Abstract
Intraoperative ultrasonography (IOUS) has been widely utilized in hepatic surgery both as a diagnostic technique and in the course of treatment. Since IOUS involves direct-contact imaging of the target organ, it can provide high spatial resolution without interference from the surrounding structures. Therefore, IOUS may improve the detection, characterization, localization, and local staging of hepatic tumors. IOUS is also a real-time imaging modality capable of providing interactive information and valuable guidance in a range of procedures. Recently, contrast-enhanced IOUS, IOUS elastography, and IOUS-guided hepatic surgery have attracted increasing interest and are expected to lead to the broader implementation of IOUS. Herein, we review the various applications of IOUS in the diagnosis and management of focal hepatic lesions.
Keywords: Liver neoplasms, Intraoperative care, Ultrasonography
Introduction
Intraoperative ultrasonography (IOUS) is considered to be one of the most sensitive imaging modalities for assessing small focal lesions in the liver, and can affect the choice of surgical strategy and lead to greater oncological radicality [1-3].
During hepatic surgery, IOUS is usually performed after partial hepatic mobilization with incision of ligaments as occasion demands. Hepatic mobilization is important to ensure that the lesion is accessible and that the liver is scanned to a satisfactory extent [4], although hepatic mobilization can substantially distort the hepatic anatomy, which can make it difficult for inexperienced radiologists to correctly perceive the relative anatomy. In general, IOUS of the liver is performed by placing the ultrasound probe directly on the surface of the liver, meaning that there is no risk of image quality degradation due to overlying structures such as subcutaneous fat, bowel gas, or the ribs. Thus, unlike in routine transabdominal ultrasonography, ultrasound probes with relatively high frequencies (5-10 MHz) can be used in IOUS [4,5]. Moreover, dedicated transducers, such as I-shaped or flat T-shaped linear probes, are preferred to conventional linear probes in IOUS, because they can easily be inserted into deep regions, allowing nearly the entire liver to be scanned, including the hepatic dome and the right lateral portion [6]. However, convex probes with lower frequencies are also useful in IOUS, because they provide an overall view of the liver along with comprehensive information about the relationship between hepatic focal lesions and other structures, such as major vessels and adjacent organs [7]. Therefore, depending on the primary indications for IOUS, it is necessary to choose different types of probes or combinations thereof in IOUS. For example, when evaluating whether additional hepatic focal lesions are present that were not found in preoperative imaging studies, it may be appropriate to begin exploring the liver with a convex probe that has a lower frequency, because the overall visibility of the liver is essential. When localizing preoperatively detected hepatic focal lesions with IOUS, anatomical shift during surgery may make it difficult to find the target lesion. In order to identify the target lesion, it can be helpful to use a lower-frequency probe to explore a wide scanning area, including anatomical landmarks such as the hepatic vessels and/or non-target lesions that are close to the target lesion and easy to find, such as cysts. After identifying the target lesion, it may be useful to change to a linear probe with higher frequency, which provides a high spatial resolution that allows the detailed characterization of the lesion.
Furthermore, IOUS provides real-time imaging capabilities, and thus, under IOUS guidance, it is possible to perform intraoperative diagnostic and therapeutic procedures for focal hepatic lesions [4]. For example, if IOUS identifies a questionable hepatic lesion, a timely confirmative diagnosis is sometimes necessary to assess the resectability of the extrahepatic malignancy and to determine the extent of hepatic resection, which can be accomplished using IOUS-guided biopsy [6,8]. IOUS-guided therapeutic procedures for liver tumors include ethanol ablation, radiofrequency ablation (RFA), and microwave ablation (MWA). Previous studies have shown that a combination of IOUS-guided tumor ablation with hepatic resection can, in fact, extend the limits of hepatic surgery [9-11]. In this article, we examine the current role of IOUS in the field of hepatic surgery and review the clinical applications of IOUS in the diagnosis and management of focal hepatic lesions.
Clinical Applications of IOUS for Focal Hepatic Lesions
IOUS is useful during hepatic surgery for primary or secondary malignancies because it facilitates the improved detection and characterization of tumors and can be used to localize the target lesion and guide intraoperative procedures [12-14]. The role of IOUS has been evaluated most intensively in patients with colorectal liver metastases (CRLM) and hepatocellular carcinoma (HCC), in comparison to other types of liver lesions. This is because these disease entities are common hepatic malignancies that can be candidates for liver resection, and the intraoperative detection and local treatment of these lesions can have a major impact on the choice of surgical strategy [15,16].
Liver metastases are common in patients with colorectal cancer at the time of diagnosis and/or after resection of the primary cancer [17]. However, unlike hepatic metastases of many other types of cancers, the presence of CRLM does not preclude curative treatment in patients with colorectal cancer [18]. In the treatment of CRLM, the surgical resection of all macroscopically visible disease remains the gold standard and has been shown to result in improved longterm survival [18]. In addition, local tumor ablation alone or ablation combined with surgical resection has been demonstrated to achieve local tumor control even in patients with unresectable disease [19]. Therefore, the intraoperative detection and/or localization of CRLM using IOUS can play a crucial role during hepatic surgery (Fig. 1) [15]. Furthermore, recent chemotherapy regimens have been reported to have the potential to control CRLM and to make some cases of advanced CRLM resectable [17]. Another issue of note is the disappearance of CRLM after chemotherapy, as shown by a complete response on preoperative imaging. In a recent study, 66% of cases where CRLM disappeared on preoperative imaging were reported to represent a true complete response [20]. However, put another way, this figure suggests that residual disease may be present in 34% of cases where liver metastases have disappeared on preoperative imaging. For this reason, the intraoperative detection of lesions that were not found on preoperative imaging may help determine the most appropriate surgical strategy. Ferrero et al. [21] have reported that in patients with CRLM who showed a complete response on preoperative imaging, the majority of hepatic lesions that were detected with IOUS were pathologically found to represent residual disease, suggesting that lesions identified on IOUS should be treated. They also demonstrated that the nonvisualization of disappearing CRLM on IOUS was associated with pathologic complete response [21].
Fig. 1. A 48-year-old female with colon cancer liver metastases after preoperative chemotherapy.
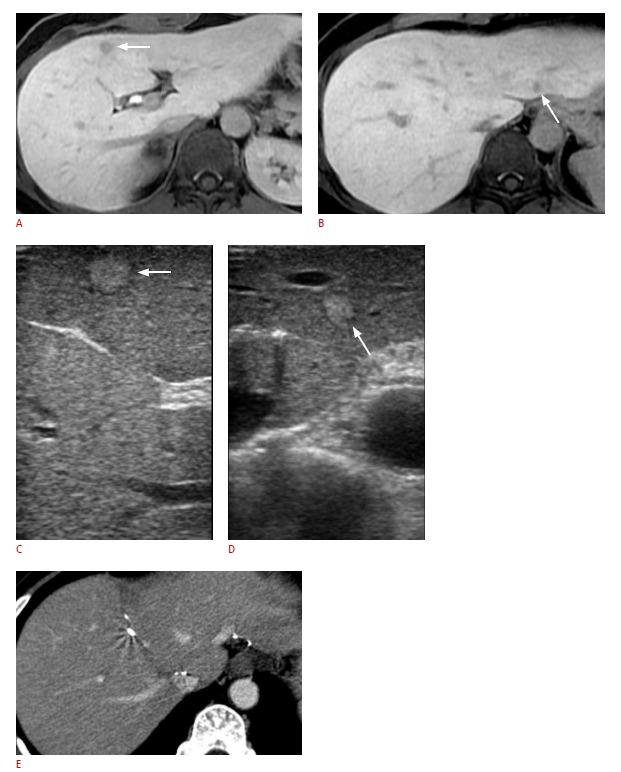
A, B. The hepatobiliary phase of gadoxetic acid-enhanced magnetic resonance (MR) images show subcentimeter hypointense lesions (arrows) in segment IV (A) and segment II (B). C, D. Non-palpable liver metastases detected on the preoperative MR image are identified as hyperechoic nodules (C, segment IV; D, segment II; arrows) on gray-scale intraoperative ultrasonography using a 7.5-MHz linear probe. E. Follow-up computed tomography after tumorectomy shows that the liver metastases were successfully resected.
HCC, which is the most common type of primary liver malignancy, is frequently associated with cirrhosis [22,23]. During surgical resection which is the standard treatment option for HCC, in addition to achieving oncological radicality, attention should be also paid to preserve the liver parenchyma, because liver function in patients with cirrhosis is usually impaired and remnant liver volume is an important prognostic factor after resection [24-26]. Hepatic tumorectomy or local tumor ablation under IOUS localization and guidance can be performed in order to minimize the volume of the liver parenchyma removed, while still achieving oncological radicality. However, in cirrhotic livers, benign or borderline hepatocellular nodules associated with cirrhosis are common, and are difficult to differentiate from HCC using gray-scale IOUS [27-29]. Contrast-enhanced IOUS (CE-IOUS) can be of use in the differential diagnosis of indeterminate nodules of this type and may help improve the detection rate of small HCCs [28-30].
IOUS: Rival or Teammate of Preoperative Imaging?
Due to its high spatial resolution, IOUS is commonly regarded as the gold standard for the staging of liver tumors [13,14]. Previous studies have also suggested that IOUS is superior to preoperative imaging modalities in identifying hepatic lesions in patients with primary or metastatic hepatic tumors [9,31]. Furthermore, the detection of additional hepatic lesions has been observed to lead to changes in the surgical strategy in a widely varying range of cases (2.7%-49%) [1,32,33]. Conlon et al. [33] reported that in patients with hepatic metastases from colorectal cancer, IOUS identified additional hepatic lesions in 47% of patients compared to preoperative magnetic resonance imaging (MRI). In another study, D’Onofrio et al. [9] compared the diagnostic performance of IOUS in patients from two different time periods (2000-2003 vs. 2004-2006), and demonstrated that IOUS was still useful in detecting unexpected hepatic metastases, despite improvements in preoperative imaging. In addition, several recent studies have demonstrated that IOUS is still superior to preoperative imaging in detecting CRLM, and that IOUS findings can have a substantial impact on the choice of surgical strategy [3,34,35]. Based on these results, it has been suggested that IOUS should be routinely employed during hepatic resection for colorectal metastases.
However, further questions about the role of IOUS have recently emerged. Due to technical advances in imaging modalities and the development of new contrast media, the preoperative detection of focal hepatic lesions has improved, even for subcentimeter lesions [36-41]. Thus, the value of IOUS in detecting unexpected focal hepatic lesions has decreased, as indicated by the results of several recent studies. For instance, Wagnetz et al. [32] reported that the sensitivities of multidetector computed tomography and MRI were equivalent or higher to that of IOUS in the identification of hepatic segments involved in hepatic malignancies, as well as having a higher predictive value for identifying tumor-free hepatic segments. Sahani et al. [42] also found MRI to be as sensitive as IOUS in the detection of focal hepatic lesions in patients with primary or metastatic liver tumors. Moreover, Kartalis et al. [43] reported that the performance of CE-IOUS in detecting tumors in patients with CRLM was no better than that of preoperative MRI.
Nevertheless, in certain aspects, IOUS is not an outdated imaging modality of diminishing significance, but an emerging tool of increasing importance. While the ability of IOUS to provide high spatial resolution has been largely obviated by recent advances in preoperative imaging, IOUS has a unique ability to provide real-time interactive information [4]. In fact, since preoperative imaging is able to detect an increasing number of focal hepatic lesions, the need for lesion localization is correspondingly greater, especially for lesions that are not palpable in the surgical field (Fig. 1) [37,39]. Furthermore, local treatment is increasingly necessary for focal hepatic lesions that are difficult to include in surgical resection procedures due to the distribution of the lesions or the impaired liver function of patients (Fig. 2) [44,45]. Technical advances in imaging techniques that fuse different imaging modalities enable the information from preoperative imaging studies and IOUS to be combined, which may overcome the disadvantages of each modality. Therefore, the role of IOUS in combination with preoperative imaging for tumor localization and treatment may be even greater than ever before.
Fig. 2. A 63-year-old female with Budd-Chiari syndrome and hepatocellular carcinoma (HCC) previously treated with transarterial embolization.
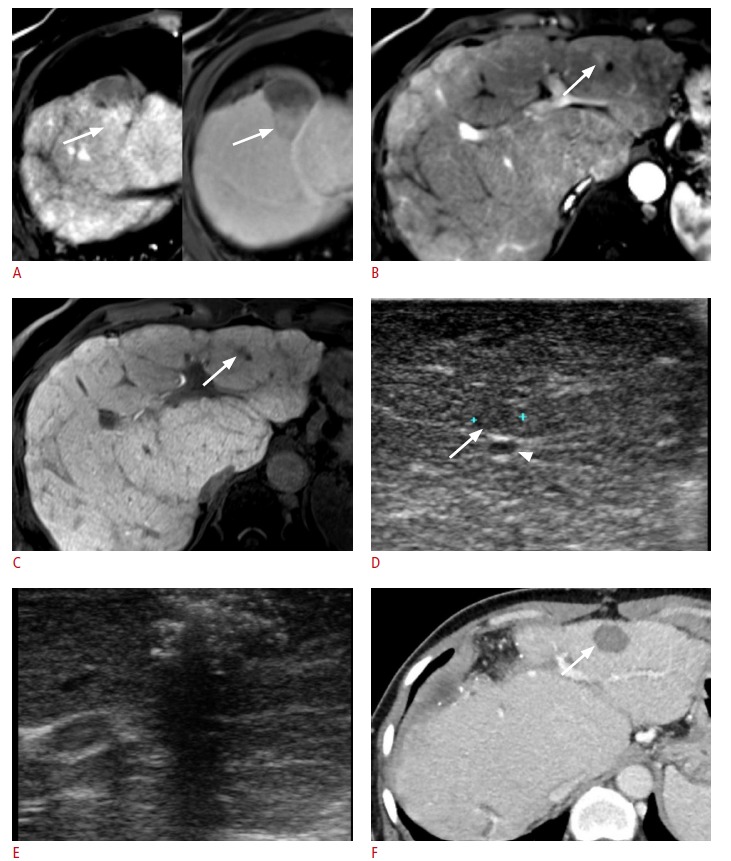
A. The arterial (left) and portal (right) phases of contrast-enhanced dynamic magnetic resonance images show the local tumor progression of HCC (arrows) in segment IV of the liver. Surgical resection was planned to treat this tumor. B, C. Preoperative magnetic resonance images show another tiny lesion (arrows) highly suspicious for HCC in segment III of the liver as a hypervascular nodule on arterial-phase imaging (B), and as hypointensity on hepatobiliary-phase imaging (C). D. Intraoperative ultrasonography (IOUS) shows the lesion in segment III near the left hepatic vein (arrowhead) as an isoechoic nodule (arrow). E. Intraoperative radiofrequency ablation was performed for the hepatic nodule with IOUS guidance. F. Follow-up computed tomography shows complete tumor ablation (arrow).
Contrast-Enhanced IOUS
Contrast-enhanced ultrasonography (CEUS) has been reported to increase both the sensitivity and specificity of the detection of focal hepatic lesions and to provide additional information that allows the better characterization of lesions compared to conventional gray-scale ultrasonography [46,47]. Second-generation contrast agents, such as SonoVue (Bracco, Milano, Italy) or Sonazoid (GE Healthcare, Oslo, Norway), are commonly used for the CEUS evaluation of focal hepatic lesions. Using these microbubble contrast agents, it is possible to obtain high lesion-to-liver contrast as well as real-time vascular phase images [48]. Since ultrasound contrast agents are pure intravascular contrast agents, the equilibrium phase of contrast-enhanced computed tomography (CT) or MRI does not exist on CEUS [46]. However, Sonazoid (perflubutane microbubble) allows the postvascular phase imaging (Kupffer-phase imaging) because this contrast agent is later taken up by Kupffer cells in the liver [49,50]. Furthermore, the long duration of the Kupffer phase of Sonazoid-enhanced CEUS allows enough time to investigate the liver precisely [51]. The intraoperative implementation of CEUS (CE-IOUS) is expected to result in improved diagnostic performance for hepatic lesions by combining the advantages of IOUS and CEUS [16,52]. CE-IOUS may provide superior detection and characterization of tiny hepatic lesions compared to gray-scale IOUS and preoperative imaging modalities (Fig. 3), and therefore may increase the accuracy of tumor staging and the frequency of treatments with curative intent by affecting the extent of surgery or by facilitating additional local treatment [16,52,53].
Fig. 3. A 70-year-old male with hepatocellular carcinoma (HCC).
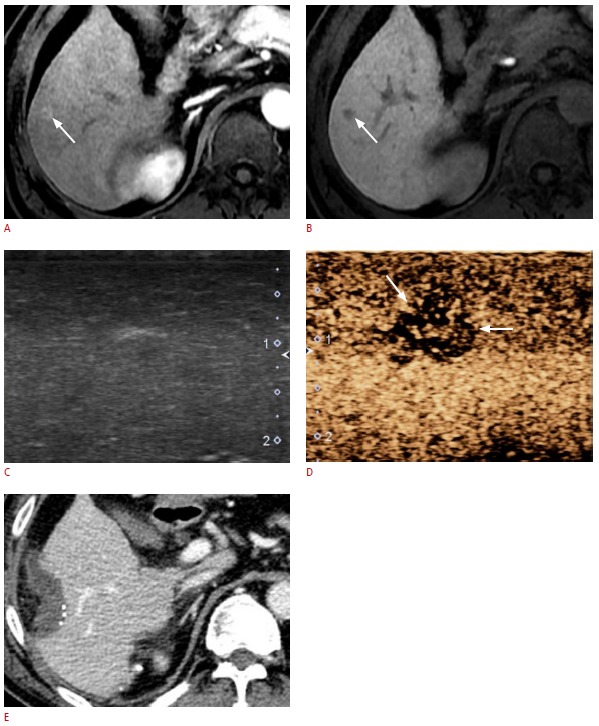
A, B. A preoperative magnetic resonance image shows a 0.8-cm nodule (arrows) in segment VI of the liver as a hyperenhancement on the hepatic arterial phase (A), and as hypointensity on the hepatobiliary phase (B). C, D. Gray-scale intraoperative ultrasonography (IOUS) (C) was not able to find the non-palpable hepatic nodule detected on preoperative magnetic resonance imaging. However, in the Kupffer-phase images of contrast-enhanced IOUS using Sonazoid (D, same scanning plane as C), the nodule (arrows) is clearly distinguished from the background parenchyma as an area of hypoechogenicity. This lesion was pathologically confirmed as HCC. E. Immediate follow-up computed tomography shows that the tumorectomy was successful.
The timely detection and differential diagnosis of CRLM is crucial for determining the extent of surgery, treatment planning, and the prediction of the patient’s prognosis [54]. The use of contrast agents can improve the diagnostic performance of IOUS [15,55,56], which is already regarded as one of the most sensitive tools for detecting CRLM [57]. Recent studies have demonstrated that the use of CE-IOUS in patients with CRLM may have an impact on surgical staging and management, as CE-IOUS can alter diagnoses initially made with gray-scale IOUS and identify additional lesions [15,55,56]. CE-IOUS may be a useful method for detecting lesions in cases of liver metastases that seem to disappear after chemotherapy, and therefore may lead to curative treatment [58-60]. A previous study by Arita et al. [60] reported that among 32 liver metastases that seemed to disappear after chemotherapy on preoperative imaging, 28 lesions were also invisible by gray-scale IOUS, while CE-IOUS using Sonazoid additionally detected 12 lesions including 11 cases of histologically confirmed residual metastasis.
CE-IOUS is also a useful diagnostic tool during the surgical treatment of HCCs in cirrhotic livers [16]. CE-IOUS can, in fact, improve the accuracy of gray-scale IOUS, because CE-IOUS can detect isoechoic HCC nodules which cannot be shown on gray-scale IOUS, as well as improving the characterization of cirrhotic nodules detected on gray-scale IOUS by obtaining dynamic contrast-enhanced images and by obtaining Kupffer-phase imaging when using Sonazoid [28,29]. Lu et al. [28] reported that CE-IOUS changed the surgical strategy in 35% of cirrhotic patients with HCC and helped avoid unnecessary treatment in 30% of patients in comparison to the results of gray-scale IOUS. In addition, Torzilli et al. [30] demonstrated that vascular enhancement patterns on CE-IOUS may assist in determining the surgical resection of IOUS-detected nodules. In another study using Sonazoid-enhanced IOUS for the differential diagnosis of HCC versus benign lesions, CE-IOUS findings of hypervascularity during the vascular phase or hypoechogenicity during the Kupffer phase were reported to show a higher accuracy than dynamic CT findings of arterial enhancement and washout during the later phases [29]. In addition, vascular-phase and Kupffer-phase imaging using Sonazoid-enhanced IOUS has been suggested to be useful in estimating the histologic grade of HCC [61]. Moreover, Sato et al. [62] demonstrated that the vasculature patterns of HCCs on CE-IOUS were related to gene expression profiles, suggesting that CE-IOUS findings can be a useful indicator for predicting the prognosis of patients.
IOUS-Guided Procedures
IOUS is a useful guidance tool in intraoperative diagnostic and therapeutic procedures [4]. Since IOUS provides excellent spatial resolution with a good sonic window and intraoperative procedures can be performed from various planes and angles that may shift over the course of an operation, IOUS guidance has clear advantages over transabdominal imaging guidance procedures with regard to accessibility, especially in procedures involving deeply located lesions or lesions hidden by overlying structures [5,63,64].
IOUS-guided biopsy has been reported to show high diagnostic accuracy and is considered a safe procedure [8,65]. During hepatic surgery for primary or secondary malignancies, IOUS provides gray-scale and/or contrast-enhanced images that can identify additional but indeterminate focal hepatic lesions. Confirmation of these hepatic lesions is sometimes required because the pathologic diagnosis of hepatic lesions can affect the resectability of extrahepatic malignancies such as pancreatic adenocarcinoma, as well as influence the extent of hepatic resection [2,6,15,52]. In addition, as we discussed earlier, recent advances in preoperative imaging have led to substantial improvements in the detection of subcentimeter liver lesions. In some cases, these lesions can be pathologically confirmed prior to surgery or intraoperatively, which may affect treatment planning [37,39]. In cases of intraoperatively or preoperatively found but unconfirmed focal hepatic lesions with the potential to affect the choice of surgical strategy, a tissue sample of the indeterminate hepatic lesions can be obtained in the operating room using IOUS-guided core-needle biopsy or fine needle aspiration. Thereafter, a timely confirmative diagnosis can be made through histopathological examination [2].
Intraoperative ethanol injection, RFA, and MWA by open surgical or laparoscopic approaches are frequently used for the local treatment of hepatic tumors [9-11]. These local therapies employ a range of basic mechanisms. In ethanol injection, the high concentration of ethanol causes dehydration and coagulation necrosis of the tumor [66]. In RFA, the thermal energy generated by high-frequency alternating currents induces coagulation necrosis [67], and in MWA, thermal energy causes coagulation necrosis similarly to RFA, although MWA uses a different part of the electromagnetic spectrum [68]. Local treatment methods can be applied even in patients who are not candidates for surgical resection of hepatic malignancies due to the number or location of tumors, because their postresection liver would have a relatively small volume, or due to coexisting liver dysfunction such as cirrhosis or chemotherapy-related liver dysfunction [44,45]. In addition, local ablation therapy for HCC may be an effective bridge in patients awaiting liver transplantation [69]. These treatments are performed under imaging guidance, most frequently using either percutaneous ultrasonography or IOUS. While percutaneous tumor ablation has advantages including being less invasive, involving less postprocedure pain, and resulting in a shorter hospital stay, intraoperative ablation has advantages over percutaneous procedures because it allows better accessibility to all areas of the liver [64,70]. Therefore, laparoscopic or open surgical ablation can be an alternative treatment for liver tumors in locations that pose difficulties for the percutaneous approach, such as the caudate lobe [63,71,72]. Furthermore, intraoperative tumor ablation can be combined with simultaneous hepatic resection (Fig. 2) or the sequential ablation of tumors that recur after surgery, which extends the spectrum of liver surgery and improves oncological radicality [73-75]. In the majority of intraoperative therapeutic procedures of this type, IOUS is utilized as a guidance tool to localize the target lesion, to help avoid injuries to vessels, bile ducts, and adjacent organs, and to assess treatment efficacy and complications [70]. Previous studies have demonstrated that IOUS-guided ablation is a relatively safe, well-tolerated, and effective treatment option that can offer excellent local control of primary and metastatic liver tumors [19,70,76-78]. Recent studies have also reported that intraoperative RFA showed a local recurrence rate equivalent to surgical resection both in small size HCCs [72,79] and CRLM [19,76], and that the outcomes of intraoperative MWA were comparable to those of intraoperative RFA for HCC treatment [80].
Emerging Applications of IOUS
Ultrasound elastography, which is a noninvasive method of estimating the elastic properties of tissue, can be useful in characterizing liver tumors [81-83]. Several recent studies have evaluated the role of intraoperative real-time ultrasound elastography in the detection and characterization of focal hepatic lesions [84-86]. Omichi et al. [84] reported that IOUS elastography detected additional lesions in 8% of cases with an obscure contour on gray-scale IOUS. The elasticity type of liver tumor, which is used to classify tumors according to the degree of strain of a tissue in comparison with the surrounding liver parenchyma, varies corresponding to the pathologic diagnosis [85] and has been reported to be helpful in distinguishing malignant tumors from benign tumors [84] and HCCs from metastatic adenocarcinomas [86]. Furthermore, IOUS elastography can be a valuable tool in monitoring local ablation treatment, because IOUS elastography provides real-time visualization of changes in tissue properties [87]. After the local ablation of liver tumors, IOUS elastography can provide an accurate gross estimation of the ablation zone by providing a more conspicuous boundary than can be obtained with gray-scale IOUS, thereby potentially improving the efficacy and safety of the procedure [88,89].
At present, virtual hepatic resection is increasingly performed preoperatively to ensure that an appropriate safety margin and the preservation of a sufficient amount of liver tissue are achieved, particularly in complicated operations or in patients with hepatic dysfunction [90]. Although preoperative CT or MRI imaging can provide excellent anatomical detail, which is important in virtual hepatic resection, performing liver surgery with intraoperative imaging guidance is nonetheless preferable, due to the deformation of the liver in patients in the operating room compared with preoperative imaging data [91]. IOUS or IOUS combined with preoperative imaging can be used to address this issue [92,93]. The feasibility and usefulness of IOUS-guided resection in patients with hepatic tumors has been demonstrated in several studies [92,94]. By offering multiplanar imaging and the simultaneous localization of ultrasound data and surgical instruments, the usage of threedimensional IOUS to guide hepatic resection has been reported to improve intraoperative orientation, allowing more accurate resection [92,95]. Finally, the combination of preoperative CT or MRI and IOUS guidance can provide updated information about anatomical shifts during surgery, which may improve the precision and safety of the procedure [93].
Conclusion
IOUS has clear strengths in the diagnosis and treatment of focal hepatic lesions compared to preoperative imaging modalities, due to its high spatial resolution and the fact that it offers real-time imaging. Although the role of IOUS in tumor detection has been reduced due to recent advances in preoperative imaging techniques, IOUS plays an increasingly important role in the intraoperative localization and characterization of lesions detected on preoperative imaging and in guiding diagnostic or therapeutic procedures. In addition, CE-IOUS may further help improve the detection and characterization of tiny hepatic lesions by providing high lesion-to-liver contrast and dynamic contrast-enhanced images with or without Kupffer-phase imaging. Furthermore, IOUS-guided local tumor ablation has advantages over the percutaneous approach, because IOUS allows better lesion accessibility and can be combined with simultaneous hepatic resection. Emerging applications of IOUS currently include the evaluation of focal hepatic lesions through elastography and IOUS-guided hepatic resection. Understanding the current role of IOUS and applying it appropriately for diagnostic or therapeutic purposes in patients with focal hepatic lesions contributes to improved patient outcomes.
Footnotes
No potential conflict of interest relevant to this article was reported.
References
- 1.Parker GA, Lawrence W, Jr, Horsley JS, 3rd, Neifeld JP, Cook D, Walsh J, et al. Intraoperative ultrasound of the liver affects operative decision making. Ann Surg. 1989;209:569–576. doi: 10.1097/00000658-198905000-00009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Marcal LP, Patnana M, Bhosale P, Bedi DG. Intraoperative abdominal ultrasound in oncologic imaging. World J Radiol. 2013;5:51–60. doi: 10.4329/wjr.v5.i3.51. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Sietses C, Meijerink MR, Meijer S, van den Tol MP. The impact of intraoperative ultrasonography on the surgical treatment of patients with colorectal liver metastases. Surg Endosc. 2010;24:1917–1922. doi: 10.1007/s00464-009-0874-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Kruskal JB, Kane RA. Intraoperative US of the liver: techniques and clinical applications. Radiographics. 2006;26:1067–1084. doi: 10.1148/rg.264055120. [DOI] [PubMed] [Google Scholar]
- 5.Silas AM, Kruskal JB, Kane RA. Intraoperative ultrasound. Radiol Clin North Am. 2001;39:429–448. doi: 10.1016/s0033-8389(05)70290-6. [DOI] [PubMed] [Google Scholar]
- 6.D'Onofrio M, Vecchiato F, Faccioli N, Falconi M, Pozzi Mucelli R. Ultrasonography of the pancreas. 7. Intraoperative imaging. Abdom Imaging. 2007;32:200–206. doi: 10.1007/s00261-006-9018-y. [DOI] [PubMed] [Google Scholar]
- 7.Donadon M, Costa G, Torzilli G. State of the art of intraoperative ultrasound in liver surgery: current use for staging and resection guidance. Ultraschall Med. 2014;35:500–511. doi: 10.1055/s-0034-1385515. [DOI] [PubMed] [Google Scholar]
- 8.Charnley RM, Sheffield JP, Hardcastle JD. Evaluation of a biopsy gun for guided biopsy of impalpable liver lesions using intraoperative ultrasound. HPB Surg. 1990;2:265–267. doi: 10.1155/1990/56823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.D'Onofrio M, Gallotti A, Martone E, Nicoli L, Mautone S, Ruzzenente A, et al. Is intraoperative ultrasound (IOUS) still useful for the detection of liver metastases? J Ultrasound. 2009;12:144–147. doi: 10.1016/j.jus.2009.09.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Gaitini D, Kopelman D, Soudak M, Epelman M, Assalia A, Hashmonai M, et al. Impact of intraoperative sonography on resection and cryoablation of liver tumors. J Clin Ultrasound. 2001;29:265–272. doi: 10.1002/jcu.1032. [DOI] [PubMed] [Google Scholar]
- 11.Kane RA. Intraoperative ultrasonography: history, current state of the art, and future directions. J Ultrasound Med. 2004;23:1407–1420. doi: 10.7863/jum.2004.23.11.1407. [DOI] [PubMed] [Google Scholar]
- 12.Nanashima A, Tobinaga S, Abo T, Kunizaki M, Takeshita H, Hidaka S, et al. Usefulness of sonazoid-ultrasonography during hepatectomy in patients with liver tumors: a preliminary study. J Surg Oncol. 2011;103:152–157. doi: 10.1002/jso.21782. [DOI] [PubMed] [Google Scholar]
- 13.Kane RA, Hughes LA, Cua EJ, Steele GD, Jenkins RL, Cady B. The impact of intraoperative ultrasonography on surgery for liver neoplasms. J Ultrasound Med. 1994;13:1–6. doi: 10.7863/jum.1994.13.1.1. [DOI] [PubMed] [Google Scholar]
- 14.Zacherl J, Scheuba C, Imhof M, Zacherl M, Langle F, Pokieser P, et al. Current value of intraoperative sonography during surgery for hepatic neoplasms. World J Surg. 2002;26:550–554. doi: 10.1007/s00268-001-0266-2. [DOI] [PubMed] [Google Scholar]
- 15.Schulz A, Dormagen JB, Drolsum A, Bjornbeth BA, Labori KJ, Klow NE. Impact of contrast-enhanced intraoperative ultrasound on operation strategy in case of colorectal liver metastasis. Acta Radiol. 2012;53:1081–1087. doi: 10.1258/ar.2012.120049. [DOI] [PubMed] [Google Scholar]
- 16.Torzilli G, Olivari N, Moroni E, Del Fabbro D, Gambetti A, Leoni P, et al. Contrast-enhanced intraoperative ultrasonography in surgery for hepatocellular carcinoma in cirrhosis. Liver Transpl. 2004;10(2 Suppl 1):S34–S38. doi: 10.1002/lt.20050. [DOI] [PubMed] [Google Scholar]
- 17.Garden OJ, Rees M, Poston GJ, Mirza D, Saunders M, Ledermann J, et al. Guidelines for resection of colorectal cancer liver metastases. Gut. 2006;55 Suppl 3:iii1–iii8. doi: 10.1136/gut.2006.098053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Penna C, Nordlinger B. Surgery of liver metastases from colorectal cancer: new promises. Br Med Bull. 2002;64:127–140. doi: 10.1093/bmb/64.1.127. [DOI] [PubMed] [Google Scholar]
- 19.Mulier S, Ni Y, Jamart J, Michel L, Marchal G, Ruers T. Radiofrequency ablation versus resection for resectable colorectal liver metastases: time for a randomized trial? Ann Surg Oncol. 2008;15:144–157. doi: 10.1245/s10434-007-9478-5. [DOI] [PubMed] [Google Scholar]
- 20.Auer RC, White RR, Kemeny NE, Schwartz LH, Shia J, Blumgart LH, et al. Predictors of a true complete response among disappearing liver metastases from colorectal cancer after chemotherapy. Cancer. 2010;116:1502–1509. doi: 10.1002/cncr.24912. [DOI] [PubMed] [Google Scholar]
- 21.Ferrero A, Langella S, Russolillo N, Vigano L, Lo Tesoriere R, Capussotti L. Intraoperative detection of disappearing colorectal liver metastases as a predictor of residual disease. J Gastrointest Surg. 2012;16:806–814. doi: 10.1007/s11605-011-1810-5. [DOI] [PubMed] [Google Scholar]
- 22.Yuen MF, Hou JL, Chutaputti A, Asia Pacific Working Party on Prevention of Hepatocellular Carcinoma Hepatocellular carcinoma in the Asia pacific region. J Gastroenterol Hepatol. 2009;24:346–353. doi: 10.1111/j.1440-1746.2009.05784.x. [DOI] [PubMed] [Google Scholar]
- 23.Nagaoki Y, Hyogo H, Aikata H, Tanaka M, Naeshiro N, Nakahara T, et al. Recent trend of clinical features in patients with hepatocellular carcinoma. Hepatol Res. 2012;42:368–375. doi: 10.1111/j.1872-034X.2011.00929.x. [DOI] [PubMed] [Google Scholar]
- 24.Kaibori M, Matsui Y, Kitade H, Kwon AH, Kamiyama Y. Hepatic resection for hepatocellular carcinoma in severely cirrhotic livers. Hepatogastroenterology. 2003;50:491–496. [PubMed] [Google Scholar]
- 25.Lin XJ, Yang J, Chen XB, Zhang M, Xu MQ. The critical value of remnant liver volume-to-body weight ratio to estimate posthepatectomy liver failure in cirrhotic patients. J Surg Res. 2014;188:489–495. doi: 10.1016/j.jss.2014.01.023. [DOI] [PubMed] [Google Scholar]
- 26.Ezaki T, Yamamoto K, Yamaguchi H, Sasaki Y, Ishida T, Mori M, et al. Hepatic resection for hepatocellular carcinoma existing with liver cirrhosis. Hepatogastroenterology. 2002;49:1363–1368. [PubMed] [Google Scholar]
- 27.Joo I, Choi BI. New paradigm for management of hepatocellular carcinoma by imaging. Liver Cancer. 2012;1:94–109. doi: 10.1159/000342404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Lu Q, Luo Y, Yuan CX, Zeng Y, Wu H, Lei Z, et al. Value of contrastenhanced intraoperative ultrasound for cirrhotic patients with hepatocellular carcinoma: a report of 20 cases. World J Gastroenterol. 2008;14:4005–4010. doi: 10.3748/wjg.14.4005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Arita J, Takahashi M, Hata S, Shindoh J, Beck Y, Sugawara Y, et al. Usefulness of contrast-enhanced intraoperative ultrasound using Sonazoid in patients with hepatocellular carcinoma. Ann Surg. 2011;254:992–999. doi: 10.1097/SLA.0b013e31822518be. [DOI] [PubMed] [Google Scholar]
- 30.Torzilli G, Palmisano A, Del Fabbro D, Marconi M, Donadon M, Spinelli A, et al. Contrast-enhanced intraoperative ultrasonography during surgery for hepatocellular carcinoma in liver cirrhosis: is it useful or useless? A prospective cohort study of our experience. Ann Surg Oncol. 2007;14:1347–1355. doi: 10.1245/s10434-006-9278-3. [DOI] [PubMed] [Google Scholar]
- 31.Jarnagin WR, Bach AM, Winston CB, Hann LE, Heffernan N, Loumeau T, et al. What is the yield of intraoperative ultrasonography during partial hepatectomy for malignant disease? J Am Coll Surg. 2001;192:577–583. doi: 10.1016/s1072-7515(01)00794-3. [DOI] [PubMed] [Google Scholar]
- 32.Wagnetz U, Atri M, Massey C, Wei AC, Metser U. Intraoperative ultrasound of the liver in primary and secondary hepatic malignancies: comparison with preoperative 1.5-T MRI and 64-MDCT. AJR Am J Roentgenol. 2011;196:562–568. doi: 10.2214/AJR.10.4729. [DOI] [PubMed] [Google Scholar]
- 33.Conlon R, Jacobs M, Dasgupta D, Lodge JP. The value of intraoperative ultrasound during hepatic resection compared with improved preoperative magnetic resonance imaging. Eur J Ultrasound. 2003;16:211–216. doi: 10.1016/s0929-8266(02)00075-7. [DOI] [PubMed] [Google Scholar]
- 34.D'Hondt M, Vandenbroucke-Menu F, Preville-Ratelle S, Turcotte S, Chagnon M, Plasse M, et al. Is intra-operative ultrasound still useful for the detection of a hepatic tumour in the era of modern pre-operative imaging? HPB (Oxford) 2011;13:665–669. doi: 10.1111/j.1477-2574.2011.00349.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Ferrero A, Langella S, Giuliante F, Vigano L, Vellone M, Zimmitti G, et al. Intraoperative liver ultrasound still affects surgical strategy for patients with colorectal metastases in the modern era. World J Surg. 2013;37:2655–2663. doi: 10.1007/s00268-013-2183-6. [DOI] [PubMed] [Google Scholar]
- 36.Kim SH, Kim SH, Lee J, Kim MJ, Jeon YH, Park Y, et al. Gadoxetic acid-enhanced MRI versus triple-phase MDCT for the preoperative detection of hepatocellular carcinoma. AJR Am J Roentgenol. 2009;192:1675–1681. doi: 10.2214/AJR.08.1262. [DOI] [PubMed] [Google Scholar]
- 37.Berger-Kulemann V, Schima W, Baroud S, Koelblinger C, Kaczirek K, Gruenberger T, et al. Gadoxetic acid-enhanced 3.0 T MR imaging versus multidetector-row CT in the detection of colorectal metastases in fatty liver using intraoperative ultrasound and histopathology as a standard of reference. Eur J Surg Oncol. 2012;38:670–676. doi: 10.1016/j.ejso.2012.05.004. [DOI] [PubMed] [Google Scholar]
- 38.Yu MH, Kim JH, Yoon JH, Kim HC, Chung JW, Han JK, et al. Small (</=1-cm) hepatocellular carcinoma: diagnostic performance and imaging features at gadoxetic acid-enhanced MR imaging. Radiology. 2014;271:748–760. doi: 10.1148/radiol.14131996. [DOI] [PubMed] [Google Scholar]
- 39.Scharitzer M, Ba-Ssalamah A, Ringl H, Kolblinger C, Grunberger T, Weber M, et al. Preoperative evaluation of colorectal liver metastases: comparison between gadoxetic acid-enhanced 3.0-T MRI and contrast-enhanced MDCT with histopathological correlation. Eur Radiol. 2013;23:2187–2196. doi: 10.1007/s00330-013-2824-z. [DOI] [PubMed] [Google Scholar]
- 40.Koh DM, Collins DJ, Wallace T, Chau I, Riddell AM. Combining diffusion-weighted MRI with Gd-EOB-DTPA-enhanced MRI improves the detection of colorectal liver metastases. Br J Radiol. 2012;85:980–989. doi: 10.1259/bjr/91771639. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Xu PJ, Yan FH, Wang JH, Lin J, Ji Y. Added value of breathhold diffusion-weighted MRI in detection of small hepatocellular carcinoma lesions compared with dynamic contrast-enhanced MRI alone using receiver operating characteristic curve analysis. J Magn Reson Imaging. 2009;29:341–349. doi: 10.1002/jmri.21650. [DOI] [PubMed] [Google Scholar]
- 42.Sahani DV, Kalva SP, Tanabe KK, Hayat SM, O'Neill MJ, Halpern EF, et al. Intraoperative US in patients undergoing surgery for liver neoplasms: comparison with MR imaging. Radiology. 2004;232:810–814. doi: 10.1148/radiol.2323030896. [DOI] [PubMed] [Google Scholar]
- 43.Kartalis N, Brismar TB, Mihocsa L, Isaksson B, Albiin N. The added value of contrast-enhanced ultrasound in patients with colorectal cancer undergoing preoperative evaluation with extensive gadobenate dimeglumine liver MRI. Eur Radiol. 2011;21:2067–2073. doi: 10.1007/s00330-011-2156-9. [DOI] [PubMed] [Google Scholar]
- 44.Seidenfeld J, Korn A, Aronson N. Radiofrequency ablation of unresectable liver metastases. J Am Coll Surg. 2002;195:378–386. doi: 10.1016/s1072-7515(02)01247-4. [DOI] [PubMed] [Google Scholar]
- 45.Curley SA, Marra P, Beaty K, Ellis LM, Vauthey JN, Abdalla EK, et al. Early and late complications after radiofrequency ablation of malignant liver tumors in 608 patients. Ann Surg. 2004;239:450–458. doi: 10.1097/01.sla.0000118373.31781.f2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Chung YE, Kim KW. Contrast-enhanced ultrasonography: advance and current status in abdominal imaging. Ultrasonography. 2015;34:3–18. doi: 10.14366/usg.14034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Piscaglia F, Lencioni R, Sagrini E, Pina CD, Cioni D, Vidili G, et al. Characterization of focal liver lesions with contrast-enhanced ultrasound. Ultrasound Med Biol. 2010;36:531–550. doi: 10.1016/j.ultrasmedbio.2010.01.004. [DOI] [PubMed] [Google Scholar]
- 48.Lencioni R. European Federation of Societies for Ultrasound in Medicine and Biology (EFSUMB) guidelines for the use of contrast agents in liver ultrasound: what is the impact in clinical practice? Eur Radiol. 2005;15 Suppl 5:E983–E103. doi: 10.1007/s10406-005-0171-0. [DOI] [PubMed] [Google Scholar]
- 49.Goto E, Masuzaki R, Tateishi R, Kondo Y, Imamura J, Goto T, et al. Value of post-vascular phase (Kupffer imaging) by contrastenhanced ultrasonography using Sonazoid in the detection of hepatocellular carcinoma. J Gastroenterol. 2012;47:477–485. doi: 10.1007/s00535-011-0512-9. [DOI] [PubMed] [Google Scholar]
- 50.Hatanaka K, Kudo M, Minami Y, Maekawa K. Sonazoid-enhanced ultrasonography for diagnosis of hepatic malignancies: comparison with contrast-enhanced CT. Oncology. 2008;75 Suppl 1:42–47. doi: 10.1159/000173423. [DOI] [PubMed] [Google Scholar]
- 51.Nakano H, Ishida Y, Hatakeyama T, Sakuraba K, Hayashi M, Sakurai O, et al. Contrast-enhanced intraoperative ultrasonography equipped with late Kupffer-phase image obtained by sonazoid in patients with colorectal liver metastases. World J Gastroenterol. 2008;14:3207–3211. doi: 10.3748/wjg.14.3207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Torzilli G. Contrast-enhanced intraoperative ultrasonography in surgery for liver tumors. Eur J Radiol. 2004;51 Suppl:S25–S29. doi: 10.1016/j.ejrad.2004.03.025. [DOI] [PubMed] [Google Scholar]
- 53.Leen E, Ceccotti P, Moug SJ, Glen P, MacQuarrie J, Angerson WJ, et al. Potential value of contrast-enhanced intraoperative ultrasonography during partial hepatectomy for metastases: an essential investigation before resection? Ann Surg. 2006;243:236–240. doi: 10.1097/01.sla.0000197708.77063.07. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Xu LH, Cai SJ, Cai GX, Peng WJ. Imaging diagnosis of colorectal liver metastases. World J Gastroenterol. 2011;17:4654–4659. doi: 10.3748/wjg.v17.i42.4654. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Takahashi M, Hasegawa K, Arita J, Hata S, Aoki T, Sakamoto Y, et al. Contrast-enhanced intraoperative ultrasonography using perfluorobutane microbubbles for the enumeration of colorectal liver metastases. Br J Surg. 2012;99:1271–1277. doi: 10.1002/bjs.8844. [DOI] [PubMed] [Google Scholar]
- 56.Shah AJ, Callaway M, Thomas MG, Finch-Jones MD. Contrastenhanced intraoperative ultrasound improves detection of liver metastases during surgery for primary colorectal cancer. HPB (Oxford) 2010;12:181–187. doi: 10.1111/j.1477-2574.2009.00141.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Cervone A, Sardi A, Conaway GL. Intraoperative ultrasound (IOUS) is essential in the management of metastatic colorectal liver lesions. Am Surg. 2000;66:611–615. [PubMed] [Google Scholar]
- 58.Zendel A, Lahat E, Dreznik Y, Zakai BB, Eshkenazy R, Ariche A. "Vanishing liver metastases"-A real challenge for liver surgeons. Hepatobiliary Surg Nutr. 2014;3:295–302. doi: 10.3978/j.issn.2304-3881.2014.09.13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Ruzzenente A, Conci S, Iacono C, Valdegamberi A, Campagnaro T, Bertuzzo F, et al. Usefulness of contrast-enhanced intraoperative ultrasonography (CE-IOUS) in patients with colorectal liver metastases after preoperative chemotherapy. J Gastrointest Surg. 2013;17:281–287. doi: 10.1007/s11605-012-2043-y. [DOI] [PubMed] [Google Scholar]
- 60.Arita J, Ono Y, Takahashi M, Inoue Y, Takahashi Y, Saiura A. Usefulness of contrast-enhanced intraoperative ultrasound in identifying disappearing liver metastases from colorectal carcinoma after chemotherapy. Ann Surg Oncol. 2014;21 Suppl 3:S390–S397. doi: 10.1245/s10434-014-3576-y. [DOI] [PubMed] [Google Scholar]
- 61.Arita J, Hasegawa K, Takahashi M, Hata S, Shindoh J, Sugawara Y, et al. Correlation between contrast-enhanced intraoperative ultrasound using Sonazoid and histologic grade of resected hepatocellular carcinoma. AJR Am J Roentgenol. 2011;196:1314–1321. doi: 10.2214/AJR.10.4310. [DOI] [PubMed] [Google Scholar]
- 62.Sato K, Tanaka S, Mitsunori Y, Mogushi K, Yasen M, Aihara A, et al. Contrast-enhanced intraoperative ultrasonography for vascular imaging of hepatocellular carcinoma: clinical and biological significance. Hepatology. 2013;57:1436–1447. doi: 10.1002/hep.26122. [DOI] [PubMed] [Google Scholar]
- 63.Kim HO, Kim SK, Son BH, Yoo CH, Hong HP, Cho YK, et al. Intraoperative radiofrequency ablation with or without tumorectomy for hepatocellular carcinoma in locations difficult for a percutaneous approach. Hepatobiliary Pancreat Dis Int. 2009;8:591–596. [PubMed] [Google Scholar]
- 64.Crucitti A, Danza FM, Antinori A, Vincenzo A, Pirulli PG, Bock E, et al. Radiofrequency thermal ablation (RFA) of liver tumors: percutaneous and open surgical approaches. J Exp Clin Cancer Res. 2003;22(4 Suppl):191–195. [PubMed] [Google Scholar]
- 65.Mortensen MB, Fristrup C, Ainsworth A, Pless T, Larsen M, Nielsen H, et al. Laparoscopic ultrasound-guided biopsy in upper gastrointestinal tract cancer patients. Surg Endosc. 2009;23:2738–2742. doi: 10.1007/s00464-009-0481-8. [DOI] [PubMed] [Google Scholar]
- 66.Koda M, Murawaki Y, Mitsuda A, Oyama K, Okamoto K, Idobe Y, et al. Combination therapy with transcatheter arterial chemoembolization and percutaneous ethanol injection compared with percutaneous ethanol injection alone for patients with small hepatocellular carcinoma: a randomized control study. Cancer. 2001;92:1516–1524. doi: 10.1002/1097-0142(20010915)92:6<1516::aid-cncr1477>3.0.co;2-i. [DOI] [PubMed] [Google Scholar]
- 67.Kim YS, Rhim H, Lim HK, Choi D, Lee MW, Park MJ. Coagulation necrosis induced by radiofrequency ablation in the liver: histopathologic and radiologic review of usual to extremely rare changes. Radiographics. 2011;31:377–390. doi: 10.1148/rg.312105056. [DOI] [PubMed] [Google Scholar]
- 68.Iannitti DA, Martin RC, Simon CJ, Hope WW, Newcomb WL, McMasters KM, et al. Hepatic tumor ablation with clustered microwave antennae: the US Phase II trial. HPB (Oxford) 2007;9:120–124. doi: 10.1080/13651820701222677. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Howard JH, Tzeng CW, Smith JK, Eckhoff DE, Bynon JS, Wang T, et al. Radiofrequency ablation for unresectable tumors of the liver. Am Surg. 2008;74:594–600. [PubMed] [Google Scholar]
- 70.Machi J, Uchida S, Sumida K, Limm WM, Hundahl SA, Oishi AJ, et al. Ultrasound-guided radiofrequency thermal ablation of liver tumors: percutaneous, laparoscopic, and open surgical approaches. J Gastrointest Surg. 2001;5:477–489. doi: 10.1016/s1091-255x(01)80085-8. [DOI] [PubMed] [Google Scholar]
- 71.Ishiko T, Beppu T, Sugiyama S, Masuda T, Takahashi M, Komori H, et al. Radiofrequency ablation with hand-assisted laparoscopic surgery for the treatment of hepatocellular carcinoma in the caudate lobe. Surg Laparosc Endosc Percutan Tech. 2008;18:272–276. doi: 10.1097/SLE.0b013e31816a24bf. [DOI] [PubMed] [Google Scholar]
- 72.El-Gendi A, El-Shafei M, Abdel-Aziz F, Bedewy E. Intraoperative ablation for small HCC not amenable for percutaneous radiofrequency ablation in Child A cirrhotic patients. J Gastrointest Surg. 2013;17:712–718. doi: 10.1007/s11605-012-2085-1. [DOI] [PubMed] [Google Scholar]
- 73.Razafindratsira T, Isambert M, Evrard S. Complications of intraoperative radiofrequency ablation of liver metastases. HPB (Oxford) 2011;13:15–23. doi: 10.1111/j.1477-2574.2010.00243.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Park IJ, Kim HC, Yu CS, Kim PN, Won HJ, Kim JC. Radiofrequency ablation for metachronous liver metastasis from colorectal cancer after curative surgery. Ann Surg Oncol. 2008;15:227–232. doi: 10.1245/s10434-007-9625-z. [DOI] [PubMed] [Google Scholar]
- 75.Cheung TT, Ng KK, Chok KS, Chan SC, Poon RT, Lo CM, et al. Combined resection and radiofrequency ablation for multifocal hepatocellular carcinoma: prognosis and outcomes. World J Gastroenterol. 2010;16:3056–3062. doi: 10.3748/wjg.v16.i24.3056. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Leblanc F, Fonck M, Brunet R, Becouarn Y, Mathoulin-Pelissier S, Evrard S. Comparison of hepatic recurrences after resection or intraoperative radiofrequency ablation indicated by size and topographical characteristics of the metastases. Eur J Surg Oncol. 2008;34:185–190. doi: 10.1016/j.ejso.2007.09.028. [DOI] [PubMed] [Google Scholar]
- 77.Eng OS, Tsang AT, Moore D, Chen C, Narayanan S, Gannon CJ, et al. Outcomes of microwave ablation for colorectal cancer liver metastases: a single center experience. J Surg Oncol. 2015;111:410–413. doi: 10.1002/jso.23849. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Stattner S, Jones RP, Yip VS, Buchanan K, Poston GJ, Malik HZ, et al. Microwave ablation with or without resection for colorectal liver metastases. Eur J Surg Oncol. 2013;39:844–849. doi: 10.1016/j.ejso.2013.04.005. [DOI] [PubMed] [Google Scholar]
- 79.Jiang K, Zhang W, Su M, Liu Y, Zhao X, Wang J, et al. Laparoscopic radiofrequency ablation of solitary small hepatocellular carcinoma in the caudate lobe. Eur J Surg Oncol. 2013;39:1236–1242. doi: 10.1016/j.ejso.2013.08.002. [DOI] [PubMed] [Google Scholar]
- 80.Simo KA, Sereika SE, Newton KN, Gerber DA. Laparoscopic-assisted microwave ablation for hepatocellular carcinoma: safety and efficacy in comparison with radiofrequency ablation. J Surg Oncol. 2011;104:822–829. doi: 10.1002/jso.21933. [DOI] [PubMed] [Google Scholar]
- 81.Guibal A, Boularan C, Bruce M, Vallin M, Pilleul F, Walter T, et al. Evaluation of shearwave elastography for the characterisation of focal liver lesions on ultrasound. Eur Radiol. 2013;23:1138–1149. doi: 10.1007/s00330-012-2692-y. [DOI] [PubMed] [Google Scholar]
- 82.Cho SH, Lee JY, Han JK, Choi BI. Acoustic radiation force impulse elastography for the evaluation of focal solid hepatic lesions: preliminary findings. Ultrasound Med Biol. 2010;36:202–208. doi: 10.1016/j.ultrasmedbio.2009.10.009. [DOI] [PubMed] [Google Scholar]
- 83.Kim JE, Lee JY, Bae KS, Han JK, Choi BI. Acoustic radiation force impulse elastography for focal hepatic tumors: usefulness for differentiating hemangiomas from malignant tumors. Korean J Radiol. 2013;14:743–753. doi: 10.3348/kjr.2013.14.5.743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Omichi K, Inoue Y, Hasegawa K, Sakamoto Y, Okinaga H, Aoki T, et al. Differential diagnosis of liver tumours using intraoperative real-time tissue elastography. Br J Surg. 2015;102:246–253. doi: 10.1002/bjs.9728. [DOI] [PubMed] [Google Scholar]
- 85.Inoue Y, Takahashi M, Arita J, Aoki T, Hasegawa K, Beck Y, et al. Intra-operative freehand real-time elastography for small focal liver lesions: "visual palpation" for non-palpable tumors. Surgery. 2010;148:1000–1011. doi: 10.1016/j.surg.2010.02.009. [DOI] [PubMed] [Google Scholar]
- 86.Kato K, Sugimoto H, Kanazumi N, Nomoto S, Takeda S, Nakao A. Intra-operative application of real-time tissue elastography for the diagnosis of liver tumours. Liver Int. 2008;28:1264–1271. doi: 10.1111/j.1478-3231.2008.01701.x. [DOI] [PubMed] [Google Scholar]
- 87.Mariani A, Kwiecinski W, Pernot M, Balvay D, Tanter M, Clement O, et al. Real time shear waves elastography monitoring of thermal ablation: in vivo evaluation in pig livers. J Surg Res. 2014;188:37–43. doi: 10.1016/j.jss.2013.12.024. [DOI] [PubMed] [Google Scholar]
- 88.Correa-Gallego C, Karkar AM, Monette S, Ezell PC, Jarnagin WR, Kingham TP. Intraoperative ultrasound and tissue elastography measurements do not predict the size of hepatic microwave ablations. Acad Radiol. 2014;21:72–78. doi: 10.1016/j.acra.2013.09.022. [DOI] [PubMed] [Google Scholar]
- 89.Van Vledder MG, Boctor EM, Assumpcao LR, Rivaz H, Foroughi P, Hager GD, et al. Intra-operative ultrasound elasticity imaging for monitoring of hepatic tumour thermal ablation. HPB (Oxford) 2010;12:717–723. doi: 10.1111/j.1477-2574.2010.00247.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Numminen K, Sipila O, Makisalo H. Preoperative hepatic 3D models: virtual liver resection using three-dimensional imaging technique. Eur J Radiol. 2005;56:179–184. doi: 10.1016/j.ejrad.2005.03.021. [DOI] [PubMed] [Google Scholar]
- 91.Heizmann O, Zidowitz S, Bourquain H, Potthast S, Peitgen HO, Oertli D, et al. Assessment of intraoperative liver deformation during hepatic resection: prospective clinical study. World J Surg. 2010;34:1887–1893. doi: 10.1007/s00268-010-0561-x. [DOI] [PubMed] [Google Scholar]
- 92.Beller S, Hunerbein M, Eulenstein S, Lange T, Schlag PM. Feasibility of navigated resection of liver tumors using multiplanar visualization of intraoperative 3-dimensional ultrasound data. Ann Surg. 2007;246:288–294. doi: 10.1097/01.sla.0000264233.48306.99. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Lango T, Vijayan S, Rethy A, Vapenstad C, Solberg OV, Marvik R, et al. Navigated laparoscopic ultrasound in abdominal soft tissue surgery: technological overview and perspectives. Int J Comput Assist Radiol Surg. 2012;7:585–599. doi: 10.1007/s11548-011-0656-3. [DOI] [PubMed] [Google Scholar]
- 94.Harms J, Feussner H, Baumgartner M, Schneider A, Donhauser M, Wessels G. Three-dimensional navigated laparoscopic ultrasonography: first experiences with a new minimally invasive diagnostic device. Surg Endosc. 2001;15:1459–1462. doi: 10.1007/s004640090071. [DOI] [PubMed] [Google Scholar]
- 95.Beller S, Hunerbein M, Lange T, Eulenstein S, Gebauer B, Schlag PM. Image-guided surgery of liver metastases by threedimensional ultrasound-based optoelectronic navigation. Br J Surg. 2007;94:866–875. doi: 10.1002/bjs.5712. [DOI] [PubMed] [Google Scholar]


