Abstract
Background
Novel urinary biomarkers are useful for the prediction of acute kidney injury (AKI). Most promising are the urine markers NGAL, IL-18, KIM-1, and LFABP. Each of these has shown considerable promise diagnosing AKI earlier than serum creatinine (Scr) using disease controls. We set out to determine reference levels of these markers in a healthy pediatric population.
Methods
Urine was collected from 368 healthy children and assayed for NGAL, IL-18, KIM-1, and LFABP using commercially available kits or assay materials. Analysis of biomarkers by linear regression and according to age groups (3–<5 years; 5–<10; 10–<15; 15–<18) was performed to determine if biomarker levels differed with age and gender.
Results
Median values were: NGAL (6.6 ng/ml; IQR 2.8–17), IL-18 (21.6 pg/ml; IQR 13.6–32.9), KIM-1 (410 pg/ml; IQR 226–703), LFABP (3.4 ng/ml; IQR 1.6–6.0). Significant gender differences were found with NGAL and IL-18 and significant age differences were found with all markers. 95th percentile values for each marker varied with age and gender greater than median values.
Conclusions
This is the largest pediatric reference range study for the urinary measurement of NGAL, IL-18, KIM-1, and LFABP and highlights age and gender differences in these markers. This information is essential for rational interpretation of studies and clinical trials utilizing these emerging AKI biomarkers.
Keywords: Neutrophil gelatinase-associated lipocalin (NGAL), Interleukin 18 (IL-18), Kidney injury molecule 1 (KIM-1), Liver fatty acid binding protein (LFABP), Reference range, Acute kidney injury
Introduction
Pediatric acute kidney injury (AKI) is on the rise, especially among the critically ill [1–3]. Partly responsible for the increase is that diseases that previously had high fatality rates, such as sepsis, congenital heart disease, and certain cancers, have increased survival due to increased quality of care [4–6]. The functional consequence of AKI is reduced glomerular filtration rate. Serum creatinine (SCr) is eliminated by glomerular filtration, increases with AKI, and is currently the primary diagnostic test of AKI. Lack of specificity and slow response to alterations in disease severity or treatment are primary reasons why SCr is an unsatisfactory biomarker for renal disease, especially in AKI. First, SCr levels change with factors unrelated to renal disease, such as age, gender, diet, muscle mass, muscle metabolism, race, strenuous exercise, and hydration status. Creatinine levels are also influenced by certain drugs [7, 8]. Furthermore, rises in SCr occur long after the renal injury is sustained. In fact, SCr concentrations may not change until approximately 50 % of kidney function has been lost. This makes SCr a poor diagnostic marker for AKI, since treatments need to be administered soon after injury to be effective. Animal studies have shown that treatments to prevent or alleviate AKI need to begin well before the SCr level begins to rise [9–11].
Over the last decade, several promising early biomarkers of AKI have been identified in urine. This article will focus on renal tubular markers. Some of the most promising of these markers include kidney injury molecule–1 (KIM-1), neutrophil gelatinase-associated lipocalin (NGAL), interleukin-18 (IL-18), and liver fatty acid binding protein (LFABP) [12, 13]. Using genomic and proteomic technology, these proteins were discovered in nephrotoxic or ischemic animal AKI models, and represent molecular events of epithelial injury. NGAL was initially discovered to be elevated in mouse models of ischemia-reperfusion injury (IRI) [14] then subsequently found to be an early marker of AKI in patients following cardiopulmonary bypass (CPB) [15, 16]. Recently, our group measured the temporal pattern of all four markers following CPB to predict AKI [17]. Urine NGAL significantly increased in AKI patients 2 h after CPB and remained elevated at all time-points. IL-18 and L-FABP were intermediate biomarkers, increasing at 6 h after CPB. KIM-1 increased at 12 h after CPB. Biomarker elevations significantly correlated with clinical outcomes and improved prediction of AKI over a clinical model. In addition to AKI, there is evidence that these markers may also be useful in predicting and monitoring progression of various forms of chronic kidney disease (CKD), such as steroid-resistant nephrotic syndrome, diabetic nephropathy, and renal decline due to atherosclerosis [18–20]. In order for these biomarkers to have clinical utility, we must determine the normative values of these markers in a healthy pediatric population. In most previous studies, control measures of these biomarkers were made in patients who were being treated but did not develop AKI (50 % rise in SCr). While the levels of biomarkers in the AKI patients was significantly elevated compared to these controls, they may also be elevated in the controls compared to healthy children.
In this study, we set out to establish a reference range for NGAL, IL-18, KIM-1, and LFABP in a population of healthy children, and to determine if levels of these markers fluctuate with age or gender.
Methods
Patients
This study was approved by the Cincinnati Children’s Hospital Medical Center Internal Review Board and was carried out in accordance with the Declaration of Helsinki. Samples included were from the Cincinnati Genomic Control Cohort (CGCC). Inclusion criteria were as follows: between 3 and 18 years of age (prior to 18th birthday) at the time of enrollment, willingness of family to participate and give consent to participate in this project, willingness for participants aged 11 years of age and older to provide assent to participate in this project, ability to complete the introductory medical history, willingness to be contacted annually for future medical history updates, and willingness to consent to long-term storage and future analysis of DNA. Subjects were excluded if they met any of the following criteria: presence of known genetic diseases or severe chronic medical conditions, such as chromosomal abnormality, first-degree relative participating in the project, unwillingness to complete family and personal health history or allow storage or genetic testing of samples, and adopted, without full contact with biological parent(s) to be able to obtain family history information. Specific exclusion criteria for the subset of patients used in our study was a history of kidney injury or disease, including, but not limited to, IGA nephropathy, kidney stones, abnormal bladder, urinary reflux, and ureteral reimplantation.
Recruits were obtained through a marketing plan developed to ensure community-based participation, designed with the help of the Clinical Trials Office. Census tract monitoring was used to ensure both the diversity of cohort as well as the representativeness (an equal number of males and females, and approximately 85 % white non-Hispanic, 12 % African American, and 3 % Asian, Hispanic, and other minorities, which represents the population distribution of the seven counties of northern Kentucky and Ohio that comprise greater Cincinnati).
Potential subjects recruited from the community were screened by telephone to ensure eligibility and scheduled for an approximately 2–4-h visit. At this visit, a questionnaire was administered by the clinical research coordinator, a brief physical exam from a licensed physician was performed and samples (blood, urine, hair) were collected. Random urine samples were collected in 4-oz. sterile specimen containers. The specimen was then given to the lab 15–60 min after collection, where it was centrifuged briefly to settle particulate matter and aliquoted prior to storage at −80 °C. Samples were collected from 2007 to 2010 and stored until measurement in 2013. All measurements were performed in one batch in a period of 1 week.
Biomarker measurements
The urine NGAL ELISA was performed using a commercially available assay (NGAL ELISA Kit 036; Bioporto, Grusbakken, Denmark) that specifically detects human NGAL [16]. The intra-assay coefficient of variation (CV) was 2.1 % and inter-assay CV was 9.1 %. Urine IL-18 and L-FABP were measured using commercially available ELISA kits (Medical & Biological Laboratories Co., Nagoya, Japan and CMIC Co., Tokyo, Japan, respectively) per manufacturer’s instructions. CVs for IL-18 and LFABP were inter (7.3 %; 6.1 %) and intra (7.5 %; 10.9 %). The urine KIM-1 [21] ELISA was constructed using commercially available reagents (Duoset DY1750, R & D Systems, Inc., Minneapolis, MN) as described previously [16]. Intra- and inter-assay CV for KIM-1 was 2 and 7.8 %, respectively. Measurements were carried out in duplicate.
Statistics
Statistical analysis was performed using SigmaPlot 12.5 (Systat Software, Inc,. Chicago, IL, USA). All groups failed the Shapiro–Wilk test for normal distributions (p<0.05). As a result, individual comparisons of the effect of gender were subjected to Mann–Whitney rank sum analysis. The effect of gender and age group on biomarker values were analyzed using a Kruskal–Wallis one-way analysis of variance on ranks followed by Dunn’s multiple comparison test. Multiple linear regression was also performed to investigate the continuous effect of age as well as gender on biomarker levels. Biomarker values were log transformed to fulfill the assumptions of linear regression modeling. p values less than 0.05 were considered significant for differences between age and sex. For multivariate linear regression analysis, variables with p values less than 0.05 were removed and 95th percentile values were also calculated for each biomarker.
Results
Urine was collected from 1,020 participants and measurements made on urine from 368 children from the Cincinnati Genomic Control Cohort (healthy children presenting to Cincinnati Children’s Hospital primary care clinic for well child visits). Children who were not excluded based on medical history (see Methods) were randomly selected with stratification to ensure equal representation among age groups and sex. Demographic data can be seen in Table 1. To determine normal reference levels, urine was measured by ELISA for NGAL, IL-18, KIM-1, and LFABP. Overall, median values were as follows: NGAL (6.6 ng/ml; interquartile range (IQR) 2.8–17), IL-18 (21.6 pg/ml; IQR 13.6–32.9), KIM-1 (410 pg/ml; IQR 226–703), LFABP (3.4 ng/ml; IQR 1.6–6.0). To determine whether the urinary biomarker levels differed with respect to age or gender, specimens were grouped by age (3–<5 years (n=94); 5–<10 (n=89); 10–<15 (n=93); 15–<18 (n=92)) and gender (M=184, F=184). To analyze the effect of gender on biomarker levels, age-grouped results were subjected to Mann–Whitney rank sum analysis. Results are shown in Fig. 1. To summarize, NGAL was significantly elevated in females vs. males in all age groups (13.1 ng/ml, IQR 5.3–26.6 vs. 3.5 ng/ml, IQR 1.9–7.9; p<.001). IL-18 was elevated in females vs. males between 10–<15 and 15–<18 years of age (31 ng/ml, IQR 22.6–47.1 vs. 19 ng/ml, IQR 12.5–27.9 and 27 ng/ml, IQR 13.6–57.7 vs. 18 ng/ml, IQR 14.4–24.9, respectively, p<.001). LFABP was slightly elevated in females between 10 and <15 years (3.5 ng/ml, IQR 2.0–5.2 vs. 1.8 ng/ml, IQR 0.5–5.7; p=0.03), but then became elevated in males between the ages 15–<18 (4.5 ng/ml, IQR 2.9–6.3 vs. 2.5 ng/ml, IQR 0.9–3.3; p<0.001). There were no gender differences between KIM-1 levels in this cohort.
Table 1.
Demographics divided by age grouping
| 3–<5 years | 5–<10 years | 10–<15 years | 15–<18 years | |
|---|---|---|---|---|
| n=Males/females | 49/45 | 45/44 | 45/48 | 45/47 |
| Age (mean±SE) | 4.04±0.06 | 7.4±0.15 | 12.4±0.15 | 16.3±0.1 |
| Height (cm) | 103.6±0.65 | 124.1±1.4 | 155.4±1.1 | 170.4±0.95 |
| Height z score | 0.46±0.97 | 0.19±1.1 | 0.37±0.98 | 0.36±0.96 |
| Weight (kg) | 17.7±0.35 | 26.9±0.82 | 50.5±1.4 | 67.1±1.7 |
| Weight z score | 0.54±1.1 | 0.36±0.98 | 0.58±0.96 | 0.57±0.99 |
| BMI | 16.4±0.2 | 18±1.1 | 20.7±0.42 | 23.1±0.55 |
| BMI z score | 0.42±1.2 | 0.40±0.94 | 0.55±0.87 | 0.39±1.0 |
| Puberty onset (pre/post %) | 100/0 | 97.8/2.2 | 16.1/84.9 | 0/100 |
| Race % | ||||
| • White | 86.2 | 86.5 | 80.6 | 82.6 |
| • Black | 12.7 | 13.5 | 17.2 | 15.2 |
| • Hispanic | 1.1 | 0 | 2.2 | 2.2 |
| Parents—highest education completed % | ||||
| • Grade school | 7.4 | 3.3 | 4.3 | 4.4 |
| • High school | 28.7 | 28.1 | 31.2 | 22.8 |
| • College/trade school | 42.6 | 55.1 | 49.4 | 54.3 |
| • Graduate degree | 21.3 | 13.5 | 15.1 | 18.5 |
| Annual income level % | ||||
| • <$20,000 | 17 | 11.2 | 8.6 | 10.9 |
| • $20,000–$50,000 | 25.6 | 29.2 | 21.5 | 14.2 |
| • $50,000–$100,000 | 43.6 | 41.6 | 50.5 | 42.4 |
| • >$100,000 | 13.8 | 18 | 19.4 | 31.5 |
Fig. 1.
Gender differences in biomarker values by age group. The four graphs represent median values for each individual biomarker in males and females, separated by age group. Error bars indicate 75th percentile. Asterisk represents a significant difference in gender values in that specific group. NGAL neutrophil gelatinase associated lipocalin, IL-18 interleukin 18, LFABP liver fatty acid binding protein, KIM-1 kidney injury molecule 1
To analyze the effects of age on biomarker values, data were subjected to Kruskal–Wallis one-way analysis of variance on ranks followed by Dunn’s multiple comparison test for each biomarker (Fig. 2). Urine NGAL was significantly higher in the 10–<15 year and 15–<18 year age groups (7.6 ng/ml, IQR 3.3–21.7 and 12.1 ng/ml, IQR 6.4–27.0, respectively; p<0.001) when compared to both the 3–<5 year group (3.6 ng/ml, IQR 1.9–12.5) and 5–<10 year age group (4.5 ng/ml, IQR 2.1–9.4). KIM-1 was significantly higher at 15–<18 years (515.6 pg/ml, IQR 195.2–866.0; p=0.002) when compared to ages 3–<5 years (336.8 pg/ml, IQR 195.2–513.1) and 5–<10 years (386.4 pg/ml, IQR 217.7–620.4). IL-18 was significantly higher in the 10–<15 year group when compared to 3–<5 years (25.4 pg/ml, IQR 15.6–37.3 vs. 18.7 pg/ml, IQR 10.3–31.0; p=0.03). LFABP was significantly higher in the 3–<5 year group (5.6 ng/ml, IQR 1.9–12.2; p<0.001) when compared to 5–<10 years (2.9 ng/ml, IQR 1.4–4.9), 10–<15 years (2.7 ng/ml, IQR 1.3–5.5) or 15–<18 years (3.1 ng/ml, IQR 2.0–5.5). Age and gender 95th percentile values for each marker can be seen in Table 2. The 95th percentile values demonstrate a much less consistent pattern than the medians, but could serve as a guide for the upper limits of the normal range.
Fig. 2.
Age-related differences in biomarker values. The four graphs represent median values for each individual biomarker separated by age group. Error bars indicate 75th percentile. The asterisk represents a significant difference and horizontal lines connect the significantly higher group to the groups they are different than, with drop lines indicating those groups. NGAL neutrophil gelatinase associated lipocalin, IL-18 interleukin 18, LFABP liver fatty acid binding protein, KIM-1 kidney injury molecule 1
Table 2.
95th percentile rank values for each marker by age and gender. The first number is the 95th percentile rank value for the complete cohort at that age group, and values for males and females, respectively, are shown in parentheses
| 95th percentile cutoffs | NGAL (ng/ml) Combined (M, F) |
KIM-1 (pg/ml) Combined (M, F) |
IL-18 (pg/ml) Combined (M, F) |
LFABP (ng/ml) Combined (M, F) |
|---|---|---|---|---|
| Complete cohort (n=368) | 57.6 (28.3, 73.1) | 1,302.0 (1,298.4, 1,444.7) | 87.9 (56.1, 104.5) | 17.0 (15.5, 18.6) |
| 3–<5 years (n=94) | 39.1 (26.1, 52.2) | 1,128.2 (983.7, 1,291.7) | 89.5 (78.3, 100.5) | 39.5 (49.4, 41.4) |
| 5–<10 years (n=89) | 58.5 (10.9, 139.5) | 1,239.5 (1,276.6, 1,212.9) | 54.3 (41.7, 79.0) | 13.1 (15.5, 13.5) |
| 10–<15 years (n=93) | 66.8 (25.5, 72.3) | 1,141.1 (1,156.6, 1,103.5) | 88.8 (58.5, 111.1) | 13.2 (13.7, 13.3) |
| 15–<18 years (n=91) | 74.7 (50.0, 138.6) | 1,876.2 (1,877.3, 1,934.5) | 138.9 (71.2, 273.1) | 8.2 (10.5, 6.7) |
NGAL neutropinil gelatinase associated lipocalin, KIM-1 kidney injury molecule 1, IL-18 interleukin 18, LFABP liver fatty acid binding protein, M male, F female
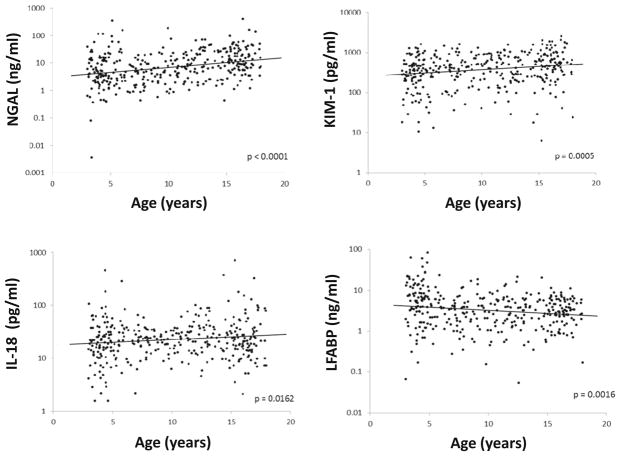
Linear regression analysis confirmed the age- and gender-grouped results. Graphical representations of the biomarker values as a function of age can be seen in Fig. 3. Multiple linear regression analysis demonstrated an increase of NGAL, KIM-1, and IL-18 with age, whereas L-FABP decreased with age (Table 3). Females had significantly higher NGAL and IL-18 levels compared to males. There was no association of any bio-marker with height, weight, or body mass index (BMI) z scores.
Fig. 3.
Graphical distribution of biomarker values by age with best-fit regression line. Each dot in the scatter plot represents the raw biomarker value for a specific participant, plotted on a logarithmic scale. NGAL neutrophil gelatinase-associated lipocalin, IL-18 interleukin 18, LFABP liver fatty acid binding protein, KIM-1 kidney injury molecule 1
Table 3.
Multivariate analysis: relationship of age and gender with biomarker levels
| Biomarker | Variable | Percent change in biomarker (95 % CI) | p value |
|---|---|---|---|
| NGAL | Age (per year increase) | 9.5 (6.9–12.2) | <0.0001 |
| Gender (percent increase in females) | 213.4 (148.1–295.9) | <0.0001 | |
| KIM-1 | Age (per year increase) | 3.8 (1.6–5.9) | 0.0005 |
| IL-18 | Age (per year increase) | 2.2 (0.4–4.0) | 0.0170 |
| Gender (percent increase in females) | 49.6 (26.3–77.2) | <0.0001 | |
| L FABP | Age (per year increase) | −3.5 (−5.6–−1.4) | 0.0016 |
NGAL neutropinil gelatinase associated lipocalin, KIM-1 kidney injury molecule 1, IL-18 interleukin 18, LFABP liver fatty acid binding protein
Discussion
This is the first large-scale study to determine normative values for all four of the most commonly investigated renal tubular biomarkers for AKI in a healthy pediatric population. This data is essential for establishing potential guidelines for clinical use of these assays for diagnostic purposes. Most studies to date have used “disease controls” to establish cutoffs for urine biomarkers [15, 17, 22–25]. “Disease controls” are simply a cohort of patients in the same clinical setting that have a different outcome than is being studied. While “disease control” data is important and necessary to determine how biomarkers change in relevant clinical scenarios, such as AKI after cardiopulmonary bypass surgery, where CPB patients who did not develop AKI are used as controls for those developing AKI, these data do not provide us insight into how these markers behave in a totally healthy individual. The samples used in this study were from the Cincinnati Genomic Control Cohort. The goal of the development of the cohort was to obtain a population-representative sample which could be utilized as a control for a diverse set of projects.
Analysis of our data demonstrates differences in normal biomarker concentrations across both age and gender. NGAL and IL-18 demonstrated significant gender differences that remained after adjusting for patient age. The elevation of NGAL in females vs. males has also been demonstrated in the adult population in several studies in both healthy and diseased populations [26–29]. IL-18 was also elevated in females after 10 years of age. Interestingly, while LFABP was elevated in females from ages 10 to <15 years, it became elevated in males from 15 to <18 years. To determine whether this flip is just an anomaly in the data or a real phenomenon will require further investigation. The biological reasons why biomarkers such as NGAL are generally higher in women are currently unknown, but represent an interesting avenue for further study.
Our dataset also revealed significant age-related differences in urinary biomarker excretion. NGAL, IL-18, and KIM-1 all increased with age. NGAL and IL-18 increased significantly after 10 years of age, while KIM-1 was elevated significantly in the 15–<18 year age group. Given the timing of the increase, it is possible that sexual development may influence levels of these markers. Therefore, age and gender may play a significant role in the determination of any cutoffs for clinical use of these markers and provide a significant impetus for developing age and gender tables for normal reference values. Interestingly, LFABP behaved in the opposite manner, displaying the highest level in the 3–<5 year group, and decreased thereafter to a steady level from 5 to <18 years of age. Sexual development was an important factor in determining age groups for analysis. We purposely selected 5–<10 and 10–<15 to represent populations largely before and after the onset of puberty. For comparison, 97.9 % of patients in the 5–<10 year group were pre onset of puberty, whereas 84.9 % of those in the 10–<15 year group were post onset of puberty. One weakness of our study is that we do not have values for children less than 3 years of age. This younger population has demonstrated differing values in biomarkers in other populations, possibly due to the immature development of the kidney [30]. For example, Cangemi et al. [31] found significantly higher urinary NGAL levels in the neonatal population than in older children. Variables such as height and weight, which are indicators of renal length and mass, could also influence biomarker levels. However, biomarkers did not correlate with height, weight, or BMI z scores in our cohort. This indicates that independent of age, these anthropometric measurements do not significantly affect biomarker values. Other factors, such as maturation of the immune system or increase in alloreactivity with age could potentially influence biomarker levels, but this is outside the scope of the current study.
For NGAL, where adult reference intervals have previously been established [28], our overall 95th percentile cutoff of 57.6 ng/ml is lower than that of other studies, which have ranged from 107 to 132 ng/ml using the automated Abbott Architect platform. While NGAL results from this platform show a strong correlation with the Bioporto ELISA used in this study, results are often shifted higher on the automated platform, which could account for a portion of the difference [16, 32]. The overall finding of a lower reference interval in children is consistent, however, with a meta-analysis of studies using NGAL to predict AKI, which found a cutoff of 170 ng/ml for adults vs. 100–135 ng/ml for children [22].
Pinning down optimal cutoff values for IL-18 has remained challenging. A meta-analysis of clinical studies of IL-18 as a biomarker for kidney injury/disease failed to find a consensus [33]. Optimal cutoffs among clinical studies of IL-18 as it relates to AKI have varied greatly, from a low of 20 pg/ml [25] to over 2,200 pg/ml [34]. The median level of urine IL-18 in our cohort of healthy children was 21.6 pg/ml with a 95th percentile cutoff of 87.9 pg/ml, which may lead to difficult clinical interpretation of these studies as they pertain to AKI. One inconsistency that may influence this variability, and ultimately its utility as a diagnostic marker, is the lack of a standard clinical assay for IL-18.
Our findings for LFABP are consistent with an earlier study which found median and IQR values for healthy volunteers to be 1.59 ng/ml and 0.89–3.05 ng/ml [35]. These values are slightly lower than our findings of 3.4 ng/ml (IQR 1.6–6.0), but they were from an adult cohort as opposed to a pediatric one. This follows along the trend of decreasing values of LFABP with maturation. While 95 % cutoffs for urinary LFABP were not found, the range of values indicative of AKI in a meta-analysis were extremely broad ranging [36]. In order to perform these comparisons to AKI studies, we had to use a biomarker-to-creatinine ratio. For this comparison, we measured creatinine in our urine samples using a modified Jaffe reaction on a Siemens Xpand plus HM Clinical Analyzer (Siemens, Munich, Germany). While the cutoff values in most studies analyzed were under 100 ng/mg creatine (range, 25–89 ng/mg), two studies were much higher, from 486 ng/mg [37] to 3,452 ng/mg [38]. The timing of the sampling may be of importance, since most renal biomarkers have distinct patterns of elevation post-surgery [17], but there was no specific trend in the timing of the samples in the meta-analysis that could explain such a large range of cutoffs. It is of interest that that our 95 % cutoff normal range values for LFABP (overall cohort—18.2 ng/mg creatinine) were below the cutoff values in the meta-analysis for AKI, and so consistent with healthy values in our population.
Our findings for KIM-1 are in line with, but range higher than, another study demonstrating healthy values for KIM-1. Chaturvedi et al. [21], who validated the assay used in this manuscript, found values ranging from 60 to 837 pg/ml and 0.07–0.399 ng/mg creatinine in 20 healthy volunteer subjects. Our overall median value of 410 pg/ml (IQR 226–703) falls within that range, but we have a broader range of values with an overall 95th percentile cutoff of 1,302 pg/ml and a much higher range for creatinine adjusted KIM-1 (median 0.359 ng/mg, with a 0.926 ng/mg 95th percentile). The study contained a small sampling of adults, and little demographic information was provided, so it is difficult to make a direct comparison to our pediatric population. However, a meta-analysis of the diagnostic value of KIM-1 [39] for AKI showed results consistent with our findings. Of the 11 studies analyzed, nine reported KIM-1 cutoff values for the diagnosis of AKI. Of those nine, all but one had a cutoff value higher than our 95th percentile value of 0.926 ng/mg, with cutoffs ranging from 0.42 to 2.817 ng/mg. The study with the 0.42 ng/mg cutoff [40] was clearly an outlier and studied a much different population than our current cohort, with a mean age of 68 years.
The topic of “normalizing” the data for hydration status with urine presents an especially difficult position with a maturing pediatric population. It is known that in the developing child, urine creatinine increases as a function of age and maturity [41]. Therefore any “correction” for creatinine applied to our biomarker levels would nullify any increase as a function of age. As a case in point, in our population, using a Spearman correlation, urine creatinine demonstrated a significant positive correlation with age (r=0.54, p<0.001). So since creatinine is dependent upon age in this population, it would not be useful as a normalization tool.
While the strengths of our study include a large representative healthy pediatric population and our laboratory’s expertise with these assays [16, 17, 24, 25, 42–46], this study is not without its weaknesses. Our study is from a single center cohort that is representative of the population of a mid-size US city (Cincinnati, OH, USA), which would not necessarily be representative globally. Also, while our assays are well established, none of them are standardized assays available on a clinical platform. As a result, our results may vary from those utilizing different assays. Also, the Cincinnati Genomic Control Cohort was not selected specifically for nephrology research, therefore certain information that would be valuable for comparison, such as glomerular filtration rate, are not available for these patients.
The value of NGAL, IL-18, KIM-1, and LFABP to predict early kidney injury and thus allow for timely treatments that may one day improve the outcome for patients with this potentially devastating condition is dependent upon quality measurements and precise normal values. This is the first study to attempt to establish these ranges for all four markers in a healthy pediatric population. These reference ranges will allow for better interpretation of clinical trials that will ultimately bring this knowledge to the clinic and improve care.
Acknowledgments
This work was funded by NIH P50 DK096418 to MB and PD. This research was supported in part by the Cincinnati Children’s Research Foundation and its Cincinnati Genomic Control Cohort.
Footnotes
Disclosures PD is a co-inventor on patents submitted for the use of NGAL as a biomarker of kidney injury.
References
- 1.Askenazi DJ, Feig DI, Graham NM, Hui-Stickle S, Goldstein SL. 3–5 year longitudinal follow-up of pediatric patients after acute renal failure. Kidney Int. 2006;69:184–189. doi: 10.1038/sj.ki.5000032. [DOI] [PubMed] [Google Scholar]
- 2.Schneider J, Khemani R, Grushkin C, Bart R. Serum creatinine as stratified in the RIFLE score for acute kidney injury is associated with mortality and length of stay for children in the pediatric intensive care unit. Crit Care Med. 2010;38:933–939. doi: 10.1097/CCM.0b013e3181cd12e1. [DOI] [PubMed] [Google Scholar]
- 3.Moffett BS, Goldstein SL. Acute kidney injury and increasing nephrotoxic-medication exposure in noncritically-ill children. Clin J Am Soc Nephrol. 2011;6:856–863. doi: 10.2215/CJN.08110910. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Peruzzi L, Bonaudo R, Amore A, Chiale F, Donadio ME, Vergano L, Coppo R. Neonatal sepsis with multi-organ failure and treated with a new dialysis device specifically designed for newborns. Case Rep Nephrol Urol. 2014;4:113–119. doi: 10.1159/000363691. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Oster ME, Lee KA, Honein MA, Riehle-Colarusso T, Shin M, Correa A. Temporal trends in survival among infants with critical congenital heart defects. Pediatrics. 2013;131:e1502–e1508. doi: 10.1542/peds.2012-3435. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Sadak KT, Fultz K, Mendizabal A, Reaman G, Garcia-Gonzalez P, Levine PH. International patterns of childhood chronic myeloid leukemia: comparisons between the United States and resource-restricted nations. Pediatr Blood Cancer. 2014;61:1774–1778. doi: 10.1002/pbc.25120. [DOI] [PubMed] [Google Scholar]
- 7.Letellier G, Desjarlais F. Analytical interference of drugs in clinical chemistry: II–the interference of three cephalosporins with the determination of serum creatinine concentration by the Jaffe reaction. Clin Biochem. 1985;18:352–356. doi: 10.1016/s0009-9120(85)80074-6. [DOI] [PubMed] [Google Scholar]
- 8.Weber JA, van Zanten AP. Interferences in current methods for measurements of creatinine. Clin Chem. 1991;37:695–700. [PubMed] [Google Scholar]
- 9.Herget-Rosenthal S, Marggraf G, Husing J, Goring F, Pietruck F, Janssen O, Philipp T, Kribben A. Early detection of acute renal failure by serum cystatin C. Kidney Int. 2004;66:1115–1122. doi: 10.1111/j.1523-1755.2004.00861.x. [DOI] [PubMed] [Google Scholar]
- 10.Devarajan P. Update on mechanisms of ischemic acute kidney injury. J Am Soc Nephrol. 2006;17:1503–1520. doi: 10.1681/ASN.2006010017. [DOI] [PubMed] [Google Scholar]
- 11.Hewitt SM, Dear J, Star RA. Discovery of protein biomarkers for renal diseases. J Am Soc Nephrol. 2004;15:1677–1689. doi: 10.1097/01.asn.0000129114.92265.32. [DOI] [PubMed] [Google Scholar]
- 12.Coca SG, Yalavarthy R, Concato J, Parikh CR. Biomarkers for the diagnosis and risk stratification of acute kidney injury: a systematic review. Kidney Int. 2008;73:1008–1016. doi: 10.1038/sj.ki.5002729. [DOI] [PubMed] [Google Scholar]
- 13.Portilla D, Dent C, Sugaya T, Nagothu KK, Kundi I, Moore P, Noiri E, Devarajan P. Liver fatty acid-binding protein as a biomarker of acute kidney injury after cardiac surgery. Kidney Int. 2007;73:465–472. doi: 10.1038/sj.ki.5002721. [DOI] [PubMed] [Google Scholar]
- 14.Mishra J, Ma Q, Prada A, Mitsnefes M, Zahedi K, Yang J, Barasch J, Devarajan P. Identification of neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury. J Am Soc Nephrol. 2003;14:2534–2543. doi: 10.1097/01.asn.0000088027.54400.c6. [DOI] [PubMed] [Google Scholar]
- 15.Mishra J, Dent C, Tarabishi R, Mitsnefes MM, Ma Q, Kelly C, Ruff SM, Zahedi K, Shao M, Bean J, Mori K, Barasch J, Devarajan P. Neutrophil gelatinase-associated lipocalin (NGAL) as a biomarker for acute renal injury after cardiac surgery. Lancet. 2005;365:1231–1238. doi: 10.1016/S0140-6736(05)74811-X. [DOI] [PubMed] [Google Scholar]
- 16.Bennett M, Dent CL, Ma Q, Dastrala S, Grenier F, Workman R, Syed H, Ali S, Barasch J, Devarajan P. Urine NGAL predicts severity of acute kidney injury after cardiac surgery: a prospective study. Clin J Am Soc Nephrol. 2008;3:665–673. doi: 10.2215/CJN.04010907. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Krawczeski CD, Goldstein SL, Woo JG, Wang Y, Piyaphanee N, Ma Q, Bennett M, Devarajan P. Temporal relationship and predictive value of urinary acute kidney injury biomarkers after pediatric cardiopulmonary bypass. J Am Coll Cardiol. 2011;58:2301–2309. doi: 10.1016/j.jacc.2011.08.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Bolignano D, Lacquaniti A, Coppolino G, Campo S, Arena A, Buemi M. Neutrophil gelatinase-associated lipocalin reflects the severity of renal impairment in subjects affected by chronic kidney disease. Kidney Blood Press Res. 2008;31:255–258. doi: 10.1159/000143726. [DOI] [PubMed] [Google Scholar]
- 19.Peralta CA, Katz R, Bonventre JV, Sabbisetti V, Siscovick D, Sarnak M, Shlipak MG. Associations of urinary levels of kidney injury molecule 1 (KIM-1) and neutrophil gelatinase-associated lipocalin (NGAL) with kidney function decline in the Multi-Ethnic Study of Atherosclerosis (MESA) Am J Kidney Dis. 2012;60:904–911. doi: 10.1053/j.ajkd.2012.05.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Kamijo-Ikemori A, Ichikawa D, Matsui K, Yokoyama T, Sugaya T, Kimura K. Urinary L-type fatty acid binding protein (L-FABP) as a new urinary biomarker promulgated by the Ministry of Health, Labour and Welfare in Japan. Rinsho Byori. 2013;61:635–640. [PubMed] [Google Scholar]
- 21.Chaturvedi S, Farmer T, Kapke GF. Assay validation for KIM-1: human urinary renal dysfunction biomarker. Int J Biol Sci. 2009;5:128–134. doi: 10.7150/ijbs.5.128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Haase M, Bellomo R, Devarajan P, Schlattmann P, Haase-Fielitz A. Accuracy of neutrophil gelatinase-associated lipocalin (NGAL) in diagnosis and prognosis in acute kidney injury: a systematic review and meta-analysis. Am J Kidney Dis. 2009;54:1012–1024. doi: 10.1053/j.ajkd.2009.07.020. [DOI] [PubMed] [Google Scholar]
- 23.Brunner HI, Mueller M, Rutherford C, Passo MH, Witte D, Grom A, Mishra J, Devarajan P. Urinary neutrophil gelatinase-associated lipocalin as a biomarker of nephritis in childhood-onset systemic lupus erythematosus. Arthritis Rheum. 2006;54:2577–2584. doi: 10.1002/art.22008. [DOI] [PubMed] [Google Scholar]
- 24.Parikh CR, Jani A, Mishra J, Ma Q, Kelly C, Barasch J, Edelstein CL, Devarajan P. Urine NGAL and IL-18 are predictive bio-markers for delayed graft function following kidney transplantation. Am J Transplant. 2006;6:1639–1645. doi: 10.1111/j.1600-6143.2006.01352.x. [DOI] [PubMed] [Google Scholar]
- 25.Parikh CR, Mishra J, Thiessen-Philbrook H, Dursun B, Ma Q, Kelly C, Dent C, Devarajan P, Edelstein CL. Urinary IL-18 is an early predictive biomarker of acute kidney injury after cardiac surgery. Kidney Int. 2006;70:199–203. doi: 10.1038/sj.ki.5001527. [DOI] [PubMed] [Google Scholar]
- 26.Schinstock CA, Semret MH, Wagner SJ, Borland TM, Bryant SC, Kashani KB, Larson TS, Lieske JC. Urinalysis is more specific and urinary neutrophil gelatinase-associated lipocalin is more sensitive for early detection of acute kidney injury. Nephrol Dial Transplant. 2013;28:1175–1185. doi: 10.1093/ndt/gfs127. [DOI] [PubMed] [Google Scholar]
- 27.Kaufeld JK, Gwinner W, Scheffner I, Haller HG, Schiffer M. Urinary NGAL ratio is not a sensitive biomarker for monitoring acute tubular injury in kidney transplant patients: NGAL and ATI in renal transplant patients. J Transplant. 2012;2012:8. doi: 10.1155/2012/563404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Cullen MR, Murray PT, Fitzgibbon MC. Establishment of a reference interval for urinary neutrophil gelatinase-associated lipocalin. Ann Clin Biochem. 2012;49:190–193. doi: 10.1258/acb.2011.011105. [DOI] [PubMed] [Google Scholar]
- 29.McWilliam SJ, Antoine DJ, Sabbisetti V, Pearce RE, Jorgensen AL, Lin Y, Leeder JS, Bonventre JV, Smyth RL, Pirmohamed M. Reference intervals for urinary renal injury biomarkers KIM-1 and NGAL in healthy children. Biomark Med. 2014 doi: 10.2217/bmm.14.36. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Parikh CR, Devarajan P, Zappitelli M, Sint K, Thiessen-Philbrook H, Li S, Kim RW, Koyner JL, Coca SG, Edelstein CL, Shlipak MG, Garg AX, Krawczeski CD. Postoperative biomarkers predict acute kidney injury and poor outcomes after pediatric cardiac surgery. J Am Soc Nephrol. 2011;22:1737–1747. doi: 10.1681/ASN.2010111163. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Cangemi G, Storti S, Cantinotti M, Fortunato A, Emdin M, Bruschettini M, Bugnone D, Melioli G, Clerico A. Reference values for urinary neutrophil gelatinase-associated lipocalin (NGAL) in pediatric age measured with a fully automated chemiluminescent platform. Clin Chem Lab Med. 2013;51:1101–1105. doi: 10.1515/cclm-2012-0540. [DOI] [PubMed] [Google Scholar]
- 32.Grenier FC, Ali S, Syed H, Workman R, Martens F, Liao M, Wang Y, Wong PY. Evaluation of the ARCHITECT urine NGAL assay: assay performance, specimen handling requirements and biological variability. Clin Biochem. 2010;43:615–620. doi: 10.1016/j.clinbiochem.2009.12.008. [DOI] [PubMed] [Google Scholar]
- 33.Liu Y, Guo W, Zhang J, Xu C, Yu S, Mao Z, Wu J, Ye C, Mei C, Dai B. Urinary interleukin 18 for detection of acute kidney injury: a meta-analysis. Am J Kidney Dis. 2013;62:1058–1067. doi: 10.1053/j.ajkd.2013.05.014. [DOI] [PubMed] [Google Scholar]
- 34.Xin C, Yulong X, Yu C, Changchun C, Feng Z, Xinwei M. Urine neutrophil gelatinase-associated lipocalin and interleukin-18 predict acute kidney injury after cardiac surgery. Ren Fail. 2008;30:904–913. doi: 10.1080/08860220802359089. [DOI] [PubMed] [Google Scholar]
- 35.Ferguson MA, Vaidya VS, Waikar SS, Collings FB, Sunderland KE, Gioules CJ, Bonventre JV. Urinary liver-type fatty acid-binding protein predicts adverse outcomes in acute kidney injury. Kidney Int. 2010;77:708–714. doi: 10.1038/ki.2009.422. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Susantitaphong P, Siribamrungwong M, Doi K, Noiri E, Terrin N, Jaber BL. Performance of urinary liver-type fatty acid-binding protein in acute kidney injury: a meta-analysis. Am J Kidney Dis. 2013;61:430–439. doi: 10.1053/j.ajkd.2012.10.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Portilla D, Dent C, Sugaya T, Nagothu KK, Kundi I, Moore P, Noiri E, Devarajan P. Liver fatty acid-binding protein as a biomarker of acute kidney injury after cardiac surgery. Kidney Int. 2008;73:465–472. doi: 10.1038/sj.ki.5002721. [DOI] [PubMed] [Google Scholar]
- 38.Li Y, Zhu M, Xia Q, Wang S, Qian J, Lu R, Che M, Dai H, Wu Q, Ni Z, Lindholm B, Axelsson J, Yan Y. Urinary neutrophil gelatinase-associated lipocalin and L-type fatty acid binding protein as diagnostic markers of early acute kidney injury after liver transplantation. Biomarkers. 2012;17:336–342. doi: 10.3109/1354750X.2012.672458. [DOI] [PubMed] [Google Scholar]
- 39.Shao X, Tian L, Xu W, Zhang Z, Wang C, Qi C, Ni Z, Mou S. Diagnostic value of urinary kidney injury molecule 1 for acute kidney injury: a meta-analysis. PLoS One. 2014;9:e84131. doi: 10.1371/journal.pone.0084131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Liangos O, Tighiouart H, Perianayagam MC, Kolyada A, Han WK, Wald R, Bonventre JV, Jaber BL. Comparative analysis of urinary biomarkers for early detection of acute kidney injury following cardiopulmonary bypass. Biomarkers. 2009;14:423–431. doi: 10.1080/13547500903067744. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Barr DB, Wilder LC, Caudill SP, Gonzalez AJ, Needham LL, Pirkle JL. Urinary creatinine concentrations in the U.S. population: implications for urinary biologic monitoring measurements. Environ Health Perspect. 2005;113:192–200. doi: 10.1289/ehp.7337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Hall IE, Yarlagadda SG, Coca SG, Wang Z, Doshi M, Devarajan P, Han WK, Marcus RJ, Parikh CR. IL-18 and urinary NGAL predict dialysis and graft recovery after kidney transplantation. J Am Soc Nephrol. 2010;21:189–197. doi: 10.1681/ASN.2009030264. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Zappitelli M, Washburn KK, Arikan AA, Loftis L, Ma Q, Devarajan P, Parikh CR, Goldstein SL. Urine neutrophil gelatinase-associated lipocalin is an early marker of acute kidney injury in critically ill children: a prospective cohort study. Crit Care. 2007;11:R84. doi: 10.1186/cc6089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Lavery AP, Meinzen-Derr JK, Anderson E, Ma Q, Bennett MR, Devarajan P, Schibler KR. Urinary NGAL in premature infants. Pediatr Res. 2008;64:423–428. doi: 10.1203/PDR.0b013e318181b3b2. [DOI] [PubMed] [Google Scholar]
- 45.Coca SG, Garg AX, Thiessen-Philbrook H, Koyner JL, Patel UD, Krumholz HM, Shlipak MG, Parikh CR. Urinary biomarkers of AKI and mortality 3 years after cardiac surgery. J Am Soc Nephrol. 2014;25:1063–1071. doi: 10.1681/ASN.2013070742. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Parikh CR, Thiessen-Philbrook H, Garg AX, Kadiyala D, Shlipak MG, Koyner JL, Edelstein CL, Devarajan P, Patel UD, Zappitelli M, Krawczeski CD, Passik CS, Coca SG. Performance of kidney injury molecule-1 and liver fatty acid-binding protein and combined biomarkers of AKI after cardiac surgery. Clin J Am Soc Nephrol. 2013;8:1079–1088. doi: 10.2215/CJN.10971012. [DOI] [PMC free article] [PubMed] [Google Scholar]