Abstract
Two patients with protein S deficiency with acquired multiple pial and dural arteriovenous fistulae (AVFs) following superior sagittal sinus (SSS) thrombosis are reported. Case 1 is a 38-year-old male with protein S deficiency who developed generalized seizure due to SSS thrombosis. Local fibrinolysis was achieved in the acute stage. His 10-month follow-up angiogram revealed an asymptomatic acquired dural AVF arising from the middle meningeal artery and the anterior cerebral artery with drainage to the thrombosed cortical vein in the right frontal lobe. Furthermore, his 2-year follow-up angiogram revealed a de novo pial AVF from the middle cerebral artery in the Sylvian fissure with drainage to the cortical vein initially thrombosed. However, this asymptomatic pial AVF caused bleeding in the ipsilateral cerebral hemisphere 12 years after onset, whereas the dural AVF spontaneously disappeared. Surgical disconnection was successfully performed to eliminate the source of hemorrhage. Case 2 is a 50-year-old male with a past history of SSS thrombosis with protein S deficiency who developed pulsatile tinnitus and generalized seizure. His angiogram showed a cortical dural AVF in the left parietal lobe and a sporadic dural AVF involving the right sigmoid sinus. The parietal lesion was eliminated by transarterial embolization followed by craniotomy. However, a de novo pial AVF emerged from the middle cerebral artery adjacent to the previously treated lesion. Of four cortical AVFs in two patients, thrombosis of cortical veins caused by protein S deficiency might play an important role in their formation. Long-term follow-up is required because this peculiar disorder has an unusual clinical course.
Keywords: acquired arteriovenous fistula, angiogenesis, protein S deficiency, superior sagittal sinus, thrombosis
Introduction
Dural arteriovenous fistulae (AVFs) have been recognized as an acquired rare disorder of abnormal communication between dural arteries and veins. The causes of this disease are thought to include sinus thrombosis, venous hypertension, and head trauma, although the etiology of this disorder remains unknown. In contrast, pial AVFs are regarded as a congenital disease frequently observed in pediatric patients. Multiple pial AVFs might be associated with hereditary hemorrhagic telangiectasia.1) Protein S is a vitamin K-dependant plasma protein functioning as a cofactor for the anticoagulant activity of activated protein C. Although there are some reports of protein S deficiency causing sinus thrombosis, cases with dural AVF are extremely rare. Moreover, to our knowledge, no previous report has described acquired pial AVFs following SSS thrombosis. In this article, two cases with protein S deficiency and SSS thrombosis of multiple AVFs involving thrombosed cortical veins are reported. The etiology of this disease and the timing of surgical intervention is discussed.
Case 1
A 38-year-old man suffered an episode of deep venous thrombosis of the leg, developed headache and generalized seizure, and was immediately brought to our hospital by ambulance in April 1998. On admission, he was lethargic, complaining of headache and nausea. Results from his blood test revealed total protein S antigen at 23% (65–130%), free protein S antigen at 16% (60–150%) and protein S activity was under 10% (60–150%). His father was also found to have a reduced level of protein S in later blood analysis, whereas his mother and brother were normal. His magnetic resonance (MR) imaging revealed an abnormal area of hyperintensity in the right frontal lobe (Fig. 1A).
Fig. 1.
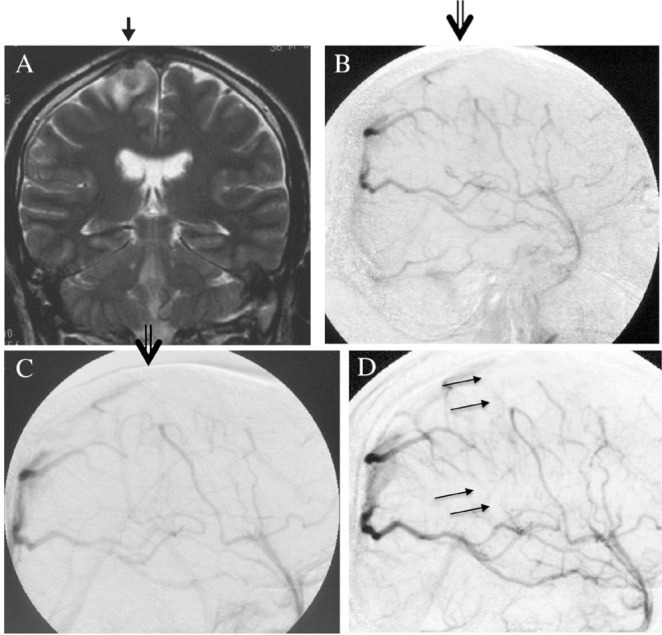
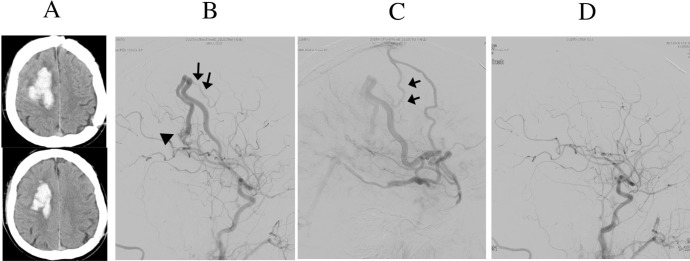
Case 1 A: The patient's initial magnetic resonance imaging T2-weighted image demonstrated a small hyperintensity abnormal lesion in the right frontal lobe (closed arrow). B: Lateral view of right carotid injection (venous phase) showing sinus occlusion in the middle of the superior sagittal sinus (open arrow). C, D: The same injection at 2 weeks after local fibrinolysis using urokinase demonstrating remaining occlusion of the superior sagittal sinus. However, no dural arteriovenous fistula was present at this point. Note that a cortical venous occlusion is indicated by the closed arrows (D).
After confirmation of an superior sagittal sinus (SSS) thrombosis in the patient's emergent angiogram (Fig. 1B), a microcatheter was advanced to the SSS via his femoral vein for local intravenous fibrinolysis. A total of 180,000 units of urokinase was administered, resulting in a sudden disappearance of his consciousness disturbance and headache. An additional 20,000 units of urokinase was administered through the microcatheter positioned in the SSS, and systemic heparinization was continued for 8 hours. As the patient had hit his head at the time of convulsion, an acute subdural hematoma occurred on the left side, possibly due to the administration of urokinase. He underwent open surgery to remove the hematoma, and was fully recovered. The 2-week follow-up angiogram showed residual SSS occlusion but no AVF at this point (Fig. 1C, D). Warfarinization was begun, and the patient's blood was regularly tested at our clinic. However, the patient's 10-month follow-up angiogram revealed an asymptomatic dural AVF in the right side, arising from the middle meningeal artery, superficial temporal artery, and anterior cerebral artery, with drainage to the Rolandic vein and two other branches that were observed on the initial angiogram as being thrombosed (Fig. 2). Neither surgery nor embolization for this lesion was performed. Furthermore, 2 years after the SSS thrombosis, angio-gram revealed a pial AVF in the right Sylvian fissure, supplied by the posterior parietal artery with drainage to the cortical vein leading to the Rolandic vein (Fig. 3). In this lesion, there was no involvement of a feeding artery from the external carotid artery. This draining vein was not detected on the initial angiogram, which is consistent with cortical venous thrombosis subsequent to SSS thrombosis (Table 1). The shunt flow of the first fistula was apparently reduced because the blood supply from the external carotid artery was discontinued. As the patient refused our proposal for surgical treatment, these two fistulae are being followed-up at our clinic without any interventional or surgical treatment. A 10-year follow-up magnetic resonance angiogram (MRA)/magnetic resonance venogram (MRV) performed in December 2008 showed that the remaining pial AVF and SSS thrombosis were similar in appearance to the previous examination. Twelve years after onset, the patient suddenly had headache and motor weakness in his left arm and leg. He was brought to the hospital by ambulance, and his CT scan demonstrated intracerebral hemorrhage in the right frontal lobe (Fig. 4A). An angiogram confirmed the development of a pial AVF and disappearance of the initial dural AVF (Fig. 4B, C). Warfarin was discontinued, and surgery was performed to eliminate the pial AVF 1 month after the bleeding. A postoperative angiogram disclosed that the patient's pial AVF had been completely cured. He resumed warfarinization and was transferred to the rehabilitation center. Figure 5 summarizes the chronological course of the angiographical findings.
Fig. 2.
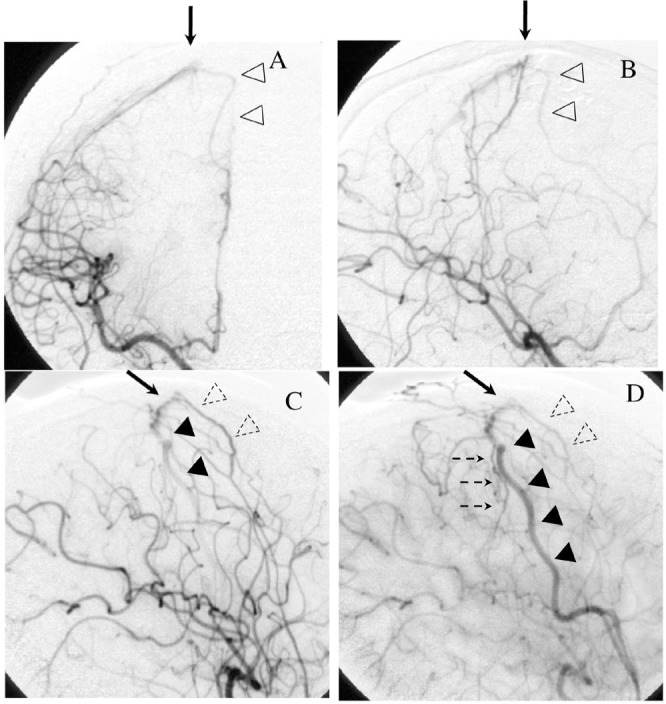
Case 1 Ten-month follow-up right carotid injection, anterior view (A), right oblique view (B), and lateral view (C, D) showing dural arteriovenous fistula (arrows) supplied by the middle meningeal artery (white dotted arrowhead), superior temporal artery and anterior cerebral artery (white arrowhead) with drainage to the Rolandic vein connecting to the superficial Sylvian vein (black arrowhead). Dotted arrows show faint contrast of thrombosed cortical veins (D). Note that the posterior parietal artery never participated in the shunt at this point.
Fig. 3.
Case 1 Two-year follow-up angiogram after the superior sagittal sinus thrombosis (A–G): right internal carotid injection showing that, in addition to the fistula of the parietal cortex, another fistula emerged from the ipsilateral Sylvian fissure, arising from the M3–4 portion of the posterior parietal artery with drainage to the previously thrombosed cortical vein shown in Figs. 1D and 2D. Irregularity of the vessel was consistent with the residual thrombosis in the lumen of this vein (dotted arrows). This draining vein finally connected with the Rolandic vein (black arrowhead). The initial shunt from the anterior cerebral artery was barely recognized (A–C). However, the shunt of the initial arteriovenous (AV) fistula was considerably reduced, as the external carotid artery no longer contributed to this fistula (D). E–G: Anterior oblique view series of right internal carotid injection confirmed this new pial AV fistula arising from the middle cerebral artery. The fistulous point was indicated (long arrows) with drainage to the previously thrombosed cortical vein (dotted arrows) connecting to the Sylvian vein (black arrowheads).
Table 1.
Reported cases of dual or pial AVF following SSS thrombosis
| Author | Age/Sex | Location | Treatment | Result | Protein S deficiency |
|---|---|---|---|---|---|
| Sugiura (1996)) 2) | 43/M | SSS | None | Not cure | |
| Galen | None | Not cure | |||
| TS | None | Not cure | |||
| Ozawa (1998) 3) | 39/M | Parietal | Embolization + craniotomy | Cure | Unverified |
| Nishio (2002) 4) | 57/M | Fronto-parietal | Embolization | Cure | Unverified |
| Toledo (2010) 5) | 60/M | Parietal | Craniotomy | Cure | Unverified |
| Our Case 1 (2012) | 38/M | Parietal | None | Cure | + |
| Parietal | Craniotomy | Cure | |||
| Our Case 2 (2012) | 50/M | Parietal | Embolization + Craniotomy | Cure | + |
| Parietal | None | Not cure | |||
| Sigmoid sinus | None | Not cure |
AVF: arteriovenous fistula, SSS: superior sagittal sinus, TS: trans-verse-sigmoid sinus.
Fig. 4.
Case 1 Twelve years later, the patient was transferred to the local hospital when he had severe headache and motor dysfunction in his left arm and leg. His computed tomography scan demonstrated intracerebral hemorrhage in the right frontal lobe (A). The lateral view of the right carotid injection confirmed the lesion (B: black arrowhead), in which the de novo draining vein arising from the corner of the main draining vein was found (B, C: black arrows). The patient underwent surgery to eliminate the fistula at the acute stage. Postoperative angiogram confirmed no presence of the fistula (D).
Fig. 5.
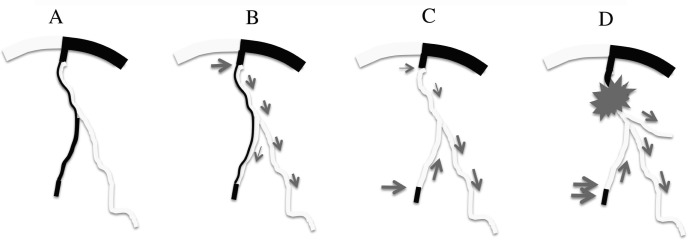
Angiographical scheme of Case 1. A: Anterior half of superior sagittal sinus and part of the cortical vein are thrombosed at the time of onset. B: Ten months after onset, a de novo dural AVF arose from the dural and pial arteries with drainage to the cortical vein. C: Two years after onset, another pial AVF occurred, while the initial dural AVF became a low-flow shunt. D: When the patient ultimately bled in the frontal lobe 12 years after the onset, the shunt flow of the pial AVF increased with the de novo draining vein arising from the main draining vein, while the dural AVF disappeared. AVF: arteriovenous fistula.
Case 2
A 50-year-old man with a 1-year history of deep venous thrombosis of the leg developed tetraparesis caused by SSS thrombosis in July 1975, and he was treated with an anticoagulant for a few years. Four years after stopping anticoagulant treatment, he began to have pulsatile tinnitus on the right side. Eleven years later, he experienced a generalized seizure and was referred to our institution from a nearby hospital for further examination and treatment. On admission, no neurological deficits were present, except for pulsatile tinnitus on the right side. Hematological examination indicated a reduced level of free protein S antigen (total 112%, free 38%).
Angiography on admission demonstrated two dural AVFs (Fig. 6). One was on the surface of the left parietal lobe originating from the bilateral middle meningeal arteries, left occipital artery, and left superficial temporal artery, with drainage to the Rolandic vein exhibiting venous congestion in the ipsilateral cerebrum. The other lesion was a sporadic sigmoid sinus dural AVF in the right frontal lobe, mainly arising from the occipital artery with drainage to the internal jugular vein. Moreover, SSS occlusion and right sigmoid sinus occlusion were also noted. It was thought that the former caused the seizure and the latter caused the pulsatile tinnitus on the right. For the former, a burr hole and transarterial embolization by direct puncture of the middle meningeal artery using IBCA (isobutyl-cyano-acrylate) was conducted. Nevertheless, the shunt remained in place, causing three postoperative attacks of aphasia. Therefore, craniotomy and AVF closure were attempted 12 years after the SSS thrombosis. The patient's postoperative course was uneventful. A 1-month follow-up angiogram showed that the previous fistula in the parietal cortex had been completely obliterated (Fig. 7A, B). However, a de novo pial AVF, which was not identified before the surgery, was found (Fig. 7C–F). This shunt arose from the middle cerebral artery directly draining to the thrombosed cortical vein near the SSS. No treatment was given as this new fistula was an asymptomatic lesion. Unfortunately, the patient died of lung cancer after 2 years. Autopsy was not performed. Figure 8 summarizes the chronological course of the patient's angiographical findings.
Fig. 6.
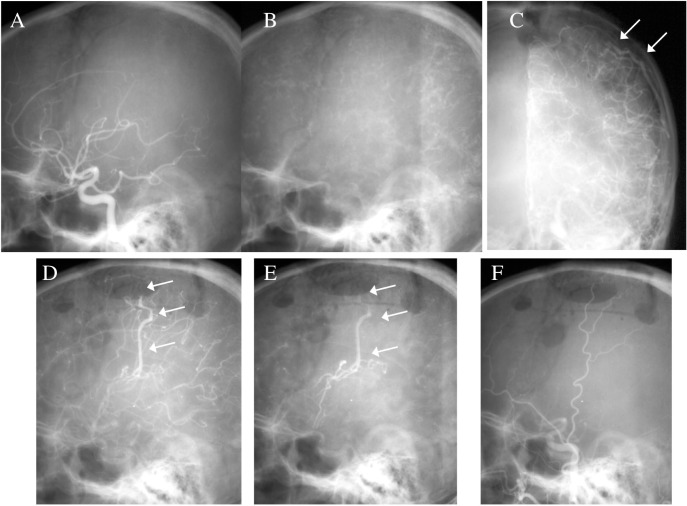
Case 2: Preoperative left external carotid injection, anterior view (A, B) and lateral view (C, D) demonstrating dural arteriovenous (AV) fistula arising from the middle meningeal artery (white arrowhead) and superficial temporal artery with drainage to the possibly thrombosed Rolandic vein (black arrowhead) connecting with the superficial Sylvian vein. In addition, the second dural AV fistula (long black arrow) involving the sigmoid sinus with anterograde drainage coexsisted, as shown by the superselective occipital artery injection (E). A sinus thrombosis involving the superior sagittal sinus and the sigmoid sinus was found (B).
Fig. 7.
Case 2 A, B: No arteriovenous (AV) fistula was found at the time of the preoperative left internal carotid injection. Note the corkscrew appearance of the cortical veins due to the superior sagittal sinus thrombosis at the venous phase (B). Angiogram after embolization and craniotomy (C–F). Anterior view of the left carotid artery injection revealing a de novo pial AV fistula supplied by the central artery (white arrows) (C). Lateral view of the left carotid injection showing that the new fistula with drainage (white arrows) was apparently distinct from the previous fistula, in a comparison with the location and shape of the draining cortical vein (D, E). The external carotid artery system was not attributed to this new fistula (F).
Fig. 8.
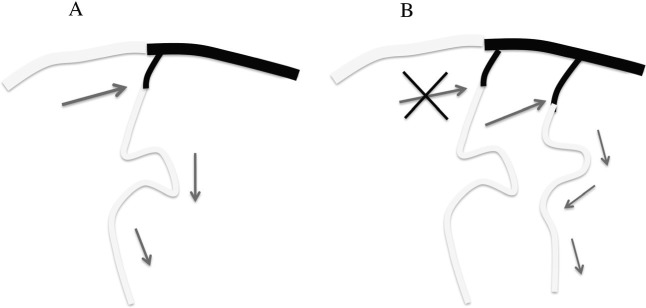
Scheme of Case 2. A: Posterior half of superior sagittal sinus and cortical vein are thrombosed. Dural AVF supplied by external carotid arteries is present. B: Initial dural AVF is obliterated by transarterial embolization and surgical excision; however, de novo pial AVF emerges adjacent to the initial lesion. AVF: arteriovenous fistula.
Discussion
I. Relationship of AVF to SSS thrombosis
It has been proposed that sinus thrombosis precedes and contributes the etiology of dural AVF.6,7) It is widely accepted that sinus occlusion is often identified when dural AVF is noted. However, only a few reports have documented the occurrence of dural AVFs that had been followed-up by angiography after the onset of sinus thrombosis. Several cases of dural AVFs after sinus thrombosis affecting SSS have been reported.2–5) Sugiura et al.2) documented a case in which multiple dural AVFs appeared in the transverse sigmoid and straight sinuses. Ozawa et al.3) reported a dural-pial AVF affecting a cortical vein. There is only one case report of acquired pial AVFs found in a previously thrombosed cortical vein, following aneurysmal subarachnoid hemorrhage.8) To our knowledge, this is the first report describing two cases of acquired pial AVF that developed after presentation of SSS thrombosis associated with protein S deficiency. In both these patients, the thrombosed cortical veins extending from the SSS thrombosis were thought to be associated with the pathological site. In the first patient, the draining vein of the temporal pial AVF was seen on the initial angiogram to be occluded at the onset of SSS thrombosis. The wall irregularity of the draining vein, as shown in Figs. 2 and 3, may be attributed to the residual venous thrombosis resulting from recanalization of the complete venous thrombosis. In the second patient, the SSS side of the draining vein was obliterated. Thus, when a pathological lesion is believed to be an intraluminal thrombosed vein, it is necessary to consider angiographical findings, specifically, the shunting point and thrombus formation in the cortical veins.
II. Relationship to protein S deficiency
Protein S, a cofactor of protein C, inactivates the coagulation factors Va and VIIIa to inhibit the blood coagulation cascade. Forty percent is present as the free type, and the remaining 60% is present as the complex binding C4b protein. A total of 18 patients with sinus thrombosis due to protein S deficiency have been previously reported.9,10) According to previous reports, SSS is frequently involved, although many of the case reports describe multiple locations. Protein S deficiency with dural AVF has been presented in only a few reports.2,11,12) However, there are reports of dural AVF associated with a variety of abnormal coagulation disorders, such as activated protein C resistance,13) antithrombin III deficiency,14) histidine-rich glycoprotein,15) and 20210A mutation of the prothrombin gene.16) Infectious disease, trauma, or dyslipidemia, which occasionally induces thrombosis, never occurred during the clinical course of those reported cases. Obviously, deep venous thrombosis and SSS thrombosis in the present two patients were caused by aggravation of the coagulation system due to protein S deficiency. This condition was favorable for the development of venous thrombosis resulting from SSS, which might increase the incidence of cortical AV fistulas.
Protein S deficiency is divided into three types according to the proposed standard of the Scientific and Standardization Committee of the International Society on Thrombosis and Haemostasis (München, July 1992). Type 1 and Type 3 are known as quantitative defects and have been frequently observed, while Type 2, known as qualitative defects, has been infrequently observed. Case 1 was regarded as Type 1 due to the reduced levels of both total protein S antigen and free protein S antigen; case 2 was regarded as Type 3 due to the normal level of total protein S antigen and a reduced level of free protein S antigen. Although the value of total protein S antigen at 23% (65–130%), free protein S antigen at 16% (60–150%) and protein S activity at less than 10% (60–150%) were remarkably decreased in case 1, there are a few similar reports in which even heterozygotes have free protein S antigen at less than 20% and protein S activity at less than 10%.17,18)
III. Why does thrombus formation cause a dural AVF?
The question of why a fistula may give rise to thrombosed sinuses or cortical veins should be addressed. After histo-logical examination of a thrombosed aneurysm specimen, Nagahiro et al. described the development of numerous de novo capillaries in the aneurysmal wall, suggesting that this may be relevant to the growing mechanism of cerebral giant aneurysms.19) The authors also observed that similar new capillaries developed in many nidi of surgical AVM specimens that were previously embolized. This suggests that a venous thrombus with or without organization provokes the formation of very fine de novo vessels due to angiogenesis in order to recanalize the occluded lumen as the biological response, and spreads to the surrounding area.20,21) The new fine capillary network may assemble to form a lumen, resulting in a draining vein. Once small fistulae arise between arteries and veins, flow of the shunt will increase.
IV. When should surgical intervention be conducted?
In case 1, a de novo pial AVF was recognized and bled 12 years later. Therefore, the patient developed hemiparesis resulting in severe disability. In reviewing this unfortunate event, we regretted the decision to forego surgery, although the patient refused our proposal for surgical treatment at the time of occurrence. Draining the vein of a new pial AVF carries a risk of delayed stenosis or obstruction due to vascular remodeling. In particular, protein S deficiency might result in venous occlusion at some point. Because surgical disconnection of an AV fistula on the brain surface is relatively safe and less invasive, we believe early surgery is acceptable and favorable if patients are under 70 years old and independent. In case 2, a second operation was not performed, not only because of lung cancer, but also because of recurrence after craniotomy. Re-treatment would have been considered if the patient's life expectancy had been long enough.
Conclusion
Two patients with multiple pial and dural AVFs following SSS thrombosis due to protein S deficiency are reported. Thrombosis in the cortical veins seemed to play an important role in the etiology of these AV fistulae associated with protein S deficiency. Long-term follow-up is required because this peculiar disorder has an unusual clinical course.
References
- 1). Matsubara S, Mandzia JL, ter Brugge K, Willinsky RA, Faughnan ME, Manzia JL: Angiographic and clinical characteristics of patients with cerebral arteriovenous malformations associated with hereditary hemorrhagic telangiectasia. AJNR Am J Neuroradiol 21: 1016– 1020, 2000. [PMC free article] [PubMed] [Google Scholar]
- 2). Sugiura Y, Miyamoto T, Takehara S, Sumiya K, Nozaki T: [Multiple dural arteriovenous fistulas following extensive sinus thrombosis: a case report]. No Shinkei Geka 24: 379– 383, 1996. (Japanese) [PubMed] [Google Scholar]
- 3). Ozawa T, Miyasaka Y, Tanaka R, Kurata A, Fujii K: Dural-pial arteriovenous malformation after sinus thrombosis. Stroke 29: 1721– 1724, 1998. [DOI] [PubMed] [Google Scholar]
- 4). Nishio A, Ohata K, Tsuchida K, Tsuyuguchi N, Hara M, Komiyama M, Tsuruno T, Murata T: Dural arteriovenous fistula involving the superior sagittal sinus following sinus thrombosis—case report. Neurol Med Chir (Tokyo) 42: 217– 220, 2002. [DOI] [PubMed] [Google Scholar]
- 5). Toledo MM, Wilson TJ, Dashti S, McDougall CG, Spetzler RF: Dural arteriovenous fistula associated with superior sagittal sinus occlusion secondary to invasion by a parafalcine meningioma: case report. Neurosurgery 67: 205– 207; discussion 207, 2010. [DOI] [PubMed] [Google Scholar]
- 6). Chaudhary MY, Sachdev VP, Cho SH, Weitzner I, Jr, Puljic S, Huang YP: Dural arteriovenous malformation of the major venous sinuses: an acquired lesion. AJNR Am J Neuroradiol 3: 13– 19, 1982. [PMC free article] [PubMed] [Google Scholar]
- 7). Houser OW, Campbell JK, Campbell RJ, Sundt TM, Jr: Arteriovenous malformation affecting the transverse dural venous sinus—an acquired lesion. Mayo Clin Proc 54: 651– 661, 1979. [PubMed] [Google Scholar]
- 8). Phatouros CC, Halbach VV, Dowd CF, Lempert TE, Malek AM, Meyers PM, Higashida RT: Acquired pial arteriovenous fistula following cerebral vein thrombosis. Stroke 30: 2487– 2490, 1999. [DOI] [PubMed] [Google Scholar]
- 9). Fujita A, Kuwamura K, Saitoh M, Sakagami Y, Takaishi Y, Suzuki S, Matsuo T, Tamaki N: [Cerebral sinus thrombosis in a patient with protein S deficiency: a case report]. No Shinkei Geka 25: 467– 472, 1997. (Japanese) [PubMed] [Google Scholar]
- 10). Kuroki K, Taguchi H, Sumida M, Onda J: Dural sinus thrombosis in a patient with protein S deficiency—case report. Neuro Med Chir (Tokyo) 39: 928– 931, 1999. [DOI] [PubMed] [Google Scholar]
- 11). Yassari R, Jahromi B, Macdonald R: Dural arteriovenous fistula after craniotomy for pilocytic astrocytoma in a patient with protein S deficiency. Surg Neurol 58: 59– 64; discussion 64, 2002. [DOI] [PubMed] [Google Scholar]
- 12). Witt O, Pereira PL, Tillmann W: Severe cerebral venous sinus thrombosis and dural arteriovenous fistula in an infant with protein S deficiency. Childs Nerv Syst 15: 128– 130, 1999. [DOI] [PubMed] [Google Scholar]
- 13). Dulli DA, Luzzio CC, Williams EC, Schutta HS: Cerebral venous thrombosis and activated protein C resistance. Stroke 27: 1731– 1733, 1996. [DOI] [PubMed] [Google Scholar]
- 14). Saito A, Takahashi N, Furuno Y, Kamiyama H, Nishimura S, Midorikawa H, Nishijima M: Multiple isolated sinus dural arteriovenous fistulas associated with antithrombin III deficiency—case report. Neurol Med Chir (Tokyo) 48: 455– 459, 2008. [DOI] [PubMed] [Google Scholar]
- 15). Shigekiyo T, Yoshida H, Kanagawa Y, Satoh K, Wakabayashi S, Matsumoto T, Koide T: Histidine-rich glycoprotein (HRG) Tokushima 2: novel HRG deficiency, molecular and cellular characterization. Thromb Haemost 84: 675– 679, 2000. [PubMed] [Google Scholar]
- 16). Gerlach R, Yahya H, Rohde S, Böhm M, Berkefeld J, Scharrer I, Seifert V, Raabe A: Increased incidence of thrombophilic abnormalities in patients with cranial dural arteriovenous fistulae. Neurol Res 25: 745– 748, 2003. [DOI] [PubMed] [Google Scholar]
- 17). Okamoto Y, Yamazaki T, Katsumi A, Kojima T, Takamatsu J, Nishida M, Saito H: A novel nonsense mutation associated with an exon skipping in a patient with hereditary protein S deficiency type I. Thromb Haemost 75: 877– 882, 1996. [PubMed] [Google Scholar]
- 18). Yamazaki T, Katsumi A, Kagami K, Okamoto Y, Sugiura I, Hamaguchi M, Kojima T, Takamatsu J, Saito H: Molecular basis of a hereditary type I protein S deficiency caused by a substitution of Cys for Arg474. Blood 87: 4643– 4650, 1996. [PubMed] [Google Scholar]
- 19). Nagahiro S, Takada A, Goto S, Kai Y, Ushio Y: Thrombosed growing giant aneurysms of the vertebral artery: growth mechanism and management. J Neurosurg 82: 796– 801, 1995. [DOI] [PubMed] [Google Scholar]
- 20). Terada T, Tsuura M, Komai N, Higashida RT, Halbach VV, Dowd CF, Wilson CB, Hieshima GB: The role of angiogenic factor bFGF in the development of dural AVFs. Acta Neurochir (Wien) 138: 877– 883, 1996. [DOI] [PubMed] [Google Scholar]
- 21). Uranishi R, Nakase H, Sakaki T: Expression of angiogenic growth factors in dural arteriovenous fistula. J Neurosurg 91: 781– 786, 1999. [DOI] [PubMed] [Google Scholar]