Abstract
Introduction
Previous research suggests that work with a suitable workload may promote health and work retention in people with disability. This study will examine whether temporary work modifications at the early stage of work disability are effective in enhancing return to work (RTW) or staying at work among workers with musculoskeletal or depressive symptoms.
Methods and analysis
A single-centre controlled trial with modified stepped wedge design will be carried out in eight enterprises and their occupational health services (OHSs) in nine cities in Finland. Patients seeking medical advice due to musculoskeletal pain (≥4 on a scale from 0–10) or depressive symptoms (≥1 positive response to 2 screening questions) and fulfilling other inclusion criteria are eligible. The study involves an educational intervention among occupational physicians to enhance the initiation of work modifications. Primary outcomes are sustained RTW (≥4 weeks at work without a new sickness absence (SA)) and the total number of SA days during a 12-month follow-up. Secondary outcomes are intensity of musculoskeletal pain (scale 0–10), pain interference with work or sleep (scale 0–10) and severity of depressive symptoms (Patient Health Questionnaire, PHQ-9), inquired via online questionnaires at baseline and 3, 6, 9 and 12 months after recruitment. Information on SA days will be collected from the medical records of the OHSs over 12 months, before and after recruitment.
The findings will give new information about the possibilities of training physicians to initiate work modifications and their effects on RTW in employees with work disability due to musculoskeletal pain or depressive symptoms.
Ethics and dissemination
The Coordinating Ethics Committee of Hospital District of Helsinki and Uusimaa has granted approval for this study. The results will be published in peer-reviewed journals.
Trial registration number
ISRCTN74743666.
Keywords: EPIDEMIOLOGY, MENTAL HEALTH, Job accommodation, Return to work
Strengths and limitations of this study.
This study protocol describes an educational intervention study in which all participating occupational physicians will attend an interactive seminar organised in small groups and allowing in-depth discussions on various possibilities for work modification.
Registers of the occupational health services and employers will be used to obtain information on the primary outcomes, and comprehensive questionnaires will be completed at 3 months intervals over 1 year for the secondary outcomes.
Implementation of work modifications will be followed with questionnaires.
A limitation of the design of the study is that it is a controlled trial. Randomisation was not considered feasible, as it would be very difficult for the occupational physicians not to apply the principles and practices discussed and agreed on in the educational seminar.
Introduction
Musculoskeletal and mental disorders are the two most common health problems associated with work disability worldwide. In the OECD countries, 6% of the working-age population receives disability benefits.1 In Finland, musculoskeletal disorders (MSDs) account for about a third, and mental disorders a fourth, of all sickness absence (SA) benefit expenditures,2 and both produce a third of all disability pensions.3 Current evidence also suggests that musculoskeletal pain and depressive symptoms often co-occur.4 5 Recently, 15% of actively working Finns were found to report such co-occurrence, which was strongly related to poor self-rated physical work ability and intentions of early retirement.6
Staying active instead of taking bed rest has been shown to improve recovery from MSDs.7–10 The question arises whether staying active at work and performing suitable work activities can prevent prolongation of work disability. Although the amount of research in the field of work disability and return to work (RTW) has steadily increased,11 there is still limited evidence on the effectiveness of interventions targeted at RTW.12 Some workplace-based interventions, including either work modifications and/or involvement of workplace key stakeholders (eg, worker, employer, RTW coordinator) have shown promising results.13–15 Some of these studies used an integrated concept in which individually and workplace directed interventions are combined.16–18 Loisel et al18 were able to show that an occupational intervention combined with clinical intervention was clearly superior to a clinical intervention alone in enhancing RTW in workers with low back pain-related work disability lasting for more than 4 weeks. Their ‘Sherbrook model’ has also been transferred to other social systems19 and shown to be effective.17 20 In a Dutch study, workplace intervention alone enhanced RTW in workers sick-listed 2–6 weeks due to low back pain.16
While some evidence exists that RTW can be enhanced in persons with MSDs, the evidence among those with depressive symptoms is more limited and conflicting.14 21–24 Most studies have examined the effects of medication and individual therapies. However, according to a recent systematic review, adding a work-directed intervention to a clinical intervention reduced the number of SA days compared with a clinical intervention alone.25 A meta-synthesis of eight qualitative studies concluded that workers with common mental disorders had difficulty deciding when they were ready to resume work and seeing how RTW solutions could be implemented at the workplace.26
It is known that the longer the work disability continues, the more difficult it is to return to work.14 After a short SA spell, most persons RTW. On the other hand, it is important already at the early stage to identify those who are at risk for prolonged sick leave and to see whether possible obstacles for RTW can be managed. Van Duijn et al27 have emphasised the need for proper timing of interventions on RTW. They concluded that only very low cost interventions—such as work modifications—could potentially be cost-effective at an early stage of SA.27 However, only a few interventions, initiated during the first 6 weeks of SA, have been carried out.28
The main aim of the current study is to examine the efficacy of temporary work modifications (eg, workplace adaptations, altered work hours, amended duties, phased RTW), initiated at an early stage of work disability, on RTW in workers seeking medical advice at the occupational health service (OHS) due to musculoskeletal pain or depressive symptoms. We hypothesise that continuing to work with a suitable workload is beneficial with regard to health outcomes and RTW, and that temporary modification of workload will enhance RTW and work retention. In addition, we hypothesise that a suitable workload can be achieved with temporary work modifications and their use can be enhanced by an educational intervention among occupational physicians (OPs).
Methods and analysis
Study population and recruitment
The study will be carried out by the Finnish Institute of Occupational Health in collaboration with eight medium-sized or large enterprises and their OHSs in nine cities in Finland. In these enterprises, the vast majority of workers will seek medical advice in their OHS for any illness. Patients seeking medical advice primarily due to musculoskeletal pain or depressive symptoms are asked to reply to the following three screening questions:
“How would you rate the intensity of your musculoskeletal pain on a numerical scale from 0 (no pain) to 10 (the worst possible)?”
“During the past month, have you often been bothered by feeling down, depressed, or hopeless? (no/yes).”29
“During the past month, have you often been bothered by little interest or pleasure in doing things? (no/yes).”29
The OPs will offer the possibility of recruiting to the study to all eligible patients fulfilling the inclusion criteria (table 1). The patients will receive general information about the study, the type of data to be gathered and what they are requested to do. All information will also appear on a written handout that the OPs will give to the patients. Participation is voluntary and the patients can withdraw from the study at any stage. Non-participation or withdrawal will not be known by workplace parties and will not affect the treatment of the patient. A written informed consent is requested concerning participation in the study, employment data from the employers’ records, as well as dates and diagnoses of SA from the medical records of the OHS.
Table 1.
Inclusion and exclusion criteria of the study
| Inclusion criteria | Exclusion criteria |
|---|---|
| 1. Musculoskeletal pain (≥4/10) or/and depressive symptoms (positive response to any of the 2 screening questions on depression) | 1. Anticipated long absence from work during the following 12 months due to other reasons, such as pregnancy, studies, military service, alternation leave, other illness or its treatment (eg, surgery, cytostatic therapy or radiation therapy) |
| 2. Age 18–60 years, male and female | 2. Serious or acute disease requiring full sickness absence (eg, febrile infection, active stage of inflammatory joint disease; serious mental disorder) |
| 3. Working full-time or nearly full-time (≥30 h/week) | 3. Other factors having significant effect on disability (eg, serious conflict at the workplace, difficult personal life situation, current problem due to a work accident, current insurance or workmen’s compensation dispute, severe alcohol or drug dependency) |
| 4. Employed in current job 4 months or longer and employment likely to continue for the following 12 months | |
| 5. Functional ability not sufficient to perform current work tasks | |
| 6. Previous sickness absence of 6 weeks or less during the preceding 3 months |
Study design
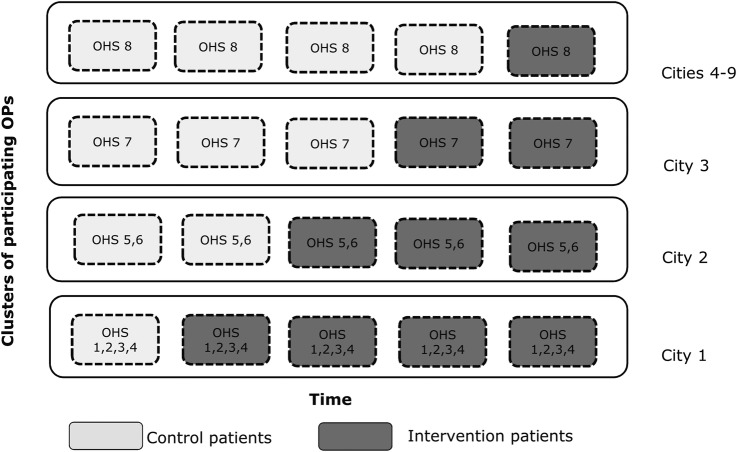
This study is a single-centre controlled trial using a modified stepped wedge design. It involves an educational intervention among OPs where the central focus is to develop individually tailored work modifications for patients with musculoskeletal pain or depressive symptoms. The physicians make the recommendations, and the more detailed planning and implementation are carried out in collaboration with the patients and their supervisors. Once this kind of process has been agreed on and started, it will continue at the workplace. Therefore, randomisation is not feasible, hence we chose to carry out a controlled trial. Furthermore, we will apply a modified stepped wedge design.30–32 In our study, groups of OPs first recruit patients to the control group and after an educational seminar they start to recruit patients to the intervention group (figures 1 and 2). Not all control patients will later seek medical advice and receive the intervention from an educated OP; therefore it is not possible to apply a classical stepped wedge design. Also, the timing of the intervention is not random in our study. The stepped wedge design is relevant and used for evaluating interventions for which there is empirical evidence or a belief that the intervention will do more good than harm.31
Figure 1.
Illustration of stepped wedge design, adapted from Brown and Lilford 2006.30 OHS, occupational health service; OP, occupational physician.
Figure 2.
Flowchart of the study. OHS, occupational health service; SA, sickness absence; WM, work modifications.
Intervention
Preliminary focus group discussions
OPs play a crucial role in initiating work modifications and as mediators between the workplace and the employee. To get a preliminary understanding of OPs’ experiences with work modifications and rationales for encouraging early RTW, focus group discussions will be carried out. Topics of the discussions are, for example, the different types of reasoning of the OPs when deciding to initiate work modifications, what kind of work modifications are needed and can be made for workers with musculoskeletal pain and depressive symptoms in different types of work, and which factors facilitate or hinder the use of work modifications. The results of the discussions will be utilised in planning educational seminars for OPs during the intervention phase (see below).
Educational seminar
Before enrolling patients to the intervention, OPs will participate in a 1 day interactive educational seminar, organised by the researchers. During the seminar, the OPs will be challenged and supported to examine their present practices in enhancing early RTW. Current evidence on factors promoting RTW in musculoskeletal and mental disorders will be reviewed and discussed. In addition, part of the seminar will be attended by representatives of the enterprise leadership who will participate in discussions on how to follow the agreed practices on early RTW in the specific enterprise. About 2 months after the seminar, the OPs will be re-interviewed on their current practices.
Prescription of work modifications
Based on a medical examination, the OP will decide whether the patient will be able to continue at work with adjusted workload without jeopardising health and recovery. For patients who have been assessed as capable to continue their work, the OP will make a prescription of work modifications with details regarding reduction of physical workload (eg, lifting, carrying, bending, repetitive movements, vibration, typing/use of mouse, etc), work hours and other adjustments or phased RTW. The prescription will be discussed with the patient, who will take it to the supervisor to be implemented as soon as possible. In our study, temporary work modifications can be prescribed for a maximum of 1 month per visit and for a maximum of 3 months per illness spell.
Data collection
Questionnaires and registers of the OHSs and the employers will provide data on outcomes and other variables presented in table 2. The patients are requested to reply to the questionnaires, all sent via secured internet connection, at baseline (BL) and at 3, 6, 9 and 12 months’ follow-up. For those who do not want to use a computer or do not have regular computer access, a paper version of the questionnaire will be sent via postal mail. Non-responders are reminded twice at 1 week intervals. More extensive questionnaires are delivered at BL and at the 12-month follow-up, while all other questionnaires are shorter.
Table 2.
Data collection from the OHS's medical files and with repeated questionnaires
| Variables | Source |
||
|---|---|---|---|
| Outcomes | OHS's medical records | ||
| Primary outcomes | |||
| Time to sustained RTW (performing work duties ≥4 weeks without a new SA spell) | Dates and diagnoses of SAs | ||
| Total number of SA days during the 12-month follow-up | |||
| Questionnaires | |||
| Secondary outcomes | BL | 3, 6, 9 months | 12 months |
| Intensity of musculoskeletal pain during the previous 7 days (0=no pain, 10=the worst possible)34 | x | x | x |
| Pain interference with work and sleep during the previous 7 days (0=not at all, 10=unable to work/sleep)34 and severity of depressive symptoms35 36 | x | x | x |
| Health, work ability and use of healthcare services | |||
| Perceived health (1=excellent, 5=poor)37 | x | x | x |
| Health-related quality of life38 39 | x | x | x |
| Current work ability vs the lifetime best (0=unable to work, 10=work ability at its best)40 41 | x | x | x |
| Current work ability vs physical and mental work demands (1=very good, 5=very poor)40 41 | x | x | x |
| Prospects to continue in current job 2 years from now, taking into consideration health (1=relatively certain, 2=not certain, 3=unlikely)40 41 | x | x | |
| Meaning of work (0=not meaning at all, 10=one of the most important things in life)42 | x | x | |
| Most critical physical and mental workload factors with regard to continuing at work | x | x | x |
| Current full/part-time sick leave (no/yes) | x | x | x |
| Sick leave during preceding 3 months (no/yes) | x | x | |
| Estimation of time to RTW (1=in less than a week, 7=RTW is unlikely) | x | x | x |
| Pain medication (1=no, 2=occasionally, 3=regularly) | x | x | x |
| Physician-diagnosed depression (1=no, 2=once, 3=several times) | x | x | x |
| Antidepressants (no/yes) | x | x | x |
| Use of healthcare services (times during the preceding 3 months; occupational health nurse/other nurse, OP/general practitioner/specialist, (occupational) physiotherapist, (occupational) psychologist, psychotherapist) | x | x | x |
| Covariates | |||
| Demographic factors | |||
| Age | x | ||
| Gender | x | ||
| Marital status | x | ||
| Education | x | ||
| Occupational factors | |||
| Occupational title | x | x | x |
| Main work task | x | x | x |
| Job seniority (years/current work task) | x | x | |
| Main work schedule in current work task (daytime job/evening-/night-/two-shift-/three-shift work, other) | x | x | x |
| Average working time (h/week), main occupation | x | x | x |
| Commuting time to work | x | x | |
| Secondary job (no/yes) | x | x | |
| Average working time (h/week), secondary job | x | x | |
| Physical and psychosocial factors at work | |||
| Physical strenuousness of work (1=light, 5=very strenuous)43 | x | x | x |
| Lifting, carrying, or pushing loads (6–15 kg, 16–25 kg, >25 kg average number of times/working day)44 | x | x | x |
| Awkward trunk postures ≥1 min at a time (modified) (1=rarely/never, 5=almost constantly/constantly)45 | x | x | x |
| Mental and social strenuousness of work (1=light, 5=very strenuous)43 | x | x | x |
| Mental work demands (1=never, 5=constantly)46 | x | x | x |
| Perceived work uncertainty (1=very little, 5=very much)47 | x | x | x |
| Workplace atmosphere (1=very good, 5=very poor)47 48 | x | x | x |
| Effort-reward imbalance (1=very much, 5=very little)49 | x | x | |
| Supervisor support (1=very often, 5=very rarely)46 | x | x | x |
| Co-worker support (1=very often, 5=very rarely)46 | x | x | x |
| Possibilities for work modifications (1=very much, 5=not at all) | x | ||
| Worsening of symptoms due to work (1=not at all, 5=very much) | x | ||
| Lifestyle factors | |||
| Height | x | ||
| Weight | x | ||
| Smoking (never-smoker, ex-smoker, occasional, regular smoker)51 | x | ||
| Alcohol consumption (density: 1=not at all, 7=daily/almost daily; volume, ≥6 doses: 1=never, 6=daily/almost daily)48 | x | ||
| Physical exercise during the previous 12 months (≥20 min per time)48 | x | x | |
| Sitting time (h/per working day, at work/leisure)48 | x | x | |
| Sleeping time (h/day)53 | x | x | |
| Sleeping problems during the preceding 4 weeks (1=never, 6=almost every night)52 | x | x | x |
| Daytime sleepiness compared to others of the same age (1=no, 2=yes, often, 3=yes, almost always, 4=can't say)53 | x | x | x |
| Use of sleeping pills (1=no, 2=no during the preceding 4 weeks, 3=less than once a week, 4=1–2 times/week, 5=more often)53 | x | x | x |
| Recommended work modifications and work task redistribution during SA | |||
| Who did the work during the sick leave (1=no one, 2=someone else, 3=I'll do it/I'll do it later, 4=don't know about the arrangements) | x | x | |
| Shortened working time during the preceding 3 months recommended by a physician (no/yes) | x | x | |
| Shortened working day (no/yes) | x | x | |
| Shortened working time (h/day) | x | x | |
| Shortened work week (no/yes) | x | x | |
| Number of working days/week | x | x | |
| Reduction in working time in other ways (no/yes) | x | x | |
| Who did the work during shortened working time (substitute) | x | x | |
| Work modifications implemented during the preceding 3 months to enhance the performance of work duties (no/yes) | x | x | |
| Would the modifications have been necessary (no/yes) | x | x | |
| What modifications have been implemented (1=work aids/tools, 2=ergonomics changes, 3=altered work hours/breaks, shift arrangements, 4=working from home, 5=reduced work load/omitted work tasks, 6=amended duties, 7=other modifications) | x | x | |
| Adequacy of modifications (1=yes, 2=yes, partly, 3=no) | x | x | |
| What kinds of modifications would additionally have been necessary | x | x | |
OHS, occupational health service; RTW, return to work; SA, sickness absence; BL, baseline; OP, occupational physician.
Information on durations and diagnoses (International Classification of Diseases and Related Health Problems, ICD-10)33 of SA will be gathered from the medical records of the OHSs over 12 months before and after recruitment (figure 2). Those whose employment preceding recruitment was shorter than 12 months will be followed from the beginning of their employment. Information on employment during the study, and absences due to disease and other causes (eg, studies, military service, parental leave, job alternation leave) will be retrieved from the employers’ records.
Outcomes
Primary outcomes
The main outcomes are (1) time to sustained RTW, that is, performing work duties at least for 4 weeks without a new SA spell and (2) total number of SA days during the 12-month follow-up.
Secondary outcomes
Secondary outcomes are: intensity of musculoskeletal pain, pain interference with work, pain interference with sleep and severity of depressive symptoms.
The respondents are asked whether they have had musculoskeletal pain during the previous 7 days (no/yes). If the answer is ‘yes’, they are asked to mention all of the specific anatomical sites (neck, shoulder, elbow/forearm, wrist/hand, lower back, hip/thigh, knee, ankle/foot, other) with pain, with an indication of the site with the most severe/harmful pain.
Intensity of pain is inquired by the question: “What is the intensity of the most harmful musculoskeletal pain?”; and pain interference with work and sleep by the questions: “How much has the most harmful pain interfered with your work/sleep during the previous 7 days?”.34 Depressive symptoms are assessed by the Finnish version35 of the Patient Health Questionnaire (PHQ-9)36 (table 2).
Health, work ability and use of healthcare services
Perceived health37 and health-related quality of life,38 39 current work ability, work ability in relation to physical and mental job demands and, from the standpoint of health, ability to work in the current job 2 years from now,40 41 will be measured. The meaning of working is asked about by a modified query from the questionnaire by England et al.42 Self-formulated open questions are used to assess the most critical physical and mental workload factors regarding continuing to work. The occurrence of current full or part-time sick leave, as well as sick leaves during the preceding 3 months and the subjects’ estimation of the time they believe they are able to RTW with regard to health, will be asked at 3-month intervals. The use of pain medication or antidepressants prescribed by a physician and the use of healthcare services, will also be ascertained (table 2).
Covariates
Demographic factors
Questionnaires will cover data on age, gender, marital status and education.
Occupational factors
The following occupational factors will be inquired: occupational title, main work task, job seniority, main work schedule in the current work task, commuting time to work, secondary job, average working time in the main occupation as well as in the secondary job (table 2).
Physical and psychosocial factors at work
The respondents will be asked to assess physical, mental and social strenuousness of work,43 the amount of lifting, carrying or pushing loads,44 and awkward trunk postures.45 Mental demands of the work are assessed by 10 items,46 and perceived work uncertainty47 and workplace atmosphere by modified questions used in national surveys.47 48 Effort-reward imbalance is studied using a single question for effort and three questions for reward.49 Supervisor and coworker support are assessed with a modified question adopted from a validated questionnaire:46 “Does your supervisor/coworker provide support and help when needed?”. Possibilities for work modifications due to health reasons when needed and participants’ evaluation on worsening of symptoms by work will be measured by self-formulated questions (table 2).
Lifestyle factors
Weight and height are asked to calculate body mass index.50 Modified questions from the Health 2000 Survey48 51 will be used to assess smoking, alcohol consumption, physical exercise, average sitting time and sleeping time. Sleeping problems will be measured by the Jenkins Sleep Problems Scale.52 Perceived daytime sleepiness and use of sleeping pills is also ascertained.51 53 (table 2).
Recommended work modifications and work task redistribution during SA
Information on implementation of work modifications at the workplaces will be gathered by self-formulated questions. We will ask who will do/did one's work tasks during a sick leave and whether working time was shortened based on recommendation by a physician. If ‘yes’, we will have further questions on how the working time was modified and who will/has performed the work tasks during the shortened working time. We will also ask whether work modifications have been done in order to enhance the performance of duties and if ‘no’, would these have been necessary. If ‘yes’, we will ask to specify them. We will also ask to describe in more detail what kind of modifications have been done, whether they were sufficient to support the performance of work duties, and what kinds of modifications would additionally have been necessary (table 2).
Statistical analyses
The intervention and control group will be compared with regard to potential confounders (age, gender, occupational group, localisation and intensity of musculoskeletal pain, severity of depressive symptoms, pre-recruitment SA, urban/rural area, public/private sector, size of enterprise). Time to sustained RTW will be compared between the intervention and control group using lifetime tables. Survival analysis will be applied to test for the statistical significance of the differences and to control for potential confounders. We will control for the effect of clusters of OPs, enterprises and cities using generalised estimation equations. If differences between intervention and control group are seen in several possible confounders, the groups will be matched on propensity score.54 55 Additionally, we will look at the post-recruitment-pre-recruitment difference in the number of SA days during the 12-month periods using difference in differences analysis (figure 2).
Ethics and dissemination
Ethical approval has been granted from the Coordinating Committee of Hospital District of Helsinki and Uusimaa. The results will be published in a peer-reviewed journal and at conference presentations.
Discussion
This study will examine the efficacy of temporary work modifications at an early stage of work disability on RTW among patients with musculoskeletal pain or depressive symptoms. The intervention consists of an educational seminar for OPs with the intention to promote the initiation of work modifications at the workplaces.
Carrying out intervention studies at the workplaces is difficult, recruitment of the workplaces and the subjects being one common challenge. Workplaces are not static. Their targets are to produce services and goods and to survive economically, which may not easily match with research purposes.56 57 It is essential that workplaces approve of the intervention study and perceive that they will gain benefits from participating in it.57 The current unstable economic situation may affect turnover of workers in the enterprises and also physicians in the OHSs, as well as activity in seeking treatment and in implementation of work modifications. To cope with this, we have recruited several enterprises. Discussing and finding appropriate work modifications for patients with depressive symptoms may be challenging, due to the sensitivity of the situation.
Work modifications are individual-based, but may have effects on coworker's work and how the work is organised at the workplace. An RCT would provide the strongest evidence for our research question. However, once physicians and the representatives of the employer have attended the education for enhancing the initiation and implementation of modifications, the old practice can no more be resumed, making randomisation a less feasible option.
Moreover, strict protocols may reduce the willingness to participate and the practitioners may decline to recruit subjects to be allocated at random. The use of the stepped wedge design may ease recruitment, since all of the physicians’ patients will get the intervention once the physician has started the intervention phase. This design will also allow control over the time effects and enable the detection of underlying trends.30 32
The primary intervention is to train the OPs to enhance the initiation of temporary work modifications, and discuss their implementation with the patient and his/her supervisor. There is a risk that an educational intervention will not produce the desired change in the activity to prescribe work modifications. Focus group discussions are carried out prior to the controlled intervention in order to obtain more insight into potentially effective work modifications, how they can be enhanced and what hindrances there may be in their implementation. New knowledge from the discussions will be utilised in the training of OPs.
The intervention study can face a problem due to controls being contaminated by the intervention, as there may be increased awareness of the study. We try to avoid this by giving the participating enterprises and their OPs, at the first stage, information primarily of the processes and principles of recruiting the controls to the study. Educational seminars for OPs will be given close to the initiation of the intervention phase.
Strengths of our study are the use of registers of the OHSs and employers to obtain information on the primary outcomes, and careful and comprehensive data collection by questionnaires at 3-month intervals over 1 year for the secondary outcomes. We will also gather data on the implemented work modifications at the workplaces.
The Finnish labour market system is based on a unique tripartite co-operation, in which organisations of wage earners and employers, and the government, negotiate and jointly agree on the development of the labour market. In practice, this means that, for example, in order to be able to implement work modifications at the workplaces, besides OHS's, employers’ and employees’ viewpoints and acceptance are also needed. Before starting the study, we had meetings with representatives of trade unions of participating industries and enterprises. Only one trade union was unwilling to recommend the study in their industry. In recruiting the enterprises to participate in the study, the human resource personnel and OHSs were involved in the meetings and gave their commitment to the study.
The research group has recently successfully conducted workplace interventions in the OHS setting. In our latest research, it was found that early partial sick leave enhanced sustained RTW. A long-term effect was seen on reduced SA58 and the intervention was observed to be more effective among patients whose current problem occurred <6 weeks before BL.59 These positive experiences, the trade unions’ support and the recent Finnish legislative changes, aimed to facilitate early RTW and prevent the prolongation of work disability in co-operation between the employer, employee and OHS provider, encouraged us to initiate the current study.
The results will give new information about the possibilities of training OPs to initiate temporary work modifications at an early stage of work disability and their effects in promoting RTW in employees with musculoskeletal pain or depressive symptoms. The findings are expected to have an impact in the work disability prevention policy in Finland and in countries with comparable social security systems.
Trial status
This study has been registered at International Standard Randomized Trial Number Register, register number ISRCTN74743666 (http://www.controlled-trials.com/ISRCTN74743666/). Patient enrolment started on 1st November 2013, and is planned to continue until June 2017. Results from the study are expected in 2018.
Footnotes
Contributors: EV-J, K-PM and TK conceived the study idea and finalised the research plan in collaboration with EH, SS, RH, TL, E-PT, IP and EM. SS and RS provided statistical expertise. EV-J, K-PM and EH participated in the recruitment of the enterprises and the OHSs. EV-J and EH took responsibility for the study management and co-ordination. EH is responsible for questionnaire data collection and RH for carrying out the focus group discussions. EH wrote the first version of the manuscript and EV-J, K-PM and SS helped in drafting. All authors provided feedback on drafts, and read and approved the final manuscript. EV-J is a guarantor of the study.
Funding: The Finnish Work Environment Fund (ref 112257) and the Academy of Finland (ref 267589) financially support the study. This work is also supported by the Work Disability Prevention CIHR Strategic Training Program, through the Canadian Institutes of Health Research (CIHR) grant(s) FRN: 53909.
Competing interests: None declared.
Patient consent: Obtained.
Ethics approval: The Coordinating Ethics Committee of Hospital District of Helsinki and Uusimaa.
Provenance and peer review: Not commissioned; peer reviewed for ethical and funding approval prior to submission.
References
- 1.OECD. Sickness, disability and work: breaking the barriers. A Synthesis of Findings across OECD Countries, 2010. http://www.oecd-ilibrary.org/social-issues-migration-health/sickness-disability-and-work-breaking-the-barriers_9789264088856-en (accessed 24 Mar 2015). [Google Scholar]
- 2.The Social Insurance Institution. Statistical yearbook of the Social Insurance Institution 2013. Official Statistics of Finland. Helsinki: Vammalan kirjapaino Oy, 2014. http://www.kela.fi/documents/10180/1630875/Statistical_Yearbook_of_the_Social_Insurance_Institution_2013.pdf/0578574a-2b93-4ca5-ac0f-650f12d15141 (accessed 24 Mar 2015). [Google Scholar]
- 3.Finnish Centre for Pensions (ETK), The Social Insurance Institution of Finland (KELA). Statistical yearbook of pensioners in Finland 2013. Official statistics of Finland. Helsinki: Erweko Oy, 2014. http://www.etk.fi/fi/gateway/PTARGS_0_2712_459_440_3034_43/http%3B/content.etk.fi%3B7087/publishedcontent/publish/etkfi/fi/julkaisut/tilastojulkaisut/tilastovuosikirjat/suomen_tyoelakkeensaajat_ja_vakuutetut_2013_7.pdf (accessed 24 Mar 2015). [Google Scholar]
- 4.Demyttenaere K, Bonnewyn A, Bruffaerts R et al. . Comorbid painful physical symptoms and depression: prevalence, work loss, and help seeking . J Affect Disord 2006;92:185–93. 10.1016/j.jad.2006.01.007 [DOI] [PubMed] [Google Scholar]
- 5.Munce SE, Stansfeld SA, Blackmore ER et al. . The role of depression and chronic pain conditions in absenteeism: results from a national epidemiologic survey. J Occup Environ Med 2007;49:1206–11. 10.1097/JOM.0b013e318157f0ba [DOI] [PubMed] [Google Scholar]
- 6.Shiri R, Kaila-Kangas L, Ahola K et al. . The relation of co-occurring musculoskeletal pain and depressive symptoms with work ability. J Occup Environ Med 2013;55:1281–5. 10.1097/JOM.0b013e3182a4ffc4 [DOI] [PubMed] [Google Scholar]
- 7.Dahm KT, Brurberg KG, Jamtvedt G et al. . Advice to rest in bed versus advice to stay active for acute low-back pain and sciatica. Cochrane Database Syst Rev 2010;(6):CD007612. [DOI] [PubMed] [Google Scholar]
- 8.Du Bois M, Donceel P. Guiding low back claimants to work: a randomized controlled trial. Spine 2012;37:1425–31. 10.1097/BRS.0b013e31824e4ada [DOI] [PubMed] [Google Scholar]
- 9.Matsudaira K, Hara N, Arisaka M et al. . Comparison of physician's advice for non-specific acute low back pain in Japanese workers: advice to rest versus advice to stay active. Ind Health 2011;49:203–8. 10.2486/indhealth.MS1193 [DOI] [PubMed] [Google Scholar]
- 10.Waddell G, Feder G, Lewis M. Systematic reviews of bed rest and advice to stay active for acute low back pain. Br J Gen Pract 1997;47:647–52. [PMC free article] [PubMed] [Google Scholar]
- 11.Rollin L, Gehanno JF. Research on return to work in European Union countries. Occup Med 2012;62:210–15. 10.1093/occmed/kqr207 [DOI] [PubMed] [Google Scholar]
- 12.Palmer KT, Harris EC, Linaker C et al. . Effectiveness of community- and workplace-based interventions to manage musculoskeletal-related sickness absence and job loss: a systematic review. Rheumatology 2012;51:230–42. 10.1093/rheumatology/ker086 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Franche RL, Cullen K, Clarke J et al. . Workplace-based return-to-work interventions: a systematic review of the quantitative literature. J Occup Rehabil 2005;15:607–31. 10.1007/s10926-005-8038-8 [DOI] [PubMed] [Google Scholar]
- 14.van Oostrom S, Boot C. Workplace interventions. In: Loisel P, Anema JR, eds. Handbook of work disability: prevention and management. New York: Springer, 2013:335–55. [Google Scholar]
- 15.Carroll C, Rick J, Pilgrim H et al. . Workplace involvement improves return to work rates among employees with back pain on long-term sick leave: a systematic review of the effectiveness and cost-effectiveness of interventions. Disabil Rehabil 2010;32:607–21. 10.3109/09638280903186301 [DOI] [PubMed] [Google Scholar]
- 16.Anema JR, Steenstra IA, Bongers PM et al. . Multidisciplinary rehabilitation for subacute low back pain: graded activity or workplace intervention or both? A randomized controlled trial. Spine 2007;32:291–8; discussion 299–300 10.1097/01.brs.0000253604.90039.ad [DOI] [PubMed] [Google Scholar]
- 17.Lambeek LC, van Mechelen W, Knol DL et al. . Randomised controlled trial of integrated care to reduce disability from chronic low back pain in working and private life. BMJ 2010;340:c1035 10.1136/bmj.c1035 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Loisel P, Abenhaim L, Durand P et al. . A population-based, randomized clinical trial on back pain management. Spine 1997;22:2911–18. 10.1097/00007632-199712150-00014 [DOI] [PubMed] [Google Scholar]
- 19.Costa-Black KM, Cheng AS, Li M et al. . The practical application of theory and research for preventing work disability: a new paradigm for occupational rehabilitation services in China? J Occup Rehabil 2011;21(Suppl 1):S15–27. 10.1007/s10926-011-9296-2 [DOI] [PubMed] [Google Scholar]
- 20.Lambeek LC, Bosmans JE, Van Royen BJ et al. . Effect of integrated care for sick listed patients with chronic low back pain: economic evaluation alongside a randomised controlled trial. BMJ 2010;341:c6414 10.1136/bmj.c6414 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Blank L, Peters J, Pickvance S et al. . A systematic review of the factors which predict return to work for people suffering episodes of poor mental health. J Occup Rehabil 2008;18:27–34. 10.1007/s10926-008-9121-8 [DOI] [PubMed] [Google Scholar]
- 22.Cornelius LR, van der Klink JJ, Groothoff JW et al. . Prognostic factors of long term disability due to mental disorders: a systematic review. J Occup Rehabil 2011;21:259–74. 10.1007/s10926-010-9261-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.de Vries G, Koeter MW, Nabitz U et al. . Return to work after sick leave due to depression; a conceptual analysis based on perspectives of patients, supervisors and occupational physicians. J Affect Disord 2012;136:1017–26. 10.1016/j.jad.2011.06.035 [DOI] [PubMed] [Google Scholar]
- 24.Furlan AD, Gnam WH, Carnide N et al. . Systematic review of intervention practices for depression in the workplace. J Occup Rehabil 2012;22:312–21. 10.1007/s10926-011-9340-2 [DOI] [PubMed] [Google Scholar]
- 25.Nieuwenhuijsen K, Faber B, Verbeek JH et al. . Interventions to improve return to work in depressed people. Cochrane Database Syst Rev 2014;12:CD006237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Andersen MF, Nielsen KM, Brinkmann S. Meta-synthesis of qualitative research on return to work among employees with common mental disorders. Scand J Work Environ Health 2012;38:93–104. 10.5271/sjweh.3257 [DOI] [PubMed] [Google Scholar]
- 27.van Duijn M, Eijkemans MJ, Koes BW et al. . The effects of timing on the cost-effectiveness of interventions for workers on sick leave due to low back pain. Occup Environ Med 2010;67:744–50. 10.1136/oem.2009.049874 [DOI] [PubMed] [Google Scholar]
- 28.Hoefsmit N, Houkes I, Nijhuis FJ. Intervention Characteristics that Facilitate Return to Work After Sickness Absence: A Systematic Literature Review. J Occup Rehabil 2012;22:462–77. 10.1007/s10926-012-9359-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Arroll B, Khin N, Kerse N. Screening for depression in primary care with two verbally asked questions: cross sectional study. BMJ 2003;327:1144–6. 10.1136/bmj.327.7424.1144 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Brown CA, Lilford RJ. The stepped wedge trial design: a systematic review. BMC Med Res Methodol 2006;6:54 10.1186/1471-2288-6-54 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Handley MA, Schillinger D, Shiboski S. Quasi-experimental designs in practice-based research settings: design and implementation considerations. J Am Board Fam Med 2011;24:589–96. 10.3122/jabfm.2011.05.110067 [DOI] [PubMed] [Google Scholar]
- 32.Mdege ND, Man MS, Taylor Nee Brown CA et al. . Systematic review of stepped wedge cluster randomized trials shows that design is particularly used to evaluate interventions during routine implementation. J Clin Epidemiol 2011;64:936–48. 10.1016/j.jclinepi.2010.12.003 [DOI] [PubMed] [Google Scholar]
- 33.WHO. International Classification of Diseases and Related Health Problems, 10th Revision (ICD-10) 2010. http://apps.who.int/classifications/icd10/browse/2010/en (accessed 24 Mar 2015).
- 34.Arokoski J, Alaranta H, Pohjolainen T et al. , eds. Fysiatria. Helsinki: Duodecim, 2009:543–5. [Google Scholar]
- 35.PHQ-9 Health Questionnaire (in Finnish). http://www.terveysportti.fi/dtk/ltk/koti?p_artikkeli=pgr00035&p_haku=PHQ-9 (accessed 24 Mar 2015).
- 36.Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 2001;16:606–13. 10.1046/j.1525-1497.2001.016009606.x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Ware JE Jr., Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 1992;30:473–83. 10.1097/00005650-199206000-00002 [DOI] [PubMed] [Google Scholar]
- 38.Cheung K, Oemar M, Oppe M et al. . EG-5D. User guide. Basic information on how to use EQ-5D. Version 2.0. EuroQol Group, 2009. http://www.euroqol.org/fileadmin/user_upload/Documenten/PDF/User_Guide_v2_March_2009.pdf (accessed 24 Mar 2015).
- 39.EuroQol G. EuroQol—a new facility for the measurement of health-related quality of life. Health policy 1990;16:199–208. 10.1016/0168-8510(90)90421-9 [DOI] [PubMed] [Google Scholar]
- 40.Ilmarinen J. The Work Ability Index (WAI). Occup Med 2007;57:160 10.1093/occmed/kqm008 [DOI] [Google Scholar]
- 41.Tuomi K, Ilmarinen J, Jahkola A et al. . Work ability index. 2nd edn. Helsinki: Finnish Institute of Occupational Health, 1998. [Google Scholar]
- 42.England G, Ruiz Quintanilla S, Maimer J. The meaning of working survey C 1995. http://users.ugent.be/~rclaes/MOW/surv_c_e.pdf (accessed 24 Mar 2015).
- 43.Perkiö-Mäkelä M, Hirvonen M. Työ ja terveys—haastattelututkimus 2012. Taulukkoraportti. (Work and Health Survey 2012. Table report. In Finnish) Helsinki: Finnish Institute of Occupational Health, 2013. [Google Scholar]
- 44.Viikari-Juntura E, Rauas S, Martikainen R et al. . Validity of self-reported physical work load in epidemiologic studies on musculoskeletal disorders. Scand J Work Environ Health 1996;22:251–9. 10.5271/sjweh.139 [DOI] [PubMed] [Google Scholar]
- 45.Washington State Dept Labor & Industries. Public Law: WAC 296-62-051, Ergonomics. Lifting and Handling Loads—Part 2. Assessing Ergonomic Hazards. http://work.alberta.ca/documents/WHS-PUB-BCL002.pdf (accessed 24 Mar 2015).
- 46.Elo A-L, Leppänen A, Lindström K et al. . Occupational stress questionnaire. User's instructions Helsinki: Finnish Institute of Occupational Health, 1992. [Google Scholar]
- 47.Lehto A-M, Sutela H. Työolojen kolme vuosikymmentä. Työolotutkimusten tuloksia 1977–2008. (Three decades of working conditions. Results of working conditions research from 1977 to 2008. In Finnish). Helsinki: Statistics Finland, 2008. http://tilastokeskus.fi/tup/julkaisut/tiedostot/isbn_978-952-467-930-5.pdf (accesseed 24 Mar 2015). [Google Scholar]
- 48.Health 2000 (http://www.terveys2000.fi/indexe.html). A Survey on health and functional capacity in Finland. Questionnaire 1. National Institute for Health and Welfare. http://www.terveys2000.fi/lomakkeet/en/t2002en.pdf (accessed 24 Mar 2015).
- 49.Taris T, Kalimo R, Schaufeli W. Inequity at work: its measurement and association with worker health. Work & Stress 2002;16:287–301. 10.1080/0267837021000054500 [DOI] [Google Scholar]
- 50.WHO. Global Database on Body Mass Index. An interactive Surveillance Tool for Monitoring Nutrition Transition. http://apps.who.int/bmi/index.jsp?introPage=intro_3.html (accessed 24 Mar 2015).
- 51.Health 2000 (http://www.terveys2000.fi/indexe.html). A Survey on health and functional capacity in Finland. Home interview. National Institute for Health and Welfare. http://www.terveys2000.fi/lomakkeet/en/t2001en.pdf (accessed 24 Mar 2015).
- 52.Jenkins CD, Stanton BA, Niemcryk SJ et al. . A scale for the estimation of sleep problems in clinical research. J Clin Epidemiol 1988;41:313–21. 10.1016/0895-4356(88)90138-2 [DOI] [PubMed] [Google Scholar]
- 53.Health 2000 (http://www.terveys2000.fi/indexe.html). A Survey on health and functional capacity in Finland. Questionnaire 3. National Institute for Health and Welfare. http://www.terveys2000.fi/lomakkeet/en/t2005en.pdf (accessed 24 Mar 2015).
- 54.Austin PC, Laupacis A. A tutorial on methods to estimating clinically and policy-meaningful measures of treatment effects in prospective observational studies: a review. Int J Biostat 2011;7:6 10.2202/1557-4679.1285 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Little RJ, Rubin DB. Causal effects in clinical and epidemiological studies via potential outcomes: concepts and analytical approaches. Annu Rev Public Health 2000;21:121–45. 10.1146/annurev.publhealth.21.1.121 [DOI] [PubMed] [Google Scholar]
- 56.Hogg-Johnson S, MacEachen E. Methodological issues in work disability prevention research. In: Loisel P, Anema JR, eds. Handbook of work disability: prevention and management. New York: Springer, 2013:125–46. [Google Scholar]
- 57.Kristensen TS. Intervention studies in occupational epidemiology. Occup Environ Med 2005;62:205–10. 10.1136/oem.2004.016097 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Viikari-Juntura E, Kausto J, Shiri R et al. . Return to work after early part-time sick leave due to musculoskeletal disorders: a randomized controlled trial. Scand J Work Environ Health 2012;38:134–43. 10.5271/sjweh.3258 [DOI] [PubMed] [Google Scholar]
- 59.Shiri R, Kausto J, Martimo KP et al. . Health-related effects of early part-time sick leave due to musculoskeletal disorders: a randomized controlled trial. Scand J Work Environ Health 2013;39:37–45. 10.5271/sjweh.3301 [DOI] [PubMed] [Google Scholar]