Abstract
PURPOSE
We aimed to determine the prevalence of paratracheal air cysts (PTACs) and the relationship of PTACs with emphysema and bronchiectasis through retrospective analysis of multidetector computed tomography (MDCT) findings.
METHODS
MDCT findings of 1027 consecutive patients who underwent routine thorax examination between January 2012 and January 2013 were evaluated retrospectively for the presence of PTACs. Localization of the PTACs, as well as their size, shape, and relationship with the trachea were examined. Presence of emphysema and bronchiectasis was recorded, and bronchiectasis severity index was calculated when present. We randomly selected 80 patients who had no visible PTACs as the control group. The findings of patients with and without PTACs were compared.
RESULTS
PTACs were determined in 82 of 1027 patients (8%), in 8.8% of females and 7.3% of males. The presence of PTACs was determined to be independent of gender (P = 0.361). Eighty-one PTACs (98.8%) were located in the right side of the trachea and 56.1% had a tracheal connection. The presence of PTACs significantly correlated with the presence and severity of bronchiectasis (P = 0.001 and P = 0.005 respectively). There was no significant relationship between the presence of PTACs and the presence of emphysema on CT images (P = 0.125).
CONCLUSION
The prevalence of PTACs was determined as 8% in this study. There was significant association between PTACs and bronchiectasis.
Paratracheal air cysts (PTACs) are small collections of air adjacent to the trachea at the level of the thoracic inlet (1). Pathological diagnosis of PTACs in surgically confirmed cases includes tracheal diverticulum, lymphoepithelial cyst, and bronchogenic cyst (1–3). These cysts are covered with ciliary columnar epithelium and connected with the trachea (4). The majority of PTACs are reported as tracheal diverticula in the literature, due to their connection with the trachea (2). The thoracic inlet between the cartilage and muscle layers in right posterolateral wall of the trachea is the most common location for PTACs. A relationship may be seen between an isolated PTAC and the trachea l lumen (5). These lesions may cause recurrent infections by acting as a reservoir for secretions.
Occasionally, PTACs can be confused with other causes of extraluminal air collections as laryngocele, pharyngocele, Zenker’s diverticulum, apical hernia of the lung, mediastinal air, apical paraseptal blebs, or bullae. To distinguish PTACs from other pathologies, its typical location in the right posterior paratracheal region at the thoracic inlet can be helpful: PTACs locate away from the lung pleura, communicate with the trachea and have rounded margins that can be differentiated from emphysematous changes (6).
PTACs are usually discovered incidentally on thorax computed tomography (CT). They may be associated with a chronic cough or chronic obstructive pulmonary diseases (COPD). The reported prevalence of PTACs ranges from 0.75% to 8.1% (4, 6–8). There have been a limited number of studies reporting the incidence of PTACs related to COPD or emphysema as detected by CT, and the reported results are variable (4, 6, 8–11). The relationship between PTACs and pulmonary emphysema or bronchiectasis is still unclear. To our knowledge, no published study has evaluated the relationship between PTACs and bronchiectasis, using a bronchiectasis severity index and objective measures to determine the extent of bronchiectasis on CT images.
The purpose of our study was to evaluate the prevalence and characteristics of PTACs, as well as their relationship with bronchiectasis and emphysema, on thorax CT scans.
Methods
Patients and study design
Between January 2012 and July 2013, the presence of PTACs was retrospectively evaluated in 1100 consecutive patients who underwent routine thorax multidetector CT for a variety of reasons. Patients with mediastinal injuries (n=73) were excluded from the study leaving a total of 1027 for evaluation (563 males and 464 females; median age, 47 years; range, 1–97 years). The local ethics committee approved this retrospective study and the requirement for informed patient consent was waived.
Imaging method
The thorax CT examinations were acquired using a multidetector row CT (Somatom Emotion 16-slice, Siemens Healthcare, Erlangen, Germany) following a standard protocol. Full inspiratory scans were obtained with or without administration of intravenous contrast medium. Slices were taken from the thoracic inlet as far as the level of lowest hemidiaphragm in supine position. The scanning parameters were 110 kV, effective tube current 55 mA, collimation 16×0.6 mm, pitch 1.5, section thickness 1 mm, reconstruction interval 0.8 mm, and tube rotation period 0.6 s. The images obtained were transferred to a picture archiving and communication system workstation. The axial images and multiplanar reconstruction reformatted images were evaluated together. All images were processed with standard mediastinal (width, 400 HU; level, 40 HU) and lung (width 1200 HU; level, −600 HU) window settings. Image analysis was performed by the same radiologist (N.B.) in all cases.
Four features of PTACs were evaluated: 1) localization with respect to the trachea (right, left, or posterior side); 2) shape (round, cylindrical, irregular); 3) size (anteroposterior, transverse, and vertical diameters of the cyst); 4) presence of visible communication with the trachea (Fig. 1). Anteroposterior and transverse diameters of the cyst were measured on the axial CT slices, while vertical diameter was obtained using the coronal reformatted images. The shape of the cyst was evaluated on the coronal reformatted CT images. The presence of emphysema or bronchiectasis was recorded in cases with PTACs (Fig. 2).
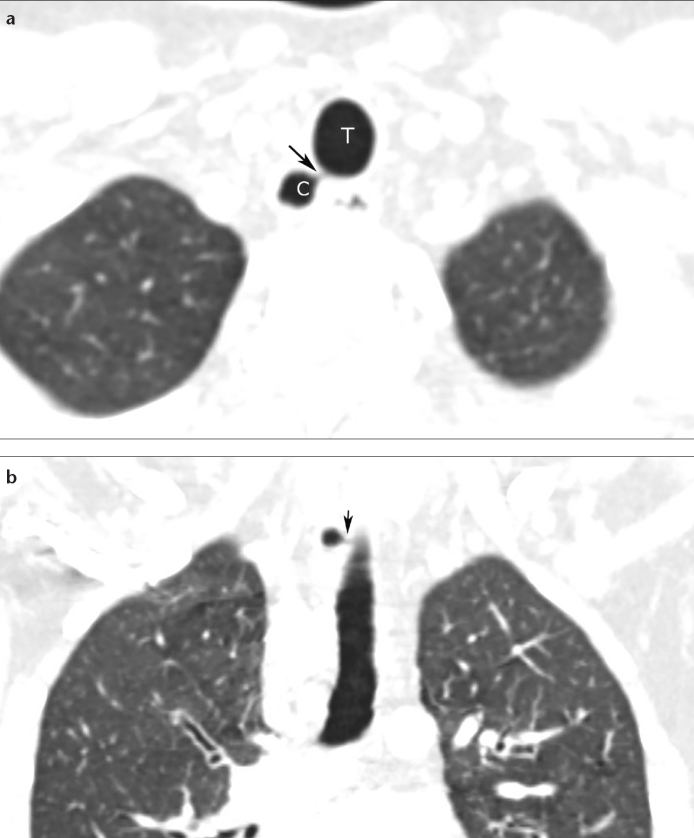
Figure 1.
a, b. Chest CT scans in a 42-year-old female with dyspnea. Axial (a) and coronal (b) CT images show a right paratracheal air cyst (C) with tracheal (T) connection (arrow).
Figure 2.
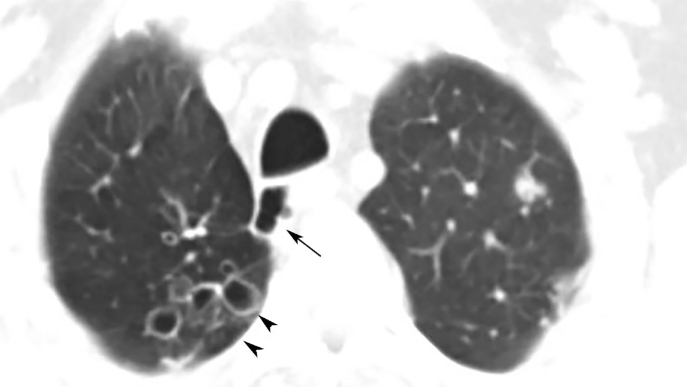
A paratracheal air cyst in a 40-year-old male with bronchiectasis. Axial lung window chest CT shows a lobulated multiseptated right paratracheal air cyst (arrow) and cystic bronchiectasis (arrowheads).
Diagnosis of bronchiectasis was based on the demonstration of bronchial dilatation relative to the adjacent pulmonary artery, lack of bronchial tapering, and visualization of bronchi in the lung periphery on CT (12).
The Reiff scoring system was used as the bronchiectasis severity index (13). We scored each lobe for: the extent of involvement (0=none, 1=one or partial bronchopulmonary segments involved, 2=two or more bronchopulmonary segments involved); the severity of bronchial dilatation (0=normal, 1=less than twice the diameter of the adjacent pulmonary artery, 2=two or three times the diameter of the adjacent pulmonary artery, 3=more than three times the diameter of the adjacent pulmonary artery); and the severity of bronchial wall thickening (0=normal, 1=half the diameter of the adjacent pulmonary artery, 2=more than half or same as the diameter of adjacent pulmonary artery, 3=more than the diameter of adjacent pulmonary artery) yielding a maximum total score of 48. Scores were obtained for each lobe (lingula considered a separate lobe), and a total value was calculated.
We randomly selected an age- and gender-matched control group of 80 patients from the 945 patients who had no PTACs, using automated computer software. We compared the presence of PTACs with the presence of emphysema and bronchiectasis. We also investigated the relationship between the presence and size of PTACs and the severity of bronchiectasis.
Statistical analysis
The data were processed by using SPSS version 15.0 (SPSS Inc., Chicago, Illinois, USA). Chi-square test was used to compare categorical variables, while Mann-Whitney U test was used to compare independent samples. Spearman correlation test was used to determine the relationship between the variables. All demographic and quantitative data were expressed as median (range). ROC analysis was used to estimate the bronchiectasis score cutoff value for detecting PTACs. Statistical significance was accepted as P < 0.05.
Results
Of 1027 patients, PTACs were determined in 82 (8%): in 41 of 563 males (7.3%) and 41 of 464 females (8.8%). The presence of PTACs was independent of gender (P = 0.361). The median age of patients with PTACs was 47 years (range, 1–97 years). There was a negative correlation between the presence of PTACs and age (P = 0.034, r=−0.066). The prevalence of PTACs according to the decades of life is shown in Table 1.
Table 1.
The prevalence of paratracheal air cysts according to the decades of life
| Age (years) | Number of subjects | PTACs presence | Prevalence (%) |
|---|---|---|---|
| 0–9 | 27 | 1 | 3.7 |
| 10–19 | 81 | 10 | 12.3 |
| 20–29 | 158 | 16 | 10.1 |
| 30–39 | 154 | 13 | 8.4 |
| 40–49 | 140 | 12 | 8.6 |
| 50–59 | 150 | 14 | 9.3 |
| 60–69 | 151 | 8 | 5.3 |
| 70–79 | 118 | 5 | 4.2 |
| 80–89 | 38 | 2 | 5.3 |
| 90–99 | 10 | 1 | 10 |
| Total | 1027 | 82 | 8 |
PTACs, paratracheal air cysts.
A single PTAC was observed in each patient and they were all in the thoracic inlet. Except for a single cyst located on the left side of the trachea, all remaining PTACs (n=81, 98.8%) were identified on the right side. The median anteroposterior diameter of the PTACs was 5.2 mm (range, 2–20 mm) and the median transverse diameter was 6.6 mm (range, 2–24 mm). Median vertical length was measured as 11 mm (range, 2–28 mm). A tracheal connection was determined in 46 PTACs (56.1%). Of these cases, 24 (52.2%) were female and 22 (47.8%) were male. No significant relationship was determined between tracheal connection and gender (P = 0.656). The cysts were round in 32 cases (39%), irregular in 24 (29.3%), and cylindrical in 26 (31.7%).
Bronchiectasis was determined in 28 patients with PTACs (34.1%) and emphysema in 14 patients (17.1%). The total number of patients with PTACs with coexisting emphysema and/or bronchiectasis was 42 (51.2%). In contrast, emphysema and/or bronchiectasis was present in 19 patients in the control group (23.8%). There was a statistically significant relationship between PTACs and COPD (emphysema and/or bronchiectasis) (P < 0.001). Coexistence of emphysema and bronchiectasis was observed radiologically in two patients with PTACs (2.4%) and in one patient of the control group (1.3%).
The bronchiectasis scores of patients with PTACs ranged from 6 to 44 with a median score of 20.5. In the control group bronchiectasis scores ranged from 3 to 38 (median score, 6). A significant difference was found between the bronchiectasis scores of patients with and without PTACs (P = 0.005). There was a significant relationship between the presence of PTACs and the presence of bronchiectasis on CT images (P = 0.001). There was a positive correlation between the presence of PTACs and bronchiectasis scores (P = 0.001, r=0.518). Using a bronchiectasis score cutoff value of 12.5 led to 85.7% sensitivity and 80% specificity for detection of PTACs (Fig. 3). The area under the ROC curve for diagnosing PTACs was 0.839 (95% confidence interval, 0.628–1.000; P = 0.002).
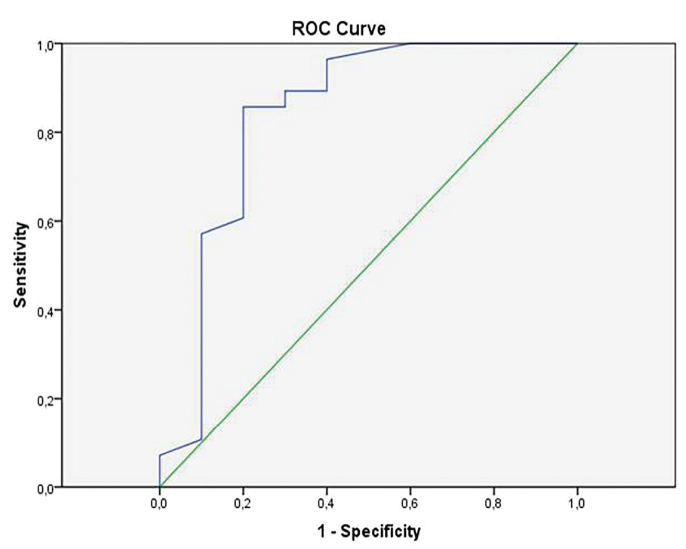
Figure 3.
The ROC curve for bronchiectasis scores in detecting PTACs. The area under the ROC curve for diagnosing PTACs is 0.839 (95% confidence interval, 0.628–1.000; P = 0.002).
The size of PTACs was not correlated with the severity of bronchiectasis (for anteroposterior dimension, P = 0.419, r=0.159; for transverse dimension, P = 0.279, r=0.212; for vertical dimension, P = 0.292, r=0.206). No significant relationship was determined between the presence of PTACs and the presence of emphysema on the CT images (P = 0.224) (Table 2).
Table 2.
Characteristics of 162 patients based on the presence of PTACs
| PTACs present (n=82) | PTACs absent (n=80) | P | ||
|---|---|---|---|---|
| Age (years), median (range) | 40 (8–95) | 42 (11–88) | 0.489 | |
| Gender | Female | 41 (50) | 39 (48.8) | 0.874 |
| Male | 41 (50) | 41 (51.3) | ||
| Bronchiectasis | Present | 28 (34.1) | 10 (12.5) | 0.001 |
| Absent | 54 (65.9) | 70 (87.5) | ||
| Emphysema | Present | 16 (19.5) | 10 (12.5) | 0.224 |
| Absent | 66 (80.5) | 70 (87.5) | ||
| COPD | Present | 42 (51.2) | 19 (23.8) | <0.001 |
| Absent | 40 (48.8) | 61 (76.3) | ||
Data are given as n (%) unless otherwise noted.
PTACs, paratracheal air cysts; COPD, chronic obstructive pulmonary disease.
Discussion
In this retrospective study PTACs were identified in 82 of 1027 patients (8%). This prevalence was close to the rate of 8.1% reported by Bae et al. (8), but significantly higher than those reported in other studies (0.75%–3.7%) (4, 6, 7, 14). The higher prevalence of PTACs in our study may be due to the high spatial resolution of multidetector CT and use of thin slices or due to ethnic differences.
In our study, PTACs were seen more often in the 2nd, 3rd, 6th, and 10th decades of life at rates of 12.3%, 10.1%, 9.3%, and 10% respectively, suggesting that PTACs are not rare findings in routine CT examinations. In their series, Bae et al. (8) found the highest incidence of PTACs in the 6th decade. Older age groups appear to have the acquired form of PTACs. In our study, only one patient in the first decade of life was found to have a PTAC. Although, previous studies reported an association between PTACs and gender (6, 9, 10), we found no such relationship. In our study, PTACs were identified on the right side of the trachea in 81 of 82 cases (98.8%). Previous studies have also reported PTACs more often on the right side (4, 6, 8, 10, 11). This preference for the right posterolateral side of the trachea is likely to be related to the weakness of the right side compared with the left side, which is supported by the esophagus at the conjunction area of the tracheal cartilaginous ring with the muscular section (2).
In our study, the median size of the PTACs was 5.17×6.60×10.95 mm. This finding is in accordance with PTAC dimensions of 7.5×4.2×11.5 mm reported by Kim et al. (11). In other studies, only the largest diameter of the cyst was measured on axial images, with or without a measurement of the vertical length (4, 6, 8, 9). Goo et al. (4) reported mean axial diameter as 10 mm and mean vertical length as 14 mm; these measurements were considerably larger than our measurements. In our study, most PTACs were round (39%), whereas in studies by Bae et al. (8) and Kim et al. (11) elongated cysts were more frequent (47.8% and 41.6%, respectively). In addition, Bae et al. (4) reported fewer irregular-shaped cysts than our study (7.2% vs. 29.3%). In our study, a connection with the trachea was established in 46 cysts (56.1%), which is a much higher rate than those reported by several previous studies (4, 8, 10, 15). However, a study by Cheng et al. (9) did report a rate of 55% for connection between the cyst and the trachea, as in our study. This high result may be due to the effect of thin slices and high spatial resolution of the multidetector CT on the determination of small cysts. Furthermore, the presence of tracheal connection was evaluated from both axial and coronal slices in our study. In other studies, presence of tracheal connection was evaluated primarily from axial slices; coronal and sagittal planes were visualized only as needed (6, 8, 11, 16).
In our study the bronchiectasis rate among PTACs cases was 34.1%, a much higher rate than those reported in other studies. We found a relationship between the presence of PTACs and the presence and severity of bronchiectasis. Inadequacy in the support and elasticity of the bronchial wall develops as a result of bronchiectasis (17). Difficulties in expiration or chronic cough lead to an obstruction which increases the internal pressure in the bronchi and weakens the bronchial wall (17). Similarly, PTACs are seen together with tracheal muscle weakness and conditions such as COPD and chronic cough which increase tracheal internal pressure (18, 19). In a study by Kim et al. (11), bronchiectasis was determined in 2.6% and emphysema in 14.6% of cases with PTACs. In that study, PTACs were not associated with respiratory symptoms or obstructive lung disease, clinically or radiologically. The emphysema and bronchiectasis rates were quite low compared to our study, probably due to inclusion of people who underwent low-dose screening chest CT in their study.
The low rate of emphysema (18.7%) in our study is close to the rate of emphysema (17.4%) reported by Bae et al. (8). The relationship between PTACs and emphysema is controversial in the literature. Goo et al. (4) suggested that PTAC may be a sign of COPD. However, in other studies no relationship was found between PTACs and emphysema (6, 8, 9, 11). Similarly, we did not find an association between PTACs and radiological emphysema in our study. These variable outcomes are probably related to the selection of the study group. Goo et al. (4) included individuals with pulmonary diseases, whereas Buterbaugh et al. (6) included patients with traumatic injury and those with an initial diagnosis of neck lesions, and we included patients who underwent CT for a variety of reasons.
Our study has some limitations. First, due to the retrospective nature of our study, the diagnosis of emphysema and bronchiectasis was made based on multidetector CT findings only, and were not corroborated by respiratory function tests. Second, a pathological correlation of PTACs could not be made. However, there is generally no requirement for pathological test results as PTACs are incidental. Third, as the study group included patients who underwent thorax CT for a variety of symptoms, the relevance of our results to the general population may be argued. However, it would not be ethical to expose healthy individuals to radiation for no apparent medical reason.
In conclusion, we determined the prevalence of PTACs as 8%, with no gender differences. Bronchiectasis was determined at a greater rate than emphysema in patients with PTACs. We observed a significant association between PTACs and the presence and severity of bronchiectasis. The presence of PTACs might suggest the existence of emphysema and bronchiectasis (COPD) radiologically.
Footnotes
Conflict of interest disclosure
The authors declared no conflicts of interest.
References
- 1.Tanaka H, Mori Y, Kurokawa K, Abe S. Paratracheal air cysts communicating with the trachea: CT findings. J Thorac Imaging. 1997;12:38–40. doi: 10.1097/00005382-199701000-00005. [DOI] [PubMed] [Google Scholar]
- 2.Infante M, Mattavelli F, Valente M, Alloisio M, Preda F, Ravasi G. Tracheal diverticulum: a rare cause and consequence of chronic cough. Eur J Surg. 1994;160:315–316. [PubMed] [Google Scholar]
- 3.Tanaka H, Igarashi T, Teramoto S, Yoshida Y, Abe S. Lymphoepithelial cysts in the mediastinum with an opening to the trachea. Respiration. 1995;62:110–113. doi: 10.1159/000196403. [DOI] [PubMed] [Google Scholar]
- 4.Goo JM, Im JG, Ahn JM, et al. Right paratracheal air cysts in the thoracic inlet: clinical and radiologic significance. AJR Am J Roentgenol. 1999;173:65–70. doi: 10.2214/ajr.173.1.10397101. [DOI] [PubMed] [Google Scholar]
- 5.Webb EM, Elicker BM, Webb WR. Using CT to diagnose nonneoplastic tracheal abnormalities: appearance of the tracheal wall. AJR Am J Roentgenol. 2000;174:1315–1321. doi: 10.2214/ajr.174.5.1741315. [DOI] [PubMed] [Google Scholar]
- 6.Buterbaugh JE, Erly WK. Paratracheal air cysts: a common finding on routine CT examinations of the cervical spine and neck that may mimic pneumomediastinum in patients with traumatic injuries. AJNR Am J Neuroradiol. 2008;29:1218–1221. doi: 10.3174/ajnr.A1058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Masamichi M, Osamu T, Toshiro K. Paratracheal air cysts in middle-aged Japanese men. J Bronchol. 2006;13:6–8. [Google Scholar]
- 8.Bae HJ, Kang EY, Yong HS, et al. Paratracheal air cysts on thoracic multidetector CT: incidence, morphological characteristics and relevance to pulmonary emphysema. Br J Radiol. 2012;86:20120218. doi: 10.1259/bjr.20120218. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Cheng HM, Chang PY, Chiang KH, Huang HW, Lee CC. Prevalence and characteristics of paratracheal air cysts and their association with emphysema in a general population. Eur J Radiol. 2011;81:2673–2677. doi: 10.1016/j.ejrad.2011.10.013. [DOI] [PubMed] [Google Scholar]
- 10.Kurt A, Tanrıvermis Sayit A, Ipek A, Gunes Tatar I. A multidetector computed tomography survey of tracheal diverticulum. Eurasian J Med. 2013;45:145–148. doi: 10.5152/eajm.2013.31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Kim JS, Kim AY, Yoon Y. Paratracheal air cysts using low-dose screening chest computed tomography: clinical significance and imaging findings. Jpn J Radiol. 2011;29:644–648. doi: 10.1007/s11604-011-0608-4. [DOI] [PubMed] [Google Scholar]
- 12.Diederich S, Roos N, Thomas M, Peters PE. Diagnostic imaging in bronchiectases. Value of CT and HRCT. Radiologe. 1996;36:550–559. doi: 10.1007/s001170050110. [DOI] [PubMed] [Google Scholar]
- 13.Reiff DB, Wells AU, Carr DH, Cole PJ, Hansell DM. CT findings in bronchiectasis: limited value in distinguishing between idiopathic and specific types. AJR Am J Roentgenol. 1995;165:261–267. doi: 10.2214/ajr.165.2.7618537. [DOI] [PubMed] [Google Scholar]
- 14.Mackinnon D. Tracheal diverticula. J Pathol Bacteriol. 1953;65:513–517. doi: 10.1002/path.1700650223. [DOI] [PubMed] [Google Scholar]
- 15.Early EK, Bothwell MR. Congenital tracheal diverticulum. Otolaryngol Head Neck Surg. 2002;127:119–121. doi: 10.1067/mhn.2002.126478. [DOI] [PubMed] [Google Scholar]
- 16.Polat AV, Elmali M, Aydin R, Ozbay A, Celenk C, Murat N. Paratracheal air cysts: prevalence and correlation with lung diseases using multidetector CT. J Med Imaging Radiat Oncol. 2013;58:144–148. doi: 10.1111/1754-9485.12095. [DOI] [PubMed] [Google Scholar]
- 17.Nicotra MB, Rivera M, Dale AM, Shepherd R, Carter R. Clinical, pathophysiologic, and microbiologic characterization of bronchiectasis in an aging cohort. Chest. 1995;108:955–961. doi: 10.1378/chest.108.4.955. [DOI] [PubMed] [Google Scholar]
- 18.Pinot D, Breen D, Peloni JM, Gaubert JY, Dutau H, Vervloet D. An incidental finding in a 34-year-old male under investigation for haemoptysis. Diagnosis: The radiological and endoscopic images demonstrate a complex defect along the posterior tracheal wall consistent with acquired tracheal diverticulum. Eur Respir J. 2009;33:1227–1229. doi: 10.1183/09031936.00131908. [DOI] [PubMed] [Google Scholar]
- 19.Kokkonouzis I, Haramis D, Kornezos I, Moschouris H, Katsenos S, Bouchara S. Tracheal diverticulum in an asymptomatic male: a case report. Cases J. 2008;1:181. doi: 10.1186/1757-1626-1-181. [DOI] [PMC free article] [PubMed] [Google Scholar]