Abstract
Objectives
To present our experience of treating symptomatic renal cysts by different techniques of laparoscopic decortication, as there are many treatment options for such cysts, each of them with advantages and drawbacks.
Patients and methods
Between January 2002 and December 2012, 51 patients underwent laparoscopic renal-cyst decortication; 15 of them had recurrent cysts after percutaneous aspiration. A retroperitoneal approach was adopted in 44 cases, transperitoneal in four and laparo-endoscopic single-site surgery (LESS) cyst decortication in three (two of them had bilateral renal cyst decortications in the same session). All patients were diagnosed by ultrasonography and computed tomography to determine the Bosniak classification of the cyst. Pain and cyst recurrence were assessed during the follow-up.
Results
All procedures were completed successfully, with no major intraoperative complications. The mean (range) operative duration was 56 (35–125) min, affected by the site and number of cysts unroofed. All patients were symptom-free except one, who had a recurrent large cyst, anteriorly located, and who underwent open cyst decortication.
Conclusions
Laparoscopic decortication of symptomatic renal cysts should be the standard of care, especially after failed percutaneous aspiration or decortication. LESS cyst decortication is a promising technique, especially with bilateral pathology. It is feasible with conventional laparoscopic instruments and gives a better cosmetic outcome.
Abbreviation: LESS, laparo-endoscopic single-site surgery
Keywords: Renal cyst, Laparoscopic decortication, Laparo-endoscopic single-site surgery
Introduction
Renal cysts are common and can represent a manifestation of an inherited or acquired disorder. Simple cysts are rare in childhood, but increase in frequency during adulthood [1]. The increasing incorporation of imaging into urological practice has produced a corresponding increase in the detection of renal cysts [2].
The indications for surgical intervention for renal cysts are pain, infection, hypertension, haemorrhage, collecting-system obstruction, or the risk of malignancy. The treatment options for symptomatic cysts include aspiration with or without instillation of sclerosing agents, percutaneous resection, and open or laparoscopic decortication [3].
Laparoscopic management has become the standard of care because it is minimally invasive and has a high success rate in terms of cyst recurrence [4]. Laparo-endoscopic single-site surgery (LESS) is increasingly used in urology, as it is less invasive than conventional laparoscopy, and can offer bilateral renal surgery in the same session and through the same port [5]. We present our experience in treating symptomatic renal cysts by different techniques of laparoscopic decortication, considering the morbidity and clinical outcome.
Patients and methods
Between January 2002 and December 2012, 51 patients (28 males and 23 females) underwent laparoscopic renal cyst deroofing, with 15 of them having recurrent cysts after percutaneous aspiration. The mean (range) age of the patients was 46 (17–65) years. Twenty-one patients had right renal cysts, 25 had left renal cysts and the remaining five had bilateral cysts. The mean (range) size of the cysts was 10.8 (8–16) cm. A retroperitoneal approach was used in 44 patients, transperitoneal in four and LESS in three (two had bilateral renal cyst decortication in the same session). The patients’ demographic data are summarised in Table 1.
Table 1.
The patients’ demographic data, and the complications classified according to the modified Clavien system.
| Variable | n (%) |
|---|---|
| Gender, male/female | 28 (55)/23 (45) |
| Laterality: | |
| Right | 21 (41) |
| Left | 25 (49) |
| Bilateral | 5 (10) |
| Presentation | |
| Renal pain | 51 (100) |
| Obstruction | 2 (4) |
| Laparoscopic approach | |
| Unilateral | 49 (96) |
| Bilateral | 2 (4) |
| Transperitoneal | 4 (8) |
| Retroperitoneal | 44 (86) |
| LESS transperitoneal | 3 (6) |
| Complications, by grade | |
| II, gonadal vessel injury | 1 (2) |
| I, fever | 3 (6) |
| I, ileus | 2 (4) |
| II, perinephric haematoma | 1 (2) |
The main presenting symptoms were renal pain in all patients, urinary tract obstruction in two, with microscopic haematuria due to lower polar cysts obstructing the upper ureter. After detecting the cysts with abdominal ultrasonography, CT with a renal-mass protocol was used and showed Bosniak type I or II cysts in all cases. Small unsymptomatic simple cysts (<5 cm) and renal cysts of higher grade (type IIF, III and IV Bosniak classification) were excluded. Urine analysis with culture and sensitivity was assessed in all patients, and urine cytology was assessed in those with haematuria.
The timeline of the procedures conforms to the development of our laparoscopic experience. The earlier patients were operated via a transperitoneal approach, later patients using a retroperitoneal approach, and recently we also used LESS.
For the retroperitoneal approach, under general anaesthesia the patients were placed in the standard lateral kidney position. A skin incision (2 cm) was made in the posterior axillary line midway between the iliac crest and the last rib. The incision was extended through the muscles and lumbar fascia. The index finger was then introduced to create sufficient space to accommodate the balloon. Three ports were used routinely. A fourth port was added in some patients, usually those with anterior upper-pole cysts. The cyst appeared in most cases as a blue dome, which was then dissected and its edge was delivered. The cyst contents were aspirated by a percutaneous needle under laparoscopic guidance, and the aspirate was sent for cytological analysis. The roof of the cyst was then excised with endoscissors and submitted together with several ‘bites’ from the floor of the cyst for a histopathological examination (Fig. 1). The cyst edge was sealed by electrocautery, and the perirenal fat was placed over the base of the cyst. Finally, a tube drain was left and the wounds were closed.
Figure 1.

Aspiration and decortication of a posterior mid-zonal intrarenal simple cyst through the retroperitoneal approach.
For the transperitoneal LESS cyst decortication we used a single-site, multiple-trocar technique. Through a peri-umbilical semicircular skin and subcutaneous incision, the first trocar was a 12-mm visual port (XCEL, Ethicon, NJ, USA), which was inserted under telescopic control. Two reusable 5-mm trocars were inserted under vision (Fig. 2). An extra-long 5-mm telescope with a 30° ‘down’ lens and conventional extra-long instruments was introduced. The procedure was completed as the conventional transperitoneal technique, with the opening of Toldt’s line, then mobilisation of the colon, identification of the cyst and percutaneous aspiration under laparoscopic guidance, then cyst deroofing and finally, an assurance of haemostasis.
Figure 2.

The technique used for single-site, multiple trocar LESS.
This method has decreased the cost per case considerably, because neither a custom-made port nor articulating instruments or telescope was used. Stepwise, the procedure is similar to a conventional transperitoneal laparoscopic cyst decortication.
In two patients we undertook bilateral renal cyst decortications in the same session, by changing the position of the patient during the procedure, leaving the primary trocar in place. At the end of the procedure the wound was closed anatomically, with a tube drain left in situ (Fig. 3). All patients were followed up for 6–12 months, assessing pain relief and cyst recurrence.
Figure 3.
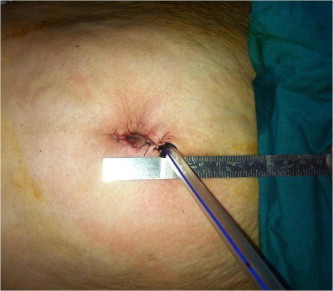
The wound after LESS, showing the emerging drain.
Results
All procedures were completed successfully, with no major intraoperative complications and no blood transfusions needed. The mean (range) operative duration was 56 (35–125) min, affected by the site and number of cysts unroofed.
There was a gonadal vessel injury in one patient that was secured. Oral feeding started 24 h after surgery but was delayed to 48 h in two patients (4%) due to a mild ileus that resolved spontaneously. There was a low-grade fever in three patients (6%). There were no urinary leakages or retroperitoneal collections. One patient who had LESS bilateral cyst decortication developed a right perinephric haematoma, which was managed conservatively.
For postoperative analgesia we used ketorolac, with a mean (range) dose of 25.2 (0–60) mg daily. The tube drain was removed 1–2 days after surgery. The hospital stay was 1–5 days and the return to normal activity was at 1–3 weeks.
Percutaneous aspiration under laparoscopic guidance showed a clear fluid, with negative cytology in all cases. No malignancy was detected on histopathological examination of the cyst walls. The patients were followed up for 6–12 months, with a clinical assessment for pain, and by abdominal ultrasonography. All patients were symptom-free, with no urinary tract obstruction. Early in our laparoscopic experience there was a recurrence in three patients. The recurrent cysts were small, at ≈2 cm, and painless in two patients. The third patient had an anterior upper-pole cyst of 7 cm in diameter, which was managed by open surgical decortication because of extensive perirenal adhesions. The various complications are also summarised in Table 1.
Discussion
Laparoscopic cyst decortication is an effective and durable treatment for symptomatic renal cysts, as assessed over a long-term follow-up. Its minimal invasiveness and greater success rate favour it over other treatments [6]. LESS is an emerging technique of minimally invasive urological surgery that is rapidly gaining in popularity. The outcome of LESS shows that it can be used safely and effectively in many urological procedures, including cyst decortication, which can be done bilaterally in the same session [7].
The percutaneous aspiration of simple renal cysts is an easy and safe procedure, and can be used to ascertain if cyst decompression results in the resolution of pain, and if not, then to justify further more invasive treatment; however, it is associated with high rate of recurrence. The percutaneous instillation of sclerosing agents into simple renal cysts is associated with success rates of 75–97%, with a complication rate of 1.3–20% [8]. In the present study we included 15 patients with a recurrence after percutaneous aspiration, and injection with sclerosing materials was tried in six of them. The percutaneous resection of renal cysts also has been advocated. The long-term results showed a 30% recurrence rate and 20% residual cysts [9].
Some authors recommended that retrograde pyelography should be used just before the start of the laparoscopic procedure, especially in those with parapelvic and parenchymal cysts, to assess cyst communication with the collecting system, and possibly an injection with methylene blue via a ureteric catheter for a final check at the end of the manoeuvre. However, we think that this is not mandatory and we did not use this in our series where there were no significant complications [10].
The retroperitoneal approach reduces the risk of hypercarbia, hypothermia, postoperative ileus, inadvertent intra-abdominal organ injury and hernia formation, compared to the transperitoneal approach, which was adopted during our early experience [11]. To date, retroperitoneoscopy is our approach of choice for managing symptomatic renal cysts.
Cysts can recur, possibly due to incomplete handling or incomplete excision of the cyst wall. To decrease the possibility of recurrence, the renal cyst wall should be completely excised if possible. If it is not possible to excise the cyst wall completely, the perinephric fat should be tacked into the cavity [12]. We report three cases of recurrence, where one of them necessitated open surgery for an anteriorly located upper-pole cyst.
LESS can be retroperitoneal or transperitoneal. For urologists, the retroperitoneal approach is preferable and familiar, hence many surgeons started retroperitoneal LESS with a simple technique such as cyst decortication [13]. Recently, we changed our practice for cyst decortication to the LESS transperitoneal approach, as it provides a wide working space, can be applied bilaterally in the same session, and is more cosmetically acceptable.
In conclusion, the laparoscopic decortication of symptomatic renal cysts should be the standard of care, especially after failed percutaneous aspiration or decortication. LESS cyst decortication is a promising technique, especially with bilateral pathology. It is feasible with conventional laparoscopic instruments and has a better cosmetic outcome. Further work is needed to assess its safety and efficiency.
Conflict of interest
None.
Funding
There was no extra funding needed.
Footnotes
Peer review under responsibility of Arab Association of Urology.
References
- 1.Hanash K.A., Al-Othman K., Mokhtar A., Al-Ghamdi A., Aslam M. Laparoscopic ablation of giant renal cyst. J Endourol. 2003;17:781–784. doi: 10.1089/089277903770802371. [DOI] [PubMed] [Google Scholar]
- 2.McHugh K., Stringer D.A., Hebert D., Babiak C.A. Simple renal cysts in children. Diagnosis and follow up with ultrasound. Radiology. 1991;178:383–385. doi: 10.1148/radiology.178.2.1987597. [DOI] [PubMed] [Google Scholar]
- 3.Rane A. Laparoscopic management of symptomatic simple renal cysts. Int Urol Nephrol. 2004;36:5–9. doi: 10.1023/b:urol.0000032669.21924.d1. [DOI] [PubMed] [Google Scholar]
- 4.Hulbert J.C. Laparoscopic management of renal cystic disease. Semin Urol. 1992;10:239–241. [PubMed] [Google Scholar]
- 5.Liu C., Pan B., Zheng S., Xu A. Laparoendoscopic single-site surgery for symptomatic renal cyst decortication using a homemade glove port device: initial experience. Urol Int. 2012;89:180–184. doi: 10.1159/000339967. [DOI] [PubMed] [Google Scholar]
- 6.Atug F., Burgess S.V., Ruiz-Deya G., Mendes-Torres F., Castle E.P., Thomas R. Long-term durability of laparoscopic decortication of symptomatic renal cysts. Urology. 2006;68:272–275. doi: 10.1016/j.urology.2006.03.009. [DOI] [PubMed] [Google Scholar]
- 7.Kaouk J.H., Autorino R., Kim F.J., Han D.H., Lee S.W., Yinghao S. Laparoendoscopic single-site surgery in urology. worldwide multi-institutional analysis of 1076 cases. Eur Urol. 2011;60:998–1005. doi: 10.1016/j.eururo.2011.06.002. [DOI] [PubMed] [Google Scholar]
- 8.Pearle M.S., Traxer O., Cadeddu J.A. Renal cystic disease: laparoscopic management. Urol Clin North Am. 2000;27:661–673. doi: 10.1016/s0094-0143(05)70116-6. [DOI] [PubMed] [Google Scholar]
- 9.Kang Y., Noble C., Gupta M. Percutaneous resection of renal cysts. J Endourol. 2001;15:735–738. doi: 10.1089/08927790152596343. [DOI] [PubMed] [Google Scholar]
- 10.Roberts W.W., Bluebond-Langner R., Boyle K.E., Jarrett T.W., Kavoussi L.R. Laparoscopic ablation of symptomatic parenchymal and peripelvic renal cysts. Urology. 2001;58:156–159. doi: 10.1016/s0090-4295(01)01145-1. [DOI] [PubMed] [Google Scholar]
- 11.Ferzli G., Raboy A., Kleinerman D., Albert P. Extraperitoneal endoscopic pelvic lymph node dissection vs. laparoscopic lymph node dissection in the staging of prostatic and bladder carcinoma. J Laparoendosc Surg. 1992;2:219–222. doi: 10.1089/lps.1992.2.219. [DOI] [PubMed] [Google Scholar]
- 12.Porpiglia F., Fiori C., Billia M., Renard J., Di Stasio A., Vaccino D. Retroperitoneal decortication of simple renal cysts vs decortication with wadding using perirenal fat tissue: results of a prospective randomized trial. BJU Int. 2009;103:1532–1536. doi: 10.1111/j.1464-410X.2008.08294.x. [DOI] [PubMed] [Google Scholar]
- 13.Chen D., Xue B., Shan Y., Yang D., Sun C. Retroperitoneal laparoendoscopic single-site surgery by single trocar technique: initial experience with renal cyst decortication. J Laparoendosc Adv Surg Tech A. 2012;22:972–977. doi: 10.1089/lap.2012.0255. [DOI] [PubMed] [Google Scholar]



