Abstract
Developing more reliable predictors of seizure outcome following temporal lobe surgery for intractable epilepsy is an important clinical goal. In this context, we investigated patients with refractory temporal lobe epilepsy (TLE) before and after temporal resection. In detail, we explored gray matter (GM) volume change in relation with seizure outcome, using a voxel-based morphometry (VBM) approach. To do so, this study was divided into two parts. The first one involved group analysis of differences in regional GM volume between the groups (good outcome (GO), e.g., no seizures after surgery; poor outcome (PO), e.g., persistent postoperative seizures; and controls, N = 24 in each group), pre- and post-surgery. The second part of the study focused on pre-surgical data only (N = 61), determining whether the degree of GM abnormalities can predict surgical outcomes. For this second step, GM abnormalities were identified, within each lobe, in each patient when compared with an ad hoc sample of age-matched controls. For the first analysis, the results showed larger GM atrophy, mostly in the frontal lobe, in PO patients, relative to both GO patients and controls, pre-surgery. When comparing pre-to-post changes, we found relative GM gains in the GO but not in the PO patients, mostly in the non-resected hemisphere. For the second analysis, only the frontal lobe displayed reliable prediction of seizure outcome. 81% of the patients showing pre-surgical increased GM volume in the frontal lobe became seizure free, post-surgery; while 77% of the patients with pre-surgical reduced frontal GM volume had refractory seizures, post-surgery. A regression analysis revealed that the proportion of voxels with reduced frontal GM volume was a significant predictor of seizure outcome (p = 0.014). Importantly, having less than 1% of the frontal voxels with GM atrophy increased the likelihood of being seizure-free, post-surgery, by seven times. Overall, our results suggest that using pre-surgical GM abnormalities within the frontal lobe is a reliable predictor of seizure outcome post-surgery in TLE. We believe that this frontal GM atrophy captures seizure burden outside the pre-existing ictal temporal lobe, reflecting either the development of epileptogenesis or the loss of a protective, adaptive force helping to control or limit seizures. This study provides evidence of the potential of VBM-based approaches to predict surgical outcomes in refractory TLE candidates.
Keywords: Seizure outcome, Voxel-based morphometry, Refractory temporal lobe epilepsy, Frontal GM abnormalities, Brain surgery
Highlights
-
•
Gray matter abnormalities within the frontal lobe predicts seizure outcome in TLE.
-
•
Poor outcome patients suffer from GM atrophy in the frontal lobe, pre-surgery.
-
•
Good outcome patients show gain of GM in the non-resected hemisphere, post-surgery.
-
•
Frontal GM atrophy captures seizure burden outside the ictal temporal lobe.
1. Introduction
Temporal lobe epilepsy (TLE) is the most frequent type of refractory epilepsy, which commonly leads to surgical treatment (Engel, 2001). However, the successful rate of brain surgery to obtain complete seizure freedom is only about 66% in this population at 1 year (Spencer and Huh, 2008; Tellez-Zenteno et al., 2005), dropping to less than 50% after 10 years (de Tisi et al., 2011). It has been suggested that poor seizure control is the result of multiple factors, including insufficient resection, or the existence of other extra-temporal ictal generators likely stemming from occult or unknown pathology elsewhere in the brain. Therefore, developing more reliable predictors of clinical (seizure) outcome following epilepsy brain surgery is an elusive, but critical continuous clinical goal. To date, the most commonly used predictors are clinical characteristics such as the presence of a lesion such as ictal mesial temporal sclerosis (MTS) or the size of the resection (see review by Zhang et al., 2013). Nevertheless, in the last years, new promising predictors of clinical outcomes in refractory TLE have been described based on pre-surgery MRI measures. For instance, using resting-state functional connectivity, Xu et al. (2014) found that compared with poor outcomes, a successful surgical outcome in TLE was associated with larger interhemispheric homotopic functional connectivity (FC) differences, pre-surgery. Using structural imaging techniques, recurrent post-surgical seizures have been associated with atrophy in multiple areas such as the thalamus (Keller et al., 2015a; Keller et al., 2015b), temporopolar, and insular cortices, (Bernhardt et al., 2010; Bernhardt et al., 2015), along with abnormal white matter tracts emerging from the thalamus (Keller et al., 2015b). In a study using voxel-based morphometry (VBM), Yasuda et al. (2010) found that poor seizure outcome (PO) was associated with a larger pattern of preoperative gray matter (GM) atrophy than good seizure outcome (GO). Importantly, these authors also studied GM change post-surgery, and observed that GO patients displayed an increase in GM postoperatively, compared to PO patients.
Such results suggest that protective neuroplastic mechanisms, a form of functional or structural reserve, may exist in patients that will become seizure free post-surgery. While these results are promising both for understanding the basis of a positive response to the surgery and improving the prediction of surgical outcome, to date, they have not yet been reproduced nor tested at the individual level, which is the major limitation in terms of clinical application.
Accordingly, the current investigation was undertaken to test the association between GM volume and seizure outcome following procedures such as standard anterior temporal lobectomy (ATL) or laser ablation of the MTS, all toward the goal of advancing our ability to use GM measures as predictors of outcome. Based on VBM, we first report on GM volume differences between good and poor outcome groups both prior to and after brain surgery. Second, we focus on pre-surgical individual whole brain GM volume and seek to determine a pattern distinguishing patients with a good versus poor seizure outcome. Based on a prior report (Yasuda et al., 2010), in addition to our initial group results, we hypothesized that individual good or poor outcomes can be identified on a pre-surgical basis by using the level of GM volume loss relative to a large normative age-matched control group. The overarching goal of this work is to try to identify a new structural GM measure, conceptualized as an index of either structural vulnerability or reserve, easily computed as part of pre-surgical workups, capable of reliably predicting individual seizure outcomes in refractory TLE patients.
2. Material and methods
2.1. Participants
2.1.1. TLE patients
A total of 61 patients with refractory TLE that underwent surgical intervention were recruited from the Thomas Jefferson University Comprehensive Epilepsy Center. The recruitment period was between 2007 and 2014, with eligible patients selected serially with no change in inclusion criteria or scanner software parameters during that time. Among eligible patients, a total of 48 (79%) were scanned both pre- and post-surgery. Patients received either a standard en bloc resection of their anterior temporal lobe (ATL, including a partial amygdalohippocampectomy [approximately 4–6 cm from the temporal pole with the size smaller for the patients with left (language dominant) TLE]) (N = 49), laser ablation of the ictal hippocampus (N = 7), or a neocortical resection with the mesial regions spared (N = 5). Using data collected at least 6 months post-surgery, patients were identified as either “good” (Engel Class I, n = 34, e.g., no seizure since the surgery) or “poor” outcome (Engel Class II or higher, n = 27, e.g., persistent post-surgical seizures) (GO and PO, respectively) (Engel et al., 1993). Details of the Thomas Jefferson Comprehensive Epilepsy Center algorithm for surgical decision making is described in Sperling et al. (1992). A combination of video/surface EEG (at least 96 h), MRI, PET, neuropsychological testing and, for a subgroup of patients (25%, n = 15), implanted electrodes and electrocorticography was used to lateralize the side of seizure focus. In order to become a good surgical candidate and be included in this study, a patient must have met the following inclusion criteria: failed at least three seizure medications; unilateral temporal lobe seizure focus; concordant MRI and/or PET findings of unilateral temporal lobe abnormality. TLE patients were excluded from the study for any of the following reasons: medical illness with central nervous system impact other than epilepsy; contraindications to MRI; multiple seizure foci (including bilateral temporal foci); extra-temporal seizures; psychiatric diagnosis other than an Axis-I Depression or Anxiety Disorder; or hospitalization for any Axis I disorder listed in the Diagnostic and Statistical Manual of Mental Disorders, IV. Patients provided written informed consent. Table 1 outlines the patients' demographic and clinical characteristics.
Table 1.
Clinical characteristics of the experimental groups.
| Group analyses at the pre- and post-surgery sessions | |||
|---|---|---|---|
| Good outcome | Poor outcome | Controls | |
| N (females) | 24 (9) | 24 (11) | 24 (9) |
| Seizure lateralization | 14 left | 13 left | |
| Age at 1st MRI scan | 41.1 (12.2) | 42.2 (12.8) | 41.1 (11.8) |
| Age at seizure onset | 19.5 (14) | 24.3 (12.9) | |
| Type of surgery | ATL: 21 | ATL: 16 | |
| Laser ablation: 2 | Laser ablation: 4 | ||
| Neocortical resection: 1 | Neocortical resection: 4 | ||
| MRI pathology | Normal MRI: 6 | Normal MRI: 14 | |
| MTS: 14 | MTS: 6 | ||
| Other temporal pathologya: 4 | Other temporal pathologya: 4 | ||
| PET | Positive: 18 | Positive: 20 | |
| Negative: 2 | Negative: 1 | ||
| Not available: 4 | Not available: 3 | ||
| Time interval between surgery and scan (days, m (std)) | 305 (195) | 296 (208) | |
| Time interval between the two scans (days, m (std)) | 400 (210) | 441 (258) | 429 (119) |
| Seizure type | CPS: 11 | CPS: 12 | |
| CPS + rare GSb: 6 | CPS + rare GSb: 5 | ||
| CPS + GSc: 7 | CPS + GSc: 7 | ||
| Prediction analyses using the pre-surgical data | ||
|---|---|---|
| Good outcome | Poor outcome | |
| N (females) | 34 (16) | 27 (14) |
| Seizure lateralization | 19 left | 13 left |
| Age (m (std)) | 40.5 (12.4) | 42.4 (13.7) |
| Type of surgery | ATL: 30 | ATL: 20 |
| Laser ablation: 3 | Laser ablation: 3 | |
| Neocortical resection: 1 | Neocortical resection: 4 | |
| MRI pathology | Normal MRI: 8 | Normal MRI: 16 |
| MTS: 18 | MTS: 7 | |
| Other temporal pathologya: 8 | Other temporal pathologya: 4 | |
| PET | Positive: 25 (74%) | Positive: 21 (78%) |
| Negative: 3 (9%) | Negative: 3 (11%) | |
| Not available: 6 (17%) | Not available: 3 (11%) | |
| Time interval between scan and surgery (days, m (std)) | 112 (156) | 116 (152) |
| Seizure type | CPS: 17 | CPS: 11 |
| CPS + rare GSb: 8 | CPS + rare GSb: 6 | |
| CPS + GSc: 9 | CPS + GSc: 10 | |
Low grade tumors (DNET, glioma, cavernoma), temporal dysplasia or general temporal atrophy. MTS: mesial temporal sclerosis.
CPS (primary type) with 5 or less generalized tonic–clonic seizure and/or secondarily generalized seizure.
CPS (primary type) with more than 5 generalized tonic–clonic seizure and/or secondarily generalized seizure in lifetime.
2.1.2. Healthy controls
A total of 119 healthy normal controls (NCs) were recruited from the Thomas Jefferson University community, in order to match the patient participants in age and gender. All controls were free of psychiatric or neurological (central nervous system) disorders based on a health screening measure. Among them, 24 were scanned twice with an average interval of 429 days (SD: 119) to match the pre- to post-scan interval for the patients. This study was approved by the Institutional Review Board for Research with Human Subjects at Thomas Jefferson University, and all participants provided a written informed consent.
2.2. MRI data acquisition
All participants underwent Magnetic Resonance Imaging on a 3-T X-series Philips Achieva clinical MRI scanner (Amsterdam, the Netherlands) using an 8-channel head coil. Both the NCs and the TLE patients underwent identical scanning sessions. In detail, each patient underwent a pre-surgical (mean = 114 days prior to surgery, N = 61) and post-surgical scan (m = 305 days after surgery, minimum of 6 months, N = 48). High resolution T1-weighted images were collected using an MPRage sequence (180 slices, 256 × 256 isotropic voxels; TR = 640 ms, TE = 3.2 ms, FOV = 256 mm, flip angle = 8°, voxel size = 1 × 1×1 mm). Subjects lay in a foam pad to comfortably stabilize the head, and were instructed to remain still throughout the scan.
2.3. Preprocessing analyses
In order to preprocess each individual T1 sequence, we used the VBM8 toolbox, available in SPM8 (http://www.fil.ion.ucl.ac.uk/spm/software/spm8). To improve the probability of detecting areas with GM volume changes in relation to surgical outcome, the images of patients with right TLE were flipped left-to-right so that all data could be analyzed together and treated as ipsilateral and contralateral to seizure onset and surgical target area. In order to minimize left-to-right bias when comparing with controls, we also side flipped the same proportion of the healthy control sample. In this context, the left hemisphere was considered the ictal hemisphere.
T1-weighted images were preprocessed using a standard routine (“estimate and write”): the images were spatially normalized to the same stereotaxic space (A Fast Diffeomorphic Registration Algorithm (DARTEL) algorithm, MNI (Montreal Neurological Institute)-152), segmented into GM, white matter and cerebrospinal fluid, non-linearly modulated (aiming to correct to local volume changes during the normalization) and smoothed with an isotropic Gaussian kernel of 8 mm. A test of quality was performed to observe homogeneity and co-registration between the data. Also, post-surgery postprocessed T1s were individually checked to ensure that the normalization step was accurate and comparable to the pre-surgery postprocessed T1s (see Supplementary Fig. 1 for an example).
2.4. Prediction of seizure outcome
2.4.1. Creation of age-matched control templates
The group of controls was split into three groups based on their age: Under 30 (N = 44, minimum age: 18), Between 30 and 40 (N = 34), and Above 40 (N = 42, up to 60 years-old). Within each control group, two maps were created based on the GM images: one average (“Avg map”) and one standard-deviation (“Std map”). Such groups were created to take into account potential age effects on GM volume (Supplementary Fig. 2).
2.4.2. Creation of individual map of GM volume abnormalities
Each of the 61 patients' pre-surgery scan was analyzed individually. To determine statistically significant differences between each patient and the controls, we calculated the Z value at each voxel in the individual patient's image using as comparison our age-matched normative control map. The Z score of each voxel i in each patient's map is given by Zi = (Xi – Avg map)/Std map. As an example, a 25 year-old patient's GM map was compared to the “under 30” control group map. As a result, each individual obtained a 3D Z-map, reflecting the difference in GM relative to the normative group.
Next, the number of voxels with either a value above Z > 2.5 (e.g., voxels showing a significant increase in GM relative to the normative sample) or under Z < −2.5 (e.g., voxels showing significant reduction of GM relative to the normative sample) was counted within each lobe, completed separately for the frontal, occipital, parietal and temporal cortices. Of note, the ipsilateral and contralateral temporal lobes were analyzed separately because of the possible distinct impact of the seizures on the ipsilateral versus contralateral temporal regions. This method and threshold chosen were based on Stufflebeam et al.'s (2011) study. Lastly, each individual patient obtained two scores indicating the proportion of voxels reflecting either an abnormal increase or decrease of GM volume within each lobe, relative to the age-matched normative sample.
Lastly, in order to test the reliability of the chosen threshold (|Z| > 2.5), we tested this method using two alternative thresholds: Z = 2 and Z = 3, and computed the proportion of voxels within each lobe as described above. We then computed correlations between the measures from the different thresholds.
2.5. Statistical analyses
2.5.1. Group analysis: pre-surgery only
To test for differences in pre-surgical GM volumes between the three groups (GO, PO, NCs), a one-way ANOVA was run on the GM volume maps. This analysis included a relative threshold masking of 0.8. Age and gender were added as covariates of no interest. Statistical whole-brain differences were reported with an initial statistical threshold of p = 0.001, uncorrected and a minimum cluster size of 30 contiguous voxels.
2.5.2. Group analysis: pre / post-surgery
Group analyses were computed on 24 GO, 24 PO, and 24 controls, where each individual had two scans. A repeated-measure ANOVA was run to test the effects of session (pre/post-surgery for patients, or sessions one and two for the NCs) and experimental group (GO, PO, NCs) on the GM volume maps. This analysis included a relative threshold masking of 0.8. In order to avoid any confounding effect between normal and true post-surgery changes, we masked the contrast comparing pre- and post-surgery conditions in the patients by the same contrast computed in the controls. Statistical whole-brain differences were reported with an initial statistical threshold of p = 0.001, uncorrected and a minimum cluster size of 30 contiguous voxels.
2.5.3. Prediction of seizure outcome using GM volume abnormalities
In order to investigate whether the GO and PO patients showed significant GM differences, several analyses were conducted. First, chi-squared tests were computed to test the proportion of patients with at least 1% of voxels showing a significant difference relative to controls. The proportion of patients with less than 1% of GM voxels different than controls was also computed (n.b., proportions reflecting increases and decreases were analyzed separately). Of note, this 1% threshold was an arbitrary choice, as there is no consensus threshold available for this individualized method. In order to avoid thresholding, non-parametric Mann–Whitney U Tests were also run to determine significant group (GO versus PO) differences on these continuous (proportion) variables.
Lastly, a logistic regression was computed to predict seizure outcome, using the proportion of voxels with increased or reduced GM volume within each lobe, separately, as the independent variable. We then re-ran the regression to compare the predictive power of these variables with the predictive power of MTS (presence/absence), a more standard clinical predictor.
3. Results
3.1. Clinical characteristics
No significant differences were revealed in age, gender, illness duration, or age at seizure onset between the GO and PO groups (p > 0.05). The proportion of patients reporting multiple generalized seizures (such as generalized tonic–clonic seizures or secondary generalized seizures, see Table 1) was not significantly different between the two groups (GO: 26%, PO: 33%; p = 0.8). The proportion of patients with a PET positive (e.g., hypometabolism in the ictal temporal lobe) versus PET negative was not different between the PO and GO groups (Table 1). Also, the number of patients that went through electrocorticography to localize the seizure onset did not differ between the two groups (chi-square = 1.3, p = 0.3; 7/34 GO vs. 10/27 PO). However, there were significantly more patients with a mesial temporal pathology in the GO than the PO group (chi-square test, p = 0.001). In detail, 77% of the patients showing a mesial temporal pathology became seizure free, post-surgery. Among the patients scanned pre- and post-surgery, when analyzing each resective procedure separately, the resection size did not differ between the GO and PO groups (2 sample t-tests, ATL: p = 0.2; laser: p = 0.2; neocortical resection: not applicable because only one GO patient had this procedure).
3.2. Group changes in GM volume
3.2.1. Pre-surgery only
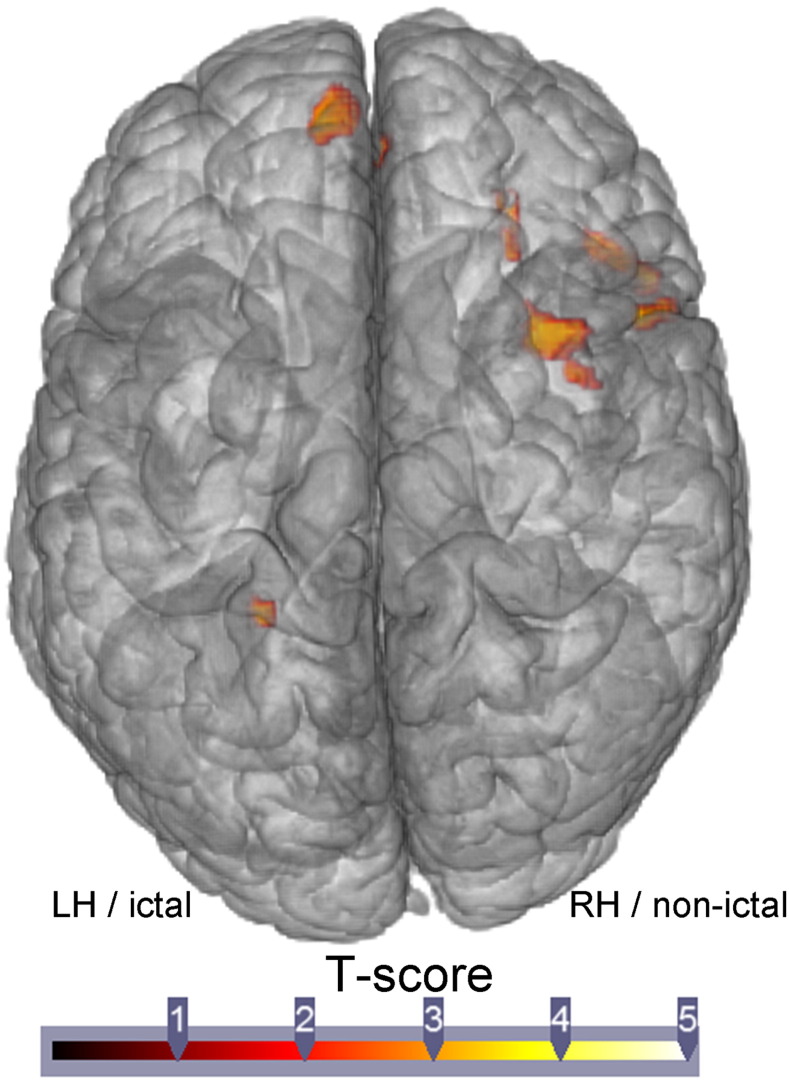
The ANOVA revealed that the GO compared to PO patients displayed several regions of higher GM volume, with these mostly located in the right/non-ictal frontal cortex (Fig. 1, Supplementary Table 1). In contrast, the PO patients showed no GM increases relative to the GO patients. When compared to controls, the GO patients showed increased GM volume in the right/non-ictal middle frontal cortex, the same area noted above with reference to the PO group. The PO patients did not show increased GM, relative to controls. In contrast, the PO group showed reduced GM volume in multiple regions mostly located in the frontal and temporal lobes, with other losses evident in the left/ictal parahippocampus/hippocampus, left/ictal sensory–motor cortex, left/ictal parietal cortex, and right/non-ictal temporal cortex, relative to the controls. Lastly, the GO group had reduced GM volume in a limited set of regions mostly located in the ictal hemisphere (cerebellum, parahippocampal gyrus/hippocampus, rolandic gyrus).
Fig. 1.
Regions showing significantly more GM volume in the GO than in the PO patients, pre-surgery.
When combining GO and PO groups, we found increased GM in the right/non-ictal parahippocampal gyrus, relative to the controls. In contrast, the patients showed multiple regions with GM atrophy mostly located in the ictal hemisphere only, involving the hippocampus extending to the thalamus, putamen, insular cortex, cerebellum, but also bilaterally, in the superior temporal cortex and medial prefrontal cortex (Supplementary Fig. 3).
3.2.2. Pre-/post-change
Regarding the surgical effect, the repeated measures ANOVA revealed a reduction of GM volume post-surgery mostly in areas proximal to the impact of the procedure, regardless of the group of the patients (Table 2). In addition, we detected decreased GM in the ictal thalamus as well as in the left/ictal angular gyrus and precuneus, for both TLE surgery groups.
Table 2.
Regions demonstrating significant structural (GM volume) change between pre- and post-surgery, within each patient group.
| Maximal pics |
|||||
|---|---|---|---|---|---|
| K | T | x | y | z | |
| GO post-pre | |||||
| R rolandic operculum | 376 | 4.88 | 56 | −18 | 22 |
| R inferior frontal | 669 | 4.8 | 48 | 20 | 18 |
| L middle frontal | 368 | 4.27 | −30 | 41 | 34 |
| L inferior frontal | 33 | 4.23 | −44 | 12 | 18 |
| R middle frontal | 215 | 4.23 | 30 | 35 | 37 |
| R middle occipital | 49 | 4.22 | 27 | −90 | 13 |
| R middle frontal | 241 | 4.21 | 29 | 20 | 49 |
| R superior frontal | 101 | 3.98 | 20 | 32 | 45 |
| R middle temporal | 96 | 3.98 | 62 | 0 | −17 |
| R cerebellum | 198 | 3.92 | 39 | −69 | −32 |
| L superior frontal | 53 | 3.82 | −12 | 27 | 52 |
| R fusiform | 138 | 3.76 | 38 | −54 | −20 |
| R middle temporal | 52 | 3.75 | 57 | −48 | −5 |
| R middle temporal | 49 | 3.59 | 59 | −45 | 10 |
| PO post–pre | |||||
| None | |||||
| GO pre–posta | |||||
| L thalamus | 5658 | 10.07 | −9 | −30 | 6 |
| L amygdala (outside the resection area) | 9.73 | −23 | 3 | −17 | |
| L parahippocampal (outside the resection area) | 8 | −23 | 9 | −24 | |
| L precuneus | 3377 | 9.42 | −14 | −40 | 1 |
| L cerebellum | 9.2 | −23 | −31 | −27 | |
| L lingual | 8.43 | −15 | −37 | −6 | |
| L fusiform | 104 | 4.92 | −41 | −64 | −15 |
| L angular | 76 | 3.94 | −51 | −69 | 25 |
| L middle occipital | 36 | 3.82 | −41 | −82 | 15 |
| L superior marginal | 33 | 3.75 | −60 | −48 | 28 |
| PO pre–posta | |||||
| L fusiform | 3920 | 8.59 | −24 | −43 | −11 |
| L precuneus | 7.57 | −14 | −40 | 1 | |
| L fusiform | 6.63 | −32 | −43 | −18 | |
| L amygdala (outside the resection area) | 4865 | 7.35 | −23 | 3 | −17 |
| L thalamus | 6.92 | −9 | −30 | 6 | |
| L superior temporal | 136 | 5.43 | −53 | −37 | 24 |
| L angular | 91 | 4.46 | −47 | −61 | 25 |
| L PCC | 79 | 4.24 | −5 | −40 | 25 |
| L middle occipital | 30 | 3.8 | −47 | −72 | 4 |
Abbreviations: L: left/ictal, PCC: posterior cingular cortex, R: Right/non-ictal.
Exclusion of the ictal temporal lobe.
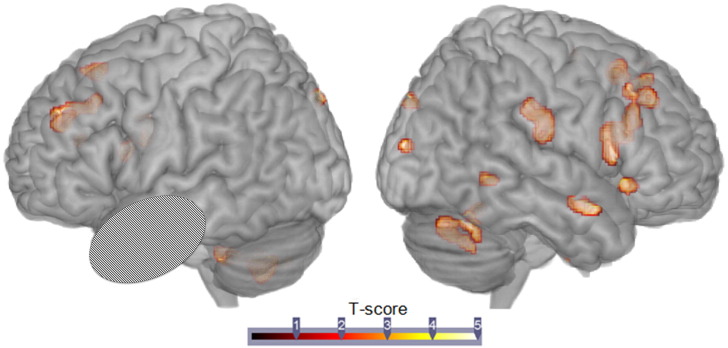
Within the GO group only, increased GM volume post-surgery was found, when compared to pre-surgery. The regions involved were mostly located in the contralateral hemisphere, including the temporal, frontal, occipital cortices and cerebellum. The only regions in the ictal hemisphere with increased GM were all located in the frontal cortex (Fig. 2). Such findings were not found in the PO group.
Fig. 2.
Regions showing relative gain of GM volume post-surgery, relative to pre-surgery, in the GO patients.
When comparing the pre-/post-surgical changes between the two patient groups, we did not reveal significant differences.
3.3. Prediction of seizure outcome
We tested whether pre-surgical GM volume status can distinguish between patients who or will not become seizure free after surgery (GO versus PO).
The only lobe demonstrating significant differences between the two patient groups was the frontal lobe. In other words, the GM abnormalities measured within the temporal, occipital or parietal lobe did not distinguish between the GO and PO groups, and did not reliably predict seizure outcome. Therefore, we will only report the results involving the frontal lobe.
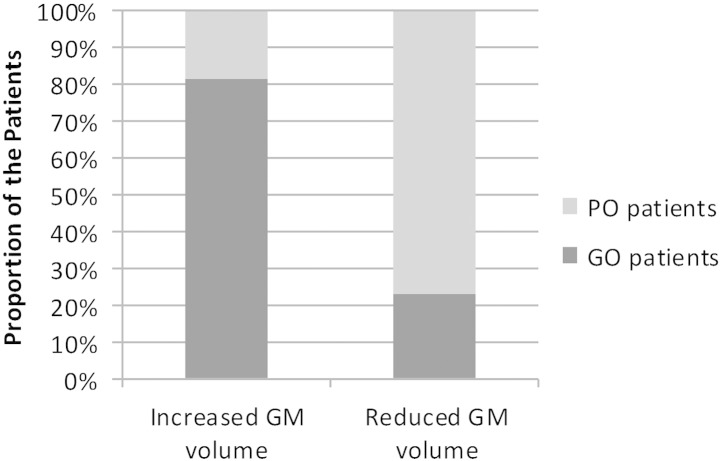
With regard to this frontal lobe finding, the proportion of GO patients with increased GM volume in the frontal lobe was significant higher than in the PO patients (22 of 34, 65% versus 9 of 27, 33%, p = 0.029, χ2 = 4.7). In contrast, the proportion of PO with reduced GM volume in the frontal lobe was slightly higher than in the GO group (13 of 27, 48% versus 9 of 34, 26%, p = 0.14). These proportions remained identical for patients who underwent a standard ATL (n = 50), with the number of patients in our sample who had other procedures too small examine in this regard (e.g., n = 11 of 61). A total of 81% of the patients showing significant increased GM volume in the frontal lobe (proportion of the voxels > 1%) became seizure free after surgery; while 77% of the patients with significant reduced GM volume in the frontal lobe (proportion of the voxels > 1%) showed seizure recurrence and poor post-operative seizure control (Fig. 3).
Fig. 3.
Proportion of GO or PO patients with significantly increased or reduced GM volume (relative to controls) within the frontal lobe, pre-surgery.
Consistently, independent sample t-tests revealed significant differences for each of these two continuous measures between the GO and PO groups. More specifically, compared to the PO patients, the GO patients demonstrated approximately three times more voxels with higher GM volume (0.51% vs. 1.58%, p = 0.001), and 27 times less voxels with reduced GM volume (1.28% vs. 0.34%, p = 0.009) in the frontal lobe.
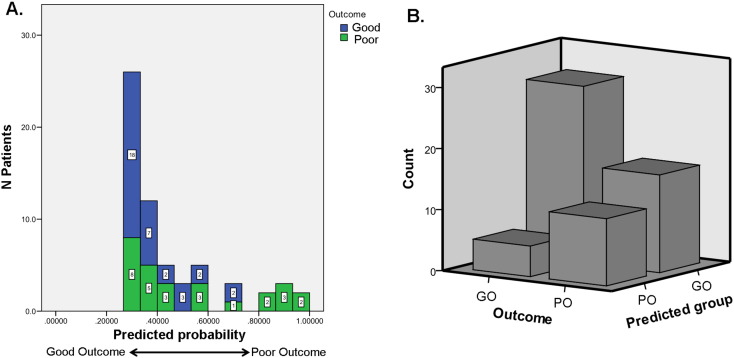
A logistic regression on seizure outcome (GO versus PO) utilizing two predictors (the proportion of voxels with either reduced or increased GM volume) revealed that the reduced GM volume measure was the most significant predictor of outcome (p = 0.014), explaining 16% of the variance (on Cox and Snell R2 coefficient), and classifying 66% of the total sample accurately. Note, a model with one variable (i.e., the proportion of voxels with reduced volume) obtained classification success at an identical level (66%), though the model itself was not significant (p = .072). In detail, 85.3% of the GO patients were well classified while only 40.7% of the PO patients were accurately classified (Fig. 4). Perhaps most important, odds ratio data indicated that when less than 1% of the voxels had reduced GM volume in the frontal lobe compared to normal controls, the likelihood of seizure freedom increased sevenfold.
Fig. 4.
Result of the logistic regression predicting seizure outcome, using the measure of the proportion of voxels with reduced GM volume in the frontal lobe. Part A shows the predictive probability of GO or PO group membership. Part B displays the resulting classification count, N.B., GO patients are better classified (N = 29/34).
Lastly, we tested the potential mediating role mesial pathology might play in the above logistic regression findings. As a single categorical predictor (i.e., the presence or absence of mesial pathology), the mesial pathology classified 70.5% of the sample accurately, and explained 16% of the model variance (p = 0.002). The odds ratio data revealed that the presence of mesial pathology increased the likelihood of seizure freedom sixfold within our TLE sample. When we added to the model the measure reflecting the proportion of voxels with reduced GM volume in the frontal lobe, the model remained significant (p = 0.032), explaining 26% of the variance, and classifying 79% of the sample accurately (85% of the GO group, and 70% of the PO). Thus, the presence of mesial pathology provided additional predictive value to the model containing solely our frontal lobe measure of GM volume reduction, but yielded improvement only in the classification of PO, not GO patients. Importantly, when examining the unique variance and classification accuracy of the variables, the odds ratios for each of the two variables remain impressive in terms of predicting seizure freedom (presence versus absence of reduced frontal GM volume: 5–1 odds of seizure freedom; presence versus absence of mesial temporal pathology: 4 to 1odds).
Overall, our results suggest that a statistical model utilizing a measure capturing the proportion of voxels with significant GM volume loss (relative to matched controls) in the frontal lobe, provides significant improvement and added value in the prediction of seizure outcome, when included in a model containing an index of mesial pathology, the more-established and better known predictor of seizure outcome following ATL.
3.4. Reliability of the thresholds
We tested the reliability of our results by examining two alternative thresholds (Z = 2 and 3; Supplementary Fig. 4) for capturing the proportion of voxels with abnormal GM volume. We found high correlations between the variables based on our primary (|Z| > 2.5) and these new thresholds. For instance, the correlation between the proportion of voxels with abnormal increased GM volume at |Z| > 2.5, and these new thresholds was r = 0.98 for |Z| > 2.0, and r = 0.99 for |Z| > 3.0 for the frontal lobe. The weakest correlation was observed for the non-ictal temporal lobe (r = .9, involving the Z = 2.5/Z = 2.0 thresholds, and r = .89, involving the Z = 2.5/Z = 3.0 thresholds). This suggests that our findings are robust with respect to proximal changes in threshold, providing a reasonable replication and confirmation of our findings.
4. Discussion
The primary purpose of this study was to determine whether pre-surgical GM structural measures are associated with seizure outcome in patients with refractory unilateral TLE. All the patients included in this study were refractory to medication and based on a comprehensive pre-surgical algorithm (MRI, PET, EEG, intracorticography, neuropsychological testing) were considered good candidates for either a resective (ATL or neocortical resection) or ablative surgical procedure.
4.1. Pre-surgery findings
Prior to surgery, regardless of the seizure outcome, the patients showed multiple regions with GM atrophy, relative to controls. In detail, we found loss of GM in the ictal hippocampus, the thalamus as well as the insular cortex, but also bilaterally, in the temporal cortex. These findings are consistent with previous studies (see review by Keller and Roberts, 2008). Indeed, thalamic abnormalities has been observed in several studies of refractory TLE, and been reported as a predictor of seizure outcome (Keller et al., 2015b; Sakamoto et al., 2009). We also found that our TLE patients as a whole demonstrated a GM increase in the non-ictal parahippocampal gyrus. This finding is consistent with resting-state fMRI studies of TLE showing decreased connectivity within the epileptogenic network in conjunction with increased connectivity within the contralateral regions (Bettus et al., 2009). Such resting-state data are considered to reflect neuroplasticity and contralateral compensatory mechanisms (Bettus et al., 2009; Doucet et al., 2013; Tracy and Doucet, 2015). Our study provides evidence of structural GM increases, supportive of this compensatory explanation.
When comparing the GO and PO groups, however, GM differences were evident, particularly in the frontal lobe. Such findings stand in agreement with other studies that used other structural measures such as cortical thinning (Bernhardt et al., 2010) or white matter stream microstructure (Bonilha et al., 2013; Keller et al., 2015b). In detail, our PO group displayed more extensive regional atrophy than both the GO and controls, mostly located in the frontal cortex, bilaterally. In contrast, the GO group mostly showed limited GM losses located in the ictal hemisphere, relative to the controls. This data is consistent with diffusion tensor imaging studies which demonstrated that compared to PO ATL patients, GO patients have fewer abnormalities in the ictal hemisphere, with these limited to the temporal and frontal cortices (see review by Bonilha and Keller, 2015). However, our data go beyond the extant literature by indicating that an advantage in frontal lobe GM may constitute a key difference in the pre-surgical status of these two groups. Our data suggest that the PO patients suffer from stronger vulnerability in their frontal lobe, possibly caused by seizure spread or diaschisis. Indeed, previous imaging studies have provided strong evidence that the frontal lobe is involved in the spread of the temporal lobe seizures. For instance, Lin et al. (2008) showed that patients with TLE specifically suffer from abnormal integrity of frontal–temporal white matter tracts within the ictal hemisphere. Using single photon emission computed tomography, Van Paesschen et al. (2003) described the frontal lobe as abnormally perfused during temporal lobe seizures, relative to the inter-ictal state. Lastly, a number of researchers have noted a common ictal propagation pathway from the mesial temporal lobe, to the ipsilateral frontal lobe (preferentially the orbitofrontal cortex), to the contralateral frontal lobe, and finally, the contralateral temporal lobe (Adam et al., 1994; Lieb et al., 1991). These data are consistent with our findings, and imply that the spread of seizures in our PO group may have impaired the frontal lobe in a more extensive way than in GO patients, producing significant consequences in terms of seizure outcome. Alternatively, previous work from our laboratory has shown that the frontal lobe may play a role in a protective mechanism, an inhibitory surround, that works against seizure spread (see Tracy et al. (2014)). Unfortunately, our study cannot discriminate between the possibility of a protective mechanism in our GO patients or more extensive seizure burden in our PO patients from seizure spread or epileptogenesis. More investigations need to be done to tests these different hypotheses.
4.2. Pre-to-post changes
When investigating the change of GM between pre- and post-surgery, we found that the relative loss of GM volume, post-surgery, was limited to ipsilateral regions to the resected area, for both the GO and PO patients. This loss is likely related to the surgical manipulation and/or tissue shrinkage over time (aging) after resection (Mueller et al., 2009). Importantly, our pre–post analysis controlled for this effect, which may explain the differences between our findings and Yasuda et al. (2010) who described post-surgical atrophy in both ipsilateral and contralateral regions. Indeed, these authors did not control for such a procedural and time-based effect. As a confirmation, we compared pre- and post-surgery GM in the GO patients (using a paired t test, without controlling for the time effect), and found a relative loss of GM volume in the contralateral hemisphere (data not shown), providing evidence that these more atrophic contralateral regions are not related to seizure control, nor the surgical procedure per se, but more likely to a time-based (aging) effect.
In contrast, when comparing post- to pre-surgery GM status, we found a relative gain in volume in multiple regions in the GO but not in the PO patients. Most of the regions showing gain were located in the contralateral (non-resected) frontal and temporal lobes, suggesting that these changes were not directly caused by the resection (Mueller et al., 2009), but other mechanisms involved in seizure control. It is important to note that the controls did not show any significant GM volume change or gain, when comparing data across the scanning sessions, noting that the time interval between this group's scans and the interval between pre- and post-surgical scans for the patients did not differ. This post-surgical gain in GM volume is considered potentially related to increased axonal and dendritic arborization, neuronal size and number (May et al., 2007; Mechelli et al., 2005; Yasuda et al., 2010). Accordingly, our data are consistent with the possibility that the GM gains in the GO group reflect brain recovery through a neuroplastic mechanism generated by the new state of seizure control.
We should note that our pre- to post-surgical comparison data are generally in agreement with the findings of Yasuda et al. (2010) despite the difference in scanners, different magnet strengths, and the different GM processing methods utilized in the two studies. This is particularly encouraging in a clinical context, suggesting that these findings are reliable and reproducible regardless of the scanner used.
4.3. Prediction of seizure outcome
Using the proportion of voxels with increased or reduced GM volume within each lobe, we investigated whether the degree of GM abnormality was a reliable predictor of seizure outcome. Results yielded by our regression approach revealed that GM abnormalities located in the frontal lobe were significant predictors of seizure outcome. To our knowledge, this is the first study describing the use of GM abnormalities to predict seizure outcome following brain surgery in patients with refractory TLE. Importantly, the regression analysis showed that this measure was as robust and effective as the presence of mesial temporal atrophy in predicting seizure outcome (66% vs. 70%), but combining the two measures did improve the model, moving the proportion accurately classified to 80% of the sample. Also, the odds ratios for both measures were relatively similar and high. Such findings are particularly encouraging from a clinical perspective, as improved outcome prediction is the major goal of pre-surgical algorithms. While the GM index we chose to use (proportion abnormal for each lobe), can readily be calculated at most surgical sites, it is important to develop site specific normative data (from the same scanner) from a large sample of healthy controls, age-matched to the TLE patient sample, as GM volume maps are known to be particularly sensitive to age (see Supplementary Fig. 2).
Importantly, our data highlight the importance of utilizing extra-temporal GM measures when predicting outcome, and provide additional confirmation that structural effects of unilateral, focal TLE are not restricted to a single region (for a review of the extra-temporal effects of TLE seizures see Tracy et al., 2015).
Unlike previous studies (Bernhardt et al., 2015; Lin et al., 2005), we did not find that abnormal GM volume in either temporal lobe was a good predictor of seizure outcome. We believe that this may be related to difference in the masks utilized for volume calculation. We did not test a mask that included only the mesial temporal lobe (hippocampus and parahippocampal gyrus); ours included the full temporal lobe. Similarly, we did not test the predictive power of subcortical regions (e.g., the thalamus), and, therefore, cannot compare our findings to studies using thalamic atrophy as a predictor of seizure outcome (Keller et al., 2015b). In this regard, comparing different size masks will be important, a tradeoff between GM signal strength versus GM signal specificity, in the determination of clinical value when using GM volume measures to predict post-surgical seizure outcome. Also, to increase reliability in the prediction, the use of bootstrapping methods and machine learning algorithms, incorporating multiple GM measures, may be of benefit for the selection of the most robust predictors of seizure outcome (Munsell et al., 2015).
4.4. Limitations
Several limitations regarding our study must be noted. Our sample was relatively small. Unfortunately, we could not fully match the GO and PO patients on the type of mesial pathology, such as MTS. While we cannot fully preclude MTS as a factor in our results, we did demonstrate, one, that the frontal lobe effect we describe goes beyond the predictive power of MTS, and, two, that the effect (or lack thereof) was present in both our GO and PO patients who did not possess MTS. As it is widely recognized that the rate of seizure freedom diminishes at longer term follow-up (e.g., 5 years after resective surgery (Tellez-Zenteno et al., 2005)), we cannot exclude the possibility that some of the GO patients will experience seizure recurrence, and are, therefore, in some sense misidentified by our current classification. Accordingly, this issue may explain why we did not find generalized seizures to be a reliable predictor of seizure outcome in our sample, in contrast to other studies (Zhang et al., 2013). Nevertheless, it is encouraging to note that 35% of our GO patients had resective surgery in 2010 or earlier, suggesting that their seizure freedom is well established.
For the purpose of investigating seizure outcome, we chose to combine patients with TLE that went through standard ATL, thermal ablation or neocortical resection procedures. Although the surgeries were localized in the temporal lobe, these are obviously very different procedures, with the seizure outcome data on thermal ablation still a work in progress (Chang et al., 2015). Germane to our findings, there is also the likelihood that these two procedures have different effects on GM subsequent to the procedure, much as neocortical temporal versus mesial temporal seizures are likely to effect extra-temporal GM (both pre- and post-surgery) in different ways (Kim et al., 2003; Umeoka et al., 2007). Unfortunately, because of low sample size, it was not possible to test the distinct effect of the different procedures, nor was it possible to examine and compare patients with mesial versus neocortical pathology. We do know that most of the patients (57%) that went through laser ablation of their mesial temporal pathology experienced a poor seizure outcome, suggesting insufficient removal of epileptogenic tissues. Yet, given our data we cannot preclude the possibility that despite these differences, temporal lobe surgery patients who possess better GM integrity in the frontal lobe before surgery, will be at an advantage in terms of seizure control. Clearly, future investigation in this area is needed.
Lastly, it is important to highlight some methodological issues. First, the threshold chosen at the group level (first part of our study) was uncorrected for multiple comparisons. This choice increased the risk of type I false positive errors, and therefore, the group differences should be interpreted with caution. However, it is important to remember that the purpose of our study was less about demonstrating outcome group differences in GM volume, and more about: (1) testing the power of GM volume to predict seizure outcome, and (2) determining the regionally specific GM measure that would be the best predictor. Hence, we undertook analyses that would be highly sensitive to predictive success, without allowing too high a rate of Type I error. Also important to note is that the second part of our study focusing on measures that capture the proportion of voxels showing GM group differences utilized analyses completely independent of the threshold chosen at the group level. We tested different thresholds and found identical results, providing reasonable confirmation of the validity of our method. The fact that our frontal lobe finding remains consistent across the two phases of our analyses provides some validation of the effect, and its reliable discrimination between the outcome groups. Therefore, we believe that our results remain valid, despite, at points, allowing for higher levels of Type I error.
Second, we decided to flip the right-sided TLE patients' brain, so that all images were in accord with respect to the site of ictal onset (i.e., on the left side). Such a method has been undertaken previously (Bernhardt et al., 2010; Lin et al., 2005; Yasuda et al., 2010), though we acknowledge that this may have prevented us from discerning specific predictive GM features unique to the right or left TLE patients (Doucet et al., 2013; Tracy and Doucet, 2015). We believe that combining the right and left TLE patients into one group remains an effective method of revealing whole-brain changes associated with TLE pathology, especially when the purpose of the study is to investigate the prediction of recurrent seizures (independently of the side of the epileptogenic focus).
5. Conclusion
Our study showed significant differences in GM volume between GO and PO TLE patients, at time points both before and after brain surgery. These results are consistent with a previous study (Yasuda et al., 2010), indicating that these findings are reliable and reproducible regardless of the scanner type, strength of magnet, and processing methods. The pre-surgical GM abnormalities we observed in the frontal lobe for the PO patients may reflect the impact of seizure spread or occult epileptogenesis. Indeed, it is consistent with evidence suggesting that seizures are less likely to stop after surgery when presurgical abnormalities are observed in brain regions located outside the resected temporal lobe (Bonilha and Keller, 2015). The pre-to-post changes showing a relative gain in GM volume post-surgery for the GO group may reflect tissue recovery from the relief of seizure burden (spread), a protective mechanism to prevent seizures from returning, or some other adaptive neuroplastic mechanism generated by the new state of seizure control (or perhaps all three). Importantly, here, we report the first evidence that patients with TLE with significantly reduced GM in the frontal lobe, pre-surgery, will more likely experience a poor seizure outcome, post-surgery. The converse is also true with our data: patients with TLE advantaged with higher GM volume in the frontal lobe, pre-surgery, will more likely experience seizure freedom after surgery. To our knowledge, this study is the first to demonstrate that an extra-temporal GM measure can reliably predict seizure outcome in refractory TLE patients, and do so as robustly as the presence of mesial temporal sclerosis, a more standard predictor. Certainly, independent investigations are needed to reproduce these results, but we hope to have demonstrated that this easy to compute regional GM measure may be of value in determining good surgical candidates, serving to improve rates of post-surgical seizure freedom in this population.
Acknowledgments
The authors thank Dr. Dorian Pustina for his participation in the data acquisition. None of the authors have any conflict of interest to disclose.
Footnotes
Supplementary data to this article can be found online at http://dx.doi.org/10.1016/j.nicl.2015.09.006.
Appendix A. Supplementary data
Supplementary materials.
References
- Adam C., Saint-Hilaire J.M., Richer F. Temporal and spatial characteristics of intracerebral seizure propagation: predictive value in surgery for temporal lobe epilepsy. Epilepsia. 1994;35(5):1065–1072. doi: 10.1111/j.1528-1157.1994.tb02556.x. [DOI] [PubMed] [Google Scholar]
- Bernhardt B.C., Bernasconi N., Concha L., Bernasconi A. Cortical thickness analysis in temporal lobe epilepsy: reproducibility and relation to outcome. Neurology. 2010;74(22):1776–1784. doi: 10.1212/WNL.0b013e3181e0f80a. [DOI] [PubMed] [Google Scholar]
- Bernhardt B.C., Hong S.J., Bernasconi A., Bernasconi N. Magnetic resonance imaging pattern learning in temporal lobe epilepsy: classification and prognostics. Ann. Neurol. 2015;77(3):436–446. doi: 10.1002/ana.24341. [DOI] [PubMed] [Google Scholar]
- Bettus G., Guedj E., Joyeux F., Confort-Gouny S., Soulier E., Laguitton V., Cozzone P.J., Chauvel P., Ranjeva J.P., Bartolomei F., Guye M. Decreased basal fMRI functional connectivity in epileptogenic networks and contralateral compensatory mechanisms. Hum. Brain Mapp. 2009;30(5):1580–1591. doi: 10.1002/hbm.20625. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bonilha L., Helpern J.A., Sainju R., Nesland T., Edwards J.C., Glazier S.S., Tabesh A. Presurgical connectome and postsurgical seizure control in temporal lobe epilepsy. Neurology. 2013;81(19):1704–1710. doi: 10.1212/01.wnl.0000435306.95271.5f. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bonilha L., Keller S.S. Quantitative MRI in refractory temporal lobe epilepsy: relationship with surgical outcomes. Quant. Imaging Med. Surg. 2015;5:204–224. doi: 10.3978/j.issn.2223-4292.2015.01.01. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chang E.F., Englot D.J., Vadera S. Minimally invasive surgical approaches for temporal lobe epilepsy. Epilepsy Behav. 2015;47:24–33. doi: 10.1016/j.yebeh.2015.04.033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- de Tisi J., Bell G.S., Peacock J.L., McEvoy A.W., Harkness W.F., Sander J.W., Duncan J.S. The long-term outcome of adult epilepsy surgery, patterns of seizure remission, and relapse: a cohort study. The Lancet. 2011;378(9800):1388–1395. doi: 10.1016/S0140-6736(11)60890-8. [DOI] [PubMed] [Google Scholar]
- Doucet G., Osipowicz K., Sharan A., Sperling M.R., Tracy J.I. Extratemporal functional connectivity impairments at rest are related to memory performance in mesial temporal epilepsy. Hum. Brain Mapp. 2013;34(9):2202–2216. doi: 10.1002/hbm.22059. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Engel J.J., Van Ness P.C., Rasmussen T.B., Ojemann L.M. Outcome with respect to epileptic seizures. In: Engel J. Jr., editor. pp. Raven; New York: 1993. pp. 609–621. [Google Scholar]
- Engel J. Mesial temporal lobe epilepsy: what have we learned? Neuroscientist. 2001;7(4):340–352. doi: 10.1177/107385840100700410. [DOI] [PubMed] [Google Scholar]
- Keller S.S., Richardson M.P., O'Muircheartaigh J., Schoene-Bake J.C., Elger C., Weber B. Morphometric MRI alterations and postoperative seizure control in refractory temporal lobe epilepsy. Hum. Brain Mapp. 2015;36(5):1637–1647. doi: 10.1002/hbm.22722. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Keller S.S., Richardson M.P., Schoene-Bake J.C., O'Muircheartaigh J., Elkommos S., Kreilkamp B., Goh Y.Y., Marson A.G., Elger C., Weber B. Thalamotemporal alteration and postoperative seizures in temporal lobe epilepsy. Ann. Neurol. 2015;77(5):760–774. doi: 10.1002/ana.24376. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Keller S.S., Roberts N. Voxel-based morphometry of temporal lobe epilepsy: an introduction and review of the literature. Epilepsia. 2008;49(5):741–757. doi: 10.1111/j.1528-1167.2007.01485.x. [DOI] [PubMed] [Google Scholar]
- Kim Y.K., Lee D.S., Lee S.K., Kim S.K., Chung C.K., Chang K.H., Choi K.Y., Chung J.K., Lee M.C. Differential features of metabolic abnormalities between medial and lateral temporal lobe epilepsy: quantitative analysis of (18)F-FDG PET using SPM. J. Nucl. Med. 2003;44:1006–1012. [PubMed] [Google Scholar]
- Lieb J.P., Dasheiff R.M., Engel J., Jr. Role of the frontal lobes in the propagation of mesial temporal lobe seizures. Epilepsia. 1991;32(6):822–837. doi: 10.1111/j.1528-1157.1991.tb05539.x. [DOI] [PubMed] [Google Scholar]
- Lin J.J., Riley J.D., Juranek J., Cramer S.C. Vulnerability of the frontal–temporal connections in temporal lobe epilepsy. Epilepsy Res. 2008;82(2–3):162–170. doi: 10.1016/j.eplepsyres.2008.07.020. [DOI] [PubMed] [Google Scholar]
- Lin J.J., Salamon N., Dutton R.A., Lee A.D., Geaga J.A., Hayashi K.M., Toga A.W., Engel J., Jr., Thompson P.M. Three-dimensional preoperative maps of hippocampal atrophy predict surgical outcomes in temporal lobe epilepsy. Neurology. 2005;65(7):1094–1097. doi: 10.1212/01.wnl.0000179003.95838.71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- May A., Hajak G., Ganssbauer S., Steffens T., Langguth B., Kleinjung T., Eichhammer P. Structural brain alterations following 5 days of intervention: dynamic aspects of neuroplasticity. Cereb. Cortex. 2007;17(1):205–210. doi: 10.1093/cercor/bhj138. [DOI] [PubMed] [Google Scholar]
- Mechelli A., Friston K.J., Frackowiak R.S., Price C.J. Structural covariance in the human cortex. J. Neurosci. 2005;25(36):8303–8310. doi: 10.1523/JNEUROSCI.0357-05.2005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mueller S.G., Laxer K.D., Barakos J., Cheong I., Garcia P., Weiner M.W. Widespread neocortical abnormalities in temporal lobe epilepsy with and without mesial sclerosis. Neuroimage. 2009;46(2):353–359. doi: 10.1016/j.neuroimage.2009.02.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Munsell B.C., Wee C.Y., Keller S.S., Weber B., Elger C., da Silva L.A.T., Nesland T., Styner M., Shen D., Bonilha L. Evaluation of machine learning algorithms for treatment outcome prediction in patients with epilepsy based on structural connectome data. Neuroimage. 2015;118:219–230. doi: 10.1016/j.neuroimage.2015.06.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sakamoto S., Takami T., Tsuyuguchi N., Morino M., Ohata K., Inoue Y., Ide W., Hashimoto I., Kamada H., Tanaka H., Hara M. Prediction of seizure outcome following epilepsy surgery: asymmetry of thalamic glucose metabolism and cerebral neural activity in temporal lobe epilepsy. Seizure. 2009;18(1):1–6. doi: 10.1016/j.seizure.2008.05.004. [DOI] [PubMed] [Google Scholar]
- Spencer S., Huh L. Outcomes of epilepsy surgery in adults and children. Lancet Neurol. 2008;7(6):525–537. doi: 10.1016/S1474-4422(08)70109-1. [DOI] [PubMed] [Google Scholar]
- Sperling M.R., O'Connor M.J., Saykin A.J., Phillips C.A., Morrell M.J., Bridgman P.A., French J.A., Gonatas N. A noninvasive protocol for anterior temporal lobectomy. Neurology. 1992;42(2):416–422. doi: 10.1212/wnl.42.2.416. [DOI] [PubMed] [Google Scholar]
- Stufflebeam S.M., Liu H., Sepulcre J., Tanaka N., Buckner R.L., Madsen J.R. Localization of focal epileptic discharges using functional connectivity magnetic resonance imaging. J. Neurosurg. 2011;114(6):1693–1697. doi: 10.3171/2011.1.JNS10482. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tellez-Zenteno J.F., Dhar R., Wiebe S. Long-term seizure outcomes following epilepsy surgery: a systematic review and meta-analysis. Brain. 2005;128(5):1188–1198. doi: 10.1093/brain/awh449. [DOI] [PubMed] [Google Scholar]
- Yasuda C.L., Valise C., Saúde A.V., Pereira A.R., Pereira F.R., Ferreira Costa A.L., Morita M.E., Betting L.E., Castellano G., Mantovani Guerreiro C.A., Tedeschi H., de Oliveira E., Cendes F. Dynamic changes in white and gray matter volume are associated with outcome of surgical treatment in temporal lobe epilepsy. Neuroimage. 2010;49(1):71–79. doi: 10.1016/j.neuroimage.2009.08.014. [DOI] [PubMed] [Google Scholar]
- Tracy J., Pustina D., Doucet G., Osipowicz K. Seizure-induced neuroplasticity and cognitive network reorganization in epilepsy. In: Tracy J., Hampstead B., Sathian K., editors. Cognitive Plasticity in Neurologic Disorders. Oxford University Press; New York: 2015. [Google Scholar]
- Tracy J.I., Doucet G.E. Resting-state functional connectivity in epilepsy: growing relevance for clinical decision making. Curr. Opin. Neurol. 2015;28(2):158–165. doi: 10.1097/WCO.0000000000000178. [DOI] [PubMed] [Google Scholar]
- Tracy J.I., Osipowicz K., Spechler P., Sharan A., Skidmore C., Doucet G., Sperling M.R. Functional connectivity evidence of cortico–cortico inhibition in temporal lobe epilepsy. Hum. Brain Mapp. 2014;35(1):353–366. doi: 10.1002/hbm.22181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Umeoka S., Matsuda K., Baba K., Usui N., Tottori T., Terada K., Usui K., Nakamura F., Inoue Y., Fujiwara T., Mihara T. Usefulness of 123I-iomazenil single-photon emission computed tomography in discriminating between mesial and lateral temporal lobe epilepsy in patients in whom magnetic resonance imaging demonstrates normal findings. J. Neurosurg. 2007;107(2):352–363. doi: 10.3171/JNS-07/08/0352. [DOI] [PubMed] [Google Scholar]
- Van Paesschen W., Dupont P., Van Driel G., Van Billoen H., Maes A. SPECT perfusion changes during complex partial seizures in patients with hippocampal sclerosis. Brain. 2003;126(5):1103–1111. doi: 10.1093/brain/awg108. [DOI] [PubMed] [Google Scholar]
- Xu Q., Zhang Z., Liao W., Xiang L., Yang F., Wang Z., Chen G., Tan Q., Jiao Q., Lu G. Time-shift homotopic connectivity in mesial temporal lobe epilepsy. American Journal of Neuroradiology. 2014;35(9):1746–1752. doi: 10.3174/ajnr.A3934. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhang J., Liu W., Chen H., Xia H., Zhou Z., Mei S., Liu Q., Li Y. Identification of common predictors of surgical outcomes for epilepsy surgery. Neuropsychiatr. Dis. Treat. 2013;9:1673–1682. doi: 10.2147/NDT.S53802. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplementary materials.