Abstract
Objectives
There is growing interest in the application of propensity scores (PS) in epidemiologic studies, especially within the field of reproductive epidemiology. This retrospective cohort study assesses the impact of a short interpregnancy interval (IPI) on preterm birth and compares the results of the conventional logistic regression analysis with analyses utilizing a PS.
Methods
The study included 96,378 singleton infants from Louisiana birth certificate data (1995–2007). Five regression models designed for methods comparison are presented.
Results
Ten percent (10.17%) of all births were preterm; 26.83% of births were from a short IPI. The PS-adjusted model produced a more conservative estimate of the exposure variable compared to the conventional logistic regression method (β-coefficient: 0.21 vs. 0.43), as well as a smaller standard error (0.024 vs. 0.028), odds ratio and 95% confidence intervals c1.15 (1.09, 1.20) vs. 1.23 (1.17, 1.30)]. The inclusion of more covariate and interaction terms in the PS did not change the estimates of the exposure variable.
Conclusions
This analysis indicates that PS-adjusted regression may be appropriate for validation of conventional methods in a large dataset with a fairly common outcome. PS’s may be beneficial in producing more precise estimates, especially for models with many confounders and effect modifiers and where conventional adjustment with logistic regression is unsatisfactory. Short intervals between pregnancies are associated with preterm birth in this population, according to either technique. Birth spacing is an issue that women have some control over. Educational interventions, including birth control, should be applied during prenatal visits and following delivery.
Keywords: birth interval, interpregnancy interval, logistic regression, pregnancy interval, preterm birth, propensity score
The main causes of neonatal death worldwide are infections, preterm birth, and asphyxia. In Louisiana, the prevalence of preterm birth is above the national percentage with 15.4% compared to 12.3% of all births, respectively (1). Interpregnancy interval – the time between the birth of one child and the conception of the next – appears to be one factor associated with preterm birth. Interpregnancy intervals less than 18 months and greater than 59 months are significantly associated with an increased risk of adverse perinatal outcomes (2).
The biological mechanism between short interpregnancy interval and poor maternal and neonatal outcomes is hypothesized to be due to insufficient time for the mother to recover from the nutritional burden and stress of the previous pregnancy (3, 4). Specifically, depleted maternal protein, low energy status, and deficiencies in folate (4, 5) and iron (6) have been considered.
It is important to determine whether short interpregnancy interval is a true independent risk factor for adverse pregnancy outcomes in Louisiana because it is an issue that women have some control over. Additionally, it is feasible that educational interventions during prenatal visits and following delivery could be applied. The difficulty in assessing the independence of the risk from interpregnancy interval is the numerous potential confounders such as behavioral risk factors, stress, and socioeconomic disadvantage that must be considered in the analysis. The use of propensity scores in the analysis may remedy this situation. This topic serves as an example for the application of propensity scores in multivariable logistic regression in a large, vital records dataset.
Regression with propensity scores may be suitable for the field of reproductive epidemiology and specifically this topic, due to the myriad confounders that are usually included during modeling. A very complicated propensity score model with many covariates, interactions, and higher order terms can be fit. The goal is to obtain the best estimated probability of exposure assignment. Over-parameterizing the model is not as much of a concern like it is with a traditional regression analysis. The propensity score for an individual is the probability of being treated (exposed) conditional on the individual’s covariate values and it can be used to balance the covariates in the two exposure groups making them more comparable (7).
Regression analysis using propensity scores has been used to check or validate the results from more traditional methods (8–10). This can lead to stronger conclusions and assertions of causal effect. Additionally, propensity scores are valuable in situations where conventional multivariable methods may not be appropriate due to few events and many confounders. Additional covariates may produce instability in the model, which can lead to decreased precision and misleading results (11). Another drawback to conventional multivariable regression analysis is that adjusting for covariates that are unevenly distributed between exposure groups may not balance the groups, resulting in residual confounding and poor validity (12). Propensity scores work best in large data sets because there is a greater chance of achieving a balance of covariates between the exposure groups (13). However, propensity scores have yet to be assessed when the outcome is common (14).
The objectives of this analysis are: (1) to assess the relationship between short interpregnancy interval and preterm birth in Louisiana and (2) to compare the results of the conventional analysis with those results from an analysis that utilizes propensity scores as a covariate in regression adjustment in order to determine the advantages and disadvantages of the propensity score approach. To achieve these goals, traditional logistic regression is performed as well as two propensity score models: one with only the covariates used in the traditional logistic regression and the second with additional potential confounders and effect modifiers. The specific aims are to determine if propensity scores would be beneficial in producing more precise estimates for the association between interpregnancy interval and preterm birth and also to assess the method’s ability to validate the results of the traditional multivariable regression analysis in a large vital records study population.
MATERIALS AND METHODS
Dataset
We conducted a retrospective cohort study using data from the State of Louisiana birth certificate registry which included 861,676 live infants born from 1995 to 2007. Only women who had a singleton birth and had a single previous pregnancy that ended in a live birth or fetal death (at least 20 weeks gestation or birthweight of at least 350 grams) were included in the study. After the exclusion, the final study population included 96,378 singleton infants for assessing the association between interpregnancy interval and preterm birth. Permission to use this dataset was granted by the State of Louisiana Vital Records. The research was conducted in accord with ethical principles and approved by the Tulane Institutional Review Board.
Definitions
Pre-term birth was defined as a gestational age less than 37 completed weeks. The interpregnancy interval between the two pregnancies was estimated as the difference between the date of delivery of the first pregnancy and the date of conception of the second pregnancy. The date of conception was estimated by subtracting the gestational age in weeks from the date of the birth. The use of propensity scores necessitated a binary exposure variable. Therefore, the observations were limited to an interpregnancy interval of 24 months or less because previous literature (2, 15) found that a long interval is also associated with preterm birth/low birth weight. Exposure was defined as less than nine months (<36 weeks) between pregnancies and unexposed pregnancies included those with an interval of nine to 24 months (36–96 weeks). A cut point of nine months was chosen because it is the median of the interval found to be significant in a prior study (2). Data entry errors in the database resulted in interval values that were negative, zero, and very short (i.e. within days and weeks of the first birth). Since it was impossible to determine what values were accurate, the short interpregnancy interval (exposure) was limited to a minimum of 4 weeks based on a study of natural interpregnancy intervals (16).
Maternal age was defined as completed years at time of delivery. Marital status was dichotomized as legally married and unmarried. Mother’s education was categorized into none or elementary (0–8 years), secondary (9–12 years), and university or more (≥13 years). Mother’s race was categorized as white, black, and other. The number of prenatal visits was dichotomized as less than or equal to three and greater than three visits, instead of the more traditional seven prenatal visit’s cutoff. Since the outcome is prematurity, the cutoff of three visits was deemed more appropriate to accommodate a shorter gestation. The month that the mother began prenatal care (PNC) was categorized into no PNC, early PNC (1–3 months), delayed PNC (4–6 months), and late PNC (7–9 months). The number of terminations the mother reported was dichotomized as none and one or more. Maternal medical risk factors include conditions such as anemia, cardiac and lung conditions, diabetes, herpes, hydramnios, hemoglobinopathy, eclampsia, and uterine bleeding. They were combined into a composite dichotomous variable of maternal health: absent or present. Tobacco and alcohol use were both categorized as user and non-user.
Low-birth weight was dichotomized as less than 2,500 grams or 2,500 or more grams at birth. Previous fetal death and previous c-section variables were defined as the previous birth ended in fetal death and the previous birth was delivered via cesarean section, respectively.
Analysis
Descriptive analysis
Univariate and bivariate analysis were performed on all possible predictors and confounding variables. Relationships between the covariates and interpregnancy interval (<9 months from birth to next pregnancy versus ≥9 months from birth to next pregnancy) and preterm birth (<37 weeks gestation versus ≥37 weeks gestation) were assessed using chi-square and t-test, as indicated.
Conventional logistic regression approach
Unadjusted logistic regression was used to produce the association between interpregnancy interval and preterm birth (Model 1). In this analysis, we define conventional multivariable logistic regression as multivariable logistic regression without the use of a propensity score. Stepwise variable selection was utilized to find variables that were associated with the outcome (P < 0.0001). These statistics and a priori knowledge of reproductive epidemiology were used to produce the final Model 2. The model included 11 variables. A third logistic regression model (Model 5) included 13 variables and their 78 first-order interaction terms – similar to Model 4. The model was over-parameterized to show the advantages of propensity score regression in extreme situations.
Propensity score approach
The propensity scores were calculated by finding the probability of a short interpregnancy interval. Multivariable logistic regression modeled the dichotomous outcome of short interpregnancy interval (<9 months) versus longer interpregnancy interval (9–23 months). All confounding variables that were included in the conventional logistic regression were included in the first propensity score model (Model 3). Using the results of the bivariate analysis, care was taken to exclude variables that were related to the exposure but not to the outcome in order to avoid a decrease in precision (17). A second model (Model 4) was generated that included any confounding or interaction terms that contributed to the model. Model 4 included the exposure variable and propensity score which consisted of 13 variables and 78 first-order interaction terms. At no time during the propensity score calculations was the outcome variable, preterm birth, included. The distribution of propensity scores were plotted and assessed for adequate overlap, which signifies comparability between the exposure levels.
The propensity scores were included as an additional covariate with the treatment variable (interpregnancy interval) in the two multivariable logistic regression models. The first model (Model 3) includes the same covariates in the propensity score as are in the conventional logistic regression and is a means of checking or validating the results of the conventional methods. Model 4 seeks to determine if the additional covariates and interaction terms allow for a more stable and precise estimate of the treatment effect. All analyses were completed with the SAS 9.2 program package (SAS Institute Inc. Cary, North Carolina).
RESULTS
Among the study population of 96,378 singleton infants, ten percent (10.17%) of all the births were preterm; 26.83% of births were considered a short interpregnancy interval. The majority of mothers were white (59.46%), married (56.81%), and had at least some secondary school education (9th–12th grade; 57.41%). Mothers of preterm infants and infants from a short interpregnancy interval tended to be younger (22.6 vs. 24.2 and 22.6 vs. 24.6, respectively; P < 0.0001). Each covariate’s relationship with a short interpregnancy interval and preterm birth can be found in Table 1.
Table 1.
Frequencies and descriptives of covariates by interpregnancy interval: <9 months from birth to next pregnancy versus ≥9 months from birth to next pregnancy and preterm birth: <37 weeks gestation versus ≥37 weeks gestation (N=96,378).
| Variable |
Exposed < 9 months n(%) |
Unexposed > 9 months n(%) |
P- value* |
Preterm Birth n(%) |
Term Birth n(%) |
P- value* |
Missing (n) |
|
| Race | ||||||||
| White | 13378 (51.73) | 43924 (62.29) | <0.0001 | 4256 (43.42) | 53046 (43.42) | <0.0001 | 0 | |
| Black | 11750 (45.43) | 24755 (35.11) | 5357 (54.65) | 31148 (35.98) | ||||
| Other | 735 (2.84) | 1836 (2.60) | 189 (1.93) | 2382 (2.75) | ||||
| Alcohol Use | ||||||||
| Yes | 88 (0.34) | 233 (0.33) | 0.81 | 40 (0.41) | 281 (0.33) | 0.17 | 169 | |
| No | 25729 (99.66) | 70159 (99.67) | 9745 (99.59) | 86143 (99.67) | ||||
| Tobacco Use | ||||||||
| Yes | 2946 (11.41) | 6583 (9.35) | <0.0001 | 1118 (11.42) | 8411 (9.73) | <0.0001 | 119 | |
| No | 22876 (88.59) | 63854 (90.65) | 8669 (88.58) | 78061 (90.27) | ||||
| # of Prenatal Visits | ||||||||
| 0–3 | 1789 (6.95) | 2323 (3.31) | <0.0001 | 1280 (13.14) | 2832 (3.28) | <0.0001 | 345 | |
| ≥4 | 23965 (93.05) | 67956 (96.69) | 8461 (86.86) | 83460 (96.72) | ||||
| Timing of First Prenatal Visit | ||||||||
| No PNC | 775 (3.01) | 833 (1.18) | <0.001 | 539 (5.53) | 1069 (1.24) | <0.0001 | 311 | |
| Early (1–3) | 18150 (70.45) | 57948 (82.43) | 6919 (70.99) | 69179 (80.14) | ||||
| Delayed (4–6) | 5590 (21.70) | 9697 (13.79) | 1880 (19.29) | 13407 (15.53) | ||||
| Late (7–9) | 1249 (4.85) | 1825 (2.60) | 408 (4.19) | 2666 (3.09) | ||||
| Low-birth weight | ||||||||
| Yes | 2516 (9.73) | 4630 (6.57) | <0.0001 | 4918 (50.18) | 2228 (2.57) | <0.0001 | 8 | |
| No | 23343 (90.27) | 65881 (93.43) | 4883 (49.82) | 84341 (97.43) | ||||
| Marital Status | ||||||||
| Married | 12001 (46.41) | 42750 (60.63) | <0.0001 | 3979 (40.60) | 50772 (58.65) | <0.0001 | 7 | |
| Unmarried | 13860 (53.59) | 27760 (39.37) | 5822 (59.40) | 35798 (41.35) | ||||
| Maternal Education | ||||||||
| 0 or Primary | 1268 (4.90) | 2393 (3.39) | <0.0001 | 476 (4.86) | 3185 (3.68) | <0.0001 | 37 | |
| Secondary | 16991 (65.72) | 38319 (54.36) | 6658 (67.95) | 48652 (56.22) | ||||
| University + | 7594 (29.37) | 29776 (42.24) | 2664 (27.19) | 34706 (40.10) | ||||
| Terminations | ||||||||
| 0 | 22101 (85.47) | 58262 (82.63) | <0.0001 | 8077 (82.42) | 72286 (83.50) | 0.0062 | 11 | |
| ≥1 | 3758 (14.53) | 12246 (17.37) | 1723 (17.58) | 14281 (16.50) | ||||
| Previous fetal death | ||||||||
| Yes | 585 (2.26) | 659 (0.93) | <0.0001 | 294 (3.00) | 950 (1.10) | <0.0001 | 0 | |
| No | 25278 (97.74) | 69856 (99.07) | 9508 (97.00) | 85626 (98.90) | ||||
| Maternal medical risk factors | ||||||||
| Absent | 20148 (77.94) | 55709 (79.03) | 0.0003 | 6414 (65.48) | 69443 (80.24) | <0.0001 | 36 | |
| Present | 5701 (22.06) | 14784 (20.97) | 3382 (34.52) | 17103 (19.76) | ||||
| Previous c-section | ||||||||
| Yes | 5464 (21.15) | 16037 (22.76) | <0.0001 | 1823 (18.61) | 19678 (22.75) | <0.0001 | 95 | |
| No | 20370 (78.85) | 54412 (77.24) | 7972 (81.39) | 66810 (77.25) | ||||
| Preterm | ||||||||
| Yes | 3419 (13.22) | 6383 (9.05) | <0.0001 | - | - | - | 0 | |
| No | 22444 (86.78) | 64132 (90.95) | - | - | ||||
| Variable |
Treatment < 9 months mean (SD) |
Control > 9 months mean (SD) |
P- value‡ |
Preterm Birth mean (SD) |
Term Birth mean (SD) |
P- value‡ |
Missing (n) |
|
| Maternal Age (years) | ||||||||
| 22.61 (4.84) | 24.58 (5.28) | <0.0001 | 22.62 (4.97) | 24.22 (5.24) | <0.0001 | 0 | ||
Chi-square Test, unless otherwise stated
Two-sample t-test
The results of the simple regression (univariate) analysis reported in Table 1 show the P-values unadjusted for propensity score. This provided convincing evidence that the covariate distributions were different between the exposure groups for the majority of variables. After adjusting for propensity scores (PS Adjusted P-value, PS Adjusted OR) in a selection of confounders, there was considerably less difference in the covariate patterns between exposure groups (Table 2). Certain covariates such as previous fetal death and maternal age (and even maternal race to an extent) remained significant (at the traditional P<0.05 significance level) even after adjustment by propensity score. The very large sample size highlights even extremely small and insignificant differences. A look at the propensity score adjusted odds ratios confirms how unremarkable this difference is between the exposure groups.
Table 2.
Simple regression analysis for the association between interpregnancy interval and selected confounding variables, both unadjusted and adjusted for propensity score (N=96,378).
| Variables | Unadjusted OR (95% CI) |
Unadjusted P- value |
PS Adjusted OR (95% CI)* |
PS Adjusted P- value |
|---|---|---|---|---|
| Maternal Race | ||||
| Black vs. white | 1.56 (1.51, 1.61) | <0.001 | 0.97 (0.94, 1.00) | 0.08 |
| Other vs. white | 1.32 (1.21, 1.44) | <0.001 | 1.10 (1.00, 1.20) | 0.04 |
| Low-Birth Weight | 1.53 (1.46, 1.61) | <0.001 | 0.96 (0.91, 1.02) | 0.19 |
| Previous Fetal Death | 2.43 (2.18, 2.73) | <0.001 | 0.87 (0.77, 0.98) | 0.02 |
| Previous C-section | 0.91 (0.88, 0.94) | <0.001 | 1.00 (0.97, 1.04) | 0.84 |
| Maternal Age | 0.92 (0.92, 0.93) | <0.001 | 0.99 (0.98, 0.99) | <0.001 |
Adjusted P-values and odds ratios were calculated with the propensity score included in the regression analysis modeling the association between the confounding variable and interpregnancy interval.
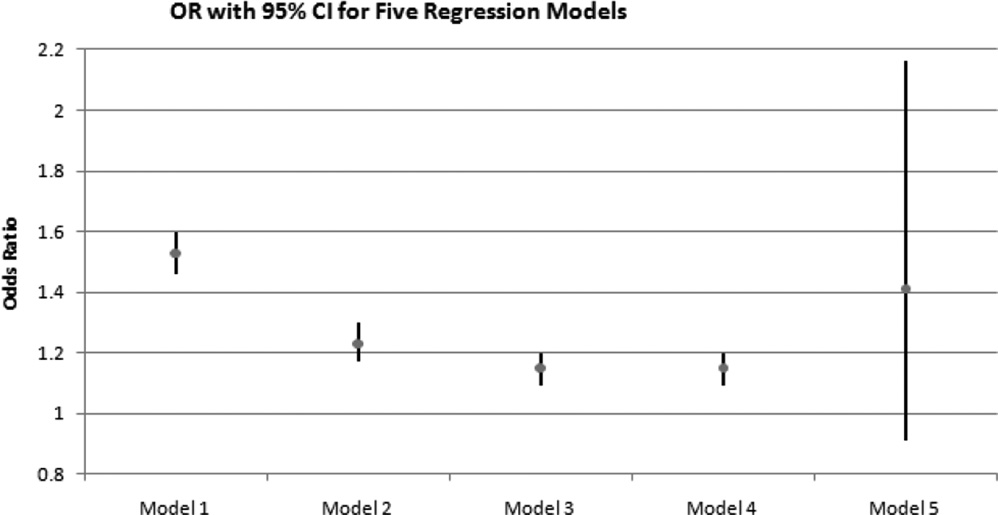
Table 3 displays the analysis results from the five logistic regression models (3 conventional, 2 propensity score adjusted). Model 2 and Model 3 are both an improvement in fit over the unadjusted logistic regression model (Model 1), as the likelihood ratio (LR) P-values are highly significant. The propensity score adjusted Model 3 produced a more conservative estimate of the exposure variable (interpregnancy interval), as well as a smaller standard error and slightly narrower confidence intervals (95% CI). Interestingly, Model 4, which included more covariate and interaction terms, did not change the estimates of the exposure variable or its associated odds ratio. However, when the same covariates and interaction terms that were used in Model 4 were included in the conventional logistic regression, the estimates became non-significant and included large standard errors and confidence intervals, a reminder of how sensitive conventional regression is to over-parameterization of the model. A graphical display of Table 3 can be found in the Figure where the association between interpregnancy interval and preterm birth according to the five models is presented.
Table 3.
Model fit statistics, main effect coefficient estimates with standard error and P-value, and the main effect odds ratio estimates with confidence intervals for the five models.
| Model | −2 log La | LRb P-value | Estimate for Main Effect (SE) |
P-value | Odds ratio for Main Effect (95% CI) |
|---|---|---|---|---|---|
| 1 | 63037.39 | <0.001c | 0.43 (0.023) | <0.001 | 1.53 (1.46, 1.60) |
| 2 | 45109.73 | <0.001d | 0.21 (0.028) | <0.001 | 1.23 (1.17, 1.30) |
| 3 | 58579.60 | <0.001d | 0.14 (0.024) | <0.001 | 1.15 (1.09, 1.20) |
| 4 | 59301.05 | <0.001d | 0.14 (0.024) | <0.001 | 1.15 (1.09, 1.20) |
| 5 | 44649.96 | <0.001e | 0.34 (0.222) | 0.13 | 1.41 (0.91, 2.16) |
Model 1 = Exposure only (unadjusted)
Model 2 = Exposure without propensity score (conventional multivariable logistic regression)
Model 3 = Exposure AND propensity score variable (same covariates as Model 2 are used in propensity score)
Model 4 = Exposure AND propensity score variable (same covariates as Model 3, plus additional covariates and interaction terms are used in propensity score)
Model 5 = Exposure without propensity score (same covariates and interaction terms as Model 4 used in conventional logistic regression)
−2logL, −2 log likelihood
LR, likelihood ratio
Model 1 compared to Null Model (Not shown)
Model compared to Model 1
Model 5 compared to Model 2
Figure.
The association (odds ratio (OR)) between birth spacing and preterm birth by unadjusted conventional logistic regression (Model 1), conventional multivariable (adjusted) logistic regression (Model 2), propensity score regression with the same covariates (Model 3), propensity score regression with additional covariates and interaction terms (Model 4), and conventional logistic regression with additional covariates and interaction terms (Model 5) (N=96,378).
DISCUSSION
The main goal of this paper was to investigate the impact of a short interpregnancy interval on preterm birth. In this analysis, the method of propensity score adjusted regression analysis was utilized to estimate the treatment effect of birth spacing on an important birth outcome in the presence of non-random assignment. To our knowledge, no such analysis has been conducted in the Louisiana population prior to this study. Our results strengthen the evidence that short intervals between pregnancies have a significant impact on the health of infants at birth in Louisiana. The data from a 1995–2007 birth cohort showed that births from pregnancies with a short interpregnancy interval are at a 15% increased risk of being preterm [OR = 1.15; 95%CI: (1.09, 1.20)]. This finding adds to the mounting evidence that better neonatal outcomes occur when the mother does not conceive within nine months of a previous birth (2, 3, 5, 15). Public health programs and post-natal hospital visits in Louisiana, and elsewhere, should incorporate this finding into their maternal and child health care.
This topic also served as a platform for comparing propensity score regression analysis to conventional regression methods. The inclusion of more covariate and interaction terms in the propensity score model did not change the estimates or variance of the exposure variable, nor the odds ratio estimate (Model 4). Propensity scores are beneficial in producing robust, less biased and more precise estimates, especially for models with many predictors and effect modifiers (18). This method is also a good alternative to control for imbalances when conventional multivariable adjustment with logistic regression is not possible due to too few events per confounder (19). In some fields of study, such as reproductive epidemiology, there are many potential confounders that researchers are interested in adjusting for in the model.
Our comparison of Model 3 to Model 4 supports the claim that over-parameterized propensity score models are much less harmful than a conventional model with too many covariates (Model 5). Another study on the effects of misspecification of propensity score models compared to conventional response models similarly found that the propensity score is preferable to conventional because it has smaller biases that will be less likely to affect the estimates when mis-specified (20). However, as in traditional analyses, propensity scores must include all important confounders; they offer no advantage over conventional analyses when confounders are omitted (20) or only a subset of the most important prognostic variables are included (18).
Another aim of this study was to show that propensity scores can be effectively used to validate conventional methods in order to make more confident conclusions. Our results indicate that the propensity score adjusted model produces a more conservative estimate of the exposure variable compared to the conventional logistic regression method (β-coefficient: 0.21 vs. 0.43) and a smaller standard error (0.024 vs. 0.028). Similarly, the odds ratio showed a slightly weaker association in the propensity score models and narrower confidence intervals [95% CI: 1.15 (1.09, 1.20) vs. 1.23 (1.17, 1.30)]. The similarity between effect estimates inspires confidence that a true association was found between short interpregnancy interval and preterm birth. A systematic review of propensity score methods also found that it gave similar results to traditional regression modeling (21). Other literature has suggested that joint consideration of propensity score matching and multivariable analysis can be used to assess the robustness of estimates (22) and is a useful tool in exploring causal effect (23). This present analysis endorses propensity score-adjusted regression as an appropriate technique for the validation of conventional methods in a large dataset with a fairly common outcome (10.17%).
The majority of the variables should be very reliable; however, maternal medical risk factor data from the birth certificate data may be less so. This is a common limitation with birth certificate data (24). There was evidence of some data entry error for the date of previous birth which resulted in interpregnancy intervals with negative, zero and very small values. It was impossible to determine where the accurate data began, therefore, a cutoff of 4 weeks was chosen based on previous literature (16). This most likely did not affect the estimates, as they comprised very few observations out of nearly 100,000. The most significant limitation may be that reverse causation is possible: high risk women (for preterm birth) may be over-represented in the exposed group, which could inflate the estimate. However, previous fetal death information was included as a variable, so some of this risk may be adjusted for.
In conclusion, the large birth certificate database confirmed that a short interpregnancy is associated with an increased risk of preterm birth in Louisiana. This analysis found that the model using propensity score regression was similar, although slightly more conservative, than traditional models. For models with many covariates, traditional logistic regression is not satisfactory; a propensity score regression model will provide more accurate and precise estimates and standard errors. When feasible, the application of a combination of methods, including propensity scores, can be utilized to better understand the data, assess the robustness of the estimates and validate more traditional methods of analysis. Propensity score adjusted regression analysis is under-utilized in reproductive epidemiology. This analysis supports their use in similar study settings: studies with large datasets, relatively common outcomes of interest, and many covariate terms.
Acknowledgments
This work was supported by the Eunice Kennedy Shriver National Institute of Child Health And Human Development (T32HD057780). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Footnotes
Disclosure: All listed authors report no conflict of interests
REFERENCES
- 1.The Henry J. Kaiser Family Foundation. [Accessed: 10 April 2011];2008 < Statehealthfacts.org>. [Google Scholar]
- 2.Conde-Agudelo A, Rosas-Bermudez A, Kafury-Goeta AC. Birth spacing and risk of adverse perinatal outcomes: a meta-analysis. JAMA. 2006;295(15):1809. doi: 10.1001/jama.295.15.1809. [DOI] [PubMed] [Google Scholar]
- 3.Miller JE. Birth intervals and perinatal health: an investigation of three hypotheses. Fam Plann Perspect. 1991;23:62. [PubMed] [Google Scholar]
- 4.Winkvist A, Rasmussen KM, Habicht JP. A new definition of maternal depletion syndrome. Am J Public Health. 1992;82:691. doi: 10.2105/ajph.82.5.691. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Smits LJ, Essed GG. Short interpregnancy intervals and unfavorable pregnancy outcome: role of folate depletion. Lancet. 2001;358:2074. doi: 10.1016/S0140-6736(01)07105-7. [DOI] [PubMed] [Google Scholar]
- 6.Scholl TO, Reilly T. Anemia, iron, and pregnancy outcome. J Nutr. 2000;130:443S–447S. doi: 10.1093/jn/130.2.443S. [DOI] [PubMed] [Google Scholar]
- 7.Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects. Biometrika. 1983;70:41–55. [Google Scholar]
- 8.Grzybowski M, Clements EA, Parsons L, et al. Mortality benefit of immediate revasularization of acute ST-segment elevation myocardial infarction in patients with contraindications to thrombolytic therapy – a propensity analysis. JAMA. 2003;290:1891–1898. doi: 10.1001/jama.290.14.1891. [DOI] [PubMed] [Google Scholar]
- 9.Mehta RL, Pascual MT, Soroko S, et al. Diuretics, mortality, and nonrecovery of renal function in acute renal failure. JAMA. 2002;288:2547–2553. doi: 10.1001/jama.288.20.2547. [DOI] [PubMed] [Google Scholar]
- 10.Ioannidis JA, Galanos O, Katritsis D, et al. Early mortality and morbidity of bilateral versus single internal thoracic artery revascularization: propensity and risk modeling. J Am Coll Cardiol. 2001;37:521–528. doi: 10.1016/s0735-1097(00)01112-8. [DOI] [PubMed] [Google Scholar]
- 11.Newgard CD, Hedges JR, Arthur M, et al. Advanced Statistics: The propensity score – A method for estimating treatment effect in observational research. Acad Emerg Med. 2004;11(9):953–960. doi: 10.1197/j.aem.2004.02.530. [DOI] [PubMed] [Google Scholar]
- 12.Sturmer T, Joshi M, Glynn RJ, et al. A review of the application of propensity score methods yielded increasing use, advantages in specific settings, but not substantially different estimates compared with conventional multivariable methods. J of Clin Epidemiol. 2006;59:437–447. doi: 10.1016/j.jclinepi.2005.07.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Little RJ, Rubin DB. Causal effects in clinical and epidemiological studies via potential outcomes: concepts and analytical approaches. Annu Rev Public Health. 2000;21:121–145. doi: 10.1146/annurev.publhealth.21.1.121. [DOI] [PubMed] [Google Scholar]
- 14.Rubin DB. Estimating causal effects from large data sets using propensity scores. Ann Inter Med. 1997;127:757–763. doi: 10.7326/0003-4819-127-8_part_2-199710151-00064. [DOI] [PubMed] [Google Scholar]
- 15.Zhu BP, Rolfs RT, Nangle BE, et al. Effect of the interval between pregnancies on perinatal outcomes. N Engl J Med. 1999;340:589. doi: 10.1056/NEJM199902253400801. [DOI] [PubMed] [Google Scholar]
- 16.Juntunen K, Kirkinen P, Kauppila A. Natural interpregnancy intervals of fertile couples: a longitudinal survey of grand grand multiparous women. Fertil Steril. 1994;62:722. doi: 10.1016/s0015-0282(16)56995-7. [DOI] [PubMed] [Google Scholar]
- 17.Brookhart MA, Schneeweiss S, Rothman KJ, et al. Variable selection for propensity score models. Am J Epidemiol. 2006;163(12):1149–1156. doi: 10.1093/aje/kwj149. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Rubin DB, Thomas N. Combining propensity score matching with additional adjustments for prognostic covariates. J Am Stat Assoc. 2000;95(450):573–585. [Google Scholar]
- 19.Cepeda MS, Boston R, Farrar JT, et al. Comparison of logistic regression versus propensity score when the number of events is low and there are multiple confounders. Am J Epidemiol. 2003;158(3):280–287. doi: 10.1093/aje/kwg115. [DOI] [PubMed] [Google Scholar]
- 20.Drake C. Effects of misspecification of the propensity score on estimators of treatment effect. Biometrics. 1993;49:1231–1236. [Google Scholar]
- 21.Shah BR, Laupacis A, Hux JE, et al. Propensity score methods gave similar results to traditional regression modeling in observational studies: a systematic review. J Clin Epidemiol. 2005;58(6):550–559. doi: 10.1016/j.jclinepi.2004.10.016. [DOI] [PubMed] [Google Scholar]
- 22.Baser O. Too much ado about propensity score models? Comparing methods of propensity score matching. Value Health. 2006;9(6):377–385. doi: 10.1111/j.1524-4733.2006.00130.x. [DOI] [PubMed] [Google Scholar]
- 23.Juhn YJ, Qin R, Urm S, et al. The influence of neighborhood environment on the incidence of childhood asthma: A propensity score approach. J Allergy Clin Immunol. 2009;125(4):838–843. doi: 10.1016/j.jaci.2009.12.998. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Vinikoor LC, Messer LC, Laraia BA, et al. Reliability of variables on the North Carolina birth certificate: a comparison with directly queried values from a cohort study. Paediatric and Perinatal Epidemiology. 2010;24:102–112. doi: 10.1111/j.1365-3016.2009.01087.x. [DOI] [PMC free article] [PubMed] [Google Scholar]