Abstract
Drug-induced liver injury is an important clinical problem and a challenge for drug development. Whereas progress in understanding rare and unpredictable (idiosyncratic) drug hepatotoxicity is severely hampered by the lack of relevant animal models, enormous insight has been gained in the area of predictable hepatotoxins, in particular acetaminophen-induced liver injury, from a broad range of experimental models. Importantly, mechanisms of toxicity obtained with certain experimental systems, such as in vivo mouse models, primary mouse hepatocytes, and metabolically competent cell lines, are being confirmed in translational studies in patients and in primary human hepatocytes. Despite this progress, suboptimal models are still being used and experimental data can be confusing, leading to controversial conclusions. Therefore, this review attempts to discuss mechanisms of drug hepatotoxicity using the most studied drug acetaminophen as an example. We compare the various experimental models that are used to investigate mechanisms of acetaminophen hepatotoxicity, discuss controversial topics in the mechanisms, and assess how these experimental findings can be translated to the clinic. The success with acetaminophen in demonstrating the clinical relevance of experimental findings could serve as an example for the study of other drug toxicities.
Keywords: Drug hepatotoxicity, Translational studies, Necrosis, Sterile inflammation
Introduction
Drug-induced liver injury (DILI) is a significant clinical problem worldwide. Fundamentally, DILI can be divided into two categories: idiosyncratic and predictive DILI. Idiosyncratic DILI is mainly caused by therapeutic doses of drugs in susceptible patients after days or months of treatment.1 It generally affects only <1 in 10,000 patients taking the drug and the symptoms can range from mild, transient liver injury and dysfunction to acute liver failure.2 The epidemiology and disease patterns of many idiosyncratic hepatotoxic drugs have been described; although the involvement of innate and adaptive immune mechanisms is thought to be critical in most cases, the actual mechanisms of liver injury remain largely unclear.3 The limited progress in the understanding of the pathogenesis of idiosyncratic DILI comes from the lack of relevant animal models and the rarity of the disease, which makes it difficult to study it in the first place. In addition, genome-wide association studies in a large cohort of DILI cases have failed to identify general risk factors for idiosyncratic DILI.4 These findings suggest that genetic determinants of DILI risk may be drug specific.4
In contrast, predictive DILI occurs mainly after intentional or accidental overdose of a drug. The most clinically relevant drug in this category is acetaminophen (APAP, paracetamol). In the US, APAP overdose is responsible for 78,000 emergency room visits and about 500 deaths per year.5 In addition, APAP hepatotoxicity is the most frequent cause of acute liver failure of any etiology, accounting for approximately 50% of all cases.6 Unlike idiosyncratic DILI, APAP hepatotoxicity can be modeled in rodents, primary hepatocytes and in certain cell lines. An increasing number of translational studies demonstrate that these animal models are valuable tools to investigate the mechanisms of toxicity and to identify potential therapeutic targets.7 However, despite the unique situation of having relevant in vivo and in vitro experimental systems available, there are still many controversies that hamper progress in understanding the mechanisms of APAP hepatotoxicity and, consequently, the reliable identification of clinically relevant therapeutic targets. This review will address these controversial topics, including intracellular signaling mechanisms of toxicity, mode of cell death, and the role of sterile inflammation from animal models to the most recent clinical findings.
Acetaminophen: Intracellular mechanisms of toxicity
Many drugs cause hepatotoxicity by forming reactive metabolites, which either initiate cell toxicity mechanisms directly or, through formation of protein adducts (haptens), can trigger immune-mediated toxicity.8,9 For APAP, it is well established that the cell death mechanisms are initiated by the formation of the presumed reactive metabolite N-acetyl-p-benzoquinone imine (NAPQI), which is generated mainly by the cytochrome P450 enzymes Cyp2e1 and 1a2 in mice and humans.10,11 Although NAPQI can be readily detoxified by conjugation with glutathione (GSH), the availability of GSH is limited in case of an overdose.12 The resulting depletion of GSH enables reactions of NAPQI with protein sulfhydryl groups of cysteine, causing the binding of APAP to cellular proteins.12 Originally, it was thought that the protein adducts formed could directly trigger cell death, but no critical protein target could be identified.13 In contrast, it was recognized that the binding to mitochondrial proteins after APAP overdose correlated with toxicity,14 suggesting that mitochondria could be a critical target. This observation was in agreement with the impaired mitochondrial respiration and increased mitochondrial oxidant stress observed after APAP overdose in mice (Fig. 1).15,16 The enhanced superoxide formation leads to generation of the potent oxidant peroxynitrite in mitochondria.17 This oxidant stress, together with the uptake of lysosomal iron,18 causes the formation of the mitochondrial membrane permeability transition (MPT) pore, which is responsible for the collapse of the membrane potential and cessation of ATP synthesis.19–21 The critical role of this oxidant stress for mitochondrial dysfunction and cell necrosis has been shown by the protective effects of delayed treatment with GSH or N-acetylcysteine (NAC)22–24 and the aggravation of injury in mice with reduced MnSod (Sod2) activity in mitochondria.25,26
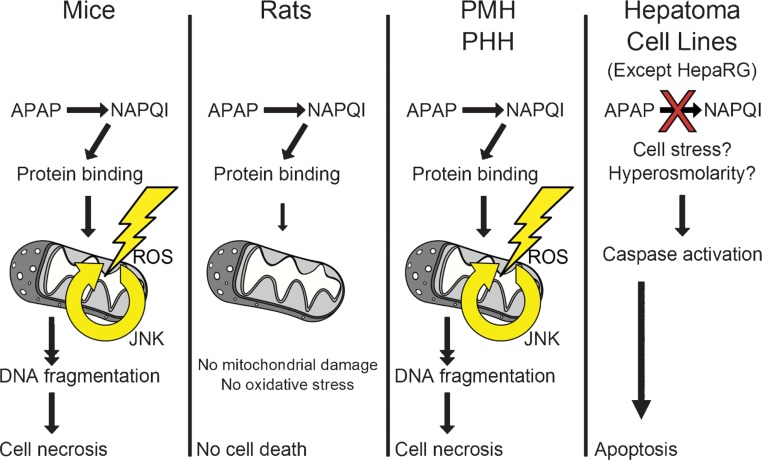
Fig. 1. Experimental models to study acetaminophen (APAP) hepatotoxicity.
The most common models used to study APAP hepatotoxicity are mice, rats, primary mouse and human hepatocytes (PMH and PHH, respectively), and hepatoma cell lines. However, the mechanisms of injury and mode of cell death differ. In mouse models and in humans, APAP-induced liver injury involves mitochondrial damage, oxidative stress, c-jun N-terminal kinase (JNK) activation, and nuclear DNA fragmentation. The mode of cell death in these models is oncotic necrosis. However, rats develop little or no oxidative stress and thus no injury, while hepatoma cells may develop injury but through different mechanisms than mouse or human hepatocytes. In the latter case, the mode of cell death is almost always apoptosis. The results suggest that mice and PHH are the best available models for the study of APAP toxicity.
Although the importance of the mitochondrial oxidant stress is well established,27 there is a discrepancy between early GSH depletion and mitochondrial dysfunction with some oxidant stress and the delayed necrosis.28 This led to the hypothesis that the initial oxidant stress is insufficient to trigger the MPT and a “second hit” is needed to amplify this oxidant stress. This second hit appears to be the mitogen-activated protein (MAP) kinase c-jun-N-terminal kinase (JNK) (Fig. 1), which is activated (phosphorylated) in the cytosol very early during APAP toxicity in mice.29 P-JNK then translocates to the mitochondria and triggers the MPT by amplifying the mitochondrial oxidant stress.29,30 The effect of P-JNK on the mitochondria is mediated by interaction with the mitochondrial protein Sab (SH3 domain-binding protein that preferentially associates with Btk), which is located in the outer membrane.31 Knock-down of Sab attenuated JNK activation and prevented APAP-induced liver injury, suggesting that Sab is a critical link between JNK activation and mitochondrial dysfunction.31 The critical role of JNK in the pathophysiology of APAP-induced liver injury has been documented by the protective effect of a JNK inhibitor and by gene knock-down experiments.32 However, JNK does not seem to be directly activated by the early events of APAP toxicity. Instead, a number of upstream kinases have been identified, all of which can be activated directly or indirectly by the early oxidant stress generated during APAP-induced mitochondrial dysfunction. These kinases include apoptosis signal-regulating kinase 1 (ASK1),33 glycogen synthase kinase-3beta (GSK-3β),34 mixed-lineage kinase 3 (MLK 3),35 receptor interacting protein kinase (RIP) 136 and RIP3.37 However, several phosphatases that counteract JNK activation have been shown to protect against APAP toxicity, including MAP kinase phosphatase 1 (Mkp-1) and protein tyrosine phosphatase 1B.38,39 Thus, the amplification of the mitochondrial oxidant stress involves a complex and redundant network of kinases and phosphatases. However, the JNK-dependent and independent kinase network may not only be involved in pro-death signaling pathways but can also promote survival mechanisms such as promoting autophagy, as discussed later.40
A consequence of the mitochondrial dysfunction is nuclear DNA damage (Fig. 1). Genomic DNA fragmentation as a hallmark of APAP toxicity in mice and mouse hepatocytes has been recognized for some time.41,42 DNA fragments can be internucleosomal fragments of approximately 180 base pairs and multiples thereof, as detected by DNA ladder.41 This implicates a role for endonucleases in this process rather than oxidant stress.17 The nuclear translocation of endonuclease G and apoptosis inducing factor (AIF) from the mitochondria correlates with the nuclear DNA fragmentation.43,44 Endonuclease G and AIF, which are mitochondrial intermembrane proteins, are released initially by mitochondrial outer membrane permeabilization through a Bcl2-associated X protein (bax) pore and later, after the MPT and mitochondrial matrix swelling, by rupture of the outer membrane.45 The DNA damage can activate DNA repair processes including poly(ADP-ribose) polymerase (PARP), which may accelerate cell death by excessive consumption of nicotinamide-adenine dinucleotide (NAD). Although APAP-induced DNA damage activates PARP and depletes NAD, the absence of the enzyme actually enhanced the injury, indicating that activation of DNA repair is beneficial.46 Thus, DNA damage caused by mitochondria-derived endonuclease and others contribute to cell necrosis, and attempts to repair the damage limit the injury and support recovery.
Damaged mitochondria are critical for the pathophysiology of APAP-induced cell death. Endogenous defense systems (autophagy) can remove damaged cell organelles and modified protein by enveloping them with membranes (autophagosomes) and fusing these structures with lysosomes.47 Autophagy is activated after APAP overdose.48 Inhibition of autophagy attenuates liver injury, suggesting that autophagy is an adaptive mechanism to stress and limits injury.48 In addition to classical autophagy mechanisms, newly recognized mitochondrial spheroids can also contribute to the removal of damaged mitochondria.49 However, these processes are only effective in the outer area of risk.47 Additional effects, such as drp1 translocation to mitochondria that promotes mitochondrial fission, appear to enhance cell death.37 The role of mitochondria biogenesis remains unclear because the protection against APAP-induced liver damage by peroxisome proliferator-activated receptor gamma coactivator (PGC)-1alpha,was caused by the activation of nuclear factor-like 2 (Nrf-2)-dependent antioxidant genes.50 Thus, adaptive mechanisms to drug-induced cellular stress are clearly affecting liver injury and could be potential drug targets.
The vast majority of APAP-induced liver injury studies focus on hepatocytes. However, non-parenchymal cells may also play a role. In addition to resident and newly recruited inflammatory cells, which will be discussed later, sinusoidal endothelial cells (SECs) can be affected by an APAP overdose.51 Direct morphological evidence of SEC damage and indirect evidence of SEC dysfunction (hemorrhage) have been reported.52–54 Nitrotyrosine staining in SECs precedes staining of hepatocytes, suggesting that SEC damage may be independent of parenchymal cell injury.55 Isolated SECs exposed to APAP from specific mouse strains show substantial GSH depletion56 and lactoferrin protects SECs from APAP-induced injury in specific mouse strains.57 The strain-dependent SEC injury correlates with Cyp2E1 levels in these SECs.57 In addition, severe SEC injury in susceptible strains leads to extensive congestion and microvascular dysfunction and also impacts parenchymal cell injury.52,56,57
All of the discussed mechanisms of APAP-induced liver injury were investigated using a number of different in vivo and in vitro models. Selecting the most appropriate experimental model, which closely resembles the human pathophysiology, is critical for the clinical relevance of the mechanisms derived from these models.
In vivo models of drug hepatotoxicity
The most frequently used preclinical species for drug hepatotoxicity are rats and mice. Testing new drugs in rats is still required for standard safety evaluations by regulatory agencies. In the case of APAP-induced DILI, the rat is clearly a poor model.12 Rats can metabolize APAP to form a reactive metabolite and cause GSH depletion and protein adducts formation, even in mitochondria.58 However, they do not develop mitochondrial oxidant stress or JNK activation and consequently develop very little if any liver injury (Fig. 1).58 It remains unclear at this point if the lack of progression in rat liver is due to the delay in protein adducts formation, or if as of yet unidentified specific protein targets are not hit by NAPQI. Although there is the potential to learn more about the initiating events, the mechanisms of injury in rats and the severity of injury do not reflect the human pathophysiology. Nevertheless, large numbers of studies are still being published that test the hepatoprotective potential of natural products using the rat model (reviewed59). In addition to using an insensitive animal model for their drug hepatotoxicity studies, another caveat of most of these investigations is that the plant extracts are largely uncharacterized and the potential effect as a P450 inhibitor of one or more of the chemicals in the extract is rarely tested.
The mouse model of APAP hepatotoxicity was established in the 1970s.12 Based on the early mechanistic understanding, NAC was developed as an antidote against APAP overdose.60 More recently, the use of gene knock-out or transgenic mice has helped to further popularize the mouse model for investigation of DILI. Most of the mechanistic insight into the pathophysiology has been gained from experiments with the murine system. Fortunately, many fundamental mechanisms of APAP hepatotoxicity in the mouse have been confirmed in patients with APAP overdose61 and in human hepatocytes.62,63 In addition, the severity of the overall liver injury is very similar between mice and humans.61 However, the injury process progresses much faster in mice than in humans, with peak alanine aminotransferase (ALT) values, as indicator of liver cell death, between 12 and 24 h in the mouse64 and 36–48 h in humans after overdose.65 The reason for this delay in humans does not appear to be reduced drug metabolism and reactive metabolite formation but may be related to delayed mitochondrial protein binding and delayed JNK activation.63 Thus, the mouse model of APAP hepatotoxicity is superior to other animal models and most closely resembles the human pathophysiology in terms of liver injury and recovery. In the future, large animal models may be needed to better mimic the acute liver failure observed in humans.66
In vitro models of APAP-induced hepatocyte cell death
In vitro models are indispensable tools to identify drug toxicity and assess molecular mechanisms. Many of the mechanistic details described in previous paragraphs were investigated in freshly isolated mouse hepatocytes. However, in addition to the obvious advantages of an isolated cell preparation, there are limitations that need to be considered.67 Among others, primary hepatocytes lack non-parenchymal cells, they are exposed to artificial media during isolation and culture, and they are generally cultured under hyperoxic conditions (room air oxygen levels).67 This may lead to numerous gene expression changes, enhanced oxidant stress, and many other potential modifications.67,68 Loss of cytochrome P450 enzyme activity over time in primary cells in culture is one of the most critical gene expression changes in studies of drug toxicity.69 This will affect the sensitivity to drugs such as APAP. Recent advances in sandwich culture techniques and 3D culture ameliorate some of these problems,67 but this improvement comes with a price. These additional manipulations are more cumbersome and time consuming and likely increase the cost of the experiments. Nevertheless, studies with primary cultured hepatocytes can provide new mechanistic understanding if the limitations are considered and the data are verified in vivo.
In contrast to primary hepatocytes, many established hepatocyte cell lines are readily available. An advantage of these cells is that they proliferate easily, can be cryopreserved and thawed out without much loss of functionality, are easy to work with, and are available in large quantities. However, most of these immortalized cell lines, including the most popular hepatoma cell lines (e.g. HepG2, Hep3B, Huh7) have a drastically modified gene expression profile and lack, among other critical proteins, essential drug metabolizing enzymes and transporters (Fig. 1).70,71 The caveat of working with these types of cells is that they still respond to cellular stress such as APAP exposure with changes in gene or protein expression.72 However, the relevance to human pathophysiology is questionable because the nature of the stress is different than a cell that has the capacity to generate a reactive metabolite. This discrepancy is most clearly demonstrated by the fact that APAP causes apoptotic cell death in hepatoma cell lines73 but necrosis in primary hepatocytes.19,28,42,63 If these hepatoma cells are transfected with a specific cytochrome P450, e.g. CYP2E1, some of the sensitivity can be restored.74
HepaRG cells are hepatoma cells isolated and differentiated from a patient with hepatocellular carcinoma that are metabolically competent, i.e. express a large number of drug metabolizing enzymes, including P450 enzymes, and transporter similar to primary hepatocytes.70 Although there are some limitations of these cells, such as being derived from a single donor and differentiating into both hepatocytes and biliary epithelial cells, the fact that they are metabolically competent hepatoma cells with unlimited availability is a major advantage over most other hepatoma cell lines.70 Consequently, upon exposure to APAP, HepaRG cells develop cell necrosis with many mechanistic characteristics similar to mouse hepatocytes but with a time line closely resembling that of human overdose patients.62
Primary human hepatocytes (PHH) are the most relevant in vitro model for studying human pathophysiology. However, availability is limited and it can be prohibitively expensive. Cryopreservation of cells can make them more easily available, but in general, cryopreserved cells are of lower quality. While these cryopreserved cells may be suitable for drug metabolism studies, they are not useful for many other types of experiments. This is especially important for drug toxicity studies. Freshly isolated cultured human cells are clearly superior as they reflect closely the gene expression pattern of the liver in vivo. Recent studies with APAP hepatotoxicity documented the very close correlation between the time line of toxicity (onset and peak of cell death) in PHH and onset and peak of ALT elevation as an indicator of liver injury in overdose patients.63,65 However, the overall sequence of events leading to cell death after APAP in PHH is very similar to mouse hepatocytes, including GSH depletion, cytosolic and mitochondrial protein adducts formation, JNK activation and translocation to mitochondria, mitochondrial dysfunction, and collapse of the mitochondrial membrane potential preceding cell death (Fig. 1).63 Importantly, APAP induces necrotic cell death in PHH similar to mouse hepatocytes.63 Overall, like the translational work with overdose patient, these studies with PHH confirm that the mouse model of APAP hepatotoxicity is the most relevant animal model for studying these mechanisms.
Despite using clinically relevant experimental models, some topics remain controversial. This is almost always an issue of experimental design and interpretation of experimental data.
Mechanisms of drug-induced cell death: Apoptosis versus necrosis
The mode of cell death during APAP hepatotoxicity is controversial. Although the vast majority of animal studies have concluded that the injury is caused by necrosis, an increasing number of reports suggest that apoptotic cell death plays a significant role. The key problem is that there are very few specific parameters for apoptosis, and even those can be misinterpreted. For example, frequently used parameters such as mitochondrial cytochrome c release, increased bax protein expression and bax translocation to the mitochondria, BH3 interacting domain death agonist (bid) cleavage, DNA strand breaks (terminal deoxynucleotidyltransferase dUTP nick end labeling (TUNEL) assay), and DNA laddering (internucleosomal DNA cleavage) are all observed during apoptosis and necrosis, not allowing any distinction between these forms of cell death.75
One of the more specific features of apoptosis is the activation of caspases, including the initiator caspase-8 and the executioner caspase-3.76 An extensive increase in caspase activity in combination with processing of procaspases to the active fragments can be easily detected during hepatic apoptosis.77 Consequently, caspase inhibitors are highly effective in preventing apoptosis in the liver.77 In contrast, during APAP-induced liver injury, no increase in caspase-3 activity is detectable, and caspase inhibitors offer no protection.78 A caveat of the use of pancaspase inhibitors is the fact that they generally require the solvent dimethyl sulfoxide (DMSO), a potent inhibitor of P450 enzymes,79 and higher doses of caspase inhibitors may inhibit other proteases through off-target effects.80
DNA fragmentation is observed during apoptotic and necrotic cell death. Predominantly small fragments are formed during apoptosis, and larger fragments are generated during APAP-induced necrosis.81 The characteristic smaller DNA fragments during apoptosis (multiples of 180–185 base-pairs) are formed by caspase-activated DNase (CAD).76 In contrast, DNA fragmentation during APAP-induced cell death is caused by mitochondria-derived endonuclease G and AIF, as discussed above.43,44 One of the most frequently used assays to visualize DNA strand breaks is the TUNEL assay. Because the assay detects DNA strand breaks, apoptotic and necrotic cells will stain positive. However, the staining patterns are different, with mainly nuclear staining in apoptotic cells and both nuclear and cytosolic staining in necrotic cells.75 The cytosolic staining is likely caused by the release of large DNA fragments due to karyorrhexis and karyolysis, which are still recognized by the terminal deoxynucleotidyltransferase.
In patients, nuclear DNA fragments were detectable in plasma after APAP overdose.61 However, similar to the mouse model, extensive procaspase-3 protein levels were observed in blood of patients with APAP-induced liver injury but not in patients without liver injury.61 In support of these findings, no caspase-3 enzyme activity was measured in any APAP overdose patient.61 In addition, the caspase-cleaved cytokeratin-18 fragment was either not detectable or represented only a minor fraction (<15%) of the total full-length cytokeratin-18 released into the blood in these patients.82 Together these results in patients and, as discussed in the previous paragraph, in PHH support the hypothesis that, similar to mice and mouse hepatocytes, the primary mode of cell death in APAP hepatotoxicity in humans is necrosis.
As the example of APAP-induced liver injury demonstrates, a clear distinction between apoptotic and necrotic cell death cannot be achieved by assessing a single parameter. Use of a combination of parameters, e.g., caspase activation, cell morphology, and DNA fragmentation, is mandatory for solid conclusions. In addition, the use of positive controls will give insight into how much parameters change with a certain percentage of apoptosis and allow more confident conclusions regarding the mode of cell death. Knowledge of the type of cell death is not only important because of the intracellular signaling pathways involved, but also because it determines the degree of inflammation that occurs in response to the tissue damage.
Pathophysiological implications of sterile inflammation
Extensive cell necrosis causes the release of cell contents, as indicated by the massive increase of liver enzymes in serum. In recent years, it has been recognized that many of these cellular components can activate various pattern recognition receptors, such as toll like receptors (TLRs).83,84 These damage-associated molecular patterns (DAMPs) released by cells include high mobility group box 1 (HMGB1) protein, nuclear DNA fragments, mitochondrial DNA (mtDNA), heat shock proteins, hyaluronic acid, and many more.83,84 DAMPs can activate TLRs on macrophages (e.g. DNA binds to TLR9, HMGB1and heat shock proteins work through TLR4) to induce the transcription of pro-inflammatory cytokines and activate the inflammasome, which can trigger the cleavage of proforms of certain interleukins (IL) and other cytokines (e.g. pro-IL-1β, and pro-IL-18). Extensive cytokine formation and release recruits neutrophils and monocytes into the liver with the potential to aggravate the initial injury. This general scheme of a sterile inflammatory response has been investigated in the mouse model of APAP-induced liver injury in vivo. During APAP hepatotoxicity, HMGB1, DNA fragments, heat shock proteins, and others are detectable in plasma,61,85,86 as are the formation of cytokines53 and the recruitment of first neutrophils53,87 and later monocytes.88 Thus, there is no doubt that the severe cell necrosis induces an extensive sterile inflammatory response in mice. However, it is controversial whether neutrophils and macrophages actually enhance the injury or contribute to the repair and recovery of the damaged liver by removing cell debris. Although a few studies have suggested direct involvement of neutrophils, most studies do not find evidence for neutrophil cytotoxicity aggravating APAP-induced liver injury (reviewed84). Importantly, liver neutrophils are not activated during the injury phase, and deficiency of key neutrophil adhesion molecules has no effect on APAP toxicity.89 In addition, release of acetylated HMGB1 as indicator of macrophage activation is delayed in mice and occurs at the end of the injury phase.85 Taken together, these findings suggest that neutrophils, in addition to monocytes, are recruited into the liver in preparation for regeneration.84,88 Cytokines generated during the sterile inflammatory response may modulate intracellular events and promote injury by inducing inducible nitric oxide synthase and enhancing peroxynitrite formation.90
In APAP overdose patients, DAMPs such as nuclear DNA fragments, mtDNA, and HMGB1 are extensively released into the plasma with a time course similar to ALT and aspartate aminotransferase (AST).61,82 Interestingly, serum levels of these DAMPs are better predictors of poor outcome (liver failure and death) than ALT or AST.82,91 Certain cytokines, including IL-6, IL-8, and monocyte chemoattractant protein 1, are substantially elevated during APAP toxicity.92 However, neutrophils are not activated in patients during the peak of liver injury.93 Neutrophil activation correlates with declining ALT levels, i.e. with the recovery phase during APAP overdose in patients.93 These findings suggest that no direct neutrophil cytotoxicity is involved in the human pathophysiology. Similarly, hepatic macrophages derived from resident Kupffer cells and recruited monocytes contribute to the tissue repair process during APAP-induced acute liver failure rather than aggravate the injury.94 In addition to removing necrotic tissue, the lost liver cells need to be replaced by proliferation of surviving cells.
Regeneration
Liver regeneration is an intricate and well-orchestrated process. The remnant liver will proliferate to reestablish the original architecture and function after surgical or toxicological insult.95,96 In some cases, the remaining hepatocytes will proliferate in a hyperplastic manner to restore the functional liver mass, while in others, liver progenitor cells will participate to generate new hepatocytes.96–98 Generally, the production of tumor necrosis factor (TNF) α and IL-6 by non-parenchymal cells will prime the hepatocytes for proliferation, and cooperative signals from vascular endothelial growth factors (VEGF), epidermal growth factors (EGF), hepatocyte growth factors (HGF), and cytokines will stimulate hepatocytes to overcome cell-cycle checkpoints to proliferate and regain the normal liver size. This is followed by termination of regeneration, which is primarily mediated by TGF-β and renewed quiescence.95,97
Considerable progress has been made in our understanding of the central mediators of liver regeneration. TNF receptor knockout mice exhibit exaggerated injury and impaired regenerative responses after APAP, which can be explained by delayed mitogenic cytokine signaling.99 In mice, APAP time-dependently induces IL-6 levels in serum and liver.23,100,101 IL-6 knockout mice are more susceptible to APAP challenge101 and display a delayed injury resolution due to impaired liver regeneration.102 In addition, APAP triggers a significant upregulation of VEGF in mice,103 while pharmacological inhibition of VEGF resulted in similar injury but decreased recovery.103 Administering human recombinant VEGF mitigates the injury after APAP and facilitates regeneration in mice.104 Indirectly, scavenging peroxynitrite by glutathione treatment also enhances regeneration in mice after APAP.100
More recent data have provided insights about additional players in liver regeneration after APAP. The Wnt/β-catenin pathway is emerging as a central player in the regulation of liver development, growth, and regeneration;105 and its importance in APAP-induced hepatotoxicity has been explored. Biphasic increases of β-catenin expression are observed in mice, and β-catenin knockout mice have reduced liver regeneration.106 Interestingly, the evaluation of human liver biopsy samples has indicated that β-catenin activation is strongly associated with patients who undergo spontaneous regeneration without liver transplantation.106 Similarly, increased serum alpha-fetoprotein, a sign of hepatic regeneration,107 correlates with a favorable outcome in APAP overdose patients.108,109 From studies like these, a better understanding of liver regeneration may lead to improved prognostic indicators that can supplement existing criteria to determine candidates for liver transplantation among APAP overdose patients.
Conclusions
APAP-induced liver injury is the most frequently encountered drug hepatotoxicity and cause of acute liver failure in the United States. In addition, APAP is the most used experimental model to generate DILI. During the last decade, there has been substantial progress in understanding the intracellular mechanisms of cell death, sterile inflammation, and recovery after APAP overdose. The most relevant models that have fueled this new knowledge are in vivo mouse models, primary mouse and human hepatocytes, and certain metabolically competent hepatoma cell lines (e.g. HepaRG) (Fig. 1). Additional models, such as humanized mice, are in development and could expand the experimental tool box. Importantly, translational studies with patients provide support for the clinical relevance of many experimental models. It can be expected that this increased insight into toxicity mechanisms in experimental models and in humans will lead to improved therapeutic interventions and better strategies to detect potential relevant hepatotoxic drugs in development. Furthermore, the success with APAP from understanding experimental systems to the human pathophysiology could serve as an example for making relevant progress in other areas of drug hepatotoxicity.
Acknowledgements
Work in the authors' laboratory was supported in part by grants from the National Institutes of Health (R01 DK070195 and R01 AA12916), the National Center for Research Resources (5P20RR021940-07), and the National Institute of General Medical Sciences (8 P20 GM103549-07) of the National Institutes of Health. Additional support came from the “Training Program in Environmental Toxicology” T32 ES007079-26A2 (to M.R.M.) from the National Institute of Environmental Health Sciences.
Abbreviations
- AIF
apoptosis inducing factor
- ALT
alanine aminotransferase
- APAP
acetaminophen
- ASK1
apoptosis signal-regulating kinase 1
- AST
aspartate aminotransferase
- Bax
Bcl2-associated X protein
- CAD
caspase-activated DNase
- DAMPs
damage-associated molecular patterns
- DILI
drug-induced liver injury
- EGF
epidermal growth factor
- DMSO
dimethyl sulfoxide
- GSH
glutathione
- GSK-3β
glycogen synthase kinase-3beta
- HGF
hepatocyte growth factor
- HMGB1
high mobility group box 1 protein
- IL
interleukins
- JNK
c-jun N-terminal kinase
- MAP
mitogen-activated protein
- Mkp-1
MAP kinase phosphatase 1
- MPT
mitochondrial membrane permeability transition
- mtDNA
mitochondrial DNA
- NAC
N-acetylcysteine
- NAD
nicotinamide-adenine dinucleotide
- NAPQI
N-acetyl-p-benzoquinone imine
- Nrf-2
nuclear factor-like 2
- PARP
poly (ADP-ribose) polymerase
- PGC
proliferator-activated receptor gamma coactivator
- PHH
primary human hepatocytes
- RIP
receptor interacting protein kinase
- SECs
sinusoidal endothelial cells
- TLR
toll like receptors
- TNF
tumor necrosis factor
- TUNEL
terminal-deoxynucleoitidyl transferased UTP nick end labeling
- VEGF
vascular endothelial growth factors
References
- 1.Kaplowitz N. Idiosyncratic drug hepatotoxicity. Nat Rev Drug Discov. 2005;4:489–499. doi: 10.1038/nrd1750. 10.1038/nrd1750. [DOI] [PubMed] [Google Scholar]
- 2.Fontana RJ. Pathogenesis of idiosyncratic drug-induced liver injury and clinical perspectives. Gastroenterology. 2014;146:914–928. doi: 10.1053/j.gastro.2013.12.032. 10.1053/j.gastro.2013.12.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Uetrecht J, Naisbitt DJ. Idiosyncratic adverse drug reactions: current concepts. Pharmacol Rev. 2013;65:779–808. doi: 10.1124/pr.113.007450. 10.1124/pr.113.007450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Urban TJ, Shen Y, Stolz A, Chalasani N, Fontana RJ, Rochon J, et al. Limited contribution of common genetic variants to risk for liver injury due to a variety of drugs. Pharmacogenet Genomics. 2012;22:784–795. doi: 10.1097/FPC.0b013e3283589a76. 10.1097/FPC.0b013e3283589a76. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Budnitz DS, Lovegrove MC, Crosby AE. Emergency department visits for overdoses of acetaminophen-containing products. Am J Prev Med. 2011;40:585–592. doi: 10.1016/j.amepre.2011.02.026. 10.1016/j.amepre.2011.02.026. [DOI] [PubMed] [Google Scholar]
- 6.Lee WM. Acute liver failure. Semin Respir Crit Care Med. 2012;33:36–45. doi: 10.1055/s-0032-1301733. 10.1055/s-0032-1301733. [DOI] [PubMed] [Google Scholar]
- 7.McGill MR, Jaeschke H. Metabolism and disposition of acetaminophen: recent advances in relation to hepatotoxicity and diagnosis. Pharm Res. 2013;30:2174–2187. doi: 10.1007/s11095-013-1007-6. 10.1007/s11095-013-1007-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Srivastava A, Maggs JL, Antoine DJ, Williams DP, Smith DA, Park BK. Role of reactive metabolites in drug-induced hepatotoxicity. Handb Exp Pharmacol. 2010;196:165–194. doi: 10.1007/978-3-642-00663-0_7. 10.1007/978-3-642-00663-0_7. [DOI] [PubMed] [Google Scholar]
- 9.Williams CD, Jaeschke H. Role of the innate and adaptive immunity during drug-induced liver injury. Toxicol Res. 2012;1:161–170. 10.1039/c2tx20032e. [Google Scholar]
- 10.Zaher H, Buters JT, Ward JM, Bruno MK, Lucas AM, Stern ST, et al. Protection against acetaminophen toxicity in CYP1A2 and CYP2E1 double-null mice. Toxicol Appl Pharmacol. 1998;152:193–199. doi: 10.1006/taap.1998.8501. 10.1006/taap.1998.8501. [DOI] [PubMed] [Google Scholar]
- 11.Raucy JL, Lasker JM, Lieber CS, Black M. Acetaminophen activation by human liver cytochromes P450IIE1 and P450IA2. Arch Biochem Biophys. 1989;271:270–283. doi: 10.1016/0003-9861(89)90278-6. 10.1016/0003-9861(89)90278-6. [DOI] [PubMed] [Google Scholar]
- 12.Mitchell JR, Jollow DJ, Potter WZ, Gillette JR, Brodie BB. Acetaminophen-induced hepatic necrosis. IV. Protective role of glutathione. J Pharmacol Exp Ther. 1973;187:211–217. [PubMed] [Google Scholar]
- 13.Cohen SD, Pumford NR, Khairallah EA, Boekelheide K, Pohl LR, Amouzadeh HR, et al. Selective protein covalent binding and target organ toxicity. Toxicol Appl Pharmacol. 1997;143:1–12. doi: 10.1006/taap.1996.8074. 10.1006/taap.1996.8074. [DOI] [PubMed] [Google Scholar]
- 14.Tirmenstein MA, Nelson SD. Subcellular binding and effects on calcium homeostasis produced by acetaminophen and a nonhepatotoxicregioisomer, 3′-hydroxyacetanilide, in mouse liver. J Biol Chem. 1989;264:9814–9819. [PubMed] [Google Scholar]
- 15.Meyers LL, Beierschmitt WP, Khairallah EA, Cohen SD. Acetaminophen-induced inhibition of hepatic mitochondrial respiration in mice. Toxicol Appl Pharmacol. 1988;93:378–387. doi: 10.1016/0041-008x(88)90040-3. 10.1016/0041-008X(88)90040-3. [DOI] [PubMed] [Google Scholar]
- 16.Jaeschke H. Glutathione disulfide formation and oxidant stress during acetaminophen-induced hepatotoxicity in mice in vivo: the protective effect of allopurinol. J Pharmacol Exp Ther. 1990;255:935–941. [PubMed] [Google Scholar]
- 17.Cover C, Mansouri A, Knight TR, Bajt ML, Lemasters JJ, Pessayre D, et al. Peroxynitrite-induced mitochondrial and endonuclease-mediated nuclear DNA damage in acetaminophen hepatotoxicity. J Pharmacol Exp Ther. 2005;315:879–887. doi: 10.1124/jpet.105.088898. 10.1124/jpet.105.088898. [DOI] [PubMed] [Google Scholar]
- 18.Kon K, Kim JS, Uchiyama A, Jaeschke H, Lemasters JJ. Lysosomal iron mobilization and induction of the mitochondrial permeability transition in acetaminophen-induced toxicity to mouse hepatocytes. Toxicol Sci. 2010;117:101–108. doi: 10.1093/toxsci/kfq175. 10.1093/toxsci/kfq175. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Kon K, Kim JS, Jaeschke H, Lemasters JJ. Mitochondrial permeability transition in acetaminophen-induced necrosis and apoptosis of cultured mouse hepatocytes. Hepatology. 2004;40:1170–1179. doi: 10.1002/hep.20437. 10.1002/hep.20437. [DOI] [PubMed] [Google Scholar]
- 20.Masubuchi Y, Suda C, Horie T. Involvement of mitochondrial permeability transition in acetaminophen-induced liver injury in mice. J Hepatol. 2005;42:110–116. doi: 10.1016/j.jhep.2004.09.015. 10.1016/j.jhep.2004.09.015. [DOI] [PubMed] [Google Scholar]
- 21.Ramachandran A, Lebofsky M, Baines CP, Lemasters JJ, Jaeschke H. Cyclophilin D deficiency protects against acetaminophen-induced oxidant stress and liver injury. Free Radic Res. 2011;45:156–164. doi: 10.3109/10715762.2010.520319. 10.3109/10715762.2010.520319. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Knight TR, Ho YS, Farhood A, Jaeschke H. Peroxynitrite is a critical mediator of acetaminophen hepatotoxicity in murine livers: protection by glutathione. J Pharmacol Exp Ther. 2002;303:468–475. doi: 10.1124/jpet.102.038968. 10.1124/jpet.102.038968. [DOI] [PubMed] [Google Scholar]
- 23.James LP, McCullough SS, Lamps LW, Hinson JA. Effect of N-acetylcysteine on acetaminophen toxicity in mice: relationship to reactive nitrogen and cytokine formation. Toxicol Sci. 2003;75:458–467. doi: 10.1093/toxsci/kfg181. 10.1093/toxsci/kfg181. [DOI] [PubMed] [Google Scholar]
- 24.Saito C, Zwingmann C, Jaeschke H. Novel mechanisms of protection against acetaminophen hepatotoxicity in mice by glutathione and N-acetylcysteine. Hepatology. 2010;51:246–254. doi: 10.1002/hep.23267. 10.1002/hep.23267. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Fujimoto K, Kumagai K, Ito K, Arakawa S, Ando Y, Oda S, et al. Sensitivity of liver injury in heterozygous Sod2 knockout mice treated with troglitazone or acetaminophen. Toxicol Pathol. 2009;37:193–200. doi: 10.1177/0192623308329282. 10.1177/0192623308329282. [DOI] [PubMed] [Google Scholar]
- 26.Ramachandran A, Lebofsky M, Weinman SA, Jaeschke H. The impact of partial manganese superoxide dismutase (SOD2)-deficiency on mitochondrial oxidant stress, DNA fragmentation and liver injury during acetaminophen hepatotoxicity. Toxicol Appl Pharmacol. 2011;251:226–233. doi: 10.1016/j.taap.2011.01.004. 10.1016/j.taap.2011.01.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Jaeschke H, McGill MR, Ramachandran A. Oxidant stress, mitochondria, and cell death mechanisms in drug-induced liver injury: lessons learned from acetaminophen hepatotoxicity. Drug Metab Rev. 2012;44:88–106. doi: 10.3109/03602532.2011.602688. 10.3109/03602532.2011.602688. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Bajt ML, Knight TR, Lemasters JJ, Jaeschke H. Acetaminophen-induced oxidant stress and cell injury in cultured mouse hepatocytes: protection by N-acetyl cysteine. Toxicol Sci. 2004;80:343–349. doi: 10.1093/toxsci/kfh151. 10.1093/toxsci/kfh151. [DOI] [PubMed] [Google Scholar]
- 29.Hanawa N, Shinohara M, Saberi B, Gaarde WA, Han D, Kaplowitz N. Role of JNK translocation to mitochondria leading to inhibition of mitochondria bioenergetics in acetaminophen-induced liver injury. J Biol Chem. 2008;283:13565–13577. doi: 10.1074/jbc.M708916200. 10.1074/jbc.M708916200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Saito C, Lemasters JJ, Jaeschke H. c-Jun N-terminal kinase modulates oxidant stress and peroxynitrite formation independent of inducible nitric oxide synthase in acetaminophen hepatotoxicity. Toxicol Appl Pharmacol. 2010;246:8–17. doi: 10.1016/j.taap.2010.04.015. 10.1016/j.taap.2010.04.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Win S, Than TA, Han D, Petrovic LM, Kaplowitz N. c-Jun N-terminal kinase (JNK)-dependent acute liver injury from acetaminophen or tumor necrosis factor (TNF) requires mitochondrial Sab protein expression in mice. J Biol Chem. 2011;286:35071–35078. doi: 10.1074/jbc.M111.276089. 10.1074/jbc.M111.276089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Gunawan BK, Liu ZX, Han D, Hanawa N, Gaarde WA, Kaplowitz N. c-Jun N-terminal kinase plays a major role in murine acetaminophen hepatotoxicity. Gastroenterology. 2006;131:165–178. doi: 10.1053/j.gastro.2006.03.045. 10.1053/j.gastro.2006.03.045. [DOI] [PubMed] [Google Scholar]
- 33.Nakagawa H, Maeda S, Hikiba Y, Ohmae T, Shibata W, Yanai A, et al. Deletion of apoptosis signal-regulating kinase 1 attenuates acetaminophen-induced liver injury by inhibiting c-Jun N-terminal kinase activation. Gastroenterology. 2008;135:1311–1321. doi: 10.1053/j.gastro.2008.07.006. 10.1053/j.gastro.2008.07.006. [DOI] [PubMed] [Google Scholar]
- 34.Shinohara M, Ybanez MD, Win S, Than TA, Jain S, Gaarde WA, et al. Silencing glycogen synthase kinase-3beta inhibits acetaminophen hepatotoxicity and attenuates JNK activation and loss of glutamate cysteine ligase and myeloid cell leukemia sequence 1. J Biol Chem. 2010;285:8244–8255. doi: 10.1074/jbc.M109.054999. 10.1074/jbc.M109.054999. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Sharma M, Gadang V, Jaeschke A. Critical role for mixed-lineage kinase 3 in acetaminophen-induced hepatotoxicity. Mol Pharmacol. 2012;82:1001–1007. doi: 10.1124/mol.112.079863. 10.1124/mol.112.079863. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Zhang YF, He W, Zhang C, Liu XJ, Lu Y, Wang H, et al. Role of receptor interacting protein (RIP)1 on apoptosis-inducing factor-mediated necroptosis during acetaminophen-evoked acute liver failure in mice. Toxicol Lett. 2014;225:445–453. doi: 10.1016/j.toxlet.2014.01.005. 10.1016/j.toxlet.2014.01.005. [DOI] [PubMed] [Google Scholar]
- 37.Ramachandran A, McGill MR, Xie Y, Ni HM, Ding WX, Jaeschke H. Receptor interacting protein kinase 3 is a critical early mediator of acetaminophen-induced hepatocyte necrosis in mice. Hepatology. 2013;58:2099–2108. doi: 10.1002/hep.26547. 10.1002/hep.26547. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Wancket LM, Meng X, Rogers LK, Liu Y. Mitogen-activated protein kinase phosphatase (Mkp)-1 protects mice against acetaminophen-induced hepatic injury. Toxicol Pathol. 2012;40:1095–1105. doi: 10.1177/0192623312447551. 10.1177/0192623312447551. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Mobasher MA, González-Rodriguez A, Santamaría B, Ramos S, Martín Má, Goya L, et al. Protein tyrosine phosphatase 1B modulates GSK3β/Nrf2 and IGFIR signaling pathways in acetaminophen-induced hepatotoxicity. Cell Death Dis. 2013;4:626. doi: 10.1038/cddis.2013.150. 10.1038/cddis.2013.150. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Saberi B, Ybanez MD, Johnson HS, Gaarde WA, Han D, Kaplowitz N. Protein kinase C (PKC) participates in acetaminophen hepatotoxicity through c-jun-N-terminal kinase (JNK)-dependent and -independent signaling pathways. Hepatology. 2014;59:1543–1554. doi: 10.1002/hep.26625. 10.1002/hep.26625. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Ray SD, Sorge CL, Raucy JL, Corcoran GB. Early loss of large genomic DNA in vivo with accumulation of Ca2+ in the nucleus during acetaminophen-induced liver injury. Toxicol Appl Pharmacol. 1990;106:346–351. doi: 10.1016/0041-008x(90)90254-r. 10.1016/0041-008X(90)90254-R. [DOI] [PubMed] [Google Scholar]
- 42.Shen W, Kamendulis LM, Ray SD, Corcoran GB. Acetaminophen-induced cytotoxicity in cultured mouse hepatocytes: effects of Ca(2+)-endonuclease, DNA repair, and glutathione depletion inhibitors on DNA fragmentation and cell death. Toxicol Appl Pharmacol. 1992;112:32–40. doi: 10.1016/0041-008x(92)90276-x. 10.1016/0041-008X(92)90276-X. [DOI] [PubMed] [Google Scholar]
- 43.Bajt ML, Cover C, Lemasters JJ, Jaeschke H. Nuclear translocation of endonuclease G and apoptosis-inducing factor during acetaminophen-induced liver cell injury. Toxicol Sci. 2006;94:217–225. doi: 10.1093/toxsci/kfl077. 10.1093/toxsci/kfl077. [DOI] [PubMed] [Google Scholar]
- 44.Bajt ML, Ramachandran A, Yan HM, Lebofsky M, Farhood A, Lemasters JJ, et al. Apoptosis-inducing factor modulates mitochondrial oxidant stress in acetaminophen hepatotoxicity. Toxicol Sci. 2011;122:598–605. doi: 10.1093/toxsci/kfr116. 10.1093/toxsci/kfr116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Bajt ML, Farhood A, Lemasters JJ, Jaeschke H. Mitochondrial bax translocation accelerates DNA fragmentation and cell necrosis in a murine model of acetaminophen hepatotoxicity. J Pharmacol Exp Ther. 2008;324:8–14. doi: 10.1124/jpet.107.129445. 10.1124/jpet.107.129445. [DOI] [PubMed] [Google Scholar]
- 46.Cover C, Fickert P, Knight TR, Fuchsbichler A, Farhood A, Trauner M, et al. Pathophysiological role of poly(ADP-ribose) polymerase (PARP) activation during acetaminophen-induced liver cell necrosis in mice. Toxicol Sci. 2005;84:201–208. doi: 10.1093/toxsci/kfi065. 10.1093/toxsci/kfi065. [DOI] [PubMed] [Google Scholar]
- 47.Ni HM, Williams JA, Jaeschke H, Ding WX. Zonated induction of autophagy and mitochondrial spheroids limits acetaminophen-induced necrosis in the liver. Redox Biol. 2013;1:427–432. doi: 10.1016/j.redox.2013.08.005. 10.1016/j.redox.2013.08.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Ni HM, Bockus A, Boggess N, Jaeschke H, Ding WX. Activation of autophagy protects against acetaminophen-induced hepatotoxicity. Hepatology. 2012;55:222–232. doi: 10.1002/hep.24690. 10.1002/hep.24690. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Ding WX, Guo F, Ni HM, Bockus A, Manley S, Stolz DB, et al. Parkin and mitofusins reciprocally regulate mitophagy and mitochondrial spheroid formation. J Biol Chem. 2012;287:42379–42388. doi: 10.1074/jbc.M112.413682. 10.1074/jbc.M112.413682. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Ye D, Wang Y, Li H, Jia W, Man K, Lo CM, et al. FGF21 protects against acetaminophen-induced hepatotoxicity by potentiating PGC-1α-mediated antioxidant capacity in mice. Hepatology. 2014 doi: 10.1002/hep.27060. [DOI] [PubMed] [Google Scholar]
- 51.McCuskey RS. Sinusoidal endothelial cells as an early target for hepatic toxicants. Clin Hemorheol Microcirc. 2006;34:5–10. [PubMed] [Google Scholar]
- 52.Walker RM, Racz WJ, McElligott TF. Acetaminophen-induced hepatotoxic congestion in mice. Hepatology. 1985;5:233–240. doi: 10.1002/hep.1840050213. 10.1002/hep.1840050213. [DOI] [PubMed] [Google Scholar]
- 53.Lawson JA, Farhood A, Hopper RD, Bajt ML, Jaeschke H. The hepatic inflammatory response after acetaminophen overdose: role of neutrophils. Toxicol Sci. 2000;54:509–516. doi: 10.1093/toxsci/54.2.509. 10.1093/toxsci/54.2.509. [DOI] [PubMed] [Google Scholar]
- 54.Ito Y, Bethea NW, Abril ER, McCuskey RS. Early hepatic microvascular injury in response to acetaminophen toxicity. Microcirculation. 2003;10:391–400. doi: 10.1038/sj.mn.7800204. 10.1038/sj.mn.7800204. [DOI] [PubMed] [Google Scholar]
- 55.Knight TR, Kurtz A, Bajt ML, Hinson JA, Jaeschke H. Vascular and hepatocellular peroxynitrite formation during acetaminophen toxicity: role of mitochondrial oxidant stress. Toxicol Sci. 2001;62:212–220. doi: 10.1093/toxsci/62.2.212. 10.1093/toxsci/62.2.212. [DOI] [PubMed] [Google Scholar]
- 56.DeLeve LD, Wang X, Kaplowitz N, Shulman HM, Bart JA, van der Hoek A. Sinusoidal endothelial cells as a target for acetaminophen toxicity. Direct action versus requirement for hepatocyte activation in different mouse strains. Biochem Pharmacol. 1997;53:1339–1345. doi: 10.1016/s0006-2952(97)00048-8. 10.1016/S0006-2952(97)00048-8. [DOI] [PubMed] [Google Scholar]
- 57.Yin H, Cheng L, Holt M, Hail N, Jr, Maclaren R, Ju C. Lactoferrin protects against acetaminophen-induced liver injury in mice. Hepatology. 2010;51:1007–1016. doi: 10.1002/hep.23476. 10.1002/hep.23476. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.McGill MR, Williams CD, Xie Y, Ramachandran A, Jaeschke H. Acetaminophen-induced liver injury in rats and mice: comparison of protein adducts, mitochondrial dysfunction, and oxidative stress in the mechanism of toxicity. Toxicol Appl Pharmacol. 2012;264:387–394. doi: 10.1016/j.taap.2012.08.015. 10.1016/j.taap.2012.08.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Jaeschke H, Williams CD, McGill MR, Xie Y, Ramachandran A. Models of drug-induced liver injury for evaluation of phytotherapeutics and other natural products. Food Chem Toxicol. 2013;55:279–289. doi: 10.1016/j.fct.2012.12.063. 10.1016/j.fct.2012.12.063. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Prescott LF, Park J, Ballantyne A, Adriaenssens P, Proudfoot AT. Treatment of paracetamol (acetaminophen) poisoning with N-acetylcysteine. Lancet. 1977;2:432–434. doi: 10.1016/s0140-6736(77)90612-2. 10.1016/S0140-6736(77)90612-2. [DOI] [PubMed] [Google Scholar]
- 61.McGill MR, Sharpe MR, Williams CD, Taha M, Curry SC, Jaeschke H. The mechanism underlying acetaminophen-induced hepatotoxicity in humans and mice involves mitochondrial damage and nuclear DNA fragmentation. J Clin Invest. 2012;122:1574–1583. doi: 10.1172/JCI59755. 10.1172/JCI59755. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.McGill MR, Yan HM, Ramachandran A, Murray GJ, Rollins DE, Jaeschke H. HepaRG cells: a human model to study mechanisms of acetaminophen hepatotoxicity. Hepatology. 2011;53:974–982. doi: 10.1002/hep.24132. 10.1002/hep.24132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Xie Y, McGill MR, Dorko K, Kumer SC, Schmitt TM, Forster J, et al. Mechanisms of acetaminophen-induced cell death in primary human hepatocytes. Toxicol Appl Pharmacol. 2014 Jun 3; doi: 10.1016/j.taap.2014.05.010. 10.1016/j.taap.2014.05.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.McGill MR, Lebofsky M, Norris HR, Slawson MH, Bajt ML, Xie Y, et al. Plasma and liver acetaminophen-protein adduct levels in mice after acetaminophen treatment: dose-response, mechanisms, and clinical implications. Toxicol Appl Pharmacol. 2013;269:240–249. doi: 10.1016/j.taap.2013.03.026. 10.1016/j.taap.2013.03.026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Larson AM. Acetaminophen hepatotoxicity. Clin Liver Dis. 2007;11:525–548. doi: 10.1016/j.cld.2007.06.006. 10.1016/j.cld.2007.06.006. [DOI] [PubMed] [Google Scholar]
- 66.Lee KC, Palacios Jimenez C, Alibhai H, Chang YM, Leckie PJ, Baker LA, et al. A reproducible, clinically relevant, intensively managed, pig model of acute liver failure for testing of therapies aimed to prolong survival. Liver Int. 2013;33:544–551. doi: 10.1111/liv.12042. 10.1111/liv.12042. [DOI] [PubMed] [Google Scholar]
- 67.Godoy P, Hewitt NJ, Albrecht U, Andersen ME, Ansari N, Bhattacharya S, et al. Recent advances in 2D and 3D in vitro systems using primary hepatocytes, alternative hepatocyte sources and non-parenchymal liver cells and their use in investigating mechanisms of hepatotoxicity, cell signaling and ADME. Arch Toxicol. 2013;87:1315–1530. doi: 10.1007/s00204-013-1078-5. 10.1007/s00204-013-1078-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Boess F, Kamber M, Romer S, Gasser R, Muller D, Albertini S, et al. Gene expression in two hepatic cell lines, cultured primary hepatocytes, and liver slices compared to the in vivo liver gene expression in rats: possible implications for toxicogenomics use of in vitro systems. Toxicol Sci. 2003;73:386–402. doi: 10.1093/toxsci/kfg064. 10.1093/toxsci/kfg064. [DOI] [PubMed] [Google Scholar]
- 69.LeCluyse E, Madan A, Hamilton G, Carroll K, DeHaan R, Parkinson A. Expression and regulation of cytochrome P450 enzymes in primary cultures of human hepatocytes. J Biochem Mol Toxicol. 2000;14:177–188. doi: 10.1002/(sici)1099-0461(2000)14:4<177::aid-jbt1>3.0.co;2-4. 10.1002/(SICI)1099-0461(2000)14:4<177::AID-JBT1>3.0.CO;2-4. [DOI] [PubMed] [Google Scholar]
- 70.Anthérieu S, Chesné C, Li R, Guguen-Guillouzo C, Guillouzo A. Optimization of the HepaRG cell model for drug metabolism and toxicity studies. Toxicol In Vitro. 2012;26:1278–1285. doi: 10.1016/j.tiv.2012.05.008. 10.1016/j.tiv.2012.05.008. [DOI] [PubMed] [Google Scholar]
- 71.Gerets HH, Tilmant K, Gerin B, Chanteux H, Depelchin BO, Dhalluin S, et al. Characterization of primary human hepatocytes, HepG2 cells, and HepaRG cells at the mRNA level and CYP activity in response to inducers and their predictivity for the detection of human hepatotoxins. Cell Biol Toxicol. 2012;28:69–87. doi: 10.1007/s10565-011-9208-4. 10.1007/s10565-011-9208-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Van Summeren A, Renes J, Bouwman FG, Noben JP, van Delft JH, Kleinjans JC, et al. Proteomics investigations of drug-induced hepatotoxicity in HepG2 cells. Toxicol Sci. 2011;120:109–122. doi: 10.1093/toxsci/kfq380. 10.1093/toxsci/kfq380. [DOI] [PubMed] [Google Scholar]
- 73.Manov I, Hirsh M, Iancu TC. N-acetylcysteine does not protect HepG2 cells against acetaminophen-induced apoptosis. Basic Clin Pharmacol Toxicol. 2004;94:213–225. doi: 10.1111/j.1742-7843.2004.pto940504.x. 10.1111/j.1742-7843.2004.pto940504.x. [DOI] [PubMed] [Google Scholar]
- 74.Dai Y, Cederbaum AI. Cytotoxicity of acetaminophen in human cytochrome P4502E1-transfected HepG2 cells. J Pharmacol Exp Ther. 1995;273:1497–1505. [PubMed] [Google Scholar]
- 75.Jaeschke H, Lemasters JJ. Apoptosis versus oncotic necrosis in hepatic ischemia/reperfusion injury. Gastroenterology. 2003;125:1246–1257. doi: 10.1016/s0016-5085(03)01209-5. 10.1016/S0016-5085(03)01209-5. [DOI] [PubMed] [Google Scholar]
- 76.Schattenberg JM, Galle PR, Schuchmann M. Apoptosis in liver disease. Liver Int. 2006;26:904–911. doi: 10.1111/j.1478-3231.2006.01324.x. 10.1111/j.1478-3231.2006.01324.x. [DOI] [PubMed] [Google Scholar]
- 77.Bajt ML, Lawson JA, Vonderfecht SL, Gujral JS, Jaeschke H. Protection against Fas receptor-mediated apoptosis in hepatocytes and nonparenchymal cells by a caspase-8 inhibitor in vivo: evidence for a postmitochondrial processing of caspase-8. Toxicol Sci. 2000;58:109–117. doi: 10.1093/toxsci/58.1.109. 10.1093/toxsci/58.1.109. [DOI] [PubMed] [Google Scholar]
- 78.Gujral JS, Knight TR, Farhood A, Bajt ML, Jaeschke H. Mode of cell death after acetaminophen overdose in mice: apoptosis or oncotic necrosis? Toxicol Sci. 2002;67:322–328. doi: 10.1093/toxsci/67.2.322. 10.1093/toxsci/67.2.322. [DOI] [PubMed] [Google Scholar]
- 79.Jaeschke H, Cover C, Bajt ML. Role of caspases in acetaminophen-induced liver injury. Life Sci. 2006;78:1670–1676. doi: 10.1016/j.lfs.2005.07.003. 10.1016/j.lfs.2005.07.003. [DOI] [PubMed] [Google Scholar]
- 80.Schotte P, Declercq W, Van Huffel S, Vandenabeele P, Beyaert R. Non-specific effects of methyl ketone peptide inhibitors of caspases. FEBS Lett. 1999;442:117–121. doi: 10.1016/s0014-5793(98)01640-8. 10.1016/S0014-5793(98)01640-8. [DOI] [PubMed] [Google Scholar]
- 81.Jahr S, Hentze H, Englisch S, Hardt D, Fackelmayer FO, Hesch RD, et al. DNA fragments in the blood plasma of cancer patients: quantitations and evidence for their origin from apoptotic and necrotic cells. Cancer Res. 2001;61:1659–665. [PubMed] [Google Scholar]
- 82.Antoine DJ, Jenkins RE, Dear JW, Williams DP, McGill MR, Sharpe MR, et al. Molecular forms of HMGB1 and keratin-18 as mechanistic biomarkers for mode of cell death and prognosis during clinical acetaminophen hepatotoxicity. J Hepatol. 2012;56:1070–1079. doi: 10.1016/j.jhep.2011.12.019. 10.1016/j.jhep.2011.12.019. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]
- 83.Kubes P, Mehal WZ. Sterile inflammation in the liver. Gastroenterology. 2012;143:1158–1172. doi: 10.1053/j.gastro.2012.09.008. 10.1053/j.gastro.2012.09.008. [DOI] [PubMed] [Google Scholar]
- 84.Jaeschke H, Williams CD, Ramachandran A, Bajt ML. Acetaminophen hepatotoxicity and repair: the role of sterile inflammation and innate immunity. Liver Int. 2012;32:8–20. doi: 10.1111/j.1478-3231.2011.02501.x. 10.1111/j.1478-3231.2011.02501.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Antoine DJ, Williams DP, Kipar A, Jenkins RE, Regan SL, Sathish JG, et al. High-mobility group box-1 protein and keratin-18, circulating serum proteins informative of acetaminophen-induced necrosis and apoptosis in vivo. Toxicol Sci. 2009;112:521–531. doi: 10.1093/toxsci/kfp235. 10.1093/toxsci/kfp235. [DOI] [PubMed] [Google Scholar]
- 86.Martin-Murphy BV, Holt MP, Ju C. The role of damage associated molecular pattern molecules in acetaminophen-induced liver injury in mice. Toxicol Lett. 2010;192:387–394. doi: 10.1016/j.toxlet.2009.11.016. 10.1016/j.toxlet.2009.11.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Cover C, Liu J, Farhood A, Malle E, Waalkes MP, Bajt ML, et al. Pathophysiological role of the acute inflammatory response during acetaminophen hepatotoxicity. Toxicol Appl Pharmacol. 2006;216:98–107. doi: 10.1016/j.taap.2006.04.010. 10.1016/j.taap.2006.04.010. [DOI] [PubMed] [Google Scholar]
- 88.Holt MP, Cheng L, Ju C. Identification and characterization of infiltrating macrophages in acetaminophen-induced liver injury. J Leukoc Biol. 2008;84:1410–1421. doi: 10.1189/jlb.0308173. 10.1189/jlb.0308173. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Williams CD, Bajt ML, Farhood A, Jaeschke H. Acetaminophen-induced hepatic neutrophil accumulation and inflammatory liver injury in CD18-deficient mice. Liver Int. 2010;30:1280–1292. doi: 10.1111/j.1478-3231.2010.02284.x. 10.1111/j.1478-3231.2010.02284.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Bourdi M, Masubuchi Y, Reilly TP, Amouzadeh HR, Martin JL, George JW, et al. Protection against acetaminophen-induced liver injury and lethality by interleukin 10: role of inducible nitric oxide synthase. Hepatology. 2002;35:289–298. doi: 10.1053/jhep.2002.30956. 10.1053/jhep.2002.30956. [DOI] [PubMed] [Google Scholar]
- 91.McGill MR, Staggs VS, Sharpe MR, Lee WM, Jaeschke H. Acute Liver Failure Study Group. Serum mitochondrial biomarkers and damage-associated molecular patterns are higher in acetaminophen overdose patients with poor outcome. Hepatology. 2014 Jun 13; doi: 10.1002/hep.27265. 10.1002/hep.27265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.James LP, Simpson PM, Farrar HC, Kearns GL, Wasserman GS, Blumer JL, et al. Cytokines and toxicity in acetaminophen overdose. J ClinPharmacol. 2005;45:1165–1171. doi: 10.1177/0091270005280296. 10.1177/0091270005280296. [DOI] [PubMed] [Google Scholar]
- 93.Williams CD, Bajt ML, Sharpe MR, McGill MR, Farhood A, Jaeschke H. Neutrophil activation during acetaminophen hepatotoxicity and repair in mice and humans. Toxicol Appl Pharmacol. 2014;275:122–133. doi: 10.1016/j.taap.2014.01.004. 10.1016/j.taap.2014.01.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Antoniades CG, Quaglia A, Taams LS, Mitry RR, Hussain M, Abeles R, et al. Source and characterization of hepatic macrophages in acetaminophen-induced acute liver failure in humans. Hepatology. 2012;56:735–746. doi: 10.1002/hep.25657. 10.1002/hep.25657. [DOI] [PubMed] [Google Scholar]
- 95.Michalopoulos GK. Liver regeneration. J Cell Physiol. 2007;213:286–300. doi: 10.1002/jcp.21172. 10.1002/jcp.21172. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Fausto N. Liver regeneration and repair: Hepatocytes, progenitor cells, and stem cells. Hepatology. 2004;39:1477–1487. doi: 10.1002/hep.20214. 10.1002/hep.20214. [DOI] [PubMed] [Google Scholar]
- 97.Taub R. Liver regeneration: from myth to mechanism. Nat Rev Mol Cell Biol. 2004;5:836–847. doi: 10.1038/nrm1489. 10.1038/nrm1489. [DOI] [PubMed] [Google Scholar]
- 98.Kofman AV, Morgan G, Kirschenbaum A, Osbeck J, Hussain M, Swenson S, et al. Dose-and time-dependent oval cell reaction in acetaminophen-induced murine liver injury. Hepatology. 2005;41:1252–1261. doi: 10.1002/hep.20696. 10.1002/hep.20696. [DOI] [PubMed] [Google Scholar]
- 99.Chiu H, Gardner CR, Dambach DM, Durham SK, Brittingham JA, Laskin JD, et al. Role of tumor necrosis factor receptor 1 (p55) in hepatocyte proliferation during acetaminophen-induced toxicity in mice. Toxicol Appl Pharmacol. 2003;193:218–227. doi: 10.1016/j.taap.2003.07.003. 10.1016/j.taap.2003.07.003. [DOI] [PubMed] [Google Scholar]
- 100.Bajt ML, Knight TR, Farhood A, Jaeschke H. Scavenging peroxynitrite with glutathione promotes regeneration and enhances survival during acetaminophen-induced liver injury in mice. J Pharmacol Exp Ther. 2003;307:67–73. doi: 10.1124/jpet.103.052506. 10.1124/jpet.103.052506. [DOI] [PubMed] [Google Scholar]
- 101.Masubuchi Y, Bourdi M, Reilly TP, Graf ML, George JW, Pohl LR. Role of interleukin-6 in hepatic heat shock protein expression and protection against acetaminophen-induced liver disease. Biochem Biophys Res Commun. 2003;304:207–212. doi: 10.1016/s0006-291x(03)00572-2. 10.1016/S0006-291X(03)00572-2. [DOI] [PubMed] [Google Scholar]
- 102.James LP, Lamps LW, McCullough S, Hinson JA. Interleukin 6 and hepatocyte regeneration in acetaminophen toxicity in the mouse. Biochem Biophys Res Commun. 2003;309:857–863. doi: 10.1016/j.bbrc.2003.08.085. 10.1016/j.bbrc.2003.08.085. [DOI] [PubMed] [Google Scholar]
- 103.Donahower B, McCullough SS, Kurten R, Lamps LW, Simpson P, Hinson JA, et al. Vascular endothelial growth factor and hepatocyte regeneration in acetaminophen toxicity. Am J Physiol Gastrointest Liver Physiol. 2006;291:G102–109. doi: 10.1152/ajpgi.00575.2005. 10.1152/ajpgi.00575.2005. [DOI] [PubMed] [Google Scholar]
- 104.Donahower BC, McCullough SS, Hennings L, Simpson PM, Stowe CD, Saad AG, et al. Human recombinant vascular endothelial growth factor reduces necrosis and enhances hepatocyte regeneration in a mouse model of acetaminophen toxicity. J Pharmacol Exp Ther. 2010;334:33–43. doi: 10.1124/jpet.109.163840. 10.1124/jpet.109.163840. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Thompson MD, Monga SP. WNT/beta-catenin signaling in liver health and disease. Hepatology. 2007;45:1298–1305. doi: 10.1002/hep.21651. 10.1002/hep.21651. [DOI] [PubMed] [Google Scholar]
- 106.Apte U, Singh S, Zeng G, Cieply B, Virji MA, Wu T, et al. Beta-catenin activation promotes liver regeneration after acetaminophen-induced injury. Am J Pathol. 2009;175:1056–1065. doi: 10.2353/ajpath.2009.080976. 10.2353/ajpath.2009.080976. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Taketa K. Alpha-fetoprotein: reevaluation in hepatology. Hepatology. 1990;12:1420–1432. doi: 10.1002/hep.1840120625. 10.1002/hep.1840120625. [DOI] [PubMed] [Google Scholar]
- 108.Schmidt LE, Dalhoff K. Alpha-fetoprotein is a predictor of outcome in acetaminophen-induced liver injury. Hepatology. 2005;41:26–31. doi: 10.1002/hep.20511. 10.1002/hep.20511. [DOI] [PubMed] [Google Scholar]
- 109.Schiødt FV, Ostapowicz G, Murray N, Satyanarana R, Zaman A, Munoz S, et al. Alpha-fetoprotein and prognosis in acute liver failure. Liver Transpl. 2006;12:1776–1781. doi: 10.1002/lt.20886. 10.1002/lt.20886. [DOI] [PubMed] [Google Scholar]