29.Cohen JA, Mannarino AP, Gibson LE, Cozza SJ, Brymer MJ, Murray L. Interventions for children and adolescents following disasters. In: Ritchie EC, Watson PJ, Friedman MJ, eds. Interventions Following Mass Violence and Disasters: Strategies for Mental Health Practice. New York, NY: The Guilford Press, 2006: 227-56. [Google Scholar]
- 30.Fernandez IF. . EMDR as treatment of post-traumatic reactions: A field study on child victims of an earthquake. Educ Child Psychol 2007; 24:65 - 94 [Google Scholar]
- 31.Field T, Seligman S, Scafidi F, Schanberg S. . Alleviating posttraumatic stress in children following hurricane Andrew. J Appl Dev Psychol 1996; 17:37 - 50; http://dx.doi.org/ 10.1016/S0193-3973(96)90004-0 [DOI] [Google Scholar]
- 32.Galante R, Foa D. . An epidemiological study of psychic trauma and treatment effectiveness for children after a natural disaster. J Am Acad Child Psychiatry 1986; 25:357 - 63; http://dx.doi.org/ 10.1016/S0002-7138(09)60257-0 [DOI] [Google Scholar]
- 33.Giannopoulou I, Dikaiakou A, Yule W. . Cognitive-behavioural group intervention for PTSD symptoms in children following the Athens 1999 earthquake: a pilot study. Clin Child Psychol Psychiatry 2006; 11:543 - 53; http://dx.doi.org/ 10.1177/1359104506067876; PMID: 17163223 [DOI] [PubMed] [Google Scholar]
- 34.Goenjian AK, Karayan I, Pynoos RS, Minassian D, Najarian LM, Steinberg AM, Fairbanks LA. . Outcome of psychotherapy among early adolescents after trauma. Am J Psychiatry 1997; 154:536 - 42; PMID: 9090342 [DOI] [PubMed] [Google Scholar]
- 35.Goenjian AK, Walling D, Steinberg AM, Karayan I, Najarian LM, Pynoos R. . A prospective study of posttraumatic stress and depressive reactions among treated and untreated adolescents 5 years after a catastrophic disaster. Am J Psychiatry 2005; 162:2302 - 8; http://dx.doi.org/ 10.1176/appi.ajp.162.12.2302; PMID: 16330594 [DOI] [PubMed] [Google Scholar]
- 36.Goodman RF, Morgan AV, Juriga S, Brown EJ. . Letting the story unfold: a case study of client-centered therapy for childhood traumatic grief. Harv Rev Psychiatry 2004; 12:199 - 212; http://dx.doi.org/ 10.1080/10673220490509534; PMID: 15371062 [DOI] [PubMed] [Google Scholar]
- 37.Hardin SB, Weinrich S, Weinrich M, Garrison C, Addy C, Hardin TL. . Effects of a long-term psychosocial nursing intervention on adolescents exposed to catastrophic stress. Issues Ment Health Nurs 2002; 23:537 - 51; http://dx.doi.org/ 10.1080/01612840290052712; PMID: 12217220 [DOI] [PubMed] [Google Scholar]
- 38.Jaycox LH, Cohen JA, Mannarino AP, Walker DW, Langley AK, Gegenheimer KL, Scott M, Schonlau M. . Children’s mental health care following Hurricane Katrina: a field trial of trauma-focused psychotherapies. J Trauma Stress 2010; 23:223 - 31; PMID: 20419730 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Karairmak O, Aydin G. . Reducing earthquake-related fears in victim and nonvictim children. J Genet Psychol 2008; 169:177 - 85; http://dx.doi.org/ 10.3200/GNTP.169.2.177-186; PMID: 18578300 [DOI] [PubMed] [Google Scholar]
- 40.Lesmana CBJ, Suryani LK, Jensen GD, Tiliopoulos N. . A spiritual-hypnosis assisted treatment of children with PTSD after the 2002 Bali terrorist attack. Am J Clin Hypn 2009; 52:23 - 34; http://dx.doi.org/ 10.1080/00029157.2009.10401689; PMID: 19678557 [DOI] [PubMed] [Google Scholar]
- 41.Mahmoudi-Gharaei J, Mohammadi MR, Yasami MT, Alirezaie N, Naderi F, Moftakhari O. . The effects of a short-term cognitive behavioral group intervention on Bam earthquake related PTSD symptoms in adolescents. Iran J Psychiatry 2009; 4:79 - 84 [Google Scholar]
- 42.Mahmoudi-Gharaei J, Mohammadi MR, Yasami MT, Joshaghani N, Naderi F. . Group cognitive-behavior therapy and supportive art and sport interventions on Bam earthquake related post traumatic stress symptoms in children: A field trial. Iran J Psychiatry 2009; 4:85 - 91 [Google Scholar]
- 43.Plummer CA, Cain DS, Fisher RM, Bankston TQ. . Practice challenges in using psychological first aid in a group format with children: A pilot study. Brief Treat Crisis Interv 2009; 8:313 - 26; http://dx.doi.org/ 10.1093/brief-treatment/mhn019 [DOI] [Google Scholar]
- 44.Ronan KR, Johnston DM. . Behaviourally-based interventions for children following volcanic eruptions: an evaluation of effectiveness. Disaster Prev Manag 1999; 8:169 - 76; http://dx.doi.org/ 10.1108/09653569910275364 [DOI] [Google Scholar]
- 45.Ronan KR, Johnston DM. . Hazards education for youth: a quasi-experimental investigation. Risk Anal 2003; 23:1009 - 20; http://dx.doi.org/ 10.1111/1539-6924.00377; PMID: 12969415 [DOI] [PubMed] [Google Scholar]
- 46.Sahin NH, Yilmaz B, Batigun A. . Psychoeducation for children and adults after the Marmara earthquake: An evaluation study. Traumatology 2011; 17:41 - 9; http://dx.doi.org/ 10.1177/1534765610395624 [DOI] [Google Scholar]
- 47.Salloum A, Overstreet S. . Evaluation of individual and group grief and trauma interventions for children post disaster. J Clin Child Adolesc Psychol 2008; 37:495 - 507; http://dx.doi.org/ 10.1080/15374410802148194; PMID: 18645741 [DOI] [PubMed] [Google Scholar]
- 48.Salloum A, Overstreet S. . Grief and trauma intervention for children after disaster: exploring coping skills versus trauma narration. Behav Res Ther 2012; 50:169 - 79; http://dx.doi.org/ 10.1016/j.brat.2012.01.001; PMID: 22317753 [DOI] [PubMed] [Google Scholar]
- 49.Shen Y-J. . Short-term group play therapy with Chinese earthquake victims: Effects on anxiety, depression, and adjustment. Int J Play Ther 2002; 11:43 - 63; http://dx.doi.org/ 10.1037/h0088856 [DOI] [Google Scholar]
- 50.Shooshtary MH, Panaghi L, Moghadam JA. . Outcome of cognitive behavioral therapy in adolescents after natural disaster. J Adolesc Health 2008; 42:466 - 72; http://dx.doi.org/ 10.1016/j.jadohealth.2007.09.011; PMID: 18407041 [DOI] [PubMed] [Google Scholar]
- 51.Taylor LK, Weems CF. . Cognitive-behavior therapy for disaster-exposed youth with posttraumatic stress: results from a multiple-baseline examination. Behav Ther 2011; 42:349 - 63; http://dx.doi.org/ 10.1016/j.beth.2010.09.001; PMID: 21658519 [DOI] [PubMed] [Google Scholar]
- 52.Vijayakumar L, Kannan GK, Ganesh Kumar B, Devarajan P. . Do all children need intervention after exposure to tsunami?. Int Rev Psychiatry 2006; 18:515 - 22; http://dx.doi.org/ 10.1080/09540260601039876; PMID: 17162691 [DOI] [PubMed] [Google Scholar]
- 53.Vila G, Porche LM, Mouren-Simeoni MC. . An 18-month longitudinal study of posttraumatic disorders in children who were taken hostage in their school. Psychosom Med 1999; 61:746 - 54; PMID: 10593625 [DOI] [PubMed] [Google Scholar]
- 54.Weems CF, Taylor LK, Costa NM, Marks AB, Romano DM, Verrett SL, Brown DM. . Effect of a school-based test anxiety intervention in ethnic minority youth exposed to Hurricane Katrina. J Appl Develop 2009; 30:218 - 26; http://dx.doi.org/ 10.1016/j.appdev.2008.11.005 [DOI] [Google Scholar]
- 55.Wolmer L, Laor N, Dedeoglu C, Siev J, Yazgan Y. . Teacher-mediated intervention after disaster: a controlled three-year follow-up of children’s functioning. J Child Psychol Psychiatry 2005; 46:1161 - 8; http://dx.doi.org/ 10.1111/j.1469-7610.2005.00416.x; PMID: 16238663 [DOI] [PubMed] [Google Scholar]
- 56.Wolmer L, Laor N, Yazgan Y. . School reactivation programs after disaster: could teachers serve as clinical mediators?. Child Adolesc Psychiatr Clin N Am 2003; 12:363 - 81; http://dx.doi.org/ 10.1016/S1056-4993(02)00104-9; PMID: 12725016 [DOI] [PubMed] [Google Scholar]
- 57.Yule W. . Post-traumatic stress disorder in child survivors of shipping disasters: the sinking of the ‘Jupiter’. Psychother Psychosom 1992; 57:200 - 5; http://dx.doi.org/ 10.1159/000288599; PMID: 1410197 [DOI] [PubMed] [Google Scholar]
- 58.Yule W, Udwin O. . Screening child survivors for post-traumatic stress disorders: experiences from the ‘Jupiter’ sinking. Br J Clin Psychol 1991; 30:131 - 8; http://dx.doi.org/ 10.1111/j.2044-8260.1991.tb00928.x; PMID: 2059745 [DOI] [PubMed] [Google Scholar]
- 59.Pfefferbaum B, Sweeton JL, Newman E, Varma V, Noffsinger MA, Shaw JA, Chrisman AK, Nitiéma P. . Child disaster mental health interventions: Part II. Timing, settings and delivery, and approaches. Disaster Health in review [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Arlington, VA: American Psychiatric Publishing, 2013. [Google Scholar]
- 61.La Greca AM, Lai BS, Llabre MM, Silverman WK, Vernberg EM, Prinstein MJ. . Children’s posdisaster trajectories of PTS symptoms: Predicting chronic distress. Child Youth Care Forum 2013; 42:351 - 69; http://dx.doi.org/ 10.1007/s10566-013-9206-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Cohen JA, Bukstein O, Walter H, Benson SR, Chrisman A, Farchione TR, Hamilton J, Keable H, Kinlan J, Schoettle U, et al. , AACAP Work Group On Quality Issues. . Practice parameter for the assessment and treatment of children and adolescents with posttraumatic stress disorder. J Am Acad Child Adolesc Psychiatry 2010; 49:414 - 30; PMID: 20410735 [PubMed] [Google Scholar]
- 63.Foa EB, Keane TM, Friedman MJ. Introduction. In: Foa EB, Keane TM, Friedman MJ, eds. Effective Treatments for PTSD: Practice Guidelines from the International Society for Traumatic Studies. New York, NY: Guilford Press, 2000:1-17. [Google Scholar]
- 64.Foa EB, Davidson JRT, Frances A. . The Expert Consensus Guideline Series: Treatment of posttraumatic stress disorder. J Clin Psychiatry 1999; 60:Suppl 16 3 - 76; PMID: 10463038 [PubMed] [Google Scholar]
- 65.Ursano RJ, Bell C, Eth S, Friedman M, Norwood A, Pfefferbaum B, Pynoos JD, Zatzick DF, Benedek DM, McIntyre JS, et al. , Work Group on ASD and PTSD, Steering Committee on Practice Guidelines. . Practice guideline for the treatment of patients with acute stress disorder and posttraumatic stress disorder. Am J Psychiatry 2004; 161:Suppl 3 - 31; PMID: 15617511 [PubMed] [Google Scholar]
- 66.Nock MK, Janis IB, Wedig MM. Research designs. In: Nezu AM, Maguth-Nazu C, eds. Evidence-based Outcome Research: A Practical Guide to Conducting Randomized Controlled Trials for Psychological Interventions. New York, NY: Oxford University Press, 2008:201-218. [Google Scholar]
- 67.Hetzel-Riggin MD, Brausch AM, Montgomery BS. . A meta-analytic investigation of therapy modality outcomes for sexually abused children and adolescents: an exploratory study. Child Abuse Negl 2007; 31:125 - 41; http://dx.doi.org/ 10.1016/j.chiabu.2006.10.007; PMID: 17306369 [DOI] [PubMed] [Google Scholar]
- 68.Gillies D, Taylor F, Gray C, O’Brien L, D’Abrew N. . Psychological therapies for the treatment of post-traumatic stress disorder in children and adolescents. [review] Cochrane Database Syst Rev 2012; 12:CD006726; PMID: 23235632 [DOI] [PubMed] [Google Scholar]
- 69.McNally RJ, Bryant RA, Ehlers A. . Does early psychological intervention promote recovery from posttraumatic stress?. Psychol Sci Public Interest 2003; 4:45 - 79 [DOI] [PubMed] [Google Scholar]
- 70.Ronan KR, Finnis K, Johnston DM. Interventions with youth and families: A prevention and stepped care model. In: Reyes G, Jacobs GA, eds. Handbook of International Disaster Psychology. Volume 2: Practices and Programs. Westport, CT: Praeger Publishers, 2006:13-35. [Google Scholar]
- 71.Foa EB, Meadows EA. . Psychosocial treatments for posttraumatic stress disorder: a critical review. Annu Rev Psychol 1997; 48:449 - 80; http://dx.doi.org/ 10.1146/annurev.psych.48.1.449; PMID: 9046566 [DOI] [PubMed] [Google Scholar]