Abstract
Patient engagement has been identified as a key strategy for improving patient outcomes. In this paper, we describe the development and pilot testing of a web-based patient centered toolkit (PCTK) prototype to improve access to health information and to engage hospitalized patients and caregivers in the plan of care. Individual and group interviews were used to identify plan of care functional and workflow requirements and user interface design enhancements. Qualitative methods within a participatory design approach supported the development of a PCTK prototype that will be implemented on intensive care and oncology units to engage patients and professional care team members developing their plan of care during an acute hospitalization.
Keywords: participatory design, plan of care, communication, health information technology, patient engagement, nursing informatics
Background and Significance
Acute care hospitals have been long recognized as complex, dynamic, and fast-paced environments characterized by suboptimal communication.[1, 2] Providing tools to support communication, patient activation and engagement can improve patient outcomes and lower healthcare costs.[3] Engaging patients in their recovery plan and providing them with information they need to be informed participants in that plan are key strategies for adverse event and error prevention.[4] The Meaningful Use legislation includes incentives for providing patients with timely information including the use of secure electronic messaging for providers to communicate with patients about their health status.[5] However, there is limited literature describing tools to activate patients and engage them in their plan of care during an acute hospitalization.
In our previous work we found that by providing all care team members including patients and family with information about a patient’s risk for falls and a personalized prevention plan, the rate of patient falls was reduced by 22%.[6] Our team has also found that effective patient education can reduce the incidence of preventable adverse drug events.[7] Others have found that interactive educational tools can improve patient adherence with their treatment plan and improve patient outcomes.[8] Based on these findings, in prior work our team conducted focus groups and interviews with patients, family caregivers, and professional providers to identify the core set of information needed to engage in their recovery during an acute hospitalization[9] and determined the following core information requirements: 1) plan of care, 2) tailored patient education, 3) communication of safety alerts, 4) diet restrictions and 5) medications. We built an electronic Bedside Communication Center (eBCC) prototype to activate patients and to bridge the communication gap between the healthcare team and patients during an acute care hospitalization. We then conducted initial usability testing with hospitalized patients on medical units and found that overall patients and family found the eBCC both useful and easy to use.[10] However, they identified some gaps in the functionality including the ability to message their care team and the ability to directly participate in developing the plan of care. The purpose of this paper is to describe the participatory design process that our team is using to engage patients, family, and health care professional stakeholders in the development of a patient-centered toolkit (PCTK) that will be implemented on intensive care and oncology units to engage patients and family in their plan of care during an acute hospitalization. The research questions are:
What are the workflow requirements needed to support patient involvement in developing the plan of care and direct communication with providers?
What are the content/user interface requirements needed to support patient involvement in developing the plan of care and direct communication with providers?
AHRQ Conceptual Framework of Patient and Family Engagement
This project is informed by the AHRQ conceptual framework of Patient and Family Engagement[11] that defines the organizational and individual characteristics and behaviors that are antecedents to patient engagement. The framework identifies anticipated outcomes of patient engagement needed to ultimately achieve the triple aim of improving the patient experience, improving the health of populations, and reducing the cost of healthcare.[12]
According to this framework, the PCTK intervention will be effective if it facilitates patient, family, and health care professional engagement in the specific behaviors needed to support safety and quality. Therefore the PCTK should focus on organizational and individual behaviors (patient, family and health care professional) that are acceptable to each stakeholder and that are feasible within the hospital setting. Engagement with stakeholders is needed to identify the specific behaviors that are acceptable and feasible and to develop a PCTK that can be used by all stakeholders in the context of acute care workflows.
Research Methods
Our specific aim was to identify the workflow and user interface requirements needed to support patient involvement in developing the plan of care and communicating with providers related to that plan during an acute hospitalization. We used an iterative participatory design approach to develop the plan of care and provider communication features of the PCTK. The study was reviewed and approved by the Partners HealthCare Human Research Committee and was conducted at Brigham and Women’s Hospital (BWH), an academic medical center in the Northeastern United States. We used a combination of individual interviews and group interviews to engage patients, family, and professional health care team members in development and refinement of a series of prototypes. Participants included former patients and their family members, and nurse and physician providers who cared for patients on the intensive care and oncology units at BWH. Interviews were conducted at the bedside with hospitalized inpatients and family members. Group interviews were conducted with discharged patients and family and with professional care team members in conference rooms at BWH. Inclusion criteria for patients included current or past inpatient admission (patient or family member) in an intensive care or oncology unit or a professional care team member working on those units, over 18 years of age, awake and alert, able to understand and speak English, able to provide feedback on their experience and on the PCTK prototype.
Iterative Participatory Software Development
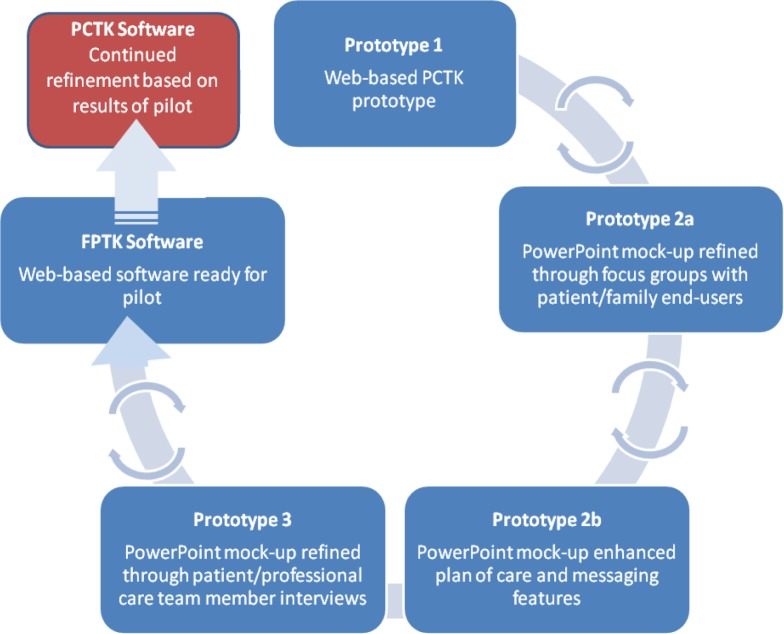
We started with a PCTK prototype that we developed previously for patients hospitalized with an acute medical condition.[9, 10] An iterative participatory software development process (see Figure 1) was used to engage stakeholders in developing a series of prototypes; each incorporating what we learned related to the user’s (patient/family and professional care team member) role and behaviors in plan of care workflow and associated communication. Through this process we aimed to identify workflow and system usability constraints that were then addressed in subsequent prototypes to produce a PCTK that would enable patients, family, and professional care team members to collaborate and communicate in regards to the plan of care.[13, 14]
Figure 1:
AHRQ Conceptual Framework of Patient and Family Engagement
The types of interviews conducted to engage end users in development and refinement of the PCTK are as follows:
Bedside interviews with patients and family (Round 1): We started with the prototype developed in our previous research (Prototype 1 see Figure 2).[9, 10] Prototype 1 was accessed via the internet on a secure mobile tablet and tested for usability at the bedside with hospitalized medical patients and family members.
Patient/Family Advisory Council group interview: Group interview with former oncology and intensive care patients and their family members using PowerPoint mock-ups (Prototypes 2a, 2b) followed by individual interviews to verify requirements and user interface enhancements.
Professional care team group interviews: Series of interviews conducted over 6 months with professional care team members to identify existing workflows and opportunities for integrating the toolkit into workflow and to identify opportunities for secondary use of data to populate the PCTK. PowerPoint mock-ups (Prototypes 2a, 2b) and the web-based software (Prototype 3) were informed by these interviews.
Bedside interviews with patients/family (Round 2): Individual interviews were conducted on oncology units using an interview guide and Prototype 3 to identify patient/family preferences related to participation in development of the plan of care and to vet the features and workflows defined by professional providers. Prototype 3 was accessed via the internet on a secure mobile tablet.
Meetings with clinical and administrative leaders and stakeholders: In addition to engaging, patients, family, and professional providers, we met with clinical and administrative leaders and stakeholders to ensure that our project fit in with the BWH organizational informatics strategy.
Figure 2:

PCTK Prototype 1
Interview guides were used to structure each group and individual interview to ensure that outstanding questions related to plan of care workflows, communication and the user interface were addressed. Investigators took detailed notes during the interviews and debriefed at weekly research team meetings where notes were reviewed, emergent themes identified, and requirements refined. Changes were incorporated into PowerPoint mock-ups and iteratively revised by the research team. Mock-ups were then shared with interview participants to validate new requirements and to vet the refinements made to the user interface.
Results
Bedside interviews with patients and family (Round 1): Eight patients and three family members participated in the first round of bedside interviews. Sessions were conducted on general medical units. While detailed results have been reported elsewhere[10], two related findings were that patients and family requested additional functionality to support their participation in the patient plan of care and for communicating directly with providers on issues related to their plan.
Patient/Family Advisory Council group interview: Discharged patients and family members participated in a group interview and follow-up individual interviews. A total of 12 patients/family members participated in the group interview. Individual follow-up was completed with one patient and one family caregiver to further explore and validate the themes identified in the group interview. While the majority of participants said that they liked the idea of providing patients and family access to information to help them participate in their POC, many said that the user interface was too busy and could be confusing for patients who are not technically savvy.
Professional care team group interviews: A total of 18 Nurses and 10 physicians participated in a series of group interviews. Overall participants said that they thought that the PCTK would be useful for some patients but they were concerned that the user interface would be difficult to navigate for older patients.
Bedside interviews with patients/family (Round 2): A total of five patients and two family members participated in the second round of bedside interviews. Table 1 includes a summary of patient/family preferences related to participation in development of the plan of care and the features and workflows defined in group interviews by professional providers.
Meetings with clinical and administrative leaders and stakeholders: Based on our meetings with clinical and administrator leaders stakeholders we learned that the 18 inch touch screen devices that we planned to install at the bedside were not feasible given the organizations plan to install bedside devices for providers as part of a larger electronic medical record implementation. We made a decision to go with mobile devices and to implement the PCTK on the iPad Air. As a result, we had to re-configure the user interface to optimize use on a mobile tablet device with a much smaller screen size. This new set of requirements led us to rework the user interface to accommodate the smaller screen size and to address the usability issues identified by patients, family, and professional stakeholders.
Table 1:
Patient/Family feedback related to Plan of care elements and workflow
| Plan of Care Elements and Workflow | Personally would use (n=7) | Thought others would use (n=7) | Favorite Element |
|---|---|---|---|
| Personal goals for hospitalization | 86% | 100% | |
| Feedback to care team on how well they are helping to accomplish goals | 71% | 100% | |
| Preferences for care | 57% | 100% | |
| Care team clinical goals | 86% | 100% | |
| Concerns related to care | 71% | 100% | |
| Medical problem list/Infobuttons | 100% | 100% | |
| Outpatient providers access to hospitalization plan of care | 71% | 100% | |
| Schedule | 100% | 100% | |
| Care team names/Pictures/Roles | 86% | 100% | 14% |
| Messaging capability re: plan of care | 86% | 100% | |
| Safety dashboard/Infobuttons | 71% | 100% | |
| Test results/Infobuttons | 100% | 100% | 28% |
| Medications/Infobuttons | 100% | 100% | 28% |
| Food and Diet | 100% | 100% | |
| Discharge check list | 86% | 100% | |
| Did not answer | 0% | 0% | 30% |
Discussion
We used an iterative participatory design approach to develop the plan of care and provider communication features of the PCTK for use with intensive care and oncology patients and family members. Participatory design is based on the classic principles of user centered design including: 1) Early focus on users and tasks; 2) Empirical measurement; and 3) Iterative design and development.[15] In our earlier work, we involved end users (patients and family members) and other stakeholders (professional care team members) in identifying the core set of information needed to engage patients in their plan of care.[9, 10] In this project, we continue to work with patients, family, and professional care team members to broaden our understanding of the information, tools and tasks associated with involving patients in the plan of care development process. Interestingly, through this approach, a set of information needs identified from our prior work was confirmed as useful by all patients and family members that participated in interviews: medical problem list, schedule, test results, medications, and food and diet. In addition to information needs identification, our approach enabled the identification of communication needs. We found that patients and family desire tools to help them communicate their goals, problems, concerns, and care preferences. They also would like to communicate directly with their professional care team members when questions and concerns about their plan of care arise. The rapid prototyping method was an effective way to involve patients, family and stakeholders in identifying usability problems and gaps in functionality that could be a barrier to use if not corrected. Our team has usability evaluation studies with clinicians to identify explicit information and communication needs in the context of a documentation workflow for goals of care[16]but to our knowledge this is the first study to define patient and family information and communication needs in the context of a documentation workflow for patient-centered care planning.
The initial prototype lacked specific tools to allow patients and family to document their personal goals, concerns, problems and preferences for care. It did include a space for patients and family to write questions that they could later share with the care team, but patients and family told us that this was insufficient; they wanted to directly communicate with their care team members. We added the care planning tools and a message board to the next prototype but soon learned from patients, family, and care team members that the user interface was too busy and that it would be difficult for older patients or patients who are not computer savvy to use. We simplified the user interface and the care planning tools in the next version of prototypes and have received positive feedback about patient and family intention to use the toolkit.
In addition to the feedback from stakeholders, our choice of hardware had an impact on the user interface. Specifically, changing from a mounted 18-inch touch screen device to an iPad Air forced us to reconfigure the interface from a horizontal to vertical tab, rearrange/remove content from the home screen, to rethink our navigation, and to leverage mobile optimized web-content. This was a difficult change to make but due to our ongoing communication with stakeholders, the issue was recognized early in the project when these types of changes could be made at a minimal cost.
In our most recent bedside interviews there was a limited sample of seven participants. Patients told us that they would use the care planning tools if they were available today and that they thought other patients would use it as well. Patients and family also reaffirmed the value of the additional information available from the PCTK such as pictures and roles of care team members, medications, test results, a discharge checklist, food and diet information, tailored information about their condition and their safety risks. Patients identified having access to their medications, schedule and laboratory results with Infobutton links to Medline Plus and other valid and reliable consumer literature as favorite features. One patient remarked, “I would like to have access to my medication schedule when the nurses are giving me my medication because all of the medications have such strange names— I like to keep track of what they are giving me”. Another family member remarked, “This is useful because you know the first thing we do when we get home is Google what these things mean.” We did have one patient who told us that although she could see how the PCTK could be useful for others that she would not use it. She said that she has the “right to ask for her paper chart” and that if she wanted information, she would request it. Given the emerging and mixed evidence of associations between engaged patients and a decrease in medication errors, these findings could inform our approach for measuring the impact of the PCTK on levels of patient engagement and adverse harm events.[17]
As we refine the PCTK software, we will continue to engage patients and family in using the software and in providing feedback on the user interface. As we have done in previous projects[18], we plan to implement the PCTK with our clinical nurse and physician champions and a subset of patients one month before go-live to ensure that we address any additional workflow or software issues before the tools are available to all patients on the oncology and intensive care units.
There are several limitations associated with this work. Our project is being conducted on a limited number of units in a single hospital. Our qualitative work has involved a limited number of patients and family and our findings may not reflect the views of other patients and family who have had similar or different experiences at BWH or at other hospitals. We consider ongoing patient, family and stakeholder involvement in the development of software as essential to designing software that is usable, useful and that will promote patient engagement in their plan of care. We will continue to engage patients and other stakeholders in this process as we further refine the PCTK software. In addition, we recognize that not all patients or family want to use computers or other devices to access information while in the hospital. Furthermore, some patients do not want to participate in developing their plan of care. The PCTK is meant to enhance current resources. A range of tools are likely needed to support hospitalized patients with different preferences and technical abilities.
Conclusion
While it is recognized that using technology to facilitate patient and family involvement in the plan of care could improve quality, safety and cost outcomes, their involvement to date is variable and evidence in this area is limited. Tools and processes are needed to provide hospitalized patients access to information about their condition and a set of tools to engage them in development of their plan of care. We found that many patients and family want to be knowledgeable about their condition and that they see value in tools that will help them to communicate their goals, problems, concerns, and care preferences. We also found that many patients, family members, and professional care team members are willing to participate in developing tools that will ultimately improve patient care and that they welcome the opportunity to make this contribution.
Figure 1:
Participatory PCTK Development Process
Figure 3:
PCTK Prototype 2
Resulting Mock-up: Distinct plan of care and communication features added to the prototype.
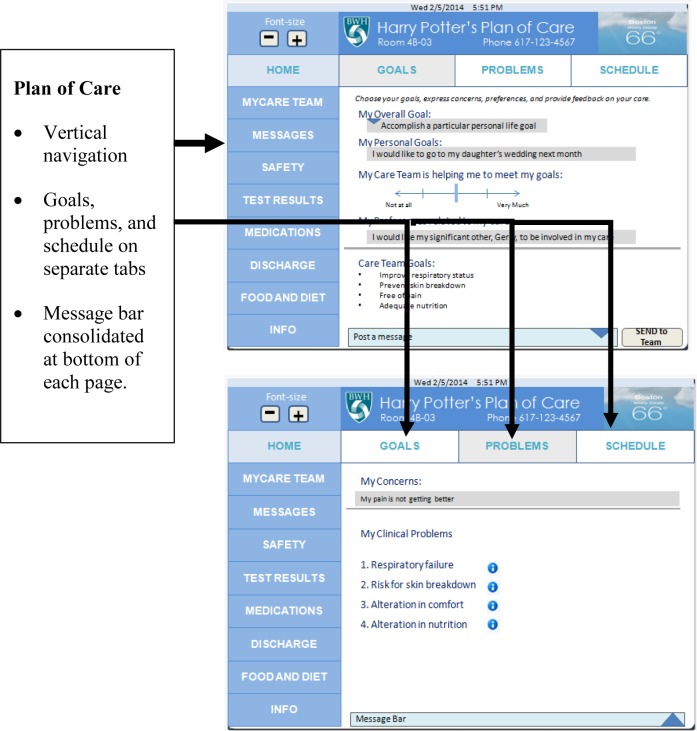
Figure 4a:
PCTK Prototype 3 (Patient Goals and Problems)
Resulting Mock-up: User interface simplified.
Figure 4b:
PCTK Prototype 3 (Patient Patient Schedule)
Acknowledgments
The authors would like to thank the BWH patients, family members, nurses, and physicians who provide ongoing feedback to inform development of the PCTK software. The BWH PROSPECT Project is part of the Libretto Consortium supported by the Gordon and Betty Moore Foundation.
References
- 1.Kripalani S, et al. Deficits in communication and information transfer between hospital-based and primary care physicians: implications for patient safety and continuity of care. JAMA. 2007;297(8):831–41. doi: 10.1001/jama.297.8.831. [DOI] [PubMed] [Google Scholar]
- 2.Quint JC. Communications problems affecting patient care in hospitals. JAMA. 1966;195(1):36–7. [PubMed] [Google Scholar]
- 3.Hibbard JH, Greene J. What the evidence shows about patient activation: better health outcomes and care experiences; fewer data on costs. Health Aff (Millwood) 2013;32(2):207–14. doi: 10.1377/hlthaff.2012.1061. [DOI] [PubMed] [Google Scholar]
- 4.AHRQ 20 Tips to Help Prevent Medical Errors: Patient Fact Sheet. 2011. [cited 2014 March 1]; Available from: http://www.ahrq.gov/consumer/20tips.htm.
- 5.HealthIT.gov Achieve Meaningful Use Stage 2. [cited 2014 March 7]; Available from: http://www.healthit.gov/providers-professionals/achieve-meaningful-use/core-measures-2/use-secure-electronic-messaging.
- 6.Dykes PC, et al. Fall prevention in acute care hospitals: a randomized trial. JAMA. 2010;304(17):1912–8. doi: 10.1001/jama.2010.1567. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Schnipper JL, et al. Role of pharmacist counseling in preventing adverse drug events after hospitalization. Arch Intern Med. 2006;166(5):565–71. doi: 10.1001/archinte.166.5.565. [DOI] [PubMed] [Google Scholar]
- 8.Houston TK, et al. Culturally appropriate storytelling to improve blood pressure: a randomized trial. Ann Intern Med. 2011;154(2):77–84. doi: 10.7326/0003-4819-154-2-201101180-00004. [DOI] [PubMed] [Google Scholar]
- 9.Caligtan CA, et al. Bedside information technology to support patient-centered care. Int J Med Inform. 2012;81(7):442–51. doi: 10.1016/j.ijmedinf.2011.12.005. [DOI] [PubMed] [Google Scholar]
- 10.Dykes PC, et al. Building and testing a patient-centric electronic bedside communication center. Journal of gerontological nursing. 2013;39(1):15–9. doi: 10.3928/00989134-20121204-03. [DOI] [PubMed] [Google Scholar]
- 11.AHRQ Guide to Patient and Family Engagement: Environmental Scan Report. 2012. [cited 2014 March 1]; Available from: http://www.ahrq.gov/research/findings/final-reports/ptfamilyscan/ptfamily1.html.
- 12.Berwick DM, Nolan TW, Whittington J. The triple aim: care, health, and cost. Health Aff (Millwood) 2008;27(3):759–69. doi: 10.1377/hlthaff.27.3.759. [DOI] [PubMed] [Google Scholar]
- 13.Rogers ML, et al. Usability Testing and the Relation of Clinical Information Systems to Patient Safety. In: Henriksen K, et al., editors. Advances in Patient Safety: From Research to Implementation: Concepts and Methodology. Rockville, MD: 2005. [PubMed] [Google Scholar]
- 14.Dabbs A, Myers B, Dew M. User-Centered Design and Interactive Health Technologies for Patients. Comput Inform Nurs. 2009;27(3):175. doi: 10.1097/NCN.0b013e31819f7c7c. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Gould J, Lewis C. Designing for usability: Key principles and what designers think. Communications of the ACM. 1985;28(3):300–11. [Google Scholar]
- 16.Collins SA, et al. Model development for EHR interdisciplinary information exchange of ICU common goals. Int J Med Inform. 2011;80(8):e141–9. doi: 10.1016/j.ijmedinf.2010.09.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Berger Z, et al. Promoting engagement by patients and families to reduce adverse events in acute care settings: a systematic review. BMJ Qual Saf. 2014 doi: 10.1136/bmjqs-2012-001769. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Dykes P, et al. Fall TIPS: strategies to promote adoption and use of a fall prevention toolkit. AMIA Annu Symp Proc. 2009;2009:153–7. [PMC free article] [PubMed] [Google Scholar]