Abstract
OBJECTIVE:
Prophylactic indomethacin reduces severe intraventricular hemorrhage but may increase spontaneous intestinal perforation (SIP) in extremely low birth weight (ELBW) infants. Early feedings improve nutritional outcomes but may increase the risk of SIP. Despite their benefits, use of these therapies varies largely by physician preferences in part because of the concern for SIP.
METHODS:
This was a cohort study of 15 751 ELBW infants in the Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network from 1999 to 2010 who survived beyond 12 hours after birth. The risk of SIP was compared between groups of infants with and without exposure to prophylactic indomethacin and early feeding in unadjusted analyses and in analyses adjusted for center and for risks of SIP.
RESULTS:
Among infants exposed to prophylactic indomethacin, the risk of SIP did not differ between the indomethacin/early-feeding group compared with the indomethacin/no-early-feeding group (adjusted relative risk [RR] 0.74, 95% confidence interval [CI] 0.49–1.11). The risk of SIP was lower in the indomethacin/early-feeding group compared with the no indomethacin/no-early-feeding group (adjusted RR 0.58, 95% CI 0.37–0.90, P = .0159). Among infants not exposed to indomethacin, early feeding was associated with a lower risk of SIP compared with the no early feeding group (adjusted RR 0.53, 95% CI 0.36–0.777, P = .0011).
CONCLUSIONS:
The combined or individual use of prophylactic indomethacin and early feeding was not associated with an increased risk of SIP in ELBW infants.
Keywords: indomethacin, intestinal perforation, necrotizing enterocolitis, neonate
What’s Known on This Subject:
Prophylactic indomethacin in extremely low birth weight infants decreases severe intraventricular hemorrhage and patent ductus arteriosus but it is unknown whether concurrent enteral feeding and prophylactic indomethacin is associated with increased risk of spontaneous intestinal perforation.
What This Study Adds:
The combination of prophylactic indomethacin and enteral feeding during the first 3 days after birth does not increase the risk of spontaneous intestinal perforation.
Prophylactic indomethacin during the first 3 days after birth in extremely low birth weight (ELBW) infants (birth weight ≤1000 g) decreases the incidence of severe intraventricular hemorrhage and patent ductus arteriosus (PDA).1,2,3 However, administration of indomethacin soon after birth in preterm infants may be associated with an increased risk for spontaneous intestinal perforation (SIP)4–8 or necrotizing enterocolitis (NEC) with intestinal perforation.10 The incidence of SIP in ELBW infants is 6%.2,9 A large case-control study that compared 633 infants with SIP with 581 control infants matched by gestational age, birth weight, and gender showed that exposure to indomethacin during the first 3 days after birth was associated with a higher risk for SIP compared with control infants (odds ratio [OR] 1.86, 95% confidence interval [CI] 1.4–2.5, P < .0001).5 A retrospective study of ELBW infants in the Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network (NRN) showed that indomethacin treatment of a PDA but not the prophylactic use of indomethacin was associated with a higher risk for SIP (adjusted OR 1.61, 95% CI 1.25–2.08, P < .05).7 However, 3 randomized controlled trials2,3,11 and a retrospective cohort study of premature infants treated with indomethacin12 showed that neither SIP nor NEC was associated with the indomethacin exposure.
Although the presence of enteral nutrition has been studied as a risk factor for development of NEC,13,14 studies have not shown an association between enteral nutrition and SIP.15–17 A case-control study8 and a randomized controlled trial11 have shown that enteral feeding concurrent with treatment of a PDA with indomethacin results in fewer days to reach full enteral feeds without evidence of increased feeding intolerance or increased SIP or necrotizing enterocolitis. The question of whether ELBW infants who receive prophylactic indomethacin should concurrently receive enteral nutrition or have their feeds withheld temporarily because of the risk of SIP remains unanswered. In the absence of a randomized controlled trial to test the safety and efficacy of prophylactic indomethacin treatment concurrent with enteral feedings and to determine if a trial is feasible, we undertook this retrospective study. The Eunice Kennedy Shriver National Institute of Child Health and Human Development NRN Generic Database (GDB; NCT00063063)18 provides prospective longitudinal data pertaining to both indomethacin treatment within the first 24 hours after birth for any indication and the occurrence and timing of SIP. The primary hypothesis was that in ELBW infants, concomitant prophylactic intravenous indomethacin within the first 24 hours after birth, and any enteral feeding within the first 3 days after birth would be associated with a ≥20% increased relative risk of SIP during the first 14 days after birth compared with those who received prophylactic indomethacin but no feeding within the first 3 days after birth.
Methods
Study Design
This was a retrospective 2-by-2 factorial cohort study of 2 neonatal exposures: (1) prophylactic intravenous indomethacin initiated during the first 24 hours after birth and (2) early enteral nutrition defined as any feeding administered during the first 3 days after birth. Data pertaining to indomethacin treatment, feeding during the first 3 days after birth, and other demographic and perinatal variables were collected prospectively as previously described.19
Population and Exposures
The study population included 15 751 ELBW (birth weight 401–1000 g) infants who survived to at least 12 hours after birth within the member NICUs of the NRN during the study period 1999–2010. This study period was selected to represent a period when the practice of prophylactic indomethacin was increasingly prevalent based on the results of 2 trials in ELBW infants during the 1990s.2,3 The primary exposures examined within the GDB cohort included prophylactic intravenous indomethacin during the first 24 hours after birth (yes/no, I+/I–) and any enteral nutrition during the first 3 days after birth (yes/no, E+/E–). The GDB includes data on the administration of indomethacin for any prophylaxis purposes within the first 24 hours after birth.18 Indomethacin for the purpose of closing a PDA (ie, treatment) is recorded separately within the database. There were 4 study cohorts based on prophylactic indomethacin and early enteral feeding status: (1) group I+E+, infants who received prophylactic indomethacin (I+) during the first 24 hours and any enteral feeding (E+) during the first 3 days after birth; (2) group I+E–, infants who received prophylactic indomethacin (I+) during the first 24 hours and did not receive enteral feeding (E–) during the first 3 days after birth; (3) group I–E+, infants who did not receive prophylactic indomethacin (I–) during the first 24 hours but received enteral feeding (E+) during the first 3 days after birth; and (4) group I–E–, infants who did not receive prophylactic indomethacin (I–) during the first 24 hours and did not receive enteral feeding (E–) during the first 3 days after birth. The I–E– group was the nonexposed referent group for comparisons unless otherwise specified to examine the interaction of feeding and indomethacin.
Outcome Measures
The primary outcome of this study was SIP without NEC occurring within the first 14 days after birth. SIP was defined as a clinical diagnosis of spontaneous gastrointestinal perforation without signs suggestive of NEC. The secondary outcomes included death before discharge, NEC with intestinal perforation during the first 14 days after birth, death or survival with severe neurodevelopmental impairment (NDI) at 18- to 22-month follow-up, severe NDI in surviving infants at 18- to 22-month follow-up, indomethacin or ibuprofen treatment of PDA, and the need for surgical PDA treatment. NEC was defined according to the modified Bell staging criteria.20 Secondary nutritional outcomes included number of days to reach full enteral feeds, days of parenteral nutrition, and days to regain birth weight. Additional secondary outcomes included proven NEC with or without surgical treatment occurring anytime beyond day 14 after birth and SIP without NEC occurring anytime beyond day 14 after birth. The study had missing outcome data for some infants. There were 13 infants with SIP for whom the specific date of documentation of SIP was missing. In addition, there were 61 infants for whom the cause of death between 12 hours and 14 days after birth was missing. These missing outcome data resulted in slight differences in population denominators for the clinical outcomes shown in Table 2.
TABLE 2.
Clinical Outcomes*
| Outcome | I+E+ n = 1186 | I+E– n = 4688 | I–E+ n = 3128 | I–E– n = 6749 | ||||
|---|---|---|---|---|---|---|---|---|
| n/Total n (%) | aRR (95% CI) | n/Total n (%) | aRR (95% CI) | n/Total n (%) | aRR (95% CI) | n/Total n (%) | aRR (95% CI) | |
| SIP during first 14 d after birtha | 32/1182 (3) | 0.58 (0.37–0.90)* | 177/4673 (4) | 0.79 (0.60–1.04) | 35/3117 (1) | 0.53 (0.36–0.77)*** | 207/6705 (3) | Referent |
| SIP after day 14 after birtha,b | 8/1185 (0.7) | 0.48* (0.23–0.98) | 52/4684 (1) | 0.56 (0.40–0.79)**** | 25/3127 (0.8) | 0.83 (0.53–1.31) | 116/6742 (2) | Referent |
| Deaths: 12 h–14 da | 43/1184 (4) | 1.53 (1.03–2.28)* | 148/4674 (3) | 1.37 (1.03–1.82)* | 74/3119 (2) | 1.57 (1.17–2.12)*** | 175/6713 (3) | |
| Death before dischargea | 146/1185 (12) | 0.96 (0.81–1.14) | 742/4674 (16) | 1.16 (1.03–1.29)* | 287/3119 (9) | 0.94 (0.83–1.07) | 1037/6714 (16) | Referent |
| NEC with intestinal perforation duringfirst 14 d after birthb | 2/1185 (0.2) | 0.40 (0.10–1.69) | 15/4684 (0.3) | 0.60 (0.32–1.12) | 11/3127 (0.4) | 1.14 (0.56–2.33) | 32/6742 (0.5) | Referent |
| Death or severe NDI at 18- to 22-mo follow-up | 335/902 (37) | 0.83 (0.75–0.91)** | 1754/3608 (49) | 1.02 (0.96–1.08) | 620/2036 (31) | 0.82 (0.76–0.89)**** | 2476/5202 (48) | Referent |
| Severe NDI in survivors at 18- to 22-mo follow-up | 184/751 (25) | 0.71 (0.61–0.83)**** | 995/2849 (35) | 0.98 (0.89–1.08) | 342/1758 (20) | 0.76 (0.68–0.84)**** | 1399/4125 (34) | Referent |
| Indomethacin or ibuprofen treatment of PDA | 236/1184 (20) | 1.15 (1.13–1.20)**** | 1332/4655 (29) | 1.11 (1.10–1.13)**** | 813/3128 (26) | 1.08 (1.07–1.10)**** | 3403/6747 (50) | Referent |
| Surgery for PDA | 72/1185 (6) | 0.42 (0.32–0.55)**** | 566/4687 (12) | 0.68 (0.60–0.77)**** | 235/3127 (8) | 0.58 (0.51–0.67)**** | 1438/6746 (21) | Referent |
| Proven NEC with or without surgical treatment after day 14 after birth | 114/1186 (10) | 1.24 (0.98–1.55) | 461/4685 (10) | 1.11 (0.95–1.30) | 239/3128 (8) | 1.05 (0.90–1.23) | 567/6743 (8) | Referent |
Denominators vary to reflect missing values. I–E– is the baseline referent group for all comparisons and for calculation of adjusted RR, adjusted for all covariates including gestational age, birth weight, male gender, race, antenatal corticosteroid administration, surfactant administration, small for gestational age (birth weight <10th percentile for gender and gestational age as determined from growth curves by Alexander et al25), 5-minute Apgar score and center. *P < .05; **P < .001; ***P < .01; ****P ≤ .0001.
Concerning missing outcome data for infants, there were 13 infants (I+E+ = 1, I+E– = 4, I–E+ = 1, and I–E– = 7) with SIP in whom the specific date of documentation of SIP was missing. In addition, there were 61 infants (I+E+ = 3, I+E– = 11, I–E+ = 10, and I–E– = 37) for whom the cause of death between 12 h and 14 d after birth was missing.
Concerning the outcomes of NEC with intestinal perforation during first 14 d after birth and SIP after day 14, the adjusted analysis does not converge if center is included because the prevalence rates are low for these outcomes. Therefore, for these 2 outcomes, RR is adjusted for all other covariates except center.
Survivors were evaluated at 18 to 22 months’ corrected age and received a comprehensive neurodevelopmental examination that included a neurologic examination and the administration of the Bayley Scales of Infant and Toddler Development, Second Edition (Bayley II) for children born from 1999 to 2005 and the Bayley Scales of Infant and Toddler Development, Third Edition (Bayley III) for children born from 2006 to 2010. For infants born from 1999 to 2005, severe NDI at 18 to 22 months’ corrected age was defined as having any of the following: Bayley II Mental Developmental Index <70 (≥2 SD below the mean), Bayley II Psychomotor Developmental Index <70, moderate to severe cerebral palsy, deafness (presence of hearing aids in both ears), and/or blindness (no useful vision in either eye).21 For infants born from 2006 to 2010, severe NDI was defined as having any of the following: Bayley III cognitive composite score <70,22 Modified Gross Motor Function Classification level ≥2,23 deafness (hearing impairment), and/or blindness (no or some functional vision in either eye).
Statistical Analyses
The NRN enrollment includes ∼1500 ELBW infants per year in the GDB. Over the 12-year study period, it was estimated that there would be a total population of 18 000 infants. A previous NRN publication has shown that 29% of these patients receive prophylactic indomethacin.11 It was estimated that ∼14% of ELBW infants may have died before receiving any prophylactic indomethacin. This resulted in an expected study population of 16 500 infants who were eligible to receive prophylactic indomethacin and any enteral feeding within the first 3 days after birth. The α was predefined as .05. The incidence of SIP was 6% and 5% in both the indomethacin (n = 601) and placebo control groups (n = 601), respectively, in the Trial of Indomethacin Prophylaxis in Preterms.2 It was estimated that for the comparison of I–E+ versus I+E+ to detect an absolute increase in the incidence of SIP from 5% to 7.2% there would be a power of 80%. The study hypothesis was that the combined exposure to prophylactic indomethacin and early feeding (any feeds ≤3 days after birth) increases the risk for SIP within 14 days after birth in ELBW infants from 5% to ≥6% absolute risk (ie, by ≥20% relative risk [RR] increase).
Baseline demographic and perinatal characteristics of the 4 groups of newborns (I+E+, I+E–, I–E+, and I–E–) were analyzed by χ2 for categorical variables (surfactant, antepartum hemorrhage, Apgar scores, race, etc) and by Wilcoxon test for continuous variables (birth weight, gestational age). Both unadjusted and adjusted analyses were performed to ascertain the effect of the 4 groups (I+E+, I+E–, I–E+, and I–E–) on the primary outcome of SIP within 14 days and all the secondary outcomes. Unadjusted analysis was performed by using χ2 tests for categorical outcomes and Wilcoxon test for continuous outcomes. Adjusted analysis was performed using multivariate logistic regression analysis and Poisson regression models with robust variance estimators.24 The model was adjusted for covariates including gestational age, birth weight, male gender, race, antenatal corticosteroid administration, surfactant administration, small for gestational age (birth weight <10th percentile for gender and gestational age as determined from growth curves by Alexander et al25), and 5-minute Apgar score. The analyses were also adjusted for site.
Unadjusted and adjusted risk ratios comparing the risk of each of the exposure groups (I+E+, I+E–, I–E+) with nonexposure group (I–E–) for the primary outcome of SIP within 14 days and all the secondary outcomes were estimated. In addition, the adjusted risk ratio comparing early feeding and no early feeding groups among infants exposed to indomethacin (I+E+ vs I+E–) was estimated. SAS Version 9.2 (Cary, NC) was used for all statistical analyses. Denominators reported reflect missing values.
Results
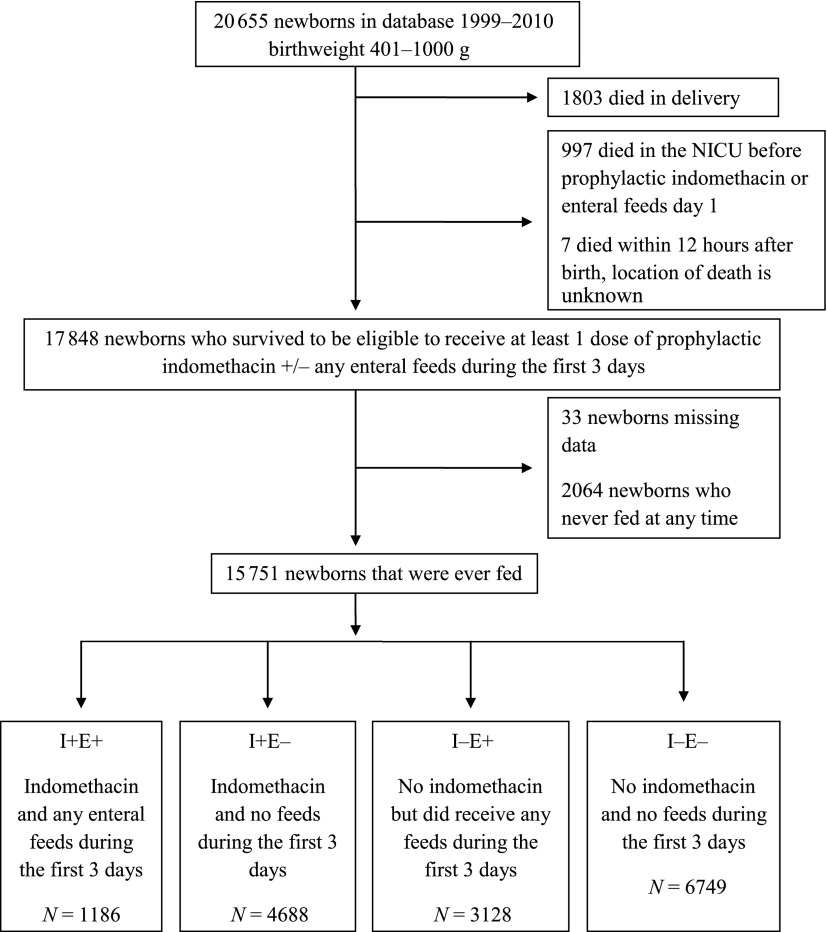
During the period of 1999–2010, 20 655 ELBW infants were enrolled in the NRN GDB registry (Fig 1). Among these infants, 15 751 ELBW infants survived >12 hours after birth and received enteral nutrition. Baseline demographic and clinical characteristics are shown in Table 1. Among infants exposed to prophylactic indomethacin, the risk of SIP did not differ between the I+E+ and I+E– groups (RR 0.74, 95% CI 0.49–1.11, P = .1467). The rate of SIP was lower in the I+E+ relative to the I–E– referent group (RR 0.58, 95% CI 0.37–0.90, P = .0159, Table 2). The unadjusted rate of SIP was increased in the I+E– group relative to the I–E– referent group (RR 1.31, 95% CI 1.08–1.57, P = .0051), but this was not significant in the adjusted analysis (RR 0.79, 95% CI 0.60–1.04, P = .0960). However, early enteral feeding in the absence of prophylactic indomethacin (I–E+) was associated with a significantly lower risk of SIP when compared with the I–E– referent group (RR 0.53, 95% CI 0.36–0.777, P = .0011).
FIGURE 1.
Selection of the study cohorts.
TABLE 1.
Baseline Characteristics of Study Cohorts
| Characteristic | I+E+ n = 1186 | I+E– n = 4688 | I–E+ n = 3128 | I–E– n = 6749 | P |
|---|---|---|---|---|---|
| Gestation, wk, median (p25, p75) | 26 (25, 27) | 25 (24, 26) | 27 (26, 29) | 26 (25, 27) | <.001 |
| Birth wt, g, median (p25, p75) | 820 (700, 910) | 750 (641, 865) | 870 (760, 945) | 766 (650, 876) | <.001 |
| Race | |||||
| White, n/total n (%) | 603/1182 (51) | 2645/4651 (57) | 1629/3099 (53) | 3507/6714 (52) | <.001 |
| Black, n/total n (%) | 547/1182 (46) | 1839/4651 (39) | 1327/3099 (43) | 2839/6714 (42) | <.001 |
| Male gender, n/total n (%) | 550/1186 (46) | 2312/4688 (49) | 1397/3128 (45) | 3301/6749 (49) | <.001 |
| Vaginal delivery, n/total n (%) | 429/1186 (36) | 1547/4682 (33) | 981/3127 (31) | 2194/6744 (32) | .025 |
| 5 min Apgar, median (p25, p75) | 7 (6, 8) | 7 (5, 8) | 8 (7, 8) | 7 (5, 8) | <.001 |
| Antenatal corticosteroid, n/total n (%) | 1031/1183 (87) | 3974/4670 (85) | 2700/3121 (86) | 5306/6711 (79) | <.001 |
| Singleton pregnancy, n/total n (%) | 926/1186 (78) | 3507/4688 (75) | 2498/3128 (80) | 5251/6749 (78) | <.001 |
| Small for gestational age, n/total n (%) | 184/1186 (15) | 586/4688 (12) | 853/3128 (27) | 1175/6748 (17) | <.001 |
| Surfactant, n/total n (%) | 925/1186 (78) | 4287/4683 (91) | 1854/3127 (59) | 5797/6733 (86) | <.001 |
| Congenital anomalies, n/total n (%) | 22/1186 (2) | 109/4688 (2) | 112/3128 (4) | 283/6749 (4) | <.001 |
Denominators vary to reflect missing values. p25, 25th percentile, p75, 75th percentile. I–E– is the baseline referent group for all comparisons.
Prophylactic indomethacin with early feeding was associated with lower death or severe NDI at 18- to 22-month follow-up (I+E+: RR 0.86, 95% CI 0.77–0.95, P = .0046) when compared with the group that did not receive indomethacin or early feeding. Early enteral feeding regardless of prophylactic indomethacin was associated with lower risk of death or severe NDI at 18- to 22-month follow-up (I+E+ and I–E+, P = .0046 and ≤0.0001, respectively) when compared with the group that did not receive prophylactic indomethacin or early feedings. Prophylactic indomethacin with early feeding was associated with less death or severe NDI at 18- to 22-month follow-up (I+E+: RR 0.82, 95% CI 0.76–0.89, P ≤ .0001) when compared with those infants who received prophylactic indomethacin but not early feeding. Early enteral feeding regardless of prophylactic indomethacin was associated with significantly fewer days to reach full enteral feed and fewer total numbers of days of parenteral nutrition (both P < .001, Table 3).
TABLE 3.
Nutritional Clinical Outcomes
| Outcome | I+E+ n = 1186 | I+E– n = 4688 | I–E+ n = 3128 | I–E– n = 6749 |
|---|---|---|---|---|
| Days to reach full enteral feeds (p25, p75), median | 19 (14, 29)* | 27 (19, 39) | 16 (11, 25)* | 26 (18, 38) |
| Days of parenteral nutrition (p25, p75), median | 19 (13, 33)* | 28.5 (18, 44)** | 17 (10, 29)* | 29 (18, 44) |
| Days to regain birth wt (p25, p75), median | 11 (7, 15)* | 11 (7, 16)* | 10 (7, 13)* | 11 (8, 16) |
II–E– is the baseline referent group for all comparisons and for significance of P values; p25, 25th percentile; p75, 75th percentile. *P < .001; **P < .01.
Discussion
This study provides observational data that the combined administration of prophylactic indomethacin during the first 24 hours after birth and any enteral nutrition during the first 3 days was not associated with increased SIP when compared with infants who did not receive prophylactic indomethacin and early feeding. Infants who received any enteral feeding during the first 3 days after birth in the absence of prophylactic indomethacin had a lower risk of SIP compared with infants in the no prophylactic indomethacin/no-early-feeding group. Among infants exposed to indomethacin, the adjusted risk of SIP did not differ significantly between those who received enteral nutrition during the first 3 days compared with those who did not receive early feeding. Early enteral feeding regardless of use of prophylactic indomethacin was associated with lower rates of death or severe NDI at 18- to 22-month follow-up (I+E+ and I–E+, both P < .001) when compared with those ELBW infants who never received either prophylactic indomethacin and any early enteral nutrition (I–E–).
SIP occurs predominantly in ELBW infants, with the diagnosis often based on clinical findings. Among SIP infants who undergo surgery, histopathologic features are distinct from NEC and are characterized by focal intestinal perforations, typically in the ileum, without evidence of mucosal ischemic injury or intestinal inflammation.26 Numerous risk factors have been associated with SIP including prematurity, low birth weight,27early indomethacin treatment with4,13,28,29 or without concurrent early postnatal corticosteroid administration,4,7,13 indomethacin treatment of a PDA later than 24 hours after birth,7 being outborn from a tertiary-level NICU, treatment with pressors, presence of a PDA,4 fetal inflammatory response, antenatal maternal antibiotic use,26 infectious agents, and intrauterine growth restriction.27 A meta-analysis showed that antenatal corticosteroids are not associated with SIP.6 A case-control study of 2105 infants identified the following risk factors for SIP: being outborn from a tertiary level NICU (mother less likely to have received antenatal corticosteroids), treatment with either dopamine or dobutamine within 14 days before SIP, the diagnosis of a PDA and treatment with hydrocortisone during the first 3 days after birth.4 Another case-control study showed that infants with SIP were more likely than control infants matched for birth weight and gestational age to have evidence of fetal inflammatory response defined as acute vasculitis of the fetal placental surface or umbilical perivasculitis (funisitis).26 Mothers of infants with SIP were more likely than controls to have received antibiotics before or at the time of delivery. There is, however, a lack of strong evidence to establish a definitive infectious mechanism for the etiology of SIP. There is a lack of strong evidence to support the theory that infants with intrauterine growth restriction have increased risk of SIP.27
Several studies have examined the association of indomethacin treatment in infants and either SIP1,2,4–7,11,12 or NEC with intestinal perforation1,2,7,10–12 with inconsistent results. The Trial of Indomethacin Prophylaxis in Preterms2 and a randomized trial by Ment et al4 reported no significant difference between the treatment and control groups for the outcomes of NEC or SIP. Prophylactic indomethacin was the intervention in both trials. A meta-analysis that included both of these trials showed no difference for the outcomes of NEC or SIP concerning treatment with prophylactic indomethacin compared with control groups.1 A trial of dexamethasone and/or hypercapnia within the first 12 hours after birth reported that indomethacin treatment in ELBW infants during the first 14 days after birth was associated with increased risk of SIP.29 Indomethacin use alone6,7or in combination with postnatal hydrocortisone4,28 or dexamethasone13,29 may be associated with SIP. Some studies have shown that early indomethacin administration within the first 12,6 24 hours,29 or 3 days4 after birth was associated with SIP. However, a retrospective of 11 960 ELBW infants in the NRN showed that indomethacin administration for PDA treatment after 24 hours after birth, but not prophylactic indomethacin, was associated with higher risk of SIP (adjusted OR 1.61, 95% CI 1.25–2.08, P < .05).7 The association of postnatal corticosteroid use as a risk factor for increased rate of SIP in ELBW infants treated with prophylactic indomethacin has been examined in 2 randomized controlled trials.28,29 ELBW infants who received concurrently prophylactic indomethacin and either hydrocortisone28 or dexamethasone29 had an increase in SIP in these trials.
A randomized controlled trial11 and a case–control study8 have examined the safety and efficacy of indomethacin and concurrent enteral feeding. A study by Clyman et al in 177 premature infants comparing trophic feeds at 15 mL/kg/day versus no feeds during indomethacin or ibuprofen PDA treatment reported that infants fed during treatment required 3 to 4 fewer days to reach 120 mL/kg/day of enteral feeds without evidence of increased feeding intolerance or increased SIP or necrotizing enterocolitis.11 Our study in contrast to that of Clyman et al examined prophylactic rather than therapeutic indomethacin in relation to early enteral nutrition. We did not examine the interaction of ibuprofen and early enteral feeding concerning SIP. An additional strength of our observational study is the large multicenter population with prospectively collected data concerning SIP.
A limitation of this study, common to all nonrandomized clinical studies, is that although statistical models can adjust for known confounders (birth weight, gestational age, etc), they do not adjust for variables not included in the model but evident to the clinician. These variables may have influenced the decision to initiate or withhold feeds. The finding that any enteral feeding during the first 3 days after birth in the absence of prophylactic indomethacin was associated with a lower risk of SIP as compared with infants who did not receive prophylactic indomethacin and early feeding may reflect a selection bias. This finding of less SIP and improved chance of survival without severe neurodevelopmental impairment in those ELBW infants who received early feeds may represent a bias. Infants who were not fed early were of lower birth weight and gestational age, more likely to be male, less likely to have had antenatal corticosteroids, more likely to have received surfactant, and more likely to have a PDA ligation. Early feeding among ELBW infants may be a marker for infants who are less ill during the first 3 days of life.30
Published studies reported that administration of prophylactic indomethacin to ELBW infants during the first 24 hours after birth reduced severe IVH and PDA1–3 and that early feedings were associated with decreased duration of parenteral nutrition and fewer days to achieve full enteral feeds and may have a protective effect regarding reduction of illness severity in ELBW infants.30 This study shows that concurrent administration of prophylactic indomethacin and early enteral feeding is associated with a lower risk of SIP in ELBW infants. This provides supporting observational data to refute the practice of withholding feeds while infants receive prophylactic indomethacin.
Acknowledgments
The National Institutes of Health and the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) provided grant support for the NRN’s GDB and Follow-up Studies.
Data collected at participating sites of the NICHD NRN were transmitted to RTI International, the data-coordinating center (DCC) for the network, which stored, managed, and analyzed the data for this study. On behalf of the NRN, Dr. Abhik Das (DCC Principal Investigator) and Dr. Shampa Saha (DCC Statistician) had full access to all the data in the study and take responsibility for the integrity of the data and accuracy of the data analysis.
We are indebted to our medical and nursing colleagues and the infants and their parents who agreed to take part in this study. The following investigators, in addition to those listed as authors, participated in this study: NRN Steering Committee Chair Michael S. Caplan, MD, University of Chicago, Pritzker School of Medicine; Alpert Medical School of Brown University and Women & Infants Hospital of Rhode Island (U10 HD27904): William Oh, MD, Betty R. Vohr, MD, Barbara Alksninis, PNP, Bonnie E. Stephens, MD, Yvette Yatchmink, MD, Robert Burke, MD, Angelita M. Hensman, RN, BSN, Teresa M. Leach, MEd CAES, Martha R. Leonard, BA BS, Lucy Noel, Rachel A. Vogt, MD, Victoria E. Watson, MS, CAS, Suzy Ventura; Case Western Reserve University, Rainbow Babies & Children’s Hospital (U10 HD21364, M01 RR80): Avroy A. Fanaroff, MD, Deanne E. Wilson-Costello, MD, Bonnie S. Siner, RN, Harriet G. Friedman, MA; Cincinnati Children’s Hospital Medical Center, University Hospital, and Good Samaritan Hospital (U10 HD27853, M01 RR8084): Kurt Schibler, MD, Edward F. Donovan, MD, Jean J. Steichen, MD, Kimberly Yolton, PhD, Barbara Alexander, RN, Kate Bridges, MD, Cathy Grisby, BSN, CCRC, Marcia Worley Mersmann, RN, Holly L. Mincey, RN, BSN, Jody Hessling, RN, Teresa L. Gratton, PA; Duke University School of Medicine, University Hospital, Alamance Regional Medical Center, and Durham Regional Hospital (U10 HD40492, M01 RR30): Ronald N. Goldberg, MD, C. Michael Cotten, MD, MHS, Kathy J. Auten, MSHS, Kimberley A. Fisher, PhD, FNP-BC, IBCLC, Katherine A. Foy, RN, Kathryn E. Gustafson, PhD, Melody B. Lohmeyer, RN, MSN; Emory University, Children’s Healthcare of Atlanta, Grady Memorial Hospital, and Emory University Hospital Midtown (U10 HD27851, M01 RR39): David P. Carlton, MD, Ira Adams-Chapman, MD, Ellen Hale, RN, Sheena Carter, PhD, Maureen Mulligan LaRossa, RN; NICHD: Linda L. Wright, MD, Elizabeth M. McClure, Med, Stephanie Wilson Archer, MA; Indiana University, University Hospital, Methodist Hospital, Riley Hospital for Children, and Wishard Health Services (U10 HD27856, M01 RR750): Brenda B. Poindexter, MD MS, James A. Lemons, MD, Anna M. Dusick, MD, Carolyn Lytle, MD, MPH, Lon G. Bohnke, MS, Greg Eaken, PhD, Dianne E. Herron, RN, Lucy C. Miller, RN, BSN, CCRC, Heike M. Minnich, PsyD, HSPP, Leslie Richard, RN, Leslie Dawn Wilson, BSN, CCRC, Faithe Hamer, BS; RTI International (U10 HD36790): W. Kenneth Poole, PhD, Dennis Wallace, PhD, Jamie E. Newman, PhD, MPH, Jeanette O’Donnell Auman, BS, Margaret Cunningham, BS, Betty K. Hastings, Elizabeth M. McClure, Med, Carolyn M. Petrie Huitema, MS, Kristin M. Zaterka-Baxter, RN, BSN; Stanford University, California Pacific Medical Center, Dominican Hospital, El Camino Hospital, and Lucile Packard Children's Hospital (U10 HD27880, M01 RR70): David K. Stevenson, MD, Susan R. Hintz, MD, MS Epi, Marian M. Adams, MD, Charles E. Ahlfors, MD, M. Bethany Ball, BS, CCRC, Joan M. Baran, PhD, Barbara Bentley, PhD, Lori E. Bond, PhD, Ginger K. Brudos, PhD, Alexis S. Davis, MD, MS, Maria Elena DeAnda, PhD, Anne M. DeBattista, RN, PNP, Jan T. Epcar, MA, Barry E. Fleisher, MD, Magdy Ismael, MD, MPH, Jean G. Kohn, MD, MPH, Carol G. Kuelper, PhD, Julie C. Lee-Ancajas, PhD, Melinda S. Proud, RCP, Renee P. Pyle, PhD, Dharshi Sivakumar, MD, MRCP, Robert D. Stebbins, MD, Nicholas H. St. John, PhD; Tufts Medical Center, Floating Hospital for Children (U10 HD53119, M01 RR54): Ivan D. Frantz III, MD, Elisabeth C. McGowan, MD, Brenda L. MacKinnon, RNC, Ellen Nylen, RN, BSN, Anne Furey, MPH, Cecelia Sibley, PT, MHA, Ana Brussa, MS, OTR/L; University of Alabama at Birmingham Health System and Children’s Hospital of Alabama (U10 HD34216, M01 RR32): Namasivayam Ambalavanan, MD, Myriam Peralta-Carcelen, MD, MPH, Kathleen G. Nelson, MD, Kirstin J. Bailey, PhD, Fred J. Biasini, PhD, Stephanie A. Chopko, PhD, Monica V. Collins, RN, BSN MaEd, Shirley S. Cosby, RN, BSN, Mary Beth Moses, PT, MS, PCS, Vivien A. Phillips, RN, BSN, Julie Preskitt, MSOT, MPH, Richard V. Rector, PhD, Sally Whitley, MA, OTR-L, FAOTA; University of California, San Diego Medical Center and Sharp Mary Birch Hospital for Women and Newborns (U10 HD40461): Neil N. Finer, MD, Yvonne E. Vaucher, MD MPH, Maynard R. Rasmussen MD, Paul R. Wozniak, MD, Kathy Arnell, RNC, Renee Bridge, RN, Clarence Demetrio, RN, Martha G. Fuller, RN, MSN, Donna Posin, OTR/L, MPA, Wade Rich, BSHS, RRT; University of Iowa Children’s Hospital and Mercy Medical Center (U10 HD53109, M01 RR59): John A. Widness, MD, Tarah T. Colaizy, MD, Dan L. Ellsbury, MD, Karen J. Johnson, RN, BSN, Diane L. Eastman, RN, CPNP, MA, Donia D. Campbell, RN; University of Miami, Holtz Children’s Hospital (U10 HD21397, M01 RR16587): Charles R. Bauer, MD, Shahnaz Duara, MD, Ruth Everett-Thomas, RN, MSN, Amy Mur Worth, RN, MS, Mary Allison, RN, Alexis N. Diaz, BA, Elaine O. Mathews, RN, Kasey Hamlin-Smith, PhD, Lisa Jean-Gilles, BA, Maria Calejo, MS, Silvia M. Frade Eguaras, BA, Silvia Hiriart-Fajardo, MD, Yamiley C. Gideon, BA, Michelle Berkovits, PhD, Alexandra Stoerger, BA, Andrea Garcia, MA, Helena Pierre, BA; University of New Mexico Health Sciences Center (U10 HD27881, U10 HD53089, M01 RR997): Kristi L. Watterberg, MD, Lu-Ann Papile, MD, Robin K. Ohls, MD, Conra Backstrom Lacy, RN, Jean R. Lowe, PhD, Rebecca Montman, BSN; University of Rochester Medical Center, Golisano Children’s Hospital (U10 HD40521, M01 RR44, NCRR UL1 024160): Dale L. Phelps, MD, Ronnie Guillet, MD, PhD, Gary J. Myers, MD, Linda J. Reubens, RN, CCRC, Erica Burnell, RN, Mary Rowan, RN, Cassandra A. Horihan, MS, Julie Babish Johnson, MSW, Diane Hust, MS, RN, CS, Rosemary L. Jensen, Emily Kushner, MA, Joan Merzbach, LMSW, Lauren Zwetsch, RN, MS, PNP, Kelly Yost, PhD; University of Tennessee Health Science Center (U10 HD21415): Sheldon B. Korones, MD, Henrietta S. Bada, MD, Tina Hudson, RN BSN, Marilyn Williams, LCSW, Kimberly Yolton, PhD; University of Texas Southwestern Medical Center at Dallas, Parkland Health & Hospital System and Children’s Medical Center Dallas (U10 HD40689, M01 RR633): Charles R. Rosenfeld, MD, Walid A. Salhab, MD, R. Sue Broyles, MD, Roy J. Heyne, MD, Sally S. Adams, PNP, Cathy Twell Boatman, MS CIMI, P. Jeannette Burchfield, RN, BSN, Cristin Dooley, PhD, LSSP, Alicia Guzman, Elizabeth Heyne, PsyD, PA-C, Jackie F. Hickman, RN, Melissa H. Leps, RN, Linda A. Madden, BSN, RN, CPNP, Nancy A. Miller, RN, Janet S. Morgan, RN, Susie Madison, RN, Gaynelle Hensley, RN, Lizette E. Torres, RN; University of Texas Health Science Center at Houston Medical School, Children’s Memorial Hermann Hospital, and Lyndon Baines Johnson General Hospital/Harris County Hospital District (U10 HD21373): Jon E. Tyson, MD, MPH, Kathleen A. Kennedy, MD, MPH, Esther G. Akpa, RN, BSN, Patty A. Cluff, RN, Beverly Foley Harris, RN, BSN, Claudia I. Franco, RNC, MSN, Anna E. Lis, RN, BSN, Sarah Martin, RN, BSN, Georgia E. McDavid, RN, Patti L. Pierce Tate, RCP, Maegan C. Simmons, RN, Patricia W. Evans, MD, Nora I. Alaniz, BS, Pamela J. Bradt, MD, MPH, Magda Cedillo, Susan Dieterich, PhD, Charles Green, PhD, Margarita Jiminez, MD, MPH, Terri Major-Kincade, MD, MPH, Brenda H. Morris, MD, M. Layne Poundstone, RN, BSN, Stacey Reddoch, BA, Saba Siddiki, MD, Laura L. Whitely, MD, Sharon L. Wright, MT; University of Utah Medical Center, Intermountain Medical Center, LDS Hospital, and Primary Children's Medical Center (U10 HD53124, M01 RR64): Roger G. Faix, MD, Bradley A. Yoder, MD, Anna Bodnar, MD, Mike Steffens, PhD, Shawna Baker, RN, Jill Burnett, RN, Jennifer J. Jensen, RN, BSN, Karen A. Osborne, RN, BSN, CCRC, Kimberlee Weaver-Lewis, RN, BSN; Wake Forest University Baptist Medical Center, Brenner Children’s Hospital, and Forsyth Medical Center (U10 HD40498, M01 RR7122): T. Michael O’Shea, MD, MPH, Robert G. Dillard, MD, Nancy J. Peters, RN, CCRP, Korinne Chiu, MA, Deborah Evans Allred, MA, LPA, Donald J. Goldstein, PhD, Raquel Halfond, MA, Barbara G. Jackson, RN, BSN, Carroll Peterson, MA, Ellen L. Waldrep, MS, Melissa Whalen Morris, MA, Gail Wiley Hounshell, PhD; Wayne State University, Hutzel Women’s Hospital, and Children’s Hospital of Michigan (U10 HD21385): Yvette R. Johnson, MD, MPH, Athina Pappas, MD, Rebecca Bara, RN, BSN, Debra Driscoll, RN, BSN, Laura Goldston, MA, Deborah Kennedy, RN, BSN, Geraldine Muran, RN, BSN, Elizabeth Billian, RN, MS, Laura Sumner, RN, BSN, Kara Sawaya, RN, BSN, Kathleen Weingarden, RN, BSN; Yale University, Yale-New Haven Children’s Hospital, and Bridgeport Hospital (U10 HD27871, UL1 RR24139, M01 RR125, M01 RR6022): Richard A. Ehrenkranz, MD, Christine Butler, MD, Harris Jacobs, MD, Patricia Cervone, RN, Nancy Close, PhD, Patricia Gettner, RN, Walter Gilliam, PhD, Sheila Greisman, RN, Monica Konstantino, RN, BSN, JoAnn Poulsen, RN, Elaine Romano, MSN, Janet Taft, RN, BSN, Joanne Williams, RN, BSN.
Glossary
- CI
confidence interval
- ELBW
extremely low birth weight
- GDB
Generic Database
- I+E+
infants who received prophylactic indomethacin during the first 24 hours and any enteral feeding during the first 3 days after birth
- I+E–
infants who received prophylactic indomethacin during the first 24 hours and did not receive enteral feeding during the first 3 days after birth
- I–E+
infants who did not receive prophylactic indomethacin during the first 24 hours but did receive enteral feeding during the first 3 days after birth
- I–E–
infants who did not receive prophylactic indomethacin during the first 24 hours and did not receive enteral feeding during the first 3 days after birth
- NDI
neurodevelopmental impairment
- NEC
necrotizing enterocolitis
- NRN
Neonatal Research Network
- OR
odds ratio
- PDA
patent ductus arteriosus
- RR
relative risk
- SIP
spontaneous intestinal perforation
Footnotes
Drs Kelleher, Salas, and Carlo conceptualized and designed the study, oversaw data analyses, and drafted and revised the manuscript; Drs Bhat, Ambalavanan, Stoll, Bell, Walsh, Laptook, Sanchez, Shankaran, Van Meurs, Ms Hale, Ms Newman, Ms Ball, and Drs Higgins and Carcelen assisted in study design and reviewed and revised the manuscript; Drs Saha and Das assisted in study design, performed the statistical analyses, and reviewed and revised the manuscript; and all authors approved the final manuscript as submitted.
FINANCIAL DISCLOSURE: The authors have indicated they have no financial relationships relevant to this article to disclose.
FUNDING: The National Institutes of Health and the Eunice Kennedy Shriver National Institute of Child Health and Human Development provided grant support for the Neonatal Research Network’s Generic Database and Follow-up Studies.
POTENTIAL CONFLICT OF INTEREST: The authors have indicated they have no potential conflicts of interest to disclose.
References
- 1.Fowlie PW, Davis PG, McGuire W. Prophylactic intravenous indomethacin for preventing mortality and morbidity in preterm infants. Cochrane Database Syst Rev. 2010;7(7):CD000174. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Schmidt B, Davis P, Moddemann D, et al. Trial of Indomethacin Prophylaxis in Preterms Investigators . Long-term effects of indomethacin prophylaxis in extremely-low-birth-weight infants. N Engl J Med. 2001;344(26):1966–1972 [DOI] [PubMed] [Google Scholar]
- 3.Ment LR, Oh W, Ehrenkranz RA, et al. Low-dose indomethacin therapy and extension of intraventricular hemorrhage: a multicenter randomized trial. J Pediatr. 1994;124(6):951–955 [DOI] [PubMed] [Google Scholar]
- 4.Attridge JT, Clark R, Walker MW, Gordon PV. New insights into spontaneous intestinal perforation using a national data set: (1) SIP is associated with early indomethacin exposure. J Perinatol. 2006;26(2):93–99 [DOI] [PubMed] [Google Scholar]
- 5.Shorter NA, Liu JY, Mooney DP, Harmon BJ. Indomethacin-associated bowel perforations: a study of possible risk factors. J Pediatr Surg. 1999;34(3):442–444 [DOI] [PubMed] [Google Scholar]
- 6.Sharma R, Hudak ML, Tepas JJ, III, et al. Prenatal or postnatal indomethacin exposure and neonatal gut injury associated with isolated intestinal perforation and necrotizing enterocolitis. J Perinatol. 2010;30(12):786–793 [DOI] [PubMed] [Google Scholar]
- 7.Wadhawan R, Oh W, Vohr BR, et al. Spontaneous intestinal perforation in extremely low birth weight infants: association with indometacin therapy and effects on neurodevelopmental outcomes at 18–22 months corrected age. Arch Dis Child Fetal Neonatal Ed. 2013;98(2):F127–F132 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Bellander M, Ley D, Polberger S, Hellström-Westas L. Tolerance to early human milk feeding is not compromised by indomethacin in preterm infants with persistent ductus arteriosus. Acta Paediatr. 2003;92(9):1074–1078 [DOI] [PubMed] [Google Scholar]
- 9.Novack CM, Waffarn F, Sills JH, Pousti TJ, Warden MJ, Cunningham MD. Focal intestinal perforation in the extremely-low-birth-weight infant. J Perinatol. 1994;14(6):450–453 [PubMed] [Google Scholar]
- 10.Fujii AM, Brown E, Mirochnick M, O’Brien S, Kaufman G. Neonatal necrotizing enterocolitis with intestinal perforation in extremely premature infants receiving early indomethacin treatment for patent ductus arteriosus. J Perinatol. 2002;22(7):535–540 [DOI] [PubMed] [Google Scholar]
- 11.Clyman R, Wickremasinghe A, Jhaveri N, et al. Enteral feeding during indomethacin and ibuprofen treatment of a patent ductus arteriosus. J Pediatr. 2013;163(2):406–411 [DOI] [PMC free article] [PubMed]
- 12.Madan JC, Kendrick D, Hagadorn JI, Frantz ID, III, National Institute of Child Health and Human Development Neonatal Research Network . Patent ductus arteriosus therapy: impact on neonatal and 18-month outcome. Pediatrics. 2009;123(2):674–681 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Paquette L, Friedlich P, Ramanathan R, Seri I. Concurrent use of indomethacin and dexamethasone increases the risk of spontaneous intestinal perforation in very low birth weight neonates. J Perinatol. 2006;26(8):486–492 [DOI] [PubMed] [Google Scholar]
- 14.Uauy RD, Fanaroff AA, Korones SB, Phillips EA, Phillips JB, Wright LL, National Institute of Child Health and Human Development Neonatal Research Network . Necrotizing enterocolitis in very low birth weight infants: biodemographic and clinical correlates. J Pediatr. 1991;119(4):630–638 [DOI] [PubMed] [Google Scholar]
- 15.Hwang H, Murphy JJ, Gow KW, Magee JF, Bekhit E, Jamieson D. Are localized intestinal perforations distinct from necrotizing enterocolitis? J Pediatr Surg. 2003;38(5):763–767 [DOI] [PubMed] [Google Scholar]
- 16.Okuyama H, Kubota A, Oue T, Kuroda S, Ikegami R, Kamiyama M. A comparison of the clinical presentation and outcome of focal intestinal perforation and necrotizing enterocolitis in very-low-birth-weight neonates. Pediatr Surg Int. 2002;18(8):704–706 [DOI] [PubMed] [Google Scholar]
- 17.Pumberger W, Mayr M, Kohlhauser C, Weninger M. Spontaneous localized intestinal perforation in very-low-birth-weight infants: a distinct clinical entity different from necrotizing enterocolitis. J Am Coll Surg. 2002;195(6):796–803 [DOI] [PubMed] [Google Scholar]
- 18.Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network. Generic Database of Very Low Birth Weight Infants (GDB). NCT00063063. Available at: http://www.clinicaltrials.gov/ct2/show/NCT00063063. Accessed July 21, 2014
- 19.Stoll BJ, Hansen NI, Bell EF, et al. Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network . Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics. 2010;126(3):443–456 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Walsh MC, Kliegman RM. Necrotizing enterocolitis: treatment based on staging criteria. Pediatr Clin North Am. 1986;33(1):179–201 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Vohr BR, Wright LL, Poole WK, McDonald SA. Neurodevelopmental outcomes of extremely low birth weight infants <32 weeks’ gestation between 1993 and 1998. Pediatrics. 2005;116(3):635–643 [DOI] [PubMed] [Google Scholar]
- 22.Vohr BR, Stephens BE, Higgins RD, et al. ; Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network. Are outcomes of extremely preterm infants improving? Impact of Bayley assessments on outcomes. J Pediatr. 2012;161(2):222–228 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Palisano RJ, Cameron D, Rosenbaum PL, Walter SD, Russell D. Stability of the gross motor function classification system. Dev Med Child Neurol. 2006;48(6):424–428 [DOI] [PubMed] [Google Scholar]
- 24.Zou G. A modified poisson regression approach to prospective studies with binary data. Am J Epidemiol. 2004;159(7):702–706 [DOI] [PubMed] [Google Scholar]
- 25.Alexander GR, Himes JH, Kaufman RB, Mor J, Kogan M. A United States national reference for fetal growth. Obstet Gynecol. 1996;87(2):163–168 [DOI] [PubMed] [Google Scholar]
- 26.Ragouilliaux CJ, Keeney SE, Hawkins HK, Rowen JL. Maternal factors in extremely low birth weight infants who develop spontaneous intestinal perforation. Pediatrics. 2007;120(6):e1458–e1464 [DOI] [PubMed] [Google Scholar]
- 27.Gordon PV. Understanding intestinal vulnerability to perforation in the extremely low birth weight infant. Pediatr Res. 2009;65(2):138–144 [DOI] [PubMed] [Google Scholar]
- 28.Watterberg KL, Gerdes JS, Cole CH, et al. Prophylaxis of early adrenal insufficiency to prevent bronchopulmonary dysplasia: a multicenter trial. Pediatrics. 2004;114(6):1649–1657 [DOI] [PubMed] [Google Scholar]
- 29.Stark AR, Carlo WA, Tyson JE, et al. National Institute of Child Health and Human Development Neonatal Research Network . Adverse effects of early dexamethasone in extremely-low-birth-weight infants. N Engl J Med. 2001;344(2):95–101 [DOI] [PubMed] [Google Scholar]
- 30.Ehrenkranz RA, Das A, Wrage LA, et al. Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network . Early nutrition mediates the influence of severity of illness on extremely LBW infants. Pediatr Res. 2011;69(6):522–529 [DOI] [PMC free article] [PubMed] [Google Scholar]