Abstract
Cardiac tamponade resulting from perforation of a cardiac chamber is a relatively rare complication of pacemaker implantation. We report the first case of perforation of the right coronary artery related to the implantation of a screw-in atrial pacing lead, presenting as life-threatening cardiac tamponade.
We report the case of a 72-year-old woman with complete atrioventricular block and dyspnea on exertion. A permanent pacemaker was implanted with bipolar Medtronic active-fixation leads positioned in the right atrial appendage and at the right ventricular basal septum without any difficulty. Approximately 3.5 h after the procedure, the patient complained of nausea, and the systolic blood pressure decreased to less than 60 mmHg. Echocardiography revealed a large pericardial effusion. Because the effects of pericardiocentesis lasted for less than an hour, the patient underwent a thoracotomy. After evacuation of a massive hemopericardium, bright red blood was seen gushing out from the right coronary artery, which was located on the opposite site of the right atrial appendage where a small portion of the screw tip was observed to be penetrating the atrial wall. The right coronary artery perforation was repaired using autologous pericardium-reinforced 7-0 prolene mattress sutures.
Perforation of the right coronary artery is a potential complication and should be part of the differential diagnosis of cardiac tamponade after pacemaker implantation.
Keywords: Pacemaker, Active-fixation atrial pacing lead, Cardiac tamponade, Right coronary artery perforation
1. Introduction
Perforation of a cardiac chamber has been reported as a relatively rare complication of pacemaker implantation; in particular, attachment of the active-fixation atrial lead to the atrial wall carries the risk of perforation that can result in cardiac tamponade [1–10].
This report describes a case of right coronary artery perforation related to implantation of an active-fixation atrial pacing lead, which has not been reported previously as a complication of pacemaker implantation.
2. Case report
A 72-year-old woman who complained of dyspnea on exertion was referred to our hospital on January 21, 2010. Electrocardiography (ECG) on admission showed complete atrioventricular block with a junctional escape rhythm of 35 bpm. Although chest radiographs revealed pulmonary congestion and an increased cardiothoracic ratio of 55%, echocardiography showed no evidence of structural heart disease or other abnormalities. Laboratory data were within normal limits, with the exception of an elevated amino-terminal fragment of the B-type natriuretic peptide prohormone concentration of 653 pg/mL.
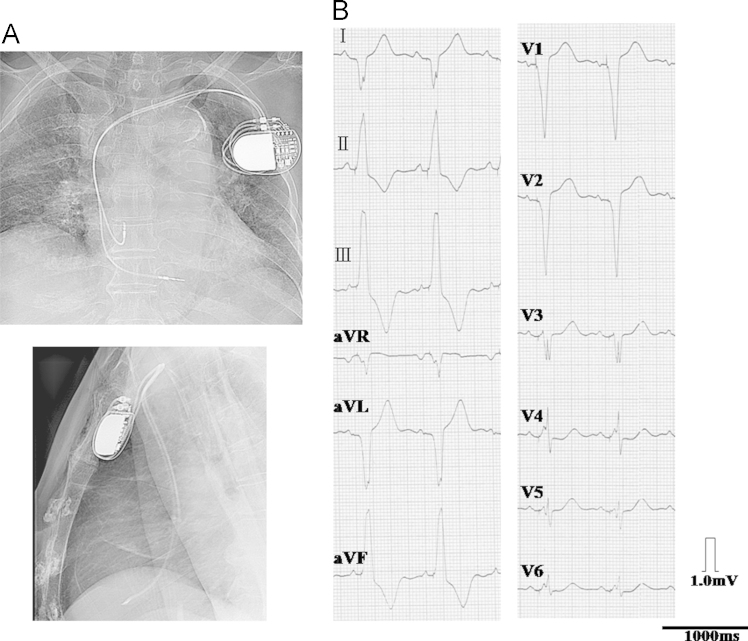
Permanent pacemaker implantation via the left subclavian vein was performed subsequently with bipolar active-fixation leads (Medtronic CapSureFix Novus, model 5076, Minneapolis, MN, USA) positioned in the right atrial appendage and at the right ventricular basal septum without any difficulty. The atrial pacing threshold was 0.7 V at 0.5 ms, the pacing impedance was 615 Ω, and the P-wave amplitude was 3.1 mV. The ventricular pacing threshold was 0.5 V at 0.5 ms, the pacing impedance was 888 Ω, and the R-wave amplitude was 6.2 mV. A generator (Sensia DR model SEDR01; Medtronic) was then connected, and ECG showed normal dual-chamber pacing. Movement of the cardiac silhouette on cinefluoroscopy in a 30° left anterior oblique view was normal at the end of the procedure. Chest radiographs obtained in the operation room showed the right atrial lead positioned in the right atrial appendage (Fig. 1). An ECG recorded 40 min after the implantation demonstrated that the pacemaker was normally functioning with atrial sensing followed by ventricular pacing (Fig. 1).
Fig. 1.
(A) Posteroanterior and left lateral chest radiographs recorded in the operation room show that the screw-in atrial lead was located in the right atrial appendage and the screw-in ventricular lead was located at the right ventricular basal septum. (B) A 12-lead ECG recorded 40 min after the pacemaker implantation demonstrates that the pacemaker was functioning normally with atrial sensing followed by ventricular pacing.
Approximately 3.5 h after the procedure, the patient complained of nausea, and the systolic blood pressure decreased to less than 60 mmHg. Echocardiography revealed a large pericardial effusion with evidence of cardiac tamponade and right atrial and ventricular notching. Emergent pericardiocentesis was performed, yielding 850 mL of blood, and a pericardial drainage catheter was left in place. However, the patient׳s hemodynamic status did not stabilize. Repeat echocardiogram showed a large, nonhomogeneous, echodense mass, consistent with thrombus, in the epicardial space. Cardiac tamponade due to a large thrombus was suspected. She was taken to the operating room to undergo thoracotomy to remove the thrombus and determine its etiology. On arrival to the operating room, sudden cardiac arrest occurred. Cardiopulmonary resuscitation was performed immediately and simultaneous thoracotomy was undertaken. A surgeon performed open chest heart massage and the heart began to beat. After evacuation of 1400 mL of hemopericardium along with several thrombi, bright red blood was seen gushing out from the right coronary artery (Fig. 2). When the surgeon pressed the right coronary artery to control the bleeding, a semi-circle of the atrial lead helix was found to be penetrating the right atrial appendage apex, which was located near the bleeding site (Fig. 3). The screw tip of the atrial lead was protruding 1.8 mm out through the wall of the right atrium. There was no active bleeding from the helix penetration site, and a thorough inspection of the pericardium and heart revealed no other bleeding sites. The right coronary artery perforation was repaired using autologous pericardium-reinforced 7-0 prolene mattress sutures. The tip of the screw on the atrial wall was covered by autologous pericardium to prevent further cardiac injury. The distance between the right coronary artery perforation site and the tip of the lead helix was estimated to be less than 10 mm.
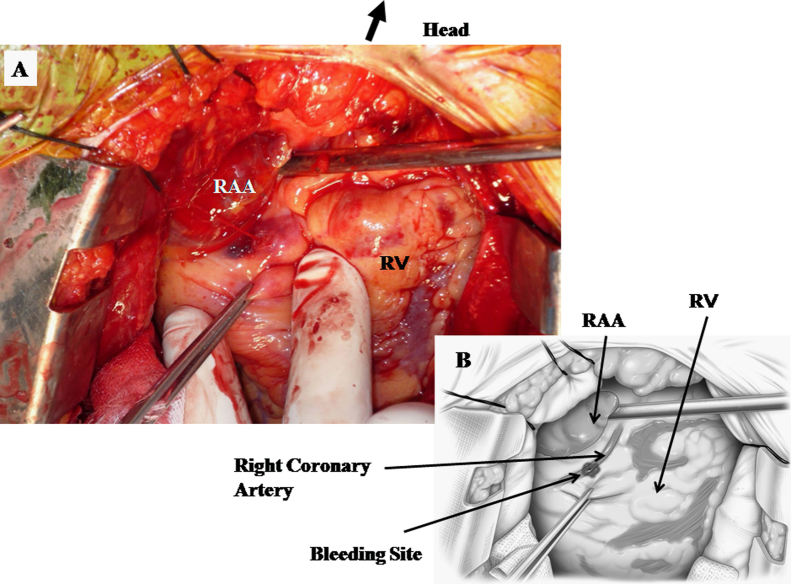
Fig. 2.
(A) Intraoperative image of bleeding from the right coronary artery. After evacuation of 1400 mL of hemopericardium along with several thrombi, we determined that bright red blood was gushing out from the right coronary artery, which was located on the opposite side of the right atrial appendage to the atrial lead screw. (B) Intraoperative drawing corresponding to (A). Bleeding site and right coronary artery are drawn illustrated. RV, right ventricle; RAA, right atrial appendage.
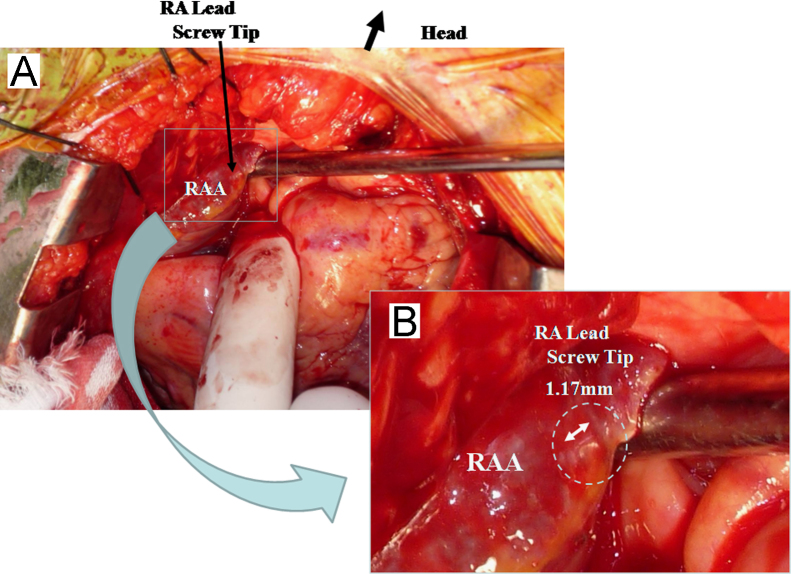
Fig. 3.
(A) Intraoperative image showing the atrial lead screw penetrating the right atrial appendage, which was located on the opposite side from the bleeding site. There was no bleeding from the screw tip penetration site. (B) The magnification of (A) is shown. A semi-circular portion of the screw penetrated the atrial wall. The diameter of the screw was 1.17 mm. RAA, right atrial appendage; RA right atrium.
The patient remained hemodynamically stable postoperatively. Two days later, the pacemaker was functioning well with pacing and sensing thresholds of the atrial lead similar to those at the time of implantation. Cardiac tamponade did not recur thereafter.
3. Discussion
The major finding in this case is that implantation of an active-fixation atrial pacing lead in the right atrial appendage caused right coronary artery perforation, resulting in life-threatening tamponade. Myocardial perforation with or without cardiac tamponade has been reported as a relatively rare complication associated with the pacemaker implantation procedure [1–10]. It is also known that active-fixation atrial leads are associated with more frequent complications compared to passive-fixation atrial leads and have been reported to cause rare complications such as pneumothorax and aortic perforation [11–13]. To the best of our knowledge, our case is the first in which the implantation of an active-fixation atrial pacing lead caused right coronary artery perforation.
The determination of the etiology of device implantation-related cardiac tamponade is often difficult. We checked the movement of the cardiac silhouette on cinefluoroscopy in a 30° left anterior oblique view in the electrophysiology laboratory at the end of the procedure and confirmed the absence of pericardial effusion and cardiac tamponade. A very small portion of the screw tip penetrated the atrial wall of the right atrial appendage in our case, but there was no bleeding from this site during open chest surgery. However, bleeding was observed from the right coronary artery, which was located on the opposite site of the right atrial appendage. These findings suggested that the screw tip of the atrial lead penetrated the atrial wall during or after the implantation and scored the right coronary artery due to the motion of the heart 3.5 h after the procedure, resulting in life-threatening cardiac tamponade refractory to intensive treatment including pericardial drainage. Perforation of the right coronary artery is a possible novel mechanism of cardiac tamponade caused by an active-fixation atrial pacing lead.
Because complications associated with active-fixation atrial leads are related to implantation sites, such as pericardial effusion in patients with the atrial lead implanted in the right atrial free wall and aortic perforation in patients with the implantation site of the mid to high atrial septum [13], the low atrial septum might be a suitable site for active-fixation atrial leads in patients without persistent fossa ovale because of the low associated complication rate [14]. The right coronary artery is partially covered by the right atrial appendage and Pang et al. reported the close proximity of the atrial lead tip to the right coronary artery when positioned in the medial right atrial appendage [15]. In addition to the atrial lead implantation site in the right atrial appendage, the motion of the right atrial appendage has to be taken into account because in this case, the right coronary artery was injured by the atrial lead tip approximately 10 mm away at the appendage apex. The right atrial appendage might be a suitable implantation site only for passive-fixation atrial leads, but not for active-fixation atrial leads, because of the risk of screw penetration and sequential collateral organ damage.
4. Conclusions
In the present case report, we show that perforation of the right coronary artery could be one of the differential diagnoses of cardiac tamponade after active-fixation atrial lead implantation.
Conflict of interest
No conflict of interest declared.
References
- 1.Green T.O., Portnow A.S., Huang S.K. Acute pericarditis resulting from an endocardial active fixation screw-in atrial lead. Pacing Clin Electrophysiol. 1994;17:21–25. doi: 10.1111/j.1540-8159.1994.tb01346.x. [DOI] [PubMed] [Google Scholar]
- 2.Trigano A.J., Taramasco V., Paganelli F. Incidence of perforation and other mechanical complications during dual active fixation. Pacing Clin Electrophysiol. 1996;19:1828–1831. doi: 10.1111/j.1540-8159.1996.tb03234.x. [DOI] [PubMed] [Google Scholar]
- 3.Kindermann M., Schwaab B., Frohlig G. Bipolar active fixation atrial leads: comparison of two new lead models. Pacing Clin Electrophysiol. 1998;21:2285–2290. doi: 10.1111/j.1540-8159.1998.tb01168.x. [DOI] [PubMed] [Google Scholar]
- 4.Aizawa K., Kaneko Y., Yamagishi T. Oozing from the pericardium as an etiology of cardiac tamponade associated with screw-in atrial leads. Pacing Clin Electrophysiol. 2001;24:381–383. doi: 10.1046/j.1460-9592.2001.00381.x. [DOI] [PubMed] [Google Scholar]
- 5.Ellenbogen K.A., Wood M.A., Shepard R.K. Delayed complications following pacemaker implantation. Pacing Clin Electrophysiol. 2002;25:1155–1158. doi: 10.1046/j.1460-9592.2002.01155.x. [DOI] [PubMed] [Google Scholar]
- 6.Sivakumaran S., Irwin M.E., Gulamhusein S.S. Postpacemaker implant pericarditis: incidence and outcomes with active-fixation leads. Pacing Clin Electrophysiol. 2002;25:833–837. doi: 10.1046/j.1460-9592.2002.t01-1-00833.x. [DOI] [PubMed] [Google Scholar]
- 7.Khan M.N., Joseph G., Khaykin Y. Delayed lead perforation: a disturbing trend. Pacing Clin Electrophysiol. 2005;28:251–253. doi: 10.1111/j.1540-8159.2005.40003.x. [DOI] [PubMed] [Google Scholar]
- 8.Spindler M., Burrows G., Kowallik P. Postpericardiotomy syndrome and cardiac tamponade as a late complication after pacemaker implantation. Pacing Clin Electrophysiol. 2001;24:1433–1434. doi: 10.1046/j.1460-9592.2001.01433.x. [DOI] [PubMed] [Google Scholar]
- 9.Geyfman V., Storm R.H., Lico S.C. Cardiac tamponade as complication of active-fixation atrial lead perforations: proposed mechanism and management algorithm. Pacing Clin Electrophysiol. 2007;30:498–501. doi: 10.1111/j.1540-8159.2007.00699.x. [DOI] [PubMed] [Google Scholar]
- 10.Piekarz J., Lelakowski J., Rydlewska A. Heart perforation in patients with permanent cardiac pacing – pilot personal observations. Arch Med Sci. 2012;8:70–74. doi: 10.5114/aoms.2012.27284. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Oginosawa Y., Haruhiko A., Nakashima Y. Right pneumothorax resulting from an endocardial screw-in atrial lead in an implantable cardioverter defibrillator system. Pacing Clin Electrophysiol. 2002;25:1278–1279. doi: 10.1046/j.1460-9592.2002.01278.x. [DOI] [PubMed] [Google Scholar]
- 12.Ho W.J., Kuo C.T., Lin K.H. Right pneumothorax resulting from an endocardial screw-in atrial lead. Chest. 1999;116:1133–1134. doi: 10.1378/chest.116.4.1133. [DOI] [PubMed] [Google Scholar]
- 13.Kashani A., Mehdirad A., Fredman C. Aortic perforation by active-fixation atrial pacing lead. Pacing Clin Electrophysiol. 2004;27:417–418. doi: 10.1111/j.1540-8159.2004.00456.x. [DOI] [PubMed] [Google Scholar]
- 14.Lau C.P., Tachapong N., Wang C.C. Prospective randomized study to assess the efficacy of site and rate of atrial pacing on long-term progression of atrial fibrillation in sick sinus syndrome: septal Pacing for Atrial Fibrillation Suppression Evaluation (SAFE) Study. Circulation. 2013;128:687–693. doi: 10.1161/CIRCULATIONAHA.113.001644. [DOI] [PubMed] [Google Scholar]
- 15.Pang B.J., Joshi S.B., Lui E.H. Proximity of pacemaker and implantable cardioverter-defibrillator leads to coronary arteries as assessed by cardiac computed tomography. Pacing Clin Electrophysiol. 2014;37:717–723. doi: 10.1111/pace.12330. [DOI] [PubMed] [Google Scholar]