Abstract
Objectives
To present the chronological development of the different positions described for percutaneous nephrolithotomy (PCNL), in an attempt to identify the reasons for their development and to highlight their specific advantages and disadvantages.
Methods
Previous reports were identified by a non-systematic search of Medline and Scopus.
Results
The classic prone position for PCNL was first described in 1976. The technique was gradually standardised and PCNL with the patient prone became the generally accepted standard approach. In the next 35 years many other positions were described, with the patient placed prone, lateral or supine in various modifications. Modifications of the classic prone position in the early 1990s aimed to provide the option of a simultaneous retrograde approach during the procedure. As PCNL became more popular the lateral position was first described in 1994, to allow the application of PCNL to patients who were unable to tolerate being prone because of their body habitus. The supine position for percutaneous access was originally described even before 1990, but become more popular after 2007 when the Galdakao modification was reported. Several other modifications of the supine position have been described, with the latest being the flank-free modified supine position, which allows the best exposure of the flank among the supine positions. Each position has its specific advantages and disadvantages.
Conclusion
Urologists who perform PCNL should be familiar with the differences in the positions and be able to use the method appropriate to each case.
Abbreviation: PCNL, percutaneous nephrolithotomy
Keywords: Perctutaneous nephrolithotomy, PCNL, Positions, Prone, Supine, Lateral, Flank, Endoscopic intrarenal surgery
Introduction
Percutaneous nephrolithotomy (PCNL) is used widely and has almost completely replaced open surgery for the removal of large and complex renal calculi. Since its first description by Fernstrom and Johansson [1], PCNL has traditionally been done with the patient prone, combining a high success rate and acceptable morbidity.
As PCNL was used more frequently it became evident that the prone position was not optimal for all patients, particularly the morbidly obese or those with respiratory compromise. This insight, and the demand for easier and more comfortable access to the entire urinary tract to combine retrograde and antegrade endoscopic surgery, led to the introduction of alternative patient positions for PCNL.
Some of these were not widely accepted in the urological community but all of them had a significant role in the dynamic process of further refinement. The purpose of the present review is to present the chronological development of the different positions (Table 1) [1–11] that have been described for PCNL, to investigate the reasons for their development, and to highlight their specific advantages and disadvantages (Table 2).
Table 1.
A timeline of positions for PCNL.
| Year | Ref | Position | Type | Comment |
|---|---|---|---|---|
| 1976 | [1] | Classic prone | Prone | First description of percutaneous stone extraction |
| 1988 | [8] | Reverse lithotomy | Prone | First simultaneous antegrade and retrograde access |
| 1990 | [9] | Original supine | Supine | First series of PCNL while supine. Initial case reports 2 years before |
| 1990 | [9] | Modified supine for simultaneous PCNL and ureteroscopy | Supine | |
| 1991 | [2] | Split-leg prone | Prone | |
| 1993 | [3] | Flank roll position | Supine | For patients having preoperative percutaneous access |
| 1994 | [4] | Lateral decubitus | Flank | First PCNL in the lateral position |
| 2007 | [10] | Galdakao-modified Valdivia | Supine | Renewed the interest for supine position |
| 2007 | [5] | Crossed-leg supine | Supine | |
| 2008 | [7] | Barts technique | Flank | Very good simultaneous ante- and retrograde access |
| 2008 | [11] | Complete supine | Supine | No support is placed under the flank |
| 2009 | [6] | Prone-flexed | Prone | |
| 2012 | In press | Barts flank-free modified | Supine | The best exposure of the flank among the supine positions |
Table 2.
Advantages and disadvantages of positions for PCNL.
| Position | Advantages | Disadvantages |
|---|---|---|
| Prone | ||
| Classic prone | Excellent exposure of lumbar area | Patient repositioning during the procedure |
| Classic prone with supporting equipment | Easier access to upper pole | Hard to manage cardio-respiratory emergencies |
| Kidney close to puncture site and less mobile | Respiratory/cardiovascular function compromised | |
| Reverse lithotomy | Depended renal pelvis and thus increased pressure (better visibility and room for movement) | Increased risk of injuries from pressure (less if special mattress is used) (less if supporting equipment is used) |
| Split leg prone | ||
| Prone-flexed | Theoretical risk of ocular complications | |
| Surgeon standing/non-ergonomic position | ||
| Theoretically greater exposure to radiation | ||
| Retrograde access not possible in classic prone (feasible in ‘split leg’ and ‘reverse lithotomy’) | ||
| Lateral | ||
| Lateral decubitus and lateral flexed | Can be used in patients with severe obesity, kyphoscoliosis | Patient repositioning is required (easier than in prone position) |
| ‘Barts technique’ | Less impact on respiratory/cardiac function | Difficult access to kidney with fluoroscopy |
| Good exposure of flank | ||
| Option for simultaneous retrograde access | ||
| General anaesthesia can be avoided | ||
| Supine | ||
| Original Valdivia | Patient is positioned and draped once | Reduced exposure of flank area (less in the ‘Barts flank-free’ position) |
| Modified Valdivia | Comfortable position for patient | Access to posterior calyces not always possible |
| Flank roll | Surgeon in ergonomic position | Kidney sometimes more mobile (difficult puncture) |
| Crossed leg | Theoretically less exposure to radiation | Instrument movements can be restricted. (less in the ‘Barts flank-free’ position) |
| Galdakao | Excellent control of airway by anaesthetists | Collapsed collecting system because of reduced pressure makes nephroscopy more demanding |
| Complete supine | Allows easier retrograde access | |
| Barts flank-free | Dependent access (spontaneous evacuation of fragments, less fluid absorption) | |
| General anaesthesia can be avoided | ||
Evidence acquisition
Using a non-systematic search of Medline and Scopus from 1976 to 2011, previous relevant reports were identified using the keywords ‘percutaneous nephrolithotomy’, ‘PCNL’, ‘position’, ‘supine’ and ‘prone’. Further reports were acquired from the references of the retrieved articles, and standard textbooks were consulted. Only papers written in English were included.
Evidence synthesis: positions for PCNL
Prone
The classic prone position (Fig. 1). When PCNL was initially described in 1976 the prone position was chosen because it was believed that this would be the safest way to avoid damage to the colon and visceral organs. The technique was standardised over the following years as a two-stage procedure. The first part is with the patient supine, to give anaesthesia and gain retrograde access to the upper urinary tract. Then the patient is repositioned prone for the main part of the procedure. Rolled supports are placed under the thorax and the upper abdomen or on both sides, extending from shoulder to hip, to facilitate ventilation [12]. Padding is placed under all pressure points (knees, feet, forehead, eyes, elbows, fingers) and the shoulders, and the elbows are carefully positioned to prevent brachial plexus injury [13]. The percutaneous tract to the kidney is established under fluoroscopy or ultrasonographic guidance, and the stone is removed.
Figure 1.
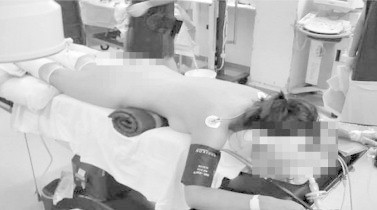
The prone position.
The main advantage of the prone position is that it exposes completely the lumbar area. This gives the surgeon ample room to place the puncture, allows several accesses/tracts, and provides enough space for manipulation with the instruments. Upper-pole puncture is facilitated in the prone position because of the posteromedial location of the upper pole, which is closer to the posterior abdominal wall [6]. However, PCNL with the patient prone has several disadvantages. First, the patient must be repositioned after the first stage. This increases the operating time, and could cause injury to the patient and jeopardise the airway access. It is very difficult or almost impossible for the anaesthetist to manage an eventual cardio-respiratory emergency. Lying on the abdomen creates further anaesthesiological difficulties by reducing lung compliance as a result of the abdominal compression, and by reducing cardiac output [7]. The patient is bedded uncomfortably with the risk of creating pressure lesions. The prone position is generally associated with an increased rate of ophthalmological complications, as seen mostly from spinal operations. Direct compression might cause injury to the orbit and corneal abrasions. Also, intra-ocular pressure is raised during the operation and is suspected to lead to the rare complication of postoperative visual loss due to ischaemic oculopathy [14,15]. For patients with ankylosing spondylitis or other spinal or lower limb deformities, the prone position might not be possible. Finally, there is a theoretically greater risk of radiation exposure for the surgeon when the patient is supine, because the surgeon stands close to the patient, working with the instruments in perpendicular direction [6].
Better patient positioning in the classic prone position (Fig. 2)
Figure 2.
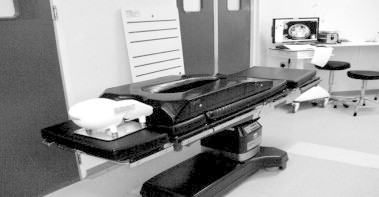
The Montreal mattress, with the Proneview helmet.
Various supporting equipments have been developed to minimise the risk of pressure injury, reduce the risk of position-related complications, and improve the ventilation and circulation of the patient. For example, the rolled supports can be replaced by the Cloward surgical saddle (Cloward Instruments Corp., Honolulu, Hawaii) [12] or the Montreal mattress (Teasdale Hospital Equipment, Manchester, UK) [16], embedding the patient in a more comfortable, slightly flexed posture with less pressure on the abdomen. To better position the head, the Proneview protective helmet system (Dupaco, Oceanside, CA, USA) was developed, which protects the critical cephalic pressure points and the airways [7].
The reverse lithotomy position
To allow simultaneous retrograde access to the upper urinary tract during PCNL, a modification of the classic prone position became necessary. In 1988, Lehman and Bagley [8] reported successful results with this combined approach in three female patients. According to the initial description, the patient is placed prone with the legs abducted at the hips, and the thighs and knees fixed in plastic cradles specifically modified for this purpose. The caudal end of the operating table is lowered as far as possible. The operator approaching from the caudal end of the table has access to the urethra, bladder and ureter with flexible instruments.
The split-leg prone position (Fig. 3)
Figure 3.
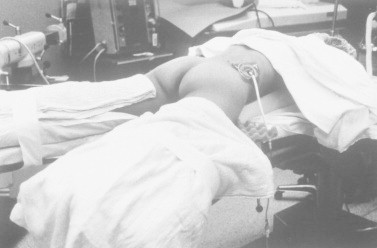
The split-leg position. (Taken from [3] with permission from the author, courtesy of Professor Michael Grasso).
The same group of authors who described the reverse lithotomy position 3 years later reported the split-leg prone position that allowed easier simultaneous percutaneous and transurethral access both in female and male patients [2]. The patient is anaesthetised while supine and then turned prone on a standard endourological table with split-leg adapters. The patient’s legs are appropriately padded, secured independently and solely abducted at the hips without being flexed. The genitalia are positioned at the bottom of the operating table, making room for retrograde access. The flank and the genital area are separately prepared and draped. Using flexible instruments, the bladder and upper urinary tract are accessed, although this can be challenging. The authors report that many endourological procedures, including intracorporeal lithotripsy, can be performed in this position [2,3].
The prone-flexed position (Fig. 4)
Figure 4.
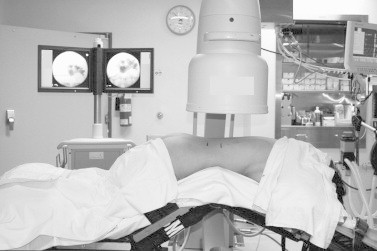
The prone-flexed position. (Taken from [6] with permission from the author, courtesy of Dr. R. John D’A. Honey).
Recently a modification of the prone position was described which incorporates a flexed position of the patient during the procedure [6]. After the patient is turned to prone the table is flexed 30–40° to open the space between the 12th rib and the posterior iliac crest. This flexion prevents the exaggeration of the anterior lordosis that occurs in the classic prone position. More working space is created, potential interference from the buttock with the nephroscope during rigid nephroscopy through the lower pole is minimised, and the kidneys are displaced inferiorly in the retroperitoneum. As a result the puncture can be made more caudally. However, this position impairs even more the patient’s respiration and circulation. Airway pressures are increased, the cardiac index is decreased and the inferior vena cava can be transiently obstructed.
Lateral positions
The lateral decubitus and lateral flexed position
Some patients are unable to tolerate anaesthesia while prone because of their body habitus. Kerbl et al. [4] in 1994 first performed PCNL in a morbidly obese patient placed in the lateral position. Later other authors reported good results using this technique in obese, kyphotic and high-risk patients [17–19]. Urologists are familiar with this position, as it is used in open and laparoscopic renal surgery.
Initially the patient is anaesthetised while supine, when the retrograde contrast studies are conducted. The patient is then turned into the lateral position with the legs slightly bent, lying on the unaffected side and exposing the flank through which the access is made. A wedge support can be placed under the patient’s torso. Both arms are supported in separate adapters and flexed slightly at the elbow. A modification of the pure lateral position, the lateral flexed position, has the additional advantage of significantly increasing the operating field. The operating table is flexed, which widens the space between the 12th rib and the iliac crest, flattening the folds of adipose tissue and facilitating percutaneous access [13].
The advantage of the lateral position is that they can be used in patients who could not tolerate being prone. Especially helpful for the morbidly obese patients is that in the lateral position the pendulous abdomen is displaced sideways, either on the operating table or on an additional support, facilitating respiration and general anaesthesia. Furthermore, as the patient is not lying prone, the procedure can be carried out safely even under regional anaesthesia, thus avoiding the risks of general anaesthesia, and allowing the patient to communicate with the anaesthetist and observe the procedure [17].
The main disadvantage in this position is the unusual fluoroscopic view of the kidney, which can also be obscured by the underlying spine. Maintaining the correct orientation and accurately puncturing the selected calyx is difficult, and can result in increased exposure to radiation of the surgical team. Using the ‘bull’s-eye’ puncture technique might not be possible, as the metal side-rails of the table interfere with the fluoroscopic image. Alternatively, the ‘triangulation’ technique [13] or ultrasonographic guidance can be used, but this requires additional expertise and equipment [17,19]. The patient must be repositioned during the procedure, although this is easier and poses fewer risks than repositioning towards the prone position.
The modified lateral position for simultaneous antegrade and retrograde access–the ‘Barts technique’ (Fig. 5)
Figure 5.
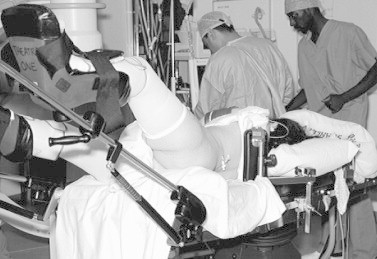
‘The Barts technique’.
This modified hybrid position was described to combine the advantages of the lateral position with the option of easier retrograde access to the upper urinary tract [20,21]. The patient is placed in the lithotomy position with the ipsilateral hemi-pelvis tilted by 45°, supported by a foam wedge. The torso is twisted to the contralateral side, with the shoulders perpendicular to the operating table. The ipsilateral lower limb is slightly flexed in a ventral direction and follows the lateral rotation of the trunk, while the contralateral lower limb remains fully abducted. In this position the flank is sufficiently exposed, providing a wide choice of puncture sites and a wide angle for handling the antegrade instruments. Percutaneous access is made close to the posterior axillary line, and the direction of the puncture needle is within the horizontal plane towards the desired calyx [21].
Simultaneous ante- and retrograde access allows the treatment of complex unilateral upper urinary tract pathology [22]. Another advantage is that repositioning of the patient is minimal, thus saving operative time and reducing the risk of injuring the patient. However, this position cannot be used for every patient as it requires musculoskeletal mobility and flexibility of the spine. Percutaneous access guided by fluoroscopy can be challenging. A similar position with the legs bent in a lower position was described recently [23].
Supine positions
The original Valdivia supine position (Fig. 6)
Figure 6.
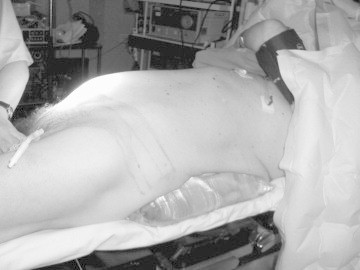
The ‘Valdivia’ supine position (courtesy of Professor José Gabriel Valdivia Uría).
In 1987–88, Valdivia-Uria et al. [9] reported a safe percutaneous access to the kidney with the patient supine and 10 years later they reported the in vivo experience [24]. Several other authors have also reported large series of patients treated in the same position [25–28]. As the abdominal wall is punctured more laterally, away from the lumbar muscles, movements of the endoscopic instruments are less restricted. The direction of the tract preserves a low pressure in the renal pelvis, and thereby reduces the risk of fluid absorption and allows even spontaneous clearance/washout of fragments. According to anatomical CT studies, the risk of colon perforation might even be less than in the prone position, as the bowel can float free in the uncompressed abdomen and is not pressed towards or behind the kidney [9,29,30].
The main drawback of the supine position is that the flank is not fully exposed, which makes access to the posterior-medially lying upper pole more difficult and provides less availability for multiple accesses. The operating table and the patient’s hips might also restrict instrument manipulation. The absence of abdominal compression leaves the kidney more mobile, which can make puncture and dilatation of the tract more challenging [25]. Some calyces are dependant and collect fragments during the disintegration of the stone. Finally, the low intrarenal pressure leaves the collecting system less expanded and therefore nephroscopy and manipulations can be more difficult.
The modified Valdivia position for simultaneous PCNL and ureteroscopy (Fig. 7)
Figure 7.
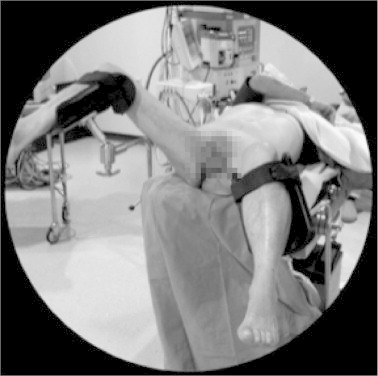
The modified ‘Valdivia’ position (courtesy of Professor José Gabriel Valdivia Uría).
This modification was described by Valdivia et al. [9] to allow simultaneous rigid ureteroscopy during PCNL. The difference from the original supine position is that the legs are flexed in supports, with the ipsilateral leg more elevated and the contralateral more descended, to facilitate the use of a rigid ureteroscope. Valdivia [13] prefers the classic supine position if a flexible ureteroscope is to be used, and proposes this modification only for rigid ureteroscope.
The modified flank roll position
At present, many departments perform percutaneous surgery after the kidney has been punctured under local anaesthesia and sedation in the radiology department. During the first years of PCNL this was the routine [31]. In 1993 Grasso et al. [3] described the modified flank roll position for patients who already had a nephrostomy in situ. These authors suggested that this position is suitable when the preoperative assessment showed that the procedure might be completed retrogradely, and a percutaneous tract would only be a complementary access for flexible instruments if needed. The patient is placed in the standard dorsal lithotomy position, having the flank with the percutaneous nephrostomy tilted by 45° and padded to allow access to the nephrostomy tube. The upper extremity lies across the thorax. Both the nephrostomy site and the genitalia are prepared and draped. The limited exposure of the flank might not allow a primary puncture and manipulations with rigid nephroscopes.
The crossed-leg supine position
This variation of the original Valdivia position was described in 2007 and consists of crossing the ipsilateral leg over the contralateral [5]. A 30° inclination of the torso is achieved by placing a cushion below the ipsilateral flank. The arms are placed similarly to those in the original Valdivia position.
According to these authors, crossing the legs increases the distance from the lower rib to the iliac crest, and facilitates calyceal puncture and nephrostomy tract dilatation. Also, the skin and muscles of the flank are stretched, which further helps to establish percutaneous access. The authors also suggested that this variation enables a more comfortable position for the assistant next to the surgeon.
The Galdakao-modified Valdivia position (Fig. 8)
Figure 8.
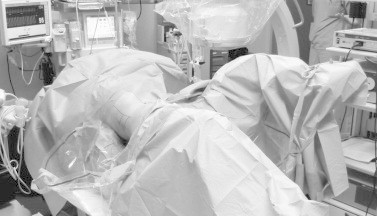
The Galdakao-modified Valdivia position (courtesy of Dr. Cesare Marco Scoffone).
This position was described by Ibarluzea et al. [10] in 2007 and renewed the attention of the urological community on supine PCNL. Other authors confirmed that the operation in this position is a safe, practical and versatile procedure, with high success rates and has important advantages over the prone position [32–34].
The main characteristic is a slight lateralisation of the Valdivia supine position, with the contralateral leg flexed. The patient is placed in an intermediate supine-lateral position with a 3-L bag placed to raise the flank. The ipsilateral leg is extended and the contralateral leg is abducted and flexed, achieving a modified lithotomy position.
The Galdakao-modified Valdivia position combines the surgical and anaesthesiological advantages of the original Valdivia position with the advantage of simultaneous retrograde access to the kidney. The patient needs to be draped only once and repositioning is not necessary. There is more space for manipulating the instruments than in the original supine position. The drawbacks of this modification do not differ from those known for the original supine position [28].
The complete supine position (Fig. 9) [35]
Figure 9.
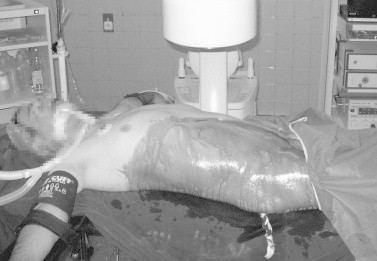
The complete supine position. (Taken from [35] with permission from the author, courtesy of Dr. Siavash Falahatkar, Professor of Urology).
PCNL in a complete supine position with no flank support was described by Falahatkar et al. [11] who reported this technique to be safe and feasible in all patients [36]. The patient is placed supine at the edge of the table, with the legs extended and the arms stretched and abducted in supports.
The advantages are similar to those of other supine positions. Also, the absence of flank support prevents the cephalad sliding of the kidney, making upper-pole puncture more feasible. To further facilitate this the authors proposed using lung inflation to lower the kidneys [37]. Finally, the fluoroscopic view of the kidney is not overlapped by the vertebrae, as can occur in semi-supine positions [11].
The flank-free supine position
In 2007 Cormio et al. [38] described a novel position for placing a nephrostomy. The patient is put in a more oblique position with two towels under the shoulder and hip, leaving the flank exposed. The ipsilateral arm is placed over the chest and the contralateral arm is abducted. The authors did not describe percutaneous surgery in this position but they showed the benefit of better exposure of the flank by removing the supporting saline bag from the loin.
The Barts flank-free modified supine position (Fig. 10)
Figure 10.
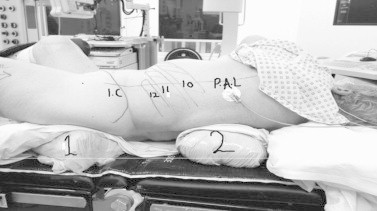
The Barts flank-free supine position.
For the last 2 years we have been using this new modification of the supine position that better exposes the flank, as described above, but also incorporates a lithotomy position, and is termed the ‘Barts flank-free modified supine position’ [39,40]. The patient is supine with a 15° tilt of the ipsilateral flank made by using a saline bag under the rib cage and a gel pad under the pelvis. The ipsilateral arm lies across the chest. The legs are placed in the lithotomy position with the ipsilateral leg relatively extended and the contralateral leg abducted and slightly elevated.
The main advantage is that it exposes the flank better than with all other supine positions for PCNL, giving optimal space for renal access and manipulation, as no support is placed immediately under the working area. The patient is comfortable with no stress in the spine, as the torso is minimally rotated. A fluoroscopic view of the kidney is easily achieved with minimal rotation of the C-arm, while better radiological safety is ensured as the surgeon’s hands are less exposed. The kidney lies in a neutral position and is less mobile, enabling an easier access and dilatation of the tract. Ideal conditions for simultaneous antegrade and retrograde access are offered. The nephrostomy tract is almost horizontal, which enables a better washout of fragments and a lower intrarenal pressure.
Comment
Although, the prone position is traditionally considered the classic format for PCNL, over the years and as PCNL became more widespread the limitations of this approach were recognised. Anaesthetic concerns, especially in the morbidly obese or other high-risk patients, and the need to reposition the patient during the procedure, were the reasons that initially provoked urologists to explore alternative positions. At the same time the significant improvements in flexible ureteroscopy [41] and intracorporeal lithotripsy [42] increased the efficacy of retrograde intrarenal surgery. As a result there was increased interest in combining simultaneous antegrade and retrograde endoscopic access to the urinary tract, and this was another reason for exploring new positions for PCNL.
In an effort to address some of the drawbacks of having patients placed on their abdomen and padded only by rolled supports, various equipment was introduced that made this position more comfortable, improved ventilation and circulation, and reduced the risk of pressure injury [7,12,13]. An additional benefit of these devices is that the hips of the patient are slightly flexed, increasing the working space on the flank.
To achieve better flank exposure the prone-flexed position was described, using the flex option of the operating table. Here the working space is increased even further as the ribs are rotated cephalad and at the same time the kidneys move caudally, allowing the puncture to be made lower on the torso, thereby reducing the risk of pleural complications. It was estimated that 45% fewer supra-11th rib punctures would be necessary to access the most superior calyx [6].
With the increasing incidence of obese patients and the evidence that stone disease is linked to the metabolic syndrome [43], it was important that solutions for PCNL in this group of patients were developed. Morbidly obese patients have a constantly elevated intra-abdominal pressure which restricts the respiratory reservoir. This is aggravated under general anaesthesia with muscle paralysis and is further worsened if the patient is placed prone. Haemodynamic compromise also occurs when prone, by compression of the inferior vena cava and iliac veins, leading to a decrease in venous return and in cardiac pre-load [17]. To overcome these problems the lateral position was introduced in PCNL. The ‘Barts technique’ combines the advantages of the lateral position with the opportunity for complete endourological treatment in one step [21]. Lateral positions have clear benefits and indications, but are mostly used in specialised centres for selected patients, mainly because access to the kidney is technically more difficult.
Professor Valdivia-Uria described the supine position 25 years ago, and its many advantages, as described above. However, there was an astonishingly small acceptance by the urological community until Ibarlueza et al. [10] described the Galdakao-modified Valdivia supine position in 2007, which allowed comfortable simultaneous antegrade and retrograde access to the whole urinary tract, as well as the possibility of combining laparoscopy and endourology (laparo-endoscopic techniques). The ‘Barts flank-free modified supine position’ is a further refinement of the supine position, as it allows easier manipulation from the percutaneous access. Probably the greatest concern that prevented (or at least delayed) the wide acceptance of supine positions was the risk of colon perforation and visceral organ injury. However, the reported rate for colon perforation in the prone and supine positions is similar (≈0.5%) [44]. Contrary to what was assumed about the anatomical position of the organs when prone, CT studies showed that the risk of colon perforation should actually be less when the patient is supine [44,45]. Both reports showed that the two positions have a similar rate of complications, similar stone-free rate and mean days of hospital stay, while supine positioning significantly decreases the operative time.
Conclusion
There has been a significant development in positions for PCNL since the first description. A multitude of variations has aimed to overcome the limitations inherent in the classical prone and initial supine positions. Urologists who perform PCNL should be familiar with the differences in the positions and be able to use the method appropriate for each patient.
Conflicts of interest
None disclosed.
Source of funding
None disclosed.
Acknowledgements
We acknowledge the following people, for their kind offer of images for this article: Mr. Junaid Masood, London, UK. Professor Michael Grasso, New York, USA. Professor Demetrius Bagley, Philadelphia, USA. Dr. R. John D’A Honey, Toronto, Canada. Professor José Gabriel Valdivia Uría, Zaragoza, Spain. Dr. Cesare Marco Scoffone, Torino, Italy. Professor Siavash Falahatkar, Rasht, Iran.
Footnotes
Peer review under responsibility of Arab Association of Urology.
References
- 1.Fernstrom I., Johansson B. Percutaneous pyelolithotomy. A new extraction technique. Scand J Urol Nephrol. 1976;10:257–259. doi: 10.1080/21681805.1976.11882084. [DOI] [PubMed] [Google Scholar]
- 2.Nord R.C.-G.A., Bagley D.H. Prone split-leg position for simultaneous retrograde ureteroscopic and percutaneous nephroscopic procedures. J Endourol. 1991;5:13–16. [Google Scholar]
- 3.Grasso M., Nord R., Bagley D.H. Prone split-leg and flank roll positioning: simultaneous antegrade and retrograde access to the upper urinary tract. J Endourol. 1993;7:307–310. doi: 10.1089/end.1993.7.307. [DOI] [PubMed] [Google Scholar]
- 4.Kerbl K., Clayman R.V., Chandhoke P.S., Urban D.A., De Leo B.C., Carbone J.M. Percutaneous stone removal with the patient in a flank position. J Urol. 1994;151:686–688. doi: 10.1016/s0022-5347(17)35048-6. [DOI] [PubMed] [Google Scholar]
- 5.Neto E.A., Mitre A.I., Gomes C.M., Arap M.A., Srougi M. Percutaneous nephrolithotripsy with the patient in a modified supine position. J Urol. 2007;178:165–168. doi: 10.1016/j.juro.2007.03.056. [DOI] [PubMed] [Google Scholar]
- 6.Ray A.A., Chung D.G., Honey R.J. Percutaneous nephrolithotomy in the prone and prone-flexed positions: anatomic considerations. J Endourol. 2009;23:1607–1614. doi: 10.1089/end.2009.0294. [DOI] [PubMed] [Google Scholar]
- 7.Papatsoris A., Masood J., El-Husseiny T., Maan Z., Saunders P., Buchholz N.P. Improving patient positioning to reduce complications in prone percutaneous nephrolithotomy. J Endourol. 2009;23:831–832. doi: 10.1089/end.2008.0611. [DOI] [PubMed] [Google Scholar]
- 8.Lehman T., Bagley D.H. Reverse lithotomy. Modified prone position for simultaneous nephroscopic and ureteroscopic procedures in women. Urology. 1988;32:529–531. doi: 10.1016/s0090-4295(98)90035-8. [DOI] [PubMed] [Google Scholar]
- 9.Valdivia J.G., Valer J., Villarroya S., Lopez J., Bayo A., Lanchares E. Why is percutaneous nephroscopy still performed with the patient prone? J Endourol. 1990;4:265–268. [Google Scholar]
- 10.Ibarluzea G., Scoffone C.M., Cracco C.M., Poggio M., Porpiglia F., Terrone C. Supine Valdivia and modified lithotomy position for simultaneous anterograde and retrograde endourological access. BJU Int. 2007;100:233–236. doi: 10.1111/j.1464-410X.2007.06960.x. [DOI] [PubMed] [Google Scholar]
- 11.Falahatkar S., Moghaddam A.A., Salehi M., Nikpour S., Esmaili F., Khaki N. Complete supine percutaneous nephrolithotripsy comparison with the prone standard technique. J Endourol. 2008;22:2513–2517. doi: 10.1089/end.2008.0463. [DOI] [PubMed] [Google Scholar]
- 12.Turner C.D., Anderson J., Gerber G.S. Improved patient positioning for percutaneous nephroscopic procedures using a surgical saddle. J Urol. 2000;163:199–200. [PubMed] [Google Scholar]
- 13.Smith A.D. 3rd ed. Wiley Chichester; West Sussex: 2012. Smith’s Textbook of Endourology. [Google Scholar]
- 14.Cheng M.A., Todorov A., Tempelhoff R., McHugh T., Crowder C.M., Lauryssen C. The effect of prone positioning on intraocular pressure in anesthetized patients. Anesthesiology. 2001;95:1351–1355. doi: 10.1097/00000542-200112000-00012. [DOI] [PubMed] [Google Scholar]
- 15.Hunt K., Bajekal R., Calder I., Meacher R., Eliahoo J., Acheson J.F. Changes in intraocular pressure in anesthetized prone patients. J Neurosurg Anesthesiol. 2004;16:287–290. doi: 10.1097/00008506-200410000-00005. [DOI] [PubMed] [Google Scholar]
- 16.Addla S.K., Rajpal S., Sutcliffe N., Adeyoju A. A simple aid to improve patient positioning during percutaneous nephrolithotomy. Ann R Coll Surg Engl. 2008;90:433–434. doi: 10.1308/003588408X301244k. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.El-Husseiny T., Moraitis K., Maan Z., Papatsoris A., Saunders P., Golden B. Percutaneous endourologic procedures in high-risk patients in the lateral decubitus position under regional anesthesia. J Endourol. 2009;23:1603–1606. doi: 10.1089/end.2009.1525. [DOI] [PubMed] [Google Scholar]
- 18.Gofrit O.N., Shapiro A., Donchin Y., Bloom A.I., Shenfeld O.Z., Landau E.H. Lateral decubitus position for percutaneous nephrolithotripsy in the morbidly obese or kyphotic patient. J Endourol. 2002;16:383–386. doi: 10.1089/089277902760261437. [DOI] [PubMed] [Google Scholar]
- 19.Karami H., Arbab A.H., Rezaei A., Mohammadhoseini M., Rezaei I. Percutaneous nephrolithotomy with ultrasonography-guided renal access in the lateral decubitus flank position. J Endourol. 2009;23:33–35. doi: 10.1089/end.2008.0433. [DOI] [PubMed] [Google Scholar]
- 20.Moraitis K., Philippou P., El-Husseiny T., Wazait H., Masood J., Buchholz N. Simultaneous antegrade/retrograde upper urinary tract access: Bart’s modified lateral position for complex upper tract endourologic pathologic features. Urology. 2012;79:287–292. doi: 10.1016/j.urology.2011.08.023. [DOI] [PubMed] [Google Scholar]
- 21.Papatsoris A.G., Zaman F., Panah A., Masood J., El-Husseiny T., Buchholz N. Simultaneous anterograde and retrograde endourologic access: ‘the Barts technique’. J Endourol. 2008;22:2665–2666. doi: 10.1089/end.2008.0283. [DOI] [PubMed] [Google Scholar]
- 22.Papatsoris A.G., Masood J., Saunders P. Supine valdivia and modified lithotomy position for simultaneous anterograde and retrograde endourological access. BJU Int. 2007;100:1192. doi: 10.1111/j.1464-410X.2007.07248_3.x. [DOI] [PubMed] [Google Scholar]
- 23.Lezrek M., Ammani A., Bazine K., Assebane M., Kasmaoui el H., Qarro A. The split-leg modified lateral position for percutaneous renal surgery and optimal retrograde access to the upper urinary tract. Urology. 2011;78:217–220. doi: 10.1016/j.urology.2011.03.012. [DOI] [PubMed] [Google Scholar]
- 24.Valdivia Uria J.G., Valle Gerhold J., Lopez Lopez J.A., Villarroya Rodriguez S., Ambroj Navarro C., Ramirez Fabian M. Technique and complications of percutaneous nephroscopy: experience with 557 patients in the supine position. J Urol. 1998;160:1975–1978. doi: 10.1016/s0022-5347(01)62217-1. [DOI] [PubMed] [Google Scholar]
- 25.Rana A.M., Bhojwani J.P., Junejo N.N., Das Bhagia S. Tubeless PCNL with patient in supine position: procedure for all seasons?–with comprehensive technique. Urology. 2008;71:581–585. doi: 10.1016/j.urology.2007.10.059. [DOI] [PubMed] [Google Scholar]
- 26.Steele D., Marshall V. Percutaneous nephrolithotomy in the supine position: a neglected approach? J Endourol. 2007;21:1433–1437. doi: 10.1089/end.2006.0375. [DOI] [PubMed] [Google Scholar]
- 27.Shoma A.M., Eraky I., El-Kenawy M.R., El-Kappany H.A. Percutaneous nephrolithotomy in the supine position. Technical aspects and functional outcome compared with the prone technique. Urology. 2002;60:388–392. doi: 10.1016/s0090-4295(02)01738-7. [DOI] [PubMed] [Google Scholar]
- 28.Ng M.T., Sun W.H., Cheng C.W., Chan E.S. Supine position is safe and effective for percutaneous nephrolithotomy. J Endourol. 2004;18:469–474. doi: 10.1089/0892779041271670. [DOI] [PubMed] [Google Scholar]
- 29.Hopper K.D., Sherman J.L., Luethke J.M., Ghaed N. The retrorenal colon in the supine and prone patient. Radiology. 1987;162:443–446. doi: 10.1148/radiology.162.2.3797658. [DOI] [PubMed] [Google Scholar]
- 30.Tuttle D.N., Yeh B.M., Meng M.V., Breiman R.S., Stoller M.L., Coakley F.V. Risk of injury to adjacent organs with lower-pole fluoroscopically guided percutaneous nephrostomy: evaluation with prone, supine, and multiplanar reformatted CT. J Vasc Interv Radiol. 2005;16:1489–1492. doi: 10.1097/01.RVI.0000175331.93499.44. [DOI] [PubMed] [Google Scholar]
- 31.Autorino R., Giannarini G. Prone or supine: is this the question? Eur Urol. 2008;54:1216–1218. doi: 10.1016/j.eururo.2008.08.069. [DOI] [PubMed] [Google Scholar]
- 32.Hoznek A., Rode J., Ouzaid I., Faraj B., Kimuli M., de la Taille A. Modified supine percutaneous nephrolithotomy for large kidney and ureteral stones: technique and results. Eur Urol. 2012;61:164–170. doi: 10.1016/j.eururo.2011.04.031. [DOI] [PubMed] [Google Scholar]
- 33.Daels F., Gonzalez M.S., Freire F.G., Jurado A., Damia O. Percutaneous lithotripsy in Valdivia–Galdakao decubitus position: our experience. J Endourol. 2009;23:1615–1620. doi: 10.1089/end.2009.1526. [DOI] [PubMed] [Google Scholar]
- 34.Scoffone C.M., Cracco C.M., Cossu M., Grande S., Poggio M., Scarpa R.M. Endoscopic combined intrarenal surgery in Galdakao-modified supine Valdivia position: a new standard for percutaneous nephrolithotomy? Eur Urol. 2008;54:1393–1403. doi: 10.1016/j.eururo.2008.07.073. [DOI] [PubMed] [Google Scholar]
- 35.Falahatkar S., Asli M.M., Emadi S.A., Enshaei A., Pourhadi H., Allahkhah A. Complete supine percutaneous nephrolithotomy (csPCNL) in patients with and without a history of stone surgery: safety and effectiveness of csPCNL. Urol Res. 2011;39:295–301. doi: 10.1007/s00240-010-0341-y. [DOI] [PubMed] [Google Scholar]
- 36.Falahatkar S., Farzan A., Allahkhah A. Is complete supine percutaneous nephrolithotripsy feasible in all patients? Urol Res. 2011;39:99–104. doi: 10.1007/s00240-010-0287-0. [DOI] [PubMed] [Google Scholar]
- 37.Falahatkar S., Enshaei A., Afsharimoghaddam A., Emadi S.A., Allahkhah A.A. Complete supine percutaneous nephrolithotomy with lung inflation avoids the need for a supracostal puncture. J Endourol. 2010;24:213–218. doi: 10.1089/end.2009.0385. [DOI] [PubMed] [Google Scholar]
- 38.Cormio L., Annese P., Corvasce T., De Siati M., Turri F.P., Lorusso F. Percutaneous nephrostomy in supine position. Urology. 2007;69:377–380. doi: 10.1016/j.urology.2007.01.020. [DOI] [PubMed] [Google Scholar]
- 39.Kumar P, Bach C, Kachrillas S, Papatsoris AG, Buchholz N, Masood J. Supine percutaneous nephrolithotomy (PCNL): ‘in vogue’ but in which position? BJU Int. 2012 [Epub May 7]. [DOI] [PubMed]
- 40.Bach C GA, Kumar P, Buchholz N, Papatsoris AG, Masood. J. The Barts ‘flank-free’ modified supine position for percutaneous nephrolithotomy (PCNL). Urol Int, in press. [DOI] [PubMed]
- 41.Papatsoris A.G., Kachrilas S., Howairis M.E., Masood J., Buchholz N. Novel technologies in flexible ureterorenoscopy. Arab J Urol. 2011;9:41–46. doi: 10.1016/j.aju.2011.03.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Papatsoris AG, Skolarikos A, Buchholz N. Intracorporeal laser lithotripsy. Arab J Urol, in press. http://dx.doi.org/10.1016/j.aju.2012.02.006. [DOI] [PMC free article] [PubMed]
- 43.Jeong I.G.K.T., Bang J.K., Park J., Kim W., Hwang S.S., Kim H.K., Park H.K. Association between metabolic syndrome and the presence of kidney stones in a screened population. Am J Kidney Dis. 2011:383–388. doi: 10.1053/j.ajkd.2011.03.021. [DOI] [PubMed] [Google Scholar]
- 44.Wu P., Wang L., Wang K. Supine versus prone position in percutaneous nephrolithotomy for kidney calculi: a meta-analysis. Int Urol Nephrol. 2011;43:67–77. doi: 10.1007/s11255-010-9801-0. [DOI] [PubMed] [Google Scholar]
- 45.Liu L., Zheng S., Xu Y., Wei Q. Systematic review and meta-analysis of percutaneous nephrolithotomy for patients in the supine versus prone position. J Endourol. 2010;24:1941–1946. doi: 10.1089/end.2010.0292. [DOI] [PubMed] [Google Scholar]



