Abstract
Objective To examine the efficacy of counselor-assisted problem solving (CAPS) in improving long-term caregiver psychological functioning following traumatic brain injury (TBI) in adolescents. Methods This randomized clinical trial compared CAPS (n = 65), a predominantly online problem-solving intervention, with an Internet resource comparison (n = 67) program. Families of adolescents with TBI completed a baseline assessment and follow-up assessments 6, 12, and 18 months later. General linear mixed models were used to examine longitudinal changes in caregiver global psychological distress, depressive symptoms, and caregiving self-efficacy. Family income and injury severity were examined as moderators of treatment efficacy. Results Family income moderated long-term changes in caregiver psychological distress. For lower-income caregivers, the CAPS intervention was associated with lower levels of psychological distress at 6, 12, and 18 months post baseline. Conclusions These findings support the utility of Web-based interventions in improving long-term caregiver psychological distress, particularly for lower-income families.
Keywords: caregiver outcomes, psychopathology, traumatic brain injury
Pediatric traumatic brain injury (TBI) has been associated with persistent, long-term caregiver psychological distress, including anxiety and depression (Wade et al., 2002; Wade, Taylor, Drotar, Stancin, & Yeates, 1998). Caregiver psychological distress (Taylor et al., 2001, 2002) and psychopathology (Connell & Goodman, 2002) impact the development and maintenance of childhood behavior problems, suggesting that caregiver functioning may be relevant to the child’s long-term behavioral functioning.
Caregiver psychological distress may be related to increased family burden and distress that often occur following pediatric TBI (Stancin et al., 2010; Wade et al., 1998, 2014). Family burden and distress have been shown to be higher following severe injury (Anderson et al., 2001; Wade et al., 2002). Aitken and colleagues (2009) reported that in the initial year following pediatric TBI, caregivers reported substantial burden, including increased worry and interference with daily routine. Although other investigators failed to find initial post-injury differences between caregivers of children with TBI and those of children with orthopedic injury, they reported greater long-term caregiver distress and burden for children with severe TBI than for those with either mild-to-moderate TBI or orthopedic injury (Wade et al., 2002). These studies indicate that pediatric TBI results in family and caregiver distress that persists long-term and varies as a function of injury severity and time since injury.
With increasing awareness of the adverse consequences of TBI for families (Aitken et al., 2009; Grados et al., 2008; Wade et al., 2004, 2002), recent research has examined the efficacy of problem-solving interventions to remediate caregiver burden (Gan, Gargaro, Kreutzer, Boschen, & Wright, 2010; Kreutzer et al., 2009). Problem-solving therapy provides a structured, yet flexible, approach for addressing the changes in family dynamics that are often present after TBI (D’Zurilla & Nezu, 2006). Prior research has established the efficacy of Web-based intervention for use in pediatric populations that are characterized by neurocognitive deficits, including pediatric epilepsy (Glueckauf et al., 2002; Hufford, Glueckauf, & Webb, 1999). Previous studies that examined adolescent outcomes following the randomized clinical trial (RCT) described below reported that the intervention was effective in reducing post-TBI externalizing behavior problems and executive dysfunction (Kurowski et al., 2013; Wade, Stancin, et al., 2014) and in improving meta-cognitive skills (Karver et al., 2013). Similar Web-based problem-solving interventions were also effective in alleviating short-term caregiver depression and psychological distress (Wade, Carey, & Wolfe, 2006). However, further research is needed to determine the long-term efficacy of this approach to family intervention.
Emerging evidence underscores the importance of considering moderators of treatment response. In a recent study that investigated outcomes following a previous iteration of a Web-based intervention for adolescents with TBI, caregivers of lower socioeconomic status (SES) benefited more from a Web-based problem-solving intervention, whereas caregivers of higher SES benefited more from access to Internet resources alone (Wade et al., 2012). Caregiver self-efficacy, or the caregiver’s belief about the ability to effectively care for their child’s needs, may also be relevant when considering post-TBI caregiver outcomes. An earlier publication that examined data from the RCT described below reported that short-term improvements in caregiving self-efficacy following the Web-based intervention were greatest among caregivers who were non-computer users prior to the treatment (Wade, Karver, et al., 2014). The moderating effect of computer usage supports prior research suggesting that Web-based problem-solving interventions may be most effective in families with fewer resources (Wade et al., 2006, 2010, 2012). Although short-term caregiver functioning following this RCT has been examined (Wade, Karver, et al., 2014), maintenance of treatment effects over time has not yet been examined.
Despite growing support for the efficacy of family problem-solving therapy in reducing caregiver distress and depression and increasing caregiving self-efficacy in the short-term (Carey, Wade, & Wolfe, 2008; Wade et al., 2012; Wade, Karver, et al., 2014), it is unclear if these positive changes persist over time. Therefore, the primary aim of this study was to examine changes in caregiver psychological distress, depression, and caregiving efficacy, over the initial 18 months following an online family problem-solving intervention referred to as counselor-assisted problem solving (CAPS). Treatment efficacy was assessed compared with an Internet resources comparison (IRC) condition involving provision of Internet resources alone. We hypothesized that the CAPS intervention, compared with the IRC, would result in a greater reduction in caregiver psychological distress and depressive symptoms and a greater increase in caregiving efficacy. Consistent with prior research suggesting that individuals with greater pre-injury vulnerabilities evidence greater response to post-TBI intervention (Wade et al., 2006, 2010; Wade, Karver, et al., 2014), we further hypothesized that severe TBI and lower family income would be associated with greater long-term response to the CAPS intervention. Finally, it is anticipated that caregiver psychological distress will decrease and caregiver self-efficacy would increase with greater time since the baseline assessment, given that caregiver distress is greatest in the initial months (Wade et al., 1998, 2002).
Method
Participants
The trial was registered with clinicaltrials.gov, assigned identifier: NCT00409448. Participants were recruited via the Trauma Registries of five major trauma-centers in the Central and Western regions of the United States. The study extended from initiation of enrollment in March 2007 to completion of the final assessment in September 2012. The study was approved by the institutional review board of each of the participating medical centers. Eligibility requirements included age 12–17 years and overnight hospitalization for a complicated mild-to-severe TBI within the previous 1–7 months. Based on the lowest documented Glasgow Coma Scale score (GCS; Teasdale & Jennett, 1974), adolescents were classified as having complicated mild TBI (lowest GCS score of 13–15 accompanied by abnormality on neuroimaging), moderate TBI (lowest GCS score of 9–12), or severe TBI (GCS score <9). The first two injury severity categories were combined into a single moderate TBI group for this study.
Additional eligibility requirements included English as the primary language spoken in the home, availability of the adolescent to participate in the intervention, and family residence within a 3-hr drive of the hospital. Exclusion criteria included: (1) insufficient child recovery by 6 months post injury to participate in the intervention (e.g., minimally responsive state), (2) psychiatric hospitalization for either child or parent during the year prior to the injury, (3) family residence in an area without high-speed Internet access, (4) child residence outside the home (e.g., detention facility), and (5) diagnosis of intellectual disability (IQ < 65) prior to the injury. Seventeen percent (52/308) of those screened were ineligible for one or more of these reasons, with a primary language other than English constituting the most common reason for exclusion. Additional information about recruitment is available in the paper by Wade, Karver, and colleagues (2014).
Participants were randomly assigned to a 6-month Internet-based intervention (either CAPS or IRC, see below). Randomization was stratified by gender and race to ensure equivalent group composition on these factors. A sealed envelope containing group assignment was handed to the participants at the end of the baseline visit, allowing interviewers to remain naïve to group assignment.
Table I summarizes sample characteristics for the two groups. Details regarding participant retention, including reasons for attrition (i.e., lost to follow-up or declined continued participation in the study), are provided in the CONSORT flowchart (Supplementary Figure), with greater detail provided in the paper by Blaha and colleagues (2015). Group comparisons failed to reveal differences in attrition rates, family income, lowest GCS score, gender, or race. The mean age at injury was 14.40 (SD = 1.68) for the CAPS group and 14.67 (SD = 1.77) for the IRC group. Mean time from injury to the initial (baseline) assessment in years was .30 (SD = .15) and .29 (SD = .13), respectively (p > .05). As part of the baseline interview, caregivers were asked if the participating child was receiving behavioral therapy or counseling services outside of that provided by the study. Participants who were receiving outside services included 15 (22.3%) in the IRC and 16 (24.6%) in CAPS at baseline, 15 (23.4%) in the IRC and 11 (18.0%) in CAPS at 6 months, 14 (22.9%) in IRC and 10 (19.2%) in CAPS at 12 months, and 12 in the IRC (22.2%) and 10 in CAPS (22.2%) at 18 months. At all time points, receipt of behavioral therapy or counseling services did not differ by group and was not associated with injury severity or family income (p > .05).
Table I.
Sample Characteristics
| Variable | Baseline | 6 months | 12 months | 18 months | |
|---|---|---|---|---|---|
| N | CAPS | 65 | 61 | 52 | 45 |
| IRC | 67 | 64 | 61 | 54 | |
| % lost to attrition | CAPS | – | 6.1% | 14.7% | 13.4% |
| IRC | – | 4.4% | 4.6% | 11.4% | |
| Income (% in each range) | CAPS | $30–59,000 = 35.3 | $30–59,000 = 34.3 | $30–59,000 = 26.9 | $30–59,000 = 26.6 |
| $60–79,000 = 35.3 | $60–79,000 = 34.3 | $60–79,000 = 34.6 | $60–79,000 = 35.5 | ||
| $80–99,000 = 15.3 | $80–99,000 = 17.3 | $80–99,000 = 20.2 | $80–99,000 = 20.0 | ||
| $ > 100,000 = 13.8 | $ > 100,000 = 14.1 | $ > 100,000 = 16.3 | $ > 100,000 = 17.7 | ||
| IRC | $30–59,000 = 38.8 | $30–59,000 = 39.0 | $30–59,000 = 38.7 | $30–59,000 = 32.4 | |
| $60–79,000 = 38.8 | $60–79,000 = 37.5 | $60–79,000 = 36.1 | $60–79,000 = 38.8 | ||
| $80–99,000 = 14.9 | $80–99,000 = 15.6 | $80–99,000 = 15.7 | $80–99,000 = 18.5 | ||
| $ > 100,000 = 7.4 | $ > 100,000 = 7.8 | $ > 100,000 = 7.5 | $ > 100,000 = 9.2 | ||
| Lowest GCS | CAPS | 10.08 (4.84) | 10.05 (4.87) | 9.80 (5.05) | 9.88 (5.11) |
| Mean (SD) | IRC | 10.03 (4.32) | 9.91 (4.34) | 9.92 (4.14) | 9.52 (4.39) |
| Child’s race (% in each category) | CAPS | White = 80.0 | White = 77.0 | White = 80.7 | White = 86.8 |
| Black = 10.7 | Black = 11.5 | Black = 9.6 | Black = 4.4 | ||
| Multiracial = 9.3 | Multiracial = 11.5 | Multiracial = 9.6 | Multiracial = 8.8 | ||
| IRC | White = 80.6 | White = 81.2 | White = 80.3 | White = 83.3 | |
| Black = 16.4 | Black = 17.1 | Black = 18.0 | Black = 14.8 | ||
| Multiracial = 2.9 | Multiracial = 1.5 | Multiracial = 1.6 | Multiracial = 1.8 | ||
| Child’s gender (% male) | CAPS | 67.6 | 70.0 | 68.0 | 66.6 |
| IRC | 62.6 | 64.0 | 69.0 | 64.1 | |
| Child’s age Mean (SD) | CAPS | 14.70 (1.67) | 15.23 (1.69) | 15.66 (1.66) | 16.19 (1.71) |
| IRC | 14.99 (1.76) | 15.56 (1.77) | 16.10 (1.84) | 15.51 (1.87) | |
| Caregiver gender (% female) | CAPS | 92.3 | 91.6 | 92.3 | 91.4 |
| IRC | 88.0 | 87.5 | 88.5 | 90.7 | |
| Caregiver race (% in each category) | CAPS | White = 84.6 | White = 81.9 | White = 86.5 | White = 88.8 |
| Black = 10.7 | Black = 11.4 | Black = 9.6 | Black = 6.6 | ||
| Multiracial = 4.6 | Multiracial = 6.6 | Multiracial = 3.8 | Multiracial = 4.4 | ||
| IRC | White = 83.5 | White = 82.8 | White = 81.9 | White = 85.1 | |
| Black = 16.4 | Black = 17.1 | Black = 18.0 | Black = 14.8 | ||
| Caregiver age Mean (SD) | CAPS | 41.90 (7.34) | 42.05 (7.44) | 42.55 (7.62) | 43.00 (7.51) |
Note. CAPS = counselor-assisted problem solving; IRC = Internet resources comparison; GCS = Glasgow Coma Scale.
Forty (59.7%) primary caregivers in the IRC group and 42 (64.6%) in the CAPS group were married. In the IRC group, primary caregivers included 57 biological mothers (85.0% of families), 8 biological fathers (11.9%), and 2 grandmothers (2.9%). In the CAPS group, caregivers included 57 biological mothers (87.6%), 1 stepmother (1.5%), 2 adoptive mothers (3.0%), 5 grandmothers (7.6%), 2 biological fathers (3.0%), and 1 other relative (1.5%).
The groups were well-matched for pre-intervention computer use (response to the baseline assessment question, “In the last week, how many hours did you spend using a computer”). Prior to the intervention, 35 families (61%) in the CAPS group reported regular computer usage as defined by 5 or more hours per week compared with 41 (65%) in the IRC group. Seventy-three percent of CAPS and 83% of the IRC caregivers reported having a computer in the home prior to treatment. Chi-squared analyses failed to reveal a significant (p < .05) group difference in pre-intervention computer use. Comparison of families who completed the final (18-month) follow-up with those who dropped out prior to this assessment also failed to reveal differences for any of the above characteristics.
Procedures and Interventions
After obtaining informed consent from the parents and assent from the adolescent, study personnel completed the baseline/pre-treatment assessment at the family’s home. During this assessment, the primary caregiver provided information about demographic characteristics and completed self-report measures of psychological distress, depression, and caregiving efficacy. All participants received new computers and Web cameras and high-speed Internet access. The estimated cost for computer equipment and high-speed Internet access for the duration of the intervention period was 1,000 USD per family. After installing the computer equipment and Internet access, families were shown how to log onto the study Web site and access the Web-based TBI resources. Follow-up assessments were conducted in families’ homes at approximately 6, 12, and 18 months post-baseline. Follow-up assessments included an interview with the primary caregiver and completion of the self-report measures that were administered at the baseline assessment (described below). Research assistants collecting these data were naïve to group assignment. To equate the time between baseline and follow-up assessments between groups and to maintain concealment of group assignment, follow-up assessments were scheduled without knowledge regarding completion of the treatment protocol. As a consequence, follow-up sessions were conducted as scheduled at 6, 12, and 18 months for eight families that had not completed the core sessions until after the 6-month follow-up.
As also reported in Wade, Karver, and colleagues (2014), the amount of time engaged in the intervention did not differ by group. Reported time spent on intervention-related Web sites was 30 minutes or less for 43% and 48% of the CAPS and IRC families, and between 30 min and 2 hr for 50% and 47%, respectively. Participants in the CAPS group completed an average of 7.23 sessions by the 6-month follow-up (range: 0–13), with all but eight participants (12%) completing four or more sessions. Time to completion of the follow-up assessments did not differ by group (p > .05).
CAPS Condition
Families in the CAPS condition were provided a family problem-solving intervention that focused on training in problem solving, communication skills, self-regulation, and anger management (Wade, Karver, et al., 2014). After completing an initial, 2-day training program, the CAPS treatment was delivered by four licensed clinical psychologists (three Caucasian females and one Caucasian male who had been licensed an average of 3.25 years, range of 0–7 years, at the start of the study period). Session objectives were outlined in a detailed treatment manual and reviewed during weekly supervision calls to maintain treatment fidelity. Supervision was provided by two Caucasian females who had been licensed 18 and 20 years, respectively, at the start of the study period. To document adherence to and any deviations from specified content, both the psychologist and participating caregivers completed end-of-session checklists.
As described in further detail by Wade, Karver, et al., 2014, the initial CAPS session involved a face-to-face meeting in the family’s home to identify goals that the family wanted to address as part of the intervention. The adolescent with TBI and one caregiver were required to attend each core session; secondary caregivers and school-age siblings, when present in the home, were encouraged to participate. Among married CAPS caregivers, only the primary caregiver participated in 21 (50%) families and both the primary and secondary caregivers participated in the other 21 families. Subsequent to the initial Skype session with the therapist, each CAPS session consisted of a didactic online module that the family completed without the psychologist’s assistance. After reviewing the modules, the family and therapist participated in a Skype session, at which time they discussed the module and ways to implement the problem-solving process around the family’s goal(s). The intervention was designed to be completed over a 6-month period with weekly online modules and Skype sessions for the first 2–3 weeks and then bi-weekly completion of modules and Skype sessions until the family completed the initial seven core online modules. During session 7, participating parents completed a measure of family burden and a self-assessment of family problem-solving and communication skills. The psychologist used this self-assessment to identify the need for additional, supplemental modules and sessions to address unresolved family concerns. Families received up to four supplemental modules and sessions and a final module and session to review progress and develop a plan for addressing future problems.
Internet Resources Comparison
The IRC was a self-guided, information-based program that provided families with access to Web-based resources about TBI. To keep the interviewers unaware of group assignment, families in the IRC also received computers and Web cameras. Families were instructed to access a home page with links to online resources including local, state, and national brain-injury associations and sites focusing on pediatric brain injury (e.g., Center on Brain Injury Research and Training, Brain Injury Partners, and the National Database of Educational Resources on TBI). Families were encouraged to spend at least 1 hr per week accessing this information throughout the 6-month intervention period and were asked to track the sites that were visited.
Measures
To assess global psychiatric symptoms and distress, caregivers completed the Global Severity Index (GSI) of the Symptom Checklist-90-R (SCL-90-R).The SCL-90-R is a 90-item self-report inventory that assesses a range of clinical symptomatology including depression (e.g., depressed mood, social withdrawal) and anxiety (e.g., somatic symptoms of anxiety, symptoms of social anxiety). The SCL-90-R has well-documented reliability and validity and is sensitive to the presence of significant psychological distress. The SCL-90-R GSI is reported as a T-score with a mean of 50 and a standard deviation of 10. Scores greater or equal to 63 are considered to be indicative of clinically significant levels of distress (Derogatis & Lazarus, 1994). Cronbach’s alpha across the four time points indicated that this measure was highly reliable (α = .97).
Caregivers also completed the Center for Epidemiologic Studies Depression Scale (CES-D), a 20-item inventory that provides an assessment of specific symptoms of depression. For this measure, caregivers rated the frequency of depressive symptoms over the past week, including depressed mood and social withdrawal. The CES-D has well-established psychometric properties, including high internal consistency, adequate test–retest reliability, and high degree of reliability and validity. Validations studies further suggest that the CES-D has a high correspondence with clinical ratings of depressive symptoms and is useful for screening individuals at risk for developing clinical depression. A raw score of 16 or greater indicates clinically significant depressive symptoms (Radloff, 1977). Cronbach’s alpha across the four time points indicated that the measure was highly reliable (α = .92).
The total score from the Caregiver Self-Efficacy Scale (CSES) served as a measure of self-perceived parenting efficacy. The CSES is 50-item parent-report scale with demonstrated reliability and validity. For the CSES, higher scores indicate greater perceived caregiving self-efficacy (Bothroyd, 1997). Because the CSES has no established criteria for determining clinical significance, proportions of participants with clinically elevated scores were not reported for this measure. Cronbach’s alpha across the four time points revealed the measure to be highly reliable (α = .93).
Analyses
General linear mixed-models analysis was used to examine caregiver outcomes longitudinally across the four assessments. The primary advantage of the mixed-models approach is the ability to incorporate estimates of intra-subject correlations across repeated assessments, making it useful for longitudinally examining changes in caregiver outcomes following the CAPS intervention. The mixed-models approach also allows for inclusion of data from all participants, even if some participants were not seen at every assessment, and does not require equal intervals between assessments.
Factors in the mixed-models analyses were treatment condition (CAPS or IRC), TBI severity (complicated mild to moderate vs. severe), time since baseline (TSBASE: 6, 12, and 18 months), and family income. Consistent with previous pediatric TBI research, family income was estimated based on the median income for the zip code of the adolescent’s primary residence (Chapman et al., 2010; Collins et al., 2014; Karver et al., 2012). Interactions were included in the models to explore differences between the two treatment conditions over time and moderating effects of TBI severity and income. Initial models were trimmed by eliminating nonsignificant higher- and then lower-level interactions. Main effects for family income and injury severity were retained even if nonsignificant. Use of backwards manual elimination of nonsignificant factors is consistent with previous research (Karver et al., 2013; Taylor et al., 2002; Van der Heijden, Donders, Stijen, & Moons, 2006; Wade, Karver, et al., 2014) and has been suggested to increase the numerical stability and generalizability of results (Hegewald, Pfahlberg, & Uter, 2003). The standard error (SE) represents variance in the model. The standardized beta (β) indicates change in the outcome variable per one standard deviation increase in the independent variable, controlling for covariates. The unstandardized (B) represents change in raw units. For the final estimation of each model, standardized estimates (β) were reported as a measure of effect size and R2 was reported to show the variance explained for each model. These measures have the advantage of offering a corrected estimate of overall goodness of fit for the model as well as for the individual predictors (Ferguson, 2009).
Generalized estimating equations (GEEs) were used to examine changes in clinically significant elevations on the SCL-90-R GSI and CES-D over the course of the study period. Factors included in the GEE analysis were treatment condition, injury severity, TSBASE, and family income. Interactions were included to explore differences between the two treatment conditions over time and moderating effects of TBI severity and income. Initial models were trimmed by eliminating nonsignificant higher- and then lower-level interactions. Inclusion of these factors allowed for examination of group differences in changes in rates of clinically significant elevations over the course of the study period while also examining the moderating influence of injury severity and family income. To assess for clinically meaningful change from baseline, Reliable Change Index (RCI) was calculated using the algorithm presented by Temkin et al. (1999). Respondents having an RCI of less than −1.64 were considered to be evidencing clinically meaningful improvement. Use of this criterion is consistent with other studies examining outcomes following pediatric TBI (Yeates et al., 2012).
Results
Findings From Mixed-Models Analysis
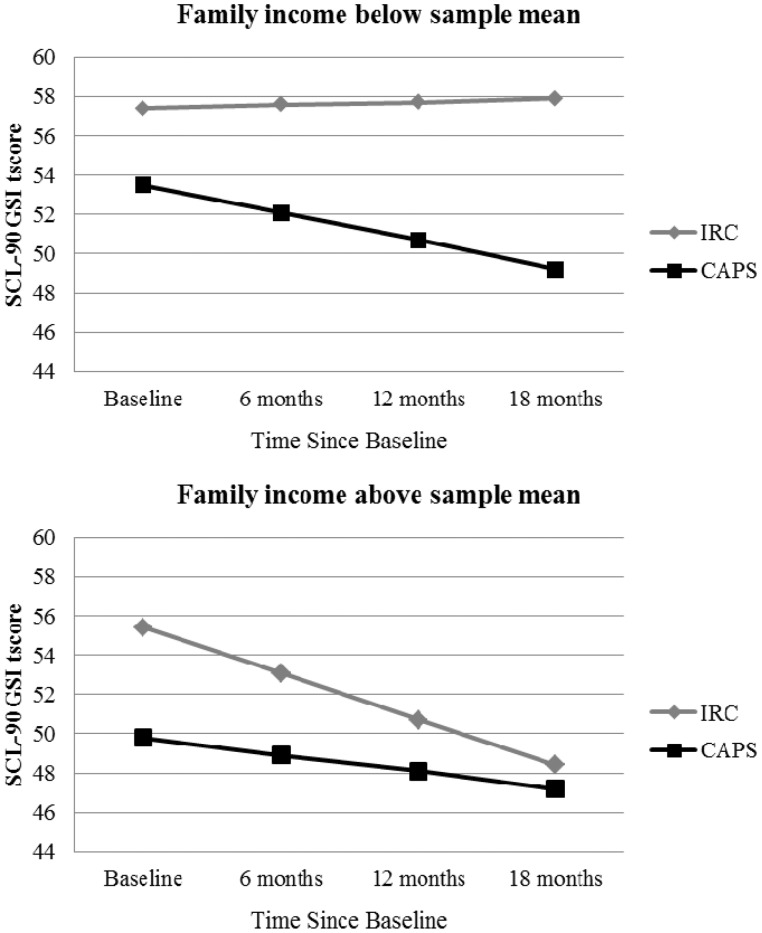
Mixed-model analysis of the SCL-90-R GSI revealed a significant interaction of group, family income, and TSBASE (F(1, 299) = 5.70, p = .02), with R2 = .14. Post hoc analyses revealed significantly lower global distress levels in the CAPS group relative to the IRC group at the 6-month (p = .04), 12-month (p = .01), and 18-month (p = .004) visits for lower-income participants. The final estimate of the model is reported in Table II and Figure 1. The untrimmed model is reported in the Supplementary Table. At 6 months (β = .45) and 12 months (β = 0.58), lower-income CAPS caregivers differed from lower-income IRC caregivers by approximately ½ standard deviation. This trend continued at 18 months, at which time lower-income CAPS and IRC caregivers differed by more than 2/3 of a standard deviation (β = 0.71). RCI analyses indicated that group differences in the lower-income participants did not meet the threshold for reliable change.
Table II.
Multivariate Regression Results
| Dependent measure | Effect | β | B | SE | t | p |
|---|---|---|---|---|---|---|
| SCL-90-R GSI | Group | .40 | 4.82 | 2.07 | 2.34 | .02* |
| Income | −.15 | −1.88 | 1.30 | −1.44 | .15 | |
| Injury severity | −.24 | −2.87 | 1.94 | −1.48 | .14 | |
| TSBASE | −.19 | −2.27 | .86 | −2.64 | .009** | |
| Group × income × TSBASE | −.25 | −3.07 | 1.29 | −2.39 | .02* | |
| Group differences, low income | ||||||
| Baseline | .33 | 3.97 | 2.82 | 1.41 | .16 | |
| 6 months | .45 | 5.53 | 2.60 | 2.13 | .04* | |
| 12 months | .58 | 7.09 | 2.65 | 2.68 | .01* | |
| 18 months | .71 | 8.65 | 2.97 | 2.92 | .004** | |
| Group differences, high income | ||||||
| Baseline | .46 | 5.68 | 3.23 | 1.76 | .08 | |
| 6 months | .34 | 4.17 | 2.98 | 1.40 | .16 | |
| 12 months | .22 | 2.66 | 2.98 | .89 | .37 | |
| 18 months | .09 | 1.16 | 3.24 | .36 | .72 | |
| R2 = .10 | ||||||
| CES-D | Group | .20 | 2.15 | 1.56 | 1.38 | .17 |
| Injury severity | −.43 | −4.56 | 1.79 | −2.55 | .01* | |
| Income | −.25 | −2.66 | .81 | −3.28 | .001** | |
| TSBASE | −.19 | −2.02 | .84 | −2.40 | .02* | |
| TSBASE × injury severity | .32 | 3.43 | 1.10 | 3.12 | .002** | |
| Differences by injury severity | ||||||
| Baseline | −.43 | −4.56 | 1.79 | −2.55 | .01* | |
| 6 months | −.27 | −2.85 | 1.62 | −1.75 | .08 | |
| 12 months | −.11 | −1.13 | 1.63 | −.69 | .49 | |
| 18 months | .06 | .58 | 1.82 | .32 | .75 | |
| R2 = .03 | ||||||
| CSES | Group | −.32 | −3.17 | 1.39 | −2.28 | .02* |
| Income | .11 | 1.11 | .71 | 1.56 | .12 | |
| TSBASE | −.06 | −.57 | .62 | −.95 | .34 | |
| R2 = .10 | ||||||
Note. Injury severity = complicated mild to moderate compared with severe TBI
*Significant at .05 alpha level.
**Significant at .01 alpha level.
TSBASE = time since baseline; SCL-90 = Symptom Checklist-90; CES-D = Center for Epideologic Studies-Depression; CSES = Caregiver Self-efficacy Scale.
Figure 1.
Mean estimates of interaction of group, income, and injury severity with SCL-90-R GSI as the dependent measure.
Note. IRC = Internet resources comparison; CAPS = counselor-assisted problem solving; SCL-90 = Symptom Checklist-90
Analysis of the CES-D revealed a significant interaction of injury severity and TSBASE (F(1, 310) = 9.73, p = .002) with R2 = .03. Examination of least square mean estimates indicated that initially higher levels of depressive symptoms among caregivers of adolescents with severe TBI at the baseline visit (p = .01) diminished and became nonsignificant over time. There was also a significant main effect of family income (p = .001), with lower income associated with higher depression. The final estimate of the model is reported in Table II and Figure 2. The untrimmed model is reported in the Supplementary Table.
Figure 2.
Mean estimates of interaction of injury severity and time with CES-D as the dependent measure.
Note. Mean estimates indicated significant group differences at baseline (p = .01) with the remaining contrasts nonsignificant (p > .05). See Table II. CES-D = Center for Epidemiologic Studies-Depression.
Examination of the CSES indicated a main effect for treatment group (F(1, 126) = 5.21, p = .02), with the CAPS group scoring higher on this measure than the IRC group. The final estimate of the model is reported in Table II. The untrimmed model is reported in the Supplementary Table. The absence of an interaction of treatment with time (i.e., change relative to baseline) suggests a preexisting group difference rather than a differential effect of the two treatments.
To explore the possibility that treatment effects were moderated by the number of sessions completed, we conducted an exploratory analysis within the CAPS group. Mixed-model analyses were again conducted with number of sessions completed included as a factor. We also examined interactions of number of sessions completed with family income, injury severity, and TSBASE. For all dependent measures, main effects of number of sessions completed and interactions were nonsignificant (p > .05).
Findings From GEE Analysis
The proportions of caregivers with clinically significant elevations on the SCL-90-R GSI and CES-D are reported in Table III. On the SCL-90-R GSI, rates of clinically significant psychological distress were 21.5% at baseline and 11.1% at 18 months for the CAPS group and 29.9% at baseline and 24.5% at 18 months for the IRC group. On the CES-D, rates of clinically significant depressive symptoms were 29.2% at baseline and 17.8% at 18 months for the CAPS group and 35.8% at baseline and 32.1% at 18 months for the IRC group. These group differences were not significant.
Table III.
Self-Reported Caregiver Psychological Distress, Depression, and Caregiving Self-Efficacy
| Baselinea | 6 monthsa,b,c | 12 months | 18 months | ||
|---|---|---|---|---|---|
| SCL-90 | CAPS | 52.3 (11.2), [22.9%] | 47.8 (12.5), [14.2%] | 50.7 (12.1), [22.4%] | 46.6 (11.8), [12.5%] |
| IRC | 57.4 (10.3), [31.2%] | 53.9 (12.0), [25.8%] | 53.9 (13.0), [30.1%] | 53.1 (12.0), [27.6%] | |
| CES-D | CAPS | 11.4 (8.7), [30.1%] | 11.1 (9.3), [31.0%] | 11.9 (11.7), [26.0%] | 8.9 (8.9), [19.0%] |
| IRC | 13.8 (9.7), [37.5%] | 15.4 (11.7), [34.9%] | 12.8 (11.8), [35.8%] | 13.6 (11.1), [34.6%] | |
| CSES | CAPS | 90.1 (7.4) | 91.9 (7.2) | 90.5 (9.4) | 91.0 (10.8) |
| IRC | 87.1 (10.8) | 87.2 (10.7) | 87.0 (10.7) | 86.9 (11.8) |
Note. Mean (SD), [Proportion clinically elevated]. Clinical elevation defined as t ≥ 63 for GSI and raw score ≥ 16 for the CES-D.
aSignificant group differences on the GSI.
bSignificant group difference on the CES-D.
cSignificant group difference of the CSES.
GSI = Global Severity Index from SCL-90-R; CES-D = Centers for Epidemiological Studies-Depression scale; CSES = Caregiver Self-efficacy Scale; IRC = Internet resources comparison; CAPS = counselor-assisted problem solving.
Results from analyses using GEE suggested that rates in clinically significant elevations over the course of the study period did not differ between the CAPS and IRC groups (p > .05). Neither injury severity nor family income moderated the relationship between the intervention received and rates of clinically significant global distress or depressive symptoms (p > .05).
Discussion
In this study, we reported findings from a large clinical trial examining the efficacy of online family problem-solving therapy in reducing caregiver distress and depression and promoting caregiver efficacy over the initial 24 months following TBI in adolescents. Specifically, we aimed to explain long-term changes in caregiver functioning and to identify moderators of treatment efficacy, including family income, injury severity, and time since the initial baseline assessment. Results of this study suggest that the CAPS intervention promoted long-term reductions in psychological distress, but had minimal effects on caregiving depressive symptoms and caregiving self-efficacy. The CAPS intervention was particularly effective in reducing caregiver psychological distress in lower-income caregivers. Although effect sizes among lower-income participants were moderate, they did not meet the threshold for reliable change.
Consistent with study hypotheses, family income moderated the efficacy of the CAPS treatment in promoting long-term reductions in caregiver psychological distress. For lower-income caregivers, the Web-based, therapist-supported CAPS intervention, compared with the information-based IRC intervention, was associated with significantly lower levels of caregiver psychological distress at 12 and 18 months post-baseline. By suggesting that interventions that offer therapist support and scaffolding may be particularly effective for lower-income caregivers, these findings are consistent with prior work indicating that families who are most vulnerable to negative post-TBI outcomes may benefit the most from a therapist-supported, post-TBI intervention (Wade et al., 2006, 2010, 2012). Lower-income families may have fewer resources to facilitate post-TBI recovery and adjustment, whereas higher-income families have more resources and thus less potential to benefit from the supports provided by the CAPS intervention.
Also consistent with study hypotheses and prior research documenting caregiver distress and burden following pediatric TBI (Anderson et al., 2001; Wade et al., 1998, 2014), caregivers of adolescents with severe TBI reported greater depressive symptoms at baseline than caregivers of adolescents with moderate TBI. However, contrary to expectations of increasingly negative outcomes of severe TBI over time (Wade et al., 2002), differences between the severe and moderate TBI groups were not maintained across follow-up assessments. From a clinical perspective, the diminishing effects of TBI severity raises the possibility that post-TBI interventions offered soon after injury, such as those provided by CAPS and IRC, may be more beneficial for families of adolescents with severe TBI than those with less severe injuries.
Contrary to study hypotheses, CAPS did not reduce symptoms of depression as assessed by the CES-D. The lack of normative corrections for the CES-D (i.e., raw scores rather than standardized scores that are corrected for age or other demographic characteristics) may limit sensitivity of this measure to change over time. Alternatively, measures that assess only depressive symptoms may lack sensitivity to the range of symptoms experienced by caregivers following TBI. Measures that more comprehensively assess psychopathology, such as the SCL-90-R GSI, may be more sensitive to caregiver psychological distress and post-intervention improvements.
Group differences in changes over follow-up in the SCL-90-R GSI were not accompanied by differences in rates of more substantial change as reflected in the RCI or in rates of scores exceeding clinical cutoffs. This lack of significant findings may be attributable to the low levels of baseline problems, which may have limited our ability to detect intervention-related improvements. Alternatively, these findings may suggest that the effects of CAPS relative to the IRC condition on symptoms of psychological distress were relatively small and comprised changes in sub-clinical symptom levels rather a reduced rate of clinical disorders. Because the proportions of parents with clinically significant elevations for the sample as a whole were substantially higher than estimated rates of psychological distress and depression in the general adult population in the United States (3.2% and 6.8%, respectively, according to Reeves et al., 2011), this may not be because of a lack of opportunity to observe clinically meaningful gains, but may instead imply that the benefits of CAPS compared with the IRC condition were relatively subtle. The influence of caregiver self-efficacy on parent psychological functioning has been documented by previous research on parent and child adjustment in both typically developing children (Jones & Prinz, 2004) and children with neurocognitive disorders (Hastings & Brown, 2002), including TBI (Wade et al., 2014). These findings indicate that interventions that bolster caregiving efficacy may be important for long-term adjustment following TBI (Wade et al., 2014). Contrary to expectations, the findings of this study failed to document an interaction of treatment with time, suggesting the presence of a preexisting group difference on the CSES rather than a differential effect of the two treatments. In explaining this lack of support, it is possible that participation in CAPS made parents more aware of limitations in parenting skills, which may have obscured any positive effects of the intervention. As another explanation, this study did not include an assessment of mastery of intervention-related skills or the extent to which they were applied. If included, such an assessment may have contributed to improved caregiving self-efficacy resulting from increased awareness of improvements in skill.
One of the study’s most important limitations is that the treatment groups were not equated for therapist attention, thus the greater effectiveness of CAPS relative to the IRC condition may have been due to this factor rather than program content. While it can be concluded that the CAPS intervention was more beneficial than access to Internet resources alone in improving caregiver psychological distress following TBI, particularly among lower-income families, we are unable to conclude that CAPS is superior to other interventions that offer therapist support. Reliance on self-report measures is another critical limitation; eliciting the perspective of a significant other or secondary caregiver would have provided a potentially less biased or more objective assessment of the caregiver. A related concern is the lack of assessment of pre-morbid caregiver functioning. Because intervention efficacy may be expected to be greater for individuals with lower pre-morbid functioning, lack of statistical control for baseline functioning may have obscured the effects of the interventions on subsequent caregiver outcomes. Additional concerns include the requirement that the family residence must be in an area with high-speed Internet access may have resulted in families living in rural areas being underrepresented. Requiring English as the language spoken by the family may have constrained sample diversity, limiting generalizations of findings to broader populations. Although census information has been used in previous research to determine family sociodemographic characteristics (Chapman et al., 2010; Collins et al., 2014; Karver et al., 2012), other authors have reported that zip code is only moderately correlated with income data from individual families (Deonandan, Campbell, Ostbye, Tummon, & Robertson, 2000). Our estimates of family income may therefore have been relatively imprecise. Additionally, randomization to the two intervention groups was not stratified by TBI severity, although TBI severity was included in analysis and the groups did not differ significantly in mean GCS scores. Finally, the approach to assessing treatment fidelity to the CAPS intervention may be vulnerable to bias both on the part of the therapist and untrained caregivers who may be unable to offer reliable evaluations of treatment fidelity. Future studies should therefore use other methods for assessing treatment fidelity, such as video or audio-taped sessions that are evaluated by an independent rater.
Future research is needed to investigate the optimal number of CAPS sessions. In a post-intervention satisfaction survey as part of this study, seven caregivers (12.2% of those who completed the survey) agreed or strongly agreed that the CAPS intervention was too long. Six (10.3%) agreed or strongly agreed that it was too short. While these findings suggest that the CAPS intervention was an appropriate length based on caregiver satisfaction, it is unknown if treatment efficacy differs by dose of intervention and if the optimal number of sessions is related to family- and injury-related factors, such as family income and injury severity. With this knowledge, future research could develop a screening tool that could be used to determine the optimal number of sessions based on family- and injury-related factors. There is also a need for research targeting the efficacy of Web-based interventions for families who live in rural areas and lower-income families. A focus on these families is especially important in view of findings from this study and previous work (Wade et al., 2006, 2010, 2012) that suggests that efficacy of post-TBI interventions is related to family income. There is also a need for research that examines moderators of Web-based interventions for youth with TBI, which may include parenting practices, family stressors, and coping style, and seeks to determine the optimal timing and intensity of these treatments. Studies are needed that examine the broader impact of family-based interventions, including outcomes in nonparticipating family members, such as siblings and secondary caregivers.
The current study is among the first to examine the efficacy of Web-based problem-solving intervention with regard to long-term psychological functioning of caregivers of adolescents with complicated mild to severe TBI. These findings contribute to our understanding of long-term changes in caregiver outcomes by demonstrating that long-term treatment efficacy varies as a function of both injury severity and family income. Knowledge of moderators of treatment efficacy affords clinicians the capability to tailor interventions to individuals and their families, thereby increasing ability to offer personally relevant mental health services.
Supplementary Data
Supplementary data can be found at: http://www.jpepsy.oxfordjournals.org/.
Acknowledgments
The authors wish to acknowledge the contributions of Kendra McMullen, Robert Blaha, Elizabeth Hagesfeld, Michelle Jacobs, Daniel Maier, Mary Ann Toth, and Nina Fox in data collection and entry; Jason Stock in data management; John Stullenberger in Web site support; and JoAnne Carey, PsyD, Britt Nielsen, PsyD, and Brad Jackson, PhD.
Funding
This work was supported by grant R01-MH073764 from the National Institute of Mental Health, grant H133G050239 from the National Institute of Disability and Rehabilitation Research, and the Colorado Traumatic Brain Injury Trust Fund Research Program, Colorado Department of Human Services, Division of Vocational Rehabilitation, Traumatic Brain Injury Program.
Conflicts of interest: None declared.
References
- Aitken M. E., McCarthy M. L., Slomine B. S., Ding R., Durbin D. R., Jaffe K. M., Paidas C. N., Dorsch A. M., Christensen J. R., Mackenzie E. J.; CHAT Study Group. (2009). Family burden after traumatic brain injury in children. Pediatrics, 123, 199–206. [DOI] [PubMed] [Google Scholar]
- Anderson V. A., Catroppa C., Haritou F., Morse S., Pentland L., Rosenfeld J., Stargatt R. (2001). Predictors of acute child and family outcome following traumatic brain injury in children. Pediatric Neurosurgery , 34, 138–148. [DOI] [PubMed] [Google Scholar]
- Blaha R. Z., Arnett A. B., Kirkwood M. W., Taylor H. G., Stancin T., Brown T. M., Wade S. L. (2015). Factors influencing attrition in a multi-site randomized clinical trial following traumatic brain injury in adolescence. Journal of Head Trauma Rehabilitation, 30, E33–E40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bothroyd R. A. (1997). Preliminary manual for the caregiver self-efficacy scale. Tampa, FL: Louis de la Parte Florida Mental Health Institute. [Google Scholar]
- Carey J. C., Wade S. L., Wolfe C. R. (2008). Lessons learned: The effect of prior technology use on web-based interventions. Cyberpsychology & Behavior, 11, 188–195. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chapman L. A., Wade S. L., Walz N. C., Taylor H. G., Stancin T., Yeates K. O. (2010). Clinically significant behavior problems during the initial 18 months following early childhood traumatic brain injury. Rehabilitation Psychology, 55, 48–57. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Collins C. L., Yeates K. O., Pommering T. L., Andridge R., Coronado V. G., Gilchrist J., Comstock R. D. (2014). Direct medical charges of pediatric traumatic brain injury in multiple clinical settings. Injury Epidemiology, 1, 1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Connell A. M., Goodman S. H. (2002). The association between psychopathology in fathers versus mothers and children’s internalizing and externalizing behavior problems: A meta-analysis. Psychological Bulletin, 128, 746–773. [DOI] [PubMed] [Google Scholar]
- Deonandan R., Campbell K., Ostbye T., Tummon I., Robertson J. (2000). A comparison of methods for measuring socio-economic status by occupation or postal area. Chronic Disease in Canada, 21, 93–103. [PubMed] [Google Scholar]
- Derogatis L. R., Lazarus L. (1994). SCL-90-R, brief symptom inventory, and matching clinical rating scales. In Maruish M. (Ed.), The use of psychological testing for treatment planning and outcome assessment (pp. 217–248). Hillsdale, NJ: Lawrence Erlbaum. [Google Scholar]
- D’Zurilla T. J., Nezu A. M. (2006). Problem-solving therapies. In Dobson K. S. (Ed.), Handbook of cognitive– behavioral therapies (3rd ed., pp. 211–245). New York, NY: Guilford Press. [Google Scholar]
- Ferguson C. J. (2009). An effect size primer: A guide for clinicians and researchers. Professional Psychology: Research and Practice, 40, 532–538. [Google Scholar]
- Gan C., Gargaro J., Kreutzer J., Boschen K., Wright V. (2010). Development and preliminary evaluation of a structured family system intervention for adolescents with brain injury and their families. Brain Injury, 24, 651–663. [DOI] [PubMed] [Google Scholar]
- Glueckauf R. L., Fritz S. P., Ecklund-Johnson E. P., Liss H. J., Dages P., Carney P. (2002). Videoconferencing-based family counseling for rural teenagers with epilepsy: Phase 1 findings. Rehabilitation Psychology , 47, 49–72. [Google Scholar]
- Grados M. A., Vasa R. A., Riddle M. A., Slomine B. S., Salorio C., Christensen J., Gerring J. (2008). New onset obsessive-compulsive symptoms in children and adolescents with severe traumatic brain injury. Depression and Anxiety, 25, 398–407. [DOI] [PubMed] [Google Scholar]
- Hastings R. P., Brown T. (2002). Behavior problems of children with Autism, parental self-efficacy, and mental health. American Journal on Mental Retardation, 107, 222–232. [DOI] [PubMed] [Google Scholar]
- Hegewald J., Pfahlberg A., Uter W. (2003, September). A backwards-manual selection macro for binary logistic regression in the SAS v.8.02 PROC LOGISTIC procedure. Paper presented at the Proceedings of the North East SAS Users Group, Washington, DC. [Google Scholar]
- Hufford B. J., Glueckauf R. L., Webb P. M. (1999). Home-based, interactive videoconferencing for adolescents with epilepsy and their families. Rehabilitation Psychology, 44, 176–193. [Google Scholar]
- Jones T. L., Prinz R. J. (2004). Potential roles of parental self-efficacy in parent and child adjustment: A review. Clinical Psychology Review , 25, 341–363. [DOI] [PubMed] [Google Scholar]
- Karver C. L., Wade S. L., Cassedy A., Taylor H. G., Stancin T., Yeates K. O., Walz N. C. (2012). Age at injury and long-term behavior problems following traumatic brain injury in young children. Rehabilitation Psychology, 57, 256–265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Karver C. L., Wade S. L., Cassedy A., Taylor H. G., Brown T. M., Kirkwood M. W., Stancin T. (2013). Cognitive reserve as a moderator of responsiveness to an online problem-solving intervention for adolescents with complicated mild to severe traumatic brain injury. Child Neuropsychology, 20, 343–357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kurowski B. G., Wade S. L., Kirkwood M. W., Brown T. M., Stancin T., Taylor H. G. (2013). Online problem-solving therapy for executive dysfunction after child traumatic brain injury. Pediatrics, 132, 158–166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kreutzer J., Stejskal T., Ketchum J., Marwitz J., Taylor L., Menzel J. (2009). A preliminary investigation of the Brain Injury Family Intervention: Impact on family members. Brain Injury, 23, 535–547. [DOI] [PubMed] [Google Scholar]
- Radloff L. S. (1977). The CES-D scale: A self-report depression for research in the general population. Applied Psychological Measurement, 1, 385–401. [Google Scholar]
- Reeves W.C., Strine T. W., Pratt L. A., Thompson W., Ahluwalia I., Dhingra S. S., McKnight-Eily L. R., Harrison L., D'Angelo D. V., Williams L., Morrow B., Gould D., Safran M. A., Centers for Disease Control, Prevention (CDC). (2011). Mental illness surveillance among adults in the United States. Morbidity and Mortality Weekly Report , 60, 1–32. [PubMed] [Google Scholar]
- Stancin T., Wade S. L., Walz N. C., Yeates K. O., Taylor H. G. (2010). Family adaptation 18 months after traumatic brain injury in early childhood. Journal of Developmental and Behavioral Pediatrics, 31, 317–325. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor H. G., Yeates K. O., Wade S. L., Drotar D., Stancin T., Burant C. (2001). Bidirectional child-family influences on outcomes of traumatic brain injury in children. Journal of the International Neuropsychological Society, 7, 755–767. [DOI] [PubMed] [Google Scholar]
- Taylor H. G., Yeates K. O., Wade S. L., Drotar D., Stancin T., Minich N. (2002). A prospective study of short- and long-term outcomes after traumatic brain injury in children: Behavior and achievement. Neuropsychology, 16, 15–27. [DOI] [PubMed] [Google Scholar]
- Teasdale G., Jennett B. (1974). Assessment of coma and impaired consciousness: A practical scale. Lancet , 2, 81–84. [DOI] [PubMed] [Google Scholar]
- Temkin N. R., Heaton R. K., Grant I., Dikmen S. S. (1999). Detecting significant change in neuropsychological test performance: A comparison of four models. Journal of the International Neuropsychological Society, 5, 357–369. [DOI] [PubMed] [Google Scholar]
- Van der Heijden G., Donders A. R., Stijen T., Moons K. (2006). Imputation of missing values is superior to complete case analysis and the missing-indicator method in multivariable diagnostic research: A clinical example. Journal of Clinical Epidemiology , 59, 1102–1109. [DOI] [PubMed] [Google Scholar]
- Wade S. L., Carey J., Wolfe C. R. (2006). An online family intervention to reduce parental distress following pediatric brain injury. Journal of Consulting and Clinical Psychology, 74, 445–454. [DOI] [PubMed] [Google Scholar]
- Wade S. L., Karver C. L., Taylor H. G., Cassedy A., Stancin T., Kirkwood M. W., Brown T. M. (2014). Counselor-Assisted Problem Solving (CAPS) improves caregiver efficacy following adolescent brain injury. Rehabilitation Psychology , 59, 1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wade S. L., Stancin T., Kirkwood M. W., Brown T. M., McMullen K. M., Taylor H. G. (2014). Counselor-assisted problem solving (CAPS) improves behavioral outcomes in older adolescents with complicated mild to severe TBI. Journal of Head Trauma Rehabilitation, 29, 198.–. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wade S. L., Stancin T., Taylor H. G., Drotar D., Yeates K. O., Minich N. M. (2004). Interpersonal stressors and resources as predictors of parental adaptation following pediatric traumatic injury. Journal of Consulting and Clinical Psychology, 72, 776–784. [DOI] [PubMed] [Google Scholar]
- Wade S. L., Taylor H. G., Drotar D., Stancin T., Yeates K. O. (1998). Family burden and adaptation during the initial year after traumatic brain injury in children. Pediatrics, 102, 110–116. [DOI] [PubMed] [Google Scholar]
- Wade S. L., Taylor H. G., Drotar D., Stancin T., Yeates K.O., Minich N. (2002). A prospective study of long-term caregiver and family adaptation following brain injury in children. Journal of Head Trauma Rehabilitation , 17, 96–111. [DOI] [PubMed] [Google Scholar]
- Wade S. L., Walz N. C., Carey J., McMullen K. M., Cass J., Mark E., Yeates K. O. (2012). A randomized trial of teen online problem-solving: Efficacy in improving caregiver outcomes after brain injury. Health Psychology, 31, 767–776. [DOI] [PubMed] [Google Scholar]
- Wade S. L., Walz N. C., Carey J., Williams K. M., Cass J., Herren L., Mark E., Yeates K. O. (2010). A randomized trial of Teen Online Problem Solving for improving executive function deficits following pediatric traumatic brain injury. Journal of Head Trauma Rehabilitation, 25, 409–415. [DOI] [PubMed] [Google Scholar]
- Yeates K. O., Kaizar E., Rusin J., Bangert B., Dietrich A., Nuss K., Wright M., Taylor H. G. (2012). Reliable change in postconcussive symptoms and its consequences among children with mild traumatic brain injury functional consequences among children with mild traumatic brain injury. Achieves of Pediatric and Adolescent Medicine , 166, 615–622. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.