Abstract
Background
Professional continuing care services enhance recovery rates among adults and adolescents, though less is known about emerging adults (18-25 years old). Despite benefit shown from emerging adults’ participation in 12-step mutual-help organizations (MHOs), it is unclear whether participation offers benefit independent of professional continuing care services. Greater knowledge in this area would inform clinical referral and linkage efforts.
Methods
Emerging adults (N = 284; 74% male; 95% Caucasian) were assessed during the year after residential treatment on outpatient sessions per week, percent days in residential treatment and residing in a sober living environment, SUD medication use, active 12-step MHO involvement (e.g., having a sponsor, completing step work, contact with members outside meetings), and continuous abstinence (dichotomized yes/no). One generalized estimating equation (GEE) model tested the unique effect of each professional service on abstinence, and, in a separate GEE model, the unique effect of 12-step MHO involvement on abstinence over and above professional services, independent of individual covariates.
Results
Apart from SUD medication, all professional continuing care services were significantly associated with abstinence over and above individual factors. In the more comprehensive model, relative to zero 12-step MHO activities, odds of abstinence were 1.3 times greater if patients were involved in one activity, and 3.2 times greater if involved in five activities (lowest mean number of activities in the sample across all follow-ups).
Conclusions
Both active involvement in 12-step MHOs and recovery-supportive, professional services that link patients with these community-based resources may enhance outcomes for emerging adults after residential treatment.
Keywords: Substance use disorders, Emerging adulthood, Continuing Care, 12-step mutual-help organizations
1. INTRODUCTION
Substance use disorders (SUDs) are widely recognized as chronic conditions, often characterized by multiple cycles of treatment, abstinence, relapse, and, in some cases, incarceration prior to full remission (Dennis and Scott, 2007; Dennis et al., 2005; McLellan et al., 2000; Substance Abuse and Mental Health Services Administration (SAMHSA), 2014; White, 2012). Not surprisingly, relapse risk appears to be greatest early post-intervention, especially during the first 90 days (Hubbard et al., 1997; Hunt et al., 1971), though there is an elevated relapse risk across the entire post-treatment year (Dennis et al., 2007; Weisner et al., 2003) and even up through 5 years of continuous abstinence (Flynn et al., 2003; Hser et al., 2001).
1.1. The role of professional continuing care in SUD recovery
This chronic relapse risk has helped catalyze an expansion of the conventional acute care paradigm to a three-phased model of SUD treatment, marked by a) initial detoxification and/or symptom stabilization, b) an acute, time-limited, more intensive treatment phase, and, c) most critically, continuing care that facilitates maintenance and/or further improvements in health and functioning over time (Dennis and Scott, 2007; Kelly and White, 2011; McKay, 2009, 2010; McLellan, 2008; Simpson, 2004; Stout et al., 1999). Based on a narrative review (McKay, 2009) and a meta-analysis (Blodgett et al., 2014), as a broad (and heterogeneous) group of interventions, continuing care generally appears to support a modest, reliable improvement in SUD outcomes. For example, Scott and Dennis (2009) showed that receiving quarterly assessments and active assistance with treatment re-engagement enhanced outcomes 2 years post-treatment. Also, McKay et al. (2010) found that telephone-based continuing care (brief assessments, feedback, and progressively less intensive counseling) enhanced outcomes over 18 months. Among adolescents, Godley et al. (2007) showed that a package of direct and active continuing care linkages coupled with interventions that facilitate community-based prosocial activities promoted better adherence to continuing care recommendations and abstinence rates 9 months post-treatment.
1.2. Emerging adulthood: A clinically unique stage of the life course
Taken together, with some exceptions (e.g., Godley et al., 2010; McKay et al., 2013), evidence suggests well-articulated, active continuing care interventions can improve post-treatment outcomes among adolescents and adults. Little is known, however, regarding professional continuing care among treatment-seeking emerging adults (e.g., 18-25 years old; Arnett, 2000), who comprise approximately one-fifth of all SUD treatment admissions (SAMHSA, 2014), and are developmentally unique in their combination of life stressors (e.g., transition to independent living) and recovery barriers (e.g., social networks with substantial proportions of substance using individuals; Kelly et al., 2013; Mason and Luckey, 2003). Emerging adults are also clinically challenging, presenting with initially lower recovery motivation (Sinha et al., 2003) and evidencing poorer treatment engagement and retention compared to adults (Choi et al., 2013; McKay and Weiss, 2001; Schuman-Olivier et al., 2014; Shin et al., 2007, 2003), as well as poorer treatment and recovery outcomes compared to both adults and adolescents (Dawson et al., 2007; Hoeppner et al., 2014; Schuman-Olivier et al., 2014; Sinha et al., 2003; Smith et al., 2011).
1.3. Emerging adults’ participation in community-based, 12-step continuing care
As with adolescents and adults, initial findings support 12-step mutual-help organizations (MHOs) as potent, community-based continuing care resources for emerging adults (Chi et al., 2009; Delucchi et al., 2008; Kelly et al., 2008, 2013). Given the overlap among 12-step MHOs and professional treatment (Borkman et al., 2007; Kelly, 2003), however, empirically-informed continuing care recommendations require a simultaneous analysis of both professional (treatment) and non-professional (MHO) approaches. For example, among adult outpatients, studies show that 12-step MHO attendance is associated with abstinence over and above participation in SUD treatment as well as treatment-sanctioned, professional continuing care (Fiorentine, 1999; Fiorentine and Hillhouse, 2000). In the current study, we examined the unique effects of both professional continuing care and 12-step MHOs on post-treatment recovery rates in a sample of emerging adults.
1.4. Aims
Aims of the current study were three-fold: 1) to describe emerging adults’ engagement in professional continuing care and 12-step MHOs over the year following residential treatment; 2) to investigate unique associations between professional continuing care services and abstinence while controlling for individual factors (e.g., recovery motivation); and 3) to investigate unique associations between 12-step MHO involvement and abstinence, controlling for professional continuing care engagement and individual factors.
2. METHODS
2.1. Treatment model
Participants were recruited from the Hazelden Betty Ford Foundation (HBFF) in Plymouth, Minnesota (formerly known as the Hazelden Center for Youth and Families [HCYF]), a Minnesota-model (McElrath, 1997) residential treatment program for adolescents and young adults. It employs 12-step facilitation, cognitive-behavioral, and motivational enhancement therapies in individual and group formats, and provides adjunctive psychiatric care when clinically indicated (Bergman et al., 2014b).
2.2. Procedure
Participants were reimbursed $20, $30, $40, and $50 for follow-up assessments at 1 month (83.8%), 3 months (81.1%), 6 months (73.2%), and 12 months (70.9%) after discharge from the index treatment episode, respectively. The study was conducted in accordance with the Institutional Review Board at Schulman Associates IRB, an independent review board.
2.3. Participants
Among possible participants who attended HBFF between October 2006 and April 2008 (i.e., 18 to 24 years old; N = 384), 79% were enrolled and consented to participate (N = 302). For more information on the original sample, refer to Kelly et al. (2012). In brief, participants were predominantly male (73.8%) and Caucasian (94.7%); mean age was 20.4 years old (SD = 1.5). Alcohol and cannabis use disorders were the most common SUDs (about 75% each), and approximately one-third and one-half of the sample met criteria for opioid and cocaine use disorders, respectively, in their lifetime (Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; American Psychiatric Association, 2000). Roughly 85% of the sample completed treatment and the average participant attended for 25.5 days (SD = 5.7). Regarding treatment payment, 61% of patients paid via insurance reimbursement and 35% via self-pay (i.e., family). Also, 50% of the sample came from areas where the median household income was below $56,000. Apart from greater likelihood of being Caucasian, on aggregate participants were demographically similar to young adults (18-24 years old) in public sector as well as adults (18 and older) in private sector treatment (Roman and Johnson, 2004; SAMHSA, 2008).
Given the current study’s focus on post-treatment continuing care, the study sample initially included 284 patients who completed at least one follow-up assessment (94%). Relative to participants who were not included in the study (n = 18), those included in the study had significantly longer days in treatment for the index episode (p < .001, d = 0.74) but were similar on several other relevant clinical characteristics at treatment admission (e.g., days abstinent in the past 90), and were significantly more likely to have at least some college experience (p = .01; Odds Ratio [OR] = 5.72) but similar on all other measured demographic characteristics (e.g., gender).
2.4. Measures
2.4.1. Professional continuing care services
Each of four continuing care services were assessed with items from the Form-90 (Miller and Del Boca, 1994). Number of outpatient sessions per week was calculated by summing number of outpatient treatment program sessions and number of SUD-related individual sessions and dividing by total weeks in the assessment period. Percentage of days in residential treatment and percentage of days in a sober living environment were calculated by dividing total days residing in each setting by total days in the assessment period. SUD medication was modeled dichotomously based on whether the patient reported taking any medication specifically to address SUD during a follow-up period (e.g., buprenorphine/naloxone). The Form-90 has been tested with adult and adolescent samples and has demonstrated good test-retest reliability and validity (Slesnick and Tonigan, 2004; Tonigan et al., 1997).
2.4.2. Substance use
Given the abstinence-focused nature of the residential program from which the sample was recruited, the primary outcome was abstinence from all substances including alcohol and other drugs during each follow-up period (Form-90; Miller and Del Boca, 1994). For ease of data interpretation and to maximize the study’s clinical application, we modeled abstinence dichotomously (yes/no), in order to convey the likelihood of abstinence given varying levels of service engagement (i.e., odds ratios; also see Analysis Plan below). Saliva tests (Cone et al., 2002) assessing for the presence of tetrahydrocannibol (THC), cocaine metabolites, opioids, amphetamines, and phencyclidine, were administered at follow-up assessments to verify self-reported abstinence among participants that lived within 50 miles of the treatment facility and could attend assessments in person (21.7% of those who completed 1-month follow-up, 18.9% at 3 months, 7.7% at 6 months, and 6.1% at 12 months). None of these participants refused the saliva test, nor were they compensated for completion. Relative to patients who did not complete saliva tests, patients completing saliva tests had significantly longer days in treatment for the index episode (but were not different on baseline percent days abstinent, commitment to abstinence, or 12-step MHO involvement, p > .05) and were significantly more likely to be male (but not different on education or ethnicity; p > .05). Abstinence was confirmed in 97% of the 109 saliva tests conducted across all follow-up assessments.
2.4.3. 12-step MHO participation
Based on data collected with the Multidimensional Mutual-Help Meeting Activity Scale (Kelly et al., 2011), we derived an index of active 12-step MHO involvement based on the sum of eight dichotomous indicators, such as having a sponsor, contacting other members outside meetings, and 12-step work (see Kelly et al., 2013; internal consistency was α = 0.87 at intake, 0.81 at 1 month, 0.88 at 3 and 6 months, and 0.95 at 12 months). Active 12-step MHO involvement was chosen rather than attendance as it is a stronger and more consistent predictor of SUD outcomes (Cloud et al., 2004; Emrick et al., 1993; Humphreys et al., 2004; Kelly et al., 2013; Kelly and Urbanoski, 2012; Stout et al., 2012; Weiss et al., 2005).
2.4.4. Motivation for abstinence
Abstinence motivation was measured at treatment intake with the five-item, Commitment to Sobriety Scale (Kelly and Greene, 2014) (minimum = 5; maximum = 30). The scale has demonstrated excellent internal consistency (α = 0.89 at intake, 0.93 at 1 month, 0.95 at 3 and 12 months, and 0.94 at 6 months) and predictive validity, as well as significant incremental validity relative to existing measures of recovery motivation (Miller and Tonigan, 1996; Morgenstern et al., 1996) in the current sample (Kelly and Greene, 2014).
2.5. Analysis plan
To examine rates of professional continuing care engagement and 12-step MHO involvement (Aim 1), we present frequencies, descriptive statistics, and inter-correlations. To examine the unique influences of professional continuing care activities on abstinence (Aim 2), and the unique influence of 12-step MHO involvement on abstinence over and above professional continuing care (Aim 3), we ran two Generalized Estimating Equation models (GEE; Liang and Zeger, 1986). We chose to test our primary hypotheses with GEE models because this approach allowed us to model dichotomous observations (abstinence during follow-up) over time (at 1-month, 3-month, 6-month, and 12-month follow-ups) nested within individuals. For these GEE models, we carried out a systematic screening process to determine covariates with a priori pools of demographic characteristics as well as treatment-related and clinical variables measured at treatment intake (initial pool of possible covariates available by request). Specifically, for each follow-up, we conducted univariate logistic regressions with each of these a priori variables as the predictor and abstinence as the outcome, then conducted one multivariate model for each follow-up including only significant univariate predictors. We retained variables as GEE covariates if they were significantly associated with abstinence in at least two multivariate models, in order to reduce multicollinearity and maximize degrees of freedom. This screening process resulted in decisions to retain abstinence motivation and length of stay for the index treatment episode, in days.
Also, as mentioned in section 2.2 above (Procedure), the number of participants completing a follow-up decreased over time. GEE models can handle missing observations provided they are missing at random. Thus, in order to reduce bias associated with missing a follow-up assessment, variables associated with missing any of the four follow-up assessments were also included in the models (ethnicity, education, and length of stay for the index treatment episode).
In the first GEE model (Aim 2), abstinence over time (at 1-, 3-, 6-, and 12-month follow-ups) was the outcome, time invariant covariates were entered on the first predictor block, and professional continuing care services over time (also at 1-, 3-, 6-, and 12-month follow-ups) were entered on the second predictor block. The second GEE model (Aim 3) was estimated as above, but with 12-step MHO involvement over time added in the third block.
In order to test whether the effects of professional continuing care services on abstinence were consistent over time, we conducted four GEE models as in Aim 2, one for each service, which also included the service by time interaction. To test whether the effect of 12-step MHO involvement on abstinence was consistent over time, we conducted a GEE model as in Aim 3, that also included a 12-step MHO involvement by time interaction. Each significant interaction was probed by conducting four post-hoc logistic regressions (where predictors were identical to models used in Aim 2 or Aim 3, for professional continuing care and 12-step MHO involvement, respectively) to examine the continuing care activity’s associations with abstinence at each time point (1-, 3-, 6-, and 12-month follow-ups).
Regarding interpretation of associations between continuous predictors and a dichotomous outcome as was the case in these analyses, a one-unit change in the predictor of interest with regression coefficient b corresponds with an odds ratio of eb (where e is a mathematical constant approximately equal to 2.718). Similarly, a two-unit change corresponds with an odds ratio of e2b, a three-unit change with an odds ratio of e3b, and so on (Twisk, 2013).
It is important to note, prior to conducting contemporaneous analyses outlined above, consistent with our recent work on this sample (Bergman et al., 2014a; Kelly et al., 2013), we first conducted time-lagged analyses (e.g., the effect of 1-month outpatient treatment on 3-month abstinence), in order to bolster support for a causal relationship between professional continuing care services/12-step MHO involvement and abstinence. The pattern of results from both the time-lagged and contemporaneous models was the same. However, to be included in time-lagged analyses, of the 284 included in the study, participants needed to have data on all of the covariates and completed two consecutive assessments at least once (1-and 3-month follow-up, 3- and 6-month follow-up, or 6- and 12-month follow-up) whereas, to be included in contemporaneous analyses, they needed to have data on all of the covariates and completed at least one assessment. Thus, time-lagged analyses included a smaller, less representative sub-sample of the whole sample (N = 284) than contemporaneous analyses (n = 246 vs. n = 281, respectively) biased toward participants with better outcomes. For example, in lagged analyses, the parameter estimate for time (i.e., abstinence over time) was positive, indicating an improvement in abstinence over time. However, raw data using the whole sample as well as other longitudinal studies show that post-treatment abstinence rates tend to decline over time. Given the disadvantages of using the time-lagged models in this context, and the similar pattern of results, we report findings from the contemporaneous models.
3. RESULTS
3.1. Professional continuing care participation and 12-step MHO involvement during the post-treatment year
As shown in Table 1, patients reported modest rates of attendance in outpatient treatment, with no more than 20% reporting attendance at any follow-up. Among all patients, on average, they attended less than one session per week. Approximately half attended a “step-down” (i.e., less intensive) residential level of care after discharge from the index treatment episode. While that proportion remained stable through 3-month follow-up, the proportion in residential treatment decreased substantially by the 6- and 12-month follow-ups. The proportion residing in a sober living environment at 1-month (approximately 20%) increased up through 6-month, and decreased by 12-month follow-up. Average percent days in a sober living environment followed a similar pattern, ranging from approximately 15 (at 1 month) to 25 (at 6 months). Rates of SUD medication were quite low across all follow-up assessments, ranging from 4 to 7%. In contrast, 12-step MHO involvement was common; participants reported involvement in five to six activities on average across the post-treatment year.
Table 1.
Continuing Care Descriptive Statistics and Abstinence over Time
| 1 month (n = 253) |
3 months (n = 245) |
6 months (n = 221) |
12 months (n = 214) |
|
|---|---|---|---|---|
| Outpatient Treatment | ||||
| Any (% yes) | 49 (19.4%) | 47 (19.2%) | 44 (19.9%) | 36 (16.8%) |
| M Weekly Sessions (SD) | 0.4 (1.2) | 0.4 (1.1) | 0.2 (0.5) | 0.1 (0.3) |
| Residential Treatment | ||||
| Any (% yes) | 135 (53.4%) | 125 (51.0%) | 48 (21.7%) | 25 (11.7%) |
| M Percent Days (SD) | 50.2 (48.4) | 39.0 (44.1) | 9.5 (23.7) | 3.6 (13.8) |
| Sober Living Environment | ||||
| Any (% yes) | 53 (20.9%) | 66 (26.9%) | 80 (36.2%) | 51 (23.8%) |
| M Percent Days (SD) | 14.5 (32.5) | 19.3 (35.9) | 25.1 (38.4) | 15.5 (32.0) |
| SUD Medication (% yes) | 17 (6.7%) | 15 (6.1%) | 8 (3.6%) | 15 (7.0%) |
| M 12-Step Involvement (0-8) | 5.5 (2.2) | 5.7 (2.6) | 5.3 (3.0) | 5.1 (3.1) |
| Abstinence (% yes) | 188 (74.6%) | 156 (63.7%) | 123 (55.7%) | 90 (42.1%) |
M = mean; SUD = substance use disorder
In addition, we descriptively tested correlations among the professional continuing care services and 12-step MHO involvement for each follow-up (not shown). Across each time point the pattern of results was largely similar. Involvement in 12-step MHOs was significantly correlated with percent days in residential treatment (rs ranged from .15 at 12-month to .35 at 3 month follow-up) and percent days in a sober living environment (rs ranged from .21 at 1-month to .36 at 6-month follow-up). Percent days in residential treatment was significantly and negatively correlated with outpatient sessions per week and percent days in a sober living environment. SUD medication was generally not correlated with 12-step MHO involvement or the other professional continuing care services. Of note, percent days in a sober living environment was positively and significantly correlated with outpatient sessions per week at 1- and 3-month follow-ups (rs = .15 and .19, respectively), but not 6- and 12-month follow-ups.
3.2. Is participation in professional continuing care associated with abstinence?
With the exception of SUD medication, each professional continuing care service was associated with abstinence, over and above covariates and other services in the model (Table 2, Model 1). Specifically, for outpatient sessions per week, relative to zero sessions, odds of abstinence were 1.25 times greater for one session per week, and correspondingly, 1.5 times greater for two, and 2 times greater for three. For sober living environment, relative to 0 of 100 days, odds of abstinence were 6.2 times greater for 100 days (i.e., 100%, or 1.00) and, correspondingly, 1.7 times greater for 30 days, 3 times greater for 60 days, and 5.2 times greater for 90 days. For residential treatment, relative to 0 of 100 days, odds of abstinence were 10.5 times greater for 100 days and, correspondingly, 2 times greater for 30 days, 4 times greater for 60 days, and 8 times greater for 90 days. Also of note, both length of stay for the index treatment episode and baseline abstinence motivation were significant predictors of abstinence (p < .05 and .01, respectively).
Table 2.
Generalized Estimating Equations Characterizing the Unique Effects of Professional Continuing Care Services (Model 1) and 12-Step Mutual-Help Organization Involvement (Model 2) on Continuous Abstinence across 1-month, 3-month, 6-month, and 12-month Follow-up Assessments
| Model 1 OR (95% CI) |
Model 2 OR (95% CI) |
|
|---|---|---|
| Time | 0.96 (.93 - 1.00)* | 0.95 (.91 - .99)** |
| Demographic Characteristics | ||
| Ethnicity (Caucasian vs. not) | 1.31 (.52 - 3.30) | 1.35 (.59 - 3.10) |
| Education (some college vs. not) | 0.78 (.52 - 1.18) | 0.79 (.52 - 1.20) |
| Clinical Characteristics | ||
| Length of Stay (days) | 1.05 (1.01 - 1.10)* | 1.05 (1.00 - 1.10)* |
| Abstinence Motivation (at intake) | 1.09 (1.05 - 1.14)** | 1.07 (1.03 - 1.11)** |
| Professional Continuing Care Services | ||
| Outpatient Sessions Per Week | 1.25 (1.02 - 1.53)* | 1.19 (.97 - 1.46) |
| % Days in Sober Living Environment | 6.24 (3.86 -10.08)** | 4.77 (2.83 - 8.03)** |
| % Days in Residential Treatment | 10.50 (6.54 - 16.58)** | 7.09 (4.31 - 11.64)** |
| SUD Medication (any vs. none) | 1.80 (.99 - 3.25) | 1.77 (.98 - 3.18) |
| Active 12-step MHO Involvement | 1.26 (1.17 - 1.35)** |
OR = odds ratio; CI = confidence interval; SUD = substance use disorder; MHO = mutual-help organization
p < .05
p < .01
3.3. Is 12-step MHO involvement associated with abstinence independent of professional continuing care participation?
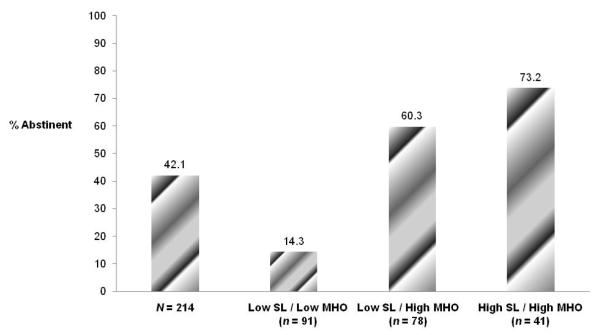
Independent of covariates and continuing care services, 12-step MHO involvement was a significant predictor of abstinence over time (p < .01; Table 2, Model 2). Relative to zero 12-step MHO activities, odds of abstinence were 1.26 times greater for one activity, 1.59 times greater for two, and 3.2 times greater for five (the lowest mean 12-step MHO involvement among all follow-ups). Although outpatient sessions per week was not significant when 12-step MHO involvement was included in the model, residential treatment and sober living remained significant. Specifically, controlling for 12-step MHO involvement, other professional continuing care services, and covariates, odds of abstinence were 4.8 times greater if residing in a sober living environment for 100% of days in a follow-up period versus none. Figure 1 illustrates this additive effect for residing in a sober living environment and 12-step MHO involvement.
Figure 1.
Raw Abstinence Rates During the 12-Month Follow-Up Period as a Function of Sober Living Environment Residence (SL) and 12-Step Mutual-Help Organization Involvement (MHO). SL was split by mean percent days (15.5% or lower [low] versus greater than 15.5% [high]), and MHO was split by mean number of activities (five or lower [low] versus six or greater [high]). Note that only four patients had High SL / Low MHO, none of whom were abstinent during follow-up (not shown).
Regarding professional continuing care interactions with time, only the residential treatment by time interaction was significant (p = .017). The interaction between 12-step MHO involvement and time was also significant (p = .003). Results of post-hoc logistic regression analyses for percent days in residential treatment revealed significant associations with abstinence at 1-, 3-, and 6-, but not the 12-month follow-up (p < .05; odds ratios [OR] = 25.81, 22.88, 13.19, and 0.70 over time, respectively). For 12-step MHO involvement, analyses revealed significant associations with abstinence at 1-, 6-, and 12-month – but not 3-month follow-up (p < .05; ORs = 1.25, 1.04, 1.43, 1.61, over time, respectively).
3.4. Subsidiary GEE interpretations
In order to explore hypotheses for future tests of mediation (e.g., “Does 12-step MHO involvement mediate the association between residing in a sober living environment and abstinence?”), we examined change in each significant continuing care service effect from the model without and with 12-step MHO involvement included (Model 1 vs. Model 2, respectively). First, the effect of outpatient sessions per week on abstinence decreased from significant to nonsignificant. Second, although they were significant predictors in both models, effects of percent days in residential treatment and sober living were smaller in Model 2 compared to Model 1. These findings indicate the positive associations between participation in professional continuing care services and abstinence may be explained, in part, by 12-step MHO involvement.
4. DISCUSSION
In the current study we examined emerging adults’ patterns of professional and non-professional continuing care utilization and associations with abstinence following residential SUD treatment. Findings indicated that attending “step-down” residential treatment and outpatient treatment, as well as residing in a sober living environment were each significant predictors of continuous abstinence. Extending prior mutual-help investigations among this cohort, findings also showed patients’ 12-step MHO involvement was predictive of abstinence over and above professional continuing care participation and other confounding variables.
4.1. Engagement with continuing care after residential treatment
First, patients were engaged with both professional and community-based (i.e., MHOs) continuing care options, consistent with a recovery management framework (Kelly and White, 2011; White, 2008). Second, this emerging adult sample was far more likely to attend “step-down” residential than outpatient continuing care (maximum of 50% versus 20% of the sample). This finding was somewhat surprising, given that among patients attending publically-funded programs, outpatient treatment is the most commonly sought modality, serving 60% of all admissions (SAMHSA, 2014). The structure of the residential program from which patients were recruited may account in part, for the sample’s unique pattern of continuing care service utilization, as patients were offered geographically-accessible, longer-term, and less-intensive residential treatment as a continuing care option. More residential than outpatient continuing care may also reflect the sample’s substance use severity (Kelly et al., 2010), where greater engagement with higher levels of care would be clinically appropriate. Also of note, residential treatment engagement in the latter two follow-up time periods may reflect response to relapse rather than step-down care associated with the initial continuing care plan.
Third, participation in medication-assisted treatment was rare, though in post-hoc exploratory analyses (not shown), rates were slightly higher among patients with an opioid use disorder, and increased marginally over time (6.7%, 11.1%, 12.0%, and 13.6% at 1-month, 3-month, 6-month, and 12-month follow-ups). Importantly, between 2006 and 2010 (the time period during which our sample was recruited), only 8% of SUD treatment programs offered medication-assisted treatment (SAMHSA, 2011). Emerging evidence regarding the efficacy and safety of the partial agonist buprenorphine/naloxone (Gray, 2007; Li et al., 2014; Mattick et al., 2014) and intramuscular extended release formulation of the antagonist naltrexone (Gastfriend, 2011), may shift clinical perspectives, leading to greater likelihood of referral for SUD medication. For example, among SUD treatment seekers in 2012, 28% of primary heroin and 18% of primary non-heroin opioid patients reported engagement with medication-assisted treatment (SAMHSA, 2014).
4.2. Professional and 12-step mutual-help continuing care are each uniquely associated with positive outcomes
Although the study was naturalistic and patients were not randomized to continuing care services, results are consistent with prior research showing that continuing care interventions provide post-treatment support for recovery efforts (Blodgett et al., 2014; McKay, 2009). Findings here suggest after an acute episode of care, programs can increase the likelihood that patients will remain abstinent in the first year by facilitating their engagement in a structured recovery-supportive setting. It is not surprising that participation in residential treatment was associated with increased odds of abstinence given the exaggerated emotional scaffolding and protection from environmental risks it offers. Critically, however, similar to other studies showing structured sober housing provides recovery benefit (Jason et al., 2007, 2006; Polcin et al., 2010), we found that residing within a sober living environment during a follow-up period uniquely enhanced the odds of abstinence by a factor of five.
Building on prior work among adults indicating additive 12-step MHO and professional service effects (Fiorentine and Hillhouse, 2000; Moos et al., 2001), analyses showed, over and above individual factors and continuing care service engagement, odds of abstinence for emerging adults who become actively involved in 12-step MHOs during the post-treatment year (i.e., in five activities, the lowest mean level of involvement at any follow-up) are more than 3 greater than those with no involvement. Regarding nonsignificant associations between 12-step MHO involvement and abstinence at 3-months and between residential treatment and abstinence at 12-months, speculatively, it could be that the greater variability in percent days in residential treatment early in the post-treatment year allows for stronger prediction of abstinence (see Table 1). However, as variability in residential treatment engagement declines over time, this provides more fertile statistical ground to detect the impact of community-based, 12-step MHO involvement effects.
Exploratory analyses also provided some preliminary insights about the relationship between professional and non-professional continuing care activities. Specifically, the effects of professional continuing care services on abstinence may have been explained, at least in part, by engaging patients with freely available 12-step MHOs, in keeping with the primary goal of many professional programs. Formal tests of mediation (e.g., MacKinnon et al., 2007) that examine whether the impact of professional continuing care services on abstinence is explained by 12-step MHO involvement are warranted.
Specifically regarding evidence for sober living environments, these housing supports provide patients with a heterogeneous array of recovery resources, both across and within settings (Polcin, 2009). Oversight and monitoring can vary substantially, including toxicology screens, mandated 12-step MHO attendance, and requirements that residents either have employment or otherwise seek employment, a strong predictor of sustaining recovery (White, 2008). Highlighted by their potential ability to bolster abstinence self-efficacy (Jason et al., 2006) and to reduce the financial burden of SUD via reductions in SUD-related illegal activity (Lo Sasso et al., 2012), as well as to facilitate 12-step MHO participation, research on a diversity of recovery-supportive housing options, the services they offer, and their relative effects on recovery rates are needed to inform and enhance clinical referral.
4.3. Limitations
Conclusions from this study should be considered carefully in light of some important limitations. First, our sample was primarily male and Caucasian and recruited from a single high-quality, residential treatment facility in the Midwest. Also, although half of participants resided in areas where the median household income was below $56,000, given families’ ability to support patients’ engagement in residential treatment, findings might not generalize to families with fewer resources and/or limited health care access. Second, we chose to focus the study on the role of SUD continuing care for emerging adults, though some research suggests concurrent psychiatric treatment may boost SUD recovery rates (Moos et al., 2001; Ray et al., 2005), indicating follow-up inquiry regarding the interplay of SUD, psychiatric, and community-based continuing care is warranted. Finally, while several steps were taken to assess the unique effects of professional continuing care services and 12-step MHO involvement (e.g., use of GEE and statistical control for variables associated with abstinence and missed follow-ups), we cannot eliminate all alternative explanations for effects attributed to these activities due to the study’s non-experimental design.
4.4. Summary, conclusions, and future directions
Research supports the clinical need to establish recovery-oriented systems of care (Hser and Anglin, 2011; White, 2008) rather than acute, unrelated, and episodic interventions. Similar to prior studies on adults and adolescents, this study found that participation in professional recovery services (step-down residential treatment and sober living environments) and community-based supports (12-step MHOs) uniquely promote improved abstinence rates among treatment-seeking emerging adults during the year after discharge from residential treatment. This study is also among the first to document additive benefits of professional and non-professional (i.e., 12-step MHO) continuing care participation specifically among this age group. In light of the consistency between these continuing care findings and others examined across the life course, however, clinicians might explicitly focus facilitation efforts on engaging patients with structured, recovery-supportive environments that link individuals with freely available 12-step MHOs after the initial episode of care. Regarding future investigations, the impact and reach of continuing care for young adults might be augmented through testing the broad array of settings and services within the sober living framework (Polcin, 2009), through adapting and testing 12-step facilitation approaches specifically for this age group to help reduce the financial burden of professional continuing care (Labbe et al., 2014), and through investigation of innovative mobile health applications (e.g., Gustafson et al., 2014) that may help overcome barriers to traditional approaches.
Highlights.
Emerging adults are a vulnerable group of treatment seekers.
We examined their professional and 12-step mutual-help continuing care.
Outpatient treatment and sober living were uniquely associated with abstinence.
12-step involvement was associated with abstinence over and above professional services.
Acknowledgments
Role of Funding Source
This work was funded by 1R21AA018185-01A2 and by an anonymous donation for youth research to the Hazelden Foundation. Dr. Hoeppner’s participation is supported by NIDA grant K01DA027097. Dr. Kelly’s participation is supported by NIAAA grant 1R21AA018185-01A2.
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Contributors
Drs. Bergman and Kelly contributed to study design, analyses, and manuscript preparation. Dr. Hoeppner was responsible for primary conduct of analyses. Ms. Nelson contributed to data collection and management. Dr. Slaymaker contributed to data collection and study design.
Conflict of Interest
No conflict declared
REFERENCES
- American Psychiatric Association . Diagnostic And Statistical Manual Of Mental Disorders. 4th Ed. APA; Washington, DC: 2000. Text Revision. [Google Scholar]
- Arnett JJ. Emerging adulthood: a theory of development from the late teens through the twenties. Am. Psychol. 2000;55:469–480. [PubMed] [Google Scholar]
- Bergman BG, Greene MC, Hoeppner BB, Slaymaker V, Kelly JF. Psychiatric comorbidity and 12-step participation: a longitudinal investigation of treated young adults. Alcohol. Clin. Exp. Res. 2014a;38:501–510. doi: 10.1111/acer.12249. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bergman BG, Greene MC, Slaymaker V, Hoeppner BB, Kelly JF. Young adults with co-occurring disorders: substance use disorder treatment response and outcomes. J. Subst. Abuse Treat. 2014b;46:420–428. doi: 10.1016/j.jsat.2013.11.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Blodgett JC, Maisel NC, Fuh IL, Wilbourne PL, Finney JW. How effective is continuing care for substance use disorders? A meta-analytic review. J. Subst. Abuse Treat. 2014;46:87–97. doi: 10.1016/j.jsat.2013.08.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Borkman T, Kaskutas LA, Owen P. Contrasting and converging philosophies of three models of alcohol/other drugs treatment: Minnesota model, social model, and addiction therapeutic communities. Alcohol. Treat. Q. 2007;25:21–38. [Google Scholar]
- Chi FW, Kaskutas LA, Sterling S, Campbell CI, Weisner C. Post-treatment 12-step involvement and 3-year outcomes among adolescents with substance use problems: social support and religiosity as mediators. Addiction. 2009;104:927–939. doi: 10.1111/j.1360-0443.2009.02524.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Choi S, Adams SM, MacMaster SA, Seiters J. Predictors of residential treatment retention among individuals with co-occurring substance abuse and mental health disorders. J. Psychoactive Drugs. 2013;45:122–131. doi: 10.1080/02791072.2013.785817. [DOI] [PubMed] [Google Scholar]
- Cloud RN, Ziegler CH, Blondell RD. What is Alcoholics Anonymous Affiliation? Subst. Use Misuse. 2004;39:1117–1136. doi: 10.1081/ja-120038032. [DOI] [PubMed] [Google Scholar]
- Cone EJ, Presley L, Lehrer M, Seiter W, Smith M, Kardos KW, Fritch D, Salamone S, Niedbala RS. Oral fluid testing for drugs of abuse: positive prevalence rates by Intercept immunoassay screening and GC-MS-MS confirmation and suggested cutoff concentrations. J. Anal. Toxicol. 2002;26:541–546. doi: 10.1093/jat/26.8.541. [DOI] [PubMed] [Google Scholar]
- Dawson DA, Goldstein RB, Grant BF. Rates and correlates of relapse among individuals in remission from DSM-IV alcohol dependence: a 3-year follow-up. Alcohol. Clin. Exp. Res. 2007;31:2036–2045. doi: 10.1111/j.1530-0277.2007.00536.x. [DOI] [PubMed] [Google Scholar]
- Delucchi KL, Matzger H, Weisner C. Alcohol in emerging adulthood: 7-year study of problem and dependent drinkers. Addict. Behav. 2008;33:134–142. doi: 10.1016/j.addbeh.2007.04.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dennis M, Scott CK. Managing addiction as a chronic condition. Addict. Sci. Clin. Pract. 2007;4:45–55. doi: 10.1151/ascp074145. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dennis ML, Foss MA, Scott CK. An eight-year perspective on the relationship between the duration of abstinence and other aspects of recovery. Eval. Rev. 2007;31:585–612. doi: 10.1177/0193841X07307771. [DOI] [PubMed] [Google Scholar]
- Dennis ML, Scott CK, Funk R, Foss MA. The duration and correlates of addiction and treatment careers. J. Subst. Abuse Treat. 2005;28:S51–S62. doi: 10.1016/j.jsat.2004.10.013. [DOI] [PubMed] [Google Scholar]
- Emrick CD, Tonigan JS, Montgomery H, Little L. Alcoholics Anonymous: what is currently known? In: McCrady BS, Miller WR, editors. Research on Alcoholics Anonymous: Opportunities and alternatives. Rutgers Center of Alcohol Studies; Piscataway, NJ: 1993. pp. 41–76. [Google Scholar]
- Fiorentine R. After drug treatment: Are 12-step programs effective in maintaining abstinence? Am. J. Drug Alcohol Abuse. 1999;25:93–116. doi: 10.1081/ada-100101848. [DOI] [PubMed] [Google Scholar]
- Fiorentine R, Hillhouse MP. Drug treatment and 12-step program participation: the additive effects of integrated recovery activities. J. Subst. Abuse Treat. 2000;18:65–74. doi: 10.1016/s0740-5472(99)00020-3. [DOI] [PubMed] [Google Scholar]
- Flynn PM, Joe GW, Broome KM, Simpson DD, Brown BS. Recovery from opioid addiction in DATOS. J. Subst. Abuse Treat. 2003;25:177–186. doi: 10.1016/s0740-5472(03)00125-9. [DOI] [PubMed] [Google Scholar]
- Gastfriend DR. Intramuscular extended-release naltrexone: current evidence. Ann. N. Y. Acad. Sci. 2011;1216:144–166. doi: 10.1111/j.1749-6632.2010.05900.x. [DOI] [PubMed] [Google Scholar]
- Godley MD, Godley SH, Dennis ML, Funk RR, Passetti LL. The effect of assertive continuing care on continuing care linkage, adherence and abstinence following residential treatment for adolescents with substance use disorders. Addiction. 2007;102:81–93. doi: 10.1111/j.1360-0443.2006.01648.x. [DOI] [PubMed] [Google Scholar]
- Godley SH, Garner BR, Passetti LL, Funk RR, Dennis ML, Godley MD. Adolescent outpatient treatment and continuing care: Main findings from a randomized clinical trial. Drug Alcohol Depend. 2010;110:44–54. doi: 10.1016/j.drugalcdep.2010.02.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gray A. Background document prepared for the third meeting of technical development group (TDG) for the WHO “Guidelines for Psychosocially Assisted Pharmacotherapy of Opioid Dependence”. Geneva, Switzerland: 2007. Systematic review of the safety of buprenorphine, methadone, and naltrexone. [Google Scholar]
- Gustafson DH, McTavish FM, Chih MY, Atwood AK, Johnson RA, Boyle MG, Levy MS, Driscoll H, Chisholm SM, Dillenburg L, Isham A, Shah D. A smartphone application to support recovery from alcoholism: a randomized clinical trial. JAMA Psychiatry. 2014;71:566–572. doi: 10.1001/jamapsychiatry.2013.4642. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hoeppner BB, Hoeppner SS, Kelly JF. Do young people benefit from AA as much, and in the same ways, as adult aged 30+? A moderated multiple mediation analysis. Drug Alcohol Depend. 2014;143:181–188. doi: 10.1016/j.drugalcdep.2014.07.023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hser Y-I, Anglin MD. Addiction treatment and recovery careers. In: Kelly JF, White WL, editors. Addiction Recovery Management: Theory, Research, And Practice. Spring Science+Business Media; New York, NY: 2011. [Google Scholar]
- Hser YI, Hoffman V, Grella CE, Anglin MD. A 33-year follow-up of narcotics addicts. Arch. Gen. Psychiatry. 2001;58:503–508. doi: 10.1001/archpsyc.58.5.503. [DOI] [PubMed] [Google Scholar]
- Hubbard RL, Craddock SG, Flynn PM, Anderson J, Etheridge RM. Overview of 1-year follow-up outcomes in the Drug Abuse Treatment Outcome Study (DATOS) Psychol. Addict. Behav. 1997;11:261–278. [Google Scholar]
- Humphreys K, Wing S, McCarty D, Chappel J, Gallant L, Haberle B, Horvath TA, Kaskutas LA, Kirk T, Kivlahan D, Laudet A, McCrady BS, McLellan AT, Morgenstern J, Townsend M, Weiss R. Self-help organizations for alcohol and drug problems: toward evidence-based practice and policy. J. Subst. Abuse Treat. 2004;26:151–158. doi: 10.1016/S0740-5472(03)00212-5. [DOI] [PubMed] [Google Scholar]
- Hunt WA, Barnett LW, Branch LG. Relapse rates in addiction programs. J. Clin. Psychol. 1971;27:455–456. doi: 10.1002/1097-4679(197110)27:4<455::aid-jclp2270270412>3.0.co;2-r. [DOI] [PubMed] [Google Scholar]
- Jason LA, Davis MI, Ferrari JR. The need for substance abuse after-care: longitudinal analysis of Oxford House. Addict. Behav. 2007;32:803–818. doi: 10.1016/j.addbeh.2006.06.014. [DOI] [PubMed] [Google Scholar]
- Jason LA, Olson BD, Ferrari JR, Lo Sasso AT. Communal housing settings enhance substance abuse recovery. Am. J. Public Health. 2006;96:1727–1729. doi: 10.2105/AJPH.2005.070839. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF. Self-help for substance-use disorders: history, effectiveness, knowledge gaps and research opportunities. Clin. Psychol. Rev. 2003;23:639–663. doi: 10.1016/s0272-7358(03)00053-9. [DOI] [PubMed] [Google Scholar]
- Kelly JF, Brown SA, Abrantes A, Kahler CW, Myers M. Social recovery model: an 8-year investigation of adolescent 12-step group involvement following inpatient treatment. Alcohol. Clin. Exp. Res. 2008;32:1468–1478. doi: 10.1111/j.1530-0277.2008.00712.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, Greene MC. Beyond motivation: initial validation of the commitment to sobriety scale. J. Subst. Abuse Treat. 2014;46:257–263. doi: 10.1016/j.jsat.2013.06.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, Magill M, Slaymaker V, Kahler C. Psychometric validation of the Leeds Dependence Questionnaire (LDQ) in a young adult clinical sample. Addict. Behav. 2010;35:331–336. doi: 10.1016/j.addbeh.2009.11.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, Stout RL, Slaymaker V. Emerging adults’ treatment outcomes in relation to 12-step mutual-help attendance and involvement. Drug Alcohol Depend. 2013;129:151–157. doi: 10.1016/j.drugalcdep.2012.10.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, Urbanoski K. Youth recovery contexts: the incremental effects of 12-step attendance and involvement on adolescent outpatient outcomes. Alcohol. Clin. Exp. Res. 2012;36:1219–1229. doi: 10.1111/j.1530-0277.2011.01727.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, Urbanoski KA, Hoeppner BB, Slaymaker V. Facilitating comprehensive assessment of 12-step experiences: a Multidimensional Measure of Mutual-Help Activity. Alcohol. Treat. Q. 2011;29:181–203. doi: 10.1080/07347324.2011.586280. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, Urbanoski KA, Hoeppner BB, Slaymaker V. “Ready, willing, and (not) able” to change: young adults’ response to residential treatment. Drug Alcohol Depend. 2012;121:224–230. doi: 10.1016/j.drugalcdep.2011.09.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly JF, White WL, editors. Addiction Recovery Management: Theory, Research, And Practice. Spring Science+Business Media; New York, NY: 2011. [Google Scholar]
- Labbe AK, Slaymaker V, Kelly JF. Toward enhancing 12-step facilitation among young people: a systematic qualitative investigation of young adults’ 12-step experiences. Subst. Abuse. 2014;35:399–407. doi: 10.1080/08897077.2014.950001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li X, Shorter D, Kosten TR. Buprenorphine in the treatment of opioid addiction: opportunities, challenges and strategies. Expert Opin. Pharmacother. 2014;15:2263–2275. doi: 10.1517/14656566.2014.955469. [DOI] [PubMed] [Google Scholar]
- Liang KY, Zeger SL. Longitudinal data analysis using generalized linear models. Biometrika. 1986;73:13–22. [Google Scholar]
- Lo Sasso AT, Byro E, Jason LA, Ferrari JR, Olson B. Benefits and costs associated with mutual-help community-based recovery homes: the Oxford House model. Eval. Program Plann. 2012;35:47–53. doi: 10.1016/j.evalprogplan.2011.06.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- MacKinnon DP, Fairchild AJ, Fritz MS. Mediation analysis. Annu. Rev. Psychol. 2007;58:593–614. doi: 10.1146/annurev.psych.58.110405.085542. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mason MJ, Luckey B. Young adults in alcohol-other drug treatment: An understudied population. Alcohol. Treat. Q. 2003;21:17–32. [Google Scholar]
- Mattick RP, Breen C, Kimber J, Davoli M. Buprenorphine maintenance versus placebo or methadone maintenance for opioid dependence. Cochrane Database Syst. Rev. 2014;2:Cd002207. doi: 10.1002/14651858.CD002207.pub4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McElrath D. The Minnesota Model. J. Psychoactive Drugs. 1997;29:141–144. doi: 10.1080/02791072.1997.10400180. [DOI] [PubMed] [Google Scholar]
- McKay JR. Continuing care research: what we’ve learned and where we’re going. J. Subst. Abuse Treat. 2009;36:131–145. doi: 10.1016/j.jsat.2008.10.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McKay JR. Treating Substance Use Disorders With Adaptive Continuing Care. American Psychological Association; Washington D.C.: 2010. [Google Scholar]
- McKay JR, Lynch KG, Coviello D, Morrison R, Cary MS, Skalina L, Plebani J. Randomized trial of continuing care enhancements for cocaine-dependent patients following initial engagement. J. Consult. Clin. Psychol. 2010;78:111–120. doi: 10.1037/a0018139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McKay JR, van Horn D, Ivey M, Drapkin ML, Rennert L, Lynch KG. Enhanced continuing care provided in parallel to intensive outpatient treatment does not improve outcomes for patients with cocaine dependence. J. Stud. Alcohol Drugs. 2013;74:642–651. doi: 10.15288/jsad.2013.74.642. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McKay JR, Weiss RV. A review of temporal effects and outcome predictors in substance abuse treatment studies with long-term follow-ups: preliminary results and methodological issues. Eval. Rev. 2001;25:113–161. doi: 10.1177/0193841X0102500202. [DOI] [PubMed] [Google Scholar]
- McLellan AT. Evolution in addiction treatment concepts and methods. In: Galanter M, Kleber HD, editors. American Psychiatric Publishing Textbook Of Substance Abuse Treatment. American Psychiatric Publishing; Arlington, VA: 2008. pp. 93–108. [Google Scholar]
- McLellan AT, Lewis DC, O’Brien CP, Kleber HD. Drug dependence, a chronic medical illness: Implications for treatment, insurance, and outcomes evaluation. JAMA. 2000;284:1689–1697. doi: 10.1001/jama.284.13.1689. [DOI] [PubMed] [Google Scholar]
- Miller WR, Del Boca FK. Measurement of drinking behavior using the Form 90 family of instruments. J. Stud. Alcohol Suppl. 1994;12:112–118. doi: 10.15288/jsas.1994.s12.112. [DOI] [PubMed] [Google Scholar]
- Miller WR, Tonigan JS. Assessing drinkers’ motivation for change: the stages of change readiness and treatment eagerness scale (SOCRATES) Psychol. Addict. Behav. 1996;10:81–89. [Google Scholar]
- Moos R, Schaefer J, Andrassy J, Moos B. Outpatient mental health care, self-help groups, and patients’ one-year treatment outcomes. J. Clin. Psychol. 2001;57:273–287. doi: 10.1002/jclp.1011. [DOI] [PubMed] [Google Scholar]
- Morgenstern J, Frey RM, McCrady BS, Labouvie E, Neighbors CJ. Examining mediators of change in traditional chemical dependency treatment. J. Stud. Alcohol. 1996;57:53–64. doi: 10.15288/jsa.1996.57.53. [DOI] [PubMed] [Google Scholar]
- Polcin DL. Communal living settings for adults recovering from substance abuse. J. Groups Addict. Recover. 2009;4:7–22. doi: 10.1080/15560350802712355. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Polcin DL, Korcha RA, Bond J, Galloway G. Sober living houses for alcohol and drug dependence: 18-month outcomes. J. Subst. Abuse Treat. 2010;38:356–365. doi: 10.1016/j.jsat.2010.02.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ray GT, Weisner CM, Mertens JR. Relationship between use of psychiatric services and five-year alcohol and drug treatment outcomes. Psychiatr. Serv. 2005;56:164–171. doi: 10.1176/appi.ps.56.2.164. [DOI] [PubMed] [Google Scholar]
- Roman PM, Johnson JA. National Treatment Center Study Summary Report: Private Treatment Centers. Institute for Behavioral Research, University of Georgia; Athens, GA: 2004. [Google Scholar]
- Schuman-Olivier Z, Weiss RD, Hoeppner BB, Borodovsky J, Albanese MJ. Emerging adult age status predicts poor buprenorphine treatment retention. J. Subst. Abuse Treat. 2014;47:202–212. doi: 10.1016/j.jsat.2014.04.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Scott CK, Dennis ML. Results from two randomized clinical trials evaluating the impact of quarterly recovery management checkups with adult chronic substance users. Addiction. 2009;104:959–971. doi: 10.1111/j.1360-0443.2009.02525.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shin SH, Lundgren L, Chassler D. Examining drug treatment entry patterns among young injection drug users. Am. J. Drug Alcohol Abuse. 2007;33:217–225. doi: 10.1080/00952990601174774. [DOI] [PubMed] [Google Scholar]
- Simpson DD. A conceptual framework for drug treatment process and outcomes. J. Subst. Abuse Treat. 2004;27:99–121. doi: 10.1016/j.jsat.2004.06.001. [DOI] [PubMed] [Google Scholar]
- Sinha R, Easton C, Kemp K. Substance abuse treatment characteristics of probation-referred young adults in a community-based outpatient program. Am. J. Drug Alcohol Abuse. 2003;29:585–597. doi: 10.1081/ada-120023460. [DOI] [PubMed] [Google Scholar]
- Slesnick N, Tonigan JS. Assessment of alcohol and other drug use by runaway youths: a test-retest study of the Form 90. Alcohol. Treat. Q. 2004;22:21–34. doi: 10.1300/J020v22n02_03. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Smith DC, Godley SH, Godley MD, Dennis ML. Adolescent Community Reinforcement Approach outcomes differ among emerging adults and adolescents. J. Subst. Abuse Treat. 2011;41:422–430. doi: 10.1016/j.jsat.2011.06.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stout RL, Kelly JF, Magill M, Pagano ME. Association between social influences and drinking outcomes across three years. J. Stud. Alcohol Drugs. 2012;73:489–497. doi: 10.15288/jsad.2012.73.489. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stout RL, Rubin A, Zwick W, Zywiak W, Bellino L. Optimizing the cost-effectiveness of alcohol treatment: a rationale for extended case monitoring. Addict. Behav. 1999;24:17–35. doi: 10.1016/s0306-4603(98)00029-x. [DOI] [PubMed] [Google Scholar]
- Substance Abuse and Mental Health Services Administration [accessed on October 12 2013];Characteristics of Young Adult (Aged 18-25) and Youth (Aged 12-17) Admissions: 2004. 2008 http://www.samhsa.gov/data/2k6/youngTX/youngTX.htm.
- Substance Abuse and Mental Health Services Administration . Data on Substance Abuse Treatment Facilities. Substance Abuse and Mental Health Services Administration; Rockville, MD: 2011. National Survey of Substance Abuse Treatment Services (N-SSATS): 2010. (DASIS Series S-59). HHS Publication No. (SMA) 11-4665. [Google Scholar]
- Substance Abuse and Mental Health Services Administration . Treatment Episode Data Set (TEDS). 2002-2012. National Admissions to Substance Abuse Treatment Services. Substance Abuse and Mental Health Services Administration; Rockville, MD: 2014. (BHSIS Series: S-71). HHS Publication No. (SMA) 14-4850. [Google Scholar]
- Tonigan JS, Miller WR, Brown JM. The reliability of Form 90: an instrument for assessing alcohol treatment outcome. J. Stud. Alcohol. 1997;58:358–364. doi: 10.15288/jsa.1997.58.358. [DOI] [PubMed] [Google Scholar]
- Twisk JWR. Applied Longitudinal Data Analysis For Epidemiology. Cambridge University Press; New York, NY: 2013. Dichotomous Outcome Variables; pp. 119–139. [Google Scholar]
- Weisner C, Matzger H, Kaskutas LA. How important is treatment? One-year outcomes of treated and untreated alcohol-dependent individuals. Addiction. 2003;98:901–911. doi: 10.1046/j.1360-0443.2003.00438.x. [DOI] [PubMed] [Google Scholar]
- Weiss RD, Griffin ML, Gallop RJ, Najavits LM, Frank A, Crits-Christoph P, Thase ME, Blaine J, Gastfriend DR, Daley D, Luborsky L. The effect of 12-step self-help group attendance and participation on drug use outcomes among cocaine-dependent patients. Drug Alcohol Depend. 2005;77:177–184. doi: 10.1016/j.drugalcdep.2004.08.012. [DOI] [PubMed] [Google Scholar]
- White WL. Recovery Management And Recovery-Oriented Systems Of Care: Scientific Rationale And Promising Practices. Northeast Addiction Technology Transfer Center, Great Lakes Addiction Technology Transfer Center, Philadelphia Department of Behavioral Health/Mental Retardation Services; Pittsburgh, PA: 2008. [Google Scholar]
- White WL. Recovery/Remission From Substance Use Disorders: An Analysis Of Reported Outcomes In 415 Scientific Reports, 1868-2011. Philadelphia Department of Behavioral Health and Intellectual Disability Services; Philadelphia, PA: 2012. [Google Scholar]